Comparing Peak Burn Injury Times and Characteristics in Australia and New Zealand
Abstract
:1. Introduction
2. Materials and Methods
2.1. Data Source
2.2. Data Management
2.3. Statistical Analysis
3. Results
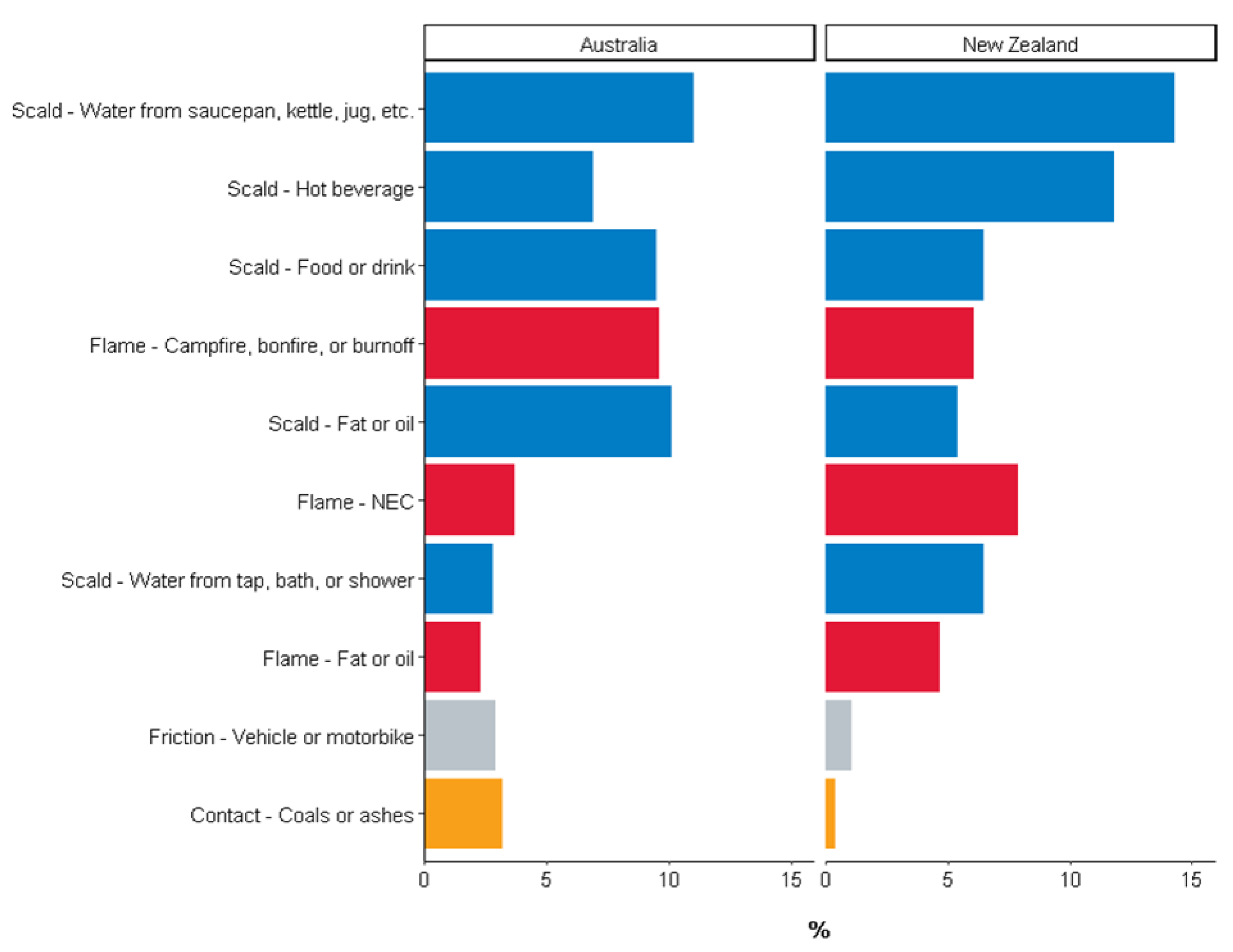
3.1. Demographic and Injury Characteristics
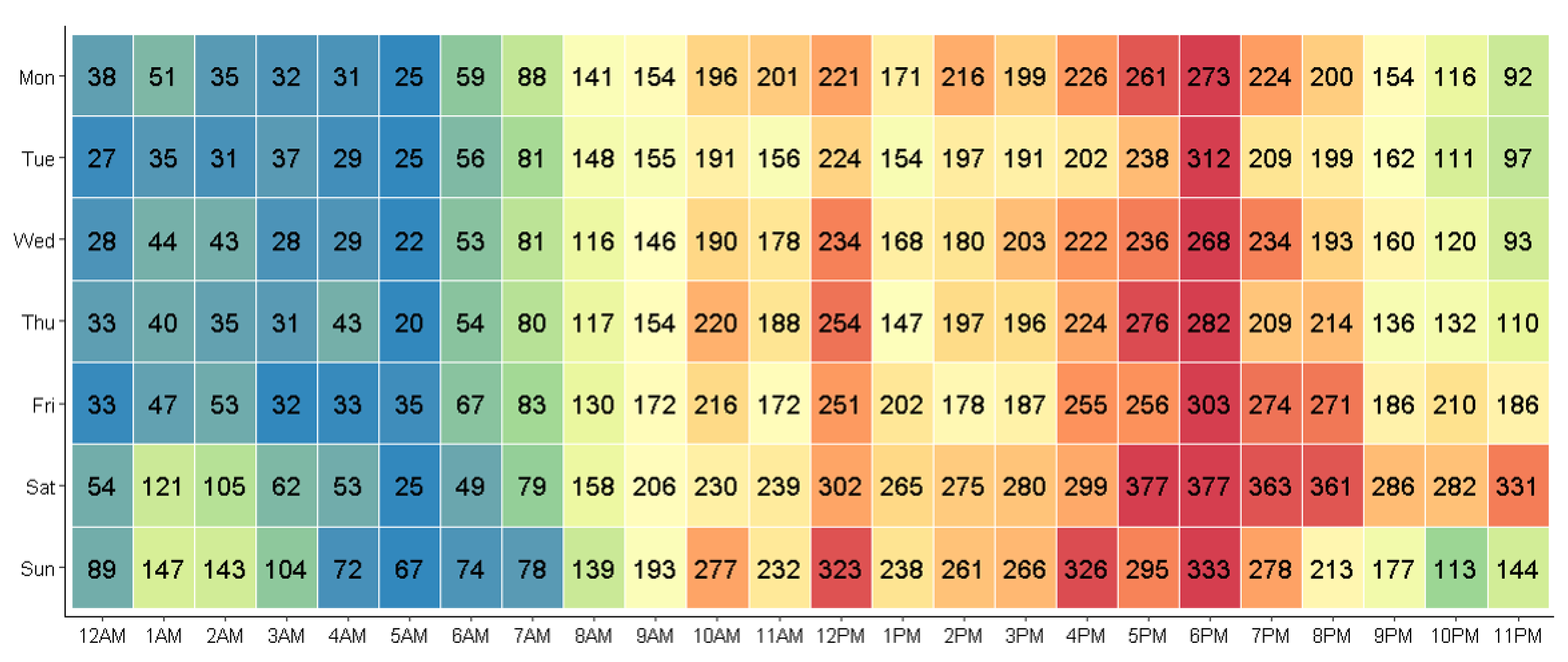
3.2. Peak Injury Times and Trends
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- World Health Organization. Disease Burden and Mortality Estimates. Available online: https://www.who.int/healthinfo/global_burden_disease/estimates/en/ (accessed on 15 September 2021).
- GBD 2017 DALYs and HALE Collaborators. Global, regional, and national disability-adjusted life-years (DALYs) for 359 diseases and injuries and healthy life expectancy (HALE) for 195 countries and territories, 1990–2017: A systematic analysis for the Global Burden of Disease Study 2017. Lancet 2018, 392, 1859–1922. [Google Scholar] [CrossRef] [Green Version]
- Ahn, C.S.; Maitz, P.K. The true cost of burn. Burn. J. Int. Soc. Burn. Inj. 2012, 38, 967–974. [Google Scholar] [CrossRef] [PubMed]
- Pereira, C.; Murphy, K.; Herndon, D. Outcome measures in burn care. Is mortality dead? Burn. J. Int. Soc. Burn. Inj. 2004, 30, 761–771. [Google Scholar] [CrossRef] [PubMed]
- Sanchez, J.L.; Bastida, J.L.; Martinez, M.M.; Moreno, J.M.; Chamorro, J.J. Socio-economic cost and health-related quality of life of burn victims in Spain. Burn. J. Int. Soc. Burn. Inj. 2008, 34, 975–981. [Google Scholar] [CrossRef] [PubMed]
- Peck, M.D. Epidemiology of burns throughout the world. Part I: Distribution and risk factors. Burn. J. Int. Soc. Burn. Inj. 2011, 37, 1087–1100. [Google Scholar] [CrossRef] [PubMed]
- Jacobs, C.; Vacek, J.; Many, B.; Bouchard, M.; Abdullah, F. An Analysis of Factors Associated with Burn Injury Outcomes in Low- and Middle-Income Countries. J. Surg. Res. 2021, 257, 442–448. [Google Scholar] [CrossRef] [PubMed]
- Tracy, L.M.; Rosenblum, S.; Gabbe, B.J. Burns Registry of Australia and New Zealand (BRANZ) 2018/19 Annual Report; Department of Epidemiology and Preventive Medicine, Monash University: Melbourne, Australia, 2020. [Google Scholar]
- Grivna, M.; Eid, H.O.; Abu-Zidan, F.M. Epidemiology of burns in the United Arab Emirates: Lessons for prevention. Burn. J. Int. Soc. Burn. Inj. 2014, 40, 500–505. [Google Scholar] [CrossRef]
- Chien, W.C.; Pai, L.; Lin, C.C.; Chen, H.C. Epidemiology of hospitalized burns patients in Taiwan. Burn. J. Int. Soc. Burn. Inj. 2003, 29, 582–588. [Google Scholar] [CrossRef]
- Celko, A.M.; Grivna, M.; Dánová, J.; Barss, P. Severe childhood burns in the Czech Republic: Risk factors and prevention. Bull. World Health Organ. 2009, 87, 374–381. [Google Scholar] [CrossRef]
- Burns Registry of Australia and New Zealand. Inclusion/Exclusion Criteria. Available online: https://www.branz.org/node/28 (accessed on 28 June 2022).
- Gabbe, B.J.; Cleland, H.; Watterson, D.M.; Schrale, R.; McRae, S.; Parker, C.; Taggart, S.; Edgar, D.W. Long term outcomes data for the Burns Registry of Australia and New Zealand: Is it feasible? Burn. J. Int. Soc. Burn. Inj. 2015, 41, 1732–1740. [Google Scholar] [CrossRef]
- Watterson, D.; Gabbe, B.J.; Cleland, H.; Edgar, D.; Cameron, P. Developing the first Bi-National clinical quality registry for burns—Lessons learned so far. Burn. J. Int. Soc. Burn. Inj. 2012, 38, 52–60. [Google Scholar] [CrossRef]
- Tracy, L.M.; Singer, Y.; Schrale, R.; Gong, J.; Darton, A.; Wood, F.; Kurmis, R.; Edgar, D.; Cleland, H.; Gabbe, B.J. Epidemiology of burn injury in older adults: An Australian and New Zealand perspective. Scars Burn. Health 2020, 6, 2059513120952336. [Google Scholar] [CrossRef]
- R Development Core Team. R: A language and environment for statistical computing. In R Foundation for Statistical Computing; R Development Core Team: Vienna, Austria, 2022. [Google Scholar]
- Wickham, H. The Split-Apply-Combine Strategy for Data Analysis. J. Stat. Softw. 2011, 40, 1–29. [Google Scholar] [CrossRef] [Green Version]
- Wickham, H. Welcome to the tidyverse. J. Open Source Softw. 2019, 4, 1686. [Google Scholar] [CrossRef]
- Neuwirth, E. RColorBrewer: ColorBrewer Palettes, R Package Version 1.1-2. 2014. Available online: https://CRAN.R-project.org/package=RColorBrewer (accessed on 15 September 2021).
- Wickham, H. Scales: Scale Functions for Visualization, R Package Version 1.0.0. 2018. Available online: https://CRAN.R-project.org/package=scales (accessed on 15 September 2021).
- Forjuoh, S.N. Burns in low- and middle-income countries: A review of available literature on descriptive epidemiology, risk factors, treatment, and prevention. Burn. J. Int. Soc. Burn. Inj. 2006, 32, 529–537. [Google Scholar] [CrossRef]
- Singer, Y.; Tracy, L.M.; Menezes, H.; Cleland, H.; Perrett, T.; Wood, F.; Harvey, L. “The home, the bathroom, the taps, and hot water”: The contextual characteristics of tap water scalds in Australia and New Zealand. Burn. J. Int. Soc. Burn. Inj. 2022, 48, 1004–1012. [Google Scholar] [CrossRef] [PubMed]
- Burgess, J.; Watt, K.; Kimble, R.M.; Cameron, C.M. Combining Technology and Research to Prevent Scald Injuries (the Cool Runnings Intervention): Randomized Controlled Trial. J. Med. Internet Res. 2018, 20, e10361. [Google Scholar] [CrossRef]
- Lin, T.M.; Wang, K.H.; Lai, C.S.; Lin, S.D. Epidemiology of pediatric burn in southern Taiwan. Burn. J. Int. Soc. Burn. Inj. 2005, 31, 182–187. [Google Scholar] [CrossRef]
- Gerelmaa, G.; Tumen-Ulzii, B.; Nakahara, S.; Ichikawa, M. Patterns of burns and scalds in Mongolian children: A hospital-based prospective study. Trop. Med. Int. Health 2018, 23, 334–340. [Google Scholar] [CrossRef] [Green Version]
- Tse, T.; Poon, C.H.; Tse, K.H.; Tsui, T.K.; Ayyappan, T.; Burd, A. Paediatric burn prevention: An epidemiological approach. Burn. J. Int. Soc. Burn. Inj. 2006, 32, 229–234. [Google Scholar] [CrossRef]
- Gunsmaa, G.; Shono, A.; Price, P.E.; Kondo, M.; Hebron, C.; Potokar, T.; Ichikawa, M. Parental acceptance and willingness to pay for a newly designed kitchen rack to reduce paediatric burns. Burn. J. Int. Soc. Burn. Inj. 2021, 48, 381–389. [Google Scholar] [CrossRef]
- Rolex Awards for Enterprise. Wijaya Godakumbura—Safe Lamps Save Lives. Available online: https://www.rolex.org/rolex-awards/science-health/wijaya-godakumbura (accessed on 15 September 2021).
- Gibson, C.; Bessey, P.Q.; Gallagher, J.J. The Global Burn Registry: A Work in Progress. J. Burn. Care Res. 2020, 41, 929–934. [Google Scholar] [CrossRef] [PubMed]
- Ngaage, L.M.; Borrelli, M.R.; Rose, J.A.; Puthumana, J.; Rada, E.M.; Nam, A.J.; Caffrey, J.; Rasko, Y. Global Burn Registry Perspective on Head and Neck Burns. Ann. Plast. Surg. 2021, 87, 33–38. [Google Scholar] [CrossRef]
- Peck, M.; Falk, H.; Meddings, D.; Sugerman, D.; Mehta, S.; Sage, M. The design and evaluation of a system for improved surveillance and prevention programmes in resource-limited settings using a hospital-based burn injury questionnaire. Inj. Prev. 2016, 22 (Suppl. S1), i56–i62. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Puthumana, J.S.; Ngaage, L.M.; Borrelli, M.R.; Rada, E.M.; Caffrey, J.; Rasko, Y. Risk factors for cooking-related burn injuries in children, WHO Global Burn Registry. Bull. World Health Organ. 2021, 99, 439–445. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Differences in Data Available Within the GBR between the Public and Private Views. Available online: https://www.who.int/docs/default-source/documents/burns/differencesbetweenpublicandprivateviews.pdf (accessed on 13 September 2021).
| BRANZ (n = 26,925) | Australia (n = 23,323) | New Zealand (n = 3602) | |
|---|---|---|---|
| Age, median (IQR) years a | 27 (8–47) | 28 (11–47) | 21 (2–42) |
| Age group a | |||
| Paediatric (< 16 years) | 8323 (30.9%) | 6771 (29.0%) | 1552 (43.1%) |
| Adult (16–64 years) | 16,227 (60.5%) | 14,456 (62.0%) | 1821 (50.6%) |
| Older adult (≥ 65 years) | 2321 (8.6%) | 2092 (9.0%) | 229 (6.4%) |
| Gender b | |||
| Male | 18,378 (68.3%) | 15,937 (68.4%) | 2441 (67.8%) |
| Other | 8537 (31.7%) | 7379 (31.6%) | 1158 (32.2%) |
| Primary cause c | |||
| Scald | 9912 (36.9%) | 8244 (35.4%) | 1668 (46.4%) |
| Flame | 9660 (35.9%) | 8413 (36.1%) | 1247 (34.7%) |
| Contact | 4012 (14.9%) | 3604 (15.5%) | 408 (11.3%) |
| Other cause | 3309 (12.3%) | 3034 (13.0%) | 275 (7.6%) |
| TBSA, median (IQR) % d | 3.0 (1.0–7.6) | 3.0 (1.0–7.0) | 5.0 (2.0–9.0) |
| Maximal depth recorded e | |||
| Superficial dermal | 3633 (15.2%) | 2832 (13.5%) | 801 (26.8%) |
| Mid-dermal | 6636 (27.7%) | 5719 (27.3%) | 917 (30.7%) |
| Deep dermal | 8138 (34.0%) | 7621 (36.4%) | 517 (17.3%) |
| Full thickness | 5514 (23.1%) | 4760 (22.7%) | 754 (25.2%) |
| Inhalation injury f | |||
| No | 25,512 (95.0%) | 22153 (95.2%) | 3359 (93.8%) |
| Yes | 1341 (5.0%) | 1118 (4.8%) | 223 (6.2%) |
| Place of injury g | |||
| Home/usual residence | 16,541 (63.1%) | 14,047 (61.6%) | 2494 (73.3%) |
| Other place | 9657 (36.9%) | 8750 (38.4%) | 907 (26.7%) |
| Injury intent h | |||
| Unintentional injury | 25,365 (94.5%) | 21,965 (94.5%) | 3400 (94.7%) |
| Other intent | 1479 (5.5%) | 1289 (5.5%) | 190 (5.3%) |
| Burn wound management in theatre i | |||
| No | 6902 (25.8%) | 6120 (26.4%) | 782 (22.0%) |
| Yes | 19,835 (74.2%) | 17,056 (73.6%) | 2779 (78.0%) |
| LOS, median (IQR) days j | 4.0 (1.6–9.8) | 4.0 (1.4–9.8) | 3.8 (2.0–9.8) |
| Discharge disposition k | |||
| Home/usual residence | 23,291 (86.7%) | 20,109 (86.4%) | 3182 (88.5%) |
| Other disposition | 3585 (13.3%) | 3173 (13.6%) | 412 (11.5%) |
| Non-Peak (n = 24,474) | Australia (6 PM; n = 1871) | New Zealand (5 PM; n = 280) | |
|---|---|---|---|
| Age, median (IQR) years a | 27.0 (9.0, 47.0) | 27.0 (6.0, 48.0) | 18.0 (1.0, 40.0) |
| Age group a | |||
| Paediatric (< 16 years) | 7523 (30.4%) | 666 (35.6%) | 134 (47.9%) |
| Adult (16–64 years) | 15,127 (61.0%) | 1019 (54.5%) | 131 (46.8%) |
| Older adult (≥ 65 years) | 2120 (8.6%) | 186 (9.9%) | 15 (5.4%) |
| Gender b | |||
| Male | 16,999 (68.6%) | 1204 (64.4%) | 175 (62.5%) |
| Other | 7767 (31.4%) | 665 (35.6%) | 105 (37.5%) |
| Primary cause c | |||
| Scald | 8924 (36.1%) | 845 (45.2%) | 143 (51.1%) |
| Flame | 8972 (36.3%) | 591 (31.6%) | 97 (34.6%) |
| Contact | 3726 (15.1%) | 258 (13.8%) | 28 (10.0%) |
| Other cause | 3122 (12.6%) | 175 (9.4%) | 12 (4.3%) |
| TBSA, median (IQR) % d | 3.0 (1.0, 7.7) | 3.0 (1.0, 7.0) | 5.5 (2.5, 10.0) |
| Maximal depth recorded e | |||
| Superficial dermal | 3340 (15.2%) | 243 (14.6%) | 50 (21.8%) |
| Mid-dermal | 6116 (27.8%) | 439 (26.3%) | 81 (35.4%) |
| Deep dermal | 7417 (33.7%) | 670 (40.1%) | 51 (22.3%) |
| Full thickness | 5150 (23.4%) | 317 (19.0%) | 47 (20.5%) |
| Inhalation injury f | |||
| No | 23,437 (94.9%) | 1809 (96.8%) | 266 (95.0%) |
| Yes | 1268 (5.1%) | 59 (3.2%) | 14 (5.0%) |
| Place of injury g | |||
| Home/usual residence | 14,949 (62.0%) | 1385 (75.6%) | 207 (78.1%) |
| Other place | 9153 (38.0%) | 446 (24.4%) | 58 (21.9%) |
| Injury intent h | |||
| Unintentional injury | 23306 (94.4%) | 1799 (96.5%) | 260 (93.5%) |
| Other intent | 1395 (5.6%) | 66 (3.5%) | 18 (6.5%) |
| Burn wound management in theatre i | |||
| No | 6325 (25.7%) | 520 (28.0%) | 57 (20.7%) |
| Yes | 18277 (74.3%) | 1339 (72.0%) | 219 (79.3%) |
| LOS, median (IQR) days j | 4.0 (1.6, 9.8) | 4.0 (1.5, 9.1) | 4.6 (2.6, 11.7) |
| Discharge disposition k | |||
| Home/usual residence | 21,371 (86.4%) | 1674 (89.7%) | 246 (87.9%) |
| Other disposition | 3358 (13.6%) | 193 (10.3%) | 34 (12.1%) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hong, R.; Perkins, M.; Gabbe, B.J.; Tracy, L.M. Comparing Peak Burn Injury Times and Characteristics in Australia and New Zealand. Int. J. Environ. Res. Public Health 2022, 19, 9578. https://doi.org/10.3390/ijerph19159578
Hong R, Perkins M, Gabbe BJ, Tracy LM. Comparing Peak Burn Injury Times and Characteristics in Australia and New Zealand. International Journal of Environmental Research and Public Health. 2022; 19(15):9578. https://doi.org/10.3390/ijerph19159578
Chicago/Turabian StyleHong, Rebecca, Monica Perkins, Belinda J. Gabbe, and Lincoln M. Tracy. 2022. "Comparing Peak Burn Injury Times and Characteristics in Australia and New Zealand" International Journal of Environmental Research and Public Health 19, no. 15: 9578. https://doi.org/10.3390/ijerph19159578
APA StyleHong, R., Perkins, M., Gabbe, B. J., & Tracy, L. M. (2022). Comparing Peak Burn Injury Times and Characteristics in Australia and New Zealand. International Journal of Environmental Research and Public Health, 19(15), 9578. https://doi.org/10.3390/ijerph19159578







