The UP150: A Multifactorial Environmental Intervention to Promote Employee Physical and Mental Well-Being
Abstract
1. Introduction
Literature Review
- Individual level: based on individual consultancies, a dynamic work station (standing and sitting desks) and on the use of treadmill or stairs in active pauses or obliged routes in the office.
- Group level: introducing, in the working daily routine, group active pauses of 10 min, promoting online physical activities, walking groups and social support network.
- Environmental communication level: using printed billboards or personalized online messages (in order to promote healthy behaviors and physical activity), pedometers and informative campaigns.
- Policy and physical environment levels: promoting the creation of safe bicycle parking, the insert of changing rooms in the workplace and health programs.
2. Materials and Methods
2.1. Sample
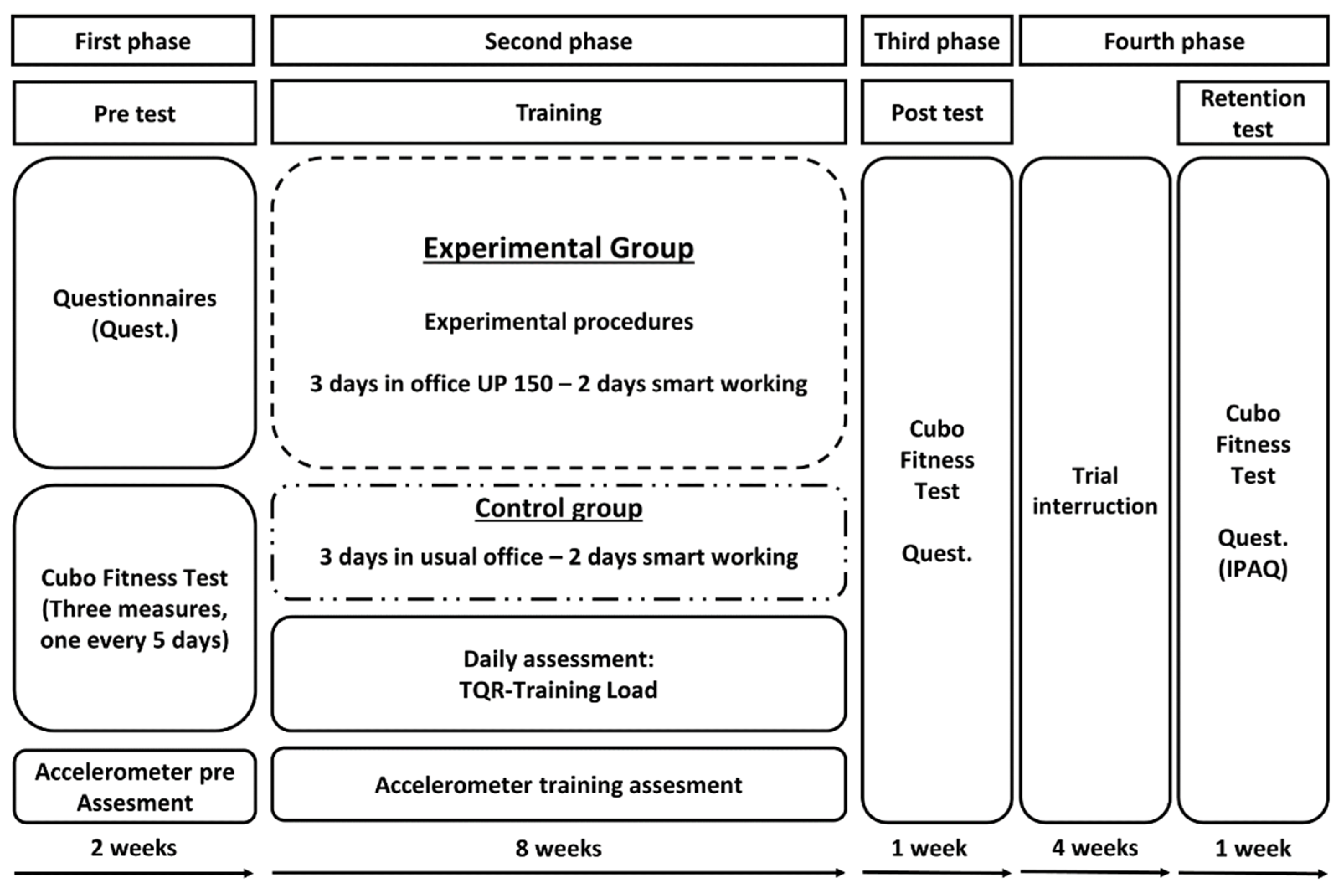
2.2. Protocol
2.3. Assessment
2.4. Procedures
2.4.1. Architectural Changes
2.4.2. App UP150
Pocket Trainer/Training Diary
Physical Activity Score
2.4.3. Wellness Coaches
2.4.4. Self-Determination Methodology
2.5. Measures
2.5.1. Cubo Fitness Test
2.5.2. Questionnaires
International Physical Activity Questionnaire (IPAQ)
NASA Task Load Index (NASA-TLX)
Short Form Healthy Survey (SF-12)
2.5.3. Accelerometers
2.5.4. Total Quality Recovery Scale (TQR)
2.5.5. Training Load
2.6. Statistical Analysis
3. Results
3.1. CFT
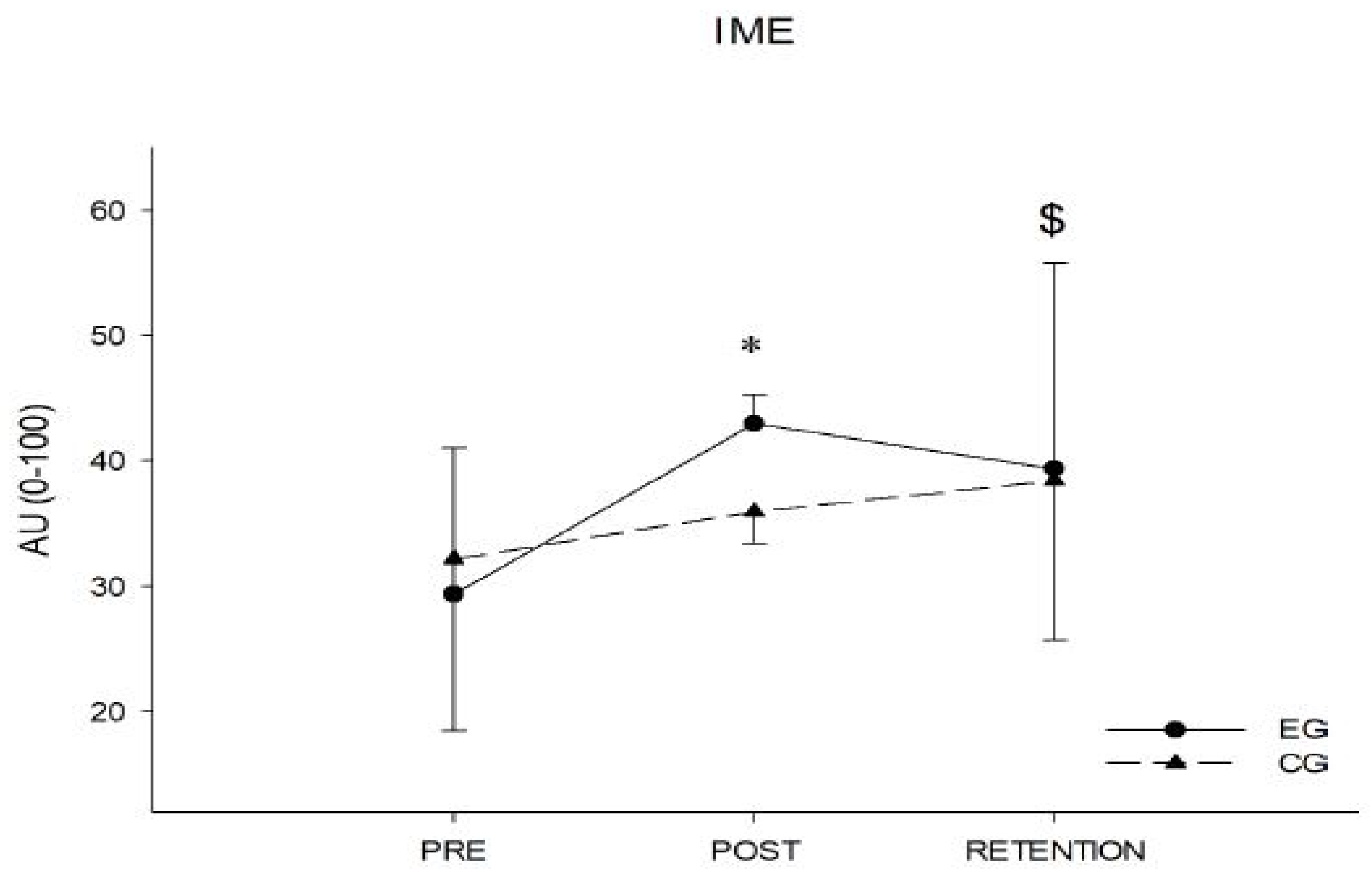
3.1.1. IME
3.1.2. SMT
3.1.3. SRT
3.1.4. SUT
3.1.5. PUT
3.1.6. RT
3.2. Questionnaires
3.2.1. IPAQ
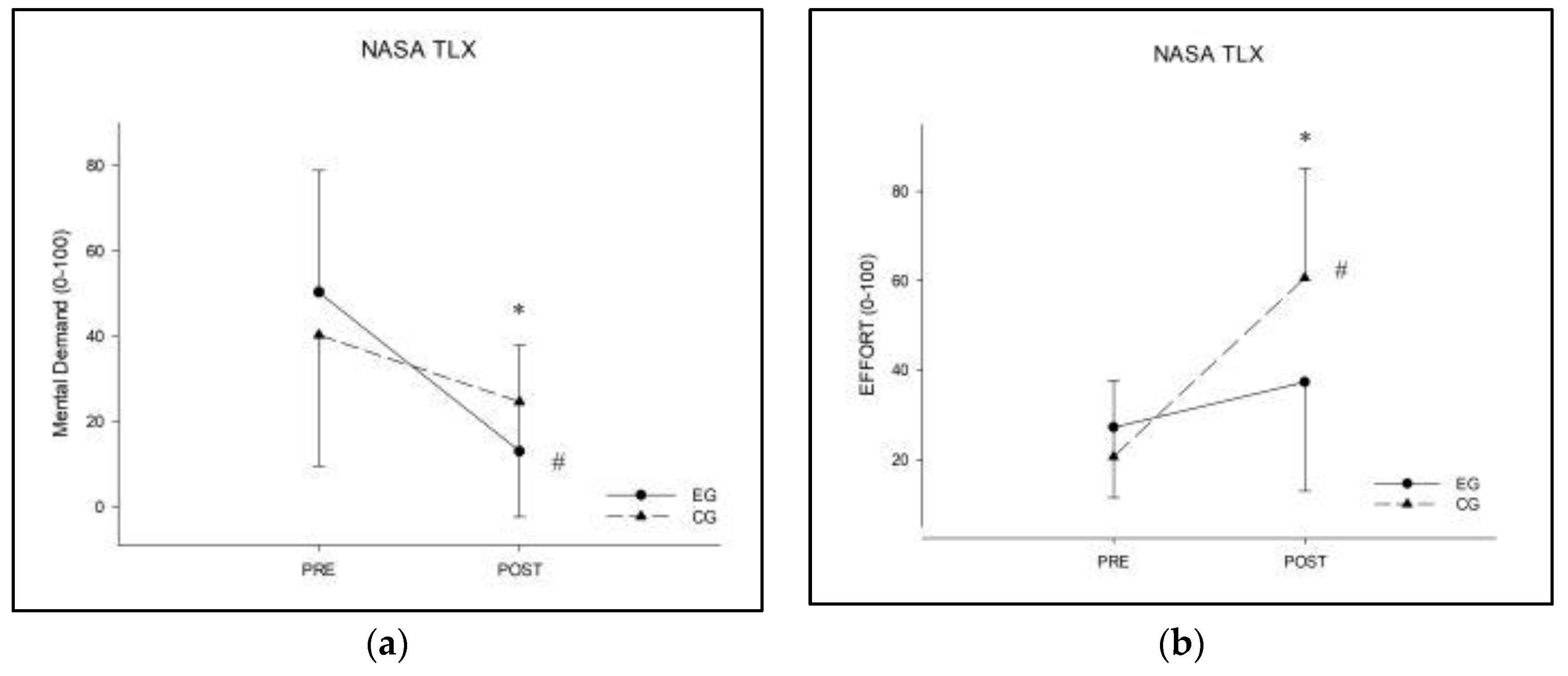
3.2.2. NASA-TLX
3.2.3. SF-12
3.3. Accelerometers
3.4. App UP150 (Experimental Group Procedures)
3.4.1. Pocket Trainer vs. Accelerometer
3.4.2. Training Diary
3.5. TQR
3.6. Training Load
4. Discussion
4.1. Cubo Fitness Test
4.2. Questionnaires
4.3. Accelerometer
4.4. TQR and Training Load
4.5. App UP150
4.6. Potential Limiations
4.7. Practical Applications and Future Perspective
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Acknowledgments
Conflicts of Interest
Appendix A
| Session 1 | Session 2 | Session 3 | ICC | |
|---|---|---|---|---|
| Ruffier (AU) | 14.4 ± 4.9 | 13.6 ± 5.1 | 12.6 ± 4.8 | 0.950 |
| Chair sit and reach (Cm) | −3.4 ± 10.5 | −3.2 ± 12.3 | −0.9 ± 15.0 | 0.944 |
| Shoulder mobility (Cm) | 52.4 ± 9.8 | 51.2 ± 9.5 | 47.3 ± 8.6 | 0.965 |
| Thirty second Seated Sit-Up (AU) | 5.8 ± 3.3 | 7.3 ± 4.0 | 7.3 ± 3.7 | 0.804 |
| Thirty second Push-up (AU) | 3.1 ± 1.7 | 3.1 ± 1.5 | 3.9 ± 1.9 | 0.804 |
| Index of Motor Efficiency (AU) | 27.3 ± 12 | 30.7 ± 13.4 | 34.8 ± 14.1 | 0.957 |
| Pre | Post | Retention | ||
|---|---|---|---|---|
| Ruffier (AU) | EG | 5.3 ± 0.9 | 4.9 ± 1.2 | 4.9 ± 1.1 |
| CG | 4.8 ± 0.7 | 4.8 ± 0.8 | 4.9 ± 0.9 | |
| Thirty second Seated Sit-Up (AU) | EG | 4.2 ± 0.7 | 4.3 ± 0.6 | 4.1 ± 0.8 |
| CG | 4.1 ± 0.6 | 4 ± 1 | 4.2 ± 0.7 | |
| Thirty second Push-up (AU) | EG | 4.8 ± 0.6 | 4.8 ± 1.1 | 4.5 ± 0.8 |
| CG | 4.7 ± 0.6 | 5.4 ± 0.9 | 4.8 ± 0.6 |
| CG | EG | ||
|---|---|---|---|
| Mean ± SD | Mean ± SD | ||
| TQR | Pre | 14.5 ± 1.7 | 13.8 ± 2.2 |
| Week 1 | 14.1 ± 1.4 | 13.7 ± 1.9 | |
| Week 2 | 14.0 ± 1.6 | 14.2 ± 2.0 | |
| Week 3 | 13.8 ± 2.0 | 14.7 ± 1.7 | |
| Week 4 | 13.7 ± 1.4 | 13.8 ± 1.9 | |
| Week 5 | 13.6 ± 1.7 | 14.2 ± 2.4 | |
| Week 6 | 13.5 ± 2.2 | 14.2 ± 2.4 | |
| Week 7 | 13.3 ± 1.7 | 14.2 ± 1.5 | |
| Week 8 | 13.6 ± 1.5 | 14.1 ± 2.3 | |
| Post | 14.0 ± 2.3 | 13.5 ± 2.6 | |
| Retention | 14.7 ± 1.9 | 15.3 ± 2.7 | |
| Training Load | Week 1 | 2980.7 ± 793.5 | 3555.6 ± 1101.7 |
| Week 2 | 3210.2 ± 649.3 | 3313.9 ± 1184.3 | |
| Week 3 | 2906.4 ± 838.1 | 3208.7 ± 815.8 | |
| Week 4 | 3280.6 ± 660.2 | 3298.1 ± 1083.3 | |
| Week 5 | 3189.4 ± 783.5 | 3284.2 ± 773.9 | |
| Week 6 | 3155.3 ± 785.4 | 3469.3 ± 635.6 | |
| Week 7 | 3002.3 ± 879.9 | 3316.7 ± 780.5 | |
| Week 8 | 3337.4 ± 730.2 | 3375.1 ± 878.0 |
References
- WHO. Healthy Workplaces: A Model for Action; WHO: Geneva, Switzerland, 2010; pp. 1–32. [Google Scholar]
- Bolisani, E.; Scarso, E.; Ipsen, C.; Kirchner, K.; Hansen, J.P. Working from home during COVID-19 pandemic: Lessons learned and issues. Manag. Mark. 2020, 15, 458–476. [Google Scholar] [CrossRef]
- Chanana, N.; Sangeeta. Employee engagement practices during COVID-19 lockdown. J. Public Aff. 2020, 21, e2508. [Google Scholar] [CrossRef] [PubMed]
- Sica, R. Dall’employee Experience All’employee Caring: Le Organizzazioni Nell’era Post COVID-19; FrancoAngeli: Milan, Italy, 2021. [Google Scholar]
- Ryan, R.M. The Oxford Handbook of Human Motivation; Oxford University Press USA: New York, NY, USA, 2012; Volume 49. [Google Scholar] [CrossRef]
- Nocon, M.; Hiemann, T.; Müller-Riemenschneider, F.; Thalau, F.; Roll, S.; Willich, S.N. Association of physical activity with all-cause and cardiovascular mortality: A systematic review and meta-analysis. Eur. J. Prev. Cardiol. 2008, 15, 239–246. [Google Scholar] [CrossRef]
- Alves, A.J.; Viana, J.L.; Cavalcante, S.L.; Oliveira, N.L.; Duarte, J.A.; Mota, J.; Oliveira, J.; Ribeiro, F. Physical activity in primary and secondary prevention of cardiovascular disease: Overview updated. World J. Cardiol. 2016, 8, 575. [Google Scholar] [CrossRef] [PubMed]
- Douglas Darden, B.S.; Caroline Richardson, M.D.; Elizabeth AJackson, M. Physical activity and exercise for secondary prevention among patients with cardiovascular disease. Curr. Cardiovasc. Risk Rep. 2013, 7, 411–416. [Google Scholar] [CrossRef] [PubMed]
- Saklayen, M.G. The global epidemic of the metabolic syndrome. Curr. Hypertens. Rep. 2018, 20, 12. [Google Scholar] [CrossRef]
- Warburton, D.E.R.; Bredin, S.S.D. Health benefits of physical activity: A systematic review of current systematic reviews. Curr. Opin. Cardiol. 2017, 32, 541–556. [Google Scholar] [CrossRef]
- Tong, X.; Chen, X.; Zhang, S.; Huang, M.; Shen, X.; Xu, J.; Zou, J. Bone angiogenesis. Biomed. Res. Int. 2019, 2019, 817–897. [Google Scholar]
- Oliveira, J.S.; Pinheiro, M.B.; Fairhall, N.; Walsh, S.; Franks, T.C.; Kwok, W.; Bauman, A.; Sherrington, C. Evidence on physical activity and the prevention of frailty and sarcopenia among older people: A systematic review to inform the world health organization physical activity guidelines. J. Phys. Act. Health 2020, 17, 1247–1258. [Google Scholar] [CrossRef]
- Kilgore, L.; Rippetoe, M. Redefining fitness for health and fitness professionals. J. Exerc. Physiol. Online 2007, 10, 34–39. [Google Scholar]
- Imboden, M.T.; Harber, M.P.; Whaley, M.H.; Finch, W.H.; Bishop, D.L.; Kaminsky, L.A. Cardiorespiratory fitness and mortality in healthy men and women. J. Am. Coll. Cardiol. 2018, 72, 2283–2292. [Google Scholar] [CrossRef]
- Westcott, W.L. Resistance training is medicine: Effects of strength training on health. Curr. Sports Med. Rep. 2012, 11, 209–216. [Google Scholar] [CrossRef]
- Pereira, F.D.; Batista, W.O.; Furtado, H.L.; da Silva, E.B.; Júnior, E.D.D.A. Functional autonomy of physically active and sedentary elderly women: Comparative causal study. Online Braz. J. Nurs. 2011, 10. Available online: http://www.objnursing.uff.br/index.php/nursing/article/view/3309/1157 (accessed on 10 November 2021). [CrossRef]
- Marcos-Pardo, P.J.; Orquin-Castrillón, F.J.; Gea-García, G.M.; Menayo-Antúnez, R.; González-Gálvez, N.; Vale, R.G.d.S.; Martínez-Rodríguez, A. Effects of a moderate-to-high intensity resistance circuit training on fat mass, functional capacity, muscular strength, and quality of life in elderly: A randomized controlled trial. Sci. Rep. 2019, 9, 7830. [Google Scholar] [CrossRef]
- Chiacchiero, M.; Dresely, B.; Silva, U.; DeLosReyes, R.; Vorik, B. The relationship between range of movement, flexibility, and balance in the elderly. Top. Geriatr. Rehabil. 2010, 26, 148–155. [Google Scholar] [CrossRef]
- Mueck-Weymann, M.; Janshoff, G.; Mueck, H. Stretching increases heart rate variability in healthy athletes complaining about limited muscular flexibility. Clin. Auton. Res. 2004, 14, 15–18. [Google Scholar] [CrossRef]
- Montero-Marín, J.; Asún, S.; Estrada-Marcén, N.; Romero, R.; Asún, R. Effectiveness of a stretching program on anxiety levels of workers in a logistic platform: A randomized controlled study. Aten. Primaria 2013, 45, 376–383. [Google Scholar] [CrossRef] [PubMed]
- Hearing, C.M.; Chang, W.C.; Szuhany, K.L.; Deckersbach, T.; Nierenberg, A.A.; Sylvia, L.G. Physical exercise for treatment of mood disorders: A critical. Curr. Behav. Neurosci. Rep. 2016, 3, 350–359. [Google Scholar] [CrossRef]
- Baek, S.-S. Role of exercise on the Brain. J. Exerc. Rehabil. 2016, 12, 380–385. [Google Scholar] [CrossRef]
- Ruegsegger, G.N.; Booth, F.W. Health benefits of exercise. Cold Spring Harb. Perspect. Med. 2018, 8, a029694. [Google Scholar] [CrossRef] [PubMed]
- Anderson, E.; Shivakumar, G. Effects of exercise and physical activity on anxiety. Front. Psychiatry 2013, 4, 10–13. [Google Scholar] [CrossRef]
- Bassett-Gunter, R.; McEwan, D.; Kamarhie, A.; Anderson, E.; Shivakumar, G. Physical activity and body image among men and boys: A meta-analysis. Body Image 2017, 22, 114–128. [Google Scholar] [CrossRef] [PubMed]
- Zelle, D.M.; Klaassen, G.; Van Adrichem, E.; Bakker, S.J.L.; Corpeleijn, E.; Navis, G. Physical inactivity: A risk factor and target for intervention in renal care. Nat. Rev. Nephrol. 2017, 13, 152–168. [Google Scholar] [CrossRef]
- Blair, S.N. Physical inactivity: The biggest public health problem of the 21st Century. Br. J. Sports Med. 2009, 43, 1–2. [Google Scholar] [CrossRef][Green Version]
- World Health Organization. Global Action Plan on Physical Activity 2018–2030: More Active People for a Healthier World; World Health Organization: Geneva, Switzerland, 2019. [Google Scholar]
- Guthold, R.; Ono, T.; Strong, K.L.; Chatterji, S.; Morabia, A. Worldwide variability in physical inactivity. A 51-country survey. Am. J. Prev. Med. 2008, 34, 486–494. [Google Scholar] [CrossRef]
- Ammar, A.; Brach, M.; Trabelsi, K.; Chtourou, H.; Boukhris, O.; Masmoudi, L.; Bouaziz, B.; Bentlage, E.; How, D.; Ahmed, M.; et al. Effects of COVID-19 home confinement on eating behaviour and physical activity: Results of the ECLB-COVID 19 international online survey. Nutrients 2020, 12, 1583. [Google Scholar] [CrossRef]
- Tison, G.H.; Avram, R.; Kuhar, P.; Abreau, S.; Marcus, G.M.; Pletcher, M.J.; Olgin, J.E. Worldwide effect of COVID-19 on physical activity: A descriptive study. Ann. Intern. Med. 2020, 173, 767–770. [Google Scholar] [CrossRef] [PubMed]
- Holtermann, A.; Straker, L.; Lee, I.-M.; Stamatakis, E.; Van Der Beek, A.J. Workplace physical activity promotion: Why so many failures and few successes? The need for new thinking. Br. J. Sports Med. 2021, 55, 650–651. [Google Scholar] [CrossRef]
- Bull, F.C.; Al-Ansari, S.S.; Biddle, S.; Borodulin, K.; Buman, M.P.; Cardon, G.; Carty, C.; Chaput, J.P.; Chastin, S.; Chou, R.; et al. World health organization 2020 guidelines on physical activity and sedentary behaviour. Br. J. Sports Med. 2020, 54, 1451–1462. [Google Scholar] [CrossRef]
- McEachan, R.R.C.; Lawton, R.J.; Jackson, C.; Conner, M.; Meads, D.M.; West, R.M. Testing a workplace physical activity intervention: A cluster randomized controlled trial. Int. J. Behav. Nutr. Phys. Act. 2011, 8, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Grimani, A.; Aboagye, E.; Kwak, L. The effectiveness of workplace nutrition and physical activity interventions in improving productivity, work performance and workability: A systematic review. BMC Public Health 2019, 19, 1676. [Google Scholar] [CrossRef]
- Pronk, N.P. Implementing movement at the workplace: Approaches to increase physical activity and reduce sedentary behavior in the context of work. Prog. Cardiovasc. Dis. 2021, 64, 17–21. [Google Scholar] [CrossRef]
- Ntoumanis, N.; Thørgersen-Ntoumani, C.; Quested, E.; Chatzisarantis, N. Theoretical approaches to physical activity promotion. In Oxford Research Encyclopedia of Psychology; Oxford University Press: Oxford, UK, 2018. [Google Scholar]
- Bardus, M.; Blake, H.; Lloyd, S.; Suggs, L.S. Reasons for participating and not participating in a E-health workplace physical activity intervention a qualitative analysis. Int. J. Work. Health Manag. 2014, 7, 229–246. [Google Scholar] [CrossRef]
- Deci, E.L.; Ryan, R.M. Self-determination theory. Handb. Theor. Soc. Psychol. 2012, 1, 416–436. [Google Scholar]
- Gagné, M. (Ed.) The Oxford Handbook of Work Engagement and Self-Determination Theory; Oxford University Press: New York, NY, USA, 2014; pp. 50–71. [Google Scholar]
- Deci, E.L.; Olafsen, A.H.; Ryan, R.M. Self-determination theory in work organizations: The state of a science. Annu. Rev. Organ. Psychol. Organ. Behav. 2017, 4, 19–43. [Google Scholar] [CrossRef]
- Teixeira, P.J.; Carraça, E.V.; Markland, D.; Silva, M.N.; Ryan, R.M. Exercise, physical activity, and self-determination theory: A systematic review. Int. J. Behav. Nutr. Phys. Act. 2012, 9, 78. [Google Scholar] [CrossRef]
- Tosi, H.L.; Locke, E.A.; Latham, G.P. A theory of goal setting and task performance. Acad. Manag. Rev. 1991, 16, 480. [Google Scholar] [CrossRef]
- Brehm, J.W. The intensity of motivation. Ann. Rev. Psychol. 1989, 40, 109–131. [Google Scholar] [CrossRef]
- Wright, R.A. Refining the prediction of effort: Brehm’s distinction between potential motivation and motivation intensity. Soc. Personal. Psychol. Compass 2008, 2, 682–701. [Google Scholar] [CrossRef]
- Maria, K.-M.; George, M. Workplace design: Conceptualizing and measuring workplace characteristics for motivation. J. Organ. Eff. People Perform. 2015, 2, 242–243. [Google Scholar]
- Sugiyama, T.; Hadgraft, N.T.; Healy, G.N.; Owen, N.; Dunstan, D.W. Perceived availability of office shared spaces and workplace sitting: Moderation by organizational norms and behavioral autonomy. Environ. Behav. 2019, 51, 856–878. [Google Scholar] [CrossRef]
- Le Deist, F.D.; Winterton, J. What is competence? Hum. Resour. Dev. Int. 2005, 8, 27–46. [Google Scholar] [CrossRef]
- Butterworth, S.; Linden, A.; McClay, W.; Leo, M.C. Effect of motivational interviewing-based health coaching on employees’ physical and mental health status. J. Occup. Health Psychol. 2006, 11, 358–365. [Google Scholar] [CrossRef] [PubMed]
- Baicker, K.; Cutler, D.; Song, Z. Workplace wellness programs can generate savings. Health Aff. 2010, 29, 304–311. [Google Scholar] [CrossRef] [PubMed]
- Blackwell, J.; Collins, M.; Scribner, C.; Guillen, J.; Moses, K.; Gregory-Mercado, K. Health and wellness coaching implemented by trainees: Impact in worksite wellness. Glob. Adv. Health Med. 2019, 8, 2164956119831226. [Google Scholar] [CrossRef] [PubMed]
- Carlsson, C.; Walden, P. Digital Support to Guide Physical Activity-Augmented Daily Routines for Young Elderly. BLED 2019 Proceedings (Online). 2019. Available online: https://aisel.aisnet.org/bled2019/20/ (accessed on 10 November 2021).
- Commissaris, D.A.; Huysmans, M.A.; Mathiassen, S.E.; Srinivasan, D.; Koppes, L.L.; Hendriksen, I.J. Interventions to reduce sedentary behavior and increase physical activity during productive work: A systematic review. Scand. J. Work. Environ. Health 2016, 42, 181–191. [Google Scholar] [CrossRef]
- Maylor, B.D.; Edwardson, C.L.; Zakrzewski-Fruer, J.K.; Champion, R.B.; Bailey, D.P. Efficacy of a multicomponent intervention to reduce workplace sitting time in office workers a cluster randomized controlled trial. J. Occup. Environ. Med. 2018, 60, 787–795. [Google Scholar] [CrossRef]
- Nooijen, C.F.; Blom, V.; Ekblom, Ö.; Ekblom, M.M.; Kallings, L.V. Improving office workers mental health and cognition a 3-Arm cluster randomized controlled trial targeting physical activity and sedentary behavior in multicomponent interventions. BMC Public Health 2019, 19, 1–10. [Google Scholar] [CrossRef]
- Rikli, R.E.; Jones, C.J. Senior Fitness Test Manual; Human Kinetics: Champaign, IL, USA, 2013. [Google Scholar]
- Manganelli, L.; Thibault-Landry, A.; Forest, J.; Carpentier, J. Self-determination theory can help you generate performance and well-being in the workplace: A review of the literature. Adv. Dev. Hum. Resour. 2018, 20, 227–240. [Google Scholar] [CrossRef]
- Invernizzi, P.L.; Signorini, G.; Bosio, A.; Scurati, R. Children over “-Enty,-Rty,-Fty”: Gamification and autonomy as an environmental education leitmotif for “children of all ages” using a new workplace narrative. J. Phys. Educ. Sport 2021, 21, 585–591. [Google Scholar] [CrossRef]
- FitzGerald, S.J.; Barlow, C.E.; Kampert, J.B.; Morrow, J.R.; Jackson, A.W.; Blair, S.N. Muscular fitness and all-cause mortality: Prospective observations. J. Phys. Act. Health 2004, 1, 7–18. [Google Scholar] [CrossRef]
- Micheo, W.; Baerga, L.; Miranda, G. Basic principles regarding strength, flexibility, and stability exercises. Pm&r 2012, 4, 805–811. [Google Scholar] [CrossRef]
- Lee, D.C.; Artero, E.G.; Sui, X.; Blair, S.N. Mortality trends in the general population: The importance of cardiorespiratory fitness. J. Psychopharmacol. 2010, 24 (Suppl. 4), 27–35. [Google Scholar] [CrossRef] [PubMed]
- Al-Mallah, M.H.; Sakr, S.; Al-Qunaibet, A. Cardiorespiratory fitness and cardiovascular disease prevention: An update. Curr. Atheroscler. Rep. 2018, 20, 1. [Google Scholar] [CrossRef]
- Lopez, A.D.; Mathers, C.D.; Ezzati, M.; Jamison, D.T.; Murray, C.J. Global and regional burden of disease and risk factors, 2001: Systematic analysis of population health data. Lancet 2006, 367, 1747–1757. [Google Scholar] [CrossRef]
- World Health Organization. The World Health Report 2002: Reducing Risks, Promoting Healthy Life; World Health Organization: Geneva, Switzerland, 2002. [Google Scholar]
- Katzmarzyk, P.T.; Craig, C.L. Musculoskeletal fitness and risk of mortality. Med. Sci. Sports Exerc. 2002, 34, 740–744. [Google Scholar] [CrossRef]
- Cunha AC, V.; Burke, T.N.; França FJ, R.; Marques, A.P. Effect of global posture reeducation and of static stretching on pain, range of motion, and quality of life in women with chronic neck pain: A randomized clinical trial. Clinics 2008, 63, 763–770. [Google Scholar] [CrossRef]
- Papini, G.; Bonomi, A.G.; Stut, W.; Kraal, J.J.; Kemps, H.M.C.; Sartor, F. Proof of concept of a 45-second cardiorespiratory fitness self-test for coronary artery disease patients based on accelerometry. PLoS ONE 2017, 12, e0183740. [Google Scholar] [CrossRef] [PubMed]
- Crotti, M.; Bosio, A.; Invernizzi, P.L. Validity and reliability of submaximal fitness tests based on perceptual variables. J. Sports Med. Phys. Fitness 2018, 58, 555–562. [Google Scholar] [CrossRef] [PubMed]
- Invernizzi, P.L.; Signorini, G.; Bosio, A.; Raiola, G.; Scurati, R. Validity and reliability of self-perception-based submaximal fitness tests in young adult females: An educational perspective. Sustainability 2020, 12, 2265. [Google Scholar] [CrossRef]
- Harre, D. Teoria Dell’allenamento; SSS: Rome, Italy, 1997; Volume 501, ISBN 8883130995. [Google Scholar]
- Freitas, S.R.; Vaz, J.R.; Gomes, L.; Silvestre, R.; Hilário, E.; Cordeiro, N.; Carnide, F.; Pezarat-Correia, P.; Mil-Homens, P. A new tool to assess the perception of stretching intensity. J. Strength Cond. Res. 2015, 29, 2666–2678. [Google Scholar] [CrossRef]
- Jones, C.J.; Rikli, R.E.; Max, J.; Noffal, G. Cluarterly for exercise and sport a the reliability and validity of a chair sit-and-reach test as a measure of hamstring flexibility in older adults. Phys. Educ. Recreat. Danc. 1998, 69, 338–343. [Google Scholar]
- Craig, C.L.; Marshall, A.L.; Sjöström, M.; Bauman, A.E.; Booth, M.L.; Ainsworth, B.E.; Pratt, M.; Ekelund, U.; Yngve, A.; Sallis, J.F.; et al. International physical activity questionnaire: 12-country reliability and validity. Med. Sci. Sports Exerc. 2003, 35, 1381–1395. [Google Scholar] [CrossRef] [PubMed]
- Hart, S.G.; Staveland, L.E. Development of NASA-TLX (Task Load Index): Results of empirical and theoretical research. Adv. Psychol. 1988, 52, 139–183. [Google Scholar] [CrossRef]
- Hart, S.G. NASA-task load index (NASA-TLX); 20 years later. Proc. Hum. Factors Ergon. Soc. 2006, 50, 904–908. [Google Scholar] [CrossRef]
- Hoonakker, P.; Carayon, P.; Gurses, A.P.; Brown, R.; Khunlertkit, A.; McGuire, K.; Walker, J.M. Measuring workload of ICU nurses with a questionnaire survey: The NASA task load index (TLX). IIE Trans. Healthc. Syst. Eng. 2011, 1, 131–143. [Google Scholar] [CrossRef] [PubMed]
- Kodraliu, G.; Mosconi, P.; Groth, N.; Carmosino, G.; Perilli, A.; Gianicolo, E.A.; Rossi, C.; Apolone, G. Subjective health status assessment: Evaluation of the italian version of the sf-12 health survey. Results from the MiOS project. J. Epidemiol. Biostat. 2001, 6, 305–316. [Google Scholar] [CrossRef] [PubMed]
- Arvidsson, D.; Fridolfsson, J.; Buck, C.; Ekblom, Ö.; Ekblom-Bak, E.; Lissner, L.; Hunsberger, M.; Börjesson, M. Reexamination of accelerometer calibration with energy expenditure as criterion: VO2net instead of MET for age-equivalent physical activity intensity. Sensors 2019, 19, 3377. [Google Scholar] [CrossRef]
- Doherty, A.; Jackson, D.; Hammerla, N.; Plötz, T.; Olivier, P.; Granat, M.H.; White, T.; Van Hees, V.T.; Trenell, M.I.; Owen, C.G.; et al. Large scale population assessment of physical activity using wrist worn accelerometers: The UK biobank study. PLoS ONE 2017, 12, e0169649. [Google Scholar] [CrossRef]
- Dieu, O.; Mikulovic, J.; Fardy, P.S.; Bui-Xuan, G.; Béghin, L.; Vanhelst, J. Physical activity using wrist-worn accelerometers: Comparison of dominant and non-dominant Wrist. Clin. Physiol. Funct. Imaging 2017, 37, 525–529. [Google Scholar] [CrossRef]
- Kenttä, G.; Hassmén, P. Overtraining and recovery. Sport. Med. 1998, 26, 1–16. [Google Scholar] [CrossRef]
- Foster, C.; Daines, E.; Hector, L.; Snyder, A.C.; Welsh, R. Athletic performance in relation to training load. Wis. Med. J. 1996, 95, 370–374. [Google Scholar] [PubMed]
- Bakeman, R. Recommended effect size statistics for repeated measures designs. Behav. Res. Methods 2005, 37, 379–384. [Google Scholar] [CrossRef]
- Cohen, J. Statistical Power Analysis for the Behavioral Sciences; Academic Press: Cambridge, MA, USA, 2013. [Google Scholar]
- Santos, E.; Rhea, M.; Simão, R.; Dias, I.; De Salles, B.F.; Novaes, J.; Leite, T.; Blair, J.C.; Bunker, D.J. Influence of moderately intense strength training on flexibility in sedentary young women. J. Strength Cond. Res. 2010, 24, 3144–3149. [Google Scholar] [CrossRef] [PubMed]
- Childs, J.D.; Teyhen, D.S.; Benedict, T.M.; Morris, J.B.; Fortenberry, A.D.; McQueen, R.M.; Preston, J.B.; Wright, A.C.; Dugan, J.L.; George, S.Z. Effects of Sit-up training versus core stabilization exercises on sit-up performance. Med. Sci. Sports Exerc. 2009, 41, 2072–2083. [Google Scholar] [CrossRef]
- Baxter, R.E.; Moore, J.H.; Pendergrass, T.L.; Crowder, T.A.; Lynch, S. Improvement in sit-up performance associated with 2 different training regimens. J. Orthop. Sport. Phys. Ther. 2003, 33, 40–47. [Google Scholar] [CrossRef] [PubMed]
- Shariat, A.; Ghannadi, S.; Anastasio, A.T.; Rostad, M.; Cleland, J.A. Novel stretching and strength-building exercise recommendations for computer-based workers during the COVID-19 quarantine. Work 2020, 66, 739–749. [Google Scholar] [CrossRef]
- Boulé, N.G.; Kenny, G.P.; Haddad, E.; Wells, G.A.; Sigal, R.J. Meta-analysis of the effect of structured exercise training on cardiorespiratory fitness in type 2 diabetes mellitus. Diabetologia 2003, 46, 1071–1081. [Google Scholar] [CrossRef]
- Branch, J.D.; Pate, R.R.; Bourque, S.P. Moderate intensity exercise training improves cardiorespiratory fitness in women. J. Women’s Health Gender-Based Med. 2000, 9, 65–73. [Google Scholar] [CrossRef]
- Dunn, A.L.; Marcus, B.H.; Kampert, J.B.; Garcia, M.E.; Kohl, H.W.; Blair, S.N. Comparison of lifestyle and structured interventions to increase physical activity and cardiorespiratory fitness: A randomized trial. J. Am. Med. Assoc. 1999, 281, 327–334. [Google Scholar] [CrossRef] [PubMed]
- Chen, H.; Chung, Y.; Chen, Y.; Ho, S.; Wu, H. Effects of different types of exercise on body composition, muscle strength, and IGF-1 in the elderly with sarcopenic obesity. J. Am. Geriatr. Soc. 2017, 65, 827–832. [Google Scholar] [CrossRef] [PubMed]
- Kopp, M.S.; Stauder, A.; Purebl, G.; Janszky, I.; Skrabski, Á. Work stress and mental health in a changing society. Eur. J. Public Health 2008, 18, 238–244. [Google Scholar] [CrossRef]
- Taelman, J.; Vandeput, S.; Spaepen, A.; Van Huffel, S. Influence of mental stress on heart rate and heart rate variability. IFMBE Proc. 2008, 22, 1366–1369. [Google Scholar] [CrossRef]
- Wahlström, J.; Lindegård, A.; Ahlborg, G.; Ekman, A.; Hagberg, M. Perceived muscular tension, emotional stress, psychological demands and physical load during VDU work. Int. Arch. Occup. Environ. Health 2003, 76, 584–590. [Google Scholar] [CrossRef]
- Wandel, M.; Roos, G. Work, food and physical activity. A qualitative study of coping strategies among men in three occupations. Appetite 2005, 44, 93–102. [Google Scholar] [CrossRef] [PubMed]
- Faulkner, G.; Rhodes, R.E.; Vanderloo, L.M.; Chulak-Bozer, T.; O’Reilly, N.; Ferguson, L.; Spence, J.C. Physical activity as a coping strategy for mental health due to the COVID-19 virus: A potential disconnect among canadian adults? Front. Commun. 2020, 5, 74. [Google Scholar] [CrossRef]
- Dyrstad, S.M.; Hansen, B.H.; Holme, I.M.; Anderssen, S.A. Comparison of self-reported versus accelerometer-measured physical activity. Med. Sci. Sports Exerc. 2013, 46, 99–106. [Google Scholar] [CrossRef]
- Marcora, S.M. Effort: Perception of. In Encyclopedia of Perception; Bruce, G.E., Ed.; Sage: Los Angeles, CA, USA, 2010; pp. 380–383. ISBN 978-1-4129-4081-8. [Google Scholar]
- Lindberg, C.M.; Srinivasan, K.; Gilligan, B.; Razjouyan, J.; Lee, H.; Najafi, B.; Mehl, M.R.; Currim, F.; Ram, S.; Lunden, M.M. Effects of office workstation type on physical activity and stress. Occup. Environ. Med. 2018, 75, 689–695. [Google Scholar] [CrossRef] [PubMed]
- Beauchemin, J.; Lee, M.Y. Solution-focused. Wellness coaching. J. Solut. Focus. Pract. 2014, 1, 6. [Google Scholar]
| Pre | Post | Retention | Delta 1 | Delta 2 | ||
|---|---|---|---|---|---|---|
| Ruffier (AU) | EG | 13.1 ± 4.5 | 10.2 ± 16.2 # | 9.9 ± 3.1 | 3.4 ± 2.2 | 0.3 ± 2.4 |
| CG | 14.0 ± 5.2 | 11.2 ± 10.8 # | 11.0 ± 3.6 | 2.8 ± 4 | 0.4 ± 3.6 | |
| 30 s Push-up (AU) | EG | 3.5 ± 1.9 | 6.6 ± 11.6 # | 5.41 ± 3.1 | 3.1 ± 2.9 | 0.6 ± 3.1 |
| CG | 3.2 ± 1.1 | 6.1 ± 10.0 # | 5.7 ± 2.4 | 2.9 ± 2.5 | 0.4 ± 2.6 | |
| 30 s Seated Sit-Up (AU) | EG | 6.3 ± 3.2 | 9.4 ± 3.1 # | 7.8 ± 4.2 | 3.3 ± 3.2 * | 0.3 ± 2.6 |
| CG | 7.0 ± 3.4 | 8.8 ± 4.0 | 9.6 ± 3.7 | 1.0 ± 2.4 | 1.0 ± 3.2 | |
| Shoulder mobility (cm) | EG | 52.4 ± 9.8 | 44.0 ± 4.7 # | 46.8 ± 9.3 | 7.6 ± 5.8 * | 2.2 ± 4.7 * |
| CG | 49.3 ± 8.4 | 47.0 ± 3.0 | 47.5 ± 8.4 | 0.5 ± 3.7 | 1.2 ± 3.6 | |
| Chair sit and reach (cm) | EG | −5.0 ± 13.0 | −0.8 ± 10.0 # | −2.5 ± 13.6 | 5.0 ± 7.2 * | 4.6 ± 5.4 * |
| CG | −0.4 ± 10.9 | 1.4 ± 11.6 | −2.2 ± 12.2 | 1.2 ± 3.6 | 0.5 ± 3.7 | |
| Index of Motor Efficiency (AU) | EG | 29.4 ± 13.7 | 43.0 ± 2.3 # | 39.4 ± 16.4 | 14.4 ± 8.7 * | 3.8 ± 8.4 |
| CG | 32.2 ± 11.7 | 36.0 ± 2.6 | 37.4 ± 12.5 | 3.1 ± 10.5 | 3.0 ± 10.1 |
| Pre | Post | Retention | Delta 1 | Delta 2 | |||
|---|---|---|---|---|---|---|---|
| IPAQ | Vigorous Activity (Met) | EG | 822.9 ± 1182.3 | 802 ± 1047.1 | 1294.1 ± 1729.8 | 34.0 ± 871.7 | 501.2 ± 1290.7 |
| CG | 830.5 ± 789.8 | 1302.2 ± 1060.5 | 1793.7 ± 1854.5 | 377.8 ± 1311.6 | 562.4 ± 2150.7 | ||
| Moderate activity (Met) | EG | 701.0 ± 1105.8 | 859.2 ± 1320.6 | 828.2 ± 1512.7 | 147.2 ± 706.1 | 140.0 ± 1905.2 | |
| CG | 634.3 ± 795.2 | 377.8 ± 261.8 | 818.9 ± 966.1 | 238.9 ± 819.4 | 430.6 ± 1033.4 | ||
| Walking activity (Met) | EG | 1604.6 ± 3145.3 | 1672.4 ± 3788.3 | 657.5 ± 720.4 | 40.0 ± 1235.5 | 1116.5 ± 3486.7 * | |
| CG | 754.9 ± 720.4 | 815.4 ± 565.3 | 1211 ± 1086.7 | 12.8 ± 905.1 | 437.2 ± 1017.3 | ||
| Sedentary activity during working day (Met) | EG | 506.8 ± 166.1 | 432.5 ± 188.0 | 411.8 ± 228.5 | 72.5 ± 154.8 | 15.9 ± 156.8 | |
| CG | 488.1 ± 150.3 | 450.0 ± 137.4 | 429.5 ± 186.6 | 42.8 ± 168.6 | 28.2 ± 120.6 | ||
| Sedentary activity during weekend (Met) | EG | 184.3 ± 103.7 | 153.3 ± 122.0 | 144.7 ± 108.9 | 34.3 ± 119.1 | 6.2 ± 123.3 | |
| CG | 233.8 ± 188.1 | 216.7 ± 204.7 | 162.1 ± 105.3 | 29.4 ± 284.4 | 63.5 ± 188.2 | ||
| Total (Met) | EG | 3128.5 ± 4781.4 | 3333.6 ± 5250.0 | 2779.8 ± 3332.9 * | 221.2 ± 1785.4 | 755.3 ± 4721.0 | |
| CG | 2219.6 ± 1708.1 | 2495.4 ± 1301.2 | 3823.6 ± 2574.1 | 126.1 ± 1711.7 | 1430.1 ± 3023.0 |
| Pre | Post | Delta 1 | |||
|---|---|---|---|---|---|
| NASA-TLX | Mental Demand | EG | 50.3 ± 28.5 | 13.0 ± 24.9 # * | 36.1 ± 44.5 |
| CG | 40.3 ± 30.7 | 24.6 ± 27.0 | 15.9 ± 41.1 | ||
| Physical Demand | EG | 8.6 ± 16.6 | 24.3 ± 21.5 # | 15.3 ± 25.0 | |
| CG | 5.7 ± 9.0 | 19.1 ± 20.9 # | 15.6 ± 18.8 | ||
| Temporal Demand | EG | 44.7 ± 27.3 | 55.5 ± 20.0 | 11.2 ± 32.6 | |
| CG | 45.2 ± 25.5 | 49.2 ± 23.8 | 7.1 ± 29.1 | ||
| Performance | EG | 22.0 ± 13.7 * | 19.0 ± 21.1 | 2.8 ± 23.7 * | |
| CG | 32.8 ± 18.3 | 9.7 ± 12.7 # | 24.9 ± 19.1 | ||
| Effort | EG | 27.2 ± 15.7 | 37.3 ± 24.4 * | 9.0 ± 30.4 * | |
| CG | 20.6 ± 17.1 | 60.6 ± 24.6 # | 43.4 ± 29.9 | ||
| Frustration | EG | 29.7 ± 35.2 | 34.8 ± 24.7 | 4.1 ± 35.5 | |
| CG | 27.2 ± 33.1 | 34.7 ± 23.5 | 11.2 ± 34.4 | ||
| Weighted sum | EG | 12.2 ± 4.1 | 12.3 ± 2.8 | 15.3 ± 25 | |
| CG | 11.5 ± 4.3 | 13.2 ± 3.9 | 15.6 ± 18.8 | ||
| SF-12 | PCS12 | EG | 53.5 ± 7.2 | 55.3 ± 5.2 | 1.8 ± 6.3 |
| CG | 56.1 ± 5.4 | 54.7 ± 5.7 | 1.4 ± 7.0 | ||
| MCS12 | EG | 37.5 ± 9.8 | 46.6 ± 8.2 # | 9.1 ± 8.0 * | |
| CG | 39.2 ± 9.0 | 42.3 ± 12.2 # | 3.1 ± 13.5 |
| CG | EG | ||
|---|---|---|---|
| Intensity | Mean ± SD | Mean ± SD | |
| Sedentary minutes | Detection 1 | 2334.5 ± 321.4 | 2442.2 ± 252.6 |
| Detection 2 | 2353.5 ± 165.0 | 2309.2 ± 331.6 | |
| Detection 3 | 2317.3 ± 294.7 | 2343.9 ± 262.4 | |
| Detection 4 | 2382.3 ± 272.5 | 2332.4 ± 269.6 | |
| Light minutes | Detection 1 | 209.0 ± 55.0 | 177.2 ± 51.8 |
| Detection 2 | 200.3 ± 56.3 | 189.6 ± 55.7 | |
| Detection 3 | 212.1 ± 55.8 | 202.1 ± 65.9 | |
| Detection 4 | 221.8 ± 46.8 | 208 ± 51.5 | |
| Moderate minutes | Detection 1 | 300.9 ± 139.0 | 307.8 ± 176.7 |
| Detection 2 | 281.7 ± 171.6 | 355.4 ± 124.8 #* | |
| Detection 3 | 345.9 ± 200.6 | 392.9 ± 153.7 #§ | |
| Detection 4 | 314.7 ± 117.3 | 425.4 ± 175.9 #§ | |
| Vigorous minutes | Detection 1 | 10.3 ± 20.3 | 6.1 ± 13.1 |
| Detection 2 | 6.6 ± 13.6 | 3.7 ± 5.0 | |
| Detection 3 | 8.1 ± 12.1 | 4.5 ± 6.5 | |
| Detection 4 | 7.3 ± 8.8 | 4.2 ± 5.5 |
| Accelerometer | PT | EG—Accelerometer | EG—PT | |
|---|---|---|---|---|
| Intensity | Mean ± SD | Mean ± SD | ||
| Light minutes | Detection 2 | Detection 1 | 189.6 ± 55.7 | 326.9 ± 248.1 * |
| Detection 3 | Detection 2 | 202.1 ± 65.9 | 342.1 ± 175.7 * | |
| Detection 4 | Detection 3 | 208 ± 51.5 | 316.8 ± 199 * | |
| Moderate minutes | Detection 2 | Detection 1 | 355.4 ± 124.8 | 127.9 ± 139.8 * |
| Detection 3 | Detection 2 | 392.9 ± 153.7 | 118.8 ± 82.3 * | |
| Detection 4 | Detection 3 | 425.4 ± 175.9 | 74.9 ± 80.9 * | |
| Vigorous minutes | Detection 2 | Detection 1 | 3.7 ± 5.0 | 15 ± 21.9 |
| Detection 3 | Detection 2 | 4.5 ± 6.5 | 25 ± 50.4 | |
| Detection 4 | Detection 3 | 4.2 ± 5.5 | 27.4 ± 72.3 |
| App UP150—Training Diary (Mean ± SD) | |||
|---|---|---|---|
| Total | Inside Office | Outside Office | |
| Cardiorespiratory Fitness (Min) | 314.9 ± 103.6 | 99.6 ± 59.0 | 214.8 ± 110.5 * |
| Muscular Fitness (Min) | 35.1 ± 52.8 | 10.2 ± 7.8 | 25.0 ± 52.2 |
| Flexibility Fitness (Min) | 8.3 ± 8.5 | 4.9 ± 4.2 | 3.4 ± 5.4 |
| Combined Fitness (Min) | 35.2 ± 46.7 | 8.9 ± 7.0 | 26.3 ± 44.2 |
| Total (Min) | 394.8 ± 132.6 | 124.2 ± 65.6 | 269.9 ± 149.4 * |
| Cardiorespiratory Fitness (Points) | 346.8 ± 103.7 | 112.3 ± 61.8 | 233.9 ± 115.4 * |
| Muscular Fitness (Points) | 47.9 ± 70.2 | 13.0 ± 9.7 | 34.8 ± 70.3 |
| Flexibility Fitness (Points) | 9.2 ± 9.4 | 5.5 ± 4.8 | 3.7 ± 6.0 |
| Combined Fitness (Points) | 62.1 ± 73.4 | 12.7 ± 12.7 | 49.4 ± 68.8 * |
| Total score (Points) | 467.3 ± 149.9 | 144.2 ± 74.4 | 322.3 ± 175.6 * |
| Target score (Points) | 191.9 ± 29.7 | ||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Invernizzi, P.L.; Signorini, G.; Scurati, R.; Michielon, G.; Benedini, S.; Bosio, A.; Staiano, W. The UP150: A Multifactorial Environmental Intervention to Promote Employee Physical and Mental Well-Being. Int. J. Environ. Res. Public Health 2022, 19, 1175. https://doi.org/10.3390/ijerph19031175
Invernizzi PL, Signorini G, Scurati R, Michielon G, Benedini S, Bosio A, Staiano W. The UP150: A Multifactorial Environmental Intervention to Promote Employee Physical and Mental Well-Being. International Journal of Environmental Research and Public Health. 2022; 19(3):1175. https://doi.org/10.3390/ijerph19031175
Chicago/Turabian StyleInvernizzi, Pietro Luigi, Gabriele Signorini, Raffaele Scurati, Giovanni Michielon, Stefano Benedini, Andrea Bosio, and Walter Staiano. 2022. "The UP150: A Multifactorial Environmental Intervention to Promote Employee Physical and Mental Well-Being" International Journal of Environmental Research and Public Health 19, no. 3: 1175. https://doi.org/10.3390/ijerph19031175
APA StyleInvernizzi, P. L., Signorini, G., Scurati, R., Michielon, G., Benedini, S., Bosio, A., & Staiano, W. (2022). The UP150: A Multifactorial Environmental Intervention to Promote Employee Physical and Mental Well-Being. International Journal of Environmental Research and Public Health, 19(3), 1175. https://doi.org/10.3390/ijerph19031175







