Digital Addiction Intervention for Children and Adolescents: A Scoping Review
Abstract
1. Introduction
1.1. Digital Addiction: A Global Health Problem
1.2. Digital Addiction Hurts Children and Adolescent Health
1.3. COVID-19 Exacerbated the Digital Addiction Problem
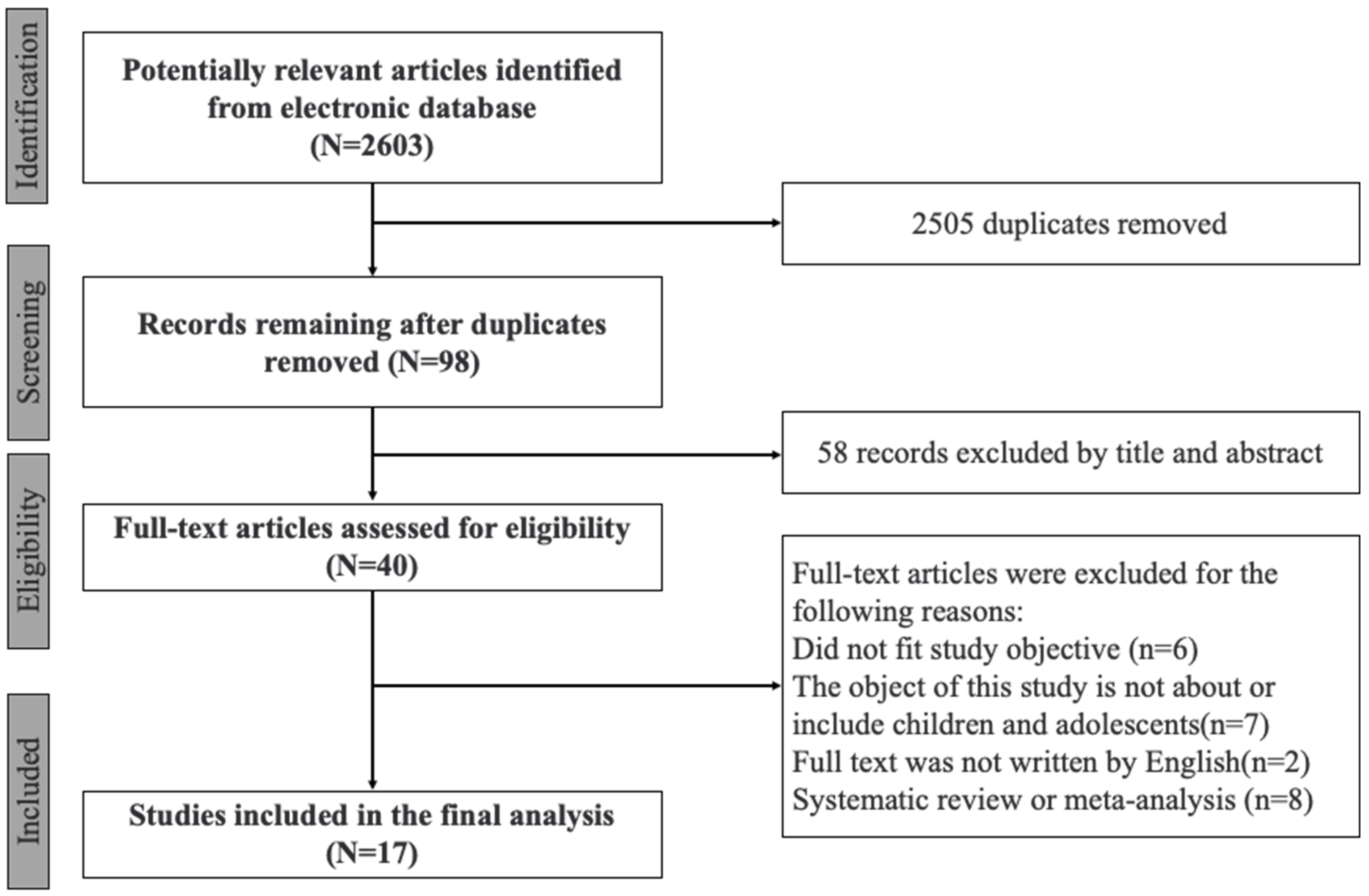
2. Methods
3. Results
3.1. Cognitive-Behavioral Therapy Intervention
3.2. CBT-Based Intervention
3.3. Family Intervention
3.4. Digital-Based Intervention
3.5. Other Interventions
4. Discussion
4.1. Five Types of DA Intervention Programs
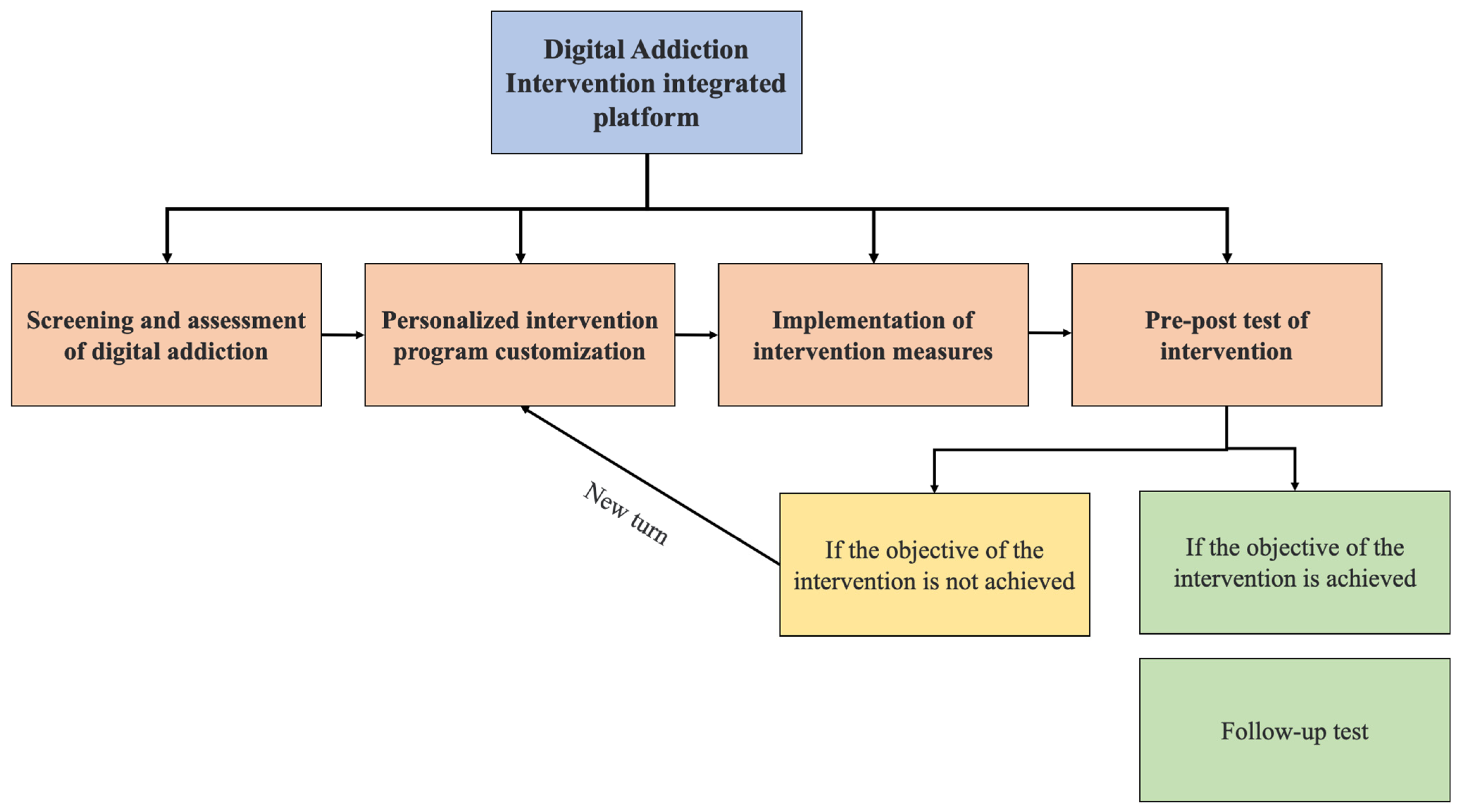
4.2. Digital Intervention to Cure Digital Addiction
4.3. Why Digital Intervention Is More Promising than Others
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Ali, R.; Jiang, N.; Phalp, K.; Muir, S.; McAlaney, J. The emerging requirement for digital addiction labels. In Proceedings of the 20th International Working Conference on Requirements Engineering: Foundation for Software Quality, Essen, Germany, 23–26 March 2015. [Google Scholar] [CrossRef]
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 5th ed.; APA: Washington, DC, USA, 2013. [Google Scholar]
- The World Health Organization. ICD-11—Mortality and Morbidity Statistics; The World Health Organization: Geneva, Switzerland, 2019. [Google Scholar]
- Cheng, C.; Li, A.Y.L. Internet addiction prevalence and quality of (real) life: A meta-analysis of 31 nations across seven world regions. Cyberpsychol. Behav. Soc. Netw. 2014, 17, 755–760. [Google Scholar] [CrossRef] [PubMed]
- Fam, J.Y. Prevalence of internet gaming disorder in adolescents: A meta-analysis across three decades. Scand. J. Psychol. 2018, 59, 524–531. [Google Scholar] [CrossRef]
- Hawi, N.S.; Samaha, M.; Griffiths, M.D. The digital addiction scale for children: Development and validation. Cyberpsychol. Behav. Soc. Netw. 2019, 22, 771–778. [Google Scholar] [CrossRef]
- Boniel-Nissim, M.; Sasson, H. Bullying victimization and poor relationships with parents as risk factors of problematic internet use in adolescence. Comput. Hum. Behav. 2018, 88, 176–183. [Google Scholar] [CrossRef]
- Niu, M.; Zhang, Y.; Zhou, J. A survey on the use of electronic devices by children aged 1-3 in Shanghai. Shanghai J. Educ. Res. 2018, 2, 56–60. [Google Scholar]
- Domingues-Montanari, S. Clinical and psychological effects of excessive screen time on children. J. Paediatr. Child Health 2017, 53, 333–338. [Google Scholar] [CrossRef]
- Laconi, S.; Pirès, S.; Chabrol, H. Internet gaming disorder, motives, game genres and psychopathology. Comput. Hum. Behav. 2017, 75, 652–659. [Google Scholar] [CrossRef]
- Hermawati, D.; Rahmadi, F.A.; Sumekar, T.A.; Winarni, T.I. Early electronic screen exposure and autistic-like symptoms. Intractable Rare Dis. Res. 2018, 7, 69–71. [Google Scholar] [CrossRef]
- Weinstein, A.; Dorani, D.; Elhadif, R.; Bukovza, Y.; Yarmulnik, A.; Dannon, P. Internet addiction is associated with social anxiety in young adults. Ann. Clin. Psychiatry 2015, 27, 4–9. [Google Scholar] [CrossRef]
- Cao, F.; Su, L. Internet addiction among Chinese adolescents: Prevalence and psychological features. Child Care Health Dev. 2007, 33, 275–281. [Google Scholar] [CrossRef]
- Li, H.; Wu, D.; Yang, J.; Luo, J.; Xie, S.; Chang, C. Tablet Use Affects Preschoolers’ Executive Function: fNIRS Evidence from the Dimensional Change Card Sort Task. Brain Sci. 2021, 11, 567. [Google Scholar] [CrossRef] [PubMed]
- Kabali, H.K.; Irigoyen, M.M.; Nunez-Davis, R.; Budacki, J.G.; Mohanty, S.H.; Leister, K.P. Exposure and use of mobile media devices by young children. Pediatrics 2015, 136, 1044–1050. [Google Scholar] [CrossRef] [PubMed]
- Domoff, S.E.; Harrison, K.; Gearhardt, A.N.; Gentile, D.A.; Lumeng, J.C.; Miller, A.L. Development and validation of the Problematic Media Use Measure: A parent report measure of screen media “addiction” in children. Psychol. Pop. Media Cult. 2019, 8, 2–11. [Google Scholar] [CrossRef] [PubMed]
- Beyens, I.; Nathanson, A.I. Electronic media use and sleep among preschoolers: Evidence for time-shifted and less consolidated sleep. Health Commun. 2019, 34, 537–544. [Google Scholar] [CrossRef]
- Han, X.; Wang, Y.; Jiang, W.; Bao, X.; Sun, Y.; Ding, W.; Cao, M.; Wu, X.; Du, Y.; Zhou, Y. Resting-state activity of prefrontal-striatal circuits in internet gaming disorder: Changes with cognitive behavior therapy and predictors of treatment response. Front. Psychiatry 2018, 9, 341. [Google Scholar] [CrossRef]
- Anitha, F.S.; Narasimhan, U.; Janakiraman, A.; Janakarajan, N.; Tamilselvan, P. Association of digital media exposure and addiction with child development and behavior: A cross-sectional study. Ind. Psychiatry J. 2021, 30, 265. [Google Scholar] [CrossRef]
- Liu, S.; Zhou, W.; Wang, J.; Chen, B.; He, G.; Jia, Y. Association between mobile phone addiction index and sugar-sweetened food intake in medical college students stratified by sex from Shanghai, China. Nutrients 2021, 13, 2256. [Google Scholar] [CrossRef]
- Uysal, G.; Balci, S. Evaluation of a School-Based Program for Internet Addiction of Adolescents in Turkey. J. Addict. Nurs. 2018, 29, 43–49. [Google Scholar] [CrossRef]
- Thompson, R.A.; Nelson, C.A. Developmental science and the media: Early brain development. Am. Psychol. 2001, 56, 5. [Google Scholar] [CrossRef]
- Hutton, J.S.; Dudley, J.; Horowitz-Kraus, T.; DeWitt, T.; Holland, S.K. Associations between screen-based media use and brain white matter integrity in preschool-aged children. JAMA Pediatr. 2020, 174, e193869. [Google Scholar] [CrossRef]
- Li, H.; Wu, D.; Yang, J.; Xie, S.; Luo, J.; Chang, C. U-Shape by Quadratic Equation: A Best-fit for Modelling Hemodynamic Changes in the DCCS Task. Preprints 2021, 2021070417. [Google Scholar]
- Zhang, X.; Zhang, J.; Zhang, K.; Ren, J.; Lu, X.; Wang, T.; Yang, H.; Guo, H.; Yuan, G.; Zhu, Z.; et al. Effects of different interventions on internet addiction: A meta-analysis of random controlled trials. J. Affect. Disord. 2022, 313, 56–71. [Google Scholar] [CrossRef]
- Vondráčková, P.; Gabrhelik, R. Prevention of Internet addiction: A systematic review. J. Behav. Addict. 2016, 5, 568–579. [Google Scholar] [CrossRef]
- Xu, L.-X.; Wu, L.-L.; Geng, X.-M.; Wang, Z.-L.; Guo, X.-Y.; Song, K.-R.; Liu, G.-Q.; Deng, L.-Y.; Zhang, J.-T.; Potenza, M.N. A review of psychological interventions for internet addiction. Psychiatry Res. 2021, 302, 114016. [Google Scholar] [CrossRef] [PubMed]
- Kuss, D.J.; Lopez-Fernandez, O. Internet addiction and problematic Internet use: A systematic review of clinical research. World J. Psychiatry 2016, 6, 143. [Google Scholar] [CrossRef]
- Arksey, H.; O’Malley, L. Scoping studies: Towards a methodological framework. Int. J. Soc. Res. Methodol. 2005, 8, 19–32. [Google Scholar] [CrossRef]
- Levac, D.; Colquhoun, H.; O’Brien, K.K. Scoping studies: Advancing the methodology. Implement. Sci. 2010, 5, 69. [Google Scholar] [CrossRef]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G.; the PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. Ann. Intern. Med. 2009, 151, 264–269. [Google Scholar] [CrossRef]
- Szász-Janocha, C.; Vonderlin, E.; Lindenberg, K. Treatment outcomes of a CBT-based group intervention for adolescents with Internet use disorders. J. Behav. Addict. 2021, 9, 978–989. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.H.; Yim, H.W.; Jo, S.J.; Jung, K.I.; Lee, K.; Park, M.H. The effects of group cognitive behavioral therapy on the improvement of depression and anxiety in adolescents with problematic Internet use. J. Korean Acad. Child Adolesc. Psychiatry 2018, 29, 73–79. [Google Scholar] [CrossRef]
- Pakpour, A.H.; Fazeli, S.; Zeidi, I.M.; Alimoradi, Z.; Georgsson, M.; Brostrom, A.; Potenza, N.M. Effectiveness of a mobile app-based educational intervention to treat internet gaming disorder among Iranian adolescents: Study protocol for a randomized controlled trial. Trials 2022, 23, 229. [Google Scholar] [CrossRef] [PubMed]
- Agbaria, Q. Cognitive behavioral intervention in dealing with Internet addiction among Arab teenagers in Israel. Int. J. Ment. Health Addict. 2022. [Google Scholar] [CrossRef] [PubMed]
- Bong, S.H.; Won, G.H.; Choi, T.Y. Effects of Cognitive-Behavioral Therapy Based Music Therapy in Korean Adolescents with Smartphone and Internet Addiction. Psychiatry Investig. 2021, 18, 110–117. [Google Scholar] [CrossRef] [PubMed]
- Kochuchakkalackal, G.; Reyes, M.E.S. Development and efficacy of acceptance and cognitive restructuring intervention program on the symptoms of internet gaming disorder and psychological well-being of adolescents: A pilot study. Int. J. Behav. Sci. 2019, 12, 141–145. [Google Scholar]
- Pornnoppadol, C.; Ratta-Apha, W.; Chanpen, S.; Wattananond, S.; Dumrongrungruang, N.; Thongchoi, K.; Panchasilawut, S.; Wongyuen, B.; Chotivichit, A.; Laothavorn, J.; et al. A comparative study of psychosocial interventions for internet gaming disorder among adolescents aged 13–17 years. Int. J. Ment. Health Addict. 2020, 18, 932–948. [Google Scholar] [CrossRef]
- Lindenberg, K.; Kindt, S.; Szász-Janocha, C. Effectiveness of Cognitive Behavioral Therapy–Based Intervention in Preventing Gaming Disorder and Unspecified Internet Use Disorder in Adolescents: A Cluster Randomized Clinical Trial. JAMA Netw. Open 2022, 5, e2148995. [Google Scholar] [CrossRef]
- Yang, S.Y.; Kim, H.S. Effects of a prevention program for internet addiction among middle school students in South Korea. Public Health Nurs. 2018, 35, 246–255. [Google Scholar] [CrossRef] [PubMed]
- Khoshgoftar, M.; Amidi Mazaheri, M.; Tarahi, M.J. The Effect of Educational Intervention Based on Health Belief Model to Decrease and Prevent Mobile Phone Addiction among Female High School Students in Iran. Int. J. Pediatr. 2019, 7, 10175–10187. [Google Scholar] [CrossRef]
- Torres-Rodriguez, A.; Griffiths, M.D.; Carbonell, X.; Oberst, U. Treatment efficacy of a specialized psychotherapy program for Internet Gaming Disorder. J. Behav. Addict. 2018, 7, 939–952. [Google Scholar] [CrossRef]
- Chau, C.L.; Tsui, Y.Y.Y.; Cheng, C. Gamification for internet gaming disorder prevention: Evaluation of a Wise IT-Use (WIT) Program for Hong Kong primary students. Front. Psychol. 2019, 10, 2468. [Google Scholar] [CrossRef]
- Lazarinis, F.; Alexandri, K.; Panagiotakopoulos, C.; Verykios, V.S. Sensitizing young children on internet addiction and online safety risks through storytelling in a mobile application. Educ. Inf. Technol. 2019, 25, 163–174. [Google Scholar] [CrossRef]
- Tseng, Y.H.; Chao, H.H.; Hung, C.L. Effect of a Strategic Physical Activity Program on Cognitive Flexibility among Children with Internet Addiction: A Pilot Study. Children 2022, 9, 798. [Google Scholar] [CrossRef] [PubMed]
- Gong, Y.; Gong, N.; Zhang, Z.; He, Y.; Tang, H. Effect of Narrative Therapy-Based Group Psychological Counseling on Internet Addiction among Adolescents. Iran. J. Public Health 2022, 51, 1331. [Google Scholar] [CrossRef] [PubMed]
- Field, T.A.; Beeson, E.T.; Jones, L.K. The new ABCs: A practitioner’s guide to neuroscience-informed cognitive-behavior therapy. J. Ment. Health Couns. 2015, 37, 206–220. [Google Scholar] [CrossRef]
- Young, K.S. Cognitive behavior therapy with Internet addicts: Treatment outcomes and implications. Cyberpsychol. Behav. 2007, 10, 671–679. [Google Scholar] [CrossRef]
- Malak, M.Z. Internet addiction and cognitive behavioral therapy. Cogn. Behav. Ther. Clin. Appl. 2018, 10, 183–199. [Google Scholar]
- Davis, R.A. A cognitive-behavioral model of pathological Internet use. Comput. Hum. Behav. 2001, 17, 187–195. [Google Scholar] [CrossRef]
- Young, K.S. Internet addiction: A new clinical phenomenon and its consequences. Am. Behav. Sci. 2004, 48, 402–415. [Google Scholar] [CrossRef]
- Young, K.S. CBT-IA: The first treatment model for internet addiction. J. Cogn. Psychother. 2011, 25, 304–312. [Google Scholar] [CrossRef]
- Malinauskas, R.; Malinauskiene, V. A meta-analysis of psychological interventions for Internet/smartphone addiction among adolescents. J. Behav. Addict. 2019, 8, 613–624. [Google Scholar] [CrossRef]
- Liu, Q.X.; Fang, X.Y.; Yan, N.; Zhou, Z.K.; Yuan, X.J.; Lan, J.; Liu, C.Y. Multi-family group therapy for adolescent Internet addiction: Exploring the underlying mechanisms. Addict. Behav. 2015, 42, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Yu, L.; Shek, D.T.L. Internet addiction in Hong Kong adolescents: A three-year longitudinal study. J. Pediatr. Adolesc. Gynecol. 2013, 26, S10–S17. [Google Scholar] [CrossRef] [PubMed]
- Ebert, D.D.; Zarski, A.C.; Christensen, H.; Stikkelbroek, Y.; Berking, M.; Riper, H. Internet and computer-based cognitive behavioral therapy for anxiety and depression in youth: A meta-analysis of randomized controlled outcome trials. PloS ONE 2015, 10, e0119895. [Google Scholar] [CrossRef]
- Young, K.S. Treatment outcomes using CBT-IA with Internet-addicted patients. J. Behav. Addict. 2013, 2, 209–215. [Google Scholar] [CrossRef]
- Gorowska, M.; Tokarska, K.; Zhou, X.; Gola, M.K.; Li, Y. Novel approaches for treating Internet Gaming Disorder: A review of technology-based interventions. Compr. Psychiatry 2022, 115, 152312. [Google Scholar] [CrossRef]
- Naslund, J.A.; Aschbrenner, K.A.; Araya, R.; Marsch, L.A.; Unützer, J.; Patel, V.; Bartels, S.J. Digital technology for treating and preventing mental disorders in low-income and middle-income countries: A narrative review of the literature. Lancet Psychiatry 2017, 4, 486–500. [Google Scholar] [CrossRef] [PubMed]
- Aboujaoude, E.; Gega, L.; Parish, M.B.; Hilty, D.M. Digital interventions in mental health: Current status and future directions. Front. Psychiatry 2022, 11, 111. [Google Scholar] [CrossRef]
- Bell, I.H.; Lim, M.H.; Rossell, S.L.; Thomas, N. Ecological momentary assessment and intervention in the treatment of psychotic disorders: A systematic review. Psychiatr. Serv. 2017, 68, 1172–1181. [Google Scholar] [CrossRef]
| Author /Year | Country | Addiction Type | Sample Size | Age (Years Old) | Participants’ Details | Assessment | Intervention | Control Group | Result | Limitations |
|---|---|---|---|---|---|---|---|---|---|---|
| Han et al., 2018 [18] | China | IGD | n = 26 | 16.81 ± 0.75 | meet the standards of the Diagnostic Questionnaire for Internet Addiction test | The Chen Internet Addiction Scale (CIAS); The Self-rating Anxiety Scale (SAS); The Self-rating Depression Scale (SDS); and The Barratt Impulsiveness Scale-11 (BIS-11) | CBT | / | CBT could regulate the abnormal low-frequency fluctuations in prefrontal–striatal regions in IGD subjects and improve IGD-related symptoms. | lack of control group; only males |
| Szász-Janocha et al., 2020 [32] | Germany | IUD | n = 54 | 13.48 ± 1.72 | self-reported or parent-reported excessive gaming or Internet use and who reported subjective psychological strain (self-selection) | The German Video Game Dependency Scale (CSAS); The compulsive internet use scale (CIUS); The Strengths and Difficulties Questionnaire; The Children’s Depression Inventory; The Social Interaction Anxiety Scale; The Fear Survey Schedule for Children-Revised; The German Questionnaire for Procrastination; The German Questionnaire for Assessment of Emotion; Regulation in Children and Adolescents; The German Student Assessment List for Social and Learning Behavior; The German General Self-Efficacy Scale | the PROTECT + program | / | Patients showed a significant reduction in IUD symptom severity at the 12-month follow up. Secondary outcome variables showed a significant reduction in self-reported depression, social anxiety, performance anxiety, and school anxiety, as well as in parental-reported general psychopathology | lack of control group; did not use objective inclusion criteria for study participation |
| Kim et al., 2018 [33] | South Korea | IA | n = 17 | 12–17 | screened for psychiatric disorders with the Mini International Neuropsychiatric Interview for Children and Adolescents (MINI-KID) | Korean Internet addiction self-report test (K-scale); Young’s Diagnostic Questionnaire (YDQ); Young’s Internet Addiction Scale (IAS); Children’s Depression Inventory (CDI); State-Trait Anxiety Inventory (STAI) | group CBT | / | After the program, the IAS, CDI, and SAI scores were lower than before. At the one-month follow-up assessment, the IAS scores remained low, and the CDI and SAI scores were even lower than after the program. | only implemented in two specific schools; no control group; self-report evaluation scales only; only voluntary participants with a willingness to decrease problematic Internet use participated in the study |
| Pakpour et al., 2022 [34] | Iran | IGD | n = 206 | 13–18 | scored 32 or higher on the nine-item Internet Gaming Disorder Scale—Short Form (IGDS-SF9) | Internet Gaming Disorder (IGDS-SF9); The Depression, Anxiety and Stress Scale (DASS-21); Insomnia Severity Index (ISI); Stages of Change Questionnaire (SOCQ); Decisional Balance Scale; and Self-efficacy Scale. | based on the TTM and CBT application (named HAPPYTEEN) | a sleep hygiene intervention via the app | This application intervention could be used as an adjunct therapy for adolescents with IGD. | lack of detailed results of the pre-post comparison |
| Agbaria, 2022 [35] | Israel | IA | E: n = 80 C: n = 80 | E: 13.45 ± 1.46; C: 13.91 ± 1.92 | high scores on Young’s (1998) Internet Addiction Test questionnaire | Adolescence Self-Control Scale; Internet Addiction Test (IAT) | CBT | Weekly classroom conversation | Higher levels of self-control were reported among the experimental group but not the control group, which contributed to a reduction in scores on the questionnaire assessing Internet addiction in the experimental group. | intervention time in after school hours; self-reporting questionnaires may be biased by reporting error, social desirability, or lack of insight into one’s behavior; did not examine individual differences, such as an adolescent’s level of impulsivity or executive functioning |
| Bong et al., 2021 [36] | South Korea | Smartphone and Internet Addiction | E: n = 67 C: n = 71 | 10–16 | classified as high-risk (>70) or problematic (>40) users based on Young Internet Addiction Scale (YIAT), or smartphone high-risk group based on Korean Smartphone Addiction Proneness Scale (SAPS) | Young Internet Addiction Scale (YIAT); Smartphone Addiction Proneness Scale (SAPS); State Anxiety Inventory for Children (SAIC); Trait Anxiety Inventory for Children (TAIC); Conners-Wells’ Adolescent Self-Report Scale-Short form (CASS(S)); Barratt Impulsiveness Scale-11 | CBT + Music therapy | CBT | Combined MT and CBT improved the symptoms of smartphone/internet addiction, anxiety, and impulsivity in adolescents. | the smartphone/internet addiction scales used in this study differed from the diagnostic criteria of internet gaming disorder in DSM-5 or gaming disorder in ICD-11; no follow up interventions |
| Kochuchakkalackal and Reyes, 2019 [37] | Philippines | IGD | n = 10 | 14–18 | have a high score in the IGD and a low score in Ryff’s Psychological Well-Being scales; play more than 30 h per week and have manifested at least five of nine symptoms of IGD in the last 12 months. | Personal Data Sheet/Demographic Information Form (DIF); Internet Gaming Disorder (IGD) Scale; Ryff’s Psychological Well-Being (PWB) Scale | The Acceptance and Cognitive Restructuring Intervention Program (ACRIP) program | / | The results show a decrease in the adolescents’ IGD level and an increase in PWB level after the feasibility test, as indicated by the mean score of the post-test; and there is a significant difference in the pre-test and post-test scores of both IGD. | a pilot study; the sample is small and single |
| Pornnoppadol et al., 2020 [38] | Thailand | IGD | E1: n = 24; E2: n = 24; E3: n = 26; C: n = 30 | 13–17 | adolescents and/or parents of adolescents aged 13–17 years with a total score meeting the cutoff for problematic online gaming in the Game Addiction Screening Test (GAST)–Parent version | Game Addiction Screening Test (GAST); Game Addiction Quality of Life Scale (GAME-Q); Game Addiction Protection Scale (GAME-P); Pediatric Symptom Checklist-17 (PSC-17) Thai version | E1:7-day Siriraj Therapeutic Residential Camp (S-TRC) E2: Parent Management Training for Game Addiction (PMT-G) E3: combined S-TRC and PMT-G | basic psychoeducation | All experimental groups showed improvement over the control group. The percentage of adolescents who remained in the addicted or probably addicted groups was less than 50% in the S-TRC, PMT-G, and combined groups. | family assessment was not conducted at recruitment; a quasi-experimental study (intervention and control only, without randomization); no data on potentially confounding variables (e.g., family dynamics) |
| Lindenberg et al., 2022 [39] | Germany | IUD | n = 422 | 15.11 ± 2.01 | screened for risk before study enrollment using the German version of the Compulsive Internet Use Scale (CIUS) and chose a CIUS score of 20 as the cutoff criterion, thus, included participants at moderate risk and high risk. subgroup: CSAS: Computerspielabhängigkeitsskala, a modified German video game dependency scale DSM-5 | The German Procrastination Questionnaire (APROF); The Strengths and Difficulties Questionnaire (SDQ); The German Depression Inventory for Children and Adolescents (DIKJ); The Social Interaction Anxiety Scale (SIAS); The German revision of the Fear Survey Schedule for Children (PHOKI); The Assessment of Emotion Regulation in Children and Adolescents (FEEL-KJ); The German Student Assessment List for Social and Learning Behavior (SSL); The German General Self-Efficacy Scale (SWE) | PROTECT (Professional Use of Technical Media) intervention | assessment only | The PROTECT intervention effectively reduced symptoms of gaming disorder and unspecified internet use disorder over 12 months. The intervention did not change incidence rates of gaming disorder or unspecified internet use disorder. | limit the generalizability of the findings; an underpowered sample for the incidence analyses assessment of incidence rates needs to improve; differences between schools remain open to speculation |
| Yang et al., 2018 [40] | South Korea | IA | E: n = 38; C: n = 56 | 13–15 | categorized in the general internet user group or potentially addicted user group according to the Internet Addiction Proneness Scale | The Self-Control Scale; The Self-Efficacy Scale; The Internet Addiction Proneness Scale; an assessment of internet addiction (internet usage time). | Integrated and applied self-efficacy and self-regulation intervention strategies | no intervention | Self-control and self-efficacy significantly increased, and Internet addiction and time spent on the Internet significantly decreased in the intervention group compared with the control group. | not a randomized control trial but a quasi-experimental design; exogenous confounding variables not included; measured with self-report, there is a possibility of social desirability bias |
| Uysal and Balci, 2018 [21] | Turkey | IA | E: n = 41; C: n = 43 | 11–16 | scored 90 or over on the Internet Addiction Scale (IAS) | The Internet Addiction Scale | Healthy Internet Use Program | no intervention | After the Healthy Internet Use Program, the difference between the baseline measurement and scores after the third month was significant. In addition, the difference in the measurement of the IAS scores between the intervention group and the control group after the ninth month was highly significant, suggesting that the Healthy Internet Use Program decreases the rate of Internet addiction among adolescents. | only implemented with the students of two schools and cannot be generalized; no exact criterion to identify Internet addiction. |
| Khoshgoftar et al., 2019 [41] | Iran | Mobile Phone Addiction | E: n = 56; C: n = 56 | E: 14.62 ± 0.52 C: 14.66 ± 0.83 | have a smartphone; interested in participation; parental consent | Persian version of mobile phone addiction scale (MPAI); Health Belief Model constructs questionnaire | The educational intervention: Health Brief Model (HBM) | the usual school curriculum | Educational intervention based on the HBM can prevent and decrease mobile phone addiction in female students. | not internet addiction sample; only a quasi-experimental study could not generalize the finding; only student intervention, lack of parent’s education |
| Torres-Rodríguez et al., 2018 [42] | Spain | IGD | E: n = 17 C: n = 17 | 12–18 | endorsing at least five or more of the nine IGD criteria according to DSM-5; scoring 71 or more on Internet Gaming Disorder Test (IGD-20 Test) | The Clinical Global Impression Scale-Severity of Illness (CGI-SI); The Clinical Global Impression Scale-Global Improvement (CGI-GI); Global Assessment of Functioning (GAF) scale; The Working Alliance Theory of Change Inventory | PIPATIC (Programa Individualizado Psicoterapéutico para la Adicción a las Tecnologías de la information y la communication) intervention program | standard CBT | Relating to the interventions examined, significant differences were found in the pre-test and post-test on the following variables: comorbid disorders, intrapersonal and interpersonal abilities, and family relationships. In addition, both groups significantly reduced IGD symptoms, and the PIPATIC group showed higher significant improvements in the other variables examined. | Self-report measures; small sample size; no randomization of group assignment; lack of a control group without treatment; homogenous sample (Spanish male subjects only) |
| Chau et al., 2019 [43] | Hongkong | IGD | n = 248 | 10.16 ± 0.97 | Typical primary student with parental consent | The self-report version of the Korean Internet Addiction Proneness Scale; Risky Online Behavior questionnaire; The Positive and Negative Affect Schedule for Children-Short Form; The Children’s Loneliness Questionnaire; The Social Anxiety Scale for Children, and Pre-post measurements of symptoms of IGD, frequency of risky online behavior, and rating of emotional well-being | Wise IT-use program | / | After the program(2-month follow up), IGD symptoms and the percentage of students who were at risk for the condition decreased | Homogenous sample: high school students residing in Hong Kong |
| Lazarinis et al., 2020 [44] | Greece | IA | n = 42 | 6–10 | Typical developmental children with parental consent | / | Storytelling application | / | The application makes children reflect on their online actions through visual stories with contrasting elements. | an application introduction essay without an experiment |
| Tseng et al., 2022 [45] | China | IA | n = 10 | 10.45 ± 0.68 | Identified using the Chen Internet Addiction Scale (CIAS) | Movement Assessment Battery for Children-Second Edition (MABC-2) | A strategic physical activity intervention | / | The post-test scores showed significant improvements in accuracy in the pure, mixed, and switch trials and the manual dexterity and total score of the MABC-2 compared with the pre-test scores. | small sample size; no control group; assessment should more detailed |
| Gong et al., 2022 [46] | China | IA | E: n= 21; C: n= 21 | adolescents | Internet addiction adolescents | The 12-item General Health Questionnaire; the Self-rating Young’s Diagnostic Questionnaire of Internet Addiction, and the Positive Affect Subscale | Narrative therapy + Pilates exercise | no intervention | Compared to the control group, the intervention group had significantly lower scores for anxiety, depression, social dysfunction, loss of interest, and significantly higher scores for mental health. In addition, the intervention group demonstrated an apparent increase in the score for positive affect after the intervention. | other factors not included; a small sample without detailed characteristic |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ding, K.; Li, H. Digital Addiction Intervention for Children and Adolescents: A Scoping Review. Int. J. Environ. Res. Public Health 2023, 20, 4777. https://doi.org/10.3390/ijerph20064777
Ding K, Li H. Digital Addiction Intervention for Children and Adolescents: A Scoping Review. International Journal of Environmental Research and Public Health. 2023; 20(6):4777. https://doi.org/10.3390/ijerph20064777
Chicago/Turabian StyleDing, Keya, and Hui Li. 2023. "Digital Addiction Intervention for Children and Adolescents: A Scoping Review" International Journal of Environmental Research and Public Health 20, no. 6: 4777. https://doi.org/10.3390/ijerph20064777
APA StyleDing, K., & Li, H. (2023). Digital Addiction Intervention for Children and Adolescents: A Scoping Review. International Journal of Environmental Research and Public Health, 20(6), 4777. https://doi.org/10.3390/ijerph20064777








