Exercise Training Program Improves Subjective Sleep Quality and Physical Fitness in Severely Obese Bad Sleepers
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Patients and Recruitment
2.3. Measurements
2.3.1. Sleep Quality Measurements
2.3.2. Anthropometric Parameters
2.3.3. Physical Fitness
2.3.4. Exercise Training Intervention
2.4. Data Analysis
3. Results
4. Discussion
5. Limitations
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Hale, L.; Emanuele, E.; James, S. Recent updates in the social and environmental determinants of sleep health. Curr. Sleep. Med. Rep. 2015, 1, 212–217. [Google Scholar] [CrossRef] [PubMed]
- Lim, D.-K.; Baek, K.-O.; Chung, I.-S.; Lee, M.-Y. Factors related to sleep disorders among male firefighters. Ann. Occup. Environ. Med. 2014, 26, 11. [Google Scholar] [CrossRef] [PubMed]
- Thielmann, B.; Schierholz, R.S.; Böckelmann, I. Subjective and Objective Consequences of Stress in Subjects with Subjectively Different Sleep Quality—A Cross-Sectional Study. Int. J. Environ. Res. Public Health 2021, 18, 9990. [Google Scholar] [CrossRef] [PubMed]
- Chaput, J.-P.; Dutil, C.; Featherstone, R.; Ross, R.; Giangregorio, L.; Saunders, T.J.; Janssen, I.; Poitras, V.J.; Kho, M.E.; Ross-White, A. Sleep duration and health in adults: An overview of systematic reviews. Appl. Physiol. Nutr. Metab. 2020, 45, S218–S231. [Google Scholar] [CrossRef]
- Vail-Smith, K.; Felts, W.M.; Becker, C. Relationship between sleep quality and health risk behaviors in undergraduate college students. Coll. Stud. J. 2009, 43, 924–930. [Google Scholar]
- Gadie, A.; Shafto, M.; Leng, Y.; Kievit, R.A. How are age-related differences in sleep quality associated with health outcomes? An epidemiological investigation in a UK cohort of 2406 adults. BMJ Open 2017, 7, e014920. [Google Scholar] [CrossRef]
- Spiesshoefer, J.; Linz, D.; Skobel, E.; Arzt, M.; Stadler, S.; Schoebel, C.; Fietze, I.; Penzel, T.; Sinha, A.-M.; Fox, H. Sleep–the yet underappreciated player in cardiovascular diseases: A clinical review from the German Cardiac Society Working Group on Sleep Disordered Breathing. Eur. J. Prev. Cardiol. 2021, 28, 189–200. [Google Scholar] [CrossRef]
- Anam, M.R.; Akter, S.; Hossain, F.; Bonny, S.Q.; Akter, J.; Zhang, C.; Rahman, M.; Mian, M.; Basher, A. Association of sleep duration and sleep quality with overweight/obesity among adolescents of Bangladesh: A multilevel analysis. BMC Public Health 2022, 22, 374. [Google Scholar] [CrossRef]
- Li, W.; Chen, D.; Ruan, W.; Peng, Y.; Lu, Z.; Wang, D. Associations of depression, sleep disorder with total and cause-specific mortality: A prospective cohort study. J. Affect. Disord. 2022, 298, 134–141. [Google Scholar] [CrossRef]
- Yang, L.; Xi, B.; Zhao, M.; Magnussen, C.G. Association of sleep duration with all-cause and disease-specific mortality in US adults. J. Epidemiol. Commun. Health 2021, 75, 556–561. [Google Scholar] [CrossRef]
- Chouchou, F.; Augustini, M.; Caderby, T.; Caron, N.; Turpin, N.A.; Dalleau, G. The importance of sleep and physical activity on well-being during COVID-19 lockdown: Reunion island as a case study. Sleep Med. 2021, 77, 297–301. [Google Scholar] [CrossRef] [PubMed]
- Hillman, D.R.; Lack, L.C. Public health implications of sleep loss: The community burden. Med. J. Aust. 2013, 199, S7–S10. [Google Scholar] [CrossRef] [PubMed]
- Streatfeild, J.; Smith, J.; Mansfield, D.; Pezzullo, L.; Hillman, D. The social and economic cost of sleep disorders. Sleep 2021, 44, zsab132. [Google Scholar] [CrossRef] [PubMed]
- Chattu, V.K.; Manzar, M.D.; Kumary, S.; Burman, D.; Spence, D.W.; Pandi-Perumal, S.R. The Global Problem of Insufficient Sleep and Its Serious Public Health Implications. Healthcare 2019, 7, 1. [Google Scholar] [CrossRef]
- Cappuccio, F.P.; Taggart, F.M.; Kandala, N.-B.; Currie, A.; Peile, E.; Stranges, S.; Miller, M.A. Meta-analysis of short sleep duration and obesity in children and adults. Sleep 2008, 31, 619–626. [Google Scholar] [CrossRef]
- Wu, Y.; Zhai, L.; Zhang, D. Sleep duration and obesity among adults: A meta-analysis of prospective studies. Sleep Med. 2014, 15, 1456–1462. [Google Scholar] [CrossRef]
- Palm, A.; Janson, C.; Lindberg, E. The impact of obesity and weight gain on development of sleep problems in a population-based sample. Sleep Med. 2015, 16, 593–597. [Google Scholar] [CrossRef]
- Rahe, C.; Czira, M.E.; Teismann, H.; Berger, K. Associations between poor sleep quality and different measures of obesity. Sleep Med. 2015, 16, 1225–1228. [Google Scholar] [CrossRef]
- Sweatt, S.K.; Gower, B.A.; Chieh, A.Y.; Liu, Y.; Li, L. Sleep quality is differentially related to adiposity in adults. Psychoneuroendocrinology 2018, 98, 46–51. [Google Scholar] [CrossRef]
- Fatima, Y.; Doi, S.A.; Mamun, A. Sleep quality and obesity in young subjects: A meta-analysis. Obes. Rev. 2016, 17, 1154–1166. [Google Scholar] [CrossRef]
- Magee, C.A.; Reddy, P.; Robinson, L.; McGregor, A. Sleep quality subtypes and obesity. Health Psychol. 2016, 35, 1289–1297. [Google Scholar] [CrossRef] [PubMed]
- Zuraikat, F.M.; Makarem, N.; Liao, M.; St-Onge, M.P.; Aggarwal, B. Measures of poor sleep quality are associated with higher energy intake and poor diet quality in a diverse sample of women from the go red for women strategically focused research network. J. Am. Heart Assoc. 2020, 9, e014587. [Google Scholar] [CrossRef] [PubMed]
- Wang, F.; Boros, S. The effect of physical activity on sleep quality: A systematic review. Eur. J. Physiother. 2021, 23, 11–18. [Google Scholar] [CrossRef]
- Ezati, M.; Keshavarz, M.; Barandouzi, Z.A.; Montazeri, A. The effect of regular aerobic exercise on sleep quality and fatigue among female student dormitory residents. BMC Sports Sci. Med. Rehabil. 2020, 12, 44. [Google Scholar] [CrossRef]
- Taheri, M.; Irandoust, K. The exercise-induced weight loss improves self-reported quality of sleep in obese elderly women with sleep disorders. Sleep Hypn. 2018, 20, 54–59. [Google Scholar] [CrossRef]
- Min, L.; Wang, D.; You, Y.; Fu, Y.; Ma, X. Effects of High-Intensity Interval Training on Sleep: A Systematic Review and Meta-Analysis. Int. J. Environ. Res. Public Health 2021, 18, 10973. [Google Scholar] [CrossRef]
- Oppert, J.m.; Bellicha, A.; van Baak, M.A.; Battista, F.; Beaulieu, K.; Blundell, J.E.; Carraça, E.V.; Encantado, J.; Ermolao, A.; Pramono, A. Exercise training in the management of overweight and obesity in adults: Synthesis of the evidence and recommendations from the European Association for the Study of Obesity Physical Activity Working Group. Obes. Rev. 2021, 22, e13273. [Google Scholar] [CrossRef]
- Bellicha, A.; van Baak, M.A.; Battista, F.; Beaulieu, K.; Blundell, J.E.; Busetto, L.; Carraça, E.V.; Dicker, D.; Encantado, J.; Ermolao, A. Effect of exercise training on weight loss, body composition changes, and weight maintenance in adults with overweight or obesity: An overview of 12 systematic reviews and 149 studies. Obes. Rev. 2021, 22, e13256. [Google Scholar] [CrossRef]
- Delgado-Floody, P.; Latorre-Román, P.Á.; Jerez-Mayorga, D.; Caamaño-Navarrete, F.; Cano-Montoya, J.; Laredo-Aguilera, J.A.; Carmona-Torres, J.M.; Cobo-Cuenca, A.I.; Pozuelo-Carrascosa, D.P.; Álvarez, C. Poor sleep quality decreases concurrent training benefits in markers of metabolic syndrome and quality of life of morbidly obese patients. Int. J. Environ. Res. Public Health 2020, 17, 6804. [Google Scholar] [CrossRef]
- Buysse, D.J.; Reynolds III, C.F.; Monk, T.H.; Berman, S.R.; Kupfer, D.J. The Pittsburgh Sleep Quality Index: A new instrument for psychiatric practice and research. Psychiatry Res. 1989, 28, 193–213. [Google Scholar] [CrossRef]
- Toor, P.; Kim, K.; Buffington, C.K. Sleep quality and duration before and after bariatric surgery. Obes. Surg. 2012, 22, 890–895. [Google Scholar] [CrossRef] [PubMed]
- Sturm, R. Increases in morbid obesity in the USA: 2000–2005. Public Health 2007, 121, 492–496. [Google Scholar] [CrossRef] [PubMed]
- Campos, G.; Khoraki, J.; Browning, M.; Pessoa, B.; Mazzini, G.; Wolfe, L. Changes in utilization of bariatric surgery in the United States from 1993 to 2016. Ann. Surg. 2020, 271, 201–209. [Google Scholar] [CrossRef] [PubMed]
- de Souza, S.A.F.; Faintuch, J.; Fabris, S.M.; Nampo, F.K.; Luz, C.; Fabio, T.L.; Sitta, I.S.; de Batista Fonseca, I.C. Six-minute walk test: Functional capacity of severely obese before and after bariatric surgery. Surg. Obes. Relat. Dis. 2009, 5, 540–543. [Google Scholar] [CrossRef] [PubMed]
- Norman, K.; Stobäus, N.; Gonzalez, M.C.; Schulzke, J.-D.; Pirlich, M. Hand grip strength: Outcome predictor and marker of nutritional status. Clin. Nutr. 2011, 30, 135–142. [Google Scholar] [CrossRef]
- Álvarez, C.; Ramírez-Campillo, R.; Lucia, A.; Ramírez-Vélez, R.; Izquierdo, M. Concurrent exercise training on hyperglycemia and comorbidities associated: Non-responders using clinical cutoff points. Scand. J. Med. Sci. Sports 2019, 29, 952–967. [Google Scholar] [CrossRef]
- Brzycki, M. Strength testing—Predicting a one-rep max from reps-to-fatigue. J. Phys. Edu. Recreat. Dance 1993, 64, 88–90. [Google Scholar] [CrossRef]
- Hopkins, W.G.; Marshall, S.W.; Batterham, A.M.; Hanin, J. Progressive statistics for studies in sports medicine and exercise science. Med. Sci. Sports Exerc. 2009, 41, 3–13. [Google Scholar] [CrossRef]
- Mendelson, M.; Borowik, A.; Michallet, A.S.; Perrin, C.; Monneret, D.; Faure, P.; Levy, P.; Pépin, J.L.; Wuyam, B.; Flore, P. Sleep quality, sleep duration and physical activity in obese adolescents: Effects of exercise training. Pediatr. Obes. 2016, 11, 26–32. [Google Scholar] [CrossRef]
- Rayward, A.T.; Duncan, M.J.; Brown, W.J.; Plotnikoff, R.C.; Burton, N.W. A cross-sectional cluster analysis of the combined association of physical activity and sleep with sociodemographic and health characteristics in mid-aged and older adults. Maturitas 2017, 102, 56–61. [Google Scholar] [CrossRef]
- Kline, C.E.; Sui, X.; Hall, M.H.; Youngstedt, S.D.; Blair, S.N.; Earnest, C.P.; Church, T.S. Dose–response effects of exercise training on the subjective sleep quality of postmenopausal women: Exploratory analyses of a randomised controlled trial. BMJ Open 2012, 2, e001044. [Google Scholar] [CrossRef]
- Kline, C.E.; Crowley, E.P.; Ewing, G.B.; Burch, J.B.; Blair, S.N.; Durstine, J.L.; Davis, J.M.; Youngstedt, S.D. The effect of exercise training on obstructive sleep apnea and sleep quality: A randomized controlled trial. Sleep 2011, 34, 1631–1640. [Google Scholar] [CrossRef] [PubMed]
- Vanderlinden, J.; Boen, F.; Puyenbroeck, S.V.; van Uffelen, J. The effects of a real-life lifestyle program on physical activity and objective and subjective sleep in adults aged 55+ years. BMC Public Health 2022, 22, 353. [Google Scholar] [CrossRef]
- Saidi, O.; Rochette, E.; Bovet, M.; Merlin, E.; Duché, P. Acute intense exercise improves sleep and decreases next morning consumption of energy-dense food in adolescent girls with obesity and evening chronotype. Pediatr. Obes. 2020, 15, e12613. [Google Scholar] [CrossRef] [PubMed]
- Alarcón-Gómez, J.; Chulvi-Medrano, I.; Martin-Rivera, F.; Calatayud, J. Effect of High-Intensity Interval Training on Quality of Life, Sleep Quality, Exercise Motivation and Enjoyment in Sedentary People with Type 1 Diabetes Mellitus. Int. J. Environ. Res. Public Health 2021, 18, 12612. [Google Scholar] [CrossRef] [PubMed]
- Jiménez-García, J.D.; Hita-Contreras, F.; de la Torre-Cruz, M.J.; Aibar-Almazán, A.; Achalandabaso-Ochoa, A.; Fábrega-Cuadros, R.; Martínez-Amat, A. Effects of HIIT and MIIT suspension training programs on sleep quality and fatigue in older adults: Randomized controlled clinical trial. Int. J. Environ. Res. Public Health 2021, 18, 1211. [Google Scholar] [CrossRef] [PubMed]
- Jurado-Fasoli, L.; De-la-O, A.; Molina-Hidalgo, C.; Migueles, J.H.; Castillo, M.J.; Amaro-Gahete, F.J. Exercise training improves sleep quality: A randomized controlled trial. Eur. J. Clin. Investig. 2020, 50, e13202. [Google Scholar] [CrossRef]
- Kishida, M.; Elavsky, S. An intensive longitudinal examination of daily physical activity and sleep in midlife women. Sleep Health 2016, 2, 42–48. [Google Scholar] [CrossRef]
- Li, J.; Zhang, Q.; Wang, Q.; Zhou, L.; Wan, X.; Zeng, X. The association between hand grip strenght and global PSQI score in the middleaged and elderly population. Sleep Biol. Rhythm. 2021, 19, 155–162. [Google Scholar] [CrossRef]
- Buchmann, N.; Spira, D.; Norman, K.; Demuth, I.; Eckardt, R.; Steinhagen-Thiessen, E. Sleep, muscle mass and muscle function in older people: A cross-sectional analysis based on data from the Berlin Aging Study II (BASE-II). Deutsch. Ärztebl. Int. 2016, 113, 253–260. [Google Scholar] [CrossRef]
- Vargas, C.A.; Guzmán-Guzmán, I.P.; Caamaño-Navarrete, F.; Jerez-Mayorga, D.; Chirosa-Ríos, L.J.; Delgado-Floody, P. Syndrome metabolic markers, fitness and body fat is associated with sleep quality in women with severe/morbid obesity. Int. J. Environ. Res. Public Health 2021, 18, 9294. [Google Scholar] [CrossRef] [PubMed]
- Leonel, L.d.S.; Tozetto, W.R.; Delevatti, R.S.; Del Duca, G.F. Effects of combined training with linear periodization and non-periodization on sleep quality of adults with obesity. Res. Q. Exerc. Sport 2022, 93, 171–179. [Google Scholar] [CrossRef] [PubMed]
- Peng, X.; Liu, N.; Zhang, X.; Bao, X.; Xie, Y.; Huang, J.; Wang, P.; Du, Q. Associations between objectively assessed physical fitness levels and sleep quality in community-dwelling elderly people in South China. Sleep Breath. 2019, 23, 679–685. [Google Scholar] [CrossRef] [PubMed]
- Sanchez-Lastra, M.A.; Ding, D.; Dalene, K.-E.; Ekelund, U.; Tarp, J. Physical activity and mortality across levels of adiposity: A prospective cohort study from the UK Biobank. Mayo Clin. Proc. 2021, 96, 105–119. [Google Scholar] [CrossRef] [PubMed]
- Saidi, O.; Colin, E.; Rance, M.; Doré, E.; Pereira, B.; Duché, P. Effect of morning versus evening exercise training on sleep, physical activity, fitness, fatigue and quality of life in overweight and obese adults. Chronobiol. Int. 2021, 38, 1537–1548. [Google Scholar] [CrossRef]
- D’Amuri, A.; Sanz, J.M.; Capatti, E.; Di Vece, F.; Vaccari, F.; Lazzer, S.; Zuliani, G.; Dalla Nora, E.; Passaro, A. Effectiveness of high-intensity interval training for weight loss in adults with obesity: A randomised controlled non-inferiority trial. BMJ Open Sport Exerc. Med. 2021, 7, e001021. [Google Scholar] [CrossRef]
- De Carvalho, F.G.; Brandao, C.F.C.; Batitucci, G.; de Oliveira Souza, A.; Ferrari, G.D.; Alberici, L.C.; Muñoz, V.R.; Pauli, J.R.; De Moura, L.P.; Ropelle, E.R. Taurine supplementation associated with exercise increases mitochondrial activity and fatty acid oxidation gene expression in the subcutaneous white adipose tissue of obese women. Clin. Nutr. 2021, 40, 2180–2187. [Google Scholar] [CrossRef]
| Participant Characteristics | Sample n = 30 |
|---|---|
| Age | 39.30 ± 11.62 |
| Sex: Female/Male | 26/4 |
| Anthropometric | |
| Size (m) | 1.59 ± 0.08 |
| Body mass (kg) | 108.82 ± 21.48 |
| BMI (kg/m2) | 42.75 ± 5.27 |
| Obesity category | |
| Moderate–Severe (30–39.9 kg/m2), n (%) | 10 (33.33) |
| Morbid obesity (≥40 kg/m2), n (%) | 20 (66.66) |
| Physical fitness | |
| 6-MWT (m) | 517 ± 95.48 |
| HGS (kg) | 31.05 ± 11.03 |
| PSQI test | |
| PSQI score | 5.96 ± 3.71 |
| Sleeper group | |
| Good sleepers n (%) | 15 (50.0) |
| Bad sleepers n (%) | 15 (50.0) |
| Groups | Good Sleepers (Control) n = 15 | Bad sleepers (Cases) n = 15 | ||||||
|---|---|---|---|---|---|---|---|---|
| Participant Characteristics | Pre-Intervention | Post-Intervention | p-Value | Cohen d | Pre-Intervention | Post-Intervention | p-Value | Cohen d |
| Age | 40.00 ± 14.26 | - | - | 40.50 ± 11.23 | - | 0.570 | ||
| Sex Female/Male | 14/1 | - | 12/3 | - | 0.283 | |||
| Anthropometric | ||||||||
| Size (m) | 1.58 ± 0.068 | - | 1.60 ± 0.106 | - | 0.546 | |||
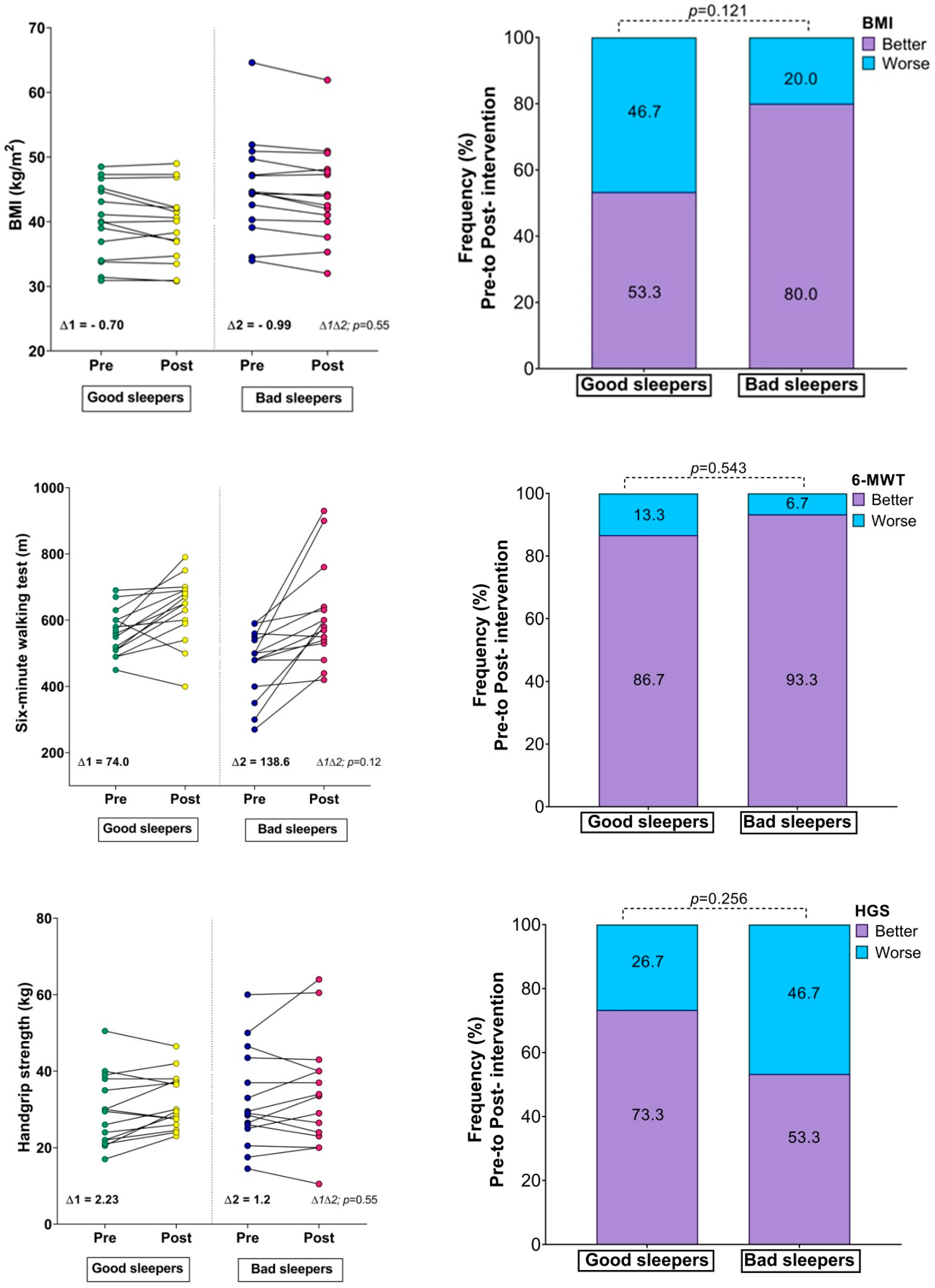
| Body mass (kg) | 102.30 ± 20.0 | 99.50 ± 19.0 | 0.068 | 0.09 | 116.37 ± 21.31 * | 113.91 ± 21.06 ¥ | 0.008 | 0.12 |
| BMI (kg/m2) | 40.20 ± 6.0 | 39.50 ± 6.0 | 0.080 | 0.12 | 45.32 ± 7.51 * | 44.33 ± 7.28 ¥ | 0.005 | 0.13 |
| Obesity category | 0.121 | |||||||
| 35–39.9 kg/m2 | 7 (46.7) | - | 3 (20.0) | - | ||||
| ≥40 kg/m2 | 8 (53.3) | - | 12 (80.0) | - | ||||
| Physical fitness | ||||||||
| 6MWT (m) | 561.33 ± 68.75 | 635.33 ± 98.91 | 0.003 | 0.87 | 472.66 ± 99.74 | 611.33 ± 148.75 | 0.001 | 1.10 |
| HGS (kg) | 29.63 ± 9.29 | 31.86 ± 7.17 | 0.049 | 0.27 | 32.46 ± 12.71 | 33.66 ± 14.66 | 0.404 | 0.09 |
| PSQI test | ||||||||
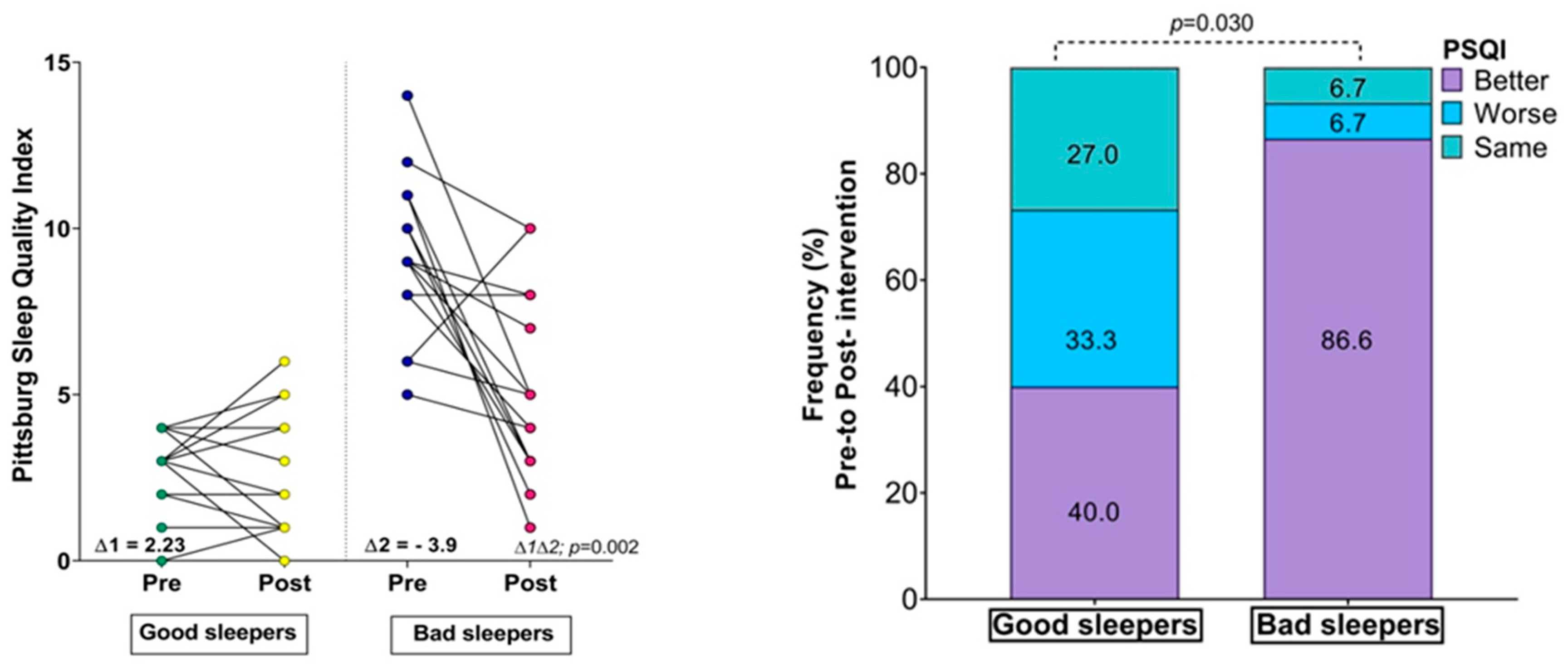
| PSQI score | 2.80 ± 1.20 | 2.66 ± 1.79 | 0.757 | 0.09 | 9.13 ± 2.38 * | 5.2 ± 2.80 ¥ | 0.001 | 1.51 |
| Sleep Quality Dimensions | ||||||||
| Subjective sleep quality (score) | 0.13 ± 0.35 | 0.26 ± 0.59 | 0.334 | 0.27 | 0.93 ± 0.70 | 0.20 ± 0.41 | <0.001 | 1.27 |
| Sleep latency(score) | 0.60 ± 0.50 | 0.66 ± 0.61 | 0.581 | 0.11 | 1.80 ± 0.77 | 1.2 ± 0.67 | 0.045 | 0.83 |
| Sleep duration(score) | 0.66 ± 0.61 | 0.4 ± 0.50 | 0.103 | 0.47 | 1.66 ± 1.04 | 0.8 ± 1.01 | 0.031 | 0.84 |
| Habitual sleep efficiency (score) | 0.33 ± 0.48 | 0.53 ± 0.63 | 0.271 | 0.40 | 2.26 ± 1.09 | 1.13 ± 1.18 | 0.015 | 0.99 |
| Sleep disturbances(score) | 0.66 ± 0.48 | 0.6 ± 0.50 | 0.334 | 0.12 | 1.2 ± 0.41 | 1.0 ± 0 | 0.082 | 0.70 |
| Sleeping medication (score) | 0 ± 0 | 0 ± 0 | - | 0.6 ± 0.91 | 0.33 ± 0.72 | 0.217 | 0.33 | |
| Daytime dysfunction (score) | 0.4 ± 0.73 | 0.2 ± 0.41 | 0.082 | 0.34 | 0.66 ± 0.61 | 0.53 ± 0.51 | 0.498 | 0.23 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Delgado-Floody, P.; Caamaño Navarrete, F.; Chirosa-Ríos, L.; Martínez-Salazar, C.; Vargas, C.A.; Guzmán-Guzmán, I.P. Exercise Training Program Improves Subjective Sleep Quality and Physical Fitness in Severely Obese Bad Sleepers. Int. J. Environ. Res. Public Health 2022, 19, 13732. https://doi.org/10.3390/ijerph192113732
Delgado-Floody P, Caamaño Navarrete F, Chirosa-Ríos L, Martínez-Salazar C, Vargas CA, Guzmán-Guzmán IP. Exercise Training Program Improves Subjective Sleep Quality and Physical Fitness in Severely Obese Bad Sleepers. International Journal of Environmental Research and Public Health. 2022; 19(21):13732. https://doi.org/10.3390/ijerph192113732
Chicago/Turabian StyleDelgado-Floody, Pedro, Felipe Caamaño Navarrete, Luis Chirosa-Ríos, Cristian Martínez-Salazar, Claudia Andrea Vargas, and Iris Paola Guzmán-Guzmán. 2022. "Exercise Training Program Improves Subjective Sleep Quality and Physical Fitness in Severely Obese Bad Sleepers" International Journal of Environmental Research and Public Health 19, no. 21: 13732. https://doi.org/10.3390/ijerph192113732
APA StyleDelgado-Floody, P., Caamaño Navarrete, F., Chirosa-Ríos, L., Martínez-Salazar, C., Vargas, C. A., & Guzmán-Guzmán, I. P. (2022). Exercise Training Program Improves Subjective Sleep Quality and Physical Fitness in Severely Obese Bad Sleepers. International Journal of Environmental Research and Public Health, 19(21), 13732. https://doi.org/10.3390/ijerph192113732










