The Adverse Effects of Air Pollution on the Eye: A Review
Abstract
:1. Introduction
1.1. The Composition of Air Pollution
1.2. The Influences of Air Pollution to Human Eyes
2. Material and Methods
3. Results and Discussion
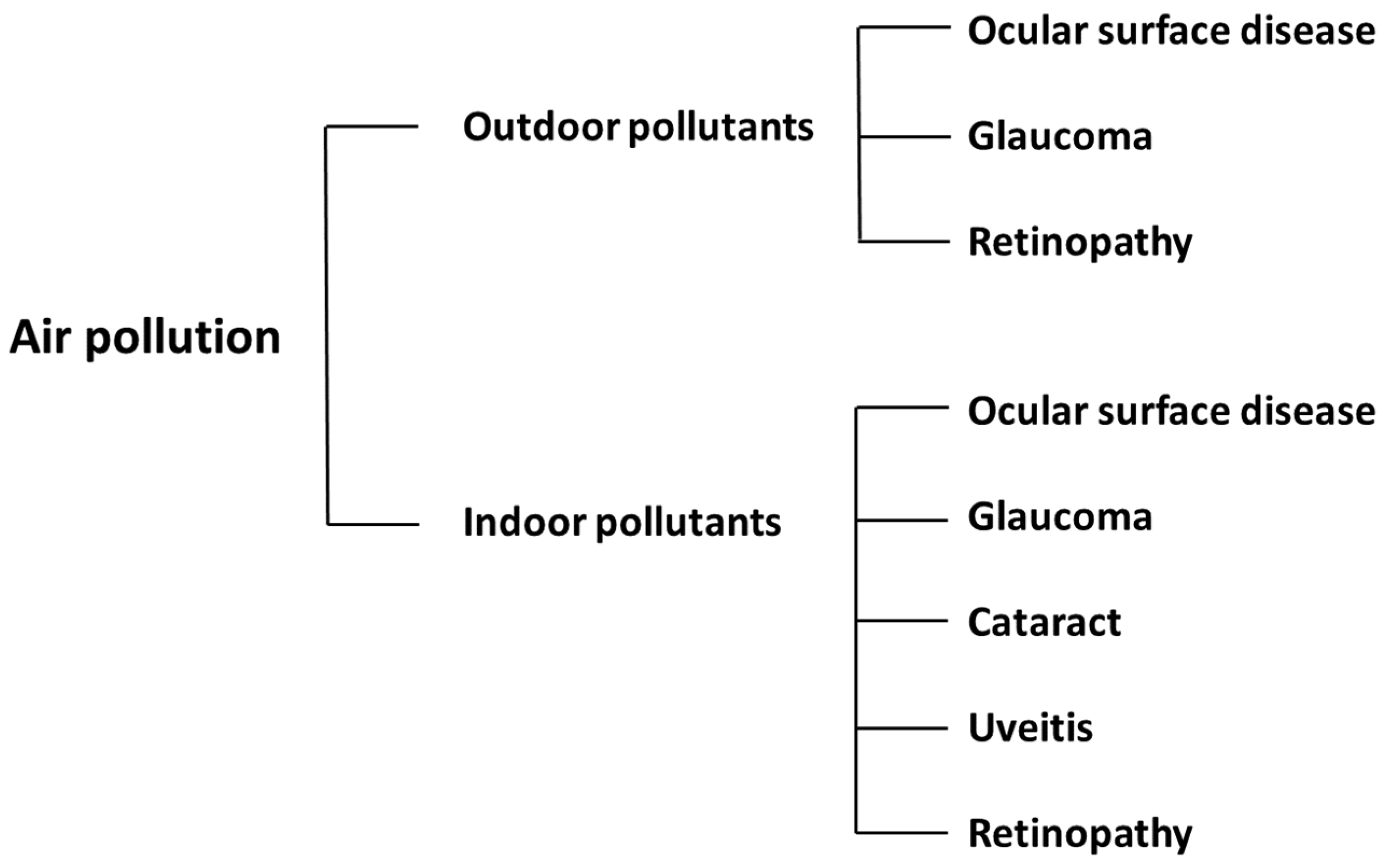
3.1. Outdoor Air Pollution
3.1.1. Ocular Surface Diseases (OSDs)
3.1.2. Glaucoma
3.1.3. Retinopathy and Maculopathy
3.2. Indoor Air Pollution
3.2.1. Ocular Surface Disease
3.2.2. Glaucoma
3.2.3. Cataract
3.2.4. Uveitis
3.2.5. Retinal and Macular Diseases
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Cohen, A.J.; Brauer, M.; Burnett, R.; Anderson, H.R.; Frostad, J.; Estep, K.; Balakrishnan, K.; Brunekreef, B.; Dandona, L.; Dandona, R.; et al. Estimates and 25-year trends of the global burden of disease attributable to ambient air pollution: An analysis of data from the Global Burden of Diseases Study 2015. Lancet 2017, 389, 1907–1918. [Google Scholar] [CrossRef] [Green Version]
- Di, Q.; Wang, Y.; Zanobetti, A.; Wang, Y.; Koutrakis, P.; Choirat, C.; Dominici, F.; Schwartz, J.D. Air Pollution and Mortality in the Medicare Population. N. Engl. J. Med. 2017, 376, 2513–2522. [Google Scholar] [CrossRef] [PubMed]
- Abellán, R.; Mansego, M.L.; Martínez-Hervás, S.; Martín-Escudero, J.C.; Carmena, R.; Real, J.T.; Redon, J.; Castrodeza-Sanz, J.J.; Chaves, F.J. Association of selected ABC gene family single nucleotide polymorphisms with postprandial lipoproteins: Results from the population-based Hortega study. Atherosclerosis 2010, 211, 203–209. [Google Scholar] [CrossRef]
- Kemp, A.C.; Horton, B.P.; Donnelly, J.P.; Mann, M.E.; Vermeer, M.; Rahmstorf, S. Climate related sea-level variations over the past two millennia. Proc. Natl. Acad. Sci. USA 2011, 108, 11017–11022. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Swenberg, J.A.; Moeller, B.C.; Lu, K.; Rager, J.E.; Fry, R.C.; Starr, T.B. Formaldehyde carcinogenicity research: 30 years and counting for mode of action, epidemiology, and cancer risk assessment. Toxicol. Pathol. 2013, 41, 181–189. [Google Scholar] [CrossRef] [Green Version]
- Zhang, J.; Smith, K.R. Indoor air pollution: A global health concern. Br. Med. Bull. 2003, 68, 209–225. [Google Scholar] [CrossRef] [Green Version]
- Eftim, S.E.; Samet, J.M.; Janes, H.; McDermott, A.; Dominici, F. Fine particulate matter and mortality: A comparison of the six cities and American Cancer Society cohorts with a medicare cohort. Epidemiology 2008, 19, 209–216. [Google Scholar] [CrossRef]
- Pope, C.A., 3rd. Air pollution and health-good news and bad. N. Engl. J. Med. 2004, 351, 1132–1134. [Google Scholar] [CrossRef] [Green Version]
- Pope, C.A., 3rd; Dockery, D.W. Health effects of fine particulate air pollution: Lines that connect. J. Air. Waste Manag. Assoc. 2006, 56, 709–742. [Google Scholar] [CrossRef]
- Saxena, R.; Srivastava, S.; Trivedi, D.; Anand, E.; Joshi, S.; Gupta, S.K. Impact of environmental pollution on the eye. Acta Ophthalmol. Scand. 2003, 81, 491–494. [Google Scholar] [CrossRef] [PubMed]
- Tuominen, I.S.; Konttinen, Y.T.; Vesaluoma, M.H.; Moilanen, J.A.; Helintö, M.; Tervo, T.M. Corneal innervation and morphology in primary Sjögren’s syndrome. Invest. Ophthalmol. Vis. Sci. 2003, 44, 2545–2549. [Google Scholar] [CrossRef] [Green Version]
- Al-Aqaba, M.A.; Dhillon, V.K.; Mohammed, I.; Said, D.G.; Dua, H.S. Corneal nerves in health and disease. Prog. Retin. Eye Res. 2019, 73, 100762. [Google Scholar] [CrossRef]
- Koh, S.; Tung, C.I.; Inoue, Y.; Jhanji, V. Effects of tear film dynamics on quality of vision. Br. J. Ophthalmol. 2018, 102, 1615–1620. [Google Scholar] [CrossRef]
- Schwela, D. Air pollution and health in urban areas. Rev. Environ. Health 2000, 15, 13–42. [Google Scholar] [CrossRef] [PubMed]
- Versura, P.; Profazio, V.; Cellini, M.; Torreggiani, A.; Caramazza, R. Eye discomfort and air pollution. Ophthalmologica 1999, 213, 103–109. [Google Scholar] [CrossRef] [PubMed]
- Mimura, T.; Ichinose, T.; Yamagami, S.; Fujishima, H.; Kamei, Y.; Goto, M.; Takada, S.; Matsubara, M. Airborne particulate matter (PM2.5) and the prevalence of allergic conjunctivitis in Japan. Sci. Total Environ. 2014, 487, 493–499. [Google Scholar] [CrossRef]
- Hong, J.; Zhong, T.; Li, H.; Xu, J.; Ye, X.; Mu, Z.; Lu, Y.; Mashaghi, A.; Zhou, Y.; Tan, M.; et al. Ambient air pollution, weather changes, and outpatient visits for allergic conjunctivitis: A retrospective registry study. Sci. Rep. 2016, 6, 23858. [Google Scholar] [CrossRef] [Green Version]
- Wang, W.; He, M.; Li, Z.; Huang, W. Epidemiological variations and trends in health burden of glaucoma worldwide. Acta Ophthalmol. 2019, 97, e349–e355. [Google Scholar] [CrossRef] [Green Version]
- Chua, S.Y.L.; Khawaja, A.P.; Morgan, J.; Strouthidis, N.; Reisman, C.; Dick, A.D.; Khaw, P.T.; Patel, P.J.; Foster, P.J. The Relationship Between Ambient Atmospheric Fine Particulate Matter (PM2.5) and Glaucoma in a Large Community Cohort. Invest Ophthalmol. Vis. Sci. 2019, 60, 4915–4923. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Raju, P.; George, R.; Ve Ramesh, S.; Arvind, H.; Baskaran, M.; Vijaya, L. Influence of tobacco use on cataract development. Br. J. Ophthalmol. 2006, 90, 1374–1377. [Google Scholar] [CrossRef] [Green Version]
- Chang, K.-H.; Hsu, P.-Y.; Lin, C.-J.; Lin, C.-L.; Juo, S.-H.H.; Liang, C.-L. Traffic-related air pollutants increase the risk for age-related macular degeneration. J. Investig. Med. 2019, 67, 1076. [Google Scholar] [CrossRef] [PubMed]
- Jetten, N.; Verbruggen, S.; Gijbels, M.J.; Post, M.J.; De Winther, M.P.; Donners, M.M. Anti-inflammatory M2, but not pro-inflammatory M1 macrophages promote angiogenesis in vivo. Angiogenesis 2014, 17, 109–118. [Google Scholar] [CrossRef] [PubMed]
- Ambient (Outdoor) Air Quality and Health. Available online: https://www.who.int/mediacentre/factsheets/fs313/en/ (accessed on 22 September 2021).
- Aitio, A.; Axelson, O.; Blair, A.; Bond, J.A.; Bucher, J.R.; Caldwell, J.; Coggon, D.; Demers, P.A.; Dragani, T.A.; Elcombe, C.R.; et al. Outdoor Air Pollution. IARC Monogr. Eval. Carcinog. Risks Hum. 2016, 109, 9–444. [Google Scholar]
- Huff, R.D.; Carlsten, C.; Hirota, J.A. An update on immunologic mechanisms in the respiratory mucosa in response to air pollutants. J. Allergy Clin. Immunol. 2019, 143, 1989–2001. [Google Scholar] [CrossRef]
- Kappos, A.D.; Bruckmann, P.; Eikmann, T.; Englert, N.; Heinrich, U.; Höppe, P.; Koch, E.; Krause, G.H.; Kreyling, W.G.; Rauchfuss, K.; et al. Health effects of particles in ambient air. Int. J. Hyg. Environ. Health 2004, 207, 399–407. [Google Scholar] [CrossRef]
- Holguin, F. Traffic, outdoor air pollution, and asthma. Immunol. Allergy Clin. N. Am. 2008, 28, 577–588. [Google Scholar] [CrossRef] [PubMed]
- Hetland, R.B.; Cassee, F.R.; Låg, M.; Refsnes, M.; Dybing, E.; Schwarze, P.E. Cytokine release from alveolar macrophages exposed to ambient particulate matter: Heterogeneity in relation to size, city and season. Part. Fibre Toxicol. 2005, 2, 4. [Google Scholar] [CrossRef] [Green Version]
- McCreanor, J.; Cullinan, P.; Nieuwenhuijsen, M.J.; Stewart-Evans, J.; Malliarou, E.; Jarup, L.; Harrington, R.; Svartengren, M.; Han, I.K.; Ohman-Strickland, P.; et al. Respiratory effects of exposure to diesel traffic in persons with asthma. N. Engl. J. Med. 2007, 357, 2348–2358. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Vohra, K.; Vodonos, A.; Schwartz, J.; Marais, E.A.; Sulprizio, M.P.; Mickley, L.J. Global mortality from outdoor fine particle pollution generated by fossil fuel combustion: Results from GEOS-Chem. Environ. Res. 2021, 195, 110754. [Google Scholar] [CrossRef]
- Bourcier, T.; Viboud, C.; Cohen, J.C.; Thomas, F.; Bury, T.; Cadiot, L.; Mestre, O.; Flahault, A.; Borderie, V.; Laroche, L. Effects of air pollution and climatic conditions on the frequency of ophthalmological emergency examinations. Br. J. Ophthalmol. 2003, 87, 809–811. [Google Scholar] [CrossRef] [Green Version]
- Chang, C.J.; Yang, H.H.; Chang, C.A.; Tsai, H.Y. Relationship between air pollution and outpatient visits for nonspecific conjunctivitis. Invest. Ophthalmol. Vis. Sci. 2012, 53, 429–433. [Google Scholar] [CrossRef] [Green Version]
- Torricelli, A.; Novaes, P.; Matsuda, M.; Alves, M.; Monteiro, M. Ocular surface adverse effects of ambient levels of air pollution. Arq. Bras. De Oftalmol. 2011, 74, 377–381. [Google Scholar] [CrossRef] [Green Version]
- Novaes, P.; do Nascimento Saldiva, P.H.; Kara-José, N.; Macchione, M.; Matsuda, M.; Racca, L.; Berra, A. Ambient levels of air pollution induce goblet-cell hyperplasia in human conjunctival epithelium. Environ. Health Perspect. 2007, 115, 1753–1756. [Google Scholar] [CrossRef] [Green Version]
- Zhong, J.-Y.; Lee, Y.-C.; Hsieh, C.-J.; Tseng, C.-C.; Yiin, L.-M. Association between Dry Eye Disease, Air Pollution and Weather Changes in Taiwan. Int. J. Environ. Res. Public Health 2018, 15, 2269. [Google Scholar] [CrossRef] [Green Version]
- Liu, H.; Begley, C.; Chen, M.; Bradley, A.; Bonanno, J.; McNamara, N.A.; Nelson, J.D.; Simpson, T. A link between tear instability and hyperosmolarity in dry eye. Invest. Ophthalmol. Vis. Sci. 2009, 50, 3671–3679. [Google Scholar] [CrossRef] [PubMed]
- Bron, A.J.; Abelson, M.B.; Ousler, G.; Pearce, E.; Tomlinson, A.; Yokoi, A.; Smith, J.A.; Begley, C.; Caffery, B.; Nichols, K. Methodologies to diagnose and monitor dry eye disease: Report of the Diagnostic Methodology Subcommittee of the International Dry Eye WorkShop (2007). Ocul. Surf. 2007, 5, 108–152. [Google Scholar]
- Tan, G.; Li, J.; Yang, Q.; Wu, A.; Qu, D.Y.; Wang, Y.; Ye, L.; Bao, J.; Shao, Y. Air pollutant particulate matter 2.5 induces dry eye syndrome in mice. Sci. Rep. 2018, 8, 17828. [Google Scholar] [CrossRef] [Green Version]
- Yoon, S.; Han, S.; Jeon, K.J.; Kwon, S. Effects of collected road dusts on cell viability, inflammatory response, and oxidative stress in cultured human corneal epithelial cells. Toxicol. Lett. 2018, 284, 152–160. [Google Scholar] [CrossRef] [PubMed]
- Li, L.; Xing, C.; Zhou, J.; Niu, L.; Luo, B.; Song, M.; Niu, J.; Ruan, Y.; Sun, X.; Lei, Y. Airborne particulate matter (PM2.5) triggers ocular hypertension and glaucoma through pyroptosis. Part. Fibre Toxicol. 2021, 18, 10. [Google Scholar] [CrossRef]
- Zeng, Y.; Li, M.; Zou, T.; Chen, X.; Li, Q.; Li, Y.; Ge, L.; Chen, S.; Xu, H. The Impact of Particulate Matter (PM2.5) on Human Retinal Development in hESC-Derived Retinal Organoids. Front. Cell Dev. Biol. 2021, 9, 607341. [Google Scholar] [CrossRef] [PubMed]
- Sun, H.Y.; Luo, C.W.; Chiang, Y.W.; Yeh, K.L.; Li, Y.C.; Ho, Y.C.; Lee, S.S.; Chen, W.Y.; Chen, C.J.; Kuan, Y.H. Association Between PM2.5 Exposure Level and Primary Open-Angle Glaucoma in Taiwanese Adults: A Nested Case-Control Study. Int. J. Environ. Res. Public Health 2021, 18, 1714. [Google Scholar] [CrossRef]
- Min, K.B.; Min, J.Y. Association of Ambient Particulate Matter Exposure with the Incidence of Glaucoma in Childhood. Am. J. Ophthalmol. 2020, 211, 176–182. [Google Scholar] [CrossRef]
- Lodovici, M.; Bigagli, E. Oxidative stress and air pollution exposure. J. Toxicol. 2011, 2011, 487074. [Google Scholar] [CrossRef]
- Baccarelli, A.; Zanobetti, A.; Martinelli, I.; Grillo, P.; Hou, L.; Giacomini, S.; Bonzini, M.; Lanzani, G.; Mannucci, P.M.; Bertazzi, P.A.; et al. Effects of exposure to air pollution on blood coagulation. J. Thromb. Haemost. 2007, 5, 252–260. [Google Scholar] [CrossRef]
- Brook, R.D.; Rajagopalan, S.; Pope, C.A., 3rd; Brook, J.R.; Bhatnagar, A.; Diez-Roux, A.V.; Holguin, F.; Hong, Y.; Luepker, R.V.; Mittleman, M.A.; et al. Particulate matter air pollution and cardiovascular disease: An update to the scientific statement from the American Heart Association. Circulation 2010, 121, 2331–2378. [Google Scholar] [CrossRef] [Green Version]
- Jarrett, S.G.; Boulton, M.E. Consequences of oxidative stress in age-related macular degeneration. Mol. Asp. Med. 2012, 33, 399–417. [Google Scholar] [CrossRef] [Green Version]
- Lee, H.; Hwang-Bo, H.; Ji, S.Y.; Kim, M.Y.; Kim, S.Y.; Park, C.; Hong, S.H.; Kim, G.Y.; Song, K.S.; Hyun, J.W.; et al. Diesel particulate matter2.5 promotes epithelial-mesenchymal transition of human retinal pigment epithelial cells via generation of reactive oxygen species. Environ. Pollut. 2020, 262, 114301. [Google Scholar] [CrossRef]
- Wei, C.C.; Lin, H.J.; Lim, Y.P.; Chen, C.S.; Chang, C.Y.; Lin, C.J.; Chen, J.J.; Tien, P.T.; Lin, C.L.; Wan, L. PM2.5 and NOx exposure promote myopia: Clinical evidence and experimental proof. Environ. Pollut. 2019, 254, 113031. [Google Scholar] [CrossRef]
- Chua, S.Y.L.; Khawaja, A.P.; Dick, A.D.; Morgan, J.; Dhillon, B.; Lotery, A.J.; Strouthidis, N.G.; Reisman, C.; Peto, T.; Khaw, P.T.; et al. Ambient Air Pollution Associations with Retinal Morphology in the UK Biobank. Investig. Ophthalmol. Vis. Sci. 2020, 61, 32. [Google Scholar] [CrossRef]
- Pan, S.C.; Huang, C.C.; Chin, W.S.; Chen, B.Y.; Chan, C.C.; Guo, Y.L. Association between air pollution exposure and diabetic retinopathy among diabetics. Environ. Res. 2020, 181, 108960. [Google Scholar] [CrossRef]
- Shan, A.; Chen, X.; Yang, X.; Yao, B.; Liang, F.; Yang, Z.; Liu, F.; Chen, S.; Yan, X.; Huang, J.; et al. Association between long-term exposure to fine particulate matter and diabetic retinopathy among diabetic patients: A national cross-sectional study in China. Environ. Int. 2021, 154, 106568. [Google Scholar] [CrossRef]
- West, S.K.; Bates, M.N.; Lee, J.S.; Schaumberg, D.A.; Lee, D.J.; Adair-Rohani, H.; Chen, D.F.; Araj, H. Is household air pollution a risk factor for eye disease? Int. J. Environ. Res. Public Health 2013, 10, 5378–5398. [Google Scholar] [CrossRef] [Green Version]
- Kabir, E.; Kim, K.H. An investigation on hazardous and odorous pollutant emission during cooking activities. J. Hazard. Mater. 2011, 188, 443–454. [Google Scholar] [CrossRef]
- Wolkoff, P. External eye symptoms in indoor environments. Indoor Air 2017, 27, 246–260. [Google Scholar] [CrossRef]
- Wolkoff, P. Indoor air pollutants in office environments: Assessment of comfort, health, and performance. Int. J. Hyg. Environ. Health 2013, 216, 371–394. [Google Scholar] [CrossRef]
- Jaén, C.; Dalton, P. Asthma and odors: The role of risk perception in asthma exacerbation. J. Psychosom. Res. 2014, 77, 302–308. [Google Scholar] [CrossRef] [Green Version]
- Luengas, A.; Barona, A.; Hort, C.; Gallastegui, G.; Platel, V.; Elias, A. A review of indoor air treatment technologies. Rev. Environ. Sci. Bio/Technol. 2015, 14, 499–522. [Google Scholar] [CrossRef]
- de Juniac, A.; Kreis, I.; Ibison, J.; Murray, V. Epidemiology of unintentional carbon monoxide fatalities in the UK. Int. J. Environ. Health Res. 2012, 22, 210–219. [Google Scholar] [CrossRef]
- Sarigiannis, D.A.; Karakitsios, S.P.; Gotti, A.; Liakos, I.L.; Katsoyiannis, A. Exposure to major volatile organic compounds and carbonyls in European indoor environments and associated health risk. Environ. Int. 2011, 37, 743–765. [Google Scholar] [CrossRef]
- Jordan, R.E.; Cheng, K.K.; Miller, M.R.; Adab, P. Passive smoking and chronic obstructive pulmonary disease: Cross-sectional analysis of data from the Health Survey for England. BMJ Open 2011, 1, e000153. [Google Scholar] [CrossRef] [Green Version]
- Blanc, P.D.; Eisner, M.D.; Katz, P.P.; Yen, I.H.; Archea, C.; Earnest, G.; Janson, S.; Masharani, U.B.; Quinlan, P.J.; Hammond, S.K.; et al. Impact of the home indoor environment on adult asthma and rhinitis. J. Occup. Environ. Med. 2005, 47, 362–372. [Google Scholar] [CrossRef]
- Rushton, L. Health impact of environmental tobacco smoke in the home. Rev. Environ. Health 2004, 19, 291–309. [Google Scholar] [CrossRef]
- Gawande, S.; Tiwari, R.R.; Narayanan, P.; Bhadri, A. Indoor Air Quality and Sick Building Syndrome: Are Green Buildings Better than Conventional Buildings? Indian J. Occup. Environ. Med. 2020, 24, 30–32. [Google Scholar]
- Martheswaran, T.; Shmunes, M.H.; Ronquillo, Y.C.; Moshirfar, M. The impact of vaping on ocular health: A literature review. Int. Ophthalmol. 2021, 41, 2925–2932. [Google Scholar] [CrossRef]
- Choi, W.; Lian, C.; Ying, L.; Kim, G.E.; You, I.C.; Park, S.H.; Yoon, K.C. Expression of Lipid Peroxidation Markers in the Tear Film and Ocular Surface of Patients with Non-Sjogren Syndrome: Potential Biomarkers for Dry Eye Disease. Curr. Eye Res. 2016, 41, 1143–1149. [Google Scholar] [CrossRef]
- Yang, Q.; Li, K.; Li, D.; Zhang, Y.; Liu, X.; Wu, K. Effects of fine particulate matter on the ocular surface: An in vitro and in vivo study. Biomed. Pharmacother. 2019, 117, 109177. [Google Scholar] [CrossRef]
- Bascom, R.; Kulle, T.; Kagey-Sobotka, A.; Proud, D. Upper respiratory tract environmental tobacco smoke sensitivity. Am. Rev. Respir. Dis. 1991, 143, 1304–1311. [Google Scholar] [CrossRef]
- Annesi-Maesano, I.; Oryszczyn, M.P.; Raherison, C.; Kopferschmitt, C.; Pauli, G.; Taytard, A.; Tunon de Lara, M.; Vervloet, D.; Charpin, D. Increased prevalence of asthma and allied diseases among active adolescent tobacco smokers after controlling for passive smoking exposure. A cause for concern? Clin. Exp. Allergy 2004, 34, 1017–1023. [Google Scholar] [CrossRef]
- Díaz, E.; Smith-Sivertsen, T.; Pope, D.; Lie, R.T.; Díaz, A.; McCracken, J.; Arana, B.; Smith, K.R.; Bruce, N. Eye discomfort, headache and back pain among Mayan Guatemalan women taking part in a randomised stove intervention trial. J. Epidemiol. Community Health 2007, 61, 74–79. [Google Scholar] [CrossRef] [Green Version]
- Vitoux, M.A.; Kessal, K.; Baudouin, C.; Laprévote, O.; Melik Parsadaniantz, S.; Achard, S.; Brignole-Baudouin, F. Formaldehyde Gas Exposure Increases Inflammation in an In Vitro Model of Dry Eye. Toxicol. Sci. 2018, 165, 108–117. [Google Scholar] [CrossRef] [Green Version]
- Gupta, S.; Fink, M.K.; Martin, L.M.; Sinha, P.R.; Rodier, J.T.; Sinha, N.R.; Hesemann, N.P.; Chaurasia, S.S.; Mohan, R.R. A rabbit model for evaluating ocular damage from acrolein toxicity in vivo. Ann. N. Y. Acad. Sci. 2020, 1480, 233–245. [Google Scholar] [CrossRef]
- Li, J.; Zhang, G.; Nian, S.; Lv, Y.; Shao, Y.; Qiao, N.; Liang, R.; Huang, L.; Luo, A. Dry eye induced by exposure to cigarette smoke pollution: An in vivo and in vitro study. Free. Radic. Biol. Med. 2020, 153, 187–201. [Google Scholar] [CrossRef]
- Lee, K.; Hong, S.; Seong, G.J.; Kim, C.Y. Cigarette Smoke Extract Causes Injury in Primary Retinal Ganglion Cells via Apoptosis and Autophagy. Curr. Eye Res. 2016, 41, 1367–1372. [Google Scholar] [CrossRef]
- Smith, C.A.; Vianna, J.R.; Chauhan, B.C. Assessing retinal ganglion cell damage. Eye 2017, 31, 209–217. [Google Scholar] [CrossRef] [Green Version]
- Lee, A.J.; Rochtchina, E.; Wang, J.J.; Healey, P.R.; Mitchell, P. Does smoking affect intraocular pressure? Findings from the Blue Mountains Eye Study. J. Glaucoma 2003, 12, 209–212. [Google Scholar] [CrossRef]
- Jain, V.; Jain, M.; Abdull, M.M.; Bastawrous, A. The association between cigarette smoking and primary open-angle glaucoma: A systematic review. Int. Ophthalmol. 2017, 37, 291–301. [Google Scholar] [CrossRef]
- Pérez-de-Arcelus, M.; Toledo, E.; Martínez-González, M.; Martín-Calvo, N.; Fernández-Montero, A.; Moreno-Montañés, J. Smoking and incidence of glaucoma: The SUN Cohort. Medicine 2017, 96, e5761. [Google Scholar] [CrossRef]
- Reports of the Surgeon General. In The Health Consequences of Smoking: A Report of the Surgeon General; Centers for Disease Control and Prevention (US): Atlanta, GA, USA, 2004.
- Nagata, M.; Kojima, M.; Sasaki, K. Effect of vitamin E eye drops on naphthalene-induced cataract in rats. J. Ocul. Pharmacol. Ther. 1999, 15, 345–350. [Google Scholar] [CrossRef]
- Xu, G.T.; Zigler, J.S., Jr.; Lou, M.F. The possible mechanism of naphthalene cataract in rat and its prevention by an aldose reductase inhibitor (ALO1576). Exp. Eye Res. 1992, 54, 63–72. [Google Scholar] [CrossRef]
- Schaumberg, D.A.; Mendes, F.; Balaram, M.; Dana, M.R.; Sparrow, D.; Hu, H. Accumulated lead exposure and risk of age-related cataract in men. JAMA 2004, 292, 2750–2754. [Google Scholar] [CrossRef] [Green Version]
- Nita, M.; Grzybowski, A. Smoking and Eye Pathologies. A Systemic Review. Part I. Anterior Eye Segment Pathologies. Curr. Pharm. Des. 2017, 23, 629–638. [Google Scholar]
- Fullerton, D.G.; Bruce, N.; Gordon, S.B. Indoor air pollution from biomass fuel smoke is a major health concern in the developing world. Trans. R. Soc. Trop. Med. Hyg. 2008, 102, 843–851. [Google Scholar] [CrossRef] [Green Version]
- Saha, A.; Kulkarni, P.K.; Shah, A.; Patel, M.; Saiyed, H.N. Ocular morbidity and fuel use: An experience from India. Occup. Environ. Med. 2005, 62, 66–69. [Google Scholar] [CrossRef]
- Pokhrel, A.K.; Smith, K.R.; Khalakdina, A.; Deuja, A.; Bates, M.N. Case-control study of indoor cooking smoke exposure and cataract in Nepal and India. Int. J. Epidemiol. 2005, 34, 702–708. [Google Scholar] [CrossRef] [Green Version]
- González, M.M.; Solano, M.M.; Porco, T.C.; Oldenburg, C.E.; Acharya, N.R.; Lin, S.C.; Chan, M.F. Epidemiology of uveitis in a US population-based study. J. Ophthalmic Inflamm. Infect. 2018, 8, 6. [Google Scholar] [CrossRef] [Green Version]
- Yuen, B.G.; Tham, V.M.; Browne, E.N.; Weinrib, R.; Borkar, D.S.; Parker, J.V.; Uchida, A.; Vinoya, A.C.; Acharya, N.R. Association between Smoking and Uveitis: Results from the Pacific Ocular Inflammation Study. Ophthalmology 2015, 122, 1257–1261. [Google Scholar] [CrossRef] [Green Version]
- Lin, P.; Loh, A.R.; Margolis, T.P.; Acharya, N.R. Cigarette smoking as a risk factor for uveitis. Ophthalmology 2010, 117, 585–590. [Google Scholar] [CrossRef] [Green Version]
- Roesel, M.; Ruttig, A.; Schumacher, C.; Heinz, C.; Heiligenhaus, A. Smoking complicates the course of non-infectious uveitis. Graefe’s Arch. Clin. Exp. Ophthalmol. 2011, 249, 903–907. [Google Scholar] [CrossRef]
- Sarir, H.; Mortaz, E.; Karimi, K.; Kraneveld, A.D.; Rahman, I.; Caldenhoven, E.; Nijkamp, F.P.; Folkerts, G. Cigarette smoke regulates the expression of TLR4 and IL-8 production by human macrophages. J. Inflamm. 2009, 6, 12. [Google Scholar] [CrossRef] [Green Version]
- Gonçalves, R.B.; Coletta, R.D.; Silvério, K.G.; Benevides, L.; Casati, M.Z.; da Silva, J.S.; Nociti, F.H., Jr. Impact of smoking on inflammation: Overview of molecular mechanisms. Inflamm. Res. 2011, 60, 409–424. [Google Scholar] [CrossRef]
- Iho, S.; Tanaka, Y.; Takauji, R.; Kobayashi, C.; Muramatsu, I.; Iwasaki, H.; Nakamura, K.; Sasaki, Y.; Nakao, K.; Takahashi, T. Nicotine induces human neutrophils to produce IL-8 through the generation of peroxynitrite and subsequent activation of NF-kappaB. J. Leukoc. Biol. 2003, 74, 942–951. [Google Scholar] [CrossRef]
- Curnow, S.J.; Falciani, F.; Durrani, O.M.; Cheung, C.M.; Ross, E.J.; Wloka, K.; Rauz, S.; Wallace, G.R.; Salmon, M.; Murray, P.I. Multiplex bead immunoassay analysis of aqueous humor reveals distinct cytokine profiles in uveitis. Invest. Ophthalmol. Vis. Sci. 2005, 46, 4251–4259. [Google Scholar] [CrossRef] [PubMed]
- Valentincic, N.V.; de Groot-Mijnes, J.D.; Kraut, A.; Korosec, P.; Hawlina, M.; Rothova, A. Intraocular and serum cytokine profiles in patients with intermediate uveitis. Mol. Vis. 2011, 17, 2003–2010. [Google Scholar]
- Khera, T.K.; Copland, D.A.; Boldison, J.; Lait, P.J.; Szymkowski, D.E.; Dick, A.D.; Nicholson, L.B. Tumour necrosis factor-mediated macrophage activation in the target organ is critical for clinical manifestation of uveitis. Clin. Exp. Immunol. 2012, 168, 165–177. [Google Scholar] [CrossRef]
- Quintana, F.J.; Basso, A.S.; Iglesias, A.H.; Korn, T.; Farez, M.F.; Bettelli, E.; Caccamo, M.; Oukka, M.; Weiner, H.L. Control of T(reg) and T(H)17 cell differentiation by the aryl hydrocarbon receptor. Nature 2008, 453, 65–71. [Google Scholar] [CrossRef] [PubMed]
- Veldhoen, M.; Hirota, K.; Westendorf, A.M.; Buer, J.; Dumoutier, L.; Renauld, J.C.; Stockinger, B. The aryl hydrocarbon receptor links TH17-cell-mediated autoimmunity to environmental toxins. Nature 2008, 453, 106–109. [Google Scholar] [CrossRef] [PubMed]
- Torii, K.; Saito, C.; Furuhashi, T.; Nishioka, A.; Shintani, Y.; Kawashima, K.; Kato, H.; Morita, A. Tobacco smoke is related to Th17 generation with clinical implications for psoriasis patients. Exp. Dermatol. 2011, 20, 371–373. [Google Scholar] [CrossRef]
- Escobar, T.; Yu, C.R.; Muljo, S.A.; Egwuagu, C.E. STAT3 activates miR-155 in Th17 cells and acts in concert to promote experimental autoimmune uveitis. Investig. Ophthalmol. Vis. Sci. 2013, 54, 4017–4025. [Google Scholar] [CrossRef] [Green Version]
- Wang, R.X.; Yu, C.R.; Mahdi, R.M.; Egwuagu, C.E. Novel IL27p28/IL12p40 cytokine suppressed experimental autoimmune uveitis by inhibiting autoreactive Th1/Th17 cells and promoting expansion of regulatory T cells. J. Biol. Chem. 2012, 287, 36012–36021. [Google Scholar] [CrossRef] [Green Version]
- Jadidi-Niaragh, F.; Mirshafiey, A. Th17 cell, the new player of neuroinflammatory process in multiple sclerosis. Scand. J. Immunol. 2011, 74, 1–13. [Google Scholar] [CrossRef]
- van Hamburg, J.P.; Asmawidjaja, P.S.; Davelaar, N.; Mus, A.M.; Colin, E.M.; Hazes, J.M.; Dolhain, R.J.; Lubberts, E. Th17 cells, but not Th1 cells, from patients with early rheumatoid arthritis are potent inducers of matrix metalloproteinases and proinflammatory cytokines upon synovial fibroblast interaction, including autocrine interleukin-17A production. Arthritis Rheum. 2011, 63, 73–83. [Google Scholar] [CrossRef]
- Zhang, L.; Li, J.M.; Liu, X.G.; Ma, D.X.; Hu, N.W.; Li, Y.G.; Li, W.; Hu, Y.; Yu, S.; Qu, X.; et al. Elevated Th22 cells correlated with Th17 cells in patients with rheumatoid arthritis. J. Clin. Immunol. 2011, 31, 606–614. [Google Scholar] [CrossRef]
- Smith, W.; Assink, J.; Klein, R.; Mitchell, P.; Klaver, C.C.; Klein, B.E.; Hofman, A.; Jensen, S.; Wang, J.J.; de Jong, P.T. Risk factors for age-related macular degeneration: Pooled findings from three continents. Ophthalmology 2001, 108, 697–704. [Google Scholar] [CrossRef]
- Khan, J.C.; Thurlby, D.A.; Shahid, H.; Clayton, D.G.; Yates, J.R.; Bradley, M.; Moore, A.T.; Bird, A.C. Smoking and age related macular degeneration: The number of pack years of cigarette smoking is a major determinant of risk for both geographic atrophy and choroidal neovascularisation. Br. J. Ophthalmol. 2006, 90, 75–80. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Smith, W.; Mitchell, P.; Leeder, S.R. Smoking and age-related maculopathy. The Blue Mountains Eye Study. Arch. Ophthalmol. 1996, 114, 1518–1523. [Google Scholar] [CrossRef]
- Bai, Y.C.; Wang, C.Y.; Lin, C.L.; Lai, J.N.; Wei, J.C. Association Between Air Pollution and the Risk of Uveitis: A Nationwide, Population-Based Cohort Study. Front. Immunol. 2021, 12, 613893. [Google Scholar] [CrossRef] [PubMed]
- Pons, M.; Marin-Castano, M.E. Nicotine increases the VEGF/PEDF ratio in retinal pigment epithelium: A possible mechanism for CNV in passive smokers with AMD. Invest. Ophthalmol. Vis. Sci. 2011, 52, 3842–3853. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Nita, M.; Grzybowski, A. Smoking and Eye Pathologies. A Systemic Review. Part II. Retina Diseases, Uveitis, Optic Neuropathies, Thyroid-Associated Orbitopathy. Curr. Pharm. Des. 2017, 23, 639–654. [Google Scholar]
- Govindaraju, V.K.; Bodas, M.; Vij, N. Cigarette smoke induced autophagy-impairment regulates AMD pathogenesis mechanisms in ARPE-19 cells. PLoS ONE 2017, 12, e0182420. [Google Scholar] [CrossRef] [Green Version]
| Pollutant(s) | Ocular Disorder(s) | Study Model | Reference |
|---|---|---|---|
| Outdoor pollutant(s) | |||
| CO | AMD | Population-based study | [21] |
| NO | Conjunctivitis | Data collection | [22,23] |
| NO2 | AMD | Population-based study | [21] |
| Conjunctivitis | Data collection | [24] | |
| Nonspecific conjunctivitis | [25] | ||
| NOx | Myopia | Data collection | [26] |
| In vivo/hamster model | |||
| O3 | Nonspecific conjunctivitis | Data collection | [25] |
| PM2.5 | DR | National cross-sectional study | [27] |
| Myopia | Data collection | [26] | |
| In vivo/hamster model | |||
| Nonspecific conjunctivitis | Data collection | [25] | |
| POAG | Nested case–control study | [28] | |
| Retinal layer thinning | Community-based cohort study | [29] | |
| PM10 | Childhood glaucoma | Retrospective cohort study | [30] |
| Nonspecific conjunctivitis | Data collection | [25] | |
| Retinal layer thinning | Community-based cohort study | [29] | |
| SO2 | Nonspecific conjunctivitis | Data collection | [25] |
| Indoor pollutant(s) | |||
| Acrolein | OSD | In vivo/rabbit model | [31] |
| Aldehydes | Tear film instability and lipid layer peroxidation | Tears from subjects | [22,23] |
| CSE | AMD | In vitro/ARPE-19 cells | [32] |
| Glaucoma | In vitro/primary rat RGCs | [33,34] | |
| Formaldehyde | OSD | In vitro/WKD cells | [35] |
| Naphthalene | Cataracts | In vivo/rat model | [36,37] |
| Nicotine | OSD | In vitro/corneal epithelial cells | [38] |
| Uveitis | Subjects’ and patients’ AqH | [39,40,41,42] | |
| PM2.5 | Dry eye syndrome | In vitro/HCE cells | [43] |
| In vivo/mouse model | |||
| Tabaco smoking | OSD | In vitro/HCE cells | [44] |
| In vivo/mouse model | |||
| Rhino-conjunctivitis | Cross-sectional study | [45] | |
| Pollutant(s) | Averaging Time | WHO 2021 Air Quality Guideline | WHO 2005 Air Quality Guideline | Change |
|---|---|---|---|---|
| PM2.5 (μg/m3) | Annual | 5 | 10 | −50% |
| 24-h | 15 | 25 | −40% | |
| PM10 (μg/m3) | Annual | 15 | 20 | −25% |
| 24-h | 45 | 50 | −10% | |
| O3 (μg/m3) | Peak season | 60 | N/A | Newly introduced |
| 8-h | 100 | 100 | Unchanged | |
| NO2 (μg/m3) | Annual | 10 | 40 | −75% |
| 24-h | 25 | N/A | Newly introduced | |
| 1-h | 200 | 200 | Unchanged | |
| SO2 (μg/m3) | 24-h | 40 | 20 | +100% |
| 10-min | 500 | 500 | Unchanged | |
| CO (mg/m3) | 24-h | 4 | N/A | Newly introduced |
| 8-h | 10 | N/A | Newly introduced | |
| 1-h | 35 | N/A | Newly introduced | |
| 15-min | 100 | N/A | Newly introduced |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lin, C.-C.; Chiu, C.-C.; Lee, P.-Y.; Chen, K.-J.; He, C.-X.; Hsu, S.-K.; Cheng, K.-C. The Adverse Effects of Air Pollution on the Eye: A Review. Int. J. Environ. Res. Public Health 2022, 19, 1186. https://doi.org/10.3390/ijerph19031186
Lin C-C, Chiu C-C, Lee P-Y, Chen K-J, He C-X, Hsu S-K, Cheng K-C. The Adverse Effects of Air Pollution on the Eye: A Review. International Journal of Environmental Research and Public Health. 2022; 19(3):1186. https://doi.org/10.3390/ijerph19031186
Chicago/Turabian StyleLin, Chia-Ching, Chien-Chih Chiu, Po-Yen Lee, Kuo-Jen Chen, Chen-Xi He, Sheng-Kai Hsu, and Kai-Chun Cheng. 2022. "The Adverse Effects of Air Pollution on the Eye: A Review" International Journal of Environmental Research and Public Health 19, no. 3: 1186. https://doi.org/10.3390/ijerph19031186
APA StyleLin, C.-C., Chiu, C.-C., Lee, P.-Y., Chen, K.-J., He, C.-X., Hsu, S.-K., & Cheng, K.-C. (2022). The Adverse Effects of Air Pollution on the Eye: A Review. International Journal of Environmental Research and Public Health, 19(3), 1186. https://doi.org/10.3390/ijerph19031186







