Profiles of Emotion Regulation and Post-Traumatic Stress Severity among Female Victims of Intimate Partner Violence
Abstract
:1. Introduction
1.1. Intimate Partner Violence
1.2. Post-Traumatic Stress Disorder (PTSD) and IPV
1.3. Emotional Regulation
1.4. Revictimization and Emotional Regulation
1.5. Current Study
2. Materials and Method
2.1. Participants
2.2. Procedure
2.3. Instruments
2.4. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Dokkedahl, S.; Kok, R.N.; Murphy, S.; Kristensen, T.R.; Bech-Hansen, D.; Elklit, A. The psychological subtype of intimate partner violence and its effect on mental health: Protocol for a systematic review and meta-analysis. Syst. Rev. 2019, 8, 198. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Violence Against Women Prevalence Estimates. 2018. Available online: https://cdn.who.int/media/docs/default-source/documents/violence-prevention/vaw_report_web_09032021_oleksandr.pdf?sfvrsn=a82ef89c_5&download=true (accessed on 20 March 2021).
- Breiding, M.J.; Chen, J.; Black, M. Intimate Partner Violence in the United States—2010; National Center for Injury Prevention and Control, Centers for Disease Control and Prevention: Atlanta, GA, USA, 2014.
- Devries, K.M.; Child, J.C.; Bacchus, L.J.; Mak, J.; Falder, G.; Graham, K.; Watts, C.; Heise, L. Intimate partner violence victimization and alcohol consumption in women: A systematic review and meta-analysis. Addiction 2014, 109, 379–391. [Google Scholar] [CrossRef] [PubMed]
- Vitoria-Estruch, S.; Romero-Martinez, A.; Lila, M.; Moya-Albiol, L. Could alcohol abuse drive intimate partner violence perpetrators’ psychophysiological response to acute stress? Int. J. Environ. Res. Public Health 2018, 15, 2729. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zilkens, R.R.; Smith, D.A.; Kelly, M.C.; Mukhtar, S.A.; Semmens, J.B.; Phillips, M.A. Sexual assault and general body injuries: A detailed cross-sectional Australian study of 1163 women. Forensic Sci. Int. 2017, 279, 112–120. [Google Scholar] [CrossRef]
- Devries, K.; Watts, C.; Yoshihama, M.; Kiss, L.; Schraiber, L.B.; Deyessa, N.; Heise, L.; Durand, J.; Mbwambo, J.; Jansen, H. Violence against women is strongly associated with suicide attempts: Evidence from the WHO multi-country study on women’s health and domestic violence against women. Soc. Sci. Med. 2011, 73, 79–86. [Google Scholar] [CrossRef]
- Ferrari, G.; Agnew-Davies, R.; Bailey, J.; Howard, L.; Howarth, E.; Peters, T.J.; Sardinha, L.; Feder, G.S. Domestic violence and mental health: A cross-sectional survey of women seeking help from domestic violence support services. Glob. Health Action 2016, 9, 29890. [Google Scholar] [CrossRef] [Green Version]
- Horn, S.R.; Feder, A. Understanding Resilience and Preventing and Treating PTSD. Harv. Rev. Psychiatry 2018, 26, 158–174. [Google Scholar] [CrossRef]
- Spencer, C.; Mallory, A.B.; Cafferky, B.M.; Kimmes, J.G.; Beck, A.R.; Stith, S.M. Mental health factors and intimate partner violence perpetration and victimization: A meta-analysis. Psychol. Violence 2019, 9, 1–17. [Google Scholar] [CrossRef]
- Lagdon, S.; Armour, C.; Stringer, M. Adult experience of mental health outcomes as a result of intimate partner violence victimization: A systematic review. Eur. J. Psychotraumatol. 2014, 5, 1–12. [Google Scholar] [CrossRef] [Green Version]
- Morina, N.; Wicherts, J.M.; Lobbrecht, J.; Priebe, S. Remission from posttraumatic stress disorder in adults: A systematic review and meta-analysis of long term outcome studies. Clin. Psychol. Revi. 2014, 34, 249–255. [Google Scholar] [CrossRef]
- Hansen, N.B.; Eriksen, S.B.; Elklit, A. Effects of an intervention program for female victims of intimate partner violence on psychological symptoms and perceived social support. Eur. J. Psychotraumatol. 2014, 5, 24797. [Google Scholar] [CrossRef] [Green Version]
- Irrizarry, W.; Rivero, M. Trastorno por estrés postraumático en mujeres víctima de violencia doméstica: Revisión de literatura integrada. NURE Inv. 2018, 15, 1–17. [Google Scholar]
- Karataş, R.D.; Altınöz, A.E.; Eşsizoğlu, A. Post-traumatic stress disorder and related factors among female victims of sexual assault required to attend a University Hospital in Turkey: A cross-sectional cohort study. CBHM 2020, 30, 79–94. [Google Scholar] [CrossRef]
- DeJonghe, E.S.; Bogat, G.A.; Levendosky, A.A.; von Eye, A. Women survivors of intimate partner violence and post-traumatic stress disorder: Prediction and prevention. J. Postgrad. Med. 2008, 54, 294–300. [Google Scholar] [CrossRef] [PubMed]
- Dillon, G.; Hussain, R.; Loxton, D.; Rahman, S. Mental and physical health and intimate partner violence against women: A review of the literature. Int. J. Family Med. 2013, 1–15. [Google Scholar] [CrossRef] [PubMed]
- Sharhabani-Arzy, R.; Amir, M.; Swisa, A. Self-criticism, dependency and posttraumatic stress disorder among a female group of help-seeking victims of domestic violence in Israel. Personal. Individ. Dif. 2005, 38, 1231–1240. [Google Scholar] [CrossRef]
- McLean, C.P.; Foa, E.B. Emotions and emotion regulation in posttraumatic stress disorder. Curr. Opin. Psychol. 2017, 14, 72–77. [Google Scholar] [CrossRef] [PubMed]
- Clohessy, S.; Ehlers, A. PTSD symptoms, response to intrusive memories and coping in ambulance service workers. Br. J. Clin. Psychol. 1999, 38, 251–265. [Google Scholar] [CrossRef] [PubMed]
- Kumpula, M.J.; Orcutt, H.K.; Bardeen, J.R.; Varkovitzky, R.L. Peritraumatic Dissociation and Experiential Avoidance as Prospective Predictors of Posttraumatic Stress Symptoms. J. Abnorm. Psychol. 2011, 120, 617–627. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Frewen, P.A.; Dozois, D.J.; Neufeld, R.W.; Lane, R.D.; Densmore, M.; Stevens, T.K.; Lanius, R.A. Emotional numbing in posttraumatic stress disorder: A functional magnetic resonance imaging study. J. Clin. Psychiatry 2012, 73, 431–436. [Google Scholar] [CrossRef]
- Powers, A.; Cross, D.; Fani, N.; Bradley, B. PTSD, emotion dysregulation, and dissociative symptoms in a highly traumatized sample. J. Psychiatr. Res. 2015, 61, 174–179. [Google Scholar] [CrossRef] [Green Version]
- Litz, B.T.; Gray, M.J. Emotional numbing in posttraumatic stress disorder: Current and future research directions. Aust. N. Z. J. Psychiatry 2002, 36, 198–204. [Google Scholar] [CrossRef]
- Gross, J.J. The emerging field of emotion regulation: An integrative review. Rev. Gen. Psychol. 1998, 2, 271–299. [Google Scholar] [CrossRef]
- Gratz, K.L.; Roemer, L. Multidimensional assessment of emotion regulation and dysregulation: Development, factor structure, and initial validation of the difficulties in emotion regulation scale. J. Psychopathol. Behav. Assess 2004, 26, 41–54. [Google Scholar] [CrossRef]
- Berking, M.; Orth, U.; Wupperman, P.; Meier, L.; Caspar, F. Prospective effects of emotion-regulation skills on emotional adjustment. J. Counsel. Psychol. 2008, 55, 485–494. [Google Scholar] [CrossRef] [Green Version]
- Seligowski, A.V.; Lee, D.J.; Bardeen, J.R.; Orcutt, H.K. Emotion regulation and posttraumatic stress symptoms: A meta-analysis. Cogn. Behav. Ther. 2015, 44, 87–102. [Google Scholar] [CrossRef] [PubMed]
- Walsh, K.; DiLillo, D.; Scalora, M.J. The cumulative impact of sexual revictimization on emotion regulation difficulties: An examination of female inmates. Violence Against Women 2011, 17, 1103–1118. [Google Scholar] [CrossRef]
- Lilly, M.M.; London, M.J.; Bridgett, D.J. Using SEM to examine emotion regulation and revictimization in predicting PTSD symptoms among childhood abuse survivors. Psychol. Trauma 2014, 6, 644–651. [Google Scholar] [CrossRef]
- Iverson, K.M.; Litwack, S.D.; Pineles, S.L.; Suvak, M.K.; Vaughn, R.A.; Resick, P.A. Predictors of intimate partner violence revictimization: The relative impact of distinct PTSD symptoms, dissociation, and coping strategies. J. Trauma. Stress 2013, 26, 102–110. [Google Scholar] [CrossRef] [PubMed]
- Kuijpers, K.F.; Van der Knaap, L.M.; Winkel, F.W. Victims’ influence on intimate partner violence revictimization: An empirical test of dynamic victim-related risk factors. J. Interpers. Violence 2012, 27, 1716–1742. [Google Scholar] [CrossRef]
- López-Ossorio, J.J.; González, J.L.; Buquerín, S.; García, L.F.; Buela-Casal, G. Risk factors related to intimate partner violence police recidivism in Spain International. Int. J. Clin. Health Psychol. 2017, 17, 107–119. [Google Scholar] [CrossRef] [PubMed]
- Classen, C.C.; Palesh, O.G.; Aggarwal, R. Sexual revictimization: A review of the empirical literature. Trauma Violence Abus. 2005, 6, 103–129. [Google Scholar] [CrossRef] [PubMed]
- Krause, E.D.; Kaltman, S.; Goodman, L.; Dutton, M.A. Role of distinct PTSD symptoms in intimate partner reabuse: A prospective study. J. Trauma. Stress 2006, 19, 507–516. [Google Scholar] [CrossRef] [PubMed]
- Ullman, S.E.; Najdowski, C.J.; Filipas, H.H. Child sexual abuse, post-traumatic stress disorder, and substance use: Predictors of revictimization in adult sexual assault survivors. J. Child Sex. Abus. 2009, 18, 367–385. [Google Scholar] [CrossRef] [PubMed]
- Alexander, P.C. Childhood trauma, attachment, and abuse by multiple partners. J. Psychol. Trauma 2009, 1, 78–88. [Google Scholar] [CrossRef]
- Portnoy, G.A.; Relyea, M.R.; Street, A.E. A Longitudinal Analysis of Women Veterans’ Partner Violence Perpetration: The Roles of Interpersonal Trauma and Posttraumatic Stress Symptoms. J. Fam. Viol. 2020, 35, 361–372. [Google Scholar] [CrossRef]
- Chesney, S.A.; Gordon, N.S. Profiles of emotion regulation: Understanding regulatory patterns and the implications for posttraumatic stress. Cogn. Emot. 2016, 1–9. [Google Scholar] [CrossRef] [Green Version]
- Aldao, A.; Nolen-Hoeksema, S. One versus many: Capturing the use of multiple emotion regulation strategies in response to an emotion-eliciting stimulus. Cogn. Emot. 2013, 27, 753–760. [Google Scholar] [CrossRef]
- Dixon-Gordon, K.L.; Aldao, A.; De Los Reyes, A. Repertoires of emotion regulation: A person-centered approach to assessing emotion regulation strategies and links to psychopathology. Cogn. Emot. 2014, 29, 1314–1325. [Google Scholar] [CrossRef]
- Eftekhari, A.; Zoellner, L.A.; Vigil, S.A. Patterns of emotion regulation and psychopathology. Anxiety Stress Coping 2009, 22, 571–586. [Google Scholar] [CrossRef] [Green Version]
- Baker, R.; Thomas, S.; Thomas, P.W.; Gower, P.; Santonastaso, M.; Whittlesea, A. The Emotional Processing Scale: Scale refinement and abridgement(EPS25). J. Psychosom. Res. 2010, 68, 83–88. [Google Scholar] [CrossRef] [PubMed]
- Echeburúa, E.; Amor, P.J.; Sarasua, B.; Zubizarreta, I.; Holgado-Tello, F.P.; Muñoz, J.M. Escala de Gravedad de Síntomas Revisada (EGS-R) del Trastorno de Estrés Postraumático según el DSM-5: Propiedades psicométricas. Ter. Psicol. 2016, 34, 111–128. [Google Scholar] [CrossRef] [Green Version]
- Echeburúa, E.; Corral, P.D.; Amor, P.J.; Zubizarreta, I.; Sarasua, B. Escala de gravedad de síntomas del trastorno de estrés postraumático: Propiedades psicométricas [Severity of symptoms of Post Traumatic Stress Scale: Psychometric properties]. Análisis Modif. Conducta 1997, 23, 503–526. [Google Scholar]
- Bremner, J.D.; Bolus, R.; Mayer, E.A. Psychometric properties of the Early Trauma Inventory-Self Report. J. Nerv. Ment. Dis. 2007, 195, 211–218. [Google Scholar] [CrossRef] [Green Version]
- Aldenderfer, M.S.; Blashfield, R.K. Cluster Analysis; Sage Publications Inc: Thousand Oaks, CA, USA, 1984. [Google Scholar]
- Clatworthy, J.; Buick, D.; Hankins, M.; Weinman, J.; Horne, R. The use and reporting of cluster analysis in health psychology: A review. Br. J. Health Psychol. 2005, 10, 329–358. [Google Scholar] [CrossRef]
- Bacher, J. Probabilistic Clustering Model for Variables of Mixed Type. Qual. Quant. 2000, 34, 223–235. [Google Scholar] [CrossRef]
- Masud, M.A.; Huang, J.; Wei, C.; Wang, J.; Khan, I.; Zhong, M. I-nice: A new approach for identifying the number of clusters and initial cluster centres. Inf. Sci. 2018, 466, 129–151. [Google Scholar] [CrossRef]
- Nylund, K.L.; Asparouhov, T.; Muthén, B.O. Deciding on the number of classes in latent class analysis and growth mixture modeling: A Monte Carlo simulation study. Struct. Equ. Modeling Multidiscip. J. 2007, 14, 535–569. [Google Scholar] [CrossRef]
- Rousseeuw, P.J. Silhouettes: A graphical aid to the interpretation and validation of cluster analysis. J. Comput. Appl. Math. 1987, 20, 53–65. [Google Scholar] [CrossRef] [Green Version]
- American Psychiatric Association—APA. The Diagnostic and Statistical Manual of Mental Disorders, DSM-5, 5th ed.; American Psychiatric Association: Washington, DC, USA, 2014. [Google Scholar]
- Cohen, J. Statistical Power Analysis for the Behavioral Sciences, 2nd ed.; LEA: New York, NY, USA, 1988. [Google Scholar]
- Goodman, L.; Dutton, M.A.; Vankos, N.; Weinfurt, K. Women’s resources and use of strategies as risk and protective factors for reabuse over time. Violence Against Women 2005, 11, 311–336. [Google Scholar] [CrossRef]
- Koenen, K.C.; Ratanatharathorn, A.; Ng, L.; McLaughlin, K.A.; Bromet, E.J.; Stein, D.J.; Karam, E.G.; Meron Ruscio, A.; Benjet, C.; Scott, K.; et al. Posttraumatic stress disorder in the World Mental Health Surveys. Psychol. Med. 2017, 47, 2260–2274. [Google Scholar] [CrossRef]
- Bardeen, J.R.; Kumpula, M.J.; Orcutt, H.K. Emotion regulation difficulties as a prospective predictor of posttraumatic stress symptoms following a mass shooting. J. Anxiety Disord. 2013, 27, 188–196. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Aldao, A.; Nolen-Hoeksema, S. When are adaptive strategies most predictive of psychopathology? J. Abnorm. Psychol. 2012, 121, 276–281. [Google Scholar] [CrossRef] [Green Version]
- Rachman, S. Emotional processing with special reference to post-traumatic stress disorder. Int. Rev. Psychiatry 2001, 13, 164–171. [Google Scholar] [CrossRef]
- Tull, M.T.; Roemer, L. Alternative explanations for emotional numbing of posttraumatic stress disorder: An examination of hyperarousal and experiential avoidance. J. Psychopathol. Behav. Assess 2003, 25, 147–154. [Google Scholar] [CrossRef]
- Ehring, T.; Quack, D. Emotion regulation difficulties in trauma survivors: The role of trauma type and PTSD symptom severity. Behav. Ther. 2010, 41, 587–598. [Google Scholar] [CrossRef]
- Cloitre, M.; Scarvalone, P.; Difede, J. Posttraumatic Stress Disorder, Self- and Interpersonal Dysfunction Among Sexually Retraumatized Women. J. Trauma. Stress 1997, 10, 437–452. [Google Scholar] [CrossRef] [PubMed]
- Matlow, R.B.; DePrince, A.P. The influence of victimization history on PTSD symptom expression in women exposed to intimate partner violence. Psychol. Trauma 2013, 5, 241–250. [Google Scholar] [CrossRef] [Green Version]
- Ford, J.D.; Steinberg, K.L.; Zhang, W.A. Randomized clinical trial comparing affect regulation and social problem-solving psychotherapies for mothers with victimization-related PTSD. Behav. Ther. 2011, 42, 560–578. [Google Scholar] [CrossRef] [PubMed]
- Finkelhor, D.; Ormrod, R.K.; Turner, H.A. Polyvictimization and trauma in a national longitudinal cohort. Dev. Psychopathol. 2007, 19, 149–166. [Google Scholar] [CrossRef] [PubMed]
- Ondé, D.; Alvarado, J.M. Análisis de clases latentes como técnica de identificación de tipologías. Int. J. Dev. Educ. Psychol. 2019, 5, 251–260. [Google Scholar]
- Benassi, M.; Garofalo, S.; Ambrosini, F.; Sant’Angelo, R.P.; Raggini, R.; De Paoli, G.; Ravani, C.; Giovagnoli, S.; Orsoni, M.; Piraccini, G. Using Two-Step Cluster Analysis and Latent Class Cluster Analysis to Classify the Cognitive Heterogeneity of Cross-Diagnostic Psychiatric Inpatients. Front. Psychol. 2020, 11, 1085. [Google Scholar] [CrossRef] [PubMed]
- Sabri, B.; Granger, D.A. Gender-based violence and trauma in marginalized populations of women: Role of biological embedding and toxic stress. Health Care Women Int. 2018, 39, 1038–1055. [Google Scholar] [CrossRef] [PubMed]
- Michopoulos, V.; Norrholm, S.D.; Jovanovic, T. Diagnostic Biomarkers for Posttraumatic Stress Disorder: Promising Horizons from Translational Neuroscience Research. Biol. Psychiatry 2015, 78, 344–353. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Le-Niculescu, H.; Roseberry, K.; Levey, D.F.; Rogers, J.; Kosary, K.; Prabha, S.; Jones, T.; Judd, S.; McCormick, M.A.; Wessel, A.R.; et al. Towards precision medicine for stress disorders: Diagnostic biomarkers and targeted drugs. Mol. Psychiatry 2020, 25, 918–938. [Google Scholar] [CrossRef] [Green Version]
- Domingo-Fernández, D.; Provost, A.; Kodamullil, A.T.; Marín-Llaó, J.; Lasseter, H.; Diaz, K.; Daskalakis, N.P.; Lancashire, L.; Hofmann-Apitius, M.; Haas, M. PTSD Biomarker Database: Deep dive metadatabase for PTSD biomarkers, visualizations and analysis tools. Database 2019. [Google Scholar] [CrossRef] [Green Version]
- Taylor, J.E.; Harvey, S.T. A meta-analysis of the effects of psychotherapy with adults sexually abused in childhood. Clin. Psychol. Rev. 2010, 30, 749–767. [Google Scholar] [CrossRef]
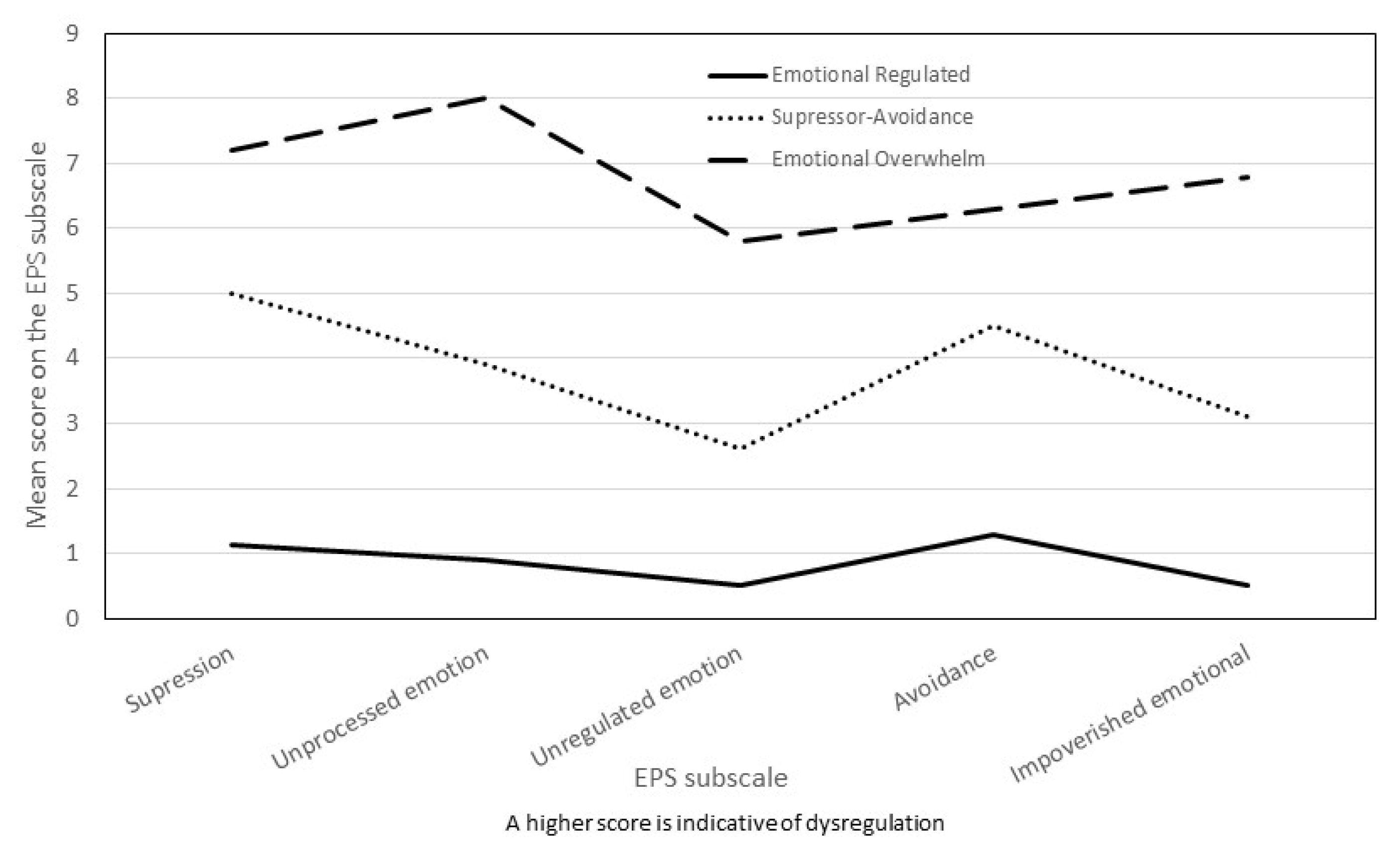
| EPS Sub-Scales | Emotional Overwhelm (n = 33) | Avoidance/ Non-Impoverished (n = 44) | Emotional Regulated (n = 43) | Total Sample (n = 120) | F(2, 120) | η2 |
|---|---|---|---|---|---|---|
| Suppression | 7.2 (1.3) | 5.0 (1.6) | 1.1 (1.2) | 4.2 (2.8) | 189.0 ** | 0.76 |
| Signs of Unprocessed Emotion | 8.0 (3.4) | 3.9 (1.7) | 0.9 (1.2) | 4.0 (3.5) | 94.6 ** | 0.62 |
| Unregulated Emotion | 5.8 (1.7) | 2.6 (1.6) | 0.5 (0.6) | 2.7 (2.5) | 141.1 ** | 0.70 |
| Avoidance | 6.3 (1.8) | 4.5 (1.7) | 1.3 (1.3) | 2.7 (2.5) | 90.3 ** | 0.61 |
| Impoverished Emotional Experience | 6.8 (3.7) | 3.1 (1.5) | 0.5 (0.7) | 3.9 (2.6) | 73.0 ** | 0.56 |
| EPS Total Score | 6.7 (3.7) | 2.7 (1.7) | 0.4 (0.6) | 3.0 (2.6) | 344.5 ** | 0.86 |
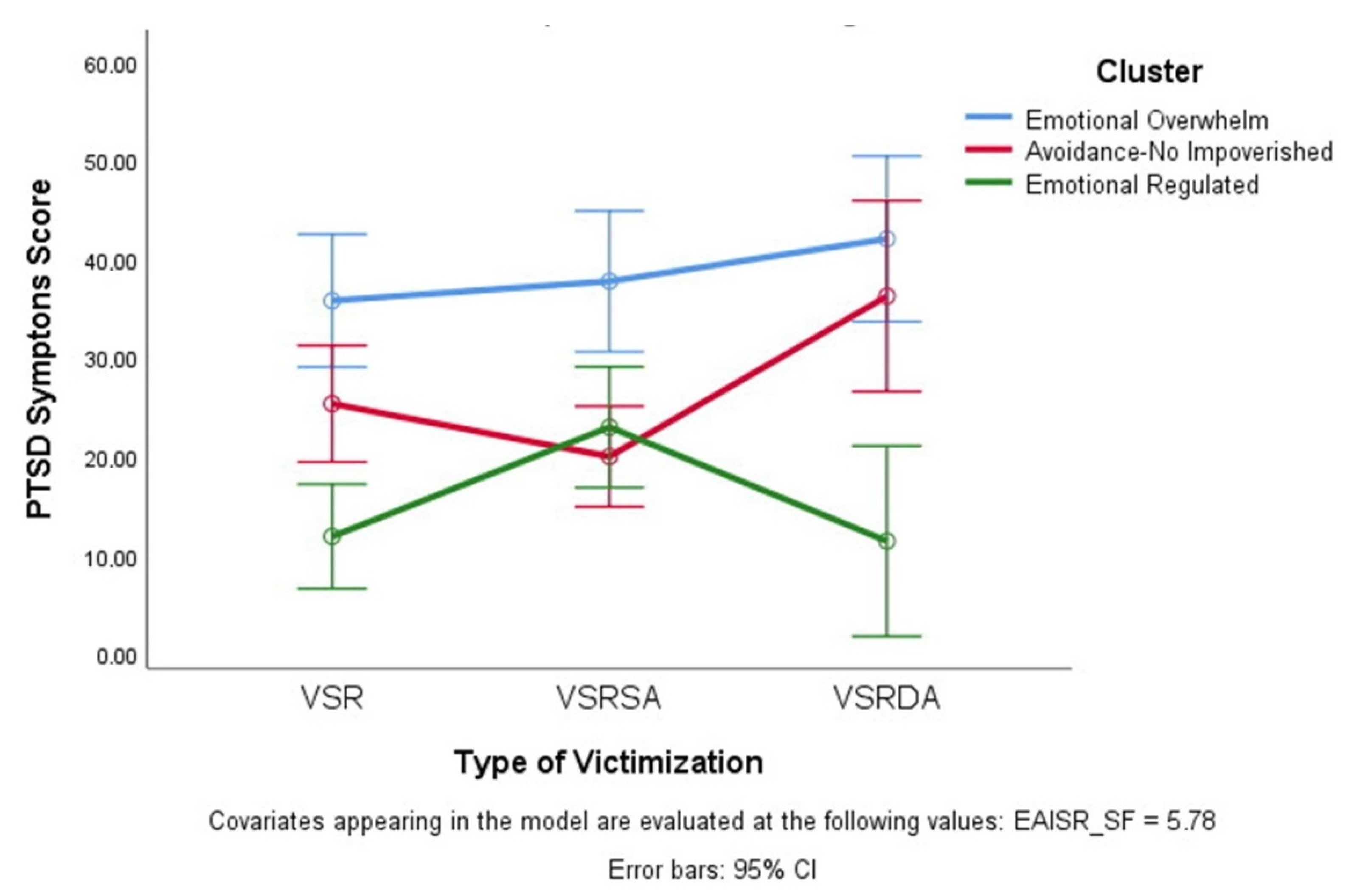
| VSR (n = 51) | VSRSA (n = 49) | VSRDA (n = 20) | Total Sample (n = 120) | |
|---|---|---|---|---|
| Emotional Regulated (n = 43) | 10.1 (8.3) | 22.5 (12.8) | 10.7 (5.2) | 14.8 (11.4) |
| Avoidance/Non-Impoverished (n = 44) | 24.9 (10.5) | 21.1 (13.7) | 37.5 (16.1) | 24.7 (13.8) |
| Emotional Overwhelm (n = 33) | 38.7 (12.6) | 36.8 (14.6) | 43.4 (13.9) | 39.2 (13.4) |
| Total Sample | 22.6 (15.4) | 25.1 (14.8) | 31.8 (18.8) | 25.1 (16.0) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Muñoz-Rivas, M.; Bellot, A.; Montorio, I.; Ronzón-Tirado, R.; Redondo, N. Profiles of Emotion Regulation and Post-Traumatic Stress Severity among Female Victims of Intimate Partner Violence. Int. J. Environ. Res. Public Health 2021, 18, 6865. https://doi.org/10.3390/ijerph18136865
Muñoz-Rivas M, Bellot A, Montorio I, Ronzón-Tirado R, Redondo N. Profiles of Emotion Regulation and Post-Traumatic Stress Severity among Female Victims of Intimate Partner Violence. International Journal of Environmental Research and Public Health. 2021; 18(13):6865. https://doi.org/10.3390/ijerph18136865
Chicago/Turabian StyleMuñoz-Rivas, Marina, Ana Bellot, Ignacio Montorio, Rosa Ronzón-Tirado, and Natalia Redondo. 2021. "Profiles of Emotion Regulation and Post-Traumatic Stress Severity among Female Victims of Intimate Partner Violence" International Journal of Environmental Research and Public Health 18, no. 13: 6865. https://doi.org/10.3390/ijerph18136865
APA StyleMuñoz-Rivas, M., Bellot, A., Montorio, I., Ronzón-Tirado, R., & Redondo, N. (2021). Profiles of Emotion Regulation and Post-Traumatic Stress Severity among Female Victims of Intimate Partner Violence. International Journal of Environmental Research and Public Health, 18(13), 6865. https://doi.org/10.3390/ijerph18136865





