Effects of Infant Massage: A Systematic Review
Abstract
:1. Introduction
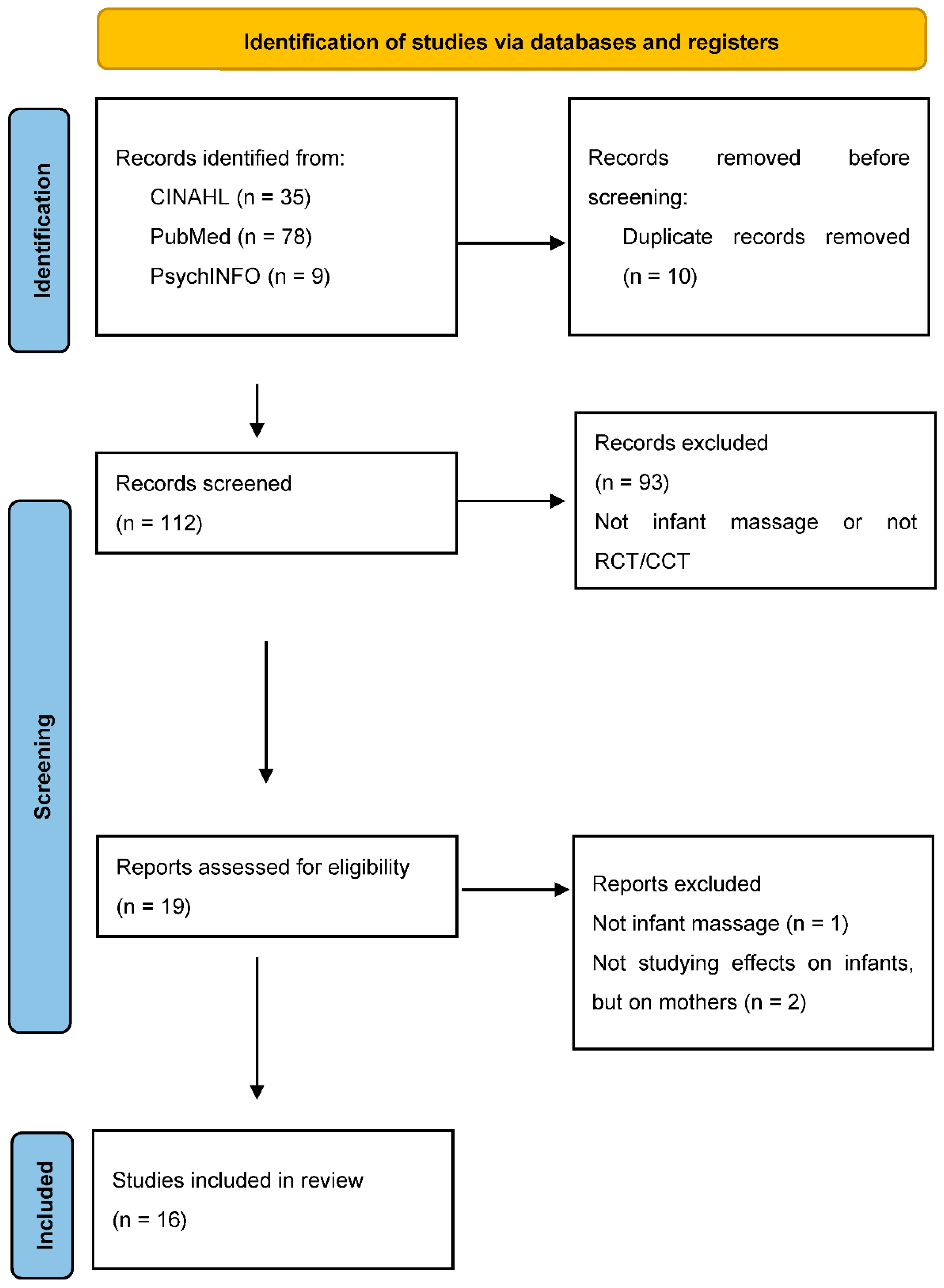
2. Materials and Methods
2.1. Design
2.2. Study Selection
- Population: infants from 0–12 months
- Intervention: infant massage administered by parents or professionals
- Control group: care as usual or other intervention
- Outcome: pain relief, jaundice, weight gain
2.3. Data Collection
2.4. Method of Analysis
3. Results
3.1. Study Characteristics
3.2. Pain Relief
3.2.1. Pain during Blood Sampling
3.2.2. Postoperative Pain
3.2.3. Colic Pain
3.3. Jaundice
3.4. Weight Gain
4. Discussion
Strengths and Limitations
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
Registration and Protocol
Appendix A. Included Studies
| Author, Year, Country | Design | Inclusion Criteria | Intervention and Control Groups | Number of Participants/Drop-outs | Time fo Follow-Up | Effects of Infant Massage | Study Quality | Outcome |
|---|---|---|---|---|---|---|---|---|
| Chik et al., 2017 China | RCT | Premature and full-term babies (weeks 30–40) | I: massage C: care as usual (cross-over) | I: 40 C: 40 Drop-out: 15 | 30 s | Less pain at venous sampling * | High | Pain relief |
| Eghbalian et al., 2017 Iran | RCT | Full-term babies with jaundice | I: massage with baby oil and phototherapy C: phototherapy | I: 67 C: 67 Drop-out: – | 4 days | Decreased levels of bilirubin day 3 and 4 * | Medium | Jaundice |
| Gözen et al., 2019 Turkey | RCT | Healthy, full-term babies | I: massage with baby oil C: care as usual | I: 44 C: 46 Drop-out: 0 | 48 h | Lower transcutan bilirubin increase * | High | Jaundice |
| Harrison et al., 2020 USA | RCT | Babies (1 day–12 months) with CCHD (Complex Congenital Heart Disease) who received their first thorax surgery | I: massage with body lotion C: rest | I: 30 C: 30 Drop out: 0 | 7 days | Less pain all days but day 7. NS | Medium | Pain relief |
| Jazayeri et al., 2021 Iran | RCT | Babies with jaundice (> week 35) | I (1): reflexology with olive oil and photo therapy I (2): massage and phototherapy C: phototherapy | I (1): 17 I (2): 17 C: 17 Drop-out: 5 | Not presented | Decreased levels of bilirubin in I (1) and I (2). * | Medium | Jaundice |
| Korkmaz & Esenay, 2020 Turkey | RCT | Full-term babies with jaundice | I: massage with baby oil and phototherapy C: phototherapy | I: 25 C: 25 Drop-out: 30 | During ongoing photo therapy | Less total serum bilirubin * | High | Jaundice |
| Liao et al., 2021 Taiwan | RCT | Prematur babies (week 28–37) | I (1): massage with MCT oil I (2): massage without oil C: care as usual | I (1): 16 I (2): 16 C: 16 Drop-out: 3 | 7 days | Day 5–7 greater weight gain in I (1) compared with I (2) and C * | High | Weight gain |
| Lori Kenari et al., 2020 Iran | RCT | Full-term babies with jaundice | I (1): massage with sunflower oil and photo therapy I (2): the kangaroo method and phototherapy C: phototherapy | I (1): 30 I (2): 30 C: 30 Drop-out: - | 72 h | Less bilirubin leves in I (1) och I (2) * | Medium | Jaundice |
| Nahidi et al., 2017 Iran | RCT | Babies with colic | I: massage with baby oil C: rocking | I: 50 C: 50 Drop-out: – | 1 week | Decreased crying incidents, crying duration and crying intensity in both I and C * | Medium | Pain relief |
| Özkan et al., 2019 Turkey | RCT | Healthy full-term babies | I (1): acupressure I (2): massage C: care as usual | I (1): 46 I (2): 47 C: 46 Drop-out: 11 | 1 min | Less pain during and 1 min after samping in I (1) och I (2). * | Medium | Pain relief |
| Rimpy & Singh, 2018 India | CCT | Premature and full-term babies with jaundice | I: massage with almond oil and phototherapy C: phototherapy | I: 20 C: 20 Drop-out: – | 3 days | Weight gain * Decreased levels of bilirubin * | Medium | Jaundice/ Weight gain |
| Roshanray et al., 2020 Iran | RCT | Healthy full-term babies | I (1): mother’s hug I (2): massage C: care as usual | I (1): 45 I (2): 45 C: 45 Drop-out: 15 | 5 min | Shorter crying duration in I (1) och I (2) compared with C * | High | Pain relief |
| Taheri et al., 2018 Iran | RCT | Healthy premature babies (week 30–36) | I: massage with sunflower oil C: care as usual | I: 22 C: 22 Drop-out: 0 | 5 days | Improved weight gain * | High | Weight gain |
| Yavaş et al., 2021 Turkey | RCT | Healthy full-term babies | I: foot massage C: care as usual | I: 64 C: 64 Drop-out: 0 | 3 min | Less pain during and after sampling * | High | Pain relief |
| Zargham-Boroujeni et al., 2017 Iran | RCT | Full-term or almost full-term babies (> week 34) | I (1): breastfeeding I (2): massage C: care as usual | I (1): 25 I (2): 25 C: 25 Drop-out: – | 30 s | Reduced pain in I (1) and I (2) * More pain relief in I (2) compared with I (1). * | Medium | Pain relief |
| Zhang & Wang, 2019 China | RCT | Prematur babies (week 32–34) | I: massage C: care as usual | I: 54 C: 58 Drop-out: – | 2 weeks | Improved weight gain * | Medium | Weight gain |
References
- Bennett, C.; Underdown, A.; Barlow, J. Massage for Promoting Mental and Physical Health in Typically Developing Infants under the Age of Six Months. Cochrane Database Syst. Rev. 2013, 2013, Cd005038. [Google Scholar] [CrossRef] [PubMed]
- Vickers, A.; Ohlsson, A.; Lacy, J.; Horsley, A. Massage for Promoting Growth and Development of Preterm and/or Low Birth-Weight Infants. Cochrane Database Syst. Rev. 2004, 2004, CD000390. [Google Scholar] [CrossRef] [PubMed]
- Stern, D.N. The Interpersonal World of the Infant: A View from Psychoanalysis and Developmental Psychology; Routledge: Abingdon, UK, 2018. [Google Scholar]
- Bowlby, J. The Making & Breaking of Affectional Bonds; Tavistock: London, UK, 1979. [Google Scholar]
- Gürol, A.; Polat, S. The Effects of Baby Massage on Attachment between Mother and Their Infants. Asian Nurs. Res. 2012, 6, 35–41. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Holditch-Davis, D.; White-Traut, R.C.; Levy, J.A.; O’Shea, T.M.; Geraldo, V.; David, R.J. Maternally Administered Interventions for Preterm Infants in the Nicu: Effects on Maternal Psychological Distress and Mother–Infant Relationship. Infant Behav. Dev. 2014, 37, 695–710. [Google Scholar] [CrossRef] [Green Version]
- Rubertsson, C.; WaldenstrÖm, U.; Wickberg, B.; Rådestad, I.; Hildingsson, I. Depressive Mood in Early Pregnancy and Postpartum: Prevalence and Women at Risk in a National Swedish Sample. J. Reprod. Infant Psychol. 2005, 23, 155–166. [Google Scholar] [CrossRef]
- Massoudi, P.; Hwang, C.P.; Wickberg, B. Fathers’ Depressive Symptoms in the Postnatal Period: Prevalence and Correlates in a Population-Based Swedish Study. Scand. J. Public Health 2016, 44, 688–694. [Google Scholar] [CrossRef]
- Skoog, M. Screening Immigrant Mothers for Postpartum Depression. Development and Feasibility of an Educational Intervention for Nurses in the Child Health Services; Lund University: Lund, Sweden, 2022. [Google Scholar]
- Garmy, P. Aktuellt Kunskapsläge Om Spädbarnsmassage—Systematisk Litteraturöversikt 2006–2011. Vård I Nord. 2012, 32, 29–33. [Google Scholar] [CrossRef] [Green Version]
- Galanakis, M.; Ntaouti, E.; Tsitsanis, G.; Chrousos, G.P. The Effects of Infant Massage on Maternal Distress: A Systematic Review. Psychology 2015, 6, 2091. [Google Scholar] [CrossRef] [Green Version]
- Cheng, C.D.; Volk, A.A.; Marini, Z.A. Supporting Fathering through Infant Massage. J. Perinat. Educ. 2011, 20, 200–209. [Google Scholar] [CrossRef] [Green Version]
- Matthiesen, A.-S.; Ransjö-Arvidson, A.B.; Nissen, E.; Uvnäs-Moberg, K. Postpartum Maternal Oxytocin Release by Newborns: Effects of Infant Hand Massage and Sucking. Birth 2001, 28, 13–19. [Google Scholar] [CrossRef]
- Fitri, S.Y.R.; Nasution, S.K.; Nurhidayah, I.; Maryam, N.N.A. Massage Therapy as a Non-Pharmacological Analgesia for Procedural Pain in Neonates: A Scoping Review. Complement. Ther. Med. 2021, 59, 102735. [Google Scholar] [CrossRef]
- Lei, M.; Liu, T.; Li, Y.; Liu, Y.; Meng, L.; Jin, C. Effects of Massage on Newborn Infants with Jaundice: A Meta-Analysis. Int. J. Nurs. Sci. 2018, 5, 89–97. [Google Scholar] [CrossRef]
- Niemi, A.K. Review of Randomized Controlled Trials of Massage in Preterm Infants. Children 2017, 4, 21. [Google Scholar] [CrossRef] [Green Version]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E. The Prisma 2020 Statement: An Updated Guideline for Reporting Systematic Reviews. Int. J. Surg. 2021, 88, 105906. [Google Scholar] [CrossRef]
- Polit, D.F.; Beck, C.T. Nursing Research: Generating and Assessing Evidence for Nursing Practice; Wolters Kluwer: Philadelphia, PA, USA, 2021. [Google Scholar]
- Rimpy, M.S. Effect of Massage Therapy on Physical and Physiological Wellbeing of Jaundiced Neonates Receiving Phototherapy: A Hospital Based Interventional Study. Amarjeet Kaur Sandhu 2018, 10, 57. [Google Scholar] [CrossRef]
- Chik, Y.-M.; Ip, W.Y.; Choi, K.C. The Effect of Upper Limb Massage on Infants’ Venipuncture Pain. Pain Manag. Nurs. 2017, 18, 50–57. [Google Scholar] [CrossRef]
- Harrison, T.M.; Brown, R.; Duffey, T.; Frey, C.; Bailey, J.; Nist, M.D.; Renner, L.; Fitch, J. Effects of Massage on Postoperative Pain in Infants with Complex Congenital Heart Disease. Nurs. Res. 2020, 69, S36–S46. [Google Scholar] [CrossRef]
- Özkan, T.K.; Küçükkelepçe, D.Ş.; Özkan, S.A. The Effects of Acupressure and Foot Massage on Pain During Heel Lancing in Neonates: A Randomized Controlled Trial. Complement. Ther. Med. 2019, 46, 103–108. [Google Scholar] [CrossRef]
- Nahidi, F.; Gazerani, N.; Yousefi, P.; Abadi, A.R. The Comparison of the Effects of Massaging and Rocking on Infantile Colic. Iran. J. Nurs. Midwifery Res. 2017, 22, 67. [Google Scholar] [CrossRef] [Green Version]
- Roshanray, A.; Rayyani, M.; Dehghan, M.; Faghih, A. Comparative Effect of Mother’s Hug and Massage on Neonatal Pain Behaviors Caused by Blood Sampling: A Randomized Clinical Trial. J. Trop. Pediatr. 2020, 66, 479–486. [Google Scholar] [CrossRef]
- Yavaş, S.; Bülbül, T.; Gavas, H.T. The Effect on Pain Level and Comfort of Foot Massages Given by Mothers to Newborns before Heel Lancing: Double-Blind Randomized Controlled Study. Jpn. J. Nurs. Sci. 2021, 18, e12421. [Google Scholar] [CrossRef] [PubMed]
- Zargham-Boroujeni, A.; Elsagh, A.; Mohammadizadeh, M. The Effects of Massage and Breastfeeding on Response to Venipuncture Pain among Hospitalized Neonates. Iran. J. Nurs. Midwifery Res. 2017, 22, 308. [Google Scholar] [PubMed]
- Eghbalian, F.; Rafienezhad, H.; Farmal, J. The Lowering of Bilirubin Levels in Patients with Neonatal Jaundice Using Massage Therapy: A Randomized, Double-Blind Clinical Trial. Infant Behav. Dev. 2017, 49, 31–36. [Google Scholar] [CrossRef] [PubMed]
- Gözen, D.; Yılmaz, Ö.E.; Dur, Ş.; Çağlayan, S.; Taştekin, A. Transcutaneous Bilirubin Levels of Newborn Infants Performed Abdominal Massage: A Randomized Controlled Trial. J. Spec. Pediatric Nurs. 2019, 24, e12237. [Google Scholar] [CrossRef]
- Jazayeri, Z.; Sajadi, M.; Dalvand, H.; Zolfaghari, M. Comparison of the Effect of Foot Reflexology and Body Massage on Physiological Indicators and Bilirubin Levels in Neonates under Phototherapy. Complement. Ther. Med. 2021, 59, 102684. [Google Scholar] [CrossRef]
- Korkmaz, G.; Esenay, F.I. Effects of Massage Therapy on Indirect Hyperbilirubinemia in Newborns Who Receive Phototherapy. J. Obstet. Gynecol. Neonatal Nurs. 2020, 49, 91–100. [Google Scholar] [CrossRef] [Green Version]
- Lori Kenari, R.; Aziznejadroshan, P.; Mojaveri, M.H.; Hajian-Tilaki, K. Comparing the Effect of Kangaroo Mother Care and Field Massage on Serum Bilirubin Level of Term Neonates with Hyperbilirubinemia under Phototherapy in the Neonatal Ward. Casp. J. Intern. Med. 2020, 11, 34. [Google Scholar]
- Liao, Y.-C.; Wan, Y.; Chen, P.; Hsieh, L. Efficacy of Medium-Chain Triglyceride Oil Massage on Growth in Preterm Infants: A Randomized Controlled Trial: A Consort-Compliant Article. Medicine 2021, 100, e26794. [Google Scholar] [CrossRef]
- Taheri, P.A.; Goudarzi, Z.; Shariat, M.; Nariman, S.; Matin, E.N. The Effect of a Short Course of Moderate Pressure Sunflower Oil Massage on the Weight Gain Velocity and Length of Nicu Stay in Preterm Infants. Infant Behav. Dev. 2018, 50, 22–27. [Google Scholar] [CrossRef]
- Zhang, X.; Wang, J. Massage Intervention for Preterm Infants by Their Mothers: A Randomized Controlled Trial. J. Spec. Pediatric Nurs. 2019, 24, e12238. [Google Scholar] [CrossRef]
- Jain, S.; Kumar, P.; McMillan, D.D. Prior Leg Massage Decreases Pain Responses to Heel Stick in Preterm Babies. J. Paediatr. Child Health 2006, 42, 505–508. [Google Scholar] [CrossRef]
- Pillai Riddell, R.R.; Racine, N.M.; Turcotte, K.; Uman, L.S.; Horton, R.E.; Osmun, L.D.; Kohut, S.A.; Stuart, J.H.; Stevens, B.; Gerwitz-Stern, A. Cochrane Review: Non-Pharmacological Management of Infant and Young Child Procedural Pain. Evid. -Based Child Health A Cochrane Rev. J. 2012, 7, 1905–2121. [Google Scholar] [CrossRef]
- Çetinkaya, B. Complementary and Alternative Therapies for Infantile Colic: A Systematic Review of the Literature. Altern. Ther. Health Med. 2021, 27, 42–47. [Google Scholar]
- Arikan, D.; Alp, H.; Gözüm, S.; Orbak, Z.; Cifçi, E.K. Effectiveness of Massage, Sucrose Solution, Herbal Tea or Hydrolysed Formula in the Treatment of Infantile Colic. J. Clin. Nurs. 2008, 17, 1754–1761. [Google Scholar]
- Bahrami, H.; Kiani, M.A.; Noras, M. Massage for Infantile Colic: Review and Literature. Int. J. Pediatr. 2016, 4, 1953–1958. [Google Scholar]
- Esfahani, M.S.; Sheykhi, S.; Abdeyazdan, Z.; Jodakee, M.; Boroumandfar, K. A Comparative Study on Vaccination Pain in the Methods of Massage Therapy and Mothers’ Breast Feeding During Injection of Infants Referring to Navabsafavi Health Care Center in Isfahan. Iran. J. Nurs. Midwifery Res. 2013, 18, 494. [Google Scholar]
- Reuter, A.; Silfverdal, S.A.; Lindblom, K.; Hjern, A. A Systematic Review of Prevention and Treatment of Infant Behavioural Sleep Problems. Acta Paediatr. 2020, 109, 1717–1732. [Google Scholar] [CrossRef]
- Abdellatif, M.; Vuong, N.L.; Tawfik, G.M.; Elfaituri, M.K.; Mansour, M.I.M.; Zaki, M.M.M.; Duong, P.D.T.; El-Qushayri, A.E.; Liang, Y.; Liu, K. Massage Therapy for the Treatment of Neonatal Jaundice: A Systematic Review and Network Meta-Analysis. J. Neonatal Nurs. 2020, 26, 17–24. [Google Scholar] [CrossRef]
- Diego, M.A.; Field, T.; Hernandez-Reif, M. Preterm Infant Weight Gain Is Increased by Massage Therapy and Exercise Via Different Underlying Mechanisms. Early Hum. Dev. 2014, 90, 137–140. [Google Scholar] [CrossRef] [Green Version]
- Field, T.; Diego, M.; Hernandez-Reif, M. Preterm Infant Massage Therapy Research: A Review. Infant Behav. Dev. 2010, 33, 115–124. [Google Scholar] [CrossRef] [Green Version]
- Garmy, P. Spädbarnsmassage—En Litteraturöversikt. Vård I Nord. 2007, 27, 30–34. [Google Scholar] [CrossRef] [Green Version]
| Outcome | Studies Published in 2017–2021 (n = 16) | Total Participants (n)/Participants with Stastistically Significant Results (n) |
|---|---|---|
| Pain relief | 7 | 717/422 |
| Jaundice | 6 | 455/455 |
| Weight gain | 4 | 244/244 |
| Total | 1416/1121 | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mrljak, R.; Arnsteg Danielsson, A.; Hedov, G.; Garmy, P. Effects of Infant Massage: A Systematic Review. Int. J. Environ. Res. Public Health 2022, 19, 6378. https://doi.org/10.3390/ijerph19116378
Mrljak R, Arnsteg Danielsson A, Hedov G, Garmy P. Effects of Infant Massage: A Systematic Review. International Journal of Environmental Research and Public Health. 2022; 19(11):6378. https://doi.org/10.3390/ijerph19116378
Chicago/Turabian StyleMrljak, Rebecca, Ann Arnsteg Danielsson, Gerth Hedov, and Pernilla Garmy. 2022. "Effects of Infant Massage: A Systematic Review" International Journal of Environmental Research and Public Health 19, no. 11: 6378. https://doi.org/10.3390/ijerph19116378
APA StyleMrljak, R., Arnsteg Danielsson, A., Hedov, G., & Garmy, P. (2022). Effects of Infant Massage: A Systematic Review. International Journal of Environmental Research and Public Health, 19(11), 6378. https://doi.org/10.3390/ijerph19116378







