How Are Information and Communication Technologies Supporting Routine Outcome Monitoring and Measurement-Based Care in Psychotherapy? A Systematic Review
Abstract
1. Introduction
2. Materials and Methods
2.1. Search Strategy
2.2. Inclusion Criteria
2.3. Exclusion Criteria
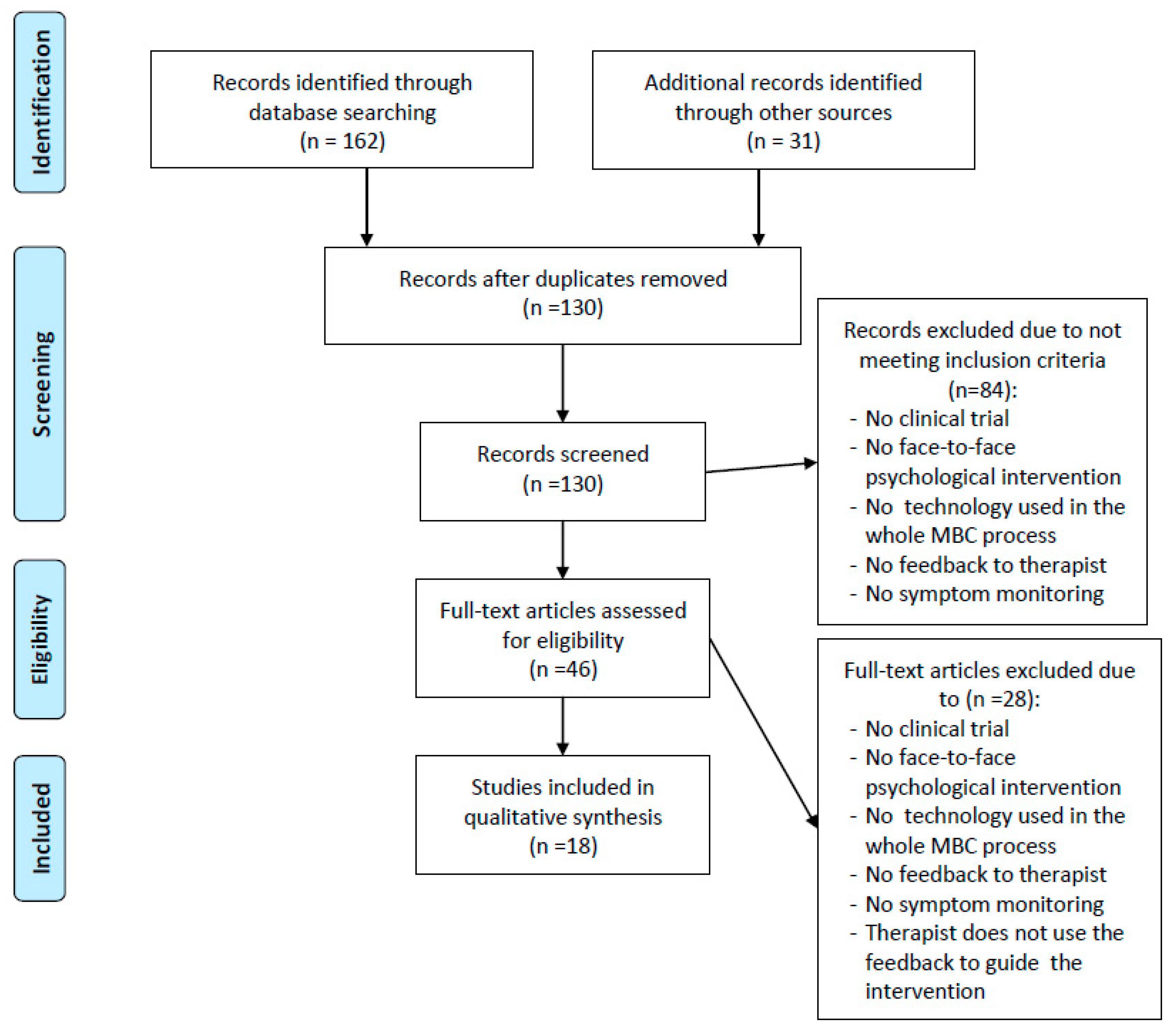
2.4. Search and Screening
2.5. Data Extraction
2.6. Risk of Bias Assessment
2.7. Synthesis of Results
2.8. Additional Analyses
3. Results
3.1. Characteristics of Included Studies
3.2. MBC Characteristics
3.2.1. Assessment Procedure Used to Track the Patient’s Status
3.2.2. Feedback Procedure
3.3. Technology Characteristics
3.3.1. Technology Feasibility
3.3.2. Clinical Effectiveness
3.4. Risk of Bias Assessment
4. Discussion
4.1. Limitations
4.2. Conclusions
Author Contributions
Funding
Conflicts of Interest
Appendix A. Complete List of Search Terms and Combinations
References
- Shimokawa, K.; Lambert, M.J.; Smart, D.W. Enhancing treatment outcome of patients at risk of treatment failure: Meta-analytic and mega-analytic review of a psychotherapy quality assurance system. J. Consult. Clin. Psychol. 2010, 78, 298–311. [Google Scholar] [CrossRef] [PubMed]
- Lambert, M.J.; Hansen, N.B.; Finch, A.E. Patient-focused research: Using patient outcome data to enhance treatment effects. J. Consult. Clin. Psychol. 2001, 69, 159–172. [Google Scholar] [CrossRef] [PubMed]
- Kaplan, S.H.; Billimek, J.; Sorkin, D.H.; Ngo-Metzger, Q.; Greenfield, S. Who can respond to treatment? Med. Care 2010, 48, S9–S16. [Google Scholar] [CrossRef] [PubMed]
- McDevitt-Murphy, M.E.; Luciano, M.T.; Zakarian, R.J. Use of ecological momentary assessment and intervention in treatment with adults. Focus (Madison) 2018, 16, 370–375. [Google Scholar] [CrossRef]
- Suso-Ribera, C.; Mesas, Á.; Medel, J.; Server, A.; Márquez, E.; Castilla, D.; Zaragozá, I.; García-Palacios, A.; Mesas, A.; Medel, J.; et al. Improving pain treatment with a smartphone app: Study protocol for a randomized controlled trial. Trials 2018, 19, 145. [Google Scholar] [CrossRef]
- Colombo, D.; Fernández-Álvarez, J.; Suso-Ribera, C.; Cipresso, P.; Valev, H.; Leufkens, T.; Sas, C.; Garcia-Palacios, A.; Riva, G.; Botella, C. The need for change: Understanding emotion regulation antecedents and consequences using ecological momentary assessment. Emotion 2020, 20, 30–36. [Google Scholar] [CrossRef]
- Beute, F.; De Kort, Y.; Ijsselsteijn, W. Restoration in its natural context: How ecological momentary assessment can advance restoration research. Int. J. Environ. Res. Public Health 2016, 13, 420. [Google Scholar] [CrossRef]
- Kendrick, T.; Moore, M.; Gilbody, S.; Churchill, R.; Stuart, B.; El-Gohary, M. Routine use of patient reported outcome measures (PROMs) for improving treatment of common mental health disorders in adults. Cochrane Database Syst. Rev. 2014, 2014. [Google Scholar] [CrossRef]
- Canadian Psychological Association. Outcomes and Progress Monitoring in Psychotherapy; A Report of the Canadian Psychological Association, Prepared by the Task Force on Outcomes and Progress Monitoring in Psychotherapy; Canadian Psychological Association: Ottawa, ON, Canada, 2018. [Google Scholar]
- Knaup, C.; Koesters, M.; Schoefer, D.; Becker, T.; Puschner, B. Effect of feedback of treatment outcome in specialist mental healthcare: Meta-analysis. Br. J. Psychiatry 2009, 195, 15–22. [Google Scholar] [CrossRef]
- Scott, K.; Lewis, C.C. Using measurement-based care to enhance any treatment. Cogn. Behav. Pract. 2015, 22, 49–59. [Google Scholar] [CrossRef]
- Lambert, M.J.; Whipple, J.L.; Smart, D.W.; Vermeersch, D.A.; Nielsen, S.L.; Hawkins, E.J. The effects of providing therapists with feedback on patient progress during psychotherapy: Are outcomes enhanced? Psychother. Res. 2001, 11, 49–68. [Google Scholar] [CrossRef] [PubMed]
- Goldberg, S.B.; Buck, B.; Raphaely, S.; Fortney, J.C. Measuring psychiatric symptoms remotely: A systematic review of remote measurement-based care. Curr. Psychiatry Rep. 2018, 20, 81. [Google Scholar] [CrossRef] [PubMed]
- Reese, R.J.; Norsworthy, L.A.; Rowlands, S.R. Does a continuous feedback system improve psychotherapy outcome? Psychotherapy 2009, 46, 418–431. [Google Scholar] [CrossRef] [PubMed]
- Lambert, M.J.; Harmon, C.; Slade, K.; Whipple, J.L.; Hawkins, E.J. Providing feedback to psychotherapists on their patients’ progress: Clinical results and practice sugges tions. J. Clin. Psychol. 2005, 61, 165–174. [Google Scholar] [CrossRef] [PubMed]
- Bickman, L.; Kelley, S.D.; Breda, C.; De Andrade, A.R.; Riemer, M. Effects of routine feedback to clinicians on mental health outcomes of youths: Results of a randomized trial. Psychiatr. Serv. 2011, 62, 1423–1429. [Google Scholar] [CrossRef]
- Carlier, I.V.E.; Meuldijk, D.; Van Vliet, I.M.; Van Fenema, E.; Van Der Wee, N.J.A.; Zitman, F.G. Routine outcome monitoring and feedback on physical or mental health status: Evidence and theory. J. Eval. Clin. Pract. 2012, 18, 104–110. [Google Scholar] [CrossRef]
- Gondek, D.; Edbrooke-Childs, J.; Fink, E.; Deighton, J.; Wolpert, M. Feedback from outcome measures and treatment effectiveness, treatment efficiency, and collaborative practice: A systematic review. Adm. Policy Ment. Health Ment. Health Serv. Res. 2016, 43, 325–343. [Google Scholar] [CrossRef]
- Imel, Z.E.; Caperton, D.D.; Tanana, M.; Atkins, D.C. Technology-enhanced human interaction in psychotherapy. J. Couns. Psychol. 2017, 64, 385–393. [Google Scholar] [CrossRef]
- Aboraya, A.; Nasrallah, H.A.; Elswick, D.E.; Elshazly, A.; Estephan, N.; Aboraya, D.; Berzingi, S.; Chumbers, J.; Berzingi, S.; Justice, J.; et al. Measurement-based care in psychiatry—Past, present, and future. Innov. Clin. Neurosci. 2018, 15, 13–26. [Google Scholar]
- Hallgren, K.A.; Bauer, A.M.; Atkins, D.C. Digital technology and clinical decision making in depression treatment: Current findings and future opportunities. Depress. Anxiety 2017, 34, 494–501. [Google Scholar] [CrossRef]
- Bauer, S.; Moessner, M. Technology-enhanced monitoring in psychotherapy and e-mental health. J. Ment. Health 2012, 21, 355–363. [Google Scholar] [CrossRef] [PubMed]
- Silk, J.S.; Forbes, E.E.; Whalen, D.J.; Jakubcak, J.L.; Thompson, W.K.; Ryan, N.D.; Axelson, D.A.; Birmaher, B.; Dahl, R.E. Daily emotional dynamics in depressed youth: A cell phone ecological momentary assessment study. J. Exp. Child Psychol. 2011, 110, 241–257. [Google Scholar] [CrossRef] [PubMed]
- Suso-Ribera, C.; Castilla, D.; Zaragozá, I.; Ribera-Canudas, M.V.; Botella, C.; García-Palacios, A. Validity, reliability, feasibility, and usefulness of Pain Monitor. A multidimensional smartphone app for daily monitoring of adults with heterogeneous chronic pain. Clin. J. Pain 2018, 34, 900–908. [Google Scholar] [CrossRef] [PubMed]
- Hegland, P.A.; Aasprang, A.; Hjelle Øygard, S.; Nordberg, S.; Kolotkin, R.; Moltu, C.; Tell, G.S.; Andersen, J.R. A review of systematic reviews on the effects of patient-reported outcome monitoring with clinical feedback systems on health-related quality of life-implications for a novel technology in obesity treatment. Clin. Obes. 2018, 8, 452–464. [Google Scholar] [CrossRef]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G.; Altman, D.G.; Antes, G.; Atkins, D.; Barbour, V.; Barrowman, N.; Berlin, J.A.; et al. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement (Chinese edition). J. Chin. Integr. Med. 2009, 7, 889–896. [Google Scholar] [CrossRef]
- Falagas, M.E.; Pitsouni, E.I.; Malietzis, G.A.; Pappas, G. Comparison of PubMed, Scopus, Web of Science, and Google Scholar: Strengths and weaknesses. FASEB J. 2008, 22, 338–342. [Google Scholar] [CrossRef]
- Eady, A.M.; Wilczynski, N.L.; Haynes, R.B. PsycINFO search strategies identified methodologically sound therapy studies and review articles for use by clinicians and researchers. J. Clin. Epidemiol. 2008, 61, 34–40. [Google Scholar] [CrossRef]
- National Heart Lung and Blood Institute (NHLBI). Study Quality Assessment Tools. Available online: https://www.nhlbi.nih.gov/health-topics/study-quality-assessment-tools (accessed on 1 May 2020).
- Smith, B.; Harms, W.D.; Burres, S.; Korda, H.; Rosen, H.; Davis, J. Enhancing behavioral health treatment and crisis management through mobile ecological momentary assessment and SMS messaging. Health Inform. J. 2012, 18, 294–308. [Google Scholar] [CrossRef]
- Pramana, G.; Parmanto, B.; Kendall, P.C.; Silk, J.S. The SmartCAT: An m-health platform for ecological momentary intervention in child anxiety treatment. Telemed. e-Health 2014, 20, 419–427. [Google Scholar] [CrossRef]
- Pinsof, W.M.; Goldsmith, J.Z.; Latta, T.A. Information technology and feedback research can bridge the scientist–practitioner gap: A couple therapy example. Couple Fam. Psychol. Res. Pract. 2012, 1, 253–273. [Google Scholar] [CrossRef]
- Aguilera, A.; Bruehlman-Senecal, E.; Demasi, O.; Avila, P. Automated Text messaging as an adjunct to cognitive behavioral therapy for depression: A clinical trial. J. Med. Internet Res. 2017, 19, e148. [Google Scholar] [CrossRef] [PubMed]
- Kumar, D.; Tully, L.M.; Iosif, A.-M.; Zakskorn, L.N.; Nye, K.E.; Zia, A.; Niendam, T.A. A mobile health platform for clinical monitoring in early psychosis: Implementation in community-based outpatient early psychosis care. JMIR Ment. Health 2018, 5, e15. [Google Scholar] [CrossRef] [PubMed]
- Aharonovich, E.; Sarvet, A.; Stohl, M.; DesJarlais, D.; Tross, S.; Hurst, T.; Urbina, A.; Hasin, D. Reducing non-injection drug use in HIV primary care: A randomized trial of brief motivational interviewing, with and without HealthCall, a technology-based enhancement. J. Subst. Abuse Treat. 2017, 74, 71–79. [Google Scholar] [CrossRef] [PubMed]
- Niendam, T.A.; Tully, L.M.; Iosif, A.M.; Kumar, D.; Nye, K.E.; Denton, J.C.; Zakskorn, L.N.; Fedechko, T.L.; Pierce, K.M. Enhancing early psychosis treatment using smartphone technology: A longitudinal feasibility and validity study. J. Psychiatr. Res. 2018, 96, 239–246. [Google Scholar] [CrossRef]
- Bauer, A.M.; Iles-Shih, M.; Ghomi, R.H.; Rue, T.; Grover, T.; Kincler, N.; Miller, M.; Katon, W.J. Acceptability of mHealth augmentation of Collaborative Care: A mixed methods pilot study. Gen. Hosp. Psychiatry 2018, 51, 22–29. [Google Scholar] [CrossRef]
- Bell, I.H.; Rossell, S.L.; Farhall, J.; Hayward, M.; Lim, M.H.; Fielding-Smith, S.F.; Thomas, N. Pilot randomised controlled trial of a brief coping-focused intervention for hearing voices blended with smartphone-based ecological momentary assessment and intervention (SAVVy): Feasibility, acceptability and preliminary clinical outcomes. Schizophr. Res. 2019. [Google Scholar] [CrossRef]
- Bell, I.H.; Fielding-Smith, S.F.; Hayward, M.; Rossell, S.L.; Lim, M.H.; Farhall, J.; Thomas, N. Smartphone-based ecological momentary assessment and intervention in a blended coping-focused therapy for distressing voices: Development and case illustration. Internet Interv. 2018, 14, 18–25. [Google Scholar] [CrossRef]
- Newnham, E.A.; Hooke, G.R.; Page, A.C. Progress monitoring and feedback in psychiatric care reduces depressive symptoms. J. Affect. Disord. 2010, 127, 139–146. [Google Scholar] [CrossRef]
- Delgadillo, J.; Overend, K.; Lucock, M.; Groom, M.; Kirby, N.; McMillan, D.; Gilbody, S.; Lutz, W.; Rubel, J.A.; De Jong, K. Improving the efficiency of psychological treatment using outcome feedback technology. Behav. Res. Ther. 2017, 99, 89–97. [Google Scholar] [CrossRef]
- Delgadillo, J.; De Jong, K.; Lucock, M.; Lutz, W.; Rubel, J.; Gilbody, S.; Ali, S.; Aguirre, E.; Appleton, M.; Nevin, J.; et al. Feedback-informed treatment versus usual psychological treatment for depression and anxiety: A multisite, open-label, cluster randomised controlled trial. Lancet Psychiatry 2018, 5, 564–572. [Google Scholar] [CrossRef]
- Miklowitz, D.J.; Price, J.; Holmes, E.A.; Rendell, J.; Bell, S.; Budge, K.; Christensen, J.; Wallace, J.; Simon, J.; Armstrong, N.M.; et al. Facilitated Integrated Mood Management for adults with bipolar disorder. Bipolar Disord. 2012, 14, 185–197. [Google Scholar] [CrossRef] [PubMed]
- Schiepek, G.; Aichhorn, W.; Gruber, M.; Strunk, G.; Bachler, E.; Aas, B. Real-time monitoring of psychotherapeutic processes: Concept and compliance. Front. Psychol. 2016, 7, 604. [Google Scholar] [CrossRef] [PubMed]
- Kaiser, T.; Laireiter, A.R. DynAMo: A modular platform for monitoring process, outcome, and algorithm-based treatment planning in psychotherapy. JMIR Med. Inform. 2017, 5, e20. [Google Scholar] [CrossRef] [PubMed]
- Lazarou, I.; Karakostas, A.; Stavropoulos, T.G.; Tsompanidis, T.; Meditskos, G.; Kompatsiaris, I.; Tsolaki, M. A novel and intelligent home monitoring system for care support of elders with cognitive impairment. J. Alzheimer’s Dis. 2016, 54, 1561–1591. [Google Scholar] [CrossRef] [PubMed]
- De Jong, K.; Timman, R.; Hakkaart-Van Roijen, L.; Vermeulen, P.; Kooiman, K.; Passchier, J.; Van Busschbach, J. The effect of outcome monitoring feedback to clinicians and patients in short and long-term psychotherapy: A randomized controlled trial. Psychother. Res. 2014, 24, 629–639. [Google Scholar] [CrossRef]
- Amble, I.; Gude, T.; Stubdal, S.; Andersen, B.J.; Wampold, B.E. The effect of implementing the Outcome Questionnaire-45.2 feedback system in Norway: A multisite randomized clinical trial in a naturalistic setting. Psychother. Res. 2015, 25, 669–677. [Google Scholar] [CrossRef]
- Janse, P.D.; De Jong, K.; Van Dijk, M.K.; Hutschemaekers, G.J.M.; Verbraak, M.J.P.M. Improving the efficiency of cognitive-behavioural therapy by using formal client feedback. Psychother. Res. 2017, 27, 525–538. [Google Scholar] [CrossRef]
- Lucock, M.; Halstead, J.; Leach, C.; Barkham, M.; Tucker, S.; Randal, C.; Middleton, J.; Khan, W.; Catlow, H.; Waters, E.; et al. A mixed-method investigation of patient monitoring and enhanced feedback in routine practice: Barriers and facilitators. Psychother. Res. 2015, 25, 633–646. [Google Scholar] [CrossRef]
| Reference | Country | Setting | Psychological Disorder | Sample size | Study Design | Type of Psychological Intervention |
|---|---|---|---|---|---|---|
| [30] | California (USA) | Specialist inpatient treatment center | PTSD | 27 Tx | SG (feasibility study) | Residential group psychotherapy (4–5 months) |
| [31] | Pittsburgh (USA) | Outpatient Psychiatric Institute and Clinic | Anxiety disorders (children from 9 to 14 years old) | 9 Tx (3 received 16-sessions CBT, 6 received 8-sessions Brief CBT) | SG (feasibility pilot trial) | “Coping Cat”: 16 CBT sessions“Brief Coping Cat”: 8 CBT sessions |
| [32] | Evanston, Illinois (USA) | Outpatient clinic at the Family Institute at Northwestern University | Couple problems | 1 Tx | Case study | Four Couple Multisystemic Psychotherapy sessions |
| [33] | California University: Berkeley (USA) | Outpatient behavioural health clinic | Depression | 85 (40 cont. + 45 Tx) | nRCT (not blinded) | 16 weeks of weekly group CBT therapy |
| [34] | California (USA) | 4 Outpatient Early Psychosis clinics | Psychotic disorder | 61 Tx | SG (feasibility study) | Early Psychosis Program (up to 5 months) |
| [35] | New York (USA) | Outpatient primary care | Substance use | 240 (83 cont. + 77 Tx + 80 Tx HealthCall) | Three-arm RCT (1:1:1 allocation ratio) | Brief (25–30 min) individual (motivational interview) psychoeducation (3 sessions: every 30 days) |
| [36] | California University (USA) | Outpatient specialist clinic | Psychotic disorder (adolescent and young) | 76 Tx | SG (feasibility pilot trial) | Early Psychosis Program (minimum 3 months) |
| [37] | Washington University (USA) | Outpatient primary care clinic affiliated with the Washington University | Depression and Anxiety | 17 Tx | SG (feasibility and acceptability pilot study) | Collaborative care program (over 6 months) |
| [38] | Melbourne (Australia) | Outpatient Specialist Voices Clinic and clinical services | Schizophrenia | 34 (17 cont. + 17 Tx) | A single-blind, parallel group, pilot RCT (1:1 allocation ratio) | Brief CBT (four in-person therapy sessions) + EMA + EMI |
| [39] | Melbourne (Australia) | Outpatient Specialist Voices clinic | Schizophrenia | 1 Tx | Case study | Brief CBT (four in-person therapy sessions) + EMA+ EMI |
| [40] | Perth (Australia) | Private inpatients and day-patients psychiatric hospital | Mood and Anxiety | 1308 (408 Tx Fb +, 439 nFb + 461 cont.) | nRCT | 10 days of intensive CBT group |
| [41] | Leeds (England) | Outpatient clinic | Depression and Anxiety | 594 (349 cont. + 245 Tx) | Quasi-experimental pre-post study | Low-intensity guided self-help CBT or High-intensity CBT, interpersonal psychotherapy and counselling |
| [42] | England | 8 outpatient clinics | Depression and Anxiety | 2233 (1057 cont. + 1176 Tx) | Multisite, open-label, cluster RCT | Low-intensity guided self-help CBT or High-intensity CBT, interpersonal psychotherapy and counselling |
| [43] | Oxford (UK) | Outpatient specialist mental health | Bipolar disorder | 19 Tx | SG (pre-post) | five sessions of psychoeducational intervention (FIMM) + pharmacotherapy |
| [44] | Salzburg (Austria) | Inpatient and a day-treatment clinic | Mood disorders; Psychoactive substance use mental disorders; Schizophrenia, schizotypal, and delusional disorders; Neurotic, stress-related, and somatoform disorders; Personality disorders, and others | 151 Tx | SG (feasibility pilot trial) | Psychotherapy (8 weeks in the day-treatment clinic and 12 weeks in the inpatient clinic) |
| [45] | Salzburg (Austria) | Outpatient clinic | Bulimia nervosa | 1 Tx | Case study | six Rogerian person-centred psychotherapy sessions |
| [46] | Thessaloniki (Greece) | Alzheimer day care centre (at home) | Dementia | 4 Tx | Case study | 15 Individual psychotherapy sessions (psychosocial intervention, CBT, relaxation techniques, etc.) |
| [47] | The Netherlands | Outpatient mental health institutions or private practices | Mood disorder, Adjustment disorder, Anxiety disorder, Relational problems, Personality disorders, and others | 475 (159 Tx FbT; 172 Tx FbTP; 144 cont. nFb) | RCT | Long and short psychotherapy (CBT, client-centered, psychodynamics) |
| Reference | Assessment Frequency and Setting | Primary Outcome Measures | Feedback to | Feedback Frequency and Setting | Type of Technology Used |
|---|---|---|---|---|---|
| [30] | Daily at a random time | Adapted questionnaire from Symptom Checklist-6, the BriefCOPE and Beck Depression Inventory-II | T and P | P: T regularly shared P progress in order to incorporate strategies in therapy sessions and treatment plan.T: They got patient information several times a week in a graph format to discuss with them during sessions, to encourage them and monitor them. | EMA and Text messages |
| [31] | Daily questions about recent emotional events (e.g., emotions, scenario, somatic symptoms, automatic thoughts) + answers on demand by the participant | Skills entries and satisfaction with the treatment. | P and T | P: They received personalized feedback from therapists.T: Information and graphs from the portal about patients’ progress were discussed in weekly CBT sessions with the patients. | Smartphone app: SmartCAT app + SmartCAT therapist portal.. |
| [32] | Online before every session | STIC: set of questionnaires | T and clinicians stakeholders | T: On-demand graphs of patient progress were provided to the therapist through STIC | STIC online |
| [33] | Once daily mood monitoring messages at random between 8 a.m. and 8 p.m. | Attendance to therapy, duration of therapy and PHQ-9 | P and T | P: They received feedback about their mood responsesT: T reviewed information from an online dashboard were patient progress is shown. T can periodically review the graphs, identify key aspects and address any important event during or between sessions. | Automated text messages and Web-based platform (HealthySMS) |
| [34] | Daily and weekly surveys (between 5 p.m. and 10:30 p.m.) | Mood, medication use, socialization and conflict | P and T | P: They discussed their feedback with the T at every session.T: They reviewed and discussed patient information (plots of symptoms over time, etc.) on the dashboard with P during sessions and between sessions. | Smartphone app: RealLife Exp + web-based platform |
| [35] | Once daily call (HealthCall) for self- monitoring | Primary drug use (frequency and amount), use of other drugs, medication adherence, and mood | P and T | P: They received the feedback at 30 and 60 days, where their information was discussed with the T.T: At 30 and 60 days, T discussed with P the generated graphs based on HealthCall about their drug use, moods and health behaviors. | Phone IVR system |
| [36] | Daily surveys (at 5 p.m. until 11:55 p.m.), weekly surveys (Sundays at 10 a.m. until Monday 11:55) and monthly in-person psychosocial assessments with research staff | Daily surveys assessing mood, medication adherence, and social interaction, weekly surveys assessing symptoms, sleep, and medication adherence | T | T: They received alerts from the dashboard when P scores were clinically significant and took the proper decisions according to the patient demand. | Ginger.io (software) = Smartphone app + Clinician dashboard |
| [37] | 3/4 times daily, weekly; 8/12 weeks | PHQ-9 and GAD-7 | P and T | P: P received notifications about their progress in the app, becoming more aware of their symptoms.T: T reviewed patient-reported information via an online dashboard and visualized patient progress graphs. | Smartphone app + online platform |
| [38] | Session 1 and 2: 10 daily evening EMA for 6 days. Session 3 and 4: 8 evening daily EMA (monitor changes in voices and coping strategies) | SEPS, PSYRATS-AH, and DASS-21 | P and T | P: In session 2, P received a summary sheet with their EMA progress.T: In session 2, EMA feedback was discussed with the P in order to guarantee understanding, detect predictors and avoid causation. | Smartphone app: MovisensXS + web-based platform |
| [39] | Session 1 and 2: 10 daily evening EMA for 6 days. Session 3 and 4: 8 evening daily EMA (monitor changes in voices and coping strategies) | SEPS, PSYRATS-AH, and DASS-21 | P and T | P: In session 2, P received a summary sheet with their EMA progress.T: In session 2, EMA feedback was discussed with the P in order to guarantee understanding, detect predictors and avoid causation. | Smartphone app: RealLife Exp + web-based platform |
| [40] | Daily self-reported measures of well-being | Well-being (WHO-5) | P and T | P: They received routinely individualized information about their progress in group discussion with the therapist.T: T received daily automatic plots of each patient’s outcomes within trajectories. | Touch-screen technology in therapy rooms |
| [41] | Weekly (session-by-session) | PHQ-9 and GAD-7 | P and T | P: They received their feedback in session with the therapist, where the information was reviewed, discussed and used to guide the treatment plan.T: They had access to patient progress graphs and response curves from the monitoring system, and they were warned automatically when a P was not-on-track. | Computer PCMIS |
| [42] | Weekly (session-by-session) | PHQ-9 and GAD-7 | P and T | P: They received their feedback in session with the therapist, where the information was reviewed, discussed and used to guide the treatment plan.T: They had access to patient progress graphs and response curves from the monitoring system, and they were warned automatically when a P was not-on-track. | Computer PCMIS |
| [43] | Twice a day (only during psychoeducation sessions) and once a week | Daily: mood and sleepWeekly: QIDS, ASRM and mood management strategies questionnaire | P and T | P: P received their feedback at every session with the T.T: T reviewed patient progress from daily mood rating and weekly scales from the previous week and discussed with the P the relationship between his/her mood changes and stressors. | Phone text messages or e-mails (True Colours mood monitoring system) |
| [44] | Daily process monitoring (during evenings). | TPQ | T | T: On demand. Feedback was used for individualizing therapeutic decisions. | SNS |
| [45] | Daily measures of psychotherapy process. Weekly measure of therapy outcome. | IEQ daily, weekly SCL-90 (Bulimia) | P, T and researchers | P: They viewed their progress and estimated their moods and symptoms during the past day.T: They had access to P data from the system in order to adapt the intervention delivered. | Smartphone: DynAMo web app |
| [46] | Daily monitoring | Sleep patterns, physical activity, and activities of daily living | P, T and caregivers | P and caregiver: They could see a proportionate share of the information adapted to their needs.T: Information collected was available at all times in order to design personalized interventions. | Tablet app (assistive technology: wearable, sleep, movement, presence sensors) |
| [47] | Once a week just before therapy session (at waiting room) | OQ-45 | P and T, or only T | P: P can access the feedback via email or into their portal system.T: T could access the feedback via email or in their portal system and could discuss the feedback information (progress charts and a message) with the P based on the OQ-45 patient’s scores. | Computer: Web-based monitoring app |
| Reference | Sample Size | Feasibility of Technology | Clinical Effectiveness |
|---|---|---|---|
| [30] | 27 Tx | Monthly: 92.7% | NA |
| [31] | 9 Tx | Completion rate was 82.8%. Patients reported the app being easy to use. All parents report treatment satisfaction and would recommend the program. | NA |
| [33] | 85 (40 cont. + 45 Tx) | NA | Technology-supported MBC significantly increased treatment adherence (median of 13.5 weeks before dropping out) compared to traditional CBT (median of 3 weeks before dropping out). Effect sizes of technology-supported MBC CBT on depressive symptoms’ severity (z = −5.80) were larger than for traditional CBT (z = −3.12), but differences were not significant |
| [34] | 61 Tx | Moderate survey completion (daily = 40%; weekly = 39%). In general, both T (66%) and P (85%) reported they would continue using the app as part of the treatment. | NA |
| [35] | 240 (83 cont. + 77 Tx + 80 Tx) | HealthCall shows a great retention rate and response rate (64.1%), supporting feasibility, patient acceptability and generalizability. | At 12-month follow-up, reductions in non-injection drug use were comparable in traditional and technology-supported MBC motivational interviewing and superior than in the control condition. In the subset of patients with drug dependence, drug use was significantly lower in the technology-supported MBC condition at 12 months post-treatment. At 60 days, treatment retention in the technology-supported MBC group (88.8%) was superior than in the motivational intervention only condition (81.8%) and the control condition (78.3%) |
| [36] | 76 Tx | Feasibility and acceptability of the smartphone app as an adjunct treatment tool is supported by the high response rate sate (weekly surveys: 77%; daily surveys: 69%) | NA |
| [37] | 17 Tx | The feasibility and acceptability of the mobile platform is supported by the high early response rate (weekly = 88%). | NA |
| [38] | 34 (17 cont. + 17 Tx) | High completion rates (74%) of EMA questionnaires and good satisfaction of participants support the feasibility and acceptability of the study, respectively. | Compared with the usual treatment, the technology-supported MBC treatment resulted in large improvements in confidence in coping with voices (Hedges g = 1.45) and medium improvements in understanding of voices (Hedges g = 0.61) and in psychotic symptoms (Hedges g = 0.51). Both groups showed similar changes in the impact of psychosis. |
| [40] | 1308 (408 Tx Fb +, 439 nFb + 461 cont.) | High rates of touch-screen questionnaire completion (over 90%). | Technology-supported MBC for NOT patients was more effective than traditional CBT or monitoring without feedback in reducing depressive symptoms and the impact of emotions on functioning, as well as on increasing vitality. By contrast, changes in well-being, anxiety, and stress were comparable across conditions. |
| [41] | 594 (349 cont. + 245 Tx) | MBC technology was generally acceptable and feasible to integrate in routine practice. | Technology-supported MBC achieved comparable reductions in depression and anxiety compared to controls, but with significantly less time (adjusted mean = 10.25, SE = 0.45 vs. adjusted mean = 6.59, SE = 0.51) and cost (between £65.88 and £129.20 cost reductions per treatment). Cases in the control condition were twice as likely to become not-on-track patients compared to those in the technology-supported MBC. |
| [42] | 2233 (1057 cont. + 1176 Tx) | NA | NOT patients in the technology-enhanced MBC condition obtained significantly larger reductions in depressive (d = 0.23) and anxiety symptom severity (d = 0.19), as well as improved work and social adjustment (d = 0.19) compared with active controls (traditional CBT). |
| [43] | 19 Tx | High response rate (daily = 81%, weekly = 88%) | NA |
| [44] | 151 Tx | High average compliance rates (78.3%) and low average missing data rates (13%) amongst the inpatients support the feasibility. | NA |
| [47] | 475 (159 Tx FbT; 172 Tx FbTP; 144 cont. nFb) | NA | In short-term interventions (less than 35 weeks), receiving feedback was protective of negative outcomes in NOT cases (d = 1.28). No significant differences between conditions were found for on-track patients, but there was a trend for the technology-supported MBC group to be more effective (d = 0.24 at 35 weeks and d = 0.29 at 78 weeks) and to have lower deterioration rates (z = 1.3), especially when feedback was provided to both patient and therapist. |
| [32] | [39] | [45] | [46] | |
|---|---|---|---|---|
| 1. Was the study question or objective clearly stated? | Yes | Yes | Yes | Yes |
| 2. Was the study population clearly and fully described, including a case definition? | No | Yes | No | Yes |
| 3. Were the cases consecutive? | NA | NA | NA | No |
| 4. Were the subjects comparable? | NA | NA | No | Yes |
| 5. Was the intervention clearly described? | Yes | Yes | Yes | Yes |
| 6. Were the outcome measures clearly defined, valid, reliable, and implemented consistently across all study participants? | Yes | Yes | Yes | Yes |
| 7. Was the length of follow-up adequate? | NR | No | No | NR |
| 8. Were the statistical methods well-described? | Yes | Yes | Yes | Yes |
| 9. Were the results well-described? | Yes | Yes | Yes | Yes |
| Total score (maximum 9 points) | 5 | 6 | 5 | 7 |
| [41] | [43] | |
|---|---|---|
| 1. Was the study question or objective clearly stated? | Yes | Yes |
| 2. Were eligibility/selection criteria for the study population prespecified and clearly described? | Yes | Yes |
| 3. Were the participants in the study representative of those who would be eligible for the test/service/intervention in the general or clinical population of interest? | NR | Yes |
| 4. Were all eligible participants that met the prespecified entry criteria enrolled? | NR | No |
| 5. Was the sample size sufficiently large to provide confidence in the findings? | Yes | No |
| 6. Was the test/service/intervention clearly described and delivered consistently across the study population? | Yes | Yes |
| 7. Were the outcome measures prespecified, clearly defined, valid, reliable, and assessed consistently across all study participants? | Yes | Yes |
| 8. Were the people assessing the outcomes blinded to the participants’ exposures/interventions? | No | NA |
| 9. Was the loss to follow-up after baseline 20% or less? Were those lost to follow-up accounted for in the analysis? | Yes/Yes | Yes/Yes |
| 10. Did the statistical methods examine changes in outcome measures from before to after the intervention? Were statistical tests done that provided p values for the pre-to-post changes? | Yes | Yes |
| 11. Were outcome measures of interest taken multiple times before the intervention and multiple times after the intervention (i.e., did they use an interrupted time-series design)? | Yes | Yes |
| 12. If the intervention was conducted at a group level (e.g., a whole hospital, a community, etc.) did the statistical analysis take into account the use of individual-level data to determine effects at the group level? | Yes | Yes |
| Total score (maximum 12 points) | 9 | 9 |
| [30] | [31] | [34] | [36] | [37] | [44] | |
|---|---|---|---|---|---|---|
| 1. Was the research question or objective in this paper clearly stated? | Yes | Yes | Yes | Yes | Yes | Yes |
| 2. Was the study population clearly specified and defined? | Yes | Yes | Yes | Yes | Yes | Yes |
| 3. Was the participation rate of eligible persons at least 50%? | NR | NR | Yes | Yes | No | NR |
| 4. Were all the subjects selected or recruited from the same or similar populations? Were inclusion and exclusion criteria for being in the study prespecified and applied uniformly to all participants? | Yes | Yes | Yes | Yes | Yes | Yes |
| 5. Was a sample size justification, power description, or variance and effect estimates provided? | NR | NR | NR | NR | NR | NR |
| 6. For the analyses in this paper, were the exposure(s) of interest measured prior to the outcome(s) being measured? | Yes | Yes | Yes | NA | Yes | Yes |
| 7. Was the timeframe sufficient so that one could reasonably expect to see an association between exposure and outcome if it existed? | NA | NA | NA | NA | NA | NA |
| 8. For exposures that can vary in amount or level, did the study examine different levels of the exposure as related to the outcome (e.g., categories of exposure, or exposure measured as continuous variable)? | NA | NA | NA | NA | NA | NA |
| 9. Were the exposure measures clearly defined, valid, reliable, and implemented consistently across all study participants? | Yes | Yes | Yes | Yes | Yes | Yes |
| 10. Was the exposure(s) assessed more than once over time? | Yes | Yes | Yes | Yes | Yes | Yes |
| 11. Were the outcome measures clearly defined, valid, reliable, and implemented consistently across all study participants? | Yes | Yes | Yes | Yes | Yes | Yes |
| 12. Were the outcome assessors blinded to the exposure status of participants? | NA | NA | NA | NA | NA | NA |
| 13. Was loss to follow-up after baseline 20% or less? | Yes | Yes | No | No | No | No |
| 14. Were key potential confounding variables measured for their impact on the relationship between exposure(s) and outcome(s)? | NA | NA | NA | NA | NA | NA |
| Total score (maximum 14 points) | 8 | 8 | 8 | 7 | 7 | 7 |
| [33] | [35] | [38] | [40] | [42] | [47] | |
|---|---|---|---|---|---|---|
| 1. Was the study described as randomized, a randomized trial, a randomized clinical trial, or an RCT? | No | Yes | Yes | No | Yes | Yes |
| 2. Was the method of randomization adequate (i.e., use of randomly generated assignment)? | NA | Yes | Yes | NA | Yes | Yes |
| 3. Was the treatment allocation concealed (so that assignments could not be predicted)? | NA | Yes | Yes | NA | Yes | Yes |
| 4. Were study participants and providers blinded to treatment group assignment? | No | No | No | No | No | No |
| 5. Were the people assessing the outcomes blinded to the participants’ group assignments? | No | NA | Yes | No | No | NA |
| 6. Were the groups similar at baseline on important characteristics that could affect outcomes (e.g., demographics, risk factors, co-morbid conditions)? | Yes | Yes | Yes | Yes | Yes | No |
| 7. Was the overall drop-out rate from the study at endpoint 20% or lower of the number allocated to treatment? | Yes | Yes | Yes | NR | No | No |
| 8. Was the differential drop-out rate (between treatment groups) at endpoint 15 percentage points or lower? | Yes | Yes | Yes | NR | Yes | Yes |
| 9. Was there high adherence to the intervention protocols for each treatment group? | Yes | Yes | Yes | NR | Yes | Yes |
| 10. Were other interventions avoided or similar in the groups (e.g., similar background treatments)? | Yes | NR | Yes | NR | Yes | NR |
| 11. Were outcomes assessed using valid and reliable measures, implemented consistently across all study participants? | Yes | Yes | Yes | No | Yes | Yes |
| 12. Did the authors report that the sample size was sufficiently large to be able to detect a difference in the main outcome between groups with at least 80% power? | No | Yes | No | NR | Yes | Yes |
| 13. Were outcomes reported or subgroups analyzed prespecified (i.e., identified before analyses were conducted)? | Yes | Yes | Yes | Yes | Yes | Yes |
| 14. Were all randomized participants analyzed in the group to which they were originally assigned, i.e., did they use an intention-to-treat analysis? | Yes | No | Yes | NR | Yes | Yes |
| Total score (maximum 14 points) | 8 | 10 | 12 | 2 | 11 | 9 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gual-Montolio, P.; Martínez-Borba, V.; Bretón-López, J.M.; Osma, J.; Suso-Ribera, C. How Are Information and Communication Technologies Supporting Routine Outcome Monitoring and Measurement-Based Care in Psychotherapy? A Systematic Review. Int. J. Environ. Res. Public Health 2020, 17, 3170. https://doi.org/10.3390/ijerph17093170
Gual-Montolio P, Martínez-Borba V, Bretón-López JM, Osma J, Suso-Ribera C. How Are Information and Communication Technologies Supporting Routine Outcome Monitoring and Measurement-Based Care in Psychotherapy? A Systematic Review. International Journal of Environmental Research and Public Health. 2020; 17(9):3170. https://doi.org/10.3390/ijerph17093170
Chicago/Turabian StyleGual-Montolio, Patricia, Verónica Martínez-Borba, Juana María Bretón-López, Jorge Osma, and Carlos Suso-Ribera. 2020. "How Are Information and Communication Technologies Supporting Routine Outcome Monitoring and Measurement-Based Care in Psychotherapy? A Systematic Review" International Journal of Environmental Research and Public Health 17, no. 9: 3170. https://doi.org/10.3390/ijerph17093170
APA StyleGual-Montolio, P., Martínez-Borba, V., Bretón-López, J. M., Osma, J., & Suso-Ribera, C. (2020). How Are Information and Communication Technologies Supporting Routine Outcome Monitoring and Measurement-Based Care in Psychotherapy? A Systematic Review. International Journal of Environmental Research and Public Health, 17(9), 3170. https://doi.org/10.3390/ijerph17093170







