Gender Differences in Unhealthy Lifestyle Behaviors among Adults with Diabetes in the United States between 1999 and 2018
Abstract
1. Introduction
2. Methods
2.1. Study Population
2.2. Definitions
2.3. Statistical Analyses
3. Results
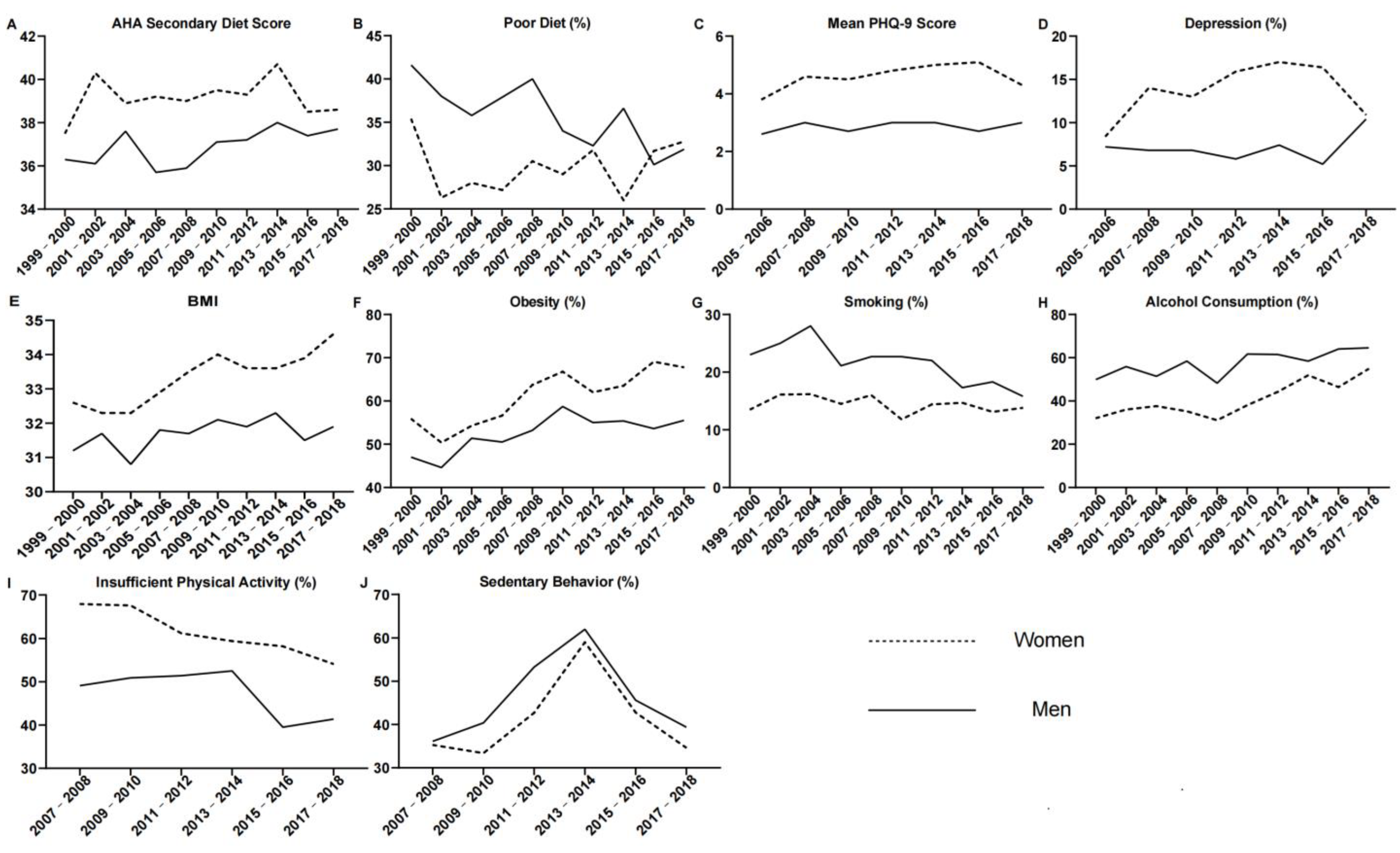
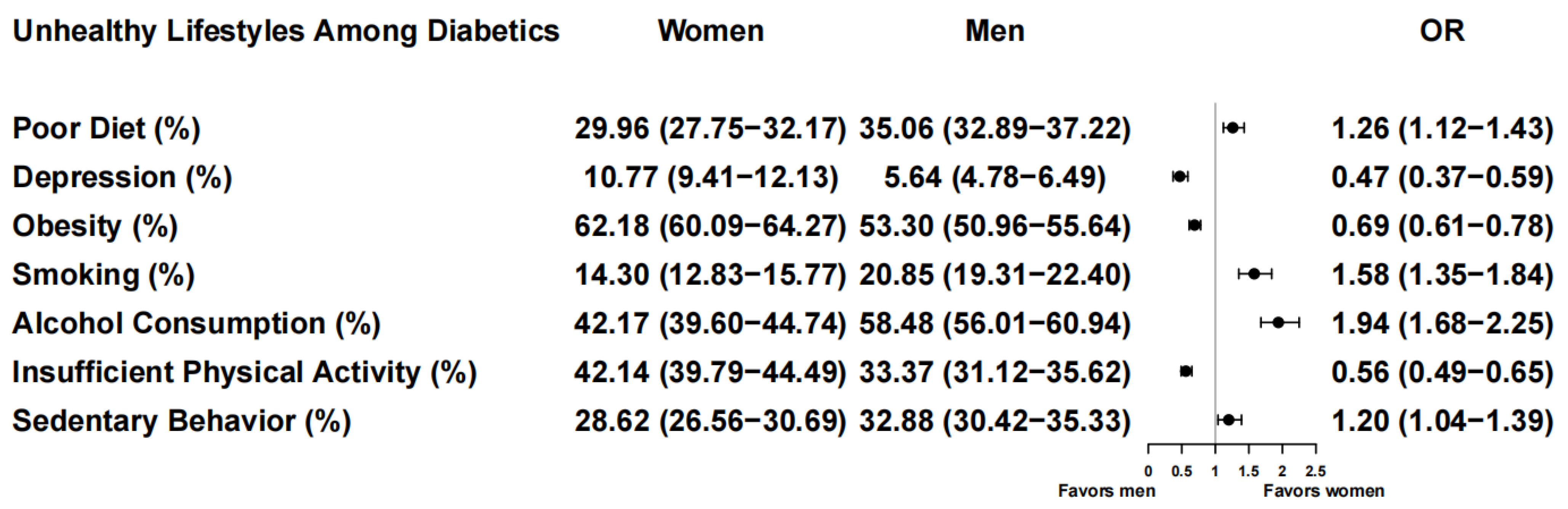
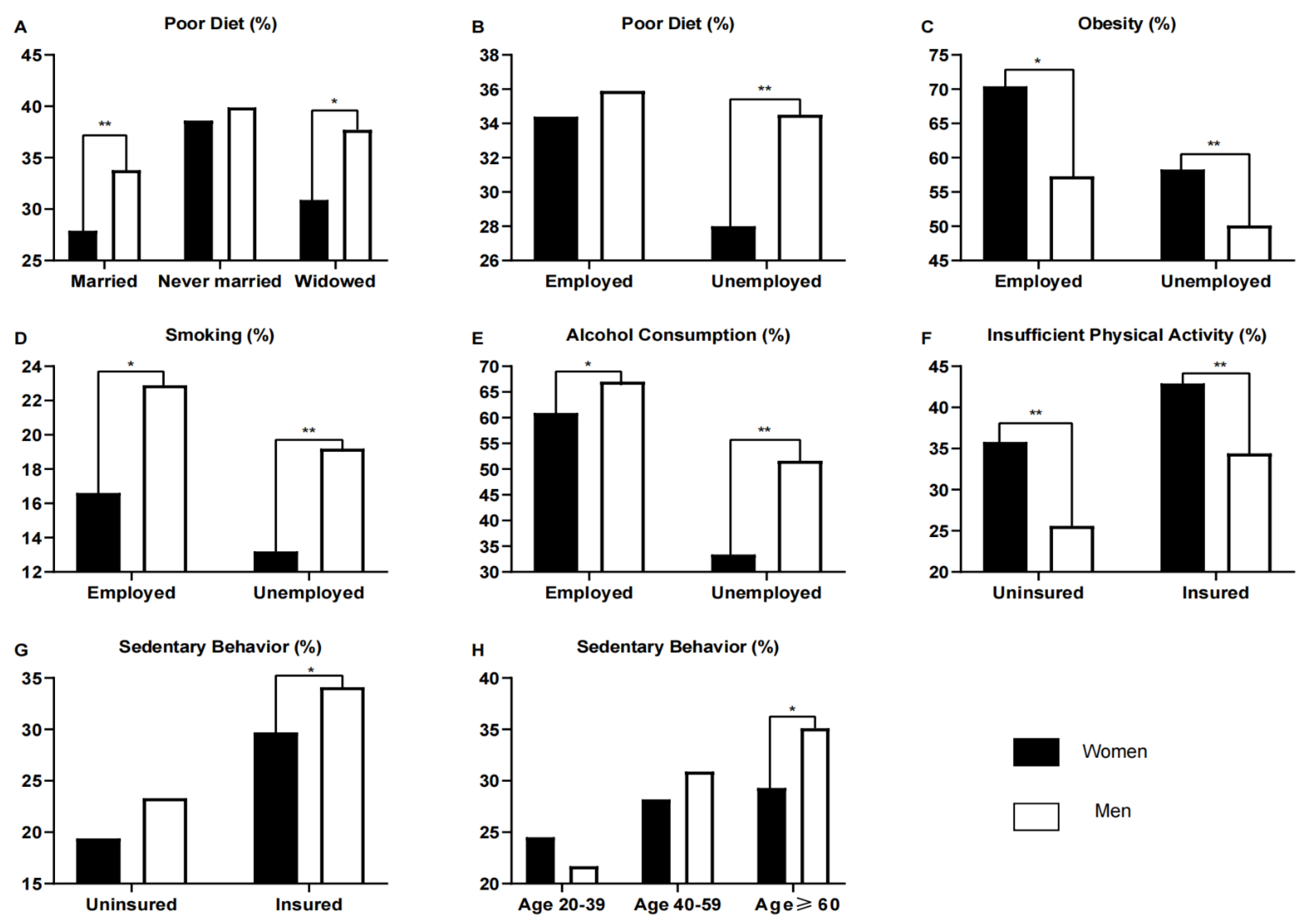
3.1. Gender Differences in Diet
3.2. Gender Differences in Negative Emotion
3.3. Gender Differences in BMI
3.4. Gender Differences in Smoking and Alcohol Consumption
3.5. Gender Differences in Physical Activity and Sedentary Behavior
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Brussels, B. IDF Diabetes Atlas, 10th ed.; International Diabetes Federation: Geneva, Switzerland, 2021; Available online: https://diabetesatlas.org/atlas/tenth-edition/ (accessed on 6 December 2021).
- Chatterjee, S.; Khunti, K.; Davies, M.J. Type 2 diabetes. Lancet 2017, 389, 2239–2251. [Google Scholar] [CrossRef] [PubMed]
- Joseph, J.J.; Deedwania, P.; Acharya, T.; Aguilar, D.; Bhatt, D.L.; Chyun, D.A.; Di Palo, K.E.; Golden, S.H.; Sperling, L.S. Comprehensive Management of Cardiovascular Risk Factors for Adults with Type 2 Diabetes: A Scientific Statement from the American Heart Association. Circulation 2022, 145, E722–E759. [Google Scholar] [CrossRef] [PubMed]
- Ng, M.; Fleming, T.; Robinson, M.; Thomson, B.; Graetz, N.; Margono, C.; Mullany, E.C.; Biryukov, S.; Abbafati, C.; Abera, S.F.; et al. Global, regional, and national prevalence of overweight and obesity in children and adults during 1980-2013: A systematic analysis for the Global Burden of Disease Study 2013. Lancet 2014, 384, 766–781. [Google Scholar] [CrossRef]
- Pan, A.; Wang, Y.; Talaei, M.; Hu, F.B.; Wu, T. Relation of active, passive, and quitting smoking with incident type 2 diabetes: A systematic review and meta-analysis. Lancet Diabetes Endocrinol. 2015, 3, 958–967. [Google Scholar] [CrossRef] [PubMed]
- Gepner, Y.; Golan, R.; Harman-Boehm, I.; Henkin, Y.; Schwarzfuchs, D.; Shelef, I.; Durst, R.; Kovsan, J.; Bolotin, A.; Leitersdorf, E.; et al. Effects of Initiating Moderate Alcohol Intake on Cardiometabolic Risk in Adults with Type 2 Diabetes A 2-Year Randomized, Controlled Trial. Ann. Intern. Med. 2015, 163, 569. [Google Scholar] [CrossRef] [PubMed]
- Smith, A.D.; Crippa, A.; Woodcock, J.; Brage, S. Physical activity and incident type 2 diabetes mellitus: A systematic review and dose-response meta-analysis of prospective cohort studies. Diabetologia 2016, 59, 2527–2545. [Google Scholar] [CrossRef] [PubMed]
- Wilmot, E.G.; Edwardson, C.L.; Achana, F.A.; Davies, M.J.; Gorely, T.; Gray, L.J.; Khunti, K.; Yates, T.; Biddle, S.J.H. Sedentary time in adults and the association with diabetes, cardiovascular disease and death: Systematic review and meta-analysis. Diabetologia 2012, 55, 2895–2905. [Google Scholar] [CrossRef]
- Ciumărnean, L.; Milaciu, M.V.; Negrean, V.; Orășan, O.H.; Vesa, S.C.; Sălăgean, O.; Iluţ, S.; Vlaicu, S.I. Cardiovascular Risk Factors and Physical Activity for the Prevention of Cardiovascular Diseases in the Elderly. Int. J. Environ. Res. Public Health 2021, 19, 207. [Google Scholar] [CrossRef]
- Yancy, W.S.; Mayer, S.B.; Coffman, C.J.; Smith, V.A.; Kolotkin, R.L.; Geiselman, P.J.; Gieselman, P.J.; McVay, M.A.; Oddone, E.Z.; Voils, C.I. Effect of Allowing Choice of Diet on Weight Loss a Randomized Trial. Ann. Intern. Med. 2015, 162, 805. [Google Scholar] [CrossRef]
- DiPietro, L.; Gribok, A.; Stevens, M.S.; Hamm, L.F.; Rumpler, W. Three 15-min Bouts of Moderate Postmeal Walking Significantly Improves 24-h Glycemic Control in Older People at Risk for Impaired Glucose Tolerance. Diabetes Care 2013, 36, 3262–3268. [Google Scholar] [CrossRef]
- American Diabetes Association. 2. Classification and Diagnosis of Diabetes: Standards of Medical Care in Diabetes-2019. Diabetes Care 2019, 42, S13–S28. [Google Scholar] [CrossRef] [PubMed]
- Rhys, W. IDF Diabetes Atlas, 9th ed.; International Diabetes Federation: Geneva, Switzerland, 2019; Available online: https://diabetesatlas.org/resources/ (accessed on 20 November 2021).
- Sattar, N.; Rawshani, A.; Franzen, S.; Rawshani, A.; Svensson, A.M.; Rosengren, A.; McGuire, D.K.; Eliasson, B.; Gudbjörnsdottir, S. Age at Diagnosis of Type 2 Diabetes Mellitus and Associations with Cardiovascular and Mortality Risks Findings from the Swedish National Diabetes Registry. Circulation 2019, 139, 2228–2237. [Google Scholar] [CrossRef] [PubMed]
- Cheng, Y.J.; Kanaya, A.M.; Araneta, M.R.G.; Saydah, S.H.; Kahn, H.S.; Gregg, E.W.; Fujimoto, W.Y.; Imperatore, G. Prevalence of Diabetes by Race and Ethnicity in the United States, 2011–2016. JAMA 2019, 322, 2389–2398. [Google Scholar] [CrossRef]
- Marino, M.; Angier, H.; Springer, R.; Valenzuela, S.; Hoopes, M.; O’Malley, J.; Suchocki, A.; Heintzman, J.; DeVoe, J.; Huguet, N. The Affordable Care Act: Effects of Insurance on Diabetes Biomarkers. Diabetes Care 2020, 43, 2074–2081. [Google Scholar] [CrossRef] [PubMed]
- Anderson, J.E.; Greene, M.A.; Griffin, J.W.; Kohrman, D.B.; Lorber, D.; Saudek, C.D.; Schatz, D.; Siminerio, L. Diabetes and Employment. Diabetes Care 2014, 37, S112–S117. [Google Scholar]
- Trief, P.M.; Himes, C.L.; Orendorff, R.; Weinstock, R.S. The Marital Relationship and Psychosocial Adaptation and Glycemic Control of Individuals with Diabetes. Diabetes Care 2001, 24, 1384–1389. [Google Scholar] [CrossRef]
- Agardh, E.; Allebeck, P.; Hallqvist, J.; Moradi, T.; Sidorchuk, A. Type 2 diabetes incidence and socio-economic position: A systematic review and meta-analysis. Leuk. Res. 2011, 40, 804–818. [Google Scholar] [CrossRef]
- Mathisen, J.; Jensen, A.K.G.; Andersen, I.; Andersen, G.S.; Hvidtfeldt, U.A.; Rod, N.H. Education and incident type 2 diabetes: Quantifying the impact of differential exposure and susceptibility to being overweight or obese. Diabetologia 2020, 63, 1764–1774. [Google Scholar] [CrossRef]
- Yamada, Y.; Matsuo, H.; Segawa, T.; Watanabe, S.; Kato, K.; Kameyama, T.; Yokoi, K.; Ichihara, S.; Metoki, N.; Yoshida, H.; et al. Assessment of genetic factors for type 2 diabetes mellitus. Int. J. Mol. Med. 2006, 18, 299–308. [Google Scholar] [CrossRef]
- Ding, E.L.; Song, Y.Q.; Malik, V.S.; Liu, S.M. Sex differences of endogenous sex hormones and risk of type 2 diabetes—A systematic review and meta-analysis. JAMA-J. Am. Med. Assoc. 2006, 295, 1288–1299. [Google Scholar] [CrossRef]
- National Health and Nutrition Examination Survey. Available online: https://www.cdc.gov/nchs/nhanes/index.htm (accessed on 10 September 2021).
- Fang, M.; Wang, D.; Coresh, J.; Selvin, E. Trends in Diabetes Treatment and Control in US Adults, 1999-2018. New Engl. J. Med. 2021, 384, 2219–2228. [Google Scholar] [CrossRef]
- Rehm, C.D.; Penalvo, J.L.; Afshin, A.; Mozaffarian, D. Dietary Intake Among US Adults, 1999-2012. JAMA-J. Am. Med. Assoc. 2016, 315, 2542–2553. [Google Scholar] [CrossRef]
- Patel, J.S.; Oh, Y.; Rand, K.L.; Wu, W.; Cyders, M.A.; Kroenke, K.; Stewart, J.C. Measurement invariance of the patient health questionnaire-9 (PHQ-9) depression screener in US adults across sex, race/ethnicity, and education level: NHANES 2005–2016. Depress. Anxiety 2019, 36, 813–823. [Google Scholar] [CrossRef]
- Inoue, Y.; Qin, B.; Poti, J.; Sokol, R.; Gordon-Larsen, P. Epidemiology of Obesity in Adults: Latest Trends. Curr. Obes. Rep. 2018, 7, 276–288. [Google Scholar] [CrossRef]
- Guthold, R.; Stevens, G.A.; Riley, L.M.; Bull, F.C. Worldwide trends in insufficient physical activity from 2001 to 2016: A pooled analysis of 358 population-based surveys with 1.9 million participants. Lancet Glob. Health 2018, 6, e1077–e1086. [Google Scholar] [CrossRef]
- Salk, R.H.; Hyde, J.S.; Abramson, L.Y. Gender differences in depression in representative national samples: Meta-analyses of diagnoses and symptoms. Psychol. Bull. 2017, 143, 783–822. [Google Scholar] [CrossRef]
- Goossens, G.H.; Jocken, J.W.E.; Blaak, E.E. Sexual dimorphism in cardiometabolic health: The role of adipose tissue, muscle and liver. Nat. Rev. Endocrinol. 2021, 17, 47–66. [Google Scholar] [CrossRef]
- He, X.; Rebholz, C.M.; Daya, N.; Lazo, M.; Selvin, E. Alcohol consumption and incident diabetes: The Atherosclerosis Risk in Communities (ARIC) study. Diabetologia 2019, 62, 770–778. [Google Scholar] [CrossRef]
- Wakabayashi, I. Light-to-Moderate Alcohol Drinking Reduces the Impact of Obesity on the Risk of Diabetes Mellitus. J. Stud. Alcohol Drugs 2014, 75, 1032–1038. [Google Scholar] [CrossRef]
- US Department of Health and Human Services. US Department of Agriculture Dietary Guidelines for Americans: 2015–2020, 8th ed.; U.S. Department of Health and Human Services; U.S. Department of Agriculture: Washington, DC, USA, 2015. Available online: https://health.gov/dietaryguidelines/2015/guidelines/ (accessed on 2 January 2020).
- Robles, T.F.; Slatcher, R.B.; Trombello, J.M.; McGinn, M.M. Marital quality and health: A meta-analytic review. Psychol. Bull. 2014, 140, 140–187. [Google Scholar] [CrossRef]
- Schultz, W.M.; Kelli, H.M.; Lisko, J.C.; Varghese, T.; Shen, J.; Sandesara, P.; Quyyumi, A.A.; Taylor, H.A.; Gulati, M.; Harold, J.G. Socioeconomic Status and Cardiovascular Outcomes Challenges and Interventions. Circulation 2018, 137, 2166–2178. [Google Scholar] [CrossRef] [PubMed]
- Lo, C.C.; Cheng, T.C. Race, unemployment rate, and chronic mental illness: A 15-year trend analysis. Soc. Psychiatry Psychiatr. Epidemiol. 2014, 49, 1119–1128. [Google Scholar] [CrossRef] [PubMed]
- Lipton, B.J. Association between Health Insurance and Health among Adults with Diabetes: Evidence from Medicare. J. Am. Geriatr. Soc. 2019, 68, 388–394. [Google Scholar] [CrossRef] [PubMed]
- Rogers, M.A.M.; Lee, J.M.; Tipirneni, R.; Banerjee, T.; Kim, C. Interruptions in Private Health Insurance and Outcomes in Adults with Type 1 Diabetes: A Longitudinal Study. Health Aff. 2018, 37, 1024–1032. [Google Scholar] [CrossRef]
- Xu, G.; Liu, B.; Sun, Y.; Du, Y.; Snetselaar, L.G.; Hu, F.B.; Bao, W. Prevalence of diagnosed type 1 and type 2 diabetes among US adults in 2016 and 2017: Population based study. BMJ 2018, 362, k1497. [Google Scholar] [CrossRef]
| Men (N = 578) | Women (N = 516) | Men vs. Women | |
|---|---|---|---|
| Age (%) | p = 0.100 | ||
| 20–39 y | 4.32 (1.92–6.72) | 8.24 (5.25–11.23) | |
| 40–59 y | 28.61 (22.71–34.52) | 26.72 (20.23–33.21) | |
| ≥60 y | 67.07 (60.08–74.05) | 65.04 (56.84–73.24) | |
| Race/Ethnicity (%) | p = 0.236 | ||
| Non-Hispanic White | 63.27 (55.85–70.68) | 58.00 (51.86–64.14) | |
| Non-Hispanic Black | 10.45 (6.78–14.13) | 15.27 (9.91–20.64) | |
| Hispanic | 13.29 (9.35–17.24) | 15.94 (12.26–19.62) | |
| Others | 12.99 (9.06–16.91) | 10.79 (6.71–14.87) | |
| Insurance Status (%) | p = 0.851 | ||
| Uninsured | 8.10 (3.09–13.12) | 7.65 (5.26–10.03) | |
| Insured | 91.78 (86.78–96.77) | 92.21 (89.91–94.51) | |
| Employment Status (%) | p = 0.038 | ||
| Unemployed | 42.53 (36.91–48.14) | 34.49 (28.35–40.64) | |
| Employed | 57.44 (51.80–63.08) | 65.51 (59.36–71.65) | |
| Marital Status (%) | p < 0.001 | ||
| Married or living with partner | 73.98 (68.07–79.88) | 56.70 (51.39–62.02) | |
| Never married | 6.90 (4.52–9.27) | 6.32 (3.65–8.99) | |
| Widowed, divorced, separated | 19.06 (13.48–24.65) | 36.90 (31.03–42.76) | |
| Education Status (%) | p = 0.024 | ||
| Below High School | 59.75 (53.40–66.11) | 49.27 (43.93–54.61) | |
| High school graduate or GED | 25.08 (19.95–30.20) | 32.41 (26.84–37.98) | |
| Some college or above | 14.84 (11.03–18.65) | 18.25 (13.96–22.54) | |
| Family Income Status (%) | p = 0.302 | ||
| PIR < 1.30 | 15.78 (11.61–19.95) | 19.14 (16.39–21.90) | |
| PIR: 1.30–3.49 | 35.27 (29.28–41.26) | 39.40 (32.35–46.46) | |
| PIR ≥ 3.50 | 38.19 (29.91–46.46) | 30.99 (24.23–37.74) | |
| AHA Secondary Diet Score | 37.67 (±0.83) | 38.63 (±0.99) | −0.97 (±1.13) |
| Poor Diet (%) | 31.86 (25.19–38.53) | 32.78 (25.81–39.76) | −0.93 (−10.50–8.65) |
| PHQ-9 score | 3.02 (±0.26) | 4.33 (±0.28) | −1.31 (±0.40) |
| Depression (%) | 10.44 (6.86–14.02) | 10.89 (6.73–15.05) | −0.45 (−5.89–5.00) |
| BMI (kg/m2) | 31.95 (±0.53) | 34.61 (±0.55) | −2.67 (±0.59) |
| Obesity (%) | 55.52 (48.98–62.07) | 67.76 (62.44–73.07) | −12.23 (−20.60–−3.87) |
| Smoking (%) | 15.79 (11.49–20.09) | 13.76 (8.61–18.91) | 2.03 (−4.63–8.68) |
| Alcohol Consumption (%) | 64.57 (56.37–72.77) | 54.91 (47.17–62.65) | 9.66 (−1.53–20.84) |
| Insufficient Physical Activity (%) | 41.38 (35.25–47.51) | 54.13 (47.53–60.73) | −12.75 (−21.69–−3.81) |
| Sedentary Behavior (%) | 39.38 (33.60–45.16) | 34.62 (29.17–40.06) | 4.76 (−3.12–12.64) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Wang, Y.; Cao, P.; Liu, F.; Chen, Y.; Xie, J.; Bai, B.; Liu, Q.; Ma, H.; Geng, Q. Gender Differences in Unhealthy Lifestyle Behaviors among Adults with Diabetes in the United States between 1999 and 2018. Int. J. Environ. Res. Public Health 2022, 19, 16412. https://doi.org/10.3390/ijerph192416412
Wang Y, Cao P, Liu F, Chen Y, Xie J, Bai B, Liu Q, Ma H, Geng Q. Gender Differences in Unhealthy Lifestyle Behaviors among Adults with Diabetes in the United States between 1999 and 2018. International Journal of Environmental Research and Public Health. 2022; 19(24):16412. https://doi.org/10.3390/ijerph192416412
Chicago/Turabian StyleWang, Yu, Peihua Cao, Fengyao Liu, Yilin Chen, Jingyu Xie, Bingqing Bai, Quanjun Liu, Huan Ma, and Qingshan Geng. 2022. "Gender Differences in Unhealthy Lifestyle Behaviors among Adults with Diabetes in the United States between 1999 and 2018" International Journal of Environmental Research and Public Health 19, no. 24: 16412. https://doi.org/10.3390/ijerph192416412
APA StyleWang, Y., Cao, P., Liu, F., Chen, Y., Xie, J., Bai, B., Liu, Q., Ma, H., & Geng, Q. (2022). Gender Differences in Unhealthy Lifestyle Behaviors among Adults with Diabetes in the United States between 1999 and 2018. International Journal of Environmental Research and Public Health, 19(24), 16412. https://doi.org/10.3390/ijerph192416412






