A Narrative Review of Factors Historically Influencing Telehealth Use across Six Medical Specialties in the United States
Abstract
1. Introduction
1.1. Problem of Interest
1.2. Purpose, Scope, and Research Questions
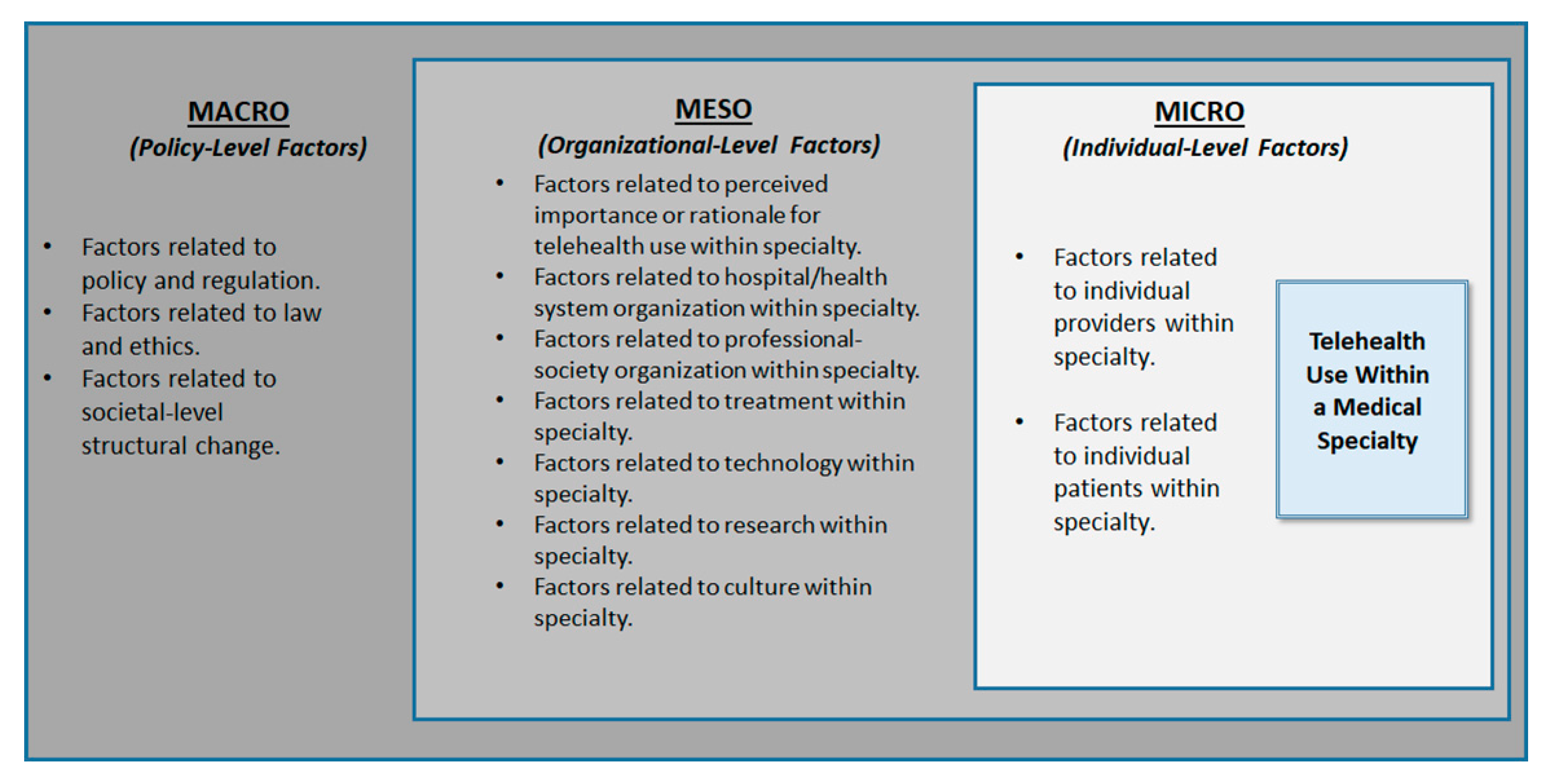
- What macro- (policy), meso- (organizational), and micro-level (individual) factors (barriers or facilitators) historically influenced telehealth use in six medical specialties, including three specialties identified as having lower telehealth use (allergy-immunology, family medicine, gastroenterology) and three identified as having higher telehealth use (psychiatry, cardiology, radiology) in the US?
- Which factors (barriers or facilitators) are associated with relatively lower use of telehealth services in some medical specialties and relatively higher use in other specialties in the US?
2. Existing Literature on Telehealth Use
3. Developing a Conceptual Framework
4. Narrative Review Methodology
4.1. Synthesis of Themes to Generate Insights
4.2. Expectation of Theme Saturation
4.3. Database Search
4.4. Eligibility Criteria
4.5. Processes Used to Explore and Synthesize Themes in the Data
5. Results
5.1. The “MACRO” Level
5.1.1. Factors Related to Policy and Regulation
5.1.2. Factors Related to Law and Ethics
5.1.3. Factors Related to Societal-Level Structural Change
5.2. The “MESO” Level
5.2.1. Factors Related to Perceived Importance or Rationale for Telehealth Use within the Specialty
5.2.2. Factors Related to Hospital and Health System Organization within the Specialty
5.2.3. Factors Related to Professional-Society Organization within the Specialty
5.2.4. Factors Related to Treatment within the Specialty
5.2.5. Factors Related to Technology within the Specialty
5.2.6. Factors Related to Research within the Specialty
5.2.7. Factors Related to Culture within the Specialty
5.3. The “MICRO” Level
5.3.1. Factors Related to Providers within the Specialty
5.3.2. Factors Related to Patients within the Specialty
6. Discussion
6.1. Summary of Findings
6.2. Implications for Widespread Sustainability of Telehealth Use
6.3. Limitations, Strengths, and Future Research Avenues
7. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Schwamm, L.H. Telehealth: Seven strategies to successfully implement disruptive technology and transform health care. Health Aff. 2014, 33, 200–206. [Google Scholar] [CrossRef]
- Taylor., P.R. An approach to designing viable and sustainable telehealth services. Stud. Health Technol. Inform. 2013, 188, 108–113. [Google Scholar]
- Kane, C.K.; Gillis, K. The Use of Telemedicine by Physicians: Still the Exception Rather Than the Rule. Health Aff. 2018, 37, 1923–1930. [Google Scholar] [CrossRef]
- Lin, C.C.; Dievler, A.; Robbins, C.; Sripipatana, A.; Quinn, M.; Nair, S. Telehealth in Health Centers: Key Adoption Factors, Barriers, And Opportunities. Health Aff. 2018, 37, 1967–1974. [Google Scholar] [CrossRef]
- E-Visit. 5 Healthcare Specialties Leading the Way in Telemedicine. Available online: https://blog.evisit.com/virtual-care-blog/top-specialties-for-telemedicine (accessed on 1 December 2020).
- Adler-Milstein, J.; Kvedar, J.; Bates, D.W. Telehealth among US hospitals: Several factors, including state reimbursement and licensure policies, influence adoption. Health Aff. 2014, 33, 207–215. [Google Scholar] [CrossRef] [PubMed]
- Kho, J.; Gillespie, N.; Martin-Khan, M. A systematic scoping review of change management practices used for telemedicine service implementations. BMC Health Serv. Res. 2020, 20, 815. [Google Scholar] [CrossRef] [PubMed]
- Hakim, A.; Gaviria-Agudelo, C.; Edwards, K.; Olson, D.; PIDS Telehealth Working Group. Pre-Coronavirus Disease 2019 Telehealth Practices Among Pediatric Infectious Diseases Specialists in the United States. J. Pediatr. Infect. Dis. Soc. 2020. [Google Scholar] [CrossRef]
- Persaud, Y.K.; Portnoy, J.M. Ten Rules for Implementation of a Telemedicine Program to Care for Patients with Asthma. J. Allergy Clin. Immunol. Pract. 2020, 9, 13–21. [Google Scholar] [CrossRef] [PubMed]
- Lee, T.; Kim, L. Telemedicine in Gastroenterology: A Value-Added Service for Patients. Clin. Gastroenterol. Hepatol. 2020, 18, 530–533. [Google Scholar] [CrossRef]
- Spivak, S.; Spivak, A.; Cullen, B.; Meuchel, J.; Johnston, D.; Chernow, R.; Green, C.; Mojtabai, R. Telepsychiatry Use in U.S. Mental Health Facilities, 2010–2017. Psychiatr. Serv. 2020, 71, 121–127. [Google Scholar] [CrossRef] [PubMed]
- Dubin, J.M.; Wyant, W.A.; Balaji, N.C.; Ong, W.L.; Kettache, R.H.; Haffaf, M.; Zouari, S.; Santillan, D.; Autrán Gómez, A.M.; Sadeghi-Nejad, H.; et al. Telemedicine Usage Among Urologists During the COVID-19 Pandemic: Cross-Sectional Study. J. Med. Internet Res. 2020, 22, e21875. [Google Scholar] [CrossRef]
- Gilman, M.; Stensland, J. Telehealth and Medicare: Payment policy, current use, and prospects for growth. Medicare Medicaid Res. Rev. 2013, 3. [Google Scholar] [CrossRef] [PubMed]
- Brown, N.A. State Medicaid and private payer reimbursement for telemedicine: An overview. J. Telemed. Telecare 2006, 12, 32–39. [Google Scholar] [CrossRef]
- Mended Hearts. Telemedicine’s Expanded Role in Cardiac Care. Available online: https://mendedhearts.org/story/telemedicines-expanding-role-in-cardiac-care (accessed on 2 September 2020).
- Mustafa, S.S.; Shaker, M.S.; Munblit, D.; Greenhawt, M. Paediatric allergy practice in the era of coronavirus disease 2019. Curr. Opin. Allergy Clin. Immunol. 2021, 21, 159–165. [Google Scholar] [CrossRef]
- Shachar, C.; Engel, J.; Elwyn, G. Implications for Telehealth in a Postpandemic Future. JAMA 2020, 323, 2375. [Google Scholar] [CrossRef] [PubMed]
- Institute for Healthcare Improvement. Recommendations for Designing High Quality Telehealth. Available online: http://www.ihi.org/communities/blogs/recommendations-for-designing-high-quality-telehealth (accessed on 15 August 2020).
- Costich, M.; Robbins-Milne, L.; Bracho-Sanchez, E.; Lane, M.; Friedman, S. Design and implementation of an interactive, competency-based pilot pediatric telemedicine curriculum. Med. Educ. Online 2021, 26, 1911019. [Google Scholar] [CrossRef] [PubMed]
- Hebert, M. Telehealth success: Evaluation framework development. Stud. Health Technol. Inform. 2001, 84, 11604908. [Google Scholar]
- Moehr, J.; Schaafsma, J.; Anglin, C.; Pantazi, S.; Grimm, N.; Anglin, S. Success factors for telehealth—A case study. Int. J. Med. Inform. 2006, 75, 755–763. [Google Scholar] [CrossRef]
- Dovigi, E.; Kwok, E.Y.L.; English, J.C. A Framework-Driven Systematic Review of the Barriers and Facilitators to Teledermatology Implementation. Curr. Dermatol. Rep. 2020, 9, 353–361. [Google Scholar] [CrossRef]
- Smith, T.; McNeil, K.; Mitchell, R.; Boyle, B.; Ries, N. A study of macro-, meso- and micro-barriers and enablers affecting extended scopes of practice: The case of rural nurse practitioners in Australia. BMC Nurs. 2019, 18, 1–12. [Google Scholar] [CrossRef]
- Yellowlees, P.M. Successfully developing a telemedicine system. J. Telemed. Telecare 2005, 11, 331–335. [Google Scholar] [CrossRef]
- Broens, T.H.; Vollenbroek-Hutten, M.M.; Hermens, H.J.; van Halteren, A.T.; Nieuwenhuis, L.J. Determinants of successful telemedicine implementations: A literature study. J. Telemed. Telecare 2007, 13, 303–309. [Google Scholar] [CrossRef]
- Almathami, H.K.Y.; Win, K.T.; Vlahu-Gjorgievska, E. Barriers and Facilitators That Influence Telemedicine-Based, Real-Time, Online Consultation at Patients’ Homes: Systematic Literature Review. J. Med. Internet Res. 2020, 22, e16407. [Google Scholar] [CrossRef]
- Koivunen, M.; Saranto, K. Nursing professionals’ experiences of the facilitators and barriers to the use of telehealth applications: A systematic review of qualitative studies. Scand. J. Caring Sci. 2017, 32, 24–44. [Google Scholar] [CrossRef]
- Foster, M.V.; Sethares, K.A. Facilitators and Barriers to the Adoption of Telehealth in Older Adults. CIN Comput. Inform. Nurs. 2014, 32, 523–533. [Google Scholar] [CrossRef] [PubMed]
- Van Dyk, L. A Review of Telehealth Service Implementation Frameworks. Int. J. Environ. Res. Public Health 2014, 11, 1279–1298. [Google Scholar] [CrossRef] [PubMed]
- Attewell, P. Technology diffusion and organizational learning: The case of business computing. Organ. Sci. 1992, 3, 1–19. [Google Scholar] [CrossRef]
- Khoja, S.; Scott, R.; Mohsin, M.; Ishaq, A.F.M.; Casebeer, A.L. Developing a conceptual-framework for e-health readiness assessment tools for developing countries. ICT Develop. 2006, 8, 79–81. [Google Scholar]
- Khoja, S.; Scott, R.E.; Casebeer, A.L.; Mohsin, M.; Ishaq, A.; Gilani, S. e-Health Readiness Assessment Tools for Healthcare Institutions in Developing Countries. Telemed. e-Health 2007, 13, 425–432. [Google Scholar] [CrossRef] [PubMed]
- Cilliers, L.; Flowerday, S.V. Health information systems to improve health care: A telemedicine case study. SA J. Inf. Manag. 2013, 15, 5. [Google Scholar] [CrossRef]
- Alikarami, R.; Moghadam, R.A.; Javadi, S.R.S.; Vahdat, D. Evaluation of effecting factors on success of telemedicine systems (using models of TAM and UTAUT). Can. J. Netw. Inf. Secur. 2011, 2, 5–9. [Google Scholar]
- Finch, T.; Mair, F.; May, C. Teledermatology in the UK: Lessons in service innovation. Br. J. Dermatol. 2006, 156, 521–527. [Google Scholar] [CrossRef] [PubMed]
- Buchachi, F.; Pakenham-Walsh, N. Information technology of health in developing countries. Chest 2007, 132, 1624–1630. [Google Scholar] [CrossRef] [PubMed]
- Pelletier-Fleury, N.; Fargeon, V.; Lano’e, J.; Fardeau, M. Transaction costs economics as a conceptual framework for the analysis of barriers to the diffusion of telemedicine. Health Policy 1997, 106, 1–14. [Google Scholar] [CrossRef]
- Tanriverdi, H.; Iacono, C.S. Knowledge barriers to diffusion of telemedicine. In Proceedings of the International Conference of the Association for Information Systems, Helsinki, Finland, 14–16 August 1998; pp. 39–50. [Google Scholar]
- Khoja, S.; Durrani, H.; Scott, R.; Sajwani, A.; Piryani, U. Conceptual framework for development of comprehensive e-Health evaluation tool. Telemed. e-Health 2013, 19, 48–53. [Google Scholar] [CrossRef]
- Damschroder, L.J.; Aron, D.C.; Keith, R.E.; Kirsh, S.R.; Alexander, J.A.; Lowery, J.C. Fostering implementation of health services research findings into practice: A consolidated framework for advancing implementation science. Implement. Sci. 2009, 4, 1–15. [Google Scholar] [CrossRef]
- Christie, H.L.; Bartels, S.L.; Boots, L.M.; Tange, H.J.; Verhey, F.R.; de Vugt, M.E. A systematic review on the implementation of eHealth interventions for informal caregivers of people with dementia. Internet Interv. 2018, 13, 51–59. [Google Scholar] [CrossRef] [PubMed]
- Batsis, J.A.; McClure, A.C.; Weintraub, A.B.; Sette, D.; Rotenberg, S.; Stevens, C.J.; Gilbert-Diamond, D.; Kotz, D.F.; Bartels, S.J.; Cook, S.B.; et al. Barriers and facilitators in implementing a pilot, pragmatic, telemedicine-delivered healthy lifestyle program for obesity management in a rural, academic obesity clinic. Implement. Sci. Commun. 2020, 1, 1–9. [Google Scholar] [CrossRef]
- Warner, G.; Lawson, B.; Sampalli, T.; Burge, F.; Gibson, R.; Wood, S. Applying the consolidated framework for implementation research to identify barriers affecting implementation of an online frailty tool into primary health care: A qualitative study. BMC Health Serv. Res. 2018, 18, 395. [Google Scholar] [CrossRef]
- Xyrichis, A.; Iliopoulou, K.; Mackintosh, N.J.; Bench, S.; Terblanche, M.; Philippou, J.; Sandall, J. Healthcare stakeholders’ perceptions and experiences of factors affecting the implementation of critical care telemedicine (CCT): Qualitative evidence synthesis. Cochrane Database Syst. Rev. 2021, 2, CD012876. [Google Scholar] [CrossRef] [PubMed]
- Hadjistavropoulos, H.; Nugent, M.; Dirkse, D.; Pugh, N. Implementation of internet-delivered cognitive behavior therapy within community mental health clinics: A process evaluation using the consolidated framework for implementation research. BMC Psychiatry 2017, 17, 1–15. [Google Scholar] [CrossRef] [PubMed]
- Portnoy, J.M.; Pandya, A.; Waller, M.; Elliott, T. Telemedicine and emerging technologies for health care in allergy/immunology. J. Allergy Clin. Immunol. 2020, 145, 445–454. [Google Scholar] [CrossRef] [PubMed]
- Hare, N.; Bansal, P.; Bajowala, S.S.; Abramson, S.L.; Chervinskiy, S.; Corriel, R.; Hauswirth, D.W.; Kakumanu, S.; Mehta, R.; Rashid, Q.; et al. Work Group Report: COVID-19: Unmasking Telemedicine. J. Allergy Clin. Immunol. Pract. 2020, 8, 2461.e3–2473.e3. [Google Scholar] [CrossRef] [PubMed]
- Portnoy, J.M.; Waller, M.; De Lurgio, S.; Dinakar, C. Telemedicine is as effective as in-person visits for patients with asthma. Ann. Allergy Asthma Immunol. 2016, 117, 241–245. [Google Scholar] [CrossRef]
- Elliott, T.; Shih, J.; Dinakar, C.; Portnoy, J.; Fineman, S. American College of Allergy, Asthma & Immunology Position Paper on the Use of Telemedicine for Allergists. Ann. Allergy Asthma Immunol. 2017, 119, 512–517. [Google Scholar] [CrossRef]
- Chongmelaxme, B.; Lee, S.W.H.; Dhippayom, T.; Saokaew, S.; Chaiyakunapruk, N.; Dilokthornsakul, P. The Effects of Telemedicine on Asthma Control and Patients’ Quality of Life in Adults: A Systematic Review and Meta-analysis. J. Allergy Clin. Immunol. Pract. 2019, 7, 199.e11–216.e11. [Google Scholar] [CrossRef]
- Nguyen, M.; Waller, M.; Pandya, A.; Portnoy, J. A Review of Patient and Provider Satisfaction with Telemedicine. Curr. Allergy Asthma Rep. 2020, 20, 1–7. [Google Scholar] [CrossRef]
- Greiwe, J. Using Telemedicine in a Private Allergy Practice. J. Allergy Clin. Immunol. Pract. 2019, 7, 2560–2567. [Google Scholar] [CrossRef]
- Shih, J.; Portnoy, J. Tips for Seeing Patients via Telemedicine. Curr. Allergy Asthma Rep. 2018, 18, 50. [Google Scholar] [CrossRef]
- Click, B.; Regueiro, M. The Inflammatory Bowel Disease Medical Home: From Patients to Populations. Inflamm. Bowel Dis. 2019, 25, 1881–1885. [Google Scholar] [CrossRef]
- Beard, J.A.; Franco, D.L.; Click, B.H. The Burden of Cost in Inflammatory Bowel Disease: A Medical Economic Perspective and the Future of Value-Based Care. Curr. Gastroenterol. Rep. 2020, 22, 6. [Google Scholar] [CrossRef]
- Regueiro, M.; Click, B.; Holder, D.; Shrank, W.; McAnallen, S.; Szigethy, E. Constructing an Inflammatory Bowel Disease Patient–Centered Medical Home. Clin. Gastroenterol. Hepatol. 2017, 15, 1148.e4–1153.e4. [Google Scholar] [CrossRef]
- Huang, V.W. Distance management of inflammatory bowel disease: Systematic review and meta-analysis. World J. Gastroenterol. 2014, 20, 829–842. [Google Scholar] [CrossRef]
- Berg, E.A.; Picoraro, J.A.; Miller, S.D.; Srinath, A.; Franciosi, J.P.; Hayes, C.E.; Farrell, P.R.; Cole, C.R.; LeLeiko, N.S. COVID-19—A Guide to Rapid Implementation of Telehealth Services: A Playbook for the Pediatric Gastroenterologist. J. Pediatr. Gastroenterol. Nutr. 2020, 70, 734–740. [Google Scholar] [CrossRef]
- Huntzinger, M.; Bielefeldt, K. Expanding the Scope of Telemedicine in Gastroenterology. Fed. Pract. 2018, 35, 26–31. [Google Scholar]
- Allen, J.I.; Kaushal, N. New Models of Gastroenterology Practice. Clin. Gastroenterol. Hepatol. 2018, 16, 3–6. [Google Scholar] [CrossRef] [PubMed]
- Dobrusin, A.; Hawa, F.; Gladshteyn, M.; Corsello, P.; Harlen, K.; Walsh, C.X.; Alaparthi, L.; Weinstein, M.; Baig, N.; Sousa, A.; et al. Gastroenterologists and Patients Report High Satisfaction Rates with Telehealth Services During the Novel Coronavirus 2019 Pandemic. Clin. Gastroenterol. Hepatol. 2020, 18, 2393.e2–2397.e2. [Google Scholar] [CrossRef] [PubMed]
- George, L.A.; Cross, R.K. Remote Monitoring and Telemedicine in IBD: Are We There Yet? Curr. Gastroenterol. Rep. 2020, 22, 12. [Google Scholar] [CrossRef]
- Bilal, M.; Sawhney, M.S.; Feuerstein, J.D. Coronavirus disease-2019: Implications for the gastroenterologist. Curr. Opin. Gastroenterol. 2021, 37, 23–29. [Google Scholar] [CrossRef] [PubMed]
- Moore, M.A.; Coffman, M.; Jetty, A.; Klink, K.; Petterson, S.; Bazemore, A. Family Physicians Report Considerable Interest in, but Limited Use of, Telehealth Services. J. Am. Board Fam. Med. 2017, 30, 320–330. [Google Scholar] [CrossRef] [PubMed]
- Powell, R.E.; Henstenburg, J.M.; Cooper, G.; Hollander, J.E.; Rising, K.L. Patient Perceptions of Telehealth Primary Care Video Visits. Ann. Fam. Med. 2017, 15, 225–229. [Google Scholar] [CrossRef]
- Krist, A.H.; DeVoe, J.E.; Cheng, A.; Ehrlich, T.; Jones, S.M. Redesigning Primary Care to Address the COVID-19 Pandemic in the Midst of the Pandemic. Ann. Fam. Med. 2020, 18, 349–354. [Google Scholar] [CrossRef]
- Noel, K.; Messina, C.; Hou, W.; Schoenfeld, E.; Kelly, G. Tele-transitions of care (TTOC): A 12-month, randomized controlled trial evaluating the use of Telehealth to achieve triple aim objectives. BMC Fam. Pract. 2020, 21, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Phillips, R.L., Jr.; Bazemore, A.W.; DeVoe, J.E.; Weida, T.J.; Krist, A.H.; Dulin, M.F.; Biagioli, F.E. A Family Medicine Health Technology Strategy for Achieving the Triple Aim for US Health Care. Fam. Med. 2015, 47, 628–635. [Google Scholar]
- Martin, J.C.; Avant, R.F.; Bowman, M.A.; Bucholtz, J.R.; Dickinson, J.R.; Evans, K.L.; Green, L.A.; Henley, D.E.; Jones, W.A.; Matheny, S.C.; et al. Future of Family Medicine Project Leadership Committee. The Future of Family Medicine: A collaborative project of the family medicine community. Ann. Fam. Med. 2004, 2, S3–S32. [Google Scholar] [CrossRef] [PubMed]
- Rubin, R. COVID-19′s Crushing Effects on Medical Practices, Some of Which Might Not Survive. JAMA 2020, 324, 321. [Google Scholar] [CrossRef]
- Wakefield, B.J.; Koopman, R.J.; Keplinger, L.E.; Bomar, M.; Bernt, B.; Johanning, J.L.; Kruse, R.L.; Davis, J.W.; Wakefield, D.S.; Mehr, D.R. Effect of Home Telemonitoring on Glycemic and Blood Pressure Control in Primary Care Clinic Patients with Diabetes. Telemed. e-Health 2014, 20, 199–205. [Google Scholar] [CrossRef] [PubMed]
- Kuehn, B.M. Telemedicine Helps Cardiologists Extend Their Reach. Circulation 2016, 134, 1189–1191. [Google Scholar] [CrossRef]
- Hale, T.M.; Jethwani, K.; Kandola, M.S.; Saldana, F.; Kvedar, J.C.; Nandigam, H.; Roettl, J. A Remote Medication Monitoring System for Chronic Heart Failure Patients to Reduce Readmissions: A Two-Arm Randomized Pilot Study. J. Med. Internet Res. 2016, 18, e91. [Google Scholar] [CrossRef] [PubMed]
- Varma, N.; Marrouche, N.F.; Aguinaga, L.; Albert, C.M.; Arbelo, E.; Choi, J.-I.; Chung, M.K.; Conte, G.; Dagher, L.; Epstein, L.M.; et al. HRS/EHRA/APHRS/LAHRS/ACC/AHA Worldwide Practice Update for Telehealth and Arrhythmia Monitoring During and After a Pandemic. Circ. Arrhythmia Electrophysiol. 2020, 13, e009007. [Google Scholar] [CrossRef] [PubMed]
- Schwamm, L.H.; Chumbler, N.; Brown, E.; Fonarow, G.C.; Berube, D.; Nystrom, K.; Suter, R.; Zavala, M.; Polsky, D.; Radhakrishnan, K.; et al. Recommendations for the Implementation of Telehealth in Cardiovascular and Stroke Care: A Policy Statement from the American Heart Association. Circulation 2017, 135, e24–e44. [Google Scholar] [CrossRef] [PubMed]
- Riegel, B.; Moser, D.K.; Buck, H.G.; Dickson, V.V.; Dunbar, S.B.; Lee, C.S.; Lennie, T.A.; Lindenfeld, J.; Mitchell, J.E.; Treat-Jacobson, D.J.; et al. Self-Care for the Prevention and Management of Cardiovascular Disease and Stroke. J. Am. Hear. Assoc. 2017, 6, e006997. [Google Scholar] [CrossRef]
- Chowdhury, D.; Hope, K.D.; Arthur, L.C.; Weinberger, S.M.; Ronai, C.; Johnson, J.N.; Snyder, C.S. Telehealth for Pediatric Cardiology Practitioners in the Time of COVID-19. Pediatr. Cardiol. 2020, 41, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Dolan, J.; Mandras, S.; Mehta, J.P.; Navas, V.; Tarver, I.J.; Chakinala, M.M.; Rahaghi, F.F. Reducing rates of readmission and development of an outpatient management plan in pulmonary hypertension: Lessons from congestive heart failure management. Pulm. Circ. 2020, 10. [Google Scholar] [CrossRef] [PubMed]
- Schwamm, L.H.; Holloway, R.G.; Amarenco, P.; Audebert, H.J.; Bakas, T.; Chumbler, N.R.; Handschu, R.; Jauch, E.C.; Knight, W.A.; Levine, S.R.; et al. A Review of the Evidence for the Use of Telemedicine within Stroke Systems of Care. Stroke 2009, 40, 2616–2634. [Google Scholar] [CrossRef] [PubMed]
- MacKinnon, G.E.; Brittain, E.L. Mobile Health Technologies in Cardiopulmonary Disease. Chest 2020, 157, 654–664. [Google Scholar] [CrossRef]
- Blood, A.J.; Fischer, C.M.; Fera, L.E.; MacLean, T.E.; Smith, K.V.; Dunning, J.R.; Bosque-Hamilton, J.W.; Aronson, S.J.; Gaziano, T.A.; Macrae, C.A.; et al. Rationale and design of a navigator-driven remote optimization of guideline-directed medical therapy in patients with heart failure with reduced ejection fraction. Clin. Cardiol. 2019, 43, 4–13. [Google Scholar] [CrossRef]
- Mongelli, F.; Georgakopoulos, P.; Pato, M.T. Challenges and Opportunities to Meet the Mental Health Needs of Underserved and Disenfranchised Populations in the United States. Focus 2020, 18, 16–24. [Google Scholar] [CrossRef]
- Yellowlees, P.; Shore, J.; Roberts, L. Practice Guidelines for Videoconferencing-Based Telemental Health—October 2009. Telemed. e-Health 2010, 16, 1074–1089. [Google Scholar] [CrossRef]
- Shore, J.H.; Yellowlees, P.; Caudill, R.; Johnston, B.; Turvey, C.; Mishkind, M.; Krupinski, E.; Myers, K.; Shore, P.; Kaftarian, E.; et al. Best Practices in Videoconferencing-Based Telemental Health April 2018. Telemed. e-Health 2018, 24, 827–832. [Google Scholar] [CrossRef]
- Shulman, M.; John, M.; Kane, J.M. Home-Based Outpatient Telepsychiatry to Improve Adherence with Treatment Appointments: A Pilot Study. Psychiatr. Serv. 2017, 68, 743–746. [Google Scholar] [CrossRef] [PubMed]
- Yellowlees, P.; Parish, M.B.; González, Á.; Chan, S.; Hilty, N.; Iosif, A.M.; McCarron, R.; Odor, A.; Scher, L.; Sciolla, A.; et al. Asynchronous Telepsychiatry: A Component of Stepped Integrated Care. Telemed. e-Health 2018, 24, 375–378. [Google Scholar] [CrossRef] [PubMed]
- Yuen, E.K.; Gros, D.F.; Price, M.; Zeigler, S.; Tuerk, P.W.; Foa, E.B.; Acierno, R. Randomized Controlled Trial of Home-Based Telehealth Versus In-Person Prolonged Exposure for Combat-Related PTSD in Veterans: Preliminary Results. J. Clin. Psychol. 2015, 71, 500–512. [Google Scholar] [CrossRef] [PubMed]
- Hubley, S.; Lynch, S.B.; Schneck, C.; Thomas, M.; Shore, J. Review of key telepsychiatry outcomes. World J. Psychiatry 2016, 6, 269–282. [Google Scholar] [CrossRef]
- Antonacci, D.J.; Bloch, R.M.; Saeed, S.A.; Yildirim, Y.; Talley, J. Empirical evidence on the use and effectiveness of telepsychiatry via videoconferencing: Implications for forensic and correctional psychiatry. Behav. Sci. Law 2008, 26, 253–269. [Google Scholar] [CrossRef]
- Mahmoud, H.; Vogt, E. Telepsychiatry: An Innovative Approach to Addressing the Opioid Crisis. J. Behav. Health Serv. Res. 2018, 46, 680–685. [Google Scholar] [CrossRef]
- Ramtekkar, U.; Bridge, J.A.; Thomas, G.; Butter, E.; Reese, J.; Logan, E.; Lin, S.; Axelson, D. Pediatric Telebehavioral Health: A Transformational Shift in Care Delivery in the Era of COVID-19. JMIR Ment. Health 2020, 7, e20157. [Google Scholar] [CrossRef] [PubMed]
- Bashshur, R.L.; Krupinski, E.A.; Thrall, J.H.; Bashshur, N. The Empirical Foundations of Teleradiology and Related Applications: A Review of the Evidence. Telemed. e-Health 2016, 22, 868–898. [Google Scholar] [CrossRef]
- Krupinski, E.; McNeill, K.; Haber, K.; Ovitt, T. High-Volume Teleradiology Service: Focus on Radiologist Satisfaction. J. Digit. Imaging 2003, 16, 203–209. [Google Scholar] [CrossRef]
- Siegal, D.S.; Wessman, B.; Zadorozny, J.; Palazzolo, J.; Montana, A.; Rawson, J.V.; Norbash, A.; Brown, M.L. Operational Radiology Recovery in Academic Radiology Departments After the COVID-19 Pandemic: Moving Toward Normalcy. J. Am. Coll. Radiol. 2020, 17, 1101–1107. [Google Scholar] [CrossRef]
- Johnson, N.D. Teleradiology 2010: Technical and organizational issues. Pediatr. Radiol. 2010, 40, 1052–1055. [Google Scholar] [CrossRef]
- Pedrosa, I.; Browning, T.; Kwon, J.K.; Morriss, M.; Matsler, L.; Pinho, M.C.; Lamus, D.; Pillai, A.; Karow, S.P.; Garinn, J.; et al. Response to COVID-19: Minimizing Risks, Addressing Challenges and Maintaining Operations in a Complex Academic Radiology Department. J. Comput. Assist. Tomogr. 2020, 44, 479–484. [Google Scholar] [CrossRef] [PubMed]
- Hryhorczuk, A.L.; Hanneman, K.; Eisenberg, R.L.; Meyer, E.C.; Brown, S.D. Radiologic Professionalism in Modern Health Care. Radiographics 2015, 35, 1779–1788. [Google Scholar] [CrossRef] [PubMed]
- Itri, J.N. Patient-centered Radiology. Radiographics 2015, 35, 1835–1846. [Google Scholar] [CrossRef] [PubMed]
- American College of Cardiology. Telehealth in cardiology: The Future is Today. Available online: https://www.acc.org/membership/sections-and-councils/health-care-innovation-section/section-updates/2019/11/26/12/42/telehealth-in-cardiology-the-future-is-today (accessed on 10 September 2020).
- Weinstein, R.S.; Lopez, A.M.; Joseph, B.A.; Erps, K.A.; Holcomb, M.; Barker, G.P.; Krupinski, E.A. Telemedicine, Telehealth, and Mobile Health Applications That Work: Opportunities and Barriers. Am. J. Med. 2014, 127, 183–187. [Google Scholar] [CrossRef] [PubMed]
| Search Terms | Search Results |
|---|---|
| (Allergy) AND (telehealth OR telemedicine) AND (barrier OR facilitator) | 76 |
| (Gastroenterology) AND (telehealth OR telemedicine) AND (barrier OR facilitator) | 50 |
| (Family medicine) AND (telehealth OR telemedicine) AND (barrier OR facilitator) | 389 |
| (Cardiology) AND (telehealth OR telemedicine) AND (barrier OR facilitator) | 158 |
| (Psychiatry) AND (telehealth OR telemedicine) AND (barrier OR facilitator) | 593 |
| (Radiology) AND (telehealth OR telemedicine) AND (barrier OR facilitator) | 155 |
| Total number of records | 1421 |
| Factor | Key Themes | Insights into Barriers and Facilitators |
|---|---|---|
| The “MACRO” Level | ||
| Factors related to policy and regulation | All six medical specialties | |
| ‘National coverage and reimbursement restrictions for services offered by telemedicine.’ | Barrier | |
| ‘Variation in coverage and payment for telehealth services across states and private payers.’ | Barrier | |
| Factors related to law and ethics | All six medical specialties | |
| ‘State-to-state variation in policies and protocols related to provider licensure and credentialing.’ | Barrier | |
| ‘Concerns associated with privacy and security of data.’ | Barrier | |
| ‘Liability issues associated with cyber malpractice.’ | Barrier | |
| Factors related to societal-level structural change | All six medical specialties | |
| ‘Rapidly escalating costs of healthcare.’ | Barrier or Facilitator | |
| ‘Projected shortages in workforce.’ | Barrier or Facilitator | |
| ‘Demographic changes at the population level.’ | Barrier or Facilitator | |
| ‘Increasing preference for telehealth services among patient groups.’ | Barrier or Facilitator | |
| ‘Advancing technology.’ | Barrier or Facilitator | |
| ‘Growing use of wearable devices among patients.’ | Barrier or Facilitator | |
| ‘Fluctuating professional demands (e.g., need for subspecialty expertise).’ | Barrier or Facilitator | |
| The “MESO” Level | ||
| Factors related to perceived importance or rationale for telehealth use within the specialty | Specialties with lower telehealth use | |
| ‘Historical rationale of increasing access to care,’ conveying limited perceived importance of telehealth use within the specialty. | Barrier | |
| Specialties with higher telehealth use | ||
| ‘Historical rationale of improving patient outcomes, experience, and overall quality of care.’ | Facilitator | |
| ‘Historical rationale of reducing costs and/or increasing revenues’ (e.g., by decreasing inefficiencies or hospitalizations and/or by attracting patients).’ | Facilitator | |
| ‘Historical rationale of promoting population health.’ | Facilitator | |
| Factors related to hospital/health system organization within the specialty | Specialties with lower telehealth use | |
| ‘Hospitals or health systems have historically provided limited (low) support for telehealth use within the specialty.’ | Barrier | |
| Specialties with higher telehealth use | ||
| ‘Hospitals or health systems have historically provided high support for telehealth use within the specialty (to align with the Triple Aim framework).’ | Facilitator | |
| Factors related to professional-society organization within the specialty | Specialties with lower telehealth use | |
| ‘Specialty-society organization has historically provided low, reactive support for telehealth use within the specialty.’ | Barrier | |
| Specialties with higher telehealth use | ||
| ‘Specialty-society organization has historically provided high, proactive support for telehealth use within the specialty.’ | Facilitator | |
| Specialty-society organization has historically been proactive in advancing telehealth use by influencing both macro-level factors (e.g., coverage or payment policies) and micro-level factors (e.g., provider culture and practices).’ | Facilitator | |
| Factors related to treatment within the specialty | Specialties with lower telehealth use | |
| ‘Care or treatment is based on traditional in-person encounters.’ | Barrier | |
| Specialties with higher telehealth use | ||
| ‘Care or treatment is designed to be holistic and patient-centered.’ | Facilitator | |
| Factors related to technology within the specialty | Specialties with lower telehealth use | |
| ‘Telemedicine technology is restricted to interactive real-time video.’ | Barrier | |
| Specialties with higher telehealth use | ||
| All three telemedicine technologies (modalities) are in use, ‘interactive real-time audio/video;’ ‘store-and-forward telemedicine;’ and ‘remote patient monitoring.’ | Facilitator | |
| Factors related to research within the specialty | Specialties with lower telehealth use | |
| ‘There is limited research on outcomes related to telehealth services within the specialty.’ | Barrier | |
| Specialties with higher telehealth use | ||
| ‘There is extensive research on outcomes related to telehealth services within the specialty.’ | Facilitator | |
| Factors related to culture within the specialty | Specialties with lower telehealth use | |
| ‘Provider culture is driven by reimbursement’ | Barrier | |
| ‘Providers are resistant to telehealth use due to lack of training.’ | Barrier | |
| ‘Providers tend to play the traditional role of gatekeeper.’ | Barrier | |
| ‘Providers are concerned about changing the physician-patient relationship.’ | Barrier | |
| Specialties with higher telehealth use | ||
| ‘Provider culture is driven by entrepreneurialism or risk and can be characterized as pioneering and patient-centric’ | Facilitator | |
| The “MICRO” Level | ||
| Factors related to providers within the specialty | Specialties with lower telehealth use | |
| ‘Telehealth practices of providers are provider-centric.’ | Barrier | |
| Specialties with higher telehealth use | ||
| ‘Telehealth practices of providers are patient-centric.’ | Facilitator | |
| Factors related to patients within the specialty | Specialties with lower telehealth use | |
| ‘Patients exhibit lower engagement in telehealth use.’ | Barrier | |
| Specialties with higher telehealth use | ||
| ‘Patients exhibit higher engagement in telehealth use.’ | Facilitator | |
| # | Lead Author and Year | Type of Article | Levels of Emphasis | Descriptive Summary |
|---|---|---|---|---|
| Allergy-immunology | ||||
| 1 | Portnoy et al., 2020 [46] | Review | Macro, Meso, Micro | Describes how the use of telemedicine, when combined with information technologies such as electronic health records, has the potential to cause a transformational change in the way care is delivered in allergy-immunology. |
| 2 | Hare et al., 2020 [47] | Specialty Workgroup Report | Macro, Meso, Micro | This work group report was developed to provide guidance to allergy-immunology clinicians as they navigate the swiftly evolving telemedicine landscape. |
| 3 | Portnoy et al., 2016 [48] | Clinical Trial | Meso, Micro | Children with asthma seen by telemedicine or in-person visits can achieve comparable degrees of asthma control. |
| 4 | Elliott et al., 2017 [49] | Position Statement | Macro, Meso, Micro | This article serves to offer policy and position statements of the use of telemedicine pertinent to the allergy and immunology subspecialty. |
| 5 | Chongmelaxme et al., 2019 [50] | Meta-Analysis | Meso, Micro | Combined telemedicine involving tele-case management or tele consultation are effective in improving asthma control and quality of life in adults. |
| 6 | Nguyen et al., 2020 [51] | Review | Micro | Providers tend to be satisfied with telemedicine if they have input into its development, there is administrative support, the technology is reliable and easy to use, as well as if there is adequate reimbursement. |
| 7 | Greiwe, 2019 [52] | Review | Micro | Telemedicine and telehealth technologies can be used to strengthen medical services and overcome many of the barriers that have previously existed by providing safe, accessible, cost-effective, and convenient healthcare at the touch of a button. |
| 8 | Shih and Portnoy, 2018 [53] | Review | Micro | Discusses the utilization of digital exam equipment, in vitro tests for diagnosis, and spirometry at the patient location; there are few clear advantages of seeing patients in-person over virtual visits. |
| Gastroenterology | ||||
| 9 | Click and Regueiro, 2019 [54] | Review | Macro, Meso, Micro | Explores the rationale behind initial construction of value-based IBD specialty medical homes. |
| 10 | Beard et al., 2020 [55] | Review | Macro, Meso, Micro | The future of value-based care in IBD is bright, with ample opportunities for growth. |
| 11 | Regueiro et al., 2017 [56] | Review | Meso, Micro | Describes how the IBD specialty medical home was constructed and implemented at the University of Pittsburgh Medical Center. |
| 12 | Huang et al., 2014 [57] | Meta-Analysis | Meso, Micro | This systematic review found that distance management of IBD significantly decreases clinic visit utilization. |
| 13 | Berg et al., 2020 [58] | Clinical Review | Macro, Meso, Micro | This pandemic article discusses best practice recommendations for introducing and expanding telehealth in pediatric gastroenterology. |
| 14 | Huntzinger and Bielefeldt, 2018 [59] | Program Review | Meso, Micro | This article discusses a specialty outreach program, which relied on telemedicine to reach patients with gastrointestinal and liver diseases in a large service area. |
| 15 | Allen and Kaushal, 2018 [60] | Clinical Review | Macro, Meso, Micro | Prior to 2000, a typical community GI practice comprised one to eight physicians. This article describes five new models of practice that have emerged in the past decade and have become viable choices for beginning and seasoned gastroenterologists alike. |
| 16 | Dobrusin et al., 2019 [61] | Original Research | Meso, Micro | Reports on the results of a survey of GI patients’ and physicians’ satisfaction with telehealth during the COVID-19 pandemic. |
| 17 | George and Cross, 2020 [62] | Review | Meso, Micro | The use of telehealth video conference and remote patient monitoring with web-based applications and text messaging in IBD care has been shown to ease financial burdens of chronic disease and lead to improved clinical outcomes. |
| 18 | Bilal et al., 2021 [63] | Review | Macro, Meso, Micro | Gastroenterologists need to rapidly adapt to the challenges being faced and need to make both system- and practice-based changes to the endoscopy unit and outpatient clinic practices. |
| Family medicine | ||||
| 19 | Moore et al., 2017 [64] | Original Research | Meso, Micro | This study found telehealth use was limited among family physicians. Lack of training and lack of reimbursement were found to be key barriers to telehealth use. |
| 20 | Powell et al., 2017 [65] | Original Research | Meso, Micro | Patients identified convenience, efficiency, communication, privacy, and comfort as domains that are potentially important to consider when assessing video visits vs. in-person encounters. |
| 21 | Krist et al., 2020 [66] | Clinical Review | Macro, Meso, Micro | Throughout the pandemic, primary care practices bore tremendous financial burden, even closing at a time when they were most needed. |
| 22 | Noel et al., 2020 [67] | Randomized Controlled Trial | Meso, Micro | Telehealth can improve transitions of care after hospital discharge by improving patient engagement and adherence to medications. |
| 23 | Phillips et al., 2015 [68] | Review | Macro, Meso, Micro | This article explores primary care health IT deployment to date, its shortcomings in support of the nation’s Triple Aim framework, and offers strategies and tactics that family medicine could pursue to improve the utility of health IT for primary care. |
| 24 | Martin et al., 2004 [69] | Original Research | Macro, Meso, Micro | System-wide changes will be needed to ensure high-quality healthcare for all Americans. |
| 25 | Rubin, 2020 [70] | Clinical Review | Macro, Meso | Discusses how the pandemic has accelerated the closure of many family practices. |
| 26 | Wakefield et al., 2016 [71] | Randomized Controlled Trial | Meso, Micro | Practices need to be selective in their use of telemonitoring with patients, limiting it to patients who have motivation for a significant change in care, such as starting insulin. |
| Cardiology | ||||
| 27 | Kuehn, 2016 [72] | Review | Macro, Meso, Micro | Increasingly, cardiologists across the country are leveraging technology to provide remote care. |
| 28 | Hale et al., 2016 [73] | Randomized Controlled Trial | Meso, Micro | Telehealth medication adherence technologies are a promising method to improve patient self-management. |
| 29 | Varma et al., 2020 [74] | Review | Meso, Micro | In light of the current pandemic, monitoring strategies should focus on selecting high-risk patients in need of close surveillance and using alternative remote recording devices to protect healthcare workers. |
| 30 | Schwamm et al., 2017 [75] | Position Statement | Meso, Micro | Identifies legal and regulatory barriers that impede telehealth adoption or delivery, proposes steps to overcome these barriers, and identifies areas for future research. |
| 31 | Riegel et al., 2017 [76] | Position Statement | Macro, Meso, Micro | Although there are many nuances to the relationships between self-care and outcomes, there is strong evidence that self-care is effective in achieving the goals of the treatment plan and cannot be ignored. |
| 32 | Chowdhury et al., 2020 [77] | Review | Meso, Micro | The use of adapted staffing and billing models and expanded means of remote monitoring will aid in the incorporation of telehealth into more widespread pediatric cardiology practice. |
| 33 | Dolan et al., 2020 [78] | Review | Meso, Micro | Multidisciplinary intervention resulted in decreased all-cause readmission and congestive heart failure readmission. |
| 34 | Schwamm et al., 2009 [79] | Review | Meso, Micro | Evidence-based recommendations included for various levels of care. |
| 35 | MacKinnon and Brittain, 2020 [80] | Review | Meso, Micro | MHealth is continuously developing as a result of technologic advancements and better understandings of mHealth utility. |
| 36 | Blood et al., 2020 [81] | Original Research | Meso, Micro | A navigator-led remote management strategy for optimization of guideline directed medical therapy may represent a scalable population-level strategy. |
| Psychiatry | ||||
| 37 | Mongelli et al., 2020 [82] | Original Research | Macro, Meso, Micro | Telepsychiatry and improvements in training of the mental health workforce are listed as useful implementations to overcome the treatment gap for patients seeking mental healthcare. |
| 38 | Yellowlees et al., 2010 [83] | Clinical Review | Meso, Micro | This article discusses guidelines ATA for the practices of tele mental health and applications for the practice of telemedicine in clinical psychiatry. |
| 39 | Shore et al., 2018 [84] | Specialty Workgroup Report | Meso, Micro | This article updates and consolidates guidance developed by The American Telemedicine Association (ATA) and The American Psychiatric Association (APA) on tele mental health services. |
| 40 | Shulman et al., 2017 [85] | Randomized Controlled Trial | Meso, Micro | A greater number of participants in the telepsychiatry group reported less subjective difficulty in keeping appointments. |
| 41 | Yellowlees et al., 2018 [86] | Randomized Controlled Trial | Meso, Micro | Describes a 5-year clinical trial comparing asynchronous telepsychiatry (ATP) with synchronous telepsychiatry (STP) consultations. |
| 42 | Yuen et al., 2015 [87] | Randomized Controlled Trial | Meso, Micro | Results suggest that prolonged exposure can be delivered via home-based telehealth with outcomes and satisfaction ratings comparable to in-person practices for certain symptoms. |
| 43 | Hubley et al., 2016 [88] | Systematic Review | Macro, Meso, Micro | A large evidence base supports telepsychiatry as a delivery method for mental health services. |
| 44 | Antonacci et al., 2008 [89] | Review | Macro, Meso, Micro | The review discusses implications for mental healthcare across settings and populations and comment on future directions and potential uses in forensic or correctional psychiatry. |
| 45 | Mahmoud and Vogt, 2019 [90] | Original Research | Macro, Meso | A comprehensive strategy to address opioid crisis, must incorporate the adoption of telepsychiatry to overcoming barriers to treatment and enhancing access to care. |
| 46 | Ramtekkar et al., 2020 [91] | Original Research | Meso, Micro | The pandemic forced a sudden shift from traditional in-person visits to alternative modalities. This paper identifies strategies and discuss considerations for long-term sustainability after the pandemic. |
| Radiology | ||||
| 47 | Bashshur et al., 2016 [92] | Systematic Review | Macro, Meso Micro | A consistent trend of concordance between the two modalities (teleradiology and conventional radiology) was observed in terms of diagnostic accuracy and reliability. |
| 48 | Krupinski et al., 2003 [93] | Original Research | Meso, Micro | Overall, radiologists are satisfied, although some improvements can be made. |
| 49 | Siegal et al., 2020 [94] | Position Statement | Meso, Micro | Radiology practices should be aware of the common approaches and preparations academic radiology departments have taken to reopening imaging in the post–COVID-19 disease world. |
| 50 | Johnson, 2010 [95] | Review | Macro, Meso Micro | This review aims to provide a background history to the current teleradiology services provided. It also addresses the limitations and issues involved in organizing such a service. |
| 51 | Pedrosa et al., 2020 [96] | Clinical Review | Meso, Micro | Describes the implementation of a response plan in an academic radiology department during COVID-19, challenges encountered, and tactics used to address these challenges. |
| 52 | Hryhorczuk et al., 2015 [97] | Review | Macro, Meso, Micro | Modern financial structures provide radiologists with both entrepreneurial opportunities as well as the temptation for unprofessional conduct. |
| 53 | Itri, 2015 [98] | Review | Macro, Meso, Micro | Radiologists must adapt to the changing landscape by focusing on their most important consumer: the patient. |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rangachari, P.; Mushiana, S.S.; Herbert, K. A Narrative Review of Factors Historically Influencing Telehealth Use across Six Medical Specialties in the United States. Int. J. Environ. Res. Public Health 2021, 18, 4995. https://doi.org/10.3390/ijerph18094995
Rangachari P, Mushiana SS, Herbert K. A Narrative Review of Factors Historically Influencing Telehealth Use across Six Medical Specialties in the United States. International Journal of Environmental Research and Public Health. 2021; 18(9):4995. https://doi.org/10.3390/ijerph18094995
Chicago/Turabian StyleRangachari, Pavani, Swapandeep S. Mushiana, and Krista Herbert. 2021. "A Narrative Review of Factors Historically Influencing Telehealth Use across Six Medical Specialties in the United States" International Journal of Environmental Research and Public Health 18, no. 9: 4995. https://doi.org/10.3390/ijerph18094995
APA StyleRangachari, P., Mushiana, S. S., & Herbert, K. (2021). A Narrative Review of Factors Historically Influencing Telehealth Use across Six Medical Specialties in the United States. International Journal of Environmental Research and Public Health, 18(9), 4995. https://doi.org/10.3390/ijerph18094995






