Mechanical Properties of Polymer-Based Blanks for Machined Dental Restorations
Abstract
1. Introduction
2. Materials and Methods
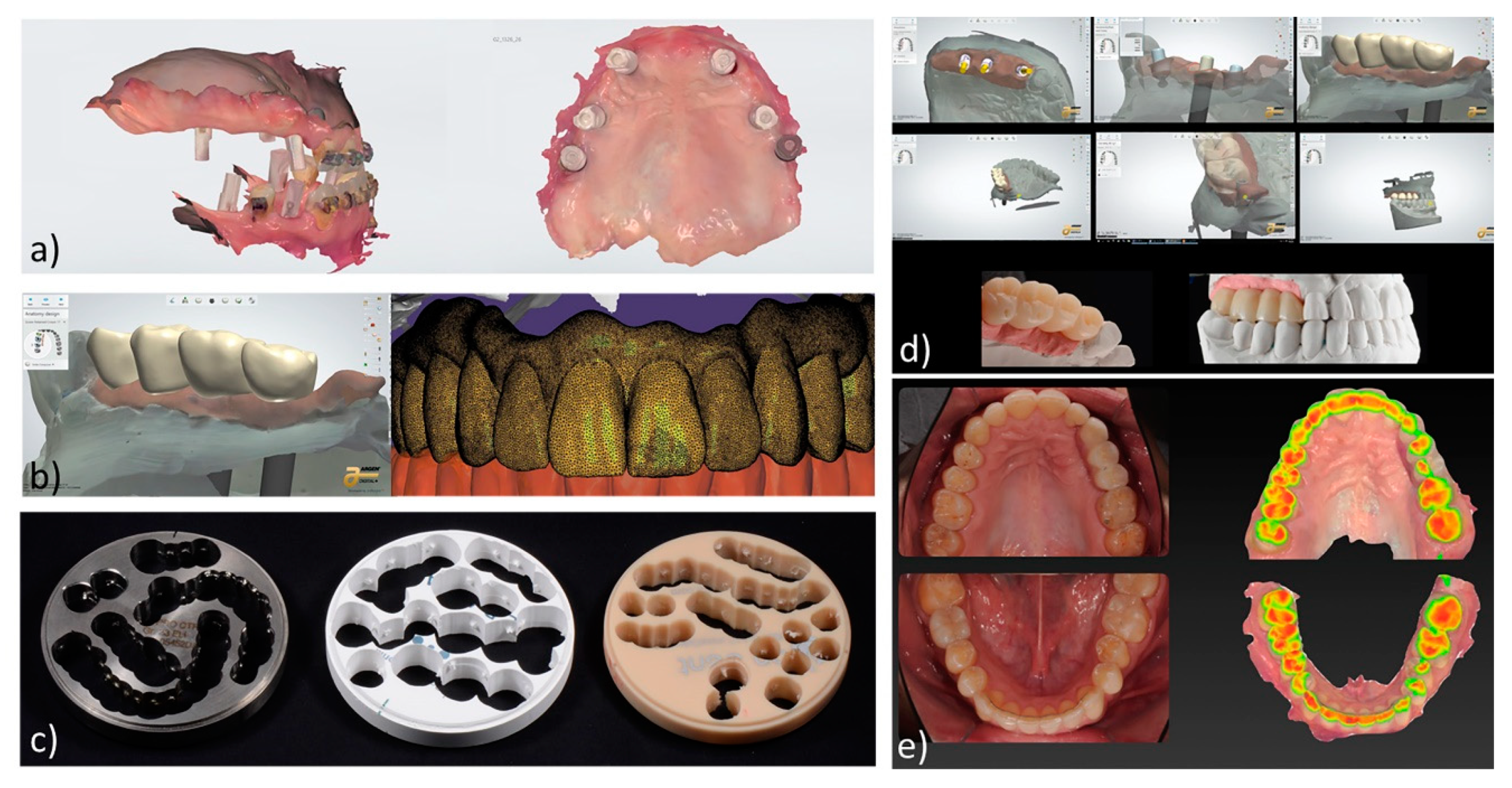
2.1. Indications/Technological Considerations
2.2. Indentation Experiments
2.3. Statistical Analysis
3. Results
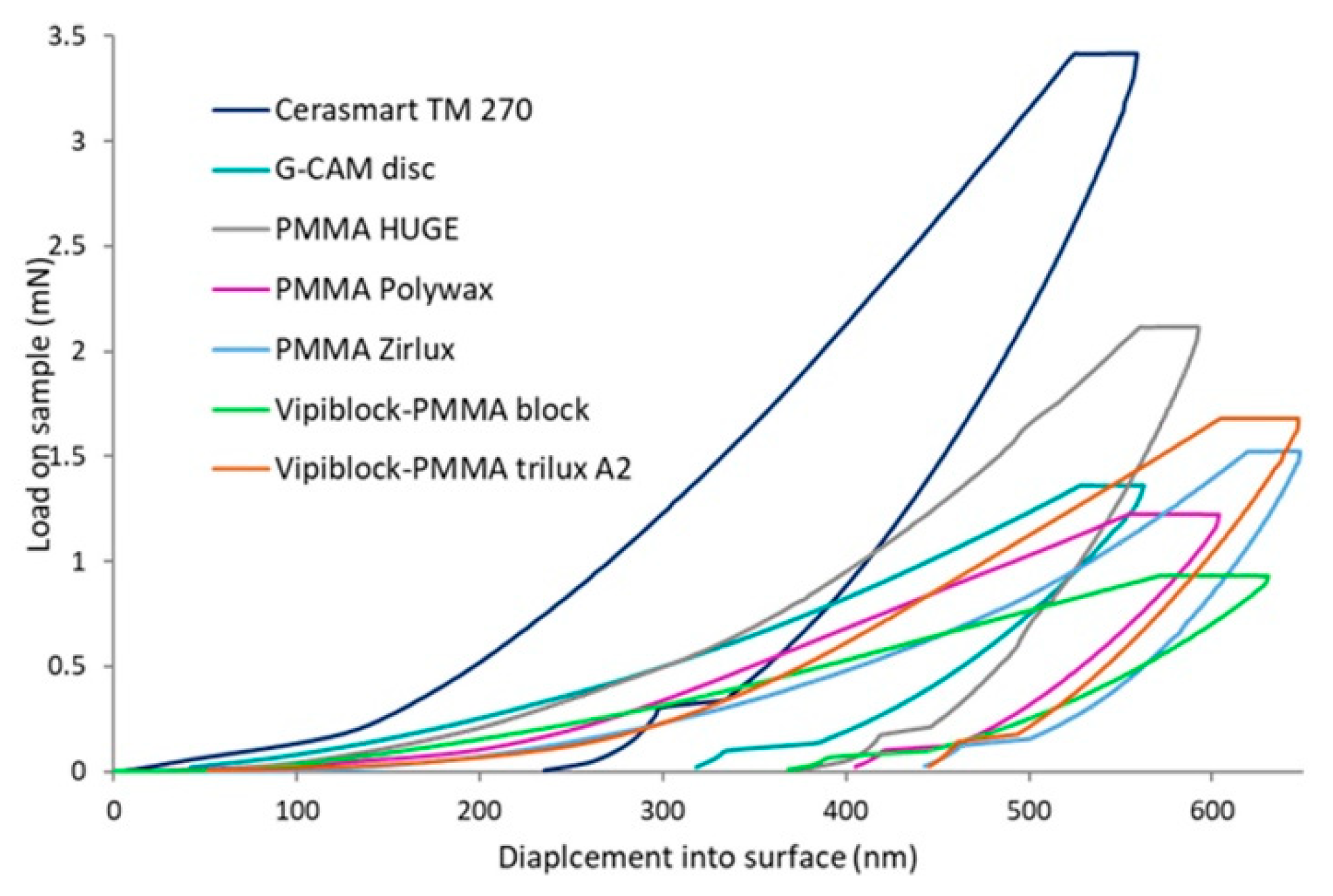
3.1. Load-Displacement Curves
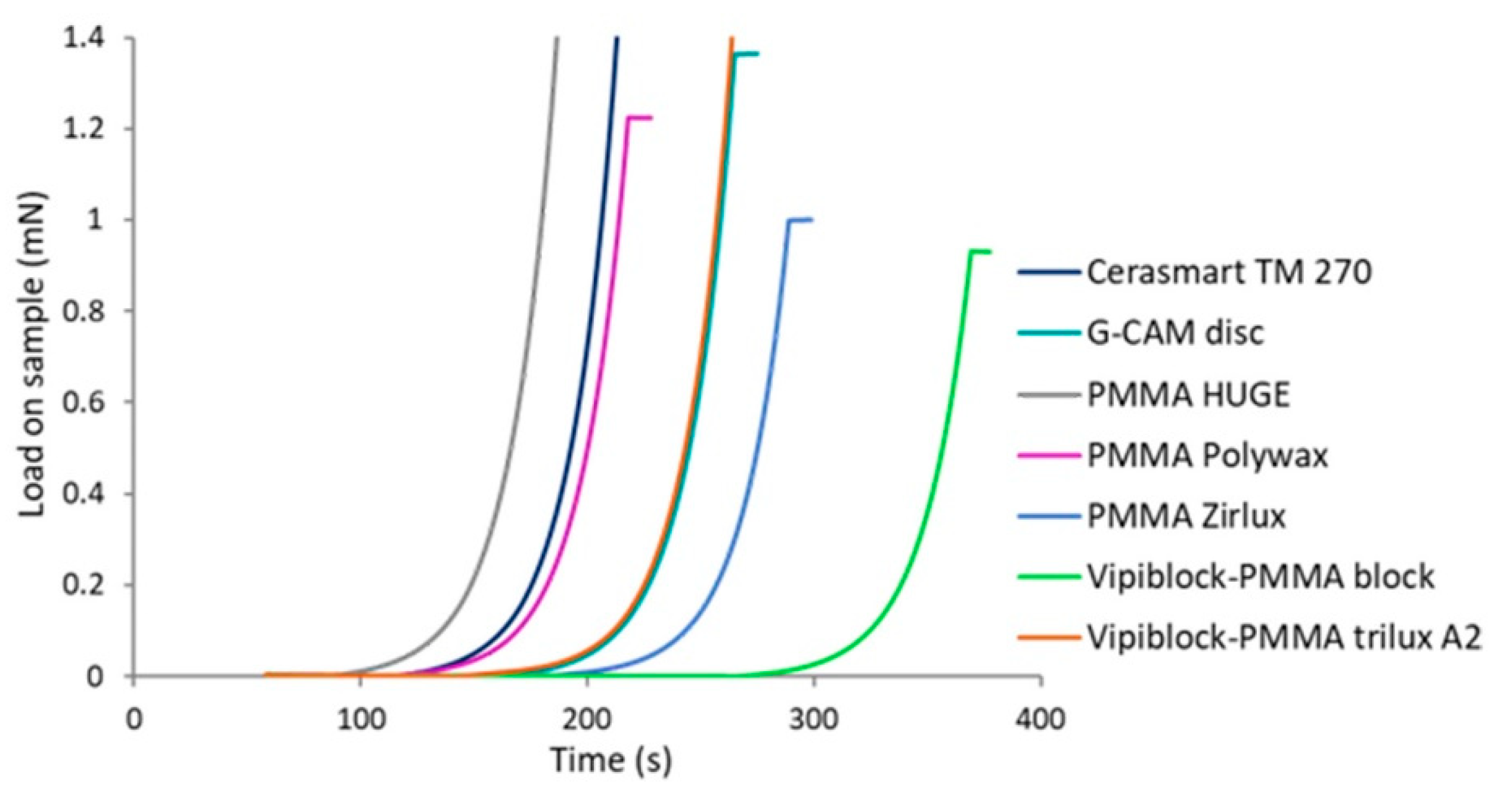
3.2. Load during Loading Stage
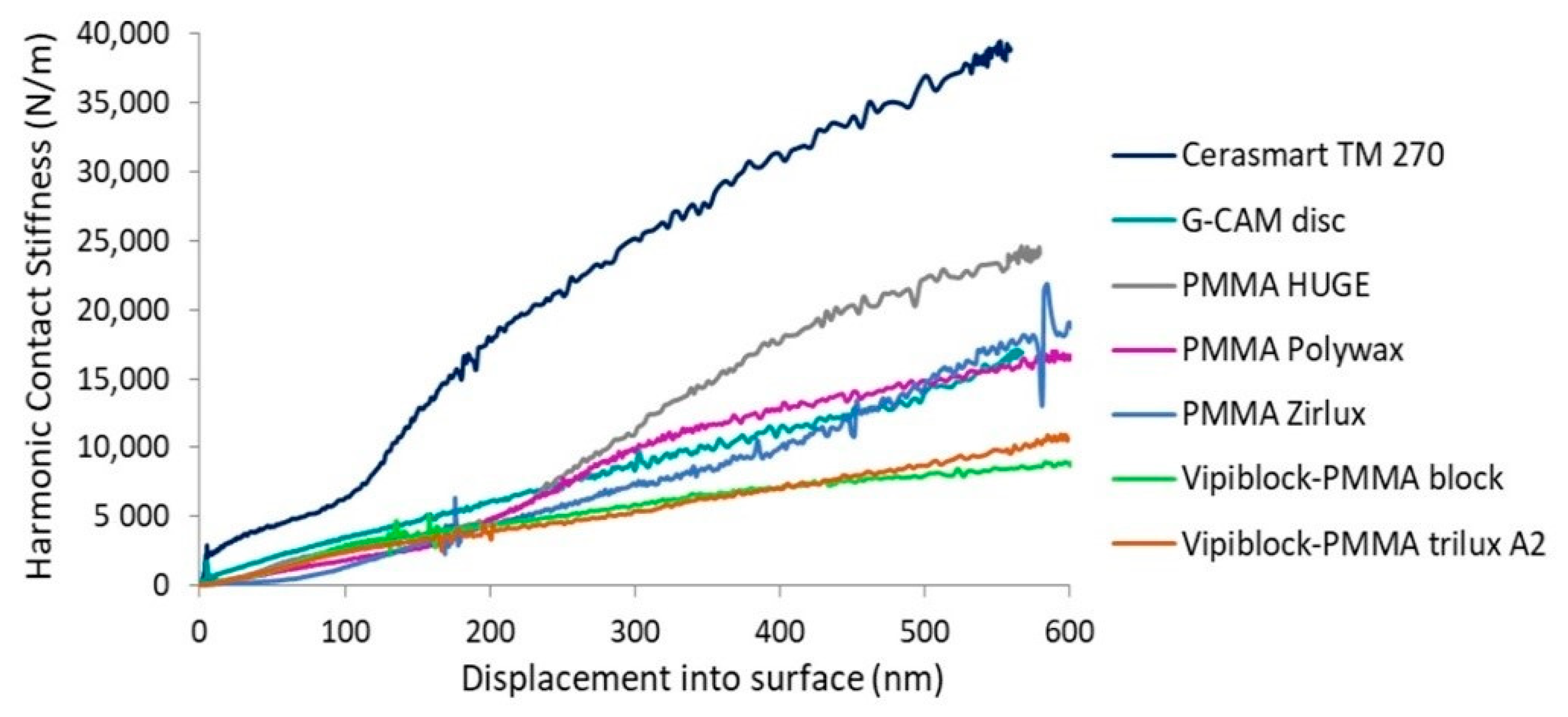
3.3. Continuous Contact Stiffness
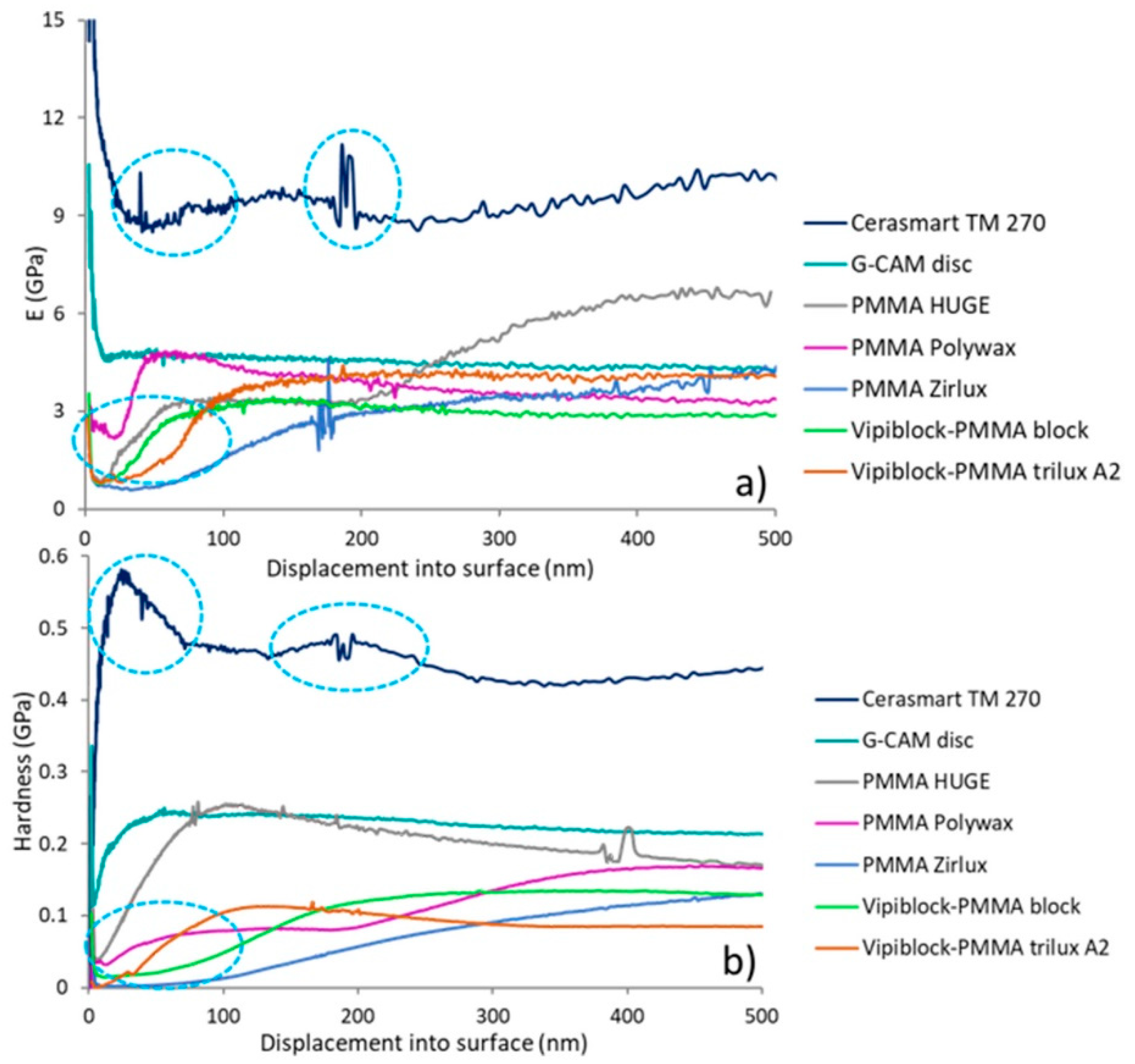
3.4. Indentation: Micro-Elastic Modulus and Micro-Hardness
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Sakaguchi, R.L.; Powers, J.M. Craig’s Restorative Dental Materials-E-Book, 13th ed.; Elsevier Health Sciences: Philadelphia, PA, USA, 2012; pp. 1–5. [Google Scholar]
- Yadav, R.; Kumar, M. Dental restorative composite materials: A review. J. Oral Biosci. 2019, 61, 78–83. [Google Scholar] [CrossRef] [PubMed]
- Pratap, B.; Gupta, R.K.; Bhardwaj, B.; Nag, M. Resin based restorative dental materials: Characteristics and future perspectives. Jpn. Dent. Sci. Rev. 2019, 55, 126–138. [Google Scholar] [CrossRef] [PubMed]
- Elmougy, A.; Schiemann, A.M.; Wood, D.; Pollington, S.; Martin, N. Characterisation of machinable structural polymers in restorative dentistry. Dent. Mater. 2018, 34, 1509–1517. [Google Scholar] [CrossRef] [PubMed]
- Storelli, S.; Del Fabbro, M.; Scanferla, M.; Palandrani, G.; Romeo, E. Implant supported cantilevered fixed dental rehabilitations in partially edentulous patients: Systematic review of the literature. Part I. Clin. Oral Implant. Res. 2018, 29, 253–274. [Google Scholar] [CrossRef] [PubMed]
- Aglietta, M.; Siciliano, V.I.; Zwahlen, M.; Brägger, U.; Pjetursson, B.E.; Lang, N.P.; Salvi, G.E. A systematic review of the survival and complication rates of implant sup-ported fixed dental prostheses with cantilever extensions after an observation period of at least 5 years. Clin. Oral Implant. Res. 2009, 20, 441–451. [Google Scholar] [CrossRef] [PubMed]
- Schmid, E.; Morandini, M.; Roccuzzo, A.; Ramseier, C.A.; Sculean, A.; Salvi, G.E. Clinical and radiographic outcomes of implant-supported fixed dental prostheses with cantilever extension. A retrospective cohort study with a follow-up of at least 10 years. Clin. Oral Implant. Res. 2020, 31, 1243–1252. [Google Scholar] [CrossRef]
- Schmid, E.; Roccuzzo, A.; Morandini, M.; Ramseier, C.A.; Sculean, A.; Salvi, G.E. Clinical and radiographic evaluation of implant-supported single-unit crowns with can-tilever extension in posterior areas: A retrospective study with a follow-up of at least 10 years. Clin. Oral Implant. Res. 2021, 23, 189–196. [Google Scholar]
- Roccuzzo, A.; Jensen, S.S.; Worsaae, N.; Gotfredsen, K. Implant-supported 2-unit cantilevers compared with single crowns on adjacent implants: A comparative retrospec-tive case series. J. Prosthet. Dent. 2020, 123, 717–723. [Google Scholar] [CrossRef]
- Liu, P.R. A panorama of dental CAD/CAM restorative systems. Compendium 2005, 26, 507–513. [Google Scholar]
- Uzun, G. An overview of dental CAD/CAM systems. Biotechnol. Biotechnol. Equip. 2008, 22, 530–535. [Google Scholar] [CrossRef][Green Version]
- Fasbinder, D.J. Restorative material options for CAD/CAM restorations. Compendium 2002, 23, 911–922. [Google Scholar]
- Beuer, F.; Schweiger, J.; Edelhoff, D. Digital dentistry: An overview of recent developments for CAD/CAM generated restorations. Br. Dent. J. 2008, 204, 505–511. [Google Scholar] [CrossRef]
- Otto, T.; De Nisco, S. Computer-aided direct ceramic restorations: A 10-year prospective clinical study of Cerec CAD/CAM inlays and onlays. Int. J. Prosthodont. 2002, 15, 1–7. [Google Scholar]
- Abdullah, A.O.; Tsitrou, E.A.; Pollington, S. Comparative in vitro evaluation of CAD/CAM vs conventional provisional crowns. J. Appl. Oral Sci. 2016, 24, 258–263. [Google Scholar] [CrossRef] [PubMed]
- Yao, J.; Li, J.; Wang, Y.; Huang, H. Comparison of the flexural strength and marginal accuracy of traditional and CAD/CAM interim materials before and after thermal cycling. J. Prosthet. Dent. 2014, 112, 649–657. [Google Scholar] [CrossRef] [PubMed]
- Lin, H.; Lv, L.; Jin, T. Investigation on the influences of hygrothermal aging on the indentation size effects and micro-indentation measurements of PMMA. Part I: Experimental results. Appl. Sci. 2020, 10, 5454. [Google Scholar] [CrossRef]
- Chakraborty, H.; Sinha, A.; Mukherjee, N.; Ray, D.; Chattopadhyay, P.P. A study on nanoindentation and tribological behaviour of multifunctional ZnO/PMMA nanocomposite. Mater. Lett. 2013, 93, 137–140. [Google Scholar] [CrossRef]
- Karimzadeh, A.; Koloor, S.S.R.; Ayatollahi, M.R.; Bushroa, A.R.; Yahya, M.Y. Assessment of nano-indentation method in mechanical characterization of heterogeneous nanocomposite materials using experimental and computational approaches. Sci. Rep. 2019, 9, 1–14. [Google Scholar] [CrossRef]
- Liu, T.; Phang, I.Y.; Shen, L.; Chow, S.Y.; Zhang, W.D. Morphology and mechanical properties of multiwalled carbon nanotubes reinforced nylon-6 composites. Macromolecules 2004, 37, 7214–7222. [Google Scholar] [CrossRef]
- Subramani, K.; Chan, Y.L.; Ngan, A.H.; King, N.M. Nanomechanical characterization of mineralized tissues in the oral cavity. In Emerging Nanotechnologies in Dentistry; Elsevier, William Andrew Publishing: Norwich, NY, USA, 2018; pp. 289–306. [Google Scholar]
- Chen, Z.; Wang, X.; Atkinson, A.; Brandon, N. Spherical indentation of porous ceramics: Elasticity and hardness. J. Eur. Ceram. 2016, 36, 1435–1445. [Google Scholar] [CrossRef]
- Beyaoui, M.; Mazeran, P.E.; Arvieu, M.F.; Bigerelle, M.; Guigon, M. Analysis of nanoindentation curves in the case of bulk amorphous polymers. Int. J. Mater. Res. 2009, 100, 943–949. [Google Scholar] [CrossRef]
- Jin, T.; Zhou, Z.; Liu, Z.; Xiao, G.; Yuan, G.; Shu, X. Sensitivity of PMMA nanoindentation measurements to strain rate. J. Appl. Polym. Sci. 2015, 132. [Google Scholar] [CrossRef]
- Aramfard, M.; Deng, C. Nanoindentation Techniques in Dental Biomaterials. In Dental Biomaterials; World Scientific: Singapore, 2019; pp. 33–66. [Google Scholar] [CrossRef]
- Wang, H.; Zhu, L.; Xu, B. Principle and Methods of Nanoindentation Test. In Residual Stresses and Nanoindentation Testing of Films and Coatings; Springer: Singapore, 2018; pp. 21–36. [Google Scholar]
- Hainsworth, S.V.; Chandler, H.W.; Page, T.F. Analysis of nanoindentation load-displacement loading curves. J. Mater. Res. 1996, 11, 1987–1995. [Google Scholar] [CrossRef]
- Huang, H.; Yan, J. On the mechanism of secondary pop-out in cyclic nanoindentation of single-crystal silicon. J. Mater. Res. 2015, 30, 1861–1868. [Google Scholar] [CrossRef]
- Caer, C.; Patoor, E.; Berbenni, S.; Lecomte, J.S. Stress induced pop-in and pop-out nanoindentation events in CuAlBe shape memory alloys. Mater. Sci. Eng. 2013, 587, 304–312. [Google Scholar] [CrossRef]
- Pathak, S.; Riesterer, J.L.; Kalidindi, S.R.; Michler, J. Understanding pop-ins in spherical nanoindentation. Appl. Phys. 2014, 105, 161913. [Google Scholar] [CrossRef]
- Gong, J.; Peng, Z.; Miao, H. Analysis of the nanoindentation load–displacement curves measured on high-purity fine-grained alumina. J. Eur. Ceram. 2005, 25, 649–654. [Google Scholar] [CrossRef]
- Han, Q.; Qu, Z.; Ye, Z. Research on the mechanical behaviour of shale based on multiscale analysis. R. Soc. Open Sci. 2018, 5, 181039. [Google Scholar] [CrossRef]
- Wang, D.; Zhang, H.; Nagaumi, H.; Jia, P.; Cui, J. Microstructural homogeneity, mechanical properties, and wear behavior of in situ Mg2Si particles reinforced Al–matrix composites fabricated by hot rolling. J. Mater. Res. Technol. 2020, 9, 1882–1892. [Google Scholar] [CrossRef]

| Commercial Name | Composition | Mechanical Characteristics * | Manufacturer/ Country | |
|---|---|---|---|---|
| Flexural Strength | Elastic Modulus | |||
| Vipiblock—PMMA block | PMMA, EDMA, organically modified ceramics | >100 MPa | >2200 MPa | VIPI Odonto Products Ltd./ Pirassununga, Brazil |
| Vipiblock—PMMA trilux monocrom A2 | ||||
| PMMA Zirlux | Multilayered PMMA | >100 MPa | >2200 MPa | Henry Schein, Inc./ Melville, NY, USA |
| PMMA Polywax | Multilayered PMMA | Bilkim Co. Ltd./ Izmir, Turkey | ||
| PMMA HUGE | Multilayer PMMA block | >120 MPa | >2200 MPa | Shandong Huge Dental Material Corporation/Shanghai, China |
| G-CAM disc | PMMA doped with graphene | >140 MPa | >3200 MPa | Graphenano Dental S.L./ Valencia, Spain |
| Cerasmart 270 | Hybrid ceramic | 246 MPa | 9600 MPa | GC Corporation/ Tokyo, Japan |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ciocan, L.T.; Ghitman, J.; Vasilescu, V.G.; Iovu, H. Mechanical Properties of Polymer-Based Blanks for Machined Dental Restorations. Materials 2021, 14, 7293. https://doi.org/10.3390/ma14237293
Ciocan LT, Ghitman J, Vasilescu VG, Iovu H. Mechanical Properties of Polymer-Based Blanks for Machined Dental Restorations. Materials. 2021; 14(23):7293. https://doi.org/10.3390/ma14237293
Chicago/Turabian StyleCiocan, Lucian Toma, Jana Ghitman, Vlad Gabriel Vasilescu, and Horia Iovu. 2021. "Mechanical Properties of Polymer-Based Blanks for Machined Dental Restorations" Materials 14, no. 23: 7293. https://doi.org/10.3390/ma14237293
APA StyleCiocan, L. T., Ghitman, J., Vasilescu, V. G., & Iovu, H. (2021). Mechanical Properties of Polymer-Based Blanks for Machined Dental Restorations. Materials, 14(23), 7293. https://doi.org/10.3390/ma14237293








