The Preventive Child and Youth Healthcare Service in the Netherlands: The State of the Art and Challenges Ahead
Abstract
1. Introduction
2. Three Basic Principles
3. Economic, Population, Societal and Health Characteristics
4. Child and Youth Health
5. Preventive Child and Youth Healthcare
5.1. Basic Child and Youth Healthcare
5.2. Special Care
6. Impact and Returns
7. Discussion/Reflection
7.1. Access for All
7.2. Coordinating Care
7.3. Insights from the Use of CYH Data in a National Database
7.4. Implications for the Future
8. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- UNICEF Convention on the Rights of the Child. 2019. Available online: https://www.unicef.nl/files/Unicef-kinderrechtenverdrag-2019.pdf (accessed on 29 April 2022).
- Sameroff, A. A unified theory of development: A dialectic integration of nature and nurture. Child Dev. 2010, 81, 6–22. [Google Scholar] [CrossRef] [PubMed]
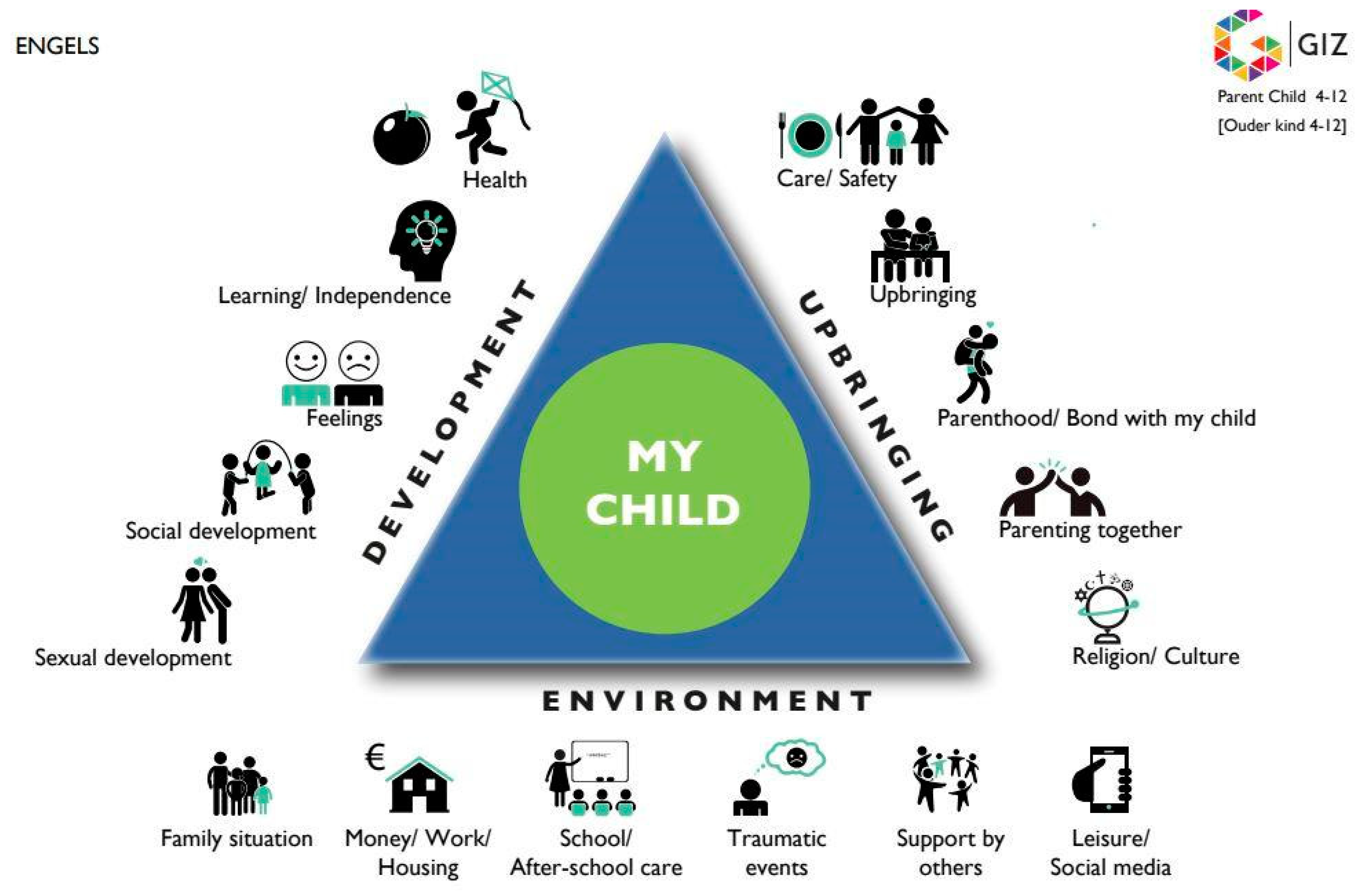
- Netherlands Center Youth Health (NCJ). Joint Assessment of Care Needs, in Dutch: Gezamenlijk Inschatten van Zorgbehoeften GIZ-Methodiek [GIZ Methodology]. Available online: https://www.ncj.nl/GIZ/ (accessed on 29 April 2022).
- Bontje, M.C.A.; de Ronde, R.W.; Dubbeldeman, E.M.; Kamphuis, M.; Reis, R.; Crone, M.R. Parental engagement in preventive youth health care: Effect evaluation. CYSR 2021, 120, 105724. [Google Scholar] [CrossRef]
- Elwyn, G.; Coulter, A.; Laitner, S.; Walker, E.; Watson, P.; Thomson, R. Implementing shared decision making in the NHS. BMJ 2010, 341, c5146. [Google Scholar] [CrossRef] [PubMed]
- Statistics Netherlands. Population Register Data. Available online: http://opendata.cbs.nl/statline/#/CBS/nl (accessed on 29 April 2022).
- Van Gils, P.; Suijkerbuijk, A.; Polder, J.; de Wit, G.A.; Koopmanschap, M. Nederlandse preventie-uitgaven onder de loep. TSG 2020, 98, 92–96. [Google Scholar] [CrossRef]
- Eurostat. European Statistics. Available online: http://ec.europa.eu/eurostat/data/database (accessed on 29 April 2022).
- Volksgezondheid en Zorg Informatie. Information about Health and Disease, Risk Factors, Care and Prevention in the Netherlands. Available online: https://www.vzinfo.nl/ (accessed on 29 April 2022).
- De Graaf, R.; ten Have, M.; van Gool, C.; van Dorsselaer, S. Prevalence of mental disorders and trends from 1996 to 2009. Results from the Netherlands Mental Health Survey and Incidence Study-2. Soc. Psychiatry Psychiatr. Epidemiol. 2012, 47, 203–213. [Google Scholar] [CrossRef]
- National Institute for Public Health, The Netherlands, Ministry of Health, Welfare and Sports. Available online: https://www.volksgezondheidenzorg.info/onderwerp/English (accessed on 29 April 2022).
- Lanting, C.I.; Wouwe, K.; van Dommelen, P.; van der Pal-de Bruin, K.M.; Josselin-de Jong, S.; Kleinjan, M.; van Laar, M. Roken tijdens de Zwangerschap: Percentages over de Periode 2001–2015; TNO: Leiden, The Netherlands, 2015; Available online: https://repository.tno.nl//islandora/object/uuid:f76c0e68-6e40-4926-964c-d668dd20d5d3 (accessed on 29 April 2022).
- Perinatal Figures in the Netherlands. In Information about the Mother, Pregnancy, Delivery and Child, Registered by Obstetricians, Gynecologists and Pediatricians; Perined, Utrecht, The Netherlands, 2021. Available online: https://www.peristat.nl/ (accessed on 29 April 2022).
- Statline. Available online: https://opendata.cbs.nl/statline/#/CBS/nl/dataset/81565NED/table (accessed on 29 April 2022).
- World Health Organization/Europe. Spotlight on Adolescent Health and Well-Being. Findings From the 2017 Health Behaviour in School-Aged Children (HBSC) Survey in Europe and Canada; International Report, 2020; World Health Organization/Europe: Copenhagen, Denmark, 2020; Available online: https://apps.who.int/iris/bitstream/handle/10665/332091/9789289055000-eng.pdf (accessed on 29 April 2022)ISBN 978-92-890-5500-0.
- Van Hal, L.; Tierolf, B.; van Rooijen, M.; van der Hoff, M. Een Actueel Perspectief op Kinderen en Jongeren Met Een Chronische Aandoening in Nederland: Omvang, Samenstelling en Participatie; Verwey-Jonker Instituut: Utrecht, The Netherlands, 2019; Available online: https://www.verwey-jonker.nl/wp-content/uploads/2020/07/217026_actueel_perspectief_op_kinderen_en_WEB-1.pdf (accessed on 29 April 2022).
- Van Muilekom, M.M.; Luijten, M.A.; Teela, L.; Polderman, J.C.; Terwee, C.B.; Zijlmans, J.; Klaufus, L.H.; Popma, A.; Oostrom, K.J.; van Oers, H.A.; et al. Impact van covid-19-maatregelen op de mentale en sociale gezondheid van kinderen. Ned. Tijdschr. Voor Geneeskd. 2021, 165, D6296. [Google Scholar]
- Van Berkel, S.R.; Prevoo, M.J.L.; Linting, M.; Pannebakker, F.D.; Alink, L.R.A. Prevalence of child maltreatment in the Netherlands: An update and cross-time comparison. Child Abuse Negl. 2020, 103, 104439. [Google Scholar] [CrossRef]
- Vink, R.M.; Van Dommelen, P.; van der Pal, S.M.; Eekhout, I.; Pannebakker, F.D.; Klein Velderman, M.; Haagmans, M.; Mulder, T.; Dekker, M. Self-reported adverse childhood experiences and quality of life among children in the two last grades of Dutch elementary education. Child Abuse Negl. 2019, 95, 104051. [Google Scholar] [CrossRef]
- NCD Risk Factor Collaboration (NCD-RisC). Height and body-mass index trajectories of school-aged children and adolescents from 1985 to 2019 in 200 countries and territories: A pooled analysis of 2181 population-based studies with 65 million participants. Lancet 2020, 396, 1511–1524. [Google Scholar] [CrossRef]
- Stevens, G.J.W.M.; van Dorsselaer, S.; Boer, M.; de Roos, S.; Duinhof, E.L.; ter Bogt, T.F.M.; van den Eijnden, R.J.J.M.; Kuyper, L.; Visser, D.; Vollebergh, W.A.M.; et al. Gezondheid en Welzijn Van Jongeren in Nederland; Utrecht University: Utrecht, The Netherlands, 2017; Available online: https://dspace.library.uu.nl/handle/1874/376901 (accessed on 29 April 2022)ISBN 978-90-829085-0-3.
- Dunnink, G. Standpunt Bereik van de Jeugdgezondheidszorg; National Institute for Public Health and the Environment (RIVM) of the Ministry of Health, Welfare and Sport: Bilthoven, The Netherlands, 2010; Available online: https://www.rivm.nl/bibliotheek/rapporten/295001015.pdf (accessed on 29 April 2022).
- Tasks of Public Healthcare. Taken Publieke Gezondheidszorg. Available online: https://wetten.overheid.nl/BWBR0024705/2020-03-19#HoofdstukII (accessed on 29 April 2022).
- The 2019 Rotterdam EUSUHM Declaration on Youth Health Care in Europe. Available online: https://eusuhm.org/publications/declarations/2019-rotterdam/ (accessed on 29 April 2022).
- The Healthy School Approach. De Gezonde School Aanpak. Available online: https://www.gezondeschool.nl/aanpak/wat-is-gezonde-school#:~:text=Gezonde%20School%20is%20een%20programma%20dat%20onderwijsprofessionals%20helpt,aan%20een%20gezondheidsthema%20dat%20de%20school%20zelf%20kiest (accessed on 29 April 2022).
- Lifestyle Interventions. Leefstijlinterventies. Loket Gezond Leven. National Institute for Public Health and the Environment (RIVM). Available online: https://www.loketgezondleven.nl/leefstijlinterventies/interventies-zoeken-algemeen (accessed on 29 April 2022).
- Juffer, F.; Bakermans-Kranenburg, M.J. Working with Video-feedback Intervention to promote Positive Parenting and Sensitive Discipline (VIPP-SD): A case study. J. Clin. Psychol. 2018, 74, 1346–1357. [Google Scholar] [CrossRef]
- Mejdoubi, J.; van den Heijkant, S.C.C.M.; van Leerdam, F.J.M.; Heymans, M.W.; Crijnen, A.; Hira Sing, R.A. The Effect of VoorZorg, the Dutch Nurse-Family Partnership, on Child Maltreatment and Development: A Randomized Controlled Trial. PLoS ONE 2015, 10, e0120182. [Google Scholar] [CrossRef] [PubMed]
- Vanneste, Y.T.M.; Mathijssen, J.J.; van de Goor, I.A.; Rots-de Vries, C.M.; Feron, F.J. Addressing medical absenteeism in pre-vocational secondary students: Effectiveness of a public health intervention, using a quasi-experimental design. BMC Public Health 2016, 16, 1107. [Google Scholar] [CrossRef] [PubMed]
- Van den Toren, S.J.; Franse, C.B.; Vanneste, Y.T.M.; Bannink, R.; Lugtenberg, M.; Mulder, W.C.; de Kroon, M.L.A.; van Grieken, A.; Raat, H. Addressing sickness absence among adolescents and young adults: An evaluation of the Medical Advice for Sick-reported Students intervention. BMC Public Health 2020, 20, 1851. [Google Scholar] [CrossRef] [PubMed]
- Pijl, E.K.; Vanneste, Y.T.M.; Mathijssen, J.J.P.; Feron, F.J.M.; de Rijk, A.E. Process Evaluation of the Child and Youth Healthcare Intervention ‘Medical Advice for Sick-Reported Students in Primary School’ (MASS-PS). Int. J. Environ. Res. Public Health 2022, 19, 4409. [Google Scholar] [CrossRef] [PubMed]
- Poulton, R.; Caspi, A.; Milne, B.J.; Thomson, W.M.; Taylor, A.; Sears, M.R.; Moffitt, T.E. Association between children’s experience of socioeconomic disadvantage and adult health: A life-course study. Lancet 2002, 360, 1640–1645. [Google Scholar] [CrossRef]
- Hughes, K.; Bellis, M.A.; Hardcastle, K.A.; Sethi, D.; Butchart, A.; Mikton, C.; Jones, L.; Dunne, M.P. The effect of multiple adverse childhood experiences on health: A systematic review and meta-analysis. Lancet Public Health 2017, 2, e356–e366. [Google Scholar] [CrossRef]
- Van Huizen, T.; Plantenga, J. Do children benefit from universal early childhood education and care? A meta-analysis of evidence from natural experiments. Econ. Educ. Rev. 2018, 66, 206–222. [Google Scholar] [CrossRef]
- Felitti, V.J.; Anda, R.; Nordenberg, D.; Williamson, D.; Spitz, A.; Edwards, V.; Koss, M.; Marks, J. Relationship of childhood abuse and household dysfunction to many of the leading causes of death in adults: The Adverse Childhood Experiences (ACE) Study. Am. J. Prev. Med. 1998, 14, 245–258. [Google Scholar] [CrossRef]
- Belli, P.; Bustreo, F.; Preker, A. Investing in children’s health: What are the economic benefits? Bull. World Health Organ. 2015, 83, 777–784. [Google Scholar]
- Heckman, J.J. Skill formation and the economics of investing in disadvantaged children. Science 2006, 312, 1900–1902. [Google Scholar] [CrossRef]
- Spencer, N.J.; Blackburn, C.M.; Read, J.M. Disabling chronic conditions in childhood and socioeconomic disadvantage: A systematic review and meta-analyses of observational studies. BMJ Open 2015, 5, e007062. [Google Scholar] [CrossRef]
- Prinsen, B.; Steinbuch-Linstra, I.; Krähe, A. Investeren in opvoeden en opgroeien loont! Tijdschr Jeugdgezondheidsz 2015, 47, 6–9. [Google Scholar] [CrossRef]
- Dam, P. Kosteneffectiviteit van de Jeugdgezondheidszorg. Verdonck, Klooster & Associates, B.V. Zoetermeer. 2012. Available online: https://vzinfo.nl/publicaties/kosteneffectiviteit-van-jeugdgezondheidszorg (accessed on 29 April 2022).
- Müller-Nordhorn, J.; Schneider, A.; Grittner, U.; Neumann, K.; Keil, T.; Willich, S.N.; Binting, S. International time trends in sudden unexpected infant death, 1969–2012. BMC Pediatr 2020, 20, 377. [Google Scholar] [CrossRef] [PubMed]
- Kanits, F.; L’Hoir, M.P.; Boere-Boonekamp, M.M.; Engelberts, A.C.; Feskens, E. Renewed Attention Needed for Prevention of Sudden Unexpected Death in Infancy in the Netherlands. Front. Pediatr. 2021, 9, 757530. [Google Scholar] [CrossRef] [PubMed]
- Heijmans, M.; Brabers, A.; Rademakers, J. Health Literacy in The Netherlands. Health Literacy in Nederland. Utrecht: Nivel, 2018. Available online: https://www.nivel.nl/sites/default/files/bestanden/Gezondheidsvaardigheden_in_Nederland.pdf (accessed on 29 April 2022).
- Berkman, N.D.; Sheridan, S.L.; Donahue, K.E.; Halpern, D.J.; Crotty, K. Low health literacy and health outcomes: An updated systematic review. Ann. Intern. Med. 2011, 155, 97–107. [Google Scholar] [CrossRef]
- Wolff, M.S.; Detmar, S.B.; Verkerk, P.H.; Reijneveld, S.A.; Geerdes-Maas, T. Verkenning JGZ Indicatoren. TNO 2021 R10002. TNO, Leiden, 2021. Available online: http://resolver.tudelft.nl/uuid:8f51371b-7e1b-452d-aeaf-f6a702f511ac (accessed on 29 April 2022).
| Indicator | 2000 | 2010 | 2020 |
|---|---|---|---|
| Population | |||
| Total number (in millions) | 15.9 | 16.6 | 17.4 |
| Density (people per km2) | 468 | 491 | 517 |
| Live births (n) | 206,619 | 184,397 | 164,262 |
| Children and young adults in the ages of 0–20 y (% of total) | 24.4 | 23.7 | 21.7 |
| Life expectancy at birth (y) | 78.1 | 80.8 | 81.4 |
| Non-western migrants (% of total Dutch population) | 8.9 | 11.2 | 13.7 |
| People at risk of poverty and/or social exclusion (% of total Dutch population) a | 10.4 | 6.6 | 15.8 |
| Health | |||
| Overweight: | |||
| % of adult population | 44.3 | 48.2 | 51.0 |
| % of children and young adults in the ages of 4 to 20 years | 11.8 a | 13.6 | 15.1 |
| Smokers (% of ages > 12 y) | 32.0 | 26.3 | 20.1 |
| Preterm births (<37 weeks) and/or SGA births (< p 10) (% of live births) | 8 | 8 | 15 |
| Immunisation rate: | |||
| DTaP-IPV (% of children in the ages of 12–23 months) | 95.6 | 95.0 | 93.1 |
| MMR (% of children in the ages of 12–23 months) | 95.6 | 96.2 | 93.6 |
| Economics | |||
| GDP (in 1000 euros per capita) | 40 | 44 | 46 |
| Health expenditure: | |||
| % of GDP | 7.7 | 10.2 | 11.2 |
| in euros per capita | 2187 | 3907 | 5137 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Vanneste, Y.T.M.; Lanting, C.I.; Detmar, S.B. The Preventive Child and Youth Healthcare Service in the Netherlands: The State of the Art and Challenges Ahead. Int. J. Environ. Res. Public Health 2022, 19, 8736. https://doi.org/10.3390/ijerph19148736
Vanneste YTM, Lanting CI, Detmar SB. The Preventive Child and Youth Healthcare Service in the Netherlands: The State of the Art and Challenges Ahead. International Journal of Environmental Research and Public Health. 2022; 19(14):8736. https://doi.org/10.3390/ijerph19148736
Chicago/Turabian StyleVanneste, Yvonne T. M., Caren I. Lanting, and Symone B. Detmar. 2022. "The Preventive Child and Youth Healthcare Service in the Netherlands: The State of the Art and Challenges Ahead" International Journal of Environmental Research and Public Health 19, no. 14: 8736. https://doi.org/10.3390/ijerph19148736
APA StyleVanneste, Y. T. M., Lanting, C. I., & Detmar, S. B. (2022). The Preventive Child and Youth Healthcare Service in the Netherlands: The State of the Art and Challenges Ahead. International Journal of Environmental Research and Public Health, 19(14), 8736. https://doi.org/10.3390/ijerph19148736






