Mass Gathering Medicine in Soccer Leagues: A Review and Creation of the SALEM Tool
Abstract
1. Introduction
2. Healthcare Risks of Football MG Events
3. Influential Factors of the Healthcare System’s Response
4. MG in Football and History of Disasters
5. Impact of the COVID-19 Pandemic on Football
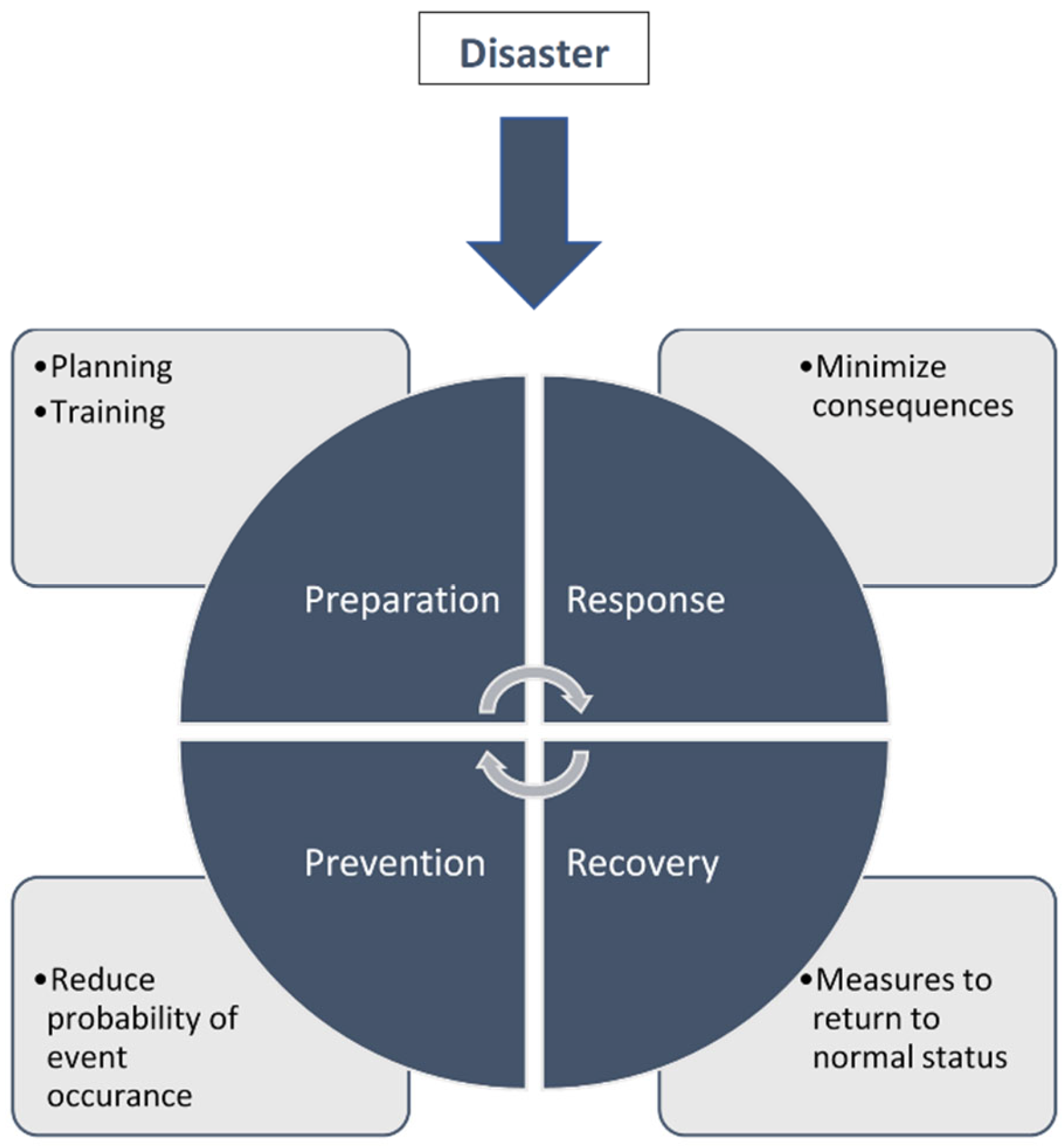
6. Preparation and Planning for Football MG Events
7. SALEM Tool: A Mass Gatherings Risk Assessment Framework
8. Key Insights and Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- WHO. Public Health for Mass Gatherings: Key Considerations. World Health Organisation. Available online: https://apps.who.int/iris/bitstream/handle/10665/162109/WHO_HSE_GCR_2015.5_eng.pdf;jsessionid=20CDEF66BA427C7DB54004047BD811E4?sequence=1 (accessed on 21 June 2021).
- Aitsi-Selmi, A.; Murray, V.; Heymann, D.; McCloskey, B.; Azhar, E.I.; Petersen, E.; Zumla, A.; Dar, O. Reducing risks to health and wellbeing at mass gatherings: The role of the sendai framework for disaster risk reduction. Int. J. Infect. Dis. 2016, 47, 101–104. [Google Scholar] [CrossRef]
- McCloskey, B.; Endericks, T.; Catchpole, M.; Zambon, M.; McLauchlin, J.; Shetty, N.; Manuel, R.; Turbitt, D.; Smith, G.; Crook, P.; et al. London 2012 Olympic and Paralympic Games: Public health surveillance and epidemiology. Lancet 2014, 383, 2083–2089. [Google Scholar] [CrossRef]
- Memish, Z.A.; Zumla, A.; Alhakeem, R.F.; Assiri, A.; Turkestani, A.; Al Harby, K.D.; Alyemni, M.; Dhafar, K.; Gautret, P.; Barbeschi, M.; et al. Hajj: Infectious disease surveillance and control. Lancet 2014, 383, 2073–2082. [Google Scholar] [CrossRef]
- Smallwood, C.A.H.; Arbuthnott, K.G.; Banczak-Mysiak, B.; Borodina, M.; Coutinho, A.P.; Payne-Hallström, L.; Lipska, E.; Lyashko, V.; Miklasz, M.; Miskiewicz, P.; et al. Euro 2012 European football championship finals: Planning for a health legacy. Lancet 2014, 383, 2090–2097. [Google Scholar] [CrossRef]
- Abubakar, I.; Gautret, P.; Brunette, G.W.; Blumberg, L.; Johnson, D.; Poumerol, G.; Memish, Z.A.; Barbeschi, M.; Khan, A.S. Global perspectives for prevention of infectious diseases associated with mass gatherings. Lancet. Infect. Dis. 2012, 12, 66–74. [Google Scholar] [CrossRef]
- Schwartz, B.; Nafziger, S.; Milsten, A.; Luk, J.; Yancey, A. Mass gathering medical care: Resource document for the national association of EMS physicians position statement. Prehosp. Emerg. Care 2015, 19, 559–568. [Google Scholar]
- Tavan, A.; Tafti, A.D.; Nekoie-Moghadam, M.; Ehrampoush, M.; Vafaei Nasab, M.R.; Tavangar, H.; Fallahzadeh, H. Risks threatening the health of people participating in mass gatherings: A systematic review. J. Educ. Health Promot. 2019, 8, 209. [Google Scholar] [CrossRef] [PubMed]
- Jones, D.S. Olympic medicine. N. Engl. J. Med. 2012, 367, 289–292. [Google Scholar] [CrossRef]
- Ahmed, Q.A.; Memish, Z.A. From the “Madding Crowd” to mass gatherings-religion, sport, culture and public health. Travel Med. Infect. Dis. 2019, 28, 91–97. [Google Scholar] [CrossRef] [PubMed]
- Boston Athletic Association. Boston Marathon History: Boston Marathon Facts. 2014. Available online: http://216.235.243.43/races/boston-marathon/boston-marathon-history/boston-marathon-facts.aspx (accessed on 21 June 2021).
- FIFA. FIFA Survey: Approximately 250 Million Footballers Worldwide; FIFA: Zürich, Switzerland, 2013. [Google Scholar]
- Hines, K. Mass gathering medicine. Trauma 2000, 2, 143–151. [Google Scholar]
- AlNsour, M.; Fleischauer, A. Public health considerations for mass gatherings in the Middle East and North Africa (MENA) region. East. Mediterr. Health J. 2013, 19 (Suppl. S2), S42–S47. [Google Scholar] [CrossRef]
- Cariappa, M.P.; Singh, B.P.; Mahen, A.; Bansal, A.S. Kumbh Mela 2013: Healthcare for the millions. Med. J. Armed Forces India 2015, 71, 278–281. [Google Scholar] [CrossRef]
- Blumberg, L.; Regmi, J.; Endricks, T.; McCloskey, B.; Petersen, E.; Zumla, A.; Barbeschi, M. Hosting of mass gathering sporting events during the 2013–2016 Ebola virus outbreak in West Africa: Experience from three African countries. Int. J. Infect. Dis. 2016, 47, 38–41. [Google Scholar] [CrossRef] [PubMed]
- Sokhna, C.; Mboup, B.M.; Sow, P.G.; Camara, G.; Dieng, M.; Sylla, M.; Gueye, L.; Sow, D.; Diallo, A.; Parola, P.; et al. Communicable and non-communicable disease risks at the Grand Magal of Touba: The largest mass gathering in Senegal. Travel Med. Infect. Dis. 2017, 19, 56–60. [Google Scholar] [CrossRef] [PubMed]
- Ishola, D.A.; Phin, N. Could influenza transmission be reduced by restricting mass gatherings? Towards an evidence-based policy framework. J. Epidemiol. Glob. Health 2011, 1, 33–60. [Google Scholar] [CrossRef] [PubMed]
- WHO. Communicable Disease Alert and Response for Mass Gatherings; World Health Organization: Geneva, Switzerland, 2008. [Google Scholar]
- Yezli, S.; Assiri, A.; Nabulsi, H.; Awam, A.; Blumberg, L.; Endericks, T.; Stergachis, A.; Reicher, S.; McCloskey, B.; Petersen, E.; et al. From mass gatherings medicine to mass gatherings health: Conclusions from the 3rd International Conference on mass gatherings medicine, Riyadh, Kingdom of Saudi Arabia. Int. J. Infect. Dis. 2018, 66, 128–130. [Google Scholar] [CrossRef] [PubMed]
- Odone, A.; Delmonte, D.; Scognamiglio, T.; Signorelli, C. COVID-19 deaths in Lombardy, Italy: Data in context. Lancet Public Health 2020, 5, e310. [Google Scholar] [CrossRef]
- Signorelli, C.; Scognamiglio, T.; Odone, A. COVID-19 in Italy: Impact of containment measures and prevalence estimates of infection in the general population. Acta Biomed. 2020, 91, 175–179. [Google Scholar] [CrossRef]
- Signorelli, C.; Odone, A.; Riccò, M.; Bellini, L.; Croci, R.; Oradini-Alacreu, A.; Fiacchini, D.; Burioni, R. Major sports events and the transmission of sars-cov-2: Analysis of seven case-studies in europe. Acta Biomed. 2020, 91, 242–244. [Google Scholar] [CrossRef]
- Bieler, D. ‘A Biological Bomb’: Champions League Match in Italy Linked to Epicentre of Coronavirus Outbreak. The Independent. 2020. Available online: https://www.independent.co.uk/news/world/coronavirus-italy-champions-league-atlanta-valencia-milan-bergamo-a9426616.html (accessed on 28 June 2021).
- Soomaroo, L.; Murray, V. Disasters at mass gatherings: Lessons from history. PLoS Curr. 2012, 4, RRN1301. [Google Scholar] [CrossRef]
- Salamati, P.; Rahimi-Movaghar, V. Hajj stampede in Mina, 2015: Need for intervention. Arch. Trauma Res. 2016, 5, e36308. [Google Scholar] [CrossRef]
- Shujaa, A.; Alhamid, S. Health response to Hajj mass gathering from emergency perspective, narrative review. Turk. J. Emerg. Med. 2015, 15, 172–176. [Google Scholar] [CrossRef] [PubMed]
- Alhadhira, A.; Molloy, M.S.; Casasola, M.; Sarin, R.R.; Massey, M.; Voskanyan, A.; Ciottone, G.R. Use of dimensional analysis in the X-, Y-, and Z-Axis to predict occurrence of injury in human stampede. Disaster Med. Public Health Prep. 2019, 14, 248–255. [Google Scholar] [CrossRef]
- Ranse, J.; Zeitz, K. Chain of survival at mass gatherings: A case series of resuscitation events. Prehosp. Disaster Med. 2010, 25, 457–463. [Google Scholar] [CrossRef]
- Turris, S.A.; Lund, A.; Hutton, A.; Bowles, R.; Ellerson, E.; Steenkamp, M.; Ranse, J.; Arbon, P. Mass-gathering health research foundational theory: Part 2—Event modeling for mass gatherings. Prehosp. Disaster Med. 2014, 29, 655–663. [Google Scholar] [CrossRef] [PubMed]
- Health conditions for travellers to Saudi Arabia for the pilgrimage to Mecca (Hajj). Relev. Epidemiol. Hebd. 2013, 88, 343–347.
- Hutton, A.; Zeitz, K.; Brown, S.; Arbon, P. Assessing the psychosocial elements of crowds at mass gatherings. Prehosp. Disaster Med. 2011, 26, 414–421. [Google Scholar] [CrossRef] [PubMed]
- Hopkins, N.; Reicher, S. The psychology of health and well-being in mass gatherings: A review and a research agenda. J. Epidemiol. Glob. Health 2016, 6, 49–57. [Google Scholar] [CrossRef] [PubMed]
- Hutton, A.; Ranse, J.; Gray, K.L.; Turris, S.; Lund, A.; Munn, M.B. Psychosocial influences on patient presentations: Considerations for research and evaluation at mass-gathering events. Prehosp. Disaster Med. 2020, 35, 197–205. [Google Scholar] [CrossRef]
- Bennett, S.A. Demonisation as explanation? A systems theory-informed analysis of the origins of, and reaction to the 1946 Burnden Park and 1989 Hillsborough football stadium disasters. Int. J. Disaster Risk Reduct. 2017, 21, 405–418. [Google Scholar] [CrossRef]
- Helbing, D.; Farkas, I.J.; Vicsek, T. 11. Crowd disasters and simulation of panic situations. In The Science of Disasters; Springer: Berlin/Heidelberg, Germany, 2002; Volume 2, p. 331. [Google Scholar]
- Akin, Y. 6 Not just a game: The Kayseri vs. Sivas football disaster. Soccer Soc. 2004, 5, 219–232. [Google Scholar] [CrossRef]
- Darby, P.; Johnes, M.; Mellor, G. Football disasters: A conceptual frame. Soccer Soc. 2004, 5, 125–133. [Google Scholar] [CrossRef]
- Walker, G. 3 ‘The ibrox stadium disaster of 1971’. Soccer Soc. 2004, 5, 169–182. [Google Scholar] [CrossRef]
- Darby, P. 8 A context of vulnerability: The zambian air disaster, 1993. Soccer Soc. 2004, 5, 248–264. [Google Scholar] [CrossRef]
- Molloy, M.S. Management of mass gatherings. In Koenig and Schultz’s Disaster Medicine: Comprehensive Principles and Practices; Schultz, C.H., Koenig, K.L., Eds.; Cambridge University Press: Cambridge, UK, 2016; pp. 265–293. ISBN 9781107040755. [Google Scholar]
- Zeller, M. Sport and Society in the Soviet Union: The Politics of Football after Stalin; Bloomsbury Publishing: New York, NY, USA, 2018. [Google Scholar]
- Broeze, C.L.; Falder, S.; Rea, S.; Wood, F. Burn disasters—An audit of the literature. Prehosp. Disaster Med. 2010, 25, 555–579. [Google Scholar] [CrossRef] [PubMed]
- Logan, C.; Gosseye, J. Architecture and the Spectre of the Crowd. Archit. Theory Rev. 2019, 23, 171–177. [Google Scholar] [CrossRef]
- Elshawarby, M.K. Football Stadiums’ Disasters, University of Peloponnese. 2015. Available online: https://amitos.library.uop.gr/xmlui/bitstream/handle/123456789/4803/Mohamed%20Shawarby%20Thesis%20-%20Final%20Version%2026-4-2016.pdf?sequence=1l (accessed on 28 June 2021).
- Kerr, G.W. Emergency medical planning at soccer matches. Int. Sport Med. J. 2003, 4, 1–5. [Google Scholar]
- Alegi, P. 7 ‘Like cows driven to a dip’: The 2001 ellis park stadium disaster in South Africa. Soccer Soc. 2004, 5, 233–247. [Google Scholar] [CrossRef]
- Pollard, R.; Gómez, M.A. Home advantage in football in South-West Europe: Long-term trends, regional variation, and team differences. Eur. J. Sport Sci. 2009, 9, 341–352. [Google Scholar] [CrossRef]
- Madzimbamuto, F.D. A hospital response to a soccer stadium stampede in Zimbabwe. Emerg. Med. J. 2003, 20, 556–559. [Google Scholar] [CrossRef][Green Version]
- Künzler, D. Ivory coast BT. In The Palgrave International Handbook of Football and Politics; De Waele, J.-M., Gibril, S., Gloriozova, E., Spaaij, R., Eds.; Springer International Publishing: Cham, Germany, 2018; pp. 385–402. ISBN 978-3-319-78777-0. [Google Scholar]
- Hughson, J.; Moore, K.; Spaaij, R.; Maguire, J. (Eds.) Football hooliganism. In Routledge Handbook of Football Studies; Taylor & Francis: Oxfordshire, UK, 2016; pp. 364–374. [Google Scholar]
- Abaza, M. Violence, dramaturgical repertoires and neoliberal imaginaries in Cairo. Theory Cult. Soc. 2016, 33, 111–135. [Google Scholar] [CrossRef]
- Bledsoe, B.; Songer, P.; Buchanan, K.; Westin, J.; Hodnick, R.; Gorosh, L. Burning man 2011: Mass gathering medical care in an austere environment. Prehosp. Emerg. Care 2012, 16, 469–476. [Google Scholar] [CrossRef] [PubMed]
- Dong, Y.-H.; Liu, F.; Liu, Y.-M.; Jiang, X.-R.; Zhao, Z.-X. Emergency preparedness for mass gatherings: Lessons of “12.31” stampede in Shanghai Bund. Chin. J. Traumatol. 2017, 20, 240–242. [Google Scholar] [CrossRef] [PubMed]
- Polkinghorne, B.G.; Massey, P.D.; Durrheim, D.N.; Byrnes, T.; MacIntyre, C.R. Prevention and surveillance of public health risks during extended mass gatherings in rural areas: The experience of the tamworth country music festival, Australia. Public Health 2013, 127, 32–38. [Google Scholar] [CrossRef] [PubMed]
- Thackway, S.; Churches, T.; Fizzell, J.; Muscatello, D.; Armstrong, P. Should cities hosting mass gatherings invest in public health surveillance and planning? Reflections from a decade of mass gatherings in Sydney, Australia. BMC Public Health 2009, 9, 324. [Google Scholar] [CrossRef]
- WHO. General Information on Risk Communication; WHO: Geneva, Switzerland, 2020. [Google Scholar]
- Flynn, B.W.; Philbin, J.P. Risk and crisis communications. In Integrating Emergency Management and Disaster Behavioral Health: One Picture through Two Lenses; Butterworth-Heinemann: Oxford, UK, 2017; ISBN 9780128036396. [Google Scholar]
- Abrams, E.M.; Greenhawt, M. Risk communication during COVID-19. J. Allergy Clin. Immunol. Pract. 2020, 8, 1791–1794. [Google Scholar] [CrossRef]
- Ranse, J.; Hutton, A.; Keene, T.; Lenson, S.; Luther, M.; Bost, N.; Johnston, A.N.B.; Crilly, J.; Cannon, M.; Jones, N.; et al. Health service impact from mass gatherings: A systematic literature review. Prehosp. Disaster Med. 2017, 32, 71–77. [Google Scholar] [CrossRef]
- Steffen, R.; Bouchama, A.; Johansson, A.; Dvorak, J.; Isla, N.; Smallwood, C.; Memish, Z.A. Non-communicable health risks during mass gatherings. Lancet Infect. Dis. 2012, 12, 142–149. [Google Scholar] [CrossRef]
- Smith, W.P.; Wessels, V.; Naicker, D.; Leuenberger, E.; Fuhri, P.; Wallis, L.A. Development of a mass-gathering medical resource matrix for a developing world scenario. Prehosp. Disaster Med. 2010, 25, 547–552. [Google Scholar] [CrossRef]
- Ranse, J.; Hutton, A.; Turris, S.A.; Lund, A. Enhancing the minimum data set for mass-gathering research and evaluation: An integrative literature review. Prehosp. Disaster Med. 2014, 29, 280–289. [Google Scholar] [CrossRef]
- Elliott, D.; Smith, D. Football stadia disasters in the United Kingdom: Learning from tragedy? Ind. Environ. Cris. Q. 1993, 7, 205–229. [Google Scholar] [CrossRef]
- Popplewell, O. The Papers of the Popplewell Inquiry into Crowd Safety at Sports Grounds. University of Bradford Special Collections. 1985. Available online: https://www.bradford.ac.uk/library/special-collections/collections/papers-of-the-popplewell-inquiry/l (accessed on 28 June 2021).
- Rt Hon Lord Justice Taylor. Final Report into the Hillsborough Stadium Disaster. 1989. Available online: https://www.jesip.org.uk/uploads/media/incident_reports_and_inquiries/Hillsborough%20Stadium%20Disaster%20final%20report.pdf (accessed on 28 June 2021).
- Impact of the COVID-19 Pandemic on Association Football [Internet]. 2020. Available online: https://en.wikipedia.org/wiki/Impact_of_the_COVID-19_pandemic_on_association_football (accessed on 22 July 2020).
- ESPN. Coronavirus: Player at Italian Third Tier is First European Footballer Diagnosed; ESPN: Bristol, CT, USA, 2020. [Google Scholar]
- Corsini, A.; Bisciotti, G.N.; Eirale, C.; Volpi, P. Football cannot restart soon during the COVID-19 emergency! A critical perspective from the Italian experience and a call for action. Br. J. Sports Med. 2020, 54, 1186–1187. [Google Scholar] [CrossRef] [PubMed]
- Beijing Halts Sports Events after New Covid Cases. 2020. Available online: https://www.sportbusiness.com/news/beijing-halts-sports-events-after-new-covid-cases/ (accessed on 22 July 2020).
- Amid COVID-19 outbreak, J. League Postpones All Matches until March 15. Available online: https://www.japantimes.co.jp/sports/2020/02/25/soccer/j-league/jleague-cancels-levain-cup-coronavirus/ (accessed on 22 July 2020).
- Wuhan Coronavirus: Lunar New Year Cup Cancelled by Government Just Hours after HKFA Promotes The Event. Available online: https://www.scmp.com/sport/hong-kong/article/3047415/wuhan-virus-lunar-new-year-cup-go-ahead-hong-kong-despite (accessed on 22 July 2020).
- OFFICIAL: CAF Postpone Interclubs Competitions Semi-Finals. Available online: https://www.kingfut.com/2020/09/10/caf-interclubs-competitions-postponed/ (accessed on 22 July 2020).
- Coronavirus: Saudi Football League Looking at August 20 Return Date. Available online: https://english.alarabiya.net/coronavirus/2020/05/13/Coronavirus-Saudi-football-league-looking-at-August-20-return-date (accessed on 22 July 2020).
- Arabian Business. Almost 100 Saudi Football Players, Staff Test Positive for Covid-19; Arabian Business: Dubai, United Arab Emirates, 2020. [Google Scholar]
- WHO. Guidance on Mass Gatherings & Sports Events; World Health Organization: Geneva, Switzerland, 2020. [Google Scholar]
- WHO. Considerations for Sports Federations/Sports Event Organizers When Planning Mass Gatherings in the Context of COVID-19; World Health Organization: Geneva, Switzerland, 2020. [Google Scholar]
- Saudi Center for Disease Prevention and Control Sports Exercise Protocols. 2020. Available online: https://covid19.cdc.gov.sa/professionals-health-workers/preventive-protocols-from-29-10-1441/sports-exercise-protocols-en/ (accessed on 28 June 2021).
- The Official Saudi Press Agency. Prince Mohammed bin Salman Cup’s Professional League to Resume, with Precautionary Measures; The Official Saudi Press Agency: Riyadh, Saudi Arabia, 2020. [Google Scholar]
- Al Hilal-Update on AFC Champions League. AFC Champions League. 2020. Available online: https://www.the-afc.com/competitions/afc-champions-league/latest/news/latest-update-on-afc-champions-league-west-x5334 (accessed on 28 June 2021).
- Kramer, E.; Dvořák, J. Football Emergency Medicine Manual, 2nd ed.; FIFA: Zürich, Switzerland, 2015. [Google Scholar]
- Alaska, Y.A.; Aldawas, A.D.; Aljerian, N.A.; Memish, Z.A.; Suner, S. The impact of crowd control measures on the occurrence of stampedes during Mass Gatherings: The Hajj experience. Travel Med. Infect. Dis. 2017, 15, 67–70. [Google Scholar] [CrossRef] [PubMed]
- Johansson, A.; Batty, M.; Hayashi, K.; Al Bar, O.; Marcozzi, D.; Memish, Z.A. Crowd and environmental management during mass gatherings. Lancet Infect. Dis. 2012, 12, 150–156. [Google Scholar] [CrossRef]
- Sharma, U.; Desikachari, B.; Sarma, S. Content validity of the newly developed risk assessment tool for religious mass gathering events in an Indian setting (mass gathering risk assessment tool-MGRAT). J. Fam. Med. Prim. Care 2019, 8, 2207. [Google Scholar] [CrossRef]
- Gallego, V.; Berberian, G.; Lloveras, S.; Verbanaz, S.; Chaves, T.S.S.; Orduna, T.; Rodriguez-Morales, A.J. The 2014 FIFA World Cup: Communicable disease risks and advice for visitors to Brazil—A review from the Latin American society for travel medicine (SLAMVI). Travel Med. Infect. Dis. 2014, 12, 208–218. [Google Scholar] [CrossRef]
- Khorram-Manesh, A. Facilitating multiagency collaboration before mass gatherings—The development of MAGRAT (mass gathering risk assessment tool). Biomed. J. Sci. Tech. Res. 2020, 24, 18607–18616. [Google Scholar] [CrossRef]
- Sharma, U.; Desikachari, B.R.; Sarma, S. Protocol for development of a risk assessment tool for planning and management of religious mass-gathering events of India—A health system-strengthening initiative. Pilot Feasibility Stud. 2019, 5, 1–9. [Google Scholar] [CrossRef]
- WHO. WHO Mass Gathering COVID-19 Risk Assessment Tool—Generic Events. Available online: https://www.who.int/publications/i/item/10665-333185 (accessed on 12 September 2021).
- COVID-19 Mass Gathering Event Risk Assessment Tool | East Cambridgeshire District Council. Available online: https://www.eastcambs.gov.uk/community/covid-19-mass-gathering-event-risk-assessment-tool (accessed on 12 September 2021).
- McCloskey, B.; Zumla, A.; Lim, P.L.; Endericks, T.; Arbon, P.; Cicero, A.; Borodina, M. A risk-based approach is best for decision making on holding mass gathering events. Lancet 2020, 395, 1256–1257. [Google Scholar] [CrossRef]
- Khan, A.; Yezli, S.; Ciottone, G.; Borodina, M.; Ranse, J.; Gautret, P.; Turris, S.; Lund, A.; Memish, Z.A.; Sharma, A.; et al. Recommendations from the 4th international conference on mass gatherings medicine, Saudi Arabia. East. Mediterr. Health J. 2020, 26, 503–505. [Google Scholar] [CrossRef]
- Bieh, K.L.; Khan, A.; El-Ganainy, A.; Alotaibi, B.; Ghallab, S.; Abdulmalek, N.; Mukhtar, N.; Jokhdar, H. Guidance for health risk assessment at recurrent mass gatherings: The Jeddah tool framework. Prehosp. Disaster Med. 2021, 36, 348–353. [Google Scholar] [CrossRef] [PubMed]
- Ministry of Health Saudi Arabia. COVID-19 Health Risk Assessment (HRA) Related to Infection Transmission in Events and Gatherings—Salem Tool (V 1.0); Ministry of Health Saudi Arabia: Riyadh, Saudi Arabia, 2020.
- Khan, A.; Lezor Bieh, K.; El-Ganainy, A.; Ghallab, S.; Assiri, A.; Jokhdar, H.; Lezor, K.; Manager, B. Estimating the COVID-19 risk during the Hajj pilgrimage. J. Travel Med. 2020, taaa157. [Google Scholar] [CrossRef] [PubMed]
- Yezli, S.; Khan, A.A. The Jeddah tool. A health risk assessment framework for mass gatherings. Saudi Med. J. 2020, 41, 121–122. [Google Scholar] [CrossRef] [PubMed]
- Ministry of Hajj and Umrah. Hajj 1441H is Decided to Take Place This Year with Limited Number of Pilgrims from All Nationalities Residing in Saudi Arabia. Available online: https://www.spa.gov.sa/viewfullstory.php?lang=en&newsid=2100951 (accessed on 18 September 2021).
- Jokhdar, H.; Khan, A.; Asiri, S.; Motair, W.; Assiri, A.; Alabdulaali, M. COVID-19 mitigation plans during Hajj 2020: A success story of zero cases. Health Secur. 2020, 19, 133–139. [Google Scholar] [CrossRef] [PubMed]
- Memish, Z.A.; Stephens, G.M.; Steffen, R.; Ahmed, Q.A. Emergence of medicine for mass gatherings: Lessons from the Hajj. Lancet Infect. Dis. 2012, 12, 56–65. [Google Scholar] [CrossRef]
| Location and Stadium | Football Event | Incident | Casualties | Date |
|---|---|---|---|---|
| Bolton, England Burnden Park Stadium [35] | English Football Association Challenge Cup match | A wall collapsed in the stadium before the match crushing fans and sparking a stampede | 33 deaths 400 injured | March 1946 |
| Santiago, Chile Estadio Nacional de Chile [36] | The finals match of the South American soccer tournament | Human crush between fans entering the stadium | 6 deaths Unknown injuries | March 1955 |
| Lima, Peru The National Stadium [36] | Olympic qualifying match | Human crush and asphyxiation between fans due to overcrowded exiting after police fired tear gas | 318 deaths 500 injured | May 1964 * |
| Kayseri, Turkey Kayseri Atatürk Stadium [37] | Turkish league match | Human crush sparked by stone-throwing and weapon clashes between fans of the two teams | 40 deaths 600 injured | September 1967 |
| Buenos Aires, Argentina [38] | First-division league match | Asphyxiation and Human crush against closed Stadium exit between fans unaware of the closed passage | 74 deaths 150 injured | June 1968 |
| Glasgow, UK Ibrox Stadium [39] | Football match | Human crush between fans entering and exiting the stadium | 66 deaths 140 injured | January 1971 |
| Salvador, Brazil Estádio Fonte Nova [36] | Football match | Human crush sparked by a fight between fans | 4 deaths 1500 injured | March 1971 |
| Cairo, Egypt Zamalek stadium [40] | Friendly football match | Human crush due to overcrowding during the influx of fans | 49 deaths 50 injured | February 1974 |
| Yaounde, Cameroon [40] | World Cup qualifying match | Mass fight among fans of two teams | 2 deaths Unknown injuries | October 1976 |
| Port-au-Prince, Haiti [41] | World Cup qualifying match | Human crush and gunshots sparked by panic after firecracker | 6 deaths | December 1976 |
| Piraeus, Greece Karaiskakis Stadium [36] | Derby football match | Human crush among fans exiting stadium through the partially closed exit | 21 deaths 55 injured | February 1981 |
| Moscow, Soviet Union Central Lenin Stadium [42] | European Cup match | Human crush and asphyxiation between exiting and returning fans | 66 deaths 61 injured | October 1982 |
| Bradford, UK Valley Parade stadium [43] | English league football match | Fire in the Valley Parade stadium | 56 deaths 240 injured | May 1985 |
| Brussels, Belgium Heysel Stadium [44] | European Champions Cup Final match | Human crush among Italian fans escaping English fans against a collapsing wall | 39 deaths 600 injured | May 1985 |
| Tripoli, Libya Tripoli International Stadium [45] | Football match | Human crush sparked by knife-wielding fan and triggering the collapse of a part of the stadium | 20 deaths Unknown injuries | March 1987 |
| Kathmandu, Nepal Dasarath Rangasala Stadium [46] | International football match | Human crush against closed stadium exit sparked by a hailstorm | 93 deaths 100 injured | March 1988 |
| Sheffield, UK Hillsborough Stadium [35] | The FA Cup semi-final match | Human crush due to overcrowding during the influx of fans | 96 deaths 766 injured | April 1989 |
| Orkney, South Africa Oppenheimer Stadium [47] | A friendly association football match | Human crush among fans escaping from fan brawls | 43 deaths 100 injured | January 1991 |
| Bastia, the French island of Corsica Stade Armand Cesari [48] | French Cup semi-final match | Stadium terrace collapse underneath fans before the match | 17 deaths 1900 injured | May 1992 |
| Lusaka, Zambia Independence Stadium [45] | World Cup qualifying game. | Human crush during overcrowded fan exit celebrating victory | 15 deaths 52 injured | June 1996 |
| Guatemala City, Guatemala Estadio Doroteo Guamuch Flores [45] | World Cup qualifying match | Human crush due to overcrowding during the influx of fans | 83 deaths 140 injured | October 1996 |
| Harare, Zimbabwe National Sports Stadium [49] | World Cup qualifying match | Human crush during overcrowded fan exit after police fired tear gas | 13 deaths Unknown injuries | July 2000 |
| Salvador, Brazil Estádio Fonte Nova [45] | Local derby match | Upper terrace collapse | 7 deaths 10 injuries | 2007 |
| Johannesburg, South Africa Ellis Park Stadium [47] | South African league match | Human crush due to overcrowding during the influx of fans | 43 deaths Unknown injuries | April 2001 |
| Abidjan, Ivory Coast Stade Félix Houphouët-Boigny [50] | World Cup qualification match | Human crush due to overcrowding of fans before the match after police fired tear gas | 20 deaths 135 injuries | March 2009 |
| Port Said, Egypt Port Said Stadium [51] | Egyptian Premier League football match | Human crush among fans exiting the stadium | 74 deaths Unknown injuries | February 2012 |
| Kinshasa, Congo Tata Raphaël Stadium [45] | Congo league match | Human crush among fans sparked by police firing tear gas | 15 deaths 24 injuries | May 2014 |
| Cairo, Egypt Air Defense Stadium [52] | Egyptian Premier League football match | Human crush due to overcrowding during the influx of fans sparked by police firing tear gas | 28 deaths Unknown injuries | February 2015 |
| 1 | The category of the event (music festivals, exhibitions, or sports competitions, etc.) |
| 2 | The expected number of attendees |
| 3 | The criteria of attendees (families, sports club fans, community support groups, international stars, or VIP) |
| 4 | The nature of attendees’ movements (static audience, young children who need constant monitoring, people with motor disabilities, people who require personal assistance) |
| 5 | The age group of attendees |
| 6 | The site of the event (open area, specific walled area, inside a building, spacious or narrow area) |
| 7 | Available health resources (district hospitals, public hospitals, small hospitals, mobile clinic) |
| 8 | The distance to the nearest public or reference hospital |
| 9 | Time for the nearest general or reference hospital |
| 10 | Duration of the event per day |
| 11 | The number of days for the event |
| 12 | Possibility of drugs misuse |
| 13 | The time of the event |
| 14 | The expected temperature at the venue of the event |
| 15 | Types of activities in the event (high-risk activities, high competition among participants (ex: wrestling), the interaction between the attendees (for example the final matches), presence of cars or vehicles, including offers or race, presence of fireworks, presence of firearms or flames) |
| 16 | Accidents that occurred in previous activities or the same place or expected accidents |
| 17 | Food catering services (applying and controlling the specified standards for food catering services, municipality approval is obtained, and valid food catering services are provided) |
| Low-risk events | Events categorized as low severity recommend risk communication (at the population level), improved monitoring and surveillance, and medical care for the event |
| Medium-risk events | Medium severity events recommend risk communication (dedicated to the event), active surveillance, medical care for the event, and protective measures for the event (personal protective equipment, handwashing) |
| High-risk events | High-risk events recommend reducing the number of guests/visitors, adjustment of the crowd flow and seating arrangements, and reducing communication between participants, regulators, and service providers |
| Severe-risk events | Events with severe risk recommend restructuring the event, changing or moving the event site, postponing or rescheduling the event, or canceling the event |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Khan, A.A.; Sabbagh, A.Y.; Ranse, J.; Molloy, M.S.; Ciottone, G.R. Mass Gathering Medicine in Soccer Leagues: A Review and Creation of the SALEM Tool. Int. J. Environ. Res. Public Health 2021, 18, 9973. https://doi.org/10.3390/ijerph18199973
Khan AA, Sabbagh AY, Ranse J, Molloy MS, Ciottone GR. Mass Gathering Medicine in Soccer Leagues: A Review and Creation of the SALEM Tool. International Journal of Environmental Research and Public Health. 2021; 18(19):9973. https://doi.org/10.3390/ijerph18199973
Chicago/Turabian StyleKhan, Anas A., Abdulrahman Y. Sabbagh, Jamie Ranse, Michael S. Molloy, and Gregory R. Ciottone. 2021. "Mass Gathering Medicine in Soccer Leagues: A Review and Creation of the SALEM Tool" International Journal of Environmental Research and Public Health 18, no. 19: 9973. https://doi.org/10.3390/ijerph18199973
APA StyleKhan, A. A., Sabbagh, A. Y., Ranse, J., Molloy, M. S., & Ciottone, G. R. (2021). Mass Gathering Medicine in Soccer Leagues: A Review and Creation of the SALEM Tool. International Journal of Environmental Research and Public Health, 18(19), 9973. https://doi.org/10.3390/ijerph18199973






