The Research Centers in Minority Institutions (RCMI) Consortium: A Blueprint for Inclusive Excellence
Abstract
:1. Introduction
1.1. The Challenge of Achieving Diversity in the Biomedical Research Workforce
1.2. The Impact of the RCMI Consortium on Workforce Diversity and Health Equity
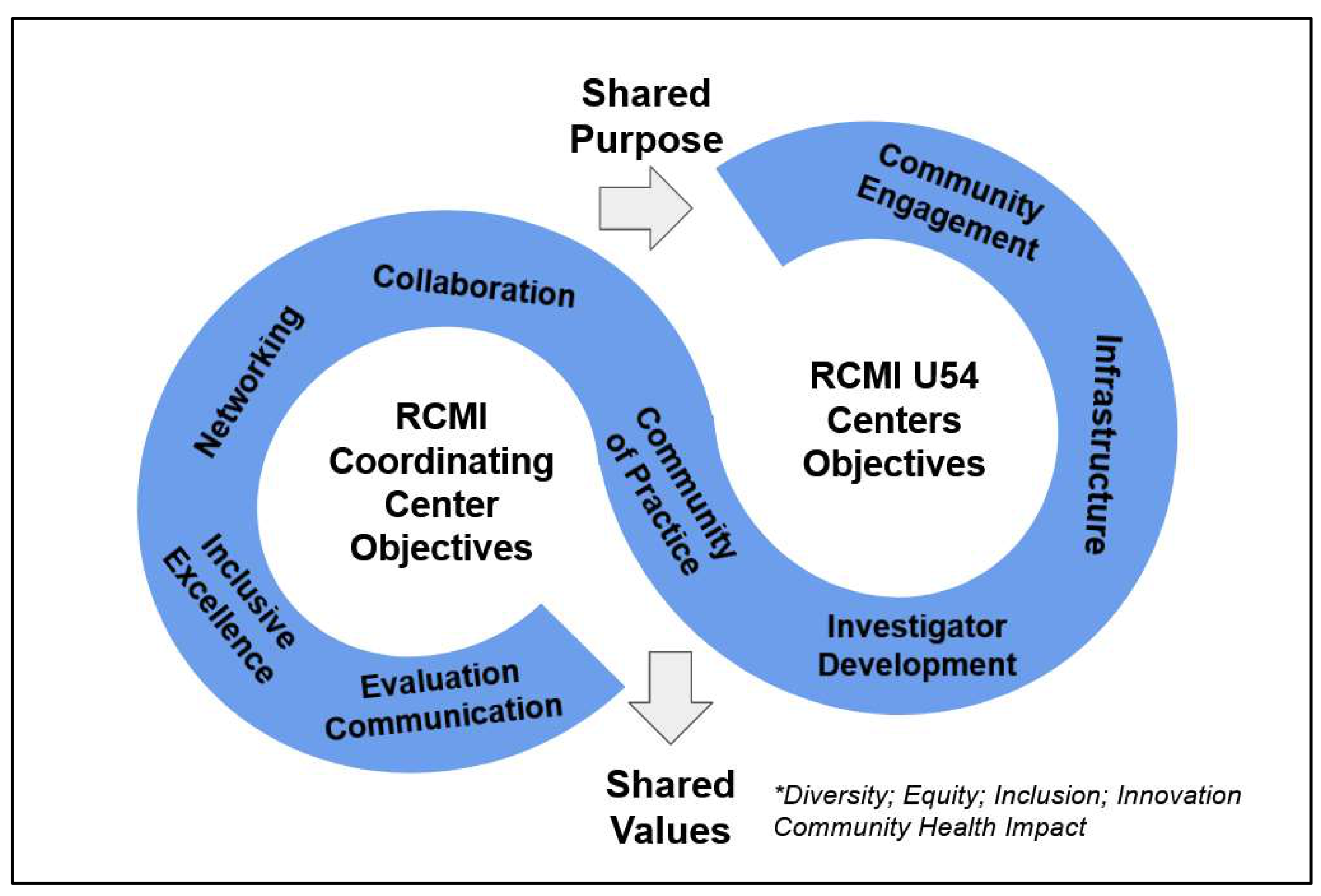
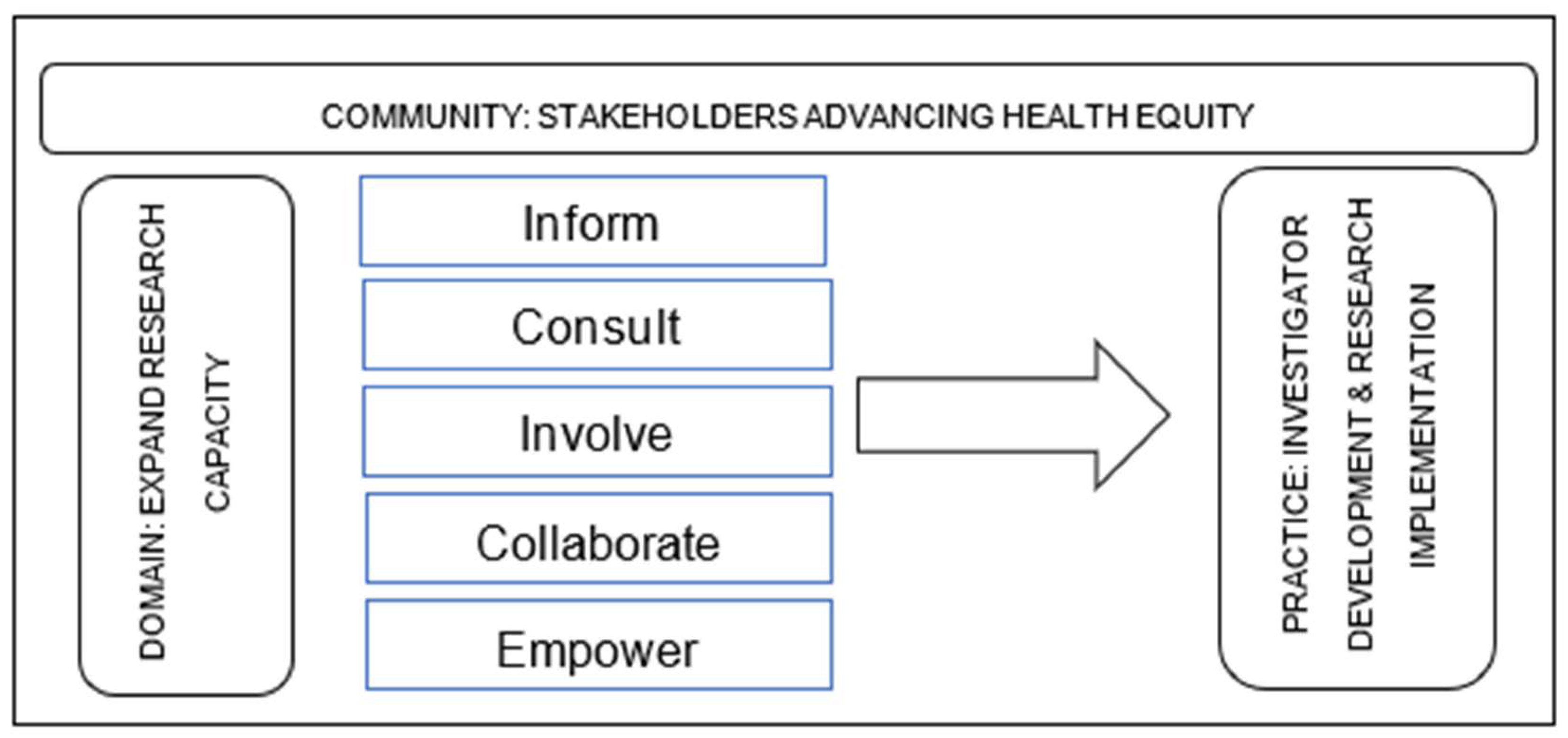
1.3. Theoretical Framework
1.4. How the Study Is Unique and Builds on Existing Literature
2. Methods
2.1. RCMI U54 Centers Needs Assessment
2.2. Community of Practice and Stakeholder Engagement
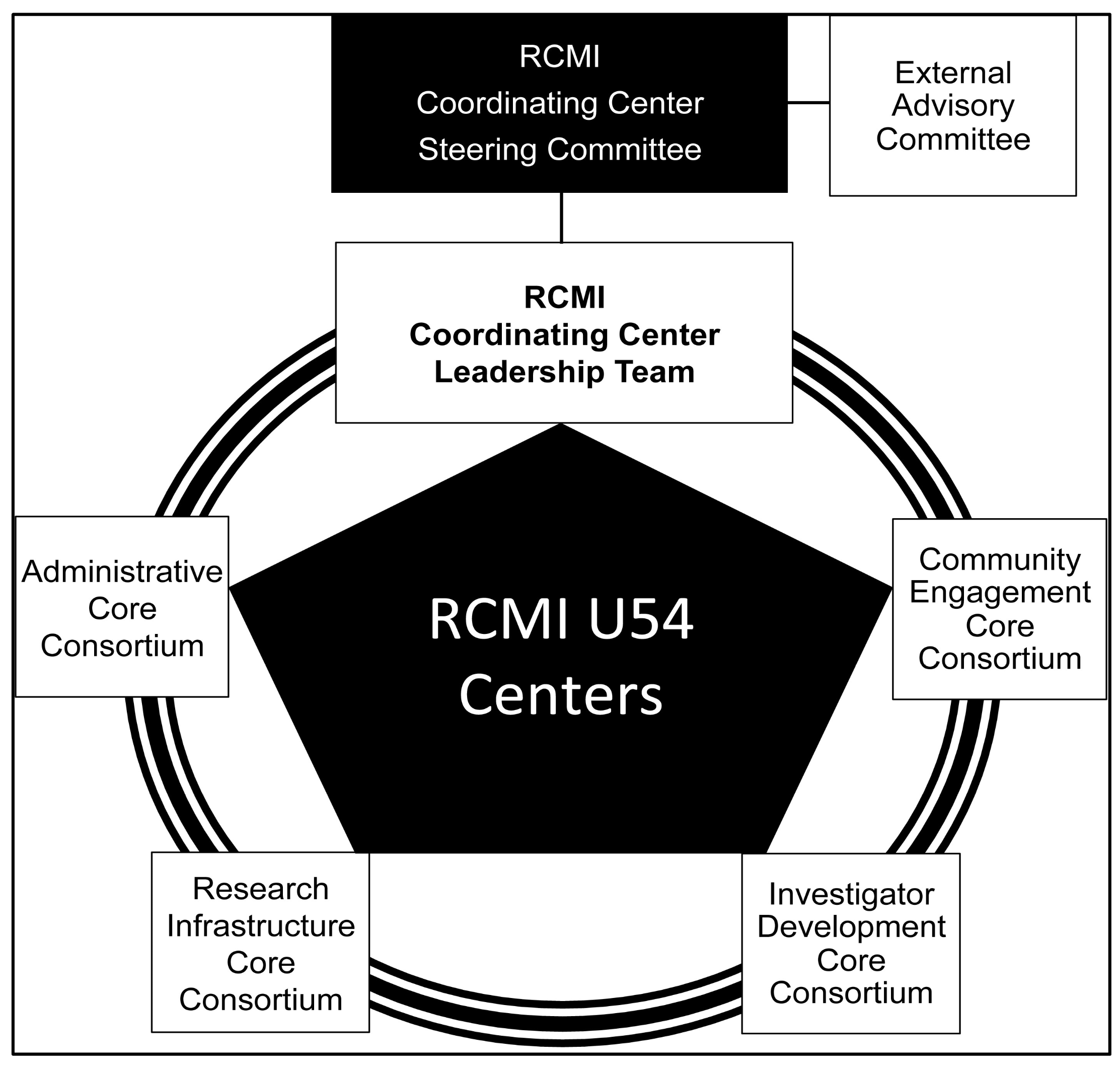
2.3. RCMI Consortium Centralized Database for Collaboration and Data Collection
3. Results
3.1. RCMI Consortium Institutions with Active U54 Center Awards
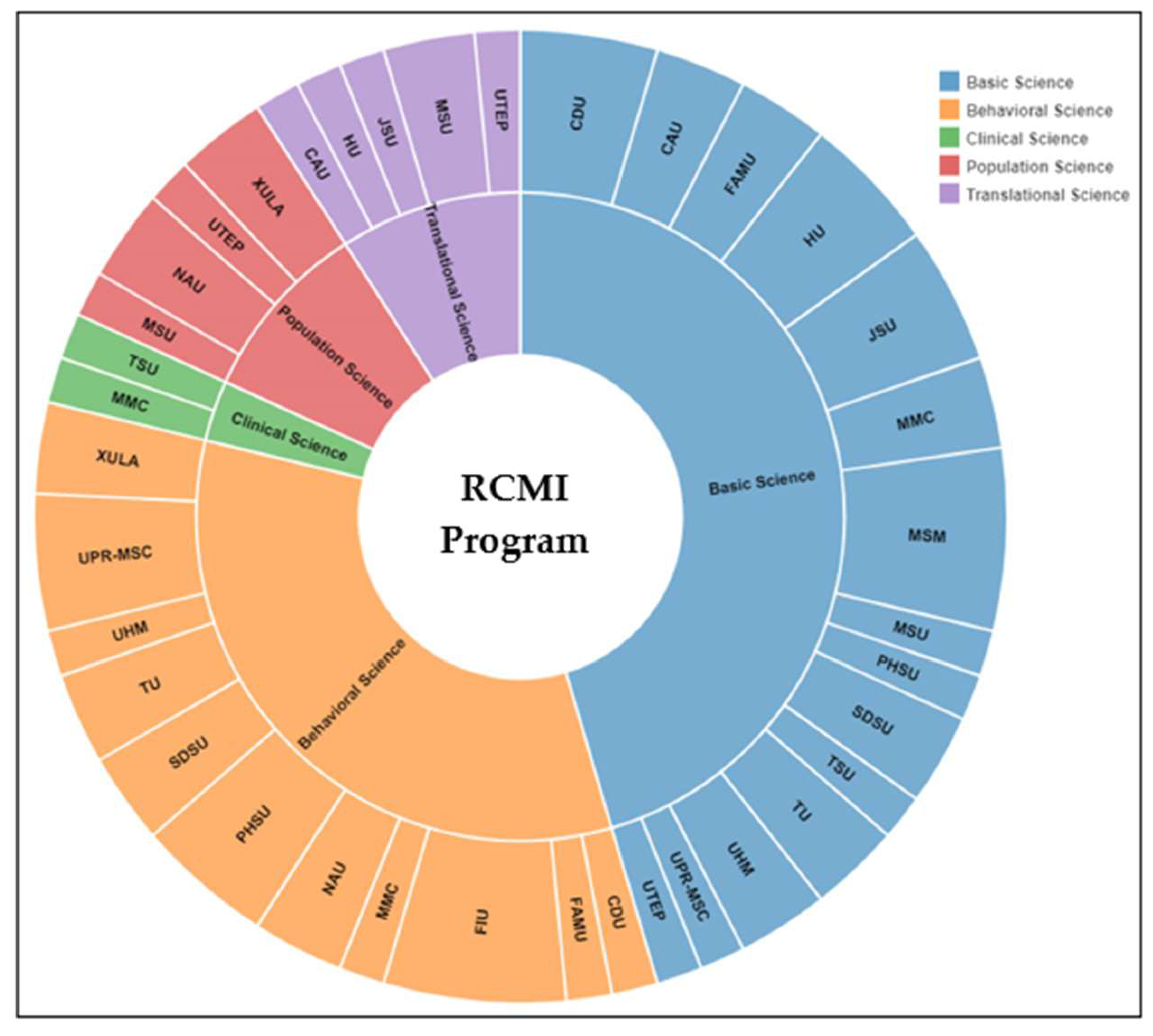
3.2. RCMI U54 Centers Prioritize Community Engagement Expertise and Investigator Development for Research Collaboration
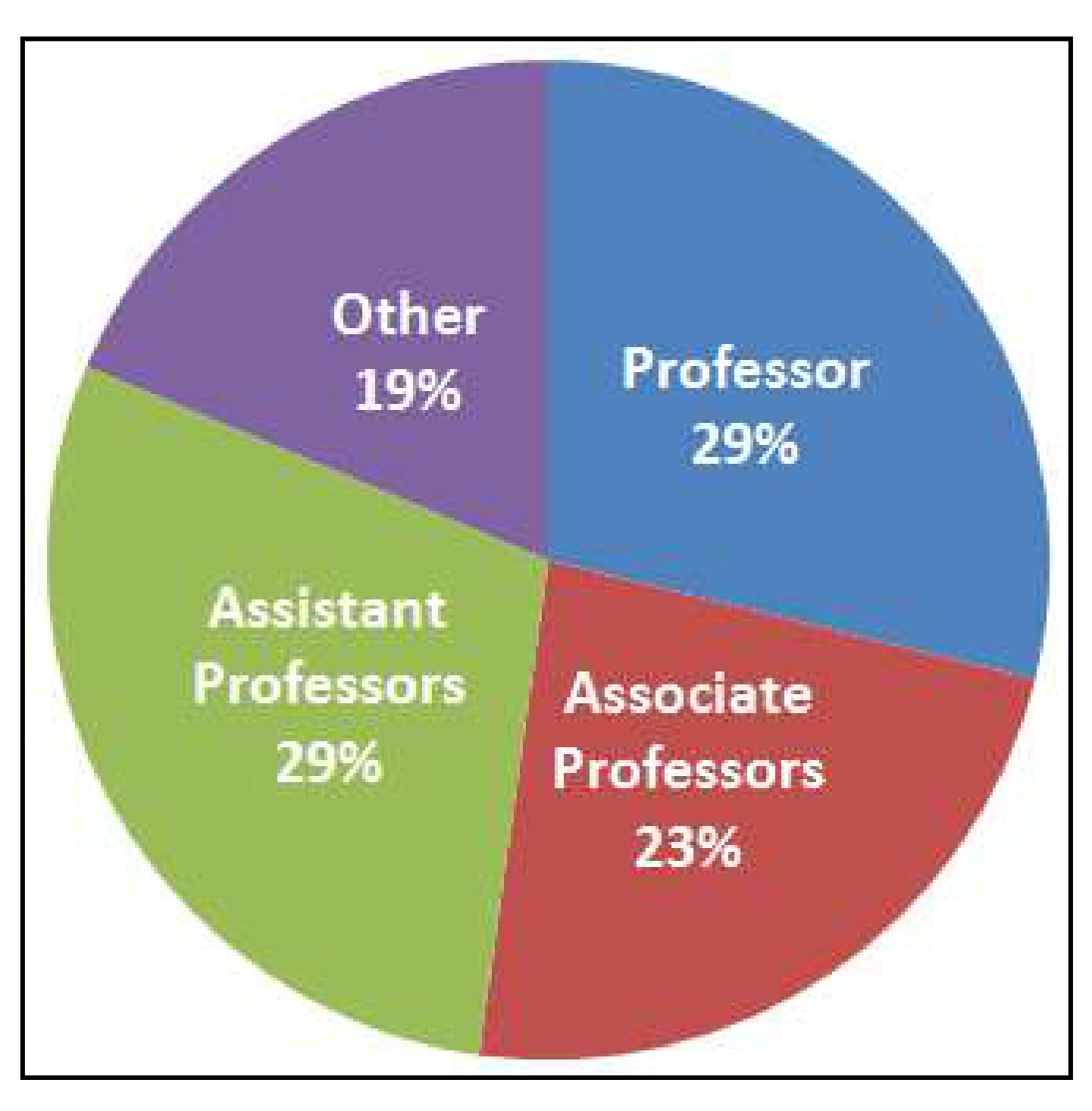
3.3. Registered Investigators in the Centralized RCMI Profiles Database
3.4. Sample of Research Domains of Early Stage Investigators
3.5. Use Case: RCMI Consortium Collaboration with the National Research Mentoring Network (NRMN)
3.6. RCMI-CC Realist Evaluation (RE) Logic Model
4. Discussion
Future Plans
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Institute of Medicine. Rising Above the Gathering Storm: Energizing and Employing America for a Brighter Economic Future; The National Academies Press: Washington, DC, USA, 2007. [Google Scholar]
- World Economic Forum. Available online: https://www.weforum.org›agenda›2019/04›businesscasefordiversityintheworkplaceisnowoverwhelming (accessed on 3 June 2021).
- Nielsen, M.W.; Alegria, S.; Börjeson, L.; Etzkowitz, H.; Falk-Krzesinski, H.J.; Joshi, A.; Leahey, E.; Smith-Doerr, L.; Woolley, A.W.; Schiebinger, L. Gender diversity leads to better science. Proc. Natl. Acad. Sci. USA 2017, 114, 1740–1742. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Valantine, H.A.; Collins, F.S. National Institutes of Health addresses the science of diversity. Proc. Natl. Acad. Sci. USA 2015, 112, 12240–12242. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- European Commission (European Commission Centre for Strategy and Evaluation Services). The Costs and Benefits of Diversity: A Study on Methods and Indicators to Measure the Cost Effectiveness of Diversity Policies in Enterprises. Executive Summary; Centre for Strategy and Evaluation Service: Kent, UK, 2003. [Google Scholar]
- Pew Research Center. “Women and Men in STEM Often at Odds over Workplace Equity.” Chapter 1: Diversity in the STEM Workforce Varies Widely Across Jobs. 2018. Available online: https://www.pewresearch.org›2018/01/09› (accessed on 2 March 2021).
- National Academies of Sciences, Engineering, and Medicine. Minority Serving Institutions: America’s Underutilized Resource for Strengthening the STEM Workforce; The National Academies Press: Washington, DC, USA, 2019. [Google Scholar] [CrossRef]
- Espinosa, L.L.; Turk, J.M.; Taylor, M. Pulling Back the Curtain: Enrollment and Outcomes at Minority Serving Institutions; American Council on Education: Washington, DC, USA, 2017. [Google Scholar]
- Marybeth, G.; Conrad, C.F. Minority Serving Institutions: Educating All Students; Penn Center: Philadelphia, PA, USA, 2013. [Google Scholar]
- Ofili, E.O.; Tchounwou, P.B.; Fernandez-Repollet, E.; Yanagihara, R.; Akintobi, T.H.; Lee, J.E.; Malouhi, M.; Garner, S.T.; Hayes, T.T.; Baker, A.R.; et al. The Research Centers in Minority Institutions (RCMI) Translational Research Network: Building and Sustaining Capacity for Multi-Site Basic Biomedical, Clinical and Behavioral Research. Ethn. Dis. 2019, 29, 135–144. [Google Scholar] [CrossRef] [PubMed]
- Ofili, E.O.; Tchounwou, P.B.; Fernandez-Repollet, E.; Yanagihara, R.; Akintobi, T.H.; Lee, J.E.; Malouhi, M.; Garner, S.T., Jr.; Hayes, T.T.; Baker, A.R.; et al. The Research Centers in Minority Institutions (RCMI) Program was Established in 1985 in Response to Committee Report Language (House Report 98-911) attached to H.R. 6028, the Departments of Labor, Health and Human Services, and Education and Related Agencies Appropriation Act. 1985. Ethn. Dis. 2019, 29, 135–144. [Google Scholar] [CrossRef]
- US Department of Health and Human Services; Office of the Secretary; Office of the Assistant Secretary for Planning and Evaluation and Office of Minority Health. HHS Action Plan to Reduce Racial and Ethnic Health Disparities Implementation Progress Report; Office of the Assistant Secretary for Planning and Evaluation: Washington, DC, USA, 2015.
- National Institutes of Health Minority Health and Health Disparities Strategic Plan 2021 to 2025: Taking the Next Steps. Available online: https://www.nimhd.nih.gov/docs/nimhd-strategic-plan-2021-2025.pdf (accessed on 3 June 2021).
- Jackson, C.S.; Gracia, J.N. Addressing Health and Health-Care Disparities: The Role of a Diverse Workforce and the Social Determinants of Health. Public Health Rep. 2014, 129, 57–61. [Google Scholar] [CrossRef] [Green Version]
- Working Group on Diversity in the Biomedical Research Workforce. Draft Report of the Advisory Committee to the Director Working Group on Diversity in the Biomedical Research Workforce. 13 June 2012. Last accessed 16 January 2019. Available online: https://acd.od.nih.gov/documents/reports/DiversityBiomedicalResearchWorkforceReport.pdf (accessed on 25 May 2021).
- Ginther, D.K.; Schaffer, W.T.; Schnell, J.; Masimore, B.; Liu, F.; Haak, L.L.; Kington, R. Race, Ethnicity, and NIH Research Awards. Science 2011, 333, 1015–1019. [Google Scholar] [CrossRef] [Green Version]
- Valantine HA and Wilson RM, Co-Chairs. NIH Scientific Workforce Diversity Actions and Progress: 2014–2019. Available online: https://acd.od.nih.gov/documents/presentations/06132019Diversity.pdf (accessed on 25 May 2021).
- Sorkness, C.A.; Pfund, C.; Ofili, E.O.; Okuyemi, K.S.; Vishwanatha, J.K.; Zavala, M.E.; Pesavento, T.; Fernandez, M.; Tissera, A.; Nrmn on behalf of the NRMN Team; et al. A new approach to mentoring for research careers: The National Research Mentoring Network. BMC Proc. 2017, 11, 171–182. [Google Scholar] [CrossRef] [Green Version]
- McCreath, H.E.; Norris, K.C.; Calderόn, N.E.; Purnell, D.L.; MacCalla, N.M.G.; Seeman, T.E. Evaluating efforts to diversify the biomedical workforce: The role and function of the Coordination and Evaluation Center of the Diversity Program Consortium. BMC Proc. 2017, 11, 27. [Google Scholar] [CrossRef] [Green Version]
- Hall, M.; Engler, J.; Hemming, J.; Alema-Mensah, E.; Baez, A.; Lawson, K.; Quarshie, A.; Stiles, J.; Pemu, P.; Thompson, W.; et al. Using a Virtual Community (the Health Equity Learning Collaboratory) to Support Early-Stage Investigators Pursuing Grant Funding. Int. J. Environ. Res. Public Health 2018, 15, 2408. [Google Scholar] [CrossRef] [Green Version]
- Weber-Main, A.M.; McGee, R.; Boman, K.E.; Hemming, J.; Hall, M.; Unold, T.; Harwood, E.M.; Risner, L.E.; Smith, A.; Lawson, K.; et al. Grant application outcomes for biomedical researchers who participated in the National Research Mentoring Network’s Grant Writing Coaching Programs. PLoS ONE 2020, 15, e0241851. [Google Scholar] [CrossRef]
- Webb Hooper, M.; Napoles, A.M.; Perez-Stable, E.J. COVID-19 and Racial/Ethnic Disparities. JAMA 2020, 323, 2466–2467. [Google Scholar] [CrossRef]
- National Science Foundation Report on Science and Engineering Degrees, by Race/Ethnicity of Recipients: 2002–2012. Available online: https://www.nsf.gov/statistics/degreerecipients/ (accessed on 25 May 2021).
- Estape, E.S.; Quarshie, A.; Segarra, B.; Martin, M.S.; Ríos, R.; Martínez, K.; Ali, J.; Nwagwu, U.; Ofili, E.; Pemu, P. Promoting Diversity in the Clinical and Translational Research Workforce. J. Natl. Med. Assoc. 2018, 110, 598–605. [Google Scholar] [CrossRef]
- Stephens, D.S.; West, A.C.; Ofili, E.O.; Boyan, B.D.; Blumberg, H.M. The Atlanta Clinical and Translational Science Institute. Clin. Transl. Sci. 2011, 4, 143–145. [Google Scholar] [CrossRef]
- Price, E.G.; Powe, N.R.; Kern, D.E.; Golden, S.H.; Wand, G.S.; Cooper, L.A. Improving the Diversity Climate in Academic Medicine: Faculty Perceptions as a Catalyst for Institutional Change. Acad. Med. 2009, 84, 95–105. [Google Scholar] [CrossRef] [Green Version]
- Pololi, L.H.; Krupat, E.; Civian, J.T.; Ash, A.S.; Brennan, R.T. Why Are a Quarter of Faculty Considering Leaving Academic Medicine? A Study of Their Perceptions of Institutional Culture and Intentions to Leave at 26 Representative U.S. Medical Schools. Acad. Med. 2012, 87, 859–869. [Google Scholar] [CrossRef]
- Pololi, L.H.; Civian, J.T.; Brennan, R.T.; Dottolo, A.L.; Krupat, E. Experiencing the Culture of Academic Medicine: Gender Matters, A National Study. J. Gen. Intern. Med. 2013, 28, 201–207. [Google Scholar] [CrossRef] [Green Version]
- Pololi, L.H.; Evans, A.T.; Gibbs, B.K.; Krupat, E.; Brennan, R.T.; Civian, J.T. The Experience of Minority Faculty Who Are Underrepresented in Medicine, at 26 Representative U.S. Medical Schools. Acad. Med. 2013, 88, 1308–1314. [Google Scholar] [CrossRef]
- Edwards, R.A.H.; Šúri, M.; Huld, T.A.; Dallemand, J.F. GIS-Based Assessment of Cereal Straw Energy Resource in the European Union. Available online: http://citeseerx.ist.psu.edu/viewdoc/download? (accessed on 10 February 2020).
- Policy and Global Affairs. Promising Practices for Addressing the Underrepresentation of Women in Science, Engineering, and Medicine; National Academies Press: Washington, DC, USA, 2020. [Google Scholar]
- Smith, S.U.; Hayes, S.; Shea, P. A Critical Review of the Use of Wenger’s Community of Practice (CoP) Theoretical Framework in Online and Blended Learning Research, 2000–2014. Online Learn. 2017, 21, 209–237. [Google Scholar] [CrossRef] [Green Version]
- Wenger, E. Communities of Practice: Learning, Meaning, and Identity; Cambridge University Press: Cambridge, UK, 1999. [Google Scholar]
- Pawson, R.; Tilley, N. An Introduction to Scientific Realist Evaluation. In Evaluation for the 21st Century: A Handbook; SAGE Publications Inc.: Merced, CA, USA, 2014; pp. 405–418. [Google Scholar]
- De Souza, D.E. Elaborating the Context-Mechanism-Outcome configuration (CMOc) in realist evaluation: A critical realist perspective. Evaluation 2013, 19, 141–154. [Google Scholar] [CrossRef]
- Dalkin, S.M.; Greenhalgh, J.; Jones, D.; Cunningham, B.; Lhussier, M. What’s in a mechanism? Development of a key concept in realist evaluation. Implement. Sci. 2015, 10, 1–7. [Google Scholar] [CrossRef] [Green Version]
- Rubio, D.M.; Mayowski, C.A.; Norman, M.K. A Multi-Pronged Approach to Diversifying the Workforce. Int. J. Environ. Res. Public Health 2018, 15, 2219. [Google Scholar] [CrossRef] [Green Version]
- Fleming, E.; Perkins, J.; Easa, D.; Conde, J.G.; Baker, R.S.; Southerland, W.M.; Dottin, R.; Benabe, J.E.; Ofili, E.O.; Bond, V.C.; et al. The role of translational research in addressing health disparities: A conceptual framework. Ethn. Dis. 2008, 18, S2–S155. [Google Scholar]
- Fleming, E.S.; Perkins, J.; Easa, D.; Conde, J.G.; Baker, R.S.; Southerland, W.M.; Dottin, R.; Benabe, J.E.; Ofili, E.O.; Bond, V.C.; et al. Addressing health disparities through multi-institutional, multidisciplinary collaboratories. Ethn. Dis. 2008, 18, S2–S161. [Google Scholar]
- Ofili, E.O.; Fair, A.; Norris, K.; Verbalis, J.G.; Poland, R.; Bernard, G.; Stephens, D.S.; Dubinett, S.M.; Imperato-McGinley, J.; Dottin, R.P.; et al. Models of Interinstitutional Partnerships between Research Intensive Universities and Minority Serving Institutions (MSI) across the Clinical Translational Science Award (CTSA) Consortium. Clin. Transl. Sci. 2013, 6, 435–443. [Google Scholar] [CrossRef]
- Salazar, M.R.; Lant, T.K.; Kane, A. To join or not to join: An investigation of individual facilitators and inhibitors of medical faculty participation in interdisciplinary research teams. Clin. Transl. Sci. 2011, 4, 274–278. [Google Scholar] [CrossRef] [Green Version]
- Salazar, M.R.; Lant, T.K.; Fiore, S.M.; Salas, E. Facilitating Innovation in Diverse Science Teams through Inte-Grative Capacity. Small Group Res. 2012, 43, 527–558. Available online: http://sgr.sagepub.com/content/43/5/527.full.pdf (accessed on 15 October 2014). [CrossRef]
- Salazar, M.; Lant, T.; Kane, A. Knowledge Workers and Interdisciplinary Team Structures for Knowledge Creation: Predicting Participation Choices. Clin. Transl. Sci. 2011, 4, 274–278. [Google Scholar]
- Salazar, M.; Doiron, K.; Widmer, K.; Lant, K. Leader Integrative Capabilities: A Catalyst for Effective Inter-Disciplinary Teams. In Strategies for Team Science Success; Springer: Cham, Switzerland, 2019. [Google Scholar]
- Gunawardena, C.; Hermans, M.B.; Sanchez, D.; Richmond, C.; Bohley, M.; Tuttle, R. A theoretical framework for building online communities of practice with social networking tools. EMI Educ. Media Int. 2009, 46, 3–16. [Google Scholar] [CrossRef] [Green Version]
- Stakeholder Template and Analysis. Available online: https://www.groupmap.com/map-templates/stakeholder-analysis/26 (accessed on 10 March 2021).
- King, G. An Introduction to the Dataverse Network as an Infrastructure for Data Sharing. Sociol. Methods Res. 2007, 36, 173–199. [Google Scholar] [CrossRef]
- Dalkey, N. The Delphi method: An experimental study of group opinion. Futures 1969, 1, 408–426. [Google Scholar] [CrossRef]
- NIH. All of Us Program. Available online: http://researchallofus.org (accessed on 10 March 2021).
- Cooksy, L.J.; Gill, P.; Kelly, P. The program logic model as an integrative framework for a multimethod evaluation. Eval. Program Plan. 2001, 24, 119–128. [Google Scholar] [CrossRef]
- W.K. Kellogg Foundation. Using Logic Models to Bring Together Planning, Evaluation, and Action: Logic Model Devel-opment Guide. 2004 [Cited 5 October 2016]. Available online: http://www.wkkf.org/resource-directory/resource/2006/02/wk-kellogg-foundationlogic-model-development-guide (accessed on 20 November 2020).
- Rubio, D.M. Common metrics to assess the efficiency of clinical research. Eval. Health Prof. 2013, 36, 432–446. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Rubio, D.M.; Blank, A.E.; Dozier, A.; Hites, L.; Gilliam, V.A.; Hunt, J.; Rainwater, J.; Trochim, W.M. Developing common metrics for the Clinical and Translational Science Awards (CTSAs): Lessons learned. Clin. Transl. Sci. 2015, 8, 451–459. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wilkinson, M.D.; Dumontier, M.; Aalbersberg, I.J.; Appleton, G.; Axton, M.; Baak, A.; Blomberg, N.; Boiten, J.-W.; da Silva Santos, L.B.; Bourne, P.E.; et al. The FAIR Guiding Principles for scientific data management and stewardship. Sci. Data 2016, 3, 160018. [Google Scholar] [CrossRef] [Green Version]
- Sweeney, L.; Crosas, M.; Bar-Sinai, M. Sharing Sensitive Data with Confidence: The Datatags System. Technol. Sci. 2015, 1–34. Available online: http://techscience.org/a/2015101601 (accessed on 25 May 2021).
- Bergeron, D.A.; Gaboury, I. Challenges related to the analytical process in realist evaluation and latest devel-opments on the use of NVivo from a realist perspective. Int. J. Soc. Res. Methodol. 2020, 23, 355–365. [Google Scholar] [CrossRef]
- Dalkin, S.; Forster, N.; Hodgson, P.; Lhussier, M.; Carr, S.M. Using computer assisted qualitative data analysis software (CAQDAS; NVivo) to assist in the complex process of realist theory generation, refinement and testing. Int. J. Soc. Res. Methodol. 2021, 24, 123–134. [Google Scholar] [CrossRef]
- A Randomized Controlled Study to Test the Effectiveness of Developmental Network Coaching in the Career Advancement of Diverse Early Stage Investigators. A National Research Menoring Network Intervention; Grant Number U01GM132771 (PI E. Ofili); National Institutes of General Medical Sciences (NIGMS). Available online: https://www.nigms.nih.gov/training/dpc/Pages/nrmn.aspx (accessed on 3 June 2021).
- Ending Structural Racism. Available online: https://www.nih.gov/ending-structural-racism/unite (accessed on 25 May 2021).
- Angus, D.; Rintel, S.; Wiles, J. Making sense of big text: A visual-first approach for analysing text data using Leximancer and Discursis. Int. J. Soc. Res. Methodol. 2013, 16, 261–267. [Google Scholar] [CrossRef]
| Charles R. Drew University, Los Angeles, CA. | Ponce Health Sciences University, Ponce, PR. |
| Clark Atlanta University, Atlanta, GA | San Diego State University, San Diego, CA. |
| Florida Agricultural & Mechanical University, Tallahassee, FL. | Texas Southern University, Houston, TX. |
| Florida International University, Miami, FL. | Tuskegee University, Tuskegee, AL. |
| Howard University, Washington, DC. | University of California, Riverside, Riverside, CA. |
| Jackson State University, Jackson, MS. | University of Hawaii at Manoa, Honolulu, HI. |
| Meharry Medical College, Nashville, TN. | University of Houston, Houston, TX, USA |
| Morehouse School of Medicine, Atlanta, GA. | University of Puerto Rico, Medical Sciences Campus, San Juan, PR. |
| Morgan State University, Baltimore, MD. | University of Texas at El Paso, El Paso, TX. |
| North Carolina Central University, Durham, NC. | Xavier University of Louisiana, New Orleans, LA. |
| Northern Arizona University, Flagstaff, AZ. |
| Registered Investigators and Collaborative Publications | Number of Records |
|---|---|
| Number of existing records | 1281 |
| Number of newly registered investigators (January–April 2021) | 974 |
| Number of updated records | 1240 |
| Number of affiliated with active RCMI institutions | 1959 |
| Number of inter-institutional unique publications (2000–2021) 560 Investigators and 2284 direct connections | 871 |
| Total Number of Active Investigators | 2252 |
| Institution Name | Publications | Institution Name | Publications |
|---|---|---|---|
| Charles R. Drew University (CDU) | 3256 | Ponce Health Sciences University (PHSU) | 678 |
| City College of New York (CCNY) * | 1961 | San Diego State University (SDSU) | 1221 |
| Clark Atlanta University (CAU) | 726 | Texas Southern University (TSU) | 798 |
| Florida A&M University (FAMU) | 1010 | Tuskegee University (TU) | 333 |
| Florida International University (FIU) | 1463 | Universidad Central Del Caribe (UCC) * | 877 |
| Howard University (HU) | 1938 | University of California Riverside (UCR) | 316 |
| Hunter College (HC) * | 2278 | University of Hawaii at Manoa (UHM) | 9668 |
| Jackson State University (JSU) | 1726 | University of Houston (UH) | 1162 |
| Meharry Medical College (MMC) | 2263 | University of Puerto Rico (UPR-MSC) | 3862 |
| Morehouse School of Medicine (MSM) | 2577 | University of Texas at El Paso (UTEP) | 1893 |
| Morgan State University (MSU) | 599 | University of Texas at San Antonio (UTSA) * | 4477 |
| North Carolina Central University (NCCU) | 550 | Xavier University of Louisiana (XULA) | 685 |
| Northern Arizona University (NAU) | 1098 | Total | 47,415 |
| Resources/Inputs | Scientific Activities | Scientific/DEI Outputs (Institution) | Outcomes | Community & Health Equity Impact |
|---|---|---|---|---|
| Financial Resources Financial Administration Pilot project funds | Funding Research Project Applications (new and continuing) Research Awards | Scientific Outputs New and renewing R01 New and renewing R01 equivalent New and renewing program awards Peer reviewed Publications Patent Disclosures | Individual Investigator Appointments and promotion Tenure track/equivalent Research awards Leadership Awards Mentoring awards Teaching Awards | Health Disparity Population Impact Practice Guidelines that impact health equity |
| Infrastructure Resources Research Space Research Infrastructure Mentoring/NRMN Training Career Development | Collaborations Multi-PI R01 Awards Multi-site Research Team based Publications | Community, Health Equity and Public Health Benefits Health promotion Population Health Public health impact | ||
| Human Resources Diverse faculty & Students URG/Women/LGBTQ Community partners Health system partners | Community Engagement Community partnered & Community led research Awards NIH & Industry Trials | DEI Outputs Doctoral degrees awarded to URG/Women/LGBTQ Training grants awarded to URG/Women/LGBTQ Health equity research awards Recruitment of URG participants | RCMI Center & Institution New Research Awards from NIMHD /NIH ICs Research Endowment | Economic Benefits Commercial products Financial savings (ROI) |
| Knowledge Resources Methodology Biological/Clinical materials and tools Information Services Health Technology | Innovation & Regulatory Research Ethics Research Compliance Incubator/SBIR Data Collection Data Analysis | RCMI Consortium & National Service on RCMI Steering Committee National Advisory Boards National Awards/Honors | Policy and Legislation with Health Equity Lens Advisory activities Policies and legislation | |
| External Environment Influence: Structural and Systemic Racism; Politics; Health Equity; HHS/NIH Policy | ||||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ofili, E.O.; Sarpong, D.; Yanagihara, R.; Tchounwou, P.B.; Fernández-Repollet, E.; Malouhi, M.; Idris, M.Y.; Lawson, K.; Spring, N.H.; Rivers, B.M. The Research Centers in Minority Institutions (RCMI) Consortium: A Blueprint for Inclusive Excellence. Int. J. Environ. Res. Public Health 2021, 18, 6848. https://doi.org/10.3390/ijerph18136848
Ofili EO, Sarpong D, Yanagihara R, Tchounwou PB, Fernández-Repollet E, Malouhi M, Idris MY, Lawson K, Spring NH, Rivers BM. The Research Centers in Minority Institutions (RCMI) Consortium: A Blueprint for Inclusive Excellence. International Journal of Environmental Research and Public Health. 2021; 18(13):6848. https://doi.org/10.3390/ijerph18136848
Chicago/Turabian StyleOfili, Elizabeth O., Daniel Sarpong, Richard Yanagihara, Paul B. Tchounwou, Emma Fernández-Repollet, Mohamad Malouhi, Muhammed Y. Idris, Kimberly Lawson, Nadine H. Spring, and Brian M. Rivers. 2021. "The Research Centers in Minority Institutions (RCMI) Consortium: A Blueprint for Inclusive Excellence" International Journal of Environmental Research and Public Health 18, no. 13: 6848. https://doi.org/10.3390/ijerph18136848
APA StyleOfili, E. O., Sarpong, D., Yanagihara, R., Tchounwou, P. B., Fernández-Repollet, E., Malouhi, M., Idris, M. Y., Lawson, K., Spring, N. H., & Rivers, B. M. (2021). The Research Centers in Minority Institutions (RCMI) Consortium: A Blueprint for Inclusive Excellence. International Journal of Environmental Research and Public Health, 18(13), 6848. https://doi.org/10.3390/ijerph18136848











