Influence of the Use of Wii Games on Physical Frailty Components in Institutionalized Older Adults
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Experimental Protocol
2.3. Main Outcomes—Instruments
- Static Balance: Static balance was evaluated using the Berg equilibrium scale. This instrument assesses the functional limitations related to the practice of Android Virtual that requires static balance [10]. It is composed of 14 items that represent daily activities the population faces in their lives [22]. Some of them are scored according to the quality of execution, while others are evaluated according to the time required to complete the task [23].
- The evaluator applied the items and briefly demonstrated each one or read the instructions aloud [22]. During the test, the user’s performance on each task was evaluated with a score between 0 and 4, where 0 was the lowest level of function and 4 the highest, noting additional comments if necessary. Although a score of 0 to 20 was classified as “high falling risk,” “moderate falling risk” from 21 to 41, and “slight falling risk” from 41 to 56; considering this last score as a normal value, this study analyzed static balance by total score. Thus, the higher the score, the better their balance. This is a useful instrument in the older adults and in individuals referred to rehabilitation who present deficits in balance, regardless of age. This tool provides information on the most difficult balancing tasks to perform, facilitates the identification of suitable users for an intervention, and identifies people with the highest falling risk [24]. It is also beneficial for the design of interventions, follow-up, and evaluation of their efficacy. This tool is validated in Spain, with a reliability of 0.98, and is considered one of the best tests for assessing balance at present [23].
- Walking Speed: To measure walking speed, the “Gait Speed” test was used. To do this, the person walked six or eight meters in a straight line, which required a global walking length of about 10 m, considering the start and end of the walk, with respect to the marked measurement points. The time used to travel that distance “at normal, comfortable speed” was timed and considered the normal value. In primary care, it is usually performed at 3–4 m due to space limitations. It is advised to repeat this process four times and consider the best time [25]. The cutoff points most commonly used to determine the risk threshold are usually between 1 and 0.8 m/sec.
- Falling Risk: The Downton fall risk was used to assess falling risk [26]. The Downton fall risk index includes 11 risk items, which are scored one point each. Scores were summed to a total index score, ranging 0–11. Although a score of 3 or more indicates a high risk of falling; this study used the total score, where a higher score indicated greater risk of falling (11 was the highest) [23].
- Physical performance: In the same line, the Short Physical Performance Battery (SPPB or Guralnik test) was used. It consisted of performing three tests: balance (in three positions: feet together, semitandem, and tandem), walk (about 2.4 to 4 m), and get up and sit in a chair five times. It is important to follow the sequence of the tests, since, if the patient starts by standing up and sitting down, he/she can become fatigued and give falsely low performances in the other two subtests. The average administration time, with training, was between 6 and 10 min. The normative values for the Spanish population have been established in various population cohort studies and in primary care. The score and evaluation of the total SPPB result was the sum of the three subtests and ranged from 0 (worst) to 12 (12 indicating the highest degree of lower extremity functioning) [27].
- Frailty Phenotype: The Frailty Phenotype was determined by Fried Frailty Scale [28]. This scale examines different factors: (a) unintentional weight loss >4.5 kg or >5% in the last year; (b) self-perception of exhaustion; and (c) weakness quantified by means of maximum digital grip strength with a dynamometer adjusted for sex and body mass index (BMI). To assess weakness, the patient was seated, preferably with the dominant hand and the elbow at 90°. The highest value of 3 measurements (separated by one minute) was considered. The cutoff values to determinate weakness for men were BMI ≤ 24 kg/m2, grip strength ≤ 29 kg; BMI 24.1–26 kg/m2, grip strength ≤ 30 kg; BMI 26.1–28 kg/m2, grip strength ≤ 30 kg; and BMI > 28 kg/m2, grip strength ≤ 32 kg. For women, the cutoff values were BMI ≤ 23 kg/m2, grip strength ≤ 17 kg; BMI 23.1–26 kg/m2, grip strength ≤ 17.3 kg; BMI 26.1–29 kg/m2, grip strength ≤ 18 kg; and BMI > 29 kg/m2, grip strength ≤ 21 kg; (d) Slow gait speed, based on the time required for walking 15 ft (4.57 m) at a normal step. Walk time ≥7 s for men ≤173 cm in height or women ≤159 cm in height or walk time ≥6 s for men whose height was > 173 cm or women whose height was > 159 cm was considered as slowness; (e) Low activity level, energy expenditure of physical activity per week < 383 kcal for men, which corresponds to a minimum of 2.30 h of physical activity per week, or <270 kcal for women, which is equivalent to a minimum of 2 h of activity per week. The presence of 1 or 2 previous characteristics is considered a state of prefrailty, and frailty, by the presence of 3 or more [28,29].
2.4. Statistical Analysis
3. Results
4. Discussion
4.1. Limitations, Strengths, and Future Lines of Research
4.2. Practical Applications
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Machón, M.; Vergara, I.; Dorronsoro, M.; Larrañaga, N.; Vrotsou, K.; Larrañaga, I. Current situation of the Research on Living Conditions and Health Status of Elderly People in Spain. Enferm. Clin. 2016, 26, 15–22. [Google Scholar] [CrossRef]
- Da Silva, A. Intervención no Farmacológica en Enfermos con Apatía en la Demencia. Ph.D. Thesis, University of Burgos, Burgos, Spain, 2015. [Google Scholar]
- Rendón, M.C.; Rodríguez, M.A. Valoración Clínica Geriátrica Integral en Medicina Familiar. Rev. Med. Inst. Mex. Seguro Soc. 2011, 49, 171–177. [Google Scholar] [CrossRef]
- López, R.; Mancilla, E.; Villalobos, A.; Herrera, P. Manual de Prevención de Caídas en el Adulto Mayor, 1st ed.; Ministerio de Salud de Chile: Santiago, Chile, 2010; pp. 13–17.
- Sánchez, L.M.; González, U.; González, A.; Bacallao, J. Calidad de Vida Psíquica y Estado de Salud Física en el Adulto Mayor. Revista Habanera de Ciencias Médicas 2014, 13, 337–342. [Google Scholar]
- Van Diest, M.; Stegenga, J.; Wôrtche, H.J.; Verkerke, G.J.; Postem, K.; Lamoth, C.J. Exergames for Unsupervised Balance Training at Home: A Pilot Study in Healthy Older Adults. Gait Posture 2015, 44, 161–167. [Google Scholar] [CrossRef]
- Garcia, J.; Schoene, D.; Lord, S.; Delbaere, K.; Valenzuela, T.; Navarro, A. Bespoke Kinect Stepping Exergame for Improving Physical and Cognitive Function in Older People: A Pilot Study. Games Health J. 2016, 5, 382–388. [Google Scholar] [CrossRef] [PubMed]
- Formiga, F. Las Caídas, un Síndrome Geriátrico por Excelencia. Rev. Esp. Geriatr. Gerontol. 2009, 44, 299–300. [Google Scholar] [CrossRef]
- Cerda, L. Manejo del Trastorno de Marcha del Adulto Mayor. Rev. Med. Clin. Las Condes 2014, 25, 265–275. [Google Scholar] [CrossRef]
- Debra, J. Equilibrio y Movilidad con Personas Mayore, 2nd ed.; Editorial Paidotribo: Badalona, Spain, 2014. [Google Scholar]
- Contreras, K.; Cubillos, R.; Hernández, O.; Reveco, C.; Santis, N. Rehabilitación Virtual en la Intervención de Terapia Ocupacional. Rev. Chil. Terap. Ocup. 2014, 14, 197–209. [Google Scholar] [CrossRef]
- Cohen, G.; Firth, K.; Biddle, S.; Lloy, M.J.; Simmens, S. The First Therapeutic Game Specifically Designed and Evaluated for Alzheimer’s Disease. Am. J. Alzheimer’s Dis. Other Dement. 2008, 23, 540–551. [Google Scholar] [CrossRef]
- Shih, C.H. A Standing Location Detector Enabling People with Developmental Disabilities to Control Environmental Stimulation through Simple Physical Activities with Nintendo Wii Balance Boards. Res. Dev. Disabil. 2011, 3, 699–704. [Google Scholar] [CrossRef] [PubMed]
- White, K.; Schofield, G.; Kilding, A.E. Energy Expended by Boys Playing Active Video games. J. Sci. Med. Sport 2011, 4, 130–134. [Google Scholar] [CrossRef] [PubMed]
- Lange, B.; Flynn, S.; Proffitt, R.; Chang, C.Y.; Rizzo, A.Z. Development of an Interactive Game-Based Rehabilitation Tool for Dynamic Balance Training. Top. Stroke Rehabil. 2010, 17, 345–352. [Google Scholar] [CrossRef]
- Vieira, G.; Simoes, M.D.; Mori, L.; Ribeiro, J.M.; Pereira, L.A.; Varise, E.M.; Carvas, N.J.; Lange, B.; Jacob Filho, W.; Pompeu, J.E. Feasibility, Safety, Acceptability, and Functional Outcomes of Playing Nintendo Wii Fit PlusTM for Frail Older Adults: A Randomized Feasibility Clinical Trial. Maturitas 2018, 118, 20–28. [Google Scholar] [CrossRef]
- Nilsagard, Y.E.; Forsberg, A.S.; Von Koch, L. Balance Exercise for Persons with Multiple Sclerosis Using Wii Games: A Randomised, Controlled Multi-centre Study. Mult. Scler. 2013, 19, 209–216. [Google Scholar] [CrossRef] [PubMed]
- Toulotte, C.; Toursel, C.; Olivier, N. Wii Fit® Training vs. Adapted Physical Activities: Which One is The Most Appropriate to Improve the Balance of Independent Senior Subjects? A randomized Controlled Study. Clin. Rehabil. 2012, 26, 827–835. [Google Scholar] [CrossRef]
- Andresen, E.M.; Wolinsky, R.; Miller, P.; Wilson, M.M.; Malmtrom, T.; Miller, D. Cross-sectional and Longitudinal Risk Factors for Falls, Fear of Falling, and Falls Efficacy in a Cohort of Middle-aged African Americans. Gerontologist 2006, 46, 49–57. [Google Scholar] [CrossRef]
- Lavedán, A.; Jürschik, P.; Botigué, T.; Nuin, C.; Viladrosa, M. Prevalencia y Factores Asociados a Caídas en Adultos Mayores que Viven en la Comunidad. Atención Primaria 2015, 47, 367–375. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Instituto Nacional de Estadística (INE). Encuesta Personas Mayores. 2019. Available online: https://www.ine.es/jaxiT3/Tabla.htm?t=1488 (accessed on 22 January 2021).
- Berg, K.; Wood-Dauphinée, S.; Williams, J.I.; Gayton, D. Measuring Balance in the Elderly: Preliminary Development of an Instrument. Physiother. Can. 1989, 41, 304–311. [Google Scholar] [CrossRef]
- Shumway-Cook, A.; Baldwin, M.; Polissar, N.L.; Gruber, W. Predicting the Probability for Falls in Community-Dwelling Older Adults. Phys. Ther. 1997, 77, 812–819. [Google Scholar] [CrossRef] [PubMed]
- Phelan, E.; Mahoney, J.; Voit, J.; Stevens, J. Assessment and Management of Fall Risk in Primary Care Settings. Med. Clin. N. Am. 2015, 99, 281–293. [Google Scholar] [CrossRef] [PubMed]
- Consejo Interterritorial del SNS. Documento de Consenso sobre Prevención de Fragilidad y Caídas en la Persona mayor. Estrategia de Promoción de la Salud y Prevención en el SNS, 1st ed.; Ministerio de Sanidad y Consumo: Madrid, Spain, 2014. [Google Scholar]
- Downton, J.H. Falls in the Elderly, 1st ed.; Edward Arnold: London, UK, 1993. [Google Scholar]
- Vasunilashorn, S.; Coppin, A.K.; Patel, K.V.; Lauretani, F.; Ferrucci, L.; Bandinelli, S.; Guralnik, J.M. Use of the Short Physical Performance Battery Score to predict loss of ability to walk 400 meters: Analysis from the InCHIANTI study. J. Gerontol. Ser. A Biomed. Sci. Med. Sci. 2009, 64, 223–229. [Google Scholar] [CrossRef]
- Fried, L.; Tangen, C.; Walston, J.; Newman, A.; Hirsch, C.; Gottdiener, J.; Seeman, T.; Tracy, R.; Kop, W.J.; Burke, G.; et al. Frailty in Older Adults: Evidence for a Phenotype. J. Gerontol. A Biol. Sci. Med. Sci. 2001, 56, 146–156. [Google Scholar] [CrossRef]
- Huded, C.; Huded, J.M.; Friedman, J.L. Frailty Status and Outcomes after Transcatheter Aortic Valve Implantation. Am. J. Cardiol. 2016, 117, 1966–1971. [Google Scholar] [CrossRef] [PubMed]
- Hubbard, R.E.; Lang, I.A.; Llewellyn, D.J.; Rockwood, K. Frailty, body mass index, and abdominal obesity in older people. J. Gerontol. Ser. A Biomed. Sci. Med. Sci. 2010, 65, 377–381. [Google Scholar] [CrossRef]
- Gordon, E.H.; Peel, N.M.; Samanta, M.; Theou, O.; Howlett, S.E.; Hubbard, R.E. Sex differences in frailty: A systematic review and meta-analysis. Exp. Gerontol. 2017, 89, 30–40. [Google Scholar] [CrossRef]
- Ferguson, C.J. An Effect Size Primer: A Guide for Clinicians and Researchers. Prof. Psychol. Res. Pract. 2009, 40, 532–538. [Google Scholar] [CrossRef]
- Manchester, D.; Woollacott, M.; Zederdauer-Hylton, N.; Marin, O. Visual, Vestibular and Somatosensory Contributions to Balance Control in the Older adult. J. Am. Geriatr. Soc. 1989, 44, 118–127. [Google Scholar] [CrossRef]
- Castell, M.V.; Sánchez, M.; Julián, R.; Queipo, R.; Martín, S.; Otero, A. Frailty Prevalence and Slow Walking Speed in Persons Age 65 and Older: Implications for Primary Care. BMC Fam. Pract. 2013, 14, 86. [Google Scholar] [CrossRef] [PubMed]
- Casals, C.; Casals, J.L.; Suárez, E.; Aguilar, M.P.; Estébanez, F.M.; Vázquez, M.A. Frailty in Older Adults with Type 2 Diabetes Mellitus and its Relation with Glucemic Control, Lipid Profile, Blood Pressure, Balance, Disability Grade and Nutritional Status. Nutr. Hosp. 2019, 35, 820–826. [Google Scholar] [CrossRef]
- Hamer, M.; Ingle, L.; Carroll, S.; Stamatakis, E. Physical Activity and Cardiovascular Mortality Risk: Possible Protective Mechanisms? Med. Sci. Sports Exerc. 2011, 44, 84–88. [Google Scholar] [CrossRef]
- Campa, F.; Silva, A.M.; Toselli, S. Changes in Phase Angle and Handgrip Strength Induced by Suspension Training in Older Women. Int. J. Sports Med. 2018, 39, 442–449. [Google Scholar] [CrossRef]
- Dos Santos, L.; Ribeiro, A.S.; Nunes, J.P.; Tomeleri, C.M.; Nabuco, H.; Nascimento, M.A.; Sugihara Junior, P.; Fernandes, R.R.; Campa, F.; Toselli, S.; et al. Effects of Pyramid Resistance-Training System with Different Repetition Zones on Cardiovascular Risk Factors in Older Women: A Randomized Controlled Trial. Int. J. Environ. Res. Public Health 2020, 17, 6115. [Google Scholar] [CrossRef]
- Dos Santos, L.; Ribeiro, A.S.; Gobbo, L.A.; Nunes, J.P.; Cunha, P.M.; Campa, F.; Toselli, S.; Schoenfeld, B.J.; Sardinha, L.B.; Cyrino, E.S. Effects of Resistance Training with Different Pyramid Systems on Bioimpedance Vector Patterns, Body Composition, and Cellular Health in Older Women: A Randomized Controlled Trial. Sustainability 2020, 12, 6658. [Google Scholar] [CrossRef]
- Yagúe, M.P.; Yagúe, M.M.; Lekuona, A.; Sanz, M.C. Los Videojuegos en el Tratamiento Fisioterápico de la Parálisis Cerebral. Fisioterapia 2016, 38, 295–302. [Google Scholar] [CrossRef]
- Cinek, A.; Razak, A.; Tarakci, E. Interactive Video Game-Based Approaches Improve Mobility and Mood in Older Adults: A Nonrandomized, Controlled Trial. J. Bodyw. Mov. Ther. 2020, 24, 252–259. [Google Scholar] [CrossRef]
- Manlapaz, D.; Jayakarany, P.; Chapple, C.; Sole, G. A Narrative Synthesis of Nintendo Wii Fit Gaming Protocol in Addressing Balance among Healthy Older Adults: What System Works? Games Health J. 2017, 6, 65–74. [Google Scholar] [CrossRef] [PubMed]
- Jeoung, B.J.; Lee, Y.C.H. A Study of Relationship between Frailty and Physical Performance in Elderly Women. J. Exerc. Rehabil. 2015, 11, 215–219. [Google Scholar] [CrossRef] [PubMed]
- Narazaki, K.; Matsuo, E.; Honda, T.; Nofuji, Y.; Yonemoto, K.; Kumagai, S. Physical Fitness Measures as Potential Markers of Low Cognitive Function in Japanese Community-Dwelling Older Adults without Apparent Cognitive Problems. J. Sports Sci. Med. 2014, 13, 590–596. [Google Scholar] [PubMed]
| Study Period | Control (n = 40; 23 Women) | 95% CI | Wii (n = 40; 22 Women) | 95% CI | p-Value (t × G) | η2 p | Statistical Power |
|---|---|---|---|---|---|---|---|
| Body Mass (kg) | |||||||
| T1 | 76.35 ± 13.54 | 72.15–80.55 | 74.60 ± 13.01 | 70.57–78.63 | 0.366 | 0.011 | 0.154 |
| T2 | 76.18 ± 12.48 | 72.31–80.05 | 75.10 ± 12.57 | 71.20–79.00 | |||
| Waist Circumference (cm) | |||||||
| T1 | 96.73 ± 14.47 | 92.25–101.21 | 96.97 ± 14.74 | 91.40–101.54 | 0.597 | 0.004 | 0.111 |
| T2 | 96.45 ± 14.16 | 92.06–100.84 | 96.63 ± 14.51 * | 92.13–101.13 | |||
| Arm Circumference (cm) | |||||||
| T1 | 31.18 ± 37.99 | 19.41–42.95 | 31.25 ± 37.99 | 19.48–43.02 | 0.172 | 0.024 | 0.322 |
| T2 | 31.31 ± 37.78 | 16.60–43.02 | 31.88 ± 38.69 | 19.89–43.83 | |||
| Leg Circumference (cm) | |||||||
| T1 | 49.86 ± 11.34 | 46.35–53.37 | 49.65 ± 12.37 | 45.82–53.48 | 0.551 | 0.005 | 0.062 |
| T2 | 49.80 ± 11.13 | 46.35–53.25 | 49.51 ± 12.00 | 45.79–53.23 | |||
| Frailty Phenotype | Sample | T1 | T2 | ||
|---|---|---|---|---|---|
| Control | Wii | Control | Wii | ||
| Prefrailty | n (%) | 30 (56.6%) | 23 (43.4%) | 26 (43.3%) | 34 (56.7%) |
| Frailty | n (%) | 10 (37.0%) | 17 (63.0%) | 14 (70.0%) | 6 (30.0%) |
| p | 0.098 | 0.039 | |||
| Study Period | Control (n = 40; 23 Women) | 95% CI | Wii (n = 40; 22 Women) | 95% CI | p-Value (txG) | η2 p | Statistical Power |
|---|---|---|---|---|---|---|---|
| Right Grip Strength (kg) | |||||||
| TI | 14.09 ± 6.36 | 12.12–16.06 | 13.71 ± 6.18 | 11.79–15.63 | 0.650 | 0.003 | 0.073 |
| T2 | 14.54 ± 6.42 | 12.55–16.53 | 14.44 ± 6.22 | 12.51–16.37 | |||
| Left Grip Strength (kg) | |||||||
| TI | 12.96 ± 5.58 | 11.23–14.69 | 12.85 ± 5.80 | 11.05–14.65 | 0.196 | 0.023 | 0.251 |
| T2 | 13.29 ± 5.67 * | 11.53–15.05 | 13.52 ± 5.85 * | 11.71–15.33 | |||
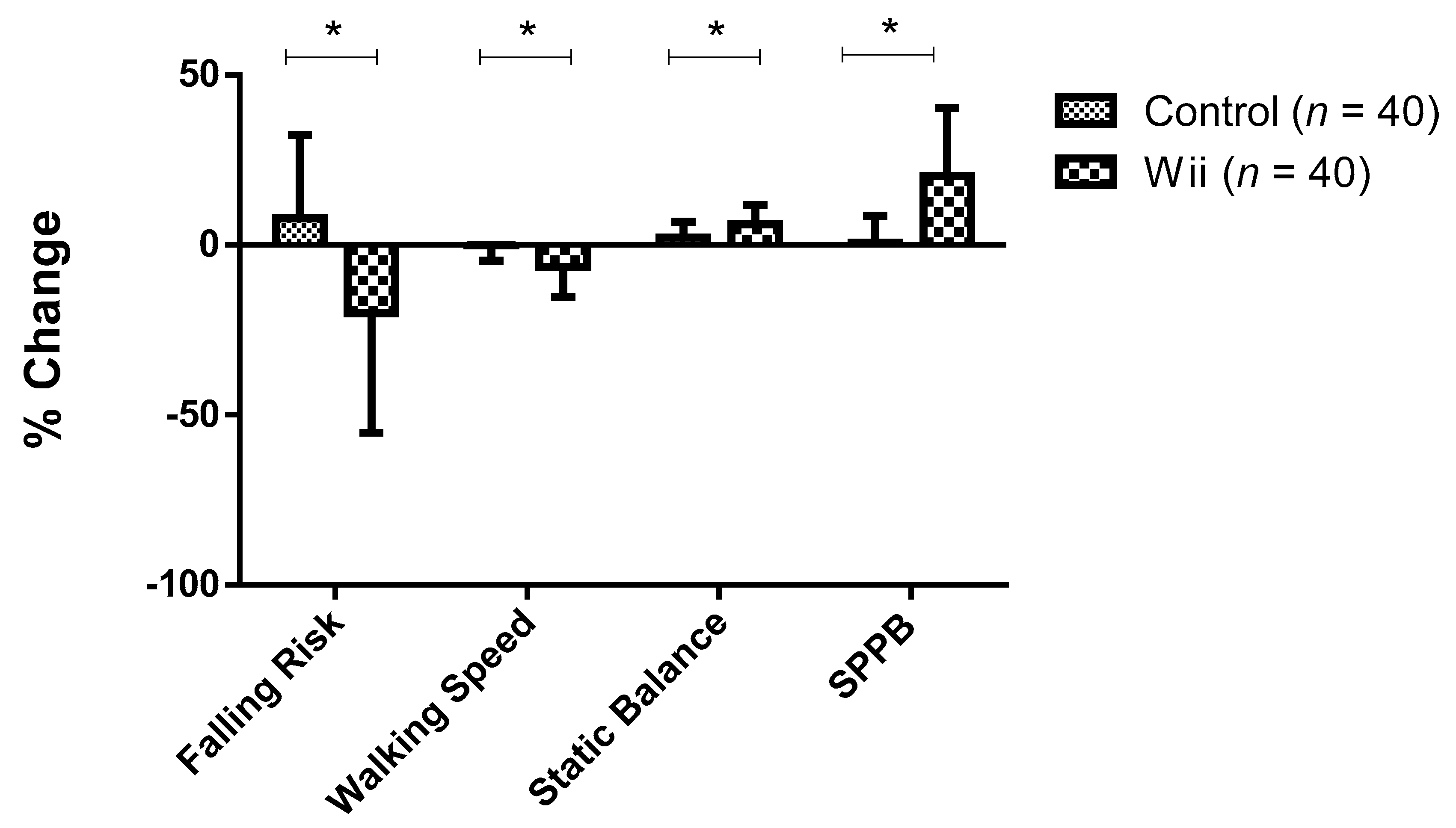
| Falling Risk (Total Score) | |||||||
| TI | 3.58 ± 2.09 | 2.93–4.23 | 3.75 ± 2.07 | 3.11–4.39 | <0.001 | 0.248 | 0.998 |
| T2 | 3.80 ± 2.17 * | 3.13–4.47 | 2.98 ± 1.76 * | 2.43–3.53 | |||
| Walking Speed (sec) | |||||||
| TI | 20.35 ± 7.40 | 18.06–22.64 | 21.24 ± 7.41 | 18.94–23.54 | <0.001 | 0.198 | 0.986 |
| T2 | 20.33 ± 7.45 | 18.02–22.64 | 19.96 ± 7.26 * | 17.71–22.21 | |||
| Static Balance (Total Score) | |||||||
| TI | 38.45 ± 11.85 | 34.78–42.12 | 39.03 ± 10.67 | 35.72–42.34 | <0.001 | 0.186 | 0.979 |
| T2 | 39.18 ± 12.04 * | 35.45–42.91 | 41.08 ± 10.52 * | 37.82–44.34 | |||
| Short Physical Performance Battery (Total Score) | |||||||
| TI | 6.20 ± 2.23 | 5.51–6.89 | 6.33 ± 1.66 | 5.82–6.84 | <0.001 | 0.208 | 0.990 |
| T2 | 6.23 ± 2.24 | 5.54–6.92 | 7.70 ± 2.62 *,& | 6.89–8.51 | |||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
González-Bernal, J.J.; Jahouh, M.; González-Santos, J.; Mielgo-Ayuso, J.; Fernández-Lázaro, D.; Soto-Cámara, R. Influence of the Use of Wii Games on Physical Frailty Components in Institutionalized Older Adults. Int. J. Environ. Res. Public Health 2021, 18, 2723. https://doi.org/10.3390/ijerph18052723
González-Bernal JJ, Jahouh M, González-Santos J, Mielgo-Ayuso J, Fernández-Lázaro D, Soto-Cámara R. Influence of the Use of Wii Games on Physical Frailty Components in Institutionalized Older Adults. International Journal of Environmental Research and Public Health. 2021; 18(5):2723. https://doi.org/10.3390/ijerph18052723
Chicago/Turabian StyleGonzález-Bernal, Jerónimo J., Maha Jahouh, Josefa González-Santos, Juan Mielgo-Ayuso, Diego Fernández-Lázaro, and Raúl Soto-Cámara. 2021. "Influence of the Use of Wii Games on Physical Frailty Components in Institutionalized Older Adults" International Journal of Environmental Research and Public Health 18, no. 5: 2723. https://doi.org/10.3390/ijerph18052723
APA StyleGonzález-Bernal, J. J., Jahouh, M., González-Santos, J., Mielgo-Ayuso, J., Fernández-Lázaro, D., & Soto-Cámara, R. (2021). Influence of the Use of Wii Games on Physical Frailty Components in Institutionalized Older Adults. International Journal of Environmental Research and Public Health, 18(5), 2723. https://doi.org/10.3390/ijerph18052723










