A Scoping Review of Psychosocial Risks to Health Workers during the Covid-19 Pandemic
Abstract
1. Introduction
- (1)
- Job content, e.g., conflicting demands, lack of role clarity, lack of training and development opportunities, and lack of workers’ influence over the way the job is done.
- (2)
- Work organisation and management, e.g., excessive workloads and work intensity, lack of workers’ involvement in making decisions that affect the worker (autonomy), poorly managed organisational changes, ineffective communication, working time arrangements, and poor work-life balance.
- (3)
- The social context of the job, e.g., lack of support from management or colleagues, psychological and sexual harassment, third-party violence, and job insecurity [9].
2. Materials and Methods
2.1. Scoping Review Design and Data Collection
- (1)
- Identifying the research question with a broad scope: What are the main categories and factors of psychosocial risks to healthcare workers during the Covid-19 pandemic and the related prevention measures?
- (2)
- Identifying relevant studies.
- (3)
- Selecting studies as per the study protocol.
- (4)
- Charting the data. Relevant information was extracted into an Excel sheet from the reviewed literature.
- (5)
- Collating, summarising, and reporting the results in tables and charts according to key themes, with an analytical summary of the findings.
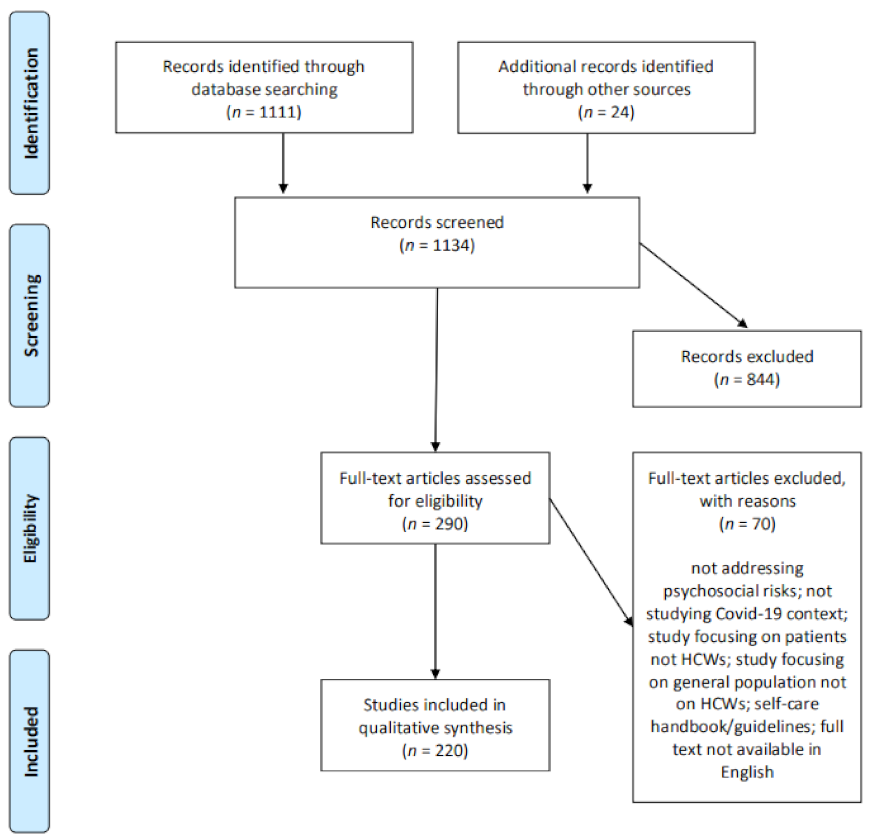
2.2. Identification of Relevant Studies
2.3. Study Selection
2.4. Data Chart and Results Overview
2.5. Study/Publication Types
2.6. Regions and Countries
2.7. Studied Settings, Occupations and Sample Characteristics
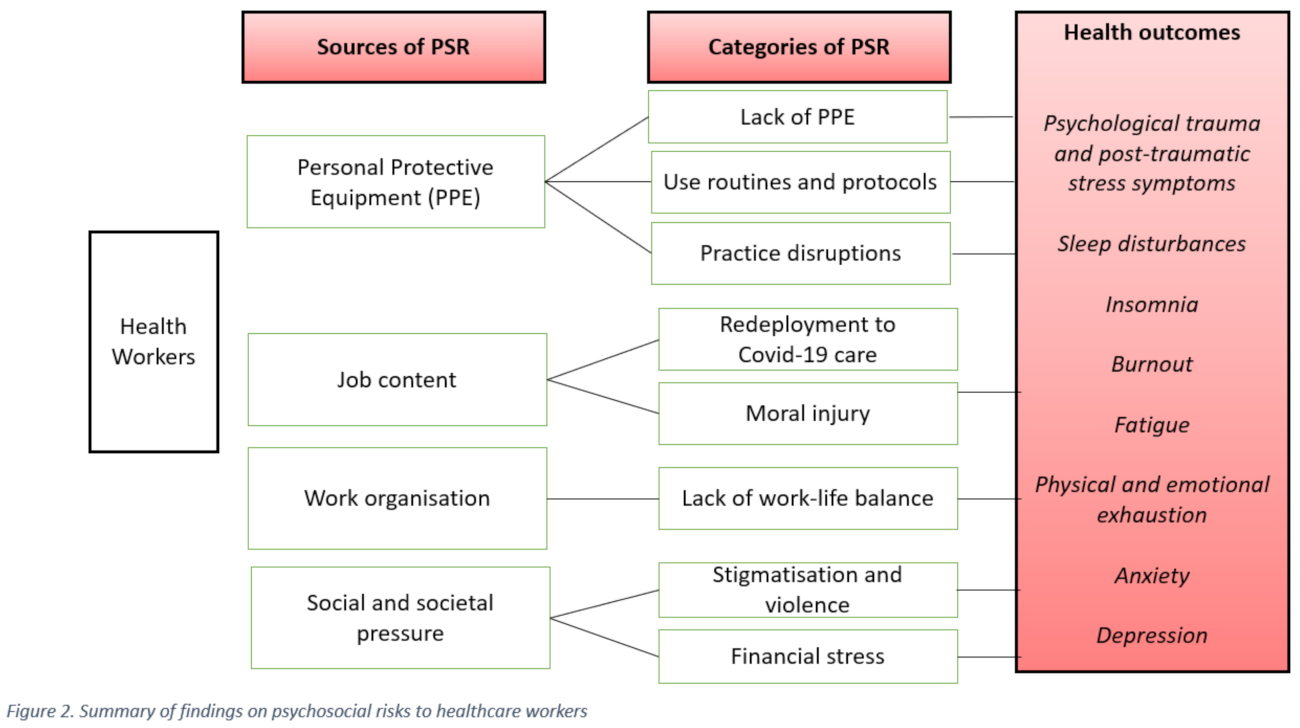
3. Results
3.1. Negative Outcomes for Healthcare Workers
3.2. Psychosocial Risks and Personal Protective Equipment (PPE)
3.2.1. Anxiety Related with the Risk of Infection Due to Lack of Adequate PPE
3.2.2. PPE Use Routines and Protocols Related with Anxiety and Physical Discomfort
3.2.3. PPE and Practice Disruptions
3.3. Psychosocial Risks and Job Content
3.3.1. Redeployment of HCWs to Covid-19 Care
3.3.2. Moral Injury
3.4. Psychosocial Risks and Work Organisation
Work Overload and Lack of Work-Life Balance
3.5. Societal and Social Demands as Sources of Psychosocial Risks
3.5.1. Stigmatisation and Violence against HCWs
3.5.2. Financial Stress
3.6. Interventions and Recommendations
4. Discussion
- (a)
- The long-term impact of the identified psychosocial factors. Evidence is needed regarding the psychological and physical health cost that HCWs pay while being exposed to the first as well as the second wave of the pandemic. Longitudinal study designs may be particularly helpful for studying the long-term effect of the pandemic on HCWs well-being, especially in the light of the care that has been postponed due to the pandemic and will burden health systems in the years to come.
- (b)
- Psychosocial risks for different occupational groups of healthcare workers. Evidence should be collected regarding the risk factors that are particular for speech therapists, paramedics, support, catering, cleaning, and administrative staff in healthcare settings as well as for carers and therapists working in community settings. More evidence is also needed regarding the risk factors for HCWs employed in primary care settings, and social care, as well as in settings that were set particularly for the control of the pandemic (e.g., emergency lines workers, and people who administer Covid-19 tests). The emergence of new variants of the virus, such as the Variant of Concern (VOC) B.1.1.7, with substantially increased transmissibility compared to other variants, calls for new studies on the exposure of healthcare workers.
- (c)
- The intersecting inequalities in psychosocial risks for healthcare workers, particularly for female HCWs. More evidence is needed regarding the actual mechanisms and contexts that increase intersectional vulnerabilities, such as precarious employment, in order to suggest effective prevention and intervention strategies, including: empirical evidence regarding the impact of the pandemic on the physical and psychological well-being of HCWs who identify as ethnic and racial minorities; and evidence on ethnic and/or racial inequalities in mental health outcomes among HCWs.
- (d)
- Finally, an analysis of the combination of workplace and broader societal policy measures that can prevent and mitigate the identified psychosocial risks to healthcare workers is needed to strengthen the preparedness of health systems for future pandemics. Since the Covid-19 pandemic is the first to impact European health systems in a century, country specific analyses on HCWs’ working and employment conditions in relation to psychosocial risks merit further research.
Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- WHO Director-General’s Statement on IHR Emergency Committee on Novel Coronavirus (2019-nCoV). 30 January 2020. Available online: https://www.who.int/director-general/speeches/detail/who-director-general-s-statement-on-ihr-emergency-committee-on-novel-coronavirus-(2019-ncov) (accessed on 26 January 2021).
- Luo, M.; Guo, L.; Yu, M.; Wang, H. The Psychological and Mental Impact of Coronavirus Disease 2019 (COVID-19) on Medical Staff and General Public–A Systematic Review and Meta-analysis. Psychiatry Res. 2020, 291, 113190. [Google Scholar] [CrossRef]
- Sheraton, M.; Deo, N.; Dutt, T.; Surani, S.; Hall-Flavin, D.; Kashyap, R. Psychological effects of the COVID 19 pandemic on healthcare workers globally: A systematic review. Psychiatry Res. 2020, 292, 113360. [Google Scholar] [CrossRef]
- Kisely, S.; Warren, N.; McMahon, L.; Dalais, C.; Henry, I.; Siskind, D. Occurrence, prevention, and management of the psychological effects of emerging virus outbreaks on healthcare workers: Rapid review and meta-analysis. BMJ 2020, 369, m1642. [Google Scholar] [CrossRef]
- Philip, J.; Cherian, V. Factors Affecting the Psychological Well-being of Health Care Workers during an Epidemic: A Thematic Review. Indian J. Psychol. Med. 2020, 42, 323–333. [Google Scholar] [CrossRef]
- Shreffler, J.; Petrey, J.; Huecker, M. The Impact of COVID-19 on Healthcare Worker Wellness: A Scoping Review. West. J. Emerg. Med. 2020, 21, 1059–1066. [Google Scholar] [CrossRef] [PubMed]
- Eurofound. Psychosocial Risks. Available online: https://www.eurofound.europa.eu/topic/psychosocial-risks (accessed on 15 February 2021).
- Hupke, M.; Van den Broek, K.; Kudasz, F. Psychosocial Risks and Workers Health. OSH Wiki. 2020. Available online: https://oshwiki.eu/wiki/Psychosocial_risks_and_workers_health#Definition_of_psychosocial_hazards_and_risks (accessed on 12 February 2021).
- EU-OSHA. Psychosocial Risks and Stress at Work. Available online: https://osha.europa.eu/en/themes/psychosocial-risks-and-stress (accessed on 12 February 2021).
- Adriaenssens, J.; De Gucht, V.; Maesc, S. Determinants and prevalence of burnout in emergency nurses: A systematic review of 25 years of research. Int. J. Nurs. Stud. 2015, 52, 649–661. [Google Scholar] [CrossRef]
- European Agency for Safety and Health at Work (EU-OSHA). Current and Emerging Issues in the Healthcare Sector, including Home and Community Care; European Risk Observatory Report; Publications Office of the European Union: Luxembourg, 2014. [Google Scholar]
- Eurofound. Working Conditions and Workers’ Health; Publications Office of the European Union: Luxembourg, 2019. [Google Scholar]
- European Institute for Gender Equality (EIGE). Gender Equality and Long-term Care at Home; Publications Office of the European Union: Luxembourg, 2020. [Google Scholar]
- Di Tecco, C.; Nielsen, K.; Ghelli, M.; Ronchetti, M.; Marzocchi, I.; Persechino, B.; Iavicoli, S. Improving Working Conditions and Job Satisfaction in Healthcare: A Study Concept Design on a Participatory Organizational Level Intervention in Psychosocial Risks Management. Int. J. Environ. Res. Public Health 2020, 17, 3677. [Google Scholar] [CrossRef]
- Eurofound. Working Conditions in Sectors; Publications Office of the European Union: Luxembourg, 2020. [Google Scholar]
- Barello, S.; Falcó-Pegueroles, A.; Rosa, D.; Tolotti, A.; Graffigna, G.; Bonetti, L. The psychosocial impact of flu influenza pandemics on healthcare workers and lessons learnt for the COVID-19 emergency: A rapid review. Int. J. Public Health 2020, 65, 1205–1216. [Google Scholar] [CrossRef]
- Blanco-Donoso, L.M.; Garrosa, E.; Moreno-Jiménez, J.; Gálvez-Herrer, M.; Moreno-Jiménez, B. Occupational psychosocial risks of health professionals in the face of the crisis produced by the COVID-19: From the identification of these risks to immediate action. Int. J. Nurs. Stud. Adv. 2020, 2, 100003. [Google Scholar] [CrossRef]
- Wagner, A.; Rieger, M.A.; Manser, T.; Sturm, H.; Hardt, J.; Martus, P.; Hammer, A. Healthcare professionals’ perspectives on working conditions, leadership, and safety climate: A cross-sectional study. BMC Health Serv. Res. 2019, 19, 53. [Google Scholar] [CrossRef]
- Jennings, B.M. Work Stress and Burnout among Nurses: Role of the Work Environment and Working Conditions. In Patient Safety and Quality: An Evidence-Based Handbook for Nurses; Hughes, R.G., Ed.; Agency for Healthcare Research and Quality (US): Rockville, MD, USA, April 2008; Chapter 26. Available online: https://www.ncbi.nlm.nih.gov/books/NBK2668/ (accessed on 12 February 2021).
- Nursing Times. Stress and Abuse Remain High among NHS Nurses, Reveals Survey. 18 February 2020. Available online: https://www.nursingtimes.net/news/workforce/stress-and-abuse-remain-high-among-nhs-nurses-reveals-survey-18-02-2020/#:~:text=In%202019%2C%2044%25%20of%20registered,2018%20and%2041.1%25%20in%202015.&text=An%20increasing%20proportion%20of%20nursing,violence%20by%20patients%20and%20relatives (accessed on 12 February 2021).
- Michel, J.P.; Ecarnot, F. The shortage of skilled workers in Europe: Its impact on geriatric medicine. Eur. Geriatr. Med. 2020, 11, 345–347. [Google Scholar] [CrossRef]
- WHO. State of the World’s Nursing 2020: Investing in Education, Jobs and Leadership; Licence: CC BY-NC-SA 3.0 IGO; World Health Organization: Geneva, Switzerland, 2020. [Google Scholar]
- Ruotsalainen, S.; Jantunen, S.; Sinervo, T. Which factors are related to Finnish home care workers’ job satisfaction, stress, psychological distress and perceived quality of care?—A mixed method study. BMC Health Serv. Res. 2020, 20, 896. [Google Scholar] [CrossRef]
- Scozzafave, M.C.S.; Leal, L.A.; Soares, M.I.; Henriques, S.H. Psychosocial risks related to the nurse in the psychiatric hospital and management strategies. Rev. Bras. Enferm. 2019, 72, 834–840. [Google Scholar] [CrossRef]
- Leyva-Vela, B.; Jesús Llorente-Cantarero, F.; Henarejos-Alarcón, S.; Martínez-Rodríguez, A. Psychosocial and physiological risks of shift work in nurses: A cross-sectional study. Cent. Eur. J. Public Health 2018, 26, 183–189. [Google Scholar] [CrossRef] [PubMed]
- Ferri, P.; Guadi, M.; Marcheselli, L.; Balduzzi, S.; Magnani, D.; Di Lorenzo, R. The impact of shift work on the psychological and physical health of nurses in a general hospital: A comparison between rotating night shifts and day shifts. Risk Manag. Healthc. Policy 2016, 9, 203–211. [Google Scholar] [CrossRef]
- Lin, S.H.; Liao, W.C.; Chen, M.Y.; Fan, J.Y. The impact of shift work on nurses’ job stress, sleep quality and self-perceived health status. J. Nurs. Manag. 2014, 22, 604–612. [Google Scholar] [CrossRef] [PubMed]
- Delp, L.; Wallace, S.P.; Geiger-Brown, J.; Muntaner, C. Job stress and job satisfaction: Home care workers in a consumer-directed model of care. Health Serv. Res. 2010, 45, 922–940. [Google Scholar] [CrossRef] [PubMed]
- Zoeckler, J.M. Occupational Stress among Home Healthcare Workers: Integrating Worker and Agency-Level Factors. NEW SOLUTIONS J. Environ. Occup. Health Policy 2018, 27, 524–542. [Google Scholar] [CrossRef]
- Vento, S.; Cainelli, F.; Vallone, A. Violence against Healthcare Workers: A Worldwide Phenomenon with Serious Consequences. Front. Public Health 2020, 8, 570459. [Google Scholar] [CrossRef]
- Eurofound. Violence and Harassment in European Workplaces: Causes, Impacts and Policies; Eurofound: Dublin, Ireland, 2015. [Google Scholar]
- Kuhlmann, E.; Falkenbach, M.; Klasa, K.; Pavolini, E.; Ungureanu, M.A. Migrant carers in Europe in times of COVID-19: A call to action for European health workforce governance and a public health approach. Eur. J. Public Health 2020, 30, iv22–iv27. [Google Scholar] [CrossRef]
- Baumann, A.; Hunsberger, M.; Crea-Arsenio, M.; Akhtar-Danesh, N.; Alameddine, M. A government policy on full-time nursing employment in Ontario, Canada: An evaluation. Health Policy 2018, 122, 109–114. [Google Scholar] [CrossRef] [PubMed]
- Benach, J.; Vives, A.; Amable, M.; Vanroelen, C.; Tarafa, G.; Bonet, C. Precarious Employment: Understanding an Emerging Social Determinant of Health. Annu. Rev. Public Health 2014, 35, 229–253. [Google Scholar] [CrossRef] [PubMed]
- Eurofound and EU-OSHA. Psychosocial Risks in Europe: Prevalence and Strategies for Prevention; Publications Office of the European Union: Luxembourg, 2014. [Google Scholar]
- Nowrouzi, B.; Lightfoot, N.; Larivière, M.; Carter, L.; Rukholm, E.; Schinke, R.; Belanger-Gardner, D. Occupational Stress Management and Burnout Interventions in Nursing and Their Implications for Healthy Work Environments: A Literature Review. Workplace Health Safety 2015, 63, 308–315. [Google Scholar] [CrossRef]
- US OSHA. Recommended Practices for Safety and Health Programs. Worker Participation. Available online: https://www.osha.gov/shpguidelines/worker-participation.html#:~:text=To%20be%20effective%2C%20any%20safety,of%20workers%20and%20their%20representatives.&text=Worker%20participation%20means%20that%20workers,the%20safety%20and%20health%20program (accessed on 12 February 2021).
- ILO. Improving Health in the Workplace: ILO’s Framework for Action. Factsheet. 2014. Available online: https://www.ilo.org/safework/info/publications/WCMS_329350/lang--en/index.htm (accessed on 12 February 2021).
- Sucharew, H.; Macaluso, M. Methods for research evidence synthesis: The scoping review approach. J. Hosp. Med. 2019, 14, 416–418. [Google Scholar] [CrossRef] [PubMed]
- Arksey, H.; O’Malley, L. Scoping studies: Towards a methodological framework. Int. J. Soc. Res. Methodol. 2005, 8, 19–32. [Google Scholar] [CrossRef]
- Munn, Z.; Peters, M.D.; Stern, C.; Tufanaru, C.; McArthur, A.; Aromataris, E. Systematic review or scoping review? Guidance for authors when choosing between a systematic or scoping review approach. BMC Med. Res. Methodol. 2018, 18, 143. [Google Scholar] [CrossRef]
- Pham, M.T.; Rajić, A.; Greig, J.D.; Sargeant, J.M.; Papadopoulos, A.; McEwen, S.A. A scoping review of scoping re-views: Advancing the approach and enhancing the consistency. Res. Synth. Methods 2014, 5, 371–385. [Google Scholar] [CrossRef]
- Tricco, A.C.; Lillie, E.; Zarin, W.; O’Brien, K.; Colquhoun, H.; Kastner, M.; Levac, D.; Ng, C.; Sharpe, J.P.; Wilson, K. A scoping review on the conduct and reporting of scoping reviews. BMC Med. Res. Methodol. 2016, 16, 15. [Google Scholar] [CrossRef] [PubMed]
- WHO Charter for Health Worker Safety: A Priority for Patient Safety. 2020. Available online: https://www.who.int/docs/default-source/world-patient-safety-day/health-worker-safety-charter-wpsd-17-september-2020-3-1.pdf?sfvrsn=2cb6752d_2 (accessed on 26 January 2021).
- Shultz, M. Comparing test searches in PubMed and Google Scholar. J. Med Libr. Assoc. JMLA 2007, 95, 442–445. [Google Scholar] [CrossRef]
- Yin, Q.; Sun, Z.; Liu, T.; Ni, X.; Deng, X.; Jia, Y.; Shang, Z.; Zhou, Y.; Liu, W. Posttraumatic stress symptoms of health care workers during the corona virus disease. Clin. Psychol. Psychother. 2020, 27, 384–395. [Google Scholar] [CrossRef]
- Riello, M.; Purgato, M.; Bove, C.; MacTaggart, D.; Rusconi, E. Prevalence of post-traumatic symptomatology and anxiety among residential nursing and care home workers following the first COVID-19 outbreak in Northern Italy. R. Soc. Open Sci. 2020, 7, 200880. [Google Scholar] [CrossRef]
- Rossi, R.; Socci, V.; Pacitti, F.; Di Lorenzo, G.; Di Marco, A.; Siracusano, A.; Rossi, A. Mental Health Outcomes Among Frontline and Second-Line Health Care Workers During the Coronavirus Disease 2019 (COVID-19) Pandemic in Italy. JAMA Netw. Open 2020, 3, e2010185. [Google Scholar] [CrossRef]
- Luceño-Moreno, L.; Talavera-Velasco, B.; García-Albuerne, Y.; Martín-García, J. Symptoms of Posttraumatic Stress, Anxiety, Depression, Levels of Resilience and Burnout in Spanish Health Personnel during the COVID-19 Pandemic. Int. J. Environ. Res. Public Health 2020, 17, 5514. [Google Scholar] [CrossRef]
- Benham, T.; Hart, A.; Bortolin, M.; Court, M.; Groves, J.; Kraus, A.; Newbury, B.; Voskanyan, A.; Yogman, M.; AlHajjaj, F.; et al. Preparing for the Second Surge: Preventing Posttraumatic Stress Disorder and Building Resilience for Health Care Workers in the Face of COVID-19. Disaster Med. Public Health Prep. 2020, 1–4. [Google Scholar] [CrossRef]
- Raudenská, J.; Steinerová, V.; Javůrková, A.; Urits, I.; Kaye, A.D.; Viswanath, O.; Varrassi, G. Occupational burnout syndrome and post-traumatic stress among healthcare professionals during the novel coronavirus disease 2019 (COVID-19) pandemic. Best Pract. Res. Clin. Anaesthesiol. 2020, 34, 553–560. [Google Scholar] [CrossRef]
- Wu, Y.; Wang, J.; Luo, C.; Hu, S.; Lin, X.; Anderson, A.E.; Bruera, E.; Yang, X.; Wei, S.; Qian, Y. A Comparison of Burnout Frequency among Oncology Physicians and Nurses Working on the Frontline and Usual Wards during the COVID-19 Epidemic in Wuhan, China. J. Pain Symptom Manag. 2020, 60, e60–e65. [Google Scholar] [CrossRef]
- Khanna, R.C.; Honavar, S.G.; Metla, A.L.; Bhattacharya, A.; Maulik, P.K. Psychological impact of COVID-19 on ophthalmologists-in-training and practising ophthalmologists in India. Indian J. Opthamology 2020, 68, 994–998. [Google Scholar] [CrossRef] [PubMed]
- Kotian, R.P.; Faujdar, D.; D’souza, B.; Kotian, S.P.; Kunaparaju, S.; David, L.R. A web survey to assess the perceived mental healthcare among Medical Imaging Professionals during COVID-19 pandemic. Res. Sq. 2020. [Google Scholar] [CrossRef]
- Tan, B.Y.Q.; Chew, N.W.S.; Lee, G.K.H.; Jing, M.; Goh, Y.; Yeo, L.L.L.; Zhang, K.; Chin, H.K.; Ahmad, A.; Khan, F.A.; et al. Psychological Impact of the COVID-19 Pandemic on Health Care Workers in Singapore. Ann. Intern. Med. 2020, 173, 317–320. [Google Scholar] [CrossRef] [PubMed]
- Luo, L.S.; Jin, Y.H.; Cai, L.; Pan, Z.Y.; Zeng, X.T.; Wang, X.H. COVID-19: Presumed Infection Routes and Psychological Impact on Staff in Administrative and Logistics Departments in a Designated Hospital in Wuhan, China. Front. Psychol. 2020, 11, 1501. [Google Scholar] [CrossRef]
- De los Santos, J.A.A.; Labrague, L.J. Impact of COVID-19 on the Psychological Well-Being and Turnover Intentions of Frontline Nurses in the Community: A Cross-Sectional Study in the Philippines. medRxiv 2020. [Google Scholar] [CrossRef]
- Buselli, R.; Baldanzi, S.; Corsi, M.; Chiumiento, M.; Del Lupo, E.; Carmassi, C.; Dell’Osso, L.; Cristaudo, A. Psychological Care of Health Workers during the COVID-19 Outbreak in Italy: Preliminary Report of an Occupational Health Department (AOUP) Responsible for Monitoring Hospital Staff Condition. Sustainability 2020, 12, 5039. [Google Scholar] [CrossRef]
- Ramaci, T.; Barattucci, M.; Ledda, C.; Rapisarda, V. Social Stigma during COVID-19 and its Impact on HCWs Outcomes. Sustainability 2020, 12, 3834. [Google Scholar] [CrossRef]
- Araç, S.; Dönmezdil, S. Investigation of mental health among hospital workers in the COVID-19 pandemic: A cross-sectional study. Sao Paulo Med. J. 2020, 138, 433–440. [Google Scholar] [CrossRef]
- Choudhury, T.; Debski, M.; Wiper, A.; Abdelrahman, A.; Wild, S.; Chalil, S.; More, R.; Goode, G.; Patel, B.; Abdelaziz, H.K. COVID-19 Pandemic: Looking After the Mental Health of Our Healthcare Workers. J. Occup. Environ. Med. 2020, 62, e373–e376. [Google Scholar] [CrossRef] [PubMed]
- Kannampallil, T.G.; Goss, C.W.; Evanoff, B.A.; Strickland, J.R.; McAlister, R.P.; Duncan, J. Exposure to COVID-19 patients increases physician trainee stress and burnout. PLoS ONE 2020, 15, e0237301. [Google Scholar] [CrossRef]
- Hacimusalar, Y.; Kahve, A.C.; Yasar, A.B.; Aydin, M.S. Anxiety and hopelessness levels in COVID-19 pandemic: A comparative study of healthcare professionals and other community sample in Turkey. J. Psychiatr. Res. 2020, 129, 181–188. [Google Scholar] [CrossRef]
- Korkmaz, S.; Kazgan, A.; Çekiç, S.; Tartar, A.S.; Balcı, H.N.; Atmaca, M. The anxiety levels, quality of sleep and life and problem-solving skills in healthcare workers employed in COVID-19 services. J. Clin. Neurosci. 2020, 80, 131–136. [Google Scholar] [CrossRef] [PubMed]
- Sampaio, F.; Sequeira, C.; Teixeira, L. Nurses’ Mental Health during the Covid-19 Outbreak: A Cross-Sectional Study. J. Occup. Environ. Med. 2020, 62, 783–787. [Google Scholar] [CrossRef]
- Zerbini, G.; Ebigbo, A.; Reicherts, P.; Kunz, M.; Messman, H. Psychosocial burden of healthcare professionals in times of COVID-19—A survey conducted at the University Hospital Augsburg. Ger. Med. Sci. 2020, 18, Doc05. [Google Scholar]
- Hong, S.; Ai, M.; Xu, X.; Wang, W.; Chen, J.; Zhang, Q.; Wang, L.; Kuang, L. Immediate psychological impact on nurses working at 42 government-designated hospitals during COVID-19 outbreak in China: A cross-sectional study. Nurs. Outlook 2020, 69, 6–12. [Google Scholar] [CrossRef]
- Orellana, C.I. Health workers as hate crimes targets during coviD-19 outbreak in the Americas. Rev. Salud Pública 2020, 22, e401. [Google Scholar]
- Zhang, C.; Yang, L.; Liu, S.; Ma, S.; Wang, Y.; Cai, Z.; Du, H.; Li, R.; Kang, L.; Su, M.; et al. Survey of Insomnia and Related Social Psychological Factors Among Medical Staff Involved in the 2019 Novel Coronavirus Disease Outbreak. Front. Psychiatry 2020, 11, 306. [Google Scholar] [CrossRef]
- Australian Nursing & Midwifery Federation (ANMF). Covid-19: Provisions for Casual Nurses. Evidence Brief. 26 March 2020. Available online: https://anmf.org.au/documents/ANMF_Evidence_Brief_COVID-19-Casual_Nurses.pdf (accessed on 26 January 2021).
- Mayfield-Johnson, S.; Smith, D.O.; Crosby, S.A.; Haywood, C.G.; Castillo, J.; Bryant-Williams, D.; Jay, K.; Seguinot, M.; Smith, T.; Moore, N.; et al. Insights on COVID-19 From Community Health Worker State Leaders. J. Ambul. Care Manag. 2020, 43, 268–277. [Google Scholar] [CrossRef]
- Peters, M. COVID-19: Provisions for Casual Nurses. Evidence Brief. Australian Nursing and Midwifery Federation, 2020. Available online: https://anmf.org.au/documents/ANMF_Evidence_Brief_COVID-19-Casual_Nurses.pdf (accessed on 15 February 2021).
- Felice, C.; Di Tanna, G.L.; Zanus, G.; Grossi, U. Impact of COVID-19 Outbreak on Healthcare Workers in Italy: Results from a National E-Survey. J. Community Health 2020, 45, 675–683. [Google Scholar] [CrossRef]
- Martínez-López, J.Á.; Lázaro-Pérez, C.; Gómez-Galán, J.; Fernández-Martínez, M.D.M. Psychological Impact of COVID-19 Emergency on Health Professionals: Burnout Incidence at the Most Critical Period in Spain. J. Clin. Med. 2020, 9, 3029. [Google Scholar] [CrossRef]
- Maraqa, B.; Nazzal, Z.; Zink, T. Palestinian Health Care Workers’ Stress and Stressors during COVID-19 Pandemic: A Cross-Sectional Study. J. Prim. Care Community Health 2020, 11, 2150132720955026. [Google Scholar] [CrossRef]
- Paiano, M.; Jaques, A.E.; Nacamura, P.A.B.; Salci, M.A.; Radovanovic, C.A.T.; Carreira, L. Mental health of healthcare professionals in China during the new coronavirus pandemic: An integrative review. Rev. Bras. Enferm. 2020, 73 (Suppl. 2). [Google Scholar] [CrossRef]
- Pandey, N.; Kaushal, V.; Puri, G.D.; Taneja, S.; Biswal, M.; Mahajan, P.; Guru, R.R.; Malhotra, P.; Sehgal, I.S.; Dhooria, S.; et al. Transforming a General Hospital to an Infectious Disease Hospital for COVID-19 Over 2 Weeks. Front. Public Health 2020, 8, 382. [Google Scholar] [CrossRef] [PubMed]
- Rana, W.; Mukhtar, S.; Mukhtar, S. Mental health of medical workers in Pakistan during the pandemic COVID-19 outbreak. Asian J. Psychiatry 2020, 51, 102080. [Google Scholar] [CrossRef]
- Chow, C.; Shahdadpuri, R.; Kai-Qian, K.; Hwee, C.Y. The Next Pandemic: Supporting COVID-19 Frontline Doctors through Film Discussion. J. Med Humanit. 2020, 41, 585–595. [Google Scholar] [CrossRef]
- Neuwirth, M.M.; Mattner, F.; Otchwemah, R. Adherence to personal protective equipment use among healthcare workers caring for confirmed COVID-19 and alleged non-COVID-19 patients. Antimicrob. Resist. Infect. Control. 2020, 9, 199. [Google Scholar] [CrossRef]
- Thomas, T.; Laher, A.E.; Mahomed, A.; Stacey, S.; Motara, F.; Mer, M. Challenges around COVID-19 at a tertiary-level healthcare facility in South Africa and strategies implemented for improvement. S. Afr. Med. J. 2020, 110, 964–967. [Google Scholar]
- McDougall, R.J.; Gillam, L.; Ko, D.; Hlmes, I.; Delany, C. Balancing health worker well-being and duty to care: An ethical approach to staff safety in COVID-19 and beyond. J. Med. Ethics 2020. [Google Scholar] [CrossRef]
- Degado, J.; Siow, S.; de Groot, J.M. The Value of Communities of Practice as a Learning Process to Increase Resilience in Healthcare Teams. Eur. J. Med. Nat. Sci. 2020, 4, 8–24. [Google Scholar]
- Araújo, B.C.L.; Lima, T.R.C.D.M.; Gois-Santos, V.T.D.; Santos, V.S.; Simões, S.D.M.; Martins-Filho, P.R. Speech therapy practice in hospital settings and COVID-19 pandemic. Rev. Associação Médica Brasileira 2020, 66 (Suppl. 2), 10–12. [Google Scholar] [CrossRef]
- Kimura, Y.; Ueha, R.; Furukawa, T.; Oshima, F.; Fujitani, J.; Nakajima, J.; Kaneoka, A.; Aoyama, H.; Fujimoto, Y.; Umezaki, T. Society of swallowing and dysphagia of Japan: Position statement on dysphagia management during the COVID-19 outbreak. Auris Nasus Larynx 2020, 47, 715–726. [Google Scholar] [CrossRef] [PubMed]
- Vera San Juan, N.; Aceituno, D.; Djellouli, N.; Sumray, K.; Regenold, N.; Syversen, A.; Vindrola-Padros, C. Mental health and well-being of healthcare workers during the COVID-19 pandemic in the UK: Contrasting guidelines with experiences in practice. BJPsych Open 2021, 7, E15. [Google Scholar] [CrossRef] [PubMed]
- Ferry, A.V.; Wereski, R.; Strachan, E.E.; Mills, N.L. Predictors of healthcare worker burnout during the COVID-19 pandemic. medRxiv 2020. [Google Scholar] [CrossRef]
- Tomlin, J.; Dalgleish-Warburton, B. Lamph, Psychosocial Support for Healthcare Workers during the COVID-19 Pandemic. Front. Psychol. 2020, 11, 1960. [Google Scholar] [CrossRef] [PubMed]
- Balasubramanian, A.; Paleri, V.; Bennett, R.; Paleri, V. Impact of COVID-19 on the mental health of surgeons and coping strategies. Head Neck 2020, 42, 1638–1644. [Google Scholar] [CrossRef]
- Albott, C.S.; Wozniak, J.R.; McGlinch, B.P.; Wall, M.H.; Gold, B.S.; Vinogradov, S. Battle Buddies: Rapid Deployment of a Psychological Resilience Intervention for Health Care Workers During the COVID-19 Pandemic. Anesth. Analg. 2020, 131, 43–54. [Google Scholar] [CrossRef]
- Duarte, M.D.L.C.; Silva, D.G.D.; Bagatini, M.M.C. Nursing and mental health: A reflection in the midst of the coronavirus pandemic. Scielo Prepr. 2020. [Google Scholar] [CrossRef]
- Orrù, G.; Marzetti, F.; Conversano, C.; Vagheggini, G.; Miccoli, M.; Ciacchini, R.; Panait, E.; Gemignani, A. Secondary Traumatic Stress and Burnout in Healthcare Workers during COVID-19 Outbreak. Int. J. Environ. Res. Public Health 2021, 18, 337. [Google Scholar] [CrossRef]
- Hossain, F.; Clatty, A. Self-care strategies in response to nurses’ moral injury during COVID-19 pandemic. Nurs. Ethics 2020, 30, 0969733020961825. [Google Scholar] [CrossRef] [PubMed]
- Frawley, T.; van Gelderen, F.; Somanadhan, S.; Coveney, K.; Phelan, A.; Lynam-Loane, P.; De Brún, A. The impact of COVID-19 on health systems, mental health and the potential for nursing. Irish J. Psychol. Med. 2020, 16, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Zaka, A.; Shamloo, S.E.; Fiorente, P.; Tafuri, A. COVID-19 pandemic as a watershed moment: A call for systematic psychological health care for frontline medical staff. J. Health Psychol. 2020, 25, 883–887. [Google Scholar] [CrossRef]
- Horsch, A.; Lalor, J.; Downe, S. Moral and Mental Health Challenges Faced by Maternity Staff during the Covid-19 Pandemic. Psychol. Trauma 2020, 12 (Suppl. 1), 141–142. [Google Scholar] [CrossRef]
- Fontana, M.; McCauley, L.; Fitzgerald, M.; Eckert, G.J.; Yanca, E.; Eber, R. Impact of COVID-19 on Life Experiences of Essential Workers Attending a Dental Testing Facility. JDR Clin. Transl. Res. 2020, 6, 24–39. [Google Scholar] [CrossRef]
- Mahendran, K.; Patel, S.; Sproat, C. Psychosocial effects of the COVID-19 pandemic on staff in a dental teaching hospital. Br. Dent. J. 2020, 229, 127–132. [Google Scholar] [CrossRef]
- Milgrom, Y.; Tal, Y.; Finestone, A.S. Comparison of hospital worker anxiety in COVID-19 treating and non-treating hospitals in the same city during the COVID-19 pandemic. Isr. J. Health Policy Res. 2020, 9, 55. [Google Scholar] [CrossRef]
- Nanjundaswamy, M.H.; Pathak, H.; Chaturvedi, S.K. Perceived stress and anxiety during COVID-19 among psychiatry trainees. Asian J. Psychiatry 2020, 54, 102282. [Google Scholar] [CrossRef] [PubMed]
- Hayden, J.C.; Parkin, R. The challenges of COVID-19 for community pharmacists and opportunities for the future. Ir. J. Psychol. Med. 2020, 37, 198–203. [Google Scholar] [CrossRef]
- Eurofound. Work Organisation. Available online: https://www.eurofound.europa.eu/topic/work-organisation#:~:text=Work%20organisation%20is%20about%20the,Read%20more (accessed on 26 January 2021).
- Williams, R.; Murray, E.; Neal, A.; Kemp, M.V. Top Ten Messages for Supporting Healthcare Staff During the COVID-19 Pandemic. Royal College of Psychiatrists, 2020. Available online: https://www.rcpsych.ac.uk/docs/default-source/about-us/covid-19/top-ten-messages-williams-et-al.pdf?sfvrsn=990e3861_0 (accessed on 26 January 2021).
- Rodríguez, B.O.; Sánchez, T.L. The Psychosocial Impact of COVID-19 on health care workers. Int. Braz. J. Urol. 2020, 46 (Suppl. 1), 195–200. [Google Scholar] [CrossRef]
- Alizadeh, A.; Khankeh, H.R.; Barati, M.; Ahmadi, Y.; Hadian, A.; Azizi, M. Psychological distress among Iranian health-care providers exposed to coronavirus disease 2019 (COVID-19): A qualitative study. BMC Psychiatry 2020, 20, 494. [Google Scholar] [CrossRef] [PubMed]
- Ripp, J.; Peccoralo, L.; Charney, D. Attending to the Emotional Well-Being of the Health Care Workforce in a New York City Health System during the COVID-19 Pandemic. Acad. Med. 2020, 95, 1136–1139. [Google Scholar] [CrossRef] [PubMed]
- Shanafelt, T.; Ripp, J.; Trockel, M. Understanding and Addressing Sources of Anxiety among Health Care Professionals during the COVID-19 Pandemic. JAMA 2020, 323, 2133–2134. [Google Scholar] [CrossRef] [PubMed]
- Miotto, K.; Sanford, J.; Brymer, M.J.; Bursch, B.; Pynoos, R.S. Implementing an emotional support and mental health response plan for healthcare workers during the COVID-19 pandemic. Psychol. Trauma Theory Res. Pract. Policy 2020, 12, 165–167. [Google Scholar] [CrossRef] [PubMed]
- Bansal, P.; Bingemann, T.A.; Greenhawt, M.; Mosnaim, G.; Nanda, A.; Oppenheimer, J.; Sharma, H.; Stukus, D.; Shaker, M. Clinician Wellness during the COVID-19 Pandemic: Extraordinary Times and Unusual Challenges for the Allergist/Immunologist. J. Allergy Clin. Immunol. Pract. 2020, 8, 1781–1790. [Google Scholar] [CrossRef] [PubMed]
- Gautam, M.; Kaur, M.; Mahr, G. COVID-19-Associated Psychiatric Symptoms in Health Care Workers: Viewpoint From Internal Medicine and Psychiatry Residents. Psychosomatics 2020, 61, 579–581. [Google Scholar] [CrossRef]
- Moraveji, S.; Thaker, A.M.; Muthusamy, V.R.; Banerjee, S. Protocols, Personal Protective Equipment Use, and Psychological/Financial Stressors in Endoscopy Units during the COVID-19 Pandemic: A Large Survey of Hospital-Based and Ambulatory Endoscopy Centers in the United States. Gatroenterology 2020, 159, 1568–1570. [Google Scholar] [CrossRef]
- Owens, I.T. Supporting nurses’ mental health during the pandemic. Nursing 2020, 50, 54–57. [Google Scholar] [CrossRef]
- Maben, J.; Bridges, J. Covid-19: Supporting nurses’ psychological and mental health. JCN J. Clin. Nurs. 2020, 29, 2742–2750. [Google Scholar] [CrossRef] [PubMed]
- Poonian, J.; Walsham, N.; Kilner, T.; Bradbury, E.; Brooks, K.; West, E. Managing healthcare worker well-being in an Australian emergency department during the COVID-19 pandemic. Emerg. Med. Australas. 2020, 32, 700–702. [Google Scholar] [CrossRef] [PubMed]
- Bender, W.R.; Srinivas, S.; Coutifaris, P.; Acker, A.; Hirshberg, A. The Psychological Experience of Obstetric Patients and Health Care Workers after Implementation of Universal SARS-CoV-2 Testing. Am. J. Perinatol. 2020, 37, 1271–1279. [Google Scholar] [CrossRef] [PubMed]
- Wei, E.; Segall, J.; Villanueva, Y.; Dang, L.B.; Gasca, V.I.; Gonzalez, M.P.; Roman, M.; Mendez-Justiniano, I.; Cohen, A.G.; Cho, H.J. Coping with Trauma, Celebrating Life: Reinventing Patient And Staff Support During The COVID-19 Pandemic. Health Aff. (Millwood) 2020, 39, 1597–1600. [Google Scholar] [CrossRef] [PubMed]
- Giorgi, G.; Lecca, L.I.; Alessio, F.; Finstad, G.L.; Bondanini, G.; Lulli, L.G.; Arcangeli, G.; Mucci, N. COVID-19-Related Mental Health Effects in the Workplace: A Narrative Review. Int. J. Environ. Res. Public Health 2020, 17, 7857. [Google Scholar] [CrossRef] [PubMed]
- Evanoff, B.A.; Strickland, J.R.; Dale, A.M.; Hayibor, L.; Page, E.; Duncan, J.G.; Kannampallil, T.; Gray, D.L. Work-Related and Personal Factors Associated with Mental Well-Being During the COVID-19 Response: Survey of Health Care and Other Workers. J. Med. Internet Res. 2020, 22, e21366. [Google Scholar] [CrossRef]
- Ananda-Rajah, M.; Veness, B.; Berkovic, D.; Parker, C.; Kelly, G.; Ayton, D. Hearing the voices of Australian healthcare workers during the COVID-19 pandemic. medRxiv 2020. [Google Scholar] [CrossRef]
- Ahmed, F.; Zhao, F.; Faraz, N.A. How and When Does Inclusive Leadership Curb Psychological Distress During a Crisis? Evidence from the COVID-19 Outbreak. Front. Psychol. 2020, 11, 1898. [Google Scholar] [CrossRef] [PubMed]
- Walton, M.; Murray, E.; Christian, M.D. Mental health care for medical staff and affiliated healthcare workers during the COVID-19 pandemic. Eur. Heart J. Acute Cardiovasc. Care 2020, 9, 241–247. [Google Scholar] [CrossRef] [PubMed]
- Heath, C.; Sommerfield, A.; von Ungern-Sternberg, B.S. Resilience strategies to manage psychological distress among healthcare workers during the COVID-19 pandemic: A narrative review. Anaesthesia 2020, 75, 1364–1371. [Google Scholar] [CrossRef]
- Fawaz, M.; Anshasi, H.; Samaha, A. Nurses at the Front Line of COVID-19: Roles, Responsibilities, Risks, and Rights. Am. J. Trop. Med. Hyg. 2020, 103, 1341–1342. [Google Scholar] [CrossRef] [PubMed]
- Chersich, M.F.; Gray, G.; Fairlie, L.; Eichbaum, Q.; Mayhew, S.; Allwood, B.; Rees, H. COVID-19 in Africa: Care and protection for frontline healthcare workers. Glob. Health 2020, 16, 46. [Google Scholar] [CrossRef] [PubMed]
- Datta, S.S.; Mukherjee, A.; Ghose, S.; Bhattacharya, S.; Gyawali, B. Addressing the Mental Health Challenges of Cancer Care Workers in LMICs During the Time of the COVID-19 Pandemic. JCO Glob. Oncol. 2020, 6, 1490–1493. [Google Scholar] [CrossRef] [PubMed]
- Derksen, C.; Keller, F.M.; Lippke, S. Obstetric Healthcare Workers’ Adherence to Hand Hygiene Recommendations during the COVID-19 Pandemic: Observations and Social-Cognitive Determinants. Appl. Psychol. Health Well-Being 2020, 12, 1286–1305. [Google Scholar] [CrossRef]
- Taylor, W.D.; Blackford, J.U. Mental Health Treatment for Front-Line Clinicians During and After the Coronavirus Disease 2019 (COVID-19) Pandemic: A Plea to the Medical Community. Ann. Intern. Med. 2020, 173, 574–575. [Google Scholar] [CrossRef]
- Verger, P.; Scronias, D.; Dauby, N.; Adedzi Kodzo Awoenam, N.; Gobert, C.; Bergeat, M.; Gagneur, A.; Dubé, E. Attitudes of healthcare workers towards COVID-19 vaccination: A survey in France and French-speaking parts of Belgium and Canada, 2020. Euro Surveill. 2021, 26, 2002047. [Google Scholar] [CrossRef]
- Houghton, C.; Meskell, P.; Delaney, H.; Smalle, M.; Glenton, C.; Booth, A.; Chan, X.H.S.; Devane, D.; Biesty, L.M. Barriers and facilitators to healthcare workers’ adherence with infection prevention and control (IPC) guidelines for respiratory infectious diseases: A rapid qualitative evidence synthesis. Cochrane Database Syst. Rev. 2020. [Google Scholar] [CrossRef]
- Shallcross, L.; Burke, D.; Abbott, O.; Donaldson, A.; Hallatt, G.; Hayward, A.; Hopkins, S.; Krutikov, M.; Sharp, K.; Wardman, L.; et al. Factors associated with SARS-CoV-2 infection and outbreaks in long-term care facilities in England: A national cross-sectional survey. Lancet Healthy Longev. 2021. [Google Scholar] [CrossRef]
- Romeyke, T.; Noehammer, E.; Stummer, H. COVID-19 Patient with Severe Comorbidity in Multimodal Acute Care Setting with Non-Invasive Medical Ventilation: A Clinical Outcome Report. Clin. Pract. 2021, 11, 81–91. [Google Scholar] [CrossRef] [PubMed]
- Sampaio, F.; Sequeira, C.; Teixeira, L. Impact of COVID-19 outbreak on nurses’ mental health: A prospective cohort study. Environ. Res. 2021, 194, 110620. [Google Scholar] [CrossRef] [PubMed]
| Characteristic | Categories | N | (%) |
|---|---|---|---|
| Settings | Hospitals & Medical Centres | 101 | 45.9 |
| Multiple Settings | 14 | 6.3 | |
| Community Settings | 7 | 3.2 | |
| Primary Care | 2 | 1 | |
| Psychiatry facilities | 2 | 1 | |
| Geriatric facilities | 1 | 0.4 | |
| Testing Clinic | 1 | 0.4 | |
| University | 1 | 0.4 | |
| Not specified | 91 | 41.4 | |
| Occupations | Medical HCW | 63 | 28.7 |
| Nurses | 29 | 13.3 | |
| Doctors | 11 | 5 | |
| Medical & Non-Medical HCW | 30 | 13.8 | |
| Pharmacists | 2 | 1 | |
| Dentists | 2 | 1 | |
| Surgeons | 2 | 1 | |
| Residents | 1 | 0.4 | |
| Paramedics | 1 | 0.4 | |
| Students | 1 | 0.4 | |
| Caregivers | 1 | 0.4 | |
| Not specified | 76 | 34.6 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Franklin, P.; Gkiouleka, A. A Scoping Review of Psychosocial Risks to Health Workers during the Covid-19 Pandemic. Int. J. Environ. Res. Public Health 2021, 18, 2453. https://doi.org/10.3390/ijerph18052453
Franklin P, Gkiouleka A. A Scoping Review of Psychosocial Risks to Health Workers during the Covid-19 Pandemic. International Journal of Environmental Research and Public Health. 2021; 18(5):2453. https://doi.org/10.3390/ijerph18052453
Chicago/Turabian StyleFranklin, Paula, and Anna Gkiouleka. 2021. "A Scoping Review of Psychosocial Risks to Health Workers during the Covid-19 Pandemic" International Journal of Environmental Research and Public Health 18, no. 5: 2453. https://doi.org/10.3390/ijerph18052453
APA StyleFranklin, P., & Gkiouleka, A. (2021). A Scoping Review of Psychosocial Risks to Health Workers during the Covid-19 Pandemic. International Journal of Environmental Research and Public Health, 18(5), 2453. https://doi.org/10.3390/ijerph18052453





