Effects on Children’s Physical and Mental Well-Being of a Physical-Activity-Based School Intervention Program: A Randomized Study
Abstract
1. Introduction
2. Methods
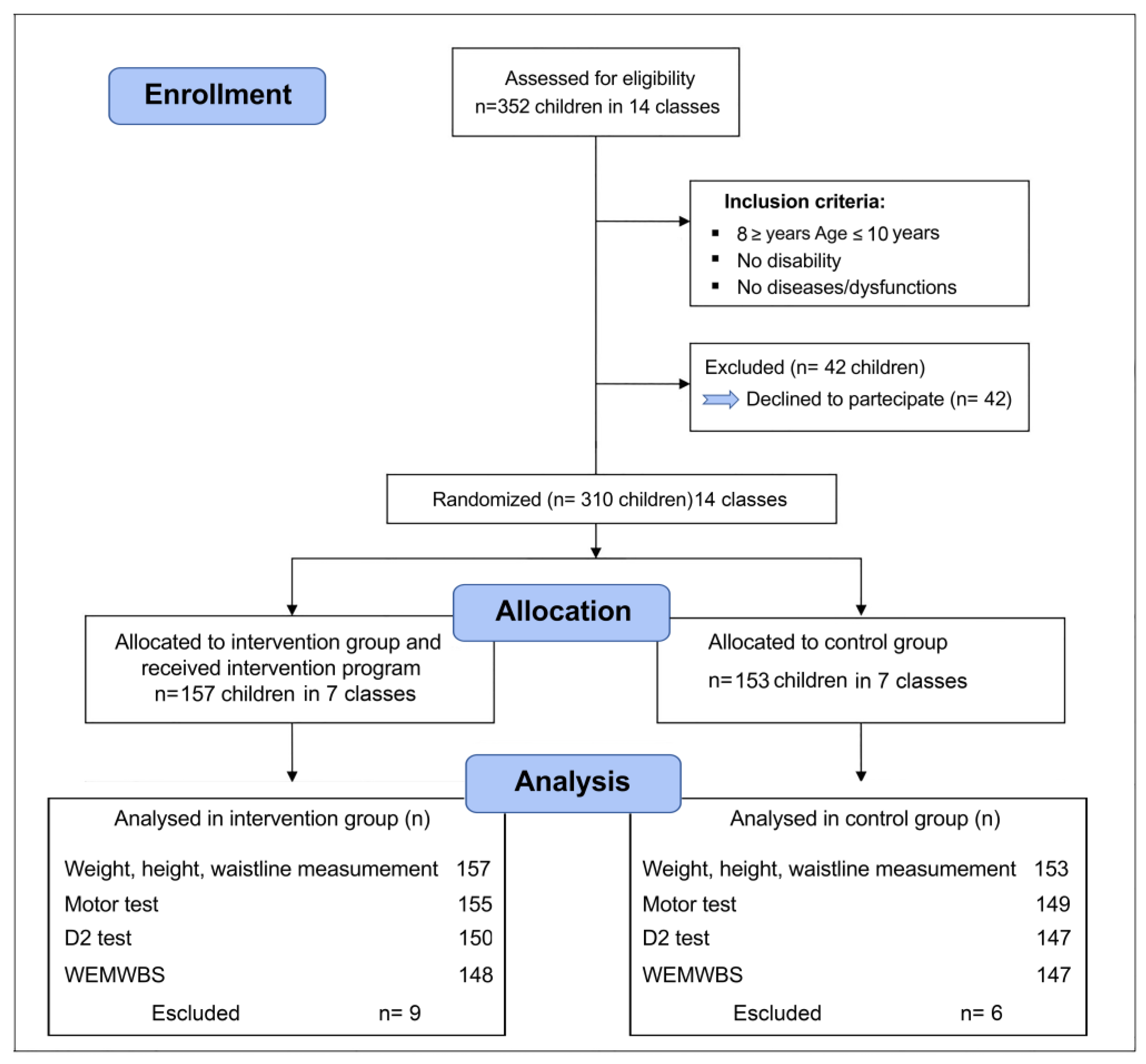
2.1. Participants and Procedures
2.2. Randomization
2.3. Training Intervention
2.4. Measures
2.5. Statistical Analysis
3. Results
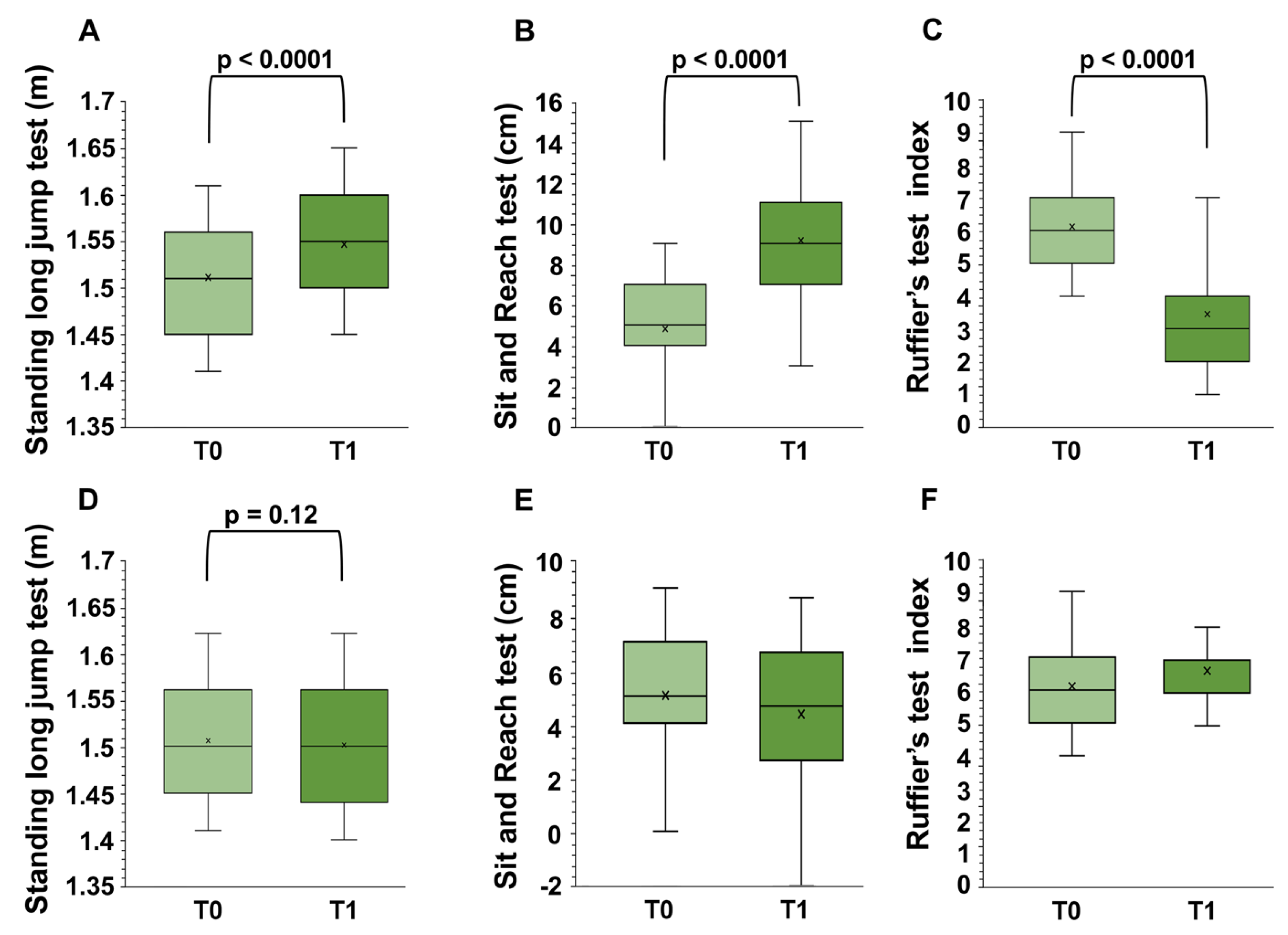
3.1. Motor Test Results
3.2. Cognitive Test
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Di Maglie, A.; Marsigliante, S.; My, G.; Colazzo, S.; Muscella, A. Effects of a physical activity intervention on schoolchildren fitness. Physiol. Rep. 2022, 10, e15115. [Google Scholar] [CrossRef] [PubMed]
- Battaglia, G.; Giustino, V.; Tabacchi, G.; Alesi, M.; Galassi, C.; Modica, C.; Palma, A.; Bellafiore, M. Effectiveness of a Physical Education Program on the Motor and Pre-literacy Skills of Preschoolers from the Training-To-Health Project: A Focus on Weight Status. Front. Sport. Act. Living 2020, 2, 579421. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Guidelines on Physical Activity, Sedentary Behaviour and Sleep for Children under 5 Years of Age; World Health Organization: Geneva, Switzerland, 2020. [Google Scholar]
- Tabacchi, G.; Battaglia, G.; Alesi, M.; Paoli, A.; Palma, A.; Bellafiore, M. Food literacy predictors and associations with physical and emergent literacy in pre-schoolers: Results from the Training-to-Health Project. Public Health Nutr. 2020, 23, 356–365. [Google Scholar] [CrossRef] [PubMed]
- Tremblay, M.S.; LeBlanc, A.G.; Kho, M.E.; Saunders, T.J.; Larouche, R.; Colley, R.C.; Goldfield, G.; Gorber, S.C. Systematic review of sedentary behaviour and health indicators in school-aged children and youth. Int. J. Behav. Nutr. Phys. Act. 2011, 21, 98. [Google Scholar] [CrossRef] [PubMed]
- Lipowski, M.; Lipowska, M.; Jochimek, M.; Krokosz, D. Resiliency as a factor protecting youths from risky behaviour: Moderating effects of gender and sport. Eur. J. Sport. Sci. 2016, 16, 246–255. [Google Scholar] [CrossRef] [PubMed]
- Janssen, I.; Leblanc, A.G. Systematic review of the health benefits of physical activity and fitness in school-aged children and youth. Int. J. Behav. Nutr. Phys. Act. 2010, 7, 40. [Google Scholar] [CrossRef]
- Leung, M.M.; Agaronov, A.; Grytsenko, K.; Yeh, M.C. Intervening to Reduce Sedentary Behaviors and Childhood Obesity among School-Age Youth: A Systematic Review of Randomized Trials. J. Obes. 2012, 685430. [Google Scholar] [CrossRef]
- Westerterp, K.R. Exercise, energy balance and body composition. Eur. J. Clin. Nutr. 2018, 72, 1246–1250. [Google Scholar] [CrossRef]
- de Greeff, J.W.; Bosker, R.J.; Oosterlaan, J.; Visscher, C.; Hartman, E. Effects of physical activity on executive functions, attention, and academic performance in preadolescent children: A meta-analysis. J. Sci. Med. Sport. 2018, 21, 501–507. [Google Scholar] [CrossRef]
- Tomporowski, P.D. Effects of acute bouts of exercise on cognition. Acta Psychol. 2003, 112, 297–324. [Google Scholar] [CrossRef]
- Gallotta, M.C.; Emerenziani, G.P.; Iazzoni, S.; Meucci, M.; Baldari, C.; Guidetti, L. Impacts of coordinative training on normal weight and overweight/obese children’s attentional performance. Front. Hum. Neurosci. 2015, 9, 577. [Google Scholar] [CrossRef] [PubMed]
- Pesce, C.; Crova, C.; Cereatti, L.; Casella, R.; Bellucci, M. Physical activity and mental performance in preadolescents: Effects of acute exercise on free-recall memory. Ment. Health Phys. Act. 2009, 2, 16–22. [Google Scholar] [CrossRef]
- Hillman, C.H.; Pontifex, M.B.; Raine, L.B.; Castelli, D.M.; Hall, E.E.; Kramer, A.F. The effect of acute treadmill walking on cognitive control and academic achievement in preadolescent children. Neuroscience 2009, 159, 1044–1054. [Google Scholar] [CrossRef] [PubMed]
- Gu, X.; Keller, M.J.; Weiller-Abels, K.H.; Zhang, T. The roles of physical activity and sedentary behavior on Hispanic children’s mental health: A motor skill perspective. Qual. Life Res. 2018, 27, 185–193. [Google Scholar] [CrossRef] [PubMed]
- Åvitsland, A.; Leibinger, E.; Haugen, T.; Lerum, Ø.; Solberg, R.B.; Kolle, E.; Dyrstad, S.M. The association between physical fitness and mental health in Norwegian adolescents. BMC Public Health 2020, 20, 776. [Google Scholar] [CrossRef] [PubMed]
- Chen, J.; Wang, X.; Wu, S.; Zhong, J.; Chen, W. Potential Predictors of Psychological Wellbeing in Elementary School Students. Children 2021, 8, 798. [Google Scholar] [CrossRef]
- Gale, C.R.; Cooper, R.; Craig, L.; Elliott, J.; Kuh, D.; Richards, M.; Starr, J.M.; Whalley, L.J.; Deary, I.J. Cognitive function in childhood and lifetime cognitive change in relation to mental wellbeing in four cohorts of older people. PLoS ONE 2012, 7, e44860. [Google Scholar] [CrossRef]
- Llewellyn, D.J.; Lang, I.A.; Langa, K.M.; Huppert, F.A. Cognitive function, and psychological well-being: Findings from a population-based cohort. Age Ageing 2008, 37, 685–689. [Google Scholar] [CrossRef]
- Diener, E. Subjective well-being. The science of happiness and a proposal for a national index. Am. Psychol. 2000, 55, 34–43. [Google Scholar] [CrossRef]
- Ryff, C.D.; Singer, B.H.; Dienberg Love, G. Positive health: Connecting well-being with biology. Philos. Trans. R. Soc. London. Ser. B Biol. Sci. 2004, 359, 1383–1394. [Google Scholar] [CrossRef]
- Ugwueze, F.C.; Agbaje, O.S.; Umoke, P.C.I.; Ozoemena, E.L. Relationship between Physical Activity Levels and Psychological Well-Being Among Male University Students in Southeast, Nigeria: A Cross-Sectional Study. Am. J. Mens Health 2021, 15, 15579883211008337. [Google Scholar] [CrossRef] [PubMed]
- Chen, P.; Wang, D.; Shen, H.; Yu, L.; Gao, Q.; Mao, L.; Jiang, F.; Luo, Y.; Xie, M.; Zhang, Y.; et al. Physical activity and health in Chinese children and adolescents: Expert consensus statement. Br. J. Sport. Med. 2020, 54, 1321–1331. [Google Scholar] [CrossRef]
- Ip, P.; Ho, F.K.; Louie, L.H.; Chung, T.W.; Cheung, Y.F.; Lee, S.L.; Hui, S.S.; Ho, W.K.; Ho, D.S.; Wong, W.H.; et al. Childhood Obesity and Physical Activity-Friendly School Environments. J. Pediatr. 2017, 191, 110–116. [Google Scholar] [CrossRef] [PubMed]
- Fairclough, S.; Stratton, G.; Baldwin, G. The Contribution of Secondary School Physical Education to Lifetime Physical Activity. Eur. Phys. Educ. Rev. 2002, 8, 69–84. [Google Scholar] [CrossRef]
- Morell-Azanza, L.; Ojeda-Rodríguez, A.; Ochotorena-Elicegui, A.; Martín-Calvo, N.; Chueca, M.; Marti, A.; Julian, A.S. Changes in objectively measured physical activity after a multidisciplinary lifestyle intervention in children with abdominal obesity: A randomized control trial. BMC Pediatr. 2019, 19, 90. [Google Scholar] [CrossRef] [PubMed]
- Claver, F.; Jiménez, R.; Gil-Arias, A.; Moreno, A.; Moreno, M.P. The Cognitive and Motivation Intervention Program in Youth Female Volleyball Players. J. Hum. Kinet. 2017, 59, 55–65. [Google Scholar] [CrossRef] [PubMed]
- Ariz, U.; Fernández-Atutxa, A.; Rivas-Fang, O.; Ruiz-Litago, F. Physical Activity at School Recess: A Key Element in Balancing Social Disparities. J. Sch. Health 2022, 92, 1005–1012. [Google Scholar] [CrossRef] [PubMed]
- Kuczmarski, R.J.; Ogden, C.L.; Grummer-Strawn, L.M.; Flegal, K.M.; Guo, S.S.; Wei, R.; Mei, Z.; Curtin, L.R.; Roche, A.F.; Johnson, C.L. CDC growth charts: United States. Adv. Data 2000, 8, 1–27. [Google Scholar]
- Meng, L.H.; Mi, J.; Cheng, H.; Hou, D.Q.; Zhao, X.Y.; Ding, X.Y. Using waist circumference and waist-to-height ratio to access central obesity in children and adolescents. Chin. J. Evid.-Based Pediatr. 2007, 2, 245–252. [Google Scholar]
- Woolcott, O.O.; Bergman, R.N. Relative Fat Mass as an estimator of whole-body fat percentage among children and adolescents: A cross-sectional study using NHANES. Sci. Rep. 2019, 9, 15279. [Google Scholar] [CrossRef]
- Eurofit, C.O.E. Handbook for the Eurofit Test on Physical Fitness; Council of Europe: Strasbourg, France, 1993. [Google Scholar]
- Bruggeman, B.S.; Vincent, H.K.; Chi, X.; Filipp, S.L.; Mercado, R.; Modave, F.; Guo, Y.; Gurka, M.J.; Bernier, A. Simple tests of cardiorespiratory fitness in a pediatric population. PLoS ONE 2020, 15, e0238863. [Google Scholar] [CrossRef] [PubMed]
- Castro-Piñero, J.; Chillón, P.; Ortega, F.B.; Montesinos, J.L.; Sjöström, M.; Ruiz, J.R. Criterion-related validity of sit-and-reach and modified sit-and-reach test for estimating hamstring flexibility in children and adolescents aged 6–17 years. Int. J. Sport. Med. 2009, 30, 658–662. [Google Scholar] [CrossRef] [PubMed]
- Gallotta, M.C.; Guidetti, L.; Franciosi, E.; Emerenziani, G.P.; Bonavolontà, V.; Baldari, C. Effects of varying type of exertion on children’s attention capacity. Med. Sci. Sport. Exerc. 2012, 44, 550–555. [Google Scholar] [CrossRef] [PubMed]
- Gallotta, M.C.; Emerenziani, G.P.; Franciosi, E.; Meucci, M.; Guidetti, L.; Baldari, C. Acute physical activity and delayed attention in primary school students. Scand. J. Med. Sci. Sport. 2015, 25, e331–e338. [Google Scholar] [CrossRef] [PubMed]
- Tennant, R.; Hiller, L.; Fishwick, R.; Platt, S.; Joseph, S.; Weich, S.; Parkinson, J.; Secker, J.; Stewart-Brown, S. The Warwick-Edinburgh Mental Well-being Scale (WEMWBS): Development and UK validation. Health Qual. Life Outcomes 2007, 5, 63. [Google Scholar] [CrossRef]
- Chen, W.; Gu, X.; Chen, J.; Wang, X. Association of Cardiorespiratory Fitness and Cognitive Function with Psychological Well-Being in School-Aged Children. Int. J. Environ. Res. Public Health 2022, 19, 1434. [Google Scholar] [CrossRef]
- Clarke, A.; Friede, T.; Putz, R.; Ashdown, J.; Martin, S.; Blake, A.; Adi, Y.; Parkinson, J.; Flynn, P.; Platt, S.; et al. Warwick-Edinburgh Mental Well-being Scale (WEMWBS): Validated for teenage school students in England and Scotland. A mixed methods assessment. BMC Public Health 2011, 11, 487. [Google Scholar] [CrossRef]
- Spinelli, A.; Buoncristiano, M.; Kovacs, V.A.; Yngve, A.; Spiroski, I.; Obreja, G.; Starc, G.; Pérez, N.; Rito, A.I.; Kunešová, M.; et al. Prevalence of Severe Obesity among Primary School Children in 21 European Countries. Obes. Facts 2019, 12, 244–258. [Google Scholar] [CrossRef]
- Lauria, L.; Spinelli, A.; Buoncristiano, M.; Nardone, P. Decline of childhood overweight and obesity in Italy from 2008 to 2016: Results from 5 rounds of the population-based surveillance system. BMC Public Health 2019, 19, 618. [Google Scholar] [CrossRef]
- Marsigliante, S.; Ciardo, V.; Di Maglie, A.; My, G.; Muscella, A. Efficacy of school-based intervention programs in reducing overweight: A randomized trial. Front. Nutr. 2022, 9, 1001934. [Google Scholar] [CrossRef]
- Nardone, P.; Pierannunzio, D.; Ciardullo, S.; Lazzeri, G.; Cappello, N.; Spinelli, A.; the 2018 HBSC-Italia Group. Dietary habits among Italian adolescents and their relation to socio-demographic characteristics. Ann. Ist Super Sanità 2020, 56, 504–513. [Google Scholar] [CrossRef] [PubMed]
- Ding, D.; Mutrie, N.; Bauman, A.; Pratt, M.; Hallal, P.R.C.; Powell, K.E. Physical activity guidelines 2020: Comprehensive and inclusive recommendations to activate populations. Lancet 2020, 396, 1780–1782. [Google Scholar] [CrossRef] [PubMed]
- Fu, L.; Cheng, H.; Zhao, X.; Hou, D.; Xie, X.; Mi, J. Distinct causal effects of body fat distribution on cardiometabolic traits among children: Findings from the BCAMS study. Nutr. Metab. Cardiovasc. Dis. 2022, 32, 1753–1765. [Google Scholar] [CrossRef] [PubMed]
- Must, A.; Phillips, S.M.; Naumova, E.N. Occurrence and timing of childhood overweight and mortality: Findings from the Third Harvard Growth Study. J. Pediatr. 2012, 160, 743–750. [Google Scholar] [CrossRef] [PubMed]
- Ashwell, M.; Gunn, P.; Gibson, S. Waist-to-height ratio is a better screening tool than waist circumference and BMI for adult cardiometabolic risk factors: Systematic review and meta-analysis. Obes. Rev. 2012, 13, 275–286. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.H.; Park, J.S.; Kim, W.; Shin, D.G.; Kim, Y.J.; Kim, D.S.; Choi, D.J.; Han, K.R.; Kim, C.J.; Cho, M.C.; et al. Korean Acute Myocardial Infarction Registry Investigators. Impact of body mass index and waist-to-hip ratio on clinical outcomes in patients with ST-segment elevation acute myocardial infarction (from the Korean Acute Myocardial Infarction Registry). Am. J. Cardiol. 2008, 102, 957–965. [Google Scholar] [CrossRef] [PubMed]
- Lo, K.; Wong, M.; Khalechelvam, P.; Tam, W. Waist-to-height ratio, body mass index and waist circumference for screening paediatric cardio-metabolic risk factors: A meta-analysis. Obes. Rev. 2016, 17, 1258–1275. [Google Scholar] [CrossRef] [PubMed]
- Nambiar, S.; Hughes, I.; Davies, P.S. Developing waist-to-height ratio cut-offs to define overweight and obesity in children and adolescents. Public Health Nutr. 2010, 13, 1566–1574. [Google Scholar] [CrossRef]
- Pfisterer, J.; Rausch, C.; Wohlfarth, D.; Bachert, P.; Jekauc, D.; Wunsch, K. Effectiveness of Physical-Activity-Based Interventions Targeting Overweight and Obesity among University Students-A Systematic Review. Int. J. Environ. Res. Public Health 2022, 19, 9427. [Google Scholar] [CrossRef]
- Kriemler, S.; Zahner, L.; Schindler, C.; Meyer, U.; Hartmann, T.; Hebestreit, H.; Brunner-La Rocca, H.P.; van Mechelen, W.; Puder, J.J. Effect of school based physical activity programmed (KISS) on fitness and adiposity in primary schoolchildren: Cluster randomized controlled trial. BMJ 2010, 340, c785. [Google Scholar] [CrossRef]
- van de Kop, J.H.; van Kernebeek, W.G.; Otten, R.H.J.; Toussaint, H.M.; Verhoeff, A.P. School-Based Physical Activity Interventions in Prevocational Adolescents: A Systematic Review and Meta-Analyses. J. Adolesc. Health 2019, 65, 185–194. [Google Scholar] [CrossRef] [PubMed]
- van Sluijs, E.M.; McMinn, A.M.; Griffin, S.J. Effectiveness of interventions to promote physical activity in children and adolescents: Systematic review of controlled trials. BMJ 2007, 335, 703. [Google Scholar] [CrossRef] [PubMed]
- Battaglia, G.; Giustino, V.; Tabacchi, G.; Lanza, M.; Schena, F.; Biino, V.; Giuriato, M.; Gallotta, M.C.; Guidetti, L.; Baldari, C.; et al. Interrelationship between Age, Gender, and Weight Status on Motor Coordination in Italian Children and Early Adolescents Aged 6–13 Years Old. Front. Pediatr. 2021, 9, 738294. [Google Scholar] [CrossRef] [PubMed]
- Caspersen, C.J.; Powell, K.E.; Christenson, G.M. Physical activity, exercise, and physical fitness: Definitions and distinctions for health-related research. Public Health Rep. 1985, 100, 126–131. [Google Scholar] [PubMed]
- Raghuveer, G.; Hartz, J.; Lubans, D.R.; Takken, T.; Wiltz, J.L.; Mietus-Snyder, M.; Perak, A.M.; Baker-Smith, C.; Pietris, N.; Edwards, N.M. American Heart Association Young Hearts Athero, Hypertension and Obesity in the Young Committee of the Council on Lifelong Congenital Heart Disease and Heart Health in the Young. Cardiorespiratory Fitness in Youth: An Important Marker of Health: A Scientific Statement from the American Heart Association. Circulation 2020, 142, e101–e118. [Google Scholar] [CrossRef]
- Ortega, F.B.; Lee, D.C.; Sui, X.; Kubzansky, L.D.; Ruiz, J.R.; Baruth, M.; Castillo, M.J.; Blair, S.N. Psychological well-being, cardiorespiratory fitness, and long-term survival. Am. J. Prev. Med. 2010, 39, 440–448. [Google Scholar] [CrossRef]
- Esteban-Cornejo, I.; Cadenas-Sanchez, C.; Contreras-Rodriguez, O.; Verdejo-Roman, J.; Mora-Gonzalez, J.; Migueles, J.H.; Henriksson, P.; Davis, C.L.; Verdejo-Garcia, A.; Catena, A.; et al. A whole brain volumetric approach in overweight/obese children: Examining the association with different physical fitness components and academic performance. The Active Brains project. Neuroimage 2017, 159, 346–354. [Google Scholar] [CrossRef]
- Donnelly, J.E.; Hillman, C.H.; Castelli, D.; Etnier, J.L.; Lee, S.; Tomporowski, P.; Lambourne, K.; Szabo-Reed, A.N. Physical Activity, Fitness, Cognitive Function, and Academic Achievement in Children: A Systematic Review. Med. Sci. Sport. Exerc. 2016, 48, 1197–1222. [Google Scholar] [CrossRef]
- Chaddock-Heyman, L.; Erickson, K.I.; Holtrop, J.L.; Voss, M.W.; Pontifex, M.B.; Raine, L.B.; Hillman., C.H.; Kramer, A.F. Aerobic fitness is associated with greater white matter integrity in children. Front. Hum. Neurosci. 2014, 8, 584. [Google Scholar] [CrossRef]
- Herold, F.; Müller, P.; Gronwald, T.; Müller, N.G. Dose-Response Matters!—A Perspective on the Exercise Prescription in Exercise-Cognition Research. Front. Psychol. 2019, 10, 2338. [Google Scholar] [CrossRef]
- Ribeiro, D.; Petrigna, L.; Pereira, F.C.; Muscella, A.; Bianco, A.; Tavares, P. The Impact of Physical Exercise on the Circulating Levels of BDNF and NT 4/5: A Review. Int. J. Mol. Sci. 2021, 22, 8814. [Google Scholar] [CrossRef] [PubMed]
- Brooks, G.A.; Arevalo, J.A.; Osmond, A.D.; Leija, R.G.; Curl, C.C.; Tovar, A.P. Lactate in contemporary biology: A phoenix risen. J. Physiol. 2022, 600, 1229–1251. [Google Scholar] [CrossRef] [PubMed]
- Zhu, L.; Yu, Q.; Herold, F.; Cheval, B.; Dong, X.; Cui, L.; Xiong, X.; Chen, A.; Yin, H.; Kong, Z.; et al. Brain Structure, Cardiorespiratory Fitness, and Executive Control Changes after a 9-Week Exercise Intervention in Young Adults: A Randomized Controlled Trial. Life 2021, 11, 292. [Google Scholar] [CrossRef] [PubMed]
- Shi, Y.; Qu, S. Cognition and Academic Performance: Mediating Role of Personality Characteristics and Psychology Health. Front. Psychol. 2021, 12, 774548. [Google Scholar] [CrossRef] [PubMed]
- My, G.; Marsigliante, S.; Bianco, A.; Zangla, D.; Silva, C.M.D.; Muscella, A. Biological, Psychological, and Physical Performance Variations in Football Players during the COVID-19 Lockdown: A Prospective Cohort Study. Int. J. Environ. Res. Public Health 2022, 19, 2739. [Google Scholar] [CrossRef] [PubMed]

| Phase | Type of Exercise | Duration |
|---|---|---|
| Warm-up | Walk in place; reach both arms up and down; step side-to-side; press arms forward; roll shoulders forward; alternately lift left and right knees up and down; roll head in a half circle left and right | 3′ |
| Training (Main exercise) | Walking Circuits Jump-in and Jump-out Marching down the row Squats Jump rope Chicken dance Dinosaur stomp Geometry dance Carrots being harvested | 5′ |
| Cool-down | Yoga poses Reach for the sky; touch toes; arm circles; neck circles; knee to chest; quad stretch; hamstring stretch; breathing deep | 2′ |
| Characteristic Intervention Group | All (n = 157) | Boys (n = 72) | Girls (n = 85) |
|---|---|---|---|
| Age, y | 9.9 ± 0.7 | 10.0 ± 0.4 | 9.8 ± 0.6 |
| Weight, kg | 40.4 ± 10.2 | 41.6 ± 9.8 | 39.7 ± 9.4 |
| BMI | 18.9 ± 2.6 | 19.5 ± 3.2 | 18.6 ± 2.4 |
| BMI, percentile | 61.3 ± 11.6 | 62.3 ± 9.3 | 58.3 ± 8.3 |
| Waistline | 59.1 ± 5.4 | 62.2 ± 5.2 | 57.8 ± 3.4 |
| RFM | 25.1 ± 1.2 | 27.33 ± 2.7 | 25.1 ± 1.2 * |
| Control Group | All (n = 153) | Boys (n = 67) | Girls (n = 86) |
| Age, y | 9.9 ± 0.5 | 10.0 ± 0.7 | 9.8 ± 0.7 |
| Weight, kg | 40.5 ± 9.9 | 40.9 ± 10.3 | 38.7 ± 10.2 |
| BMI | 19.0 ± 3.7 | 19.35± 2.9 | 19.1 ± 2.4 |
| BMI, percentile | 62.5 ± 9.8 | 62.9 ± 11.6 | 58.9 ± 10.1 |
| Waistline | 58.8 ± 4.6 | 61.9 ± 5.4 | 57.7 ± 3.8 |
| RFM | 26.2 ± 2.7 | 25.1 ± 1.6 | 27.8 ± 2.2 * |
| T0 | T1 | ||||||
|---|---|---|---|---|---|---|---|
| All (n = 157) | Boys (n = 72) | Girls (n = 85) | All (n = 153) | Boys (n = 67) | Girls (n = 86) | p | |
| Intervention group | |||||||
| WHR | 0.44 ± 0.04 | 0.45 ± 0.01 | 0.42 ± 0.03 | 0.43 ± 0.03 | 0.44 ± 0.01 | 0.41 ± 0.03 | 0.0002 |
| RFM | 24.9 ± 1.6 | 25.1 ± 1.3 | 24.7 ± 1.8 | 26.4 ± 3.6 | 27.3 ± 2.7 | 25.5 ± 4.1 | <0.0001 |
| Control group | |||||||
| WHR | 0.44 ± 0.01 | 0.45 ± 0.04 | 0.42 ± 0.03 | 0.44 ± 0.04 | 0.45 ± 0.02 | 0.42 ± 0.01 | >0.05 |
| RFM | 24.6 ± 2.7 | 24.8 ± 2.0 | 24.6 ± 2.2 | 25.1 ± 1.8 | 25.2 ± 2.1 | 24.8 ± 2.4 | >0.05 |
| T0 | T1 | ||||||
|---|---|---|---|---|---|---|---|
| All (n = 157) | Boys (n = 72) | Girls (n = 85) | All (n = 153) | Boys (n = 67) | Girls (n = 86) | p | |
| Intervention group | |||||||
| TN | 379.35 ± 76 | 372.75 ± 83 | 385.75 ± 97 | 473.21 ± 80 | 460.43 ± 71 | 483.76 ± 0.03 | |
| CP | 120.75 ± 48 | 117.13 ± 32 | 124.87 ± 28 | 147.88 ± 72 | 141.32 ± 28 | 155.52 ± 41 | <0.0001 |
| E% | 12.1 ± 6 | 13.76 ± 3 | 10.4 ± 8 | 6.7 ± 6 | 7.9 ± 2 | 5.5 ± 5 | |
| Control group | |||||||
| TN | 379.85 ± 94 | 375.59 ± 91 | 383.3 ± 101 | 392.56 ± 112 | 388.21 ± 102 | 397,65 ± 97 | |
| CP | 121.67 ± 36 | 106.35 ± 41 | 127.27 ± 47 | 128.63 ± 76 | 114.56 ± 2.1 | 130.56 ± 84 | >0.05 |
| E% | 12.5 ± 6 | 13.9 ± 7 | 11.1 ± 8 | 9.5 ± 7 | 11.2 ± 8 | 7.9 ± 3 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Marsigliante, S.; Gómez-López, M.; Muscella, A. Effects on Children’s Physical and Mental Well-Being of a Physical-Activity-Based School Intervention Program: A Randomized Study. Int. J. Environ. Res. Public Health 2023, 20, 1927. https://doi.org/10.3390/ijerph20031927
Marsigliante S, Gómez-López M, Muscella A. Effects on Children’s Physical and Mental Well-Being of a Physical-Activity-Based School Intervention Program: A Randomized Study. International Journal of Environmental Research and Public Health. 2023; 20(3):1927. https://doi.org/10.3390/ijerph20031927
Chicago/Turabian StyleMarsigliante, Santo, Manuel Gómez-López, and Antonella Muscella. 2023. "Effects on Children’s Physical and Mental Well-Being of a Physical-Activity-Based School Intervention Program: A Randomized Study" International Journal of Environmental Research and Public Health 20, no. 3: 1927. https://doi.org/10.3390/ijerph20031927
APA StyleMarsigliante, S., Gómez-López, M., & Muscella, A. (2023). Effects on Children’s Physical and Mental Well-Being of a Physical-Activity-Based School Intervention Program: A Randomized Study. International Journal of Environmental Research and Public Health, 20(3), 1927. https://doi.org/10.3390/ijerph20031927








