Singapore’s Pandemic Preparedness: An Overview of the First Wave of COVID-19
Abstract
1. Introduction
1.1. Country Profile
1.2. Health Care System
- Medisave—a national medical savings scheme where all workers are required to save between 6.5%–9% of their monthly wage in a special savings account. These funds can be used to pay for medical expenses including hospitalisation and some approved outpatient treatments for the worker or an immediate family member.
- MediShield—a catastrophic medical insurance scheme which covers large hospitalisation bills resulting from serious injury or prolonged illness. Premiums are deducted from Singaporeans Medisave accounts and the scheme operates on an opt-out basis where newborns are automatically covered from their parents account.
- Medifund—a financial safety net established by the government to assist people needing financial support to pay hospital and healthcare bills.
- ElderShield—a severe disability insurance scheme providing basic financial protection to those who need long term care, especially during old age. It operates on an opt-out basis with Singaporeans automatically covered when they reach 40 years of age, with premiums being paid from their Medisave accounts [36].
1.3. Non-Pharmaceutical Interventions
- Establishment of a network of Public Health Preparedness Clinics (PHPCs) which are primary health clinics established in times of national need
- Hospitalise and isolate the infected
- Trace contacts rigorously
- Make social messaging clear
1.4. Observed and Expected Economic Impact
1.5. Media Coverage
1.6. Social & Political Disruption
2. Materials and Methods
2.1. Epidemiology
2.2. Mathematical Modelling
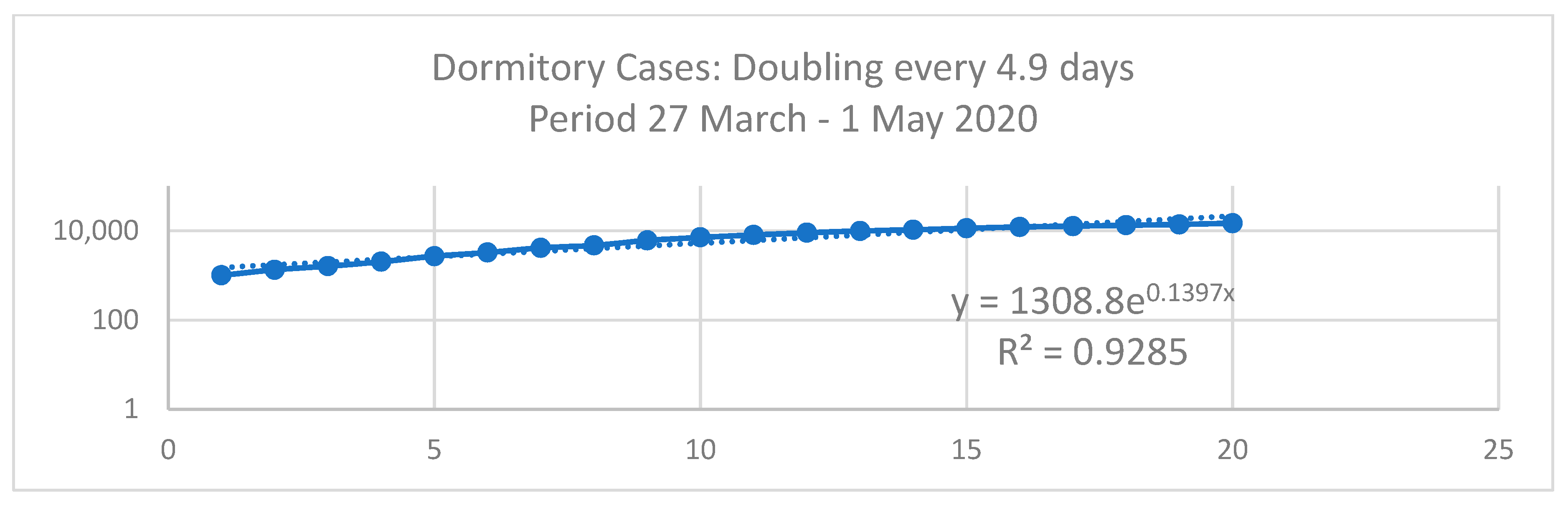
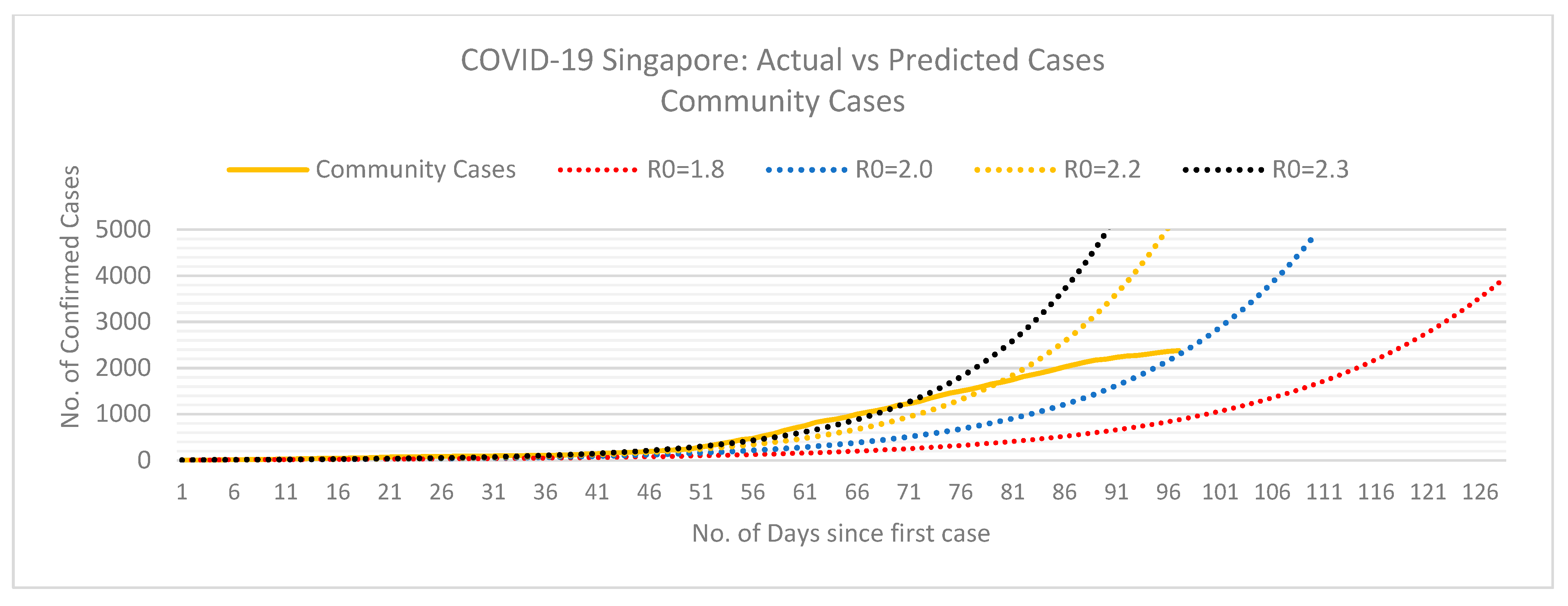
2.2.1. Doubling Time
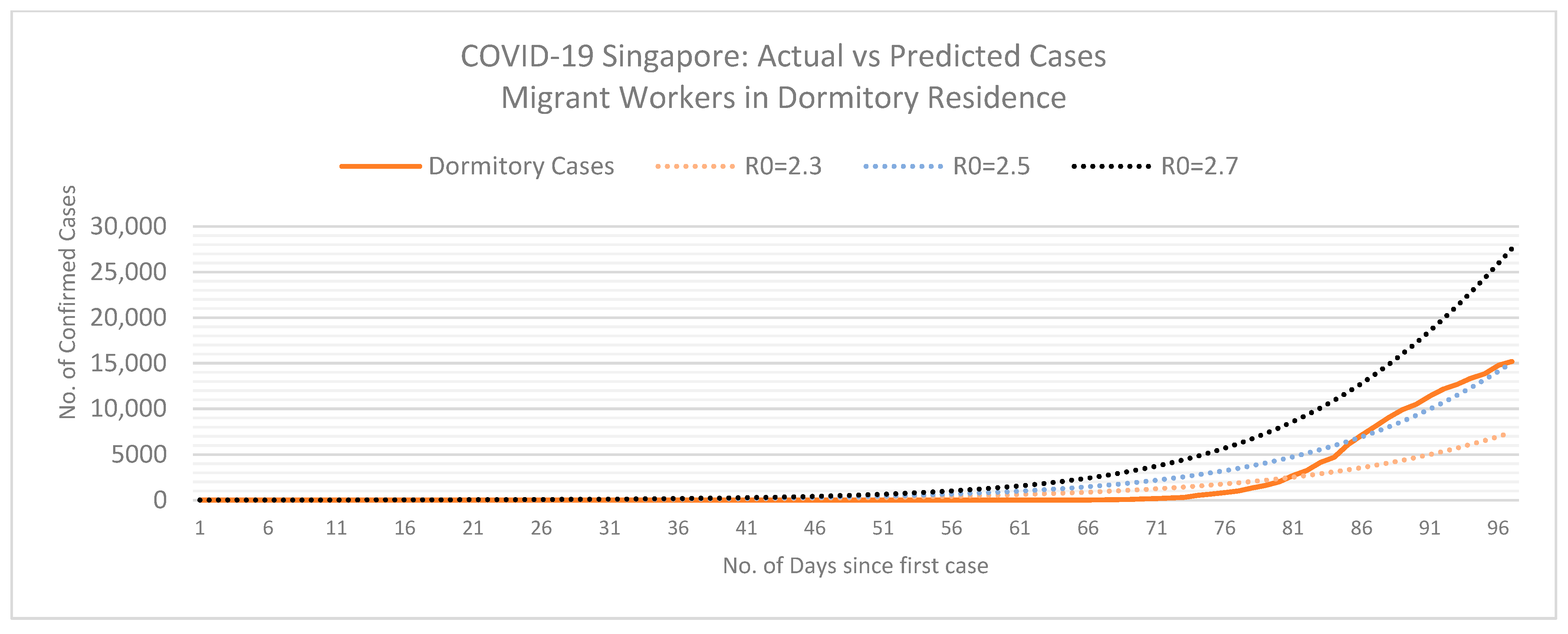
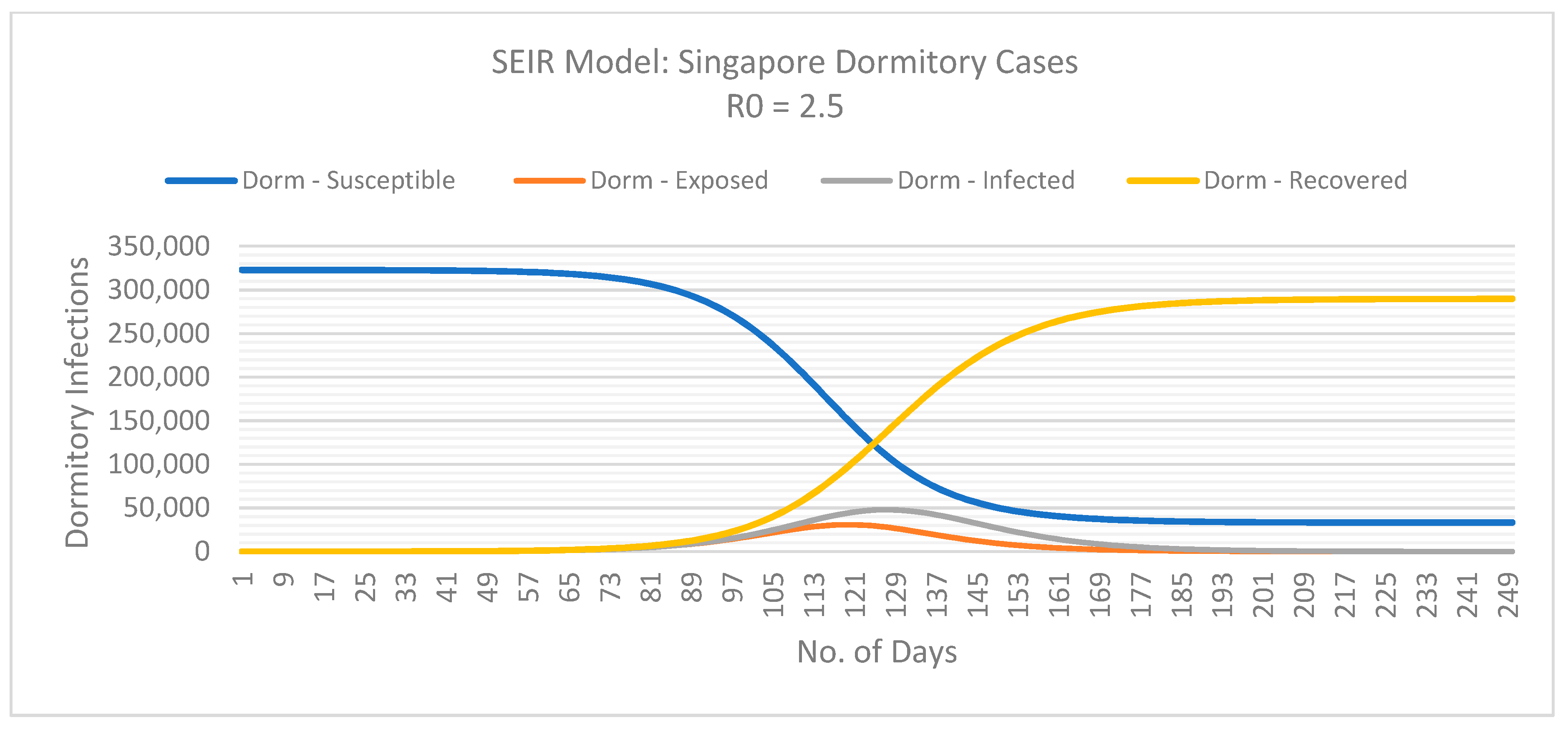
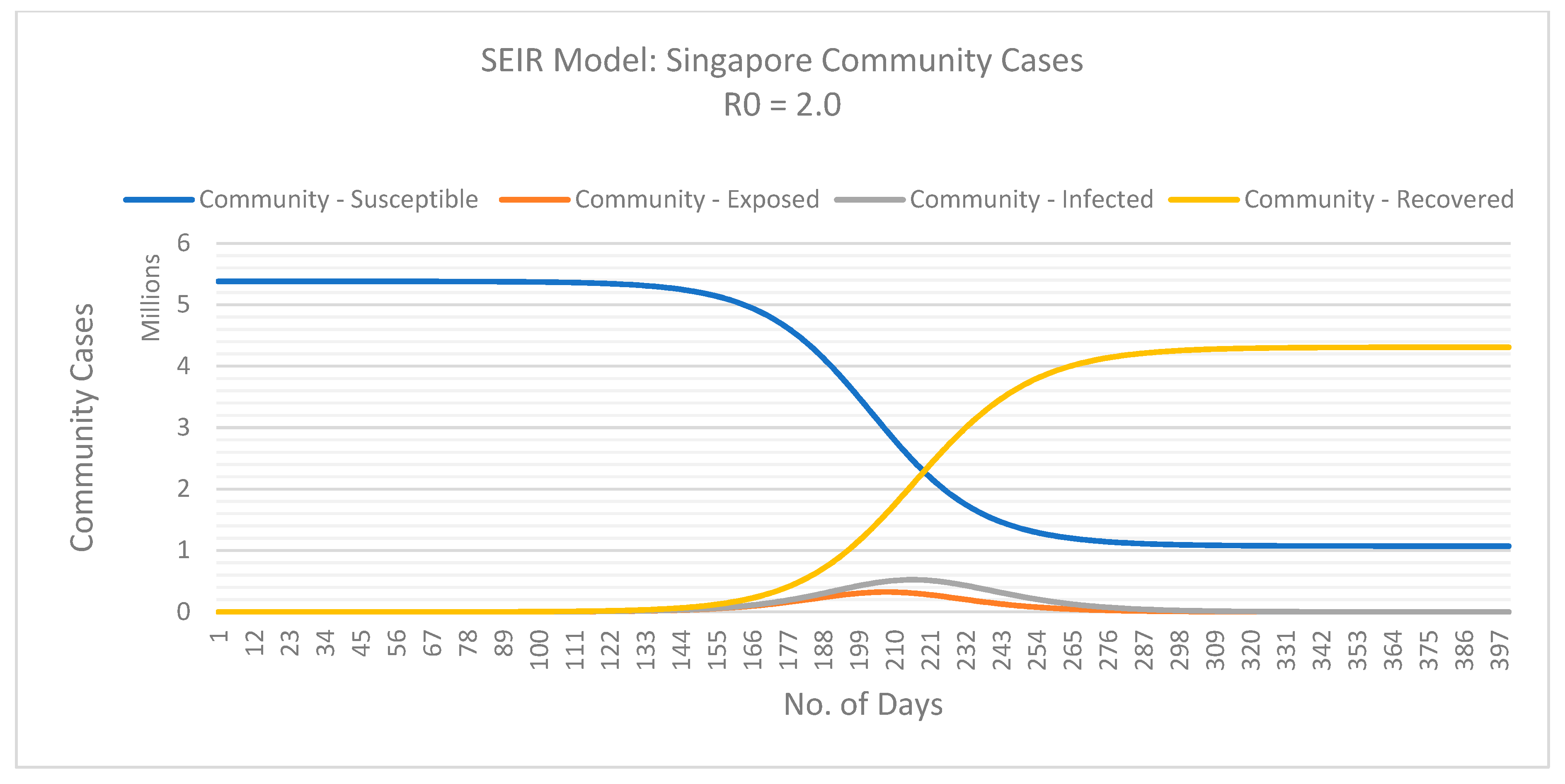
2.2.2. SEIR Model
- S = S(t); is the number of susceptible individuals at time t,
- E = E(t); is the number of exposed individuals at time t,
- I = I(t); is the number of infectious individuals at time t, and
- R = R(t); is the number of recovered/removed individuals at time t.
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Appendix A
References
- World Health Organization. Coronavirus Disease 2019 (COVID-19) Situation Report—82. Available online: https://www.who.int/docs/default-source/coronaviruse/situation-reports/20200411-sitrep-82-covid-19.pdf?sfvrsn=74a5d15_2 (accessed on 11 April 2020).
- Hsu, L.Y.; Tan, M.-H. What Singapore Can Teach the U.S. About Responding to Covid-19. Available online: https://www.statnews.com/2020/03/23/singapore-teach-united-states-about-covid-19-response/ (accessed on 12 April 2020).
- Chiew, C.J.; Li, Z.; Lee, V.J. Reducing onward spread of COVID-19 from imported cases: Quarantine and ‘stay at home’ measures for travellers and returning residents to Singapore. J. Travel Med. 2020. [Google Scholar] [CrossRef] [PubMed]
- Lee, V.J.; Chiew, C.J.; Khong, W.X. Interrupting transmission of COVID-19: Lessons from containment efforts in Singapore. J. Travel Med. 2020. [Google Scholar] [CrossRef] [PubMed]
- Ministry of Health Singapore. Additional Precautionary Measures to Prevent Further Importation and Spread of Covid-19 Cases 13th March 2020. Available online: https://www.moh.gov.sg/news-highlights/details/additional-precautionary-measures-to-prevent-further-importation-and-spread-of-covid-19-cases (accessed on 12 April 2020).
- John Hopkins University & Medicine. Coronavirus Resource Center. Available online: https://coronavirus.jhu.edu/map.html (accessed on 12 April 2020).
- The Institute for Disease Modelling. SEIR and SEIRS Models. Available online: https://idmod.org/docs/tuberculosis/model-seir.html (accessed on 12 April 2020).
- Moen, J. Singapore Geography. Available online: https://www.worldatlas.com/webimage/countrys/asia/singapore/sgland.htm (accessed on 8 April 2020).
- Trocki, C.A. Singapore: Wealth, Power and the Culture of Control; Routledge: London, UK, 2006. [Google Scholar]
- Economist Intelligence Unit. Singapore: Country Profile. Available online: https://country.eiu.com/singapore (accessed on 7 April 2020).
- Ho, R.; Kennard, A.; WInstead, R.O.; Leinbach, T.R. Singapore. Available online: https://www.britannica.com/place/Singapore (accessed on 5 April 2020).
- Department of Statistics Singapore. Population Trends 2019. Available online: https://www.singstat.gov.sg/-/media/files/publications/population/population2019.pdf (accessed on 8 April 2020).
- Parliament of Singapore. Constitution of the Republic of Singapore. Available online: https://sso.agc.gov.sg/Act/CONS1963 (accessed on 5 April 2020).
- Tupas, R. English-knowing bilingualism in Singapore: Economic pragmatism, ethnic relations and class. Engl. Lang. Educ. Across Greater China 2011, 46–69. [Google Scholar] [CrossRef]
- Schwab, K. The Global Competitiveness Report. 2019. Available online: http://www3.weforum.org/docs/WEF_TheGlobalCompetitivenessReport2019.pdf (accessed on 7 April 2020).
- Department of Statistics Singapore. Singapore Economy. Available online: https://www.singstat.gov.sg/modules/infographics/economy (accessed on 8 April 2020).
- World Shipping Council. Top 50 World Container Ports. Available online: http://www.worldshipping.org/about-the-industry/global-trade/top-50-world-container-ports/ (accessed on 6 April 2020).
- Department of Statistics Singapore. Tourism: Statistics on the Tourism Sector and Hotel Industry Are Compiled by the Singapore Tourism Board. Available online: https://www.singstat.gov.sg/find-data/search-by-theme/industry/tourism/latest-data (accessed on 8 April 2020).
- ATKearney. 2019 Global Cities Report. Available online: https://www.kearney.com/global-cities/2019 (accessed on 9 April 2020).
- Ministry of Manpower Singapore. Foreign Workforce Numbers. Available online: https://www.mom.gov.sg/documents-and-publications/foreign-workforce-numbers (accessed on 2 May 2020).
- Sadarangani, S.P.; Lim, P.L.; Vasoo, S. Infectious diseases and migrant worker health in Singapore: A receiving country’s perspective. J. Travel Med. 2017, 24. [Google Scholar] [CrossRef] [PubMed]
- Teo, J. Should Standards in Foreign Worker Dormitories be Raised? Available online: https://www.facebook.com/123724534368517/posts/3665600290180906/?d=n (accessed on 3 May 2020).
- Leung, H. Singapore Was a Coronavirus Success Story—Until an Outbreak Showed How Vulnerable Workers Can Fall Through the Cracks. Available online: https://time.com/5825261/singapore-coronavirus-migrant-workers-inequality/ (accessed on 3 May 2020).
- Ministry of Manpower Singapore. Sick Leave Eligibility and Entitlement. Available online: https://www.mom.gov.sg/employment-practices/leave/sick-leave/eligibility-and-entitlement (accessed on 15 April 2020).
- Ministry of Manpower Singapore. Employment Act: Who it Covers. Available online: https://www.mom.gov.sg/employment-practices/employment-act/who-is-covered (accessed on 15 April 2020).
- Quazi, H. Nature and Extent of Presenteeism in Singapore. In Presenteeism: The Invisible Cost to Organizations; Quazi, H., Ed.; Palgrave Macmillan: London, UK, 2013; pp. 61–87. [Google Scholar] [CrossRef]
- Bhaskaran, M. Challenges facing the Singapore Economy. Southeast Asian Aff. 2014, 290–302. [Google Scholar]
- Hofstede, G.; Hofstede, G.J.; Minkov, M. Cultures and Organizations: Software of the Mind: Intercultural Cooperation and its Importance for Survival, 3rd ed.; McGraw-Hill: New York, NY, USA, 2010. [Google Scholar]
- Epidemiology & Disease Control Division Ministry of Health Singapore; Institute for Health Metrics and Evaluation. The Burden of Disease in Singapore, 1990–2017. Available online: https://www.moh.gov.sg/docs/librariesprovider5/default-document-library/gbd_2017_singapore_reportce6bb0b3ad1a49c19ee6ebadc1273b18.pdf (accessed on 8 April 2020).
- Wong, C.; Lee, H. Healthcare in Singapore: Challenges and management. Int. Med. Commun. 2008, 51, 343–346. [Google Scholar]
- Ministry of Health Singapore. Health Manpower. Available online: https://www.moh.gov.sg/resources-statistics/singapore-health-facts/health-manpower (accessed on 7 April 2020).
- Department of Statistics Singapore. Health: Statistics on Health and on the Healthcare Sector are Compiled by the Ministry of Health. Available online: https://www.singstat.gov.sg/find-data/search-by-theme/society/health/latest-data (accessed on 8 April 2020).
- OECD. Health at a Glance: Asia/Pacific 2018; OECD Publications Centre: Paris, France, 2018. [Google Scholar]
- The World Bank. Current Health Expenditure (% of GDP). Available online: https://data.worldbank.org/indicator/SH.XPD.CHEX.GD.ZS (accessed on 10 April 2020).
- AusHSI. Market Failure and Information Problems in Healthcare. Available online: https://www.aushsi.org.au/market-failure-and-information-problems-in-healthcare/ (accessed on 9 April 2020).
- Ministry of Health Singapore. Singapore’s Healthcare Financing System. Available online: https://www.moh.gov.sg/docs/librariesprovider5/resources-statistics/educational-resources/3menglish_final.pdf (accessed on 7 April 2020).
- Flahault, A. Personal Communication—Draft Framework for Rating Health System Performance and Sustainability. Draft conceptual framework description ed.; 2020; in press. [Google Scholar]
- Communicable Diseases Division Ministry of Health Singapore. Communicable Diseases Surveillance in Singapore 2017. Available online: https://www.moh.gov.sg/resources-statistics/reports/communicable-diseases-surveillance-in-singapore-2017 (accessed on 7 April 2020).
- Keogh-Brown, M.R.; Smith, R.D. The economic impact of SARS: How does the reality match the predictions? Health Policy 2008, 88, 110–120. [Google Scholar] [CrossRef] [PubMed]
- Ministry of Health Singapore. MOH Pandemic Readiness and Response Plan for Influenza and Other Acute Respiratory Diseases (Revised April 2014). Available online: https://www.moh.gov.sg/docs/librariesprovider5/diseases-updates/interim-pandemic-plan-public-ver-_april-2014.pdf (accessed on 6 April 2020).
- Civil Service College Singapore. Singapore’s Whole-of-Government Approach in Crisis Management. Available online: https://www.csc.gov.sg/articles/singapore’s-whole-of-government-approach-in-crisis-management (accessed on 10 April 2020).
- Lum, L.H.; Badaruddin, H.; Salmon, S.; Cutter, J.; Lim, A.Y.; Fisher, D. Pandemic Preparedness: Nationally-Led Simulation to Test Hospital Systems. Ann. Acad. Med. Singap. 2016. [Google Scholar] [CrossRef]
- National Centre for Infectious Diseases. About NCID. Available online: https://www.ncid.sg/About-NCID/Pages/default.aspx (accessed on 8 April 2020).
- World Health Organization. Pneumonia of Unknown Cause—China. Available online: https://www.who.int/csr/don/05-january-2020-pneumonia-of-unkown-cause-china/en/ (accessed on 6 April 2020).
- Ministry of Health Singapore. Past Updates on COVID-19 Local Situation. Available online: https://www.moh.gov.sg/covid-19/past-updates (accessed on 7 April 2020).
- Ministry of Trade and Industry Singapore. Singapore’s GDP Contracted by 2.2 Per Cent in the First Quarter of 2020. MTI Downgrades 2020 GDP Growth Forecast to “−4.0 to −1.0 Per Cent”. Available online: https://www.mti.gov.sg/-/media/MTI/Newsroom/Press-Releases/2020/03/AdvEst_1Q20.pdf (accessed on 12 April 2020).
- Geddie, J.; Aravindan, A. Trade Bellwether Singapore Signals Deep Recession for World as Virus Batters Economy. Available online: https://www.reuters.com/article/us-singapore-economy-gdp/trade-bellwether-singapore-signals-deep-recession-for-world-as-virus-batters-economy-idUSKBN21D02L (accessed on 13 April 2020).
- Singapore Tourism Board. STB Rallies Tourism Sector to Face Biggest Challenge Since SARS. Available online: https://www.stb.gov.sg/content/stb/en/media-centre/media-releases/stb-rallies-tourismsectortofacebiggestchallengesincesars.html (accessed on 13 April 2020).
- International Monetary Fund. Policy Responses to COVID-19. Available online: https://www.imf.org/en/Topics/imf-and-covid19/Policy-Responses-to-COVID-19#S (accessed on 12 April 2020).
- Government of Singapore. Solidarity Budget Booklet English. Available online: https://www.singaporebudget.gov.sg/budget_2020/solidarity-budget/solidarity-budget-measures/solidarity-budget-booklet-eng (accessed on 13 April 2020).
- Government of Singapore. Government to Continue Support Measures to Protect Livelihoods and Stabilise Businesses During Extended Circuit Breaker Period. Available online: https://www.singaporebudget.gov.sg/budget_2020/about-budget/budget-media-releases/government-to-continue-support-measures-to-protect-livelihoods-and-stabilise-businesses-during-extended-circuit-breaker-period (accessed on 3 May 2020).
- Gourinchas, P.-O. Flattening the Pandemic and Recession Curves. Available online: https://clausen.berkeley.edu/flattening-the-pandemic-and-recession-curves/ (accessed on 12 April 2020).
- Depoux, A.; Martin, S.; Karafillakis, E.; Preet, R.; Wilder-Smith, A.; Larson, H. The pandemic of social media panic travels faster than the COVID-19 outbreak. J. Travel Med. 2020. [Google Scholar] [CrossRef] [PubMed]
- Ministry of Health Singapore. Updates on COVID-19 (Coronavirus disease 2019) Local Situation. Available online: https://www.moh.gov.sg/covid-19 (accessed on 3 April 2020).
- Government of Singapore. Gov.sg on WhatsApp: How to Sign up. Available online: https://www.gov.sg/article/govsg-on-whatsapp (accessed on 3 April 2020).
- Prime Minister’s Office Singapore. Newsroom. Available online: https://www.pmo.gov.sg/Newsroom (accessed on 3 April 2020).
- Teo, J. Coronavirus: WHO Praises Singapore’s Containment of Covid-19 Outbreak. Available online: https://www.straitstimes.com/singapore/health/coronavirus-who-praises-singapores-containment-of-covid-19-outbreak (accessed on 3 April 2020).
- Prime Minister’s Office Singapore. PM Lee Hsien Loong’s Interview with CNN. Available online: https://www.pmo.gov.sg/Newsroom/PM-interview-with-CNN (accessed on 6 April 2020).
- Immigration & Checkpoints Authority Singapore. Singapore Permanent Resident Breached Stay-Home Notice Requirements; Loses Singapore Permanent Residence Status and Will Be Barred from Re-Entering Singapore. Available online: https://www.ica.gov.sg/news-and-publications/media-releases/media-release/singapore-permanent-resident-breached-stay-home-notice-requirements-loses-singapore-permanent-residence-status-and-will-be-barred-from-re-entering-singapore (accessed on 3 April 2020).
- Amnesty International. Singapore: Over 20,000 Migrant Workers in Quarantine Must be Protected from Mass Infection. Available online: https://www.amnesty.org/en/latest/news/2020/04/singapore-migrant-workers-quarantine-protected-mass-infection/ (accessed on 10 April 2020).
- Teo, J. Delivered Remarks by Manpower Minister Josephine Teo at MTF Press Conference on 1 May 2020. Available online: https://www.sgpc.gov.sg/sgpcmedia/media_releases/mom/press_release/P-20200501-2/attachment/Delivered%20Remarks%20by%20Manpower%20Minister%20Josephine%20Teo%20at%20MTF%20press%20conference%20on%201%20May%202020.pdf (accessed on 3 May 2020).
- Government of Singapore. COVID-19: There’s no Need to Rush to Buy Essential Items. Available online: https://www.gov.sg/article/covid-19-theres-no-need-to-rush-to-buy-essential-items (accessed on 11 April 2020).
- Ministry of Trade and Industry Singapore. Issuance of Letters by the Price Controller to Sellers that have Received Consumer Complaints. Available online: https://www.mti.gov.sg/-/media/MTI/Newsroom/COVID-19/v2/30-Jan-Pricecontroller.pdf (accessed on 11 April 2020).
- Zhuo, T. Leak of closed-door Chan Chun Sing meeting ‘deeply disappointing’ and a ‘betrayal’, says Singapore Chinese Chamber president. Available online: https://str.sg/JG6F (accessed on 11 April 2020).
- Ministry of Health Singapore. Clarifications on Misinformation Regarding COVID-19. Available online: https://www.moh.gov.sg/covid-19/clarifications (accessed on 11 April 2020).
- Ho, C.S.; Chee, C.Y.; Ho, R.C. Mental Health Strategies to Combat the Psychological Impact of COVID-19 Beyond Paranoia and Panic. Ann. Acad. Med. Singap. 2020, 49, 155–160. [Google Scholar] [CrossRef] [PubMed]
- Government of Singapore. PM Lee: The COVID-19 Situation in Singapore (8 February 2020). Available online: https://www.gov.sg/article/pm-lee-hsien-loong-on-the-covid-19-situation-in-singapore (accessed on 11 April 2020).
- Ministry of Health Singapore. COVID-19 Situation Report Archive. Available online: https://www.moh.gov.sg/covid-19/situation-report (accessed on 1 May 2020).
- World Health Organization. Coronavirus disease (COVID-19) Weekly Epidemiological Update and Weekly Operational Update. Available online: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/situation-reports (accessed on 29 December 2020).
- European Centre for Disease Prevention and Control. COVID-19. Available online: https://qap.ecdc.europa.eu/public/extensions/COVID-19/COVID-19.html (accessed on 14 November 2020).
- Ministry of Foreign Affairs Singapore. Latest Update on Coronavirus (COVID-19) Situation- 19 March 2020. Available online: https://www.mfa.gov.sg/Overseas-Mission/Seoul/Announcements/Latest-Update-on-Coronavirus-Situation--19-March-2020 (accessed on 12 April 2020).
- Sasaki, K. COVID-19 Dynamics with SIR Model. Available online: https://www.lewuathe.com/covid-19-dynamics-with-sir-model.html (accessed on 12 April 2020).
- Riou, J.; Althaus, C.L. Pattern of early human-to-human transmission of Wuhan 2019 novel coronavirus (2019-nCoV), December 2019 to January 2020. Eurosurveillance 2020, 25. [Google Scholar] [CrossRef] [PubMed]
- Lauer, S.A.; Grantz, K.H.; Bi, Q.; Jones, F.K.; Zheng, Q.; Meredith, H.; Azman, A.S.; Reich, N.G.; Lessler, J. The incubation period of 2019-nCoV from publicly reported confirmed cases: Estimation and application. medRxiv 2020. [Google Scholar] [CrossRef]
- Pung, R.; Chiew, C.J.; Young, B.E.; Chin, S.; Chen, M.I.C.; Clapham, H.E.; Cook, A.R.; Maurer-Stroh, S.; Toh, M.P.H.S.; Poh, C.; et al. Investigation of three clusters of COVID-19 in Singapore: Implications for surveillance and response measures. Lancet 2020, 395, 1039–1046. [Google Scholar] [CrossRef]
- Hamzah, F.B.; Lau, C.; Nazri, H.; Ligot, D.V.; Lee, G.; Tan, C.L. CoronaTracker: Worldwide COVID-19 Outbreak Data Analysis and Prediction. Bull. World Health Organ. 2020. [Google Scholar] [CrossRef]
- World Health Organization. Report of the WHO-China Joint Mission on Coronavirus Disease 2019 (COVID-19). Available online: https://www.who.int/docs/default-source/coronaviruse/who-china-joint-mission-on-covid-19-final-report.pdf (accessed on 12 April 2020).
- Wilasang, C.; Sararat, C.; Jitsuk, N.C.; Yolai, N.; Thammawijaya, P.; Auewarakul, P.; Modchang, C. Reduction in effective reproduction number of COVID-19 is higher in countries employing active case detection with prompt isolation. J. Travel Med. 2020, 27. [Google Scholar] [CrossRef] [PubMed]
- Wilder-Smith, A.; Bar-Yam, Y.; Fisher, D. Lockdown to contain COVID-19 is a window of opportunity to prevent the second wave. J. Travel Med. 2020, 27. [Google Scholar] [CrossRef] [PubMed]
- Chen, S.; Chen, Q.; Yang, J.; Lin, L.; Li, L.; Jiao, L.; Geldsetzer, P.; Wang, C.; Wilder-Smith, A.; Bärnighausen, T. Positive impact of facility-based isolation of mild COVID-19 cases on effectively curbing the pandemic: A mathematical modelling study. J. Travel Med. 2020. [Google Scholar] [CrossRef] [PubMed]
- Yi, H.; Ng, S.T.; Farwin, A.; Pei Ting Low, A.; Chang, C.M.; Lim, J. Health equity considerations in COVID-19: Geospatial network analysis of the COVID-19 outbreak in the migrant population in Singapore. J. Travel Med. 2020. [Google Scholar] [CrossRef] [PubMed]
- Singapore Ministry of Manpower. Advisories on COVID-19. Available online: https://www.mom.gov.sg/covid-19 (accessed on 4 May 2020).
- Cook, M.J.; Dri, G.G.; Logan, P.; Tan, J.B.; Flahault, A. COVID-19 Down Under: Australia’s Initial Pandemic Experience. Int. J. Environ. Res. Public Health 2020, 17, 8939. [Google Scholar] [CrossRef]
- Chu, I.Y.-H.; Alam, P.; Larson, H.J.; Lin, L. Social consequences of mass quarantine during epidemics: A systematic review with implications for the COVID-19 response. J. Travel Med. 2020, 27. [Google Scholar] [CrossRef] [PubMed]
| Date of Implementation | Measure(s) |
|---|---|
| 2-Jan | Singapore MOH issues health advisory and temperature checks at Changi Airport from Wuhan arrivals initiated |
| 20-Jan | Temperature screening at Changi Airport was extended to all travellers coming from China. The public advised to adopt good personal hygiene measures and seek medical attention promptly if they are unwell. |
| 23-Jan | First confirmed local case, border control measures enhanced and extended to land and sea checkpoints. First meeting of whole-of-government response taskforce |
| 25-Jan | MOH imposed a visitor limit of two per patient in hospitals to slow the spread of the virus. Some hospitals have discouraged children from visiting. |
| 31-Jan | New visitors with travel history in mainland China or with PRC passports are not allowed entry |
| 1-Feb | Surgical masks issued to each household to alleviate shortages and price gouging. Only people who are unwell should wear masks. Safe distancing measures progressively implemented. |
| 3-Feb | Precautionary Measures advised in Preschools including travel declarations, temperature screening and health checks |
| 7-Feb | Risk assessment raised to DORSCON Orange
|
| 14-Feb | PHPC system is in place, establishing 900 GP clinics specially designated to manage people suffering from respiratory illness |
| 17-Feb | Implementation of 14 day stay-home notices for all travellers returning from mainland China |
| 25-Feb | Travel restrictions implemented for visitors from some areas of the Republic of Korea |
| 3-Mar | Travel restrictions implemented for visitors from Iran, Northern Italy, Japan and the Republic of Korea |
| 13-Mar | Travel restrictions implemented for visitors from Italy, France, Spain and Germany, as well as additional social distancing measures within Singapore. |
| 17-Mar | Singaporean students studying overseas advised to return home |
| 18-Mar | Singaporeans advised to defer all travel abroad. All inbound visitors must remain in their place of residence for 14 days |
| 21-Mar | Government Technology Agency launches the TraceTogether application which can use Bluetooth technology to track close contacts, enabling wide scale contact tracing |
| 23-Mar | Travel restrictions all short-term visitors are not allowed to enter or transit through Singapore. Returning Citizens and residents are issued 14 day stay at home notices |
| 24-Mar | Tighter measures to minimise further spread of COVID-19 implemented including closing all bars and entertainment venues. Schools and retail malls remain open. |
| 26-Mar | All gatherings outside of school and work limited to 10 or fewer until 30/4 |
| 27-Mar | Ministry of Education announces 1 day of Home-Based Learning (HBL) |
| 7-Apr | ‘Circuit Breaker’ measures implemented 7 April to 4 May
|
| 18-Apr | 180,000 foreign workers in the construction industry issued stay-home notices |
| 21-Apr | ‘Circuit Breaker’ measures extended for 4 weeks through to 1 June 2020 |
| 1-May | An inter-agency taskforce of 3000 officers from six public agencies including the Ministries of Manpower and Health, and the Singapore Armed Forces is established. This taskforce will:
|
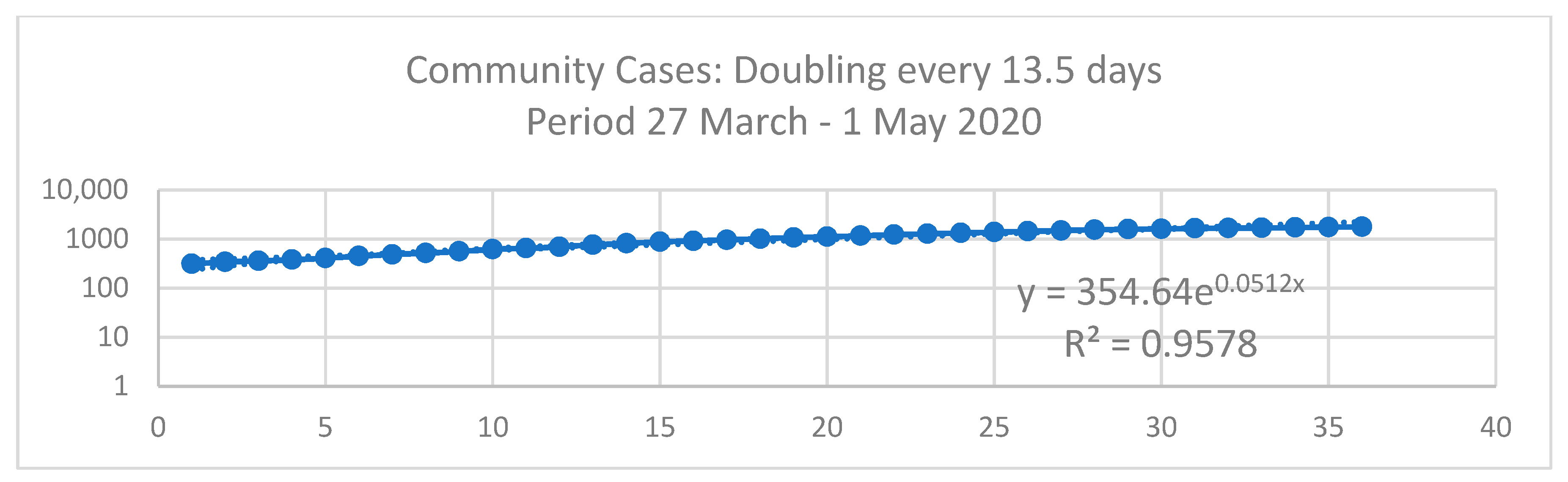
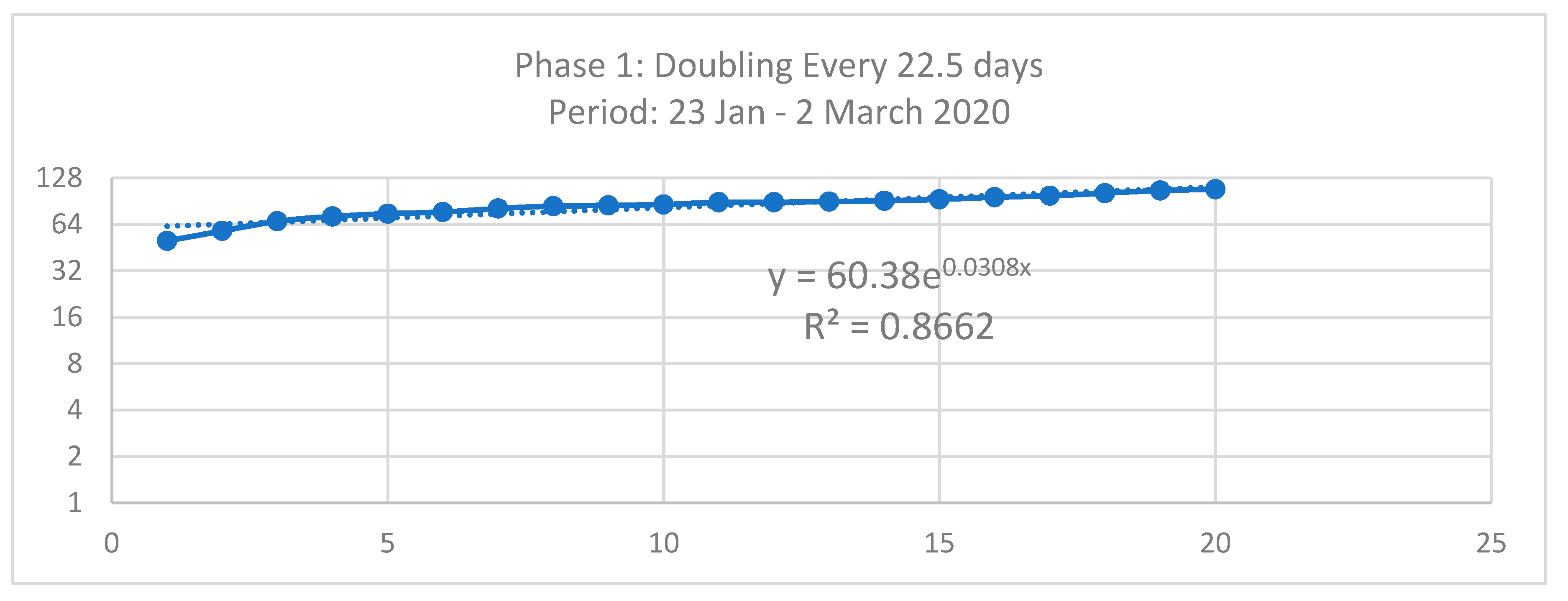
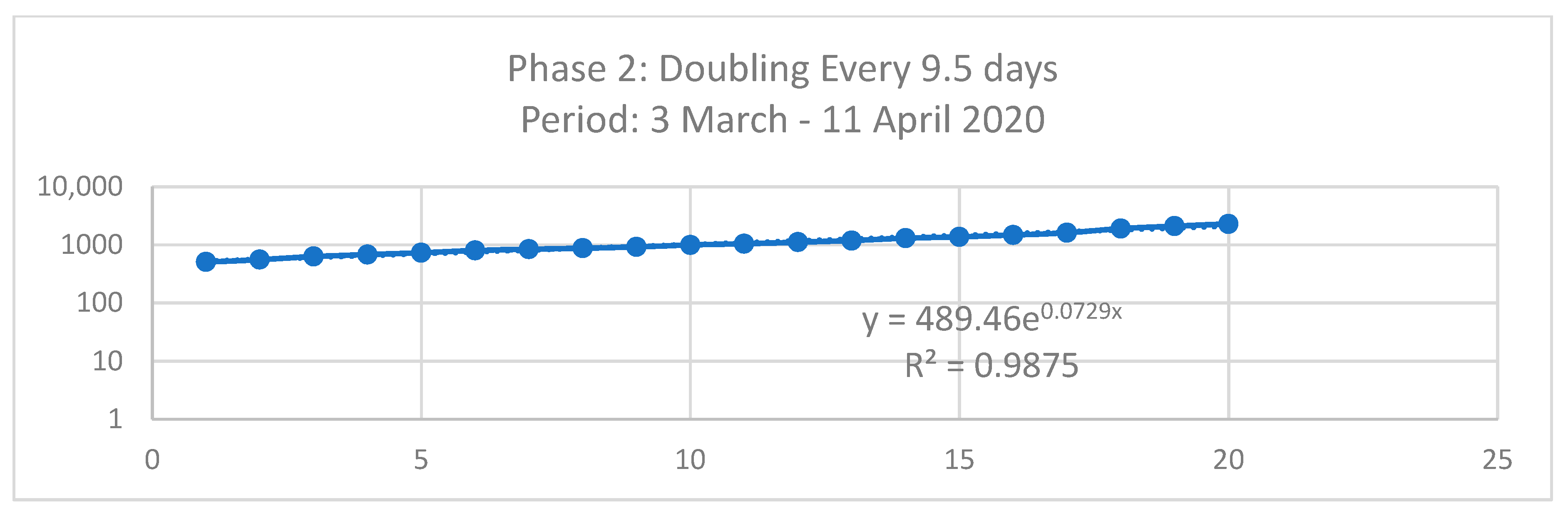
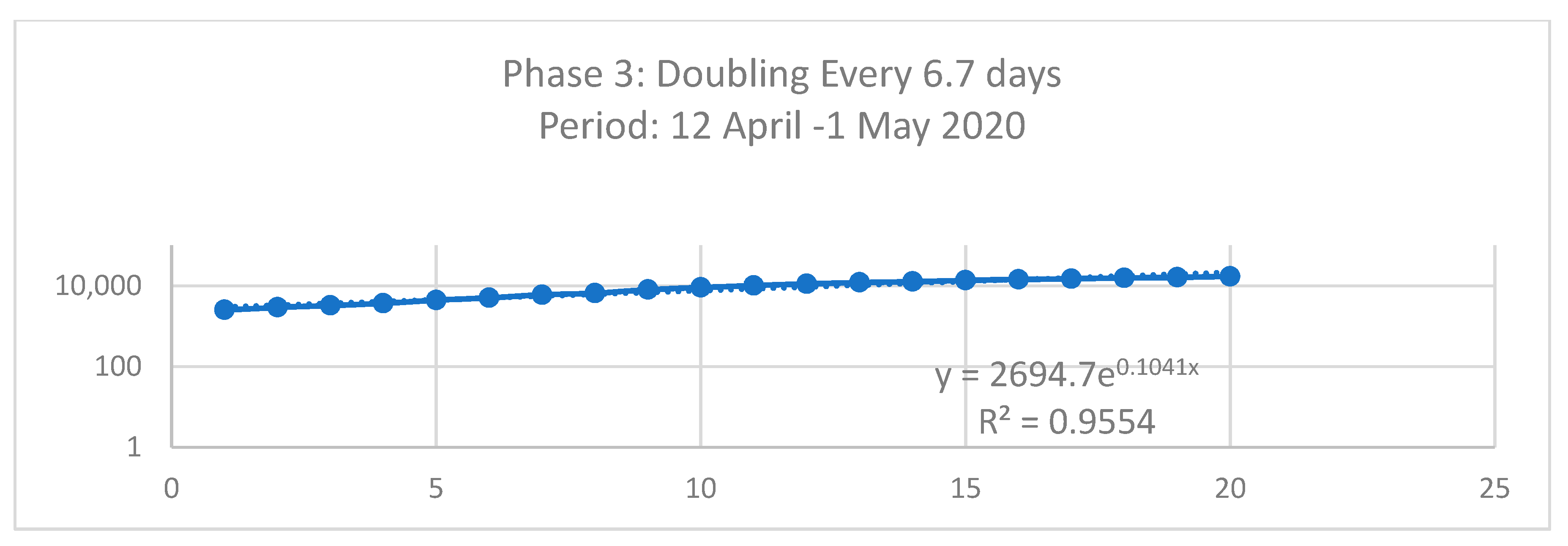
| y = AeBx | Phase 1 | Phase 2 | Phase 3 | Dormitory | Community |
|---|---|---|---|---|---|
| Doubling Time (Td) = Ln(2)/B | 0.0308 | 0.0729 | 0.1041 | 0.1397 | 0.0512 |
| 22.5 Days | 9.5 Days | 6.7 Days | 4.9 Days | 13.5 Days |
| Equations | Values | Definitions |
|---|---|---|
| R0 = ß/ƴ | S = Susceptible; initial | |
| β: rate of spread; β = R0*γ | E = Exposed; initial | |
| Y: duration of incubation | 5.2 days | I = Infected; initial |
| σ = 1/Y; rate of latent (exposed)individuals becoming infectious | 0.192 | R = Recovered; initial |
| D: average duration of recovery = total duration incubation period | 8.8 | ß = Rate of spread of infection |
| γ: Recovery rate; γ = 1/D | 0.113 | σ = Incubation rate |
| Sn = Sn − 1 ((Sn − 1/S) * (ß*In − 1)) | ƴ = Recovery rate | |
| En = En − 1 + (Sn − 1/S) * (ß*In − 1) (En − 1*σ) | T = time interval; usually days | |
| In = In − 1 + (En − 1*σ) (In − 1*ƴ) | n = number of people on day n | |
| Rn = Rn − 1 + (In − 1 * ƴ) | N = total number of people = S + E + I + R |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tan, J.B.; Cook, M.J.; Logan, P.; Rozanova, L.; Wilder-Smith, A. Singapore’s Pandemic Preparedness: An Overview of the First Wave of COVID-19. Int. J. Environ. Res. Public Health 2021, 18, 252. https://doi.org/10.3390/ijerph18010252
Tan JB, Cook MJ, Logan P, Rozanova L, Wilder-Smith A. Singapore’s Pandemic Preparedness: An Overview of the First Wave of COVID-19. International Journal of Environmental Research and Public Health. 2021; 18(1):252. https://doi.org/10.3390/ijerph18010252
Chicago/Turabian StyleTan, Jia Bin, Matthew James Cook, Prishanee Logan, Liudmila Rozanova, and Annelies Wilder-Smith. 2021. "Singapore’s Pandemic Preparedness: An Overview of the First Wave of COVID-19" International Journal of Environmental Research and Public Health 18, no. 1: 252. https://doi.org/10.3390/ijerph18010252
APA StyleTan, J. B., Cook, M. J., Logan, P., Rozanova, L., & Wilder-Smith, A. (2021). Singapore’s Pandemic Preparedness: An Overview of the First Wave of COVID-19. International Journal of Environmental Research and Public Health, 18(1), 252. https://doi.org/10.3390/ijerph18010252