Did Mindful People Do Better during the COVID-19 Pandemic? Mindfulness Is Associated with Well-Being and Compliance with Prophylactic Measures
Abstract
:1. Introduction
1.1. Mindfulness as a Protective Factor during the COVID-19 Crisis
1.2. Relationship between Mindfulness and Sleep Quality and Mood
1.3. Relationship between Mindfulness and Compliance with Prophylactic Measures
1.4. Previous Evidence Collected during the COVID-19 Crisis
1.5. Our Contribution
2. Method
2.1. Data and Survey
2.2. Mindfulness Attention Awareness Scale
2.3. Well-Being
2.4. Compliant Behaviors
2.5. Control Variables
3. Results
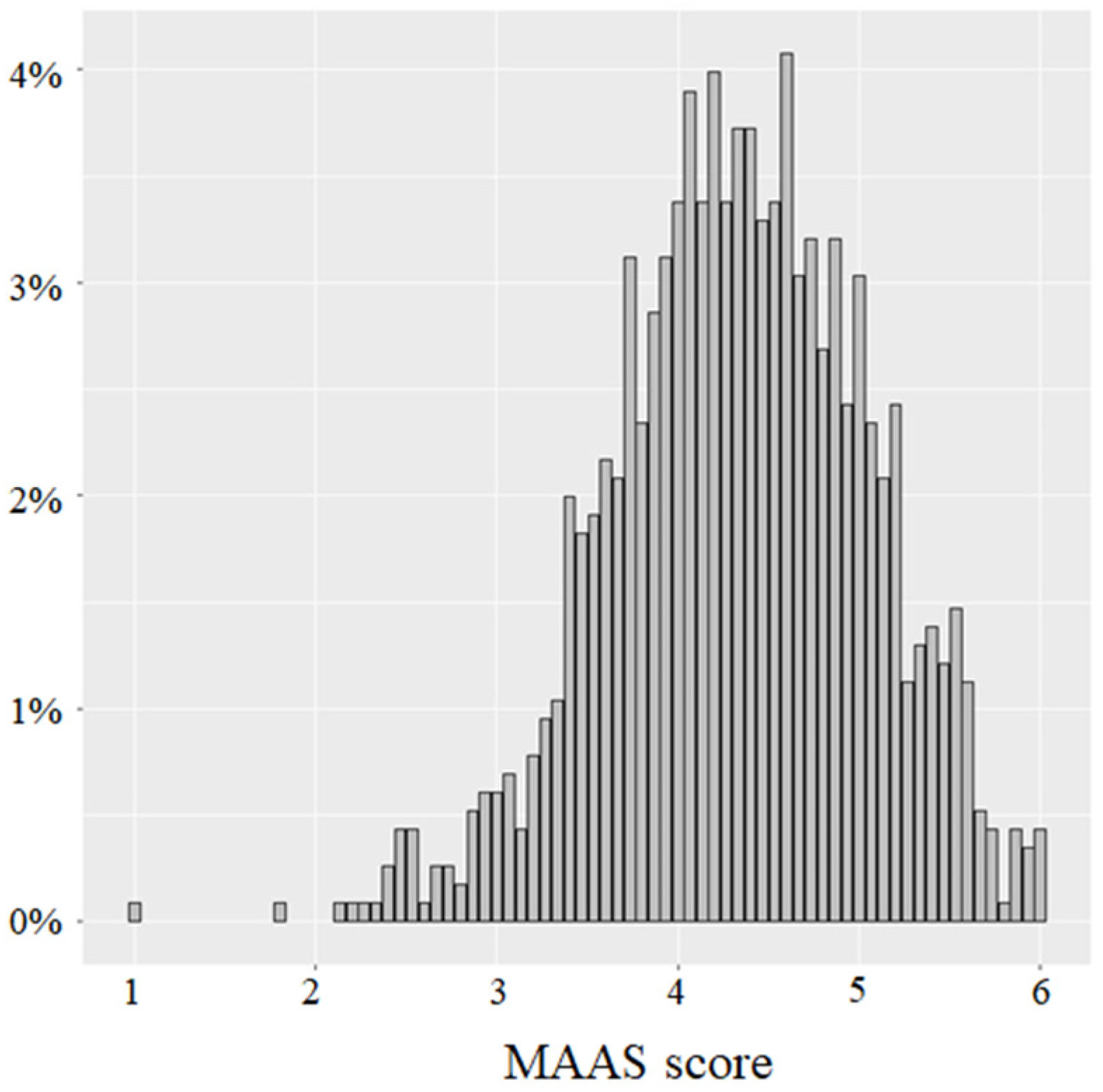
3.1. Distribution and Descriptive Statistics of the MAAS Scores
3.2. Distribution and Correlation of Dependent Variables
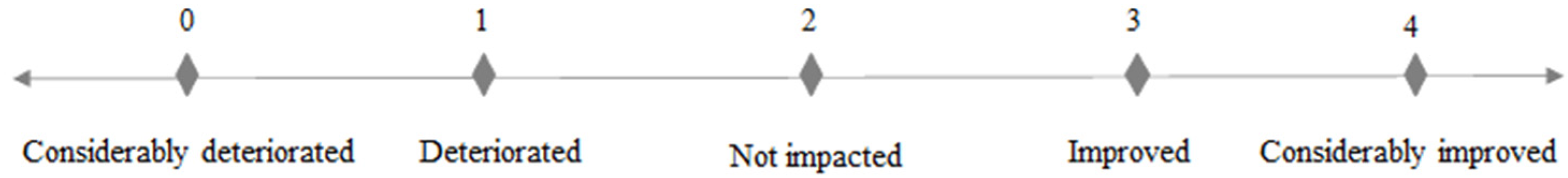
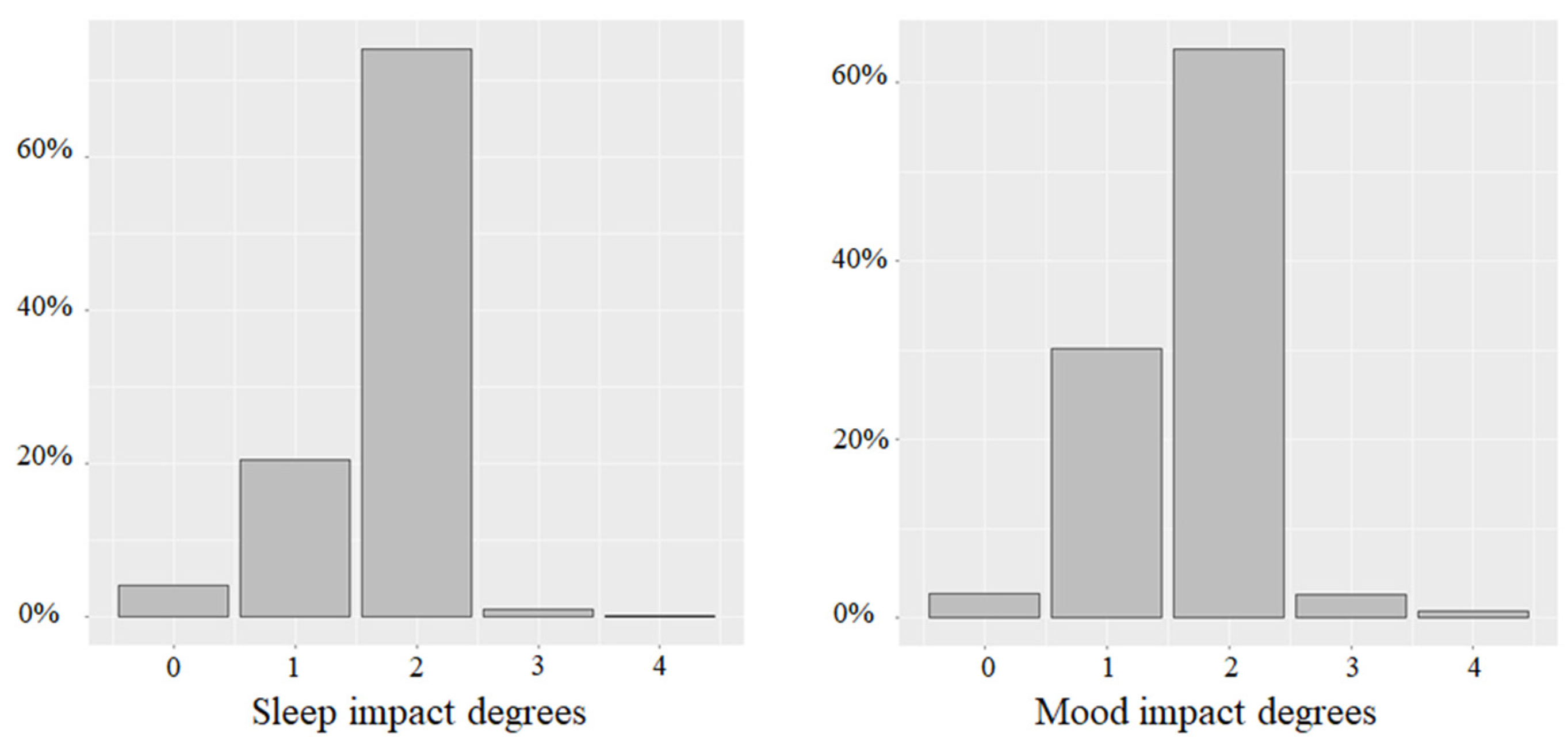
3.2.1. Well-Being
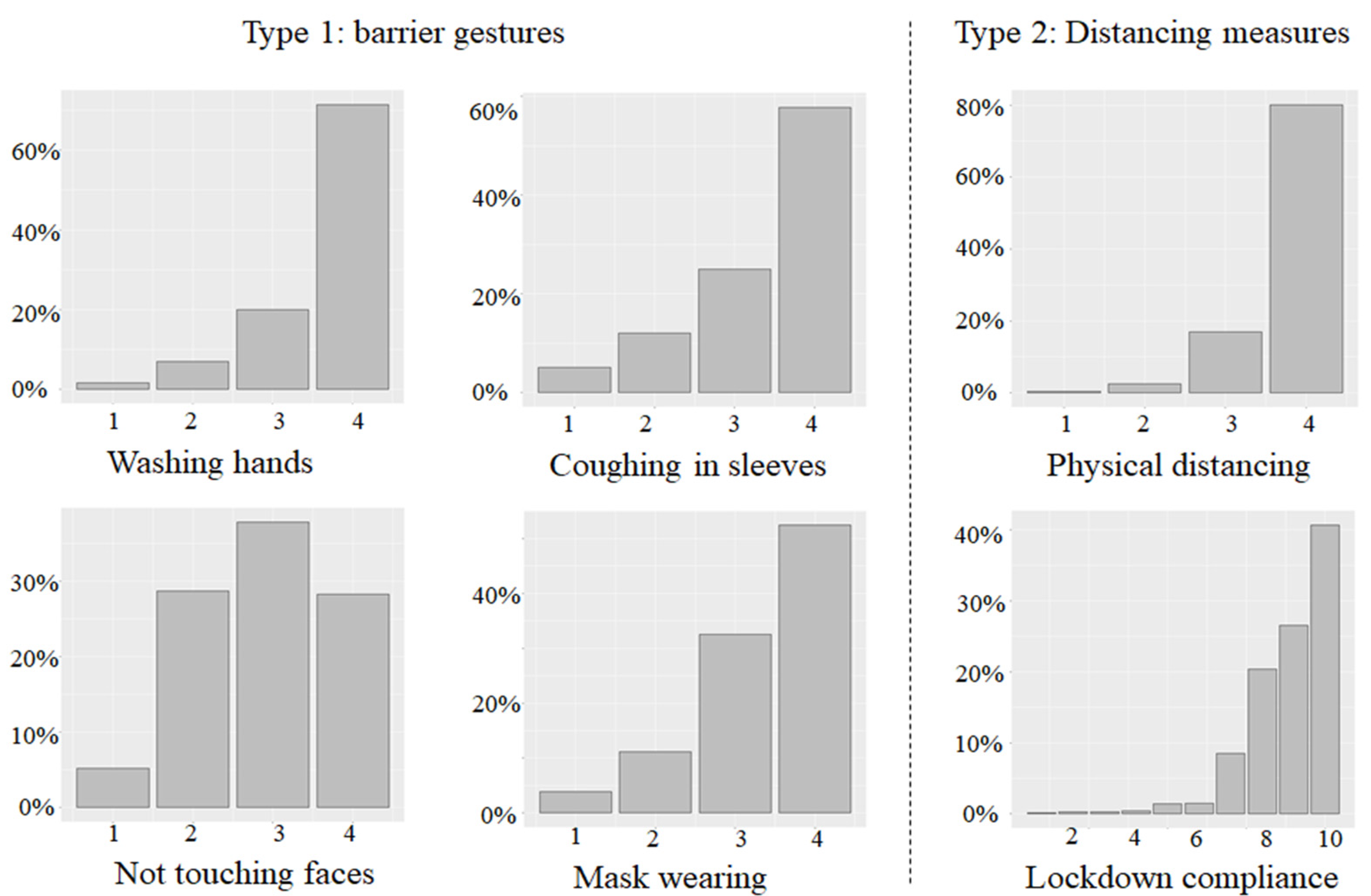
3.2.2. Compliant Behaviors
3.3. Explanatory Power of Mindfulness
3.3.1. Well-Being
3.3.2. Compliant Behaviors
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A. MAAS English and French Version


References
- Fu, L.; Wang, B.; Yuan, T.; Chen, X.; Ao, Y.; Fitzpatrick, T.; Li, P.; Zhou, Y.; Lin, Y.F.; Duan, Q.; et al. Clinical characteristics of coronavirus disease 2019 (COVID-19) in China: A systematic review and meta-analysis. J. Infect. 2020, 80, 656–665. [Google Scholar] [CrossRef]
- Guo, Y.R.; Cao, Q.D.; Hong, Z.S.; Tan, Y.Y.; Chen, S.D.; Jin, H.J.; Tan, K.S.; Wang, D.Y.; Yan, Y. The origin, transmission and clinical therapies on coronavirus disease 2019 (COVID-19) outbreak—An update on the status. Mil. Med. Res. 2020, 7, 11. [Google Scholar] [CrossRef] [Green Version]
- Rajkumar, R.P. COVID-19 and mental health: A review of the existing literature. Asian J. Psychiatry 2020, 52, 102066. [Google Scholar] [CrossRef]
- Talevi, D.; Socci, V.; Carai, M.; Carnaghi, G.; Faleri, S.; Trebbi, E.; di Bernardo, A.; Capelli, F.; Pacitti, F. Mental health outcomes of the COVID-19 pandemic. Riv. Psichiatr. 2020, 55, 137–144. [Google Scholar]
- Vindegaard, N.; Benros, M.E. COVID-19 pandemic and mental health consequences: Systematic review of the current evidence. Brain Behav. Immun. 2020, 89, 531–542. [Google Scholar] [CrossRef]
- Cherikh, F.; Frey, S.; Bel, C.; Attanasi, G.; Alifano, M.; Iannelli, A. Behavioral Food Addiction During Lockdown: Time for Awareness, Time to Prepare the Aftermath. Obes. Surg. 2020, 30, 3585–3587. [Google Scholar] [CrossRef]
- Attanasi, G.; Maffioletti, A.; Shalukhina, T.; Bel, C.; Cherikh, F. Gender Differences in the Impact of COVID-19 Lockdown on Potentially Addictive Behaviors: An Emotion-Mediated Analysis. Front. Psychol. 2021, 12, 1–16. [Google Scholar] [CrossRef]
- Zhang, D.; Lee, E.K.P.; Mak, E.C.W.; Ho, C.Y.; Wong, S.Y.S. Mindfulness-based interventions: An overall review. Br. Med. Bull. 2021, 138, 41–57. [Google Scholar] [CrossRef] [PubMed]
- Xu, J.; Helen, J.; Noorbhai, L.; Patel, A.; Li, A. Virtual mindfulness interventions to promote well-being in adults: A mixed-methods systematic review. J. Affect. Disord. 2022, 300, 571–585. [Google Scholar] [CrossRef]
- Hanh, T.N.; Hoa, M.Q. The Miracle of being Awake; Buddhist Publication Society: Kandy, Sri Lanka, 1976. [Google Scholar]
- Kiken, L.G.; Garland, E.L.; Bluth, K.; Palsson, O.S.; Gaylord, S.A. From a state to a trait: Trajectories of state mindfulness in meditation during intervention predict changes in trait mindfulness. Personal. Individ. Differ. 2015, 81, 41–46. [Google Scholar] [CrossRef] [Green Version]
- Kabat-Zinn, J. Where You Go, There You are: Mindfulness Meditation in Everyday Life; Hyperion: New York, NY, USA, 1994. [Google Scholar]
- Bishop, S.R.; Lau, M.; Shapiro, S.; Carlson, L.; Anderson, N.D.; Carmody, J.; Segal, Z.V.; Abbey, S.; Speca, M.; Velting, D.; et al. Mindfulness: A proposed operational definition. Clin. Psychol. Sci. Pract. 2004, 11, 230–241. [Google Scholar] [CrossRef]
- Grossman, P.; Niemann, L.; Schmidt, S.; Walach, H. Mindfulness-based stress reduction and health benefits: A meta-analysis. J. Psychosom. Res. 2004, 57, 35–43. [Google Scholar] [CrossRef]
- Hofmann, S.G.; Sawyer, A.T.; Witt, A.A.; Oh, D. The effect of mindfulness-based therapy on anxiety and depression: A meta-analytic review. J. Consult. Clin. Psychol. 2010, 78, 169. [Google Scholar] [CrossRef] [PubMed]
- Song, Y.; Lindquist, R. Effects of mindfulness-based stress reduction on depression, anxiety, stress and mindfulness in Korean nursing students. Nurse Educ. Today 2015, 35, 86–90. [Google Scholar] [CrossRef]
- Strohmaier, S. The relationship between doses of mindfulness-based programs and depression, anxiety, stress, and mindfulness: A dose-response meta-regression of randomized controlled trials. Mindfulness 2020, 11, 1315–1335. [Google Scholar] [CrossRef]
- Murphy, M.J.; Mermelstein, L.C.; Edwards, K.M.; Gidycz, C.A. The benefits of dispositional mindfulness in physical health: A longitudinal study of female college students. J. Am. Coll. Health 2012, 60, 341–348. [Google Scholar] [CrossRef]
- Carlson, L.E.; Speca, M.; Faris, P.; Patel, K.D. One year pre–post intervention follow-up of psychological, immune, endocrine and blood pressure outcomes of mindfulness-based stress reduction (MBSR) in breast and prostate cancer outpatients. Brain Behav. Immun. 2007, 21, 1038–1049. [Google Scholar] [CrossRef]
- Kong, F.; Wang, X.; Zhao, J. Dispositional mindfulness and life satisfaction: The role of core self-evaluations. Personal. Individ. Differ. 2014, 56, 165–169. [Google Scholar] [CrossRef]
- Moore, A.; Malinowski, P. Meditation, mindfulness and cognitive flexibility. Conscious. Cogn. 2009, 18, 176–186. [Google Scholar] [CrossRef]
- Jha, A.P.; Stanley, E.A.; Kiyonaga, A.; Wong, L.; Gelfand, L. Examining the protective effects of mindfulness training on working memory capacity and affective experience. Emotion 2010, 10, 54. [Google Scholar] [CrossRef]
- Mrazek, M.D.; Franklin, M.S.; Phillips, D.T.; Baird, B.; Schooler, J.W. Mindfulness training improves working memory capacity and GRE performance while reducing mind wandering. Psychol. Sci. 2013, 24, 776–781. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Becker, P.M. Overview of sleep management during COVID-19. Sleep Med. 2021, 91, 211–218. [Google Scholar] [CrossRef] [PubMed]
- Kshirsagar, M.M.; Dodamani, A.S.; Dodamani, G.A.; Khobragade, V.R.; Deokar, R.N. Impact of COVID-19 on Mental Health: An Overview. Rev. Recent Clin. Trials 2021, 16, 227–231. [Google Scholar] [CrossRef] [PubMed]
- Simonelli, G.; Petit, D.; Delage, J.P.; Michaud, X.; Lavoie, M.D.; Morin, C.M.; Godbout, R.; Robillard, R.; Vallières, A.; Carrier, J.; et al. Sleep in times of crises: A scoping review in the early days of the COVID-19 crisis. Sleep Med. Rev. 2021, 60, 101545. [Google Scholar] [CrossRef]
- Wu, T.; Jia, X.; Shi, H.; Niu, J.; Yin, X.; Xie, J.; Wang, X. Prevalence of mental health problems during the COVID-19 pandemic: A systematic review and meta-analysis. J. Affect. Disord. 2021, 281, 91–98. [Google Scholar] [CrossRef]
- Liu, L.; Ni, S.-Y.; Yan, W.; Lu, Q.-D.; Zhao, Y.-M.; Xu, Y.-Y.; Mei, H.; Shi, L.; Yuan, K.; Han, Y.; et al. Mental and neurological disorders and risk of COVID-19 susceptibility, illness severity and mortality: A systematic review, meta-analysis and call for action. EClinicalMedicine 2021, 40, 101111. [Google Scholar] [CrossRef]
- Ceban, F.; Nogo, D.; Carvalho, I.P.; Lee, Y.; Nasri, F.; Xiong, J.; Lui, L.M.W.; Subramaniapillai, M.; Gill, H.; Liu, R.N.; et al. Association between Mood Disorders and Risk of COVID-19 Infection, Hospitalization, and Death: A Systematic Review and Meta-analysis. JAMA Psychiatry 2021, 78, 1079–1091. [Google Scholar] [CrossRef]
- Janssen, M.; Heerkens, Y.; Kuijer, W.; Van Der Heijden, B.; Engels, J. Effects of mindfulness-based stress reduction on employees’ mental health: A systematic review. PLoS ONE 2018, 13, e0191332. [Google Scholar] [CrossRef]
- Frank, J.L.; Reibel, D.; Broderick, P.; Cantrell, T.; Metz, S. The Effectiveness of Mindfulness-Based Stress Reduction on Educator Stress and Well-Being: Results from a Pilot Study. Mindfulness 2015, 6, 208–216. [Google Scholar] [CrossRef]
- Ding, X.; Wang, X.; Yang, Z.; Tang, R.; Tang, Y.Y. Relationship Between Trait Mindfulness and Sleep Quality in College Students: A Conditional Process Model. Front. Psychol. 2020, 11, 1–9. [Google Scholar] [CrossRef]
- Dawson, A.F.; Brown, W.W.; Anderson, J.; Datta, B.; Donald, J.N.; Hong, K.; Allan, S.; Mole, T.B.; Jones, P.B.; Galante, J. Mindfulness-Based Interventions for University Students: A Systematic Review and Meta-Analysis of Randomised Controlled Trials. Appl. Psychol. Health Well-Being 2020, 12, 384–410. [Google Scholar] [CrossRef] [PubMed]
- Rodrigues, M.F.; Nardi, A.E.; Levitan, M. Mindfulness in mood and anxiety disorders: A review of the literature. Trends Psychiatry Psychother. 2017, 39, 207–215. [Google Scholar] [CrossRef] [PubMed]
- Wimmer, L.; von Stockhausen, L.; Bellingrath, S. Improving emotion regulation and mood in teacher trainees: Effectiveness of two mindfulness trainings. Brain Behav. 2019, 9, e01390. [Google Scholar] [CrossRef]
- Bellosta-Batalla, M.; del Carmen Blanco-Gandía, M.; Rodríguez-Arias, M.; Cebolla, A.; Pérez-Blasco, J.; Moya-Albiol, L. Brief mindfulness session improves mood and increases salivary oxytocin in psychology students. Stress Health 2020, 36, 469–477. [Google Scholar] [CrossRef] [PubMed]
- Swickert, R.; Bailey, E.; Hittner, J.; Spector, A.; Benson-Townsend, B.; Silver, N.C. The Mediational Roles of Gratitude and Perceived Support in Explaining the Relationship Between Mindfulness and Mood. J. Happiness Stud. 2019, 20, 815–828. [Google Scholar] [CrossRef]
- Mirnics, Z.; Hittner, J.B.; Swickert, R.; Kövi, Z. Gratitude and social support mediate the association between mindfulness and mood: A cross-cultural replication study. J. Health Psychol. 2022, 27, 246–252. [Google Scholar] [CrossRef]
- Mukhtar, S. Psychological health during the coronavirus disease 2019 pandemic outbreak. Int. J. Soc. Psychiatry 2020, 66, 512–516. [Google Scholar] [CrossRef]
- Weis, R.; Ray, S.D.; Cohen, T.A. Mindfulness as a way to cope with COVID-19-related stress and anxiety. Couns. Psychother. Res. 2021, 21, 8–18. [Google Scholar] [CrossRef]
- Saricali, M.; Satici, S.A.; Satici, B.; Gocet-Tekin, E.; Griffiths, M.D. Fear of COVID-19, Mindfulness, Humor, and Hopelessness: A Multiple Mediation Analysis. Int. J. Ment. Health Addict. 2020, 1–14. [Google Scholar] [CrossRef]
- Antonova, E.; Schlosser, K.; Pandey, R.; Kumari, V. Coping with COVID-19: Mindfulness-based approaches for mitigating mental health crisis. Front. Psychiatry 2021, 12, 322. [Google Scholar] [CrossRef]
- Weng, H.Y.; Fox, A.S.; Shackman, A.J.; Stodola, D.E.; Caldwell, J.Z.; Olson, M.C.; Rogers, G.M.; Davidson, R.J. Compassion training alters altruism and neural responses to suffering. Psychol. Sci. 2013, 24, 1171–1180. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Leiberg, S.; Klimecki, O.; Singer, T. Short-term compassion training increases prosocial behavior in a newly developed prosocial game. PLoS ONE 2011, 6, e17798. [Google Scholar] [CrossRef] [PubMed]
- Iwamoto, S.K.; Alexander, M.; Torres, M.; Irwin, M.R.; Christakis, N.A.; Nishi, A. Mindfulness Meditation Activates Altruism. Sci. Rep. 2020, 10, 6511. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Luberto, C.M.; Shinday, N.; Song, R.; Philpotts, L.L.; Park, E.R.; Fricchione, G.L.; Gloria, Y. A Systematic Review and Meta-analysis of the Effects of Meditation on Empathy, Compassion, and Prosocial Behaviors. Mindfulness 2018, 9, 708–724. [Google Scholar] [CrossRef]
- Campos-Mercade, P.; Meier, A.N.; Schneider, F.H.; Wengström, E. Prosociality predicts health behaviors during the COVID-19 pandemic. J. Public Econ. 2021, 195, 104367. [Google Scholar] [CrossRef]
- Falk, A.; Becker, A.; Dohmen, T.; Enke, B.; Huffman, D.; Sunde, U. Global evidence on economic preferences. In Quarterly Journal of Economics; Oxford University Press: Oxford, UK, 2018; Volume 133, pp. 1645–1692. [Google Scholar]
- Bursky, M.; Kosuri, M.; Walsh Carson, K.; Babad, S.; Iskhakova, A.; Nikulina, V. The Utility of Meditation and Mindfulness-Based Interventions in the Time of COVID-19: A Theoretical Proposition and Systematic Review of the Relevant Prison 2011, Quarantine and Lockdown Literature. Psychol. Rep. 2021, 003329412110487. [Google Scholar] [CrossRef]
- Kulkarni, M.S.; Kakodkar, P.; Nesari, T.M.; Dubewar, A.P. Combating the psychological impact of COVID-19 pandemic through yoga: Recommendation from an overview. J. Ayurveda Integr. Med. 2022, 13, 100433. [Google Scholar] [CrossRef]
- Conversano, C.; Di Giuseppe, M.; Miccoli, M.; Ciacchini, R.; Gemignani, A.; Orrù, G. Mindfulness, age and gender as protective factors against psychological distress during Covid-19 pandemic. Front. Psychol. 2020, 11, 1900. [Google Scholar] [CrossRef]
- Yuan, Y. Mindfulness training on the resilience of adolescents under the COVID-19 epidemic: A latent growth curve analysis. Personal. Individ. Differ. 2021, 172, 110560. [Google Scholar] [CrossRef]
- Zhu, J.L.; Schülke, R.; Vatansever, D.; Xi, D.; Yan, J.; Zhao, H.; Xie, X.; Feng, J.; Chen, M.Y.; Sahakian, B.J.; et al. Mindfulness practice for protecting mental health during the COVID-19 pandemic. Transl. Psychiatry 2021, 11, 329. [Google Scholar] [CrossRef]
- Brown, K.W.; Ryan, R.M. The benefits of being present: Mindfulness and its role in psychological well-being. J. Personal. Soc. Psychol. 2003, 84, 822. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Smit, B.; Stavrulaki, E. The Efficacy of a Mindfulness-Based Intervention for College Students under Extremely Stressful Conditions. Mindfulness 2021, 12, 3086–3100. [Google Scholar] [CrossRef] [PubMed]
- Thimmapuram, J.; Pargament, R.; Bell, T.; Schurk, H.; Madhusudhan, D.K. Heartfulness meditation improves loneliness and sleep in physicians and advance practice providers during COVID-19 pandemic. Hosp. Pract. 2021, 49, 194–202. [Google Scholar] [CrossRef] [PubMed]
- Nourian, M.; Nikfarid, L.; Khavari, A.M.; Barati, M.; Allahgholipour, A.R. The Impact of an Online Mindfulness-Based Stress Reduction Program on Sleep Quality of Nurses Working in COVID-19 Care Units: A clinical trial. Holist. Nurs. Pract. 2021, 35, 257–263. [Google Scholar] [CrossRef] [PubMed]
- Mirolli, M.; Simione, L.; Martoni, M. Accept Anxiety to Improve Sleep: The Impact of the COVID-19 Lockdown on the Relationships between Mindfulness, Distress, and Sleep Quality. Int. J. Environ. Res. Public Health 2021, 18, 13149. [Google Scholar] [CrossRef]
- Zheng, M.X.; Masters-Waage, T.C.; Yao, J.; Lu, Y.; Tan, N.; Narayanan, J. Stay Mindful and Carry on: Mindfulness Neutralizes COVID-19 Stressors on Work Engagement via Sleep Duration. Front. Psychol. 2020, 11, 610156. [Google Scholar] [CrossRef]
- Lim, J.; Leow, Z.; Ong, J.; Pang, L.S.; Lim, E. Effects of Web-Based Group Mindfulness Training on Stress and Sleep Quality in Singapore During the COVID-19 Pandemic: Retrospective Equivalence Analysis. JMIR Ment. Health 2021, 8, e21757. [Google Scholar] [CrossRef]
- Haliwa, I.; Lee, J.; Wilson, J.; Shook, N.J. Mindfulness and engagement in COVID-19 preventive behavior. Prev. Med. Rep. 2020, 20, 101246. [Google Scholar] [CrossRef]
- Bailey, B.; Whelen, M.L.; Strunk, D.R. Adhering to COVID-19 health guidelines: Examining demographic and psychological predictors of adherence. Appl. Psychol. Health Well-Being 2021, 13, 968–985. [Google Scholar] [CrossRef]
- Chrisinger, B.W.; Rich, T.; Lounsbury, D.; Peng, K.; Zhang, J.; Heaney, C.A.; Lu, Y.; Hsing, A.W. Coping with the COVID-19 pandemic: Contemplative practice behaviors are associated with better mental health outcomes and compliance with Shelter-In-Place orders in a prospective cohort study. Prev. Med. Rep. 2021, 23, 101451. [Google Scholar] [CrossRef]
- Bazzoli, A.; Probst, T.M.; Lee, H.J. Economic stressors, covid-19 attitudes, worry, and behaviors among U.S. working adults: A mixture analysis. Int. J. Environ. Res. Public Health 2021, 18, 2338. [Google Scholar] [CrossRef] [PubMed]
- Blayac, T.; Dubois, D.; Duchêne, S.; Nguyen-Van, P.; Ventelou, B.; Willinger, M. Population preferences for inclusive COVID-19 policy responses. Lancet Public Health 2021, 6, e9. [Google Scholar] [CrossRef]
- Blayac, T.; Dubois, D.; Duchêne, S.; Nguyen-Van, P.; Ventelou, B.; Willinger, M. Designing acceptable anti-COVID-19 policies by taking into account individuals’ preferences: Evidence from a Discrete Choice Experiment. Work. Pap. 2021. [Google Scholar]
- Blayac, T.; Dubois, D.; Duchêne, S.; Nguyen-Van, P.; Rafaï, I.; Ventelou, B.; Willinger, M. Nudging for lockdown: Behavioural insights from an online experiment. Soc. Psychol. Forthcom. 2022, in press. [Google Scholar] [CrossRef]
- Rafaï, I.; Blayac, T.; Dubois, D.; Duchêne, S.; Nguyen-Van, P.; Ventelou, B.; Willinger, M. Stated preferences outperform elicited preferences for predicting compliance with Covid-19 prophylactic measures. SSRN 2022, 4031918. [Google Scholar] [CrossRef]
- Wang, Z.; Rafaï, I.; Willinger, M. How age affects risk and time preferences: Evidence from a representative sample. SSRN 2022, 4031930. [Google Scholar] [CrossRef]
- Vitiello, M.V.; Larsen, L.H.; Moe, K.E. Age-related sleep change: Gender and estrogen effects on the subjective–objective sleep quality relationships of healthy, non complaining older men and women. J. Psychosom. Res. 2004, 56, 503–510. [Google Scholar] [CrossRef]
- Clark, C.; Davila, A.; Regis, M.; Kraus, S. Predictors of COVID-19 voluntary compliance behaviors: An international investigation. Glob. Transit. 2020, 2, 76–82. [Google Scholar] [CrossRef]
- Almutairi, A.F.; BaniMustafa, A.A.; Alessa, Y.M.; Almutairi, S.B.; Almaleh, Y. Public trust and compliance with the precautionary measures against COVID-19 employed by authorities in Saudi Arabia. Risk Manag. Healthc. Policy 2020, 13, 753. [Google Scholar] [CrossRef]
- Alifano, M.; Attanasi, G.; Iannelli, F.; Cherikh, F.; Iannelli, A. COVID-19 Pandemic: A European Perspective on Health Economic Policies. J. Behav. Econ. Policy 2020, 4, 35–43. [Google Scholar]
- Slovic, P. The Perception of Risk; Earthscan: London, UK, 2000. [Google Scholar]
- Carlson, L.E.; Brown, K.W. Validation of the Mindful Attention Awareness Scale in a cancer population. J. Psychosom. Res. 2005, 58, 29–33. [Google Scholar] [CrossRef] [PubMed]
- Barajas, S.; Garra, L. Mindfulness and psychopathology: Adaptation of the Mindful Attention Awareness Scale (MAAS) in a Spanish sample. Clínica Salud 2014, 25, 49–56. [Google Scholar] [CrossRef] [Green Version]
- Montes, S.A.; Ledesma, R.D.; García, N.M.; Poó, F.M. The mindful attention awareness scale (MAAS) in an argentine population. Meas. Eval. Couns. Dev. 2014, 47, 43–51. [Google Scholar] [CrossRef]
- Solehati, T.; Kosasih, C.E.; Hermayanti, Y.; Mediani, H.S. The Psychological and Sleep-Related Impact of Coronavirus Disease 2019 (COVID-19): A Systematic Review. Natl. Public Health J. 2021, 16, 65–74. [Google Scholar] [CrossRef]
- Kimhi, S.; Marciano, H.; Eshel, Y.; Adini, B. Resilience and demographic characteristics predicting distress during the COVID-19 crisis. Soc. Sci. Med. 2020, 265, 113389. [Google Scholar] [CrossRef]
- Yan, S.; Xu, R.; Stratton, T.D.; Kavcic, V.; Luo, D.; Hou, F.; Jiang, Y. Sex differences and psychological stress: Responses to the COVID-19 pandemic in China. BMC Public Health 2021, 21, 79. [Google Scholar] [CrossRef]
- Chambers, R.; Gullone, E.; Allen, N.B. Mindful emotion regulation: An integrative review. Clin. Psychol. Rev. 2009, 29, 560–572. [Google Scholar] [CrossRef]
- Howell, A.J.; Digdon, N.L.; Buro, K.; Sheptycki, A.R. Relations among mindfulness, well-being, and sleep. Personal. Individ. Differ. 2008, 45, 773–777. [Google Scholar] [CrossRef]
- Jain, S.; Shapiro, S.L.; Swanick, S.; Roesch, S.C.; Mills, P.J.; Bell, I.; Schwartz, G.E. A randomized controlled trial of mindfulness meditation versus relaxation training: Effects on distress, positive states of mind, rumination, and distraction. Ann. Behav. Med. 2007, 33, 11–21. [Google Scholar] [CrossRef]
- Shapiro, S.L.; Bootzin, R.R.; Figueredo, A.J.; Lopez, A.M.; Schwartz, G.E. The efficacy of mindfulness-based stress reduction in the treatment of sleep disturbance in women with breast cancer: An exploratory study. J. Psychosom. Res. 2003, 54, 85–91. [Google Scholar] [CrossRef]
- Carlson, L.E.; Garland, S.N. Impact of mindfulness-based stress reduction (MBSR) on sleep, mood, stress and fatigue symptoms in cancer outpatients. Int. J. Behav. Med. 2005, 12, 278–285. [Google Scholar] [CrossRef] [PubMed]
- Black, D.S.; O’Reilly, G.A.; Olmstead, R.; Breen, E.C.; Irwin, M.R. Mindfulness meditation and improvement in sleep quality and daytime impairment among older adults with sleep disturbances: A randomized clinical trial. JAMA Intern. Med. 2015, 175, 494–501. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Anderson, S.C.; Edwards, A.M.; Yerlanov, M.; Mulberry, N.; Stockdale, J.E.; Iyaniwura, S.A.; Falcao, R.C.; Otterstatter, M.C.; Irvine, M.A.; Janjua, N.Z.; et al. Quantifying the impact of COVID-19 control measures using a Bayesian model of physical distancing. PLoS Comput. Biol. 2020, 16, e1008274. [Google Scholar] [CrossRef] [PubMed]
- Flaxman, S.; Mishra, S.; Gandy, A.; Unwin, H.J.T.; Mellan, T.A.; Coupland, H.; Whittaker, C.; Zhu, H.; Berah, T.; Eaton, J.W.; et al. Estimating the effects of non-pharmaceutical interventions on COVID-19 in Europe. Nature 2020, 584, 257–261. [Google Scholar] [CrossRef] [PubMed]
- Dehning, J.; Zierenberg, J.; Spitzner, F.P.; Wibral, M.; Neto, J.P.; Wilczek, M.; Priesemann, V. Inferring change points in the spread of COVID-19 reveals the effectiveness of interventions. Science 2020, 369, eabb9789. [Google Scholar] [CrossRef]
- Farrell, K.; Durand, H.; McSharry, J.; Meade, O.; Kenny, E.; Noone, C.; O’Connor, L.L.; Lavoie, K.L.; Byrne, M.; Mooney, R.; et al. Exploring barriers and facilitators of physical distancing in the context of the COVID-19 pandemic: A qualitative interview study. HRB Open Res. 2021, 4, 50. [Google Scholar] [CrossRef]
- Wright, L.; Steptoe, A.; Fancourt, D. Patterns of compliance with COVID-19 preventive behaviours: A latent class analysis of 20,000 UK adults. J. Epidemiol. Community Health 2022, 76, 247–253. [Google Scholar] [CrossRef]
- Harper, C.A.; Satchell, L.P.; Fido, D.; Latzman, R.D. Functional fear predicts public health compliance in the COVID-19 pandemic. Int. J. Ment. Health Addict. 2020, 19, 1875–1888. [Google Scholar] [CrossRef]
- Bargain, O.; Aminjonov, U. Trust and compliance to public health policies in times of COVID-19. J. Public Econ. 2020, 192, 104316. [Google Scholar] [CrossRef]
- Karpen, S.C. The social psychology of biased self-assessment. Am. J. Pharm. Educ. 2018, 82, 6299. [Google Scholar] [CrossRef]
- Murphy, J.J.; Allen, P.G.; Stevens, T.H.; Weatherhead, D. A meta-analysis of hypothetical bias in stated preference valuation. Environ. Resour. Econ. 2005, 30, 313–325. [Google Scholar] [CrossRef] [Green Version]
- Harrison, G.W.; Rutström, E.E. Experimental evidence on the existence of hypothetical bias in value elicitation methods. Handb. Exp. Econ. Results 2008, 1, 752–767. [Google Scholar]
- Kim, Y.H.; Kwon, H.; Lee, J.; Chiu, C.Y. Why do people overestimate or underestimate their abilities? A cross-culturally valid model of cognitive and motivational processes in self-assessment biases. J. Cross-Cult. Psychol. 2016, 47, 1201–1216. [Google Scholar] [CrossRef]
- Wuepper, D.; Clemm, A.; Wree, P. The preference for sustainable coffee and a new approach for dealing with hypothetical bias. J. Econ. Behav. Organ. 2019, 158, 475–486. [Google Scholar] [CrossRef]
- Knapp, S.; Gottlieb, M.C.; Handelsman, M.M. Enhancing professionalism through self-reflection. Prof. Psychol. Res. Pract. 2017, 48, 167–174. [Google Scholar] [CrossRef]
- Grossman, P. Defining mindfulness by how poorly I think I pay attention during everyday awareness and other intractable problems for psychology’s (re)invention of mindfulness: Comment on Brown et al. Psychol. Assess. 2011, 23, 1034–1040. [Google Scholar] [CrossRef]
- Brown, K.W.; Ryan, R.M.; Loverich, T.M.; Biegel, G.M.; West, A.M. Out of the armchair and into the streets: Measuring mindfulness advances knowledge and improves interventions: Reply to Grossman. Psychol. Assess. 2011, 23, 1041–1046. [Google Scholar] [CrossRef]
- Van Dam, N.T.; Earleywine, M.; Borders, A. Measuring mindfulness? An item response theory analysis of the Mindful Attention Awareness Scale. Personal. Individ. Differ. 2010, 49, 805–810. [Google Scholar] [CrossRef]
- Sauer, S.; Walach, H.; Schmidt, S.; Hinterberger, T.; Lynch, S.; Büssing, A.; Kohls, N. Assessment of Mindfulness: Review on State of the Art. Mindfulness 2013, 4, 3–17. [Google Scholar] [CrossRef]
- Baer, R.A.; Smith, G.T.; Hopkins, J.; Krietemeyer, J.; Toney, L. Using self-report assessment methods to explore facets of mindfulness. Assessment 2006, 13, 27–45. [Google Scholar] [CrossRef] [Green Version]
- Coffey, K.A.; Hartman, M. Mechanisms of action in the inverse relationship between mindfulness and psychological distress. Complementary Health Pract. Rev. 2008, 13, 79–91. [Google Scholar] [CrossRef] [Green Version]
- Van Bavel, J.J.; Baicker, K.; Boggio, P.S.; Capraro, V.; Cichocka, A.; Cikara, M.; Willer, R. Using social and behavioural science to support COVID-19 pandemic response. Nat. Hum. Behav. 2020, 4, 460–471. [Google Scholar] [CrossRef] [PubMed]
- Behan, C. The benefits of meditation and mindfulness practices during times of crisis such as COVID-19. Ir. J. Psychol. Med. 2020, 37, 256–258. [Google Scholar] [CrossRef] [PubMed]
- Aikens, K.A.; Astin, J.; Pelletier, K.R.; Levanovich, K.; Baase, C.M.; Park, Y.Y.; Bodnar, C.M. Mindfulness goes to work: Impact of an online workplace intervention. J. Occup. Environ. Med. 2014, 56, 721–731. [Google Scholar] [CrossRef] [Green Version]
- Pots, W.T.; Fledderus, M.; Meulenbeek, P.A.; Peter, M.; Schreurs, K.M.; Bohlmeijer, E.T. Acceptance and commitment therapy as a web-based intervention for depressive symptoms: Randomised controlled trial. Br. J. Psychiatry 2016, 208, 69–77. [Google Scholar] [CrossRef] [Green Version]
- Zhang, H.; Zhang, A.; Liu, C.; Xiao, J.; Wang, K. A Brief Online Mindfulness-Based Group Intervention for Psychological Distress Among Chinese Residents During COVID-19: A Pilot Randomized Controlled Trial. Mindfulness 2021, 12, 1502–1512. [Google Scholar] [CrossRef]
| INSEE Census | Accepted (N = 5331) | Completed (N = 1154) | |
|---|---|---|---|
| Gender | |||
| Male | 47.72% | 47.77% | 51.17% |
| Female | 52.28% | 52.23% | 48.83% |
| Age | |||
| [18, 24] | 10.66% | 8.59% | 8.25% |
| [25, 34] | 15.72% | 15.52% | 13.90% |
| [35, 49] | 25.59% | 25.44% | 24.24% |
| [50, 64] | 24.72% | 27.45% | 28.32% |
| [65, +∞] | 23.31% | 23.00% | 25.28% |
| Professional and Social Categories (INSEE definition: PCS) | |||
| Agriculteurs exploitants (Farmers) | 0.94% | 0.86% | 0.78% |
| Artisans, commerçants, chefs entreprise (Craftsmen, merchants, business leaders) | 3.33% | 3.56% | 4.17% |
| Cadres, professions intellectuelles sup, professions libérales (Executives, superior intellectual professions, liberal professions) | 8.83% | 9.01% | 16.94% |
| Professions intermédiaires (Intermediate professions) | 13.96% | 15.57% | 18.16% |
| Employés (Employees) | 16.57% | 16.87% | 14.60% |
| Ouvriers (Workers) | 13.38% | 13.00% | 7.73% |
| Retraités (Retired) | 26.44% | 28.24% | 29.89% |
| Autres sans activité professionnelle (Others without professional activity) | 16.55% | 12.89% | 7.73% |
| Geographical Area (UDA-9 definition) | |||
| REGION PARISIENNE | 18.79% | 18.69% | 17.29% |
| BP OUEST | 9.31% | 9.25% | 8.34% |
| BP EST | 7.76% | 7.75% | 7.73% |
| NORD | 6.41% | 6.34% | 5.13% |
| OUEST | 13.63% | 13.51% | 13.64% |
| EST | 8.52% | 8.52% | 10.08% |
| SUD OUEST | 10.94% | 11.26% | 12.16% |
| SUD EST | 12.10% | 12.12% | 12.60% |
| MEDITERANEE | 12.53% | 12.57% | 13.03% |
| Urban Unit (INSEE definition) | |||
| <2000 inhabitants | 22.51% | 22.29% | 21.98% |
| Between 2 k and 20 k | 17.38% | 17.67% | 17.99% |
| Between 20 k and 100 k | 13.55% | 13.73% | 13.55% |
| More than 100 k | 29.88% | 30.02% | 31.28% |
| Parisian urban unit | 16.67% | 16.29% | 15.20% |
| Variable | Description | Mean (SD) | Median |
|---|---|---|---|
| Gender | 1 = the individual reports being a male (NA = the individual reports “other”: removed for the analysis) | 51.09% (0.50) | 1 |
| Age | In years | 50.65 (16.98) | 52 |
| Monthly Income | Respondent’s monthly household income. 0 = “<EUR 1000”; 1 = “EUR 1000~2000”; 2 = “EUR 2000~3000”; 3 = “EUR 3000~4000”; 4 = “EUR 4000~5000”; 5 = “EUR 5000~6000”; 6 = “EUR 6000~7000”; 7 = “EUR 7000~8000”; 8 = “EUR 8000~9000”; 9 = “EUR 9000~10,000”; 10 = “EUR 10,000~15,000”; 11 = “>EUR 15,000” (NA = “I don’t know/I don’t want to reply”: removed from the analysis) | 3.00 (2.28) | 3 |
| Education Level | 0 = “No diploma”; 1 = “Certificate from primary school to high school”; 2 = “Bachelor’s degree”; 3 = “Master’s degree or PhD” | 2.15 (0.78) | 2 |
| Vulnerable Person | 1 = the respondent suffers a chronic illness that makes them vulnerable to the threat of COVID-19 | 44.89% (0.68) | 0 |
| Living Conditions | 1 = the respondent lives with someone who is vulnerable to the threat of COVID-19 because of their age or a chronic illness | 20.80% (0.41) | 0 |
| Study | Sample Size (Representative?) | Country | Mean | Standard Deviation | |
|---|---|---|---|---|---|
| [54] Brown and Ryan (2003) | 74 (No) | USA | 3.97 | 0.64 | 0.86 |
| [75] Carlson and Brown (2005) | 149 (No) | Canada | 4.45 | 0.77 | 0.87 |
| [76] Barajas and Garra (2014) | 100 (No) | Spain | 4.08 | 0.68 | 0.88 |
| [77] Montes et al. (2014) 1 | 367 (No) | Argentina | 3.88 | - | 0.87 |
| Our sample | 1154 (Yes) | France | 4.33 | 0.71 | 0.84 |
| Lockdown Compliance | Mask Wearing | Coughing in Sleeves | Not Touching Faces | Physical Distancing | |
|---|---|---|---|---|---|
| Washing hands | 0.239 *** | 0.159 *** | 0.225 *** | 0.216 *** | 0.118 *** |
| Physical distancing | 0.226 *** | 0.211 *** | 0.0512 · | 0.215 *** | |
| Not touching faces | 0.193 *** | 0.212 *** | 0.147 *** | ||
| Coughing in sleeves | 0.108 *** | 0.125 *** | |||
| Mask wearing | 0.228 *** |
| Ordered Probit Regression | (1) | (2) |
|---|---|---|
| Dependent Variable | Sleep Quality Impact Degree | Mood Impact Degree |
| MAAS score | 0.1285 * (0.0568) | 0.1516 ** (0.0525) |
| Men | 0.3174 *** (0.0816) | 0.1230 · (0.0744) |
| Age | 0.0060 * (0.0026) | 0.0103 *** (0.0023) |
| Monthly Income | 0.0354 · (0.0190) | 0.0278 (0.0172) |
| Education Level | −0.0833 (0.0562) | −0.0209 (0.0510) |
| Vulnerable Person | −0.1667 ** (0.0609) | −0.0593 (0.0565) |
| Living Conditions | −0.0374 (0.1002) | −0.0382 (0.0921) |
| /cut1 | −0.9351 ** (0.2920) | −0.7524 ** (0.2707) |
| /cut2 | 0.1342 (0.2895) | 0.7816 ** (0.2694) |
| /cut3 | 3.1413 *** (0.3124) | 3.09371 *** (0.2824) |
| /cut4 | 3.8110 *** (0.3654) | 3.6338 *** (0.2960) |
| N | 1027 | 1027 |
| Log-likelihood | −726.9622 | −880.4104 |
| AIC | 1475.924 | 1782.821 |
| Dependent Variable | Marginal Effect Type | Level 0 “Considerably Deteriorated” | Level 1 “Deteriorated” | Level 2 “No Impact” | Level 3 “Improved” | Level 4 “Considerably Improved” |
|---|---|---|---|---|---|---|
| Sleep Quality | MEM | −0.0099 * (0.0045) | −0.0290 * (0.0129) | 0.0350 * (0.0155) | 3.2506 × 10−3 * (1.6519 × 10−3) | 6.9100 × 10−4 5.4182 × 10−4 |
| AME | −0.0107 * (0.0049) | −0.0275 * (0.0122) | 0.0338 * (0.0149) | 3.6363 × 10−3 · (1.8597 × 10−3) | 8.8847 × 10−4 · 6.7763 × 10−4 | |
| Mood | MEM | −0.0081 ** (0.0030) | −0.0460 ** (0.0161) | 0.0430 ** (0.0151) | 0.0076 ** (0.0029) | 3.5500 × 10−3 * (1.5778 × 10−3) |
| AME | −0.0089 ** (0.0033) | −0.0440 ** (0.0151) | 0.0409 ** (0.0141) | 0.0078 ** (0.0030) | 0.0041 * (0.0018) |
| Ordered Probit Models | (1) | (2) | (3) | (4) | (5) | (6) |
|---|---|---|---|---|---|---|
| Dependent Variable | Washing Hands | Coughing in Sleeves | Not Touching Faces | Mask Wearing | Physical Distancing | Lockdown |
| MAAS Score | 0.1094 · (0.0582) | 0.1518 ** (0.0538) | 0.0922 · (0.0488) | 0.0966 · (0.0525) | 0.1356 * (0.0628) | 0.1506 ** (0.0488) |
| Gender | −0.5998 *** (0.0841) | −0.2792 *** (0.0759) | −0.2555 *** (0.0695) | −0.3272 *** (0.0748) | −0.1513 (0.0910) | −0.3474 *** (0.0693) |
| Age | −0.0062 * (0.0025) | −0.0114 *** (0.0024) | 0.0059 ** (0.0022) | 0.0124 *** (0.0023) | 0.0227 *** (0.0029) | 0.0049 * (0.0021) |
| Monthly Income | 0.0208 (0.0194) | 0.0083 (0.0175) | 0.0168 (0.0160) | −0.0034 (0.0168) | 0.0167 (0.0218) | 0.0191 (0.0160) |
| Education Level | −0.0216 (0.0546) | 0.1145 * (0.0509) | 0.0043 (0.0472) | 0.0017 (0.0508) | 0.0434 (0.0629) | 0.0052 (0.0468) |
| Vulnerable Person | 0.0174 (0.0625) | −0.0612 (0.0566) | −0.0146 (0.0528) | 0.1785 ** (0.0580) | −0.0087 (0.0688) | 0.0712 (0.0528) |
| Living Conditions | 0.1296 (0.1031) | 0.1036 (0.0934) | 0.0052 (0.0863) | 0.1650 · (0.0947) | 0.0751 (0.1173) | 0.1070 (0.0858) |
| /cut2 | −2.3148 *** (0.3084) | −1.4880 *** (0.2790) | −1.0392 *** (0.2544) | −0.8406 ** (0.2726) | −0.9646 ** (0.3494) | −2.0832 *** (0.3307) |
| /cut3 | −1.5240 *** (0.2967) | −0.7793 ** (0.2749) | 0.1837 (0.2509) | −0.1126 (0.2685) | −0.2280 (0.3235) | −1.8556 *** (0.2973) |
| /cut4 | −0.7030 * (0.2936) | 0.0101 (0.2737) | 1.2012 *** (0.2525) | 0.9066 *** (0.2693) | 0.9099 ** (0.3219) | −1.6636 *** (0.2808) |
| /cut5 | −1.4964 *** (0.2710) | |||||
| /cut6 | −1.1633 *** (0.2594) | |||||
| /cut7 | −0.9306 *** (0.2550) | |||||
| /cut8 | −0.3251 (0.2503) | |||||
| /cut9 | 0.4114 · (0.2495) | |||||
| /cut10 | 1.1208 *** (0.2510) | |||||
| N | 1026 | 995 | 1007 | 1003 | 1025 | 1027 |
| Log-likelihood | −804.4848 | −1041.968 | −1228.808 | −1035.511 | −569.0606 | −1464.038 |
| AIC | 1628.97 | 2103.936 | 2477.617 | 2091.022 | 1158.121 | 2960.076 |
| Dependent Variable | Marginal Effect Type | Level 1 “Never” | Level 2 “Sometimes” | Level 3 “Often” | Level 4 “Very Often” |
|---|---|---|---|---|---|
| Washing Hands | MEM | −3.7441 × 10−3 · (2.1203 × 10−3) | −0.0121 · (0.0065) | −0.0206 · (0.0110) | 0.0364 · (0.0193) |
| AME | −0.0045 · (0.0025) | −0.0121 · (0.0065) | −0.0185 · (0.0098) | 0.0351 · (0.0186) | |
| Coughing in Sleeves | MEM | −0.0145 ** (0.0053) | −0.0229 ** (0.0083) | −0.0220 ** (0.0081) | 0.0595 ** (0.0211) |
| AME | −0.0155 ** (0.0058) | −0.0218 ** (0.0078) | −0.0200 ** (0.0071) | 0.0573 ** (0.0201) | |
| Not Touching Faces | MEM | −0.0092 · (0.0049) | −0.0242 · (0.0128) | 2.1515 × 10−3 (1.6241 × 10−3) | 0.0312 · (0.0165) |
| AME | −0.0094 · (0.0051) | −0.0235 · (0.0124) | 2.0568 × 10−3 · (1.5472 × 10−3) | 0.0309 · (0.0163) | |
| Mask Wearing | MEM | −0.0072 · (0.0040) | −0.0138 · (0.0075) | −0.0174 · (0.0096) | 0.0384 · (0.0209) |
| AME | −0.0080 · (0.0045) | −0.0131 · (0.0072) | −0.0155 · (0.0084) | 0.0366 · (0.0198) |
| Dependent Variable | Marginal Effect Type | Level 1 “Never” | Level 2 “Sometimes” | Level 3 “Often” | Level 4 “Very Often” |
|---|---|---|---|---|---|
| Physical Distancing | MEM | −1.1141 × 10−3 (7.1219 × 10−4) | −0.0055 * (0.0027) | −0.0291 * (0.0135) | 0.0357 * (0.0165) |
| AME | −0.0018 (0.0011) | −0.0065 * (0.0032) | −0.0265 * (0.0123) | 0.0349 * (0.0161) |
| Dependent Variable | Marginal Effect Type | Level 1~10 (From “Not at All” to “Strictly”) | ||||||
|---|---|---|---|---|---|---|---|---|
| 1~4 | 5 | 6 | 7 | 8 | 9 | 10 | ||
| Lockdown Compliance | MEM | n.s. | −4.0928 × 10−3 * (1.6652 × 10−3) | −4.3991 × 10−3 * (1.7395 × 10−3) | −0.0178 ** (0.0060) | −0.0244 ** (0.0081) | −3.3087 × 10−3 · (1.8140 × 10−3) | 0.0579 ** (0.0187) |
| AME | n.s. | −4.2632 × 10−3 (1.7452 × 10−3) | −4.4565 × 10−3 * (1.7648 × 10−3) | −0.0230 ** (0.0075) | −0.0174 ** (0.0058) | −3.0658 × 10−3 · (1.6639 × 10−3) | 0.0565 ** (0.0182) | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Wen, X.; Rafaï, I.; Duchêne, S.; Willinger, M. Did Mindful People Do Better during the COVID-19 Pandemic? Mindfulness Is Associated with Well-Being and Compliance with Prophylactic Measures. Int. J. Environ. Res. Public Health 2022, 19, 5051. https://doi.org/10.3390/ijerph19095051
Wen X, Rafaï I, Duchêne S, Willinger M. Did Mindful People Do Better during the COVID-19 Pandemic? Mindfulness Is Associated with Well-Being and Compliance with Prophylactic Measures. International Journal of Environmental Research and Public Health. 2022; 19(9):5051. https://doi.org/10.3390/ijerph19095051
Chicago/Turabian StyleWen, Xinyue, Ismaël Rafaï, Sébastien Duchêne, and Marc Willinger. 2022. "Did Mindful People Do Better during the COVID-19 Pandemic? Mindfulness Is Associated with Well-Being and Compliance with Prophylactic Measures" International Journal of Environmental Research and Public Health 19, no. 9: 5051. https://doi.org/10.3390/ijerph19095051
APA StyleWen, X., Rafaï, I., Duchêne, S., & Willinger, M. (2022). Did Mindful People Do Better during the COVID-19 Pandemic? Mindfulness Is Associated with Well-Being and Compliance with Prophylactic Measures. International Journal of Environmental Research and Public Health, 19(9), 5051. https://doi.org/10.3390/ijerph19095051







