Human Gingival Fibroblast Adhesion and Proliferation on Hydroxyapatite-Coated Zirconia Abutment Surfaces
Abstract
1. Introduction
2. Materials and Methods
2.1. CAD/CAM Fabrication of Zirconia Specimens
2.2. Surface Treatment
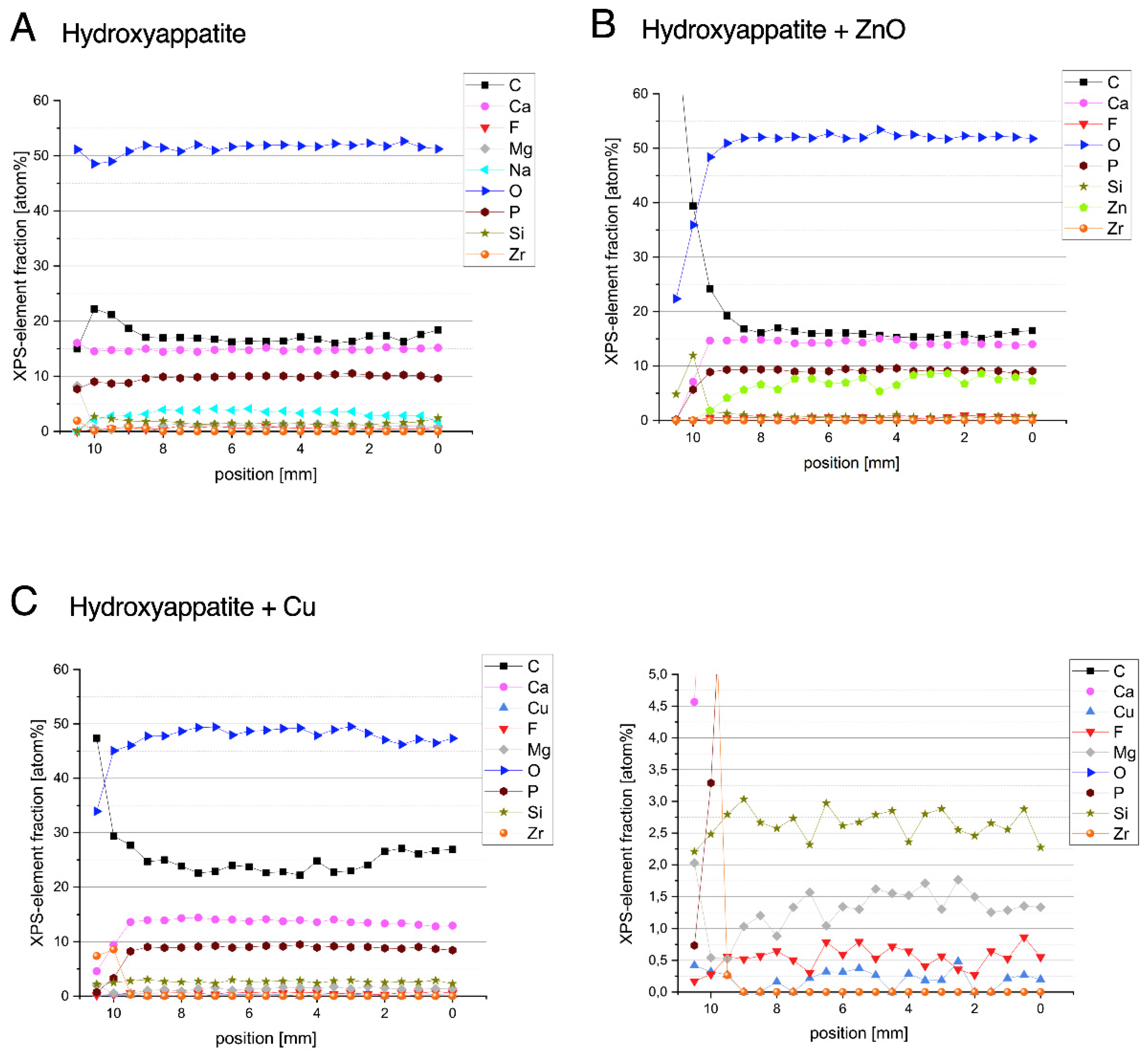
2.3. Surface Characterization
2.4. Cell Culture
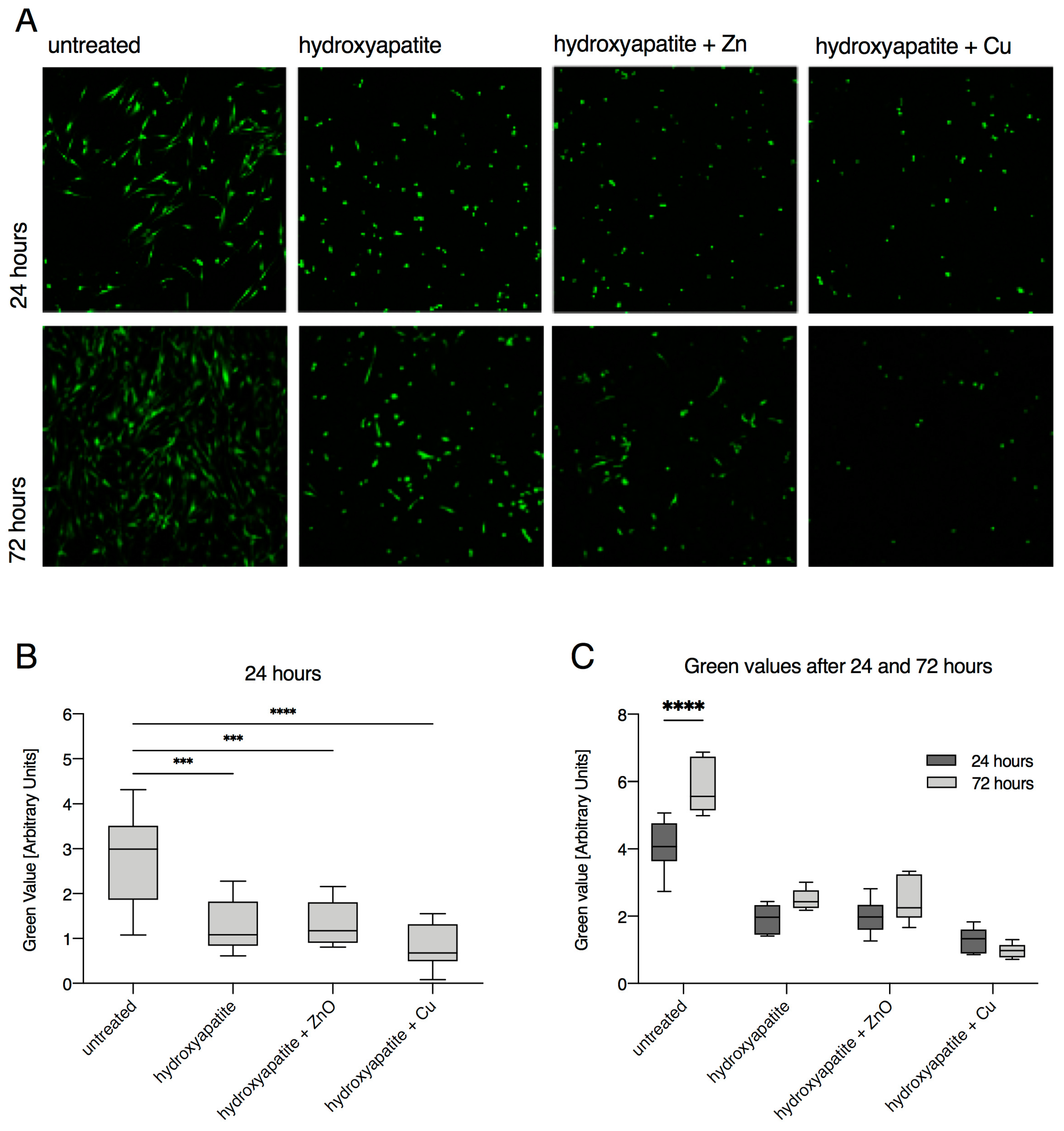
2.5. Confocal Laser Scanning Microscopy
2.6. Scanning Electron Microscopy
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Brånemark, P.-I.; Breine, U.; Adell, R.; Hansson, B.; Lindström, J.; Ohlsson, Å. Intra-osseous anchorage of dental prostheses: I. Experimental studies. Scand. J. Plast. Reconstr. Surg. 1969, 3, 81–100. [Google Scholar] [CrossRef] [PubMed]
- Mombelli, A.; Van Oosten, M.; Schürch, E., Jr.; Lang, N. The microbiota associated with successful or failing osseointegrated titanium implants. Oral Microbiol. Immunol. 1987, 2, 145–151. [Google Scholar] [CrossRef] [PubMed]
- Jepsen, S.; Berglundh, T.; Genco, R.; Aass, A.M.; Demirel, K.; Derks, J.; Figuero, E.; Giovannoli, J.L.; Goldstein, M.; Lambert, F.; et al. Primary prevention of peri-implantitis: Managing peri-implant mucositis. J. Clin. Peiodontol. 2015, 42, S152–S157. [Google Scholar] [CrossRef] [PubMed]
- Renvert, S.; Polyzois, I. Risk indicators for peri-implant mucositis: A systematic literature review. J. Clin. Periodontol. 2015, 42, S172–S186. [Google Scholar] [CrossRef]
- Lang, N.P.; Bosshardt, D.D.; Lulic, M. Do mucositis lesions around implants differ from gingivitis lesions around teeth? J. Clin. Periodontol. 2011, 38, 182–187. [Google Scholar] [CrossRef]
- Al Mugeiren, O.M.; Baseer, M.A. Dental implant bioactive surface modifiers: An update. J. Int. Soc. Prev. Community Dent. 2019, 9, 1. [Google Scholar] [CrossRef]
- Sculean, A.; Chappuis, V.; Cosgarea, R. Coverage of mucosal recessions at dental implants. Periodontol. 2000 2017, 73, 134–140. [Google Scholar] [CrossRef]
- Ivanovski, S.; Lee, R. Comparison of peri-implant and periodontal marginal soft tissues in health and disease. Periodontol. 2000 2018, 76, 116–130. [Google Scholar] [CrossRef]
- Moon, I.S.; Berglundh, T.; Abrahamsson, I.; Linder, E.; Lindhe, J. The barrier between the keratinized mucosa and the dental implant: An experimental study in the dog. J. Clin. Periodontol. 1999, 26, 658–663. [Google Scholar] [CrossRef]
- Wang, Y.; Zhang, Y.; Miron, R.J. Health, maintenance, and recovery of soft tissues around implants. Clin. Implant Dent. Relat. Res. 2016, 18, 618–634. [Google Scholar] [CrossRef]
- Barillas, L.; Testrich, H.; Cubero-Sesin, J.M.; Quade, A.; Vargas, V.I.; Polák, M.; Fricke, K. Bioactive plasma sprayed coatings on polymer substrates suitable for orthopedic applications: A study with PEEK. IEEE Trans. Radiat. Plasma Med. Sci. 2018, 2, 520–525. [Google Scholar] [CrossRef]
- Fukumoto, M.; Nie, M.; Yasui, T. Preparation and evaluation of ordinary attritor milled Ti-Al powders and corresponding thermal sprayed coatings. Mater. Trans. 2006, 47, 1717–1722. [Google Scholar] [CrossRef][Green Version]
- Sun, L.; Berndt, C.C.; Gross, K.A.; Kucuk, A. Material fundamentals and clinical performance of plasma-sprayed hydroxyapatite coatings: A review. J. Biomed. Mater. Res. 2001, 58, 570–592. [Google Scholar] [CrossRef] [PubMed]
- Auclair-Daigle, C.; Bureau, M.; Legoux, J.G.; Yahia, L.H. Bioactive hydroxyapatite coatings on polymer composites for orthopedic implants. J. Biomed. Mater. Res. Part A 2005, 73, 398–408. [Google Scholar] [CrossRef]
- Beauvais, S.; Decaux, O. Plasma sprayed biocompatible coatings on PEEK implants. In Proceedings of the 2007 International Thermal Spray Conference, Beijing, China, 14–16 May 2007; pp. 371–377. [Google Scholar]
- Benčina, M.; Resnik, M.; Starič, P.; Junkar, I. Use of plasma technologies for antibacterial surface properties of metals. Molecules 2021, 26, 1418. [Google Scholar] [CrossRef]
- Jung, R.E.; Grohmann, P.; Sailer, I.; Steinhart, Y.N.; Fehér, A.; Hämmerle, C.; Strub, J.R.; Kohal, R. Evaluation of a one-piece ceramic implant used for single-tooth replacement and three-unit fixed partial dentures: A prospective cohort clinical trial. Clin. Oral Implant. Res. 2016, 27, 751–761. [Google Scholar] [CrossRef]
- Ruan, H.; Fan, C.; Zheng, X.; Zhang, Y.; Chen, Y. In vitro antibacterial and osteogenic properties of plasma sprayed silver-containing hydroxyapatite coating. Chin. Sci. Bull. 2009, 54, 4438–4445. [Google Scholar] [CrossRef]
- Moraschini, V.; Poubel, L.D.C.; Ferreira, V.; Barboza, E.D.S. Evaluation of survival and success rates of dental implants reported in longitudinal studies with a follow-up period of at least 10 years: A systematic review. Int. J. Oral Maxillofac. Surg. 2015, 44, 377–388. [Google Scholar] [CrossRef]
- Noumbissi, S.; Scarano, A.; Gupta, S. A Literature review study on atomic ions dissolution of titanium and its alloys in implant dentistry. Materials 2019, 12, 368. [Google Scholar] [CrossRef]
- Quirynen, M.; Bollen, C. The influence of surface roughness and surface-free energy on supra-and subgingival plaque formation in man: A review of the literature. J. Clin. Periodontol. 1995, 22, 1–14. [Google Scholar] [CrossRef]
- Rimondini, L.; Cerroni, L.; Carrassi, A.; Torricelli, P. Bacterial colonization of zirconia ceramic surfaces: An in vitro and in vivo study. Int. J. Oral Maxillofac. Implant. 2002, 17, 739–798. [Google Scholar]
- Siegrist, B.E.; Brecx, M.C.; Gusberti, F.A.; Joss, A.; Lang, N.P. In vivo early human dental plaque formation on different supporting substances. A scanning electron microscopic and bacteriological study. Clin. Oral Implant. Res. 1991, 2, 38–46. [Google Scholar] [CrossRef] [PubMed]
- Köunönen, M.; Hormia, M.; Kivilahti, J.; Hautaniemi, J.; Thesleff, I. Effect of surface processing on the attachment, orientation, and proliferation of human gingival fibroblasts on titanium. J. Biomed. Mater. Res. 1992, 26, 1325–1341. [Google Scholar] [CrossRef]
- Mustafa, K.; Lopez, B.S.; Hultenby, K.; Wennerberg, A.; Arvidson, K. Attachment and proliferation of human oral fibroblasts to titanium surfaces blasted with TiO2 particles. A scanning electron microscopic and histomorphometric analysis. Clin. Oral Implant. Res. 1998, 9, 195–207. [Google Scholar] [CrossRef] [PubMed]
- Pae, A.; Lee, H.; Kim, H.-S.; Kwon, Y.-D.; Woo, Y.-H. Attachment and growth behaviour of human gingival fibroblasts on titanium and zirconia ceramic surfaces. Biomed. Mater. 2009, 4, 025005. [Google Scholar] [CrossRef]
- Mustafa, K.; Odén, A.; Wennerberg, A.; Hultenby, K.; Arvidson, K. The influence of surface topography of ceramic abutments on the attachment and proliferation of human oral fibroblasts. Biomaterials 2005, 26, 373–381. [Google Scholar] [CrossRef]
- Tsui, Y.; Doyle, C.; Clyne, T. Plasma sprayed hydroxyapatite coatings on titanium substrates Part 1: Mechanical properties and residual stress levels. Biomaterials 1998, 19, 2015–2029. [Google Scholar] [CrossRef]
- Degidi, M.; Artese, L.; Piattelli, A.; Scarano, A.; Shibli, J.A.; Piccirilli, M.; Perrotti, V.; Iezzi, G. Histological and immunohistochemical evaluation of the peri-implant soft tissues around machined and acid-etched titanium healing abutments: A prospective randomised study. Clin. Oral Investig. 2012, 16, 857–866. [Google Scholar] [CrossRef]
- Brett, P.; Harle, J.; Salih, V.; Mihoc, R.; Olsen, I.; Jones, F.; Tonetti, M. Roughness response genes in osteoblasts. Bone 2004, 35, 124–133. [Google Scholar] [CrossRef]
- Phan, T.-N.; Buckner, T.; Sheng, J.; Baldeck, J.; Marquis, R. Physiologic actions of zinc related to inhibition of acid and alkali production by oral streptococci in suspensions and biofilms. Oral Microbiol. Immunol. 2004, 19, 31–38. [Google Scholar] [CrossRef]
- Fröber, K.; Bergs, C.; Pich, A.; Conrads, G. Biofunctionalized zinc peroxide nanoparticles inhibit peri-implantitis associated anaerobes and Aggregatibacter actinomycetemcomitans pH-dependent. Anaerobe 2020, 62, 102153. [Google Scholar] [CrossRef] [PubMed]
- Liu, R.; Memarzadeh, K.; Chang, B.; Zhang, Y.; Ma, Z.; Allaker, R.P.; Ren, L.; Yang, K. Antibacterial effect of copper-bearing titanium alloy (Ti-Cu) against Streptococcus mutans and Porphyromonas gingivalis. Sci. Rep. 2016, 6, 29985. [Google Scholar] [CrossRef] [PubMed]
- Greenstein, G.; Polson, A. The role of local drug delivery in the management of periodontal diseases: A comprehensive review. J. Periodontol. 1998, 69, 507–520. [Google Scholar] [CrossRef] [PubMed]
- Abrahamsson, I.; Berglundh, T.; Wennström, J.; Lindhe, J. The peri-implant hard and soft tissues at different implant systems. A comparative study in the dog. Clin. Oral Implant. Res. 1996, 7, 212–219. [Google Scholar] [CrossRef]


| Particle Sizes of the Powder | Coating Thickness | |||
|---|---|---|---|---|
| Powder | d(p) (µm) | Range (µm) | Powder | Thickness (µm) |
| HAp | 93.78 | 20–180 | HAp | 36.49 |
| Cu | 67.79 | 20–130 | HAp + 3wt% Cu | 32.94 |
| ZnO | 2.60 | 0.5–50 | HAp + 3 wt% ZnO | 19.75 |
| n = | Median | 25% Percentile | 75% Percentile | Minimum | Maximum | |
|---|---|---|---|---|---|---|
| untreated | 12 | 0.18 | 0.14 | 0.24 | 0.12 | 0.29 |
| hydroxyapatite | 12 | 10.55 | 7.41 | 15.61 | 5.99 | 37.30 |
| hydroxyapatite + ZnO | 12 | 11.75 | 9.08 | 14.95 | 6.26 | 19.68 |
| hydroxyapatite + Cu | 12 | 10.47 | 9.47 | 12.80 | 8.88 | 84.59 |
| n = | Median | 25% Percentile | 75% Percentile | Minimum | Maximum | |
|---|---|---|---|---|---|---|
| untreated | 12 | 2.99 | 1.86 | 3.51 | 1.076 | 4.318 |
| hydroxyapatit | 12 | 1.08 | 0.83 | 1.82 | 0.6126 | 2.277 |
| hydroxyapatite + ZnO | 12 | 1.17 | 0.90 | 1.80 | 0.80 | 2.15 |
| hydroxyapatite + Cu | 12 | 0.67 | 0.49 | 1.31 | 0.08 | 1.55 |
| Cell Cluture | n = | Median | 25% Percentile | 75% Percentile | Minimum | Maximum | Significance p ≤ 0.05 | |
|---|---|---|---|---|---|---|---|---|
| untreated | 24 h | 6 | 4.06 | 3.63 | 4.76 | 2.73 | 5.07 | <0.0001 |
| 72 h | 6 | 5.56 | 5.15 | 6.73 | 4.99 | 6.87 | ||
| hydroxyapatite | 24 h | 6 | 1.97 | 1.45 | 2.32 | 1.40 | 2.43 | 0.2841 |
| 72 h | 6 | 2.42 | 2.24 | 2.77 | 2.17 | 3.01 | ||
| hydroxyapatite + ZnO | 24 h | 6 | 1.97 | 1.59 | 2.33 | 1.26 | 2.81 | 0.4663 |
| 72 h | 6 | 2.24 | 1.95 | 3.24 | 1.66 | 3.33 | ||
| hydroxyapatite + Cu | 24 h | 6 | 1.33 | 0.89 | 1.60 | 0.85 | 1.83 | 0.7891 |
| 72 h | 6 | 0.97 | 0.77 | 1.14 | 0.71 | 1.30 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bunz, O.; Steegmann, M.-C.; Benz, K.; Testrich, H.; Quade, A.; Naumova, E.A.; Arnold, W.H.; Fricke, K.; Piwowarczyk, A.; Dittmar, T. Human Gingival Fibroblast Adhesion and Proliferation on Hydroxyapatite-Coated Zirconia Abutment Surfaces. Materials 2022, 15, 3625. https://doi.org/10.3390/ma15103625
Bunz O, Steegmann M-C, Benz K, Testrich H, Quade A, Naumova EA, Arnold WH, Fricke K, Piwowarczyk A, Dittmar T. Human Gingival Fibroblast Adhesion and Proliferation on Hydroxyapatite-Coated Zirconia Abutment Surfaces. Materials. 2022; 15(10):3625. https://doi.org/10.3390/ma15103625
Chicago/Turabian StyleBunz, Oskar, Marie-Christine Steegmann, Korbinian Benz, Holger Testrich, Antje Quade, Ella A. Naumova, Wolfgang H. Arnold, Katja Fricke, Andree Piwowarczyk, and Thomas Dittmar. 2022. "Human Gingival Fibroblast Adhesion and Proliferation on Hydroxyapatite-Coated Zirconia Abutment Surfaces" Materials 15, no. 10: 3625. https://doi.org/10.3390/ma15103625
APA StyleBunz, O., Steegmann, M.-C., Benz, K., Testrich, H., Quade, A., Naumova, E. A., Arnold, W. H., Fricke, K., Piwowarczyk, A., & Dittmar, T. (2022). Human Gingival Fibroblast Adhesion and Proliferation on Hydroxyapatite-Coated Zirconia Abutment Surfaces. Materials, 15(10), 3625. https://doi.org/10.3390/ma15103625






