Increased Risk of Developing Depression in Disability after Stroke: A Korean Nationwide Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Data Source
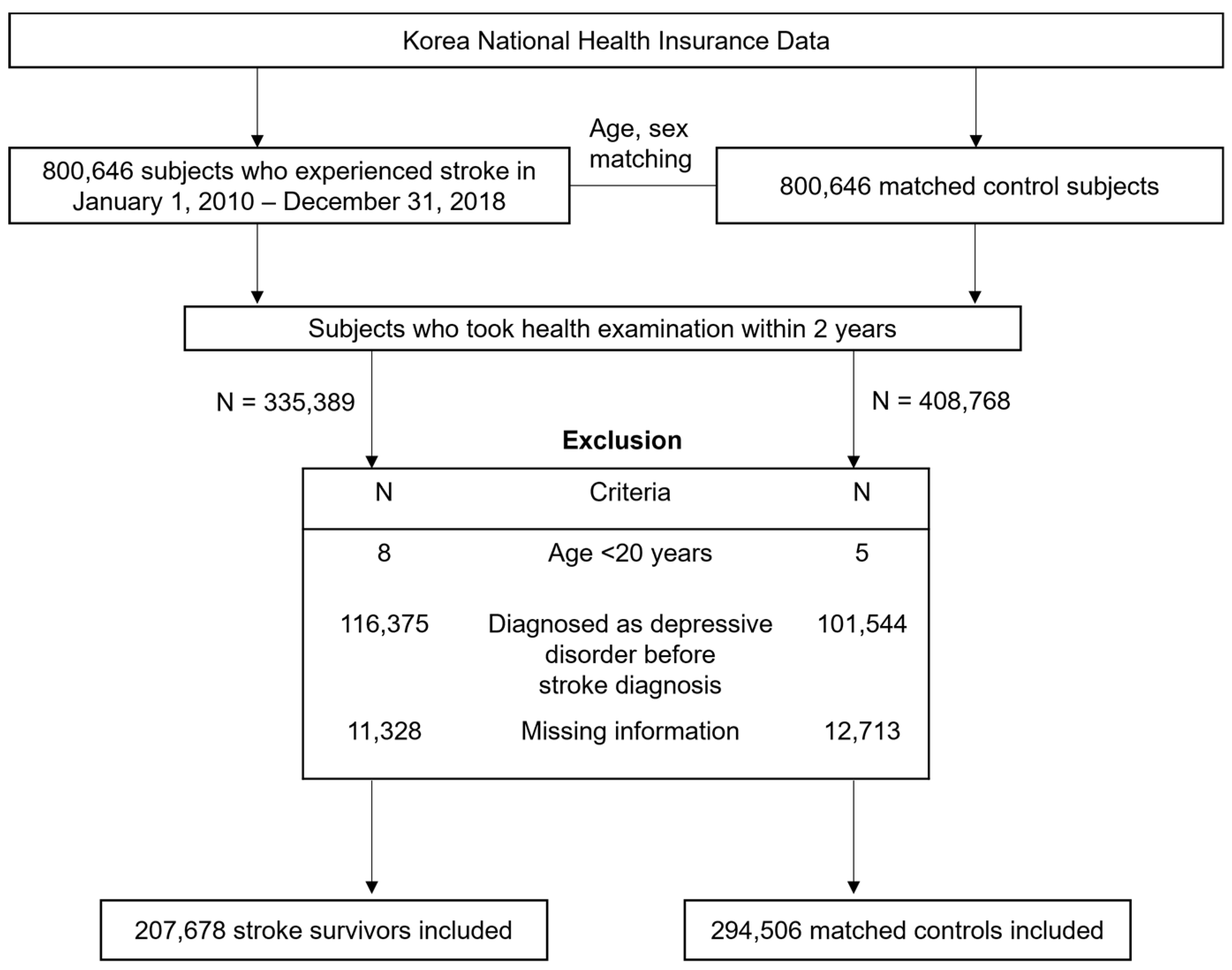
2.2. Study Population
2.3. Assessment of Stroke Severity
2.4. Study Outcomes and Follow-Up
2.5. Covariates
2.6. Statistical Analysis
3. Results
3.1. Baseline Demographics
3.2. Risk of Depression in Stroke Survivors Compared to Matched Control Subjects
3.3. Risk of Depression in Stroked Survivors by Survival Periods
3.4. Risk of Depression in Stroked Survivors by Age and Sex
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Feigin, V.L.; Stark, B.A.; Johnson, C.O.; Roth, G.A.; Bisignano, C.; Abady, G.G.; Abbasifard, M.; Abbasi-Kangevari, M.; Abd-Allah, F.; Abedi, V.; et al. Global, regional, and national burden of stroke and its risk factors, 1990–2019: A systematic analysis for the Global Burden of Disease Study 2019. Lancet Neurol. 2021, 20, 795–820. [Google Scholar] [CrossRef]
- Yoon, S.-J.; Bae, S.-C.; Lee, S.-I.; Chang, H.; Jo, H.S.; Sung, J.-H.; Park, J.-H.; Lee, J.-Y.; Shin, Y. Measuring the Burden of Disease in Korea. J. Korean Med. Sci. 2007, 22, 518–523. [Google Scholar] [CrossRef]
- Carmo JFd Morelato, R.L.; Pinto, H.P.; Oliveira, E.R.A.d. Disability after stroke: A systematic review. Fisioter. Mov. 2015, 28, 407–418. [Google Scholar] [CrossRef]
- Gaete, J.M.; Bogousslavsky, J. Post-stroke depression. Expert Rev. Neurother. 2008, 8, 75–92. [Google Scholar] [CrossRef] [PubMed]
- Robinson, R.G.; Jorge, R.E. Post-Stroke Depression: A Review. Am J Psychiatry. 2016, 173, 221–231. [Google Scholar] [CrossRef]
- Hackett, M.L.; Pickles, K. Part I: Frequency of Depression after Stroke: An Updated Systematic Review and Meta-Analysis of Observational Studies. Int. J. Stroke 2014, 9, 1017–1025. [Google Scholar] [CrossRef] [PubMed]
- Jørgensen, T.S.; Wium-Andersen, I.K.; Wium-Andersen, M.K.; Jørgensen, M.B.; Prescott, E.; Maartensson, S.; Kragh-Andersen, P.; Osler, M. Incidence of depression after stroke, and associated risk factors and mortality outcomes, in a large cohort of Danish patients. JAMA Psychiatry 2016, 73, 1032–1040. [Google Scholar] [CrossRef]
- Turner-Stokes, L.; Hassan, N. Depression after stroke: A review of the evidence base to inform the development of an integrated care pathway. Part 1: Diagnosis, frequency and impact. Clin. Rehabil. 2002, 16, 231–247. [Google Scholar] [CrossRef]
- Paolucci, S. Epidemiology and treatment of post-stroke depression. Neuropsychiatr. Dis. Treatment. 2008, 4, 145. [Google Scholar]
- Hackett, M.L.; Yapa, C.; Parag, V.; Anderson, C. Frequency of Depression After Stroke. Stroke 2005, 36, 1330–1340. [Google Scholar] [CrossRef]
- Robinson, R.G.; Price, T.R. Post-stroke depressive disorders: A follow-up study of 103 patients. Stroke 1982, 13, 635–641. [Google Scholar] [CrossRef] [PubMed]
- Andersen, G.; Vestergaard, K.; Ingemann-Nielsen, M.; Lauritzen, L. Risk factors for post-stroke depression. Acta Psychiatr. Scand. 1995, 92, 193–198. [Google Scholar] [CrossRef]
- Aben, I.; Denollet, J.; Lousberg, R.; Verhey, F.; Wojciechowski, F.; Honig, A. Personality and vulnerability to depression in stroke patients: A 1-year prospective follow-up study. Stroke 2002, 33, 2391–2395. [Google Scholar] [CrossRef] [PubMed]
- Appelros, P.; Viitanen, M. Prevalence and predictors of depression at one year in a Swedish population-based cohort with first-ever stroke. J. Stroke Cerebrovasc. Dis. 2004, 13, 52–57. [Google Scholar] [CrossRef] [PubMed]
- Shin, D.W.; Cho, B.; Guallar, E. Korean National Health Insurance Database. JAMA Intern. Med. 2016, 176, 138. [Google Scholar] [CrossRef]
- Shin, D.W.; Cho, J.; Park, J.H.; Cho, B. National General Health Screening Program in Korea: History, current status, and future direction. Precis. Futur. Med. 2022, 6, 9–31. [Google Scholar] [CrossRef]
- Lee, S.W.; Lee, H.-Y.; Ihm, S.H.; Park, S.H.; Kim, T.H.; Kim, H.C. Status of hypertension screening in the Korea National General Health Screening Program: A questionnaire survey on 210 screening centers in two metropolitan areas. Clin. Hypertens. 2017, 23, 23. [Google Scholar] [CrossRef] [PubMed]
- Cheol Seong, S.; Kim, Y.Y.; Khang, Y.H.; Heon Park, J.; Kang, H.J.; Lee, H.; Do, C.H.; Song, J.S.; Hyon Bang, J.; Ha, S.; et al. Data Resource Profile: The National Health Information Database of the National Health Insurance Service in South Korea. Int. J. Epidemiol. 2017, 46, 799–800. [Google Scholar] [CrossRef]
- Lee, H.R.; Yoo, J.E.; Choi, H.; Han, K.; Jung, J.H.; Park, J.; Lee, H.; Shin, D.W. Tuberculosis and Risk of Ischemic Stroke: A Nationwide Cohort Study. Stroke 2022, 53, 3401–3409. [Google Scholar] [CrossRef]
- Jeong, S.-M.; Lee, H.R.; Han, K.; Jeon, K.H.; Kim, D.; Yoo, J.E.; Cho, M.H.; Chun, S.; Lee, S.P.; Nam, K.-W.; et al. Association of Change in Alcohol Consumption with Risk of Ischemic Stroke. Stroke 2022, 53, 2488–2496. [Google Scholar] [CrossRef]
- Choi, E.-K. Cardiovascular Research Using the Korean National Health Information Database. Korean Circ. J. 2020, 50, 754–772. [Google Scholar] [CrossRef] [PubMed]
- Shin, D.W.; Park, J.; Yeob, K.E.; Yoon, S.J.; Jang, S.N.; Kim, S.Y.; Park, J.H.; Park, J.H.; Kawachi, I. Disparities in prostate cancer diagnosis, treatment, and survival among men with disabilities: Retrospective cohort study in South Korea. Disabil. Health J. 2021, 14, 101125. [Google Scholar] [CrossRef] [PubMed]
- Shin, D.W.; Yu, J.; Cho, J.; Lee, S.K.; Ms, J.H.J.; Han, K.; Kim, S.Y.; Yoo, J.E.; Yeob, K.E.; Kim, Y.Y.; et al. Breast cancer screening disparities between women with and without disabilities: A national database study in South Korea. Cancer 2020, 126, 1522–1529. [Google Scholar] [CrossRef]
- Park, M.J.; Yoo, J.; Han, K.; Shin, D.W.; Fava, M.; Mischoulon, D.; Jeon, H.J. High body weight variability is associated with increased risk of depression: A nationwide cohort study in South Korea. Psychol. Med. 2022, 1–9. [Google Scholar] [CrossRef]
- Kim, H.; Lee, K.-N.; Shin, D.W.; Han, K.; Jeon, H.J. Association of comorbid mental disorders with cardiovascular disease risk in patients with type 2 diabetes: A nationwide cohort study. Gen. Hosp. Psychiatry 2022, 79, 33–41. [Google Scholar] [CrossRef] [PubMed]
- Kim, M.; Kim, H.; Han, K.; Yoo, J.; Yang, K.; Jeon, H.J. Changes in alcohol consumption and the risk of cardiovascular diseases in patients with depression who had not consumed alcohol: A nationwide cohort study. J. Psychiatr. Res. 2022, 155, 458–464. [Google Scholar] [CrossRef]
- Kim, K.H. Comparative Study on Three Algorithms of the ICD-10 Charlson Comorbidity Index with Myocardial Infarction Patients. J. Prev. Med. Public Health 2010, 43, 42–49. [Google Scholar] [CrossRef]
- Facucho-Oliveira, J.; Esteves-Sousa, D.; Espada-Santos, P.; Moura, N.; Albuquerque, M.; Fraga, A.M.; Sousa, S.; Cintra, P.; Mendonça, L.; Pita, F. Depression after stroke. Pract. Neurol. 2021, 21, 384–391. [Google Scholar] [CrossRef]
- White, J.H.; Attia, J.; Sturm, J.; Carter, G.; Magin, P. Predictors of depression and anxiety in community dwelling stroke survivors: A cohort study. Disabil. Rehabilitation 2014, 36, 1975–1982. [Google Scholar] [CrossRef]
- Ezema, C.I.; Akusoba, P.C.; Nweke, M.C.; Uchewoke, C.U.; Agono, J.; Usoro, G. Influence of Post-Stroke Depression on Functional Independence in Activities of Daily Living. Ethiop. J. Health Sci. 2019, 29, 841–846. [Google Scholar] [CrossRef] [PubMed]
- Das, J.; Rajanikant, G.K. Post stroke depression: The sequelae of cerebral stroke. Neurosci. Biobehav. Rev. 2018, 90, 104–114. [Google Scholar] [CrossRef] [PubMed]
- Winstein, C.J.; Stein, J.; Arena, R.; Bates, B.; Cherney, L.R.; Cramer, S.C.; DeRuyter, F.; Eng, J.J.; Fisher, B.; Harvey, R.L.; et al. Guidelines for Adult Stroke Rehabilitation and Recovery. Stroke 2016, 47, e98–e169. [Google Scholar] [CrossRef] [PubMed]
- Gittler, M.; Davis, A.M. Guidelines for Adult Stroke Rehabilitation and Recovery. JAMA 2018, 319, 820–821. [Google Scholar] [CrossRef] [PubMed]
- Gainotti, G.; Antonucci, G.; Marra, C.; Paolucci, S. Relation between depression after stroke, antidepressant therapy, and functional recovery. J. Neurol. Neurosurg. Psychiatry 2001, 71, 258–261. [Google Scholar] [CrossRef]
- Chemerinski, E.; Robinson, R.G.; Kosier, J.T. Improved Recovery in Activities of Daily Living Associated With Remission of Poststroke Depression. Stroke 2001, 32, 113–117. [Google Scholar] [CrossRef] [PubMed]
- Grabowska-Fudala, B.; Jaracz, K.; Górna, K.; Miechowicz, I.; Wojtasz, I.; Jaracz, J.; Kaźmierski, R. Depressive symptoms in stroke patients treated and non-treated with intravenous thrombolytic therapy: A 1-year follow-up study. J. Neurol. 2018, 265, 1891–1899. [Google Scholar] [CrossRef] [PubMed]
- Koivunen, R.-J.; Harno, H.; Tatlisumak, T.; Putaala, J. Depression, anxiety, and cognitive functioning after intracerebral hemorrhage. Acta Neurol. Scand. 2015, 132, 179–184. [Google Scholar] [CrossRef] [PubMed]
- Kotila, M.; Numminen, H.; Waltimo, O.; Kaste, M. Depression after stroke: Results of the FINNSTROKE Study. Stroke 1998, 29, 368–372. [Google Scholar] [CrossRef]
- House, A.; Dennis, M.; Mogridge, L.; Warlow, C.; Hawton, K.; Jones, L. Mood Disorders in the Year after First Stroke. Br. J. Psychiatry 1991, 158, 83–92. [Google Scholar] [CrossRef]
- Andersen, G.; Vestergaard, K.; Riis, J.Ø.; Lauritzen, L. Incidence of post-stroke depression during the first year in a large unselected stroke population determined using a valid standardized rating scale. Acta Psychiatrica Scandinavica. 1994, 90, 190–195. [Google Scholar] [CrossRef]
- Loubinoux, I.; Kronenberg, G.; Endres, M.; Schumann-Bard, P.; Freret, T.; Filipkowski, R.K.; Kaczmarek, L.; Popa-Wagner, A. Post-stroke depression: Mechanisms, translation and therapy. J. Cell. Mol. Med. 2012, 16, 1961–1969. [Google Scholar] [CrossRef]
- Villa, R.F.; Ferrari, F.; Moretti, A. Post-stroke depression: Mechanisms and pharmacological treatment. Pharmacol. Ther. 2018, 184, 131–144. [Google Scholar] [CrossRef] [PubMed]
- Bryer, J.B.; Starkstein, S.E.; Votypka, V.; Parikh, R.M.; Price, T.R.; Robinson, R.G. Reduction of CSF monoamine metabolites in poststroke depression: A preliminary report. J. Neuropsychiatry Clin. Neurosci. 1992, 4, 440–442. [Google Scholar] [PubMed]
- Medeiros, G.C.; Roy, D.; Kontos, N.; Beach, S.R. Post-stroke depression: A 2020 updated review. Gen. Hosp. Psychiatry 2020, 66, 70–80. [Google Scholar] [CrossRef]
- Guo, J.; Wang, J.; Sun, W.; Liu, X. The advances of post-stroke depression: 2021 update. J. Neurol. 2021, 269, 1236–1249. [Google Scholar] [CrossRef] [PubMed]
- Otte, C.; Gold, S.M.; Penninx, B.W.; Pariante, C.M.; Etkin, A.; Fava, M.; Mohr, D.C.; Schatzberg, A.F. Major depressive disorder. Nat. Rev. Dis. Primers. 2016, 2, 16065. [Google Scholar] [CrossRef] [PubMed]
- Noonan, K.; Carey, L.M.; Crewther, S.G. Meta-analyses Indicate Associations between Neuroendocrine Activation, Deactivation in Neurotrophic and Neuroimaging Markers in Depression after Stroke. J. Stroke Cerebrovasc. Dis. 2013, 22, e124–e135. [Google Scholar] [CrossRef] [PubMed]
- Mitchell, A.J. Clinical implications of poststroke hypothalamo-pituitary adrenal axis dysfunction: A critical literature review. J. Stroke Cerebrovasc. Dis. 1997, 6, 377–388. [Google Scholar] [CrossRef]
- Zhou, Y.; Danbolt, N.C. Glutamate as a neurotransmitter in the healthy brain. J. Neural Transm. 2014, 121, 799–817. [Google Scholar] [CrossRef] [PubMed]
- Haroon, E.; Miller, A.H.; Sanacora, G. Inflammation, Glutamate, and Glia: A Trio of Trouble in Mood Disorders. Neuropsychopharmacology 2016, 42, 193–215. [Google Scholar] [CrossRef]
- Folstein, M.F.; Maiberger, R.; McHugh, P.R. Mood disorder as a specific complication of stroke. J. Neurol. Neurosurg. Psychiatry 1977, 40, 1018–1020. [Google Scholar] [CrossRef] [PubMed]
- Sanacora, G.; Treccani, G.; Popoli, M. Towards a glutamate hypothesis of depression: An emerging frontier of neuropsychopharmacology for mood disorders. Neuropharmacology 2012, 62, 63–77. [Google Scholar] [CrossRef] [PubMed]
- Cheng, S.Y.; Zhao, Y.D.; Li, J.; Chen, X.Y.; Wang, R.D.; Zeng, J.W. Plasma levels of glutamate during stroke is associated with development of post-stroke depression. Psychoneuroendocrinology 2014, 47, 126–135. [Google Scholar] [CrossRef] [PubMed]
- Hong, W.; Zhao, Z.; Wang, D.; Li, M.; Tang, C.; Li, Z.; Xu, R.; Chan, C.C. Altered gray matter volumes in post-stroke depressive patients after subcortical stroke. NeuroImage Clin. 2020, 26, 102224. [Google Scholar] [CrossRef] [PubMed]
- Droppa, K.; Karim, H.T.; Tudorascu, D.L.; Karp, J.F.; Reynolds, C.F., III; Aizenstein, H.J.; Butters, M.A. Association between change in brain gray matter volume, cognition, and depression severity: Pre- and post- antidepressant pharmacotherapy for late-life depression. J. Psychiatr. Res. 2017, 95, 129–134. [Google Scholar] [CrossRef] [PubMed]
- Jiang, Y.; Duan, M.; Chen, X.; Zhang, X.; Gong, J.; Dong, D.; Li, H.; Yi, Q.; Wang, S.; Wang, J.; et al. Aberrant Prefrontal–Thalamic–Cerebellar Circuit in Schizophrenia and Depression: Evidence from a Possible Causal Connectivity. Int. J. Neural Syst. 2019, 29, 1850032. [Google Scholar] [CrossRef]
- Kim, I.H.; Rossi, M.A.; Aryal, D.K.; Rácz, B.; Kim, N.; Uezu, A.; Wang, F.; Wetsel, W.C.; Weinberg, R.J.; Yin, H.; et al. Spine pruning drives antipsychotic-sensitive locomotion via circuit control of striatal dopamine. Nat. Neurosci. 2015, 18, 883–891. [Google Scholar] [CrossRef]
- Rubin-Falcone, H.; Weber, J.; Kishon, R.; Ochsner, K.; Delaparte, L.; Doré, B.; Raman, S.; Denny, B.T.; Oquendo, M.A.; Mann, J.J.; et al. Neural predictors and effects of cognitive behavioral therapy for depression: The role of emotional reactivity and regulation. Psychol. Med. 2019, 50, 146–160. [Google Scholar] [CrossRef]
- Sacchet, M.D.; Levy, B.J.; Hamilton, J.P.; Maksimovskiy, A.; Hertel, P.T.; Joormann, J.; Anderson, M.C.; Wagner, A.D.; Gotlib, I.H. Cognitive and neural consequences of memory suppression in major depressive disorder. Cogn. Affect. Behav. Neurosci. 2016, 17, 77–93. [Google Scholar] [CrossRef]
- Messina, I.; Sambin, M.; Palmieri, A.; Viviani, R. Neural Correlates of Psychotherapy in Anxiety and Depression: A Meta-Analysis. PLoS ONE 2013, 8, e74657. [Google Scholar] [CrossRef]
- Ayerbe, L.; Ayis, S.; Wolfe, C.; Rudd, A.G. Natural history, predictors and outcomes of depression after stroke: Systematic review and meta-analysis. Br. J. Psychiatry 2013, 202, 14–21. [Google Scholar] [CrossRef]
- Ayerbe, L.; Ayis, S.; Crichton, S.; Wolfe, C.D.; Rudd, A.G. The natural history of depression up to 15 years after stroke: The South London Stroke Register. Stroke 2013, 44, 1105–1110. [Google Scholar] [CrossRef]
- SShi, Y.; Yang, D.; Zeng, Y.; Wu, W. Risk Factors for Post-stroke Depression: A Meta-analysis. Front. Aging Neurosci. 2017, 9, 218. [Google Scholar] [CrossRef] [PubMed]
- De Ryck, A.; Brouns, R.; Geurden, M.; Elseviers, M.; De Deyn, P.P.; Engelborghs, S. Risk factors for poststroke depression: Identification of inconsistencies based on a systematic review. J. Geriatr. Psychiatry Neurol. 2014, 27, 147–158. [Google Scholar] [CrossRef] [PubMed]
- Wong, Y.J.; Tsai, P.C.; Liu, T.; Zhu, Q.; Wei, M. Male Asian international students’ perceived racial discrimination, masculine identity, and subjective masculinity stress: A moderated mediation model. J. Couns. Psychol. 2014, 61, 560–569. [Google Scholar] [CrossRef]
- Shin, Y.-C.; Lee, D.; Seol, J.; Lim, S.-W. What kind of stress is associated with depression, anxiety and suicidal ideation in Korean employees? J. Korean Med. Sci. 2017, 32, 843–849. [Google Scholar] [CrossRef] [PubMed]
- Alajbegovic, A.; Djelilovic-Vranic, J.; Nakicevic, A.; Todorovic, L.; Tiric-Campara, M. Post stroke depression. Med. Arch. 2014, 68, 47–50. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Zhao, Y.D.; Zeng, J.W.; Chen, X.Y.; Wang, R.D.; Cheng, S.Y. Serum Brain-derived neurotrophic factor levels in post-stroke depression. J Affect Disord. 2014, 168, 373–379. [Google Scholar] [CrossRef]

| Control Group | Stroke Survivors | p-Value | Control Group | Stroke Survivors without Disability | Stroke Survivors with Disability | p-Value | |
|---|---|---|---|---|---|---|---|
| (N = 294,506) | (N = 207,678) | (N = 294,506) | (N = 185,183) | (N = 22,495) | |||
| Age | 64.56 ± 12.2 | 64.6 ± 12.11 | 0.268 | 64.56 ± 12.2 | 64.38 ± 12.26 | 66.42 ± 10.61 | <0.001 |
| Sex, male | 182,928 (62.1) | 129,674 (62.4) | 0.019 | 182,928 (62.1) | 115,021 (62.1) | 14,653 (65.1) | <0.001 |
| Income, low 25% | 55,466 (18.8) | 44,770 (21.6) | <0.001 | 55,466 (18.8) | 39,216 (21.2) | 5554 (24.7) | <0.001 |
| Place, urban | 129,826 (44.1) | 84,428 (40.7) | <0.001 | 129,826 (44.1) | 75,758 (40.9) | 8670 (38.5) | <0.001 |
| Regular exercise | 65,370 (22.2) | 38,795 (18.7) | <0.001 | 65,370 (22.2) | 34,908 (18.9) | 3887 (17.3) | <0.001 |
| Follow up duration | 4.89 ± 2.59 | 3.31 ± 2.8 | <0.001 | 4.89 ± 2.59 | 3.33 ± 2.81 | 3.19 ± 2.77 | <0.001 |
| DM | 52,235 (17.7) | 60,984 (29.4) | <0.001 | 52,235 (17.7) | 53,423 (28.9) | 7561 (33.6) | <0.001 |
| HTN | 145,176 (49.3) | 158,136 (76.1) | <0.001 | 145,176 (49.3) | 139,678 (75.4) | 18,458 (82.1) | <0.001 |
| Dyslipidemia | 97,759 (33.2) | 138,773 (66.8) | <0.001 | 97,759 (33.2) | 123,697 (66.8) | 15,076 (67.0) | <0.001 |
| Smoking | <0.001 | <0.001 | |||||
| None | 172,707 (58.6) | 113,310 (54.6) | 172,707 (58.6) | 100,907 (54.5) | 12,403 (55.1) | ||
| Ex- | 66,065 (22.4) | 37,369 (18.0) | 66,065 (22.4) | 33,245 (18.0) | 4124 (18.3) | ||
| Current | 55,734 (18.9) | 56,999 (27.5) | 55,734 (18.9) | 51,031 (27.6) | 5968 (26.5) | ||
| Alcohol consumption | <0.001 | <0.001 | |||||
| None | 174,887 (59.4) | 122,215 (58.9) | 174,887 (59.4) | 108,200 (58.4) | 14,015 (62.3) | ||
| Mild | 98,326 (33.4) | 66,813 (32.2) | 98,326 (33.4) | 60,287 (32.6) | 6526 (29.0) | ||
| Heavy | 21,293 (7.2) | 18,650 (9.0) | 21,293 (7.2) | 16,696 (9.0) | 1954 (8.7) | ||
| CCI | 1.58 ± 1.75 | 4.15 ± 2.31 | <0.001 | 1.58 ± 1.75 | 4.15 ± 2.31 | 4.57 ± 2.37 | <0.001 |
| BMI | 24.07 ± 3.07 | 24.22 ± 3.24 | <0.001 | 24.07 ± 3.07 | 24.22 ± 3.24 | 24.44 ± 3.33 | <0.001 |
| Waist circumference | 83.07 ± 8.53 | 83.83 ± 8.7 | <0.001 | 83.07 ± 8.53 | 83.83 ± 8.7 | 85.03 ± 8.72 | <0.001 |
| Glucose | 103.47 ± 26.1 | 110.35 ± 37.96 | <0.001 | 103.47 ± 26.1 | 110.35 ± 37.96 | 111.34 ± 38.29 | <0.001 |
| SBP | 127.12 ± 15.33 | 132.28 ± 17.74 | <0.001 | 127.12 ± 15.33 | 132.28 ± 17.74 | 132.99 ± 17.68 | <0.001 |
| DBP | 77.45 ± 9.84 | 80.54 ± 11.52 | <0.001 | 77.45 ± 9.84 | 80.54 ± 11.52 | 80.64 ± 11.35 | <0.001 |
| Total cholesterol | 195 ± 38.12 | 197.89 ± 40.78 | <0.001 | 195 ± 38.12 | 197.89 ± 40.78 | 196.38 ± 40.6 | <0.001 |
| TG | 117.8 (117.58–118.03) | 126.64 (126.35–126.93) | <0.001 | 117.8 (117.58–118.03) | 126.43 (126.12–126.74) | 128.42 (127.54–129.3) | <0.001 |
| GFR | 85.68 ± 43.19 | 83.92 ± 40.03 | <0.001 | 85.68 ± 43.19 | 83.92 ± 40.03 | 84.02 ± 42.15 | <0.001 |
| N | IR (per 1000 PYs) | HR (95% CI) | |||
|---|---|---|---|---|---|
| Unadjusted | Adjusted (Model 1) | Adjusted (Model 2) | |||
| Comparison between stroke survivors and control group | |||||
| Control | 294,506 | 34.40 | 1 (ref.) | 1 (ref.) | 1 (ref.) |
| Stroke survivors | 207,678 | 98.05 | 2.69 (2.66–2.73) | 2.21 (2.18–2.24) | 2.12 (2.09–2.15) |
| Comparison between stroke survivors with, and without disability, and control group | |||||
| Control | 294,506 | 34.40 | 1 (ref.) | 1 (ref.) | 1 (ref.) |
| No disability after stroke | 185,183 | 93.28 | 2.57 (2.54–2.60) | 2.13 (2.10–2.16) | 2.04 (2.02–2.07) |
| Disability after stroke | 22,495 | 138.95 | 3.77 (3.69–3.85) | 2.87 (2.80–2.93) | 2.74 (2.68–2.81) |
| Comparison between stroke survivors without disability, with disability by the severity degrees, and control group | |||||
| Control | 294,506 | 34.40 | 1 (ref.) | 1 (ref.) | 1 (ref.) |
| No disability after stroke | 185,183 | 93.29 | 2.57 (2.54–2.60) | 2.13 (2.11–2.16) | 2.05 (2.02–2.07) |
| Mild disability after stroke | 14,705 | 123.69 | 3.39 (3.30–3.48) | 2.57 (2.50–2.65) | 2.46 (2.39–2.53) |
| Severe disability after stroke | 7790 | 173.91 | 4.60 (4.45–4.75) | 3.53 (3.41–3.65) | 3.39 (3.28–3.51) |
| First 1 Year | After 1-Year Lag | After 5-Year Lag | ||||
|---|---|---|---|---|---|---|
| IR (per 1000 PYs) | aHR (95% CI) | IR (per 1000 PYs) | aHR (95% CI) | IR (per 1000 PYs) | aHR (95% CI) | |
| Comparison between stroke survivors and control group | ||||||
| Control | 31.69 | 1 (ref.) | 35.08 | 1 (ref.) | 37.59 | 1 (ref.) |
| Stroke survivors | 220.73 | 5.02 (4.89–5.16) | 58.93 | 1.37 (1.34–1.39) | 48.64 | 1.17 (1.12–1.21) |
| Comparison between stroke survivors with, and without disability, and control group | ||||||
| Control | 31.69 | 1 (ref.) | 35.08 | 1 (ref.) | 37.59 | 1 (ref.) |
| No disability after stroke | 207.61 | 4.79 (4.67–4.92) | 57.07 | 1.34 (1.32–1.37) | 47.61 | 1.16 (1.11–1.20) |
| Disability after stroke | 328.26 | 7.14 (6.89–7.40) | 75.15 | 1.58 (1.53–1.63) | 57.81 | 1.25 (1.15–1.35) |
| Comparison between stroke survivors without disability, with disability by the severity degrees, and control group | ||||||
| Control | 31.69 | 1 (ref.) | 35.08 | 1 (ref.) | 37.59 | 1 (ref.) |
| No disability after stroke | 207.61 | 4.79 (4.67–4.92) | 57.07 | 1.34 (1.32–1.37) | 47.61 | 1.16 (1.11–1.20) |
| Mild disability after stroke | 278.46 | 6.09 (5.84–6.35) | 73.58 | 1.54 (1.48–1.60) | 59.38 | 1.28 (1.17–1.40) |
| Severe disability after stroke | 431.83 | 9.29 (8.87–9.73) | 78.87 | 1.67 (1.58–1.77) | 53.79 | 1.17 (1.01–1.36) |
| N | Depression Event | IR (per 1000 PYs) | aHR (95% CI) | p for Interaction | ||
| By age | ||||||
| Age < 65 | Control | 137,526 | 14,432 | 20.93 | 1 (ref.) | <0.001 |
| No disability after stroke | 87,533 | 24,556 | 76.36 | 2.72(2.66–2.78) | ||
| Mild disability after stroke | 5511 | 2237 | 109.39 | 3.66 (3.50–3.83) | ||
| Severe disability after stroke | 3323 | 1669 | 170.62 | 5.39 (5.12–5.67) | ||
| Age ≥ 65 | Control | 156,980 | 35,148 | 46.76 | 1 (ref.) | |
| No disability after stroke | 97,650 | 32,944 | 111.75 | 1.76 (1.73–1.79) | ||
| Mild disability after stroke | 9194 | 3940 | 133.6 | 2.04 (1.98–2.12) | ||
| Severe disability after stroke | 4467 | 2124 | 176.58 | 2.62 (2.51–2.74) | ||
| N | Depression Event | IR (per 1000 PYs) | aHR (95% CI) | p for Interaction | ||
| By sex | ||||||
| Male | Control | 182,928 | 25,659 | 28.49 | 1 (ref.) | <0.001 |
| No disability after stroke | 115,021 | 32,899 | 83.95 | 2.19 (2.15–2.23) | ||
| Mild disability after stroke | 9532 | 3734 | 113.65 | 2.73 (2.63–2.83) | ||
| Severe disability after stroke | 5121 | 2401 | 164.12 | 3.78 (3.62–3.95) | ||
| Female | Control | 111,578 | 23,921 | 44.24 | 1 (ref.) | |
| No disability after stroke | 70,162 | 24,601 | 109.58 | 1.89 (1.86–1.93) | ||
| Mild disability after stroke | 5173 | 3734 | 142.99 | 2.16 (2.07–2.25) | ||
| Severe disability after stroke | 2669 | 2401 | 193.84 | 2.92 (2.76–3.08) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Choi, H.L.; Yang, K.; Han, K.; Kim, B.; Chang, W.H.; Kwon, S.; Jung, W.; Yoo, J.E.; Jeon, H.J.; Shin, D.W. Increased Risk of Developing Depression in Disability after Stroke: A Korean Nationwide Study. Int. J. Environ. Res. Public Health 2023, 20, 842. https://doi.org/10.3390/ijerph20010842
Choi HL, Yang K, Han K, Kim B, Chang WH, Kwon S, Jung W, Yoo JE, Jeon HJ, Shin DW. Increased Risk of Developing Depression in Disability after Stroke: A Korean Nationwide Study. International Journal of Environmental Research and Public Health. 2023; 20(1):842. https://doi.org/10.3390/ijerph20010842
Chicago/Turabian StyleChoi, Hea Lim, Kyojin Yang, Kyungdo Han, Bongsung Kim, Won Hyuk Chang, Soonwook Kwon, Wonyoung Jung, Jung Eun Yoo, Hong Jin Jeon, and Dong Wook Shin. 2023. "Increased Risk of Developing Depression in Disability after Stroke: A Korean Nationwide Study" International Journal of Environmental Research and Public Health 20, no. 1: 842. https://doi.org/10.3390/ijerph20010842
APA StyleChoi, H. L., Yang, K., Han, K., Kim, B., Chang, W. H., Kwon, S., Jung, W., Yoo, J. E., Jeon, H. J., & Shin, D. W. (2023). Increased Risk of Developing Depression in Disability after Stroke: A Korean Nationwide Study. International Journal of Environmental Research and Public Health, 20(1), 842. https://doi.org/10.3390/ijerph20010842







