Effort–Reward Imbalance at Work and Drug Misuse: Evidence from a National Survey in the U.S.
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Population
2.2. Measures
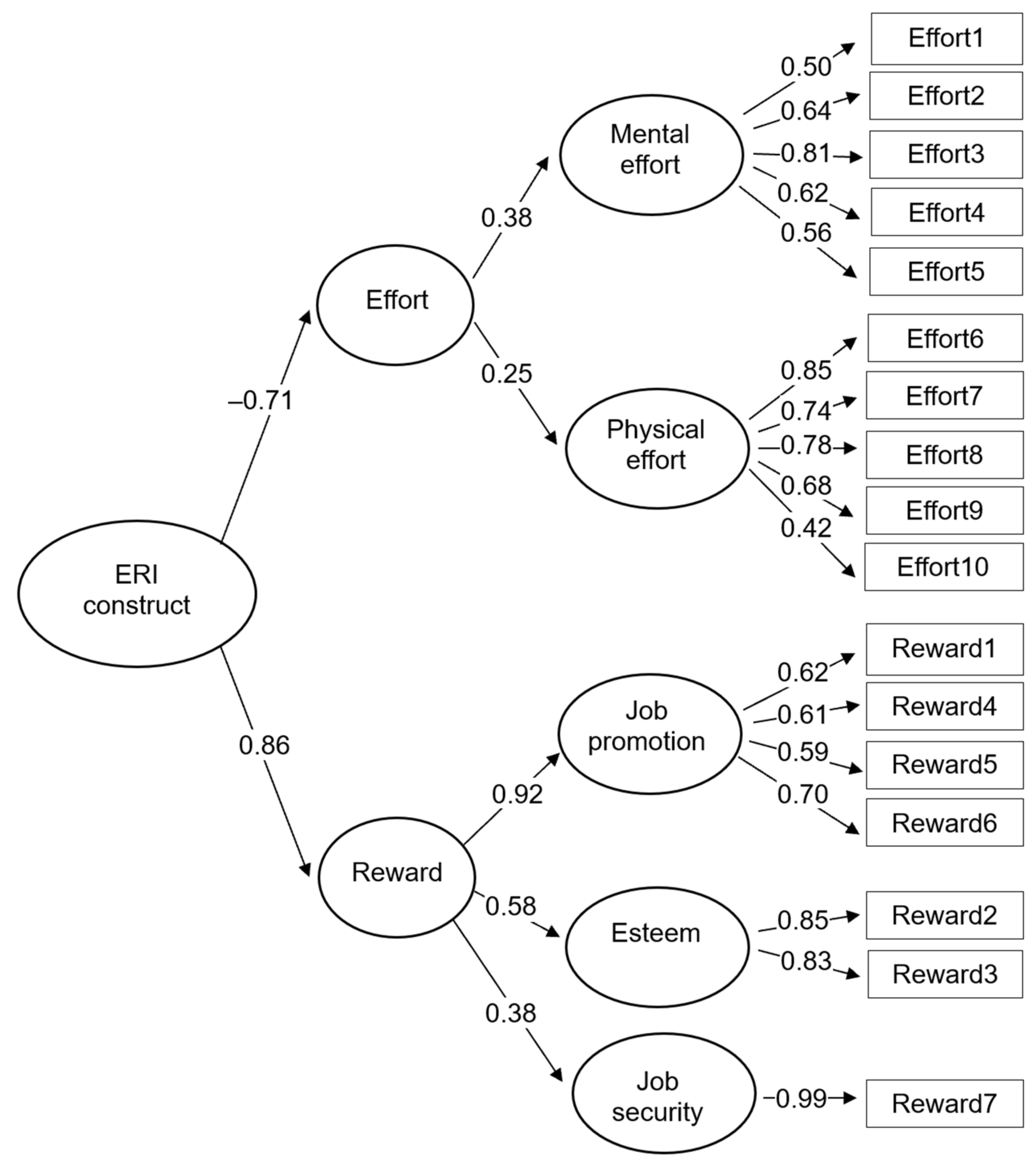
2.3. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
| Effort |
| (1) How often do you have to work very intensively—that is, you are very busy trying to get things done? |
| (2) How often do different people or groups at work demand things from you that you think are hard to combine? |
| (3) How often do you have too many demands made on you? |
| (4) How often do you have enough time to get everything done? |
| (5) How often do you have a lot of interruption? |
| (6) How often does your job require a lot of physical effort? |
| (7) How often does your job require you to lift loads weighing 50 pounds or greater? |
| (8) How often does your job require you to crouch, stoop, or kneel? |
| (9) How often does your job require you to stand for long periods of time? |
| (10) How often does your job require you to use stairs or inclines? |
|
| Reward |
| (1) To what extent do you feel cheated about the chances you have had to work at good jobs? |
| (2) To what extent do you feel a good deal of pride, when you think about the work you do on your job? |
| (3) To what extent do you feel that others respect the work you do on your job? |
| (4) To what extent do you feel that most people have more rewarding jobs than you do? |
| (5) To what extent do you feel that you’ve had opportunities that are as good as most people’s, when it comes to your work life? |
| (6) To what extent do you feel that it makes you discouraged that other people have much better jobs that you do. |
| (7) If you wanted to stay in your present job, what are the chances that you could keep it for the next two years? |
|
References
- Hawkins, D.; Punnett, L.; Davis, L.; Kriebel, D. The contribution of occupation-specific factors to the deaths of despair, Massachusetts, 2005–2015. Ann. Work Expo. Health 2021, 65, 819–832. [Google Scholar] [CrossRef] [PubMed]
- Venkataramani, A.S.; Bair, E.F.; O’Brien, R.L.; Tsai, A.C. Association between automotive assembly plant closures and opioid overdose mortality in the United States: A difference-in-differences analysis. JAMA Intern. Med. 2020, 180, 254–262. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Shaw, W.S.; Roelofs, C.; Punnett, L. Work environment factors and prevention of opioid-related deaths. Am. J. Public Health 2020, 110, 1235–1241. [Google Scholar] [CrossRef] [PubMed]
- Choi, B. Opioid use disorder, job strain, and high physical job demands in US workers. Int. Arch. Occup. Environ. Health 2020, 93, 577–588. [Google Scholar] [CrossRef]
- Kowalski-McGraw, M.; Green-McKenzie, J.; Pandalai, S.P.; Schulte, P.A. Characterizing the interrelationships of prescription opioid and benzodiazepine drugs with worker health and workplace hazards. J. Occup. Environ. Med. 2017, 59, 1114–1126. [Google Scholar] [CrossRef]
- Howard, J.; Osborne, J. Cannabis and work: Need for more research. Am. J. Ind. Med. 2020, 63, 963–972. [Google Scholar] [CrossRef]
- Phillips, J.A.; Holland, M.G.; Baldwin, D.D.; Meuleveld, L.G.; Mueller, K.L.; Perkison, B.; Upfal, M.; Dreger, M. Marijuana in the workplace: Guidance for occupational health professionals and employers: Joint guidance statement of the American Association of Occupational Health Nurses and the American College of Occupational and Environmental Medicine. J. Occup. Environ. Med. 2015, 57, 459–475. [Google Scholar] [CrossRef]
- Hazle, M.C.; Hill, K.P.; Westreich, L.M. Workplace cannabis policies: A moving target. Cannabis Cannabinoid Res. 2020. [Google Scholar] [CrossRef]
- Airagnes, G.; Lemogne, C.; Kab, S.; Hoertel, N.; Goldberg, M.; Wahrendorf, M.; Siegrist, J.; Roquelaure, Y.; Limosin, F.; Zins, M. Effort-reward imbalance and long-term benzodiazepine use: Longitudinal findings from the CONSTANCES cohort. J. Epidemiol. Community Health 2019, 73, 993–1001. [Google Scholar] [CrossRef]
- Giurgiu, D.I.; Jeoffrion, C.; Grasset, B.; Dessomme, B.K.; Moret, L.; Roquelaure, Y.; Caubet, A.; Verger, C.; Laraqui Cel, H.; Lombrail, P.; et al. Psychosocial and occupational risk perception among health care workers: A Moroccan multicenter study. BMC Res. Notes 2015, 8, 408. [Google Scholar] [CrossRef] [Green Version]
- Cooper, R.; Bixler, E.A. Comprehensive workplace policies and practices regarding employee opioid use. New Solut. 2021, 31, 219–228. [Google Scholar] [CrossRef]
- Theorell, T. (Ed.) Handbook of Socioeconomic Determinants of Occupational Health; Springer Nature: Cham, Switzerland, 2020. [Google Scholar]
- Jahoda, M. Reflections on Marienthal and after. J. Occup. Organ. Psych. 1992, 65, 355–358. [Google Scholar] [CrossRef]
- Karasek, R. Job demands, job decision latitude, and mental strain: Implications for job redesign. Adm. Sci. Q. 1979, 24, 285–308. [Google Scholar] [CrossRef]
- Siegrist, J. Adverse health effects of high effort-low reward conditions at work. J. Occup. Health Psychol. 1996, 1, 27–43. [Google Scholar] [CrossRef]
- Henry, J.P.; Stephens, P.M. Stress, Health, and the Social Environment: A Sociobiologic Approach to Medicine; Springer: New York, NY, USA, 1977. [Google Scholar]
- McEwen, B.M. Physiology and neurobiology of stress and adaptation: Central role of the brain. Physiol. Rev. 2007, 87, 873–904. [Google Scholar] [CrossRef] [Green Version]
- Karasek, R.; Theorell, T. Healthy Work. Stress, Productivity, and the Reconstruction of Working Life; Basic Books: New York, NY, USA, 1990. [Google Scholar]
- Siegrist, J.; Li, J. Handbook of Socioeconomic Determinants of Occupational Health; Theorell, T., Ed.; Springer Nature: Cham, Switzerland, 2020; Volume 1, Chapter 19; pp. 355–382. [Google Scholar]
- Evanoff, B.A.; Rohlman, D.S.; Strickland, J.R.; Dale, A.M. Influence of work organization and work environment on missed work, productivity, and use of pain medications among construction apprentices. Am. J. Ind. Med. 2020, 63, 269–276. [Google Scholar] [CrossRef]
- Airagnes, G.; Lemogne, C.; Goldberg, M.; Hoertel, N.; Roquelaure, Y.; Limosin, F.; Zins, M. Job exposure to the public in relation with alcohol, tobacco and cannabis use: Findings from the CONSTANCES cohort study. PLoS ONE 2018, 13, e0196330. [Google Scholar] [CrossRef] [Green Version]
- Milner, A.; Scovelle, A.J.; King, T.L.; Madsen, I. Exposure to work stress and use of psychotropic medications: A systematic review and meta-analysis. J. Epidemiol. Community Health 2019, 73, 569–576. [Google Scholar] [CrossRef]
- Tan, E.C.; Pan, K.Y.; Hanson, L.L.; Fastbom, J.; Westerlund, H.; Wang, H.X. Psychosocial job strain and polypharmacy: A national cohort study. Scand. J. Work Environ. Health 2020, 46, 589–598. [Google Scholar] [CrossRef]
- Lassalle, M.; Chastang, J.F.; Niedhammer, I. Working conditions and psychotropic drug use: Cross-sectional and prospective results from the French national SIP study. J. Psychiatr. Res. 2015, 63, 50–57. [Google Scholar] [CrossRef] [Green Version]
- Lavigne, É.; Bourbonnais, R. Psychosocial work environment, interpersonal violence at work and psychotropic drug use among correctional officers. Int. J. Law Psychiatry 2010, 33, 122–129. [Google Scholar] [CrossRef]
- Jones, J.D.; Mogali, S.; Comer, S.D. Polydrug abuse: A review of opioid and benzodiazepine combination use. Drug Alcohol Depend. 2012, 125, 8–18. [Google Scholar] [CrossRef] [Green Version]
- Karjalainen, K.; Kuussaari, K.; Kataja, K.; Tigerstedt, C.; Hakkarainen, P. Measuring concurrent polydrug use in general populations: A critical assessment. Eur. Addict. Res. 2017, 23, 163–169. [Google Scholar] [CrossRef]
- Muntaner, C.; Anthony, J.C.; Crum, R.M.; Eaton, W.W. Psychosocial dimensions of work and the risk of drug dependence among adults. Am. J. Epidemiol. 1995, 142, 183–190. [Google Scholar] [CrossRef]
- Reed, P.L.; Storr, L.L.; Anthony, J.C. Drug dependence enviromics: Job strain in the work environment and risk of becoming drug-dependent. Am. J. Epidemiol. 2006, 163, 404–411. [Google Scholar] [CrossRef] [Green Version]
- Ryff, C.; Almeida, D.M.; Ayanian, J.; Carr, D.S.; Cleary, P.D.; Coe, C.; Davidson, R.J.; Krueger, R.F.; Lachman, M.E.; Marks, N.F.; et al. Midlife in the United States (MIDUS 2), 2004–2006; Inter-University Consortium for Political and Social Research: Ann Arbor, MI, USA, 15 September 2021. [Google Scholar] [CrossRef]
- Siegrist, J.; Starke, D.; Chandola, T.; Godin, I.; Marmot, M.; Niedhammer, I.; Peter, R. The measurement of effort-reward imbalance at work: European comparisons. Soc. Sci. Med. 2004, 58, 1483–1499. [Google Scholar] [CrossRef]
- Kessler, R.C.; Andrews, G.; Mroczek, D.; Ustun, B.; Wittchen, H.U. The World Health Organization composite international diagnostic interview short-form (CIDI-SF). Int. J. Methods Psychiatr. Res. 1998, 7, 171–185. [Google Scholar] [CrossRef]
- Kessler, R.C.; McGonagle, K.A.; Zhao, S.; Nelson, C.B.; Hughes, M.; Eshleman, S.; Wittchen, H.U.; Kendler, K.S. Lifetime and 12-month prevalence of DSM-III-R psychiatric disorders in the United States. Results from the National Comorbidity Survey. Arch. Gen. Psychiatry 1994, 51, 8–19. [Google Scholar] [CrossRef] [PubMed]
- Glei, D.A.; Stokes, A.; Weinstein, M. Changes in mental health, pain, and drug misuse since the mid-1990s: Is there a link? Soc. Sci. Med. 2020, 246, 112789. [Google Scholar] [CrossRef]
- U.S. Department of Agriculture; U.S. Department of Health and Human Services. Dietary Guidelines for Americans, 2020–2025. 2020. Available online: https://www.dietaryguidelines.gov/sites/default/files/2020-12/Dietary_Guidelines_for_Americans_2020-2025.pdf (accessed on 10 December 2021).
- Hendy, H.M.; Black, P.; Can, S.H.; Fleischut, A.; Aksen, D. Opioid abuse as maladaptive coping to life stressors in U.S. adults. J. Drug Issues 2018, 48, 560–571. [Google Scholar] [CrossRef]
- Head, J.; Stansfeld, S.A.; Siegrist, J. Psychosocial work environment and alcohol dependence. Occup. Environ. Med. 2004, 61, 219–224. [Google Scholar] [CrossRef] [Green Version]
- Schultz, W. Behavioral theories and the neurophysiology of reward. Annu. Rev. Psychol. 2006, 57, 87–115. [Google Scholar] [CrossRef] [Green Version]
- Eisenberger, N.I. The neural bass of social pain: Evidence for shared representation with physical pain. Psychosom. Med. 2012, 74, 126–135. [Google Scholar] [CrossRef] [Green Version]
- Blum, K.; Cull, J.G.; Braverman, E.R.; Comings, D.E. Reward deficiency syndrome. Am. Sci. 1996, 84, 132–145. [Google Scholar]
- Montano, D.; Li, J.; Siegrist, J. Work Stress and Health in a Globalized Economy: The Model of Effort–Reward Imbalance; Siegrist, J., Wahrendorf, M., Eds.; Springer: Cham, Switzerland, 2016; Volume 1, Chapter 2; pp. 21–42. [Google Scholar]
- Tsutsumi, A.; Kayaba, K.; Nagami, M.; Miki, A.; Kawano, Y.; Ohya, Y.; Odagiri, Y.; Shimomitsu, T. The effort-reward imbalance model: Experience in Japanese working population. J. Occup. Health 2002, 44, 398–407. [Google Scholar] [CrossRef] [Green Version]
- Li, J.; Yang, W.; Cheng, Y.; Siegrist, J.; Cho, S.-I. Effort-reward imbalance at work and job dissatisfaction in Chinese healthcare workers: A validation study. Int. Arch. Occ. Environ. Health 2005, 78, 198–204. [Google Scholar] [CrossRef]
- Juárez-Garcia, A.; Vera-Calzaretta, A.; Blanco-Gomez, G.; Gomez-Ortiz, V.; Hernandez-Mendoza, E.; Jacinto-Ubillus, J.; Choi, B. Validity of the effort/reward imbalance questionnaire in health professionals from six Latin-American countries. Am. J. Ind. Med. 2015, 58, 636–649. [Google Scholar] [CrossRef]
- Gillen, M.; Yen, I.H.; Trupin, L.; Swig, L.; Rugulies, R.; Mullen, K.; Font, A.; Burian, D.; Ryan, G.; Janowitz, I.; et al. The association of socioeconomic status and psychosocial and physical workplace factors with musculoskeletal injury in hospital workers. Am. J. Ind. Med. 2007, 50, 245–260. [Google Scholar] [CrossRef]
- Choi, B.; Ko, S.; Dobson, M.; Schnall, P.L.; Garcia-Rivas, J.; Israel, L.; Baker, D. Short-term test-retest reliability of the Job Content Questionnaire and Effort-Reward Imbalance Questionnaire items and scales among professional firefighters. Ergonomics 2014, 57, 897–911. [Google Scholar] [CrossRef]
- Burgel, B.J.; Elshatarat, R.A. Psychosocial work factors and low back pain in taxi drivers. Am. J. Ind. Med. 2017, 60, 734–746. [Google Scholar] [CrossRef]
- Feaster, M.; Arah, O.A.; Krause, N. Effort-reward imbalance and ambulatory blood pressure among female Las Vegas hotel room cleaners. Am. J. Ind. Med. 2019, 62, 523–534. [Google Scholar] [CrossRef]
- Mutambudzi, M.; Siegrist, J.; Meyer, J.D.; Li, J. Association between effort-reward imbalance and self-reported diabetes mellitus in older U.S. workers. J. Psychosom. Res. 2018, 104, 61–64. [Google Scholar] [CrossRef]
- Koch, P.; Schablon, A.; Latza, U.; Nienhaus, A. Musculoskeletal pain and effort-reward imbalance—A systematic review. BMC Public Health 2014, 14, 37. [Google Scholar] [CrossRef] [Green Version]
- Rugulies, R.; Aust, B.; Madsen, I.E. Effort-reward imbalance at work and risk of depressive disorders. A systematic review and meta-analysis of prospective cohort studies. Scand. J. Work Environ. Health 2017, 43, 294–306. [Google Scholar] [CrossRef]
- Friedman, S.R.; Krawczyk, N.; Perlman, D.C.; Mateu-Gelabert, P.; Ompad, D.C.; Hamilton, L.; Nikolopoulos, G.; Guarino, H.; Cerdá, M. The opioid/overdose crisis as a dialectics of pain, despair, and one-sided struggle. Front. Public Health 2020, 8, 540423. [Google Scholar] [CrossRef]
- Hill, K.P. Medical marijuana for treatment of chronic pain and other medical and psychiatric problems: A clinical review. JAMA 2015, 313, 2474–2483. [Google Scholar] [CrossRef]
- de Jonge, J.; van der Linden, S.; Schaufeli, W.; Peter, R.; Siegrist, J. Factorial invariance and stability of the Effort-Reward Imbalance Scales: A longitudinal analysis of two samples with different time lags. Int. J. Behav. Med. 2008, 15, 62–72. [Google Scholar] [CrossRef]
| Variables | N (%) | |
|---|---|---|
| Age (years) | ≤45 | 702 (31.75) |
| 46–55 | 827 (37.40) | |
| ≥56 | 682 (30.85) | |
| Gender | Men | 1083 (48.98) |
| Women | 1128 (51.02) | |
| Marital status | Married | 1626 (73.55) |
| Never married | 194 (8.77) | |
| Others | 391 (17.68) | |
| Race | White | 2036 (92.09) |
| Black | 72 (3.25) | |
| Others | 103 (4.66) | |
| Education: | High school or less | 590 (26.68) |
| Some college | 629 (28.45) | |
| University or more | 992 (44.87) | |
| Annual household income (US $) | <60,000 | 820 (37.09) |
| 60,000–99,999 | 719 (32.52) | |
| ≥100,000 | 672 (30.39) | |
| Current smoking | No | 1882 (85.12) |
| Yes | 329 (14.88) | |
| Alcohol drinking | Low or moderate | 2159 (97.65) |
| Heavy | 52 (2.35) | |
| Leisure-time physical activity | Low | 520 (23.52) |
| Moderate | 795 (35.96) | |
| High | 896 (40.52) | |
| Pain | No | 1562 (70.65) |
| Yes | 649 (29.35) | |
| Depressive affect | No | 2047 (92.58) |
| Yes | 164 (7.42) |
| Drug Misuse: No | Drug Misuse: Yes | p | |
|---|---|---|---|
| Any drug misuse | N = 1956 (88.47%) | N = 255 (11.53%) | |
| Effort | 24.36 (5.19) | 25.49 (5.04) | 0.0011 |
| Mental effort | 12.90 (2.98) | 12.90 (2.96) | 0.9632 |
| Physical effort | 11.46 (3.97) | 12.58 (4.08) | <0.0001 |
| Reward | 24.29 (3.42) | 23.78 (3.58) | 0.0269 |
| Job promotion | 13.65 (2.29) | 13.32 (2.34) | 0.0317 |
| Esteem | 7.11 (1.30) | 6.94 (1.35) | 0.0622 |
| Job security | 3.53 (0.83) | 3.52 (0.81) | 0.7633 |
| E-R ratio | 0.72 (0.22) | 0.77 (0.24) | 0.0002 |
| Opioid misuse | N = 2125 (96.11%) | N = 86 (3.89%) | |
| Effort | 24.42 (5.18) | 26.08 (5.24) | 0.0037 |
| Mental effort | 12.88 (2.98) | 13.34 (3.00) | 0.1633 |
| Physical effort | 11.54 (3.97) | 12.74 (4.40) | 0.0063 |
| Reward | 24.28 (3.42) | 23.14 (3.88) | 0.0027 |
| Job promotion | 13.64 (2.28) | 12.84 (2.59) | 0.0016 |
| Esteem | 7.10 (1.31) | 6.82 (1.41) | 0.0572 |
| Job security | 3.54 (0.83) | 3.46 (0.84) | 0.4425 |
| E-R ratio | 0.72 (0.22) | 0.83 (0.32) | 0.0017 |
| Sedatives misuse | N = 2122 (95.97%) | N = 89 (4.03%) | |
| Effort | 24.49 (5.20) | 24.36 (4.82) | 0.8096 |
| Mental effort | 12.92 (2.97) | 12.42 (3.25) | 0.1195 |
| Physical effort | 11.58 (4.010 | 11.94 (3.60) | 0.3960 |
| Reward | 24.24 (3.45) | 24.09 (3.40) | 0.6884 |
| Job promotion | 13.61 (2.30) | 13.55 (2.16) | 0.7968 |
| Esteem | 7.09 (1.31) | 6.96 (1.33) | 0.3249 |
| Job security | 3.53 (0.83) | 3.58 (0.76) | 0.5459 |
| E-R ratio | 0.73 (0.22) | 0.73 (0.21) | 0.9916 |
| Cannabis misuse | N = 2108 (95.34%) | N = 103 (4.66%) | |
| Effort | 24.42 (5.20) | 25.82 (4.65) | 0.0079 |
| Mental effort | 12.91 (3.00) | 12.67 (2.56) | 0.3610 |
| Physical effort | 11.52 (3.98) | 13.14 (4.06) | <0.0001 |
| Reward | 24.24 (3.45) | 24.14 (3.27) | 0.7913 |
| Job promotion | 13.62 (2.30) | 13.44 (2.19) | 0.4280 |
| Esteem | 7.08 (1.31) | 7.16 (1.29) | 0.5995 |
| Job security | 3.53 (0.83) | 3.55 (0.76) | 0.7915 |
| E-R ratio | 0.73 (0.23) | 0.77 (0.19) | 0.0895 |
| Other drug misuse | N = 2159 (97.65%) | N = 52 (2.35%) | |
| Effort | 24.45 (5.15) | 26.06 (6.38) | 0.0773 |
| Mental effort | 12.89 (2.98) | 13.06 (3.16) | 0.6956 |
| Physical effort | 11.56 (3.98) | 13.00 (4.41) | 0.0101 |
| Reward | 24.27 (3.43) | 22.54 (3.64) | 0.0003 |
| Job promotion | 13.64 (2.28) | 12.54 (2.42) | 0.0006 |
| Esteem | 7.10 (1.30) | 6.54 (1.58) | 0.0135 |
| Job security | 3.53 (0.83) | 3.46 (0.78) | 0.5327 |
| E-R ratio | 0.73 (0.22) | 0.85 (0.31) | 0.0078 |
| Model I | Model II | Model III | ||
|---|---|---|---|---|
| Any drug misuse | ||||
| Effort | (increase per SD) | 1.20 (1.05, 1.38) | 1.19 (1.04, 1.37) | 1.16 (1.01, 1.34) |
| Mental effort | (increase per SD) | 0.98 (0.85, 1.12) | 0.97 (0.85, 1.11) | 0.93 (0.81, 1.07) |
| Physical effort | (increase per SD) | 1.32 (1.14, 1.52) | 1.30 (1.13, 1.50) | 1.29 (1.12, 1.49) |
| Reward | (decrease per SD) | 1.11 (0.98, 1.27) | 1.11 (0.97, 1.27) | 1.08 (0.95, 1.24) |
| Job promotion | (decrease per SD) | 1.10 (0.97, 1.25) | 1.10 (0.96, 1.26) | 1.07 (0.94, 1.23) |
| Esteem | (decrease per SD) | 1.11 (0.98, 1.26) | 1.10 (0.97, 1.25) | 1.08 (0.95, 1.23) |
| Job security | (decrease per SD) | 1.01 (0.88, 1.15) | 1.01 (0.88, 1.15) | 1.00 (0.88, 1.14) |
| E-R ratio | (increase per SD) | 1.24 (1.08, 1.42) | 1.23 (1.06, 1.41) | 1.18 (1.03, 1.37) |
| Opioid misuse | ||||
| Effort | (increase per SD) | 1.30 (1.04, 1.63) | 1.30 (1.03, 1.62) | 1.24 (0.99, 1.56) |
| Mental effort | (increase per SD) | 1.17 (0.93, 1.46) | 1.16 (0.92, 1.44) | 1.10 (0.88, 1.38) |
| Physical effort | (increase per SD) | 1.28 (1.01, 1.62) | 1.28 (1.01, 1.61) | 1.24 (0.99, 1.57) |
| Reward | (decrease per SD) | 1.29 (1.06, 1.57) | 1.29 (1.05, 1.57) | 1.23 (1.00, 1.51) |
| Job promotion | (decrease per SD) | 1.29 (1.06, 1.57) | 1.28 (1.05, 1.57) | 1.23 (0.99, 1.50) |
| Esteem | (decrease per SD) | 1.20 (0.98, 1.45) | 1.20 (0.98, 1.46) | 1.16 (0.96, 1.42) |
| Job security | (decrease per SD) | 1.06 (0.86, 1.30) | 1.06 (0.86, 1.30) | 1.05 (0.86, 1.30) |
| E-R ratio | (increase per SD) | 1.43 (1.15, 1.78) | 1.43 (1.14, 1.78) | 1.35 (1.07, 1.69) |
| Sedatives misuse | ||||
| Effort | (increase per SD) | 1.02 (0.82, 1.27) | 1.02 (0.82, 1.28) | 1.00 (0.79, 1.25) |
| Mental effort | (increase per SD) | 0.89 (0.71, 1.10) | 0.89 (0.71, 1.10) | 0.84 (0.67, 1.06) |
| Physical effort | (increase per SD) | 1.14 (0.90, 1.43) | 1.14 (0.90, 1.43) | 1.13 (0.90, 1.43) |
| Reward | (decrease per SD) | 1.04 (0.83, 1.29) | 1.03 (0.83, 1.28) | 1.00 (0.80, 1.25) |
| Job promotion | (decrease per SD) | 1.01 (0.81, 1.26) | 1.01 (0.81, 1.26) | 0.99 (0.79, 1.24) |
| Esteem | (decrease per SD) | 1.13 (0.93, 1.38) | 1.12 (0.91, 1.36) | 1.09 (0.89, 1.34) |
| Job security | (decrease per SD) | 0.90 (0.72, 1.13) | 0.90 (0.71, 1.13) | 0.89 (0.70, 1.12) |
| E-R ratio | (increase per SD) | 1.05 (0.84, 1.32) | 1.05 (0.84, 1.32) | 1.01 (0.80, 1.27) |
| Cannabis misuse | ||||
| Effort | (increase per SD) | 1.14 (0.92, 1.41) | 1.09 (0.87, 1.36) | 1.09 (0.87, 1.36) |
| Mental effort | (increase per SD) | 0.83 (0.68, 1.03) | 0.82 (0.66, 1.02) | 0.81 (0.65, 1.01) |
| Physical effort | (increase per SD) | 1.38 (1.11, 1.72) | 1.32 (1.05, 1.66) | 1.32 (1.05, 1.66) |
| Reward | (decrease per SD) | 0.94 (0.76, 1.16) | 0.95 (0.77, 1.19) | 0.95 (0.76, 1.19) |
| Job promotion | (decrease per SD) | 0.98 (0.80, 1.21) | 1.00 (0.81, 1.24) | 1.00 (0.81, 1.24) |
| Esteem | (decrease per SD) | 0.89 (0.71, 1.11) | 0.89 (0.71, 1.11) | 0.89 (0.71, 1.11) |
| Job security | (decrease per SD) | 0.97 (0.78, 1.19) | 0.99 (0.80, 1.22) | 0.99 (0.80, 1.22) |
| E-R ratio | (increase per SD) | 1.08 (0.87, 1.34) | 1.05 (0.84, 1.32) | 1.06 (0.84, 1.33) |
| Other drug misuse | ||||
| Effort | (increase per SD) | 1.27 (0.96, 1.69) | 1.24 (0.93, 1.65) | 1.19 (0.89, 1.59) |
| Mental effort | (increase per SD) | 1.05 (0.79, 1.40) | 1.03 (0.78, 1.38) | 0.95 (0.71, 1.28) |
| Physical effort | (increase per SD) | 1.34 (0.99, 1.80) | 1.30 (0.97, 1.76) | 1.30 (0.97, 1.75) |
| Reward | (decrease per SD) | 1.42 (1.11, 1.82) | 1.42 (1.11, 1.82) | 1.38 (1.08, 1.78) |
| Job promotion | (decrease per SD) | 1.37 (1.07, 1.75) | 1.36 (1.06, 1.75) | 1.34 (1.04, 1.74) |
| Esteem | (decrease per SD) | 1.37 (1.09, 1.72) | 1.36 (1.09, 1.71) | 1.35 (1.07, 1.69) |
| Job security | (decrease per SD) | 1.04 (0.80, 1.36) | 1.05 (0.80, 1.37) | 1.04 (0.79, 1.35) |
| E-R ratio | (increase per SD) | 1.44 (1.09, 1.92) | 1.43 (1.07, 1.91) | 1.36 (1.01, 1.83) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Li, J.; Matthews, T.A.; Chen, L.; Seamans, M.; Leineweber, C.; Siegrist, J. Effort–Reward Imbalance at Work and Drug Misuse: Evidence from a National Survey in the U.S. Int. J. Environ. Res. Public Health 2021, 18, 13334. https://doi.org/10.3390/ijerph182413334
Li J, Matthews TA, Chen L, Seamans M, Leineweber C, Siegrist J. Effort–Reward Imbalance at Work and Drug Misuse: Evidence from a National Survey in the U.S. International Journal of Environmental Research and Public Health. 2021; 18(24):13334. https://doi.org/10.3390/ijerph182413334
Chicago/Turabian StyleLi, Jian, Timothy A. Matthews, Liwei Chen, Marissa Seamans, Constanze Leineweber, and Johannes Siegrist. 2021. "Effort–Reward Imbalance at Work and Drug Misuse: Evidence from a National Survey in the U.S." International Journal of Environmental Research and Public Health 18, no. 24: 13334. https://doi.org/10.3390/ijerph182413334
APA StyleLi, J., Matthews, T. A., Chen, L., Seamans, M., Leineweber, C., & Siegrist, J. (2021). Effort–Reward Imbalance at Work and Drug Misuse: Evidence from a National Survey in the U.S. International Journal of Environmental Research and Public Health, 18(24), 13334. https://doi.org/10.3390/ijerph182413334






