Sedentary Work and Physiological Markers of Health
Abstract
1. Introduction
2. Methods
2.1. Participants
2.2. Measures
2.2.1. Survey
2.2.2. Physical Health Assessment
2.2.3. Hemoglobin A1c
2.2.4. Accelerometry
2.2.5. Vascular Endothelial Function
2.3. Analyses
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Tremblay, M.S.; Aubert, S.; Barnes, J.D.; Saunders, T.J.; Carson, V.; Latimer-Cheung, A.E.; Chastin, S.F.M.; Altenburg, T.M.; Chinapaw, M.J.M.; Altenburg, T.M.; et al. Sedentary Behavior Research Network (SBRN)—Terminology Consensus Project process and outcome. Int. J. Behav. Nutr. Phys. Act. 2017, 14, 75. [Google Scholar] [CrossRef]
- Chau, J.Y.; Grunseit, A.; Midthjell, K.; Holmen, J.; Holmen, T.L.; Bauman, A.E.; Van der Ploeg, H.P. Sedentary behaviour and risk of mortality from all-causes and cardiometabolic diseases in adults: Evidence from the HUNT3 population cohort. Br. J. Sports Med. 2015, 49, 737–742. [Google Scholar] [CrossRef]
- de Rezende, L.F.M.; Rey-López, J.P.; Matsudo, V.K.R.; do Carmo Luiz, O. Sedentary behavior and health outcomes among older adults: A systematic review. BMC Public Health 2014, 14, 333. [Google Scholar] [CrossRef] [PubMed]
- Hamilton, M.T.; Hamilton, D.G.; Zderic, T.W. Role of low energy expenditure and sitting in obesity, metabolic syndrome, type 2 diabetes, and cardiovascular disease. Diabetes 2007, 56, 2655–2667. [Google Scholar] [CrossRef] [PubMed]
- Healy, G.N.; Matthews, C.E.; Dunstan, D.W.; Winkler, E.A.H.; Owen, N. Sedentary time and cardio-metabolic biomarkers in US adults: NHANES 2003–06. Eur. Heart J. 2011, 32, 590–597. [Google Scholar] [CrossRef] [PubMed]
- Held, C.; Iqbal, R.; Lear, S.A.; Rosengren, A.; Islam, S.; Mathew, J.; Yusuf, S. Physical activity levels, ownership of goods promoting sedentary behaviour and risk of myocardial infarction: Results of the INTERHEART study. Eur. Heart J. 2012, 33, 452–466. [Google Scholar] [CrossRef]
- Petersen, C.B.; Bauman, A.; Grønbæk, M.; Helge, J.W.; Thygesen, L.C.; Tolstrup, J.S. Total sitting time and risk of myocardial infarction, coronary heart disease and all-cause mortality in a prospective cohort of Danish adults. Int. J. Behav. Nutr. Phys. Act. 2014, 11, 13. [Google Scholar] [CrossRef]
- Proper, K.I.; Singh, A.S.; van Mechelen, W.; Chinapaw, M.J.M. Sedentary behaviors and health outcomes among adults: A systematic review of prospective studies. Am. J. Prev. Med. 2011, 40, 174–182. [Google Scholar] [CrossRef]
- van der Ploeg, H.P.; Chey, T.; Korda, R.J.; Banks, E.; Bauman, A. Sitting time and all-cause mortality risk in 222 497 Australian adults. Arch. Intern. Med. 2012, 172, 494–500. [Google Scholar] [CrossRef]
- Wilmot, E.G.; Edwardson, C.L.; Achana, F.A.; Davies, M.J.; Gorely, T.; Gray, L.J.; Khunti, K.; Yates, T.; Biddle, S.J.H. Sedentary time in adults and the association with diabetes, cardiovascular disease and death: Systematic review and meta-analysis. Diabetologia 2012, 55, 2895–2905. [Google Scholar] [CrossRef]
- Bankoski, A.; Harris, T.B.; McClain, J.J.; Brychta, R.J.; Caserotti, P.; Chen, K.Y.; Berrigan, D.; Troiano, R.P.; Koster, A. Sedentary activity associated with metabolic syndrome independent of physical activity. Diabetes Care 2011, 34, 497–503. [Google Scholar] [CrossRef]
- Diaz, K.M.; Howard, V.J.; Hutto, B.; Colabianchi, N.; Vena, J.E.; Blair, S.N.; Hooker, S.P. Patterns of Sedentary Behavior in US Middle-Age and Older Adults: The REGARDS Study. Med. Sci. Sports Exerc. 2016, 48, 430–438. [Google Scholar] [CrossRef]
- Miller, R.; Brown, W. Steps and sitting in a working population. Int. J. Behav. Med. 2004, 11, 219–224. [Google Scholar] [CrossRef]
- Owen, N.; Healy, G.N.; Dempsey, P.C.; Salmon, J.; Timperio, A.; Clark, B.K.; Goode, A.D.; Koorts, H.; Ridgers, N.D.; Hadgraft, N.T.; et al. Sedentary Behavior and Public Health: Integrating the Evidence and Identifying Potential Solutions. Annu. Rev. Public Health 2020, 41, 265–287. [Google Scholar] [CrossRef]
- Dunstan, D.W.; Kingwell, B.A.; Larsen, R.; Healy, G.N.; Cerin, E.; Hamilton, M.T.; Shaw, J.E.; Bertovic, D.A.; Zimmet, P.Z.; Salmon, J.; et al. Breaking Up Prolonged Sitting Reduces Postprandial Glucose and Insulin Responses. Diabetes Care 2012, 35, 976–983. [Google Scholar] [CrossRef]
- Peddie, M.C.; Bone, J.L.; Rehrer, N.J.; Skeaff, C.M.; Gray, A.R.; Perry, T.L. Breaking prolonged sitting reduces postprandial glycemia in healthy, normal-weight adults: A randomized crossover trial. Am. J. Clin. Nutr. 2013, 98, 358–366. [Google Scholar] [CrossRef] [PubMed]
- Thosar, S.S.; Bielko, S.L.; Mather, K.J.; Johnston, J.D.; Wallace, J.P. Effect of prolonged sitting and breaks in sitting time on endothelial function. Med. Sci. Sports Exerc. 2015, 47, 843–849. [Google Scholar] [CrossRef] [PubMed]
- Davignon, J.; Ganz, P. Role of endothelial dysfunction in atherosclerosis. Circulation 2004, 109, III27–III32. [Google Scholar] [CrossRef]
- Halcox, J.P.J.; Schenke, W.H.; Zalos, G.; Mincemoyer, R.; Prasad, A.; Waclawiw, M.A.; Nour, K.R.A.; Quyyumi, A.A. Prognostic value of coronary vascular endothelial dysfunction. Circulation 2002, 106, 653–658. [Google Scholar] [CrossRef]
- Schächinger, V.; Britten, M.B.; Zeiher, A.M. Prognostic Impact of Coronary Vasodilator Dysfunction on Adverse Long-Term Outcome of Coronary Heart Disease. Circulation 2000, 101, 1899–1906. [Google Scholar] [CrossRef] [PubMed]
- Alberts, B.; Johnson, A.; Lewis, J.; Raff, M.; Roberts, K.; Walter, P. Molecular biology of the cell. 4th edn. Ann. Bot. 2003, 91, 401. [Google Scholar] [CrossRef]
- Thijssen, D.H.J.; Black, M.A.; Pyke, K.E.; Padilla, J.; Atkinson, G.; Harris, R.A.; Parker, B.; Widlansky, M.E.; Tschakovsky, M.E.; Green, D.J. Assessment of flow-mediated dilation in humans: A methodological and physiological guideline. Am. J. Physiol. Heart Circ. Physiol. 2011, 300, H2–H12. [Google Scholar] [CrossRef] [PubMed]
- Nicolo, M.L.; Shewokis, P.A.; Boullata, J.; Sukumar, D.; Smith, S.; Compher, C.; Volpe, S.L. Sedentary behavior time as a predictor of hemoglobin A1c among adults, 40 to 59 years of age, living in the United States: National Health and Nutrition Examination Survey 2003 to 2004 and 2013 to 2014. Nutr. Health 2019, 25, 275–279. [Google Scholar] [CrossRef] [PubMed]
- Edelman, D.; Olsen, M.K.; Dudley, T.K.; Harris, A.C.; Oddone, E.Z. Utility of Hemoglobin A1c in Predicting Diabetes Risk. J. Gen. Intern. Med. 2004, 19, 1175–1180. [Google Scholar] [CrossRef] [PubMed]
- Adams, R.J.; Appleton, S.L.; Hill, C.L.; Wilson, D.H.; Taylor, A.W.; Chittleborough, C.R.; Gill, T.K.; Ruffin, R.E. Independent association of HbA(1c) and incident cardiovascular disease in people without diabetes. Obes. Silver Spring Md 2009, 17, 559–563. [Google Scholar] [CrossRef] [PubMed]
- Fuller, J.H.; Shipley, M.J.; Rose, G.; Jarrett, R.J.; Keen, H. Coronary-heart-disease risk and impaired glucose tolerance. The Whitehall study. Lancet Lond. Engl. 1980, 1, 1373–1376. [Google Scholar] [CrossRef]
- Kahn, S.E.; Hull, R.L.; Utzschneider, K.M. Mechanisms linking obesity to insulin resistance and type 2 diabetes. Nature 2006, 444, 840–846. [Google Scholar] [CrossRef]
- Kannel, W.B.; McGee, D.L. Diabetes and glucose tolerance as risk factors for cardiovascular disease: The Framingham study. Diabetes Care 1979, 2, 120–126. [Google Scholar] [CrossRef]
- Krogh-Madsen, R.; Thyfault, J.P.; Broholm, C.; Mortensen, O.H.; Olsen, R.H.; Mounier, R.; Plomgaard, P.; van Hall, G.; Booth, F.W.; Pedersen, B.K. A 2-wk reduction of ambulatory activity attenuates peripheral insulin sensitivity. J. Appl. Physiol. Bethesda Md 1985 2010, 108, 1034–1040. [Google Scholar] [CrossRef]
- Larsen, R.N.; Kingwell, B.A.; Robinson, C.; Hammond, L.; Cerin, E.; Shaw, J.E.; Healy, G.N.; Hamilton, M.T.; Owen, N.; Dunstan, D.W. Breaking up of prolonged sitting over three days sustains, but does not enhance, lowering of postprandial plasma glucose and insulin in overweight and obese adults. Clin. Sci. Lond. Engl. 1979 2015, 129, 117–127. [Google Scholar] [CrossRef]
- Restaino, R.M.; Walsh, L.K.; Morishima, T.; Vranish, J.R.; Martinez-Lemus, L.A.; Fadel, P.J.; Padilla, J. Endothelial dysfunction following prolonged sitting is mediated by a reduction in shear stress. Am. J. Physiol. Heart Circ. Physiol. 2016, 310, H648–H653. [Google Scholar] [CrossRef] [PubMed]
- Church, T.S.; Thomas, D.M.; Tudor-Locke, C.; Katzmarzyk, P.T.; Earnest, C.P.; Rodarte, R.Q.; Martin, C.K.; Blair, S.N.; Bouchard, C. Trends over 5 Decades in U.S. Occupation-Related Physical Activity and Their Associations with Obesity. PLoS ONE 2011, 6, e19657. [Google Scholar] [CrossRef]
- Bureau of Labor Statistics Data. Available online: https://data.bls.gov/timeseries/TUU10101AA01002867 (accessed on 30 July 2020).
- Mikus, C.R.; Oberlin, D.J.; Libla, J.L.; Taylor, A.M.; Booth, F.W.; Thyfault, J.P. Lowering physical activity impairs glycemic control in healthy volunteers. Med. Sci. Sports Exerc. 2012, 44, 225–231. [Google Scholar] [CrossRef] [PubMed]
- Pereira, M.A.; Mullane, S.L.; Toledo, M.J.L.; Larouche, M.L.; Rydell, S.A.; Vuong, B.; Feltes, L.H.; Mitchell, N.R.; de Brito, J.N.; Hasanaj, K.; et al. Efficacy of the ‘Stand and Move at Work’ multicomponent workplace intervention to reduce sedentary time and improve cardiometabolic risk: A group randomized clinical trial. Int. J. Behav. Nutr. Phys. Act. 2020, 17, 133. [Google Scholar] [CrossRef] [PubMed]
- Thorp, A.A.; Healy, G.N.; Winkler, E.; Clark, B.K.; Gardiner, P.A.; Owen, N.; Dunstan, D.W. Prolonged sedentary time and physical activity in workplace and non-work contexts: A cross-sectional study of office, customer service and call centre employees. Int. J. Behav. Nutr. Phys. Act. 2012, 9, 128. [Google Scholar] [CrossRef] [PubMed]
- Elliot, D.L.; Goldberg, L.; Kuehl, K.S.; Moe, E.L.; Breger, R.K.R.; Pickering, M.A. The PHLAME (Promoting Healthy Lifestyles: Alternative Models’ Effects) firefighter study: Outcomes of two models of behavior change. J. Occup. Environ. Med. 2007, 49, 204–213. [Google Scholar] [CrossRef] [PubMed]
- Chau, J.Y.; Van Der Ploeg, H.P.; Dunn, S.; Kurko, J.; Bauman, A.E. Validity of the occupational sitting and physical activity questionnaire. Med. Sci. Sports Exerc. 2012, 44, 118–125. [Google Scholar] [CrossRef]
- Zercher, A.; Schulman, L.; Boone, J. Quantitative Measurement of Hemoglobin A1c on the DCA Vantage Point-of-Care Analyzer as a Diagnostic Test for Diabetes: An Internal Validation Study. 2014. Available online: https://www.procarebv.nl/wp-content/uploads/2019/03/Precision-study.pdf (accessed on 20 March 2019).
- Troiano, R.P.; Berrigan, D.; Dodd, K.W.; Mâsse, L.C.; Tilert, T.; McDowell, M. Physical activity in the United States measured by accelerometer. Med. Sci. Sports Exerc. 2008, 40, 181–188. [Google Scholar] [CrossRef] [PubMed]
- Freedson, P.S.; Melanson, E.; Sirard, J. Calibration of the Computer Science and Applications, Inc. accelerometer. Med. Sci. Sports Exerc. 1998, 30, 777–781. [Google Scholar] [CrossRef]
- Nohria, A.; Gerhard-Herman, M.; Creager, M.A.; Hurley, S.; Mitra, D.; Ganz, P. Role of nitric oxide in the regulation of digital pulse volume amplitude in humans. J. Appl. Physiol. 2006, 101, 545–548. [Google Scholar] [CrossRef]
- Bonetti, P.O.; Pumper, G.M.; Higano, S.T.; Holmes, D.R.; Kuvin, J.T.; Lerman, A. Noninvasive identification of patients with early coronary atherosclerosis by assessment of digital reactive hyperemia. J. Am. Coll. Cardiol. 2004, 44, 2137–2141. [Google Scholar] [CrossRef]
- Kuvin, J.T.; Mammen, A.; Mooney, P.; Alsheikh-Ali, A.A.; Karas, R.H. Assessment of peripheral vascular endothelial function in the ambulatory setting. Vasc. Med. Lond. Engl. 2007, 12, 13–16. [Google Scholar] [CrossRef] [PubMed]
- Kuvin, J.T.; Patel, A.R.; Sliney, K.A.; Pandian, N.G.; Sheffy, J.; Schnall, R.P.; Karas, R.H.; Udelson, J.E. Assessment of peripheral vascular endothelial function with finger arterial pulse wave amplitude. Am. Heart J. 2003, 146, 168–174. [Google Scholar] [CrossRef]
- Faul, F.; Buchner, A.; Erdfelder, E.; Lang, A. G G*Power 3.1.9.4. 2019. Available online: https://www.psychologie.hhu.de/arbeitsgruppen/allgemeine-psychologie-und-arbeitspsychologie/gpower.html (accessed on 28 August 2020).
- Bergouignan, A.; Latouche, C.; Heywood, S.; Grace, M.S.; Reddy-Luthmoodoo, M.; Natoli, A.K.; Owen, N.; Dunstan, D.W.; Kingwell, B.A. Frequent interruptions of sedentary time modulates contraction- and insulin-stimulated glucose uptake pathways in muscle: Ancillary analysis from randomized clinical trials. Sci. Rep. 2016, 6, 32044. [Google Scholar] [CrossRef] [PubMed]
- Pekarski, S.E. A gravitational hypothesis of essential hypertension as a natural adaptation to increased gravitational stress caused by regular, prolonged sitting typical of modern life. Med. Sci. Monit. Int. Med. J. Exp. Clin. Res. 2004, 10, HY27–HY32. [Google Scholar]
- Charkoudian, N.; Rabbitts, J.A. Sympathetic neural mechanisms in human cardiovascular health and disease. Mayo Clin. Proc. 2009, 84, 822–830. [Google Scholar] [CrossRef]
| Worksite | ||||||
|---|---|---|---|---|---|---|
| Total N = 241 | 1 N = 55 | 2 N = 75 | 3 N = 68 | 4 N = 43 | p | |
| Sex(male) | 22.3% | 35.2% | 32.9% | 8.8% | 9.3% | <0.001 |
| Race (white) | 70.2% | 48.1% | 78.1% | 72.1% | 81.4% | 0.001 |
| Race | NA | |||||
| White | 64.7% | 43.6% | 70.7% | 69.1% | 74.4% | |
| Black | 9.5% | 20.0% | 1.3% | 14.7% | 2.3% | |
| Native American | 2.1% | 5.5% | 2.7% | 0.0% | 0.0% | |
| Asian | 1.7% | 1.8% | 0.0% | 2.9% | 2.3% | |
| Pacific Islanders | 2.5% | 1.8% | 2.7% | 0.0% | 7.0% | |
| Other | 14.1% | 21.8% | 16.0% | 10.3% | 7.0% | |
| Multi-Racial | 5.4% | 5.5% | 6.7% | 2.9% | 7.0% | |
| Hispanic | 19.7% | 24.1% | 28.8% | 10.3% | 14.0% | 0.028 |
| Education | 0.012 | |||||
| HS or Less | 31.5% | 22.2% | 45.2% | 23.5% | 32.6% | |
| Some College | 48.7% | 59.3% | 45.2% | 50.0% | 39.5% | |
| Bachelors or Higher | 19.7% | 18.5% | 9.6% | 26.5% | 27.9% | |
| Children | 43.5% | 41.5% | 54.8% | 36.8% | 37.2% | 0.121 |
| Caregiver for Adult | 18.5% | 16.7% | 24.7% | 11.8% | 20.9% | 0.243 |
| Smoke | 14.3% | 14.8% | 24.7% | 8.8% | 4.7% | 0.010 |
| Blood Pressure Medication | 16.4% | 20.4% | 12.3% | 11.8% | 25.6% | 0.157 |
| M(SD) | M(SD) | M(SD) | M(SD) | M(SD) | ||
| Age | 39.72 (11.64) | 40.34 (11.18) | 35.45 (9.98) a,b | 42.01 (11.63) a | 42.59 (13.10) b | 0.001 |
| Diastolic blood pressure | 81.43 (12.27) | 87.13 (13.02) e,f,g | 81.19 (12.22) e | 78.04 (10.50) f | 79.93 (11.85) g | <0.001 |
| Systolic blood pressure | 126.10 (18.35) | 133.35 (22.73) c,d | 123.39 (16.43) c | 123.31 (15.93) d | 125.98 (16.88) | 0.007 |
| Percent body fat | 38.90 (10.25) | 37.08 (10.69) h | 37.50 (10.83) i | 39.27 (10.20) | 43.01 (7.49) h,i | 0.019 |
| Hemoglobin A1c | 5.74 (1.20) | 6.01 (1.63) | 5.66 (1.21) | 5.54 (0.63) | 5.84 (1.15) | 0.144 |
| EndoScore | 2.03 (0.49) | 1.86 (0.41) | 2.17 (0.50) | 2.02 (0.50) | 2.07 (0.53) | 0.408 |
| Median (IQR) | Median (IQR) | Median (IQR) | Median (IQR) | Median (IQR) | ||
| Physical activity | 1.25 (2.06) | 1.50 (2.13) | 1.00 (1.75) | 1.25 (2.25) | 1.00 (2.50) | 0.442 |
| BMI | 32.10 (12.90) | 31.90 (11.40) | 31.70 (11.50) | 30.30 (12.35) | 34.60 (16.20) | 0.259 |
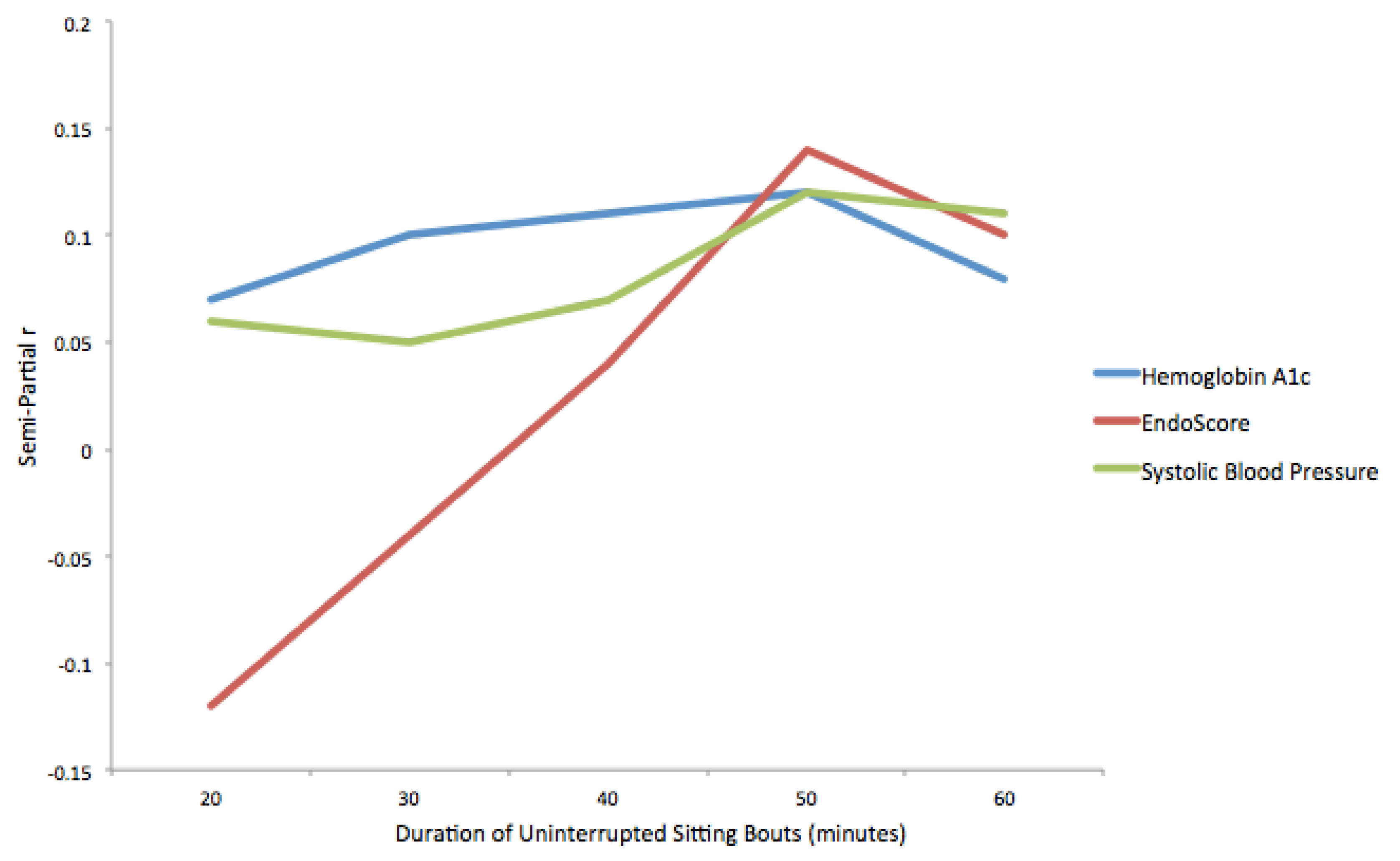
| Hemoglobin A1c | N | b | p | 95% CI | Semi-Partial r |
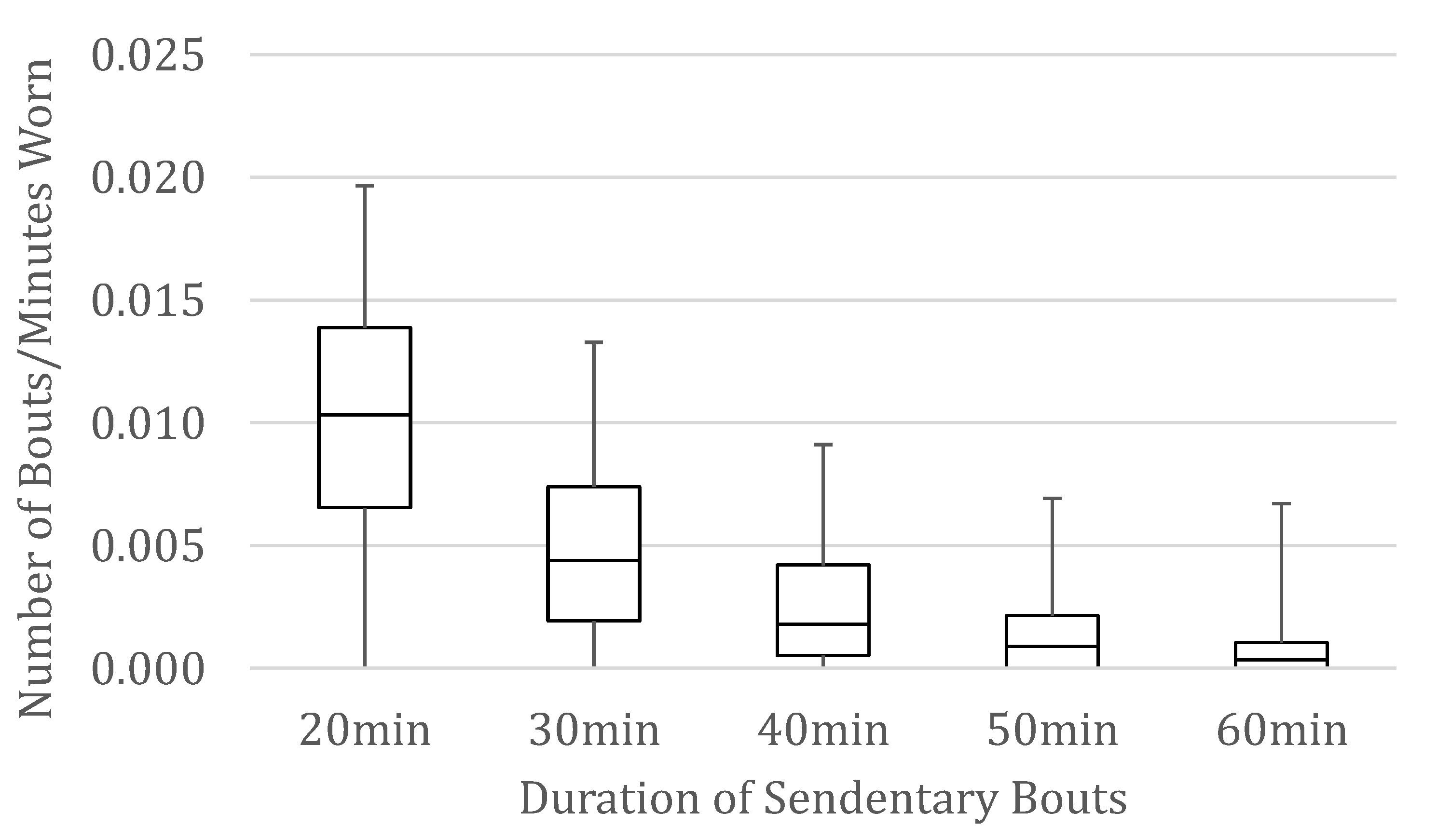
| Frequency of 20+ min bouts | 236 | 17.42 | 0.305 | −15.97–50.81 | 0.07 |
| Frequency of 30+ min bouts | 236 | 37.74 | 0.111 | −8.72–84.21 | 0.10 |
| Frequency of 40+ min bouts | 236 | 52.09 | 0.106 | −11.22–115.40 | 0.11 |
| Frequency of 50+ min bouts | 236 | 83.10 | 0.070 | −6.94–173.15 | 0.12 |
| Frequency of 60+ min bouts | 236 | 78.14 | 0.229 | −49.41–205.68 | 0.08 |
| EndoScore | N | b | p | 95% CI | Semi-Partial r |
| Frequency of 20+ min bouts | 56 | −12.00 | 0.393 | 15.96–−0.12 | −0.12 |
| Frequency of 30+ min bouts | 56 | −5.59 | 0.782 | −45.85–34.68 | −0.04 |
| Frequency of 40+ min bouts | 56 | 8.65 | 0.765 | −49.053–66.359 | 0.04 |
| Frequency of 50+ min bouts | 56 | 37.81 | 0.301 | −34.84–110.47 | 0.14 |
| Frequency of 60+ min bouts | 56 | 34.72 | 0.476 | −62.413–131.844 | 0.10 |
| Systolic Blood Pressure | N | B | p | 95% CI | Semi-Partial r |
| Frequency of 20+ min bouts | 237 | 220.45 | 0.388 | −281.71–722.61 | 0.06 |
| Frequency of 30+ min bouts | 237 | 299.22 | 0.401 | −400.92–999.36 | 0.05 |
| Frequency of 40+ min bouts | 237 | 562.95 | 0.245 | −388.90–1514.11 | 0.07 |
| Frequency of 50+ min bouts | 237 | 1266.54 | 0.066 | −84.30–2617.37 | 0.12 |
| Frequency of 60+ min bouts | 237 | 1628.13 | 0.093 | −273.54–3529.78 | 0.11 |
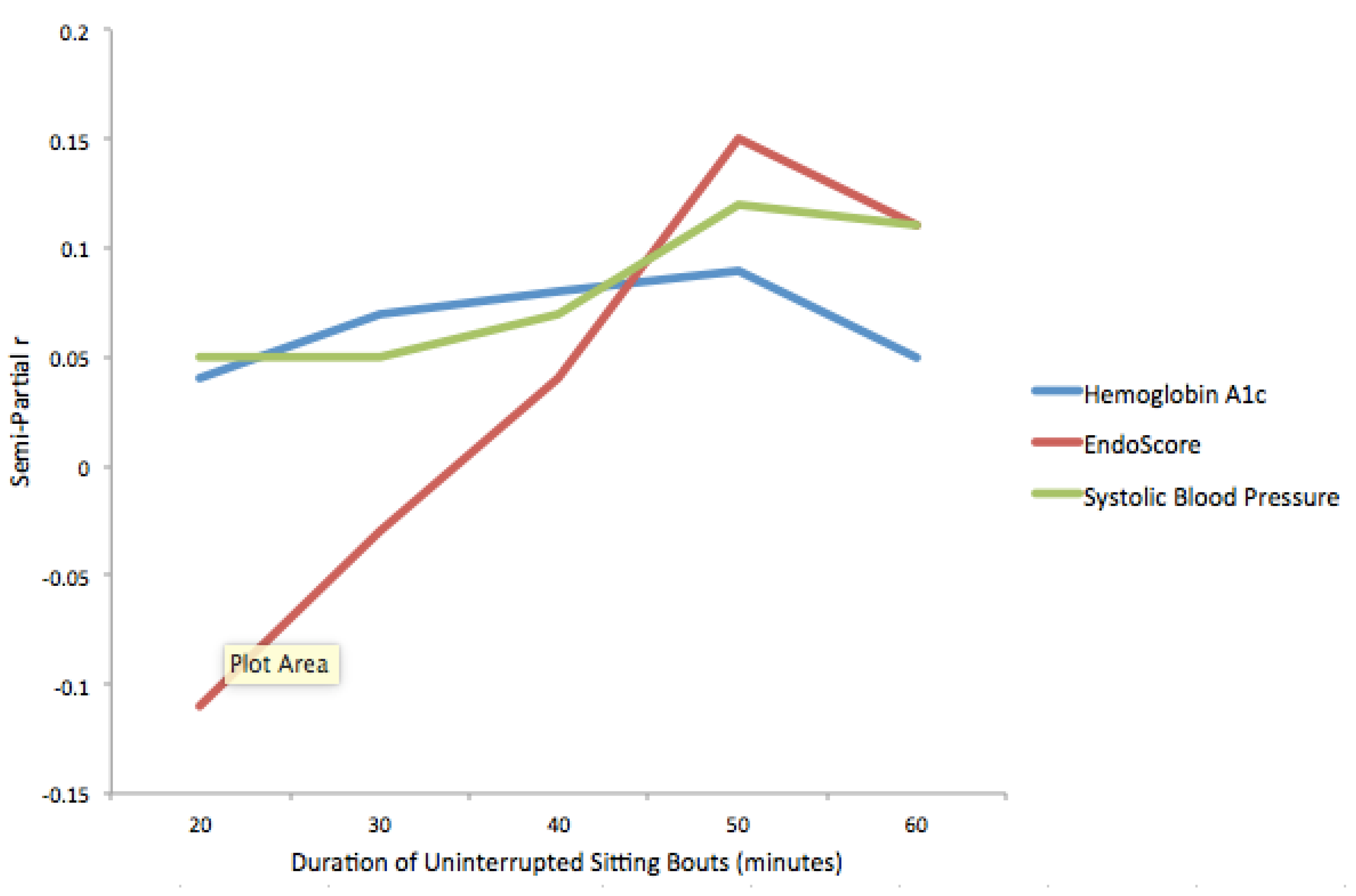
| Hemoglobin A1c | N | b | p | 95% CI | Semi-Partial r |
| Frequency of 20+ min bouts | 234 | 9.96 | 0.550 | −22.84–42.77 | 0.04 |
| Frequency of 30+ min bouts | 234 | 26.40 | 0.258 | −19.47–72.27 | 0.07 |
| Frequency of 40+ min bouts | 234 | 40.47 | 0.203 | −21.95–102.88 | 0.08 |
| Frequency of 50+ min bouts | 234 | 66.29 | 0.141 | −22.13–154.71 | 0.09 |
| Frequency of 60+ min bouts | 234 | 52.72 | 0.406 | −72.13–177.57 | 0.05 |
| EndoScore | N | b | p | 95% CI | Semi-Partial r |
| Frequency of 20+ min bouts | 56 | −11.25 | 0.427 | −39.42–16.93 | −0.11 |
| Frequency of 30+ min bouts | 56 | −4.70 | 0.817 | −45.21–35.82 | −0.03 |
| Frequency of 40+ min bouts | 56 | 9.37 | 0.747 | −48.61–67.34 | 0.04 |
| Frequency of 50+ min bouts | 56 | 40.55 | 0.271 | −32.58–113.67 | 0.15 |
| Frequency of 60+ min bouts | 56 | 38.42 | 0.434 | −59.41–136.26 | 0.11 |
| Systolic Blood Pressure | N | b | p | 95% CI | Semi-Partial r |
| Frequency of 20+ min bouts | 235 | 207.14 | 0.427 | −306.01–720.30 | 0.05 |
| Frequency of 30+ min bouts | 235 | 281.89 | 0.440 | −435.76–999.54 | 0.05 |
| Frequency of 40+ min bouts | 235 | 553.74 | 0.264 | −420.40–1527.88 | 0.07 |
| Frequency of 50+ min bouts | 235 | 1262.39 | 0.072 | −115.48–2640.27 | 0.12 |
| Frequency of 60+ min bouts | 235 | 1611.05 | 0.102 | −323.07–3545.17 | 0.11 |
| Variable | Mean (SD) |
|---|---|
| % Work Hours Sitting or Lying | 83.07 (12.91) |
| % Work Hours Standing | 13.22 (12.29) |
| % Work Hours Stepping | 3.70 (3.18) |
| % Work Hours in Sedentary Activity | 77.81 (8.89) |
| % Work Hours in Light Activity | 19.35 (8.29) |
| % Work Hours in Moderate Activity | 2.67 (1.79) |
| Hemoglobin A1c | N | b | p | 95% CI | Semi-Partial r |
| % Work Hours Sitting or Lying | 234 | 0.00 | 0.819 | −0.01–0.01 | 0.02 |
| % Work Hours Standing | 234 | 0.00 | 0.948 | −0.01–0.01 | −0.00 |
| % Work Hours Stepping | 234 | 0.03 | 0.248 | −0.08–0.02 | −0.07 |
| % Work Hours in Sedentary Activity | 234 | 0.01 | 0.566 | −0.01–0.02 | 0.04 |
| % Work Hours in Light Activity | 234 | −0.01 | 0.565 | −0.024–0.013 | −0.04 |
| % Work Hours in Moderate Activity | 234 | −0.00 | 0.989 | −0.09–0.09 | −0.00 |
| EndoScore | N | b | p | 95% CI | Semi-Partial r |
| % Work Hours Sitting or Lying | 56 | −0.01 | 0.112 | −0.02–0.00 | −0.21 |
| % Work Hours Standing | 56 | 0.01 | 0.136 | −0.00–0.15 | 0.20 |
| % Work Hours Stepping | 56 | 0.03 | 0.435 | −0.04–0.09 | 0.11 |
| % Work Hours in Sedentary Activity | 56 | −0.01 | 0.409 | −0.02–0.01 | −0.11 |
| % Work Hours in Light Activity | 56 | 0.01 | 0.333 | −0.01–0.02 | 0.13 |
| % Work Hours in Moderate Activity | 56 | −0.01 | 0.834 | −0.11–0.09 | −0.03 |
| Systolic Blood Pressure | N | b | p | 95% CI | Semi-Partial r |
| % Work Hours Sitting or Lying | 235 | −0.15 | 0.127 | −0.33–0.04 | −0.10 |
| % Work Hours Standing | 235 | 0.15 | 0.139 | −0.05–0.341 | 0.10 |
| % Work Hours Stepping | 235 | 0.73 | 0.053 | −0.01–1.46 | 0.12 |
| % Work Hours in Sedentary Activity | 235 | 0.05 | 0.707 | −0.22–0.33 | 0.02 |
| % Work Hours in Light Activity | 235 | −0.11 | 0.442 | −0.41–0.18 | −0.05 |
| % Work Hours in Moderate Activity | 235 | 0.67 | 0.335 | −0.70–2.03 | 0.06 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Wipfli, B.; Wild, S.; Donovan, C.; Hanson, G.C.; Thosar, S.S. Sedentary Work and Physiological Markers of Health. Int. J. Environ. Res. Public Health 2021, 18, 3230. https://doi.org/10.3390/ijerph18063230
Wipfli B, Wild S, Donovan C, Hanson GC, Thosar SS. Sedentary Work and Physiological Markers of Health. International Journal of Environmental Research and Public Health. 2021; 18(6):3230. https://doi.org/10.3390/ijerph18063230
Chicago/Turabian StyleWipfli, Brad, Sara Wild, Courtney Donovan, Ginger C. Hanson, and Saurabh S. Thosar. 2021. "Sedentary Work and Physiological Markers of Health" International Journal of Environmental Research and Public Health 18, no. 6: 3230. https://doi.org/10.3390/ijerph18063230
APA StyleWipfli, B., Wild, S., Donovan, C., Hanson, G. C., & Thosar, S. S. (2021). Sedentary Work and Physiological Markers of Health. International Journal of Environmental Research and Public Health, 18(6), 3230. https://doi.org/10.3390/ijerph18063230






