Self-Guided Smartphone Application to Manage Chronic Musculoskeletal Pain: A Randomized, Controlled Pilot Trial
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants and Study Setting
2.2. Study Instruments
2.3. Procedure
2.4. Data Analysis
3. Results
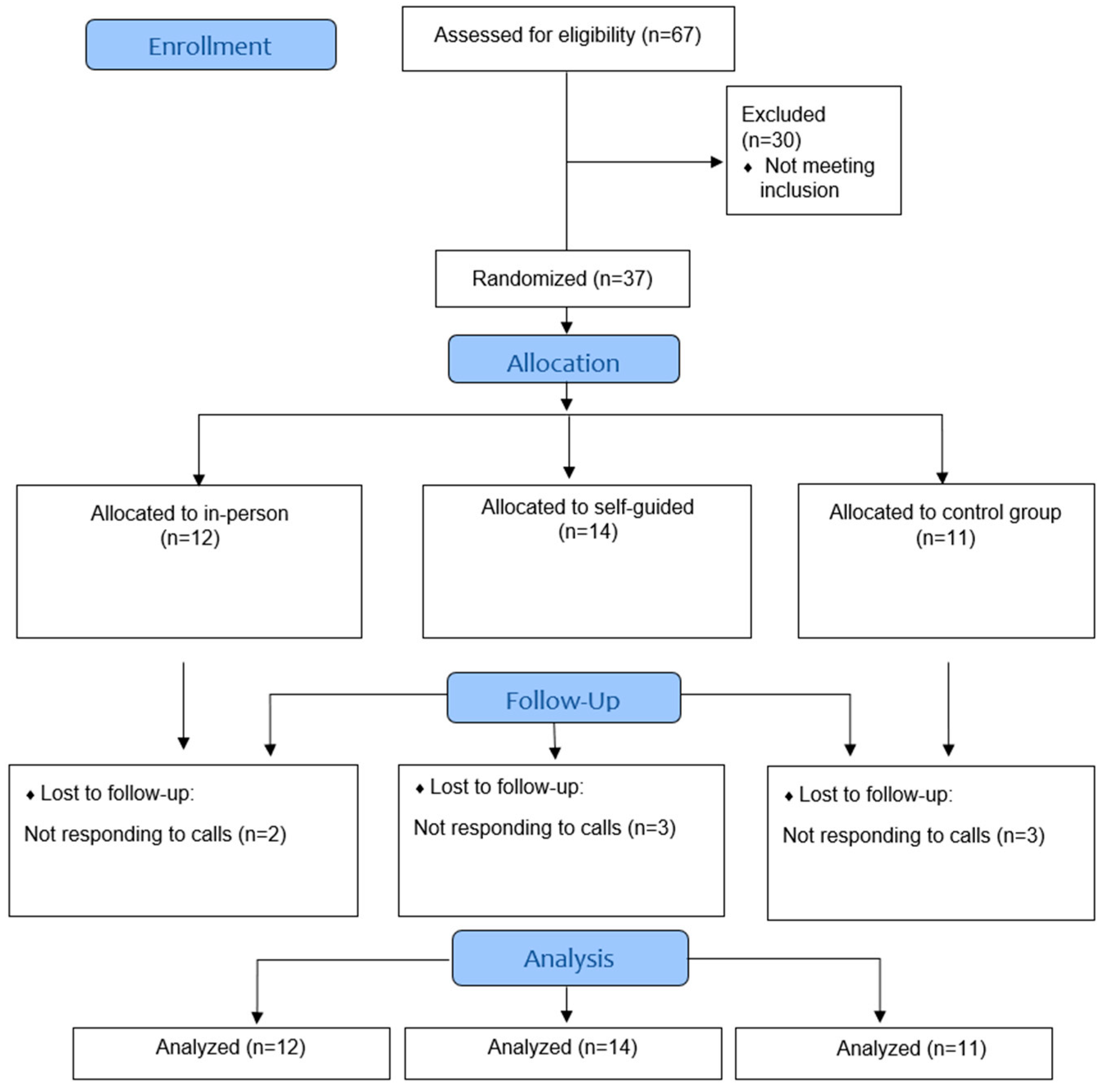
3.1. Recruitment
3.2. Demographic Characteristics of Study Participants
3.3. APA Treatment Outcomes
3.3.1. Physical Function (RMDQ)
3.3.2. Pain Intensity (Average)
3.3.3. Pain Catastrophizing and Fear Avoidance
3.3.4. Anxiety, Depression, Sleep Quality, and Fatigue (PROMIS 29)
3.3.5. Patient’s Global Impression of Change
3.3.6. Satisfaction with APA
3.4. Adherence to APA Practice
3.5. Qualitative Findings
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Dieleman, J.L.; Cao, J.; Chapin, A.; Chen, C.; Li, Z.; Liu, A.; Horst, C.; Kaldjian, A.; Matyasz, T.; Scott, K.W.; et al. US health care spending by payer and health condition, 1996–2016. JAMA 2020, 323, 863–884. [Google Scholar] [CrossRef] [PubMed]
- Fatoye, F.; Gebrye, T.; Odeyemi, I. Real-world incidence and prevalence of low back pain using routinely collected data. Rheumatol. Int. 2019, 39, 619–626. [Google Scholar] [CrossRef] [PubMed]
- Dahlhamer, J.; Lucas, J.; Zelaya, C.; Nahin, R.; Mackey, S.; DeBar, L.; Kerns, R.; Von Korff, M.; Porter, L.; Helmick, C. Prevalence of chronic pain and high-impact chronic pain among adults—United States, 2016. MMWR Morb. Mortal. Wkly. Rep. 2018, 67, 1001–1006. [Google Scholar] [CrossRef] [PubMed]
- Committee Interagency Pain Research National Pain Strategy: A Comprehensive Population Health-Level Strategy for Pain. Available online: https://www.iprcc.nih.gov/sites/default/files/documents/NationalPainStrategy_508C.pdf (accessed on 18 October 2022).
- Skelly, A.C.; Chou, R.; Dettori, J.R.; Turner, J.A.; Friedly, J.L.; Rundell, S.D.; Fu, R.; Brodt, E.D.; Wasson, N.; Kantner, S.; et al. Noninvasive Nonpharmacological Treatment for Chronic Pain: A Systematic Review Update. In Comparative Effectiveness Review No. 227. (Prepared by the Pacific Northwest Evidence-Based Practice Center under Contract No. 290-2015-00009-I.) AHRQ Publication No. 20-EHC009; Agency for Healthcare Research and Quality: Rockville, MD, USA, 2020. [Google Scholar]
- International Association for the Study of Pain, Definitions of Chronic Pain Syndromes. Available online: https://www.iasp-pain.org/advocacy/definitions-of-chronic-pain-syndromes/ (accessed on 18 October 2022).
- Institute of Medicine of the National Academies Report. Relieving Pain in America: A Blueprint for Transforming Prevention, Care, Education, and Research; The National Academies Press: Washington, DC, USA, 2011. [Google Scholar]
- Fast Facts: Low Back and Neck Pain. Available online: https://www.boneandjointburden.org/docs/PRF%207%20FNL%20print-USBJI%20Fast%20Facts%20Low%20Back%20Pain.pdf (accessed on 18 October 2022).
- Centers for Disease Control and Prevention. Severe Headache or Migraine, Low Back Pain, and Neck Pain Among Adults Aged 18 and Over, by Selected Characteristics: United States, Selected Years 1997–2016. Available online: https://www.cdc.gov/nchs/hus/contents2017.htm#041 (accessed on 18 October 2022).
- The Burden of Musculoskeletal Diseases in the United States: Prevalence, Societal and Economic Costs: Low Back and Neck Pain. Available online: https://www.boneandjointburden.org/fourth-edition/iia0/low-back-and-neck-pain (accessed on 17 October 2022).
- Gaskin, D.J.; Richard, P. The economic costs of pain in the United States. J. Pain 2012, 13, 715–724. [Google Scholar] [CrossRef] [PubMed]
- Johnson-Jennings, M.; Duran, B.; Hakes, J.; Paffrath, A.; Little, M.M. The influence of undertreated chronic pain in a national survey: Prescription medication misuse among American indians, Asian Pacific Islanders, Blacks, Hispanics and whites. SSM-Popul. Health 2020, 11, 100563. [Google Scholar] [CrossRef] [PubMed]
- Herman, P.M.; Broten, N.; Lavelle, T.A.; Sorbero, M.E.; Coulter, I.D. Health care costs and opioid use associated with high-impact chronic spinal pain in the United States. Spine 2019, 44, 1154–1161. [Google Scholar] [CrossRef]
- Qaseem, A.; Wilt, T.J.; McLean, R.M.; Forciea, M.A. Noninvasive treatments for acute, subacute, and chronic low back pain: A clinical practice guideline from the American College of Physicians. Ann. Intern. Med. 2017, 166, 514–530. [Google Scholar] [CrossRef]
- Petzke, F.; Klose, P.; Welsch, P.; Sommer, C.; Hauser, W. Opioids for chronic low back pain: An updated systematic review and meta-analysis of efficacy, tolerability and safety in randomized placebo-controlled studies of at least 4 weeks of double-blind duration. Eur. J. Pain 2020, 24, 497–517. [Google Scholar] [CrossRef]
- Bunce, V.; Wieske, J. Health Insurance Mandates in the States 2009; Council for Affordable Health Insurance: Alexandria, VA, USA, 2009. [Google Scholar]
- Zhang, Y.; Lao, L.; Chen, H.; Ceballos, R. Acupuncture use among American adults: What acupuncture practitioners can learn from national health interview survey 2007? Evid.-Based Complement. Altern. Med. 2012, 2012, 710750. [Google Scholar] [CrossRef]
- Cook, C.; Sheets, C. Clinical equipoise and personal equipoise: Two necessary ingredients for reducing bias in manual therapy trials. J. Man. Manip. Ther. 2011, 19, 55–57. [Google Scholar] [CrossRef] [PubMed]
- Freedman, B. Equipoise and the ethics of clinical research. N. Engl. J. Med. 1987, 317, 141–145. [Google Scholar] [CrossRef] [PubMed]
- Chou, R.; Huffman, L.H. Nonpharmacologic therapies for acute and chronic low back pain: A review of the evidence for an American Pain Society/American College of Physicians clinical practice guideline. Ann. Intern. Med. 2007, 147, 492–504. [Google Scholar] [CrossRef]
- Geneen, L.J.; Moore, R.A.; Clarke, C.; Martin, D.; Colvin, L.A.; Smith, B.H. Physical activity and exercise for chronic pain in adults: An overview of Cochrane Reviews. Cochrane Database Syst. Rev. 2017, 4, Cd011279. [Google Scholar]
- Krein, S.L.; Metreger, T.; Kadri, R.; Hughes, M.; Kerr, E.A.; Piette, J.D.; Kim, H.M.; Richardson, C.R. Veterans walk to beat back pain: Ttudy rationale, design and protocol of a randomized trial of a pedometer-based internet mediated intervention for patients with chronic low back pain. BMC Musculoskelet. Disord. 2010, 11, 205. [Google Scholar] [CrossRef]
- Centers for Medicare and Medicaid Services. Decision Memo for Acupuncture for Chronic Low Back Pain (CAG-00452N). Available online: https://www.cms.gov/medicare-coverage-database/details/nca-decision-memo.aspx?NCAId=295 (accessed on 26 September 2022).
- Eleswarapu, A.S.; Divi, S.N.; Dirschl, D.R.; Mok, J.M.; Stout, C.; Lee, M.J. How effective is physical therapy for common low back pain diagnoses?: A multivariate analysis of 4597 patients. Spine 2016, 41, 1325–1329. [Google Scholar] [CrossRef] [PubMed]
- Chen, L.; Houghton, M.; Seefeld, L.; Malarick, C.; Mao, J. A survey of selected physician views on acupuncture in pain management. Pain Med. 2010, 11, 530–534. [Google Scholar] [CrossRef] [PubMed]
- Yuan, J.; Purepong, N.; Kerr, D.P.; Park, J.; Bradbury, I.; McDonough, S. Effectiveness of acupuncture for low back pain: A systematic review. Spine 2008, 33, E887–E900. [Google Scholar] [CrossRef] [PubMed]
- Cui, J.; Wang, S.; Ren, J.; Zhang, J.; Jing, J. Use of acupuncture in the USA: Changes over a decade (2002–2012). Acupunct. Med. 2017, 35, 200–207. [Google Scholar] [CrossRef] [PubMed]
- Morone, N.E.; Greco, C.M.; Moore, C.G.; Rollman, B.L.; Lane, B.; Morrow, L.A.; Glynn, N.W.; Weiner, D.K. A Mind-Body Program for Older Adults With Chronic Low Back Pain: A Randomized Clinical Trial. JAMA Intern. Med. 2016, 176, 329–337. [Google Scholar] [CrossRef]
- Morone, N.E.; Rollman, B.L.; Moore, C.G.; Li, Q.; Weiner, D.K. A mind–body program for older adults with chronic low back pain: Results of a pilot study. Pain Med. 2009, 10, 1395–1407. [Google Scholar] [CrossRef]
- Cherkin, D.C.; Sherman, K.J.; Balderson, B.H.; Cook, A.J.; Anderson, M.L.; Hawkes, R.J.; Hansen, K.E.; Turner, J.A. Effect of Mindfulness-Based Stress Reduction vs. Cognitive Behavioral Therapy or Usual Care on Back Pain and Functional Limitations in Adults with Chronic Low Back Pain: A Randomized Clinical Trial. JAMA 2016, 315, 1240–1249. [Google Scholar] [CrossRef]
- Hall, A.M.; Maher, C.G.; Lam, P.; Ferreira, M.; Latimer, J. Tai chi exercise for treatment of pain and disability in people with persistent low back pain: A randomized controlled trial. Arthritis Care Res. 2011, 63, 1576–1583. [Google Scholar] [CrossRef]
- Weifen, W.; Muheremu, A.; Chaohui, C.; Md, L.W.; Lei, S. Effectiveness of Tai Chi Practice for Non-Specific Chronic Low Back Pain on Retired Athletes: A Randomized Controlled Study. J. Musculoskelet. Pain 2013, 21, 37–45. [Google Scholar] [CrossRef]
- Nambi, G.S.; Inbasekaran, D.; Khuman, R.; Devi, S.; Shanmugananth; Jagannathan, K. Changes in pain intensity and health related quality of life with Iyengar yoga in nonspecific chronic low back pain: A randomized controlled study. Int. J. Yoga 2014, 7, 48–53. [Google Scholar] [CrossRef]
- Cramer, H.; Lauche, R.; Haller, H.; Dobos, G. A systematic review and meta-analysis of yoga for low back pain. Clin. J. Pain 2013, 29, 450–460. [Google Scholar] [CrossRef]
- Henschke, N.; Ostelo, R.; van Tulder, M.W.; Vlaeyen, J.W.S.; Morley, S.; Assendelft, W.J.J.; Main, C.J. Behavioural treatment for chronic low-back pain. Cochrane Database Syst. Rev. 2010, 2010, CD002014. [Google Scholar] [CrossRef]
- Rubinstein, S.M.; de Zoetes, A.; van Middelkoop, M.; Assendelft, W.J.J.; de Boer, M.R.; van Tulder, M.W. Benefits and harms of spinal manipulative therapy for the treatment of chronic low back pain: Systematic review and meta-analysis of randomised controlled trials. BMJ 2019, 13, 1689. [Google Scholar] [CrossRef]
- Du, S.; Yuan, C.; Xiao, X.; Chu, J.; Qiu, Y.; Qian, H. Self-management programs for chronic musculoskeletal pain conditions: A systematic review and meta-analysis. Patient Educ. Couns. 2011, 85, e299–e310. [Google Scholar] [CrossRef]
- Kroon, F.P.; van der Burg, L.R.; Buchbinder, R.; Osborne, R.H.; Johnston, R.V.; Pitt, V. Self-management education programmes for osteoarthritis. Cochrane Database Syst. Rev. 2014, 1, Cd008963. [Google Scholar] [CrossRef]
- Nolte, S.; Osborne, R.H. A systematic review of outcomes of chronic disease self-management interventions. Qual. Life Res. Int. J. Qual. Life Asp. Treat. Care Rehabil. 2013, 22, 1805–1816. [Google Scholar] [CrossRef]
- Du, S.; Hu, L.; Dong, J.; Xu, G.; Chen, X.; Jin, S.; Zhang, H.; Yin, H. Self-management program for chronic low back pain: A systematic review and meta-analysis. Patient Educ. Couns. 2016, 100, 37–49. [Google Scholar] [CrossRef]
- Nogier, P. Handbook to Auriculotherapy, 1st ed.; Maisonneuve: Moulins-les-Metz, France, 1981. [Google Scholar]
- Nogier, R. How did Paul Nogier establish the map of the ear? Med. Acupunct. 2014, 26, 76–83. [Google Scholar] [CrossRef]
- Nogier, P. Points Reflexes Auricularis; Maisonneuve SA: Moulin Les-Metz, France, 1987. [Google Scholar]
- Yeh, C.H.; Huang, L.C. Comprehensive and systematic auricular diagnosis protocol. Med. Acupunct. 2013, 25, 423–436. [Google Scholar] [CrossRef]
- Oleson, T. Auriculotherapy Manual: Chinese and Western Systems of Ear Acupuncture, 4th ed.; Churchill Livingstone, Elsevier: Edinburgh, UK, 2014. [Google Scholar]
- Huang, L.C. Auricular Medicine: A Complete Manual of Auricular Diagnosis and Treatment, 1st ed.; Auricular International Research & Training: Orlando, FL, USA, 2005. [Google Scholar]
- Alimi, D.; Geissmann, A.; Gardeur, D. Auricular acupuncture stimulation measured on functional magnetic resonance imaging. Med. Acupunct. 2002, 13, 18–21. [Google Scholar]
- Romoli, M.; Allais, G.; Airola, G.; Benedetto, C.; Mana, O.; Giacobbe, M.; Pugliese, A.M.; Battistella, G.; Fornari, E. Ear acupuncture and fMRI: A pilot study for assessing the specificity of auricular points. Neurol. Sci. 2014, 35 (Suppl. 1), 189–193. [Google Scholar] [CrossRef]
- Yeh, C.H.; Chien, L.C.; Albers, K.M.; Margolis, L.; Liu, R.Y.; Suen, L.; Ren, D. Function of auricular point acupressure in inducing changes in inflammatory cytokines during chronic low back pain: A pilot study. Med. Acupunct. 2014, 26, 31–39. [Google Scholar] [CrossRef]
- Lin, W.C.; Yeh, C.H.; Chien, L.C.; Morone, N.E.; Glick, R.M.; Albers, K.M. The anti-inflammatory actions of auricular point acupressure for chronic low back pain. Evid.-Based Complement. Altern. Med. 2015, 2015, 103570. [Google Scholar] [CrossRef]
- Kawi, J.; Yeh, C.H.; Li, M.C.; Caswell, K.; Mazraani, M.; Lukkahatain, N.; Mensah, S.; Taylor, J.; Budhathoki, C.; Christo, P. Auricular point acupressure smartphone application to manage chronic musculoskeletal pain: A longitudinal, one-group, open pilot trial. Glob. Adv. Health Med. 2021. [Google Scholar] [CrossRef]
- Yeh, C.; Kawi, J.; Ni, A.; Christo, P. Evaluating auricular point acupressure for chronic low back pain self-management using technology: A feasibility study. Pain Manag. Nurs. 2022, 23, 301–310. [Google Scholar] [CrossRef]
- Suen, K.P.L.; Yeh, C.H. Auricular diagnosis in chronic illnesses. Med. Acupunct. 2014, 26, 125–129. [Google Scholar] [CrossRef]
- Arai, Y.C.; Sakakima, Y.; Kawanishi, J.; Nishihara, M.; Ito, A.; Tawada, Y.; Maruyama, Y. Auricular acupuncture at the "shenmen" and "point zero" points induced parasympathetic activation. Evid.-Based Complement. Altern. Med. eCAM 2013, 2013, 945063. [Google Scholar] [CrossRef]
- Bandura, A. Self-efficacy: Toward a unifying theory of behavioral change. Psychol. Rev. 1977, 84, 191–215. [Google Scholar] [CrossRef]
- Bandura, A. Self-Efficacy in Changing Societies; Cambridge University Press: Cambridge, UK, 1995. [Google Scholar]
- Roland, M.; Fairbank, J. The Roland-Morris disability questionnaire and the Oswestry disability questionnaire. Spine 2000, 25, 3115–3124. [Google Scholar] [CrossRef]
- Roland, M.; Morris, R. A study of the natural history of back pain. Part I: Development of a reliable and sensitive measure of disability in low-back pain. Spine 1983, 8, 141–144. [Google Scholar] [CrossRef]
- Jordan, K.; Dunn, K.M.; Lewis, M.; Croft, P. A minimal clinically important difference was derived for the Roland-Morris Disability Questionnaire for low back pain. J. Clin. Epidemiol. 2006, 59, 45–52. [Google Scholar] [CrossRef]
- Dworkin, R.H.; Turk, D.C.; McDermott, M.P.; Peirce-Sandner, S.; Burke, L.B.; Cowan, P.; Farrar, J.T.; Hertz, S.; Raja, S.N.; Rappaport, B.A.; et al. Interpreting the clinical importance of group differences in chronic pain clinical trials: IMMPACT recommendations. Pain 2009, 146, 238–244. [Google Scholar] [CrossRef]
- Sullivan, M.J.L.; Bishop, S.R.; Pivik, J. The pain catastrophizing scale: Development and validation. Psychol. Assess. 1995, 7, 524–532. [Google Scholar] [CrossRef]
- Waddell, G.; Newton, M.; Henderson, I.; Somerville, D.; Main, C.J. A Fear-avoidance beliefs questionnaire (FABQ) and the role of fear-avoidance beliefs in chronic low back pain and disability. Pain 1993, 52, 157–168. [Google Scholar] [CrossRef]
- Craig, B.M.; Reeve, B.B.; Brown, P.M.; Cella, D.; Hays, R.D.; Lipscomb, J.; Simon Pickard, A.; Revicki, D.A. US valuation of health outcomes measured using the PROMIS-29. Value Health 2014, 17, 846–853. [Google Scholar] [CrossRef]
- Hays, R.D.; Spritzer, K.L.; Schalet, B.D.; Cella, D. PROMIS((R))-29 v2.0 profile physical and mental health summary scores. Qual. Life Res. Int. J. Qual. Life Asp. Treat. Care Rehabil. 2018, 27, 1885–1891. [Google Scholar] [CrossRef]
- Hays, R.D.; Revicki, D.A.; Feeny, D.; Fayers, P.; Spritzer, K.L.; Cella, D. Using Linear Equating to Map PROMIS((R)) Global Health Items and the PROMIS-29 V2.0 Profile Measure to the Health Utilities Index Mark 3. Pharmacoeconomics 2016, 34, 1015–1022. [Google Scholar] [CrossRef]
- Hurst, H.; Bolton, J. Assessing the clinical significance of change scores recorded on subjective outcome measures. J. Manip. Physiol. Ther. 2004, 27, 26–35. [Google Scholar] [CrossRef]
- Yeh, C.H.; Chien, L.C.; Chiang, Y.C.; Huang, L.C. Auricular point acupressure for chronic low back pain: A feasibility study for 1-week treatment. Evid. Based Complement. Alternat. 2012, 2012, 383257. [Google Scholar] [CrossRef]
- Lin, W.C.; Burke, L.E.; Schlenk, E.A.; Yeh, C.H. Use of an ecological momentary asessment aplication to asess the efects of aricular point acupressure for chronic low back pain. CIN Comput. Inform. Nurs. 2019, 37, 276–282. [Google Scholar]
- Yeh, C.H.; Suen, L.K.P.; Chien, L.C.; Margolis, L.; Bhatnagar, S.; Teika, T.; Hoffman, S.; Liang, Z.; Glick, R.; Morone, N.E. Day-to-day changes of auricular point acupressure to manage chronic low back pain: A 29-day randomized control study. Pain Med. 2015, 16, 1857–1869. [Google Scholar] [CrossRef]
- Dworkin, R.H.; Turk, D.C.; Wyrwich, K.W.; Beaton, D.; Cleeland, C.S.; Farrar, J.T.; Haythornthwaite, J.A.; Jensen, M.P.; Kerns, R.D.; Ader, D.N.; et al. Interpreting the clinical importance of treatment outcomes in chronic pain clinical trials: IMMPACT recommendations. J. Pain 2008, 9, 105–121. [Google Scholar] [CrossRef]
- Miles, M.B.; Huberman, A.M. Qualitative Data Analysis: An Expanded Sourcebook, 2nd ed.; Sage Publications: Thousand Oaks, CA, USA, 1994. [Google Scholar]
- National Cancer for Complementary and Integrative Health Pilot Studies: Common Uses and Misuses. Available online: https://www.nccih.nih.gov/grants/pilot-studies-common-uses-and-misuses (accessed on 30 June 2022).
- Chou, R.; Deyo, R.; Friedly, J.; Skelly, A.; Hashimoto, R.; Weimer, M.; Fu, R.; Dana, T.; Kraegel, P.; Griffin, J.; et al. Nonpharmacologic Therapies for Low Back Pain: A Systematic Review for an American College of Physicians Clinical Practice Guideline. Ann. Intern. Med. 2017, 166, 493–505. [Google Scholar] [CrossRef]
- Enthoven, W.T.; Roelofs, P.D.; Deyo, R.A.; van Tulder, M.W.; Koes, B.W. Non-steroidal anti-inflammatory drugs for chronic low back pain. Cochrane Database Syst. Rev. 2016, 2, CD012087. [Google Scholar] [CrossRef]
| In-Person mAPA (n = 14) | Self-Guided mAPA (n = 12) | Control (n = 11) | Overall (n = 37) | |
|---|---|---|---|---|
| Age, years | ||||
| Mean (SD) (range) | 50.4 (20.70) (21–81) | 51.2 (17.49) (19–75) | 50.1 (13.95) (20–70) | 50.5 (17.39) (19–81) |
| Gender, n (%) | ||||
| Female | 11 (79) | 8 (67) | 8 (73) | 27 (73) |
| Male | 3 (21) | 4 (33) | 3 (27) | 10 (27) |
| Race, n (%) | ||||
| Asian | 1 (7) | 3 (25) | 1 (9) | 5 (14) |
| Black or African American | 2 (14) | 2 (17) | 3 (27) | 7 (19) |
| More than one race | 1 (7) | 1 (8) | 2 (18) | 4 (11) |
| White | 10 (71) | 6 (50) | 5 (45) | 21 (57) |
| Ethnicity, n (%) | ||||
| Hispanic or Latino | 2 (14) | 1 (8) | 1 (9) | 4 (11) |
| Not Hispanic or Latino | 12 (86) | 11 (92) | 8 (73) | 31 (84) |
| Prefer not to say | 0 (0) | 0 (0) | 2 (18) | 2 (5) |
| Employment Situation, n (%) | ||||
| Working (full-time) | 9 (64) | 2 (17) | 5 (45) | 16 (43) |
| Not employed | 5 (36) | 10 (83) | 6 (55) | 21 (57) |
| Education Level, n (%) | ||||
| High school | 0 (0) | 0 (0) | 2 (18) | 2 (5) |
| Some college | 2 (14) | 4 (33) | 1 (9) | 7 (19) |
| College graduate | 6 (43) | 4 (33) | 6 (55) | 16 (43) |
| Post-graduate degree | 6 (43) | 4 (33) | 2 (18) | 12 (33) |
| Smoking, n (%) | ||||
| Current smoker | 1 (7) | 1 (8) | 3 (27) | 5 (14) |
| Never smoked | 11 (79) | 9 (75) | 4 (36) | 24 (65) |
| Previously smoked, but quit | 2 (14) | 2 (17) | 4 (36) | 8 (22) |
| BMI Mean (SD) | 26.25 (7.00) | 21.92 (8.23) | 29.38 (8.76) | 25.77 (8.29) |
| Duration of musculoskeletal pain, n (%) | ||||
| 6 months to 1 year | 0 (0) | 1 (8) | 1 (9) | 2 (5) |
| 1–5 years | 7 (50) | 3 (25) | 6 (55) | 16 (43) |
| More than 5 years | 7 (50) | 8 (67) | 4 (36) | 19 (52) |
| Number of pain areas or locations related to musculoskeletal pain, n (%) | ||||
| 1 | 2 (14) | 0 (0) | 1 (9) | 3 (8) |
| 2 | 2 (14) | 3 (25) | 0 (0) | 5 (14) |
| 3 | 5 (36) | 4 (33) | 8 (73) | 17 (46) |
| 4 | 1 (7) | 2 (17) | 1 (9) | 4 (11) |
| 5 | 2 (14) | 1 (8) | 0 (0) | 3 (8) |
| More than 5 | 2 (14) | 2 (17) | 1 (9) | 5 (14) |
| Pain intensity at location #1, mean (SD) | 6.1 (1.99) | 5.3 (1.83) | 7.2 (1.17) | 6.2 (1.84) |
| Pain intensity at location #2, mean (SD) | 6.0 (2.22) | 5.4 (1.36) | 6.9 (1.58) | 6.1 (1.83) |
| Pain intensity at location #3, mean (SD) | 5.4 (2.19) | 4.8 (1.49) | 5.5 (2.25) | 5.3 (1.99) |
| Primary pain location, n (%) | ||||
| Back | 8 (57) | 5 (45) | 5 (45) | 18 (49) |
| Neck | 2 (14) | 1 (9) | 3 (27) | 6 (16) |
| Foot | 1 (7) | 2 (18) | 1 (9) | 4 (11) |
| Knee | 0 (0) | 1 (9) | 2 (18) | 3 (8) |
| Hip | 3 (21) | 0 (0) | 0 (0) | 3 (8) |
| Hands | 0 (0) | 1 (9) | 0 (0) | 1 (3) |
| Shoulder | 0 (0) | 1 (9) | 0 (0) | 1 (3) |
| Missing | 0 (0) | 1 (9) | 0 (0) | 1 (3) |
| Use of Pain Medication = Yes (n (%)) | |||
|---|---|---|---|
| In-Person mAPA | Self-Guided mAPA | Control | |
| Baseline | 14 (100) | 12 (100) | 11 (100) |
| Post-APA | 11 (79) | 10 (83) | 11 (100) |
| 1M follow-up | 11 (79) | 9 (75) | 11 (100) |
| In-Person mAPA | Self-Guided mAPA | Control | Cohen’s d In-Person vs. Control | Cohen’s d Self-Guided vs. Control | Cohen’s d In-Person vs. Self-Guided | Cronbach’s Alpha | |
|---|---|---|---|---|---|---|---|
| Physical Function (RMDQ) | 0.923 | ||||||
| Baseline Mean (SD) | 5.7 (5.78) | 3.8 (4.90) | 7.3 (7.82) | ||||
| Post-APA Mean (SD) (%) † | 3.8 (5.10) (−0.32) | 2.9 (4.63) (−0.42) | 7.1 (7.27) (−0.06) | 0.02 | −0.01 | 0.06 | |
| Mean Change (SD) | −1.1 (3.24) | −1.7 (2.00) | −0.5 (2.25) | ||||
| ≥30% Reduction, n (%) † | 4 (29) | 3 (25) | 0 (0) | ||||
| 1M Follow-up Mean (SD) (%) † | 3.5 (3.50) (−0.29) | 2.9 (4.40) (−0.48) | 6.0 (7.38) (−0.25) | −0.04 | −0.03 | −0.02 | |
| Mean Change (SD) | −1.4 (2.50) | −0.1 (2.85) | 0.3 (6.66) | ||||
| ≥30% Reduction, n (%) † | 4 (29) | 3 (25) | 0 (0) | ||||
| Pain Intensity (Average) | Single item | ||||||
| Baseline Mean (SD) | 5.4 (1.69) | 5.5 (1.44) | 6.8 (2.04) | ||||
| Post-APA Mean (SD) (%) † | 3.0 (1.41) (−0.45) | 2.6 (1.51) (−0.48) | 6.5 (1.75) (−0.01) | −1.45 | −1.25 | 0.09 | |
| Mean Change (SD) | −2.5 (1.37) | −2.7 (2.11) | −0.4 (1.63) | ||||
| ≥30% Reduction, n (%) † | 7 (50) | 6 (50) | 0 (0) | ||||
| 1M Follow-up Mean (SD) (%) † | 3.2 (1.40) (−0.42) | 2.9 (1.83) (−0.45) | 5.7 (1.64) (−0.11) | −0.91 | −0.81 | 0.05 | |
| Mean Change (SD) | −2.4 (1.43) | −2.4 (2.01) | −1.5 (2.12) | ||||
| ≥30% Reduction, n (%) † | 8 (57) | 5 (42) | 0 (0) | ||||
| Pain Catastrophizing | 0.949 | ||||||
| Baseline Mean (SD) | 13.4 (14.12) | 15.1 (11.86) | 22.7 (17.07) | ||||
| Post-APA Mean (SD) (%) † | 8.6 (9.96) (−0.47) | 11.2 (6.89) (−0.25) | 16.7 (13.21) (−0.23) | 0.09 | −0.07 | 0.09 | |
| ≥30% Reduction, n (%) † | 6 (43) | 6 (50) | 0 (0) | ||||
| 1M Follow-up Mean (SD) (%) † | 6.0 (5.67) (−0.52) | 7.4 (6.54) (−0.47) | 17.3 (10.71) (−0.13) | −0.13 | −0.02 | −0.14 | |
| ≥30% Reduction, n (%) † | 7 (50) | 7 (58) | 0 (0) | ||||
| Fear Avoidance of Physical Activity | 0.879 | ||||||
| Baseline Mean (SD) | 13.1 (8.28) | 11.6 (5.54) | 14.7 (10.02) | ||||
| Post-APA Mean (SD) (%) † | 10.3 (7.04) (−0.30) | 11.2 (7.08) (0.02) | 13.6 (9.76) (−0.14) | 0.13 | 0.48 | −0.46 | |
| ≥30% Reduction, n (%) † | 7 (50) | 2 (17) | 0 (0) | ||||
| 1M Follow-up Mean (SD) (%) † | 9.5 (6.52) (−0.22) | 6.6 (6.02) (−0.51) | 17.1 (8.25) (0.09) | −0.61 | −1.40 | 0.12 | |
| ≥30% Reduction, n (%) † | 5 (36) | 7 (58) | 0 (0) | ||||
| Anxiety | 0.972 | ||||||
| Baseline Mean (SD) | 51.0 (10.20) | 53.4 (11.95) | 51.6 (9.23) | ||||
| Post-APA Mean (SD) (%) † | 51.1 (8.68) (−0.01) | 52.8 (11.89) (−0.03) | 57.5 (10.64) (0.12) | −1.07 | −1.11 | 0.10 | |
| 1M Follow-up Mean (SD) (%) † | 50.9 (10.19) (−0.02) | 52.8 (9.90) (0.00) | 55.2 (9.06) (0.09) | −0.60 | −0.55 | −0.08 | |
| Depression | 0.965 | ||||||
| Baseline Mean (SD) | 49.8 (7.52) | 49.6 (7.84) | 48.6 (7.84) | ||||
| Post-APA Mean (SD) (%) † | 49.6 (8.58) (−0.02) | 46.3 (7.08) (−0.07) | 53.2 (10.69) (0.10) | −0.95 | −1.27 | 0.49 | |
| 1M Follow-up Mean (SD) (%) † | 47.9 (8.07) (−0.05) | 47.6 (8.50) (−0.03) | 50.4 (9.89) (0.04) | −0.92 | −0.63 | −0.17 | |
| Fatigue | 0.986 | ||||||
| Baseline Mean (SD) | 53.5 (10.07) | 54.7 (13.24) | 55.2 (11.21) | ||||
| Post-APA Mean (SD) (%) † | 50.6 (8.21) (−0.07) | 53.5 (12.02) (−0.00) | 57.7 (13.31) (0.05) | −0.96 | −0.53 | −0.35 | |
| 1M Follow-up Mean (SD) (%) † | 47.9 (9.33) (−0.11) | 54.4 (17.05) (−0.03) | 57.7 (12.76) (0.05) | −1.08 | −0.45 | −0.45 | |
| Sleep | 0.913 | ||||||
| Baseline Mean (SD) | 53.5 (6.83) | 50.3 (7.01) | 54.9 (8.01) | ||||
| Post-APA Mean (SD) (%) † | 49.6 (4.45) (−0.07) | 51.8 (4.19) (−0.00) | 55.3 (7.35) (0.02) | −0.96 | −0.53 | −0.35 | |
| 1M Follow-up Mean (SD) (%) † | 52.3 (4.19) (−0.02) | 49.9 (6.25) (−0.04) | 56.5 (6.76) (0.04) | −1.08 | −0.45 | −0.45 |
| In-Person mAPA n (%) | Self-Guided mAPA n (%) | |
|---|---|---|
| One week after APA | ||
| Completely satisfied | 1 (7) | 3 (25) |
| Somewhat satisfied | 9 (64) | 7 (58) |
| Not satisfied | 2 (14) | 0 (0) |
| Missing | 2 (14) | 2 (17) |
| Two weeks after APA | ||
| Completely satisfied | 2 (14) | 3 (25) |
| Somewhat satisfied | 9 (64) | 6 (50) |
| Not satisfied | 1 (7) | 1 (8) |
| Missing | 2 (14) | 2 (17) |
| Three weeks after APA | ||
| Completely satisfied | 2 (14) | 5 (42) |
| Somewhat satisfied | 9 (64) | 4 (33) |
| Not satisfied | 0 (0) | 1 (8) |
| Missing | 3 (21) | 2 (17) |
| Four weeks after APA | ||
| Completely satisfied | 1 (7) | 3 (25) |
| Somewhat satisfied | 10 (71) | 6 (50) |
| Not satisfied | 0 (0) | 1 (8) |
| Missing | 3 (21) | 2 (17) |
| One month after 4 weeks of APA (1M follow-up) | ||
| Completely satisfied | 1 (7) | 5 (42) |
| Somewhat satisfied | 10 (71) | 3 (25) |
| Not satisfied | 0 (0) | 1 (8) |
| Missing | 3 (21) | 3 (25) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Yeh, C.H.; Kawi, J.; Grant, L.; Huang, X.; Wu, H.; Hardwicke, R.L.; Christo, P.J. Self-Guided Smartphone Application to Manage Chronic Musculoskeletal Pain: A Randomized, Controlled Pilot Trial. Int. J. Environ. Res. Public Health 2022, 19, 14875. https://doi.org/10.3390/ijerph192214875
Yeh CH, Kawi J, Grant L, Huang X, Wu H, Hardwicke RL, Christo PJ. Self-Guided Smartphone Application to Manage Chronic Musculoskeletal Pain: A Randomized, Controlled Pilot Trial. International Journal of Environmental Research and Public Health. 2022; 19(22):14875. https://doi.org/10.3390/ijerph192214875
Chicago/Turabian StyleYeh, Chao Hsing, Jennifer Kawi, Lauren Grant, Xinran Huang, Hulin Wu, Robin L. Hardwicke, and Paul J. Christo. 2022. "Self-Guided Smartphone Application to Manage Chronic Musculoskeletal Pain: A Randomized, Controlled Pilot Trial" International Journal of Environmental Research and Public Health 19, no. 22: 14875. https://doi.org/10.3390/ijerph192214875
APA StyleYeh, C. H., Kawi, J., Grant, L., Huang, X., Wu, H., Hardwicke, R. L., & Christo, P. J. (2022). Self-Guided Smartphone Application to Manage Chronic Musculoskeletal Pain: A Randomized, Controlled Pilot Trial. International Journal of Environmental Research and Public Health, 19(22), 14875. https://doi.org/10.3390/ijerph192214875






