Calling for Help—Peer-Based Psychosocial Support for Medical Staff by Telephone—A Best Practice Example from Germany
Abstract
1. Introduction
1.1. Psychosocial Support
1.2. Anonymous Psychosocial Support by Telephone—Study Situation
1.3. PSU-HELPLINE—Psychosocial Support by Telephone
- (1)
- How burdened do the callers feel and how helpful do they find the conversation on the PSU-HELPLINE?
- (2)
- Which burdens do the callers mention?
- (3)
- How can a telephone support service reduce the psychosocial stress of the callers?
2. Materials and Methods
2.1. Design, Setting and Data Collection
2.2. Study Participants
2.3. Research Ethics
2.4. Bias
2.5. Study Size
2.6. Statistical Methods—Quantitative Part
2.7. Content Analysis—Qualitative Part
3. Results
3.1. Structure of the Sample
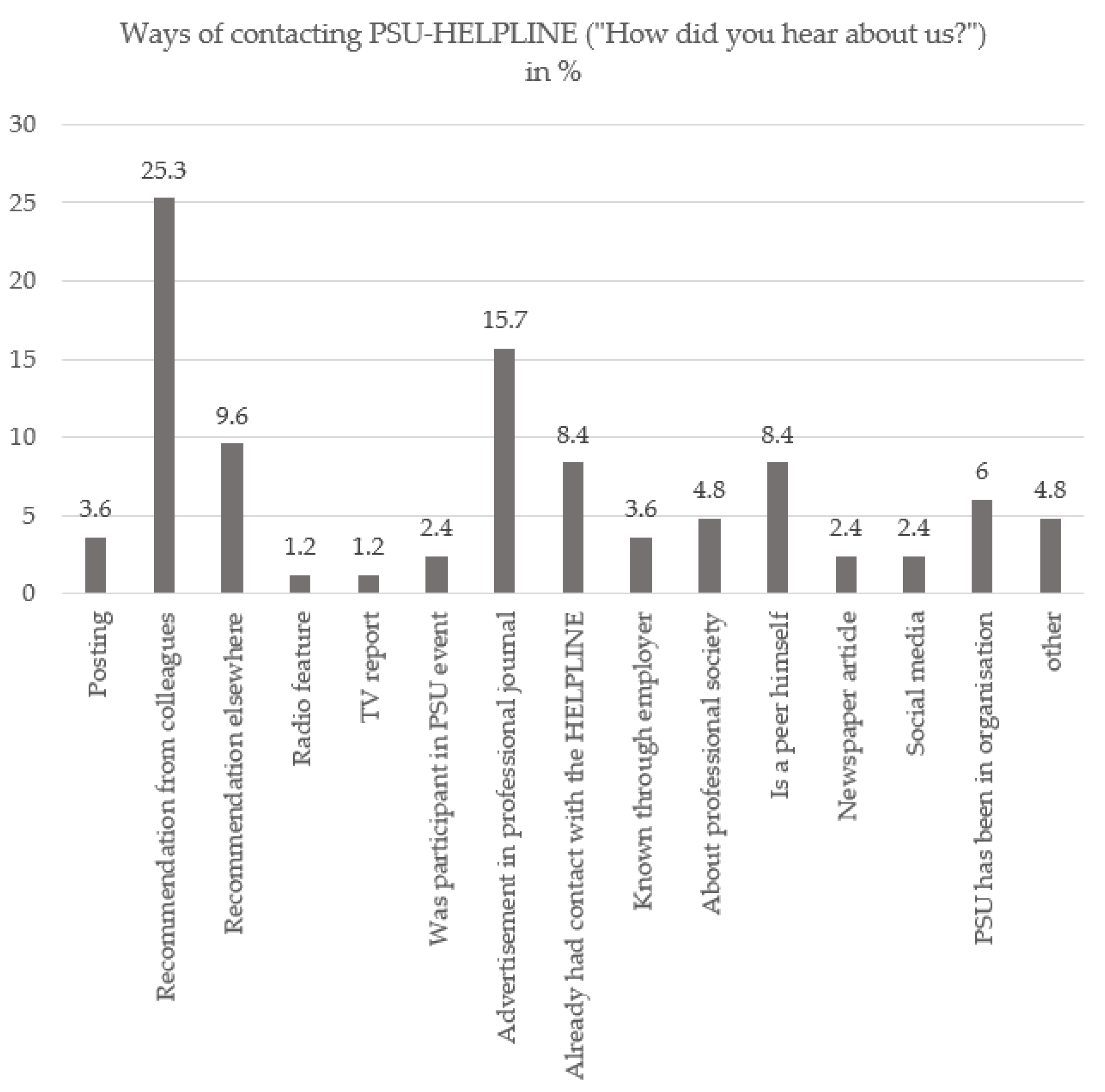
3.2. Descriptive Data—Calls
3.3. Descriptive Data—Burden
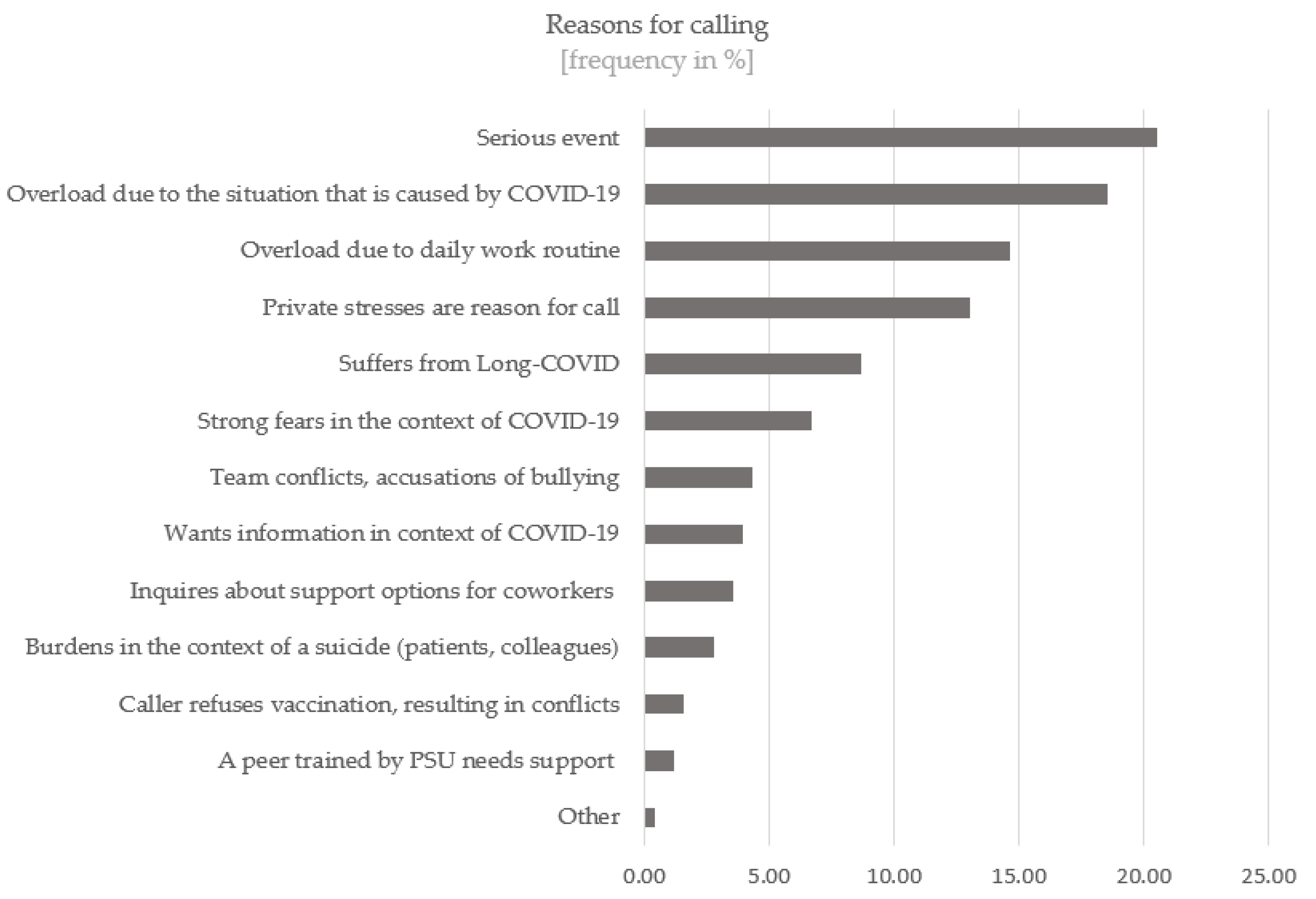
3.4. Content-Analytical Evaluation—Categories “Reasons for Calling at PSU-HELPLINE”
3.5. Content-Analytical Evaluation—“Effect Factors” Categories
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Hannemann, J.; Abdalrahman, A.; Erim, Y.; Morawa, E.; Jerg-Bretzke, L.; Beschoner, P.; Geiser, F.; Hiebel, N.; Weidner, K.; Steudte-Schmiedgen, S.; et al. The impact of the COVID-19 pandemic on the mental health of medical staff considering the interplay of pandemic burden and psychosocial resources—A rapid systematic review. PLoS ONE 2022, 17, e0264290. [Google Scholar] [CrossRef]
- O’Sullivan, D.; Rahamathulla, M.; Pawar, M. The Impact and Implications of COVID-19: An Australian Perspective. Int. J. Community Soc. Dev. 2020, 2, 134–151. [Google Scholar] [CrossRef]
- Waterman, S.; Hunter, E.C.M.; Cole, C.L.; Evans, L.J.; Greenberg, N.; Rubin, G.J.; Beck, A. Training peers to treat Ebola centre workers with anxiety and depression in Sierra Leone. Int. J. Soc. Psychiatry 2018, 64, 156–165. [Google Scholar] [CrossRef] [PubMed]
- Maben, J.; Bridges, J. Covid-19: Supporting nurses’ psychological and mental health. J. Clin. Nurs. 2020, 29, 2742–2750. [Google Scholar] [CrossRef]
- Schulze, S.; Holmberg, C. Bedeutung und Belastung von Pflegekräften während der Corona-Krise. Public Health Forum 2021, 29, 32–35. [Google Scholar] [CrossRef]
- De Medeiros, K.S.; Ferreira de Paiva, L.M.; Macêdo, L.T.d.A.; Farias de Souza, W.; Da Soares Silva, L.A.; Sarmento, A.C.A.; Costa, A.P.F.; Freitas, C.L.; Gonçalves, A.K. Prevalence of Burnout Syndrome and other psychiatric disorders among health professionals during the COVID-19 pandemic: A systematic review and meta-analysis protocol. PLoS ONE 2021, 16, e0260410. [Google Scholar] [CrossRef]
- Tyssen, R.; Vaglum, P. Mental Health Problems among Young Doctors: An Updated Review of Prospective Studies. Harv. Rev. Psychiatry 2002, 10, 154–165. [Google Scholar] [CrossRef]
- Braun, M.; Schönfeldt-Lecuona, C.; Kessler, H.; Beck, J.; Beschoner, P.; Freudenmann, R.W. Burnout, Depression und Substanzgebrauch bei deutschen Psychiatern und Nervenärzten. Nervenheilkunde 2008, 27, 800–804. [Google Scholar] [CrossRef]
- Hinzmann, D.; Schießl, A.; Koll-Krüsmann, M.; Schneider, G.; Kreitlow, J. Peer-Support in der Akutmedizin. Anästhesiol. Intensivmed. 2019, 60, 95–101. [Google Scholar] [CrossRef]
- Wu, A.W. Medical error: The second victim: The doctor who makes the mistake needs help too. BMJ 2000, 320, 726–727. [Google Scholar] [CrossRef]
- Scott, S.D.; Hirschinger, L.E.; Cox, K.R.; McCoig, M.; Brandt, J.; Hall, L.W. The natural history of recovery for the healthcare provider “second victim” after adverse patient events. Qual. Saf. Health Care 2009, 18, 325–330. [Google Scholar] [CrossRef]
- Hodkinson, A.; Zhou, A.; Johnson, J.; Geraghty, K.; Riley, R.; Zhou, A.; Panagopoulou, E.; Chew-Graham, C.A.; Peters, D.; Esmail, A.; et al. Associations of physician burnout with career engagement and quality of patient care: Systematic review and meta-analysis. BMJ 2022, 378, e070442. [Google Scholar] [CrossRef]
- Zaçe, D.; Hoxhaj, I.; Orfino, A.; Viteritti, A.M.; Janiri, L.; Di Pietro, M.L. Interventions to address mental health issues in healthcare workers during infectious disease outbreaks: A systematic review. J. Psychiatr. Res. 2021, 136, 319–333. [Google Scholar] [CrossRef]
- Drudi, L.M.; Nishath, T.; Ma, X.; Mouawad, N.J.; O’Banion, L.A.; Shalhub, S. The impact of the COVID-19 pandemic on wellness among vascular surgeons. Semin. Vasc. Surg. 2021, 34, 43–50. [Google Scholar] [CrossRef]
- Strametz, R.; Raspe, M.; Ettl, B.; Huf, W.; Pitz, A. Handlungsempfehlung: Stärkung der Resilienz von Behandelnden und Umgang mit Second Victims im Rahmen der COVID-19-Pandemie zur Sicherung der Leistungsfähigkeit des Gesundheitswesens. Zentralbl. Arbeitsmed. Arb. Ergon. 2020, 70, 264–268. [Google Scholar] [CrossRef] [PubMed]
- Peterson, A.L. Experiencing stigma as a nurse with mental illness. J. Psychiatr. Ment. Health Nurs. 2017, 24, 314–321. [Google Scholar] [CrossRef]
- Verhaeghe, M.; Bracke, P. Associative stigma among mental health professionals: Implications for professional and service user well-being. J. Health Soc. Behav. 2012, 53, 17–32. [Google Scholar] [CrossRef]
- Michalsen, A.; Hillert, A.; Schießl, A.; Hinzmann, D. Burnout in der Intensivmedizin. Dtsch. Med. Wochenschr. 2018, 143, 21–26. [Google Scholar] [CrossRef]
- Lane, M.A.; Newman, B.M.; Taylor, M.Z.; OʼNeill, M.; Ghetti, C.; Woltman, R.M.; Waterman, A.D. Supporting Clinicians After Adverse Events: Development of a Clinician Peer Support Program. J. Patient Saf. 2018, 14, e56–e60. [Google Scholar] [CrossRef]
- Albott, C.S.; Wozniak, J.R.; McGlinch, B.P.; Wall, M.H.; Gold, B.S.; Vinogradov, S. Battle Buddies: Rapid Deployment of a Psychological Resilience Intervention for Health Care Workers During the COVID-19 Pandemic. Anesth. Analg. 2020, 131, 43–54. [Google Scholar] [CrossRef]
- David, E.; DePierro, J.M.; Marin, D.B.; Sharma, V.; Charney, D.S.; Katz, C.L. COVID-19 Pandemic Support Programs for Healthcare Workers and Implications for Occupational Mental Health: A Narrative Review. Psychiatr. Q. 2022, 93, 227–247. [Google Scholar] [CrossRef] [PubMed]
- Hu, Y.-Y.; Fix, M.L.; Hevelone, N.D.; Lipsitz, S.R.; Greenberg, C.C.; Weissman, J.S.; Shapiro, J. Physicians’ needs in coping with emotional stressors: The case for peer support. Arch. Surg. 2012, 147, 212–217. [Google Scholar] [CrossRef] [PubMed]
- Hinzmann, D.; Schießl, A.; Kreitlow, J.; Igl, A.; Koll-Krüsmann, M.; Heininger, S. „Let‘s talk about … us“. Die Situation an deutschen Klinken mit Blick aus der Anästhesiologie und Intensivmedizin vor der Covid-19 Pandemie. BDA-Befragung zur psychosozialen Unterstützung in der Akutmedizin im Herbst 2019. Anästhesiol. Intensivmed. 2021, 62, 92–99. [Google Scholar] [CrossRef]
- Pollock, A.; Campbell, P.; Cheyne, J.; Cowie, J.; Davis, B.; McCallum, J.; McGill, K.; Elders, A.; Hagen, S.; McClurg, D.; et al. Interventions to support the resilience and mental health of frontline health and social care professionals during and after a disease outbreak, epidemic or pandemic: A mixed methods systematic review. Cochrane Database Syst. Rev. 2020, 11, CD013779. [Google Scholar] [CrossRef] [PubMed]
- Geoffroy, P.A.; Le Goanvic, V.; Sabbagh, O.; Richoux, C.; Weinstein, A.; Dufayet, G.; Lejoyeux, M. Psychological Support System for Hospital Workers During the Covid-19 Outbreak: Rapid Design and Implementation of the Covid-Psy Hotline. Front. Psychiatry 2020, 11, 511. [Google Scholar] [CrossRef]
- Maunder, R.; Hunter, J.; Vincent, L.; Bennett, J.; Peladeau, N.; Leszcz, M.; Sadavoy, J.; Verhaeghe, L.M.; Steinberg, R.; Mazzulli, T. The immediate psychological and occupational impact of the 2003 SARS outbreak in a teaching hospital. CMAJ 2003, 168, 1245–1251. [Google Scholar]
- Feinstein, R.E.; Kotara, S.; Jones, B.; Shanor, D.; Nemeroff, C.B. A health care workers mental health crisis line in the age of COVID-19. Depress. Anxiety 2020, 37, 822–826. [Google Scholar] [CrossRef]
- Gonzalez, A.; Cervoni, C.; Lochner, M.; Marangio, J.; Stanley, C.; Marriott, S. Supporting health care workers during the COVID-19 pandemic: Mental health support initiatives and lessons learned from an academic medical center. Psychol. Trauma 2020, 12, S168–S170. [Google Scholar] [CrossRef]
- DGPs, Deutsche Gesellschaft für Psychologie e.V. Ethische Prinzipien psychologischer Forschung. Available online: https://www.dgps.de/aktuelles/details/ethische-prinzipien-psychologischer-forschung/ (accessed on 26 September 2022).
- Mayring, P. Qualitative Inhaltsanalyse: Grundlagen und Techniken, 13th ed.; Beltz: Weinheim, Germany, 2022; ISBN 3407258984. [Google Scholar]
- Grawe, K.; Donati, R.; Bernauer, F. Psychotherapie im Wandel: Von der Konfession zur Profession, 4th ed.; Hogrefe Verl. für Psychologie: Göttingen, Germany, 1994. [Google Scholar]
- Richter-Kuhlmann, E. Arztgesundheit: Selbstfürsorge kommt zu kurz. Dtsch. Ärzteblatt 2019, 116, 4–6. [Google Scholar]
- Bruce, S.M.; Conaglen, H.M.; Conaglen, J.V. Burnout in physicians: A case for peer-support. Intern. Med. J. 2005, 35, 272–278. [Google Scholar] [CrossRef]
| % | n | |
|---|---|---|
| Gender (n = 328) | ||
| Female | 83.2 | 273 |
| Male | 16.8 | 55 |
| Age (n = 217) | ||
| <30 years | 20.3 | 44 |
| 30–50 years | 52.5 | 114 |
| 51–70 years | 24.9 | 54 |
| >70 years | 2.3 | 5 |
| Profession (n = 342) | ||
| Nursing | 24.3 | 83 |
| Elderly care | 18.4 | 63 |
| Medical doctor | 30.4 | 104 |
| Medical assistant | 3.8 | 13 |
| Employee emergency service | 1.5 | 5 |
| Relative | 1.2 | 4 |
| Self-employed | 0.9 | 3 |
| Other | 19.6 | 67 |
| Effect Factor | Explanation |
|---|---|
| Psychoeducation | Understanding of own reactions is increased |
| Validation | Hearing and understanding that it is appropriate to feel the way you feel |
| Information | Knowing where to turn to for help |
| Preservation of resources | Things are running better again in the team as a result of the advice given to the leaders |
| Change of perspective | Understanding of each other is increased |
| Containing | Feeling accepted |
| Problem solving | Knowing what you can do for yourself, for the team, for the patients |
| Resource activation | Providing materials to the staff and developing a plan for what might do you good |
| Problem actualisation | Picking up and structuring issues through conversation |
| Acceptance of change | Reflections on not having to be perfect, not being able to have all the answers |
| Emotion reduction | Expressing anger, being able to vent without offending |
| Connectedness | To experience that the consultant understands what you are talking about |
| Self-efficacy | Feeling relieved because you have already thought of many things yourself, feeling confirmed and strengthened by the conversation |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hinzmann, D.; Forster, A.; Koll-Krüsmann, M.; Schießl, A.; Schneider, F.; Sigl-Erkel, T.; Igl, A.; Heininger, S.K. Calling for Help—Peer-Based Psychosocial Support for Medical Staff by Telephone—A Best Practice Example from Germany. Int. J. Environ. Res. Public Health 2022, 19, 15453. https://doi.org/10.3390/ijerph192315453
Hinzmann D, Forster A, Koll-Krüsmann M, Schießl A, Schneider F, Sigl-Erkel T, Igl A, Heininger SK. Calling for Help—Peer-Based Psychosocial Support for Medical Staff by Telephone—A Best Practice Example from Germany. International Journal of Environmental Research and Public Health. 2022; 19(23):15453. https://doi.org/10.3390/ijerph192315453
Chicago/Turabian StyleHinzmann, Dominik, Andrea Forster, Marion Koll-Krüsmann, Andreas Schießl, Frederick Schneider, Tanja Sigl-Erkel, Andreas Igl, and Susanne Katharina Heininger. 2022. "Calling for Help—Peer-Based Psychosocial Support for Medical Staff by Telephone—A Best Practice Example from Germany" International Journal of Environmental Research and Public Health 19, no. 23: 15453. https://doi.org/10.3390/ijerph192315453
APA StyleHinzmann, D., Forster, A., Koll-Krüsmann, M., Schießl, A., Schneider, F., Sigl-Erkel, T., Igl, A., & Heininger, S. K. (2022). Calling for Help—Peer-Based Psychosocial Support for Medical Staff by Telephone—A Best Practice Example from Germany. International Journal of Environmental Research and Public Health, 19(23), 15453. https://doi.org/10.3390/ijerph192315453






