We Need Engaged Workers! A Structural Equation Modeling Study from the Positive Organizational Psychology in Times of COVID-19 in Chile
Abstract
:1. Introduction
2. Theoretical Framework
2.1. Healthy Organizational Practices
2.2. Engagement and Burnout
3. Materials and Methods
3.1. Instruments
3.2. Statistical Analysis
4. Results
5. Discussion
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Appendix A
- In this organization, mechanisms and strategies have been launched over the last year to facilitate the reconciliation of work life and private life of its employees
- In this organization, mechanisms and strategies have been implemented over the last year to guarantee the prevention and management of mobbing
- In this organization, mechanisms and strategies have been put in place over the last year to facilitate the development of workers’ skills
- In this organization, mechanisms and strategies have been put in place over the last year to facilitate the career development of workers
- In this organization, mechanisms and strategies have been implemented over the last year to ensure well-being and quality of life at work
- In this organization, mechanisms and strategies have been put in place over the last year to guarantee that workers receive fair rewards in accordance with the effort we make
- In this organization, mechanisms and strategies have been put in place over the last year to guarantee social responsibility issues in the organization
- In this organization, mechanisms and strategies have been put in place over the last year to facilitate communication from the management to the workers, as well as from the workers to the management
- In this organization, mechanisms and strategies have been put in place over the last year to inform about the objectives of the organization so that they are known by all.
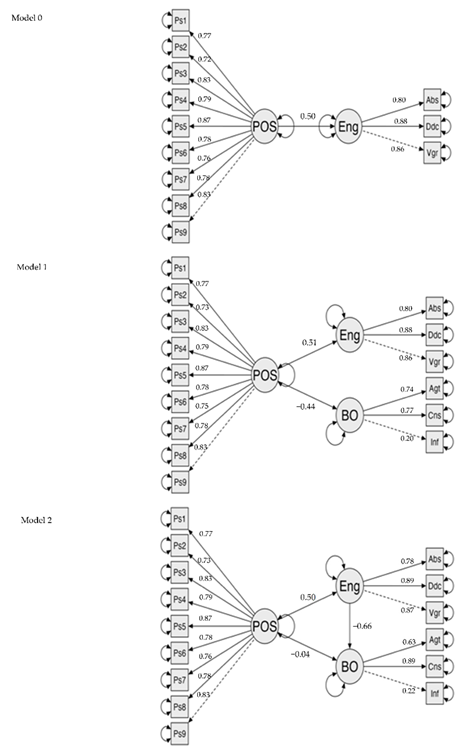
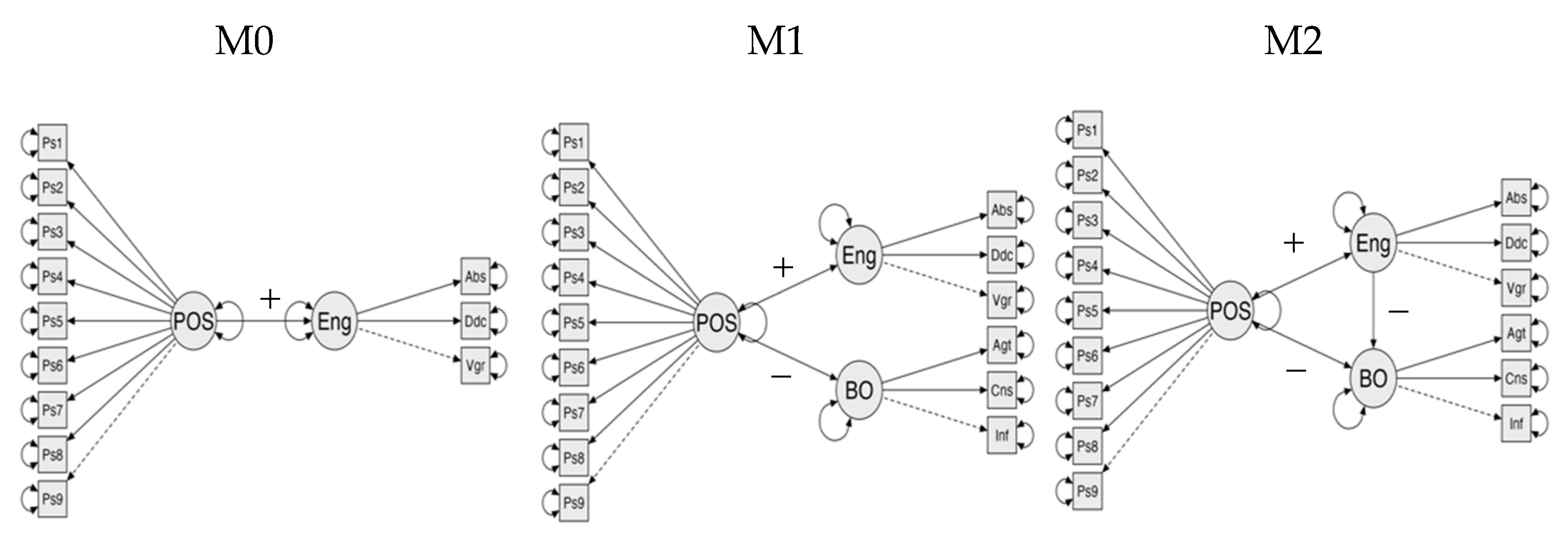
Appendix B. Factor Loading in the Three Different Models
References
- Izaguirre-Torres, D.; Siche, R. COVID-19 disease will cause a global catastrophe in terms of mental health: A hypothesis. Med. Hypotheses 2020, 143, 109846. [Google Scholar] [CrossRef]
- Yao, H.; Chen, J.-H.; Xu, Y.-F. Patients with mental health disorders in the COVID-19 epidemic. Lancet Psychiatry 2020, 7, 547–560. [Google Scholar] [CrossRef]
- Wang, C.; Pan, R.; Wan, X.; Tan, Y.; Xu, L.; Ho, C.S.; Ho, R.C. Immediate psychological responses and associated factors during the initial stage of the 2019 coronavirus disease (COVID-19) epidemic among the general population in China. Int. J. Environ. Res. Public Health 2020, 17, 1729. [Google Scholar] [CrossRef] [Green Version]
- Li, Z.; Ge, J.; Yang, M.; Feng, J.; Qiao, M.; Jiang, R.; Yang, C. Vicarious traumatization in the general public, members, and non-members of medical teams aiding in COVID-19 control. Brain Behav. Immun. 2020, 88, 916–919. [Google Scholar] [CrossRef]
- Brooks, S.K.; Webster, R.K.; Smith, L.E.; Woodland, L.; Wessely, S.; Greenberg, N.; Rubin, G.J. The psychological impact of quarantine and how to reduce it: Rapid review of the evidence. Lancet 2020, 395, 912–920. [Google Scholar] [CrossRef] [Green Version]
- Helms, J.; Kremer, S.; Merdji, H.; Clere-Jehl, R.; Schenck, M.; Kummerlen, C.; Meziani, F. Neurologic features in severe SARS-CoV-2 infection. N. Engl. J. Med. 2020, 382, 2268–2270. [Google Scholar] [CrossRef]
- Grover, S.; Dua, D.; Sahoo, S.; Mehra, A.; Nehra, R.; Chakrabarti, S. Why all COVID-19 hospitals should have mental health professionals: The importance of mental health in a worldwide crisis! Asian J. Psychiatry 2020, 51, 102156. [Google Scholar] [CrossRef]
- Fiorillo, A.; Sampogna, G.; Giallonardo, V.; Del Vecchio, V.; Luciano, M.; Albert, U.; Carmassi, C.; Carrà, G.; Cirulli, F.; Dell’Osso, B.; et al. Effects of the lockdown on the mental health of the general population during the COVID-19 pandemic in Italy: Results from the COMET Collaborative Network. Eur. Psychiatry 2020, 63, E87. [Google Scholar] [CrossRef]
- Salanova. M. How to survive COVID-19? Notes from organisational resilience (¿Cómo sobrevivir al COVID-19? Apuntes desde la resiliencia organizacional). Int. J. Soc. Psychol. 2020, 35, 670–676. [Google Scholar] [CrossRef]
- Salanova, M.; Llorens, S.; Cifre, E.; Martínez, I. We Need a Hero! Toward a Validation of the Healthy and Resilient Organization (HERO) Model. Group Organ. Manag. 2012, 37, 785–822. [Google Scholar] [CrossRef]
- de Sire, A.; Marotta, N.; Raimo, S.; Lippi, L.; Inzitari, M.; Tasselli, A.; Gimigliano, A.; Palermo, L.; Invernizzi, M.; Ammendolia, A. Psychological Distress and Work Environment Perception by Physical Therapists from Southern Italy during COVID-19 Pandemic: The C.A.L.A.B.R.I.A Study. Int. J. Environ. Res. Public Health 2021, 18, 9676. [Google Scholar] [CrossRef]
- Sonnentag, S.; Mojza, E.J.; Demerouti, E.; Bakker, A.B. Reciprocal relations between recovery and work engagement: The moderating role of job stressors. J. Appl. Psychol. 2012, 97, 842–853. [Google Scholar] [CrossRef]
- Rich, B.; Jeffrey, A.L.; Eean, C. Job Engagement: Antecedents and Effects on Job Performance. Acad. Manag. J. 2010, 53, 617–635. [Google Scholar] [CrossRef]
- Bakker, A.; Bal, P. Weekly work engagement and performance: A study among starting teachers. J. Occup. Organ. Psychol. 2010, 83, 189–206. [Google Scholar] [CrossRef]
- Bakker, A.; Tims, M.; Derks, D. Proactive personality and job performance: The role of job crafting and work engagement. Hum. Relat. 2010, 65, 1359–1378. [Google Scholar] [CrossRef]
- Tims, M.; Bakker, A.B.; Derks, D.; van Rhenen, W. Job Crafting at the Team and Individual Level. Group Organ. Manag. 2013, 38, 427–454. [Google Scholar] [CrossRef]
- Van Wingerden, J.; Derks, D.; Bakker, A.B. The Impact of Personal Resources and Job Crafting Interventions on Work Engagement and Performance. Hum. Resour. Manag. 2015, 56, 51–67. [Google Scholar] [CrossRef]
- Bailey, C.; Madden, A.; Alfes, K.; Fletcher, L. The Meaning, Antecedents and Outcomes of Employee Engagement: A Narrative Synthesis. Int. J. Manag. Rev. 2015, 19, 31–53. [Google Scholar] [CrossRef] [Green Version]
- Amor, A.M.; Xanthopoulou, D.; Calvo, N.; Abeal Vázquez, J.P. Structural empowerment, psychological empowerment, and work engagement: A cross-country study. Eur. Manag. J. 2021, 39, 779–789. [Google Scholar] [CrossRef]
- Salanova, M.; Llorens, S.; Martínez, I.M. Contributions from positive organizational psychology to develop healthy and resilient organizations. Papeles Psicol. 2016, 37, 177–184. [Google Scholar]
- Cameron, K.; Mora, C.; Leutscher, T.; Calarco, M. Effects of positive practices on organizational effectiveness. J. Appl. Behav. Sci. 2011, 47, 266–308. [Google Scholar] [CrossRef]
- Alfes, K.; Shantz, A.D.; Truss, C.; Soane, E.C. The link between perceived human resource management practices, engagement and employee behaviour: A moderated mediation model. Int. J. Hum. Resour. Manag. 2013, 24, 330–351. [Google Scholar] [CrossRef] [Green Version]
- Acosta, H.; Torrente, P.; Llorens, S.; Salanova, M. Prácticas organizacionales saludables: Un análisis exploratorio de su impacto relativo sobre el engagement con el trabajo. Rev. Peru. Psicol. Trab. Soc. 2013, 2, 107–120. [Google Scholar]
- Shuck, B.; Twyford, D.; Reio, T.G.; Shuck, A. Human Resource Development Practices and Employee Engagement: Examining the Connection with Employee Turnover Intentions. Hum. Resour. Dev. Q. 2014, 25, 239–270. [Google Scholar] [CrossRef]
- Zhong, L.; Wayne, S.J.; Liden, R.C. Job engagement, perceived organizational support, high-performance human resource practices, and cultural value orientations: A cross-level investigation. J. Organ. Behav. 2015, 37, 823–844. [Google Scholar] [CrossRef]
- Matziari, A.; Montgomery, A.J.; Georganta, K.; Doulougeri, K. The Relationship between Organizational Practices and Values with Burnout and Engagement. Curr. Psychol. 2016, 36, 276–285. [Google Scholar] [CrossRef]
- Solares, J.; Peñalver, J.; Meneghel, I.; Salanova, M. Desarrollando Equipos Empáticos: La influencia de las prácticas organizacionales saludables en la empatía colectiva. Rev. Psicol. 2016, 6, 51–63. [Google Scholar]
- Salanova, M.; Acosta-Antognoni, H.; Llorens, S.; Le Blanc, P. We Trust You! A Multilevel-Multireferent Model Based on Organizational Trust to Explain Performance. Int. J. Environ. Res. Public Health 2021, 18, 4241. [Google Scholar] [CrossRef]
- Wang, C.; Pan, R.; Wan, X.; Tan, Y.; Xu, L.; McIntyre, R.; Choo, F.; Tran, B.; Ho, R.; Sharma, V.; et al. A longitudinal study on the mental health of general population during the COVID-19 epidemic in China. Brain Behav. Inmunity 2020, 87, 40–48. [Google Scholar] [CrossRef]
- Acuña-Hormazabal, A.; Mendoza-Llanos, R.; Pons-Peregot, O. Burnout, engagement, and perception of management practice in pandemic by COVID-19 in south-central Chilean workers. Estud. Gerenc. 2021, 37, 104–112. [Google Scholar] [CrossRef]
- Luceño-Moreno, L.; Talavera-Velasco, B.; García-Albuerne, Y.; Martín-García, J. Symptoms of Posttraumatic Stress, Anxiety, Depression, Levels of Resilience and Burnout in Spanish Health Personnel during the COVID-19 Pandemic. Int. J. Environ. Res. Public Health 2020, 17, 5514. [Google Scholar] [CrossRef] [PubMed]
- Torrès, O.; Benzari, A.; Fisch, C.; Mukerjee, J.; Swalhi, A.; Thurik, R. Risk of burnout in French entrepreneurs during the COVID-19 crisis. Small Bus. Econ. 2021, 58, 717–739. [Google Scholar] [CrossRef]
- Seligman, M.; Csikszentmihalyi, M. Positive psychology: An introduction. Am. Psychol. 2000, 55, 5–14. [Google Scholar] [CrossRef]
- Seligman, M.; Csikszentmihalyi, M. Positive Psychology: An Introduction. In Flow and the Foundations of Positive Psychology; Springer: Dordrecht, The Netherlands, 2014; pp. 279–298. [Google Scholar] [CrossRef]
- Kim, H.; Doiron, K.; Warren, M.; Donaldson, S. The international landscape of positive psychology research: A systematic review. Int. J. Wellbeing 2018, 8, 50–70. [Google Scholar] [CrossRef]
- Clark, J.V. A healthy organization. Calif. Manag. Rev. 1962, 4, 16–30. [Google Scholar] [CrossRef]
- Potthoff, E. Precedence for healthy business financing. Betrieb 1973, 26, 2–4. [Google Scholar]
- Cooper, C.L.; Cartwright, S. Healthy Mind; Healthy Organization—A Proactive Approach to Occupational Stress. Hum. Relat. 1994, 47, 455–471. [Google Scholar] [CrossRef]
- Wright, P.; McMahan, G. Theoretical perspectives for strategic human resources management. J. Manag. 1992, 18, 295–320. [Google Scholar] [CrossRef]
- Lyubomirsky, S.; King, L.; Diener, E. The benefits of frequent positive affect: Does happiness lead to success? Psychol. Bull. 2005, 131, 803–855. [Google Scholar] [CrossRef] [Green Version]
- Alfes, K.; Shantz, A.; Truss, C. The link between perceived HRM practices, performance and well-being: The moderating effect of trust in the employer. Hum. Resour. Manag. J. 2012, 22, 409–427. [Google Scholar] [CrossRef]
- Schaufeli, W.; Bakker, A.; Van Rhenen, W. How changes in job demands and resources predict burnout, work engagement, and sickness absenteeism. J. Organ. Behav. 2009, 30, 893–917. [Google Scholar] [CrossRef] [Green Version]
- Bakker, A.; Demerouti, E.; Sanz-Vergel, A. Burnout and Work Engagement: The JD–R Approach. Annu. Rev. Organ. Psychol. Organ. Behav. 2014, 1, 389–411. [Google Scholar] [CrossRef]
- Saari, T.; Melin, H.; Balabonova, E.; Efendiev, A. The job demands and resources as antecedents of work engagement Comparative research on Finland and Russia. Baltic J. Manag. 2017, 12, 240–254. [Google Scholar] [CrossRef]
- Maslach, C.; Jackson, S.E. The measurement of experienced burnout. J. Occup. Behav. 1981, 2, 99–113. [Google Scholar] [CrossRef]
- Bakker, A.B.; Schaufeli, W.B.; Leiter, M.P.; Taris, T.W. Work engagement: An emerging concept in occupational health psychology. Work. Stress 2008, 22, 187–200. [Google Scholar] [CrossRef]
- Parker, S.K.; Bindl, U.; Strauss, K. Making things happen: A model of proactive motivation. J. Manag. 2010, 36, 827–856. [Google Scholar] [CrossRef] [Green Version]
- Parker, S.K.; Griffin, M.A. Understanding active psychological states: Embedding engagement in a wider nomological net and closer attention to performance. Eur. J. Work. Organ. Psychol. 2011, 20, 60–67. [Google Scholar] [CrossRef]
- Hussein, S. Work Engagement, Burnout and Personal Accomplishments among Social Workers: A Comparison between Those Working in Children and Adults’ Services in England. Adm. Policy Ment. Health Ment. Health Serv. Res. 2018, 45, 911–923. [Google Scholar] [CrossRef] [Green Version]
- Bakker, A.B.; Emmerik, H.V.; Euwema, M.C. Crossover of Burnout and Engagement in Work Teams. Work. Occup. 2006, 33, 464–489. [Google Scholar] [CrossRef]
- Cole, M.S.; Walter, F.; Bedeian, A.G.; O’Boyle, E.H. Job Burnout and Employee Engagement. J. Manag. 2011, 38, 1550–1581. [Google Scholar] [CrossRef]
- Ahmed, O.; Hossain, K.; Ferdousi Siddique, R.; Jobe, M. COVID-19 fear, stress, sleep quality and coping activities during lockdown, and personality traits: A person-centered approach analysis. Personal. Individ. Differ. 2021, 178, 110873. [Google Scholar] [CrossRef]
- Schaufeli, W.; Martínez, I.; Pinto, A.; Salanova, M.; Bakker, A. Burnout and Engagement in University Students: A Cross-National Study. J. Cross Cult. Psychol. 2002, 33, 464–481. [Google Scholar] [CrossRef] [Green Version]
- Maslach, C.; Jackson, S.; Leiter, M. Maslach burnout inventory. Palo Alto: Consult. Psychol. Press 1986, 21, 3463–3464. [Google Scholar]
- Moreno-Jiménez, B.; Rodríguez-Carvajal, R.; Escobar, E. La evaluación del burnout profesional. Factorializacion del MBI-GS. Un análisis preliminar. Ansiedad Estrés 2001, 7, 69–78. [Google Scholar]
- Lloret-Segura, S.; Ferreres-Traver, A.; Hernández-Baeza, A.; Tomás-Marco, I. El análisis factorial exploratorio de los ítems: Una guía práctica, revisada y actualizada. Introducción Determinación de la adecuación del Análisis. An. Psicol. 2014, 30, 1151–1169. [Google Scholar] [CrossRef]
- Ximénez, M.C.; García, A.G. Comparación de los métodos de estimación de máxima verosimilitud y mínimos cuadrados no ponderados en el análisis factorial confirmatorio mediante simulación Monte Carlo. Psicothema 2005, 17, 528–535. [Google Scholar]
- Schermelleh-Engel, K.; Moosbrugger, H. Evaluating the Fit of Structural Equation Models: Tests of Significance and Descriptive Goodness-of-Fit Measures. Methods Psychol. Res. Online 2003, 8, 23–74. [Google Scholar]
- Herrero, J. El Análisis Factorial Confirmatorio en el estudio de la Estructura y Estabilidad de los Instrumentos de Evaluación: Un ejemplo con el Cuestionario de Autoestima CA-14. Psychosoc. Interv. 2010, 19, 289–300. [Google Scholar] [CrossRef]
- JASP Team. JASP (Version 0.16) [Computer Software]. 2021. Available online: https://jasp-stats.org (accessed on 30 December 2021).
- Mehta, P. Work from home—Work engagement amid COVID-19 lockdown and employee happiness. J. Public Aff. 2021, 21, e2709. [Google Scholar] [CrossRef]
- Domínguez-Salas, S.; Gómez-Salgado, J.; Guillén-Gestoso, C.; Romero-Martín, M.; Ortega-Moreno, M.; Ruiz-Frutos, C. Health care workers’ protection and psychological safety during the COVID-19 pandemic in Spain. J. Nurs. Manag. 2021, 29, 1924–1933. [Google Scholar] [CrossRef]
- Areosa, J.; Queiros, C. Burnout: A reconfigured social pathology in the COVID-19 era? Int. J. Work. Cond. 2020, 20, 71–90. [Google Scholar]
- Peinado, M.; Anderson, K. Reducing social worker burnout during COVID-19. Int. Soc. Work. 2020, 63, 757–760. [Google Scholar] [CrossRef]
- Jalili, M.; Niroomand, M.; Hadavand, F.; Zeinali, K.; Fotouhi, A. Burnout among healthcare professionals during COVID-19 pandemic: A cross-sectional study. Int. Arch. Occup. Environ. Health 2021, 94, 1345–1352. [Google Scholar] [CrossRef] [PubMed]
- Nicola, M.; Alsafi, Z.; Sohrabi, C.; Kerwan, A.; Al-Jabir, A.; Iosifidis, C.; Agha, M.; Agha, R. The socio-economic implications of the coronavirus pandemic (COVID-19): A review. Int. J. Surg. 2020, 78, 185–193. [Google Scholar] [CrossRef]
- Caballero-Domínguez, C.C.; Campo-Arias, A. Problemas de salud mental en la sociedad: Un acercamiento desde el impacto del COVID 19 y de la cuarentena. Duazary 2020, 17, 1–3. [Google Scholar] [CrossRef]
- Lorenzo, A.; Diaz, K.; Zaldivar, D. La psicología como ciencia en el afrontamiento a la COVID-19: Apuntes generales. An. Acad. Cienc. Cuba. 2020, 10, 839. [Google Scholar]
- Duffy, R.D.; Dik, B.J.; Douglass, R.P.; England, J.W.; Velez, B.L. Work as a calling: A theoretical model. J. Couns. Psychol. 2018, 65, 423–439. [Google Scholar] [CrossRef]
- Amano, H.; Fukuda, Y.; Shibuya, K.; Ozaki, A.; Tabuchi, T. Factors Associated with the Work Engagement of Employees Working from Home during the COVID-19 Pandemic in Japan. Int. J. Environ. Res. Public Health 2021, 18, 10495. [Google Scholar] [CrossRef]
- Bartsch, C.E.; Durr, L.; Forster, A.; Koob, C. Wie sind Schlüsselressourcen und-anforderungen mit dem Arbeitsengagement Pflegender während der COVID-19-Pandemie assoziiert? Eine Querschnittstudie. Z. Evidenz Fortbild. Qual. Gesundh. 2021, 167, 57–67. [Google Scholar] [CrossRef]
- Reinwald, M.; Zimmermann, S.; Kunze, F. Working in the Eye of the Pandemic: Local COVID-19 Infections and Daily Employee Engagement. Front. Psychol. 2021, 12, 2544. [Google Scholar] [CrossRef]
- Pérez, E.; Medrano, L.A.; Sánchez Rosas, J. Path Analysis: Basic concepts and examples. Rev. Argent. Cienc. Comport. 2013, 5, 52–66. [Google Scholar] [CrossRef]
- Pajares, F.; Miller, M.D.; Johnson, M.J. Gender differences in writing self-beliefs of elementary school students. J. Educ. Psychol. 1999, 91, 50–61. [Google Scholar] [CrossRef]
| Engagement | Burnout | Healthy Organizational Rractices | ||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| M | SD | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 | 12 | 13 | 14 | |||||||||||||||
| 1. Absorption | 4.72 | 0.95 | — | |||||||||||||||||||||||||||
| 2. Dedication | 5.17 | 0.96 | 0.70 | * | — | |||||||||||||||||||||||||
| 3. Vigor | 5.09 | 0.76 | 0.70 | * | 0.75 | * | — | |||||||||||||||||||||||
| 4. Emotional exhaustion | 2.47 | 1.49 | −0.22 | * | −0.36 | * | −0.45 | * | — | |||||||||||||||||||||
| 5. Cynicism | 1.10 | 1.32 | −0.37 | * | −0.57 | * | −0.54 | * | 0.57 | * | — | |||||||||||||||||||
| 6. Professional Inefficiency | 3.38 | 2.24 | −0.25 | * | −0.17 | * | −0.10 | ♺ | 0.08 | ♺ | 0.19 | * | — | |||||||||||||||||
| 7. Reconciliation | 3.72 | 1.77 | 0.28 | * | 0.36 | * | 0.34 | * | −0.29 | * | −0.22 | * | −0.07 | — | ||||||||||||||||
| 8. Mobbing prevention | 3.51 | 2.15 | 0.22 | * | 0.34 | * | 0.30 | * | −0.24 | * | −0.25 | * | −0.07 | 0.65 | * | — | ||||||||||||||
| 9. Skill development | 3.77 | 1.85 | 0.24 | * | 0.35 | * | 0.29 | * | −0.26 | * | −0.22 | * | −0.01 | 0.62 | * | 0.65 | * | — | ||||||||||||
| 10. Career Development | 3.51 | 1.88 | 0.25 | * | 0.34 | * | 0.27 | * | −0.22 | * | −0.21 | * | −0.03 | 0.58 | * | 0.56 | * | 0.75 | * | — | ||||||||||
| 11. Labor Health | 3.92 | 1.75 | 0.29 | * | 0.38 | * | 0.36 | * | −0.32 | * | −0.27 | * | −0.08 | ♺ | 0.69 | * | 0.62 | * | 0.70 | * | 0.68 | * | — | |||||||
| 12. Equity | 3.28 | 1.98 | 0.29 | * | 0.34 | * | 0.36 | * | −0.31 | * | −0.22 | * | −0.10 | ♺ | 0.58 | * | 0.53 | * | 0.67 | * | 0.63 | * | 0.69 | * | — | |||||
| 13. Information | 4.05 | 1.74 | 0.30 | * | 0.38 | * | 0.36 | * | −0.22 | * | −0.23 | * | −0.08 | 0.53 | * | 0.50 | * | 0.55 | * | 0.56 | * | 0.64 | * | 0.60 | * | — | ||||
| 14. Communication | 4.23 | 1.66 | 0.33 | * | 0.40 | * | 0.37 | * | −0.25 | * | −0.21 | * | −0.05 | 0.61 | * | 0.51 | * | 0.57 | * | 0.57 | * | 0.66 | * | 0.56 | * | 0.71 | * | — | ||
| 15. CRS | 3.82 | 1.83 | 0.31 | * | 0.43 | * | 0.36 | * | −0.28 | * | −0.27 | * | −0.10 | ♺ | 0.58 | * | 0.60 | * | 0.65 | * | 0.66 | * | 0.71 | * | 0.63 | * | 0.67 | * | 0.68 | * |
| Models | χ2 | df | RMSEA | GFI | CFI | TLI | PNFI | Δχ2 | Δdf | p |
|---|---|---|---|---|---|---|---|---|---|---|
| M0 | 274.34 | 53 | 0.08 | 0.92 | 0.96 | 0.94 | 0.759 | |||
| M1 | 447.15 | 87 | 0.10 | 0.88 | 0.91 | 0.89 | 0.748 | 172.81 | 34 | <0.001 |
| M2 | 614.82 | 88 | 0.08 | 0.91 | 0.94 | 0.92 | 0.763 | 167.67 | 1 | <0.001 |
| Model 0 | Model 1 | Model 2 | ||||
|---|---|---|---|---|---|---|
| Predictor | β | p | β | p | β | p |
| HOP → Engagement | 0.50 | <0.001 | 0.51 | <0.001 | 0.50 | <0.001 |
| HOP → BO | −0.44 | <0.001 | −0.04 | 0.42 | ||
| Engagement → BO | −0.66 | <0.001 | ||||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mendoza-Llanos, R.; Acuña-Hormazábal, Á.; Pons-Peregort, O. We Need Engaged Workers! A Structural Equation Modeling Study from the Positive Organizational Psychology in Times of COVID-19 in Chile. Int. J. Environ. Res. Public Health 2022, 19, 7700. https://doi.org/10.3390/ijerph19137700
Mendoza-Llanos R, Acuña-Hormazábal Á, Pons-Peregort O. We Need Engaged Workers! A Structural Equation Modeling Study from the Positive Organizational Psychology in Times of COVID-19 in Chile. International Journal of Environmental Research and Public Health. 2022; 19(13):7700. https://doi.org/10.3390/ijerph19137700
Chicago/Turabian StyleMendoza-Llanos, Rodolfo, Álvaro Acuña-Hormazábal, and Olga Pons-Peregort. 2022. "We Need Engaged Workers! A Structural Equation Modeling Study from the Positive Organizational Psychology in Times of COVID-19 in Chile" International Journal of Environmental Research and Public Health 19, no. 13: 7700. https://doi.org/10.3390/ijerph19137700
APA StyleMendoza-Llanos, R., Acuña-Hormazábal, Á., & Pons-Peregort, O. (2022). We Need Engaged Workers! A Structural Equation Modeling Study from the Positive Organizational Psychology in Times of COVID-19 in Chile. International Journal of Environmental Research and Public Health, 19(13), 7700. https://doi.org/10.3390/ijerph19137700








