Prevalence and Determinants of Fatigue after COVID-19 in Non-Hospitalized Subjects: A Population-Based Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Population
2.2. Mixed-Mode Survey and Questionnaire
2.3. Assessment of Fatigue
2.4. Assessment of Comorbidity and COVID-19 Symptoms
2.5. Statistical Analysis
3. Results
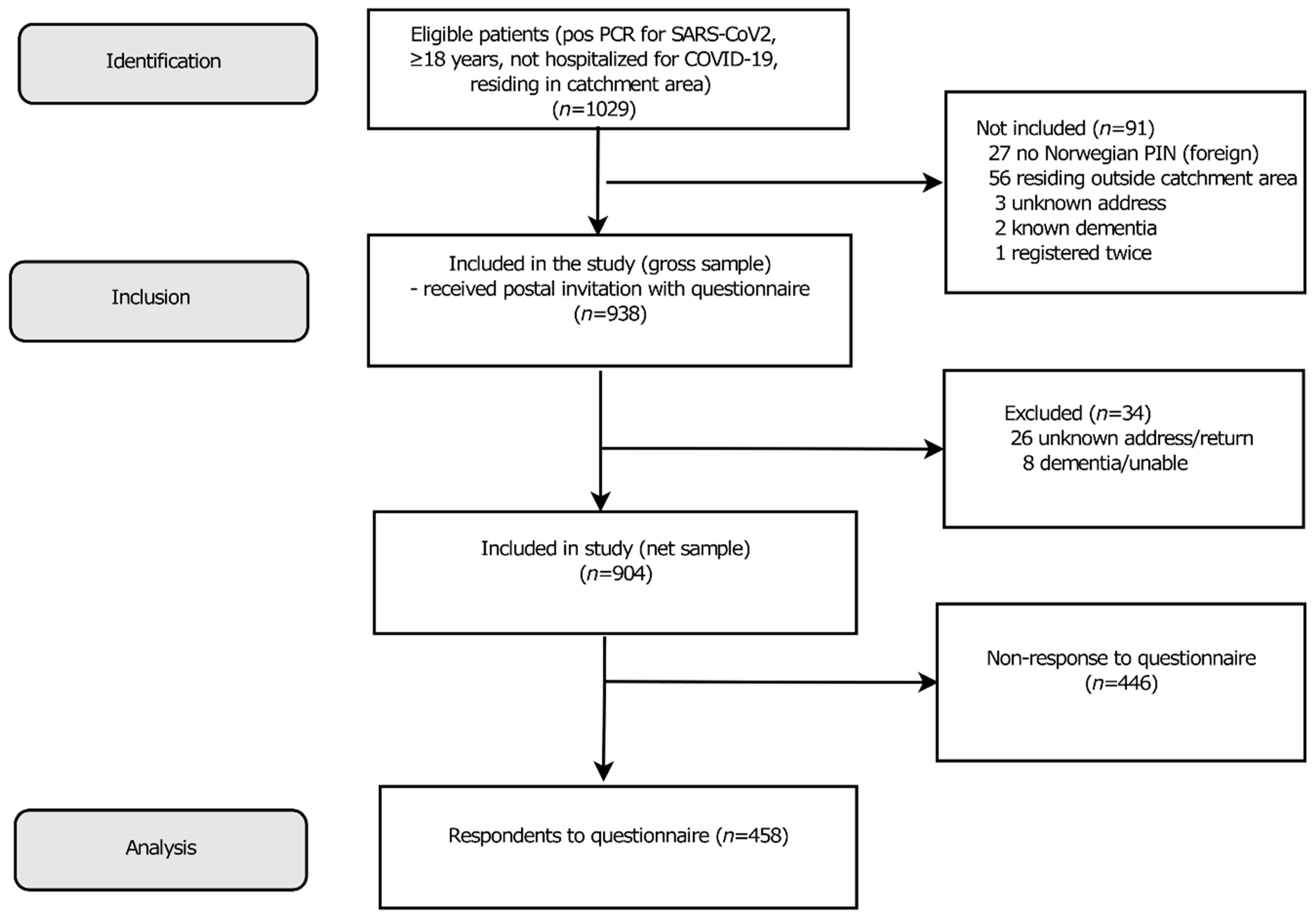
3.1. Study Population
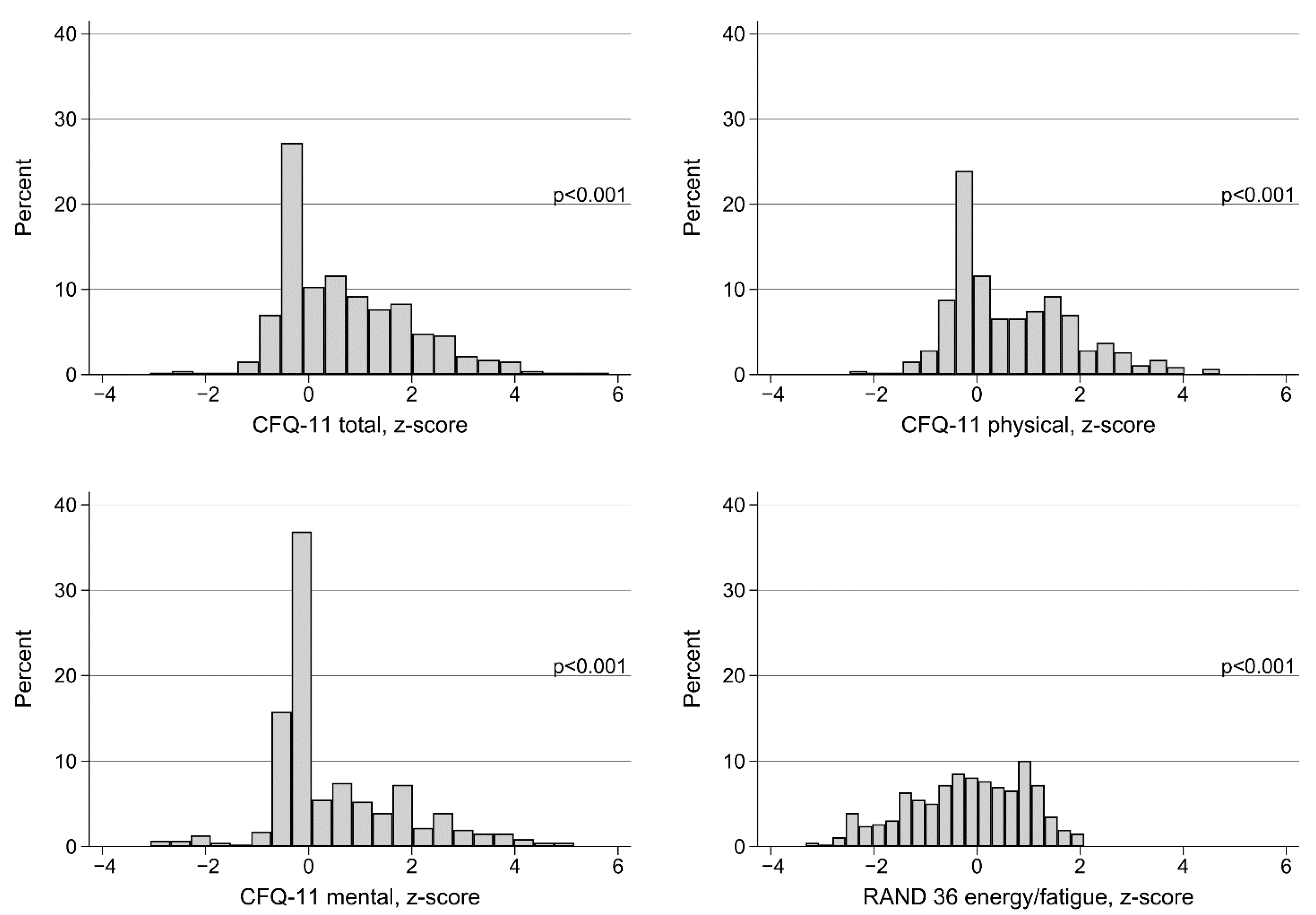
3.2. Prevalence and Symptoms of Fatigue
3.3. Determinants of Fatigue
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Huang, C.; Wang, Y.; Li, X.; Ren, L.; Zhao, J.; Hu, Y.; Zhang, L.; Fan, G.; Xu, J.; Gu, X.; et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet 2020, 395, 497–506. [Google Scholar] [CrossRef]
- Docherty, A.B.; Harrison, E.M.; Green, C.A.; Hardwick, H.E.; Pius, R.; Norman, L.; Holden, K.A.; Read, J.M.; Dondelinger, F.; Carson, G.; et al. Features of 20 133 UK patients in hospital with covid-19 using the ISARIC WHO Clinical Characterisation Protocol: Prospective observational cohort study. BMJ 2020, 369, m1985. [Google Scholar] [CrossRef] [PubMed]
- Salit, I.E. Post-infectious fatigue. Can. Fam. Physician 1987, 33, 1217–1219. [Google Scholar]
- Hickie, I.; Davenport, T.; Wakefield, D.; Vollmer-Conna, U.; Cameron, B.; Vernon, S.D.; Reeves, W.C.; Lloyd, A.; Dubbo Infection Outcomes Study Group. Post-infective and chronic fatigue syndromes precipitated by viral and non-viral pathogens: Prospective cohort study. BMJ 2006, 333, 575. [Google Scholar] [CrossRef]
- Tansey, C.M.; Louie, M.; Loeb, M.; Gold, W.L.; Muller, M.P.; de Jager, J.; Cameron, J.I.; Tomlinson, G.; Mazzulli, T.; Walmsley, S.L.; et al. One-year outcomes and health care utilization in survivors of severe acute respiratory syndrome. Arch. Intern. Med. 2007, 167, 1312–1320. [Google Scholar] [CrossRef] [PubMed]
- O’Sullivan, O. Long-term sequelae following previous coronavirus epidemics. Clin. Med. 2021, 21, e68–e70. [Google Scholar] [CrossRef]
- Lee, S.H.; Shin, H.S.; Park, H.Y.; Kim, J.L.; Lee, J.J.; Lee, H.; Won, S.D.; Han, W. Depression as a Mediator of Chronic Fatigue and Post-Traumatic Stress Symptoms in Middle East Respiratory Syndrome Survivors. Psychiatry Investig. 2019, 16, 59–64. [Google Scholar] [CrossRef]
- Mahase, E. Covid-19: What do we know about “long covid”? BMJ 2020, 370. [Google Scholar] [CrossRef]
- Yelin, D.; Wirtheim, E.; Vetter, P.; Kalil, A.C.; Bruchfeld, J.; Runold, M.; Guaraldi, G.; Mussini, C.; Gudiol, C.; Pujol, M.; et al. Long-term consequences of COVID-19: Research needs. Lancet Infect. Dis. 2020, 20, 1115–1117. [Google Scholar] [CrossRef]
- Wilson, C. Concern coronavirus may trigger post-viral fatigue syndromes. New Sci. 2020, 246, 10–11. [Google Scholar] [CrossRef]
- Marshall, M. The lasting misery of coronavirus long-haulers. Nature 2020, 585, 339–341. [Google Scholar] [CrossRef]
- Halpin, S.J.; McIvor, C.; Whyatt, G.; Adams, A.; Harvey, O.; McLean, L.; Walshaw, C.; Kemp, S.; Corrado, J.; Singh, R.; et al. Postdischarge symptoms and rehabilitation needs in survivors of COVID-19 infection: A cross-sectional evaluation. J. Med. Virol. 2020. [Google Scholar] [CrossRef]
- Carfi, A.; Bernabei, R.; Landi, F.; Gemelli Against, C.-P.-A.C.S.G. Persistent Symptoms in Patients After Acute COVID-19. JAMA 2020, 324, 603–605. [Google Scholar] [CrossRef] [PubMed]
- Liang, L.; Yang, B.; Jiang, N.; Fu, W.; He, X.; Zhou, Y.; Ma, W.L.; Wang, X. Three-month Follow-up Study of Survivors of Coronavirus Disease 2019 after Discharge. J. Korean Med. Sci. 2020, 35, e418. [Google Scholar] [CrossRef]
- Burke, R.M.; Killerby, M.E.; Newton, S.; Ashworth, C.E.; Berns, A.L.; Brennan, S.; Bressler, J.M.; Bye, E.; Crawford, R.; Harduar Morano, L.; et al. Symptom Profiles of a Convenience Sample of Patients with COVID-19—United States, January–April 2020. MMWR Morb. Mortal. Wkly. Rep. 2020, 69, 904–908. [Google Scholar] [CrossRef]
- Petersen, M.S.; Kristiansen, M.F.; Hanusson, K.D.; Danielsen, M.E.; Gaini, S.; Strom, M.; Weihe, P. Long COVID in the Faroe Islands—A longitudinal study among non-hospitalized patients. Clin. Infect. Dis. 2020. [Google Scholar] [CrossRef]
- Townsend, L.; Dyer, A.H.; Jones, K.; Dunne, J.; Mooney, A.; Gaffney, F.; O’Connor, L.; Leavy, D.; O’Brien, K.; Dowds, J.; et al. Persistent fatigue following SARS-CoV-2 infection is common and independent of severity of initial infection. PLoS ONE 2020, 15, e0240784. [Google Scholar] [CrossRef] [PubMed]
- Chalder, T.; Berelowitz, G.; Pawlikowska, T.; Watts, L.; Wessely, S.; Wright, D.; Wallace, E.P. Development of a fatigue scale. J. Psychosom. Res. 1993, 37, 147–153. [Google Scholar] [CrossRef]
- Stavem, K.; Ghanima, W.; Olsen, M.K.; Gilboe, H.M.; Einvik, G. Persistent symptoms 1.5-6 months after COVID-19 in non-hospitalised subjects: A population-based cohort study. Thorax 2020. [Google Scholar] [CrossRef]
- Loge, J.H.; Ekeberg, O.; Kaasa, S. Fatigue in the general Norwegian population: Normative data and associations. J. Psychosom. Res. 1998, 45, 53–65. [Google Scholar] [CrossRef]
- Hays, R.D.; Sherbourne, C.D.; Mazel, R.M. The RAND 36-Item Health Survey 1.0. Health Econ. 1993, 2, 217–227. [Google Scholar] [CrossRef] [PubMed]
- Brown, L.F.; Kroenke, K.; Theobald, D.E.; Wu, J. Comparison of SF-36 vitality scale and Fatigue Symptom Inventory in assessing cancer-related fatigue. Support. Care Cancer 2011, 19, 1255–1259. [Google Scholar] [CrossRef] [PubMed]
- Katz, J.N.; Chang, L.C.; Sangha, O.; Fossel, A.H.; Bates, D.W. Can comorbidity be measured by questionnaire rather than medical record review? Med. Care 1996, 34, 73–84. [Google Scholar] [CrossRef] [PubMed]
- Charlson, M.E.; Pompei, P.; Ales, K.L.; MacKenzie, C.R. A new method of classifying prognostic comorbidity in longitudinal studies: Development and validation. J. Chronic. Dis 1987, 40, 373–383. [Google Scholar] [CrossRef]
- Pawlikowska, T.; Chalder, T.; Hirsch, S.R.; Wallace, P.; Wright, D.J.; Wessely, S.C. Population based study of fatigue and psychological distress. BMJ 1994, 308, 763–766. [Google Scholar] [CrossRef]
- Garratt, A.M.; Stavem, K. Measurement properties and normative data for the Norwegian SF-36: Results from a general population survey. Health Qual. Life Outcomes 2017, 15, 51. [Google Scholar] [CrossRef]
- Rudroff, T.; Fietsam, A.C.; Deters, J.R.; Bryant, A.D.; Kamholz, J. Post-COVID-19 Fatigue: Potential Contributing Factors. Brain Sci. 2020, 10, 1012. [Google Scholar] [CrossRef]
- David, A.; Pelosi, A.; McDonald, E.; Stephens, D.; Ledger, D.; Rathbone, R.; Mann, A. Tired, weak, or in need of rest: Fatigue among general practice attenders. BMJ 1990, 301, 1199–1202. [Google Scholar] [CrossRef]
- Krogstad, H.; Loge, J.H.; Grotmol, K.S.; Kaasa, S.; Kiserud, C.E.; Salvesen, O.; Hjermstad, M.J. Symptoms in the general Norwegian adult population—Prevalence and associated factors. BMC Public Health 2020, 20, 988. [Google Scholar] [CrossRef] [PubMed]
- Whitehead, L. The measurement of fatigue in chronic illness: A systematic review of unidimensional and multidimensional fatigue measures. J. Pain Symptom Manag. 2009, 37, 107–128. [Google Scholar] [CrossRef]
- Tenforde, M.W.; Kim, S.S.; Lindsell, C.J.; Billig Rose, E.; Shapiro, N.I.; Files, D.C.; Gibbs, K.W.; Erickson, H.L.; Steingrub, J.S.; Smithline, H.A.; et al. Symptom Duration and Risk Factors for Delayed Return to Usual Health Among Outpatients with COVID-19 in a Multistate Health Care Systems Network—United States, March–June 2020. MMWR Morb. Mortal. Wkly. Rep. 2020, 69, 993–998. [Google Scholar] [CrossRef] [PubMed]
- Goertz, Y.M.J.; Van Herck, M.; Delbressine, J.M.; Vaes, A.W.; Meys, R.; Machado, F.V.C.; Houben-Wilke, S.; Burtin, C.; Posthuma, R.; Franssen, F.M.E.; et al. Persistent symptoms 3 months after a SARS-CoV-2 infection: The post-COVID-19 syndrome? ERJ Open Res. 2020, 6, 00542-2020. [Google Scholar] [CrossRef] [PubMed]
- Qi, R.; Chen, W.; Liu, S.; Thompson, P.M.; Zhang, L.J.; Xia, F.; Cheng, F.; Hong, A.; Surento, W.; Luo, S.; et al. Psychological morbidities and fatigue in patients with confirmed COVID-19 during disease outbreak: Prevalence and associated biopsychosocial risk factors. medRxiv 2020. [Google Scholar] [CrossRef]
- van den Borst, B.; Peters, J.B.; Brink, M.; Schoon, Y.; Bleeker-Rovers, C.P.; Schers, H.; van Hees, H.W.H.; van Helvoort, H.; van den Boogaard, M.; van der Hoeven, H.; et al. Comprehensive health assessment three months after recovery from acute COVID-19. Clin. Infect. Dis. 2020. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.; Xu, H.; Jiang, H.; Wang, L.; Lu, C.; Wei, X.; Liu, J.; Xu, S. Clinical features and outcomes of discharged coronavirus disease 2019 patients: A prospective cohort study. QJM 2020, 113, 657–665. [Google Scholar] [CrossRef]
- Metlay, J.P.; Fine, M.J.; Schulz, R.; Marrie, T.J.; Coley, C.M.; Kapoor, W.N.; Singer, D.E. Measuring symptomatic and functional recovery in patients with community-acquired pneumonia. J. Gen. Intern. Med. 1997, 12, 423–430. [Google Scholar] [CrossRef]
- Lam, S.P.; Tsui, E.; Chan, K.S.; Lam, C.L.; So, H.P. The validity and reliability of the functional impairment checklist (FIC) in the evaluation of functional consequences of severe acute respiratory distress syndrome (SARS). Qual. Life Res. 2006, 15, 217–231. [Google Scholar] [CrossRef] [PubMed]
- Ahmed, H.; Patel, K.; Greenwood, D.C.; Halpin, S.; Lewthwaite, P.; Salawu, A.; Eyre, L.; Breen, A.; O’Connor, R.; Jones, A.; et al. Long-term clinical outcomes in survivors of severe acute respiratory syndrome and Middle East respiratory syndrome coronavirus outbreaks after hospitalisation or ICU admission: A systematic review and meta-analysis. J. Rehabil. Med. 2020, 52, jrm00063. [Google Scholar] [CrossRef]
- Lam, M.H.; Wing, Y.K.; Yu, M.W.; Leung, C.M.; Ma, R.C.; Kong, A.P.; So, W.Y.; Fong, S.Y.; Lam, S.P. Mental morbidities and chronic fatigue in severe acute respiratory syndrome survivors: Long-term follow-up. Arch. Intern. Med. 2009, 169, 2142–2147. [Google Scholar] [CrossRef]
- Abrahamsen, R.; Svendsen, M.V.; Henneberger, P.K.; Gundersen, G.F.; Torén, K.; Kongerud, J.; Fell, A.K. Non-response in a cross-sectional study of respiratory health in Norway. BMJ Open 2016, 6, e009912. [Google Scholar] [CrossRef]
- Galea, S.; Tracy, M. Participation rates in epidemiologic studies. Ann. Epidemiol. 2007, 17, 643–653. [Google Scholar] [CrossRef] [PubMed]
- Guo, Y.; Kopec, J.A.; Cibere, J.; Li, L.C.; Goldsmith, C.H. Population Survey Features and Response Rates: A Randomized Experiment. Am. J. Public Health 2016, 106, 1422–1426. [Google Scholar] [CrossRef]
- Harrison, S.; Alderdice, F.; Henderson, J.; Redshaw, M.; Quigley, M.A. Trends in response rates and respondent characteristics in five National Maternity Surveys in England during 1995-2018. Arch. Public Health 2020, 78, 46. [Google Scholar] [CrossRef] [PubMed]
- Blumenberg, C.; Barros, A.J.D. Response rate differences between web and alternative data collection methods for public health research: A systematic review of the literature. Int. J. Public Health 2018, 63, 765–773. [Google Scholar] [CrossRef]
- Karatzias, T.; Shevlin, M.; Murphy, J.; McBride, O.; Ben-Ezra, M.; Bentall, R.P.; Vallieres, F.; Hyland, P. Posttraumatic Stress Symptoms and Associated Comorbidity During the COVID-19 Pandemic in Ireland: A Population-Based Study. J. Trauma Stress 2020, 33, 365–370. [Google Scholar] [CrossRef] [PubMed]
- Ozamiz-Etxebarria, N.; Dosil-Santamaria, M.; Picaza-Gorrochategui, M.; Idoiaga-Mondragon, N. Stress, anxiety, and depression levels in the initial stage of the COVID-19 outbreak in a population sample in the northern Spain. Cad. Saude Publica 2020, 36, e00054020. [Google Scholar] [CrossRef]
- Krishnamoorthy, Y.; Nagarajan, R.; Saya, G.K.; Menon, V. Prevalence of psychological morbidities among general population, healthcare workers and COVID-19 patients amidst the COVID-19 pandemic: A systematic review and meta-analysis. Psychiatry Res. 2020, 293, 113382. [Google Scholar] [CrossRef]
- Shevlin, M.; Nolan, E.; Owczarek, M.; McBride, O.; Murphy, J.; Gibson Miller, J.; Hartman, T.K.; Levita, L.; Mason, L.; Martinez, A.P.; et al. COVID-19-related anxiety predicts somatic symptoms in the UK population. Br. J. Health Psychol. 2020, 25, 875–882. [Google Scholar] [CrossRef] [PubMed]
- Elia, F.; Vallelonga, F. “Pandemic fatigue” or something worse? Recenti Prog. Med. 2020, 111, 788–789. [Google Scholar] [CrossRef]
| Age, Mean (Range) | 49.6 (17.7 to 87.9) |
| Sex, female | 256 (56) |
| Marital status | |
| Single/divorced/separated/widowed | 121 (26) |
| Married/cohabiting | 336 (74) |
| Born in Norway (n = 457) | 382 (84) |
| Norwegian mother tongue (n = 455) | 382 (84) |
| Both parents born in Norway (n = 434) | 357 (78) |
| Highest attainted education | |
| Primary school | 41 (9) |
| Secondary school | 174 (38) |
| University | 243 (53) |
| Smoking status (n = 453) | |
| Never smoker | 298 (66) |
| Former/current smoker | 155 (34) |
| Body mass index (kg/m2) (n = 450) | 26.8 (5.2) |
| Influenza vaccination 2nd half of 2019 (n = 456) | 141(31) |
| No. of 21 comorbidities, categorized | |
| 0 | 234 (51) |
| 1 | 129 (28) |
| ≥2 | 95 (21) |
| Diabetes | 16 (3) |
| Pulmonary disease (asthma, COPD, other) | 60 (13) |
| Depression | 30 (7) |
| Cardiovascular (heart, hypertension, vascular) | 101 (22) |
| Test lab | |
| Akershus University Hospital | 233 (51) |
| Fürst Laboratory | 61 (13) |
| Østfold Hospital | 164 (36) |
| Variable | n | Odds Ratio | 95% Confidence Interval | p |
|---|---|---|---|---|
| Age, per 10 years | 440 | 1.02 | (0.86 to 1.22) | 0.81 |
| Sex | ||||
| Female * | 245 | 1 | ||
| Male | 195 | 0.49 | (0.31 to 0.76) | 0.002 |
| Marital status | ||||
| Single/separated/divorced/widowed * | 112 | 1 | ||
| Married/cohabiting | 328 | 0.56 | (0.34 to 0.92) | 0.022 |
| Highest attained educational level | ||||
| Primary school (≤11years) | 37 | 1 | ||
| Secondary school (12–13 years) | 165 | 1.22 | (0.54 to 2.74) | 0.64 |
| University level | 238 | 1.17 | (0.53 to 2.61) | 0.70 |
| No. of comorbidities (out of 21) | ||||
| 0 * | 223 | 1 | ||
| 1 | 123 | 1.62 | (0.94 to 2.77) | 0.080 |
| ≥2 | 94 | 1.52 | (0.77 to 3.03) | 0.23 |
| Previous depression | ||||
| No * | 412 | 1 | ||
| Yes | 28 | 1.10 | (0.43 to 2.82) | 0.84 |
| No. of COVID-19 symptoms | ||||
| 0–5 * | 101 | 1 | ||
| 6–9 | 168 | 1.44 | (0.79 to 2.64) | 0.24 |
| 10–23 | 171 | 3.66 | (1.88 to 7.11) | <0.001 |
| Dyspnea during COVID-19 | ||||
| No * | 190 | 1 | ||
| Yes | 250 | 1.56 | (0.97 to 2.53) | 0.069 |
| Confusion during COVID-19 | ||||
| No * | 381 | 1 | ||
| Yes | 59 | 2.25 | (1.12 to 4.51) | 0.022 |
| Body mass index, kg/m2 | 440 | 1.03 | (0.99 to 1.08) | 0.13 |
| Smoking status | ||||
| Never smoker * | 291 | 1 | ||
| Former/current smoker | 149 | 1.34 | (0.85 to 2.13) | 0.21 |
| Time since symptom onset, days | ||||
| 41–110 * | 144 | 1 | ||
| 111–127 | 152 | 0.80 | (0.47 to 1.36) | 0.41 |
| 128–200 | 144 | 0.55 | (0.32 to 0.96) | 0.034 |
| Variable | CFQ-11 Total Score (n = 438) | RAND-36 Energy/Fatigue (n = 440) | ||||
|---|---|---|---|---|---|---|
| Coef. | 95% Confidence Interval | p | Coef. | 95% Confidence Interval | p | |
| Age, per 10 years | 0.1 | (−0.24 to 0.44) | 0.56 | 1.51 | (−0.05 to 3.07) | 0.057 |
| Sex | ||||||
| Female * | 0 | 0 | ||||
| Male | −1.78 | (−2.66 to −0.90) | <0.001 | 9.63 | (5.58 to 13.69) | <0.001 |
| Marital status | ||||||
| Single/separated/divorced/widowed * | 0 | 0 | ||||
| Married/cohabiting | −0.84 | (−1.81 to 0.12) | 0.086 | 3.53 | (−0.93 to 7.99) | 0.12 |
| Highest attained educational level | ||||||
| Primary school (≤11 years) | 0 | 0 | ||||
| Secondary school (12–13 years) | 0.03 | (−1.55 to 1.62) | 0.97 | 3.98 | (−3.37 to 11.33) | 0.29 |
| University level | −0.03 | (−1.58 to 1.52) | 0.97 | 4.42 | (−2.77 to 11.62) | 0.23 |
| No. of comorbidities (out of 21) | ||||||
| 0 * | 0 | 0 | ||||
| 1 | 0.48 | (−0.57 to 1.53) | 0.37 | −1.35 | (−6.24 to 3.54) | 0.59 |
| ≥2 | 0.22 | (−1.13 to 1.57) | 0.75 | −6.11 | (−12.35 to 0.14) | 0.055 |
| Previous depression | ||||||
| No * | 0 | 0 | ||||
| Yes | 2.38 | (0.57 to 4.18) | 0.010 | −12.05 | (−20.43 to −3.68) | 0.005 |
| No. of COVID-19 symptoms | ||||||
| 0–5 * | 0 | 0 | ||||
| 6–9 | 0.70 | (−0.44 to 1.85) | 0.23 | −8.28 | (−13.58 to −2.98) | 0.002 |
| 10–23 | 2.68 | (1.38 to 3.99) | <0.001 | −15.59 | (−21.64 to −9.55) | <0.001 |
| Dyspnea during COVID-19 | ||||||
| No * | 0 | 0 | ||||
| Yes | 1.24 | (0.29 to 2.19) | 0.010 | −6.12 | (−10.53 to −1.72) | 0.007 |
| Confusion during COVID-19 | ||||||
| No * | 0 | 0 | ||||
| Yes | 2.65 | (1.34 to 3.97) | <0.001 | −7.35 | (−13.44 to −1.26) | 0.018 |
| Body mass index, kg/m2 | 0.04 | (−0.04 to 0.12) | 0.33 | −0.50 | (−0.88 to −0.12) | 0.010 |
| Smoking status | ||||||
| Never smoker * | 0 | 0 | ||||
| Former/current smoker | 0.66 | (−0.25 to 1.56) | 0.15 | −3.91 | (−8.10 to 0.28) | 0.068 |
| Time since symptom onset, days | ||||||
| 41–110 * | 0 | 0 | ||||
| 111–127 | −0.56 | (−1.60 to 0.47) | 0.28 | 1.38 | (−3.40 to 6.17) | 0.57 |
| 128–200 | −0.41 | (−1.47 to 0.64) | 0.44 | 6.09 | (1.20 to 10.99) | 0.015 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Stavem, K.; Ghanima, W.; Olsen, M.K.; Gilboe, H.M.; Einvik, G. Prevalence and Determinants of Fatigue after COVID-19 in Non-Hospitalized Subjects: A Population-Based Study. Int. J. Environ. Res. Public Health 2021, 18, 2030. https://doi.org/10.3390/ijerph18042030
Stavem K, Ghanima W, Olsen MK, Gilboe HM, Einvik G. Prevalence and Determinants of Fatigue after COVID-19 in Non-Hospitalized Subjects: A Population-Based Study. International Journal of Environmental Research and Public Health. 2021; 18(4):2030. https://doi.org/10.3390/ijerph18042030
Chicago/Turabian StyleStavem, Knut, Waleed Ghanima, Magnus K. Olsen, Hanne M. Gilboe, and Gunnar Einvik. 2021. "Prevalence and Determinants of Fatigue after COVID-19 in Non-Hospitalized Subjects: A Population-Based Study" International Journal of Environmental Research and Public Health 18, no. 4: 2030. https://doi.org/10.3390/ijerph18042030
APA StyleStavem, K., Ghanima, W., Olsen, M. K., Gilboe, H. M., & Einvik, G. (2021). Prevalence and Determinants of Fatigue after COVID-19 in Non-Hospitalized Subjects: A Population-Based Study. International Journal of Environmental Research and Public Health, 18(4), 2030. https://doi.org/10.3390/ijerph18042030






