Bioelectric Effect of a Microcurrent Toothbrush on Plaque Removal
Abstract
1. Introduction
2. Material and Methods
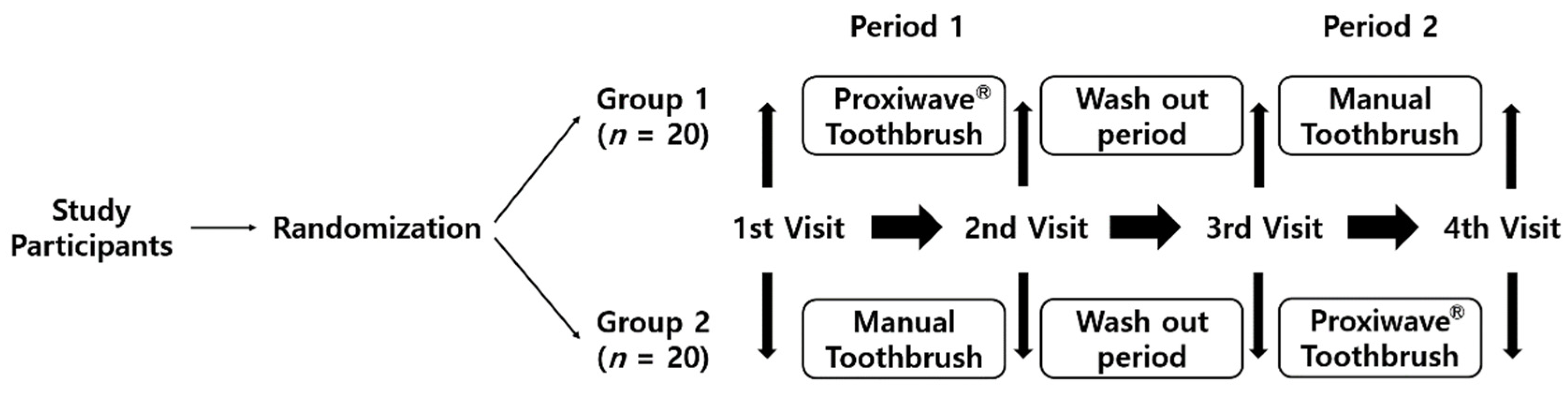
2.1. Study Design
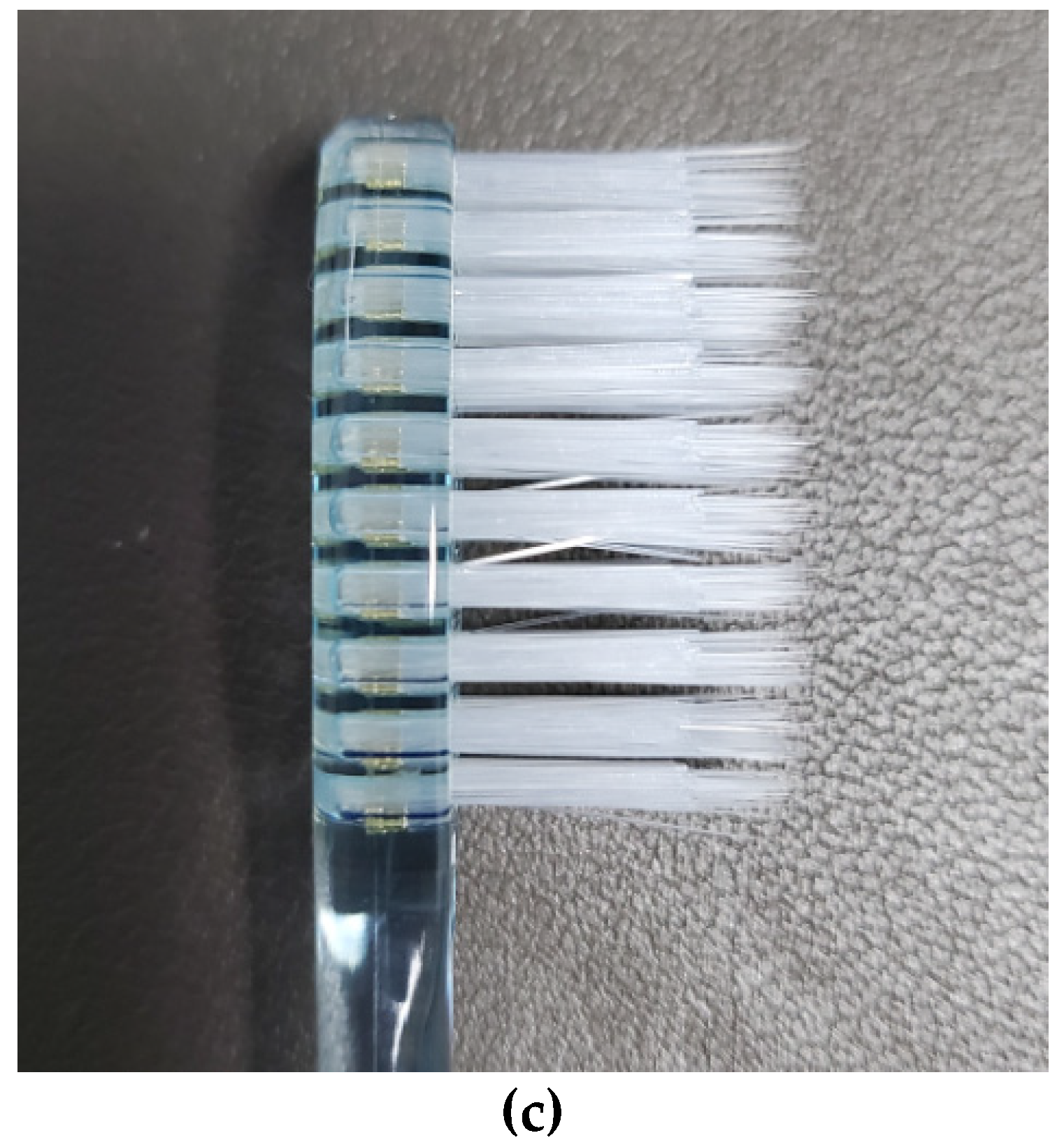
2.2. Brush
2.3. Participants
2.4. Clinical Measurements
2.5. Data Analysis
2.6. Safety Assessment
3. Results
Safety
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Marsh, P.D. Dental plaque: Biological significance of a biofilm and community life-style. J. Clin Periodontol. 2005, 32, 7–15. [Google Scholar] [CrossRef] [PubMed]
- Löe, H.; Theilade, E.; Jensen, S.B. Experimental Gingivitis in Man. J. Periodontol. 1965, 36, 177–187. [Google Scholar] [CrossRef]
- Lovdal, A.; Arno, A.; Waerhaug, J. Incidence of clinical manifestations of periodontal disease in light of oral hygiene and calculus formation. J. Amer. Dent. Assoc. 1939, 56, 21–33. [Google Scholar] [CrossRef] [PubMed]
- Löe, H. Mechanical and chemical control of dental plaque. J. Clinl. Periodontol. 1979, 6, 32–36. [Google Scholar] [CrossRef] [PubMed]
- Ciancio, S.G.; Mather, M.L. A clinical comparison of two electric toothbrushes with different mechanical actions. Clin. Prev. Dent. 1990, 12, 5–7. [Google Scholar]
- Sälzer, S.; Slot, D.E.; Van der Weijden, F.A.; Dörfer, C.E. Efficacy of inter-dental mechanical plaque control in managing gingivitis—A meta-review. J. Clin. Periodontol. 2015, 42, 92–105. [Google Scholar] [CrossRef] [PubMed]
- Westfelt, E. Rationale of mechanical plaque control. J. Clin. Periodontol. 1996, 23, 263–267. [Google Scholar] [CrossRef] [PubMed]
- Jepsen, S. Role of m toothbrushes in effective plaque control: Advantages and limitations. In Proceedings of European Workship on Mechanical Plaque Control, 1st ed.; Lang, N.P., Attstrom, R., Love, H., Eds.; Quintessence Publishing: Batavia, IL, USA; pp. 121–137.
- Costerton, J.W.; Stewart, P.S.; Greenberg, E.P. Bacterial biofilms: A common cause of persistent infections. Science 1999, 284, 1318–1322. [Google Scholar] [CrossRef]
- Daubert, D.M.; Weinstein, B.F. Biofilm as a risk factor in implant treatment. Periodontology 2000 2019, 81, 29–40. [Google Scholar] [CrossRef]
- Hentzer, M.; Givskov, M.; Eberl, L. Quorum sensing in biofilms: Gossip in slime city. In Microbial Biofilms; Ghannoum, M., O’Toole, G.A., Eds.; ASM Press: Washington, DC, USA, 2004; pp. 118–140. [Google Scholar]
- Del Pozo, J.; Rouse, M.; Patel, R. Bioelectric effect and bacterial biofilms. A systematic review. Int. J. Artif. Organs. 2008, 31, 786–795. [Google Scholar] [CrossRef]
- Costerton, J.W.; Ellis, B.; Lam, K.; Johnson, F.; Khoury, A.E. Mechanism of electrical enhancement of efficacy of antibiotics in killing biofilm bacteria. Antimicrob. Agents Chemother. 1994, 38, 2803–2809. [Google Scholar] [CrossRef]
- Caubet, R.; Pedarros-Caubet, F.; Chu, M.; Freye, E.; de Belém Rodrigues, M.; Moreau, J.M.; Ellison, W.J. A radio frequency electric current enhances antibiotic efficacy against bacterial biofilms. Antimicrob. Agents Chemother. 2004, 48, 4662–4664. [Google Scholar] [CrossRef]
- Cottarel, G.; Wierzbowski, J. Combination drugs, an emerging option for antibacterial therapy. Trends Biotechnol. 2007, 25, 547–555. [Google Scholar] [CrossRef]
- Pareilleux, A.; Sicard, N. Lethal effects of electric current on Escherichia coli. Appl. Microbiol. 1970, 19, 421–424. [Google Scholar] [CrossRef] [PubMed]
- Kim, Y.W.; Subramanian, S.; Gerasopoulos, K.; Ben-Yoav, H.; Wu, H.C.; Quan, D.; Carter, K.; Meyer, M.T.; Bentley, W.E.; Ghodssi, R. Effect of electrical energy on the efficacy of biofilm treatment using the bioelectric effect. NPJ Biofilms Microbiomes. 2015, 1, 15–16. [Google Scholar] [CrossRef]
- Kim, Y.W.; Meyer, M.T.; Berkovich, A.; Subramanian, S.; Iliadisb, A.A.; Bentleyc, W.E.; Ghodssia, R. A surface acoustic wave biofilm sensor integrated with a treatment method based on the bioelectric effect. Sens. Actuator A Phys. 2016, 238, 140–149. [Google Scholar] [CrossRef]
- Lee, J.; Yoon, S.; Kim, T.; Park, S. The effects of microcurrents on inflammatory reaction induced by ultraviolet irradiation. J. Phys. Ther. Sci. 2011, 23, 693–696. [Google Scholar] [CrossRef][Green Version]
- Loe, H.; Silness, J. Periodontal disease in pregnancy. I. Prevalence and severity. Acta Odontol. Scand. 1963, 21, 533–551. [Google Scholar] [CrossRef]
- Turesky, S.; Gilmore, N.D.; Glickman, I. Reduced plaque formation by the chloromethyl analogue of victamine C. J. Periodontol. 1970, 41, 41–43. [Google Scholar] [CrossRef]
- Quigley, G.A.; Hein, J.W. Comparative cleansing efficiency of manual and power brushing. J. Amer. Dent. Assoc. 1962, 65, 26–29. [Google Scholar] [CrossRef] [PubMed]
- Goldsobel, A.B.; Prabhakar, N.; Gurfein, B.T. Prospective trial examining safety and efficacy of microcurrent stimulation for the treatment of sinus pain and congestion. Bioelectron. Med. 2019, 5, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Horiuchi, M.; Yamamoto, T.; Tomofuji, T.; Ishikawa, A.; Morita, M.; Watanabe, T. Toothbrushing promotes gingival fibroblast proliferation more effectively than removal of dental plaque. J. Clin. Periodontol. 2002, 29, 791–795. [Google Scholar] [CrossRef]
- <named-content content-type="background:white">Yu, C.; Xu, Z.X.; Hao, Y.H.; Gao, Y.B.; Yao, B.W.; Zhang, J.; Wang, B.; Hu, Z.Q.; Peng, R.Y. A novel microcurrent dressing for wound healing in a rat skin defect model. Mil. Med. Res. 2019, 6, 1–9. [Google Scholar]
- Marshall, R.; Taylor, I.; Lahr, C.; Abell, T.L.; Espinoza, I.; Gupta, N.K.; Gomez, C.R. Bioelectrical Stimulation for the Reduction of Inflammation in Inflammatory Bowel Disease. Clin. Med. Insights Gastroenterol. 2015, 8, 55–59. [Google Scholar] [CrossRef] [PubMed]
- Teorell, T. Membrane electrophoresis in relation to bioelectrical polarization effects. Nature 1948, 162, 961. [Google Scholar] [CrossRef]
- Khoury, A.E.; Lam, K.; Ellis, B.; Costerton, J.W. Prevention and control of bacterial infections associated with medical devices. ASAIO 1992, 38, 174–178. [Google Scholar] [CrossRef] [PubMed]
- Preshaw, P.M.; Hefti, A.F.; Jepsen, S.; Etienne, D.; Walker, C.; Bradshaw, M.H. Subantimicrobial dose doxycycline as adjunctive treatment for periodontitis. A review. J. Clin. Periodontol. 2004, 31, 697–707. [Google Scholar] [CrossRef]
- Hall-Stoodley, L.; Stoodley, P. Evolving concepts in biofilm infections. Cell Microbiol. 2009, 11, 1034–1043. [Google Scholar] [CrossRef]
- Vibhute, A.; Vandana, K.L. The effectiveness of manual versus powered toothbrushes for plaque removal and gingival health: A meta-analysis. J. Indian Soc. Periodontol. 2012, 16, 156–160. [Google Scholar]
- Kleber, C.J.; Putt, M.S.; Muhler, J.C. Duration and pattern of toothbrushing in children using a gel or paste dentifrice. J. Amer. Dent. Assoc. 1981, 103, 723–726. [Google Scholar] [CrossRef]
- Lee, D.W.; Moon, I.S. The plaque-removing efficacy of a single-tufted brush on the lingual and buccal surfaces of the molars. J. Periodontal Implant. Sci. 2011, 41, 131–134. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Axelsson, P. Needs-related Plaque Control Measures Based on Risk Prediction; Quintessence: Chicago, IL, USA, 1998; pp. 190–247. [Google Scholar]

| Total (n = 40) | Group 1 (n = 20) | Group 2 (n = 20) | p-Value | |
|---|---|---|---|---|
| Age | 37.58 ± 7.43 | 37.70 ± 7.15 | 37.45 ± 7.88 | 0.917 |
| Sex | 1.000 | |||
| Male | 12 (30.0) | 6 (30.0) | 6 (30.0) | |
| Female | 28 (70.0) | 14 (70.0) | 14 (70.0) | |
| Brushing time (minutes) | 2.46 ± 0.71 | 2.60 ± 0.60 | 2.33 ± 0.80 | 0.226 |
| Brushing frequency | 3.15 ± 0.58 | 3.15 ± 0.67 | 3.15 ± 0.49 | 1.000 |
| Plaque Index (PI) | Gingival Index (GI) | |||||
|---|---|---|---|---|---|---|
| Pre-Brushing | Post-Brushing | p-Value | Pre-Brushing | Post-Brushing | p-Value | |
| All surface | ||||||
| PB | 1.24 ± 0.36 | 0.88 ± 0.27 | 0.000 | 0.22 ± 0.19 | 0.11 ± 0.11 | 0.000 |
| CB | 1.22 ± 0.33 | 0.93 ± 0.33 | 0.000 | 0.19 ± 0.16 | 0.12 ± 0.13 | 0.000 |
| Interproximal surface | ||||||
| PB | 1.41 ± 0.36 | 1.05 ± 0.28 | 0.000 | 0.28 ± 0.24 | 0.13 ± 0.16 | 0.000 |
| CB | 1.40 ± 0.34 | 1.11 ± 0.36 | 0.000 | 0.23 ± 0.21 | 0.15 ± 0.17 | 0.000 |
| Lingual surface | ||||||
| PB | 1.36 ± 0.42 | 1.02 ± 0.36 | 0.000 | 0.22 ± 0.19 | 0.13 ± 0.12 | 0.001 |
| CB | 1.36 ± 0.41 | 1.05 ± 0.43 | 0.000 | 0.22 ± 0.17 | 0.15 ± 0.16 | 0.000 |
| Reduction Plaque Index (PI) | Reduction Gingival Index (GI) | |||||
|---|---|---|---|---|---|---|
| PB | CB | p-Value | PB | CB | p-Value | |
| All surface | −0.36 ± 0.29 | −0.28 ± 0.29 | 0.252 | −0.11 ± 0.12 | −0.07 ± 0.09 | 0.062 |
| Interproximal surface | −0.36 ± 0.31 | −0.29 ± 0.32 | 0.307 | −0.14 ± 0.16 | −0.08 ± 0.13 | 0.034 |
| Lingual surface | −0.33 ± 0.31 | −0.31 ± 0.36 | 0.75 | −0.08 ± 0.14 | −0.07 ± 0.12 | 0.673 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lee, J.-H.; Ha, J.-H. Bioelectric Effect of a Microcurrent Toothbrush on Plaque Removal. Int. J. Environ. Res. Public Health 2021, 18, 8255. https://doi.org/10.3390/ijerph18168255
Lee J-H, Ha J-H. Bioelectric Effect of a Microcurrent Toothbrush on Plaque Removal. International Journal of Environmental Research and Public Health. 2021; 18(16):8255. https://doi.org/10.3390/ijerph18168255
Chicago/Turabian StyleLee, Ji-Hyun, and Jin-Hee Ha. 2021. "Bioelectric Effect of a Microcurrent Toothbrush on Plaque Removal" International Journal of Environmental Research and Public Health 18, no. 16: 8255. https://doi.org/10.3390/ijerph18168255
APA StyleLee, J.-H., & Ha, J.-H. (2021). Bioelectric Effect of a Microcurrent Toothbrush on Plaque Removal. International Journal of Environmental Research and Public Health, 18(16), 8255. https://doi.org/10.3390/ijerph18168255






