A New Anorganic Equine Bone Substitute for Oral Surgery: Structural Characterization and Regenerative Potential
Abstract
:1. Introduction
2. Materials and Methods
2.1. Materials
2.2. Physicochemical and Morphological Characterization
2.3. Animals
2.4. Study Protocol and Randomization
2.5. Grafting Surgical Procedure
2.6. Sampling and Histological Preparation
2.7. Histological Measurements
2.8. Statistical Analysis of Cellular Content of Histological Samples
3. Results
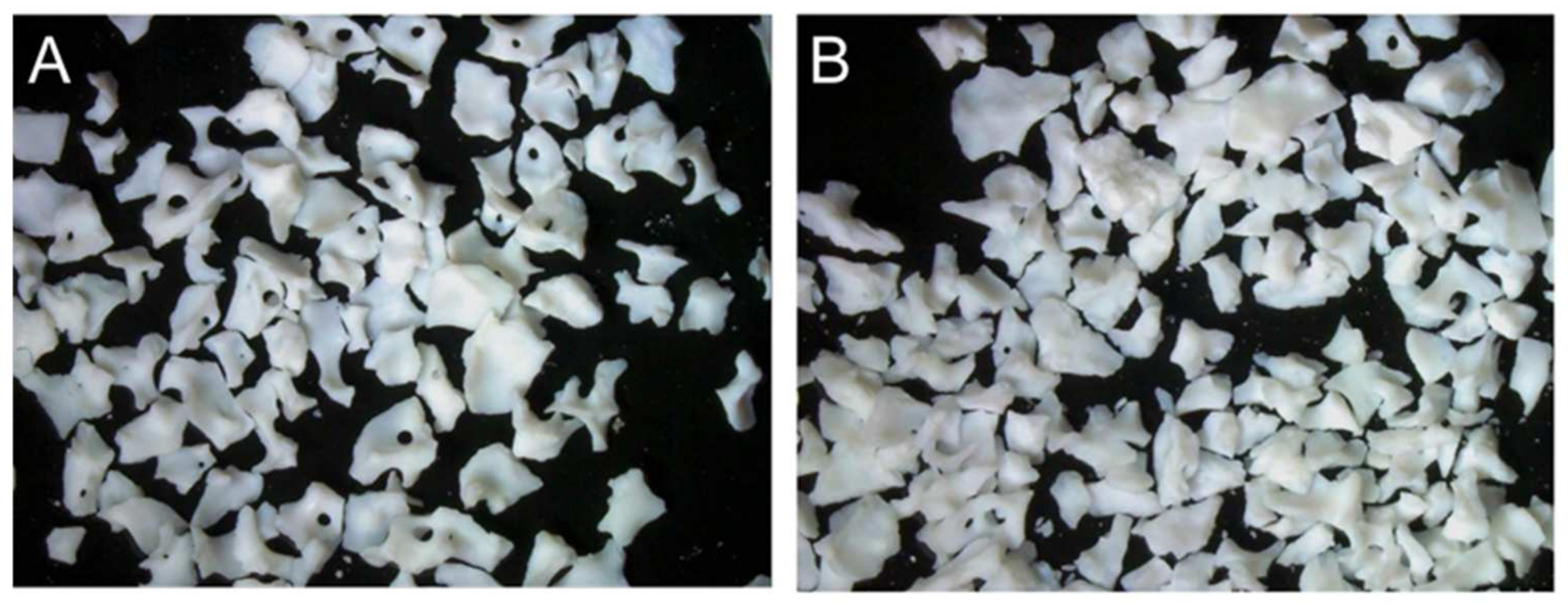
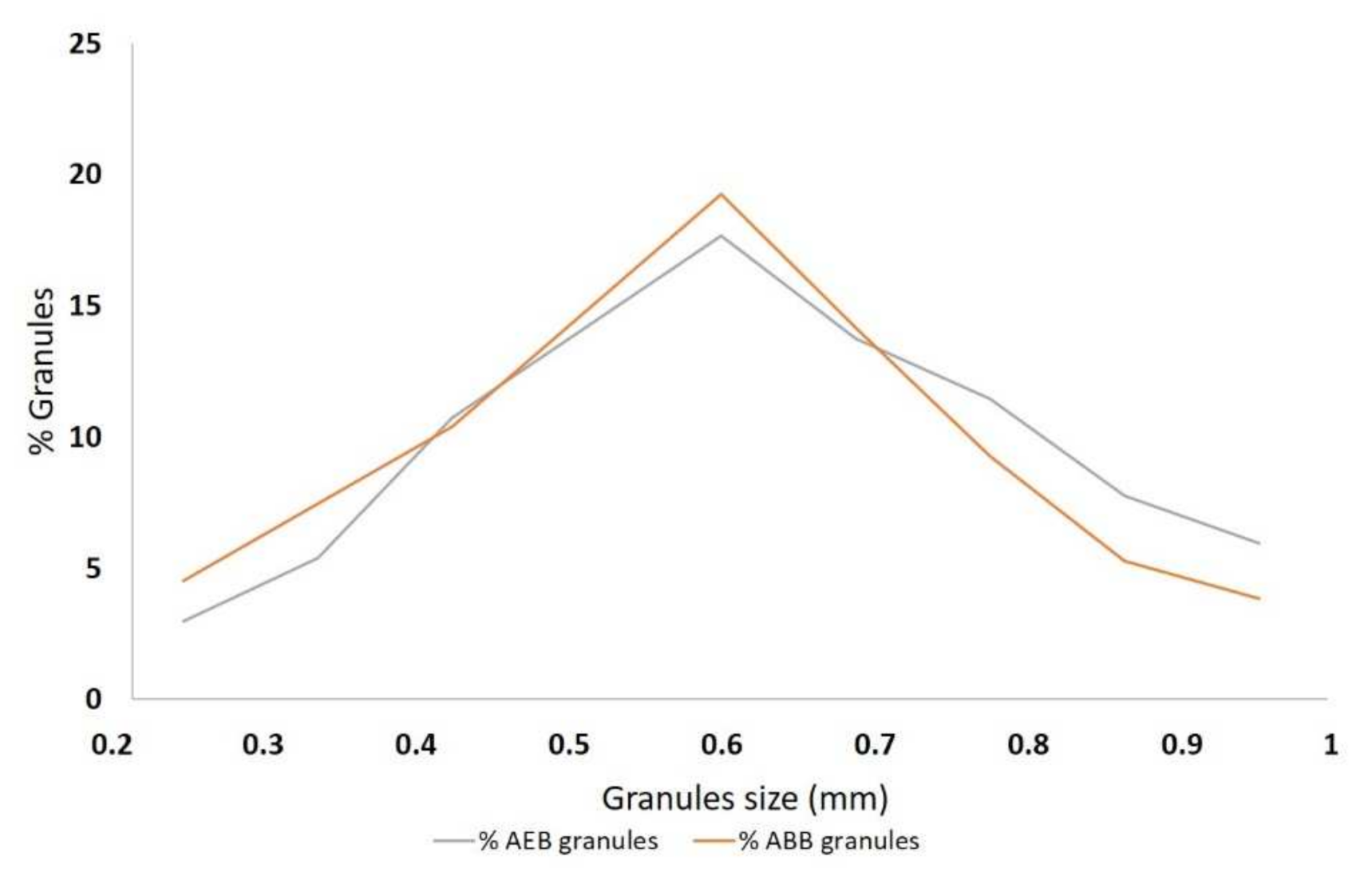
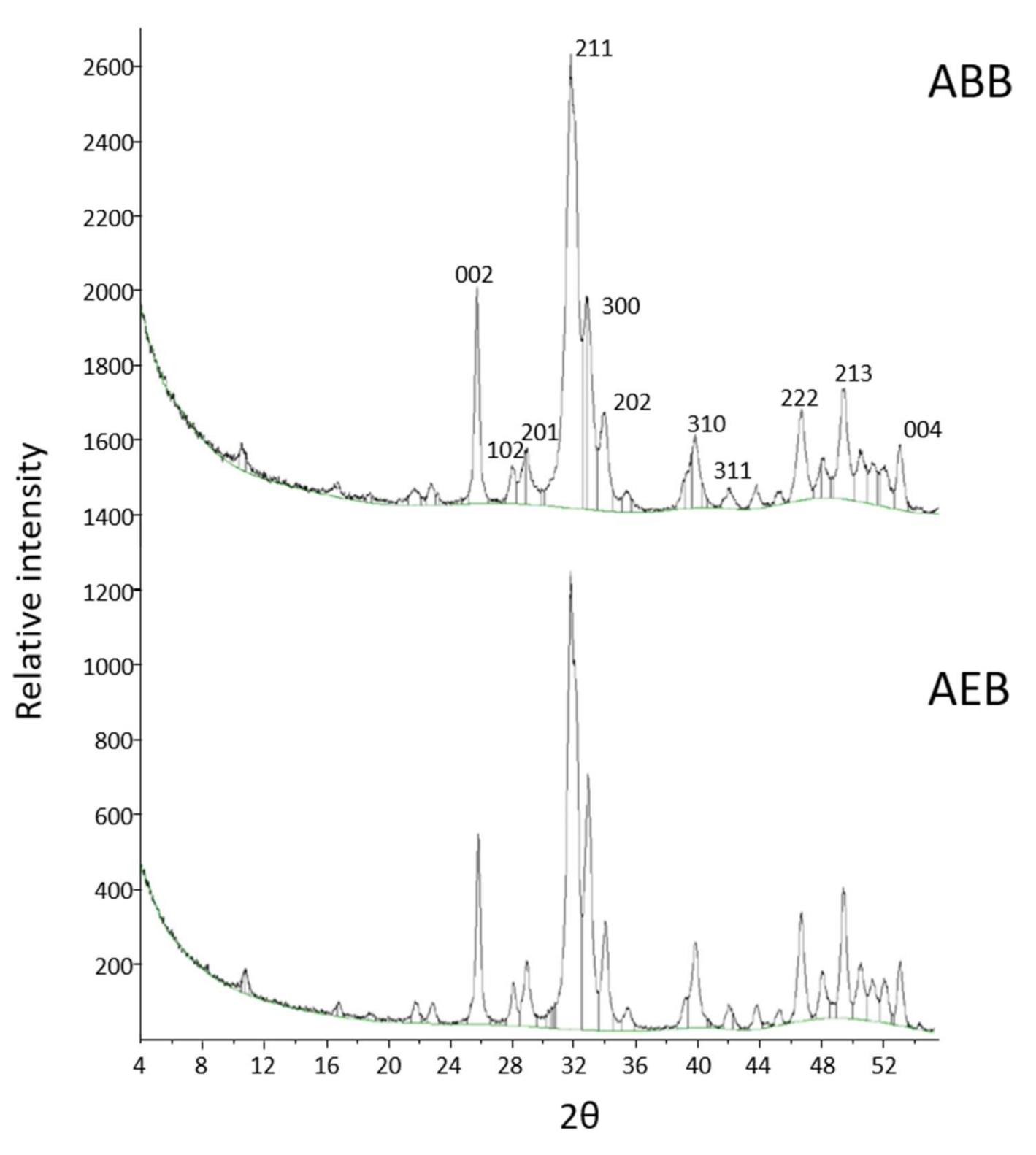
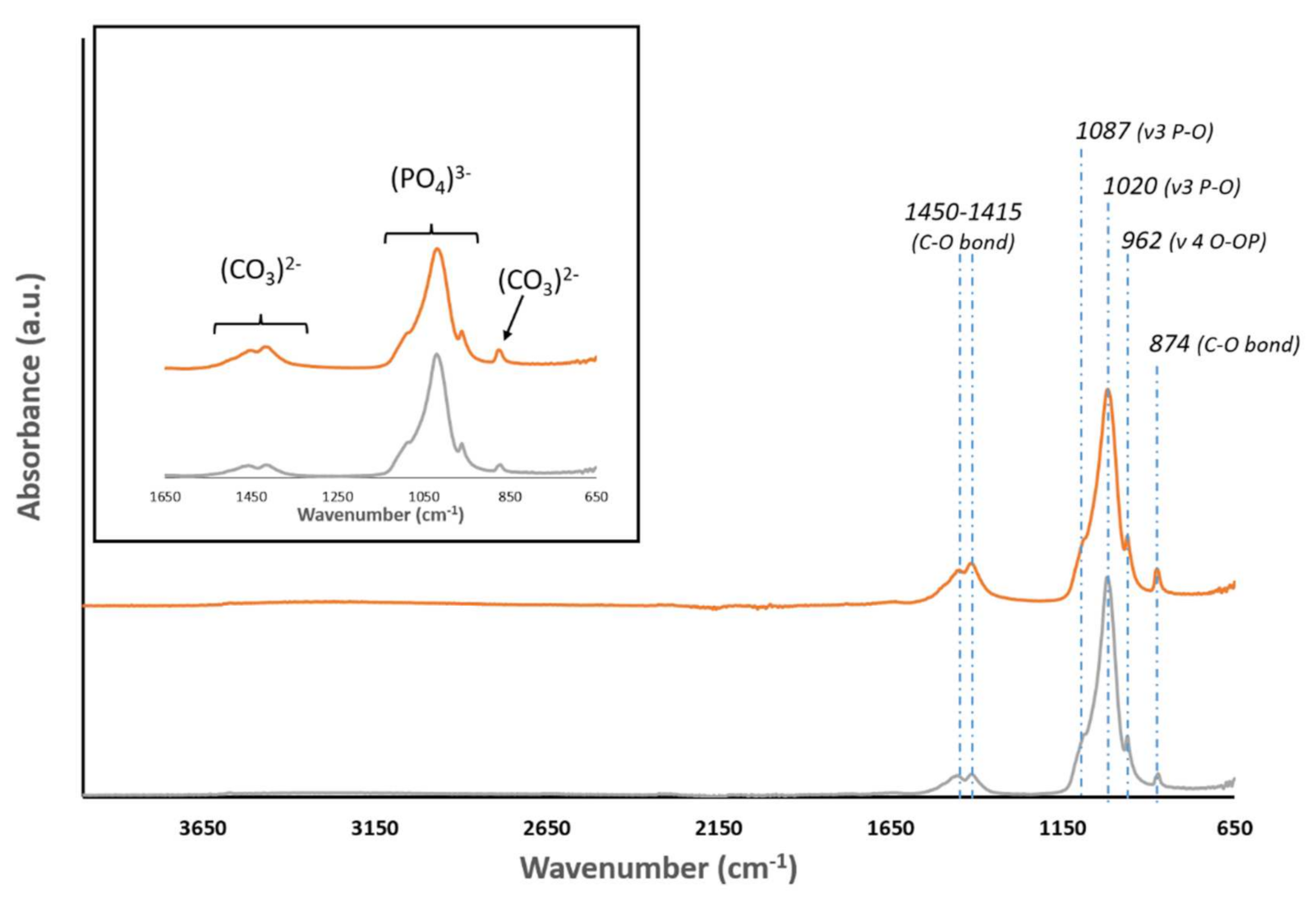
3.1. Physicochemical and Morphological Characterization of AEB
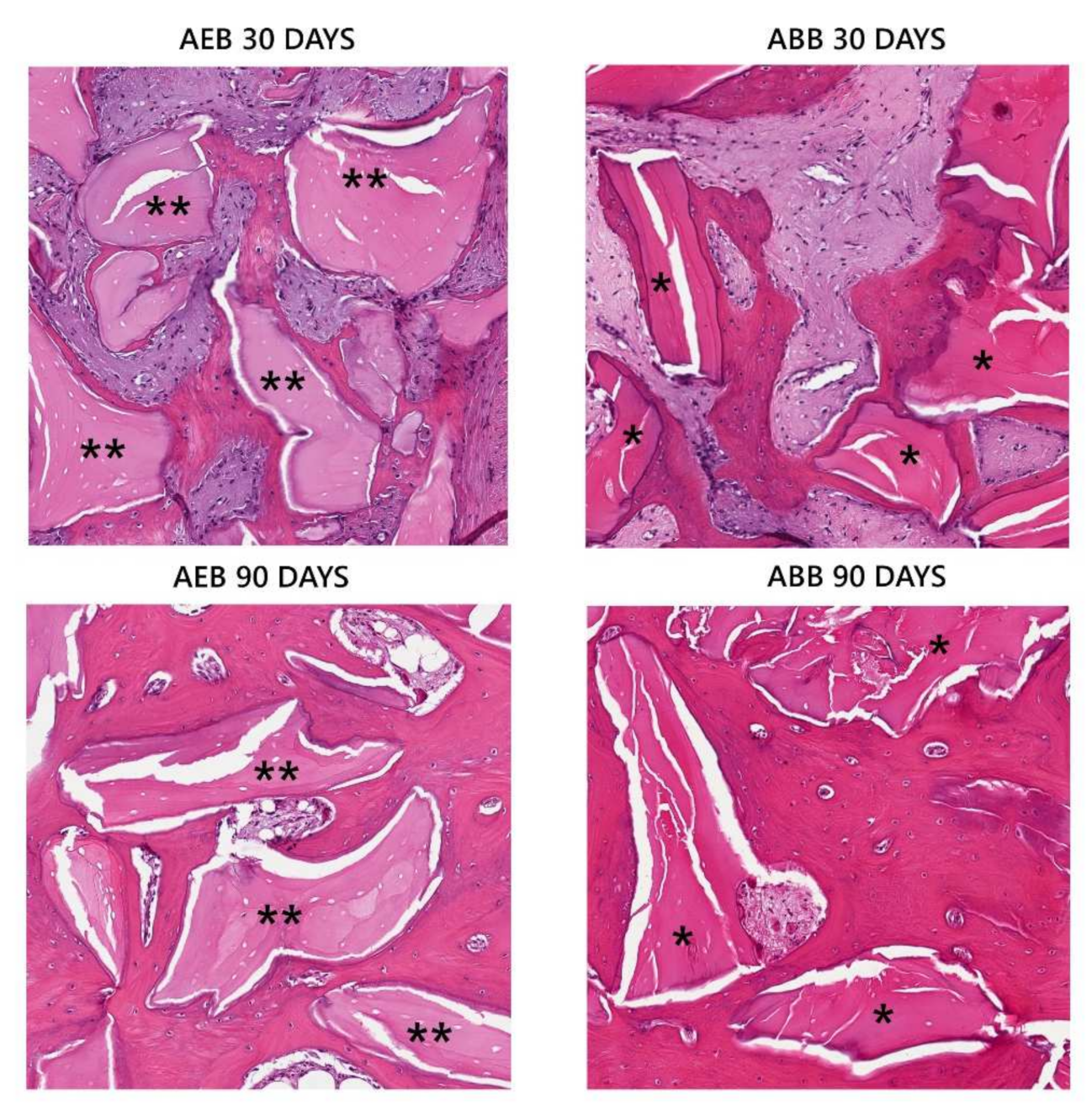
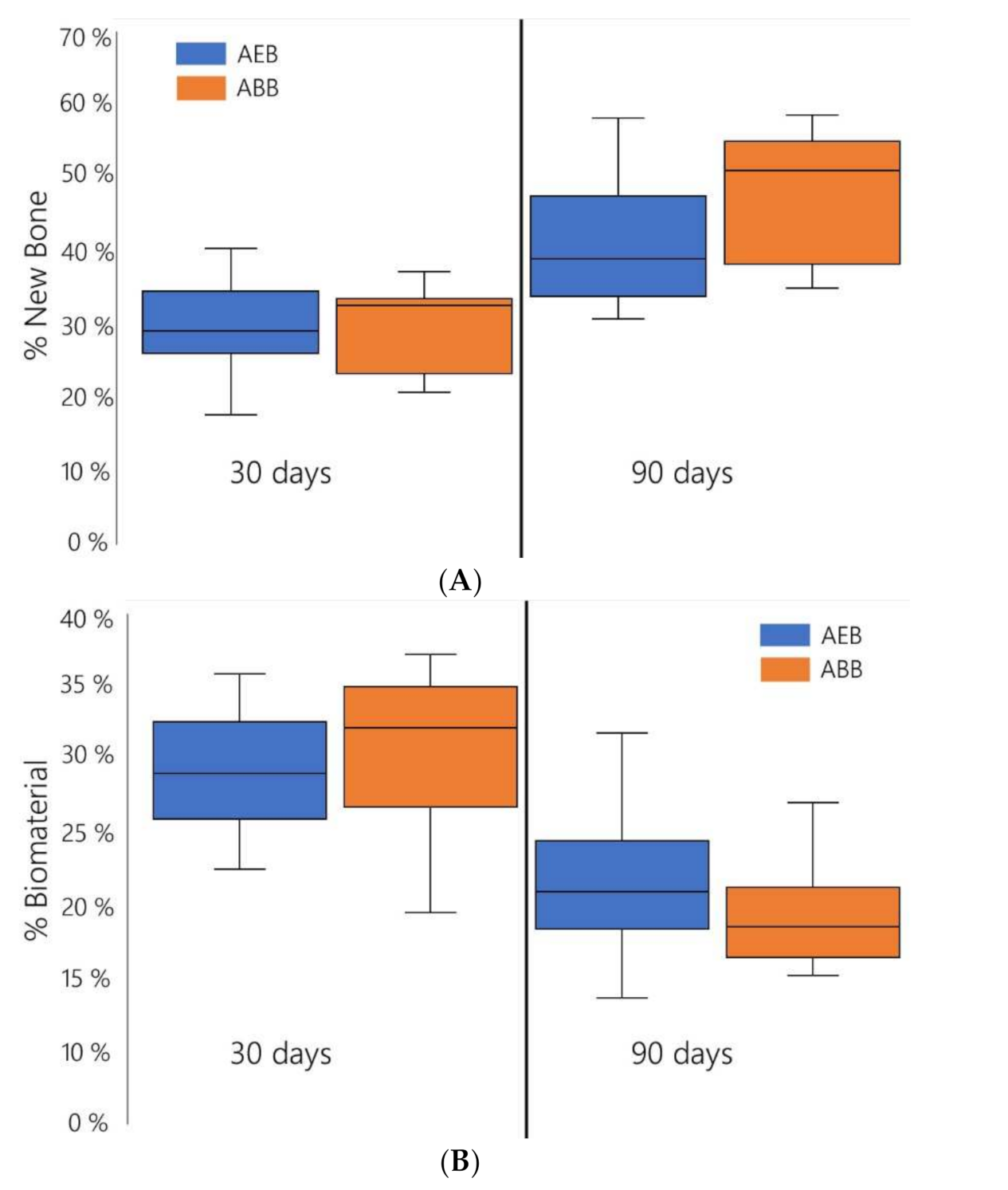
3.2. Resorption, New Bone Formation, and Local Effects after Implantation of AEB and ABB in an Animal Model
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Data Availability Statement
Conflicts of Interest
References
- Zizzari, V.L.; Zara, S.; Tete, G.; Vinci, R.; Gherlone, E.; Cataldi, A. Biologic and clinical aspects of integration of different bone substitutes in oral surgery: A literature review. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 2016, 122, 392–402. [Google Scholar] [CrossRef] [PubMed]
- Misch, C.M. Maxillary autogenous bone grafting. Oral Maxillofac. Surg. Clin. N. Am. 2011, 23, 229–238. [Google Scholar] [CrossRef] [PubMed]
- Perrotti, V.; Nicholls, B.M.; Horton, M.A.; Piattelli, A. Human osteoclast formation and activity on a xenogenous bone mineral. J. Biomed. Mater. Res. Part A 2009, 90, 238–246. [Google Scholar] [CrossRef] [PubMed]
- Russmueller, G.; Winkler, L.; Lieber, R.; Seemann, R.; Pirklbauer, K.; Perisanidis, C.; Kapeller, B.; Spassova, E.; Halwax, E.; Poeschl, W.P.; et al. In Vitro effects of particulate bone substitute materials on the resorption activity of human osteoclasts. Eur. Cells Mater. 2017, 34, 291–306. [Google Scholar] [CrossRef] [PubMed]
- Sakkas, A.; Wilde, F.; Heufelder, M.; Winter, K.; Schramm, A. Autogenous bone grafts in oral implantology-is it still a "gold standard"? A consecutive review of 279 patients with 456 clinical procedures. Int. J. Implant Dent. 2017, 3, 23. [Google Scholar] [CrossRef]
- Nkenke, E.; Weisbach, V.; Winckler, E.; Kessler, P.; Schultze-Mosgau, S.; Wiltfang, J.; Neukam, F.W. Morbidity of harvesting of bone grafts from the iliac crest for preprosthetic augmentation procedures: A prospective study. Int. J. Oral Maxillofac. Surg. 2004, 33, 157–163. [Google Scholar] [CrossRef]
- Baldini, N.; De Sanctis, M.; Ferrari, M. Deproteinized bovine bone in periodontal and implant surgery. Dent. Mater. 2011, 27, 61–70. [Google Scholar] [CrossRef]
- Thompson, T.J.U.; Gauthier, M.; Islam, M. Bone augmentation procedures in localized defects in the alveolar ridge: Clinical results with different bone grafts and bone-substitute materials. Int. J. Oral Maxillofac. Implant. 2009, 24, 218–236. [Google Scholar]
- Wozney, J.M. The bone morphogenetic protein family and osteogenesis. Mol. Reprod. Dev. 1992, 32, 160–167. [Google Scholar] [CrossRef]
- Richardson, C.R.; Mellonig, J.T.; Brunsvold, M.A.; McDonnell, H.T.; Cochran, D.L. Clinical evaluation of Bio-Oss: A bovine-derived xenograft for the treatment of periodontal osseous defects in humans. J. Clin. Periodontol. 1999, 26, 421–428. [Google Scholar] [CrossRef]
- Lee, J.H.; Yi, G.S.; Lee, J.W.; Kim, D.J. Physicochemical characterization of porcine bone-derived grafting material and comparison with bovine xenografts for dental applications. J. Periodontal Implant Sci. 2017, 47, 388–401. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Valentini, P.; Abensur, D. Maxillary sinus floor elevation for implant placement with demineralized freeze-dried bone and bovine bone (Bio-Oss): A clinical study of 20 patients. Int. J. Periodontics Restor. Dent. 1997, 17, 232–241. [Google Scholar]
- Peric Kacarevic, Z.; Kavehei, F.; Houshmand, A.; Franke, J.; Smeets, R.; Rimashevskiy, D.; Wenisch, S.; Schnettler, R.; Jung, O.; Barbeck, M. Purification processes of xenogeneic bone substitutes and their impact on tissue reactions and regeneration. Int. J. Artif. Organs 2018, 41, 789–800. [Google Scholar] [CrossRef] [PubMed]
- Carmagnola, D.; Adriaens, P.; Berglundh, T. Healing of human extraction sockets filled with Bio-Oss. Clin. Oral Implant. Res. 2003, 14, 137–143. [Google Scholar] [CrossRef] [PubMed]
- Duda, M.; Pajak, J. The issue of bioresorption of the Bio-Oss xenogeneic bone substitute in bone defects. Ann. Univ. Mariae Curie Sklodowska Med. 2004, 59, 269–277. [Google Scholar] [PubMed]
- Stavropoulos, A.; Karring, T. Guided tissue regeneration combined with a deproteinized bovine bone mineral (Bio-Oss) in the treatment of intrabony periodontal defects: 6-year results from a randomized-controlled clinical trial. J. Clin. Periodontol. 2010, 37, 200–210. [Google Scholar] [CrossRef] [PubMed]
- Aludden, H.C.; Mordenfeld, A.; Hallman, M.; Dahlin, C.; Jensen, T. Lateral ridge augmentation with Bio-Oss alone or Bio-Oss mixed with particulate autogenous bone graft: A systematic review. Int. J. Oral Maxillofac. Surg. 2017, 46, 1030–1038. [Google Scholar] [CrossRef]
- Starch-Jensen, T.; Aludden, H.; Hallman, M.; Dahlin, C.; Christensen, A.E.; Mordenfeld, A. A systematic review and meta-analysis of long-term studies (five or more years) assessing maxillary sinus floor augmentation. Int. J. Oral Maxillofac. Surg. 2018, 47, 103–116. [Google Scholar] [CrossRef]
- Benke, D.; Olah, A.; Mohler, H. Protein-chemical analysis of Bio-Oss bone substitute and evidence on its carbonate content. Biomaterials 2001, 22, 1005–1012. [Google Scholar] [CrossRef]
- Orsini, G.; Traini, T.; Scarano, A.; Degidi, M.; Perrotti, V.; Piccirilli, M.; Piattelli, A. Maxillary sinus augmentation with Bio-Oss particles: A light, scanning, and transmission electron microscopy study in man. J. Biomed. Mater. Res. Part B Appl. Biomater. 2005, 74, 448–457. [Google Scholar] [CrossRef]
- Degidi, M.; Artese, L.; Rubini, C.; Perrotti, V.; Iezzi, G.; Piattelli, A. Microvessel density and vascular endothelial growth factor expression in sinus augmentation using Bio-Oss. Oral Dis. 2006, 12, 469–475. [Google Scholar] [CrossRef] [PubMed]
- Berglundh, T.; Lindhe, J. Healing around implants placed in bone defects treated with Bio-Oss. An experimental study in the dog. Clin. Oral Implant. Res. 1997, 8, 117–124. [Google Scholar] [CrossRef] [PubMed]
- Skoglund, A.; Hising, P.; Young, C. A clinical and histologic examination in humans of the osseous response to implanted natural bone mineral. Int. J. Oral Maxillofac. Implant. 1997, 12, 194–199. [Google Scholar]
- Sartori, S.; Silvestri, M.; Forni, F.; Icaro Cornaglia, A.; Tesei, P.; Cattaneo, V. Ten-year follow-up in a maxillary sinus augmentation using anorganic bovine bone (Bio-Oss). A case report with histomorphometric evaluation. Clin. Oral Implant. Res. 2003, 14, 369–372. [Google Scholar] [CrossRef] [Green Version]
- Bedini, R.; Meleo, D.; Pecci, R. 3D microtomography characterization of dental implantology bone substitutes used in-vivo. Key Eng. Mater. 2013, 541, 97–113. [Google Scholar] [CrossRef]
- Bedini, R.; Pecci, R.; Meleo, D.; Campioni, I. Bone Substitutes Scaffold in Human Bone: Comparative Evaluation by 3D Micro-CT Technique. Appl. Sci. 2020, 10, 3451. [Google Scholar] [CrossRef]
- EU-REGULATION. COMMISSION REGULATION (EU) No 722/2012 of 8 August 2012 concerning particular requirements as regards the requirements laid down in Council Directives 90/385/EEC and 93/42/EEC with respect to active implantable medical devices and medical devices manufactured utilising tissues of animal origin (REGOLAMENTO N. 722/2012 DELLA COMMISSIONE EUROPEA dell’8 agosto 2012 relativo ai requisiti particolari per quanto riguarda i requisiti di cui alle direttive 90/385/CEE e 93/42/CEE del Consiglio per i dispositivi medici impiantabili attivi e i dispositivi medici fabbricati con tessuti d’origine animale). 2012, L 212, 3–12. Available online: https://eur-lex.europa.eu/LexUriServ/LexUriServ.do?uri=OJ:L:2012:212:0003:0012:en:PDF (accessed on 20 November 2021).
- Lovati, A.B.; Lopa, S.; Bottagisio, M.; Talo, G.; Canciani, E.; Dellavia, C.; Alessandrino, A.; Biagiotti, M.; Freddi, G.; Segatti, F.; et al. Peptide-Enriched Silk Fibroin Sponge and Trabecular Titanium Composites to Enhance Bone Ingrowth of Prosthetic Implants in an Ovine Model of Bone Gaps. Front. Bioeng. Biotechnol. 2020, 8, 563203. [Google Scholar] [CrossRef]
- Noguchi, K.; Gel, Y.R.; Brunner, E.; Konietschke, F. nparLD: An R Software Package for the Nonparametric Analysis of Longitudinal Data in Factorial Experiments. J. Stat. Softw. 2012, 50, 23. [Google Scholar] [CrossRef] [Green Version]
- Dumitrescu, C.R.; Neacsu, I.A.; Surdu, V.A.; Nicoara, A.I.; Iordache, F.; Trusca, R.; Ciocan, L.T.; Ficai, A.; Andronescu, E. Nano-Hydroxyapatite vs. Xenografts: Synthesis, Characterization, and In Vitro Behavior. Nanomaterials 2021, 11, 2289. [Google Scholar] [CrossRef]
- Sun, R.; Lv, Y.; Niu, Y.; Zhao, X.; Cao, D.; Tang, J.; Sun, X.; Chen, K. Physicochemical and biological properties of bovine-derived porous hydroxyapatite/collagen composite and its hydroxyapatite powders. Ceram. Int. 2017, 43, 16792–16798. [Google Scholar] [CrossRef]
- Thompson, T.J.U.; Gauthier, M.; Islam, M. The application of a new method of Fourier Transform Infrared Spectroscopy to the analysis of burned bone. J. Archaeol. Sci. 2009, 36, 910–914. [Google Scholar] [CrossRef] [Green Version]
- Canellas, J.; Ritto, F.G.; Figueredo, C.; Fischer, R.G.; de Oliveira, G.P.; Thole, A.A.; Medeiros, P.J.D. Histomorphometric evaluation of different grafting materials used for alveolar ridge preservation: A systematic review and network meta-analysis. Int. J. Oral Maxillofac. Surg. 2020, 49, 797–810. [Google Scholar] [CrossRef] [PubMed]
- Di Stefano, D.A.; Gastaldi, G.; Vinci, R.; Cinci, L.; Pieri, L.; Gherlone, E. Histomorphometric comparison of enzyme-deantigenic equine bone and anorganic bovine bone in sinus augmentation: A randomized clinical trial with 3-year follow-up. Int. J. Oral Maxillofac. Implant. 2015, 30, 1161–1167. [Google Scholar] [CrossRef]
- Giuliani, A.; Iezzi, G.; Mazzoni, S.; Piattelli, A.; Perrotti, V.; Barone, A. Regenerative properties of collagenated porcine bone grafts in human maxilla: Demonstrative study of the kinetics by synchrotron radiation microtomography and light microscopy. Clin. Oral Investig. 2018, 22, 505–513. [Google Scholar] [CrossRef]
- Mordenfeld, A.; Hallman, M.; Johansson, C.B.; Albrektsson, T. Histological and histomorphometrical analyses of biopsies harvested 11 years after maxillary sinus floor augmentation with deproteinized bovine and autogenous bone. Clin. Oral Implant. Res. 2010, 21, 961–970. [Google Scholar] [CrossRef]
- Scarano, A. Maxillary Sinus Augmentation with Decellularized Bovine Compact Particles: A Radiological, Clinical, and Histologic Report of 4 Cases. Biomed. Res. Int. 2017, 2017, 2594670. [Google Scholar] [CrossRef] [PubMed]
- Traini, T.; Valentini, P.; Iezzi, G.; Piattelli, A. A histologic and histomorphometric evaluation of anorganic bovine bone retrieved 9 years after a sinus augmentation procedure. J. Periodontol. 2007, 78, 955–961. [Google Scholar] [CrossRef]
- Khan, M.Q.; Sweeting, B.; Mulligan, V.K.; Arslan, P.E.; Cashman, N.R.; Pai, E.F.; Chakrabartty, A. Prion disease susceptibility is affected by beta-structure folding propensity and local side-chain interactions in PrP. Proc. Natl. Acad. Sci. USA 2010, 107, 19808–19813. [Google Scholar] [CrossRef] [Green Version]
- Artzi, Z.; Tal, H.; Dayan, D. Porous bovine bone mineral in healing of human extraction sockets. Part 1: Histomorphometric evaluations at 9 months. J. Periodontol. 2000, 71, 1015–1023. [Google Scholar] [CrossRef]
- Tapety, F.I.; Amizuka, N.; Uoshima, K.; Nomura, S.; Maeda, T. A histological evaluation of the involvement of Bio-Oss in osteoblastic differentiation and matrix synthesis. Clin. Oral Implant. Res. 2004, 15, 315–324. [Google Scholar] [CrossRef]
- Di Stefano, D.A.; Zaniol, T.; Cinci, L.; Pieri, L. Chemical, Clinical and Histomorphometric Comparison between Equine Bone Manufactured through Enzymatic Antigen-Elimination and Bovine Bone Made Non-Antigenic Using a High-Temperature Process in Post-Extractive Socket Grafting. A Comparative Retrospective Clinical Study. Dent. J. 2019, 7, 70. [Google Scholar] [CrossRef] [Green Version]
- Olszta, M.J.; Cheng, X.; Jee, S.S.; Kumar, R.; Kim, Y.Y.; Kaufman, M.J.; Douglas, E.P.; Gower, L.B. Bone structure and formation: A new perspective. Mater. Sci. Eng. R Rep. 2007, 58, 77–116. [Google Scholar] [CrossRef]
- Joschek, S.; Nies, B.; Krotz, R.; Goferich, A. Chemical and physicochemical characterization of porous hydroxyapatite ceramics made of natural bone. Biomaterials 2000, 21, 1645–1658. [Google Scholar] [CrossRef]
- Clergeau, L.P.; Danan, M.; Clergeau-Guerithault, S.; Brion, M. Healing response to anorganic bone implantation in periodontal intrabony defects in dogs. Part I. Bone regeneration. A microradiographic study. J. Periodontol. 1996, 67, 140–149. [Google Scholar] [CrossRef]
- Hislop, W.S.; Finlay, P.M.; Moos, K.F. A preliminary study into the uses of anorganic bone in oral and maxillofacial surgery. Br. J. Oral Maxillofac. Surg. 1993, 31, 149–153. [Google Scholar] [CrossRef]
- Berberi, A.; Samarani, A.; Nader, N.; Noujeim, Z.; Dagher, M.; Kanj, W.; Mearawi, R.; Salemeh, Z.; Badran, B. Physicochemical characteristics of bone substitutes used in oral surgery in comparison to autogenous bone. Biomed. Res. Int. 2014, 2014, 320790. [Google Scholar] [CrossRef]
- do Desterro Fde, P.; Sader, M.S.; Soares, G.D.; Vidigal, G.M., Jr. Can inorganic bovine bone grafts present distinct properties? Braz. Dent. J. 2014, 25, 282–288. [Google Scholar] [CrossRef] [Green Version]
- Scarano, A.; Pecora, G.; Piattelli, M.; Piattelli, A. Osseointegration in a sinus augmented with bovine porous bone mineral: Histological results in an implant retrieved 4 years after insertion. A case report. J. Periodontol. 2004, 75, 1161–1166. [Google Scholar] [CrossRef]

| Element | Abundance in AEB (g/100 g) | Abundance in ABB (g/100 g) |
|---|---|---|
| Aluminium | 0.14 | 0.12 |
| Barium | <LoQ | 0.03 |
| Calcium | 34.95 | 34.99 |
| Phosphorus | 13.15 | 12.48 |
| Magnesium | 0.82 | 0.71 |
| Strontium | 0.04 | 0.04 |
| Zinc | 0.02 | <LoQ |
| Sulphur | 0.02 | <LoQ |
| Time Points | AEB | ABB |
|---|---|---|
| Polymorphonuclear cells | ||
| 30 days | 1.25 ± 0.5 | 1 ± 0 |
| 90 days | 0.89 ± 0.3 | 0.66 ± 0.2 |
| Lymphocytes | ||
| 30 days | 1 ± 0.5 | 0.75 ± 0.5 |
| 90 days | 0.44 ± 0.5 | 0.5 ± 0.5 |
| Macrophages | ||
| 30 days | 0.63 ± 0.5 | 0.25 ± 0.5 |
| 90 days | 0.44 ± 0.5 | 0.17 ± 0.4 |
| Plasma cells | ||
| 30 days | 0 ± 0 | 0.25 ± 0.25 |
| 90 days | 0 ± 0 | 0 ± 0 |
| Giant cells | ||
| 30 days | 0 ± 0 | 0 ± 0 |
| 90 days | 0 ± 0 | 0 ± 0 |
| Necrosis | ||
| 30 days | 0 ± 0 | 0 ± 0 |
| 90 days | 0 ± 0 | 0 ± 0 |
| Time Points | AEB | ABB |
|---|---|---|
| Adipose tissue | ||
| 30 days | 0 ± 0 | 0 ± 0 |
| 90 days | 0 ± 0 | 0 ± 0 |
| Fibrosis | ||
| 30 days | 0.25 ± 0.70 | 0.5 ± 1 |
| 90 days | 0 ± 0 | 0 ± 0 |
| Neovascularization | ||
| 30 days | 1 ± 0 | 1.5 ± 0.6 |
| 90 days | 1 ± 0 | 1 ± 0 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Addis, A.; Canciani, E.; Campagnol, M.; Colombo, M.; Frigerio, C.; Recupero, D.; Dellavia, C.; Morroni, M. A New Anorganic Equine Bone Substitute for Oral Surgery: Structural Characterization and Regenerative Potential. Materials 2022, 15, 1031. https://doi.org/10.3390/ma15031031
Addis A, Canciani E, Campagnol M, Colombo M, Frigerio C, Recupero D, Dellavia C, Morroni M. A New Anorganic Equine Bone Substitute for Oral Surgery: Structural Characterization and Regenerative Potential. Materials. 2022; 15(3):1031. https://doi.org/10.3390/ma15031031
Chicago/Turabian StyleAddis, Alessandro, Elena Canciani, Marino Campagnol, Matteo Colombo, Christian Frigerio, Daniele Recupero, Claudia Dellavia, and Marco Morroni. 2022. "A New Anorganic Equine Bone Substitute for Oral Surgery: Structural Characterization and Regenerative Potential" Materials 15, no. 3: 1031. https://doi.org/10.3390/ma15031031
APA StyleAddis, A., Canciani, E., Campagnol, M., Colombo, M., Frigerio, C., Recupero, D., Dellavia, C., & Morroni, M. (2022). A New Anorganic Equine Bone Substitute for Oral Surgery: Structural Characterization and Regenerative Potential. Materials, 15(3), 1031. https://doi.org/10.3390/ma15031031








