The Relationship between the Urinary Cadmium Concentration and Cause-Specific Mortality in Subjects without Severe Renal Damage: A 35-Year Follow-Up Study in a Cadmium-Polluted Area of Japan
Abstract
:1. Introduction
2. Materials and Methods
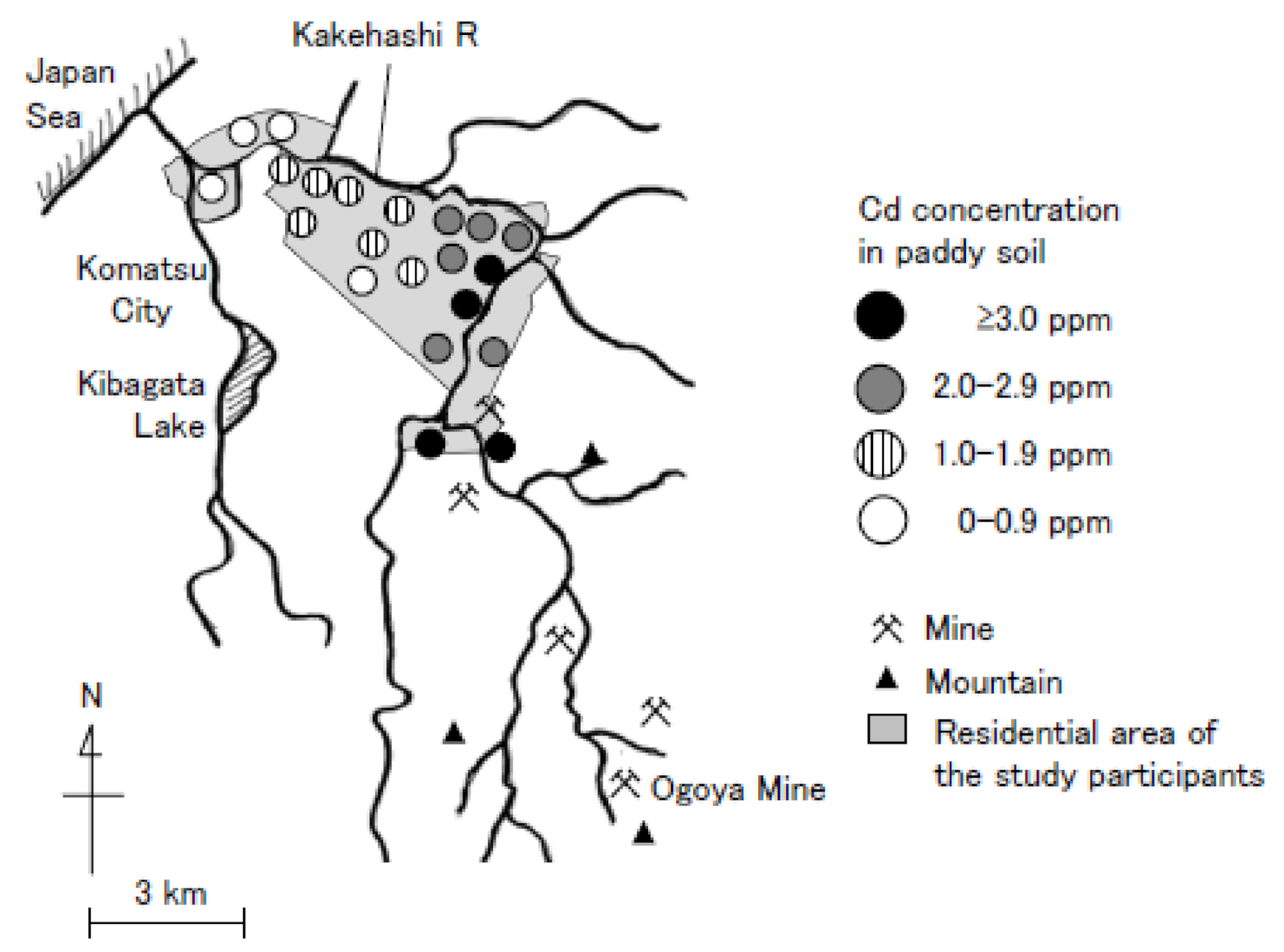
2.1. Study Population
2.2. Follow-Up
2.3. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Nishijo, M.; Nakagawa, H.; Morikawa, Y.; Tabata, M.; Senma, M.; Kitagawa, Y.; Kawano, S.; Ishizaki, M.; Sugita, N.; Nishi, M. Prognostic Factors of Renal Dysfunction Induced by Environmental Cadmium Pollution. Environ. Res. 1994, 64, 112–121. [Google Scholar] [CrossRef]
- Nakagawa, H.; Nishijo, M.; Morikawa, Y.; Tabata, M.; Miura, K.; Takahara, H.; Okumura, Y.; Yoshita, K.; Kawano, S.; Nishi, M.; et al. Increased urinary β2-microglobulin and mortality rate by cause of death in a Cadmium-polluted area. Environ. Health Prev. Med. 1996, 1, 144–148. [Google Scholar] [CrossRef]
- Nishijo, M.; Morikawa, Y.; Nakagawa, H.; Tawara, K.; Miura, K.; Kido, T.; Ikawa, A.; Kobatashi, E.; Nogawa, K. Causes of death and renal tubular dysfunction in residents exposed to cadmium in the environment. Occup. Environ. Med. 2006, 63, 545–550. [Google Scholar] [CrossRef]
- Li, Q.; Nishijo, M.; Nakagawa, H.; Morikawa, Y.; Sakurai, M.; Nakamura, K.; Kido, T.; Nogawa, K.; Dai, M. Relationship between urinary cadmium and mortality in habitants of a cadmium-polluted area: A 22-year follow-up study in Japan. Chin. Med. J. 2011, 124, 3504–3509. [Google Scholar]
- Nakagawa, H.; Nishijo, M.; Morikawa, Y.; Tabata, M.; Senma, M.; Kitagawa, Y.; Kawano, S.; Ishizaki, M.; Sugita, N.; Nishi, M.; et al. Urinary beta 2-microglobulin concentration and mortality in a cadmium-polluted area. Arch. Environ. Health 1993, 48, 428–435. [Google Scholar] [CrossRef] [PubMed]
- Nakagawa, H.; Nishijo, M.; Morikawa, Y.; Miura, K.; Tawara, K.; Kuriwaki, J.-I.; Kido, T.; Ikawa, A.; Kobayashi, E.; Nogawa, K. Urinary cadmium and mortality among inhabitants of a cadmium-polluted area in Japan. Environ. Res. 2006, 100, 323–329. [Google Scholar] [CrossRef] [PubMed]
- Nishijo, M.; Nogawa, K.; Suwazono, Y.; Kido, T.; Sakurai, M.; Nakagawa, H. Lifetime Cadmium Exposure and Mortality for Renal Diseases in Residents of the Cadmium-Polluted Kakehashi River Basin in Japan. Toxics 2020, 8, 81. [Google Scholar] [CrossRef] [PubMed]
- Sakurai, M.; Suwazono, Y.; Nishijo, M.; Nogawa, K.; Watanabe, Y.; Ishizaki, M.; Morikawa, Y.; Kido, T.; Nakagawa, H. Relationship between urinary β2 -microglobulin concentration and mortality in a cadmium-polluted area in Japan: A 35-year follow-up study. J. Appl. Toxicol. 2021, 41, 224–232. [Google Scholar] [CrossRef]
- Nishijo, M.; Nakagawa, H.; Morikawa, Y.; Tabata, M.; Senma, M.; Miura, K.; Takahara, H.; Kawano, S.; Nishi, M.; Mizukoshi, K. Mortality of inhabitants in an area polluted by cadmium: 15-year follow up. Occup. Environ. Med. 1995, 52, 181–184. [Google Scholar] [CrossRef] [Green Version]
- International Agency for Research on Cancer. Cadmium and Cadmium Compounds. In Beryllium, Cadmium, Mercury, and Exposures in the Glass Manufacturing Industry; IARC Monogr., International Agency for Research on Cancer: Lyon, France, 2012; pp. 121–145. [Google Scholar]
- Verougstraete, V.; Lison, D.; Hotz, P. Cadmium, lung and prostate cancer: A systematic review of recent epidemiological data. J. Toxicol. Environ. Health B Crit. Rev. 2003, 6, 227–255. [Google Scholar] [CrossRef]
- Mendy, A.; Gasana, J.; Vieira, E.; Mendy, A.; Gasana, J.; Vieira, E. Urinary heavy metals and associated medical conditions in the US adult population. Int. J. Environ. Health Res. 2012, 22, 105–118. [Google Scholar] [CrossRef] [PubMed]
- Lee, M.-S.; Park, S.K.; Hu, H.; Lee, S. Cadmium exposure and cardiovascular disease in the 2005 Korea National Health and Nutrition Examination Survey. Environ. Res. 2011, 111, 171–176. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Peters, J.L.; Perlstein, T.S.; Perry, M.J.; McNeely, E.; Weuve, J. Cadmium exposure in association with history of stroke and heart failure. Environ. Res. 2010, 110, 199–206. [Google Scholar] [CrossRef] [Green Version]
- Park, S.K.; Sack, C.; Sirén, M.J.; Hu, H. Environmental Cadmium and Mortality from Influenza and Pneumonia in U.S. Adults. Environ. Health Perspect. 2020, 128, 127004. [Google Scholar] [CrossRef]
- Maruzeni, S.; Nishijo, M.; Nakamura, K.; Morikawa, Y.; Sakurai, M.; Nakashima, M.; Kido, T.; Okamoto, R.; Nogawa, K.; Suwazono, Y.; et al. Mortality and causes of deaths of inhabitants with renal dysfunction induced by cadmium exposure of the polluted Jinzu River basin, Toyama, Japan; A 26-year follow-up. Environ. Health 2014, 13, 18. [Google Scholar] [CrossRef] [Green Version]
- Fine, J.; Gray, R. A proportional hazards model for the subdistribution of a competing risk. J. Am. Stat. Assoc. 1999, 94, 496–509. [Google Scholar] [CrossRef]
- Nishijo, M.; Nakagawa, H.; Morikawa, Y.; Kuriwaki, J.-I.; Miura, K.; Kido, T.; Nogawa, K. Mortality in a cadmium polluted area in Japan. Biometals 2004, 17, 535–538. [Google Scholar] [CrossRef] [PubMed]
- Inskip, H.; Beral, V.; McDowall, M. Mortality of Shipham residents: 40-year follow-up. Lancet 1982, 1, 896–899. [Google Scholar] [CrossRef]
- Staessen, J.A.; Lauwerys, R.R.; Ide, G.; Roels, H.A.; Vyncke, G.; Amery, A. Renal function and historical environmental cadmium pollution from zinc smelters. Lancet 1994, 343, 1523–1527. [Google Scholar] [CrossRef]
- Knoflach, M.; Messner, B.; Shen, Y.H.; Frotschnig, S.; Liu, G.; Pfaller, K.; Wang, X.; Matosevic, B.; Willeit, J.; Kiechl, S.; et al. Non-toxic cadmium concentrations induce vascular inflammation and promote atherosclerosis. Circ. J. 2011, 75, 2491–2495. [Google Scholar] [CrossRef] [Green Version]
- Almenara, C.C.P.; Broseghini-Filho, G.B.; Vescovi, M.V.A.; Angeli, J.K.; Faria, T.D.O.; Stefanon, I.; Vassallo, D.; Padilha, A.S. Chronic cadmium treatment promotes oxidative stress and endothelial damage in isolated rat aorta. PLoS ONE 2013, 8, e68418. [Google Scholar] [CrossRef] [PubMed]
- Angeli, J.K.; Pereira, C.A.C.; Faria, T.D.O.; Stefanon, I.; Padilha, A.S.; Vassallo, D.V. Cadmium exposure induces vascular injury due to endothelial oxidative stress: The role of local angiotensin II and COX-2. Free Radic. Biol. Med. 2013, 65, 838–848. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Obeng-Gyasi, E. Chronic cadmium exposure and cardiovascular disease in adults. J. Environ. Sci. Health Part A 2020, 55, 726–729. [Google Scholar] [CrossRef]
- Xu, C.; Weng, Z.; Zhang, L.; Xu, J.; Dahal, M.; Basnet, T.B.; Gu, A. HDL cholesterol: A potential mediator of the association between urinary cadmium concentration and cardiovascular disease risk. Ecotoxicol. Environ. Saf. 2021, 208, 111433. [Google Scholar] [CrossRef] [PubMed]
- Fagerberg, B.; Borné, Y.; Barregard, L.; Sallsten, G.; Forsgard, N.; Hedblad, B.; Persson, M.; Engström, G. Cadmium exposure is associated with soluble urokinase plasminogen activator receptor, a circulating marker of inflammation and future cardiovascular disease. Environ. Res. 2017, 152, 185–191. [Google Scholar] [CrossRef] [Green Version]
- Lampe, B.J.; Park, S.K.; Robins, T.; Mukherjee, B.; Litonjua, A.A.; Amarasiriwardena, C.; Weisskopf, M.; Sparrow, D.; Hu, H.; Lampe, B.J.; et al. Association between 24-hour urinary cadmium and pulmonary function among community-exposed men: The VA Normative Aging Study. Environ. Health Perspect. 2008, 116, 1226–1230. [Google Scholar] [CrossRef] [Green Version]
- Hu, X.; Kim, K.-H.; Lee, Y.; Fernandes, J.; Smith, M.R.; Jung, Y.-J.; Orr, M.; Kang, S.-M.; Jones, D.P.; Go, Y.-M.; et al. Environmental Cadmium Enhances Lung Injury by Respiratory Syncytial Virus Infection. Am. J. Pathol. 2019, 189, 1513–1525. [Google Scholar] [CrossRef]
- Låg, M.; Rodionov, D.; Øvrevik, J.; Bakke, O.; Schwarze, P.E.; Refsnes, M. Cadmium-induced inflammatory responses in cells relevant for lung toxicity: Expression and release of cytokines in fibroblasts, epithelial cells and macrophages. Toxicol. Lett. 2010, 193, 252–260. [Google Scholar] [CrossRef] [PubMed]
- Koller, L. Cadmium. In Immunotoxicology of Environmental and Occupational Metals.; Zelikoff, J., Thomas, P., Eds.; Taylor and Francis: London, UK, 1998; pp. 41–61. [Google Scholar]
- Cao, X.; Lin, H.; Muskhelishvili, L.; Latendresse, J.; Richter, P.; Heflich, R.H. Tight junction disruption by cadmium in an in vitro human airway tissue model. Respir. Res. 2015, 16, 30. [Google Scholar] [CrossRef] [Green Version]
- Moulis, J.-M. Cellular mechanisms of cadmium toxicity related to the homeostasis of essential metals. Biometals 2010, 23, 877–896. [Google Scholar] [CrossRef]
- Baba, H.; Tsuneyama, K.; Yazaki, M.; Nagata, K.; Minamisaka, T.; Tsuda, T.; Nomoto, K.; Hayashi, S.; Miwa, S.; Nakajima, T.; et al. The liver in itai-itai disease (chronic cadmium poisoning): Pathological features and metallothionein expression. Mod. Pathol. 2013, 26, 1228–1234. [Google Scholar] [CrossRef] [PubMed]
- Davis, D.L.; Bradlow, H.L.; Wolff, M.; Woodruff, T.; Hoel, D.G.; Anton-Culver, H. Medical hypothesis: Xenoestrogens as preventable causes of breast cancer. Environ. Health Perspect. 1993, 101, 372–377. [Google Scholar] [CrossRef] [PubMed]
- Nagata, C.; Nagao, Y.; Shibuya, C.; Kashiki, Y.; Shimizu, H. Urinary cadmium and serum levels of estrogens and androgens in postmenopausal Japanese women. Cancer Epidemiol. Biomark. Prev. 2005, 14, 705–708. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Waalkes, M.R.; Rehm, S.; Coogan, T.P.; Ward, J.M. Role of cadmium in the etiology of cancer of the prostate. In Endocrine Toxicology, 2nd ed.; Taylor and Francis: Washington, DC, USA, 1997; pp. 227–243. [Google Scholar]
- Kolonel, L.N. Association of cadmium with renal cancer. Cancer 1976, 37, 1782–1787. [Google Scholar] [CrossRef]
- Nogawa, K.; Suwazono, Y.; Nishijo, M.; Sakurai, M.; Ishizaki, M.; Morikawa, Y.; Watanabe, Y.; Kido, T.; Nakagawa, H.; Nogawa, K.; et al. Increase of lifetime cadmium intake dose-dependently increased all cause of mortality in female inhabitants of the cadmium-polluted Jinzu River basin, Toyama, Japan. Environ. Res. 2018, 164, 379–384. [Google Scholar] [CrossRef]
- Nishijo, M.; Nakagawa, H.; Suwazono, Y.; Nogawa, K.; Sakurai, M.; Ishizaki, M.; Kido, T. Cancer Mortality in Residents of the Cadmium-Polluted Jinzu River Basin in Toyama, Japan. Toxics 2018, 6, E23. [Google Scholar] [CrossRef] [Green Version]
| Men | Women | |||
|---|---|---|---|---|
| β2-MG (μg/g Cr) | β2-MG (μg/g Cr) | |||
| <1000 | ≥1000 | <1000 | ≥1000 | |
| Number of participants | 1191 | 192 | 1386 | 314 |
| Number of deaths during the follow-up period (%) | 905 (76.0) | 184 (95.8) | 816 (58.9) | 279 (88.9) |
| Total person-years of observation | 23,102 | 2142 | 4184 | 31,187 |
| Mortality rate (/1000 person-years) | 39.2 | 85.9 | 26.2 | 66.7 |
| Mean observed years per person | 19.4 | 11.2 | 22.5 | 13.3 |
| Men, n (%) | Women, n (%) | |||
|---|---|---|---|---|
| β2-MG (μg/g Cr) | β2-MG (μg/g Cr) | |||
| <1000 | ≥1000 | <1000 | ≥1000 | |
| Malignant neoplasms | 273 (22.9) | 38 (19.8) | 193 (13.9) | 38 (12.1) |
| Esophagus | 4 (0.3) | 1 (0.5) | 1 (0.1) | 3 (1.0) |
| Stomach | 49 (4.1) | 8 (4.2) | 28 (2.0) | 4 (1.3) |
| Colon, rectum | 31 (2.6) | 4 (2.1) | 28 (2.0) | 7 (2.2) |
| Liver | 33 (2.8) | 1 (0.5) | 17 (1.2) | 0 (0.0) |
| Pancreas | 25 (2.1) | 5 (2.6) | 30 (2.2) | 3 (1.0) |
| Lung | 62 (5.2) | 10 (5.2) | 22 (1.6) | 7 (2.2) |
| Prostate | 16 (1.3) | 1 (0.5) | 0 (0.0) | 0 (0.0) |
| Breast | 0 (0.0) | 0 (0.0) | 8 (0.6) | 3 (1.0) |
| Uterus | 0 (0.0) | 0 (0.0) | 2 (0.1) | 0 (0.0) |
| Ovary | 0 (0.0) | 0 (0.0) | 6 (0.4) | 1 (0.3) |
| Bladder | 6 (0.5) | 2 (1.0) | 3 (0.2) | 2 (0.6) |
| Kidney | 4 (0.3) | 0 (0.0) | 1 (0.1) | 0 (0.0) |
| Lymphatic or hematopoietic tissue | 13 (1.1) | 4 (2.1) | 16 (1.2) | 1 (0.3) |
| Endocrine, nutritional, and metabolic diseases | 14 (1.2) | 2 (1.0) | 18 (1.3) | 7 (2.2) |
| Diabetes | 8 (0.7) | 2 (1.0) | 12 (0.9) | 4 (1.3) |
| Circulatory disease | 251 (21.1) | 68 (35.4) | 275 (19.8) | 110 (35.0) |
| Cardiovascular disease | 124 (10.4) | 31 (16.1) | 141 (10.2) | 61 (19.4) |
| Ischemic heart disease | 36 (3.0) | 9 (4.7) | 31 (2.2) | 14 (4.5) |
| Heart failure | 66 (5.5) | 15 (7.8) | 84 (6.1) | 38 (12.1) |
| Cerebrovascular disease | 113 (9.5) | 32 (16.7) | 128 (9.2) | 46 (14.6) |
| Cerebral hemorrhage | 23 (1.9) | 2 (1.0) | 28 (2.0) | 7 (2.2) |
| Cerebral infarction | 58 (4.9) | 7 (3.6) | 64 (4.6) | 7 (2.2) |
| Subarachnoidal hemorrhage | 4 (0.3) | 0 (0.0) | 14 (1.0) | 2 (0.6) |
| Diseases of the respiratory system | 162 (13.6) | 24 (12.5) | 113 (8.2) | 22 (7.0) |
| Pneumonia and influenza | 96 (8.1) | 12 (6.3) | 76 (5.5) | 16 (5.1) |
| Diseases of the digestive system | 33 (2.8) | 9 (4.7) | 33 (2.4) | 17 (5.4) |
| Gastric and duodenal ulcer | 1 (0.1) | 3 (1.6) | 1 (0.1) | 2 (0.6) |
| Ileus and intestinal obstruction | 3 (0.3) | 3 (1.6) | 5 (0.4) | 2 (0.6) |
| Liver cirrhosis | 11 (0.9) | 2 (1.0) | 8 (0.6) | 3 (1.0) |
| Kidney and urinary tract diseases | 22 (1.8) | 13 (6.8) | 20 (1.4) | 15 (4.8) |
| Renal disease | 0 (0.0) | 2 (1.0) | 2 (0.1) | 2 (0.6) |
| Renal failure | 16 (1.3) | 9 (4.7) | 12 (0.9) | 12 (3.8) |
| Senility | 39 (3.3) | 14 (7.3) | 71 (5.1) | 44 (14.0) |
| External causes of mortality | 53 (4.4) | 6 (3.1) | 37 (2.7) | 9 (2.9) |
| Toxic effects of cadmium | 1 (0.1) | 0 (0.0) | 2 (0.1) | 0 (0.0) |
| β2-MG: β2-microglobulin. | ||||
| Urinary Cd Concentration (μg/g Cr) | p for Trend | ||||
|---|---|---|---|---|---|
| <5.0 | 5.0–9.9 | ≥10.0 | |||
| Men | |||||
| All-cause mortality | n | 550 | 292 | 63 | |
| Mortality rate (/1000 PY) | 37.9 | 41.1 | 42.8 | ||
| HR (95%CI) | 1.00 (reference) | 1.08 (0.94–1.24) | 1.23 (0.95–1.60) | 0.092 | |
| Malignant neoplasm | n | 171 | 88 | 14 | |
| Mortality rate (/1000 PY) | 11.8 | 12.4 | 9.5 | ||
| HR (95%CI) | 1.00 (reference) | 1.06 (0.82–1.37) | 0.87 (0.51–1.51) | 0.95 | |
| RR (95%CI) | 1.00 (reference) | 1.00 (0.78–1.30) | 0.70 (0.41–1.20) | 0.37 | |
| Stomach | n | 27 | 20 | 2 | |
| Mortality rate (/1000 PY) | 1.9 | 2.8 | 1.4 | ||
| HR (95%CI) | 1.00 (reference) | 1.53 (0.86–2.73) | 0.78 (0.19–3.27) | 0.47 | |
| RR (95%CI) | 1.00 (reference) | 1.45 (0.82–2.58) | 0.66 (0.16–2.74) | 0.64 | |
| Colon, rectum | n | 21 | 7 | 3 | |
| Mortality rate (/1000 PY) | 1.4 | 0.99 | 2.0 | ||
| HR (95%CI) | 1.00 (reference) | 0.66 (0.28–1.54) | 1.43 (0.43–1.48) | 0.85 | |
| RR (95%CI) | 1.00 (reference) | 0.65 (0.28–1.51) | 1.29 (0.39–4.28) | 0.78 | |
| Liver | n | 22 | 10 | 1 | |
| Mortality rate (/1000 PY) | 1.5 | 1.4 | 0.68 | ||
| HR (95%CI) | 1.00 (reference) | 0.96 (0.45–2.02) | 0.49 (0.07–3.65) | 0.58 | |
| RR (95%CI) | 1.00 (reference) | 0.90 (0.43–1.90) | 0.41 (0.06–3.02) | 0.40 | |
| Pancreas | n | 17 | 6 | 2 | |
| Mortality rate (/1000 PY) | 1.2 | 0.84 | 1.4 | ||
| HR (95%CI) | 1.00 (reference) | 0.73 (0.29–1.86) | 1.31 (0.30–5.70) | 0.86 | |
| RR (95%CI) | 1.00 (reference) | 0.68 (0.27–1.73) | 1.07 (0.25–4.65) | 0.69 | |
| Lung | n | 34 | 27 | 1 | |
| Mortality rate (/1000 PY) | 2.3 | 3.8 | 0.68 | ||
| HR (95%CI) | 1.00 (reference) | 1.61 (0.97–2.67) | 0.31 (0.04–2.28) | 0.62 | |
| RR (95%CI) | 1.00 (reference) | 1.57 (0.95–2.61) | 0.26 (0.04–1.89) | 0.81 | |
| Prostate | n | 13 | 3 | 0 | |
| Mortality rate (/1000 PY) | 0.90 | 0.42 | 0 | ||
| HR (95%CI) | 1.00 (reference) | 0.49 (0.14–1.73) | - | 0.42 | |
| RR (95%CI) | 1.00 (reference) | 0.45 (0.13–1.57) | 0.08 | ||
| Lymphatic or hematopoietic tissue | n | 9 | 3 | 1 | |
| Mortality rate (/1000 PY) | 0.62 | 0.42 | 0.68 | ||
| HR (95%CI) | 1.00 (reference) | 0.65 (0.18–2.42) | 1.19 (0.15–9.41) | 0.77 | |
| RR (95%CI) | 1.00 (reference) | 0.64 (0.17–2.36) | 0.99 (0.13–7.88) | 0.70 | |
| Women | |||||
| All-cause mortality | n | 228 | 404 | 184 | |
| Mortality rate (/1000 PY) | 25.1 | 26.7 | 26.4 | ||
| HR (95%CI) | 1.00 (reference) | 1.19 (1.01–1.40) | 1.22 (1.00–1.49) | 0.035 | |
| Malignant neoplasm | n | 58 | 93 | 42 | |
| Mortality rate (/1000 PY) | 6.4 | 6.1 | 6.0 | ||
| HR (95%CI) | 1.00 (reference) | 0.97 (0.70–1.35) | 0.97 (0.65–1.45) | 0.89 | |
| RR (95%CI) | 1.00 (reference) | 0.91 (0.66–1.27) | 0.90 (0.61–1.35) | 0.61 | |
| Stomach | n | 9 | 11 | 8 | |
| Mortality rate (/1000 PY) | 0.99 | 0.73 | 1.15 | ||
| HR (95%CI) | 1.00 (reference) | 0.75 (0.31–1.80) | 1.19 (0.46–3.09) | 0.64 | |
| RR (95%CI) | 1.00 (reference) | 0.70 (0.29–1.70) | 1.14 (0.44–2.92) | 0.79 | |
| Colon, rectum | n | 8 | 15 | 5 | |
| Mortality rate (/1000 PY) | 0.88 | 0.99 | 0.72 | ||
| HR (95%CI) | 1.00 (reference) | 1.16 (0.49–2.75) | 0.87 (0.28–2.68) | 0.87 | |
| RR (95%CI) | 1.00 (reference) | 1.09 (0.46–2.58) | 0.80 (0.26–2.45) | 0.73 | |
| Liver | n | 5 | 10 | 2 | |
| Mortality rate (/1000 PY) | 0.55 | 0.66 | 0.29 | ||
| HR (95%CI) | 1.00 (reference) | 1.20 (0.41–3.51) | 0.53 (0.10–2.75) | 0.55 | |
| RR (95%CI) | 1.00 (reference) | 1.14 (0.39–3.33) | 0.50 (0.10–2.57) | 0.43 | |
| Pancreas | n | 9 | 13 | 8 | |
| Mortality rate (/1000 PY) | 0.99 | 0.86 | 1.15 | ||
| HR (95%CI) | 1.00 (reference) | 0.87 (0.37–2.04) | 1.19 (0.46–3.08) | 0.76 | |
| RR (95%CI) | 1.00 (reference) | 0.83 (0.36–1.95) | 1.14 (0.44–2.96) | 0.83 | |
| Lung | n | 7 | 12 | 3 | |
| Mortality rate (/1000 PY) | 0.77 | 0.79 | 0.43 | ||
| HR (95%CI) | 1.00 (reference) | 1.11 (0.44–2.85) | 0.62 (0.16–2.43) | 0.58 | |
| RR (95%CI) | 1.00 (reference) | 1.00 (0.39–2.53) | 0.56 (0.14–2.22) | 0.43 | |
| Lymphatic or hematopoietic tissue | n | 5 | 7 | 4 | |
| Mortality rate (/1000 PY) | 0.55 | 0.46 | 0.57 | ||
| HR (95%CI) | 1.00 (reference) | 0.85 (0.27–2.67) | 1.05 (0.28–3.93) | 0.97 | |
| RR (95%CI) | 1.00 (reference) | 0.81 (0.26–2.56) | 1.03 (0.28–3.81) | 1.00 | |
| Urinary Cd Concentration (μg/g Cr) | p for Trend | ||||
|---|---|---|---|---|---|
| <5.0 | 5.0–9.9 | ≥10.0 | |||
| Men | |||||
| Circulatory disease | n | 158 | 74 | 19 | |
| Mortality rate (/1000 PY) | 10.9 | 10.4 | 12.9 | ||
| HR (95%CI) | 1.00 (reference) | 0.94 (0.71–1.24) | 1.29 (0.80–2.09) | 0.67 | |
| RR (95%CI) | 1.00 (reference) | 0.86 (0.65–1.15) | 1.11 (0.68–1.82) | 0.73 | |
| Cardiovascular disease | n | 77 | 33 | 14 | |
| Mortality rate (/1000 PY) | 5.3 | 4.6 | 9.5 | ||
| HR (95%CI) | 1.00 (reference) | 0.85 (0.56–1.28) | 1.92 (1.08–3.40) | 0.29 | |
| RR (95%CI) | 1.00 (reference) | 0.79 (0.52–1.20) | 1.72 (0.96–3.10) | 0.56 | |
| Ischemic heart disease | n | 20 | 11 | 5 | |
| Mortality rate (/1000 PY) | 1.4 | 1.5 | 3.4 | ||
| HR (95%CI) | 1.00 (reference) | 1.11 (0.53–2.31) | 2.64 (0.99–7.04) | 0.13 | |
| RR (95%CI) | 1.00 (reference) | 1.06 (0.51–2.21) | 2.27 (0.84–6.05) | 0.24 | |
| Heart failure | n | 42 | 19 | 5 | |
| Mortality rate (/1000 PY) | 2.9 | 2.7 | 3.4 | ||
| HR (95%CI) | 1.00 (reference) | 0.86 (0.50–1.48) | 1.20 (0.47–3.04) | 0.94 | |
| RR (95%CI) | 1.00 (reference) | 0.82 (0.48–1.44) | 1.07 (0.42–2.72) | 0.76 | |
| Cerebrovascular disease | n | 73 | 35 | 5 | |
| Mortality rate (/1000 PY) | 5.0 | 4.9 | 3.4 | ||
| HR (95%CI) | 1.00 (reference) | 0.98 (0.65–1.47) | 0.75 (0.30–1.86) | 0.63 | |
| RR (95%CI) | 1.00 (reference) | 0.90 (0.60–1.36) | 0.59 (0.24–1.46) | 0.26 | |
| Cerebral hemorrhage | n | 13 | 10 | 0 | |
| Mortality rate (/1000 PY) | 0.90 | 1.4 | 0 | ||
| HR (95%CI) | 1.00 (reference) | 1.51 (0.66–3.44) | - | 0.95 | |
| RR (95%CI) | 1.00 (reference) | 1.46 (0.64–3.36) | - | 0.81 | |
| Cerebral infarction | n | 42 | 14 | 2 | |
| Mortality rate (/1000 PY) | 2.9 | 2.0 | 1.4 | ||
| HR (95%CI) | 1.00 (reference) | 0.77 (0.42–1.41) | 0.63 (0.15–2.60) | 0.31 | |
| RR (95%CI) | 1.00 (reference) | 0.63 (0.34–1.16) | 0.42 (0.10–1.73) | 0.07 | |
| Subarachnoidal hemorrhage | n | 2 | 2 | 0 | |
| Mortality rate (/1000 PY) | 0.14 | 0.28 | 0 | ||
| HR (95%CI) | - | - | - | ||
| RR (95%CI) | |||||
| Women | |||||
| Circulatory disease | n | 75 | 138 | 62 | |
| Mortality rate (/1000 PY) | 8.3 | 9.1 | 8.9 | ||
| HR (95%CI) | 1.00 (reference) | 1.30 (0.98–1.73) | 1.33 (0.94–1.86) | 0.08 | |
| RR (95%CI) | 1.00 (reference) | 1.17 (0.87–1.57) | 1.20 (0.85–1.71) | 0.28 | |
| Cardiovascular disease | n | 37 | 67 | 37 | |
| Mortality rate (/1000 PY) | 4.1 | 4.4 | 5.3 | ||
| HR (95%CI) | 1.00 (reference) | 1.36 (0.90–2.05) | 1.71 (1.07–2.71) | 0.02 | |
| RR (95%CI) | 1.00 (reference) | 1.13 (0.74–1.71) | 1.46 (0.91–2.35) | 0.13 | |
| Ischemic heart disease | n | 10 | 15 | 6 | |
| Mortality rate (/1000 PY) | 1.10 | 0.99 | 0.86 | ||
| HR (95%CI) | 1.00 (reference) | 1.07 (0.48–2.40) | 0.97 (0.35–2.70) | 0.98 | |
| RR (95%CI) | 1.00 (reference) | 0.91 (0.41–2.05) | 0.85 (0.31–2.34) | 0.75 | |
| Heart failure | n | 20 | 38 | 26 | |
| Mortality rate (/1000 PY) | 2.2 | 2.5 | 3.7 | ||
| HR (95%CI) | 1.00 (reference) | 1.53 (0.88–2.66) | 2.37 (1.31–4.30) | 0.004 | |
| RR (95%CI) | 1.00 (reference) | 1.17 (0.67–2.05) | 1.94 (1.06–3.54) | 0.038 | |
| Cerebrovascular disease | n | 34 | 69 | 25 | |
| Mortality rate (/1000 PY) | 3.7 | 4.6 | 3.6 | ||
| HR (95%CI) | 1.00 (reference) | 1.36 (0.90–2.07) | 1.11 (0.66–1.87) | 0.57 | |
| RR (95%CI) | 1.00 (reference) | 1.23 (0.81–1.85) | 1.00 (0.60–1.67) | 0.89 | |
| Cerebral hemorrhage | n | 6 | 20 | 2 | |
| Mortality rate (/1000 PY) | 0.66 | 1.32 | 0.29 | ||
| HR (95%CI) | 1.00 (reference) | 2.05 (0.82–5.11) | 0.46 (0.09–2.26) | 0.64 | |
| RR (95%CI) | 1.00 (reference) | 1.98 (0.79–4.94) | 0.44 (0.09–2.18) | 0.47 | |
| Cerebral infarction | n | 23 | 28 | 13 | |
| Mortality rate (/1000 PY) | 2.5 | 1.8 | 1.9 | ||
| HR (95%CI) | 1.00 (reference) | 0.87 (0.50–1.53) | 0.92 (0.46–1.84) | 0.77 | |
| RR (95%CI) | 1.00 (reference) | 0.70 (0.40–1.21) | 0.73 (0.37–1.45) | 0.33 | |
| Subarachnoidal hemorrhage | n | 2 | 8 | 4 | |
| Mortality rate (/1000 PY) | 0.22 | 0.53 | 0.57 | ||
| HR (95%CI) | 1.00 (reference) | 2.34 (0.54–11.0) | 2.56 (0.47–14.0) | 0.28 | |
| RR (95%CI) | 1.00 (reference) | 2.38 (0.50–11.2) | 2.59 (0.47–14.2) | 0.23 | |
| Urinary Cadmium Concentration (μg/g Cr) | p for Trend | ||||
|---|---|---|---|---|---|
| <5.0 | 5.0–9.9 | ≥10.0 | |||
| Men | |||||
| Endocrine, nutritional, and metabolic diseases | n | 8 | 6 | 0 | |
| Mortality rate (/1000 PY) | 0.55 | 0.84 | 0 | ||
| HR (95%CI) | 1.00 (reference) | 1.53 (0.53–4.41) | - | 0.98 | |
| RR (95%CI) | 1.00 (reference) | 1.50 (0.52–4.32) | - | 0.89 | |
| Diseases of the respiratory system | n | 95 | 53 | 14 | |
| Mortality rate (/1000 PY) | 6.5 | 7.5 | 9.5 | ||
| HR (95%CI) | 1.00 (reference) | 1.14 (0.81–1.59) | 1.63 (0.93–2.85) | 0.11 | |
| RR (95%CI) | 1.00 (reference) | 1.08 (0.77–1.52) | 1.36 (0.77–2.42) | 0.32 | |
| Pneumonia and influenza | n | 59 | 26 | 11 | |
| Mortality rate (/1000 PY) | 4.1 | 3.7 | 7.5 | ||
| HR (95%CI) | 1.00 (reference) | 0.92 (0.58–1.46) | 2.10 (1.10–4.00) | 0.19 | |
| RR (95%CI) | 1.00 (reference) | 0.83 (0.52–1.33) | 1.73 (0.90–3.31) | 0.51 | |
| Diseases of the digestive system | n | 16 | 11 | 6 | |
| Mortality rate (/1000 PY) | 1.1 | 1.5 | 4.1 | ||
| HR (95%CI) | 1.00 (reference) | 1.40 (0.65–3.03) | 3.81 (1.49–9.74) | 0.014 | |
| RR (95%CI) | 1.00 (reference) | 1.37 (0.63–2.96) | 3.52 (1.39–8.95) | 0.028 | |
| Liver cirrhosis | n | 5 | 5 | 1 | |
| Mortality rate (/1000 PY) | 0.34 | 0.70 | 0.68 | ||
| HR (95%CI) | 1.00 (reference) | 2.05 (0.59–7.09) | 1.91 (0.22–16.3) | 0.68 | |
| RR (95%CI) | 1.00 (reference) | 2.04 (0.60–6.95) | 1.87 (0.22–15.9) | 0.25 | |
| Kidney and urinary tract diseases | n | 14 | 6 | 2 | |
| Mortality rate (/1000 PY) | 0.96 | 0.84 | 1.36 | ||
| HR (95%CI) | 1.00 (reference) | 0.83 (0.32–2.17) | 1.67 (0.38–7.39) | 0.81 | |
| RR (95%CI) | 1.00 (reference) | 0.80 (0.31–2.10) | 1.27 (0.29–5.56) | 0.96 | |
| Senility | n | 20 | 17 | 2 | |
| Mortality rate (/1000 PY) | 1.4 | 2.4 | 1.4 | ||
| HR (95%CI) | 1.00 (reference) | 1.64 (0.85–3.16) | 1.17 (0.27–5.05) | 0.27 | |
| RR (95%CI) | 1.00 (reference) | 1.60 (0.83–3.08) | 0.88 (0.20–3.80) | 0.40 | |
| External causes of mortality | n | 31 | 18 | 4 | |
| Mortality rate (/1000 PY) | 2.1 | 2.5 | 2.7 | ||
| HR (95%CI) | 1.00 (reference) | 1.19 (0.67–2.13) | 1.33 (0.47–3.77) | 0.47 | |
| RR (95%CI) | 1.00 (reference) | 1.14 (0.64–2.04) | 1.19 (0.41–3.39) | 0.62 | |
| Women | |||||
| Endocrine, nutritional, and metabolic diseases | n | 2 | 12 | 4 | |
| Mortality rate (/1000 PY) | 0.22 | 0.79 | 0.57 | ||
| HR (95%CI) | 1.00 (reference) | 3.72 (0.83–16.7) | 2.79 (0.51–15.3) | 0.25 | |
| RR (95%CI) | 1.00 (reference) | 3.46 (0.78–15.4) | 2.58 (0.47–14.2) | 0.20 | |
| Diseases of the respiratory system | n | 35 | 50 | 28 | |
| Mortality rate (/1000 PY) | 3.9 | 3.3 | 4.0 | ||
| HR (95%CI) | 1.00 (reference) | 1.06 (0.68–1.65) | 1.37 (0.83–2.27) | 0.24 | |
| RR (95%CI) | 1.00 (reference) | 0.82 (0.53–1.27) | 1.08 (0.65–1.78) | 0.87 | |
| Pneumonia and influenza | n | 18 | 36 | 22 | |
| Mortality rate (/1000 PY) | 2.0 | 2.4 | 3.2 | ||
| HR (95%CI) | 1.00 (reference) | 1.55 (0.87–2.77) | 2.22 (1.17–4.19) | 0.014 | |
| RR (95%CI) | 1.00 (reference) | 1.17 (0.66–2.05) | 1.68 (0.90–3.13) | 0.11 | |
| Diseases of the digestive system | n | 9 | 13 | 11 | |
| Mortality rate (/1000 PY) | 0.99 | 0.86 | 1.6 | ||
| HR (95%CI) | 1.00 (reference) | 1.02 (0.43–2.41) | 1.95 (0.80–4.74) | 0.15 | |
| RR (95%CI) | 1.00 (reference) | 0.87 (0.37–2.03) | 1.71 (0.71–4.10) | 0.28 | |
| Liver cirrhosis | n | 2 | 3 | 3 | |
| Mortality rate (/1000 PY) | 0.22 | 0.20 | 0.43 | ||
| HR (95%CI) | - | - | - | ||
| RR (95%CI) | |||||
| Kidney and urinary tract diseases | n | 4 | 12 | 4 | |
| Mortality rate (/1000 PY) | 0.44 | 0.79 | 0.57 | ||
| HR (95%CI) | 1.00 (reference) | 2.07 (0.66–6.52) | 1.56 (0.38–6.33) | 0.49 | |
| RR (95%CI) | 1.00 (reference) | 1.75 (0.56–5.44) | 1.33 (0.33–5.41) | 0.61 | |
| Senility | n | 22 | 38 | 11 | |
| Mortality rate (/1000 PY) | 2.4 | 2.5 | 1.6 | ||
| HR (95%CI) | 1.00 (reference) | 1.38 (0.80–2.36) | 0.93 (0.45–1.95) | 0.93 | |
| RR (95%CI) | 1.00 (reference) | 1.04 (0.61–1.77) | 0.70 (0.33–1.45) | 0.38 | |
| External causes of mortality | n | 7 | 17 | 13 | |
| Mortality rate (/1000 PY) | 0.77 | 1.1 | 1.9 | ||
| HR (95%CI) | 1.00 (reference) | 1.47 (0.61–3.56) | 2.51 (1.00–6.30) | 0.044 | |
| RR (95%CI) | 1.00 (reference) | 1.41 (0.59–3.40) | 2.44 (0.97–6.16) | 0.057 | |
| Urinary Cd Concentration (μg/g Cr) | p for Trend | ||||
|---|---|---|---|---|---|
| <5.0 | 5.0–9.9 | ≥10.0 | |||
| Men | |||||
| Malignant neoplasms | n | 7 | 14 | 17 | |
| Mortality rate (/1000 PY) | 12.7 | 18.8 | 20.1 | ||
| HR (95%CI) | 1.00 (reference) | 1.22 (0.48–3.10) | 1.30 (0.53–3.17) | 0.58 | |
| RR (95%CI) | 1.00 (reference) | 1.34 (0.56–3.21) | 1.55 (0.66–3.64) | 0.31 | |
| Endocrine, nutritional, and metabolic diseases | n | 0 | 2 | 0 | |
| Mortality rate (/1000 PY) | 0 | 2.7 | 0 | ||
| Circulatory disease | n | 19 | 23 | 26 | |
| Mortality rate (/1000 PY) | 34.6 | 30.9 | 30.7 | ||
| HR (95%CI) | 1.00 (reference) | 0.66 (0.36–1.23) | 0.74 (0.41–1.34) | 0.40 | |
| RR (95%CI) | 1.00 (reference) | 0.61 (0.32–1.15) | 0.72 (0.40–1.32) | 0.40 | |
| Cardiovascular disease | n | 10 | 7 | 14 | |
| Mortality rate (/1000 PY) | 18.2 | 9.4 | 16.5 | ||
| HR (95%CI) | 1.00 (reference) | 0.37 (0.14–0.99) | 0.71 (0.31–1.62) | 0.62 | |
| RR (95%CI) | 1.00 (reference) | 0.36 (0.13–0.98) | 0.79 (0.35–1.78) | 0.82 | |
| Heart failure | n | 4 | 4 | 7 | |
| Mortality rate (/1000 PY) | 7.3 | 5.4 | 8.3 | ||
| HR (95%CI) | 1.00 (reference) | 0.48 (0.12–1.95) | 0.87 (0.25–3.02) | 0.99 | |
| RR (95%CI) | 1.00 (reference) | 0.51 (0.13–2.01) | 1.00 (0.29–3.43) | 0.85 | |
| Cerebrovascular disease | n | 9 | 12 | 11 | |
| Mortality rate (/1000 PY) | 16.4 | 16.1 | 13.0 | ||
| HR (95%CI) | 1.00 (reference) | 0.74 (0.31–1.77) | 0.66 (0.27–1.60) | 0.38 | |
| RR (95%CI) | 1.00 (reference) | 0.73 (0.30–1.76) | 0.69 (0.28–1.67) | 0.45 | |
| Diseases of the respiratory system | n | 5 | 8 | 11 | |
| Mortality rate (/1000 PY) | 9.1 | 10.7 | 13.0 | ||
| HR (95%CI) | 1.00 (reference) | 0.99 (0.31–3.13) | 1.25 (0.43–3.65) | 0.63 | |
| RR (95%CI) | 1.00 (reference) | 1.02 (0.30–3.43) | 1.38 (0.46–4.17) | 0.52 | |
| Pneumonia and influenza | n | 2 | 3 | 7 | |
| Mortality rate (/1000 PY) | 3.6 | 4.0 | 8.3 | ||
| HR (95%CI) | 1.00 (reference) | 0.87 (0.14–5.30) | 1.90 (0.39–9.27) | 0.30 | |
| RR (95%CI) | 1.00 (reference) | 0.99 (0.14–6.98) | 2.26 (0.43–11.7) | 0.25 | |
| Diseases of the digestive system | n | 1 | 6 | 2 | |
| Mortality rate (/1000 PY) | 1.8 | 8.1 | 2.4 | ||
| Kidney and urinary tract diseases | n | 2 | 7 | 4 | |
| Mortality rate (/1000 PY) | 3.6 | 9.4 | 4.7 | ||
| HR (95%CI) | 1.00 (reference) | 2.00 (0.41–9.83) | 1.02 (0.19–5.68) | 0.84 | |
| RR (95%CI) | 1.00 (reference) | 2.41 (0.48–12.2) | 1.24 (0.23–6.64) | 1.00 | |
| Senility | n | 3 | 6 | 5 | |
| Mortality rate (/1000 PY) | 5.5 | 8.1 | 5.9 | ||
| HR (95%CI) | 1.00 (reference) | 0.68 (0.16–2.91) | 0.87 (0.20–3.83) | 0.94 | |
| RR (95%CI) | 1.00 (reference) | 0.73 (0.20–2.69) | 0.90 (0.22–3.59) | 0.96 | |
| Women | |||||
| Malignant neoplasms | n | 1 | 11 | 26 | |
| Mortality rate (/1000 PY) | 4.4 | 8.4 | 9.8 | ||
| HR (95%CI) | 1.00 (reference) | 1.94 (0.25–15.1) | 2.25 (0.30–16.9) | 0.42 | |
| RR (95%CI) | 1.00 (reference) | 2.46 (0.32–19.2) | 2.91 (0.38–22.3) | 0.29 | |
| Endocrine, nutritional, and metabolic diseases | n | 0 | 2 | 5 | |
| Mortality rate (/1000 PY) | 0 | 1.5 | 1.9 | ||
| Circulatory disease | n | 9 | 44 | 57 | |
| Mortality rate (/1000 PY) | 39.8 | 33.6 | 21.5 | ||
| HR (95%CI) | 1.00 (reference) | 1.02 (0.50–2.10) | 0.75 (0.37–1.53) | 0.16 | |
| RR (95%CI) | 1.00 (reference) | 1.10 (0.52–2.29) | 0.74 (0.36–1.52) | 0.083 | |
| Cardiovascular disease | n | 4 | 26 | 31 | |
| Mortality rate (/1000 PY) | 17.7 | 19.9 | 11.7 | ||
| HR (95%CI) | 1.00 (reference) | 1.28 (0.44–3.68) | 0.86 (0.30–2.46) | 0.27 | |
| RR (95%CI) | 1.00 (reference) | 1.55 (0.54–4.44) | 0.96 (0.34–2.70) | 0.23 | |
| Heart failure | n | 2 | 17 | 19 | |
| Mortality rate (/1000 PY) | 8.8 | 13.0 | 7.2 | ||
| HR (95%CI) | 1.00 (reference) | 1.76 (0.40–7.65) | 1.16 (0.27–5.01) | 0.52 | |
| RR (95%CI) | 1.00 (reference) | 2.09 (0.50–8.78) | 1.28 (0.30–5.34) | 0.47 | |
| Cerebrovascular disease | n | 5 | 18 | 23 | |
| Mortality rate (/1000 PY) | 22.1 | 13.8 | 8.7 | ||
| HR (95%CI) | 1.00 (reference) | 0.81 (0.30–2.18) | 0.59 (0.22–1.55) | 0.19 | |
| RR (95%CI) | 1.00 (reference) | 0.81 (0.29–2.24) | 0.57 (0.21–1.53) | 0.16 | |
| Diseases of the respiratory system | n | 4 | 5 | 13 | |
| Mortality rate (/1000 PY) | 17.7 | 3.8 | 4.9 | ||
| HR (95%CI) | 1.00 (reference) | 0.24 (0.07–0.92) | 0.34 (0.11–1.07) | 0.30 | |
| RR (95%CI) | 1.00 (reference) | 0.26 (0.07–1.00) | 0.37 (0.11–1.20) | 0.42 | |
| Pneumonia and influenza | n | 3 | 4 | 9 | |
| Mortality rate (/1000 PY) | 13.3 | 3.1 | 3.4 | ||
| HR (95%CI) | 1.00 (reference) | 0.28 (0.06–1.28) | 0.34 (0.09–1.31) | 0.31 | |
| RR (95%CI) | 1.00 (reference) | 0.29 (0.07–1.28) | 0.36 (0.10–1.37) | 0.41 | |
| Diseases of the digestive system | n | 2 | 7 | 8 | |
| Mortality rate (/1000 PY) | 8.8 | 5.3 | 3.0 | ||
| HR (95%CI) | 1.00 (reference) | 0.69 (0.14–3.36) | 0.47 (0.10–2.21) | 0.28 | |
| RR (95%CI) | 1.00 (reference) | 0.81 (0.17–3.90) | 0.50 (0.11–2.42) | 0.26 | |
| Kidney and urinary tract diseases | n | 0 | 4 | 11 | |
| Mortality rate (/1000 PY) | 0 | 3.1 | 4.2 | ||
| Senility | n | 6 | 11 | 27 | |
| Mortality rate (/1000 PY) | 26.5 | 8.4 | 10.2 | ||
| HR (95%CI) | 1.00 (reference) | 0.42 (0.15–1.13) | 0.56 (0.23–1.37) | 0.62 | |
| RR (95%CI) | 1.00 (reference) | 0.36 (0.13–1.03) | 0.64 (0.26–1.58) | 0.90 | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sakurai, M.; Suwazono, Y.; Nishijo, M.; Nogawa, K.; Watanabe, Y.; Yoneda, K.; Ishizaki, M.; Morikawa, Y.; Kido, T.; Nakagawa, H. The Relationship between the Urinary Cadmium Concentration and Cause-Specific Mortality in Subjects without Severe Renal Damage: A 35-Year Follow-Up Study in a Cadmium-Polluted Area of Japan. Int. J. Environ. Res. Public Health 2021, 18, 7747. https://doi.org/10.3390/ijerph18157747
Sakurai M, Suwazono Y, Nishijo M, Nogawa K, Watanabe Y, Yoneda K, Ishizaki M, Morikawa Y, Kido T, Nakagawa H. The Relationship between the Urinary Cadmium Concentration and Cause-Specific Mortality in Subjects without Severe Renal Damage: A 35-Year Follow-Up Study in a Cadmium-Polluted Area of Japan. International Journal of Environmental Research and Public Health. 2021; 18(15):7747. https://doi.org/10.3390/ijerph18157747
Chicago/Turabian StyleSakurai, Masaru, Yasushi Suwazono, Muneko Nishijo, Kazuhiro Nogawa, Yuuka Watanabe, Kazuka Yoneda, Masao Ishizaki, Yuko Morikawa, Teruhiko Kido, and Hideaki Nakagawa. 2021. "The Relationship between the Urinary Cadmium Concentration and Cause-Specific Mortality in Subjects without Severe Renal Damage: A 35-Year Follow-Up Study in a Cadmium-Polluted Area of Japan" International Journal of Environmental Research and Public Health 18, no. 15: 7747. https://doi.org/10.3390/ijerph18157747
APA StyleSakurai, M., Suwazono, Y., Nishijo, M., Nogawa, K., Watanabe, Y., Yoneda, K., Ishizaki, M., Morikawa, Y., Kido, T., & Nakagawa, H. (2021). The Relationship between the Urinary Cadmium Concentration and Cause-Specific Mortality in Subjects without Severe Renal Damage: A 35-Year Follow-Up Study in a Cadmium-Polluted Area of Japan. International Journal of Environmental Research and Public Health, 18(15), 7747. https://doi.org/10.3390/ijerph18157747







