Physical Activity and Risk of Cardiovascular Disease—A Meta-Analysis of Prospective Cohort Studies
Abstract
:1. Introduction
2. Methods
2.1. Study Selection and Data Extraction
2.2. Statistical Analysis
3. Results
| Study | Country | Population | Follow-up duration | Measurement of physical activity | No. of cases | Adjustments |
|---|---|---|---|---|---|---|
| CHD | ||||||
| Donahue et al. [17] | USA | 7,644 men, age 45–69 years | 12 years | Leisure time PA index based on average time of activities | 888 cases | Age, alcohol, smoking |
| Folsom et al. [18] | USA | 6,188 men and 7,852 women, age 45–64 years | Up to 7 years | Leisure time PA and occupational PA indices based on average frequency of activities | 320 cases | Age, race, study center, education, smoking, alcohol, hormone replacement therapy (women), diabetes, waist/hip ratio, cholesterol, blood pressure, anti-hypertensive medication use, fibrinogen. |
| Manson et al. [19] | USA | 72,488 women, age 40–65 years | 8 years | Leisure time PA score based on average time of activities, and expressed as energy expenditure | 645 cases | Age, period during the study, smoking, BMI, menopausal status, parental history of myocardial infarction, vitamin-supplement, alcohol, history of hypertension, diabetes, hypercholesterolemia, and aspirin use |
| Kaprio et al. [20] | Finland | 8,205 twin men, age 25–69 years | Up to 20 years | Leisure time PA score based on average frequency, duration, and intensity of activities, and expressed as energy expenditure | 723 cases | Age, BMI, smoking, hypertension, diabetes |
| Lee et al. [21] | USA | 7,307 men, mean age 66.1 years | 5 years | Leisure time PA score based on average frequency and duration of activities, and expressed as energy expenditure | 482 cases | Age, duration per exercise episode, smoking, hypertension, diabetes, early parental death, vitamin/mineral supplements, alcohol, red meat and vegetable consumption, participation in vigorous activities |
| Sesso et al. [22] | USA | 12,516 men, mean age 57.7 years | Up to 16 years | Leisure time PA score based on average frequency and duration of activities, and expressed as energy expenditure | 2,135 cases | Age, BMI, alcohol, hypertension, diabetes, smoking, early parental death |
| Lee et al. [23] | USA | 39,372 healthy women, age 45 years or older | Average 5 years | Leisure time PA score based on average time of activities, and expressed as energy expenditure | 244 cases | Age, smoking, alcohol, diet, menopausal status, use of postmenopausal hormones, and parental history of early myocardial infarction |
| Lee et al. [24] | USA | 7,337 men, mean age 66 years | Average 5.3 years | Leisure time PA score based on average frequency, duration, and intensity of activities, and expressed as energy expenditure | 551 cases | Age, smoking; alcohol, red meat, vegetables, early parental mortality, BMI, history of hypertension, cholesterol, and diabetes |
| Conroy et al. [25] | USA | 37,169 healthy women, age 45 years or older | Average 9 years | Leisure time PA score based on average time of activities, and expressed as energy expenditure | 477 cases | Age, smoking, alcohol, diet, use of hormone therapy, menopausal status, and family history of CHD |
| Li et al. [26] | USA | 88,393 women, age 34–59 years | 20 years | Leisure time PA index based on average time of activities | 2,358 cases | Age, smoking, parental history of CHD, postmenopausal status and hormone use, aspirin use, alcohol consumption, and BMI |
| Hu et al. [27] | Finland | 47,840 men and women, age 25–64 years | 18.9 years | Leisure time PA and occupational PA indices based on average intensity of activities | 4,660 case | Age, BMI, blood pressure, cholesterol, education, alcohol, smoking, history of diabetes |
| Weinstein et al. [28] | USA | 38,987 women, age 45 years or older | 10.9 years | Leisure time PA score based on average time of activities, and expressed as energy expenditure | 948 cases | Age, parental history of myocardial infarction, alcohol, smoking, use of hormone therapy, and dietary factors |
| Stroke | ||||||
| Wannamethee et al. [29] | UK | 5,694 men, age 40–59 years | Up to 9.5 years | Leisure time PA score based on average frequency, duration, and intensity of activities, and expressed as energy expenditure | 68 cases | Age, smoking, BMI, social class, drinking |
| Kiely et al. [30] | USA | 3,258 men and 4,161 women, mean age 55 years | Up to 32 years | Leisure time PA index based on average time of activities | 680 cases | Age, occupation, blood pressure, smoking, cholesterol, total vital capacity, BMI, glucose intolerance, atrial fibrillation, left ventricular hypertrophy, valvular disease, history of congestive heart failure and ischemic heart disease |
| Lee et al. [31] | USA | 11,130 men, mean age 58 years | Up to 13 years | Leisure time PA score based on average frequency and duration of activities, and expressed as energy expenditure | 378 cases | Age, smoking, alcohol, early parental death |
| Lee et al. [32] | USA | 21,823 men, age 40–84 years | 11.1 years | Leisure time PA index based on average frequency of vigorous exercise | 533 cases | Age, smoking, alcohol, BMI, history of hypertension, high cholesterol, diabetes, angina, parental history of early myocardial infarction |
| Hu et al. [33] | USA | 72,488 women, age 40–65 years | 8 years | Leisure time PA score based on average time of activities, and expressed as energy expenditure | 258 cases | Age, smoking, BMI, menopausal status, parental history of early myocardial infarction, alcohol, aspirin, history of hypertension, diabetes, or hypercholesterolemia |
| Hu et al. [34] | Finland | 47,721 men and women, age 25–64 years | 19 years | Leisure time PA and occupational PA indices based on average intensity of activities | 2,863 case | Age, area, study year, BMI, blood pressure, cholesterol, education, smoking, alcohol, diabetes |
| Myint et al. [35] | UK | 22,602 men and women, age 40–79 years | 8.6 years | Combined leisure time PA and occupational PA index based on average time and intensity of activities | 361 cases | Age, blood pressure, BMI, cholesterol, smoking, history of diabetes |
| Williams [36] | USA | 29,279 men and 12,123 women, mean age 44.8 years for men and 38.9 for women | 7.7 years | Running distance | 119 cases | Age, smoking |
| Sattelmair et al. [37] | USA | 39,315 healthy women, age ≥ 45 years | 11.9 years | Leisure time PA score based on average time of activities, and expressed as energy expenditure | 579 cases | Age, smoking, alcohol, diet, menopausal status, parental history of myocardial infarction, migraine aura, BMI, history of diabetes, elevated cholesterol, hypertension |
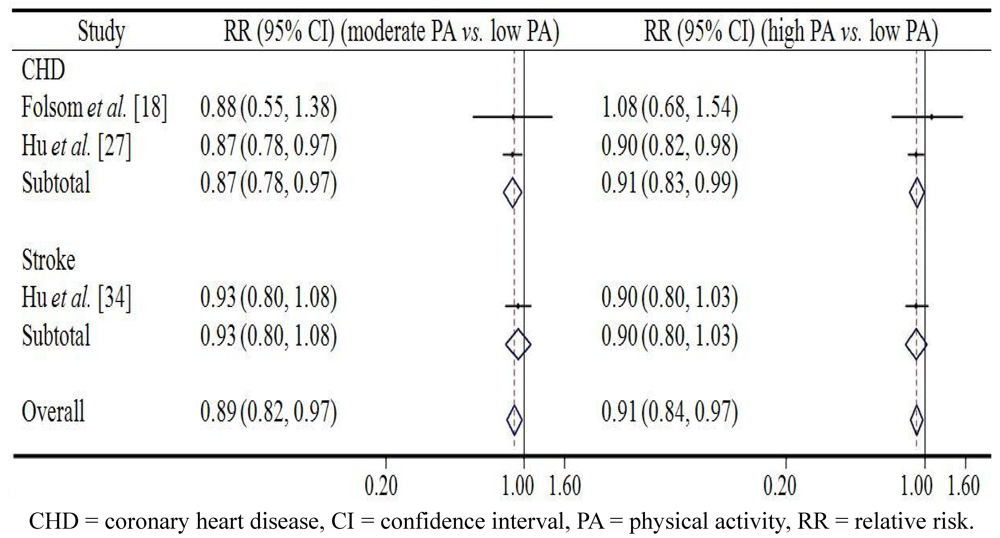
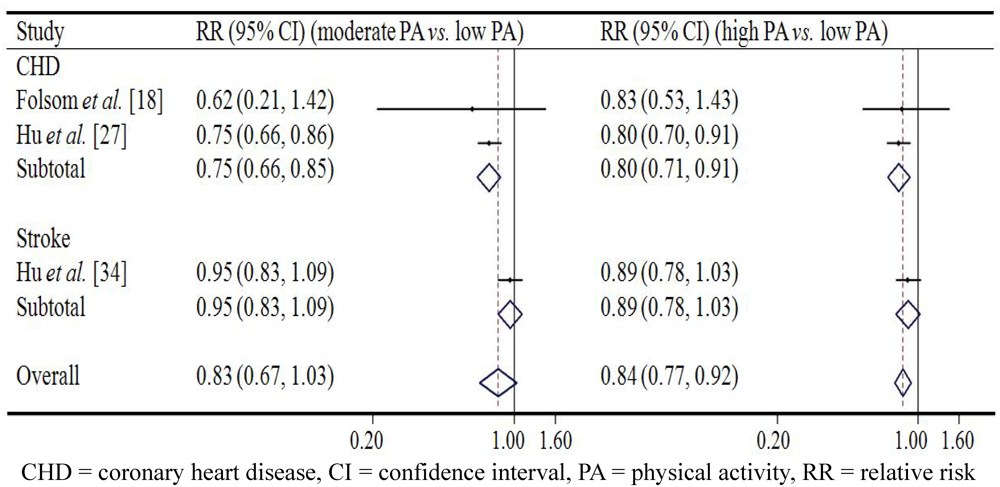
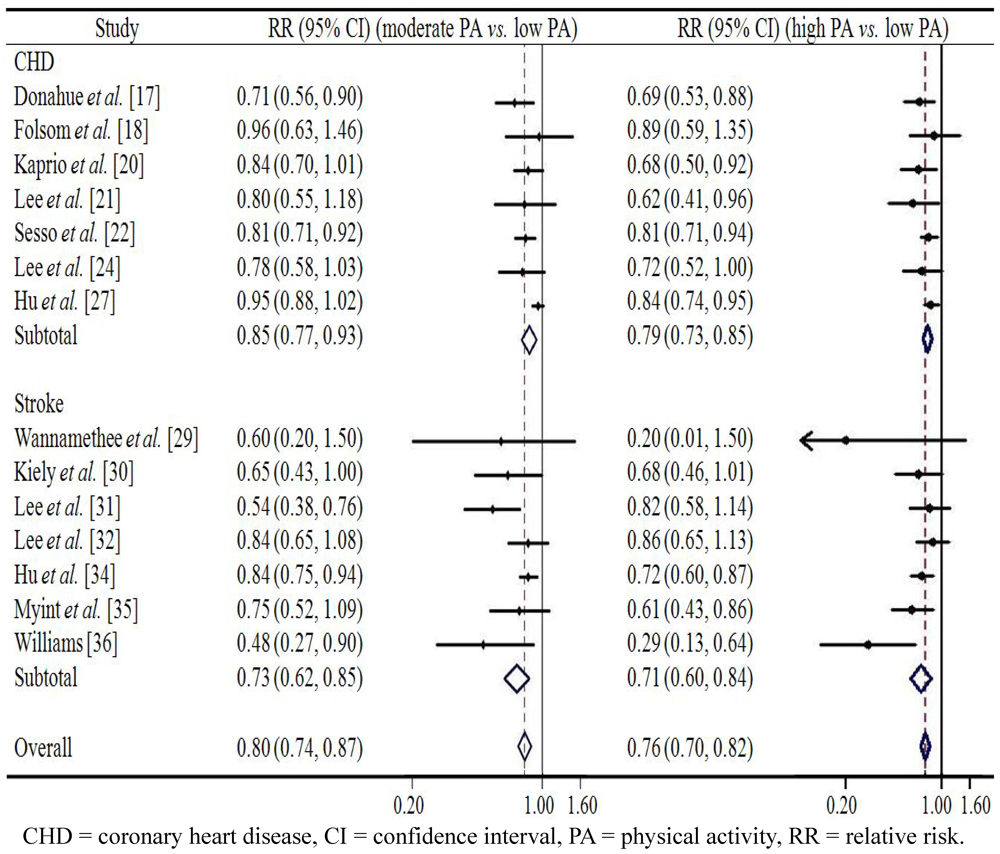
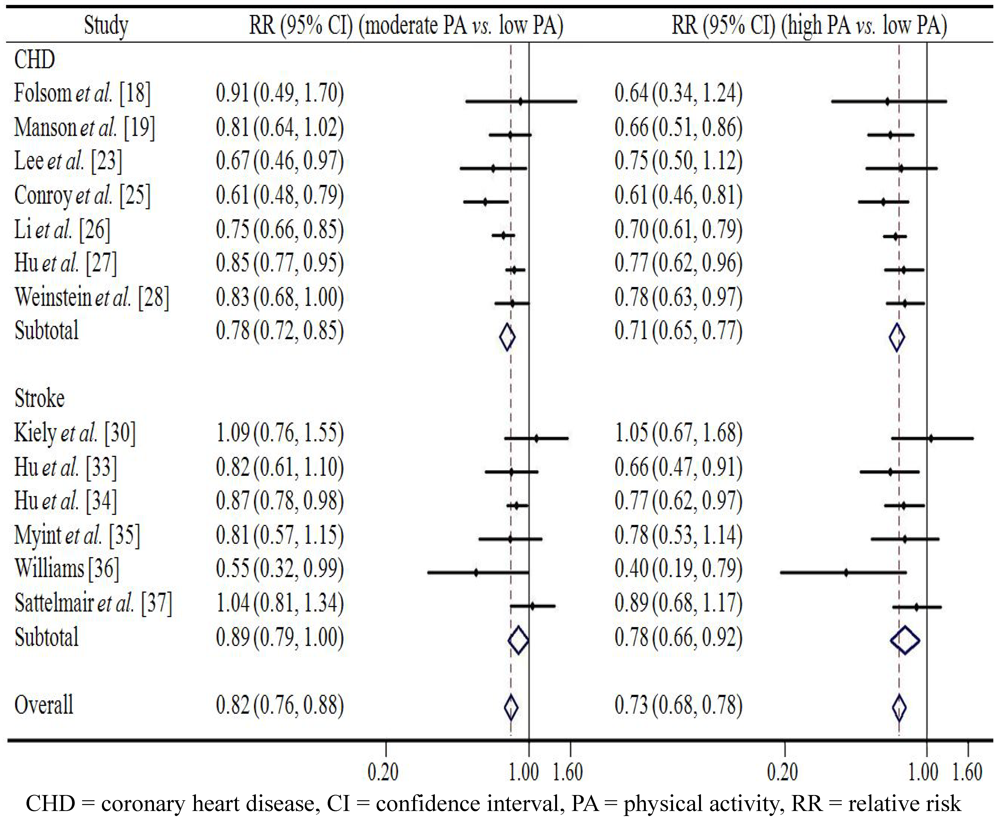
4. Discussion
Acknowledgments
Conflict of Interest
References
- Yusuf, S.; Reddy, S.; Ounpuu, S.; Anand, S. Global burden of cardiovascular diseases: Part I: General considerations, the epidemiologic transition, risk factors, and impact of urbanization. Circulation 2001, 104, 2746–2753. [Google Scholar] [CrossRef]
- Smith, S.C., Jr. Reducing the global burden of ischemic heart disease and stroke: A challenge for the cardiovascular community and the United Nations. Circulation 2011, 124, 278–279. [Google Scholar]
- Sofi, F.; Capalbo, A.; Cesari, F.; Abbate, R.; Gensini, G.F. Physical activity during leisure time and primary prevention of coronary heart disease: An updated meta-analysis of cohort studies. Eur. J. Cardiovasc. Prev. Rehabil. 2008, 15, 247–257. [Google Scholar]
- O’Donovan, G.; Blazevich, A.J.; Boreham, C.; Cooper, A.R.; Crank, H.; Ekelund, U.; Fox, K.R.; Gately, P.; Giles-Corti, B.; Gill, J.M.; et al. The ABC of physical activity for health: A consensus statement from the British Association of Sport and Exercise Sciences. J. Sports Sci. 2010, 28, 573–591. [Google Scholar] [CrossRef]
- Wendel-Vos, G.C.; Schuit, A.J.; Feskens, E.J.; Boshuizen, H.C.; Verschuren, W.M.; Saris, W.H.; Kromhout, D. Physical activity and stroke. A meta-analysis of observational data. Int. J. Epidemiol. 2004, 33, 787–798. [Google Scholar] [CrossRef]
- Goldstein, L.B. Physical activity and the risk of stroke. Expert Rev. Neurother. 2010, 10, 1263–1265. [Google Scholar]
- Shiroma, E.J.; Lee, I.M. Physical activity and cardiovascular health: Lessons learned from epidemiological studies across age, gender, and race/ethnicity. Circulation 2010, 122, 743–752. [Google Scholar] [CrossRef]
- Diep, L.; Kwagyan, J.; Kurantsin-Mills, J.; Weir, R.; Jayam-Trouth, A. Association of physical activity level and stroke outcomes in men and women: A meta-analysis. J. Womens Health (Larchmt) 2010, 19, 1815–1822. [Google Scholar] [CrossRef]
- Howley, E.T. Type of activity: Resistance, aerobic and leisure versus occupational physical activity. Med. Sci. Sports Exerc. 2001, 33, S364–S369. [Google Scholar] [CrossRef]
- Holtermann, A.; Hansen, J.V.; Burr, H.; Søgaard, K.; Sjøgaard, G. The health paradox of occupational and leisure-time physical activity. Br. J. Sports Med. 2012, in press. [Google Scholar]
- Carnethon, M.R. Physical activity and cardiovascular disease: How much is enough? Am. J. Lifestyle Med. 2009, 3, S44–S49. [Google Scholar] [CrossRef]
- Stroup, D.F.; Berlin, J.A.; Morton, S.C.; Olkin, I.; Williamson, G.D.; Rennie, D.; Moher, D.; Becker, B.J.; Sipe, T.A.; Thacker, S.B. Meta-analysis of observational studies in epidemiology: A proposal for reporting. Meta-analysis of Observational Studies in Epidemiology (MOOSE) group. J. Am. Med. Assoc. 2000, 283, 2008–2012. [Google Scholar]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G. PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. J. Clin. Epidemiol. 2009, 62, 1006–1012. [Google Scholar]
- Knapp, G.; Biggerstaff, B.J.; Hartung, J. Assessing the amount of heterogeneity in random-effects meta-analysis. Biom. J. 2006, 48, 271–285. [Google Scholar]
- Begg, C.B.; Mazumdar, M. Operating characteristics of a rank correlation test for publication bias. Biometrics 1994, 50, 1088–1101. [Google Scholar]
- Sterne, J. Meta-Analysis in STATA: An Updated Collection from the Stata Journal; Stata Press: College Station, TX, USA, 2009; pp. 1–259. [Google Scholar]
- Donahue, R.P.; Abbott, R.D.; Reed, D.M.; Yano, K. Physical activity and coronary heart disease in middle-aged and elderly men: The Honolulu Heart Program. Am. J. Public Health 1988, 78, 683–685. [Google Scholar]
- Folsom, A.R.; Arnett, D.K.; Hutchinson, R.G.; Liao, F.; Clegg, L.X.; Cooper, L.S. Physical activity and incidence of coronary heart disease in middle-aged women and men. Med. Sci. Sports Exerc. 1997, 29, 901–909. [Google Scholar]
- Manson, J.E.; Hu, F.B.; Rich-Edwards, J.W.; Colditz, G.A.; Stampfer, M.J.; Willett, W.C.; Speizer, F.E.; Hennekens, C.H. A prospective study of walking as compared with vigorous exercise in the prevention of coronary heart disease in women. N. Engl. J. Med. 1999, 341, 650–658. [Google Scholar]
- Kaprio, J.; Kujala, U.M.; Koskenvuo, M.; Sarna, S. Physical activity and other risk factors in male twin-pairs discordant for coronary heart disease. Atherosclerosis 2000, 150, 193–200. [Google Scholar]
- Lee, I.M.; Sesso, H.D.; Paffenbarger, R.S., Jr. Physical activity and coronary heart disease risk in men: Does the duration of exercise episodes predict risk? Circulation 2000, 102, 981–986. [Google Scholar]
- Sesso, H.D.; Paffenbarger, R.S., Jr.; Lee, I.M. Physical activity and coronary heart disease in men: The Harvard Alumni Health Study. Circulation 2000, 102, 975–980. [Google Scholar]
- Lee, I.M.; Rexrode, K.M.; Cook, N.R.; Manson, J.E.; Buring, J.E. Physical activity and coronary heart disease in women: Is “no pain, no gain” passé? J. Am. Med. Assoc. 2001, 285, 1447–1454. [Google Scholar] [CrossRef]
- Lee, I.M.; Sesso, H.D.; Oguma, Y.; Paffenbarger, R.S., Jr. Relative intensity of physical activity and risk of coronary heart disease. Circulation 2003, 107, 1110–1116. [Google Scholar]
- Conroy, M.B.; Cook, N.R.; Manson, J.E.; Buring, J.E.; Lee, I.M. Past physical activity, current physical activity, and risk of coronary heart disease. Med. Sci. Sports Exerc. 2005, 37, 1251–1256. [Google Scholar]
- Li, T.Y.; Rana, J.S.; Manson, J.E.; Willett, W.C.; Stampfer, M.J.; Colditz, G.A.; Rexrode, K.M.; Hu, F.B. Obesity as compared with physical activity in predicting risk of coronary heart disease in women. Circulation 2006, 113, 499–506. [Google Scholar]
- Hu, G.; Jousilahti, P.; Borodulin, K.; Barengo, N.C.; Lakka, T.A.; Nissinen, A.; Tuomilehto, J. Occupational, commuting and leisure-time physical activity in relation to coronary heart disease among middle-aged Finnish men and women. Atherosclerosis 2007, 194, 490–497. [Google Scholar]
- Weinstein, A.R.; Sesso, H.D.; Lee, I.M.; Rexrode, K.M.; Cook, N.R.; Manson, J.E.; Buring, J.E.; Gaziano, J.M. The joint effects of physical activity and body mass index on coronary heart disease risk in women. Arch. Intern. Med. 2008, 168, 884–890. [Google Scholar]
- Wannamethee, G.; Shaper, A.G. Physical activity and stroke in British middle aged men. BMJ 1992, 304, 597–601. [Google Scholar]
- Kiely, D.K.; Wolf, P.A.; Cupples, L.A.; Beiser, A.S.; Kannel, W.B. Physical activity and stroke risk: The Framingham Study. Am. J. Epidemiol. 1994, 140, 608–620. [Google Scholar]
- Lee, I.M.; Paffenbarger, R.S. Physical activity and stroke incidence. The Harvard Alumni Health Study. Stroke 1998, 29, 2049–2054. [Google Scholar] [CrossRef]
- Lee, I.M.; Hennekens, C.H.; Berger, K.; Buring, J.E.; Manson, J.E. Exercise and risk of stroke in male physicians. Stroke 1999, 30, 1–6. [Google Scholar]
- Hu, F.B.; Stampfer, M.J.; Colditz, G.A.; Ascherio, A.; Rexrode, K.M.; Willett, W.C.; Manson, J.E. Physical activity and risk of stroke in women. J. Am. Med. Assoc. 2000, 283, 2961–2967. [Google Scholar]
- Hu, G.; Sarti, C.; Jousilahti, P.; Silventoinen, K.; Barengo, N.C.; Tuomilehto, J. Leisure time, occupational, and commuting physical activity and the risk of stroke. Stroke 2005, 36, 1994–1999. [Google Scholar] [CrossRef]
- Myint, P.K.; Luben, R.N.; Wareham, N.J.; Welch, A.A.; Bingham, S.A.; Day, N.E.; Khaw, K.T. Combined work and leisure physical activity and risk of stroke in men and women in the European prospective investigation into Cancer-Norfolk Prospective Population Study. Neuroepidemiology 2006, 27, 122–129. [Google Scholar]
- Williams, P.T. Reduction in incident stroke risk with vigorous physical activity: Evidence from 7.7-year follow-up of the national runners’ health study. Stroke 2009, 40, 1921–1923. [Google Scholar] [CrossRef]
- Sattelmair, J.R.; Kurth, T.; Buring, J.E.; Lee, I.M. Physical activity and risk of stroke in women. Stroke 2010, 41, 1243–1250. [Google Scholar]
- U.S. Department of Health and Human Services. 2008 Physical Activity Guidelines for Americans. 2008. Available online: http://www.health.gov/PAGuidelines/pdf/paguide.pdf (accessed on 6 January 2012).
- Sattelmair, J.; Pertman, J.; Ding, E.L.; Kohl, H.W., 3rd; Haskell, W.; Lee, I.M. Dose response between physical activity and risk of coronary heart disease: A meta-analysis. Circulation 2011, 124, 789–795. [Google Scholar]
- Kohl, H.W., 3rd. Physical activity and cardiovascular disease: Evidence for a dose response. Med. Sci. Sports Exerc. 2001, 33, S472–S483. [Google Scholar]
- Kukkonen-Harjula, K. Physical activity and cardiovascular health-work and leisure differ. Scand. J. Work Environ. Health 2007, 33, 401–404. [Google Scholar]
- Karlqvist, L.K.; Härenstam, A.; Leijon, O.; Schéele, P. MOA Research Group. Excessive physical demands in modern worklife and characteristics of work and living conditions of persons at risk. Scand. J. Work Environ. Health 2003, 29, 363–377. [Google Scholar] [CrossRef]
- Mora, S.; Cook, N.; Buring, J.E.; Ridker, P.M.; Lee, I.M. Physical activity and reduced risk of cardiovascular events: Potential mediating mechanisms. Circulation 2007, 116, 2110–2118. [Google Scholar]
- Alevizos, A.; Lentzas, J.; Kokkoris, S.; Mariolis, A.; Korantzopoulos, P. Physical activity and stroke risk. Int. J. Clin. Pract. 2005, 59, 922–930. [Google Scholar]
- Bowles, D.K.; Laughlin, M.H. Mechanism of beneficial effects of physical activity on atherosclerosis and coronary heart disease. J. Appl. Physiol. 2011, 111, 308–310. [Google Scholar]
- Jakicic, J.M. The effect of physical activity on body weight. Obesity (Silver Spring) 2009, 17, S34–S38. [Google Scholar] [CrossRef]
- van Poppel, M.N.; Chinapaw, M.J.; Mokkink, L.B.; van Mechelen, W.; Terwee, C.B. Physical activity questionnaires for adults: A systematic review of measurement properties. Sports Med. 2010, 40, 565–600. [Google Scholar]
- Yusuf, S.; Reddy, S.; Ounpuu, S.; Anand, S. Global burden of cardiovascular diseases: Part II: Variations in cardiovascular disease by specific ethnic groups and geographic regions and prevention strategies. Circulation 2001, 104, 2855–2864. [Google Scholar]
- Kim, A.S.; Johnston, S.C. Global variation in the relative burden of stroke and ischemic heart disease. Circulation 2011, 124, 314–323. [Google Scholar]
- Dans, A.; Ng, N.; Varghese, C.; Tai, E.S.; Firestone, R.; Bonita, R. The rise of chronic non-communicable diseases in Southeast Asia: Time for action. Lancet 2011, 377, 680–689. [Google Scholar]
© 2012 by the authors; licensee MDPI, Basel, Switzerland. This article is an open-access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Li, J.; Siegrist, J. Physical Activity and Risk of Cardiovascular Disease—A Meta-Analysis of Prospective Cohort Studies. Int. J. Environ. Res. Public Health 2012, 9, 391-407. https://doi.org/10.3390/ijerph9020391
Li J, Siegrist J. Physical Activity and Risk of Cardiovascular Disease—A Meta-Analysis of Prospective Cohort Studies. International Journal of Environmental Research and Public Health. 2012; 9(2):391-407. https://doi.org/10.3390/ijerph9020391
Chicago/Turabian StyleLi, Jian, and Johannes Siegrist. 2012. "Physical Activity and Risk of Cardiovascular Disease—A Meta-Analysis of Prospective Cohort Studies" International Journal of Environmental Research and Public Health 9, no. 2: 391-407. https://doi.org/10.3390/ijerph9020391
APA StyleLi, J., & Siegrist, J. (2012). Physical Activity and Risk of Cardiovascular Disease—A Meta-Analysis of Prospective Cohort Studies. International Journal of Environmental Research and Public Health, 9(2), 391-407. https://doi.org/10.3390/ijerph9020391






