Childhood and Adult Trauma Experiences of Incarcerated Persons and Their Relationship to Adult Behavioral Health Problems and Treatment
Abstract
:1. Introduction
2. Methods
2.1. Setting
2.2. Instrument
2.3. Procedures
2.4. Participants
2.5. Variables
2.6. Weighting
2.7. Descriptive Analysis
2.8. Statistical Analysis
2.8.1. Missing Data
2.8.2. Hierarchical (Generalized) Linear Model
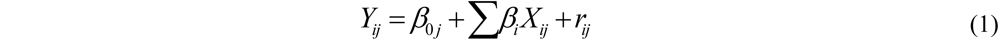
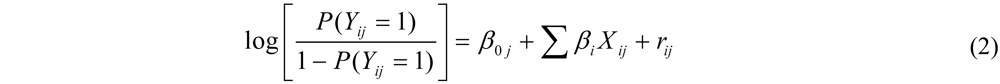
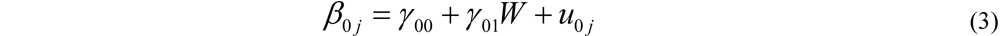
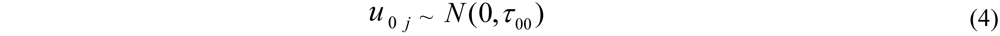
3. Results
3.1. Respondents’ Trauma Experience
| Gender and race/ethnicity | Physical Trauma | Sexual Trauma | Both Physical and Sexual Trauma | ||||||
|---|---|---|---|---|---|---|---|---|---|
| Minor (age < 18) | Adult (age 18+) | Minor and Adult | Minor (age < 18) | Adult (age 18+) | Minor and Adult | Minor (age < 18) | Adult (age 18+) | Minor and Adult | |
| Male, all (n = 3,895) | 44.7 (43.1–46.3) | 31.5 (30.0–33.0) | 25.1 (23.7–26.5) | 10.9 (9.9–11.9) | 4.5 (3.9–5.2) | 3.7 (3.1–4.4) | 9.6 (8.7–10.6) | 3.7 (3.1–4.3) | 3.2 (2.6–3.8) |
| White (n = 596) | 52.4 (48.4–56.4) | 36.4 (32.5–40.3) | 29.8 (26.1–33.5) | 14.5 (11.6–17.4) | 3.9 (2.3–5.4) | 2.9 (1.5–4.3) | 12.4 (9.7–15.1) | 3.0 (1.6–4.4) | 2.3 (1.1–3.6) |
| Black (n = 2,003) | 43.6 (41.4–45.8) | 31.0 (29.0–33.1) | 23.7 (21.8–25.6) | 8.5 (7.3–9.7) | 3.8 (2.9–4.6) | 2.9 (2.1–3.6) | 7.5 (6.3–8.7) | 2.7 (2.0–3.5) | 2.3 (1.6–2.9) |
| Hispanic (n = 984) | 40.0 (36.9–43.1) | 28.1 (25.3–30.9) | 23.2 (20.5–25.8) | 12.1 (10.0–14.2) | 5.4 (3.9–6.8) | 4.8 (3.5–6.2) | 11.0 (9.0–13.0) | 5.1 (3.8–6.5) | 4.6 (3.3–5.9) |
| Other a (n = 312) | 51.9 (46.3–57.5) | 35.7 (30.4–41.1) | 31.2 (26.1–36.4) | 15.9 (11.8–20.0) | 8.1 (5.0–11.1) | 7.8 (4.8–10.8) | 14.0 (10.1–17.9) | 6.7 (3.9–9.5) | 6.7 (3.9–9.5) |
3.2. Behavioral Health Treatment and Trauma Experience
| Behavioral health treatment | Physical trauma | Sexual trauma | Abandonment | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Minor (age < 18) N = 1,741 | Adult (age 18+) N = 1,226 | Minor and Adult N = 981 | No Reported Trauma N = 1,909 | Minor (age < 18) N = 415 | Adult (age 18+) N = 175 | Minor and Adult N = 144 | No Reported Trauma N = 3,449 | Minor (age < 18) N = 768 | Adult (age 18+) N = 712 | Minor and Adult N = 445 | No Reported Trauma N = 2,860 | |
| Depression treatment | 21.1 (19.2–23.1) | 20.5 (18.3–22.8) | 22.2 (19.6–24.8) | 11.1 (9.7–12.5) | 32.1 (27.6–36.7) | 27.4 (20.6–34.2) | 27.6 (20.1–35.2) | 13.7 (12.5–14.8) | 26.9 (23.7–30.0) | 25.9 (22.6–29.1) | 29.0 (24.7–33.3) | 12.3 (11.1–13.5) |
| Anxiety disorder treatment | 10.9 (9.4–12.4) | 11.2 (9.4–13.0) | 12.5 (10.4–14.6) | 4.9 (3.9–5.9) | 16.1 (12.5–19.8) | 16.4 (10.7–22.0) | 15.8 (9.6–21.9) | 6.5 (5.7–7.3) | 14.1 (11.6–16.6) | 14.0 (11.4–16.6) | 16.2 (12.7–19.7) | 5.6 (4.8–6.5) |
| Drug or alcohol treatment | 28.7 (26.6–30.9) | 30.1 (27.5–32.7) | 30.2 (27.3–33.1) | 23.9 (22.0–25.8) | 32.3 (27.8–36.9) | 27.6 (20.9–34.3) | 28.2 (20.8–35.7) | 25.7 (24.2–27.2) | 29.6 (26.3–32.8) | 34.5 (31.0–38.0) | 33.4 (29.0–37.8) | 24.6 (23.1–26.2) |
3.3. Behavioral Health Problems Related to Trauma Experience
| Independent variables | Incarcerated Men (N = 3,877) | ||||||
|---|---|---|---|---|---|---|---|
| Depression treatment a | Depression symptoms | Anxiety treatment a | Anxiety symptoms | Substance abuse treatment a | Substance abuse problems | ||
| Level 2 (Reliability) | 0.214 | 0.843 | 0.001 | 0.014 | 0.789 | 0.677 | |
| Mean age of inmates in each prison | 1.03 * | −0.02 | 1.07 * | −0.02 * | 1.02 | −0.005 | |
| Level 1 | |||||||
| Age | 1.01 | −0.01 * | 1.00 | −0.03 ** | 1.01 | −0.009 * | |
| Race: White | 2.66 ** | 0.79 ** | 4.66 ** | 0.56 ** | 1.81 * | 0.63 ** | |
| Latino | 1.30 * | 0.46 ** | 1.23 | 0.16 | 0.83 * | 0.009 | |
| Other b | 1.52 * | 0.39 * | 1.47 | 0.25 | 0.87 | −0.06 | |
| Education (>high school/GED vs. less) | 0.80 * | −0.47 ** | 0.98 | −0.24 * | 0.91 | −0.11 * | |
| Time incarcerated since 18 | 1.00 | 0.02 * | 1.01 | 0.02 * | 1.04 ** | 0.03 ** | |
| Type of crime: Sex Crime | 0.96 | −0.15 | 0.73 | −0.22 | 0.52 * | −0.67 ** | |
| Violent Crime | 1.00 | −0.27 * | 1.25 | −0.15 | 0.74 * | −0.002 | |
| Physical trauma <18 (Yes = 1) | 1.40 * | −0.003 | 1.42 * | 0.17 | 1.03 | 0.14 * | |
| Sexual trauma <18 (Yes = 1) | 2.06 ** | 0.44 * | 1.52 * | 0.38 * | 1.41 * | 0.31 ** | |
| Physical trauma 18+ (Yes = 1) | 1.04 | 0.40 * | 1.22 | 0.28 * | 1.12 | 0.33 ** | |
| Sexual trauma 18+ (Yes = 1) | 0.87 | 0.39 | 1.30 | 0.39 | 0.81 | 0.28 * | |
| Abandoned <18 (Yes = 1) | 1.42 * | 0.60 ** | 1.35 | 0.48 ** | 0.89 | 0.11 | |
| Abandoned 18+ (Yes = 1) | 1.44 * | 0.92 ** | 1.43 * | 0.68 ** | 1.50 ** | 0.31 ** | |
| Test Statistics | |||||||
| Chi-square | 9.68 | 45.84 | 5.32 | 7.31 | 62.94 | 32.81 | |
| Df | 8 | 8 | 8 | 8 | 8 | 8 | |
| p-value | 0.288 | <0.001 | >0.5 | >0.5 | <0.001 | p < 0.001 | |
| Independent variable | Incarcerated Men (N = 3,877) | ||||
|---|---|---|---|---|---|
| Interpersonal Problems | Self-regulation Problems | Aggression | Hopelessness | ||
| Level 2 (Reliability) | 0.366 | 0.030 | 0.001 | 0.567 | |
| Mean age of inmate population | −0.03 ** | −0.004 | −0.25 ** | 0.004 | |
| Level 1 | |||||
| Age | −0.04 ** | −0.03 ** | −0.26 ** | −0.02 * | |
| Race: White | 0.51 ** | 0.34 ** | 1.47 * | 1.09 ** | |
| Latino | −0.03 | −0.03 | −1.22 * | 0.47 ** | |
| Other a | 0.15 | −0.03 | 0.04 | 0.50 * | |
| Education (>high school/GED vs. less) | −0.23 ** | −0.22 ** | −1.19 * | −0.55 ** | |
| Time incarcerated since 18 | 0.04 ** | 0.04 ** | 0.22 ** | 0.04 ** | |
| Type of crime: Sex Crime | −0.28 * | −0.73 ** | −1.08 | −0.09 | |
| Violent Crime | 0.58 ** | 0.03 | 2.35 ** | −0.10 | |
| Physical trauma <18 (Yes = 1) | 0.48 ** | 0.44 ** | 2.70 ** | −0.17 | |
| Sexual trauma <18 (Yes = 1) | 0.34 * | 0.35 * | 0.42 | 0.55 * | |
| Physical trauma 18+ (Yes = 1) | 0.65 ** | 0.45 ** | 2.48 ** | 0.59 ** | |
| Sexual trauma 18+ (Yes = 1) | 0.52 * | 0.46 * | 1.54 | 0.85 * | |
| Abandoned <18 (Yes = 1) | 0.27 * | 0.28 * | 1.79 * | 0.44 * | |
| Abandoned 18+ (Yes =1) | 0.51 ** | 0.42 ** | 1.55 * | 0.42 * | |
| Test Statistics | |||||
| Chi-square | 12.09 | 5.01 | 4.30 | 21.12 | |
| Df | 8 | 8 | 8 | 8 | |
| p-value | 0.147 | >0.5 | >0.5 | 0.007 | |
4. Discussion
5. Conclusions
Acknowledgements
Conflict of Interest
References
- Miller-Perrin, C.; Perrin, R. Child Maltreatment: An Introduction; Sage Publications: Thousand Oaks, CA, USA, 2007. [Google Scholar]
- Stavrianos, C.; Stavrianou, P.; Vasiliadis, L.; Karamouzi, A.; Mihailidou, D.; Mihail, G. Emotional maltreatment of children. Soc. Sci. 2011, 6, 441–446. [Google Scholar]
- Harlow, C. Prior Abuses Reported by Inmates and Probationers (Publication No. NCJ 172879); U.S. Department of Justice, Bureau of Justice Statistics: Washington, DC, USA, 1999. [Google Scholar]
- Wolff, N.; Shi, J.; Siegel, J. Patterns of victimization among male and female inmates: Evidence of an enduring legacy. Violence Vict. 2009, 24, 469–484. [Google Scholar] [CrossRef]
- Widom, C.S.; Czaja, S.; Dutoon, M. Childhood victimization and lifetime revictimization. Child Abus. Negl. 2008, 32, 785–796. [Google Scholar] [CrossRef]
- Wolff, N.; Shi, J. Trauma and Incarcerated Persons. In The Handbook of Correctional Mental Health, 2nd; Scott, C.L., Ed.; American Psychiatric Publishing, Inc.: Arlington, VA, USA, 2010; pp. 277–320. [Google Scholar]
- U.S. Deparatment of Health and Human ServicesAdministration on ChildrenYouth and FamiliesChild Maltreatment 2005; U.S. Government Printing Office: Washington, DC, USA, 2007.
- Garbarino, J.; Garbarino, A. Emotional Maltreatment of Children; National Committee to Prevent Child Abuse: Chicago, IL, USA, 1994. [Google Scholar]
- Henley, A. The Abandoned Child. In Deviancy and the Family; Bryant, C.D., Wells, G.J., Eds.; F. A. Davis: Philadelphia, PA, USA, 1973; pp. 199–208. [Google Scholar]
- Maniglio, R. The impact of child sexual abuse on health: A systematic review of reviews. Clin. Psychol. Rev. 2009, 29, 647–657. [Google Scholar] [CrossRef]
- Kalmuss, D.S. The intergenerational transmission of marital aggression. J. Marriage Fam. 1984, 46, 11–19. [Google Scholar] [CrossRef]
- Straus, M.A.; Gelles, R.J.; Steinmetz, S. Behind Closed Doors: Violence in the American Family; Anchor Press: Doubleday, NY, USA, 1980. [Google Scholar]
- Widom, C.S. Child abuse, neglect, and violent criminal behavior. Criminology 1989, 27, 251–271. [Google Scholar] [CrossRef]
- Ireland, T.; Widom, C.S. Childhood victimization and risk for alcohol and drug arrests. Int. J. Addict. 1994, 29, 235–274. [Google Scholar]
- Dutton, D.; Hart, S. Evidence for long-term, specific effects of childhood abuse and neglect on criminal behavior in men. Int. J. Offender Ther. Comp. Criminol. 1992, 36, 129–137. [Google Scholar] [CrossRef]
- Chapman, D.; Whitfield, C.; Felitti, V.; Dube, S.; Edwards, V.; Anda, R. Adverse childhood experiences and the risk of depressive disorders in adulthood. J. Affect. Disord. 2004, 82, 217–225. [Google Scholar] [CrossRef]
- Stein, J.A.; Golding, J.M.; Siegel, J.M.; Burnam, M.A.; Sorenson, S.B. Long-Term Psychological Sequelae of Child Sexual Abuse: The Los Angeles Epidemiologic Catchment Area Study. In Lasting Effects of Child Sexual Abuse; Sage, F., Wyatt, G.E., Powell, G.J., Eds.; Sage Publications: Newbury Park, CA, USA, 1988; Volume 100, pp. 135–154. [Google Scholar]
- Springer, K.; Sheridan, J.; Kuo, D.; Carnes, M. Long-term physical and mental health consequences of childhood physical abuse: Results from a large population-based sample of men and women. Child Abus. Negl. 2007, 31, 517–530. [Google Scholar] [CrossRef]
- Afifi, T.; Boman, J.; Fleisher, W.; Sareen, J. The relationship between child abuse, parental divorce, and lifetime mental disorders and suicidality in a nationally representative adult sample. Child Abus. Negl. 2009, 33, 139–147. [Google Scholar] [CrossRef]
- Widom, C.S.; DuMont, K.A.; Czaja, S.J. A prospective investigation of major depressive disorder and comorbidity in abused and neglected children grown up. Arch. Gen. Psychiatry 2007, 64, 49–56. [Google Scholar]
- Fergusson, D.M.; Boden, J.M.; Horwood, L.J. Exposure to childhood sexual and physical abuse and adjustment in early adulthood. Child Abus. Negl. 2008, 32, 607–619. [Google Scholar] [CrossRef]
- Ballanger, J.C.; Davidson, J.R.; Lecrubier, Y.; Nutt, D.J.; Marshall, R.D.; Nemeroff, C.B.; Shalev, A.Y.; Yehuda, R. Consensus statement update on posttraumatic stress disorder from the international consensus group on depression and anxiety. J. Clin. Psychiatry 2004, 65, 55–62. [Google Scholar]
- Breslau, M.; Kessler, R.C.; Chilcoat, H.D.; Schultz, L.R.; Davis, G.C.; Andreski, P. Trauma and posttraumatic stress disorder in the community. Arch. Gen. Psychology 1998, 55, 626–632. [Google Scholar]
- McClellan, D.S.; Farabee, D.; Crouch, B.M. Early victimization, drug use, and criminality: A comparison of male and female prisoners. Crim. Justice Behav. 1997, 24, 455–467. [Google Scholar] [CrossRef]
- Chilcoat, M.D.; Breslau, N. Posttraumatic stress disorder and drug disorders: Testing causal pathways. Arch. Gen. Psychiatry 1998, 559, 13–17. [Google Scholar]
- Widom, C.S.; White, H.; Czaja, S.; Marmorstein, N. Long term effects of child abuse and neglect on alcohol use and excessive drinking in middle adulthood. J. Stud. Alcohol. Drugs 2007, 68, 317–325. [Google Scholar]
- Felitti, V.; Anda, R.; Nordenberg, D.; Williamson, D.F.; Spitz, A.; Edwards, V.; Koss, M.P.; Marks, J. Relationship of childhood abuse and household dysfunction in many of the leading causes of death in adults. Am. J. Prev. Med. 1998, 14, 245–258. [Google Scholar] [CrossRef]
- Brodsky, B.S.; Oquendo, M.; Ellis, S.P.; Haas, G.L.; Malone, K.M.; Mann, J.J. The relationship of childhood abuse to impulsivity and suicidal behavior in adults with major depression. Am. J. Psychiatry 2001, 158, 1871–1877. [Google Scholar] [CrossRef]
- Dube, S.R.; Anda, R.F.; Felitti, V.J.; Chapman, D.P.; Williamson, D.F.; Giles, W.H. Childhood abuse, household dysfunction, and the risk of attempted suicide throughout the life Span: Findings from the adverse childhood experiences study. JAMA 2001, 286, 3089–3096. [Google Scholar]
- van der Kolk, B.A.; Pelcovitz, D.; Roth, S.; Mandel, F.S.; McFarlane, A.; Herman, J.L. Dissociation, somatization, and affect dysregulation: The complexity of adaptation of trauma. Am. J. Psychiatry 1996, 153, 83–93. [Google Scholar]
- Pribor, E.F.; Dinwiddie, S.H. Psychiatric correlates of incest in childhood. Am. J. Psychiatry 1992, 149, 52–56. [Google Scholar]
- Silverman, A.B.; Reinherz, H.Z.; Giaconia, R.M. The long-term sequelae of child and adolescent abuse: A longitudinal community study. Child Abus. Negl. 1996, 20, 709–723. [Google Scholar] [CrossRef]
- Johnson, J.G.; Smailes, E.M.; Cohen, P.; Brown, J.; Bernstein, DP. Associations between four types of childhood neglect and personality disorder symptoms during adolescence and early adulthood: Findings of a community-based longitudinal study. J. Pers. Disord. 2000, 14, 171–187. [Google Scholar] [CrossRef]
- Bryant, F.B.; Smith, B.D. Refining the architecture of aggression: A measurement model for the buss-perry aggression questionnaire. J. Res. Pers. 2001, 35, 138–167. [Google Scholar] [CrossRef]
- Diamond, P.; Wang, E.W.; Buffington-Vollum, J. Factor structure of the Buss-Perry Aggression Questionnaire (BPAQ) with mentally ill male prisoners. Crim. Justice Behav. 2005, 32, 546–564. [Google Scholar] [CrossRef]
- Beck, A.; Weissman, A.; Lester, D.; Trexler, L. The measurement of pessimism: The hopelessness scale. J. Consult. Clin. Psychol. 1974, 42, 861–865. [Google Scholar] [CrossRef]
- Velting, D.M. Personality and negative expectancies: Trait structure of the beck hopelessness scale. Personal. Individ. Differ. 1999, 26, 913–921. [Google Scholar] [CrossRef]
- Durham, T.W. Norms, reliability and item analysis of the hopelessness scale in general psychiatric, forensic psychiatric and college populations. J. Clin. Psychol. 1982, 38, 597–600. [Google Scholar] [CrossRef]
- Holden, R.R.; Fekken, G.C. Test-retest reliability of the hopelessness scale and its items in a university population. J. Clin. Psychol. 1988, 43, 597–600. [Google Scholar]
- Beck, A.T.; Steer, R.A. Manual for the Beck Hopelessness Scale; Psychological Corporation: San Antonio, TX, USA, 1988. [Google Scholar]
- Raudenbush, S.W.; Bryk, A.S. Hierarchical Linear Models: Applications and Data Analysis Methods, 2nd ed; Sage Publications: Thousand Oaks, CA, USA, 2002. [Google Scholar]
- McQueen, D.; Itzin, C.; Kennedy, R.; Sinason, V.; Maxted, F. Psychoanalytic Psychotherapy after Child Abuse: The Treatment of Adults and Children Who Have Experienced Sexual Abuse, Violence, and Neglect in Childhood; Karnac Books Ltd: London, UK, 2009. [Google Scholar]
- Rich, D.J.; Gingerich, K.J.; Rosen, L.A. Childhood emotional abuse and associated psychopathy in college students. J. Coll. Stud. Psychother. 1997, 11, 13–28. [Google Scholar] [CrossRef]
- Chapple, C. Examining intergenerational violence: Violent role modeling or weak parental controls? Violence Vict. 2003, 18, 143–162. [Google Scholar] [CrossRef]
- Raes, F.; Hermans, D. On the mediating role of subtypes of rumination in the relationship between childhood emotional abuse and depressed mood: Brooding versus reflection. Depress. Anxiety 2008, 25, 1067–1070. [Google Scholar] [CrossRef]
- Wright, M.O.; Crawford, E.; Del Castillo, D. Childhood emotional maltreatment and later psychological distress among college students: The mediating role of maladaptive schemas. Child Abus. Negl. 2009, 33, 59–68. [Google Scholar] [CrossRef]
- Hien, D.A.; Wells, E.A.; Jiang, H.; Suarez-Morales, L.; Campbell, A.; Cohen, L.; Miele, G.M.; Killeen, T; Brigham, G.S.; Zhang, Y; et al. Multi-site randomized trial of behavioral interventions for women with co-occurring PTSD and substance use disorders. J. Consult. Clin. Psychol. 2009, 77, 607–619. [Google Scholar] [CrossRef]
- Najavits, L.M. Seeking safety: An Evidence-Based Model for Substance Abuse and Trauma/PTSD. In Therapists’ Guide to Evidence-based Relapse Prevention: Practical Resources for the Mental Health Professional; Witkiewitz, K.A., Marlatt, G.A., Eds.; Elsevier Press: San Diego, CA, USA, 2007; pp. 141–167. [Google Scholar]
- Fallot, R.D.; Harris, M. The Trauma Recovery and Empowerment Model (TREM): Conceptual and practical issues in a group intervention for women. Commun. Ment. Health J. 2002, 38, 475–485. [Google Scholar] [CrossRef]
Appendix
| Variables | N | Range | M(SD) | |
|---|---|---|---|---|
| Dependent Variables | ||||
| Depression treatment in prison | 3,958 | 0–1 | 0.15(0.36) | |
| Depression symptoms | 3,959 | 0–12 | 2.52 (2.95) | |
| Anxiety disorder treatment in prison | 3,958 | 0–1 | 0.07(0.26) | |
| Anxiety symptoms | 3,959 | 0–9 | 2.22 (2.48) | |
| Substance abuse treatment in prison | 3,958 | 0–1 | 0.26 (0.44) | |
| Substance/alcohol in community | 3,904 | 0–4 | 1.46(1.36) | |
| Interpersonal problems | 3,904 | 0–7 | 1.81(2.01) | |
| Self-regulation problems | 3,899 | 0–6 | 2.12(1.73) | |
| Anger-Buss-Perry Aggression Scale total score | 3,949 | 12–60 | 28.5(11.2) | |
| Beck Hopelessness Scale | 3,965 | 0–19 | 3.21(3.14) | |
| Independent Variables | ||||
| Level-2, mean age | 10 | 23.2–44.7 | 34.0(7.2) | |
| Age | 3,893 | 18–79 | 33.3(10.1) | |
| White | 3,898 | 0,1 (Y) | 0.16 (0.37) | |
| Latino | 3,898 | 0,1 (Y) | 0.25(0.43) | |
| Other race | 3,898 | 0,1 (Y) | 0.08(0.27) | |
| Education/GED | 3,898 | 0,1 (Y) | 0.61 (0.49) | |
| Years served in prison since age 18 | 3,943 | 0–60 | 7.6 (6.7) | |
| Current offense: Sex offense | 3,956 | 0,1 (Y) | 0.05 (0.22) | |
| Current offense: Violent offense | 3,956 | 0,1 (Y) | 0.24 (0.43) | |
| Physical trauma < 18 | 3,895 | 0,1 (Y) | 0.45 (0.50) | |
| Sexual trauma < 18 | 3,895 | 0,1 (Y) | 0.11 (0.31) | |
| Physical trauma 18+ | 3,895 | 0,1 (Y) | 0.31 (0.46) | |
| Sexual trauma 18+ | 3,895 | 0,1 (Y) | 0.04 (0.21) | |
| Abandoned < 18 | 3,895 | 0,1 (Y) | 0.20 (0.40) | |
| Abandoned 18+ | 3895 | 0,1 (Y) | 0.18 (0.39) | |
© 2012 by the authors; licensee MDPI, Basel, Switzerland. This article is an open-access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Wolff, N.; Shi, J. Childhood and Adult Trauma Experiences of Incarcerated Persons and Their Relationship to Adult Behavioral Health Problems and Treatment. Int. J. Environ. Res. Public Health 2012, 9, 1908-1926. https://doi.org/10.3390/ijerph9051908
Wolff N, Shi J. Childhood and Adult Trauma Experiences of Incarcerated Persons and Their Relationship to Adult Behavioral Health Problems and Treatment. International Journal of Environmental Research and Public Health. 2012; 9(5):1908-1926. https://doi.org/10.3390/ijerph9051908
Chicago/Turabian StyleWolff, Nancy, and Jing Shi. 2012. "Childhood and Adult Trauma Experiences of Incarcerated Persons and Their Relationship to Adult Behavioral Health Problems and Treatment" International Journal of Environmental Research and Public Health 9, no. 5: 1908-1926. https://doi.org/10.3390/ijerph9051908
APA StyleWolff, N., & Shi, J. (2012). Childhood and Adult Trauma Experiences of Incarcerated Persons and Their Relationship to Adult Behavioral Health Problems and Treatment. International Journal of Environmental Research and Public Health, 9(5), 1908-1926. https://doi.org/10.3390/ijerph9051908




