Photorefraction with Spot Vision Screener versus Visual Acuity Testing as Community-Based Preschool Vision Screening at the Age of 3.5 Years in Japan
Abstract
1. Introduction
2. Materials and Methods
2.1. Flow of 3.5-Year-Old Health-Screening Program
2.2. Study Population
2.3. Visual Acuity Testing at Home
2.4. Questionnaire for Vision-Related Problems
2.5. Visual Acuity Testing and Spot Vision Screener in Health Center
2.6. Criteria to Issue a Notice for the Tertiary Examinations
2.7. Primary Outcome and Statistical Analyses
3. Results
3.1. Visual Acuity Testing and Spot Vision Screener
3.2. Diagnoses in the Tertiary Examinations by Ophthalmologists
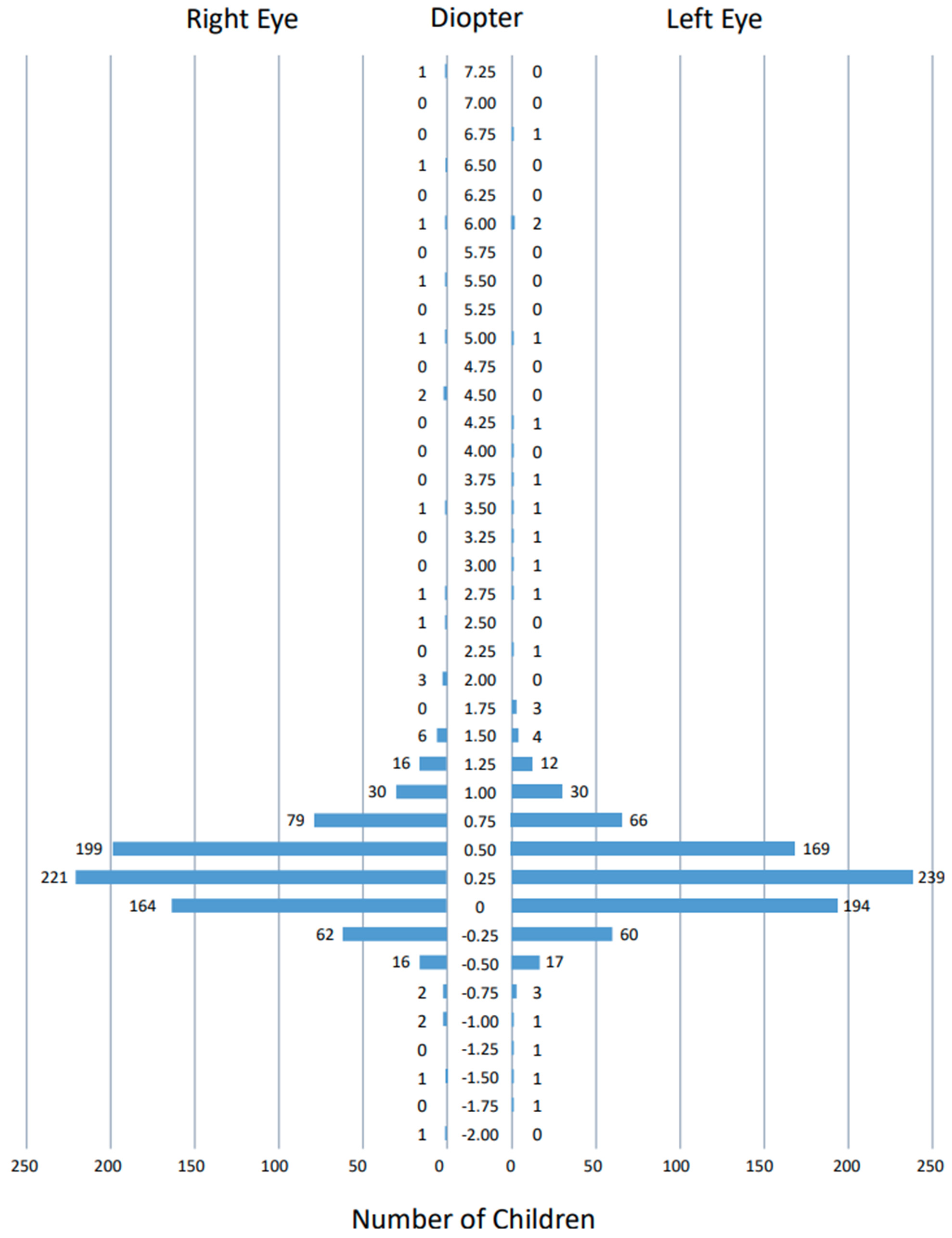
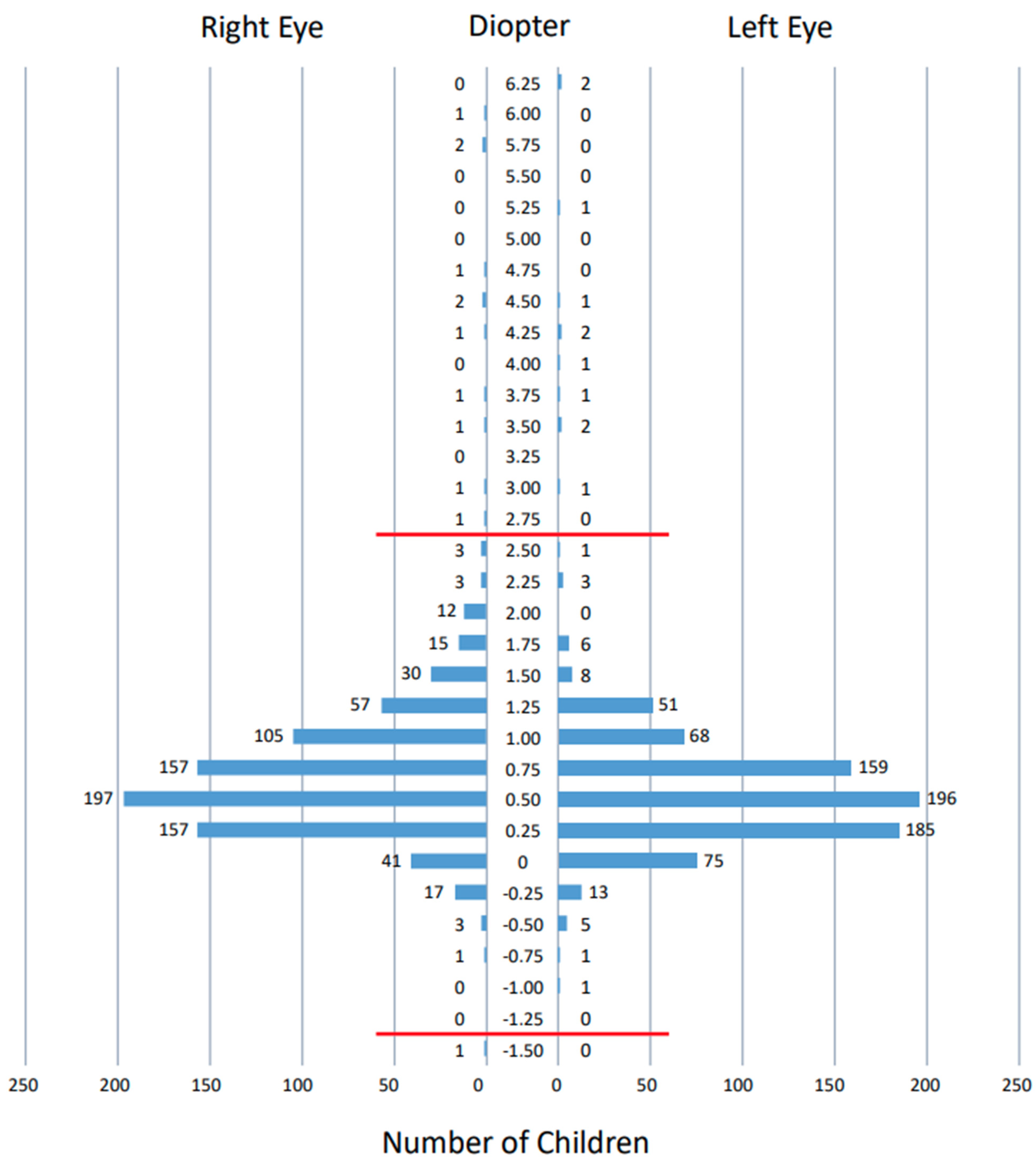
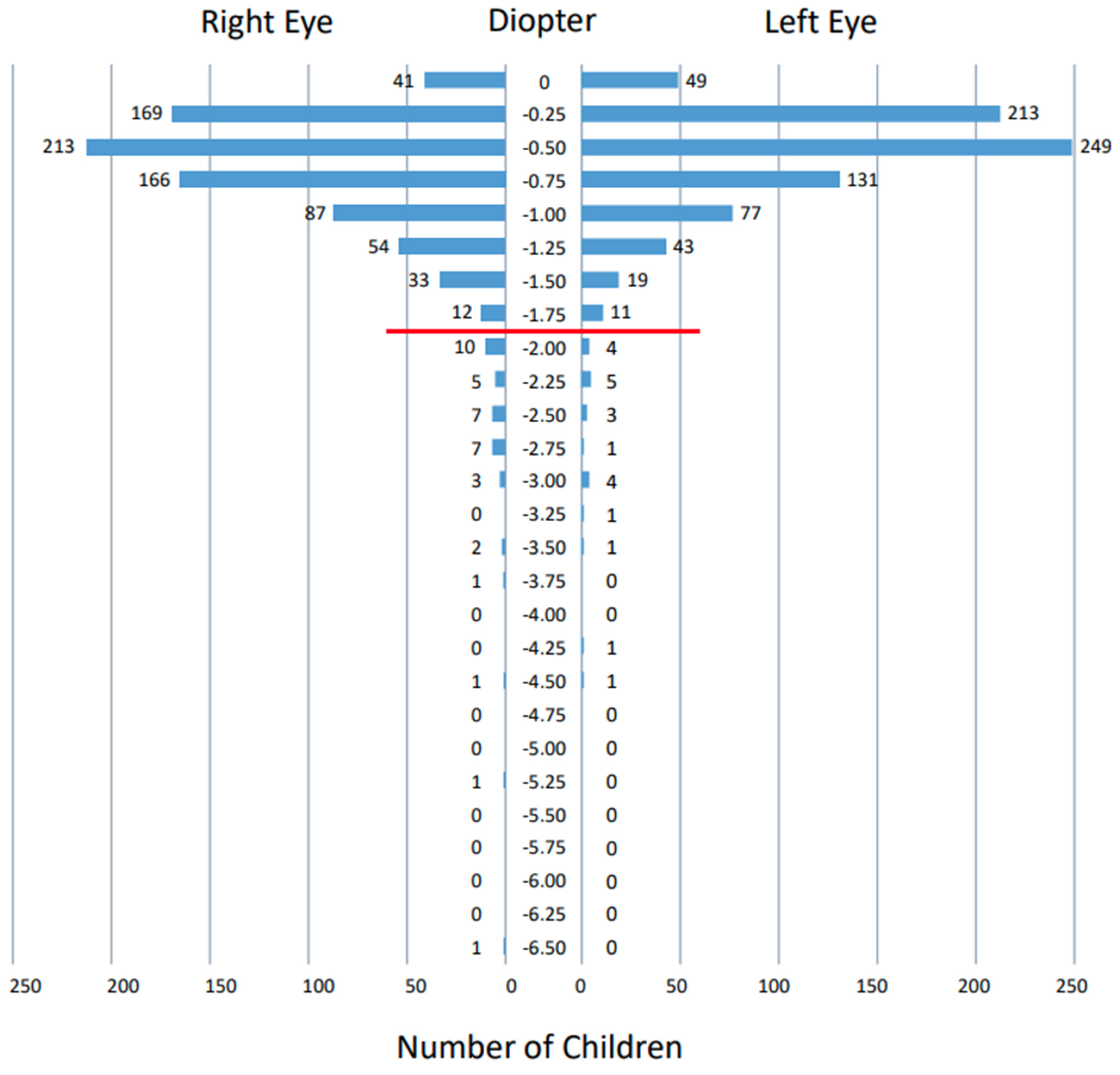
3.3. Measurements by Spot Vision Screener
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Yazawa, K.; Suga, J.; Wakita, S.; Sumitomo, M.; Uemura, Y. The Tokyo Metropolitan Home Vision Screening Program for Amblyopia in 3-Year-Old Children. Am. J. Ophthalmol. 1992, 114, 416–419. [Google Scholar] [CrossRef]
- Matsuo, T.; Matsuo, C.; Matsuoka, H.; Kio, K. Detection of strabismus and amblyopia in 1.5- and 3-year-old children by a preschool vision-screening program in Japan. Acta Med. Okayama 2007, 61, 9–16. [Google Scholar] [PubMed]
- Matsuo, T.; Matsuo, C.; Kio, K.; Ichiba, N.; Matsuoka, H. Is refraction with a hand-held autorefractometer useful in addition to visual acuity testing and questionnaires in preschool vision screening at 3.5 years in Japan? Acta Med. Okayama 2009, 63, 195–202. [Google Scholar] [PubMed]
- Harvey, E.M.; Miller, J.M.; Wagner, L.K.; Dobson, V. Reproducibility and accuracy of measurements with a hand held autorefractor in children. Br. J. Ophthalmol. 1997, 81, 941–948. [Google Scholar] [CrossRef]
- El-Defrawy, S.; Clarke, W.N.; Belec, F.; Pham, B. Evaluation of a hand-held autorefractor in children younger than 6. J. Pediatr. Ophthalmol. Strabismus 1998, 35, 107–109. [Google Scholar] [CrossRef]
- Cordonnier, M.; Dramaix, M. Screening for abnormal levels of hyperopia in children: A non-cycloplegic method with a hand held refractor. Br. J. Ophthalmol. 1998, 82, 1260–1264. [Google Scholar] [CrossRef][Green Version]
- Cordonnier, M.; Dramaix, M. Screening for refractive errors in children: Accuracy of the hand held refractor Retinomax to screen for astigmatism. Br. J. Ophthalmol. 1999, 83, 157–161. [Google Scholar] [CrossRef]
- Barry, J.C.; Konig, H.H. Non-cycloplegic screening for amblyopia via refractive findings with the Nikon Retinomax hand held autorefractor in 3 year old kindergarten children. Br. J. Ophthalmol. 2001, 85, 1179–1182. [Google Scholar] [CrossRef]
- Peterseim, M.M.W.; Papa, C.E.; Wilson, M.E.; Davidson, J.D.; Shtessel, M.; Husain, M.; Cheeseman, E.W.; Wolf, B.J.; Trivedi, R. The effectiveness of the Spot Vision Screener in detecting amblyopia risk factors. J. Am. Assoc. Pediatr. Ophthalmol. Strabismus 2014, 18, 539–542. [Google Scholar] [CrossRef]
- Forcina, B.D.; Peterseim, M.M.; Wilson, M.E.; Cheeseman, E.W.; Feldman, S.; Marzolf, A.L.; Wolf, B.J.; Trivedi, R.H. Performance of the Spot Vision Screener in Children Younger than 3 Years of Age. Am. J. Ophthalmol. 2017, 178, 79–83. [Google Scholar] [CrossRef]
- Satou, T.; Nogami, T.; Takahashi, Y.; Ito, M.; Niida, T. The Repeatability of Values Measured Using the Spot Vision Screener in Healthy Children and Children with Refractive Errors. J. Binocul. Vis. Ocul. Motil. 2019, 69, 82–86. [Google Scholar] [CrossRef] [PubMed]
- Srinivasan, G.; Russo, D.; Taylor, C.; Guarino, A.; Tattersall, P.; Moore, B. Validity of the Spot Vision Screener in detecting vision disorders in children 6 months to 36 months of age. J. Am. Assoc. Pediatr. Ophthalmol. Strabismus 2019, 23, 278.e1–278.e6. [Google Scholar] [CrossRef] [PubMed]
- Tatara, S.; Maeda, F.; Mizuno, N.; Noguchi, A.; Yaoeda, K.; Abe, H. Refraction and pupil diameter in 3-year- and 1-month-old children as measured by Spot Vision Screener. Sci. Rep. 2019, 9, 15622–15626. [Google Scholar] [CrossRef] [PubMed]
- Gaiser, H.; Moore, B.; Srinivasan, G.; Solaka, N.; He, R. Detection of Amblyogenic Refractive Error Using the Spot Vision Screener in Children. Optom. Vis. Sci. 2020, 97, 324–331. [Google Scholar] [CrossRef] [PubMed]
- Misra, N.; Khanna, R.C.; Mettla, A.L.; Marmamula, S.; Keeffe, J.E. Agreement and diagnostic accuracy of vision screening in preschool children between vision technicians and spot vision screener. Indian J. Ophthalmol. 2021, 69, 117–121. [Google Scholar] [CrossRef] [PubMed]
- Hayashi, S.; Suzuki, I.; Inamura, A.; Iino, Y.; Nishitsuka, K.; Nishina, S.; Yamashita, H. Effectiveness of the Spot Vision Screener in screening 3-year-old children with potential amblyopia in Japan. Jpn. J. Ophthalmol. 2021, 65, 537–545. [Google Scholar] [CrossRef]
- Kapoor, V.; Shah, S.P.; Beckman, T.; Gole, G. Community based vision screening in preschool children; performance of the Spot Vision Screener and optotype testing. Ophthalmic Epidemiol. 2021, 1–9. [Google Scholar] [CrossRef]
- Matsuo, T.; Matsuo, C. The Prevalence of Strabismus and Amblyopia in Japanese Elementary School Children. Ophthalmic Epidemiol. 2005, 12, 31–36. [Google Scholar] [CrossRef]
- Matsuo, T.; Matsuo, C. Comparison of prevalence rates of strabismus and amblyopia in Japanese elementary school children between the years 2003 and 2005. Acta Med. Okayama 2007, 61, 329–334. [Google Scholar]
- Matsuo, T.; Yorifuji, T. Television-watching in the early years of life and the association with parents’ concerns about decreased visual acuity in their elementary school-aged child: Results of a nationwide population-based longitudinal survey of Japan. Jpn. J. Ophthalmol. 2021, 65, 561–568. [Google Scholar] [CrossRef]
- Matsuo, T. Intraocular lens implantation in unilateral congenital cataract with minimal levels of persistent fetal vasculature in the first 18 months of life. SpringerPlus 2014, 3, 361. [Google Scholar] [CrossRef] [PubMed]
- Matsuo, T. How far is observation allowed in patients with ectopia lentis? SpringerPlus 2015, 4, 461. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Matsuo, T. Clinical decision upon resection or observation of ocular surface dermoid lesions with the visual axis unaffected in pediatric patients. SpringerPlus 2015, 4, 534. [Google Scholar] [CrossRef][Green Version]
- Matsuo, T. The timing for diagnosis of anisometropia in Japanese children with congenital eyelid ptosis. Clin. Surg. 2020, 5, 2842. [Google Scholar]
- Aoba, K.; Matsuo, T.; Hamasaki, I.; Hasebe, K. Clinical factors underlying a single surgery or repetitive surgeries to treat superior oblique muscle palsy. SpringerPlus 2015, 4, 166. [Google Scholar] [CrossRef]
- Matsuo, T.; Yamane, T.; Fujiwara, H.; Ohtsuki, H.; Watanabe, Y. Predictive Factors for Long-Term Outcome of Stereoacuity in Japanese Patients with Pure Accommodative Esotropia. Strabismus 2005, 13, 79–84. [Google Scholar] [CrossRef] [PubMed]
- Matsuo, T.; Kawaishi, Y.; Kuroda, R.; Ohtsuki, H.; Watanabe, Y. Long-term visual outcome in primary microtropia. Jpn. J. Ophthalmol. 2003, 47, 507–511. [Google Scholar] [CrossRef]

| Vision Test at Home | |
|---|---|
| Yes or No |
| Yes or No |
| Yes or No |
| Yes or No |
| Yes or No |
| Questions for symptoms | |
| Yes or No |
| Yes or No |
| Yes or No |
| |
| Yes or No |
| Yes or No |
| Yes or No |
| Yes or No |
| Yes or No |
| Yes or No |
| Yes or No |
| Yes or No |
| Yes or No |
| Yes or No |
| Yes or No |
| Yes or No |
|
| Visual Acuity Testing Results | No Pass at Spot Vision Screener Standard | Pass at Spot Vision Screener Standard | Total |
|---|---|---|---|
| Pass at testing in Health Center | 10 | 0 | 10 |
| Failure in Health Center (in total) | 20 | 43 | 63 |
| 0.5 in the right eye, 0.1 in the left eye | 2 | 1 | 3 |
| 0.1 in the right eye, 0.5 in the left eye | 2 | 3 | 5 |
| 0.1 in both eyes | 10 | 7 | 17 |
| Unmeasurable in both eyes | 6 | 32 | 38 |
| Reasons for Issuance | Notice | Diagnoses on Returned Documents | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Visual acuity testing standard | Spot vision screener standard | Others | Required but not issued | Reasons for non-issuance | Issued in total | Issued and retuned with no findings | Issued and returned with findings | Issued but not returned | |||
| Pass | No pass | none | 6 | Followed | 6 | 45 | 4 | 38 (12 *) | 3 | Anisometropic amblyopia Ametropic amblyopia Accommodative esotropia Intermittent exotropia Hyperopia/hyperopic astigmatism Mixed astigmatism Myopic astigmatism Anisocoria Entropion | 4 8 1 3 13 6 3 1 1 |
| No pass | No pass | none | 5 | Followed | 5 | 15 | 0 | 12 (6 *) | 3 | Anisometropic amblyopia Ametropic amblyopia Accommodative esotropia Hyperopia/hyperopic astigmatism Mixed astigmatism Myopic astigmatism Down syndrome | 5 4 1 1 1 1 1 |
| No pass | Pass | none | 10 | Followed No wish Unknown | 5 1 4 | 33 | 7 | 13 (2 *) | 13 | Anisometropic amblyopia Ametropic amblyopia Intermittent exotropia Hyperopia/hyperopic astigmatism Mixed astigmatism Myopic astigmatism | 2 4 2 2 1 1 |
| Pass | Pass | photophobia | 0 | 2 | 2 | 0 | 0 | ||||
| In total | 21 | 95 | 13 | 63 | 19 | ||||||
| Pass at Visual Acuity Testing Standard | No pass at Visual Acuity Testing Standard | Total | |
|---|---|---|---|
| Anisometropia, astigmatism | 2 | 0 | 2 |
| Anisometropia | 4 | 1 | 5 |
| Anisometropia, hyperopia | 4 | 6 | 10 |
| Anisometropia, hyperopic astigmatism | 0 | 0 | 0 |
| Astigmatism in either eye | 18 | 4 | 22 |
| Astigmatism in both eyes | 16 | 4 | 20 |
| Hyperopia in either eye | 0 | 0 | 0 |
| Hyperopia in both eyes | 4 | 2 | 6 |
| Myopia in both eyes | 0 | 2 | 2 |
| Strabismus | 8 | 3 | 11 |
| Anisocoria | 1 | 0 | 1 |
| In total | 57 | 22 | 79 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Matsuo, T.; Matsuo, C.; Kayano, M.; Mitsufuji, A.; Satou, C.; Matsuoka, H. Photorefraction with Spot Vision Screener versus Visual Acuity Testing as Community-Based Preschool Vision Screening at the Age of 3.5 Years in Japan. Int. J. Environ. Res. Public Health 2022, 19, 8655. https://doi.org/10.3390/ijerph19148655
Matsuo T, Matsuo C, Kayano M, Mitsufuji A, Satou C, Matsuoka H. Photorefraction with Spot Vision Screener versus Visual Acuity Testing as Community-Based Preschool Vision Screening at the Age of 3.5 Years in Japan. International Journal of Environmental Research and Public Health. 2022; 19(14):8655. https://doi.org/10.3390/ijerph19148655
Chicago/Turabian StyleMatsuo, Toshihiko, Chie Matsuo, Masami Kayano, Aya Mitsufuji, Chiyori Satou, and Hiroaki Matsuoka. 2022. "Photorefraction with Spot Vision Screener versus Visual Acuity Testing as Community-Based Preschool Vision Screening at the Age of 3.5 Years in Japan" International Journal of Environmental Research and Public Health 19, no. 14: 8655. https://doi.org/10.3390/ijerph19148655
APA StyleMatsuo, T., Matsuo, C., Kayano, M., Mitsufuji, A., Satou, C., & Matsuoka, H. (2022). Photorefraction with Spot Vision Screener versus Visual Acuity Testing as Community-Based Preschool Vision Screening at the Age of 3.5 Years in Japan. International Journal of Environmental Research and Public Health, 19(14), 8655. https://doi.org/10.3390/ijerph19148655






