Comparison of the Effectiveness and Safety of Heterologous Booster Doses with Homologous Booster Doses for SARS-CoV-2 Vaccines: A Systematic Review and Meta-Analysis
Abstract
:1. Introduction
2. Methods
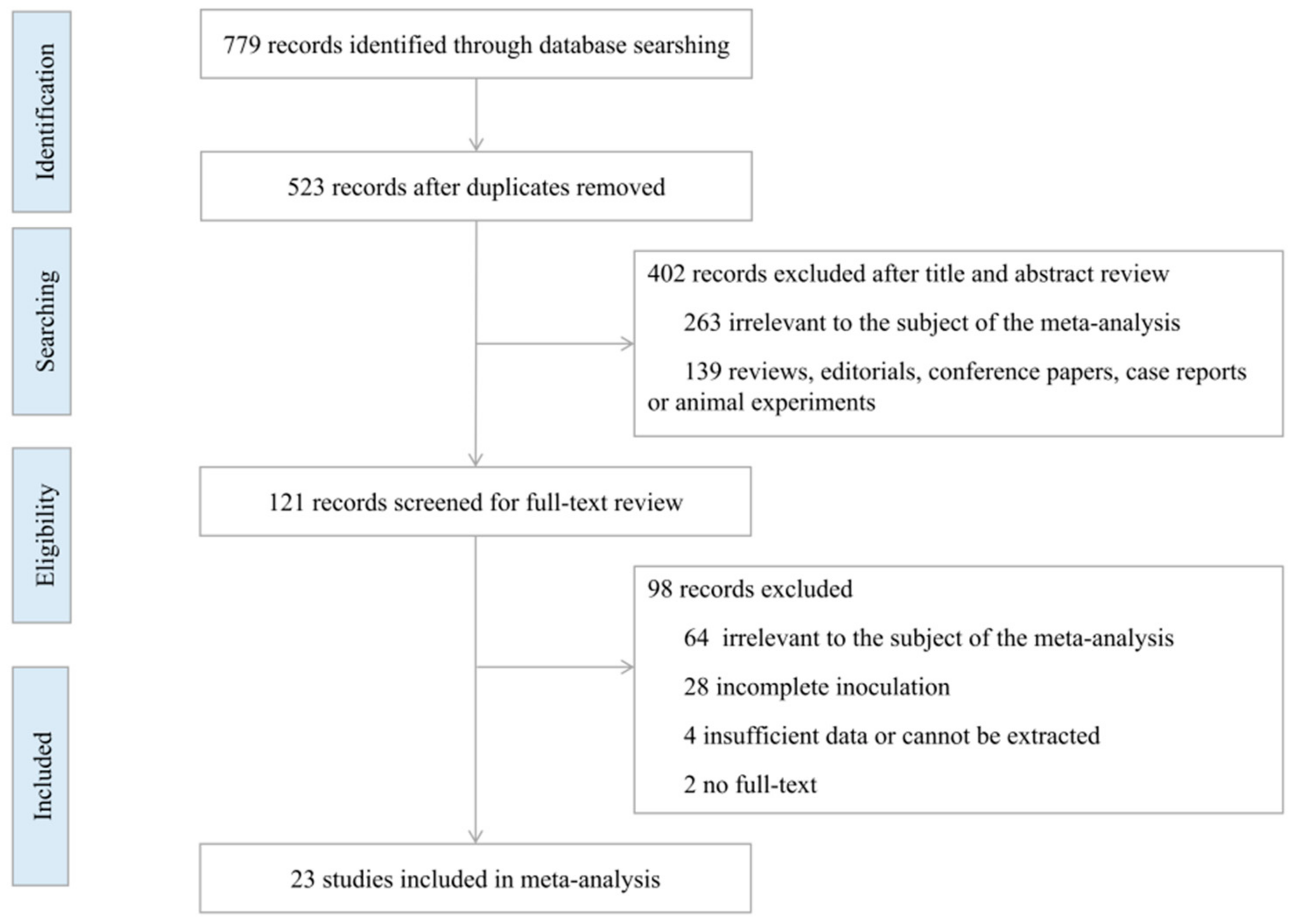
2.1. Search Strategy and Selection Criteria
2.2. Data Extraction
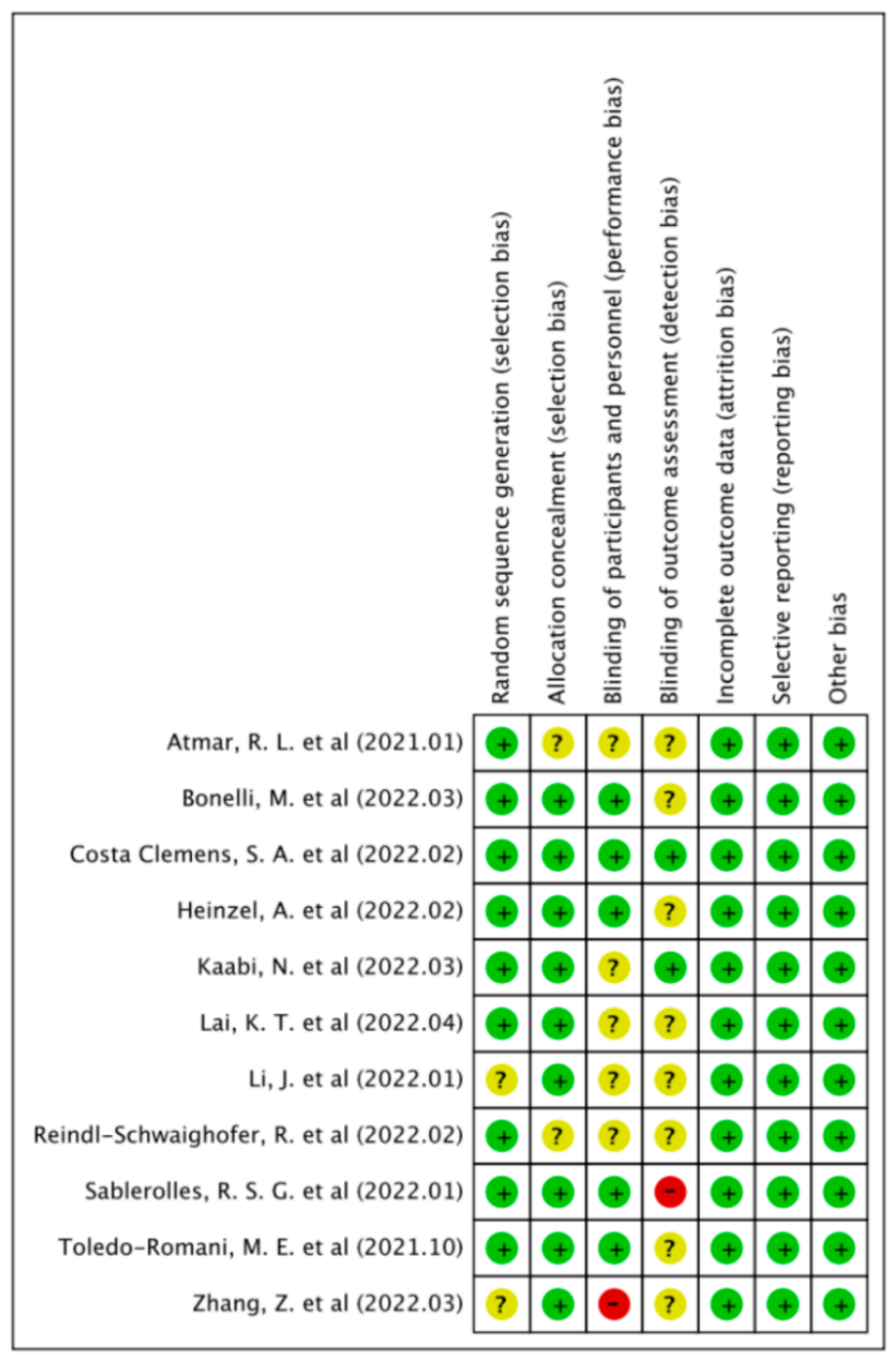
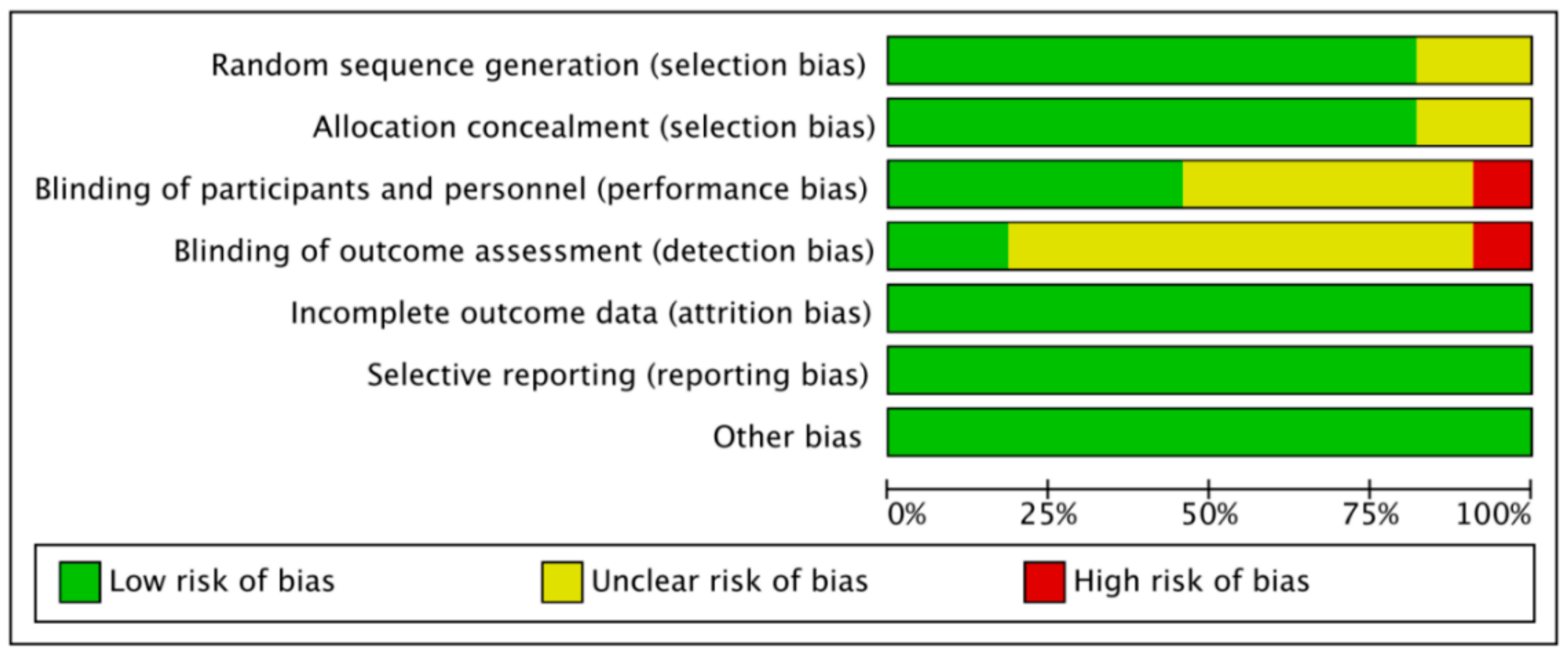
2.3. Quality Assessment
2.4. Data Synthesis and Statistical Analysis
3. Results
3.1. Basic Characteristics
3.2. Comparison of Safety between Heterologous Booster and Homologous Booster
3.3. Comparison of Immunogenicity between Heterologous Booster and Homologous Booster
3.4. Comparison of Vaccine Effectiveness between Heterologous Booster and Homologous Booster
3.5. Quality Evaluation and Publication Bias
| First Author (Published Time) | Selection | Comparability | Outcome | Number of Stars | Risk of Bias | |||||
|---|---|---|---|---|---|---|---|---|---|---|
| Representativeness of the Exposed Cohort | Selection of the Non-Exposed Cohort | Ascertainment of Exposure | Demonstration that Outcome of Interest Was Not Present at Start of Study | Comparability of Cohorts on the Basis of the Design or Analysis | Assessment of Outcome | Was Follow-Up Long Enough for Outcomes to Occur | Adequacy of Follow-Up of Cohorts | |||
| Ai, J. et al., 2022 [25] | 0 | 0 | 1 | 1 | 2 | 1 | 1 | 1 | 7 | Low |
| Natarajan, K. et al., 2022 [28] | 1 | 1 | 1 | 1 | 2 | 1 | 1 | 1 | 9 | Low |
| Jara, A. et al., 2022 [29] | 1 | 1 | 1 | 1 | 2 | 1 | 1 | 1 | 9 | Low |
| Menni, C. et al., 2022 [32] | 1 | 1 | 1 | 1 | 2 | 1 | 1 | 1 | 9 | Low |
| Khong, K. W. et al., 2022 [33] | 1 | 1 | 1 | 1 | 2 | 1 | 1 | 1 | 9 | Low |
| Çağlayan, D. et al., 2022 [34] | 1 | 1 | 1 | 1 | 2 | 1 | 1 | 1 | 9 | Low |
| Angkasekwinai, N. et al., 2022 [38] | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 8 | Low |
| Mok, C. K. P. et al., 2022 [39] | 1 | 1 | 1 | 1 | 2 | 1 | 1 | 1 | 9 | Low |
| Starrfelt, J. et al., 2022 [36] | 1 | 1 | 1 | 1 | 2 | 1 | 1 | 1 | 9 | Low |
| Baum, U. et al., 2022 [44] | 1 | 1 | 1 | 1 | 2 | 1 | 1 | 1 | 9 | Low |
| First Author (Published Time) | Selection | Comparability | Exposure | Number of Stars | Risk of Bias | |||||
|---|---|---|---|---|---|---|---|---|---|---|
| Is the Case Definition Adequate? | Representativeness of the Cases | Selection of Controls | Definition of Controls | Comparability of Cases and Controls on the Basis of the Design or Analysis | Ascertainment of Exposure | Same Method of Ascertainment for Cases and Controls | Non-Response Rate | |||
| Ranzani, Otavio T. et al., 2022 [42] | 1 | 1 | 1 | 1 | 2 | 1 | 1 | 0 | 8 | Low |
| Andrews, N. et al., 2022 [43] | 1 | 1 | 1 | 1 | 2 | 1 | 1 | 0 | 8 | Low |
4. Discussion
Differences in Effectiveness between Homologous and Heterologous Boosters for SARS-CoV-2 Variants
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| SARS-Cov-2 | severe acute respiratory syndrome coronavirus 2 |
| COVID-19 | coronavirus disease 2019 |
| VE | vaccine effectiveness |
| CI | confidence interval |
| OR | odds ratios |
| ICU | intensive care unit |
| GMTs | geometric mean neutralizing titers |
| SMD | standard mean difference |
| PRISMA | preferred reporting items for systematic reviews and meta-analyses |
| WHO | World Health Organization |
| rt-PCR | reverse-transcription polymerase chain reaction |
| RCTs | randomized controlled trial |
| NAAT | nucleic acid amplification test |
References
- Akande, O.W.; Akande, T.M. COVID-19 pandemic: A global health burden. Niger. Postgrad. Med. J. 2020, 27, 147–155. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. WHO Coronavirus (COVID-19) Dashboard. 2022. Available online: https://covid19.who.int (accessed on 10 July 2022).
- World Health Organization. Coronavirus Disease (COVID-19): Vaccines. 2022. Available online: https://www.who.int/news-room/questions-and-answers/item/coronavirus-disease-(covid-19)-vaccines?adgroupsurvey=%7Badgroupsurvey%7D&gclid=CjwKCAjw_o-HBhAsEiwANqYhp_ZinKdR5N3rlvVfpDQU_0xaeUGWru7XUg-RVhFvrLPo1iM19w4lzBoCHzQQAvD_BwE (accessed on 10 July 2022).
- Our World in Data. Coronavirus (COVID-19) Vaccinations. 2022. Available online: https://ourworldindata.org/covid-vaccinations (accessed on 10 July 2022).
- World Health Organization. Vaccine Equity. 2022. Available online: https://www.who.int/campaigns/vaccine-equity (accessed on 10 July 2022).
- World Health Organization. Strategy to Achieve Global COVID-19 Vaccination by Mid-2022. Available online: https://www.who.int/publications/m/item/strategy-to-achieve-global-covid-19-vaccination-by-mid-2022 (accessed on 10 July 2022).
- Feikin, D.R.; Higdon, M.M.; Abu-Raddad, L.J.; Andrews, N.; Araos, R.; Goldberg, Y.; Groome, M.; Huppert, A.; O’Brien, K.; Smith, P.G.; et al. Duration of effectiveness of vaccines against SARS-CoV-2 infection and COVID-19 disease: Results of a systematic review and meta-regression. Lancet 2022, 399, 924–944. [Google Scholar] [CrossRef]
- World Health Organization. Interim Statement on Booster Doses for COVID-19 Vaccination. 2022. Available online: https://www.who.int/news/item/22-12-2021-interim-statement-on-booster-doses-for-covid-19-vaccination---update-22-december-2021 (accessed on 10 July 2022).
- Krause, P.R.; Fleming, T.R.; Peto, R.; Longini, I.M.; Figueroa, J.P.; Sterne, J.A.C.; Cravioto, A.; Rees, H.; Higgins, J.P.T.; Boutron, I.; et al. Considerations in boosting COVID-19 vaccine immune responses. Lancet 2021, 398, 1377–1380. [Google Scholar] [CrossRef]
- World Health Organization. WHO SAGE Values Framework for the Allocation and Prioritization of COVID-19 Vaccination. 2022. Available online: https://www.who.int/publications/i/item/who-sage-values-framework-for-the-allocation-and-prioritization-of-covid-19-vaccination (accessed on 10 July 2022).
- Chiu, N.C.; Chi, H.; Tu, Y.K.; Huang, Y.N.; Tai, Y.L.; Weng, S.L.; Chang, L.; Huang, D.T.N.; Huang, F.Y.; Lin, C.Y. To mix or not to mix? A rapid systematic review of heterologous prime-boost covid-19 vaccination. Expert Rev. Vaccines 2021, 20, 1211–1220. [Google Scholar] [CrossRef]
- World Health Organization. Interim Recommendations for Heterologous COVID-19 Vaccine Schedules. Available online: https://www.who.int/publications/i/item/WHO-2019-nCoV-vaccines-SAGE-recommendation-heterologous-schedules (accessed on 10 July 2022).
- Au, W.Y.; Cheung, P.P.-H. Effectiveness of heterologous and homologous COVID-19 vaccine regimens: Living systematic review with network meta-analysis. Br. Med. J. Clin. Res. Ed. 2022, 377, e069989. [Google Scholar] [CrossRef]
- Li, J.; Hou, L.; Guo, X.; Jin, P.; Wu, S.; Zhu, J.; Pan, H.; Wang, X.; Song, Z.; Wan, J.; et al. Heterologous AD5-nCOV plus CoronaVac versus homologous CoronaVac vaccination: A randomized phase 4 trial. Nat. Med. 2022, 28, 401–409. [Google Scholar] [CrossRef]
- Li, J.X.; Wu, S.P.; Guo, X.L.; Tang, R.; Huang, B.Y.; Chen, X.Q.; Chen, Y.; Hou, L.H.; Liu, J.X.; Zhong, J.; et al. Safety and immunogenicity of heterologous boost immunisation with an orally administered aerosolised Ad5-nCoV after two-dose priming with an inactivated SARS-CoV-2 vaccine in Chinese adults: A randomised, open-label, single-centre trial. Lancet Respir. Med. 2022, 10, 739–748. [Google Scholar] [CrossRef]
- Ai, J.; Zhang, H.; Zhang, Q.; Zhang, Y.; Lin, K.; Fu, Z.; Song, J.; Zhao, Y.; Fan, M.; Wang, H.; et al. Recombinant protein subunit vaccine booster following two-dose inactivated vaccines dramatically enhanced anti-RBD responses and neutralizing titers against SARS-CoV-2 and Variants of Concern. Cell Res. 2022, 32, 103–106. [Google Scholar] [CrossRef]
- Zeng, G.; Wu, Q.; Pan, H.; Li, M.; Yang, J.; Wang, L.; Wu, Z.; Jiang, D.; Deng, X.; Chu, K.; et al. Immunogenicity and safety of a third dose of CoronaVac, and immune persistence of a two-dose schedule, in healthy adults: Interim results from two single-centre, double-blind, randomised, placebo-controlled phase 2 clinical trials. Lancet Infect. Dis. 2022, 22, 483–495. [Google Scholar] [CrossRef]
- Cao, Y.; Hao, X.; Wang, X.; Wu, Q.; Song, R.; Zhao, D.; Song, W.; Wang, Y.; Yisimayi, A.; Wang, W.; et al. Humoral immunogenicity and reactogenicity of CoronaVac or ZF2001 booster after two doses of inactivated vaccine. Cell Res. 2022, 32, 107–109. [Google Scholar] [CrossRef]
- Atmar, R.L.; Lyke, K.E.; Deming, M.E.; Jackson, L.A.; Branche, A.R.; Sahly, H.M.E.; Rostad, C.A.; Martin, J.M.; Johnston, C.; Rupp, R.E.; et al. Homologous and Heterologous Covid-19 Booster Vaccinations. N. Engl. J. Med. 2022, 386, 1046–1057. [Google Scholar] [CrossRef]
- World Health Organization. Status of COVID-19 Vaccines within WHO EUL/PQ Evaluation Process. 2022. Available online: https://extranet.who.int/pqweb/sites/default/files/documents/Status_COVID_VAX_07July2022.pdf (accessed on 10 July 2022).
- World Health Organization. WHO Validates 11th Vaccine for COVID-19. 2022. Available online: https://www.who.int/news/item/19-05-2022-who-validates-11th-vaccine-for-covid-19 (accessed on 10 July 2022).
- World Health Organization. COVID-19 Vaccines with WHO Emergency Use Listing. 2022. Available online: https://extranet.who.int/pqweb/vaccines/vaccinescovid-19-vaccine-eul-issued (accessed on 10 July 2022).
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ 2021, 372, n71. [Google Scholar] [CrossRef]
- Atmar, R.L.; Lyke, K.E.; Deming, M.E.; Jackson, L.A.; Branche, A.R.; Sahly, H.M.E.; Rostad, C.A.; Martin, J.M.; Johnston, C.; Rupp, R.E.; et al. Heterologous SARS-CoV-2 Booster Vaccinations—Preliminary Report. medRxiv 2021. [Google Scholar] [CrossRef]
- Ai, J.; Zhang, H.; Zhang, Y.; Lin, K.; Zhang, Y.; Wu, J.; Wan, Y.; Huang, Y.; Song, J.; Fu, Z.; et al. Omicron variant showed lower neutralizing sensitivity than other SARS-CoV-2 variants to immune sera elicited by vaccines after boost. Emerg. Microbes infect. 2022, 11, 337–343. [Google Scholar] [CrossRef]
- Reindl-Schwaighofer, R.; Heinzel, A.; Mayrdorfer, M.; Jabbour, R.; Hofbauer, T.M.; Merrelaar, A.; Eder, M.; Regele, F.; Doberer, K.; Spechtl, P.; et al. Comparison of SARS-CoV-2 Antibody Response 4 Weeks after Homologous vs Heterologous Third Vaccine Dose in Kidney Transplant Recipients: A Randomized Clinical Trial. JAMA Intern. Med. 2022, 182, 165–171. [Google Scholar] [CrossRef]
- Clemens, S.A.C.; Weckx, L.; Clemens, R.; Mendes, A.V.A.; Souza, A.R.; Silveira, M.B.V.; da Guarda, S.N.F.; de Nobrega, M.M.; de Moraes Pinto, M.I.; Gonsalez, I.G.S.; et al. Heterologous versus homologous COVID-19 booster vaccination in previous recipients of two doses of CoronaVac COVID-19 vaccine in Brazil (RHH-001): A phase 4, non-inferiority, single blind, randomised study. Lancet 2022, 399, 521–529. [Google Scholar] [CrossRef]
- Natarajan, K.; Prasad, N.; Dascomb, K.; Irving, S.A.; Yang, D.H.; Gaglani, M.; Klein, N.P.; Desilva, M.B.; Ong, T.C.; Grannis, S.J.; et al. Effectiveness of Homologous and Heterologous COVID-19 Booster Doses Following 1 Ad.26.COV2.S (Janssen [Johnson & Johnson]) Vaccine Dose against COVID-19-Associated Emergency Department and Urgent Care Encounters and Hospitalizations among Adults-VISION Network, 10 States, December 2021–March 2022. MMWR Morb. Mortal. Wkly. Rep. 2022, 71, 495–502. [Google Scholar]
- Jara, A.; Undurraga, E.A.; Zubizarreta, J.R.; González, C.; Pizarro, A.; Acevedo, J.; Leo, K.; Paredes, F.; Bralic, T.; Vergara, V.; et al. Effectiveness of homologous and heterologous booster doses for an inactivated SARS-CoV-2 vaccine: A large-scale prospective cohort study. Lancet Glob. Health 2022, 10, e798–e806. [Google Scholar] [CrossRef]
- Sablerolles, R.S.G.; Rietdijk, W.J.R.; Goorhuis, A.; Postma, D.F.; Visser, L.G.; Geers, D.; Schmitz, K.S.; Garrido, H.M.G.; Koopmans, M.P.G.; Dalm, V.A.S.H.; et al. Immunogenicity and Reactogenicity of Vaccine Boosters after Ad26.COV2.S Priming. N. Engl. J. Med. 2022, 386, 951–963. [Google Scholar] [CrossRef]
- Lai, K.T.-W.; Loong, E.Y.-T.L.W.; Fung, T.L.-H.; Luk, L.W.-P.; Lau, C.-C.; Zee, J.S.-T.; Ma, E.S.-K.; Tang, B.S.-F. Safety and Immunogenicity of a Booster Vaccination by CoronaVac or BNT162b2 in Previously Two-Dose Inactivated Virus Vaccinated Individuals with Negative Neutralizing Antibody. Vaccines 2022, 10, 556. [Google Scholar] [CrossRef]
- Menni, C.; May, A.; Polidori, L.; Louca, P.; Wolf, J.; Capdevila, J.; Hu, C.; Ourselin, S.; Steves, C.J.; Valdes, A.M.; et al. COVID-19 vaccine waning and effectiveness and side-effects of boosters: A prospective community study from the ZOE COVID Study. Lancet Infect. Dis. 2022, 22, 1002–1010. [Google Scholar] [CrossRef]
- Khong, K.W.; Liu, D.; Leung, K.Y.; Lu, L.; Lam, H.Y.; Chen, L.; Chan, P.C.; Lam, H.M.; Xie, X.; Zhang, R.; et al. Antibody Response of Combination of BNT162b2 and CoronaVac Platforms of COVID-19 Vaccines against Omicron Variant. Vaccines 2022, 10, 160. [Google Scholar] [CrossRef] [PubMed]
- Çağlayan, D.; Süner, A.F.; Şiyve, N.; Güzel, I.; Irmak, Ç.; Işik, E.; Appak, O.; Celik, M.; Ozturk, G.; Cavus, S.A.; et al. An analysis of antibody response following the second dose of CoronaVac and humoral response after booster dose with BNT162b2 or CoronaVac among healthcare workers in Turkey. J. Med. Virol. 2022, 94, 2212–2221. [Google Scholar] [CrossRef] [PubMed]
- Bonelli, M.; Mrak, D.; Tobudic, S.; Sieghart, D.; Mandl, P.; Kornek, B.; Simader, E.; Radner, H.; Perkmann, T.; Haslacher, H. Additional Heterologous versus Homologous Booster Vaccination in Immunosuppressed Patients without SARS-CoV-2 Antibody Seroconversion after Primary mRNA Vaccination: A Randomized Controlled Trial. Arthritis Rheumatol. 2021, 73, 4125–4126. [Google Scholar] [CrossRef]
- Starrfelt, J.; Danielsen, A.S.; Buanes, E.A.; Juvet, L.K.; Lyngstad, T.M.; Ro, G.Ø.I.; Veneti, L.; Meijerink, H. Age and product dependent vaccine effectiveness against SARS-CoV-2 infection and hospitalisation among adults in Norway: A national cohort study, July–November 2021. medRxiv 2022. [Google Scholar] [CrossRef]
- Heinzel, A.; Schretzenmeier, E.; Regele, F.; Hu, K.; Raab, L.; Eder, M.; Aigner, C.; Jabbour, R.; Aschauer, C.; Stefanski, A.L.; et al. Three-month follow-up of heterologous vs. homologous third vaccination in kidney transplant recipients. medRxiv 2022. [Google Scholar] [CrossRef]
- Angkasekwinai, N.; Niyomnaitham, S.; Sewatanon, J.; Phumiamorn, S.; Sukapirom, K.; Senawong, S.; Toh, Z.Q.; Umrod, P.; Somporn, T.; Chumpol, S.; et al. The immunogenicity and reactogenicity of four COVID-19 booster vaccinations against SARS-CoV-2 variants of concerns (Delta, Beta, and Omicron) following CoronaVac or ChAdOx1 nCoV-19 primary series. medRxiv 2021. [Google Scholar] [CrossRef]
- Mok, C.K.P.; Cheng, S.M.S.; Chen, C.; You, K.; Chan, T.O.; Lai, K.C.; Ling, K.C.; Sun, Y.; Ho, L.L.; Peiris, M.; et al. A RCT of a third dose CoronaVac or BNT162b2 vaccine in adults with two doses of CoronaVac. medRxiv 2021. [Google Scholar] [CrossRef]
- Toledo-Romani, M.E.; Carmenate, M.G.; Silva, C.V.; Rodriguez, W.B.; Pérez, M.M.; Gonzalez, M.C.R.; Moreno, B.P.; Hernandez, I.C.M.; Romero, R.G.-M.; Tabio, O.S.; et al. Efficacy and safety of SOBERANA 02, a COVID-19 conjugate vaccine in heterologous three-dose combination. medRxiv 2021. [Google Scholar] [CrossRef]
- Zhang, Z.; Wu, S.; Liu, Y.; Li, K.; Fan, P.; Song, X.; Wang, Y.; Zhao, Z.; Zhang, X.; Shang, J.; et al. Aerosolized Ad5-nCoV booster vaccination elicited potent immune response against the SARS-CoV-2 Omicron variant after inactivated COVID-19 vaccine priming. medRxiv 2022. [Google Scholar] [CrossRef]
- Ranzani, O.T.; Hitchings, M.D.T.; de Melo, R.L.; de França, G.V.A.; de Fernandes, C.F.R.; Lind, M.L.; Torres, M.S.S.; Tsuha, D.H.; David, L.C.S.; Said, R.F.C.; et al. Effectiveness of an Inactivated COVID-19 Vaccine with Homologous and Heterologous Boosters against the Omicron (B.1.1.529) Variant. medRxiv 2022. [Google Scholar] [CrossRef]
- Andrews, N.; Stowe, J.; Kirsebom, F.; Toffa, S.; Rickeard, T.; Gallagher, E.; Gower, C.; Kall, M.; Groves, N.; O’Connell, A.-M.; et al. Effectiveness of COVID-19 vaccines against the Omicron (B.1.1.529) variant of concern. medRxiv 2021. [Google Scholar] [CrossRef]
- Baum, U.; Poukka, E.; Leino, T.; Kilpi, T.; Nohynek, H.; Palmu, A.A. High vaccine effectiveness against severe COVID-19 in the elderly in Finland before and after the emergence of Omicron. medRxiv 2022. [Google Scholar] [CrossRef]
- Kaabi, N.A.; Yang, Y.K.; Du, L.F.; Xu, K.; Shao, S.; Liang, Y.; Kang, Y.; Su, J.G.; Zhang, J.; Yang, T.; et al. Safety and immunogenicity of a hybrid-type vaccine booster in BBIBP-CorV recipients: A randomized controlled phase 2 trial. medRxiv 2022. [Google Scholar] [CrossRef]
- Naito, T.; Tsuchida, N.; Kusunoki, S.; Kaneko, Y.; Tobita, M.; Hori, S.; Ito, S. Reactogenicity and immunogenicity of BNT162b2 or mRNA-1273 COVID-19 booster vaccinations after two doses of BNT162b2 among healthcare workers in Japan: A prospective observational study. Expert Rev. Vaccines 2022, 1–11. [Google Scholar] [CrossRef]
- Adams, K.; Rhoads, J.P.; Surie, D.; Gaglani, M.; Ginde, A.A.; McNeal, T.; Ghamande, S.; Huynh, D.; Talbot, H.K.; Casey, J.D.; et al. Vaccine Effectiveness of Primary Series and Booster Doses against Omicron Variant COVID-19-Associated Hospitalization in the United States. medRxiv 2022. [Google Scholar] [CrossRef]
- Bar-On, Y.M.; Goldberg, Y.; Mandel, M.; Bodenheimer, O.; Freedman, L.; Kalkstein, N.; Mizrahi, B.; Alroy-Preis, S.; Ash, N.; Milo, R.; et al. Protection of BNT162b2 Vaccine Booster against COVID-19 in Israel. N. Engl. J. Med. 2021, 385, 1393–1400. [Google Scholar] [CrossRef]
- Burckhardt, R.M.; Dennehy, J.J.; Poon, L.L.M.; Saif, L.J.; Enquist, L.W. Are COVID-19 Vaccine Boosters Needed? The Science behind Boosters. J. Virol. 2022, 96, e0197321. [Google Scholar] [CrossRef]
- Plumb, I.D.; Feldstein, L.R.; Barkley, E.; Posner, A.B.; Bregman, H.S.; Hagen, M.B.; Gerhart, J.L. Effectiveness of COVID-19 mRNA Vaccination in Preventing COVID-19-Associated Hospitalization among Adults with Previous SARS-CoV-2 Infection—United States, June 2021–February 2022. MMWR Morb. Mortal. Wkly. Rep. 2022, 71, 549–555. [Google Scholar] [CrossRef]
- Korves, C.; Izurieta, H.S.; Smith, J.; Zwain, G.M.; Powell, E.I.; Balajee, A.; Ryder, K.M.; Young-Xu, Y. Relative effectiveness of booster vs. 2-dose mRNA COVID-19 vaccination in the Veterans Health Administration: Self-controlled risk interval analysis. Vaccine 2022, 40, 4742–4747. [Google Scholar] [CrossRef]
- Du, Y.; Chen, L.; Shi, Y. Booster COVID-19 vaccination against the SARS-CoV-2 Omicron variant: A systematic review. Hum. Vaccines Immunother. 2022, 18, 2062983. [Google Scholar] [CrossRef] [PubMed]
| Safety Events | Number of Data Source | Heterologous Booster (n/N) | Homologous Booster (n/N) | OR | 95% CI | p-Value | Weight (%) | I2 | P-Heterogeneity |
|---|---|---|---|---|---|---|---|---|---|
| Systematic Adverse Reaction (within 7 Days after Boosting) | |||||||||
| Systematic adverse reaction | 2 | 42029/155484 | 2074/142400 | 6.02 | 0.34–107.31 | >0.05 | 100 | 99.70% | <0.05 |
| Malaise or fatigue | 13 | 677/1913 | 421/1645 | 1.745 | 1.047–2.906 | <0.05 | 100 | 79.70% | <0.05 |
| Chills | 9 | 455/1737 | 182/1155 | 1.428 | 0.808–2.524 | >0.05 | 100 | 82.60% | <0.05 |
| Fever | 15 | 351/2861 | 126/2227 | 1.930 | 1.199–3.107 | <0.05 | 100 | 59.30% | <0.05 |
| Headache | 15 | 893/2861 | 454/2227 | 1.418 | 0.940–2.140 | >0.05 | 100 | 81.50% | <0.05 |
| Nausea | 11 | 159/1775 | 100/1536 | 1.114 | 0.788–1.574 | >0.05 | 100 | 16.30% | >0.05 |
| Vomiting | 3 | 2/945 | 1/965 | 2.02 | 0.183–22.318 | >0.05 | 100 | - | - |
| Abdominal pain | 2 | 2/169 | 0/128 | 2.518 | 0.258–24.563 | >0.05 | 100 | 0.00% | >0.05 |
| Diarrhea | 7 | 34/1253 | 16/1160 | 1.522 | 0.758–3.055 | >0.05 | 100 | 0 | >0.05 |
| Arthralgia | 8 | 179/1685 | 123/1477 | 1.055 | 0.644–1.730 | >0.05 | 100 | 55.30% | <0.05 |
| Myalgia | 15 | 884/2861 | 401/2227 | 1.825 | 1.079–3.089 | <0.05 | 100 | 88.10% | <0.05 |
| Skin rash | 2 | 5/138 | 2/109 | 1.734 | 0.329–9.144 | >0.05 | 100 | - | - |
| Dizziness | 2 | 7/936 | 4/944 | 1.597 | 0.261–9.786 | >0.05 | 100 | 38.10% | >0.05 |
| Serious adverse events (SAE) | 2 | 0/145 | 0/119 | - | - | - | - | - | - |
| Systematic Adverse Reaction (within 28 Days after Boosting) | |||||||||
| Arthralgia | 2 | 14/123 | 9/130 | 2.084 | 0.741–5.866 | >0.05 | 100 | 0.00% | >0.05 |
| Malaise or fatigue | 2 | 32/123 | 16/130 | 4.140 | 1.729–9.916 | <0.05 | 100 | 0.00% | >0.05 |
| Myalgia | 2 | 16/123 | 9/130 | 2.694 | 0.953–7.614 | >0.05 | 100 | 0.00% | >0.05 |
| Injection Site Adverse Reaction (within 7 Days after Boosting) | |||||||||
| Injection site adverse reaction | 6 | 125599/155621 | 102419/142630 | 1.053 | 0.535–2.070 | >0.05 | 100 | 84.80% | <0.05 |
| Erythema or redness | 7 | 48/1556 | 47/1391 | 0.806 | 0.420–1.548 | >0.05 | 100 | 37.60% | >0.05 |
| Induration or swelling | 7 | 93/1556 | 79/1389 | 0.802 | 0.385–1.670 | >0.05 | 100 | 65.90% | <0.05 |
| Index | Number of Study | Heterologous Booster (n/N) | Homologous Booster (n/N) | Effect (SMD) | 95% CI | p-Value | Weight (%) | I2 | P-Heterogeneity | ||
|---|---|---|---|---|---|---|---|---|---|---|---|
| GMT of Neutralizing Antibody for VOCs | |||||||||||
| Anti-RBD IgG (14 days After Boosting) | 8 | 1124 | 1067 | 1.244 | 0.900–1.588 | 0 | <0.05 | 100 | 90.90% | 0 | <0.05 |
| GMT of Neutralizing Antibody for VOCs | |||||||||||
| Anti-wild-type (14 days after boosting) | 4 | 295 | 303 | 1.028 | 0.654–1.402 | 0 | <0.05 | 100 | 77.90% | 0.004 | <0.05 |
| Anti-wild-type (28 days after boosting) | 4 | 206 | 212 | 0.967 | 0.571–1.363 | 0 | <0.05 | 100 | 67.90% | 0.025 | <0.05 |
| Anti-Delta (14 days after boosting) | 4 | 295 | 303 | 0.833 | 0.509–1.157 | 0 | <0.05 | 100 | 71.80% | 0.014 | <0.05 |
| Index | Number of Data Source | Heterologous Booster (n/N) | Homologous Booster (n/N) | OR | 95% CI | p-Value | Weight (%) | I2 | P-Heterogeneity | ||
| Response Rate of Antibody | |||||||||||
| response rate of anti-spike IgG (28 days after boosting) | 2 | 264/321 | 115/205 | 5.536 | 2.738–11.195 | 0 | <0.05 | 100% | 0 | 0.495 | >0.05 |
| response rate of neutralizing antibody (nearly 1 month after boosting) | 4 | 160/289 | 93/234 | 1.446 | 0.864–2.422 | 0.161 | >0.05 | 100% | 0 | 0.49 | >0.05 |
| Response Rate of T cell | |||||||||||
| response rate of gama interferon (14 days after boosting in patients who were negative in baseline) | 4 | 54/87 | 2/18 | 16.3 | 3.439–77.272 | 0 | <0.05 | 100% | 0 | 0.321 | >0.05 |
| Homologous Booster Dose | ||||||||
|---|---|---|---|---|---|---|---|---|
| Outcomes | No. of Studies | Vaccine Effectiveness (%) | 95% CI | I2 | P-Heterogeneity | p Value for Subgroup Differences | Weight (%) | |
| Prevention of SARS-CoV-2 Infection | ||||||||
| Article type | Published | 3 | 85.80% | 84.3–87.2% | 98.30% | 0 | 0 | 66.51 |
| Preprint | 5 | 80.50% | 78.4–82.5% | 92.90% | 0 | 0 | 33.49 | |
| Study design | Cohort study | 7 | 83.30% | 82.1–84.5% | 96.60% | 0 | 0 | 92.84 |
| RCT | 1 | 92.40% | 88.1–96.7% | - | - | 0 | 7.16 | |
| Immune condition | mRNA vaccine ×3 | 6 | 86.40% | 84.8–88.0% | 96.50% | 0 | 0 | 55.29 |
| inactivated vaccine ×3 | 1 | 78.80% | 76.9–80.7% | - | - | 0 | 37.55 | |
| SOBERANA ×2 + SOBERANA plus ×1 | 1 | 92.40% | 88.1–96.7% | - | - | 0 | 7.16 | |
| Overall | 8 | 84.00% | 82.8–85.1% | 96.40% | 0 | 100 | ||
| Prevention of Symptomatic COVID-19 | ||||||||
| Article type | Published | 1 | 75.50% | 60.4–90.6% | - | - | 0 | 96.2 |
| Preprint | 1 | 15% | 12–18% | - | - | 0 | 3.8 | |
| Overall | 2 | 17.30% | 14.4–20.2% | 98.30% | 0 | 0 | 100 | |
| Prevention of Emergency Department and Urgent Care Admissions | ||||||||
| Immune condition | mRNA vaccine ×3 | 1 | 83.00% | 82.0–83.7% | - | - | 0 | 99.1 |
| adenovirus vector vaccine ×2 | 1 | 54.00% | 44.0–64.0% | - | - | 0 | 0.99 | |
| Overall | 2 | 82.70% | 81.7–83.7% | 96.90% | 0 | 0 | 100 | |
| Prevention of COVID-19 Hospital Admissions | ||||||||
| Article type | published | 3 | 88.70% | 87.5–90.0% | 89.10% | 0 | 0 | 38.44 |
| preprint | 1 | 93.20% | 92.4–94.0% | - | - | 0 | 61.56 | |
| Immune condition | mRNA vaccine ×3 | 2 | 94.20% | 93.3–95.0% | 97.60% | 0 | 0 | 88.92 |
| inactivated vaccine ×3 | 1 | 86.30% | 83.9–88.7 | - | - | 0 | 10.69 | |
| adenovirus vector vaccine ×2 | 1 | 67.00% | 54.5–79.5% | - | - | 0 | 0.39 | |
| Overall | 4 | 93.20% | 92.4–94.0% | 96.90% | 0 | 0 | 100 | |
| Heterologous Booster Dose | ||||||||
| Outcomes | No. of Studies | Vaccine Effectiveness (%) | 95% CI | I2 | P-Heterogeneity | p-Value for Subgroup Differences | Weight (%) | |
| Prevention of SARS-CoV-2 Infection | ||||||||
| Immune condition | adenovirus vector vaccine ×1 + mRNA vaccine ×1 | 2 | 90.70% | 89.1–92.2% | 5.60% | 0.303 | 0 | 2.42 |
| inactivated vaccine ×2 + recombinant vaccine ×1 | 1 | 93.20% | 92.4–94.0% | - | - | 0 | 8.68 | |
| inactivated vaccine ×2 + mRNA vaccine ×1 | 1 | 96.50% | 96.2–96.7% | - | - | 0 | 88.9 | |
| Overall | 4 | 96.10% | 95.8%-96.3% | 97.30% | 0 | 0 | 100 | |
| Prevention of Symptomatic COVID-19 | ||||||||
| Article type | Published | 1 | 71.40% | 49.3–93.5% | - | - | 0 | 0.06 |
| Preprint | 1 | 56.80% | 56.3–57.4% | - | - | 0 | 99.94 | |
| Immune condition | adenovirus vector vaccine ×2 + mRNA vaccine ×1 | 1 | 71.40% | 49.3–93.5% | - | - | 0 | 0.06 |
| inactivated vaccine ×2 + mRNA vaccine ×1 | 1 | 56.80% | 56.3–57.4% | - | - | 0 | 99.94 | |
| Overall | 2 | 56.80% | 56.3–57.4% | 40.30% | 0.196 | 0 | 100 | |
| Prevention of COVID-19 Hospital Admissions | ||||||||
| Immune condition | adenovirus vector vaccine ×1 + mRNA vaccine ×1 | 1 | 78.00% | 71.0–85.0% | - | - | 0 | 0.21 |
| inactivated vaccine ×2 + mRNA vaccine ×1 | 1 | 96.10% | 96.3–96.9% | - | - | 0 | 16.03 | |
| inactivated vaccine ×2 + recombinant vaccine ×1 | 1 | 97.40% | 97.3–98.1% | - | - | 0 | 83.76 | |
| Overall | 3 | 97.40% | 97.1–97.7% | 95.30% | 0 | 0 | 100 | |
| Prevention of COVID-19 ICU Admissions | ||||||||
| Immune condition | inactivated vaccine ×2 + mRNA vaccine ×1 | 1 | 96.20% | 94.9–97.6% | - | - | 0 | 6.3 |
| inactivated vaccine ×2 + recombinant vaccine ×1 | 1 | 98.90% | 98.6–99.3% | - | - | 0 | 93.7 | |
| Overall | 2 | 98.70% | 98.4–99.1% | 93.10% | 0 | 0 | 100 | |
| Prevention of COVID-19-Related Death | ||||||||
| Immune condition | inactivated vaccine ×2 + mRNA vaccine ×1 | 1 | 96.80% | 94.5–99.1% | - | - | 0 | 7.7 |
| inactivated vaccine ×2 + recombinant vaccine ×1 | 1 | 98.10% | 97.5–98.8% | - | - | 0 | 92.3 | |
| Overall | 2 | 98.00% | 97.4–98.6% | 15.50% | 1.277 | 0 | 100 | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Deng, J.; Ma, Y.; Liu, Q.; Du, M.; Liu, M.; Liu, J. Comparison of the Effectiveness and Safety of Heterologous Booster Doses with Homologous Booster Doses for SARS-CoV-2 Vaccines: A Systematic Review and Meta-Analysis. Int. J. Environ. Res. Public Health 2022, 19, 10752. https://doi.org/10.3390/ijerph191710752
Deng J, Ma Y, Liu Q, Du M, Liu M, Liu J. Comparison of the Effectiveness and Safety of Heterologous Booster Doses with Homologous Booster Doses for SARS-CoV-2 Vaccines: A Systematic Review and Meta-Analysis. International Journal of Environmental Research and Public Health. 2022; 19(17):10752. https://doi.org/10.3390/ijerph191710752
Chicago/Turabian StyleDeng, Jie, Yirui Ma, Qiao Liu, Min Du, Min Liu, and Jue Liu. 2022. "Comparison of the Effectiveness and Safety of Heterologous Booster Doses with Homologous Booster Doses for SARS-CoV-2 Vaccines: A Systematic Review and Meta-Analysis" International Journal of Environmental Research and Public Health 19, no. 17: 10752. https://doi.org/10.3390/ijerph191710752
APA StyleDeng, J., Ma, Y., Liu, Q., Du, M., Liu, M., & Liu, J. (2022). Comparison of the Effectiveness and Safety of Heterologous Booster Doses with Homologous Booster Doses for SARS-CoV-2 Vaccines: A Systematic Review and Meta-Analysis. International Journal of Environmental Research and Public Health, 19(17), 10752. https://doi.org/10.3390/ijerph191710752