Validation of the COVID-19 Digital Health Literacy Instrument in the Italian Language: A Cross-Sectional Study of Italian University Students
Abstract
:1. Introduction
1.1. Health Literacy and COVID-19
1.2. Digital Health Literacy Assessment
2. Materials and Methods
2.1. Method for Survey
2.2. Data Collection
2.3. Development of the Survey Form
2.4. COVID-19 Digital Health Literacy Instrument
2.5. Statistical Analysis
3. Results
3.1. Description of the Sample
3.2. COVID-19 DHLI in the Italian Language: Items Responses and Correlation Analysis
3.3. COVID-19 DHLI in the Italian Language: Reliability and Principal Component Analysis (PCA)
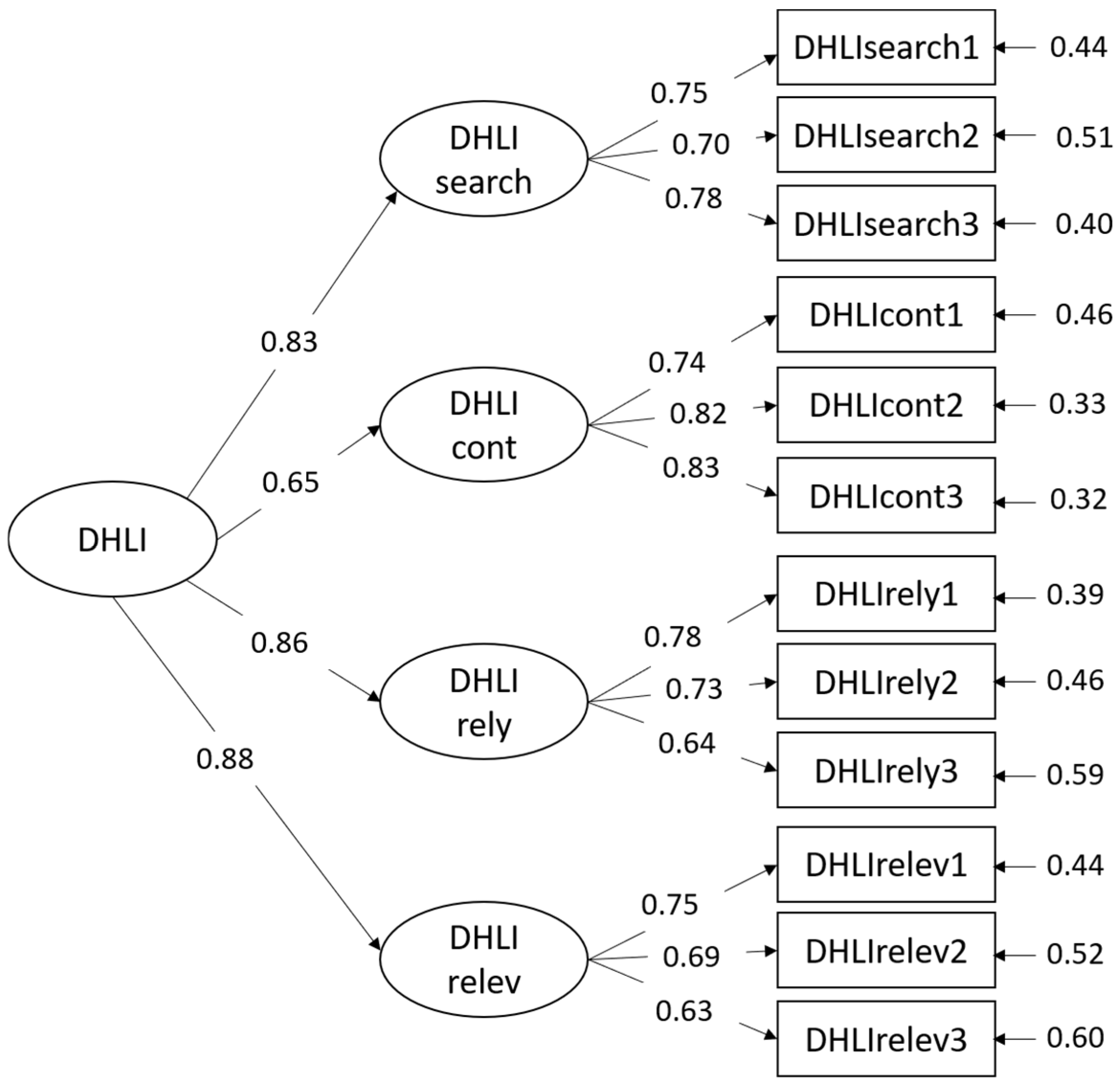
3.4. COVID-19 DHLI in the Italian Language: Confirmatory Factor Analysis (CFA)
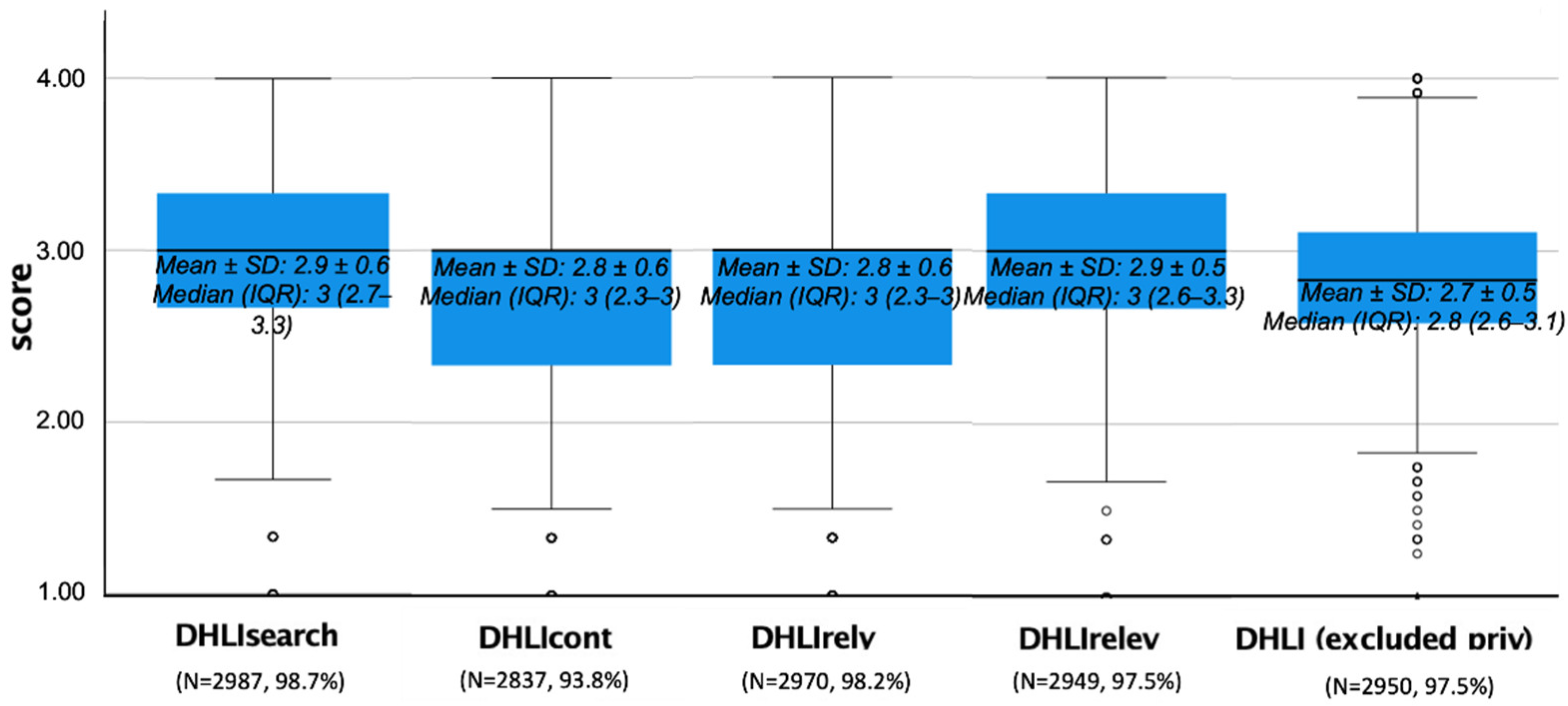
3.5. COVID-19 DHLI Subscales and Scale Scores
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Hua, J.; Shaw, R. Corona Virus (COVID-19) “Infodemic” and Emerging Issues through a Data Lens: The Case of China. Int. J. Environ. Res. Public Health 2020, 17, 2309. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zarocostas, J. How to fight an infodemic. Lancet 2020, 395, 676. [Google Scholar] [CrossRef]
- Okan, O.; Bollweg, T.M.; Berens, E.-M.; Hurrelmann, K.; Bauer, U.; Schaeffer, D. Coronavirus-Related Health Literacy: A Cross-Sectional Study in Adults during the COVID-19 Infodemic in Germany. Int. J. Environ. Res. Public Health 2020, 17, 5503. [Google Scholar] [CrossRef] [PubMed]
- Eysenbach, G. How to fight an infodemic: The four pillars of infodemic management. J. Med. Internet Res. 2020, 22, e21820. [Google Scholar] [CrossRef] [PubMed]
- Dadaczynski, K.; Okan, O.; Messer, M.; Leung, A.; Rosário, R.; Darlington, E.; Rathmann, K. Digital health literacy and online information seeking in times of COVID-19. A cross-sectional survey among university students in Germany. J. Med. Internet Res. 2021, 23, e24097. [Google Scholar] [CrossRef]
- Vrdelja, M.; Vrbovšek, S.; Klopčič, V.; Dadaczynski, K.; Okan, O. Facing the Growing COVID-19 Infodemic: Digital Health Literacy and Information-Seeking Behaviour of University Students in Slovenia. Int. J. Environ. Res. Public Health 2021, 18, 8507. [Google Scholar] [CrossRef]
- Chong, Y.Y.; Cheng, H.Y.; Chan, H.Y.L.; Chien, W.T.; Wong, S.Y.S. COVID-19 pandemic, infodemic and the role of eHealth literacy. Int. J. Nurs. Stud. 2020, 108, 103644. [Google Scholar] [CrossRef]
- Centers for Disease Control and Prevention. Coronavirus Diseae (COVID-19): Stigma and Resilence. Available online: https://www.cdc.gov/coronavirus/%0A2019-ncov/about/related-stigma.html (accessed on 13 October 2021).
- Hartley, K.; Vu, M.K. Fighting fake news in the COVID-19 era: Policy insights from an equilibrium model. Policy Sci. 2020, 53, 735–758. [Google Scholar] [CrossRef]
- Kummervold, P.E.; Wynn, R. Health information accessed on the Internet: The development in 5 European countries. Int. J. Telemed. Appl. 2012, 2012, 297416. [Google Scholar] [CrossRef] [Green Version]
- European Parliament. The Rise of Digital Health Technologies during the Pandemic; European Parliament: Strasbourg, France, 2021. [Google Scholar]
- European Commission. European Citizens’ Digital Health Literacy; European Union: Brussels, Belgium, 2014. [Google Scholar]
- Tangcharoensathien, V.; Calleja, N.; Nguyen, T.; Purnat, T.; D’Agostino, M.; Garcia-Saiso, S.; Landry, M.; Rashidian, A.; Hamilton, C.; AbdAllah, A.; et al. Framework for managing the COVID-19 infodemic: Methods and results of an online, crowdsourced who technical consultation. J. Med. Internet Res. 2020, 22, 1–8. [Google Scholar] [CrossRef]
- WHO. Health Promotion Glossary; World Health Organization: Geneva, Switzerland, 1998. [Google Scholar]
- CSDH (Commission on the Social Determinants of Health). Closing the Gap in a Generation: Health Equity through Action on the Social Determinants of Health; World Health Organization: Geneva, Switzerland, 2008. [Google Scholar]
- International Union for Health Promotion and Education. IUHPE Position Statement on Health Literacy: A Practical Vision for a Health Literate World. IUHPE Global Working Group on Health Literacy; IUHPE: Paris, France, 2018. [Google Scholar]
- McDaid, D. Investing in health literacy. Policy briefs and summaries. In World Health Organization, European Observatory on Health Systems and Policies; WHO Regional Office for Europe: Copenhagen, Denmark, 2016. [Google Scholar]
- Nutbeam, D. The evolving concept of health literacy. Soc. Sci. Med. 2008, 67, 2072–2078. [Google Scholar] [CrossRef] [PubMed]
- Nutbeam, D. Health literacy as a public health goal: A challenge for contemporary health education and communication strategies into the 21st century. Health Promot. Int. 2000, 15, 259–267. [Google Scholar] [CrossRef] [Green Version]
- WHO. Health Literacy. The Solid Facts; WHO Regional Office for Europe: Copenhagen, Denmark, 2013. [Google Scholar]
- WHO. Shanghai Declaration on Promoting Health in the 2030 Agenda for Sustainable Development. In Proceedings of the 9th Global Conference on Health Promotion, Shanghai, China, 21–24 November 2016. [Google Scholar]
- Castro-Sanchez, E.; Chang, P.W.S.; Vila-Candel, R.; Escobedo, A.; Holmes, A.H. Health literacy and infectious diseases: Why does it matter. Int. J. Infect. Dis. 2016, 43, 103–110. [Google Scholar] [CrossRef] [Green Version]
- Lorini, C.; Santomauro, F.; Donzellini, M.; Capecchi, L.; Bechini, A.; Boccalini, S.; Bonanni, P.; Bonaccorsi, G. Health literacy and vaccination: A systematic review. Hum. Vaccin. Immunother. 2018, 14, 478–488. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sentell, T.; Vamos, S.; Okan, O. Interdisciplinary perspectives on health literacy research around the world: More important than ever in a time of COVID-19. Int. J. Environ. Res. Public Health 2020, 17, 3010. [Google Scholar] [CrossRef] [PubMed]
- Paakkari, L.; Okan, O. COVID-19: Health literacy is an underestimated problem. Lancet Public Health 2020, 5, e249–e250. [Google Scholar] [CrossRef]
- Iskander, M. The COVID-19 Infodemic: A Reminder of the Importance of Health Literacy. Roundtable J. Health Policy 2021, 3, 23–28. [Google Scholar]
- Abel, T.; McQueen, D. Critical health literacy and the COVID-19 crisis. Health Promot. Int. 2020, 35, 1612–1613. [Google Scholar] [CrossRef]
- Van den Broucke, S. Why health promotion matters to the COVID-19 pandemic, and vice versa. Health Promot. Int. 2020, 35, 181–186. [Google Scholar] [CrossRef] [Green Version]
- WHO. Draft WHO European Roadmap for Implementation of Health Literacy Initiatives through the Life Course; WHO Regional Office for Europe: Copenhagen, Denmark, 2019. [Google Scholar]
- Norman, C. eHealth literacy 2.0: Problems and opportunities with an evolving concept. J. Med. Internet Res. 2011, 13, e125. [Google Scholar] [CrossRef]
- Levin-Zamir, D.; Lemish, D.; Gofin, R. Media Health Literacy (MHL): Development and measurement of the concept among adolescents. Health Educ. Res. 2011, 26, 323–335. [Google Scholar] [CrossRef] [PubMed]
- Norman, C.D.; Skinner, H.A. eHEALS: The eHealth Literacy Scale. J. Med. Internet Res. 2006, 8, e27. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hsu, W.; Chiang, C.; Yang, S. The effect of individual factors on health behaviors among college students: The mediating effects of eHealth literacy. J. Med. Internet Res. 2014, 16, e287. [Google Scholar] [CrossRef]
- Neter, E.; Brainin, E. eHealth literacy: Extending the digital divide to the realm of health information. J. Med. Internet Res. 2012, 14, e19. [Google Scholar] [CrossRef] [PubMed]
- Patil, U.; Kostareva, U.; Hadley, M.; Manganello, J.A.; Okan, O.; Dadaczynski, K.; Massey, P.M.; Agner, J.; Sentell, T. Health Literacy, Digital Health Literacy, and COVID-19 Pandemic Attitudes and Behaviours in U.S. College Students: Implications for Interventions. Int. J. Environ. Res. Public Health 2021, 18, 3301. [Google Scholar] [CrossRef]
- Van der Vaart, R.; Drossaert, C. Development of the Digital Health Literacy Instrument: Measuring a Broad Spectrum of Health 1.0 and Health 2.0 Skills. J. Med. Internet Res. 2017, 19, e27. [Google Scholar] [CrossRef] [Green Version]
- Chan, C.V.; Kaufman, D.R. A framework for characterizing eHealth literacy demands and barriers. J. Med. Internet Res. 2011, 13, e94. [Google Scholar] [CrossRef]
- Norgaard, O.; Furstrand, D.; Klokker, L.; Karnoe, A.; Batterham, R.; Kayser, L.; Osborne, R.H. The e-health literacy framework: A conceptual framework for characterizing e-health users and their interaction with e-health systems. Knowl. Manag. E-Learn. 2015, 7, 522–540. [Google Scholar] [CrossRef]
- Van Deursen, A.J.A.M.; van Dijk, J.A.G.M. Internet Skills Performance Tests: Are People Ready for eHealth? J. Med. Internet Res. 2011, 13, e35. [Google Scholar] [CrossRef]
- Van der Vaart, R.; van Deursen, A.J.A.M.; Drossaert, C.H.C.; Taal, E.; van Dijk, J.A.M.G.; van de Laar, M.A.F.J. Does the eHealth Literacy Scale (eHEALS) Measure What it Intends to Measure? Validation of a Dutch Version of the eHEALS in Two Adult Populations. J. Med. Internet Res. 2011, 13, e86. [Google Scholar] [CrossRef]
- Soellner, R.; Huber, S.; Reder, M. The Concept of eHealth Literacy and Its Measurement. J. Media Psychol. 2014, 26, 29–38. [Google Scholar] [CrossRef]
- Levin-Zamir, D.; Bertschi, I. Media health literacy, eHealth literacy and health behaviour across the lifespan: Current progress and future challenges. In International Handbook of Health Literacy. Research, Practice and Policy across the Lifespan; Okan, O., Bauer, U., Levin-Zamir, D., Pinheiro, P., Sørensen, K., Eds.; Policy Press: Bristol, UK, 2019; pp. 275–290. [Google Scholar]
- Quinn, S.; Bond, R.; Nugent, C. Quantifying health literacy and eHealth literacy using existing instruments and browser-based software for tracking online health information seeking behavior. Comput. Hum. Behav. 2017, 69, 256–267. [Google Scholar] [CrossRef]
- Dadaczynski, K.; Okan, O.; Messer, M.; Rathmann, K. University students’ sense of coherence, future worries and mental health: Findings from the German COVID-HL-survey. Health Promot. Int. 2022, 37, daab070. [Google Scholar] [CrossRef]
- Dodd, R.H.; Dadaczynski, K.; Okan, O.; McCaffery, K.J.; Pickles, K. Psychological wellbeing and academic experience of university students in australia during COVID-19. Int. J. Environ. Res. Public Health 2021, 18, 866. [Google Scholar] [CrossRef]
- OECD. Education at a Glance 2020; Education at a Glance; OECD: Paris, France, 2020; ISBN 9789264500785. [Google Scholar]
- Horgan, Á.; Sweeney, J. University Students’ Online Habits and Their Use of the Internet for Health Information. CIN Comput. Inform. Nurs. 2012, 30, 402–408. [Google Scholar] [CrossRef]
- Rennis, L.; McNamara, G.; Seidel, E.; Shneyderman, Y. Google It!: Urban Community College Students’ Use of the Internet to Obtain Self-Care and Personal Health Information. Coll. Stud. J. 2015, 49, 414–426. [Google Scholar]
- Heuberger, R.; Ivanitskaya, L. Preferred Sources of Nutrition Information: Contrasts Between Younger and Older Adults. J. Intergener. Relatsh. 2011, 9, 176–190. [Google Scholar] [CrossRef]
- Rosario, R.; Martins, M.R.O.; Augusto, C.; Silva, M.J.; Martins, S.; Duarte, A.; Fronteira, I.; Ramos, N.; Okan, O.; Dadaczynski, K. Associations between COVID-19-Related Digital Health Literacy and Online Information-Seeking Behavior among Portuguese University Students. Int. J. Environ. Res. Public Health 2020, 17, 8987. [Google Scholar] [CrossRef]
- Schäfer, S.K.; Sopp, M.R.; Schanz, C.G.; Staginnus, M.; Göritz, A.S.; Michael, T. Impact of COVID-19 on Public Mental Health and the Buffering Effect of a Sense of Coherence. Psychother. Psychosom. 2020, 89, 386–392. [Google Scholar] [CrossRef]
- Nguyen, L.H.T.; Vo, M.T.H.; Tran, L.T.M.; Dadaczynski, K.; Okan, O.; Murray, L.; Van Vo, T. Digital Health Literacy About COVID-19 as a Factor Mediating the Association Between the Importance of Online Information Search and Subjective Well-Being Among University Students in Vietnam. Front. Digit. Health 2021, 3, 1–10. [Google Scholar] [CrossRef]
- Credé, M.; Niehorster, S. Adjustment to College as Measured by the Student Adaptation to College Questionnaire: A Quantitative Review of its Structure and Relationships with Correlates and Consequences. Educ. Psychol. Rev. 2012, 24, 133–165. [Google Scholar] [CrossRef]
- Stellefson, M.; Hanik, B.; Chaney, B.; Chaney, D.; Tennant, B.; Chavarria, E.A. Ehealth literacy among college students: A systematic review with implications for ehealth education. J. Med. Internet Res. 2011, 13, e102. [Google Scholar] [CrossRef] [PubMed]
- Rababah, J.A.; Al-Hammouri, M.M.; Drew, B.L.; Aldalaykeh, M. Health literacy: Exploring disparities among college students. BMC Public Health 2019, 19, 1401. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Amoah, P.A.; Leung, A.Y.M.; Parial, L.L.; Poon, A.C.Y.; Tong, H.H.Y.; Ng, W.I.; Li, X.; Wong, E.M.L.; Kor, P.P.K.; Molassiotis, A. Digital Health Literacy and Health-Related Well-Being Amid the COVID-19 Pandemic: The Role of Socioeconomic Status Among University Students in Hong Kong and Macao. Asia-Pac. J. Public Health 2021, 33, 613–616. [Google Scholar] [CrossRef]
- Zakar, R.; Iqbal, S.; Zakar, M.Z.; Fischer, F. COVID-19 and health information seeking behavior: Digital health literacy survey amongst university students in Pakistan. Int. J. Environ. Res. Public Health 2021, 18, 4009. [Google Scholar] [CrossRef]
- Velasco, V.; Gragnano, A.; Gruppo Regionale HBSC Lombardia 2018; Vecchio, L.P. Health Literacy Levels among Italian Students: Monitoring and Promotion at School. Int. J. Environ. Res. Public Health 2021, 18, 9943. [Google Scholar] [CrossRef]
- Zanobini, P.; Lorini, C.; Lastrucci, V.; Minardi, V.; Possenti, V.; Masocco, M.; Garofalo, G.; Mereu, G.; Bonaccorsi, G. Health Literacy, Socio-Economic Determinants, and Healthy Behaviours: Results from a Large Representative Sample of Tuscany Region, Italy. Int. J. Environ. Res. Public Health 2021, 18, 12432. [Google Scholar] [CrossRef]
- Lastrucci, V.; Lorini, C.; Caini, S.; Florence Health Literacy Research Group; Bonaccorsi, G. Health literacy as a mediator of the relationship between socioeconomic status and health: A cross-sectional study in a population-based sample in Florence. PLoS ONE 2019, 14, e0227007. [Google Scholar] [CrossRef] [Green Version]
- Lorini, C.; Lastrucci, V.; Paolini, D.; Bonaccorsi, G.; Florence Health Literacy Research Group. Measuring health literacy combining performance-based and self-assessed measures: The roles of age, educational level and financial resources in predicting health literacy skills. A cross-sectional study conducted in Florence (Italy). BMJ Open 2020, 10, e035987. [Google Scholar] [CrossRef]
- Eurostat-Statistical Office of the European Communities. European Semester: Thematic Factsheet–Tertiary Education Attainment; Eurostat: Luxembourg, 2016. [Google Scholar]
- Dadaczynski, K.; Okan, O.; Rathmann, K. COVID-19 Health Literacy Survey in University Students (COVID-HL-Survey). In Questionnaire and Scale Documentation; Public Health Centre Fulda (PHZF) at the Fulda University of Applied Sciences & Interdisciplinary Centre for Health Literacy Research at Bielefeld University: Bielefeld, Germany, 2020. [Google Scholar]
- Martins, C.; Augusto, C.; Martins, M.R.O.; Silva, M.J.; Okan, O.; Dadaczynski, K.; Duarte, A.; Fronteira, I.; Ramos, N.; Rosário, R. Adaptation and validation of the Digital Health Literacy Instrument for Portuguese university students. Health Promot. J. Aust. 2022, 1–9. [Google Scholar] [CrossRef]
- COVID-HL Network. Available online: https://covid-hl.eu/research/survey/ (accessed on 25 November 2021).
- Calandri, E.; Graziano, F.; Begotti, T.; Cattelino, E.; Gattino, S.; Rollero, C.; Fedi, A. Adjustment to COVID-19 Lockdown Among Italian University Students: The Role of Concerns, Change in Peer and Family Relationships and in Learning Skills, Emotional, and Academic Self-Efficacy on Depressive Symptoms. Front. Psychol. 2021, 12, 643088. [Google Scholar] [CrossRef] [PubMed]
- Lastrucci, V.; Lorini, C.; Del Riccio, M.; Gori, E.; Chiesi, F.; Sartor, G.; Zanella, B.; Boccalini, S.; Bechini, A.; Puggelli, F.; et al. SARS-CoV-2 Seroprevalence Survey in People Involved in Different Essential Activities during the General Lock-Down Phase in the Province of Prato (Tuscany, Italy). Vaccines 2020, 8, 778. [Google Scholar] [CrossRef] [PubMed]
- Worldometers. Available online: https://www.worldometers.info/coronavirus/country/italy/ (accessed on 25 November 2021).
- Streiner, D.L.; Norman, G.R. Health Measurement Scales; Oxford University Press: Oxford, UK, 2008. [Google Scholar]
- Boateng, G.O.; Neilands, T.B.; Frongillo, E.A.; Melgar-Quiñonez, H.R.; Young, S.L. Best practices for developing and validating scales for health, social, and behavioral research: A primer. Front. Public Health 2018, 6, 149. [Google Scholar] [CrossRef] [PubMed]
- Hair, J.F.; Gabriel, M.L.D.S.; Silva, D.D.; Braga, S. Development and validation of attitudes measurement scales: Fundamental and practical aspects. RAUSP Manag. J. 2019, 54, 490–507. [Google Scholar] [CrossRef]
- Cronbach, L.J. Coefficient alpha and the internal structure of tests. Psychometrika 1951, 16, 297–334. [Google Scholar] [CrossRef] [Green Version]
- Streiner, D.L. Starting at the beginning: An introduction to coefficient alpha and internal consistency. J. Pers. Assess 2003, 80, 99–103. [Google Scholar] [CrossRef]
- Tabachnick, B.G.; Fidell, L.S. Using Multivariate Statistics, 5th ed.; Allyn & Bacon/Pearson Education: Boston, MA, USA, 2007. [Google Scholar]
- Bartlett, M.S. A note on the multiplying factors for various chi-squared Approximations. J. R. Stat. Soc. 1954, 16, 296–298. [Google Scholar]
- Hu, L.T.; Bentler, P.M. Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Struct. Equ. Model. 1999, 6, 1–55. [Google Scholar] [CrossRef]
- Meade, A.W.; Johnson, E.C.; Braddy, P.W. Power and sensitivity of alternative fit indices in tests of measurement invariance. J. Appl. Psychol. 2008, 93, 568–592. [Google Scholar] [CrossRef]
- Schweizer, K. Some guidelines concerning the modeling of traits and abilities in test construction. Eur. J. Psychol. Assess. 2010, 26, 1–2. [Google Scholar] [CrossRef]
- Schermelleh-Engel, K.; Moosbrugger, H.; Müller, H. Evaluating the fit of structural equation models: Tests of significance and descriptive goodness-of-fit measures. Methods Psychol. Res. Online 2003, 8, 23–74. [Google Scholar]
- Almaleh, R.; Helmy, Y.; Farhat, E.; Hasan, H.; Abdelhafez, A. Assessment of health literacy among outpatient clinics attendees at Ain Shams University Hospitals. Egypt: A cross-sectional study. Public Health 2017, 151, 137–145. [Google Scholar] [CrossRef] [PubMed]
- Halbach, S.M.; Ernstmann, N.; Kowalski, C.; Pfaff, H.; Pförtner, T.K.; Wesselmann, S.; Enders, A. Unmet information needs and limited health literacy in newly diagnosed breast cancer patients over the course of cancer treatment. Patient Educ. Couns. 2016, 99, 1511–1518. [Google Scholar] [CrossRef] [PubMed]
- Lorini, C.; Lastrucci, V.; Mantwill, S.; Vettori, V.; Bonaccorsi, G.; Florence Health Literacy Research Group. Measuring health literacy in Italy: A validation study of the HLS-EU-Q16 and of the HLS-EU-Q6 in Italian language, conducted in Florence and its surroundings. Ann. Dell’istituto Super. Sanita 2019, 55, 10–18. [Google Scholar] [CrossRef]
- Palumbo, R.; Annarumma, C.; Adinolfi, P.; Musella, M.; Piscopo, G. The Italian Health Literacy Project: Insights from the assessment of health literacy skills in Italy. Health Policy 2016, 120, 1087–1094. [Google Scholar] [CrossRef]
| Area (Subscales) | Items | Missing n (%) | Very Difficult n (%) | Difficult n (%) | Easy n (%) | Very Easy n (%) | Mean ± SD | Median (IQR) |
|---|---|---|---|---|---|---|---|---|
| DHLI—information searching (DHLIsearch) | DHLIsearch1 | 35 (1.2) | 81 (2.7) | 806 (26.6) | 1671 (55.2) | 432 (14.3) | 2.8 ± 0.7 | 3 (2–3) |
| DHLIsearch2 | 43 (1.4) | 25 (0.8) | 359 (11.9) | 1874 (62.0) | 724 (23.9) | 3.1 ± 0.6 | 3 (3–3) | |
| DHLIsearch3 | 40 (1.3) | 133 (4.4) | 938 (31.0) | 1470 (48.6) | 444 (14.7) | 2.7 ± 0.7 | 3 (2–3) | |
| DHLI—adding self-generated content (DHLIcont) | DHLIcont1 | 197 (6.5) | 62 (2.0) | 600 (19.8) | 1760 (58.2) | 406 (13.4) | 2.9 ± 0.6 | 3 (3–3) |
| DHLIcont2 | 188 (6.3) | 136 (4.5) | 762 (25.2) | 1481 (49.0) | 458 (15.1) | 2.8 ± 0.8 | 3 (2–3) | |
| DHLIcont3 | 192 (6.3) | 138 (4.6) | 856 (28.3) | 1472 (48.7) | 367 (12.1) | 2.7 ± 0.7 | 3 (2–3) | |
| DHLI—evaluating reliability (DHLIrel) | DHLIrely1 | 56 (1.9) | 220 (7.3) | 1145 (37.9) | 1280 (42.3) | 324 (10.7) | 2.6 ± 0.8 | 3 (2–3) |
| DHLIrely2 | 61 (2.0) | 158 (5.2) | 945 (31.2) | 1375 (45.5) | 486 (16.1) | 2.7 ± 0.8 | 3 (2–3) | |
| DHLIrely3 | 61 (2.0) | 43 (1.4) | 389 (12.9) | 1725 (57.0) | 807 (26.7) | 3.1 ± 0.6 | 3 (3–4) | |
| DHLI—determining relevance (DHLIrelev) | DHLIrelev1 | 78 (2.6) | 19 (0.6) | 438 (14.5) | 1994 (65.9) | 496 (16.4) | 3.0 ± 0.6 | 3 (3–3) |
| DHLIrelev2 | 87 (2.9) | 41 (1.4) | 681 (22.5) | 1801 (59.5) | 415 (13.7) | 2.9 ± 0.6 | 3 (3–3) | |
| DHLIrelev3 | 77 (2.5) | 73 (2.4) | 549 (18.1) | 1755 (58.0) | 571 (18.9) | 2.9 ± 0.7 | 3 (3–3) | |
| Area (Subscales) | Items | Missing n (%) | Often n (%) | Several Times n (%) | Once n (%) | Never n (%) | Mean ± SD | Median (IQR) |
| DHLI—protecting privacy (DHLIpriv) | DHLIpriv1 | 271 (9.0) | 181 (6.0) | 702 (23.2) | 651 (21.5) | 1220 (40.3) | 3.1 ± 1.0 | 3 (2–4) |
| DHLIpriv2 | 254 (8.4) | 112 (3.7) | 371 (12.3) | 483 (16) | 1805 (59.7) | 3.4 ± 0.9 | 4 (3–4) | |
| DHLIpriv3 | 257 (8.5) | 17 (0.6) | 93 (3.1) | 234 (7.7) | 2424 (80.1) | 3.8 ± 0.5 | 4 (4–4) |
| ITEMS | DHLI Search1 | DHLI Search2 | DHLI Search3 | DHLI Cont1 | DHLI Cont2 | DHLI Cont3 | DHLI Rely1 | DHLI Rely2 | DHLI Rely3 | DHLI Relev1 | DHLI Relev2 | DHLI Relev3 | DHLI Priv1 | DHLI Priv2 |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| DHLIsearch2 | 0.51 ° | |||||||||||||
| DHLIsearch3 | 0.56 ° | 0.56 ° | ||||||||||||
| DHLIcont1 | 0.33 ° | 0.39 ° | 0.36 ° | |||||||||||
| DHLIcont2 | 0.28 ° | 0.31 ° | 0.32 ° | 0. 58 ° | ||||||||||
| DHLIcont3 | 0.32 ° | 0.34 ° | 0.36 ° | 0.57 ° | 0.68 ° | |||||||||
| DHLIrely1 | 0.55 ° | 0.36 ° | 0.45 ° | 0.33 ° | 0. 29 ° | 0.32 ° | ||||||||
| DHLIrely2 | 0.37 ° | 0.30 ° | 0.35 ° | 0.29 ° | 0.26 ° | 0.27 ° | 0.58 ° | |||||||
| DHLIrely3 | 0.34 ° | 0.38 ° | 0.34 ° | 0.31 ° | 0.28 ° | 0.29 ° | 0.44 ° | 0.48 ° | ||||||
| DHLIrelev1 | 0.44 ° | 0.43 ° | 0.44 ° | 0.39 ° | 0.34 ° | 0.33 ° | 0.48 ° | 0.45 ° | 0.45 ° | |||||
| DHLIrelev2 | 0.33 ° | 0.33 ° | 0.36 ° | 0.35 ° | 0.33 ° | 0.33 ° | 0.34 ° | 0.31 ° | 0.37 ° | 0.49 ° | ||||
| DHLIrelev3 | 0.30 ° | 0.28 ° | 0.32 ° | 0.33 ° | 0.30 ° | 0.29 ° | 0.34 ° | 0.33 ° | 0.36 ° | 0.42 ° | 0.55 ° | |||
| DHLIpriv1 | 0.14 ° | 0.15 ° | 0.16 ° | 0.18 ° | 0.17 ° | 0.22 ° | 0.16 ° | 0.14 ° | 0.12 ° | 0.18 ° | 0.16 ° | 0.15 ° | ||
| DHLIpriv2 | 0.06 ° | 0.04 ° | 0.03 # | 0.03 # | −0.003 # | 0.04 # | 0.06 ° | 0.07 ° | 0.07 ° | 0.03 # | 0.08 ° | 0.04 ° | 0.14 ° | |
| DHLIpriv3 | 0.07 ° | 0.11 ° | 0.04 * | 0.042 * | 0.01 # | 0.01 # | 0.04 * | 0.09 ° | 0.11 ° | 0.08 ° | 0.10 ° | 0.06 ° | 0.14 ° | 0.42 ° |
| Items | For the Entire Scale | For the Entire Scale If Item Deleted | For the Entire Scale Excluding DHLIpriv | By Subscales |
|---|---|---|---|---|
| DHLIsearch1 | 0.847 | 0.835 | 0.881 | 0.783 |
| DHLIsearch2 | 0.837 | |||
| DHLIsearch3 | 0.834 | |||
| DHLIcont1 | 0.836 | 0.834 | ||
| DHLIcont2 | 0.838 | |||
| DHLIcont3 | 0.836 | |||
| DHLIrely1 | 0.832 | 0.758 | ||
| DHLIrely2 | 0.836 | |||
| DHLIrely3 | 0.837 | |||
| DHLIrelev1 | 0.834 | 0.739 | ||
| DHLIrelev2 | 0.837 | |||
| DHLIrelev3 | 0.840 | |||
| DHLIpriv1 | 0.857 | - | 0.392 | |
| DHLIpriv2 | 0.864 | |||
| DHLIpriv3 | 0.853 |
| ITEMS | MODEL 1 Components—by the Data (Based on Eighenvalues) * | MODEL 2 Components—by the Data Excluding DHLIpriv (Based on Eighenvalues) § | MODEL 3 Components—by Literature (5 Components) ° | MODEL 4 Components—by Literature Excluding DHLIpriv (4 Components) # | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 | 2 | 3 | 4 | 1 | 2 | 3 | 1 | 2 | 3 | 4 | 5 | 1 | 2 | 3 | 4 | |
| DHLIsearch1 | 0.796 | 0.166 | 0.147 | 0.034 | 0.792 | 0.181 | 0.152 | 0.797 | 0.166 | 0.149 | 0.03 | 0.052 | 0.127 | 0.739 | 0.352 | 0.103 |
| DHLIsearch2 | 0.717 | 0.098 | 0.267 | 0.07 | 0.716 | 0.1 | 0.274 | 0.731 | 0.115 | 0.29 | 0.104 | −0.091 | 0.204 | 0.788 | 0.114 | 0.164 |
| DHLIsearch3 | 0.747 | 0.159 | 0.25 | 0.01 | 0.744 | 0.165 | 0.255 | 0.754 | 0.166 | 0.261 | 0.022 | −0.009 | 0.198 | 0.778 | 0.202 | 0.184 |
| DHLIcont1 | 0.261 | 0.216 | 0.745 | 0.014 | 0.244 | 0.22 | 0.758 | 0.261 | 0.219 | 0.748 | 0.013 | 0.059 | 0.755 | 0.233 | 0.152 | 0.195 |
| DHLIcont2 | 0.163 | 0.202 | 0.831 | −0.029 | 0.146 | 0.196 | 0.845 | 0.158 | 0.2 | 0.826 | −0.042 | 0.105 | 0.860 | 0.113 | 0.15 | 0.149 |
| DHLIcont3 | 0.216 | 0.164 | 0.83 | 0.025 | 0.207 | 0.162 | 0.836 | 0.208 | 0.158 | 0.821 | 0.004 | 0.142 | 0.846 | 0.181 | 0.145 | 0.121 |
| DHLIrely1 | 0.638 | 0.433 | 0.103 | 0.025 | 0.635 | 0.443 | 0.09 | 0.611 | 0.403 | 0.066 | −0.052 | 0.341 | 0.157 | 0.363 | 0.734 | 0.116 |
| DHLIrely2 | 0.493 | 0.528 | 0.037 | 0.073 | 0.49 | 0.54 | 0.03 | 0.461 | 0.492 | −0.01 | −0.021 | 0.41 | 0.135 | 0.136 | 0.851 | 0.124 |
| DHLIrely3 | 0.41 | 0.56 | 0.088 | 0.088 | 0.391 | 0.575 | 0.1 | 0.397 | 0.546 | 0.07 | 0.048 | 0.201 | 0.156 | 0.159 | 0.652 | 0.295 |
| DHLIrelev1 | 0.431 | 0.572 | 0.236 | 0.042 | 0.427 | 0.577 | 0.23 | 0.425 | 0.565 | 0.227 | 0.019 | 0.136 | 0.222 | 0.341 | 0.441 | 0.459 |
| DHLIrelev2 | 0.12 | 0.74 | 0.26 | 0.088 | 0.11 | 0.743 | 0.265 | 0.134 | 0.756 | 0.279 | 0.118 | −0.07 | 0.192 | 0.193 | 0.156 | 0.816 |
| DHLIrelev3 | 0.082 | 0.779 | 0.196 | 0.005 | 0.065 | 0.773 | 0.209 | 0.091 | 0.788 | 0.207 | 0.022 | −0.031 | 0.149 | 0.116 | 0.202 | 0.810 |
| DHLIpriv1 | 0.078 | 0.089 | 0.329 | 0.343 | - | - | - | 0.007 | 0.011 | 0.226 | 0.148 | 0.836 | - | - | - | - |
| DHLIpriv2 | 0.025 | 0.006 | −0.018 | 0.821 | - | - | - | 0.032 | 0.013 | −0.012 | 0.828 | 0.075 | - | - | - | - |
| DHLIpriv3 | 0.034 | 0.079 | −0.018 | 0.821 | - | - | - | 0.044 | 0.09 | −0.007 | 0.835 | 0.047 | - | - | - | - |
| Explained variance | 35.9% | 9.9% | 8.7% | 6.8% | 43.8% | 11.2% | 8.6% | 35.9% | 9.9% | 8.7% | 6.8% | 5.9% | 43.8% | 11.2% | 8.6% | 7.2% |
| Fit Statistics | MODEL A (1 Factor) | MODEL B (4 Factors) | MODEL C (4 + 1 Factors) | |
|---|---|---|---|---|
| Chi2 | 3826.24 | 741.18 | 784.64 | |
| GDL | 54 | 48 | 50 | |
| Overall Model Fit | RMSEA (90% CI) | 0.159 (0.155–0.163) | 0.072 (0.068–0.077) | 0.073 (0.068–0.077) |
| SRMR | 0.08310 | 0.03981 | 0.04205 | |
| Model comparison | GFI | 0.8128 | 0.957 | 0.955 |
| CFI | 0.8865 | 0.977 | 0.976 | |
| NNFI | 0.8613 | 0.968 | 0.968 | |
| Model parsimony | PNFI | 0.7240 | 0.7093 | 0.7379 |
| PGFI | 0.5627 | 0.5891 | 0.6121 | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lorini, C.; Velasco, V.; Bonaccorsi, G.; Dadaczynski, K.; Okan, O.; Zanobini, P.; Vecchio, L.P. Validation of the COVID-19 Digital Health Literacy Instrument in the Italian Language: A Cross-Sectional Study of Italian University Students. Int. J. Environ. Res. Public Health 2022, 19, 6247. https://doi.org/10.3390/ijerph19106247
Lorini C, Velasco V, Bonaccorsi G, Dadaczynski K, Okan O, Zanobini P, Vecchio LP. Validation of the COVID-19 Digital Health Literacy Instrument in the Italian Language: A Cross-Sectional Study of Italian University Students. International Journal of Environmental Research and Public Health. 2022; 19(10):6247. https://doi.org/10.3390/ijerph19106247
Chicago/Turabian StyleLorini, Chiara, Veronica Velasco, Guglielmo Bonaccorsi, Kevin Dadaczynski, Orkan Okan, Patrizio Zanobini, and Luca P. Vecchio. 2022. "Validation of the COVID-19 Digital Health Literacy Instrument in the Italian Language: A Cross-Sectional Study of Italian University Students" International Journal of Environmental Research and Public Health 19, no. 10: 6247. https://doi.org/10.3390/ijerph19106247
APA StyleLorini, C., Velasco, V., Bonaccorsi, G., Dadaczynski, K., Okan, O., Zanobini, P., & Vecchio, L. P. (2022). Validation of the COVID-19 Digital Health Literacy Instrument in the Italian Language: A Cross-Sectional Study of Italian University Students. International Journal of Environmental Research and Public Health, 19(10), 6247. https://doi.org/10.3390/ijerph19106247










