Detection of Neuromuscular Deficits in Movement Pattern among Uninjured Federated Youth Basketball Players: A Cross-Sectional Study
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Participants
2.3. Outcomes
2.4. Procedure
2.5. Data Sources/Measurement
2.6. Bias
2.7. Statistical Analyses
3. Results
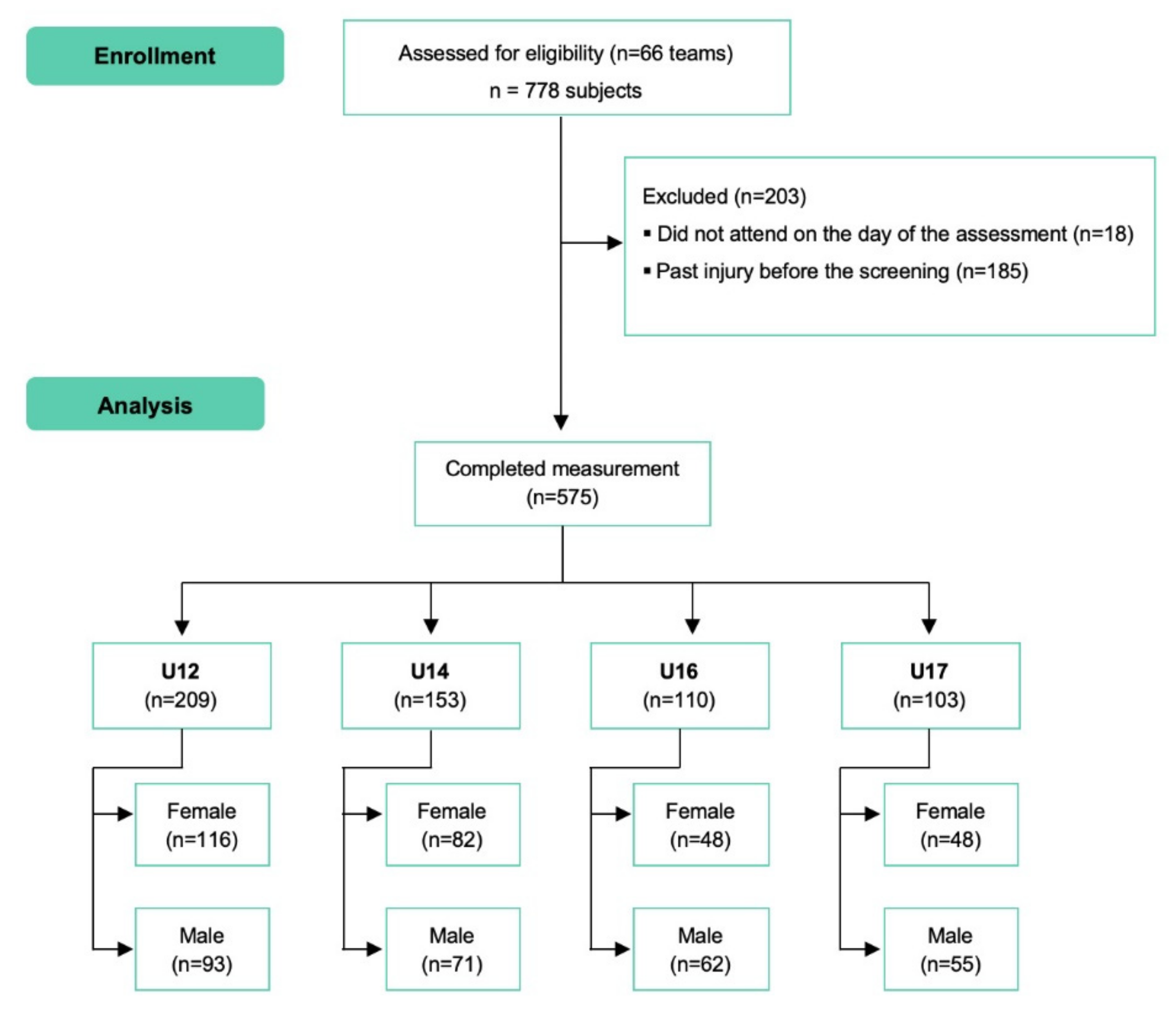
3.1. Description of Sample
3.2. Ankle Joint Dorsiflexion
3.3. Functional Ankle Stability
3.4. Dynamic Lower Extremity Valgus
3.5. Lumbopelvic Stability and Dynamic Postural Control
3.6. Neuromuscular Deficits during Continuous Tuck Jumps
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Drakos, M.C.; Domb, B.; Starkey, C.; Callahan, L.; Allen, A.A. Injury in the National Basketball Association: A 17-year overview. Sports Health 2010, 2, 284–290. [Google Scholar] [CrossRef] [PubMed]
- Hootman, J.M.; Dick, R.; Agel, J. Epidemiology of collegiate injuries for 15 sports: Summary and recommendations for injury prevention initiatives. J. Athl. Train. 2007, 42, 311–319. [Google Scholar] [PubMed]
- Rodas, G.; Bove, T.; Caparrós, T.; Langohr, K.; Medina, D.; Hamilton, B.; Sugimoto, D.; Casals, M. Ankle Sprain Versus Muscle Strain Injury in Professional Men’ss Basketball: A 9-Year Prospective Follow-up Study. Orthop. J. Sports Med. 2019, 7, 2325967119849035. [Google Scholar] [CrossRef] [Green Version]
- Cherni, Y.; Jlid, M.C.; Mehrez, H.; Shephard, R.J.; Paillard, T.; Chelly, M.S.; Hermassi, S. Eight Weeks of Plyometric Training Improves Ability to Change Direction and Dynamic Postural Control in Female Basketball Players. Front. Physiol. 2019, 10, 726. [Google Scholar] [CrossRef] [Green Version]
- Taylor, J.B.; Wright, A.A.; Dischiavi, S.L.; Townsend, M.A.; Marmon, A.R. Activity demands during multidirectional team sports: A systematic review. Sports Med. 2017, 47, 2533–2551. [Google Scholar] [CrossRef]
- Andreoli, C.V.; Chiaramonti, B.C.; Buriel, E.; Pochini, A.C.; Ejnisman, B.; Cohen, M. Epidemiology of sports injuries in basketball: Integrative systematic review. BMJ Open Sport Exerc. Med. 2018, 4, e000468. [Google Scholar] [CrossRef]
- Clifton, D.R.; Hertel, J.; Onate, J.A.; Currie, D.W.; Pierpoint, L.A.; Wasserman, E.B.; Knowles, S.B.; Dompier, T.P.; Comstock, R.D.; Marshall, S.W.; et al. The first decade of web-based sports injury surveillance: Descriptive epidemiology of injuries in US High School Girls’ Basketball (2005–2006 through 2013–2014) and National Collegiate Athletic Association Women’s Basketball (2004–2005 through 2013–2014). J. Athl. Train. 2018, 53, 1037–1048. [Google Scholar] [CrossRef] [Green Version]
- Clifton, D.R.; Onate, J.A.; Hertel, J.; Pierpoint, L.A.; Currie, D.W.; Wasserman, E.B.; Knowles, S.B.; Dompier, T.P.; Marshall, S.W.; Comstock, R.D.; et al. The first decade of web-based sports injury surveillance: Descriptive epidemiology of injuries in US High School Boys’ Basketball (2005–2006 through 2013–2014) and National Collegiate Athletic Association Men’s Basketball (2004–2005 through 2013–2014). J. Athl. Train. 2018, 53, 1025–1036. [Google Scholar] [CrossRef] [Green Version]
- Pasanen, K.; Ekola, T.; Vasankari, T.; Kannus, P.; Heinonen, A.; Kujala, U.M.; Parkkari, J. High ankle injury rate in adolescent basketball: A 3-year prospective follow-up study. Scand. J. Med. Sci. Sports 2017, 27, 643–649. [Google Scholar] [CrossRef]
- Zuckerman, S.L.; Wegner, A.M.; Roos, K.G.; Djoko, A.; Dompier, T.P.; Kerr, Z.Y. Injuries sustained in National Collegiate Athletic Association men’s and women’s basketball, 2009/2010–2014/2015. Br. J. Sports Med. 2018, 52, 261–268. [Google Scholar] [CrossRef]
- Leppänen, M.; Pasanen, K.; Kannus, P.; Vasankari, T.; Kujala, U.M.; Heinonen, A.; Parkkari, J. Epidemiology of overuse injuries in youth team sports: A 3-year prospective study. Int. J. Sports Med. 2017, 38, 847–856. [Google Scholar] [CrossRef] [PubMed]
- Emery, C.A. Risk factors for injury in child and adolescent sport: A systematic review of the literature. Clin. J. Sport Med. 2003, 13, 256–268. [Google Scholar] [CrossRef] [PubMed]
- Agresta, C.; Church, C.; Henley, J.; Duer, T.; O’Brien, K. Single-Leg Squat Performance in Active Adolescents Aged 8-17 Years. J. Strength Cond. Res. 2017, 31, 1187–1191. [Google Scholar] [CrossRef] [PubMed]
- Ereña, J.L. La planificación del entrenamiento como posible causa generadora de lesiones en el baloncesto. In Proceedings of Jornadas Sobre Prevención de Lesiones en Baloncesto; INO Reproducciones: Zaragoza, Spain, 2003; pp. 35–73. [Google Scholar]
- Moseid, C.H.; Myklebust, G.; Slaastuen, M.K.; Bar-Yaacov, J.B.; Kristiansen, A.H.; Fagerland, M.W.; Bahr, R. The association between physical fitness level and number and severity of injury and illness in youth elite athletes. Scand. J. Med. Sci. Sports 2019, 29, 1736–1748. [Google Scholar] [CrossRef] [PubMed]
- Monfort, S.M.; Comstock, R.D.; Collins, C.L.; Onate, J.A.; Best, T.M.; Chaudhari, A.M. Association between ball-handling versus defending actions and acute noncontact lower extremity injuries in high school basketball and soccer. Am. J. Sports Med. 2015, 43, 802–807. [Google Scholar] [CrossRef] [PubMed]
- Bahr, R.; Krosshaug, T. Understanding injury mechanisms: A key component of preventing injuries in sport. Br. J. Sports Med. 2005, 39, 324–329. [Google Scholar] [CrossRef]
- Cook, G.; Burton, L.; Hoogenboom, B.J.; Voight, M. Functional movement screening: The use of fundamental movements as an assessment of function—part 1. Int. J. Sports Phys. Ther. 2014, 9, 396–409. [Google Scholar]
- Prangley, I. Assessing and developing the kinetic chain. In Sports Injury Prevention and Rehabilitation: Integrating Medicine and Science for Performance Solutions; Joyce, D., Lewindon, D., Eds.; Taylor & Francis Group: London, UK, 2016; pp. 77–94. [Google Scholar]
- Steele, J.; Sheppard, J. Landing mechanics in injury prevention and performance rehabilitation. In Sports Injury Prevention and Rehabilitation: Integrating Medicine and Science for Performance Solutions; Joyce, D., Lewindon, D., Eds.; Taylor & Francis Group: London, UK, 2016; pp. 121–138. [Google Scholar]
- Taylor, J.B.; Ford, K.R.; Hegedus, E.J. Biomechanics of Lower Extremity Movements and Injury in Basketball. In Basketball Sports Medicine and Science; Laver, L., Kocaoglu, B., Cole, B., Arundale, A., Bytomski, J., Amendola, A., Eds.; Springer: Berlin, Germany, 2020; pp. 37–51. [Google Scholar]
- Taylor, J.B.; Ford, K.R.; Hegedus, E.J. Biomechanics of Upper Extremity Movements and Injury in Basketball. In Basketball Sports Medicine and Science; Laver, L., Kocaoglu, B., Cole, B., Arundale, A., Bytomski, J., Amendola, A., Eds.; Springer: Berlin, Germany, 2020; pp. 53–64. [Google Scholar]
- Torres, L.; Cuzzolin, F. Strength Training for Basketball: A methodological framework based on basketball and player’s needs. In Basketball Sports Medicine and Science; Laver, L., Kocaoglu, B., Cole, B., Arundale, A., Bytomski, J., Amendola, A., Eds.; Springer: Berlin, Germany, 2020; pp. 779–789. [Google Scholar]
- Alderete, J.L.; Osma, J.J. Baloncesto: Técnica de Entrenamiento y Formación de Equipos Base; Gymnos: Madrid, Spain, 1999. [Google Scholar]
- Schelling, X.; Torres-Ronda, L. An integrative approach to strength and neuromuscular power training for basketball. Strength Cond. J. 2016, 38, 72–80. [Google Scholar] [CrossRef]
- Bond, C.; Dorman, J.; Odney, T.; Roggenbuck, S.; Young, S.; Munce, T. Evaluation of the functional movement screen and a novel basketball mobility test as an injury prediction tool for collegiate basketball players. J. Strength Cond. Res. 2019, 33, 1589–1600. [Google Scholar] [CrossRef]
- Calatayud, J.; Martin, F.; Gargallo, P.; García-Redondo, J.; Colado, J.C.; Marín, P.J. The validity and reliability of a new instrumented device for measuring ankle dorsiflexion range of motion. Int. J. Sports Phys. Ther. 2015, 10, 197–202. [Google Scholar]
- Bennell, K.L.; Talbot, R.C.; Wajswelner, H.; Techovanich, W.; Kelly, D.H.; Hall, A.J. Intra-rater and inter-rater reliability of a weight-bearing lunge measure of ankle dorsiflexion. Aust. J. Physiother. 1998, 44, 175–180. [Google Scholar] [CrossRef] [Green Version]
- Trojian, T.H.; McKeag, D.B. Single leg balance test to identify risk of ankle sprains. Br. J. Sports Med. 2006, 40, 610–613. [Google Scholar] [CrossRef] [PubMed]
- Ugalde, V.; Brockman, C.; Bailowitz, Z.; Pollard, C.D. Single leg squat test and its relationship to dynamic knee valgus and injury risk screening. Phys. Med. Rehabil. 2015, 7, 229–235. [Google Scholar] [CrossRef] [PubMed]
- Crossley, K.M.; Zhang, W.J.; Schache, A.G.; Bryant, A.; Cowan, S.M. Performance on the single-leg squat task indicates hip abductor muscle function. Am. J. Sports Med. 2011, 39, 866–873. [Google Scholar] [CrossRef] [PubMed]
- Whatman, C.; Hume, P.; Hing, W. The reliability and validity of physiotherapist visual rating of dynamic pelvis and knee alignment in young athletes. Phys. Ther. Sport 2013, 14, 168–174. [Google Scholar] [CrossRef]
- Ageberg, E.; Bennell, K.L.; Hunt, M.A.; Simic, M.; Roos, E.M.; Creaby, M.W. Validity and inter-rater reliability of medio-lateral knee motion observed during a single-limb mini squat. BMC Musculoskelet. Disord. 2010, 11, 265–272. [Google Scholar] [CrossRef] [Green Version]
- Cook, G.; Burton, L.; Hoogenboom, B. Pre-participation screening: The use of fundamental movements as an assessment of function—part 1. N. Am. J. Sports Phys. Ther. 2006, 1, 62–72. [Google Scholar]
- Svilar, L. Essentials of Physical Performance in Elite Basketball: Testing, Training, Load Monitoring, Periodization and Recovery; Data Status: Novi Sad, Serbia, 2019. [Google Scholar]
- Fort-Vanmeerhaeghe, A.; Montalvo, A.M.; Lloyd, R.S.; Read, P.; Myer, G.D. Intra- and Inter-Rater Reliability of the Modified Tuck Jump Assessment. J. Sports Sci. Med. 2017, 16, 117–124. [Google Scholar]
- Herrington, L.; Myer, G.D.; Munro, A. Intra and inter-tester reliability of the tuck jump assessment. Phys. Ther. Sport. 2013, 14, 152–155. [Google Scholar] [CrossRef]
- Smits-Engelsman, B.; Klerks, M.; Kirby, A. Beighton score: A valid measure for generalized hypermobility in children. J. Pediatr. 2011, 158, 119–123. [Google Scholar] [CrossRef]
- Harris, A.J. Manuel D’application Des Tests de Latéralité; Éditions du Centre de Psychologie Appliquée: Paris, France, 1958. [Google Scholar]
- Hewett, T.E.; Myer, G.D.; Ford, K.R. Anterior cruciate ligament injuries in female athletes: Part 1, mechanisms and risk factors. Am. J. Sports Med. 2006, 34, 299–311. [Google Scholar] [CrossRef] [PubMed]
- Murphy, D.F.; Connolly, D.A.; Beynnon, B.D. Risk factors for lower extremity injury: A review of the literature. Br. J. Sports Med. 2003, 37, 13–29. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gonzalo-Skok, O.; Serna, J.; Rhea, M.R.; Marín, P.J. Age differences in measures of functional movement and performance in highly youth basketball players. Int. J. Sports Phys. Ther. 2017, 12, 812–821. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tao, H.; Husher, A.; Schneider, Z.; Strand, S.; Ness, B. The relationship between single leg balance and isometric ankle and hip strength in a healthy population. Int. J. Sports Phys. Ther. 2020, 15, 712–721. [Google Scholar] [CrossRef]
- Halabchi, F.; Angoorani, H.; Mirshahi, M.; Pourgharib Shahi, M.H.; Mansournia, M.A. The Prevalence of Selected Intrinsic Risk Factors for Ankle Sprain among Elite Football and Basketball Players. Asian J. Sports Med. 2016, 7, e35287. [Google Scholar] [CrossRef] [Green Version]
- Paz, G.A.; Maia, M.; Farias, D.; Santana, H.; Miranda, H.; Lima, V.; Herrington, L. Kinematic analysis of knee valgus during drop vertical jump and forward step-up in young basketball players. Int. J. Sports Phys. Ther. 2016, 11, 212–219. [Google Scholar]
- Steffen, K.; Nilstad, A.; Kristianslund, E.K.; Myklebust, G.; Bahr, R.; Krosshaug, T. Association between Lower Extremity Muscle Strength and Noncontact ACL Injuries. Med. Sci. Sports Exerc. 2016, 48, 2082–2089. [Google Scholar] [CrossRef] [Green Version]
- Powers, C.M. The influence of abnormal hip mechanics on knee injury: A biomechanical perspective. J. Orthop. Sports Phys. Ther. 2010, 40, 42–51. [Google Scholar] [CrossRef] [Green Version]
- Kulas, A.S.; Hortobágyi, T.; DeVita, P. Trunk position modulates anterior cruciate ligament forces and strains during a single-leg squat. Clin. Biomech. 2012, 27, 16–21. [Google Scholar] [CrossRef]
- Shultz, S.J.; Schmitz, R.J.; Benjaminse, A.; Collins, M.; Ford, K.; Kulas, A.S. ACL Research Retreat VII: An Update on Anterior Cruciate Ligament Injury Risk Factor Identification, Screening, and Prevention. J. Athl. Train. 2015, 50, 1076–1093. [Google Scholar] [CrossRef] [Green Version]
- Delahunt, E.; Remus, A. Risk Factors for Lateral Ankle Sprains and Chronic Ankle Instability. J. Athl. Train. 2019, 54, 611–616. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Biabanimoghadam, M.; Motealleh, A.; Cowan, S.M. Core muscle recruitment pattern during voluntary heel raises is different between patients with patellofemoral pain and healthy individuals. Knee 2016, 23, 382–386. [Google Scholar] [CrossRef] [PubMed]
- Cowling, E.J.; Steele, J.R. Is lower limb muscle synchrony during landing affected by gender? Implications for variations in ACL injury rates. J. Electromyogr. Kinesiol. 2001, 11, 263–268. [Google Scholar] [CrossRef]
- Butler, R.J.; Crowell, H.P.; Davis, I.M. Lower extremity stiffness: Implications for performance and injury. Clin. Biomech. 2003, 18, 511–517. [Google Scholar] [CrossRef]
- Podraza, J.T.; White, S.C. Effect of knee flexion angle on ground reaction forces, knee moments and muscle co-contraction during an impact-like deceleration landing: Implications for the non-contact mechanism of ACL injury. Knee 2010, 17, 291–295. [Google Scholar] [CrossRef]
- Pollard, C.D.; Sigward, S.M.; Ota, S.; Langford, K.; Powers, C.M. The influence of in-season injury prevention training on lower-extremity kinematics during landing in female soccer players. Clin. J. Sport Med. 2006, 16, 223–227. [Google Scholar] [CrossRef]
- Fort-Vanmeerhaeghe, A.; Gual, G.; Romero-Rodríguez, D.; Unnitha, V. Lower Limb Neuromuscular Asymmetry in Volleyball and Basketball Players. J. Hum. Kinet. 2016, 50, 135–143. [Google Scholar] [CrossRef]
| Outcomes | U12 (n = 209) | U14 (n = 153) | U16 (n = 110) | U17 (n = 103) |
|---|---|---|---|---|
| Gender a, female | 116 (56.00%) | 82 (54.00%) | 48 (44.00%) | 48 (47.00%) |
| Weight b, kg | 44.04 (8.08) | 53.71 (10.76) | 63.76 (13.50) | 67.27 (12.89) |
| Height b, cm | 154.70 (7.45) | 163.89 (8.92) | 173.30 (14.59) | 176.94 (11.75) |
| Wingspan b, cm | 152.97 (11.26) | 164.07 (14.45) | 174.48 (11.27) | 178.77 (13.98) |
| BMI b, kg/m2 | 18.31 (2.48) | 19.89 (3.00) | 21.11 (3.56) | 21.42 (3.06) |
| Hypermobility a | 10 (5.00%) | 14 (9.00%) | 14 (13.00%) | 12 (12.00%) |
| Right handed a | 182 (87.00%) | 139 (91.00%) | 101 (92.00%) | 73 (89.00%) |
| Gender | Age Categories | Dominant Leg | Non-Dominant Leg | p Value | ||||
|---|---|---|---|---|---|---|---|---|
| Mean (SD) | SE | Interval | Mean (SD) | SE | Interval | |||
| Female | U12 (n = 116) | 10.54 (2.42) | 0.25 | [4.00, 19.50] | 10.26 (2.55) | 0.23 | [2.00, 16.00] | 0.371 |
| U14 (n = 82) | 11.05 (2.49) | 0.32 | [6.00, 17.00] | 11.36 (2.68) | 0.34 | [6.00, 17.00] | 0.500 | |
| U16 (n = 48) | 11.32 (1.61) | 0.26 | [7.50, 14.50] | 11.01 (1.65) | 0.27 | [6.50, 15.00] | 0.859 | |
| U17 (n = 48) | 11.03 (2.05) | 0.34 | [8.00, 16.50] | 11.23 (2.07) | 0.34 | [8.00, 16.00] | 0.674 | |
| Male | U12 (n = 93) | 9.29 (2.26) | 0.25 | [4.00, 17.00] | 9.57 (2.08) | 0.23 | [4.50, 17.00] | 0.399 |
| U14 (n = 71) | 10.52 (2.61) | 0.37 | [4.50, 16.00] | 10.60 (2.45) | 0.34 | [5.00, 17.00] | 0.876 | |
| U16 (n = 62) | 11.27 (2.95) | 0.37 | [3.00, 19.00] | 11.46 (2.89) | 0.36 | [2.50, 19.00] | 0.877 | |
| U17 (n = 55) | 10.21 (1.85) | 0.28 | [6.50, 15.50] | 10.07 (2.13) | 0.32 | [5.00, 15.50] | 0.732 | |
| Gender | Age Categories | Dominant Leg | Non-Dominant Leg | p Value |
|---|---|---|---|---|
| Female | U12 (n = 116) | 111 (96.10%) | 113 (97.80%) | 0.472 |
| U14 (n = 82) | 79 (96.00%) | 77 (93.70%) | 0.315 | |
| U16 (n = 48) | 45 (94.70%) | 43 (89.50%) | 0.395 | |
| U17 (n = 48) | 48 (100%) | 47 (97.30%) | 0.314 | |
| Male | U12 (n = 93) | 89 (95.70%) | 86 (93.00%) | 0.349 |
| U14 (n = 71) | 70 (98.40%) | 71 (100%) | 0.539 | |
| U16 (n = 62) | 61 (98.40%) | 60 (96.90%) | 0.512 | |
| U17 (n = 55) | 51 (93.30%) | 86 (93.00%) | 1.000 |
| Gender | Age Categories | Dominant Leg | Non-Dominant Leg | p Value |
|---|---|---|---|---|
| Female | U12 (n = 116) | 105 (82.70%) | 113 (89.00%) | 0.150 |
| U14 (n = 82) | 49 (79.00%) | 53 (85.50%) | 0.347 | |
| U16 (n = 48) | 40 (84.20%) | 40 (84.20%) | 1.000 | |
| U17 (n = 48) | 39 (81.10%) | 40 (83.80%) | 0.760 | |
| Male | U12 (n = 93) | 79 (95.20%) | 80 (96.40%) | 0.699 |
| U14 (n = 71) | 47 (92.20%) | 44 (86.30%) | 0.338 | |
| U16 (n = 62) | 47 (76.60%) | 47 (75.00%) | 0.798 | |
| U17 (n = 55) | 45 (82.20%) | 53 (95.60%) | 0.044 * |
| Outcome | Age Categories | Female (n = 294) | Male (n = 281) | p Value |
|---|---|---|---|---|
| Lumbopelvic instability | U12 (n = 209) | 110 (94.50%) | 93 (100%) | <0.001 ** |
| U14 (n = 153) | 81 (98.40%) | 67(94.10%) | 0.728 | |
| U16 (n = 110) | 47 (97.40%) | 50 (81.30%) | 0.007 * | |
| U17 (n = 103) | 48 (100%) | 54 (97.80%) | 0.197 | |
| Dynamic postural control deficiencies | U12 (n = 209) | 111 (96.10%) | 93 (100%) | 0.067 |
| U14 (n = 153) | 79 (96.80%) | 65 (92.20%) | 0.276 | |
| U16 (n = 110) | 43 (89.50%) | 53 (85.90%) | 0.605 | |
| U17 (n = 103) | 45 (94.60%) | 43 (77.80%) | 0.032 * |
| Item | Age Categories | Female (n = 294) | Male (n = 281) | p Value |
|---|---|---|---|---|
| Lower extremity valgus at landing | U12 (n = 209) | 111 (96.10%) | 91 (97.60%) | 0.547 |
| U14 (n = 153) | 77 (93.50%) | 65 (92.20%) | 0.774 | |
| U16 (n = 110) | 44 (92.10%) | 51 (82.80%) | 0.187 | |
| U17 (n = 103) | 44 (91.90%) | 45 (82.20%) | 0.201 | |
| Thighs do not reach parallel (peak of jump) | U12 (n = 209) | 94 (81.10%) | 75 (80.70%) | 0.945 |
| U14 (n = 153) | 71 (87.10%) | 64 (90.20%) | 0.607 | |
| U16 (n = 110) | 47 (97.40%) | 47 (76.60%) | 0.005 * | |
| U17 (n = 103) | 39 (81.10%) | 45 (82.20%) | 0.897 | |
| Thighs not equal side to side during flight | U12 (n = 209) | 111 (96.10%) | 89 (95.20%) | 0.758 |
| U14 (n = 153) | 77 (93.50%) | 70 (98.00%) | 0.248 | |
| U16 (n = 110) | 43 (89.50%) | 57 (92.20%) | 0.640 | |
| U17 (n = 103) | 40 (83.80%) | 50 (91.10%) | 0.313 | |
| Foot placement not shoulder width apart | U12 (n = 209) | 102 (88.20%) | 87 (94.00%) | 0.163 |
| U14 (n = 153) | 75 (91.90%) | 67 (94.10%) | 0.653 | |
| U16 (n = 110) | 43 (89.50%) | 47 (75.00%) | 0.075 | |
| U17 (n = 103) | 45 (94.60%) | 43 (77.80%) | 0.032 * | |
| Foot placement not parallel (front to back) | U12 (n = 209) | 108 (92.90%) | 87 (94.00%) | 0.763 |
| U14 (n = 153) | 77 (93.50%) | 67 (94.10%) | 0.901 | |
| U16 (n = 110) | 44 (92.10%) | 52 (84.40%) | 0.258 | |
| U17 (n = 103) | 44 (91.90%) | 55 (100%) | 0.052 | |
| Foot contact timing not equal (asymmetrical landing) | U12 (n = 209) | 102 (88.20%) | 84 (90.40%) | 0.622 |
| U14 (n = 153) | 75 (91.90%) | 59 (82.40%) | 0.124 | |
| U16 (n = 110) | 38 (78.90%) | 50 (81.20%) | 0.777 | |
| U17 (n = 103) | 39 (81.10%) | 48 (86.70%) | 0.491 | |
| Excessive landing contact noise | U12 (n = 209) | 95 (81.90%) | 82 (88.00%) | 0.238 |
| U14 (n = 153) | 73 (88.70%) | 57 (80.40%) | 0.218 | |
| U16 (n = 110) | 44 (92.10%) | 50 (81.20%) | 0.134 | |
| U17 (n = 103) | 39 (81.10%) | 43 (77.80%) | 0.713 | |
| Pause between jumps | U12 (n = 209) | 98 (84.30%) | 82 (88.00%) | 0.454 |
| U14 (n = 153) | 66 (80.60%) | 61 (86.30%) | 0.426 | |
| U16 (n = 110) | 38 (78.90%) | 49 (79.70%) | 0.929 | |
| U17 (n = 103) | 39 (81.10%) | 39 (71.10%) | 0.295 | |
| Technique declines prior 10 s | U12 (n = 209) | 106 (91.30%) | 86 (92.80%) | 0.710 |
| U14 (n = 153) | 77 (93.50%) | 68 (96.10%) | 0.551 | |
| U16 (n = 110) | 44 (92.10%) | 57 (92.20%) | 0.988 | |
| U17 (n = 103) | 44 (91.90%) | 45 (82.20%) | 0.201 | |
| Does not land in same footprint (consistent point of landing) | U12 (n = 209) | 107 (92.10%) | 86 (92.80%) | 0.863 |
| U14 (n = 153) | 73 (88.70%) | 68 (96.10%) | 0.150 | |
| U16 (n = 110) | 44 (92.10%) | 58 (93.70%) | 0.751 | |
| U17 (n = 103) | 40 (83.80%) | 45 (82.20%) | 0.852 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Adillón, C.; Gallegos, M.; Treviño, S.; Salvat, I. Detection of Neuromuscular Deficits in Movement Pattern among Uninjured Federated Youth Basketball Players: A Cross-Sectional Study. Int. J. Environ. Res. Public Health 2022, 19, 4077. https://doi.org/10.3390/ijerph19074077
Adillón C, Gallegos M, Treviño S, Salvat I. Detection of Neuromuscular Deficits in Movement Pattern among Uninjured Federated Youth Basketball Players: A Cross-Sectional Study. International Journal of Environmental Research and Public Health. 2022; 19(7):4077. https://doi.org/10.3390/ijerph19074077
Chicago/Turabian StyleAdillón, Cristina, Montse Gallegos, Silvia Treviño, and Isabel Salvat. 2022. "Detection of Neuromuscular Deficits in Movement Pattern among Uninjured Federated Youth Basketball Players: A Cross-Sectional Study" International Journal of Environmental Research and Public Health 19, no. 7: 4077. https://doi.org/10.3390/ijerph19074077
APA StyleAdillón, C., Gallegos, M., Treviño, S., & Salvat, I. (2022). Detection of Neuromuscular Deficits in Movement Pattern among Uninjured Federated Youth Basketball Players: A Cross-Sectional Study. International Journal of Environmental Research and Public Health, 19(7), 4077. https://doi.org/10.3390/ijerph19074077






