Defining the South African Acute Respiratory Infectious Disease Season
Abstract
1. Introduction
2. Materials and Methods
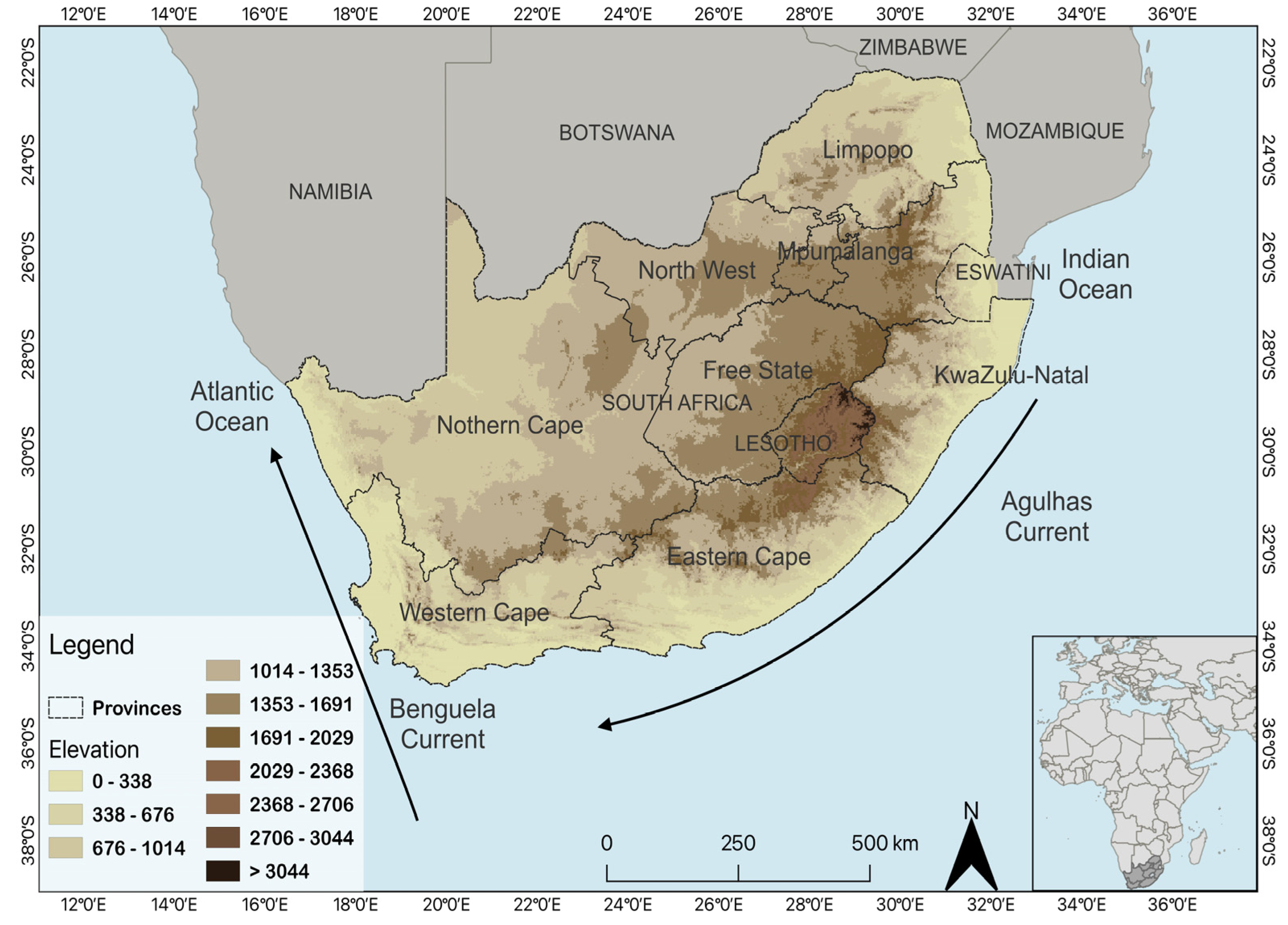
2.1. Study Site
2.2. Data Sources
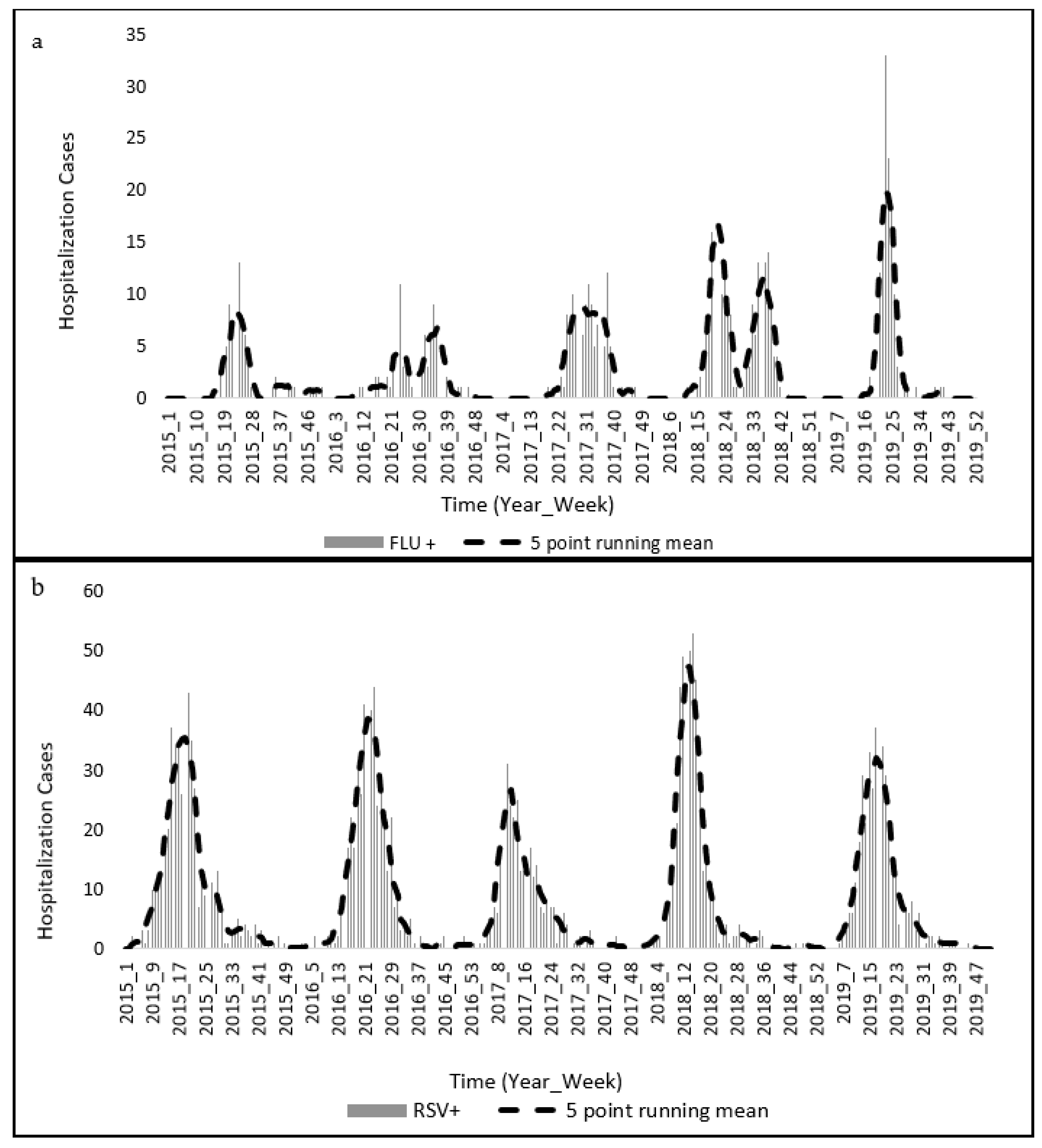
2.3. Hospitalization Cases
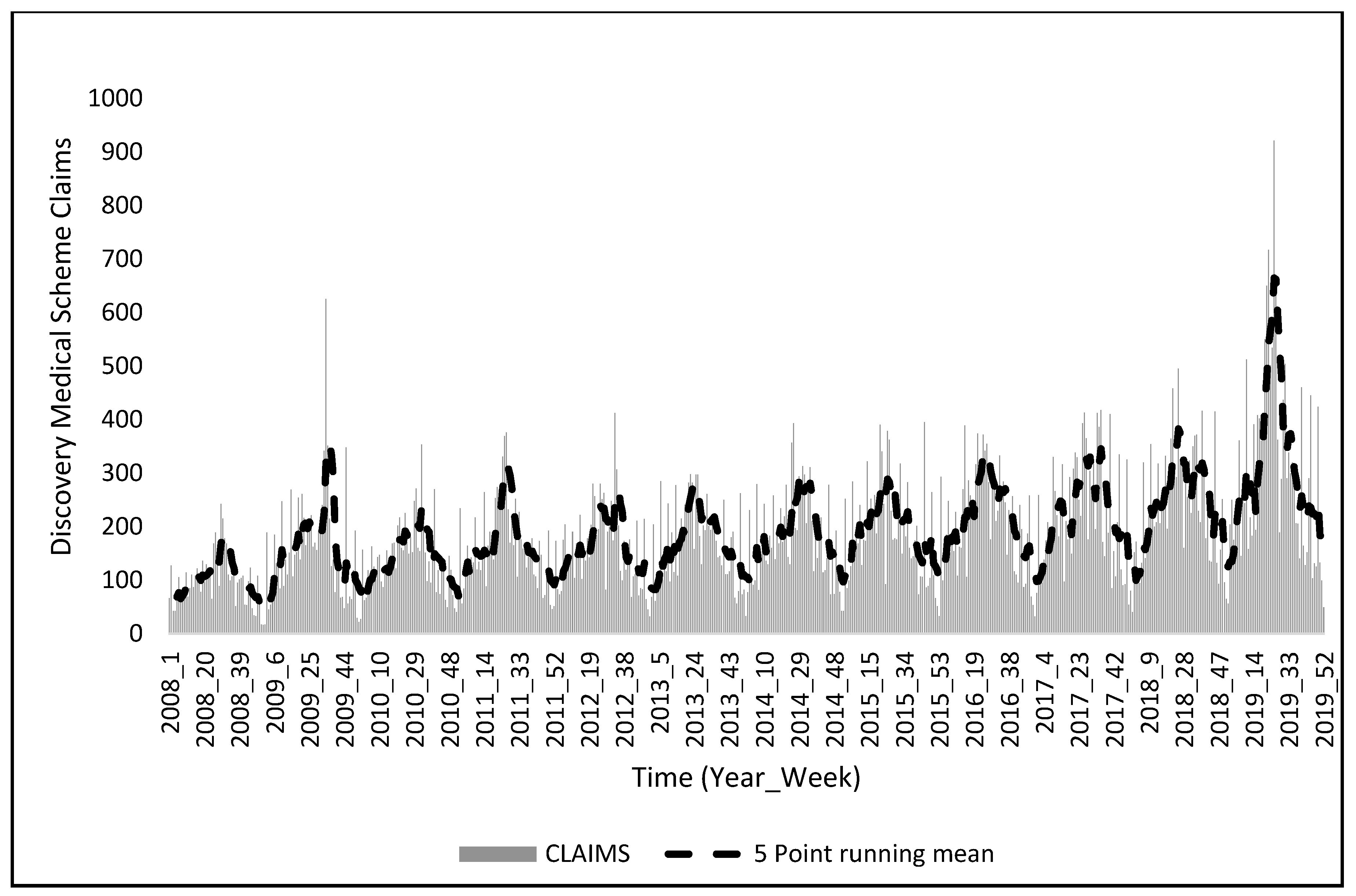
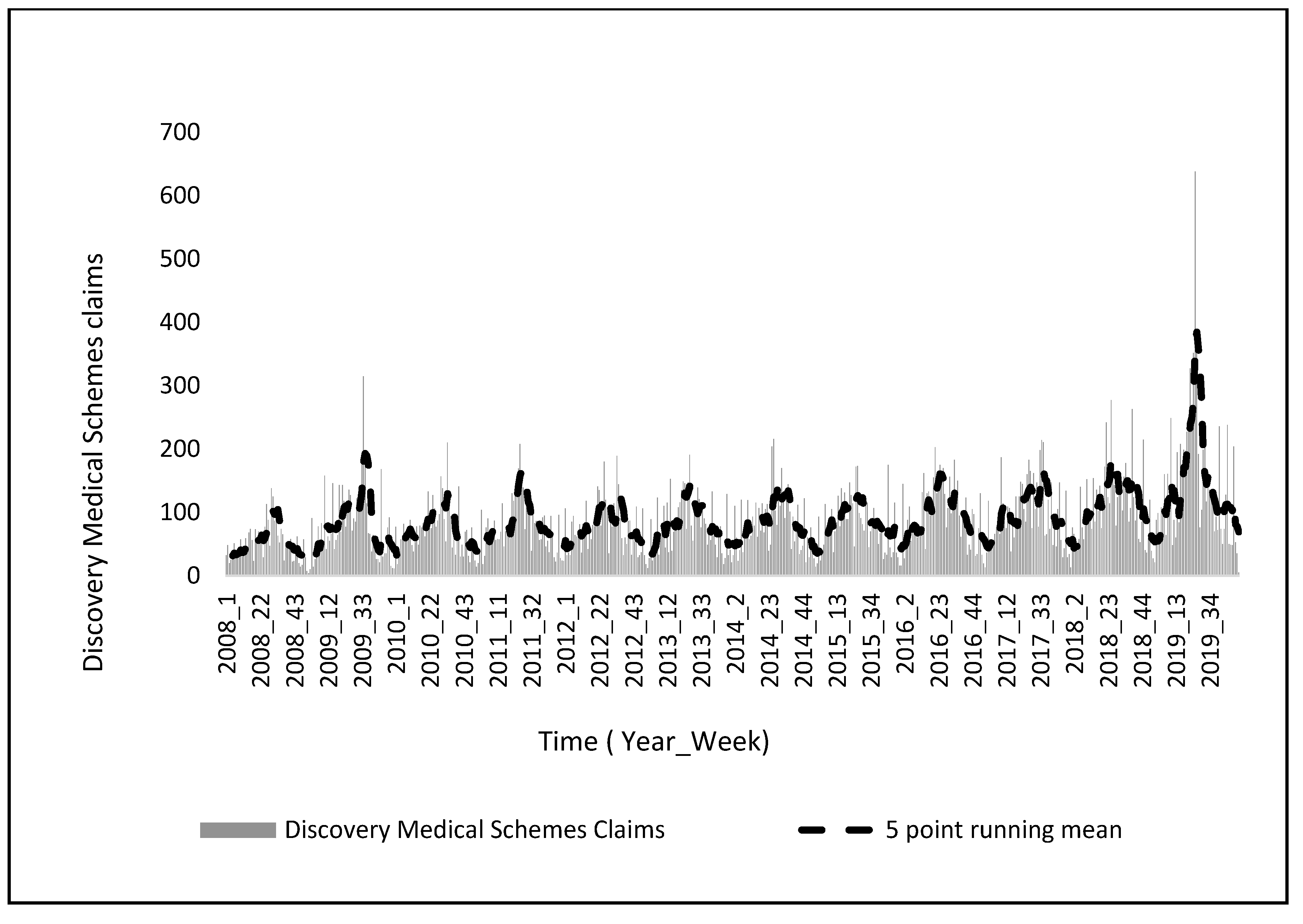
2.4. Medical Insurance Scheme Claims
2.5. Data Analysis
3. Results
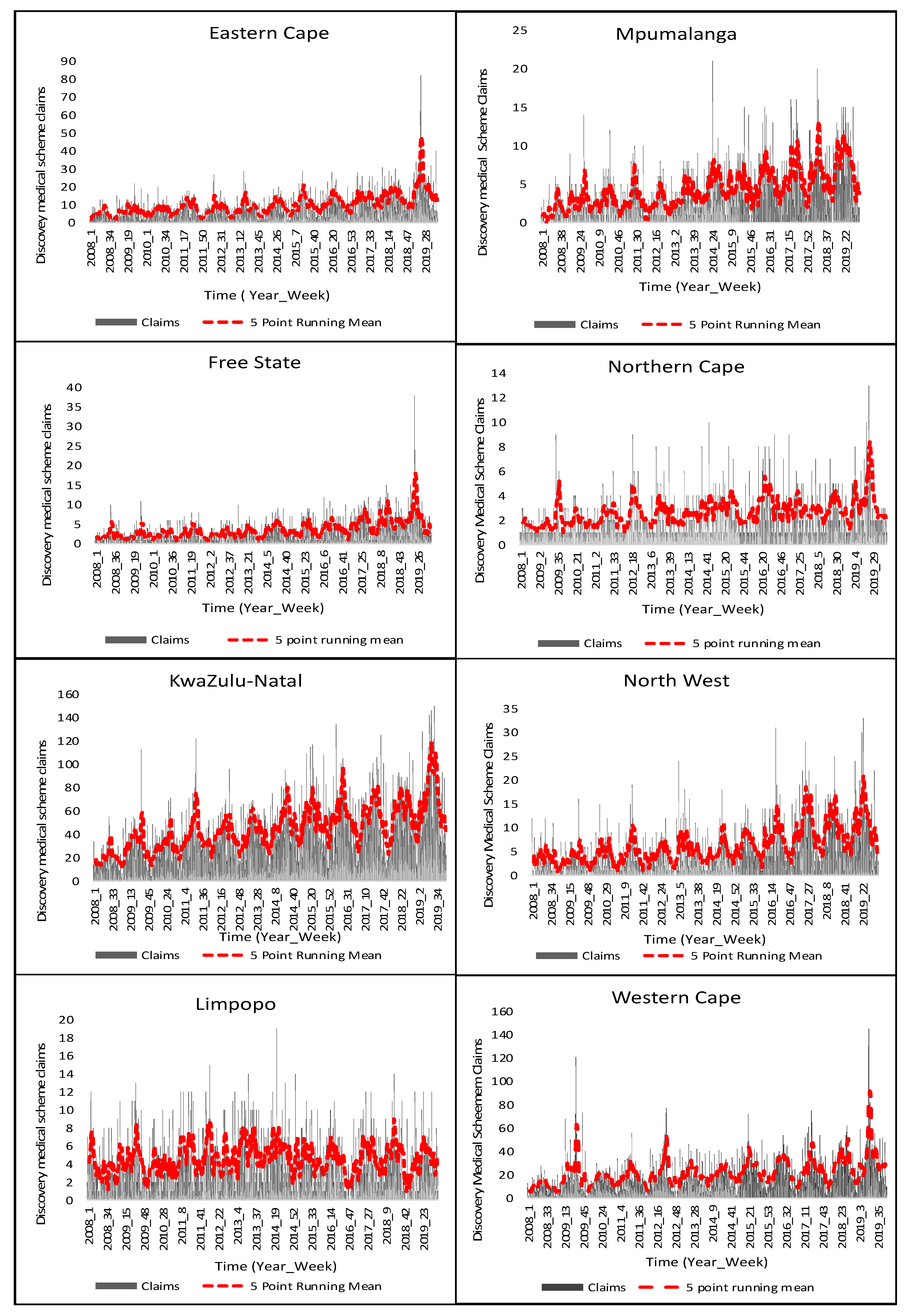
3.1. Weekly Trends in Hospitalization Cases and Medical Insurance Claims
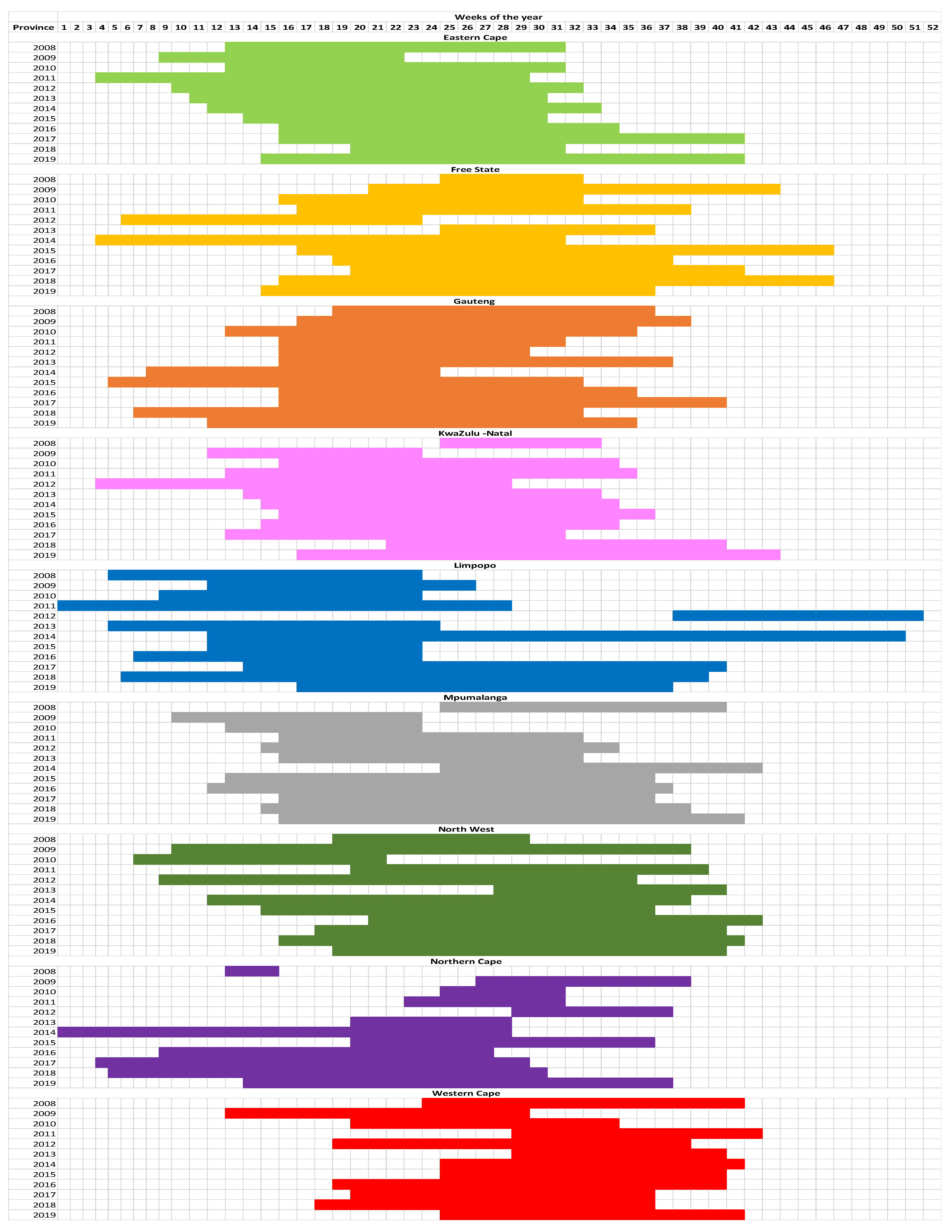
3.2. Defining the Acute Infectious Respiratory Disease Season
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Chumakov, M.P.; Voroshilova, M.K.; Antsupova, A.S.; Boiko, V.M.; Blinova, M.I.; Priimiagi, L.S.; Rodin, V.I.; Seibil, V.B.; Siniak, K.M.; Smorodintsev, A.A. Live enteroviral vaccines for the emergency nonspecific prevention of mass respiratory diseases during fall-winter epidemics of influenza and acute respiratory diseases. Zhurnal Mikrobiol. Epidemiol. I Immunobiol. 1992, 12, 37–40. [Google Scholar]
- Cooper, R.J.; Hoffman, J.R.; Bartlett, J.G.; Besser, R.E.; Gonzales, R.; Hickner, J.M.; Sande, M.A.; American Academy of Family Physicians; American College of Physicians-American Society of Internal Medicine; Centres for Disease Control. Principles of appropriate antibiotic use for acute pharyngitis in adults: Background. Ann. Intern. Med. 2001, 134, 509–517. [Google Scholar] [CrossRef] [PubMed]
- Fendrick, A.M.; Monto, A.S.; Nightengale, B.; Sarnes, M. The economic burden of non-influenza-related viral respiratory tract infection in the United States. Arch. Intern. Med. 2003, 163, 487–494. [Google Scholar] [CrossRef]
- Nicholson, S.E. The nature of rainfall variability over Africa on time scales of decades to millenia. Glob. Planet. Chang. 2000, 26, 137–158. [Google Scholar] [CrossRef]
- Molinari, N.A.; Ortega-Sanchez, I.R.; Messonnier, M.L.; Thompson, W.W.; Wortley, P.M.; Weintraub, E.; Bridges, C.B. The annual impact of seasonal influenza in the US: Measuring disease burden and costs. Vaccine 2007, 25, 5086–5096. [Google Scholar] [CrossRef] [PubMed]
- WHO. Vaccines against influenza WHO position paper—November 2012. Wkly. Epidemiol. Rec. 2012, 87, 461–476. [Google Scholar]
- NICD. Available online: https://www.nicd.ac.za/flu-season-is-around-the-corner/#:~:text=Although%20the%20timing%20of%20the,years%20has%20been%2019%20weeks (accessed on 12 July 2022).
- Serfling, R.E. Methods for current statistical analysis of excess pneumonia-influenza deaths. Public Health Rep. 1963, 78, 494–506. [Google Scholar] [CrossRef]
- Cowling, B.J.; Wong, I.O.L.; Ho, L.M.; Riley, S.; Leung, G.M. Methods for monitoring influenza surveillance data. Int. J. Epidemiol. 2006, 35, 1314–1321. [Google Scholar] [CrossRef]
- Vega, T.; Lozano, J.E.; Meerhoff, T.; Snacken, R.; Beauté, J.; Jorgensen, P.; Ortiz de Lejarazu, R.; Domegan, L.; Mossong, J.; Nielsen, J.; et al. Influenza surveillance in Europe: Comparing intensity levels calculated using the moving epidemic method. Influenza Other Respir. Viruses 2015, 5, 234–246. [Google Scholar] [CrossRef]
- Meerhoff, T.J.; Paget, W.J.; Aguilera, J.F.; van der Velden, J. Harmonizing the virological surveillance of influenza in Europe: Results of an 18-country survey. Virus Res. 2004, 103, 31–33. [Google Scholar] [CrossRef]
- Wang, J.; Guan, Y.; Wu, L.; Guan, X.; Cai, W.; Huang, J.; Dong, W.; Zhang, B. Changing Lengths of the Four Seasons by Global Warming. Geophys. Res. Lett. 2021, 48, e2020GL091753. [Google Scholar] [CrossRef]
- Smit, A.J.; Fitchett, J.M.; Engelbrecht, F.A.; Scholes, R.J.; Dzhivhuho, G.; Sweijd, A.N. Winter Is Coming: A Southern Hemisphere Perspective of the Environmental Drivers of SARS-CoV-2 and the Potential Seasonality of COVID-19. Int. J. Res. Public Health 2020, 17, 5634. [Google Scholar] [CrossRef]
- Wright, C.Y.; Kapwata, T.; Jean du Preez, D.; Wernecke, B.; Garland, R.M.; Nkosi, V.; Landman, W.A.; Dyson, L.; Norval, M. Major climate change-induced risks to human health in South Africa. Environ. Res. 2021, 196, 110973. [Google Scholar] [CrossRef] [PubMed]
- Cannell, J.J.; Vieth, R.; Umhau, J.; Holick, M.; Grant, W.; Madronich, S.; Garland, C.; Giovannucci, E. Epidemic influenza and vitamin D. Epidemiol. Infect. 2006, 134, 1129–1140. [Google Scholar] [CrossRef]
- Huang, D.; Taha, M.S.; Norcera, A.L.; Workman, M.D.; Amiji, M.M.; Bleier, B.S. Cold exposure impairs extracellular vesicle swarm-mediated nasal antiviral immunity. J. Allergy Clin. Immunol. 2022, 150, 1249–1566. [Google Scholar] [CrossRef] [PubMed]
- CDC. Available online: https://www.cdc.gov/flu/about/season/flu-season.htm (accessed on 12 July 2022).
- Biggerstaff, M.; Kniss, K.; Jernigan, D.B.; Brammer, L.; Bresee, J.; Garg, S.; Burns, E.; Reed, C. Systematic Assessment of Multiple Routine and Near Real-Time Indicators to Classify the Severity of Influenza Seasons and Pandemics in the United States, 2003–2004 through 2015–2016. Am. J. Epidemiol. 2018, 187, 1040–1050. [Google Scholar] [CrossRef] [PubMed]
- Petrie, J.G.; Lauring, A.S.; Martin, E.T.; Kaye, K.S. Hospital Associated Respiratory Virus Infection in Children and Adults: It Does Not Just Occur During Cold and Flu Season. Open Forum Infect. Dis. 2020, 7, ofaa200. [Google Scholar] [CrossRef]
- Eurich, D.T.; Marrie, T.J.; Johnstone, J.; Majumdar, S.R. Mortality Reduction with Influenza Vaccine in Patients with Pneumonia Outside “Flu” Season Pleiotropic Benefits or Residual Confounding? Am. J. Respir. Crit. Care Med. 2008, 178, 527–533. [Google Scholar] [CrossRef]
- Landman, W.A.; Malherbe, J.; Engelbrecht, F. South Africa’s present-day climate. In Understanding the Social and Environmental Implications of Global Change; Mambo, J., Faccer, K., Eds.; Africa Sun Media: Stellenbosch, South Africa, 2017. [Google Scholar]
- Lennard, C. Multi-Scale Drivers of the South African Weather and Climate. In The Geography of South Africa; Knight, J., Rogerson, C.M., Eds.; Springer: Cham, Switzerland, 2019. [Google Scholar]
- Botai, C.M.; Botai, J.O.; Adeola, A.M. The spatial distribution of temporal precipitation contrasts in South Africa. S. Afr. J. Sci. 2018, 114, 70–78. [Google Scholar] [CrossRef]
- Lennard, C.; Hegerl, G. Relating changes in synoptic circulation to the surface rainfall response using self-organising maps. Clim. Dyn. 2015, 44, 861–879. [Google Scholar] [CrossRef]
- Schulze, R.E.; Maharaj, M. Rainfall seasonality. In South African Atlas of Climatology and Agrohydrology; WRC Report 1489/1/06; Schulze, R.E., Ed.; Water Research Commission: Pretoria, South Africa, 2007. [Google Scholar]
- Roffe, S.J.; Fitchett, J.M.; Curtis, C.J. Classifying and mapping rainfall seasonality in South Africa: A review. S. Afr. Geogr. J. 2019, 101, 158–174. [Google Scholar] [CrossRef]
- Taljaard, J.J. Atmospheric Circulation Systems, Synoptic Climatology, and Weather Phenomena of South Africa. Part 6. Rainfall in South Africa; Technical Paper No. 32; Government Print: Pretoria, South Africa, 1996.
- Tyson, P.D.; Preston-Whyte, R.A. The Weather and Climate of Southern Africa; Oxford University Press: Cape Town, South Africa, 2000. [Google Scholar]
- Jury, M.R. Climate trends across South Africa since 1980. Water SA 2018, 44, 297–307. [Google Scholar] [CrossRef]
- Maphumulo, W.T.; Bhengu, B.R. Challenges of quality improvement in the healthcare of South Africa post-apartheid: A critical review. Curations 2019, 42, 1901. [Google Scholar] [CrossRef] [PubMed]
- Republic of South Africa Department of Health. National Health Insurance for South Africa: Towards Universal Health Coverage; Republic of South Africa Department of Health: Pretoria, South Africa, 2015.
- Mail & Guardian. Available online: http://mg.co.za/article/2015-08-22-nhi-to-reduce-cost-of-healthcare (accessed on 6 August 2022).
- NHI White Paper Released. SA News. Available online: http://www.sanews.gov.za/south-africa/nhi-white-paper-released (accessed on 12 August 2022).
- Suliman, R.; Mtsweni, J. Adding up the numbers: COVID-19 in South Africa. S. Afr. J. Sci. 2022, 118, 13874. [Google Scholar] [CrossRef]
- Horwitz, S. Baragwanath Hospital, Soweto: A History of Medical Care 1941–1990; Wits University Press: Johannesburg, South Africa, 2013. [Google Scholar]
- Huddle, K.R.L. Baragwanath Hospital, Soweto: A History of Medical Care 1941–1990: A Short Review; Adler Museum Bulletin 39; Wits University Press: Johannesburg, South Africa, 2013. [Google Scholar]
- NICD. Available online: https://www.nicd.ac.za/influenza-season-approaching/ (accessed on 12 July 2022).
- Battisti, D.S.; Naylor, R.L. Historical warnings of future food insecurity with unprecedented seasonal heat. Science 2009, 323, 240–244. [Google Scholar] [CrossRef]
- Tshiala, M.F.; Olwoch, J.M.; Engelbrecht, F.A. Analysis of temperature trends over Limpopo Province, South Africa. J. Geogr. Geol. 2011, 3, 13–21. [Google Scholar] [CrossRef]
- De Cian, E.; Lanzi, E.; Roson, R. Seasonal temperature variations, and energy demand. Clim. Chang. 2013, 116, 805–825. [Google Scholar] [CrossRef]
- Fitchett, J.; Robinson, D.; Hoogendoorn, G. Climate suitability for tourism in South Africa. J. Sustain. Tour. 2016, 25, 851–867. [Google Scholar] [CrossRef]
- Lazenby, M.J.; Landman, W.A.; Garland, R.M.; DeWitt, D.G. Seasonal temperature prediction skill over southern Africa and human health. Meteorol. Appl. 2014, 21, 963–974. [Google Scholar] [CrossRef]
- Ziervogel, G.; New, M.; Van Garderen, E.A.; Midgley, G.; Taylor, A.; Hamann, R. Climate change impacts and adaptation in South Africa. Clim. Chang. 2014, 5, 605–620. [Google Scholar] [CrossRef]
- Van der Walt, A.J.; Fitchett, J.M. Statistical classification of South African seasonal divisions based on daily temperature data. S. Afr. J. Sci. 2020, 116, 1–15. [Google Scholar] [CrossRef]
- UNHCR. Available online: https://emergency.unhcr.org/entry/115610/disease-surveillance-thresholds (accessed on 28 July 2022).
- Parham, P.E.; Michael, E. Modeling the Effects of Weather and Climate Change on Malaria Transmissions. Environ. Health Perspect. 2010, 118, 620–626. [Google Scholar] [CrossRef] [PubMed]
- Tempia, S.; Walaza, S.; Bhiman, J.N.; McMorrow, M.L.; Moyes, J.; Mkhencele, T.; Meiring, S.; Quan, V.; Bishop, K.; McAnerney, J.M.; et al. The decline of influenza and respiratory syncytial virus detection in facility-based surveillance during the COVID-19 pandemic, South Africa, January to October 2020. Eurosurveillance 2021, 26, 2001600. [Google Scholar] [CrossRef]
- Jassat, W.; Karim, S.S.A.; Mudara, C.; Welch, R.; Ozougwu, L.; Groome, M.J.; Govender, N.; von Gottberg, A.; Wolter, N.; Wolmarans, M.; et al. Clinical severity of COVID-19 in patients admitted to hospital during the omicron wave in South Africa: A retrospective observational study. Lancet 2022, 10, 961–969. [Google Scholar] [CrossRef] [PubMed]
- Albuquerque, E. Brazil and the middle-income trap: Its historical roots. Seoul J. Econ. 2019, 32, 23–62. [Google Scholar]

Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Motlogeloa, O.; Fitchett, J.M.; Sweijd, N. Defining the South African Acute Respiratory Infectious Disease Season. Int. J. Environ. Res. Public Health 2023, 20, 1074. https://doi.org/10.3390/ijerph20021074
Motlogeloa O, Fitchett JM, Sweijd N. Defining the South African Acute Respiratory Infectious Disease Season. International Journal of Environmental Research and Public Health. 2023; 20(2):1074. https://doi.org/10.3390/ijerph20021074
Chicago/Turabian StyleMotlogeloa, Ogone, Jennifer M. Fitchett, and Neville Sweijd. 2023. "Defining the South African Acute Respiratory Infectious Disease Season" International Journal of Environmental Research and Public Health 20, no. 2: 1074. https://doi.org/10.3390/ijerph20021074
APA StyleMotlogeloa, O., Fitchett, J. M., & Sweijd, N. (2023). Defining the South African Acute Respiratory Infectious Disease Season. International Journal of Environmental Research and Public Health, 20(2), 1074. https://doi.org/10.3390/ijerph20021074





