Mental Resilience of Medical Practitioners in Singapore during COVID-19: Survey Results from a Webinar Course on Resilience
Abstract
:1. Introduction
2. Method
2.1. Participants
2.2. Measures
2.3. Data Analyses
3. Results
3.1. Sample Characteristics
3.2. Main Analyses
3.3. Impact of COVID-19 Exposure
3.3.1. Domain: Family and Friends
3.3.2. Domain: Myself
3.3.3. Domain: Practice/Work Setting
3.4. Impact of Practice/Work Setting
3.4.1. Domain: Family and Friends
3.4.2. Domain: Myself
3.4.3. Domain: Community
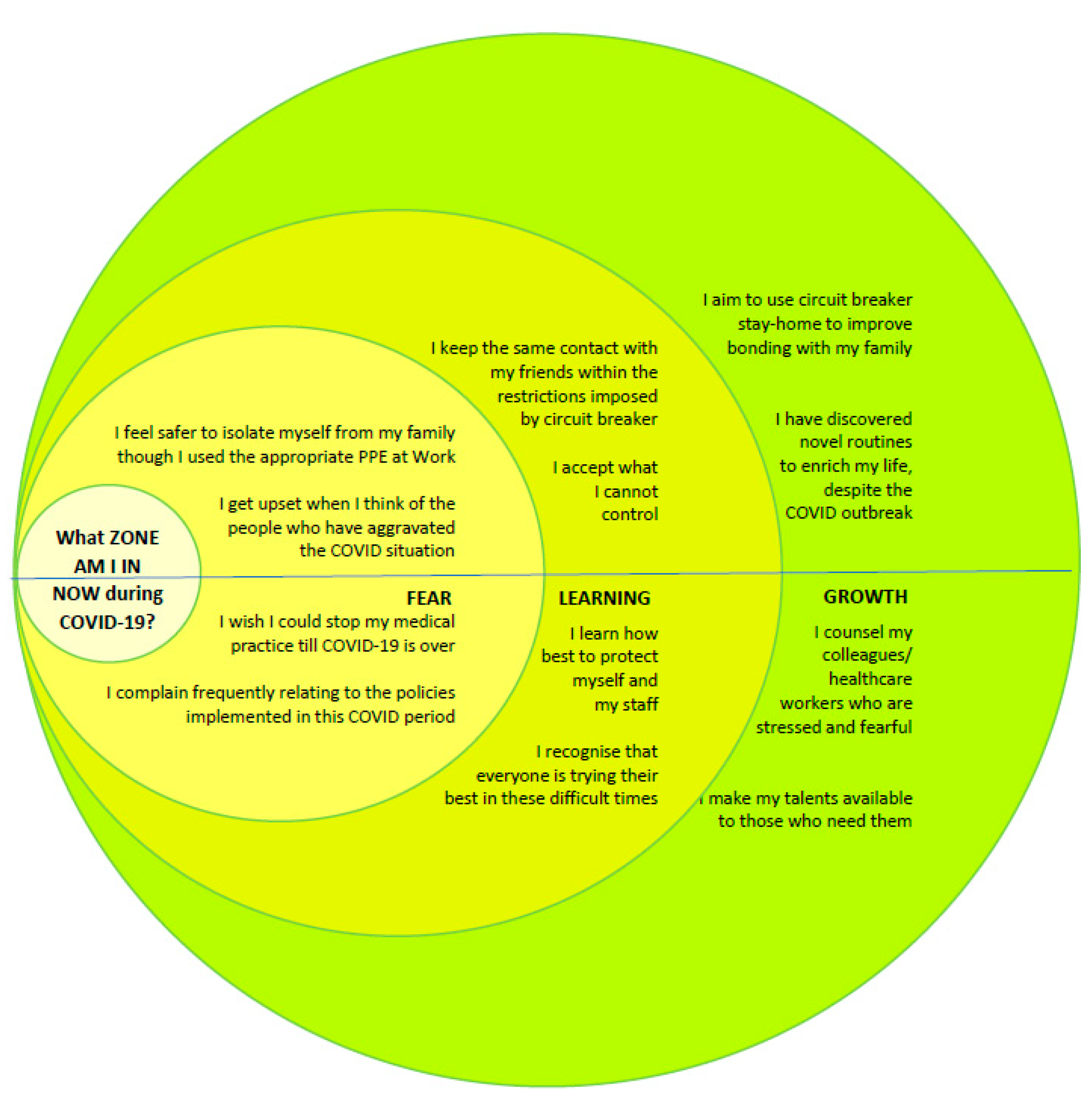
3.5. What Zone Am I in Now?
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- World Health Organization. Coronavirus Disease (COVID-19) Dashboard. Available online: https://covid19.who.int/ (accessed on 19 April 2021).
- Sahu, A.K.; Amrithanand, V.T.; Mathew, R.; Aggarwal, P.; Nayer, J.; Bhoi, S. COVID-19 in health care workers—A systematic review and meta-analysis. Am. J. Emerg. Med. 2020, 38, 1727–1731. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, L.H.; Drew, D.A.; Graham, M.A.; Joshi, A.D.; Guo, C.G.; Ma, W.; Mehta, R.S.; Warner, E.T.; Sikavi, D.R.; Lo, C.H.; et al. Risk of COVID-19 among front-line health-care workers and the general community: A prospective cohort study. Lancet Public Health 2020, 5, E475–E483. [Google Scholar] [CrossRef]
- Medscape. In Memoriam: Healthcare Workers Who Have Died of COVID-19. 2020. Available online: https://www.medscape.com/viewarticle/927976 (accessed on 7 December 2020).
- Worldometer. Available online: https://www.worldometers.info/coronovirus (accessed on 19 April 2021).
- Raudenská, J.; Steinerová, V.; Javůrková, A.; Urits, I.; Kaye, A.D.; Viswanath, O.; Varrassi, G. Occupational burnout syndrome and post-traumatic stress among healthcare professionals during the novel coronavirus disease 2019 (COVID-19) pandemic. Best Pract. Res. Clin. Anaesthesiol. 2020, 34, 553–560. [Google Scholar] [CrossRef] [PubMed]
- Spoorthy, M.S.; Pratapa, S.K.; Mahant, S. Mental health problems faced by healthcare workers due to the COVID-19 pandemic—A review. Asian J. Psychiatr. 2020, 51, 102119. [Google Scholar] [CrossRef] [PubMed]
- Robertson, H.D.; Elliott, A.M.; Burton, C.; Iversen, L.; Murchie, P.; Porteous, T.; Matheson, C. Resilience of primary healthcare professionals: A systematic review. Br. J. Gen. Pract. 2016, 66, e423–e433. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Di Monte, C.; Monaco, S.; Mariani, R.; Di Trani, M. From Resilience to Burnout: Psychological features of Italian general practitioners during COVID-19 emergency. Front. Psychol. 2020, 11, 577201. [Google Scholar] [CrossRef] [PubMed]
- Health, C.; Sommerfield, A.; von Sternberg-Ungern, B.S. Resilience strategies to manage psychological distress among healthcare workers during the COVID-19 pandemic: A narrative review. Anaesthesia 2020, 75, 1364–1371. [Google Scholar] [CrossRef] [PubMed]
- Seçer, İ.; Ulaş, S.; Karaman-Özlü, Z. The effect of the fear of COVID-19 on healthcare ‘professionals’ psychological adjustment skills: Mediating role of experiential avoidance and psychological resilience. Front. Psychol. 2020, 11, 561536. [Google Scholar] [CrossRef] [PubMed]
- COVID-19: Singapore Experience. The Singapore Family Physician. 2020. Available online: https://www.cfps.org.sg/publications/the-singapore-family-physician/issue/188 (accessed on 6 April 2021).
- Cawcutt, K.A.; Starlin, R.; Rupp, M.E. Fighting fear in healthcare workers during the COVID-19 pandemic. Infect. Control Hosp. Epidemiol. 2020, 41, 1192–1193. [Google Scholar] [CrossRef] [PubMed]
- Martin-Delgado, J.; Viteri, E.; Mula, A.; Serpa, P.; Pacheco, G.; Prada, D.; Campos de Andrade Lourenção, D.; Campos Pavan Baptista, P.; Ramirez, G.; Mira, J.J. Availability of personal protective equipment and diagnostic and treatment facilities for healthcare workers involved in COVID-19 care: A cross-sectional study in Brazil, Colombia, and Ecuador. PLoS ONE 2020, 15, e0242185. [Google Scholar] [CrossRef] [PubMed]
- Chua, A.Q.; Tan, M.M.J.; Verma, M.; Han, E.K.L.; Hsu, L.Y.; Cook, A.R.; Teo, Y.Y.; Lee, V.J.; Legido-Quigley, H. Health system resilience in managing the COVID-19 pandemic: Lessons from Singapore. BMJ Global Health 2020, 5, e003317. [Google Scholar] [CrossRef] [PubMed]
- Walton, M.; Murray, E.; Christian, M.D. Mental health care for medical staff and affiliated healthcare workers during the COVID-19 pandemic. Eur. Heart J. Acute Cardiovasc. Care 2020, 9, 241–247. [Google Scholar] [CrossRef] [PubMed]
- Tomlin, J.; Dalgleish-Warburton, B.; Lamph, G. Psychosocial support for healthcare workers during the COVID-19 pandemic. Front. Psychol. 2020, 11, 1960. [Google Scholar] [CrossRef] [PubMed]
- Taylor, S.; Landry, C.A.; Rachor, G.S.; Paluszek, M.M.; Asmundson, G.J. Fear and avoidance of healthcare workers: An important, under-recognized form of stigmatization during the COVID-19 pandemic. J. Anxiety Disord. 2020, 75, 102289. [Google Scholar] [CrossRef] [PubMed]
- Abdelhafiz, A.S.; Alorabi, M. Social stigma: The hidden threat of COVID-19. Front. Public Health. 2020, 8, 429. [Google Scholar] [CrossRef] [PubMed]
- Dye, T.D.; Alcantara, L.; Siddiqi, S.; Barbosu, M.; Sharma, S.; Panko, T.; Pressman, E. Risk of COVID-19-related bullying, harassment and stigma among healthcare workers: An analytical cross-sectional global study. BMJ Open 2020, 10, e046620. [Google Scholar] [CrossRef]
- De Brier, N.; Stroobants, S.; Vandekerckhove, P.; De Buck, E. Factors affecting mental health of health care workers during coronavirus disease outbreaks (SARS, MERS & COVID-19): A rapid systematic review. PLoS ONE 2020, 15, e0244052. [Google Scholar] [CrossRef]
- Sim, H.S.; How, C.H. Mental health and psychosocial support during healthcare emergencies—COVID-19 pandemic. Singap. Med. J. 2020, 61, 357–362. [Google Scholar] [CrossRef] [PubMed]
- Muller, R.A.E.; Stensland, R.S.Ø.; van de Velde, R.S. The mental health impact of the covid-19 pandemic on healthcare workers, and interventions to help them: A rapid systematic review. Psychiatry Res. 2020, 293, 113441. [Google Scholar] [CrossRef] [PubMed]
| Age | Area of Practice, n (%) | Total, n (100%) | |||
|---|---|---|---|---|---|
| Private Community | Public Community | Hospital | Others | ||
| 34 years and below | 20 (5.0%) | 4 (1.0%) | 6 (1.5) | 1 (0.2%) | 31 (7.7%) |
| 35–44 years old | 32 (7.9%) | 7 (1.7%) | 8 (2.0%) | 1 (0.2%) | 48 (11.9%) |
| 45–64 years old | 209 (51.9%) | 15 (3.7%) | 19 (4.7%) | 15 (3.7%) | 258 (64.0%) |
| 65 years and above | 50 (12.4%) | 5 (1.2%) | 2 (0.5%) | 9 (2.2%) | 66 (16.4%) |
| Total | 311 (77.2%) | 31 (7.7%) | 35 (8.7%) | 26 (6.5%) | 403 (100%) |
| Domains | Zones | ||
|---|---|---|---|
| Fear, n (%) | Learning, n (%) | Growth, n (%) | |
| Relating to family and friends | 137 (34.0%) | 108 (26.8%) | 158 (39.2%) |
| COVID Encounters | |||
| No | 40 (28.0%) | 32 (22.4%) | 71 (49.7%) |
| Positive outpatient | 56 (41.2%) | 38 (27.9%) | 42 (30.9%) |
| Suspect, later negative | 38 (32.2%) | 38 (32.2%) | 42 (35.6%) |
| Positive inpatient | 3 (50.0%) | 0 (0.0%) | 3 (50.0%) |
| Relating to myself | 47 (11.7%) | 201 (50.0%) | 155 (38.5%) |
| COVID Encounters | |||
| No | 15 (10.5%) | 73 (51.0%) | 55 (38.5%) |
| Positive outpatient | 9 (6.6%) | 74 (54.4%) | 53 (39.0%) |
| Suspect, later negative | 22 (18.6%) | 50 (42.4%) | 46 (39.0%) |
| Positive inpatient | 1 (16.7%) | 4 (66.7%) | 1 (16.7%) |
| Relating to my practice/workplace | 18 (4.5%) | 330 (81.9%) | 55 (13.6%) |
| COVID Encounters | |||
| No | 8 (5.6%) | 114 (79.7%) | 21 (14.7%) |
| Positive outpatient | 3 (2.2%) | 112 (82.4%) | 21 (15.4%) |
| Suspect, later negative | 5 (4.2%) | 100 (84.7%) | 13 (11.0%) |
| Positive inpatient | 2 (33.3%) | 4 (66.7%) | 0 (0.0%) |
| Relating to the community | 20 (5.0%) | 329 (81.6%) | 56 (13.9%) |
| COVID Encounters | |||
| No | 3 (2.1%) | 121 (84.6%) | 19 (13.3%) |
| Positive outpatient | 8 (5.9%) | 106 (77.9%) | 22 (16.2%) |
| Suspect, later negative | 7 (5.9%) | 96 (81.4%) | 15 (12.7%) |
| Positive inpatient | 2 (33.3%) | 4 (66.7%) | 0 (0.0%) |
| Domains | Zones | ||
|---|---|---|---|
| Fear, n (%) | Learning, n (%) | Growth, n (%) | |
| Relating to Family and friends | |||
| Area of Practice | |||
| Hospital | 10 (28.6%) | 10 (28.6%) | 15 (42.8%) |
| Others | 7 (26.9%) | 4 (15.4%) | 15 (57.7%) |
| Private community | 107 (34.4%) | 84 (27.0%) | 120 (38.6%) |
| Public community | 13 (41.9%) | 10 (32.3%) | 8 (25.8%) |
| Relating to Myself | |||
| Area of Practice | |||
| Hospital | 3 (8.6%) | 23 (65.7%) | 9 (25.7%) |
| Others | 2 (7.7%) | 10 (38.5%) | 14 (53.8%) |
| Private community | 38 (12.2%) | 155 (49.8%) | 118 (38.0%) |
| Public community | 4 (12.9%) | 13 (41.9%) | 14 (45.2%) |
| Relating to my Practice/workplace | |||
| Area of Practice | |||
| Hospital | 1(2.9%) | 28 (80.0%) | 8 (17.1%) |
| Others | 0 (0.0%) | 20 (76.9%) | 6 (23.1%) |
| Private community | 14 (4.5%) | 258 (83.0%) | 39 (12.5%) |
| Public community | 3 (9.7%) | 24 (77.4%) | 4 (12.9%) |
| Relating to the Community | |||
| Area of Practice | |||
| Hospital | 1(2.9%) | 24 (68.6%) | 10 (28.6%) |
| Others | 0 (0.0%) | 24 (92.3%) | 2 (7.7%) |
| Private community | 15 (4.8%) | 257 (82.6%) | 39 (12.5%) |
| Public community | 4 (12.9%) | 22 (71.0%) | 5 (16.1%) |
| Domains | Zones | |||
|---|---|---|---|---|
| Fear, n (%) | Learning, n (%) | Growth, n (%) | Mixed, n (%) | |
| Age group | ||||
| N = 403 | 5 (1.2%) | 202 (50.1%) | 29 (7.2%) | 167 (41.4%) |
| ≤34 | 1 (3.2%) | 14 (45.2%) | 1 (3.2%) | 15 (48.4%) |
| 35–44 | 1 (2.1%) | 18 (37.5%) | 2 (4.2%) | 27 (56.3%) |
| 45–64 | 3 (1.2%) | 136 (57.2%) | 23 (8.9%) | 96 (37.2%) |
| ≥65 | 0 (0.0%) | 34 (51.5%) | 3 (4.5%) | 29 (43.9%) |
| Area of Practice | ||||
| Hospital | 1 (2.9%) | 20 (57.2%) | 4 (11.4%) | 10 (28.6%) |
| Others | 0 (0.0%) | 11 (42.3%) | 5 (19.2%) | 10 (38.5%) |
| Private Community | 3 (1.0%) | 159 (51.1%) | 16 (5.1%) | 133 (42.8%) |
| Public Community | 1 (3.2%) | 12 (38.7%) | 4 (12.9%) | 14 (45.2%) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Low, C.H.C.; Goh, T.J.; Chan, Y.H.; Fung, D.S.S.; Cheong, P.Y. Mental Resilience of Medical Practitioners in Singapore during COVID-19: Survey Results from a Webinar Course on Resilience. Int. J. Environ. Res. Public Health 2021, 18, 9801. https://doi.org/10.3390/ijerph18189801
Low CHC, Goh TJ, Chan YH, Fung DSS, Cheong PY. Mental Resilience of Medical Practitioners in Singapore during COVID-19: Survey Results from a Webinar Course on Resilience. International Journal of Environmental Research and Public Health. 2021; 18(18):9801. https://doi.org/10.3390/ijerph18189801
Chicago/Turabian StyleLow, Cheng Hong Charity, Tze Jui Goh, Yiong Huak Chan, Daniel Shuen Sheng Fung, and Pak Yean Cheong. 2021. "Mental Resilience of Medical Practitioners in Singapore during COVID-19: Survey Results from a Webinar Course on Resilience" International Journal of Environmental Research and Public Health 18, no. 18: 9801. https://doi.org/10.3390/ijerph18189801
APA StyleLow, C. H. C., Goh, T. J., Chan, Y. H., Fung, D. S. S., & Cheong, P. Y. (2021). Mental Resilience of Medical Practitioners in Singapore during COVID-19: Survey Results from a Webinar Course on Resilience. International Journal of Environmental Research and Public Health, 18(18), 9801. https://doi.org/10.3390/ijerph18189801






