A Workplace Health Promotion Program for a Predominantly Military Population: Associations with General Health, Mental Well-Being and Sustainable Employability
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Population
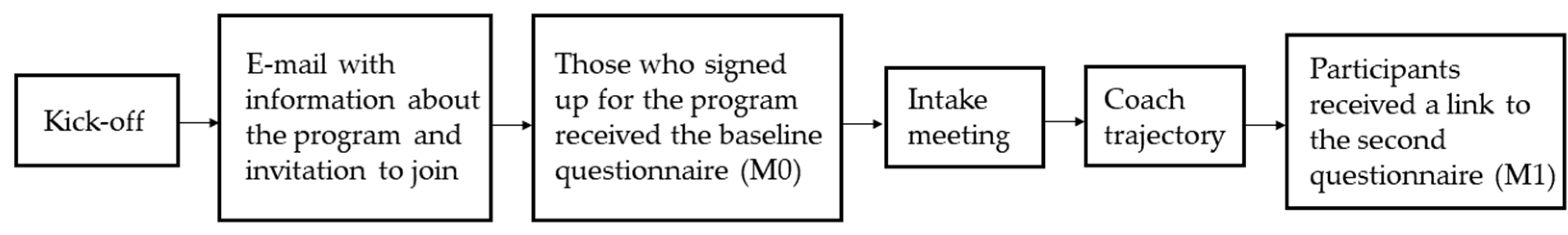
2.1.1. The Workplace Health Promotion Program
Kick-Off
Baseline Questionnaire
Intake Meeting
Coach Trajectory
The 6-Month Questionnaire
2.2. Measurements
2.2.1. Background
- Demographics: Age category (<35, 35–50, >50), sex (male, female), educational level (low, middle, high), rank (non-commissioned officer, subaltern officer, chief officer or higher), pay grade (low, middle, high), and form of employment (military, civilian, reserves, other) were measured.
- Goals set: Participants were given a range of goals and were asked to indicate for each goal whether this was a goal they had set for themselves (e.g., lose weight, improve diet, improve mental health).
- Goals reached: Participants were asked whether they had reached the goals that they had set for themselves, with the following answer categories: ‘completely reached goals that were set’, ‘almost reached the goals that were set’, ‘did not reach the goals that were set’, or ‘no goals were set’.
2.2.2. Health
- General health: The first item of the Short-Form Health Survey 12 (SF-12) “What do you think, in general, of your health?” was used, measured on a 5-point Likert scale ranging from 1 = poor to 5 = excellent, with higher scores indicating better general health [18].
- BMI: This was calculated based on self-reported height and weight (kg/m2).
2.2.3. Mental Well-Being
- Work engagement: A mean score of three items from the Utrecht Work Engagement Scale (UWES) was used. The items were measured on a five-point Likert scale ranging from 1 = never to 5 = always with higher scores indicating higher work engagement [19].
- Burn-out complaints: A mean score of four items from the Utrecht Burnout Scale (UBOS) was used. The items were measured on a five-point Likert scale ranging from 1 = never to 5 = always with higher scores indicating more burn-out complaints [20].
2.2.4. Sustainable Employability
- Recovery: As an indication of the ability to recover after work, a mean score of three items from the Demand-Induced Strain Recovery Questionnaire was used. The items were measured on a five-point Likert scale ranging from 1 = never to 5 = always, with higher scores indicating better ability to recover after work [21].
- Work-home balance: One item was used, namely “My work situation and home situation combine well”. This item was measured on a five-point Likert scale ranging from 1 = never to 5 = always with higher scores indicating a better work–home balance.
- Work ability: Work ability was defined as the degree to which employees can meet the demands of their work both physically and mentally. It was assessed with the first item of the Work Ability Index: “If during the best period of your life, your work ability would be graded a 10, how would you grade your current work ability?”, with scores ranging from 1 to 10 with higher scores indicating better work ability [22].
2.3. Statistical Analyses
3. Results
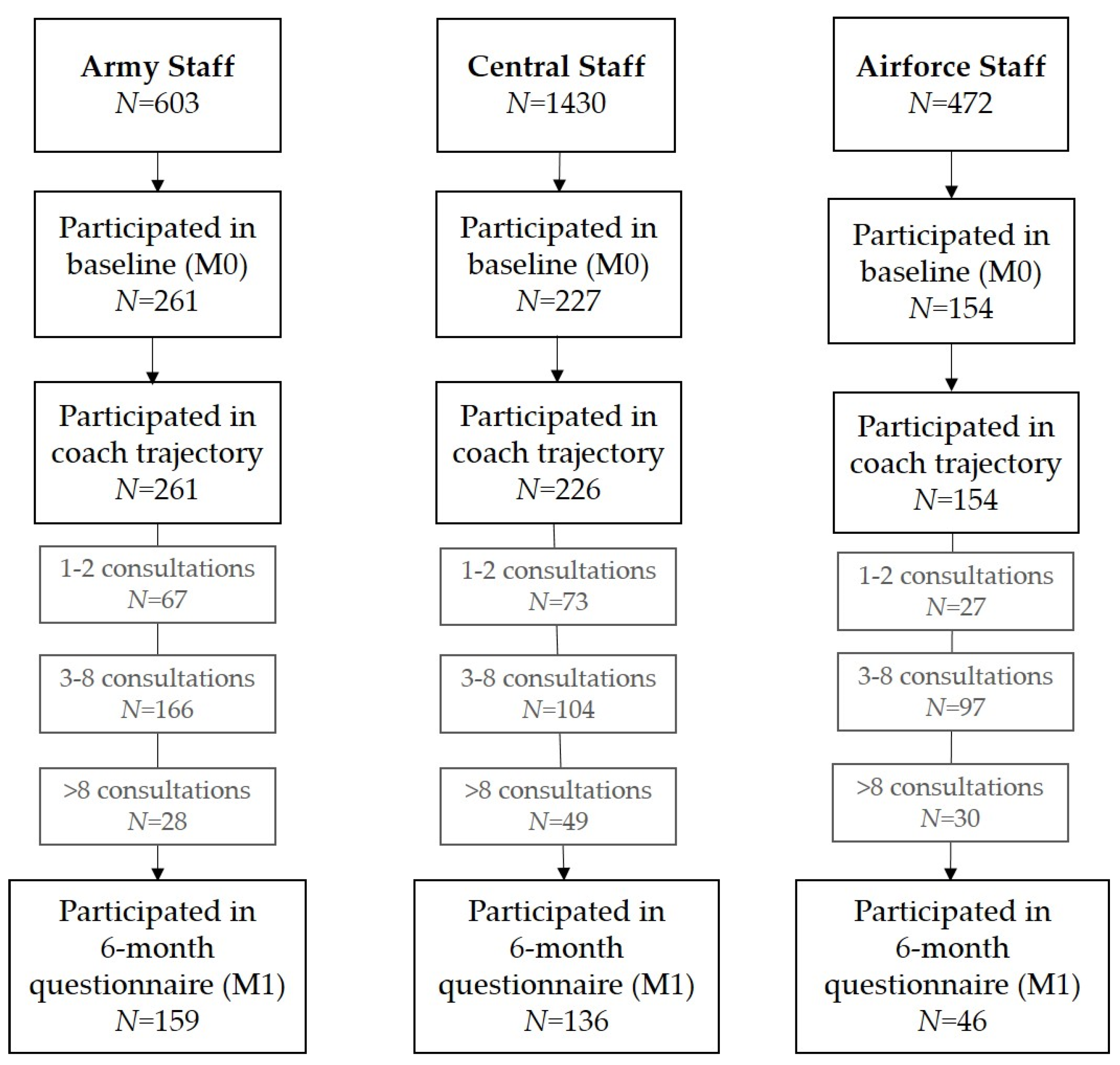
3.1. Response Rate
3.2. Sample Characteristics
3.3. Intervention Characteristics
3.4. Changes in Health, Mental Well-Being, and Sustainable Employability in 6 Months
3.5. Robustness of the Results
4. Discussion
Strengths and Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Correction Statement
Appendix A
- Fitness and operational readiness, using well-defined, scientifically validated training doctrines such as the Essentials of Tactical Strength and Conditioning by the US National Strength and Conditioning Association [33];
- Activities for health promotion and well-being, such as outdoor circuits for hiking, running or (mountain) biking; indoor lessons on yoga or spinning; social sports activities such as the Nijmeegse Vierdaagse (international 4-day walking event), the Invictus Games (international sports events for wounded, injured, and sick servicemen and women), and the Alpe d’Huzes (fund-raising cycling event for cancer at the French Alpe d’Huez);
- Basic motoric skill training in a rehabilitation context, in close co-operation with military health care professionals such as physical therapists and occupational physicians.
References
- Mathers, C.D.; Stevens, G.A.; Boerma, T.; White, R.A.; Tobias, M.I. Causes of international increases in older age life expectancy. Lancet 2015, 385, 540–548. [Google Scholar] [CrossRef] [PubMed]
- Ybema, J.F.; van Vuuren, T.; van Dam, K. HR practices for enhancing sustainable employability: Implementation, use, and outcomes. Int. J. Hum. Resour. Manag. 2020, 31, 886–907. [Google Scholar] [CrossRef]
- Van der Heijden, B.; De Vos, A. Sustainable careers: Introductory chapter. In Handbook of Research on Sustainable Careers; Edward Elgar Publishing Limited: Cheltenham, UK, 2015; Volume 1, pp. 1–19. [Google Scholar]
- Pinkstaff, S.O.; McNeil, A.; Arena, R.; Cahalin, L. Healthy living medicine in the workplace: More work to do. Prog. Cardiovasc. Dis. 2017, 59, 440–447. [Google Scholar] [CrossRef] [PubMed]
- Rongen, A.; Robroek, S.J.; van Lenthe, F.J.; Burdorf, A. Workplace health promotion: A meta-analysis of effectiveness. Am. J. Prev. Med. 2013, 44, 406–415. [Google Scholar] [CrossRef] [PubMed]
- Grimani, A.; Aboagye, E.; Kwak, L. The effectiveness of workplace nutrition and physical activity interventions in improving productivity, work performance and workability: A systematic review. BMC Public Health 2019, 19, 1676. [Google Scholar] [CrossRef] [PubMed]
- Schröer, S.; Haupt, J.; Pieper, C. Evidence-based lifestyle interventions in the workplace—An overview. Occup. Med. 2014, 64, 8–12. [Google Scholar] [CrossRef] [PubMed]
- Hulls, P.M.; Richmond, R.C.; Martin, R.M.; Chavez-Ugalde, Y.; de Vocht, F. Workplace interventions that aim to improve employee health and well-being in male-dominated industries: A systematic review. Occup. Environ. Med. 2022, 79, 77–87. [Google Scholar] [CrossRef] [PubMed]
- Marin-Farrona, M.; Wipfli, B.; Thosar, S.S.; Colino, E.; Garcia-Unanue, J.; Gallardo, L.; Felipe, J.L.; López-Fernández, J. Effectiveness of worksite wellness programs based on physical activity to improve workers’ health and productivity: A systematic review. Syst. Rev. 2023, 12, 87. [Google Scholar] [CrossRef] [PubMed]
- Larsen, L.T. Not merely the absence of disease: A genealogy of the WHO’s positive health definition. Hist. Hum. Sci. 2022, 35, 111–131. [Google Scholar] [CrossRef]
- Damen, M.A.; Detaille, S.I.; Robroek, S.J.W.; Engels, J.A.; de Lange, A.H. Factors associated with blue-collar workers’ participation in Worksite Health Promotion Programs: A scoping literature review. Health Promot. Int. 2023, 38, daad052. [Google Scholar] [CrossRef]
- Proper, K.I.; Hildebrandt, V.H.; Van der Beek, A.J.; Twisk, J.W.; Van Mechelen, W. Effect of individual counseling on physical activity fitness and health: A randomized controlled trial in a workplace setting. Am. J. Prev. Med. 2003, 24, 218–226. [Google Scholar] [CrossRef] [PubMed]
- Heirich, M.A.; Foote, A.; Erfurt, J.C.; Konopka, B. Work-site physical fitness programs: Comparing the impact of different program designs on cardiovascular risks. J. Occup. Environ. Med. 1993, 35, 510–517. [Google Scholar]
- Mastellos, N.; Gunn, L.H.; Felix, L.M.; Car, J.; Majeed, A. Transtheoretical model stages of change for dietary and physical exercise modification in weight loss management for overweight and obese adults. Cochrane Database Syst. Rev. 2014, 2, CD008066. [Google Scholar] [CrossRef] [PubMed]
- Bosnjak, M.; Ajzen, I.; Schmidt, P. The theory of planned behavior: Selected recent advances and applications. Eur. J. Psychol. 2020, 16, 352. [Google Scholar] [CrossRef] [PubMed]
- Bus, K.; Peyer, K.L.; Bai, Y.; Ellingson, L.D.; Welk, G.J. Comparison of in-person and online motivational interviewing–based health coaching. Health Promot. Pract. 2018, 19, 513–521. [Google Scholar] [CrossRef] [PubMed]
- Newnham-Kanas, C.; Morrow, D.; Irwin, J.D. Motivational Coaching: A Functional Juxtaposition of Three Methods for Health Behaviour Change: Motivational Interviewing, Coaching, and Skilled Helping. Int. J. Evid. Based Coach. Mentor. 2010, 8, 27. [Google Scholar]
- Ware, J.E., Jr.; Kosinski, M.; Keller, S.D. A 12-Item Short-Form Health Survey: Construction of scales and preliminary tests of reliability and validity. Med. Care 1996, 34, 220–233. [Google Scholar] [CrossRef] [PubMed]
- Schaufeli, W. Van burnout naar bevlogenheid Werk en welbevinden in Nederland. M & O 2015, 69, 15–31. [Google Scholar]
- Schaufeli, W.B.; Van Dierendonck, D. Handleiding van de Utrechtse Burnout Schaal (UBOS); Manual Utrecht Burnout Scale; Swets Test Publishers: Lisse, The Netherlands, 2000; pp. 177–196. [Google Scholar]
- Bova, N.; De Jonge, J.; Guglielmi, D. The demand-induced strain compensation questionnaire: A cross-national validation study. Stress Health 2015, 31, 236–244. [Google Scholar] [CrossRef]
- Ilmarinen, J. The work ability index (WAI). Occup. Med. 2007, 57, 160. [Google Scholar] [CrossRef]
- Reif, J.; Chan, D.; Jones, D.; Payne, L.; Molitor, D. Effects of a workplace wellness program on employee health, health beliefs, and medical use: A randomized clinical trial. JAMA Intern. Med. 2020, 180, 952–960. [Google Scholar] [CrossRef]
- Pesis-Katz, I.; Norsen, L.; Singh, R. Employee Wellness Programs. JAMA Intern. Med. 2021, 181, 291–292. [Google Scholar] [CrossRef]
- Hammer, L.B.; Brady, J.M.; Brossoit, R.M.; Mohr, C.D.; Bodner, T.E.; Crain, T.L.; Brockwood, K.J. Effects of a Total Worker Health® leadership intervention on employee well-being and functional impairment. J. Occup. Health Psychol. 2021, 26, 582. [Google Scholar] [CrossRef] [PubMed]
- Arnold, K.A. Transformational leadership and employee psychological well-being: A review and directions for future research. J. Occup. Health Psychol. 2017, 22, 381. [Google Scholar] [CrossRef] [PubMed]
- Gurt, J.; Schwennen, C.; Elke, G. Health-specific leadership: Is there an association between leader consideration for the health of employees and their strain and well-being? Work Stress 2011, 25, 108–127. [Google Scholar] [CrossRef]
- Bogaers, R.; Geuze, E.; van Weeghel, J.; Leijten, F.; van de Mheen, D.; Rüsch, N.; Rozema, A.; Brouwers, E. Workplace mental health disclosure, sustainable employability and well-being at work: A cross-sectional study among military personnel with mental illness. J. Occup. Rehabil. 2023, 33, 399–413. [Google Scholar] [CrossRef]
- Soeters, J.L.; Winslow, D.J.; Weibull, A. Military Culture. In Handbook of the Sociology of the Military; Kluwer: New York, NY, USA, 2003; pp. 237–254. [Google Scholar]
- Bensa, K.; Širok, K. Is It Time to Re-Shift the Research Agenda? A Scoping Review of Participation Rates in Workplace Health Promotion Programs. Int. J. Environ. Res. Public Health 2023, 20, 2757. [Google Scholar] [CrossRef]
- Sharp, M.-L.; Fear, N.T.; Rona, R.J.; Wessely, S.; Greenberg, N.; Jones, N.; Goodwin, L. Stigma as a barrier to seeking health care among military personnel with mental health problems. Epidemiol. Rev. 2015, 37, 144–162. [Google Scholar] [CrossRef] [PubMed]
- Bogaers, R.; Geuze, E.; Greenberg, N.; Leijten, F.; Varis, P.; van Weeghel, J.; van de Mheen, D.; Rozema, A.; Brouwers, E. Seeking treatment for mental illness and substance abuse: A cross-sectional study on attitudes, beliefs, and needs of military personnel with and without mental illness. J. Psychiatr. Res. 2022, 147, 221–231. [Google Scholar] [CrossRef]
- Alver, B.A.; Sell, K.; Deuster, P.A. NSCA’s Essentials of Tactical Strength and Conditioning; Human Kinetics: Champaign, IL, USA, 2017. [Google Scholar]
- de Korte, J.Q.; Veenstra, B.J.; van Rijswick, M.; Derksen, E.J.; Hopman, M.T.; Bongers, C.C.; Eijsvogels, T.M. A Heart Rate Based Algorithm to Estimate Core Temperature Responses in Elite Athletes Exercising in the Heat. Front. Sports Act. Living 2022, 4, 882254. [Google Scholar] [CrossRef]
- Brickwood, K.-J.; Watson, G.; O’Brien, J.; Williams, A.D. Consumer-based wearable activity trackers increase physical activity participation: Systematic review and meta-analysis. JMIR Mhealth Uhealth 2019, 7, e11819. [Google Scholar] [CrossRef]
- Tang, M.S.S.; Moore, K.; McGavigan, A.; Clark, R.A.; Ganesan, A.N. Effectiveness of wearable trackers on physical activity in healthy adults: Systematic review and meta-analysis of randomized controlled trials. JMIR Mhealth Uhealth 2020, 8, e15576. [Google Scholar] [CrossRef] [PubMed]
- Ferguson, T.; Olds, T.; Curtis, R.; Blake, H.; Crozier, A.J.; Dankiw, K.; Dumuid, D.; Kasai, D.; O’Connor, E.; Virgara, R.; et al. Effectiveness of wearable activity trackers to increase physical activity and improve health: A systematic review of systematic reviews and meta-analyses. Lancet Digit. Health 2022, 4, e615–e626. [Google Scholar] [CrossRef]
| Total Sample N = 341 | Army Staff Sample N = 159 | Army Staff N = 603 | Central Staff Sample N = 136 | Central Staff N = 1430 | Airforce Staff Sample N = 46 | Airforce Staff N = 472 | ||
|---|---|---|---|---|---|---|---|---|
| Sex (N = 340) | Male | 209 (61.5%) | 111 (69.8%) | 479 (79%) | 75 (55.2%) | 998 (70%) | 23 (51.1%) | 357 (75.6%) |
| Female | 131 (38.5%) | 48 (30.2%) | 124 (21%) | 61 (44.8%) | 432 (30%) | 22 (48.9%) | 115 (24.4%) | |
| Age | <35 | 42 (12.3%) | 15 (9.4%) | 56 (9%) | 17 (12.5%) | 234 (16%) | 10 (21.7%) | 91 (19.2%) |
| 35–50 | 161 (37.2%) | 69 (43.4) | 227 (38%) | 73 (53.7%) | 571 (40%) | 19 (41.3%) | 196 (41.5%) | |
| >50 | 138 (40.5%) | 75 (47.2%) | 320 (53%) | 46 (33.8%) | 628 (44%) | 17 (37.0%) | 188 (39.8%) | |
| Education * | Low and middle | 203 (59.5%) | 112 (70.5%) | - | 59 (43.4%) | - | 32 (69.6%) | - |
| High | 138 (40.5%) | 47 (29.5%) | - | 77 (56.6%) | - | 14 (30.4%) | - | |
| Rank (N = 187) | Non-commissioned officer | 21 (11.2%) | 12 (12.4%) | 49 (13%) | 6 (10.3%) | 62 (9%) | - | 51 (10.9%) |
| Subaltern officer | 32 (17.1%) | 14 (14.4%) | 71 (20%) | 8 (13.8%) | 85 (13%) | - | 25 (5.3%) | |
| Chief officer or higher | 134 (71.7%) | 71 (73.2%) | 242 (67%) | 44 (75.9%) | 526 (78%) | 19 (59.4%) | 299 (79.7%) | |
| Pay grade (N = 150) | Low (1-7) | 24 (16%) | 17 (27.9%) | 53 (22%) | - | 70 (9%) | - | 21 (21.6%) |
| Middle (8-10) | 23 (15.3%) | 8 (13.1%) | 56 (24%) | - | 130 (13%) | - | 34 (35.1%) | |
| High (11-18) | 103 (68.7%) | 36 (59%) | 127 (54%) | 63 (81.8%) | 560 (74%) | - | 42 (43.3%) | |
| Occupation | Military service member | 176 (51.6%) | 87 (54.7%) | 367 (61%) | 57 (41.9%) | 637 (44.5%) | 32 (69.5%) | 375 (79.4%) |
| Civilian service member | 150 (44.0%) | 60 (37.7%) | 236 (39%) | 77 (56.6%) | 757 (53%) | 13 (28.3%) | 97 (20.6%) | |
| Reserves/other | 15 (4.4%) | 12 (7.5%) | 0 (0%) | 2 (1.5%) | 36 (2.5%) | 1 (2.2%) | 0 (0%) |
| The Intervention Duration | Median | P25 | P75 |
|---|---|---|---|
| Duration of consultations (minutes) (N = 338) | 53 | 47 | 60 |
| Length of the coaching trajectory (days) (N = 255) | 196 | 135 | 316 |
| Number of consultations (N = 341) | 6 | 4 | 9 |
| Goals set | N | (%) | |
| Lose weight | 130 | 38.1 | |
| Improve diet | 85 | 24.9 | |
| Improve physical activity | 119 | 34.9 | |
| Improve lifestyle | 67 | 19.7 | |
| Improve sleep | 49 | 14.4 | |
| Improve work–life balance | 41 | 12.0 | |
| Improve energy | 47 | 13.8 | |
| Improve mental health | 87 | 25.5 | |
| Extent to which goals were reached | N | (%) | |
| Completely reached goals | 68 | 19.9 | |
| Almost reached the goals | 230 | 67.4 | |
| Did not reach the goals | 29 | 8.5 | |
| No goals were set | 14 | 4.1 | |
| M0 | M1 | Difference | |||
|---|---|---|---|---|---|
| M(SD) | Median | M(SD) | Median | Z | |
| Health | |||||
| General (1–5) | 3.05 (0.68) | 3.0 | 3.33 (0.73) | 3.0 | −7.338 ** |
| BMI (17.56–40.76) | 26.20 (3.70) | 25.59 | 25.75 (3.61) | 25.38 | −4.820 ** |
| Mental well-being | |||||
| Work engagement (1–5) | 3.48 (0.71) | 3.67 | 3.59 (0.70) | 3.67 | −3.344 * |
| Burn-out (1–3.75) | 1.77 (0.46) | 1.75 | 1.70 (0.50) | 1.75 | −2.707 * |
| Sustainable employability | |||||
| Recovery after work (1–5) | 2.76 (0.73) | 2.67 | 3.01 (0.70) | 3.0 | −6.889 ** |
| Work–home balance (1–5) | 4.17 (0.82) | 4.0 | 4.27 (0.69) | 4.0 | −2.307 * |
| Work ability (2–10) | 7.47 (1.27) | 8.0 | 7.79 (1.20) | 8.0 | −4.513 ** |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bogaers, R.; Sluik, D.; Helmhout, P.; Leijten, F. A Workplace Health Promotion Program for a Predominantly Military Population: Associations with General Health, Mental Well-Being and Sustainable Employability. Int. J. Environ. Res. Public Health 2024, 21, 625. https://doi.org/10.3390/ijerph21050625
Bogaers R, Sluik D, Helmhout P, Leijten F. A Workplace Health Promotion Program for a Predominantly Military Population: Associations with General Health, Mental Well-Being and Sustainable Employability. International Journal of Environmental Research and Public Health. 2024; 21(5):625. https://doi.org/10.3390/ijerph21050625
Chicago/Turabian StyleBogaers, Rebecca, Diewertje Sluik, Pieter Helmhout, and Fenna Leijten. 2024. "A Workplace Health Promotion Program for a Predominantly Military Population: Associations with General Health, Mental Well-Being and Sustainable Employability" International Journal of Environmental Research and Public Health 21, no. 5: 625. https://doi.org/10.3390/ijerph21050625
APA StyleBogaers, R., Sluik, D., Helmhout, P., & Leijten, F. (2024). A Workplace Health Promotion Program for a Predominantly Military Population: Associations with General Health, Mental Well-Being and Sustainable Employability. International Journal of Environmental Research and Public Health, 21(5), 625. https://doi.org/10.3390/ijerph21050625






