Agreement of Three Posturographic Force Plates in the Assessment of Postural Stability
Abstract
1. Introduction
2. Materials and Methods
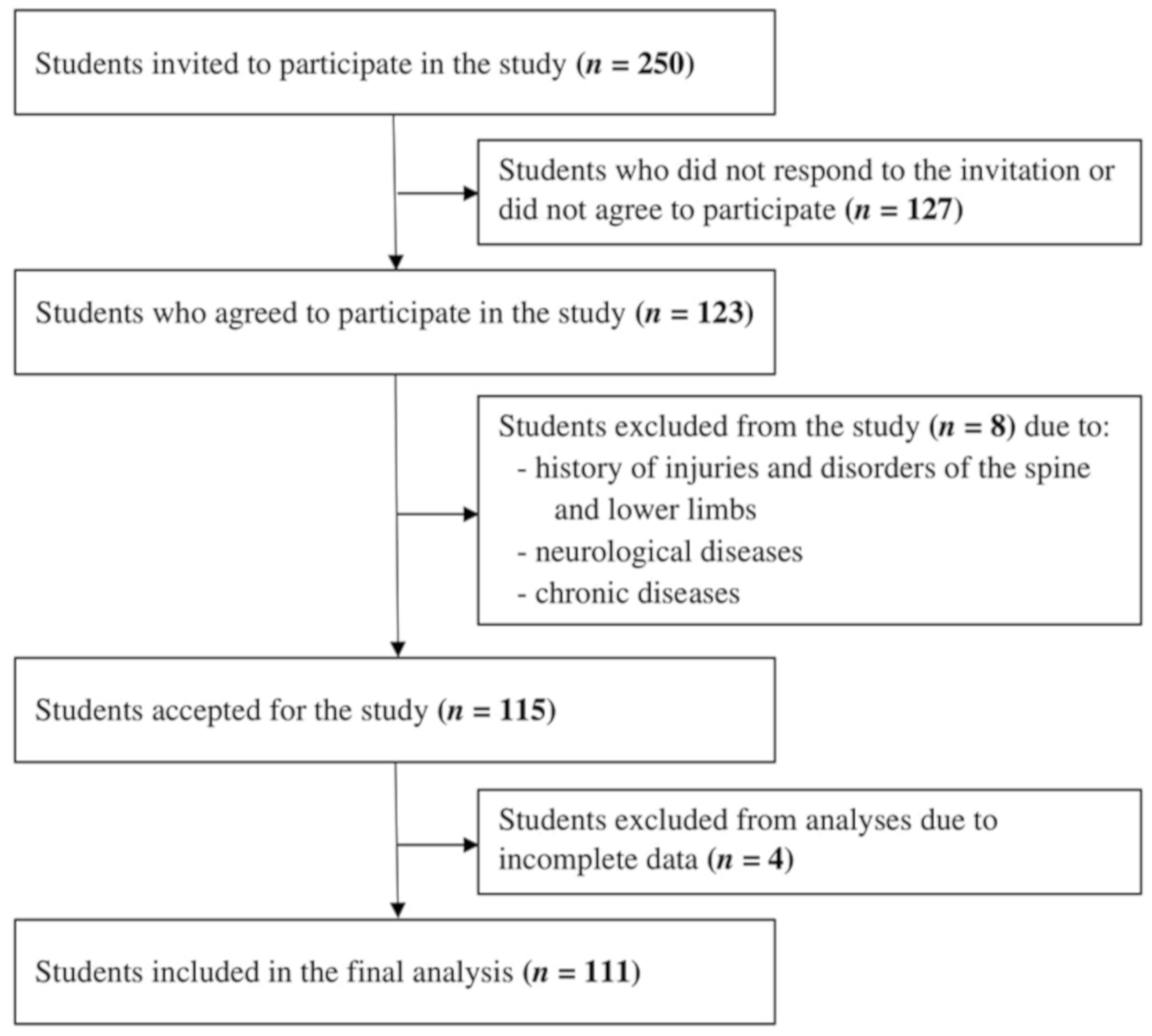
2.1. Participants
2.2. Experimental Instrumentation
2.3. Procedures
2.4. Data Analysis
- COP area (mm2) eyes open (A-EO).
- COP area (mm2) eyes closed (A-EC).
- COP area Romberg ratio (A-RR).
- COP path length (mm) eyes open (L-EO).
- COP path length (mm) eyes closed (L-EC).
- COP path length Romberg ratio (L-RR).
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Teasdale, N.; Simoneau, M. Attentional demands for postural control: The effects of aging and sensory reintegration. Gait Posture 2001, 14, 203–210. [Google Scholar] [CrossRef]
- Corbeil, P.; Blouin, J.S.; Bégin, F.; Nougier, V.; Teasdale, N. Perturbation of the postural control system induced by muscular fatigue. Gait Posture 2003, 18, 92–100. [Google Scholar] [CrossRef]
- Matłosz, P.; Domino, G. Analysis of selected parameters of Judoists’ Junior Polish Representation fitness. Sci. Rev. Phys. Cult. 2015, 5, 303–308. [Google Scholar]
- Rogind, H.; Simonsen, H.; Era, P.; Bliddal, H. Comparison of Kistler 9861A force platform and Chattecx Balance System for measurement of postural sway: Correlation and test-retest reliability. Scand. J. Med. Sci. Sport. 2003, 13, 106–114. [Google Scholar] [CrossRef] [PubMed]
- Cappello, A.; Bagalà, F.; Cedraro, A.; Chiari, L. Non-linear re-calibration of force platforms. Gait Posture 2011, 33, 724–726. [Google Scholar] [CrossRef] [PubMed]
- Olejarz, P.; Olchowik, G. Rola dynamicznej posturografii komputerowej w diagnostyce zaburzeń równowagi. Otorynolaryngologia 2011, 10, 103–110. [Google Scholar]
- Thornby, M.A. Balance and falls in the frail older person: A review of the literature. Top. Geriatr. Rehabil. 1995, 11, 35–43. [Google Scholar] [CrossRef]
- Nougier, V.; Bard, C.; Fleury, M.; Teasdale, N. Contribution of central and peripheral vision to the regulation of stance. Gait Posture 1997, 5, 34–41. [Google Scholar] [CrossRef]
- Hay, L.; Bard, C.; Fleury, M.; Teasdale, N. Availability of visual and proprioceptive afferent messages and postural control in elderly adults. Exp. Brain Res. 1996, 108, 129–139. [Google Scholar] [CrossRef]
- Simoneau, M.; Teasdale, N.; Bourdin, C.; Bard, C.; Fleury, M.; Nougier, V. Aging and postural control: Postural perturbations caused by changing the visual anchor. J. Am. Geriatr. Soc. 1999, 47, 235–240. [Google Scholar] [CrossRef]
- Teasdale, N.; Stelmach, G.E.; Breunig, A. Postural Sway Characteristics of the Elderly Under Normal and Altered Visual and Support Surface Conditions. J. Gerontol. Biol. Sci. 1991, 46, 238–244. [Google Scholar] [CrossRef] [PubMed]
- Bouisset, S.; Zattara, M. Biomechanical study of the programming of anticipatory postural adjustments associated with voluntary movement. J. Biomech. 1987, 20, 735–742. [Google Scholar] [CrossRef]
- Klous, M.; Mikulic, P.; Latash, M.L. Two aspects of feedforward postural control: Anticipatory postural adjustments and anticipatory synergy adjustments. J. Neurophysiol. 2011, 105, 2275–2288. [Google Scholar] [CrossRef] [PubMed]
- Massion, J. Movement, posture and equilibrium: Interaction and coordination. Prog. Neurobiol. 1992, 38, 35–56. [Google Scholar] [CrossRef]
- Samson, M.; Crowe, A. Intra-subject inconsistencies in quantitative assessments of body sway. Gait Posture 1996, 4, 252–257. [Google Scholar] [CrossRef]
- Santos, B.R.; Delisle, A.; Larivière, C.; Plamondon, A.; Imbeau, D. Reliability of center of pressure summary measures of postural steadiness in healthy young adults. Gait Posture 2008, 27, 408–415. [Google Scholar] [CrossRef]
- Van der Kooij, H.; Campbell, A.D.; Carpenter, M.G. Sampling duration effects on center of pressure descriptive measures. Gait Posture 2011, 34, 19–24. [Google Scholar] [CrossRef]
- Rogers, M.; Wardman, D.; Lord, S.; Fitzpatrick, R. Passive tactile sensory input improves stability during standing. Exp. Brain Res. 2001, 136, 514–522. [Google Scholar] [CrossRef]
- Raymakers, J.A.; Samson, M.M.; Verhaar, H.J.J. The assessment of body sway and the choice of the stability parameter(s). Gait Posture 2005, 21, 48–58. [Google Scholar] [CrossRef]
- Skalska, A.; Ocetkiewicz, T.; Zak, M.; Grodzicki, T. Influence of age on postural control parameters measured with a balance platform. New Med. 2004, 7, 12–16. [Google Scholar]
- Błaszczyk, J.W. The use of force-plate posturography in the assessment of postural instability. Gait Posture 2016, 44, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Carpenter, M.G.; Frank, J.S.; Winter, D.A.; Peysar, G.W. Sampling duration effects on center of pressure summary measures. Gait Posture 2001, 13, 35–40. [Google Scholar] [CrossRef]
- Kingma, H.; Gauchard, G.C.; de Waele, C.; van Nechel, C.; Bisdorff, A.; Yelnik, A.; Magnusson, M.; Perrin, P.P. Stocktaking on the development of posturography for clinical use. J. Vestib. Res. 2011, 21, 117–125. [Google Scholar] [CrossRef] [PubMed]
- Le Clair, K.; Riach, C. Postural stability measures: What to measure and for how long. Clin. Biomech. 1996, 11, 176–178. [Google Scholar] [CrossRef]
- Doyle, R.J.; Ragan, B.G.; Rajendran, K.; Rosengren, K.S.; Hsiao-Wecksler, E.T. Generalizability of Stabilogram Diffusion Analysis of center of pressure measures. Gait Posture 2008, 27, 223–230. [Google Scholar] [CrossRef]
- Scoppa, F.; Capra, R.; Gallamini, M.; Shiffer, R. Clinical stabilometry standardization. Basic definition—Acquisition interval—Sampling frequency. Gait Posture 2013, 37, 290–292. [Google Scholar] [CrossRef]
- Russo, L.; D’Eramo, U.; Padulo, J.; Foti, C.; Schiffer, R.; Scoppa, F. Day-time effect on postural stability in young sportsmen. Muscles Ligaments Tendons J. 2015, 5, 38–42. [Google Scholar] [CrossRef]
- Golriz, S.; Hebert, J.J.; Foreman, K.; Walker, B.F. The validity of a portable clinical force plate in assessment of static postural control: Concurrent validity study. Chiropr. Man. Therap. 2012, 20, 15. [Google Scholar] [CrossRef]
- Doyle, R.J.; Hsiao-Wecksler, E.T.; Ragan, B.G.; Rosengren, K.S. Generalizability of center of pressure measures of quiet standing. Gait Posture 2007, 25, 166–171. [Google Scholar] [CrossRef]
- Mikołajczyk, E.; Jankowicz-Szymańska, A. The effect of unstable-surface functional exercises on static balance in adolescents with intellectual disability—A preliminary report. Med. Stud. 2014, 30, 1–5. [Google Scholar] [CrossRef]
- Khasnis, A.; Gokula, R.M. Romberg’s test. J. Postgrad. Med. 2003, 49, 169. [Google Scholar] [PubMed]
- Tjernström, F.; Björklund, M.; Malmström, E.-M. Romberg ratio in quiet stance posturography—Test to retest reliability. Gait Posture 2015, 42, 27–31. [Google Scholar] [CrossRef] [PubMed]
- Lacour, M.; Barthelemy, J.; Borel, L.; Magnan, J.; Xerri, C.; Chays, A.; Ouaknine, M. Sensory strategies in human postural control before and after unilateral vestibular neurotomy. Exp. Brain Res. 1997, 115, 300–310. [Google Scholar] [CrossRef] [PubMed]
- Martin Bland, J.; Altman, D. Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 1986, 327, 307–310. [Google Scholar] [CrossRef]
- De Kegel, A.; Dhooge, I.; Cambier, D.; Baetens, T.; Palmans, T.; Van Waelvelde, H. Test-retest reliability of the assessment of postural stability in typically developing children and in hearing impaired children. Gait Posture 2011, 33, 679–685. [Google Scholar] [CrossRef]
- Pinsault, N.; Vuillerme, N. Test-Retest reliability of center of foot pressure measures to assess postural control during unperturbed stance. Med. Eng. Phys. 2009, 31, 276–286. [Google Scholar] [CrossRef]
| Compared Platforms | Analyzed Parameters | ||||||
|---|---|---|---|---|---|---|---|
| A-EO | A-EC | A-RR | L-EO | L-EC | L-RR | ||
| AccuGait | mean (SD) | 102 (68.4) | 204.7 (121.1) | 31.8 (25) | 662.7 (110) | 731.1 (120.1) | 4.9 (4.5) |
| Alfa | mean (SD) | 131.8 (76.6) | 211.4 (128.7) | 20.9 (25.4) | 169.1 (66.5) | 263.5 (119.6) | 20.7 (14.9) |
| CQStab2P | mean (SD) | 119.2 (81.6) | 116.1 (86.3) | −1.3 (28) | 173.2 (52.6) | 190.6 (46.5) | 5.2 (11.3) |
| ICC3 | 0.2800 | 0.1200 | 0.0053 | 0.0845 | 0.0801 | 0.0840 | |
| p | 0.0220 * | 0.2100 | 0.4800 | 0.2900 | 0.3000 | 0.2900 | |
| Compared Platforms | Analyzed Parameters | |||||
|---|---|---|---|---|---|---|
| A-EO | A-EC | A-RR | L-EO | L-EC | L-RR | |
| Spearman’s rank correlation | ||||||
| AccuGait/Alfa | 0.01 | 0.09 | 0.05 | 0.05 | 0.01 | −0.19 * |
| AccuGait/CQStab2P | 0.06 | 0.07 | 0.17 | 0.11 | 0.05 | −0.23 * |
| Alfa/CQStab2P | 0.32 * | 0.38 * | 0.20 * | 0.26 * | 0.33 * | 0.24 * |
| Concordance correlation coefficient | ||||||
| AccuGait/Alfa | 0.02 | −0.06 | −0.03 | 0.00 | −0.01 | −0.04 |
| AccuGait/CQStab2P | 0.07 | −0.03 | −0.06 | 0.00 | 0.00 | −0.14 |
| Alfa/CQStab2P | 0.22 | 0.17 | 0.10 | 0.16 | 0.14 | 0.11 |
| Friedman ANOVA | Analyzed Parameters | |||||
|---|---|---|---|---|---|---|
| A-EO | A-EC | A-RR | L-EO | L-EC | L-RR | |
| chi2 | 11.261 | 52.829 | 58.541 | 166.86 | 176.23 | 83.099 |
| p | 0.0036 | <0.0001 * | <0.0001 * | <0.0001 * | <0.0001 * | <0.0001 * |
| Compared platforms | Nemenyi post-hoc test for the analyzed parameters | |||||
| AccuGait/Alfa | 0.0023 * | 0.6200 | 0.0690 | <0.0001 * | <0.0001 * | <0.0001 * |
| AccuGait/CQStab2P | 0.2137 | <0.0001 * | <0.0001 * | <0.0001 * | <0.0001 * | 0.6200 |
| Alfa/CQStab2P | 0.2137 | <0.0001 * | <0.0001 * | 0.8200 | 0.00022 * | <0.0001 * |
| Compared Platforms | Analyzed Parameters | |||||
|---|---|---|---|---|---|---|
| A-EO | A-EC | A-RR | L-EO | L-EC | L-RR | |
| Wilcoxon matched pair test | ||||||
| AccuGait/Alfa | 0.0020 * | 0.6400 | 0.0680 | <0.0001 * | <0.0001 * | <0.0001 * |
| AccuGait/CQStab2P | 0.0620 | <0.0001 * | <0.0001 * | <0.0001 * | <0.0001 * | 0.6100 |
| Alfa/CQStab2P | 0.0410 * | <0.0001 * | <0.0001 * | <0.0001 * | <0.0001 * | <0.0001 * |
| Compared Platforms | Analyzed Parameters (z-Scores) | ||||||
|---|---|---|---|---|---|---|---|
| A-EO | A-EC | A-RR | L-EO | L-EC | L-RR | ||
| AccGait/Alfa | MD 95% LOA | −0.44 2.92 | −0.09 3.01 | 0.44 2.85 | 4.51 2.38 | 3.88 2.95 | −3.56 7.16 |
| AccGait/CQStab2P | MD 95% LOA | −0.25 2.95 | 0.73 2.46 | 1.33 3.12 | 4.47 2.09 | 4.53 2.13 | −0.07 5.69 |
| Alfa/CQStab2P | MD 95% LOA | 0.19 2.83 | 0.82 2.25 | 0.89 2.76 | −0.04 1.39 | 0.65 2.04 | 3.48 7.44 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Matłosz, P.; Wyszyńska, J.; Podgórska-Bednarz, J.; Leszczak, J.; Rachwał, M.; Przednowek, K.; Drzał-Grabiec, J.; Walicka-Cupryś, K.; Drużbicki, M.; Zadarko, E. Agreement of Three Posturographic Force Plates in the Assessment of Postural Stability. Int. J. Environ. Res. Public Health 2020, 17, 3188. https://doi.org/10.3390/ijerph17093188
Matłosz P, Wyszyńska J, Podgórska-Bednarz J, Leszczak J, Rachwał M, Przednowek K, Drzał-Grabiec J, Walicka-Cupryś K, Drużbicki M, Zadarko E. Agreement of Three Posturographic Force Plates in the Assessment of Postural Stability. International Journal of Environmental Research and Public Health. 2020; 17(9):3188. https://doi.org/10.3390/ijerph17093188
Chicago/Turabian StyleMatłosz, Piotr, Justyna Wyszyńska, Justyna Podgórska-Bednarz, Justyna Leszczak, Maciej Rachwał, Krzysztof Przednowek, Justyna Drzał-Grabiec, Katarzyna Walicka-Cupryś, Mariusz Drużbicki, and Emilian Zadarko. 2020. "Agreement of Three Posturographic Force Plates in the Assessment of Postural Stability" International Journal of Environmental Research and Public Health 17, no. 9: 3188. https://doi.org/10.3390/ijerph17093188
APA StyleMatłosz, P., Wyszyńska, J., Podgórska-Bednarz, J., Leszczak, J., Rachwał, M., Przednowek, K., Drzał-Grabiec, J., Walicka-Cupryś, K., Drużbicki, M., & Zadarko, E. (2020). Agreement of Three Posturographic Force Plates in the Assessment of Postural Stability. International Journal of Environmental Research and Public Health, 17(9), 3188. https://doi.org/10.3390/ijerph17093188










