ECG Ventricular Repolarization Dynamics during Exercise: Temporal Profile, Relation to Heart Rate Variability and Effects of Age and Physical Health
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Procedure
2.3. Data Recording
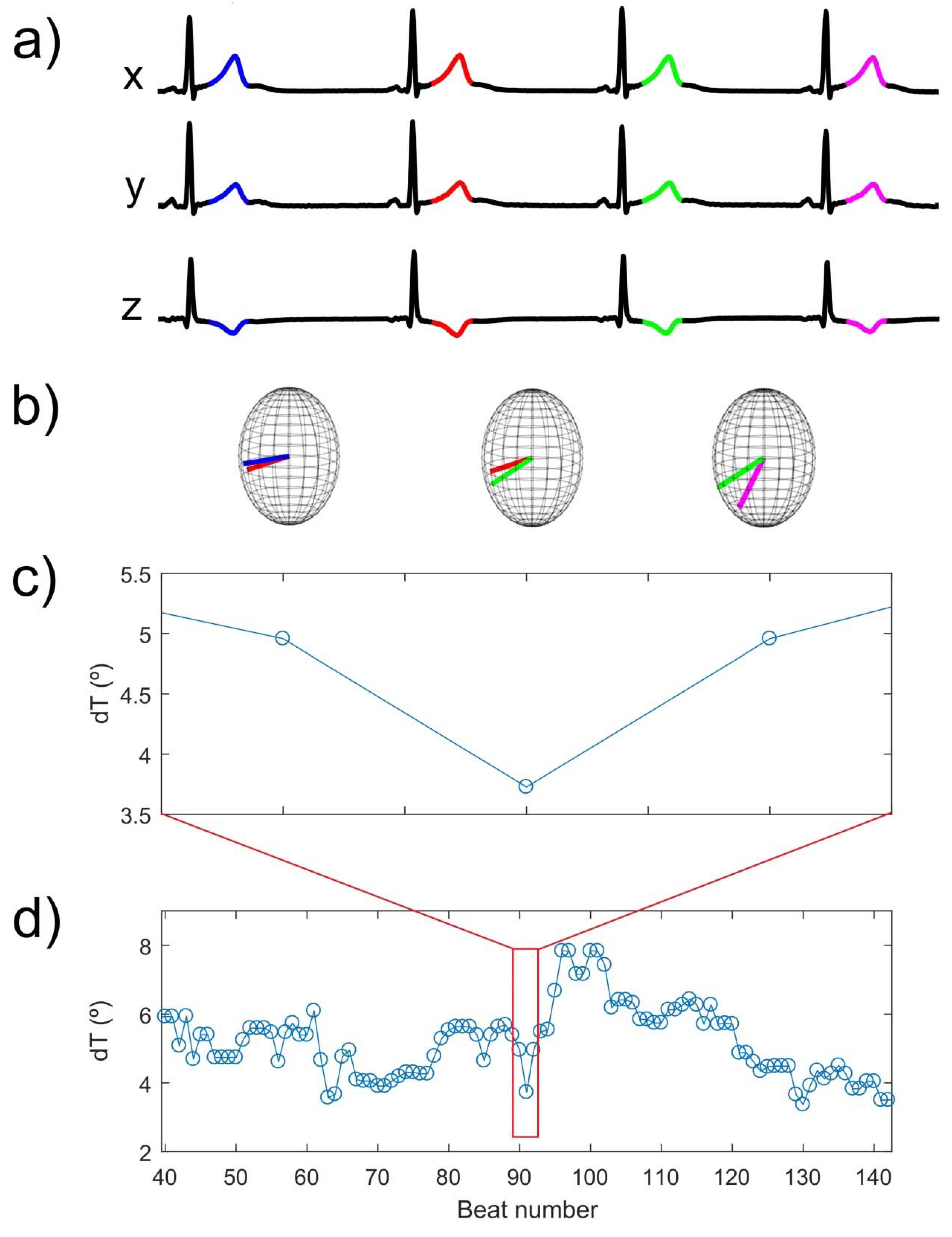
2.4. Data Analysis and Processing
2.5. Statistical Analysis
3. Results
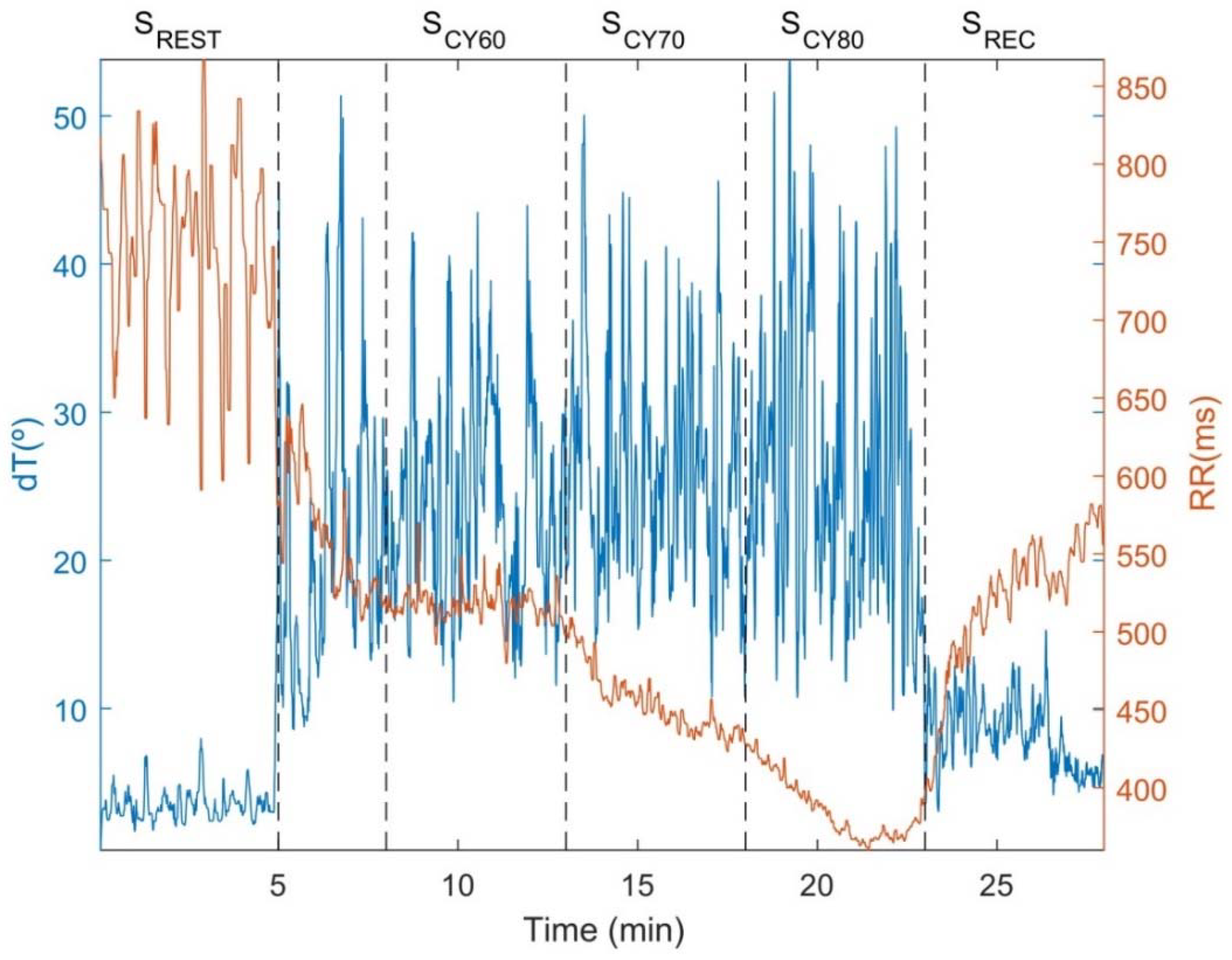
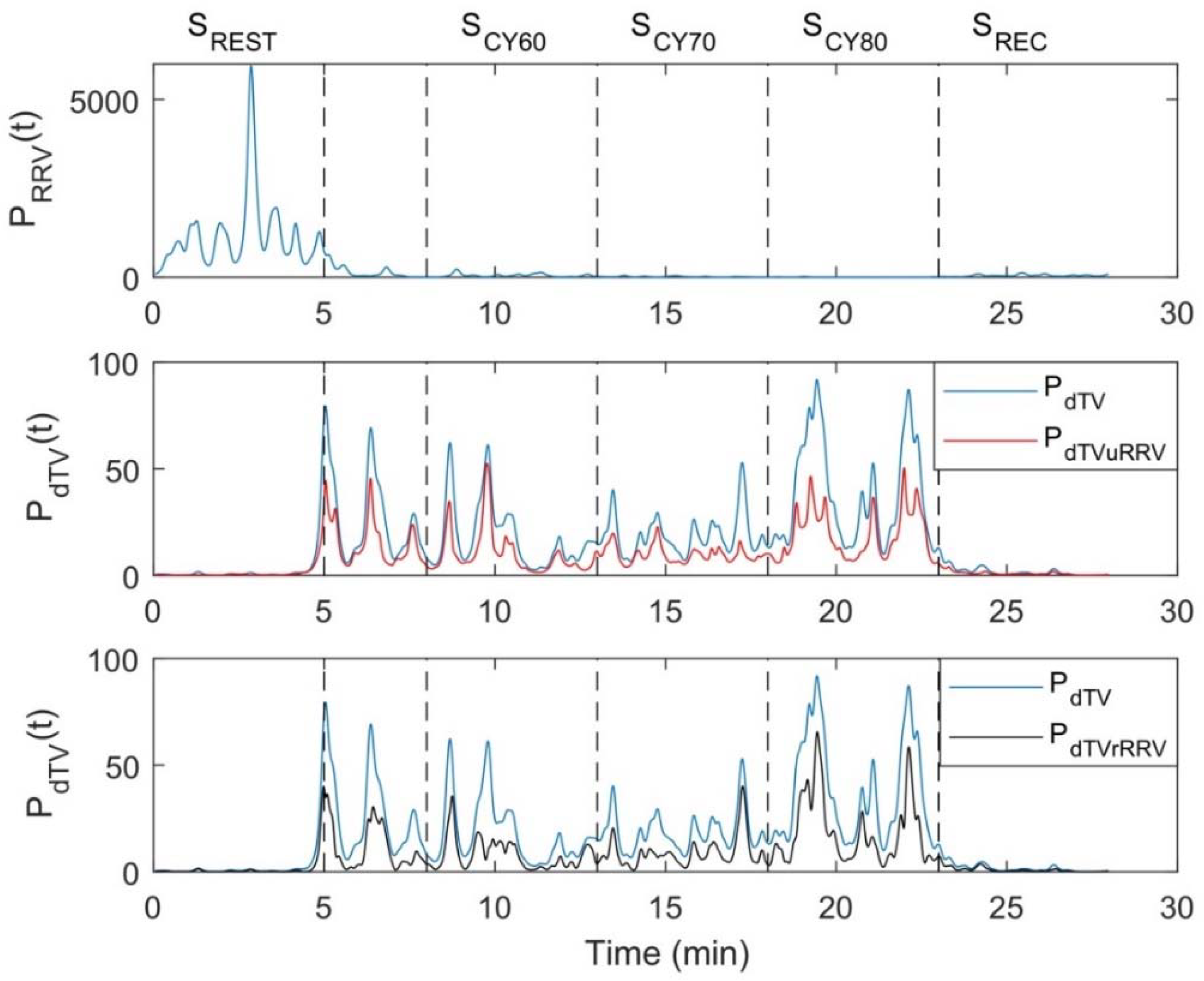
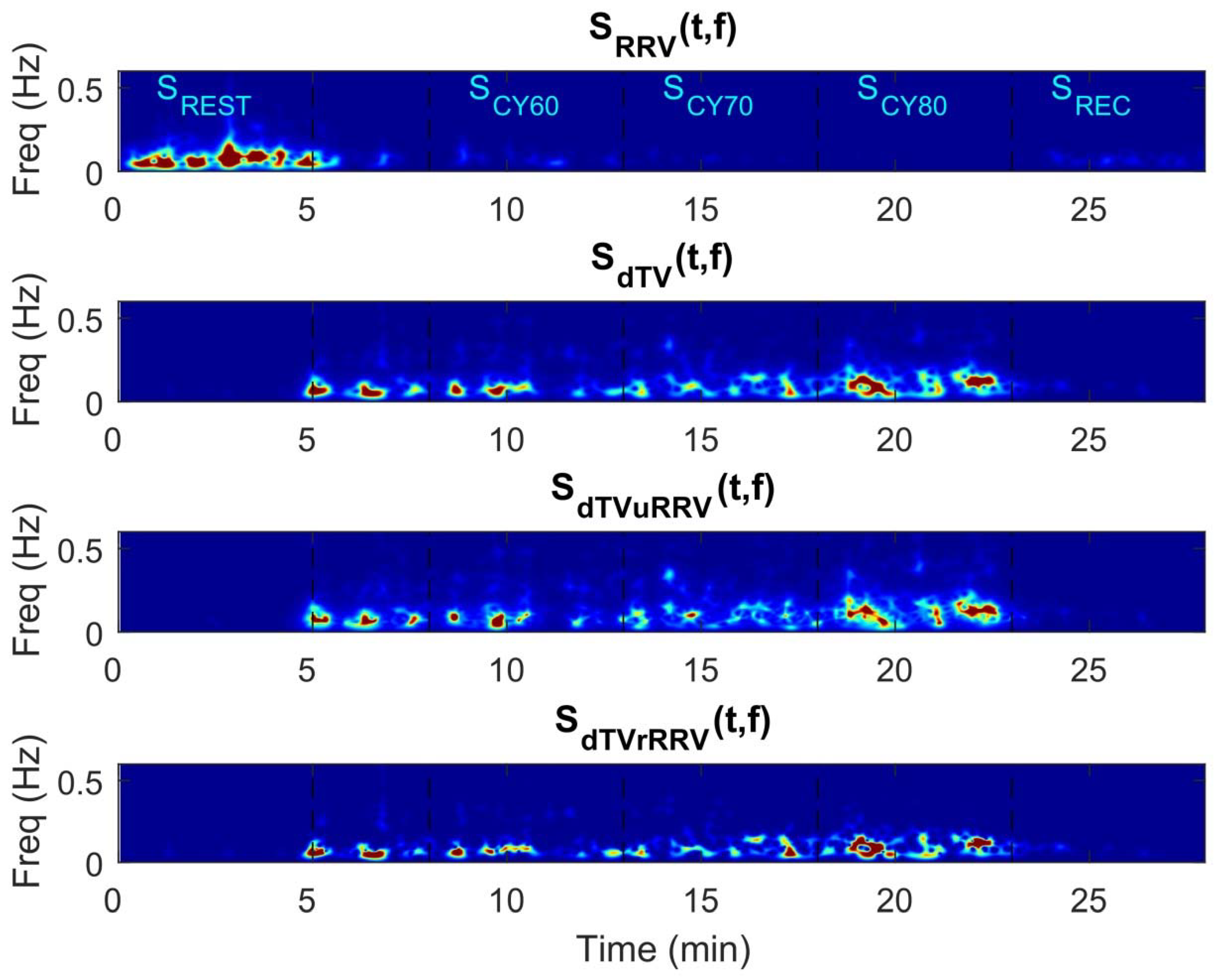
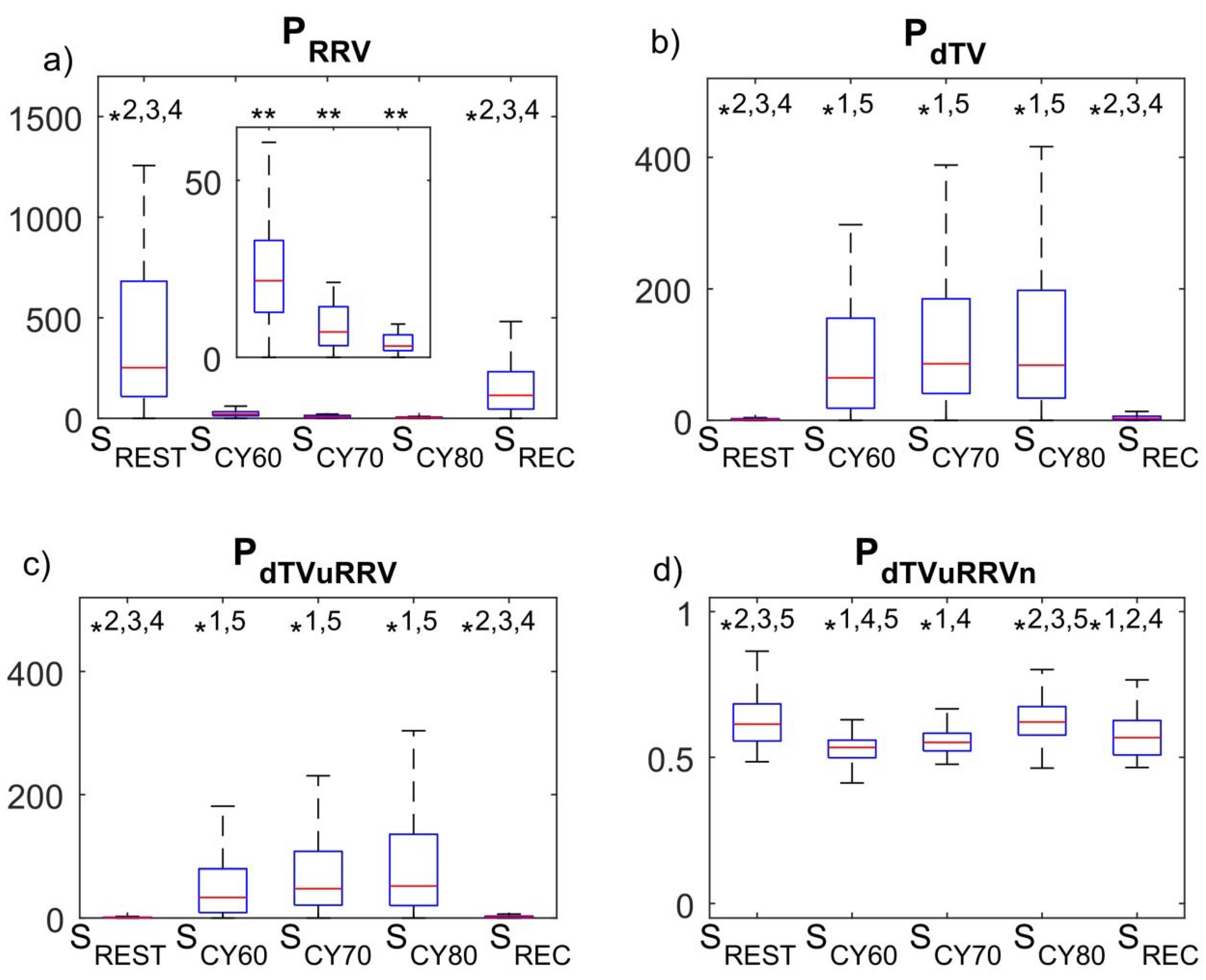
3.1. LF Oscillations of dT in Response to Exercise and Relation to HRV
3.2. Effects of Age, BMI and Cardiorespiratory Fitness Level on LF Oscillations of dT
3.3. Identification of Individuals with Elevated LF Oscillations of dT
4. Discussion
4.1. dT Mainly Oscillates in the LF Band, Being Not Completely Unrelated to HRV
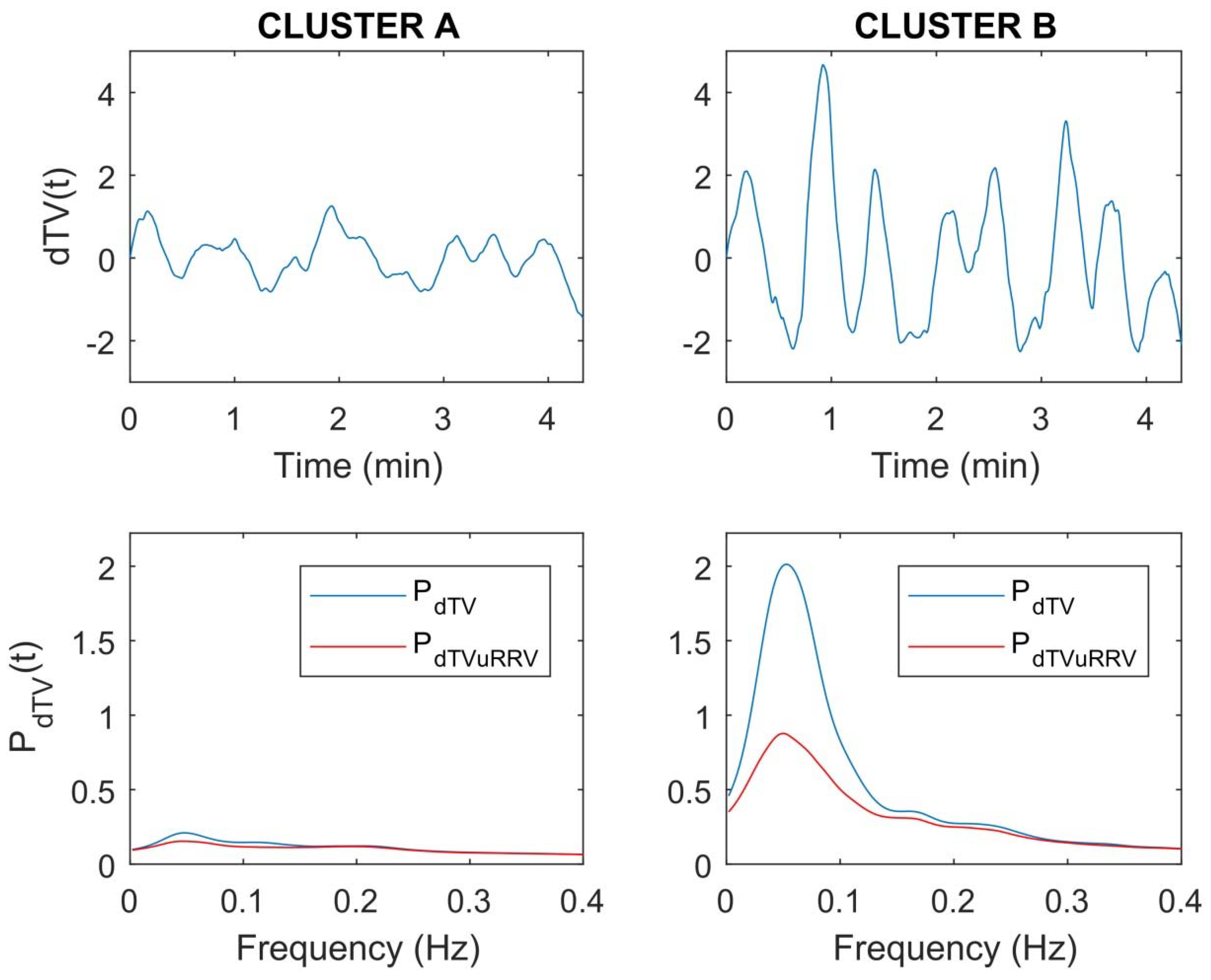
4.2. Incremental Exercise Enhances LF Oscillations of dT, with the Temporal Oscillatory Profile Being Highly Inter-Individual
4.3. LF Oscillations of dT Are Significantly Elevated in a Group of Overweight and Unfit Individuals
4.4. Strengths, Limitations and Future Research
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
| Outcome | Young Adults (n = 24) | Middle-Aged Adults (n = 21) | Older Adults (n = 21) | Main Effect | ||
|---|---|---|---|---|---|---|
| p | Effect Size | |||||
| SREST | PRRV (e−4) | 23.17 (15.06 to 43.17) O | 11.96 (7.90 to 23.84) O | 3.65 (1.86 to 10.82) Y,M | <0.001 * | 0.333 |
| PdTV | 1.31 (0.64 to 2.55) | 1.33 (0.71 to 4.95) | 0.92 (0.48 to 2.76) | 0.666 | 0.012 | |
| PdTVuRRV | 0.80 (0.39 to 1.24) | 0.64 (0.41 to 2.75) | 0.61 (0.26 to 1.41) | 0.712 | 0.010 | |
| PdTVrRRV | 0.54 (0.24 to 1.15) | 0.69 (0.31 to 2.20) | 0.43 (0.21 to 1.09) | 0.480 | 0.023 | |
| PdTVuRRVn | 0.61 (0.59 to 0.66) | 0.67 (0.59 to 0.77) | 0.62 (0.56 to 0.76) | 0.393 | 0.029 | |
| SCY60 | PRRV (e−4) | 2.43 (1.15 to 3.52) O | 1.24 (0.89 to 2.12) | 1.13 (0.71 to 1.95) Y | 0.013 * | 0.133 |
| PdTV | 63.30 (25.45 to 97.67) | 141.55 (40.01 to 192.05) | 99.11 (26.17 to 125.91) | 0.307 | 0.036 | |
| PdTVuRRV | 32.34 (12.18 to 47.36) | 72.16 (16.47 to 97.98) | 48.60 (12.91 to 71.78) | 0.340 | 0.033 | |
| PdTVrRRV | 30.55 (13.27 to 55.29) | 67.71 (19.33 to 104.23) | 42.66 (8.72 to 56.85) | 0.301 | 0.037 | |
| PdTVuRRVn | 0.54 (0.50 to 0.57) | 0.53 (0.50 to 0.55) | 0.55 (0.51 to 0.58) | 0.471 | 0.023 | |
| SCY70 | PRRV (e−4) | 0.94 (0.45 to 1.67) | 0.75 (0.33 to 1.03) | 0.44 (0.24 to 0.91) | 0.164 | 0.056 |
| PdTV | 103.00 (57.80 to 222.93) | 87.38 (66.51 to 172.59) | 88.19 (49.36 to 213.62) | 0.929 | 0.002 | |
| PdTVuRRV | 60.75 (29.50 to 122.93) | 56.59 (33.15 to 95.72) | 48.87 (26.85 to 117.75) | 0.953 | 0.001 | |
| PdTVrRRV | 43.61 (27.82 to 105.93) | 48.79 (24.36 to 76.87) | 44.75 (15.30 to 93.96) | 0.886 | 0.004 | |
| PdTVuRRVn | 0.56 (0.54 to 0.60) | 0.55 (0.54 to 0.57) | 0.55 (0.52 to 0.60) | 0.555 | 0.018 | |
| SCY80 | PRRV (e−4) | 0.32 (0.15 to 0.48) | 0.19 (0.12 to 0.36) | 0.20 (0.14 to 0.38) | 0.345 | 0.033 |
| PdTV | 151.85 (41.39 to 221.44) | 96.18 (46.42 to 143.97) | 79.23 (53.30 to 169.55) | 0.789 | 0.007 | |
| PdTVuRRV | 85.69 (21.61 to 150.95) | 58.99 (28.59 to 117.91) | 53.67 (31.37 to 116.53) | 0.898 | 0.003 | |
| PdTVrRRV | 53.54 (20.21 to 89.76) | 31.17 (16.32 to 49.83) | 31.73 (21.17 to 62.73) | 0.506 | 0.021 | |
| PdTVuRRVn | 0.62 (0.58 to 0.69) | 0.64 (0.61 to 0.70) | 0.60 (0.56 to 0.68) | 0.255 | 0.042 | |
| SREC | PRRV (e−4) | 7.09 (3.45 to 16.39) | 10.71 (5.34 to 17.35) O | 5.16 (2.28 to 9.47) M | 0.014 * | 0.130 |
| PdTV | 2.46 (1.42 to 6.59) | 2.83 (1.36 to 4.20) | 4.92 (2.86 to 7.52) | 0.086 | 0.075 | |
| PdTVuRRV | 1.25 (0.75 to 4.09) | 1.30 (0.86 to 2.32) | 2.66 (1.40 to 3.98) | 0.067 | 0.083 | |
| PdTVrRRV | 1.27 (0.60 to 2.75) | 1.43 (0.49 to 2.21) | 2.23 (0.93 to 3.67) | 0.257 | 0.042 | |
| PdTVuRRVn | 0.57 (0.54 to 0.64) | 0.58 (0.50 to 0.62) | 0.61 (0.54 to 0.64) | 0.613 | 0.015 | |
| Outcome | Non-Overweight (n = 38) | Overweight (n = 28) | p | ES | |
|---|---|---|---|---|---|
| SREST | PRRV (e−4) | 16.93 (6.18 to 30.57) | 10.09 (3.91 to 19.57) | 0.143 | 0.180 |
| PdTV | 1.10 (0.44 to 2.07) | 1.60 (0.84 to 3.37) | 0.030 * | 0.267 | |
| PdTVuRRV | 0.57 (0.27 to 1.24) | 0.75 (0.51 to 2.05) | 0.078 | 0.217 | |
| PdTVrRRV | 0.46 (0.21 to 0.80) | 0.75 (0.38 to 1.47) | 0.019 * | 0.289 | |
| PdTVuRRVn | 0.63 (0.60 to 0.71) | 0.60 (0.56 to 0.73) | 0.364 | 0.112 | |
| SCY60 | PRRV (e−4) | 1.74 (1.01 to 2.95) | 1.44 (0.73 to 2.33) | 0.173 | 0.168 |
| PdTV | 69.61 (27.79 to 165.01) | 98.71 (23.81 to 176.69) | 0.716 | 0.045 | |
| PdTVuRRV | 33.32 (12.88 to 74.32) | 47.73 (12.13 to 90.98) | 0.736 | 0.042 | |
| PdTVrRRV | 37.01 (14.92 to 78.70) | 43.54 (8.67 to 89.04) | 0.815 | 0.029 | |
| PdTVuRRVn | 0.55 (0.53 to 0.58) | 0.51 (0.50 to 0.55) | 0.002 * | 0.388 | |
| SCY70 | PRRV (e−4) | 0.72 (0.33 to 1.13) | 0.54 (0.30 to 1.26) | 0.645 | 0.057 |
| PdTV | 99.71 (56.84 to 218.33) | 87.78 (68.89 to 177.39) | 0.887 | 0.018 | |
| PdTVuRRV | 53.14 (30.30 to 116.59) | 56.33 (30.53 to 102.87) | 0.979 | 0.003 | |
| PdTVrRRV | 43.61 (26.17 to 94.15) | 46.17 (15.76 to 74.53) | 0.640 | 0.057 | |
| PdTVuRRVn | 0.56 (0.54 to 0.60) | 0.55 (0.51 to 0.59) | 0.208 | 0.155 | |
| SCY80 | PRRV (e−4) | 0.29 (0.14 to 0.41) | 0.19 (0.13 to 0.46) | 0.559 | 0.072 |
| PdTV | 116.95 (51.73 to 235.29) | 83.25 (51.81 to 150.11) | 0.392 | 0.105 | |
| PdTVuRRV | 74.30 (31.29 to 148.63) | 51.23 (25.08 to 114.92) | 0.429 | 0.097 | |
| PdTVrRRV | 43.68 (19.03 to 93.20) | 31.00 (19.81 to 55.13) | 0.270 | 0.136 | |
| PdTVuRRVn | 0.64 (0.60 to 0.69) | 0.61 (0.57 to 0.68) | 0.254 | 0.141 | |
| SREC | PRRV (e−4) | 9.47 (6.05 to 18.15) | 4.06 (2.17 to 8.44) | <0.001 * | 0.436 |
| PdTV | 2.76 (1.47 to 5.99) | 3.62 (1.68 to 6.60) | 0.517 | 0.080 | |
| PdTVuRRV | 1.27 (0.85 to 3.22) | 2.16 (1.28 to 3.82) | 0.259 | 0.139 | |
| PdTVrRRV | 1.49 (0.64 to 2.82) | 1.59 (0.45 to 3.43) | 0.825 | 0.027 | |
| PdTVuRRVn | 0.58 (0.53 to 0.64) | 0.58 (0.53 to 0.63) | 0.959 | 0.006 |
| Outcome | Fit (n = 32) | Unfit (n = 34) | p | ES | |
|---|---|---|---|---|---|
| SREST | PRRV (e−4) | 12.45 (5.61 to 24.60) | 14.25 (6.12 to 28.66) | 0.581 | 0.068 |
| PdTV | 1.10 (0.43 to 2.22) | 1.43 (0.80 to 2.70) | 0.166 | 0.171 | |
| PdTVuRRV | 0.63 (0.27 to 1.38) | 0.71 (0.43 to 1.24) | 0.419 | 0.099 | |
| PdTVrRRV | 0.45 (0.23 to 0.80) | 0.71 (0.33 to 1.44) | 0.061 | 0.231 | |
| PdTVuRRVn | 0.65 (0.60 to 0.73) | 0.61 (0.55 to 0.67) | 0.059 | 0.232 | |
| SCY60 | PRRV (e−4) | 1.23 (0.96 to 2.51) | 1.82 (0.96 to 2.91) | 0.441 | 0.095 |
| PdTV | 74.15 (19.97 to 175.41) | 92.39 (36.08 to 165.01) | 0.635 | 0.058 | |
| PdTVuRRV | 35.28 (10.57 to 91.96) | 44.43 (15.99 to 81.78) | 0.663 | 0.054 | |
| PdTVrRRV | 36.43 (10.35 to 90.40) | 48.12 (14.57 to 73.71) | 0.599 | 0.065 | |
| PdTVuRRVn | 0.55 (0.52 to 0.57) | 0.53 (0.50 to 0.55) | 0.121 | 0.191 | |
| SCY70 | PRRV (e−4) | 0.54 (0.32 to 1.03) | 0.76 (0.35 to 1.32) | 0.223 | 0.150 |
| PdTV | 85.90 (42.46 to 208.57) | 101.57 (70.22 to 175.55) | 0.496 | 0.084 | |
| PdTVuRRV | 49.52 (21.85 to 121.80) | 59.95 (34.25 to 91.91) | 0.663 | 0.054 | |
| PdTVrRRV | 38.97 (16.83 to 86.07) | 46.17 (31.58 to 78.83) | 0.488 | 0.085 | |
| PdTVuRRVn | 0.56 (0.54 to 0.60) | 0.55 (0.52 to 0.57) | 0.166 | 0.171 | |
| SCY80 | PRRV (e−4) | 0.21 (0.13 to 0.35) | 0.26 (0.14 to 0.53) | 0.133 | 0.185 |
| PdTV | 130.30 (59.72 to 291.39) | 83.25 (50.12 to 152.08) | 0.281 | 0.133 | |
| PdTVuRRV | 82.98 (37.23 to 156.10) | 49.39 (23.61 to 92.27) | 0.178 | 0.166 | |
| PdTVrRRV | 42.06 (16.91 to 108.72) | 31.45 (21.28 to 57.86) | 0.635 | 0.058 | |
| PdTVuRRVn | 0.67 (0.61 to 0.70) | 0.61 (0.58 to 0.64) | 0.016 * | 0.295 | |
| SREC | PRRV (e−4) | 8.39 (5.23 to 17.51) | 5.22 (2.89 to 13.56) | 0.063 | 0.229 |
| PdTV | 3.55 (1.93 to 6.02) | 2.86 (1.47 to 6.83) | 0.710 | 0.046 | |
| PdTVuRRV | 2.03 (0.94 to 3.08) | 1.36 (0.89 to 3.85) | 0.672 | 0.052 | |
| PdTVrRRV | 1.81 (0.86 to 2.81) | 1.44 (0.53 to 3.78) | 0.691 | 0.049 | |
| PdTVuRRVn | 0.60 (0.54 to 0.65) | 0.57 (0.53 to 0.62) | 0.178 | 0.166 |
References
- Haqqani, H.M.; Chan, K.H.; Kumar, S.; Denniss, A.R.; Gregory, A.T. The Contemporary Era of Sudden Cardiac Death and Ventricular Arrhythmias: Basic Concepts, Recent Developments and Future Directions. Hear. Lung Circ. 2019, 28, 1–5. [Google Scholar] [CrossRef]
- Emery, M.S.; Kovacs, R.J. Sudden Cardiac Death in Athletes. JACC Hear. Fail. 2018, 6, 30–40. [Google Scholar] [CrossRef]
- John, R.M.; Tedrow, U.B.; Koplan, B.A.; Albert, C.M.; Epstein, L.M.; Sweeney, M.O.; Miller, A.L.; Michaud, G.F.; Stevenson, W.G. Ventricular arrhythmias and sudden cardiac death. Lancet 2012, 380, 1520–1529. [Google Scholar] [CrossRef]
- Pueyo, E.; Smetana, P.; Caminal, P.; De Luna, A.B.; Malik, M.; Laguna, P. Characterization of QT interval adaptation to RR interval changes and its use as a a risk-stratifier of arrhythmic mortality in amiodarone-treated survivors of acute myocardial infarction. IEEE Trans. Biomed. Eng. 2004, 51, 1511–1520. [Google Scholar] [CrossRef] [PubMed]
- Ramírez, J.; Laguna, P.; Bayés De Luna, A.; Malik, M.; Pueyo, E. QT/RR and T-peak-to-end/RR curvatures and slopes in chronic heart failure: Relation to sudden cardiac death. J. Electrocardiol. 2014, 47, 842–848. [Google Scholar] [CrossRef] [PubMed]
- Ramírez, J.; Orini, M.; Mincholé, A.; Monasterio, V.; Cygankiewicz, I.; Bayés de Luna, A.; Martínez, J.P.; Laguna, P.; Pueyo, E. Sudden cardiac death and pump failure death prediction in chronic heart failure by combining ECG and clinical markers in an integrated risk model. PLoS ONE 2017, 12, e0186152. [Google Scholar] [CrossRef] [PubMed]
- La Rovere, M.T.; Pinna, G.D.; Maestri, R.; Barlera, S.; Bernardinangeli, M.; Veniani, M.; Nicolosi, G.L.; Marchioli, R.; Tavazzi, L. Autonomic markers and cardiovascular and arrhythmic events in heart failure patients: Still a place in prognostication? Data from the GISSI-HF trial. Eur. J. Heart Fail. 2012, 14, 1410–1419. [Google Scholar] [CrossRef]
- Gatzoulis, K.A.; Tsiachris, D.; Arsenos, P.; Antoniou, C.K.; Dilaveris, P.; Sideris, S.; Kanoupakis, E.; Simantirakis, E.; Korantzopoulos, P.; Goudevenos, I.; et al. Arrhythmic risk stratification in post-myocardial infarction patients with preserved ejection fraction: The PRESERVE EF study. Eur. Heart J. 2019, 40, 2940–2949. [Google Scholar] [CrossRef]
- Ang, R.; Marina, N. Low-Frequency Oscillations in Cardiac Sympathetic Neuronal Activity. Front. Physiol. 2020, 11, 236. [Google Scholar] [CrossRef]
- Rizas, K.D.; Nieminen, T.; Barthel, P.; Zürn, C.S.; Kähönen, M.; Viik, J.; Lehtimäki, T.; Nikus, K.; Eick, C.; Greiner, T.O.; et al. Sympathetic activity-associated periodic repolarization dynamics predict mortality following myocardial infarction. J. Clin. Invest. 2014, 124, 1770–1780. [Google Scholar] [CrossRef]
- Cheng, S.; Cai, M.; Liu, X.; Zhang, N.; Jin, R.; Yang, S.; Hu, Y.; Hua, W.; Zhang, S. Periodic repolarization dynamics for prediction of mortality: A systematic review and meta-analysis. Eur. Heart J. 2020, 41, ehaa946-0764. [Google Scholar] [CrossRef]
- Rizas, K.D.; McNitt, S.; Hamm, W.; Massberg, S.; Kääb, S.; Zareba, W.; Couderc, J.P.; Bauer, A. Prediction of sudden and non-sudden cardiac death in post-infarction patients with reduced left ventricular ejection fraction by periodic repolarization dynamics: MADIT-II substudy. Eur. Heart J. 2017, 38, 2110–2118. [Google Scholar] [CrossRef]
- Rizas, K.D.; Doller, A.J.; Hamm, W.; Vdovin, N.; von Stuelpnagel, L.; Zuern, C.S.; Bauer, A. Periodic repolarization dynamics as a risk predictor after myocardial infarction: Prospective validation study. Hear. Rhythm 2019, 16, 1223–1231. [Google Scholar] [CrossRef]
- Palacios, S.; Cygankiewicz, I.; Bayés de Luna, A.; Pueyo, E.; Martínez, J.P. Periodic repolarization dynamics as predictor of risk for sudden cardiac death in chronic heart failure patients. Sci. Rep. 2021. (under review). [Google Scholar]
- Bauer, A.; Klemm, M.; Rizas, K.D.; Hamm, W.; von Stülpnagel, L.; Dommasch, M.; Steger, A.; Lubinski, A.; Flevari, P.; Harden, M.; et al. Prediction of mortality benefit based on periodic repolarisation dynamics in patients undergoing prophylactic implantation of a defibrillator: A prospective, controlled, multicentre cohort study. Lancet 2019, 394, 1344–1351. [Google Scholar] [CrossRef]
- Milagro, J.; Hernández-Vicente, A.; Hernando, D.; Casajús, J.A.; Garatachea, N.; Bailón, R.; Pueyo, E. Estimation of the second ventilatory threshold through ventricular repolarization profile analysis. Scand. J. Med. Sci. Sport. 2021, 31, 339–349. [Google Scholar] [CrossRef]
- Schüttler, D.; von Stülpnagel, L.; Rizas, K.D.; Bauer, A.; Brunner, S.; Hamm, W. Effect of Hyperventilation on Periodic Repolarization Dynamics. Front. Physiol. 2020, 11, 1197. [Google Scholar] [CrossRef] [PubMed]
- Hamm, W.; von Stülpnagel, L.; Rizas, K.D.; Vdovin, N.; Klemm, M.; Bauer, A.; Brunner, S. Dynamic Changes of Cardiac Repolarization Instability during Exercise Testing. Med. Sci. Sport. Exerc. 2019, 51, 1522. [Google Scholar] [CrossRef]
- Tanaka, H.; Monahan, K.D.; Seals, D.R. Age-predicted maximal heart rate revisited. J. Am. Coll. Cardiol. 2001, 37, 153–156. [Google Scholar] [CrossRef]
- WHO Physical Status: The Use and Interpretation of Anthropometry, Report of a WHO Expert Committee; WHO: Geneva, Switzerland, 1995.
- Noonan, V.; Dean, E. Submaximal Exercise Testing: Clinical Application and Interpretation. Phys. Ther. 2000, 80, 782–807. [Google Scholar] [CrossRef]
- Shaffer, F.; Ginsberg, J.P. An Overview of Heart Rate Variability Metrics and Norms. Front. Public Heal. 2017, 5, 1–17. [Google Scholar] [CrossRef]
- Gore, C.J.; Booth, M.L.; Bauman, A.; Owen, N. Utility of pwc75% as an estimate of aerobic power in epidemiological and population-based studies. Med. Sci. Sports Exerc. 1999, 31, 348–351. [Google Scholar] [CrossRef] [PubMed]
- Batcho, C.S.; Thonnard, J.L.; Nielens, H. PWC 75%/kg, a fitness index not linked to resting heart rate: Testing procedure and reference values. Arch. Phys. Med. Rehabil. 2012, 93, 1196–1200. [Google Scholar] [CrossRef] [PubMed]
- Hillreiner, A.; Baumeister, S.E.; Sedlmeier, A.M.; Finger, J.D.; Schlitt, H.J.; Leitzmann, M.F. Association between cardiorespiratory fitness and colorectal cancer in the UK Biobank. Eur. J. Epidemiol. 2019, 35, 961–973. [Google Scholar] [CrossRef] [PubMed]
- Finger, J.D.; Gößwald, A.; Härtel, S.; Müters, S.; Krug, S.; Hölling, H.; Kuhnert, R.; Bös, K. Measurement of cardiorespiratory fitness in the German Health Interview and Examination Survey for Adults (DEGS1). Bundesgesundheitsblatt-Gesundheitsforsch. -Gesundh. 2013, 56, 885–893. [Google Scholar] [CrossRef]
- Martínez, J.P.; Almeida, R.; Olmos, S.; Rocha, A.P.; Laguna, P. A Wavelet-Based ECG Delineator Evaluation on Standard Databases. IEEE Trans. Biomed. Eng. 2004, 51, 570–581. [Google Scholar] [CrossRef]
- Hernando, D.; Bailón, R.; Almeida, R.; Hernández, A. QRS detection optimization in stress test recordings using evolutionary algorithms. Int. Conf. Comput. Cardiol. 2014, 41, 737–740. [Google Scholar] [CrossRef]
- Palacios, S.; Caiani, E.G.; Landreani, F.; Martínez, J.P.; Pueyo, E. Long-Term Microgravity Exposure Increases ECG Repolarization Instability Manifested by Low-Frequency Oscillations of T-Wave Vector. Front. Physiol. 2019, 10, 1510. [Google Scholar] [CrossRef]
- Edenbrandt, L.; Pahlm, O. Vectorcardiogram synthesized from a 12-lead ECG: Superiority of the inverse Dower matrix. J. Electrocardiol. 1988, 21, 361–367. [Google Scholar] [CrossRef]
- Orini, M.; Pueyo, E.; Laguna, P.; Bailon, R. A Time-Varying Nonparametric Methodology for Assessing Changes in QT Variability Unrelated to Heart Rate Variability. IEEE Trans. Biomed. Eng. 2018, 65, 1443–1451. [Google Scholar] [CrossRef]
- Sanson, A.; Letcher, P.; Smart, D.; Prior, M.; Toumbourou, J.W.; Oberklaid, F. Associations between early childhood temperament clusters and later psychosocial adjustment. Merrill. Palmer. Q. 2009, 55, 26–54. [Google Scholar] [CrossRef]
- Gomez-Bruton, A.; Arenaza, L.; Medrano, M.; Mora-Gonzalez, J.; Cadenas-Sanchez, C.; Migueles, J.H.; Muñoz-Hernández, V.; Merchan-Ramirez, E.; Martinez-Avila, W.D.; Maldonado, J.; et al. Associations of dietary energy density with body composition and cardiometabolic risk in children with overweight and obesity: Role of energy density calculations, under-reporting energy intake and physical activity. Br. J. Nutr. 2019, 121, 1057–1068. [Google Scholar] [CrossRef]
- Tomczak, M.; Tomczak, E. The need to report effect size estimates revisited. An overview of some recommended measures of effect size. Trends Sport Sci. 2014, 1, 19–25. [Google Scholar]
- Cohen, J. A power primer. Psychol. Bull. 1992, 112, 155–159. [Google Scholar] [CrossRef]
- Hanson, B.; Child, N.; Van Duijvenboden, S.; Orini, M.; Chen, Z.; Coronel, R.; Rinaldi, A.; Gill, J.; Taggart, P. Oscillatory behaviour of ventricular action potential duration in heart failure patients at respiratory rate and low frequency. Front. Physiol. 2014, 5, 141. [Google Scholar] [CrossRef][Green Version]
- Porter, B.; van Duijvenboden, S.; Bishop, M.J.; Orini, M.; Claridge, S.; Gould, J.; Sieniewicz, B.J.; Sidhu, B.; Razavi, R.; Rinaldi, C.A.; et al. Beat-to-beat variability of ventricular action potential duration oscillates at low frequency during sympathetic provocation in humans. Front. Physiol. 2018, 9, 147. [Google Scholar] [CrossRef]
- Van Duijvenboden, S.; Porter, B.; Pueyo, E.; Sampedro-Puente, D.A.; Fernandez-Bes, J.; Sidhu, B.; Gould, J.; Orini, M.; Bishop, M.J.; Hanson, B.; et al. Complex Interaction Between Low-Frequency APD Oscillations and Beat-to-Beat APD Variability in Humans Is Governed by the Sympathetic Nervous System. Front. Physiol. 2020, 10, 1582. [Google Scholar] [CrossRef] [PubMed]
- Sprenkeler, D.J.; Beekman, J.D.M.; Bossu, A.; Dunnink, A.; Vos, M.A. Pro-Arrhythmic Ventricular Remodeling Is Associated With Increased Respiratory and Low-Frequency Oscillations of Monophasic Action Potential Duration in the Chronic Atrioventricular Block Dog Model. Front. Physiol. 2019, 10, 1095. [Google Scholar] [CrossRef] [PubMed]
- Pueyo, E.; Orini, M.; Rodríguez, J.F.; Taggart, P. Interactive effect of beta-adrenergic stimulation and mechanical stretch on low-frequency oscillations of ventricular action potential duration in humans. J. Mol. Cell. Cardiol. 2016, 97, 93–105. [Google Scholar] [CrossRef] [PubMed]
- Sampedro-Puente, D.A.; Fernandez-Bes, J.; Porter, B.; Van Duijvenboden, S.; Taggart, P.; Pueyo, E. Mechanisms underlying interactions between low-frequency oscillations and beat-to-beat variability of celullar ventricular repolarization in response to sympathetic stimulation: Implications for arrhythmogenesis. Front. Physiol. 2019, 10, 916. [Google Scholar] [CrossRef] [PubMed]
- González del Castillo, M.; Hernando, D.; Orini, M.; Laguna, P.; Viik, J.; Bailón, R.; Pueyo, E. QT variability unrelated to RR during stress testing for identification of coronary artery disease. Philos. Trans. R. Soc. A 2021, (in press).
- Nayyar, S.; Hasan, M.A.; Roberts-Thomson, K.C.; Sullivan, T.; Baumert, M. Effect of Loss of Heart Rate Variability on T-Wave Heterogeneity and QT Variability in Heart Failure Patients: Implications in Ventricular Arrhythmogenesis. Cardiovasc. Eng. Technol. 2017, 8, 219–228. [Google Scholar] [CrossRef] [PubMed]
- Michael, S.; Graham, K.S.; Oam, G.M.D. Cardiac autonomic responses during exercise and post-exercise recovery using heart rate variability and systolic time intervals-a review. Front. Physiol. 2017, 8, 301. [Google Scholar] [CrossRef] [PubMed]
- Mezzani, A.; Hamm, L.F.; Jones, A.M.; McBride, P.E.; Moholdt, T.; Stone, J.A.; Urhausen, A.; Williams, M.A. Aerobic Exercise Intensity Assessment and Prescription in Cardiac Rehabilitation. J. Cardiopulm. Rehabil. Prev. 2012, 32, 442–467. [Google Scholar] [CrossRef] [PubMed]
- White, D.W.; Raven, P.B. Autonomic neural control of heart rate during dynamic exercise: Revisited. J. Physiol. 2014, 592, 2491–2500. [Google Scholar] [CrossRef]
- Porta, A.; Tobaldini, E.; Gnecchi-Ruscone, T.; Montano, N. RT variability unrelated to heart period and respiration progressively increases during graded head-up tilt. Am. J. Physiol. -Hear. Circ. Physiol. 2010, 298, 1406–1414. [Google Scholar] [CrossRef]
- Voss, A.; Schroeder, R.; Heitmann, A.; Peters, A.; Perz, S. Short-term heart rate variability—Influence of gender and age in healthy subjects. PLoS ONE 2015, 10, 1–33. [Google Scholar] [CrossRef] [PubMed]
- Kemp, A.H.; Koenig, J.; Thayer, J.F. From psychological moments to mortality: A multidisciplinary synthesis on heart rate variability spanning the continuum of time. Neurosci. Biobehav. Rev. 2017, 83, 547–567. [Google Scholar] [CrossRef]
- UN World Bank. World Population Ageing 2019; UN World Bank: Washington, DC, USA, 2019. [Google Scholar]
- Ortega, F.; Cadenas-Sanchez, C.; Lee, D.; Ruiz, J.; Blair, S.; Sui, X. Fitness and Fatness as Health Markers through the Lifespan: An Overview of Current Knowledge. Prog. Prev. Med. 2018, 3, e0013. [Google Scholar] [CrossRef]
- Harridge, S.D.R.; Lazarus, N.R. Physical activity, aging, and physiological function. Physiology 2017, 32, 152–161. [Google Scholar] [CrossRef]
| Outcome | Young Adults (n = 24) | Middle-Aged Adults (n = 21) | Older Adults (n = 21) |
|---|---|---|---|
| Age (years) | 25.41 ± 2.74 | 42.86 ± 3.06 | 63.82 ± 2.97 |
| Height (m) | 1.75 ± 0.06 | 1.77 ± 0.06 | 1.71 ± 0.05 |
| Weight (kg) | 71.81 ± 11.45 | 78.44 ± 10.49 | 76.53 ± 7.96 |
| BMI (kg·m−2) | 23.30 ± 2.86 | 25.09 ± 2.88 | 26.17 ± 2.82 |
| “Overweight” (%) | 20.8 (5) | 47.6 (10) | 61.9 (13) |
| PWC80% (W·kg−1) | 2.01 ± 0.61 | 2.02 ± 0.59 | 1.74 ± 0.59 |
| “Unfit” (%) | 50.0 (12) | 52.4 (11) | 52.4 (11) |
| Outcome | CLUSTER A (n = 31) | CLUSTER B (n = 35) | p | Effect Size |
|---|---|---|---|---|
| Age (years) | 32.99 ± 11.48 | 52.22 ± 14.38 | <0.001 * | 0.580 |
| Height (m) | 175.37 ± 6.07 | 173.51 ± 6.20 | 0.203 | 0.157 |
| Weight (kg) | 69.36 ± 8.88 | 80.79 ± 8.57 | <0.001 * | 0.506 |
| BMI (kg·m−2) | 22.48 ± 1.87 | 26.82 ± 2.38 | <0.001 * | 0.757 |
| % of “overweight” | 6.5 (2) | 74.3 (26) | ||
| PWC80% (W·kg−1) | 2.33 ± 0.59 | 1.57 ± 0.33 | <0.001 * | 0.628 |
| % of “unfit” | 32.3 (10) | 68.6 (24) |
| Outcome | CLUSTER A (n = 31) | CLUSTER B (n = 35) | p | ES | |
|---|---|---|---|---|---|
| SREST | PRRV (e−4) | 18.14 (6.31 to 38.94) | 9.79 (3.65 to 17.54) | 0.020 * | 0.287 |
| PdTV | 1.00 (0.41 to 1.87) | 1.50 (0.82 to 2.96) | 0.021 * | 0.284 | |
| PdTVuRRV | 0.51 (0.22 to 1.23) | 0.75 (0.49 to 1.56) | 0.039 * | 0.254 | |
| PdTVrRRV | 0.39 (0.23 to 0.79) | 0.75 (0.37 to 1.43) | 0.018 * | 0.290 | |
| PdTVuRRVn | 0.62 (0.60 to 0.70) | 0.62 (0.56 to 0.73) | 0.743 | 0.040 | |
| SCY60 | PRRV (e−4) | 1.40 (0.98 to 3.41) | 1.64 (0.89 to 2.39) | 0.400 | 0.104 |
| PdTV | 63.42 (24.28 to 162.91) | 99.78 (33.81 to 186.33) | 0.289 | 0.130 | |
| PdTVuRRV | 32.34 (11.83 to 72.16) | 53.95 (15.66 to 93.05) | 0.295 | 0.129 | |
| PdTVrRRV | 30.84 (12.45 to 74.75) | 48.50 (11.08 to 93.27) | 0.415 | 0.100 | |
| PdTVuRRVn | 0.55 (0.52 to 0.58) | 0.53 (0.50 to 0.56) | 0.141 | 0.181 | |
| SCY70 | PRRV (e−4) | 0.66 (0.32 to 1.21) | 0.60 (0.33 to 1.15) | 0.974 | 0.004 |
| PdTV | 98.08 (54.45 to 186.19) | 88.19 (69.84 to 243.71) | 0.724 | 0.043 | |
| PdTVuRRV | 56.59 (29.10 to 106.70) | 49.70 (30.67 to 126.59) | 0.733 | 0.042 | |
| PdTVrRRV | 42.96 (21.45 to 79.49) | 47.58 (22.86 to 83.74) | 0.832 | 0.026 | |
| PdTVuRRVn | 0.56 (0.54 to 0.60) | 0.55 (0.52 to 0.60) | 0.272 | 0.135 | |
| SCY80 | PRRV (e−4) | 0.24 (0.12 to 0.40) | 0.22 (0.14 to 0.43) | 0.729 | 0.043 |
| PdTV | 136.21 (53.69 to 223.58) | 79.23 (51.54 to 150.67) | 0.352 | 0.115 | |
| PdTVuRRV | 83.28 (33.82 to 152.10) | 48.80 (23.36 to 117.25) | 0.372 | 0.110 | |
| PdTVrRRV | 47.41 (19.87 to 91.11) | 30.82 (17.09 to 59.68) | 0.256 | 0.140 | |
| PdTVuRRVn | 0.64 (0.61 to 0.70) | 0.60 (0.57 to 0.67) | 0.052 | 0.240 | |
| SREC | PRRV (e−4) | 9.03 (5.18 to 17.32) | 5.29 (2.49 to 13.55) | 0.036 * | 0.259 |
| PdTV | 2.36 (1.40 to 5.70) | 3.82 (1.91 to 7.94) | 0.079 | 0.216 | |
| PdTVuRRV | 1.21 (0.83 to 3.07) | 2.35 (1.26 to 4.06) | 0.060 | 0.232 | |
| PdTVrRRV | 1.14 (0.58 to 2.55) | 1.90 (0.66 to 3.88) | 0.250 | 0.142 | |
| PdTVuRRVn | 0.59 (0.53 to 0.64) | 0.57 (0.53 to 0.63) | 0.559 | 0.072 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hernández-Vicente, A.; Hernando, D.; Vicente-Rodríguez, G.; Bailón, R.; Garatachea, N.; Pueyo, E. ECG Ventricular Repolarization Dynamics during Exercise: Temporal Profile, Relation to Heart Rate Variability and Effects of Age and Physical Health. Int. J. Environ. Res. Public Health 2021, 18, 9497. https://doi.org/10.3390/ijerph18189497
Hernández-Vicente A, Hernando D, Vicente-Rodríguez G, Bailón R, Garatachea N, Pueyo E. ECG Ventricular Repolarization Dynamics during Exercise: Temporal Profile, Relation to Heart Rate Variability and Effects of Age and Physical Health. International Journal of Environmental Research and Public Health. 2021; 18(18):9497. https://doi.org/10.3390/ijerph18189497
Chicago/Turabian StyleHernández-Vicente, Adrián, David Hernando, Germán Vicente-Rodríguez, Raquel Bailón, Nuria Garatachea, and Esther Pueyo. 2021. "ECG Ventricular Repolarization Dynamics during Exercise: Temporal Profile, Relation to Heart Rate Variability and Effects of Age and Physical Health" International Journal of Environmental Research and Public Health 18, no. 18: 9497. https://doi.org/10.3390/ijerph18189497
APA StyleHernández-Vicente, A., Hernando, D., Vicente-Rodríguez, G., Bailón, R., Garatachea, N., & Pueyo, E. (2021). ECG Ventricular Repolarization Dynamics during Exercise: Temporal Profile, Relation to Heart Rate Variability and Effects of Age and Physical Health. International Journal of Environmental Research and Public Health, 18(18), 9497. https://doi.org/10.3390/ijerph18189497









