Quality of Life in Amazonian Women during Cervical Cancer Treatment: The Moderating Role of Spirituality
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Participants
2.3. Instruments
2.4. Procedures
2.5. Data Analysis
3. Results
3.1. Sample Description
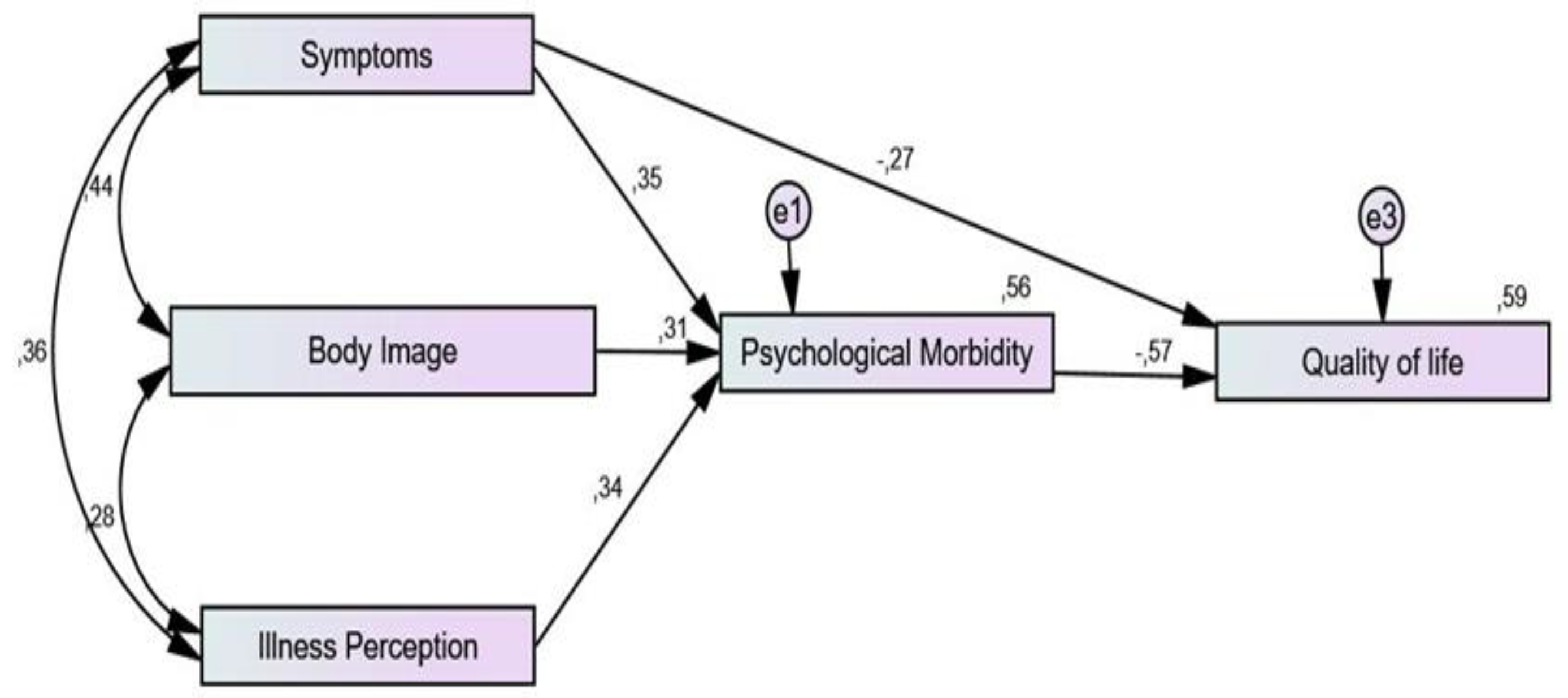
3.2. Relationships between All Variables: Path Analysis
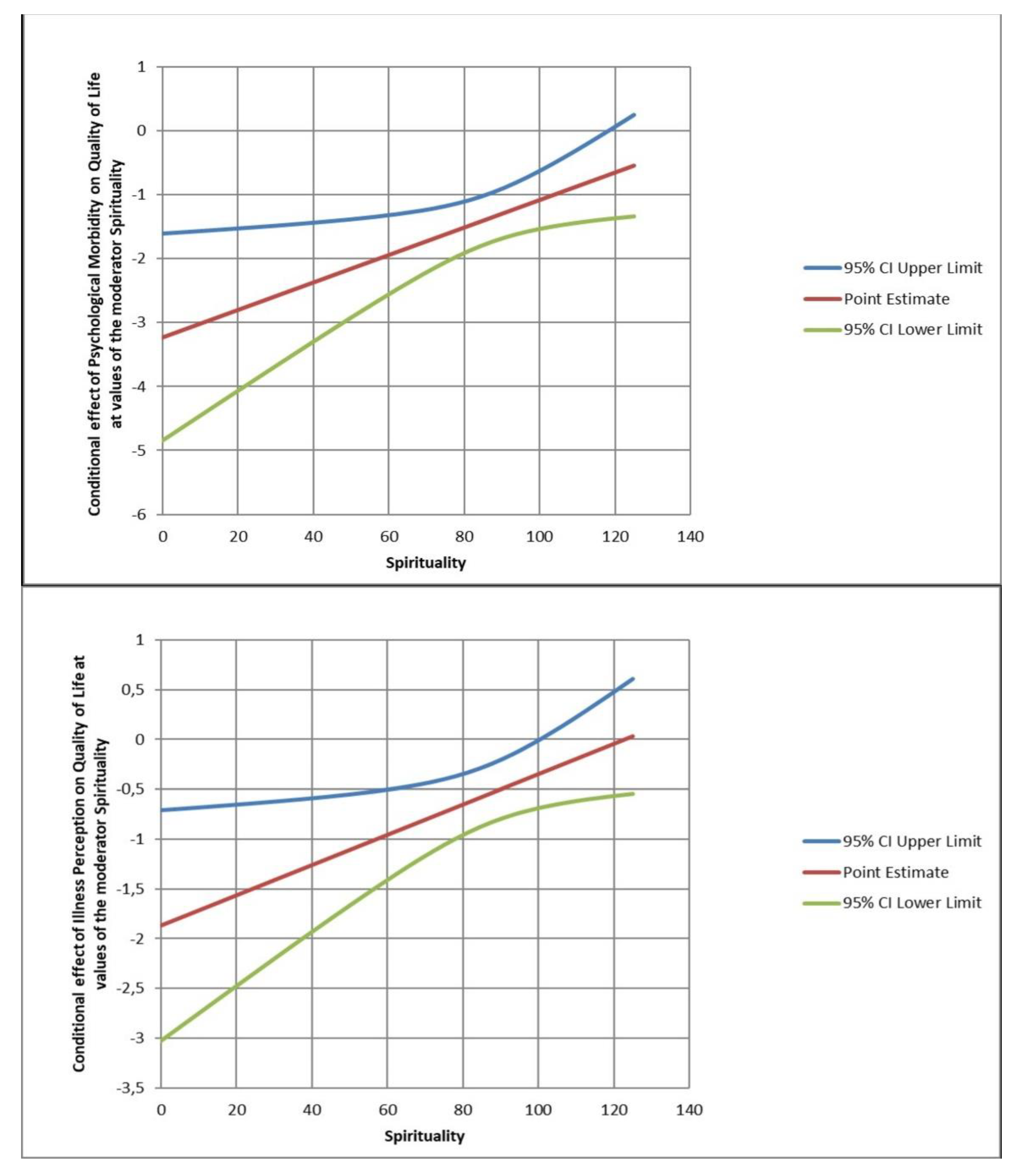
3.3. Spirituality as a Moderator between Psychological Morbidity and QoL
3.4. Spirituality as a Moderator between Illness Perception and QoL
4. Discussion
5. Conclusions
6. Implications
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- American Cancer Society. Cancer Facts & Statistics (2020). Available online: https://cancerstatisticscenter.cancer.org/# (accessed on 15 May 2022).
- National Institute of Cancer. Estimate/2018: Cancer Incidence in Brazil. Rev. Bras. Cancerol. 2018, 64, 119–120. Available online: https://rbc.inca.gov.br/site/arquivos/n_64/v01/pdf/15-review-estimate-2018-cancer-incidence-in-brazil.pdf (accessed on 23 November 2022).
- Instituto Brasileiro de Geografia e Estatística (IBGE). Censo Populacional 2010 (2010). Available online: https://censo2010.ibge.gov.br/ (accessed on 1 April 2022).
- Garnelo, L.; Sousa, A.B.L.; Silva, C.O. Health regionalization in Amazon: Progress and challenges. Ciência Saúde Coletiva 2017, 22, 1225–1234. [Google Scholar] [CrossRef] [PubMed]
- Instituto Brasileiro de Geografia e Estatística (IBGE). Cidades. (2021). Available online: https://cidades.ibge.gov.br/ (accessed on 1 April 2022).
- Arndt, V.; Koch-Gallenkamp, L.; Jansen LBertram, H.; Eberle, A.; Holleczek, B.; Brenner, H. Quality of life in long-term and very long-term cancer survivors versus population controls in Germany. Acta Oncol. 2017, 56, 190–197. [Google Scholar] [CrossRef] [PubMed]
- Sabulei, C.; Maree, J.E. An exploration into the quality of life of women treated for cervical cancer. Curations 2019, 42, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Bhatla, N.; Berek, J.S.; Fredes, M.C. Corrigendum to “Revised FIGO staging for carcinoma of the cervix uteri”. Int. J. Gynecol. Obstetrics 2019, 147, 279–280. [Google Scholar]
- Humphrey, P.; Bennett, C.; Cramp, F. The experiences of women receiving brachytherapy for cervical cancer: A systematic literature review. Radiography 2018, 24, 396–403. [Google Scholar] [CrossRef]
- Isaka, Y.; Inada, H.; Hiranuma, Y.; Ichikawa, M. Psychological impact of positive cervical cancer screening results among Japanese women. Int. J. Clin. Oncol. 2017, 22, 102–106. [Google Scholar] [CrossRef]
- Çinkir, H.Y.; Elboğa, G. The Illness Perception and its Association with Distress in Cancer Patients Receiving Chemotherapy. Turk. J. Oncol. 2020, 35, 1–7. [Google Scholar]
- Pitman, A.; Suleman, S.; Hyde, N.; Hodgkiss, A. Depression, and anxiety in patients with cancer. BMJ 2018, 361, k1415. [Google Scholar] [CrossRef]
- Lu, D.; Andrae, B.; Valdimarsdóttir, U.; Sundström, K.; Fall, K.; Sparén, P.; Fang, F. Psychologic Distress Is Associated with Cancer-Specific Mortality among Patients with Cervical Cancer. Cancer Res. 2019, 79, 3965–3972. [Google Scholar] [CrossRef]
- De Oliveira, P.F.; Queluz, F.N.F.R.A. A espiritualidade no enfrentamento do câncer. Rev. Psicol. IMED 2016, 8, 142–155. [Google Scholar] [CrossRef]
- Panzini, R.G.; Mosqueiro, B.P.; Zimpel, R.R.; Bandeira, D.R.; Rocha, N.S.; Fleck, M.P. Quality-of-life and spirituality. Int. Rev. Psychiatry 2017, 29, 263–282. [Google Scholar] [CrossRef]
- Costa, D.T.; Silva, D.M.R.D.; Cavalcanti, I.D.L.; Gomes, E.T.; Vasconcelos, J.L.D.A.; Carvalho, M.V.G.D. Religious/spiritual coping and level of hope in patients with cancer in chemotherapy. Rev. Bras. Enferm. 2019, 72, 640–645. [Google Scholar] [CrossRef]
- Mesquita, I.M.R.; Martos, C.P.; Santos, L.A.; de Oliveira, A.F.M.; Vieira, P.M.; Gonçalves, J.R.L.; de Fátima Borges, M. Perception of cancer patients on the influence of spirituality in chemotherapy treatment. Rev. Família Ciclos Vida Saúde Contexto Soc. 2019, 7, 441–447. [Google Scholar] [CrossRef]
- Ożek, A.; Nowak, P.F.; Blukacz, M. The Relationship Between Spirituality, Health-Related Behavior, and Psychological Well-Being. Front. Psychol. 2020, 11, 1997. [Google Scholar] [CrossRef]
- Ali, A.; Kohli, N.; Yadav, S. A Systematic Review of Illness Perception and Coping among Cancer Patients in India. Indian J. Health Wellbeing 2017, 8, 1309–1319. [Google Scholar]
- Foundation Center for Cancer Control of the State of Amazon. Relatório de Gestão 2018. Available online: http://www.fcecon.am.gov.br/wp-content/uploads/2014/08/Relatorio-2018.pdf (accessed on 1 April 2022).
- Fayers, P.; Bottomley, A. Quality of life research within the EORTC—The EORTC QLQ-C30. Eur. J. Cancer 2002, 38, 125–133. [Google Scholar] [CrossRef]
- Michels, F.A.S.; Latorre, M.R.D.; Maciel, M.S. Validity, reliability and understanding of the EORTC-C30 and EORTC-BR23, quality of life questionnaires specific for breast cancer. Rev. Bras. Epidemiol. 2013, 16, 352–363. [Google Scholar] [CrossRef]
- Greimel, E.R.; Kuljanic Vlasic, K.; Waldenstrom, A.C.; Duric, V.M.; Jensen, P.T.; Singer, S.; Chie, W.; Nordin, A.; Radisic, V.B.; Wydra, D. The European Organization for Research and Treatment of Cancer (EORTC) Quality-of-Life questionnaire cervical cancer module: EORTC QLQ-CX24. Cancer 2006, 107, 1812–1822. [Google Scholar] [CrossRef]
- Fregnani, C.M.S. Psychometric Properties of Two Instruments to Assess Health-Related Quality of Life in Women with Cervical Cancer. Ph.D. Thesis, Universidade de São Paulo, São Paulo, Brazil, 2013. [Google Scholar]
- Zigmond, A.S.; Snaith, R.P. The Hospital Anxiety and Depression Scale. Acta Psychiatr. Scand. 1983, 67, 361–370. [Google Scholar] [CrossRef]
- Botega, N.J.; Bio, M.R.; Zomignani, M.A.; Garcia Jr, C.; Pereira, W.A. Mood disorders among medical in-patients: A validation study of the hospital anxiety and depression scale (HAD). Rev. Saúde Pública 1995, 29, 359–363. [Google Scholar] [CrossRef] [PubMed]
- Moss-Morris, R.; Weinman, J.; Petrie, K.; Horne, R.; Cameron, L.; Buick, D. The revised Illness Perception Questionnaire (IPQ-R). Psychol. Health 2002, 17, 1–16. [Google Scholar] [CrossRef]
- Broadbent, E.; Petrie, K.J.; Main, J.; Weinman, J. The brief illness perception questionnaire. J. Psy-chosomatic Res. 2006, 60, 631–637. [Google Scholar] [CrossRef] [PubMed]
- Nogueira, G.S. Adaptation and Validation of the Brief Illness Perception Questionnaire (Brief IPQ) for the Brazilian Culture. Master’s Thesis, Universidade de Brasília, Brasília, Brazil, 2012. [Google Scholar]
- Büssing, A.; Ostermann, T.; Matthiessen, P.F. Role of religion and spirituality in medical patients: Confirmatory results with the SpREUK questionnaire. Health Qual. Life Outcomes 2005, 3, 10. [Google Scholar] [CrossRef] [PubMed]
- Pereira, M.G.; Moreira, C.; Moysés, R. Brazilian Research Version the Spiritual and Religion Attitudes in Dealing with Illness. Doctoral Theis, Research Group in Family Health & Illness, School of Psychology, University of Minho, Braga, Portugal, 2020. [Google Scholar]
- Bravin, A.M.; Trettene, A.S.; Andrade, L.G.M.; Popim, R.C. Benefits of spirituality and/or religiosity in patients with Chronic Kidney Disease: An integrative review. Rev. Bras. Enferm. 2019, 72, 541–551. [Google Scholar] [CrossRef]
- Chen, J.; You, H.; Liu, Y.; Kong, Q.; Lei, A.; Guo, X. Association between spiritual well-being, quality of life, anxiety and depression in patients with gynecological cancer in China. Medicine 2021, 100, 1–7. [Google Scholar]
- Ng, G.C.; Mohamed, S.; Sulaiman, A.H.; Zainal, N.Z. Anxiety and Depression in Cancer Patients: The Association with Religiosity and Religious Coping. J. Relig. Health 2017, 56, 575–590. [Google Scholar] [CrossRef]
- Thapa, N.; Maharjan, M.; Xiong, Y.; Jiang, D.; Nguyen, T.P.; Petrini, M.A.; Cai, H. Impact of cervical cancer on quality of life of women in Hubei, China. Sci. Rep. 2018, 8, 1–9. [Google Scholar] [CrossRef]
- Teo, I.; Cheung, Y.B.; Lim, T.Y.K.; Namuduri, R.P.; Long, V.; Tewani, K. The relationship between symptom prevalence, body image, and quality of life in Asian gynecologic cancer patients. Psycho-Oncology 2018, 27, 69–74. [Google Scholar] [CrossRef]
- Abbott-Anderson, K.; Eikenboom, K.L. A systematic review of sexual concerns reported by gynecological cancer survivors. Gynecol. Oncol. 2012, 124, 477–489. [Google Scholar] [CrossRef]
- Guler, B.; Mete, S. Effects of some characteristics of gynecological cancer diagnosis and treatment on women’s sexual life quality. Indian J. Cancer 2019, 56, 157–162. [Google Scholar] [CrossRef]
- Lopes, A.C.; Bacalhau, R.; Santos, M.; Pereira, M.; Pereira, M.G. Contribution of Sociodemographic, Clinical, and Psychological Variables to Quality of Life in Women with Cervical Cancer in the Follow-Up Phase. J. Clin. Psychol. Med. Sett. 2020, 27, 603–614. [Google Scholar] [CrossRef]
- Miranda, T.; Caldeira, S.; de Oliveira, H.F.; Lunes, D.H.; Nogueira, D.A.; Chaves, E.; Carvalho, E.C. Intercessory Prayer on Spiritual Distress, Spiritual Coping, Anxiety, Depression and Salivary Amylase in Breast Cancer Patients During Radiotherapy: Randomized Clinical Trial. J. Relig. Health 2020, 59, 365–380. [Google Scholar] [CrossRef]
- Mendes, A.S.; Arantes, T.C.; Martins, V.E.; Nicolussi, A.C. Práticas integrativas, espirituais e qualidade de vida do paciente com câncer durante o tratamento. Rev. Eletrônica Enferm. 2020, 22, 1–8. [Google Scholar] [CrossRef]

| n (%) | M (SD) | Min | Max | |
|---|---|---|---|---|
| Age | 119 | 47.54 | 26 | 75 |
| Age at Diagnosis | 119 | 46.69 (11.95) | 26 | 77 |
| Education | ||||
| <1 Year | 32 (26.9) | |||
| 1 to 3 Years | 24 (20.2) | |||
| 4 to 7 Years | 21 (17.6) | |||
| 8 to 10 Years | 42 (35.3) | |||
| Religion | ||||
| Evangelical/Protestant | 72 (63) | |||
| Catholic | 34 (29) | |||
| Spiritism (Kardecist) | 8 (4) | |||
| Stage | ||||
| Stage I | 15 (12.6) | |||
| Stage II | 41 (34.5) | |||
| StageIII | 38 (31.8) | |||
| Stage IV | 25 (21.1) | |||
| Treatment | ||||
| Chemotherapy | 3 (2.5) | |||
| Radiotherapy | 3 (2.5) | |||
| Surgery/Radiotherapy | 4 (3.3) | |||
| Surgery/Chemotherapy | 2 (1.6) | |||
| Chemotherapy/Radiotherapy | 70 (58.8) | |||
| Surgery/Radiotherapy/Chemotherapy | 37 (31.3) |
| n | M (SD) | Min | Max | |
|---|---|---|---|---|
| Quality of Life | 119 | 63.73 (19.43) | 21 | 99 |
| Psychological Morbidity | 119 | 14.51 (7.67) | 1.0 | 37.0 |
| Anxiety | 6.95 (4.30) | 0 | 19 | |
| Depression | 7.63 (4.35) | 0 | 19 | |
| Spirituality | 119 | 90.97 (11.03) | 52 | 125 |
| Reflection and Positive Interpretation | 90.28 (8.53) | 0 | 125 | |
| Spiritual Support | 83.74 (18.26) | 48 | 113 | |
| Illness Perception | 119 | 37.80 (11.35) | 9 | 63 |
| M (Mean) DP (Standard Deviation) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Moysés, R.; Marques, I.; Santos, B.D.; Benzaken, A.; Pereira, M.G. Quality of Life in Amazonian Women during Cervical Cancer Treatment: The Moderating Role of Spirituality. Int. J. Environ. Res. Public Health 2023, 20, 2487. https://doi.org/10.3390/ijerph20032487
Moysés R, Marques I, Santos BD, Benzaken A, Pereira MG. Quality of Life in Amazonian Women during Cervical Cancer Treatment: The Moderating Role of Spirituality. International Journal of Environmental Research and Public Health. 2023; 20(3):2487. https://doi.org/10.3390/ijerph20032487
Chicago/Turabian StyleMoysés, Rosana, Inês Marques, B. Daiana Santos, Adele Benzaken, and M. Graça Pereira. 2023. "Quality of Life in Amazonian Women during Cervical Cancer Treatment: The Moderating Role of Spirituality" International Journal of Environmental Research and Public Health 20, no. 3: 2487. https://doi.org/10.3390/ijerph20032487
APA StyleMoysés, R., Marques, I., Santos, B. D., Benzaken, A., & Pereira, M. G. (2023). Quality of Life in Amazonian Women during Cervical Cancer Treatment: The Moderating Role of Spirituality. International Journal of Environmental Research and Public Health, 20(3), 2487. https://doi.org/10.3390/ijerph20032487







