Developing Indicators to Measure Critical Health Literacy in the Context of Norwegian Lower Secondary Schools
Abstract
:1. Introduction
1.1. Measures of HL for Adolescents
1.2. Aims and Structure
2. Materials and Methods
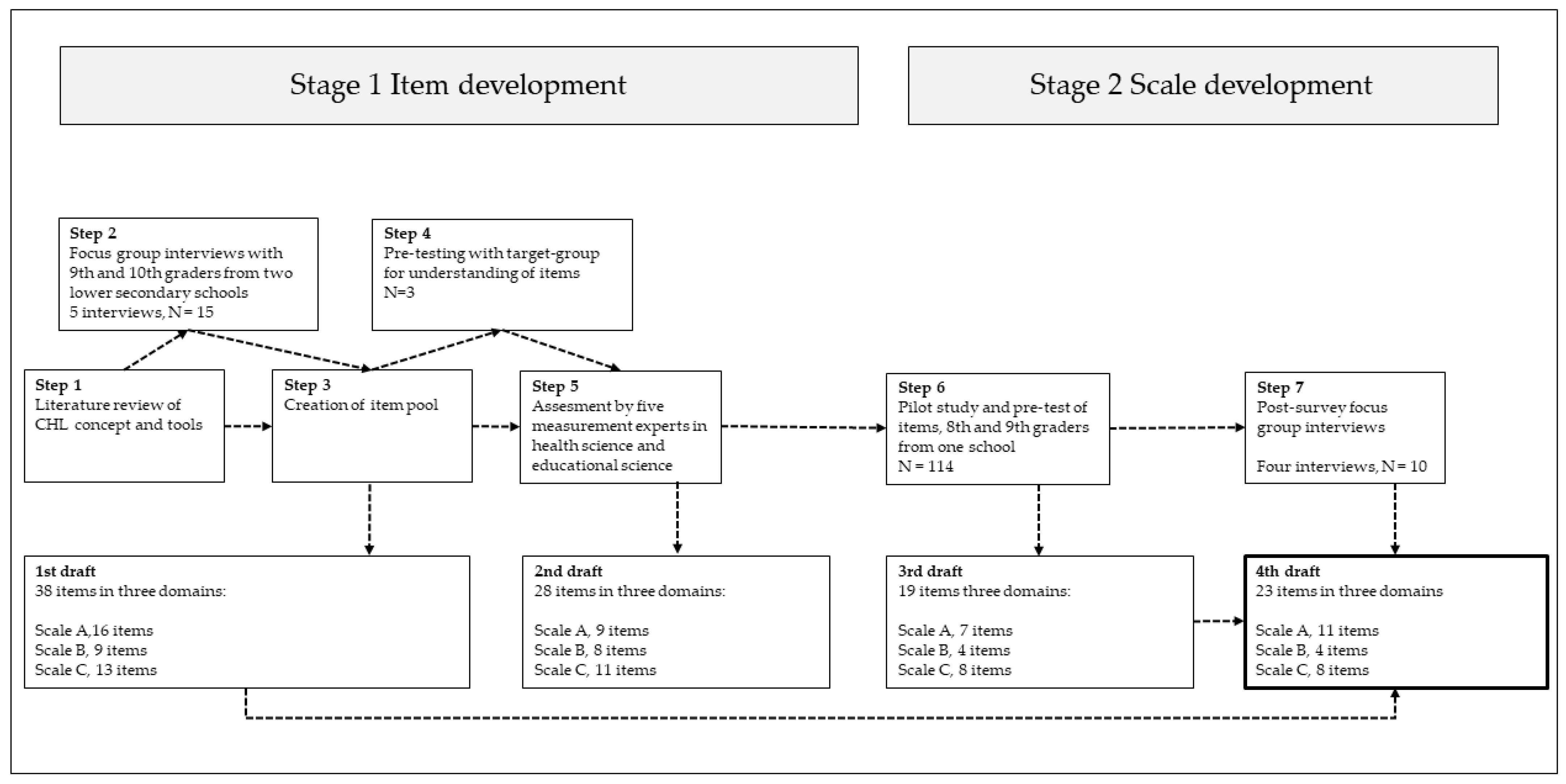
2.1. Design
2.2. Stage 1: Item Development
2.2.1. Literature Review
2.2.2. Focus Group Interviews (Step 2)
2.2.3. Pre-Testing (Steps 4–5)
2.3. Stage 2: Scale Development
2.3.1. Cross-Sectional Survey (Step 6)
2.3.2. Analysis of Psychometric Properties (Step 6)
2.3.3. Post-Survey Focus Group Interviews (Step 7)
2.4. Ethical Considerations
3. Results
3.1. Stage 1: Item Development
Focus Group Interviews (Step 1)
3.2. Stage 2: Scale Development (Step 6)
3.2.1. Scale A: Critical Information Appraisal
3.2.2. Scale B: Awareness of Social Determinants of Health
3.2.3. Scale C: Citizenship for Health and Well-Being in the School Context
3.2.4. Convergent Validity
3.3. Stage 2: Post-Survey Focus Group Interviews and Revision of the Third Draft (Step 7)
4. Discussion
Limitations and Future Research
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Paakkari, L.; Paakkari, O. Health literacy as a learning outcome in schools. Health Educ. 2012, 112, 133–152. [Google Scholar] [CrossRef] [Green Version]
- WHO. Health 2020 A European Policy Framework and Strategy for the 21st Century. 2013. Available online: https://www.euro.who.int/__data/assets/pdf_file/0011/199532/Health2020-Long.pdf (accessed on 10 February 2022).
- WHO. Shanghai Declaration on Promoting Health in the 2030 Agenda for Sustainable Development. 2016. Available online: https://www.who.int/healthpromotion/conferences/9gchp/shanghai-declaration.pdf (accessed on 7 November 2021).
- Nash, R.; Patterson, K.; Flittner, A.; Elmer, S.; Osborne, R. School-Based Health Literacy Programs for Children (2–16 Years): An International Review. J. Sch. Health 2021, 91, 632–649. [Google Scholar] [CrossRef] [PubMed]
- Paakkari, L.; Okan, O. COVID-19: Health literacy is an underestimated problem. Lancet Public Health 2020, 5, e249. [Google Scholar] [CrossRef]
- Peralta, L.; Rowling, L.; Samdal, O.; Hipkins, R.; Dudley, D. Conceptualising a new approach to adolescent health literacy. Health Educ. J. 2017, 76, 787–801. [Google Scholar] [CrossRef]
- WHO. Health Literacy in the Context of Health, Well-Being and Learning Outcomes-the Case of Children and Adolescents in Schools. Available online: https://www.euro.who.int/en/health-topics/Life-stages/child-and-adolescent-health/publications/2021/health-literacy-in-the-context-of-health,-well-being-and-learning-outcomes-the-case-of-children-and-adolescents-in-schools-the-case-of-children-and-adolescents-in-schools-2021 (accessed on 7 November 2021).
- Lovdata. Available online: https://lovdata.no/dokument/NLE/lov/1998-07-17-61 (accessed on 10 February 2022).
- Norwegian Directorate for Education and Training. Available online: https://www.udir.no/lk20/overordnet-del/?lang=eng (accessed on 5 September 2021).
- Schulenkorf, T.; Sørensen, K.; Okan, O. International Understandings of Health Literacy in Childhood and Adolescence— A Qualitative-Explorative Analysis of Global Expert Interviews. Int. J. Environ. Res. Public Health 2022, 19, 1591. [Google Scholar] [CrossRef]
- Nutbeam, D. Health literacy as a public health goal: A challenge for contemporary health education and communication strategies into the 21st century. Health Promot. Int. 2000, 15, 259–267. [Google Scholar] [CrossRef] [Green Version]
- Nutbeam, D. The evolving concept of health literacy. Soc. Sci. Med. 2008, 67, 2072–2078. [Google Scholar] [CrossRef]
- Sørensen, K. Defining health literacy: Exploring differences and commonalities. In International Handbook of Health Literacy. Research, Practice and Policy across the Lifespan; Orkan, O., Bauer, U., Levin-Zamir, D., Pinheiro, P., Sørensen, K., Eds.; Policy Press: Bristol, UK, 2019; Available online: http://library.oapen.org/handle/20.500.12657/24879 (accessed on 7 September 2021).
- Nutbeam, D. Health Promotion Glossary. Health Promot. Int. 1998, 13, 349–364. [Google Scholar] [CrossRef]
- Sorensen, K.; van den Broucke, S.; Pelikan, J.M.; Fullam, J.; Doyle, G.; Slonska, Z.; Kondilis, B.; Stoffels, V.; Osborne, R.H.; Brand, H. Measuring health literacy in populations: Illuminating the design and development process of the European Health Literacy Survey Questionnaire (HLS-EU-Q). BMC Public Health 2013, 13, 948. [Google Scholar] [CrossRef] [Green Version]
- Broder, J.; Okan, O.; Bauer, U.; Bruland, D.; Schlupp, S.; Bollweg, T.M.; Saboga-Nunes, L.; Bond, E.; Sorensen, K.; Bitzer, E.M.; et al. Health literacy in childhood and youth: A systematic review of definitions and models. BMC Public Health 2017, 17, 419. [Google Scholar] [CrossRef] [Green Version]
- Bröder, J.; Okan, O.; Bauer, U.; Schlupp, S.; Pinheiro, P. Advancing perspectives on health literacy in childhood and youth. Health Promot. Int. 2020, 35, 575–585. [Google Scholar] [CrossRef] [PubMed]
- Paakkari, L.; George, S. Ethical underpinnings for the development of health literacy in schools: Ethical premises (‘why’), orientations (‘what’) and tone (‘how’). BMC Public Health 2018, 18, 326. [Google Scholar] [CrossRef] [PubMed]
- Madsen, O.J. Livsmestring på Timeplanen: Rett Medisin for Elevene? [Life Skills on the Curricula–Prescription for Healthy Pupils?]; Spartacus: Oslo, Norway, 2020. [Google Scholar]
- Ryan, M.; Rossi, T.; Hunter, L.; Macdonald, D.; McCuaig, L. Theorising a Framework for Contemporary Health Literacies in Schools. Curric. Perspect. 2012, 32, 1–10. [Google Scholar]
- Chinn, D. Critical health literacy: A review and critical analysis. Soc. Sci. Med. 2011, 73, 60–67. [Google Scholar] [CrossRef]
- Sykes, S.; Wills, J.; Rowlands, G.; Popple, K. Understanding critical health literacy: A concept analysis. BMC Public Health 2013, 13, 150. [Google Scholar] [CrossRef] [Green Version]
- Sykes, S.; Wills, J. Challenges and opportunities in building critical health literacy. Glob. Health Promot. 2018, 25, 48–56. [Google Scholar] [CrossRef]
- Sykes, S.; Wills, J. Critical health literacy for the marginalised: Empirical findings. In International Handbook of Health Literacy-Research, Practice and Policy across the Lifespan; LSBU Open Research: Bristol, UK, 2019; pp. 167–181. [Google Scholar]
- Guo, S.J.; Armstrong, R.; Waters, E.; Sathish, T.; Alif, S.M.; Browne, G.R.; Yu, X.M. Quality of health literacy instruments used in children and adolescents: A systematic review. BMJ Open 2018, 8, e020080. [Google Scholar] [CrossRef]
- Okan, O.; Lopes, E.; Bollweg, T.M.; Bröder, J.; Messer, M.; Bruland, D.; Bond, E.; Carvalho, G.S.; Sørensen, K.; Saboga-Nunes, L.; et al. Generic health literacy measurement instruments for children and adolescents: A systematic review of the literature. BMC Public Health 2018, 18, 166. [Google Scholar] [CrossRef] [Green Version]
- Ormshaw, M.J.; Paakkari, L.T.; Kannas, L.K. Measuring child and adolescent health literacy: A systematic review of literature. Health Educ. 2013, 113, 433–455. [Google Scholar] [CrossRef]
- Perry, E.L. Health literacy in adolescents: An integrative review. J. Spec. Pediatric Nurs. 2014, 19, 210–218. [Google Scholar] [CrossRef]
- Abel, T.; Hofmann, K.; Ackermann, S.; Bucher, S.; Sakarya, S. Health literacy among young adults: A short survey tool for public health and health promotion research. Health Promot. Int. 2015, 30, 725–735. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ghanbari, S.; Ramezankhani, A.; Montazeri, A.; Mehrabi, Y. Health Literacy Measure for Adolescents (HELMA): Development and Psychometric Properties. PLoS ONE 2016, 11, e0149202. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Manganello, J.A.; DeVellis, R.F.; Davis, T.C.; Schottler-Thal, C. Development of the Health Literacy Assessment Scale for Adolescents (HAS-A). J. Commun. Healthc. 2015, 8, 172–184. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Paakkari, O.; Torppa, M.; Kannas, L.; Paakkari, L. Subjective health literacy: Development of a brief instrument for school-aged children. Scand. J. Public Health 2016, 44, 751–757. [Google Scholar] [CrossRef] [PubMed]
- Wu, A.D.; Begoray, D.L.; MacDonald, M.; Higgins, J.W.; Frankish, J.; Kwan, B.; Fung, W.; Rootman, I. Developing and evaluating a relevant and feasible instrument for measuring health literacy of Canadian high school students. Health Promot. Int. 2010, 25, 444–452. [Google Scholar] [CrossRef] [Green Version]
- Bollweg, T.M.; Okan, O.; Pinheiro, P.; Bauer, U. Development of a health literacy measurement tool for primary school children in Germany. Eur. J. Public Health 2016, 26, 68. [Google Scholar] [CrossRef] [Green Version]
- Domanska, O.M.; Bollweg, T.M.; Loer, A.K.; Holmberg, C.; Schenk, L.; Jordan, S. Development and Psychometric Properties of a Questionnaire Assessing Self-Reported Generic Health Literacy in Adolescence. Int. J. Environ. Res. Public Health 2020, 17, 2860. [Google Scholar] [CrossRef] [Green Version]
- Boateng, G.O.; Neilands, T.B.; Frongillo, E.A.; Melgar-Quiñonez, H.R.; Young, S.L. Best Practices for Developing and Validating Scales for Health, Social, and Behavioral Research: A Primer. Front. Public Health 2018, 6, 149. [Google Scholar] [CrossRef]
- Robson, C. Real World Research: A Resource for Social Scientists and Practitioner-Researchers; Blackwell: Oxford, UK, 2002; p. 599. [Google Scholar]
- DeVellis, R.F. Scale Development-Theory and Applications, 2nd ed.; Sage Publications, Inc.: Thousand Oaks, CA, USA, 2003; Volume 26. [Google Scholar]
- Walseth, K. Literacies for Health and Life Skills. 2016. Available online: https://uni.oslomet.no/hls/ (accessed on 10 February 2022).
- Friborg, O. Klassisk testteori og utvikling av spørreinstrumenter [Classical test theory and development of questionaires]. In Kvantitativ Forskningsmetodologi i Samfunns-og Helsefag [Quantitative Research Methodology in Social-and Health Sciences]; Martinussen, M., Ed.; Fagbokforl: Bergen, Norway, 2010. [Google Scholar]
- Ulleberg, P.; Nordvik, H. Faktoranalyse [Factor Analysis]; Tapir Akademisk Forlag: Trondheim, Norway, 2001; Volume 2, p. 33. [Google Scholar]
- Dziuban, C.D.; Shirkey, E.C. When is a correlation matrix appropriate for factor analysis? Some decision rules. Psychol. Bull. 1974, 81, 358–361. [Google Scholar] [CrossRef]
- Kaiser, H.F.; Rice, J. Little Jiffy, Mark Iv. Educ. Psychol. Meas. 1974, 34, 111–117. [Google Scholar] [CrossRef]
- Browne, M.W.; Cudeck, R. Alternative Ways of Assessing Model Fit. Sociol. Methods Res. 1992, 21, 230–258. [Google Scholar] [CrossRef]
- Terwee, C.B.; Bot, S.D.M.; de Boer, M.R.; van der Windt, D.A.W.M.; Knol, D.L.; Dekker, J.; Bouter, L.M.; de Vet, H.C.W. Quality criteria were proposed for measurement properties of health status questionnaires. J. Clin. Epidemiol. 2007, 60, 34–42. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Paakkari, O.; Torppa, M.; Boberova, Z.; Valimaa, R.; Maier, G.; Mazur, J.; Kannas, L.; Paakkari, L. The cross-national measurement invariance of the health literacy for school-aged children (HLSAC) instrument. Eur. J. Public Health 2019, 29, 432–436. [Google Scholar] [CrossRef] [PubMed]
- Bjørnsen, H.N.; Ringdal, R.; Espnes, G.A.; Eilertsen, M.-E.B.; Moksnes, U.K. Exploring MEST: A new universal teaching strategy for school health services to promote positive mental health literacy and mental wellbeing among Norwegian adolescents. BMC Health Serv. Res. 2018, 18, 1001. [Google Scholar] [CrossRef]
- Riiser, K.; Helseth, S.; Haraldstad, K.; Torbjørnsen, A.; Richardsen, K.R. Adolescents’ health literacy, health protective measures, and health-related quality of life during the COVID-19 pandemic. PLoS ONE 2020, 15, e0238161. [Google Scholar] [CrossRef]
- Haraldstad, K.; Christophersen, K.-A.; Eide, H.; Nativg, G.K.; Helseth, S. Health related quality of life in children and adolescents: Reliability and validity of the Norwegian version of KIDSCREEN-52 questionnaire, a cross sectional study. Int. J. Nurs. Stud. 2011, 48, 573–581. [Google Scholar] [CrossRef]
- Fayers, P.M.; Sprangers, M.A.G. Understanding self-rated health. Lancet 2002, 359, 187–188. [Google Scholar] [CrossRef]
- Joffer, J.; Jerden, L.; Ohman, A.; Flacking, R. Exploring self-rated health among adolescents: A think-aloud study. BMC Public Health 2016, 16, 156. [Google Scholar] [CrossRef]
- Revelle, W. Psych: Procedures for Psychological, Psychometric, and Personality Research [R Package Version 2.1.9]; Northwestern University: Evanston, IL, USA, 2021; Available online: https://CRAN.R-project.org/package=psych (accessed on 9 October 2021).
- Makransky, G.; Wandall, J.; Madsen, S.R.; Hood, M.; Creed, P. Development and Validation of the UiL-Scales for Measurement of Development in Life Skills—A Test Battery of Non-Cognitive Skills for Danish School Children. Scand. J. Educ. Res. 2020, 64, 612–627. [Google Scholar] [CrossRef]
- Stars, I.; Rubene, Z. A Phenomenographic Study of Adolescents’ Conceptions of Health Information Appraisal as a Critical Component of Adolescent Health Literacy. Acta Paedagog. Vilnensia 2020, 44, 62–80. [Google Scholar] [CrossRef]
- Mogford, E.; Gould, L.; DeVoght, A. Teaching critical health literacy in the US as a means to action on the social determinants of health. Health Promot. Int. 2010, 26, 4–13. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pleasant, A. Advancing Health Literacy Measurement: A Pathway to Better Health and Health System Performance. J. Health Commun. 2014, 19, 1481–1496. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ran, M.; Peng, L.; Liu, Q.; Pender, M.; He, F.; Wang, H. The association between quality of life(QOL) and health literacy among junior middle school students: A cross-sectional study. BMC Public Health 2018, 18, 1183. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Popay, J.; Bennett, S.; Thomas, C.; Williams, G.; Gatrell, A.; Bostock, L. Beyond ‘beer, fags, egg and chips’? Exploring lay understandings of social inequalities in health. Sociol. Health Illn. 2003, 25, 1–23. [Google Scholar] [CrossRef] [Green Version]
- Blaxter, M. Whose fault is it? People’s own conceptions of the reasons for health inequalities. Soc. Sci. Med. 1997, 44, 747–756. [Google Scholar] [CrossRef]
- Davidson, R.; Kitzinger, J.; Hunt, K. The wealthy get healthy, the poor get poorly? Lay perceptions of health inequalities. Soc. Sci. Med. 2006, 62, 2171–2182. [Google Scholar] [CrossRef]
- Gould, L.; Mogford, E.; DeVoght, A. Successes and Challenges of Teaching the Social Determinants of Health in Secondary Schools: Case Examples in Seattle, Washington. Health Promot. Pract. 2010, 11, 26S–33S. [Google Scholar] [CrossRef]
- Beitchman, J.H.; Corradini, A. Self-report measures for use with children: A review and comment. J. Clin. Psychol. 1988, 44, 477–490. [Google Scholar] [CrossRef]
- Bandura, A. Health Promotion by Social Cognitive Means. Health Educ. Behav. 2004, 31, 143–164. [Google Scholar] [CrossRef]
| Scale A: Critical Information Appraisal | |||||
|---|---|---|---|---|---|
| Items | F1 | F2 | h2 | u2 | com |
| chl9 | 0.86 | 0.74 | 0.26 | 1.0 | |
| chl8 | 0.76 | 0.66 | 0.34 | 1.0 | |
| chl7 | 0.68 | 0.38 | 0.62 | 1.1 | |
| chl5 | 0.90 | 0.77 | 0.23 | 1.0 | |
| chl4 | 0.68 | 0.54 | 0.46 | 1.0 | |
| chl6 | 0.40 | 0.31 | 0.69 | 1.6 | |
| chl1 | 0.33 | 0.27 | 0.73 | 1.9 | |
| Eigenvalue | 2.0 | 1.7 | |||
| Prop var | 0.28 | 0.24 | |||
| Cronbach’s α = 0.83 (αF1 = 0.80, αF2 = 0.75) | |||||
| TLI = 0.97 RSMEA = 0.055 [CI 90%, 0–0.132] | |||||
| Scale B: Awareness of Social Determinants of Health | ||||
|---|---|---|---|---|
| Items | F1 | h2 | u2 | com |
| chl12 | 0.80 | 0.63 | 0.37 | 1 |
| chl14 | 0.37 | 0.13 | 0.87 | 1 |
| chl16 | 0.55 | 0.30 | 0.70 | 1 |
| chl13 | 0.46 | 0.21 | 0.79 | 1 |
| Eigenvalue | 1.3 | |||
| Prop var | 0.32 | |||
| Cronbach’s α = 0.61 | ||||
| TLI = 1.05 RMSEA = 0.00 [CI 90%, 0–0.16] | ||||
| Scale C: Citizenship for Health and Well-Being | |||||
|---|---|---|---|---|---|
| Items | F1 | F2 | h2 | u2 | com |
| chl26 | 0.98 | 0.87 | 0.13 | 1.0 | |
| chl24 | 0.70 | 0.69 | 0.31 | 1.2 | |
| chl20 | 0.63 | 0.54 | 0.46 | 1.2 | |
| chl25 | 0.52 | 0.46 | 0.54 | 1.4 | |
| chl28 | 0.71 | 0.44 | 0.56 | 1.1 | |
| chl22 | 0.57 | 0.39 | 0.61 | 1.1 | |
| chl18 | 0.56 | 0.45 | 0.55 | 1.2 | |
| chl23 | 0.56 | 0.43 | 0.57 | 1.2 | |
| Eigenvalue | 2.4 | 1.8 | |||
| Prop var | 0.30 | 0.23 | |||
| Cronbach’s α = 0.85 (αF1 = 0.86, αF2 = 0.73) TLI = 0.95 RMSEA = 0.074 [CI 90%, 0–0.13] | |||||
| Revised or Added in Step 7 | Source | Scale A1: Critical Information Appraisal How Easy or Difficult Is It for You to… | Component |
|---|---|---|---|
| (chl4) revised | MOHLAA-Q [35] | …decide whether media information about illness can be trusted (media: internet, TV, newspapers) | Accuracy/impartiality |
| (chl6) revised | Self-developed | …decide whether information about healthy habits is also a commercial (healthy habits: what you eat/drink, physical activity) | Accuracy/impartiality |
| (chl4) revised | MOHLAA-Q | …decide whether media information about healthy habits can be trusted (healthy habits: what you eat/drink, physical activity) | Accuracy/impartiality |
| (chl8) revised | Self-developed | …find out whether health information is relevant to you when you are ill | Relevance |
| New | HLS-Child-Q15 [34] | …judge what food is healthy for you | Relevance |
| (chl9) revised | Self-developed | …judge whether information on healthy habits is relevant to you (healthy habits: what you eat/drink, physical activity) | Relevance |
| (chl4) revised | MOHLAA-Q | …judge whether information about unhealthy habits can be trusted (unhealthy habits: alcohol, tobacco, what you eat/drink) | Accuracy/impartiality |
| Revised or added in step 7 | Source | Scale A2: Critical information appraisal I am a person who… | |
| (chl1) revised | HELMA [30] | …compares health information from different sources (sources: internet, parents, friends) | Accuracy/impartiality |
| New | HLS-Child-Q15 | …can decide what I need to do to stay healthy and what doesn’t help that much | Accuracy/impartiality |
| (chl5) revised | HELMA | …can decide whether a source of health information can be trusted (source: internet, TV, newspapers) | Accuracy/impartiality |
| (chl7) revised | Self-developed | …asks for help if I am unsure about the trustworthiness of health information | Accuracy/impartiality/Help seeking |
| Revised or added in step 7 | Source | Scale B: Awareness of social determinants of health To what extent do you agree with the following statements? | |
| (chl12) unchanged | Self-developed | Some groups in society have fewer opportunities for good health. | Health inequality |
| (chl13) unchanged | Self-developed | Everybody has the same opportunities to be healthy. | Health inequality |
| (chl14) revised | Self-developed | Where you grow up could have a significant impact on your health. | Health inequality |
| (chl16) unchanged | Self-developed | It is unfair that some groups in society have poorer health than others. | Health inequality |
| Revised or added in step 7 (revised/new) | Scale C: Citizenship for health and well-being I am a person who… | ||
| (chl26) unchanged | UiL/self-developed [53] | …can support others if they are feeling sad. | Citizenship/social support |
| (chl24) unchanged | UiL/self-developed | …can help others if they are not doing well. | Citizenship/social support |
| (chl20) unchanged | Self-developed | …can contribute to the well-being of others in my class. | Citizenship/social support |
| (chl25) unchanged | UiL | …can help find solutions that are acceptable to all parties. | Citizenship/social support |
| (chl28) unchanged | Self-developed | …can easily talk to others, even if I don’t know them very well. | Citizenship/democratic participation |
| (chl18) unchanged | HELMA | …can share information about factors that influence health with others. | Citizenship/democratic participation |
| (chl23) unchanged | Self-developed | …believes my knowledge about health could be useful for others. | Citizenship/democratic participation |
| (chl22) unchanged | HLSAC [32] | …is aware of how my actions can influence others (e.g., attitude, mood). | Citizenship/democratic participation |
| Measurement Domain | Key Content | |
|---|---|---|
| Scale A Critical information appraisal of health-related information | Appraisal leads to decisions about the credibility and relevance of health-related information. Important criteria adolescents can use include the extent to which a piece of information is accurate, impartial, and relevant to them [33]. During appraisal, adolescents investigate the characteristics of information (e.g., who wrote it, when it was published, and what sources the writer used) and compare information from different sources. They apply prior knowledge and seek help [54]. Sometimes they feel helpless. | (A1) Perceived difficulty of performing cognitive tasks. (A2) Self-efficacy to perform cognitive tasks |
| Scale B Awareness of social determinants of health (SDH) | Awareness of SDH involves a deeper understanding of health and encourages an understanding that health is influenced by more than individual lifestyle choices [21]. Recognizing health inequities is crucial to understanding the causes behind these inequities [55] | Attitudes/self-reported knowledge |
| Scale C Citizenship for health and well-being in the school context | Citizenship in HL centers on the ability to understand and act on the rights and responsibilities that come with participation in a democratic collective [1]. Key components are self-efficacy to provide social support and participate in democratic discussions on matters that concern health and well-being. | Self-efficacy to perform social and communicative tasks |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Haugen, A.L.H.; Riiser, K.; Esser-Noethlichs, M.; Hatlevik, O.E. Developing Indicators to Measure Critical Health Literacy in the Context of Norwegian Lower Secondary Schools. Int. J. Environ. Res. Public Health 2022, 19, 3116. https://doi.org/10.3390/ijerph19053116
Haugen ALH, Riiser K, Esser-Noethlichs M, Hatlevik OE. Developing Indicators to Measure Critical Health Literacy in the Context of Norwegian Lower Secondary Schools. International Journal of Environmental Research and Public Health. 2022; 19(5):3116. https://doi.org/10.3390/ijerph19053116
Chicago/Turabian StyleHaugen, Anders L. Hage, Kirsti Riiser, Marc Esser-Noethlichs, and Ove Edvard Hatlevik. 2022. "Developing Indicators to Measure Critical Health Literacy in the Context of Norwegian Lower Secondary Schools" International Journal of Environmental Research and Public Health 19, no. 5: 3116. https://doi.org/10.3390/ijerph19053116
APA StyleHaugen, A. L. H., Riiser, K., Esser-Noethlichs, M., & Hatlevik, O. E. (2022). Developing Indicators to Measure Critical Health Literacy in the Context of Norwegian Lower Secondary Schools. International Journal of Environmental Research and Public Health, 19(5), 3116. https://doi.org/10.3390/ijerph19053116





