Racial Disparities in Health Risk Indicators Reported by Alabamians Diagnosed with COPD
Abstract
:1. Introduction
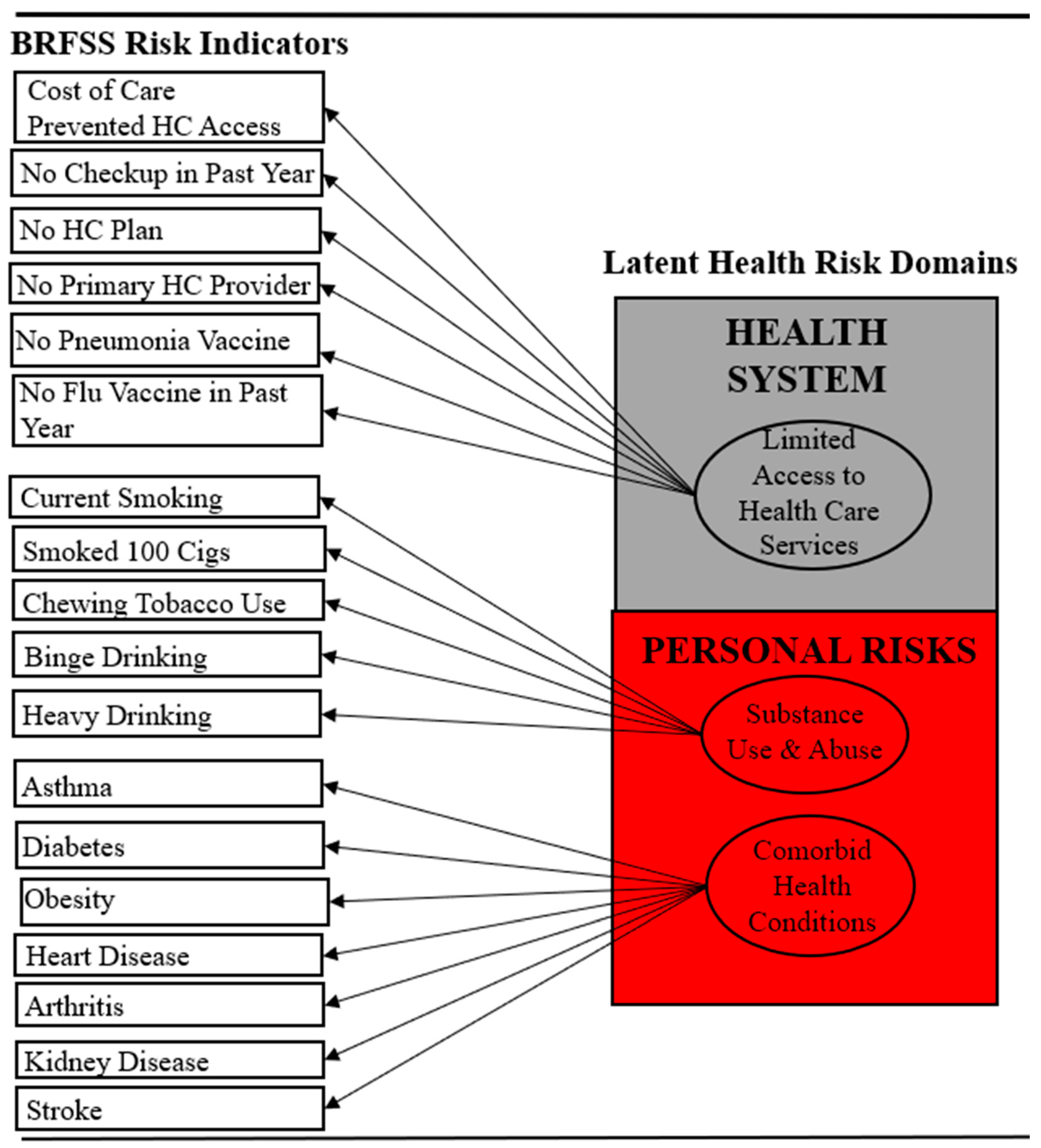
- Most Alabamians with COPD would be classified at high risk on the three health-related domains (i.e., comorbidities, substance use and abuse, and access to healthcare services); and
- The prevalence of health indicators making up each latent domain would differ according to race when most Alabamians with COPD were at intermediate or high (i.e., elevated) risk.
2. Materials and Methods
3. Results
3.1. Comorbidities
3.2. Substance Use Behaviors
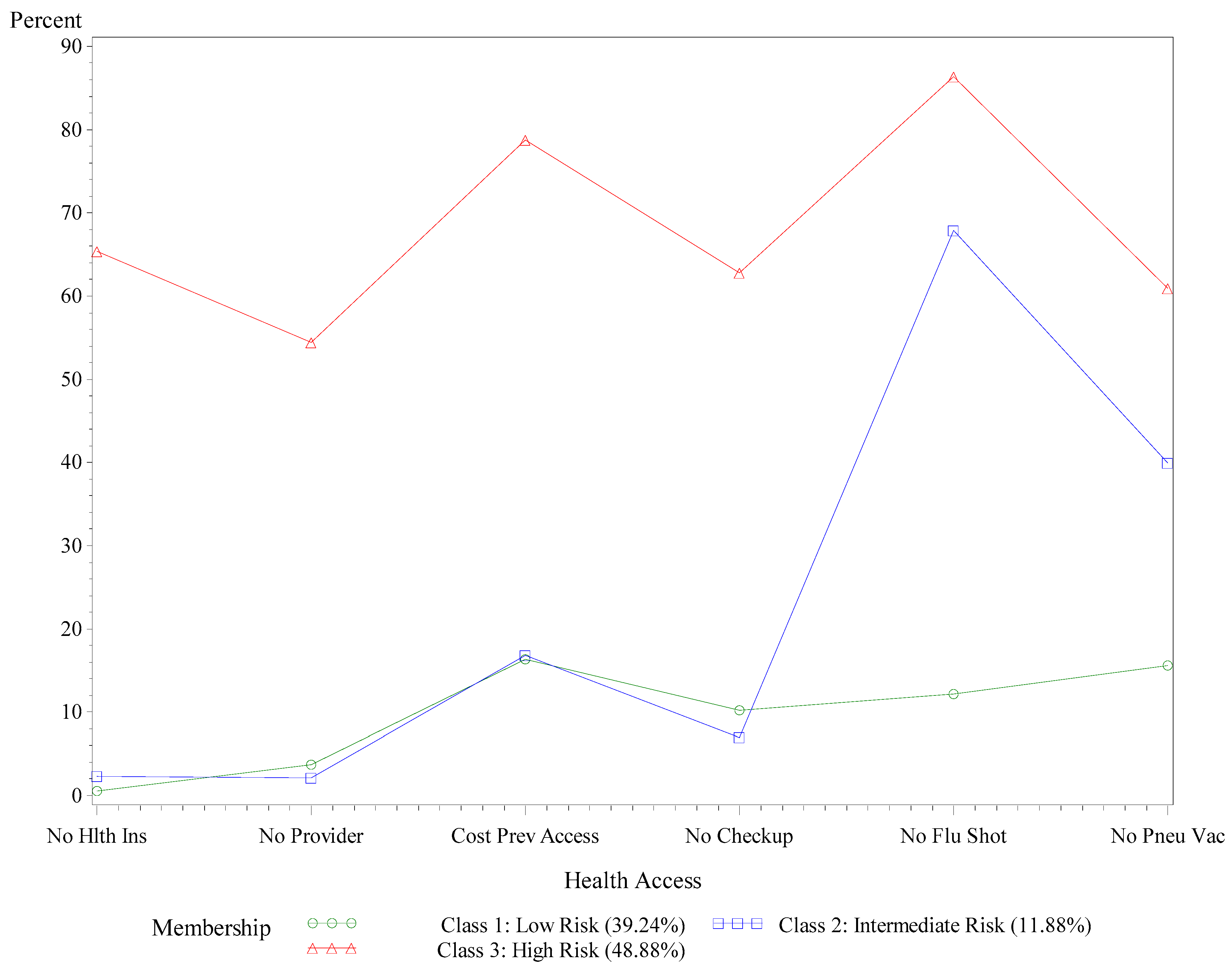
3.3. Healthcare Access
3.4. Racial Disparities in Risk Classes for Comorbidity and Limited Healthcare Access
4. Discussion
Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Greenlund, K.J.; Liu, M.M.Y.; Deokar, M.A.J.; Wheaton, A.G.; Croft, J.B. Association of Chronic Obstructive Pulmonary Disease With Increased Confusion or Memory Loss and Functional Limitations Among Adults in 21 States, 2011 Behavioral Risk Factor Surveillance System. Prev. Chronic Dis. 2016, 13, E02. [Google Scholar] [CrossRef] [Green Version]
- Wheaton, A.G.; Cunningham, T.J.; Ford, E.S.; Croft, J.B. Employment and Activity Limitations among Adults with Chronic Obstructive Pulmonary Disease—United States, 2013. MMWR Morb. Mortal. Wkly. Rep. 2015, 64, 289–295. [Google Scholar] [PubMed]
- Tselebis, A.; Pachi, A.; Ilias, I.; Kosmas, E.; Moussas, G.; Nikos, N.T.; Bratis, D. Strategies to improve anxiety and depression in patients with COPD: A mental health perspective. Neuropsychiatr. Dis. Treat. 2016, 12, 297–328. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kiley, J.P.; Gibbons, G.H. COPD national action plan: Addressing a public health need together. Chest 2017, 152, 698–699. [Google Scholar] [CrossRef] [Green Version]
- Sullivan, J.; Pravosud, V.; Mannino, D.M.; Siegel, K.; Choate, R.; Sullivan, T. National and State Estimates of COPD Morbidity and Mortality—United States, 2014–2015. Chronic Obstr. Pulm. Dis. J. COPD Found. 2018, 5, 324–333. [Google Scholar] [CrossRef]
- Croft, J.B.; Wheaton, A.G.; Liu, Y.; Xu, F.; Lu, H.; Matthews, K.; Cunningham, T.J.; Wang, Y.; Holt, J.B. Urban-Rural County and State Differences in Chronic Obstructive Pulmonary Disease—United States, 2015. MMWR Morb. Mortal. Wkly. Rep. 2018, 67, 205–211. [Google Scholar] [CrossRef] [Green Version]
- Centers for Disease Control and Prevention. Stats of the States—Alabama. Available online: https://www.cdc.gov/nchs/pressroom/states/alabama/al.htm (accessed on 13 July 2021).
- LiveStories. Alabama COPD and Asthma Death Statistics. Available online: https://www.livestories.com/statistics/alabama/copd-asthma-deaths-mortality (accessed on 13 July 2021).
- COPD in the United States: How Is Your State Doing? Alabama. Available online: https://www.copdfoundation.org/Portals/0/StateAssessmentCards/SAC_AL_2018.pdf (accessed on 13 July 2021).
- Centers for Disease Control and Prevention. Chronic Obstructive Pulmonary Disease (COPD) in Alabama. Available online: https://www.cdc.gov/copd/maps/docs/pdf/AL_COPDFactSheet.pdf (accessed on 13 July 2021).
- Centers for Disease Control and Prevention (CDC). Chronic obstructive pulmonary disease among adults—United States, 2011. MMWR Morb. Mortal. Wkly. Rep. 2012, 61, 938–943. [Google Scholar]
- Ejike, C.O.; Dransfield, M.T.; Hansel, N.N.; Putcha, N.; Raju, S.; Martinez, C.H.; Han, M.K. Chronic Obstructive Pulmonary Disease in America’s Black Population. Am. J. Respir. Crit. Care Med. 2019, 200, 423–430. [Google Scholar] [CrossRef]
- Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Division of Population Health. BRFSS Prevalence & Trends Data. 2015. Available online: https://www.cdc.gov/brfss/brfssprevalence/ (accessed on 7 July 2021).
- Mamary, A.J.; Stewart, J.I.; Kinney, G.L.; Hokanson, J.E.; Shenoy, K.; Dransfield, M.T.; Foreman, M.G.; Vance, G.B.; Criner, G.J. Race and Gender Disparities are Evident in COPD Underdiagnoses Across all Severities of Measured Airflow Obstruction. Chronic Obstr. Pulm. Dis. J. COPD Found. 2018, 5, 177–184. [Google Scholar] [CrossRef] [PubMed]
- Au, D.H.; Feemster, L.C. Chronic Obstructive Pulmonary Disease. Health Disparity and Inequity. Ann. Am. Thorac. Soc. 2014, 11, 1250–1251. [Google Scholar] [CrossRef]
- Pleasants, A.R.; Riley, I.L.; Mannino, D. Defining and targeting health disparities in chronic obstructive pulmonary disease. Int. J. Chronic Obstr. Pulm. Dis. 2016, 11, 2475–2496. [Google Scholar] [CrossRef] [Green Version]
- Mannino, D.M.; Homa, D.M.; Akinbami, L.; Ford, E.S.; Redd, S.C. Chronic obstructive pulmonary disease surveillance—United States, 1971–2000. MMWR Surveill. Summ. 2002, 51, 1–16. [Google Scholar]
- Han, M.K.; Curran-Everett, D.; Dransfield, M.T.; Criner, G.J.; Zhang, L.; Murphy, J.R.; Hansel, N.N.; DeMeo, D.L.; Hanania, N.A.; Regan, E.A.; et al. Racial differences in quality of life in patients with COPD. Chest 2011, 140, 1169–1176. [Google Scholar] [CrossRef] [Green Version]
- Biener, A.I.; Decker, S.L.; Rohde, F. Prevalence and Treatment of Chronic Obstructive Pulmonary Disease (COPD) in the United States. JAMA 2019, 322, 602. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Drummond, M.B.; Wise, R.; Hansel, N.N.; Putcha, N. Comorbidities and Chronic Obstructive Pulmonary Disease: Prevalence, Influence on Outcomes, and Management. Semin. Respir. Crit. Care Med. 2015, 36, 575–591. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Woo, H.; Brigham, E.P.; Allbright, K.; Ejike, C.; Galiatsatos, P.; Jones, M.R.; Oates, G.R.; Krishnan, A.J.; Cooper, C.B.; Kanner, E.R.; et al. Racial Segregation and Respiratory Outcomes among Urban Black Residents with and at Risk of COPD. Am. J. Respir. Crit. Care Med. 2021, 204, 536–545. [Google Scholar] [CrossRef] [PubMed]
- Ejike, C.O.; Woo, H.; Galiatsatos, P.; Paulin, L.M.; Krishnan, J.A.; Cooper, C.B.; Couper, D.J.; Kanner, R.E.; Bowler, R.P.; Hoffman, E.A.; et al. Contribution of Individual and Neighborhood Factors to Racial Disparities in Respiratory Outcomes. Am. J. Respir. Crit. Care Med. 2021, 203, 987–997. [Google Scholar] [CrossRef] [PubMed]
- Parekh, T.; Patel, S.; Kim, Y.-I.; Cherrington, A.; Bhatia, S.; Dransfield, M. Gender and Racial Social Inequalities in Chronic Obstructive Pulmonary Disease. In D102. Optimizing Outcomes in Copd; American Thoracic Society: New York, NY, USA, 2019; p. 7125. [Google Scholar]
- Gillum, R.F. Chronic obstructive pulmonary disease in blacks and whites: Pulmonary function norms and risk factors. J. Natl. Med. Assoc. 1991, 83, 393–401. [Google Scholar]
- Centers for Disease Control and Prevention. BRFSS Survey Data and Documentation. Updated 11 October 2018. Available online: https://www.cdc.gov/brfss/annualdata/annual2017.html (accessed on 21 September 2020).
- Strauss, S.M.; Rindskopf, D.M.; Astone-Twerell, J.M.; Jarlais, D.C.D.; Hagan, H. Using latent class analysis to identify patterns of hepatitis C service provision in drug-free treatment programs in the U.S. Drug Alcohol Depend. 2006, 83, 15–24. [Google Scholar] [CrossRef]
- Monga, N.; Rehm, J.; Fischer, B.; Brissette, S.; Bruneau, J.; El-Guebaly, N.; Noël, L.; Tyndall, M.; Wild, C.; Leri, F.; et al. Using latent class analysis (LCA) to analyze patterns of drug use in a population of illegal opioid users. Drug Alcohol Depend. 2007, 88, 1–8. [Google Scholar] [CrossRef]
- Guo, J.; Wall, M.; Amemiya, Y. Latent class regression on latent factors. Biostatistics 2005, 7, 145–163. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Nylund, K.L.; Asparouhov, T.; Muthén, B.O. Deciding on the Number of Classes in Latent Class Analysis and Growth Mixture Modeling: A Monte Carlo Simulation Study. Struct. Equ. Model. Multidiscip. J. 2007, 14, 535–569. [Google Scholar] [CrossRef]
- Morin, A.J.; Litalien, D. Mixture Modeling for Lifespan Developmental Research. In Oxford Research Encyclopedia of Psychology; Oxford University Press: Oxford, UK, 2019. [Google Scholar]
- Morin, A.J.; Meyer, J.P.; Creusier, J.; Biétry, F. Multiple-Group Analysis of Similarity in Latent Profile Solutions. Organ. Res. Methods 2015, 19, 231–254. [Google Scholar] [CrossRef]
- Jiang, Y.; Zack, M.M. A Latent Class Modeling Approach to Evaluate Behavioral Risk Factors and Health-Related Quality of Life. Prev. Chronic Dis. 2011, 8, A137. [Google Scholar]
- Holt, J.; Zhang, X.; Croft, J.B.; Cantrell, P. Geographic disparities in chronic obstructive pulmonary disease (COPD) hospitalization among Medicare beneficiaries in the United States. Int. J. Chronic Obstr. Pulm. Dis. 2011, 6, 321–328. [Google Scholar] [CrossRef] [Green Version]
- Scott, A.; Wilson, R.F. Social determinants of health among African Americans in a rural community in the Deep South: An ecological exploration. Rural Remote Health 2011, 11, 1634. [Google Scholar] [CrossRef]
- Yin, H.-L.; Yin, S.-Q.; Lin, Q.-Y.; Xu, Y.; Xu, H.-W.; Liu, T. Prevalence of comorbidities in chronic obstructive pulmonary disease patients. Medicine 2017, 96, e6836. [Google Scholar] [CrossRef]
- Wheaton, A.G.; Ford, E.S.; Cunningham, T.J.; Croft, J.B. Chronic obstructive pulmonary disease, hospital visits, and comorbidities—National Survey of Residential Care Facilities, 2010. J. Aging Health 2015, 27, 480–499. [Google Scholar] [CrossRef] [Green Version]
- Cunningham, T.J.; Ford, E.S.; Rolle, I.V.; Wheaton, A.G.; Croft, J.B. Association of self-reported cigarette smoking with chronic obstructive pulmonary disease and co-morbid chronic conditions in the United States. COPD 2015, 12, 276–286. [Google Scholar] [CrossRef] [Green Version]
- Stellefson, M.; Paige, S.R.; Barry, A.E.; Wang, M.Q.; Apperson, A. Risk factors associated with physical and mental distress in people who report a COPD diagnosis: Latent class analysis of 2016 behavioral risk factor surveillance system data. Int. J. Chronic Obstr. Pulm. Dis. 2019, 14, 809. [Google Scholar] [CrossRef] [Green Version]
- Tzanakis, N.; Hillas, G.; Perlikos, F.; Tsiligianni, I. Managing comorbidities in COPD. Int. J. Chronic Obstr. Pulm. Dis. 2015, 10, 95–109. [Google Scholar] [CrossRef] [Green Version]
- Ma, Y.; Tong, H.; Zhang, X.; Wang, M.; Yang, J.; Wu, M.; Han, R.; Chen, M.; Hu, X.; Yuan, Y.; et al. Chronic obstructive pulmonary disease in rheumatoid arthritis: A systematic review and meta-analysis. Respir. Res. 2019, 20, 1–8. [Google Scholar] [CrossRef]
- Dhital, R.; Basnet, S.; Paudel, P.; Acharya, Y.P.; Poudel, D.R. Prevalence of chronic obstructive pulmonary disease (COPD) among rheumatoid arthritis: Results from national inpatient database. J. Community Hosp. Intern. Med. Perspect. 2018, 8, 211–214. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.; Wheaton, A.G.; Murphy, L.B.; Xu, F.; Croft, J.B.; Greenlund, K.J. Chronic Obstructive Pulmonary Disease and Arthritis among US Adults, 2016. Prev. Chronic Dis. 2019, 16, 190035. [Google Scholar] [CrossRef] [Green Version]
- Mcguire, K.; Aviña-Zubieta, J.A.; Esdaile, J.M.; Sadatsafavi, M.; Sayre, E.C.; Abrahamowicz, M.; Lacaille, D. Risk of incident chronic obstructive pulmonary disease in rheumatoid arthritis: A population-based cohort study. Arthritis Care Res. 2019, 71, 602–610. [Google Scholar] [CrossRef]
- Hyldgaard, C.; Bendstrup, E.; Pedersen, A.B.; Ulrichsen, S.P.; Løkke, A.; Hilberg, O.; Ellingsen, T. Increased mortality among patients with rheumatoid arthritis and COPD: A population-based study. Respir. Med. 2018, 140, 101–107. [Google Scholar] [CrossRef]
- Hyldgaard, C.; Løkke, A.; Pedersen, A.B.; Ulrichsen, S.P.; Hilberg, O.; Bendstrup, E.; Ellingsen, T. Prognosis in rheumatoid arthritis patients with COPD: A nationwide, registry-based study. Epidemiology 2017, 50, OA1786. [Google Scholar] [CrossRef]
- Wshah, A.; Guilcher, S.J.; Goldstein, R.; Brooks, D. Prevalence of osteoarthritis in individuals with COPD: A systematic review. Int. J. Chronic Obstr. Pulm. Dis. 2018, 13, 1207–1216. [Google Scholar] [CrossRef] [Green Version]
- Pumar, M.I.; Gray, C.R.; Walsh, J.R.; Yang, I.A.; Rolls, T.A.; Ward, D.L. Anxiety and depression—Important psychological comorbidities of COPD. J. Thorac. Dis. 2014, 6, 1615. [Google Scholar]
- He, Y.; Zhang, M.; Lin, E.H.B.; Bruffaerts, R.; Posada-Villa, J.; Angermeyer, M.C.; Levinson, D.; de Girolamo, G.; Uda, H.; Mneimneh, Z.; et al. Mental disorders among persons with arthritis: Results from the World Mental Health Surveys. Psychol. Med. 2008, 38, 1639–1650. [Google Scholar] [CrossRef] [PubMed]
- Li, Z.; Liu, S.; Wang, L.; Smith, L. Mind–Body Exercise for Anxiety and Depression in COPD Patients: A Systematic Review and Meta-Analysis. Int. J. Environ. Res. Public Health 2019, 17, 22. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Newham, J.J.; Presseau, J.; Heslop-Marshall, K.; Russell, S.; Ogunbayo, O.J.; Netts, P.; Hanratty, B.; Kaner, E. Features of self-management interventions for people with COPD associated with improved health-related quality of life and reduced emergency department visits: A systematic review and meta-analysis. Int. J. Chronic Obstr. Pulm. Dis. 2017, 12, 1705–1720. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lambert, A.A.; Putcha, N.; Drummond, M.B.; Boriek, A.M.; Hanania, N.A.; Kim, V.; Kinney, G.L.; McDonald, M.-L.N.; Brigham, E.; Wise, R.; et al. Obesity Is Associated With Increased Morbidity in Moderate to Severe COPD. Chest 2017, 151, 68–77. [Google Scholar] [CrossRef] [Green Version]
- Cecere, L.M.; Littman, A.J.; Slatore, C.G.; Udris, E.M.; Bryson, C.L.; Boyko, E.J.; Pierson, D.J.; Au, D.H. Obesity and COPD: Associated Symptoms, Health-related Quality of Life, and Medication Use. COPD J. Chronic Obstr. Pulm. Dis. 2011, 8, 275–284. [Google Scholar] [CrossRef] [PubMed]
- Iyer, A.S.; Dransfield, M.T. The “Obesity Paradox” in Chronic Obstructive Pulmonary Disease: Can It Be Resolved? Ann. Am. Thorac. Soc. 2018, 15, 158–159. [Google Scholar] [CrossRef] [PubMed]
- Wei, Y.-F.; Tsai, Y.-H.; Lin, M.-S.; Wang, C.-C.; Cheng, S.-L.; Hsu, W.-H.; Wu, Y.-K.; Chen, N.-H.; Lee, C.-H.; Hsu, J.-Y.; et al. The impact of overweight and obesity on acute exacerbations of COPD—Subgroup analysis of the Taiwan obstructive lung disease cohort. Gen. Pract. Prim. Care 2017, 12, 2723–2729. [Google Scholar] [CrossRef] [Green Version]
- Goto, T.; Hirayama, A.; Faridi, M.K.; Camargo, C.A.; Hasegawa, K. Obesity and Severity of Acute Exacerbation of Chronic Obstructive Pulmonary Disease. Ann. Am. Thorac. Soc. 2018, 15, 184–191. [Google Scholar] [CrossRef]
- Shaya, F.T.; Maneval, M.S.; Gbarayor, C.M.; Sohn, K.; Dalal, A.A.; Du, D.; Scharf, S.M. Burden of COPD, Asthma, and Concomitant COPD and Asthma Among Adults: Racial Disparities in a Medicaid Population. Chest 2009, 136, 405–411. [Google Scholar] [CrossRef] [Green Version]
- Lisspers, K.; Johansson, G.; Jansson, C.; Larsson, K.; Stratelis, G.; Hedegaard, M.; Ställberg, B. Improvement in COPD management by access to asthma/COPD clinics in primary care: Data from the observational PATHOS study. Respir. Med. 2014, 108, 1345–1354. [Google Scholar] [CrossRef] [Green Version]
- Gaffney, A.W.; Hawks, L.; Bor, D.; White, A.C.; Woolhandler, S.; McCormick, D.; Himmelstein, D.U. National Trends and Disparities in Health Care Access and Coverage Among Adults With Asthma and COPD. Chest 2021, 159, 2173–2182. [Google Scholar] [CrossRef]
- Sanei, F.; Wilkinson, T. Influenza vaccination for patients with chronic obstructive pulmonary disease: Understanding immunogenicity, efficacy and effectiveness. Ther. Adv. Respir. Dis. 2016, 10, 349–367. [Google Scholar] [CrossRef] [Green Version]
- U.S. Department of Health and Human Services. Increase the Proportion of People Who Get the Flu Vaccine Every Year—IID-09, Healthy People 2030. Available online: https://health.gov/healthypeople/objectives-and-data/browse-objectives/vaccination/increase-proportion-people-who-get-flu-vaccine-every-year-iid-09 (accessed on 16 April 2021).
- Kwizera, R.; Parkes-Ratanshi, R.; Page, I.D.; Sekaggya-Wiltshire, C.; Musaazi, J.; Fehr, J.; Castelnuovo, B.; Kambugu, A.; Denning, D.W. Elevated Aspergillus-specific antibody levels among HIV infected Ugandans with pulmonary tuberculosis. BMC Pulm. Med. 2017, 17, 1–9. [Google Scholar] [CrossRef]
- Leung, J.M.; Niikura, M.; Yang, C.W.T.; Sin, D.D. COVID-19 and COPD. Eur. Respir. J. 2020, 56, 2002108. [Google Scholar] [CrossRef]
- Balkissoon, R. Journal Club: The Intersection of Racial/Ethnic Disparities in Coronavirus Disease 2019 and COPD. Chronic Obstr. Pulm. Dis. J. COPD Found. 2021, 8, 292–302. [Google Scholar] [CrossRef] [PubMed]
- Stellefson, M.; Paige, S.; Wang, M.Q.; Chaney, B.H. Competency-Based Recommendations for Health Education Specialists to Prevent the Spread of COVID-19 among Adults with COPD. Am. J. Health Educ. 2021, 52, 18–22. [Google Scholar] [CrossRef]
- Stellefson, M.; Wang, M.Q.; Balanay, J.A.G.; Wu, R.; Paige, S.R. Latent Health Risk Classes Associated with Poor Physical and Mental Outcomes in Workers with COPD from Central Appalachian U.S. States. Int. J. Environ. Res. Public Health 2020, 17, 6798. [Google Scholar] [CrossRef] [PubMed]
- Lee, H.; Shin, S.H.; Gu, S.; Zhao, D.; Kang, D.; Joi, Y.R.; Suh, G.Y.; Pastor-Barriuso, R.; Guallar, E.; Cho, J.; et al. Racial differences in comorbidity profile among patients with chronic obstructive pulmonary disease. BMC Med. 2018, 16, 178. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Criner, G.J.; Make, B.J.; Koppel, G.A. Racial disparities: Another important barrier to pulmonary rehabilitation participation in patients with COPD Posthospitalization. Chest 2020, 157, 1070–1072. [Google Scholar] [CrossRef]
- Chatila, W.M.; Wynkoop, W.A.; Vance, G.; Criner, G.J. Smoking Patterns in African Americans and Whites with Advanced COPD. Chest 2004, 125, 15–21. [Google Scholar] [CrossRef]


| Comorbidities | White | Black | ||||
|---|---|---|---|---|---|---|
| Asthma | Yes n (%) | No n (%) | p-value | Yes n (%) | No n (%) | p-value |
| Low Risk | 368 (27.88) | 952 (72.12) | <0.0001 | 133 (30.09) | 309 (69.91) | <0.0001 |
| Intermediate Risk | 41 (10.85) | 337 (89.15) | 255 (63.91) | 144 (36.09) | ||
| High Risk | 775 (63.27) | 450 (36.73) | 7 (25.00) | 21 (75) | ||
| Diabetes | Yes n (%) | No n (%) | p-value | Yes n (%) | No n (%) | p-value |
| Low Risk | 0 (0.00) | 1324 (100) | <0.0001 | 60 (13.61) | 381 (86.39) | <0.0001 |
| Intermediate Risk | 286 (75.46) | 93 (24.54) | 217 (55.08) | 177 (44.92) | ||
| High Risk | 519 (42.51) | 702 (57.49) | 14 (51.85) | 13 (48.15) | ||
| Obesity | Yes n (%) | No n (%) | p-value | Yes n (%) | No n (%) | p-value |
| Low Risk | 224 (17.72) | 1040 (82.28) | <0.0001 | 133 (32.44) | 277 (67.56) | <0.0001 |
| Intermediate Risk | 166 (45.60) | 198 (54.40) | 301 (80.48) | 73 (19.52) | ||
| High Risk | 678 (57.56) | 500 (42.44) | 2 (7.69) | 24 (92.31) | ||
| Cardiovascular Disease (CVD) | Yes n (%) | No n (%) | p-value | Yes n (%) | No n (%) | p-value |
| Low Risk | 68 (5.23) | 1233 (94.77) | <0.0001 | 20 (4.59) | 416 (95.41) | <0.0001 |
| Intermediate Risk | 148 (39.57) | 226 (60.43) | 103 (26.21) | 290 (73.79) | ||
| High Risk | 423 (35.67) | 763 (64.33) | 23 (82.14) | 5 (17.86) | ||
| Arthritis | Yes n (%) | No n (%) | p-value | Yes n (%) | No n (%) | p-value |
| Low Risk | 704 (53.09) | 622 (46.91) | <0.0001 | 181 (41.42) | 256 (58.58) | <0.0001 |
| Intermediate Risk | 168 (44.09) | 213 (55.91) | 376 (94.24) | 23 (5.76) | ||
| High Risk | 1192 (97.47) | 31 (2.53) | 24 (85.71) | 4 (14.29) | ||
| Stroke | Yes n (%) | No n (%) | p-value | Yes n (%) | No n (%) | p-value |
| Low Risk | 66 (4.97) | 1261 (95.03) | <0.0001 | 25 (5.64) | 418 (94.36) | <0.0001 |
| Intermediate Risk | 29 (7.69) | 348 (92.31) | 86 (21.50) | 314 (78.50) | ||
| High Risk | 345 (28.21) | 878 (71.79) | 15 (53.57) | 13 (46.43) | ||
| Depressive Disorder | Yes n (%) | No n (%) | p-value | Yes n (%) | No n (%) | p-value |
| Low Risk | 413 (31.24) | 909 (68.76) | <0.0001 | 97 (22.25) | 339 (77.75) | <0.0001 |
| Intermediate Risk | 42 (11.02) | 339 (88.98) | 232 (58.00) | 168 (42.00) | ||
| High Risk | 855 (70.31) | 361 (29.69) | 16 (57.14) | 12 (42.86) | ||
| Chronic Kidney Disease | Yes n (%) | No n (%) | p-value | Yes n (%) | No n (%) | p-value |
| Low Risk | 16 (1.20) | 1313 (98.80) | <0.0001 | 10 (2.26) | 432 (97.74) | <0.0001 |
| Intermediate Risk | 41 (10.88) | 336 (89.12) | 43 (10.72) | 358 (89.28) | ||
| High Risk | 214 (17.60) | 1002 (82.40) | 28 (100.00) | 0 (0.00) | ||
| Healthcare Indicator | White | Black | ||||
|---|---|---|---|---|---|---|
| Access to Health Insurance | Yes n (%) | No n (%) | p-value | Yes n (%) | No n (%) | p-value |
| Low Risk | 1360 (99.34) | 9 (0.66) | <0.0001 | 186 (100) | 0 (0) | <0.0001 |
| Intermediate Risk | 1211 (98.06) | 24 (1.94) | 575 (96.48) | 21 (3.52) | ||
| High Risk | 135 (40.30) | 200 (59.70) | 5 (5.56) | 85 (94.44) | ||
| Primary Care Physician | Yes n (%) | No n (%) | p-value | Yes n (%) | No n (%) | p-value |
| Low Risk | 28 (2.05) | 1341 (97.95) | <0.0001 | 31 (16.67) | 155 (83.33) | <0.0001 |
| Intermediate Risk | 184 (55.09) | 1208 (97.66) | 11 (1.84) | 586 (98.16) | ||
| High Risk | 29 (2.34) | 150 (44.91) | 41 (45.56) | 49 (54.44) | ||
| Afford Medical Costs | Yes n (%) | No n (%) | p-value | Yes n (%) | No n (%) | p-value |
| Low Risk | 1198 (87.51) | 171 (12.49) | <0.0001 | 106 (56.99) | 80 (43.01) | <0.0001 |
| Intermediate Risk | 1030 (83.40) | 205 (16.60) | 494 (83.16) | 100 (16.84) | ||
| High Risk | 70 (20.96) | 264 (79.04) | 11 (12.22) | 79 (87.78) | ||
| Check-Up in Past Year | Yes n (%) | No n (%) | p-value | Yes n (%) | No n (%) | p-value |
| Low Risk | 1253 (92.47) | 102 (7.53) | <0.0001 | 138 (75) | 46 (25) | <0.0001 |
| Intermediate Risk | 1100 (90.53) | 115 (9.47) | 579 (97.64) | 14 (2.36) | ||
| High Risk | 105 (31.91) | 224 (68.09) | 47 (52.81) | 42 (47.19) | ||
| Annual Flu Shot | Yes n (%) | No n (%) | p-value | Yes n (%) | No n (%) | p-value |
| Low Risk | 1369 (100) | 0 (0) | <0.0001 | 5 (2.87) | 169 (97.13) | <0.0001 |
| Intermediate Risk | 142 (13.15) | 938 (86.85) | 336 (62.69) | 200 (37.31) | ||
| High Risk | 41 (13.23) | 269 (86.77) | 8 (9.88) | 73 (90.12) | ||
| Pneumococcal Vaccine | Yes n (%) | No n (%) | p-value | Yes n (%) | No n (%) | p-value |
| Low Risk | 778 (100) | 0 (0) | <0.0001 | 12 (9.30) | 117 (90.70) | <0.0001 |
| Intermediate Risk | 320 (45.58) | 382 (54.42) | 246 (84.54) | 45 (15.46) | ||
| High Risk | 67 (38.29) | 108 (61.71) | 16 (35.56) | 29 (64.44) | ||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Stellefson, M.; Wang, M.-Q.; Kinder, C. Racial Disparities in Health Risk Indicators Reported by Alabamians Diagnosed with COPD. Int. J. Environ. Res. Public Health 2021, 18, 9662. https://doi.org/10.3390/ijerph18189662
Stellefson M, Wang M-Q, Kinder C. Racial Disparities in Health Risk Indicators Reported by Alabamians Diagnosed with COPD. International Journal of Environmental Research and Public Health. 2021; 18(18):9662. https://doi.org/10.3390/ijerph18189662
Chicago/Turabian StyleStellefson, Michael, Min-Qi Wang, and Caitlin Kinder. 2021. "Racial Disparities in Health Risk Indicators Reported by Alabamians Diagnosed with COPD" International Journal of Environmental Research and Public Health 18, no. 18: 9662. https://doi.org/10.3390/ijerph18189662
APA StyleStellefson, M., Wang, M.-Q., & Kinder, C. (2021). Racial Disparities in Health Risk Indicators Reported by Alabamians Diagnosed with COPD. International Journal of Environmental Research and Public Health, 18(18), 9662. https://doi.org/10.3390/ijerph18189662






