The Severe Acute Respiratory Syndrome Coronavirus-2 (SARS CoV-2) in Dentistry. Management of Biological Risk in Dental Practice
Abstract
1. Introduction
1.1. Epidemiology
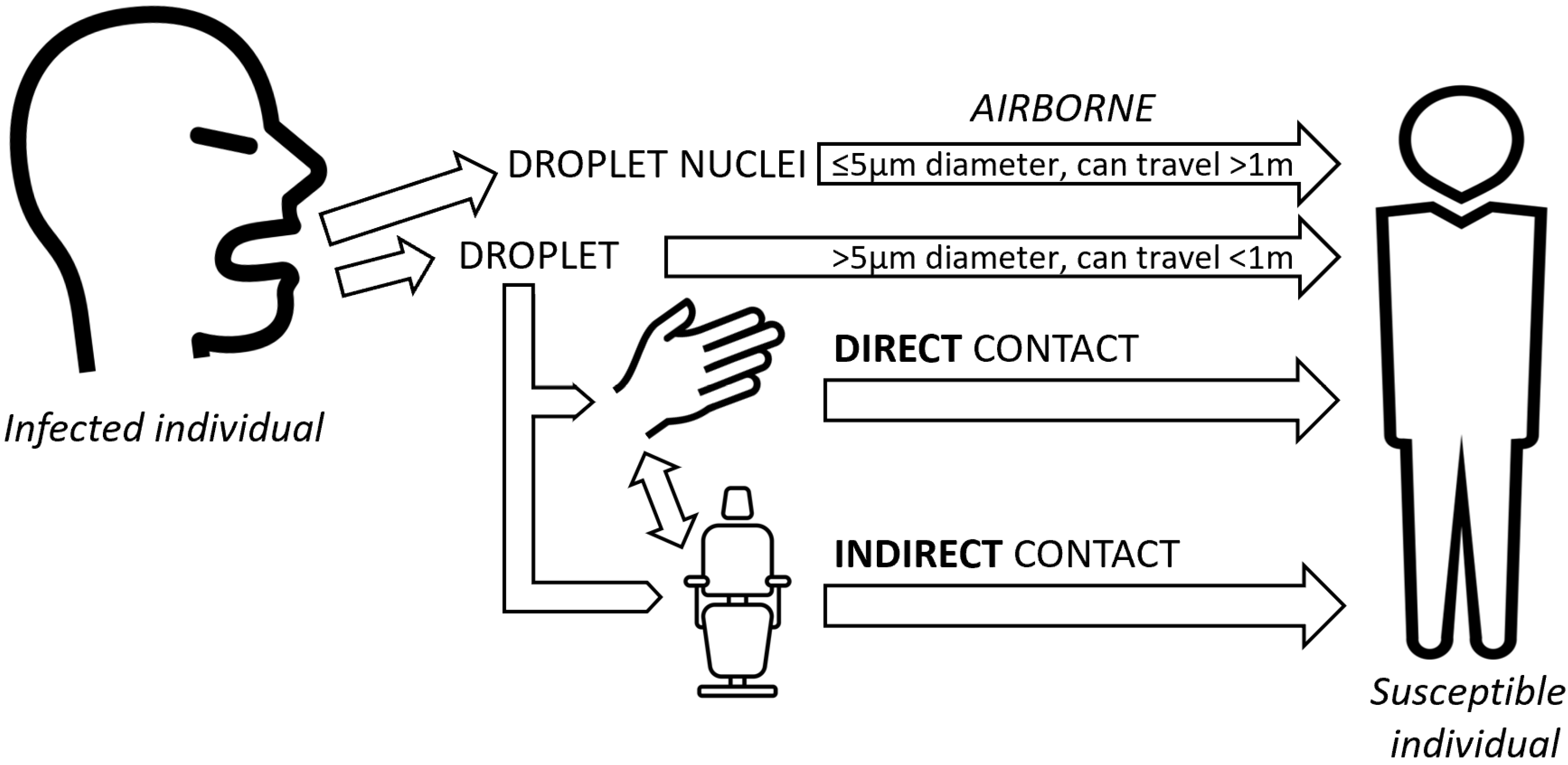
1.2. Route of Transmission
1.3. Clinical Classification
1.4. Differential Diagnosis
2. Infection Risk in Dental Practice
- The use of personal protective equipment (PPE) such as gloves, masks, visors, goggles, dental uniform, and surgical gown and shoes (see section on PPEs below).
- A set of decontamination, disinfection, and sterilization procedures aimed at inactivating, destroying, or removing pathogens from any surface or instruments [12].
3. Hygiene Measures among Dental Practice Professionals
3.1. Generic Measures
- Inform patients of the procedures for accessing the dental office.
- Inform the patient that a telephone triage will be administered and any suspicious case will be reported to competent health authorities for further investigation.
- Carry out a preliminary telephone triage upon patient access to the office in order to assess whether:
- The patient who is entering the office has symptoms of SARS-CoV-2 infection;
- Has come into contact with potentially infected people;
- Has been in areas with high risk of infection (Figure 2).
- Only schedule an appointment in the dental office if the patient cannot be deferred or in urgent cases and according to the equipment and disposable materials available.
- Assess the actual need for dental intervention before planning visits of the most vulnerable subjects (elderly or patients with respiratory, cardiovascular, or immune system diseases, etc.). Where appropriate, postpone visits [14].
- Avoid crowding by spreading appointments over time, maintaining distance in the waiting room and/or in the operating rooms (minimum safety distance of 2 m with a stay of less than 15 min) [4].
- Arrange entry into the operating rooms of individual patients and a single companion for minors, without overcoats, electronic devices, and bags, which must be left in the waiting room. In the event that personal effects should enter the operating rooms, these objects must be placed in special sealed bags.
- Ensure that hand sanitizer is available to patients and companions, possibly at the entrance of the practice or anywhere before entering the operating rooms.
- In the patient’s medical history, record the results of the telephone triage regarding the presence of suspicious and actual symptoms, potential contact with people who have been to risk areas, and the patient’s own transit/permanence in risk areas (Figure 2).
- Remind the patient that, in case of necessity, it is mandatory to cough by covering their mouth and nose, possibly with a tissue. The tissue must be disposed of immediately in a special waste container. Following this, they must proceed to wash and disinfect hands.
- Always allow fresh air in between one patient and another, and frequently in the waiting room. This action could be performed by opening the windows, taking care of the air influx, or using medical-grade air purifiers as recommended by the manufacturer.
- Consider all material that comes into direct or indirect contact with the patient and all material that has been used for patient treatment or has come in contact with any biological fluid as special waste. Manage it according to the proper disposal techniques to ensure that any infectious materials cannot contaminate or spread to other areas.
- Always use PPE. The PPE should be used as described by the instructions contained in the user manual and must be disposed of as special waste. Always check the integrity of the PPE, and, in the event of an integrity breach, eliminate PPE directly.
- Use a medical cap.
- Expose forearms (bare below the elbows);
- Remove all hand and wrist jewelry;
- Ensure fingernails are clean and short. Artificial nails or nail products are not recommended;
- Cover all cuts or abrasions with a waterproof dressing.
- Remove potentially contaminating objects from waiting rooms and operating rooms (magazines, etc.).
- Regularly sanitize common and operational areas, non-medical furnishings and equipment, and surfaces accessible to the public (handles, etc.).
- Place protections on points of sale (POSs), keyboards, etc. and change them after each use. A single-use protection could be a disposable barrier (plastic film or cover) that must be replaced after every use.
- Arrange the use of respiratory protective devices (RPDs) for all staff including secretarial staff (see section on PPEs below).
- Inform doctors and collaborators concerning the clinical triage for COVID-19 and train them to evaluate themselves. If they have manifested symptoms of a coronavirus infection (cough, cold, diarrhea, flu symptoms, temperature >37.5 °C) in the last 14 days, they should not come into the dental office and should report themselves to the competent health authorities [9].
- Suggest intensifying personal hygiene procedures at the end of the work shift.
3.2. Specific Measures
3.2.1. Precautions in Operative Areas
- Protect the surfaces of all equipment and instruments with single-use disposable barriers, and dispose of the protections among the special waste after use.
- Arrange only strictly necessary material on the surfaces of operating areas.
- Clean the operative surfaces with hydroalcoholic disinfectants at concentrations above 60%.
- Wear a uniform with long sleeves and shoes, and avoid exposed body parts.
- Wear a disposable lab coat/overcoat.
- It is also suggested that the patient mouth-rinse for 30 s with a 1% solution of hydrogen peroxide (1 part at 10-volume/3% hydrogen peroxide and 2 parts of water) or with 1% iodopovidone. This pre-operative treatment could lower the virus concentration in the patient’s mouth [3].
- Give preference to extra-oral radiological examinations over intra-oral ones to avoid the stimulation of coughing or vomiting [15].
3.2.2. Precautions from Procedures that Produce Droplets or Aerosol
- Replace and sterilize the high- and low-speed hand-pieces after each use between one patient and the next; the use of 3-way turbines and dental units equipped with valves and anti-reflux systems is recommended [8].
4. Personal Protective Equipment
4.1. Respiratory Protective Devices
4.1.1. Indications
- Wear a surgical mask in all eventualities where there is contact between the patient and other people less than 2 m away and for more than 15 min.
- Wear an FFP2 or FFP3 mask in procedures with a risk of aerosol droplet production. If not available, use a surgical mask with a face shield [3].
- Remove the mask after each aerosol risk procedure by touching only the strings.
4.1.2. Common Mistakes
- Removing the mask by touching the possibly contaminated surface. The correct procedure is as follows: After removing the gloves, put on a new pair of gloves, and remove the mask by the strings.
4.2. Gloves
4.2.1. Indications
- Disposable gloves must be used in all operating phases that involve contact with potentially infected surfaces and for direct patient assistance.
- Gloves should be inspected before use.
- A double pair of gloves can serve as additional protection.
- Before putting on gloves, cover any cuts or damaged portions of hand skin as an additional precaution.
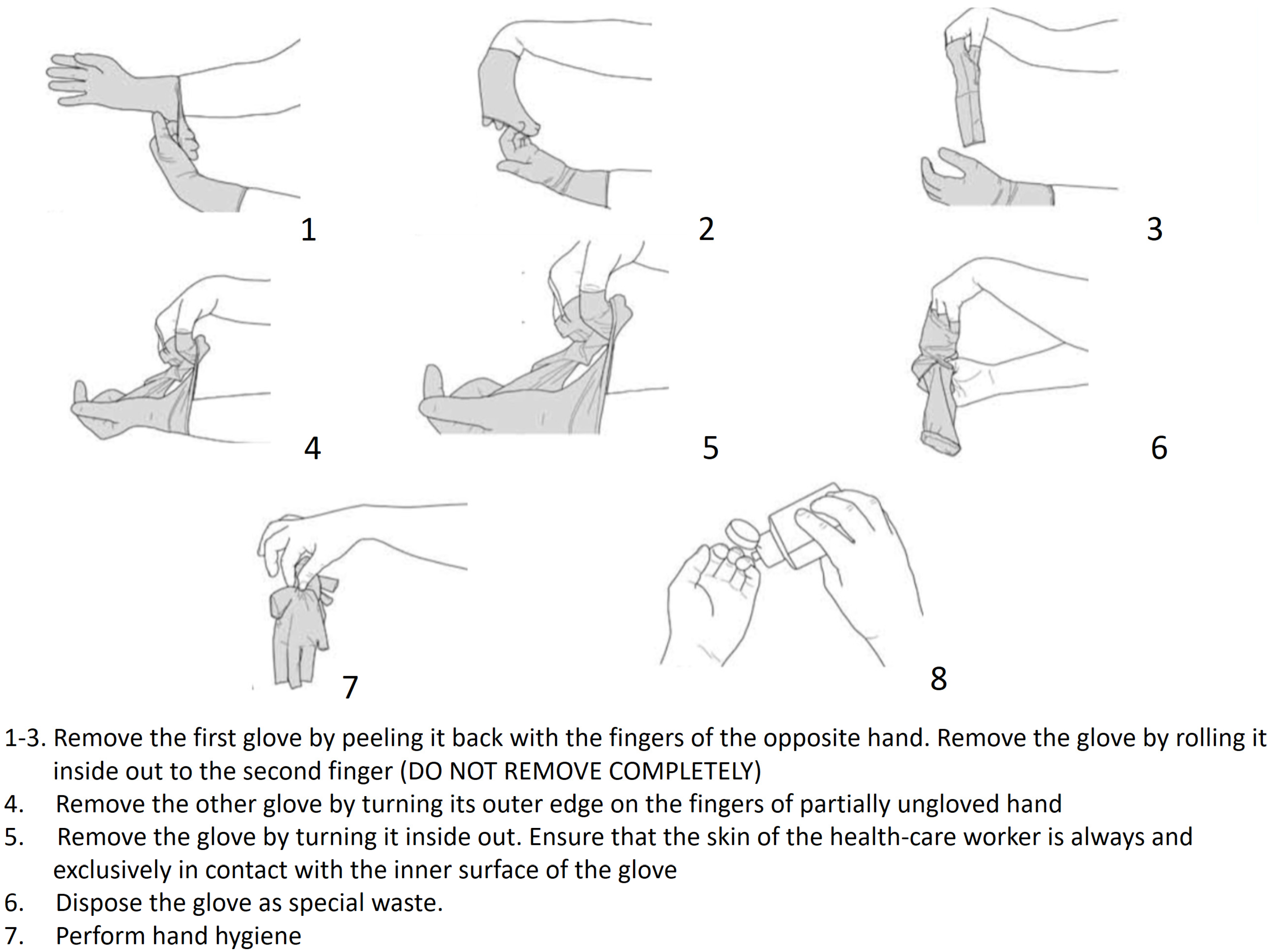
- After use, gloves should be removed using appropriate techniques to prevent hand contamination. Gloves should be removed by rolling from the wrist towards the fingers to avoid contact with skin. It is necessary to remove gloves by touching only the external part (Figure 6).
- Use sterile gloves for invasive procedures that require surgical asepsis.
4.2.2. Common Mistakes
- Using the same pair of gloves for different operations and/or for different patients.
- Not washing hands before and after using gloves.
4.3. Face and Eye Protection
4.3.1. Indications
- Eyes should be protected with goggles or a full-face shield in all procedures at risk of aerosol/droplet production.
- Glasses, visors, or face shields can be used.
- After every operation, depending on the kind of procedure, protections must be disposed of or sterilized.
4.3.2. Common Mistakes
- Only using common prescription glasses.
- Only using medical loupes.
- Removing protections after each procedure by touching the external surface. Strings must be used for removal.
4.4. Dental Uniform/Surgical Gown
4.4.1. Indications
- Always use a uniform with long sleeves and shoes.
- Change the uniform every day.
- Before washing, disinfect with a chlorine solution (500 mg/L) for 30 s [18].
- Wear a surgical gown (over the uniform) for each procedure at risk of contamination with aerosol/droplets.
- Dispose of the surgical gown after each visit. Remove the surgical gown before glove removal and touch it only from the outside.
- Remove the surgical gown by folding it with the potentially contaminated external surface inside.
- In case of contamination, replace the dental uniform as soon as possible.
4.4.2. Common Mistakes
- Applying standard precautions when handling and replacing clothing.
- Replacing the surgical gown after glove removal.
- Removing the dental uniform without a new pair of gloves.
4.5. Recommended Sequence of PPE Removal
- Remove any overcoat.
- Remove the gloves by rolling them up from the wrist, without touching the skin.
- Wash hands.
- Wear a new pair of gloves to avoid accidental contact.
- Remove the protective goggles or visor and mask, taking care to touch only the strings and not the contaminated surface.
- Remove the gloves.
- Wash hands.
5. Discussion
6. Conclusions
Funding
Conflicts of Interest
References
- Peng, X.; Xu, X.; Li, Y.; Cheng, L.; Zhou, X.; Ren, B. Transmission routes of 2019-nCoV and controls in dental practice. Int. J. Oral Sci. 2020, 12, 9. [Google Scholar] [CrossRef] [PubMed]
- Guo, Y.-R.; Cao, Q.-D.; Hong, Z.-S.; Tan, Y.-Y.; Chen, S.-D.; Jin, H.-J.; Tan, K.-S.; Wang, D.-Y.; Yan, Y. The origin, transmission and clinical therapies on coronavirus disease 2019 (COVID-19) outbreak—An update on the status. Mil. Med. Res. 2020, 7, 1–10. [Google Scholar] [CrossRef] [PubMed]
- WHO.int. 2020. Coronavirus Situation Report-83. Available online: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/situation-reports/> (accessed on 22 April 2020).
- Otter, J.A.; Donskey, C.; Yezli, S.; Douthwaite, S.; Goldenberg, S.D.; Weber, D.J. Transmission of SARS and MERS coronaviruses and influenza virus in healthcare settings: The possible role of dry surface contamination. J. Hosp. Infect. 2016, 92, 235–250. [Google Scholar] [CrossRef] [PubMed]
- Chan, J.F.-W.; Yuan, S.; Kok, K.-H.; To, K.K.-W.; Chu, H.; Yang, J.; Xing, F.; BNurs, J.L.; Yip, C.C.-Y.; Poon, R.W.-S.; et al. A familial cluster of pneumonia associated with the 2019 novel coronavirus indicating person-to-person transmission: A study of a family cluster. Lancet 2020, 395, 514–523. [Google Scholar] [CrossRef]
- Rothe, C.; Schunk, M.; Sothmann, P.; Bretzel, G.; Froeschl, G.; Wallrauch, C.; Zimmer, T.; Thiel, V.; Janke, C.; Guggemos, W.; et al. Transmission of 2019-NCOV infection from an asymptomatic contact in Germany. N. Engl. J. Med. 2020, 382, 970–971. [Google Scholar] [CrossRef] [PubMed]
- Backer, J.A.; Klinkenberg, D.; Wallinga, J. Incubation period of 2019 novel coronavirus (2019-nCoV) infections among travellers from Wuhan, China, 20–28 January. Eurosurveill 2020, 25. [Google Scholar] [CrossRef] [PubMed]
- Meng, L.; Hua, F.; Bian, Z. Coronavirus Disease 2019 (COVID-19): Emerging and Future Challenges for Dental and Oral Medicine. J. Dent. Res. 2020, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Chen, N.; Zhou, M.; Dong, X.; Qu, J.; Gong, F.; Han, Y.; Qiu, Y.; Wang, J.; Liu, Y.; Wei, Y.; et al. Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: A descriptive study. Lancet 2020, 395, 507–513. [Google Scholar] [CrossRef]
- National Health Commission of the People’s Republic of China. Chinese Clinical Guidance for COVID-19 Pneumonia Diagnosis and Treatment, 7th ed.; China National Health Commission: Beijing, China, 2020; Available online: http://kjfy.meetingchina.org/msite/news/show/cn/3337.html (accessed on 24 March 2020).
- Cascella, M.; Rajnik, M.; Cuomo, A.; Dulebohn, S.C.; Di Napoli, R. Features, evaluation and treatment coronavirus (COVID-19). In Treasure Island (FL); StatPearls Publishing: Tampa, FL, USA, 2020. [Google Scholar]
- Spagnuolo, G.; De Vito, D.; Rengo, S.; Tatullo, M. COVID-19 outbreak: An overview on dentistry. Int. J. Environ. Res. Public Health 2020, 17. [Google Scholar] [CrossRef] [PubMed]
- Xu, K.; Lai, X.; Liu, Z. Suggestions on the prevention of COVID-19 for health care workers in department of otorhinolaryngology head and neck surgery. World J. Otorhinolaryngol. Head Neck Surg. 2020. [Google Scholar] [CrossRef] [PubMed]
- Cascella, M.; Rajnik, M.; Cuomo, A.; Dulebohn, S.C.; Di Napoli, R. Features, Evaluation and Treatment Coronavirus (COVID-19); StatPearl Publishing: Tampa, FL, USA, 2020. [Google Scholar]
- Vandenberghe, B.; Jacobs, R.; Bosmans, H. Modern dental imaging: A review of the current technology and clinical applications in dental practice. Eur. Radiol. 2010, 20, 2637–2655. [Google Scholar] [CrossRef] [PubMed]
- ECDC TECHNICAL REPORT Infection Prevention and Control for COVID-19 in Healthcare Settings March. Available online: https://www.ecdc.europa.eu/en/publications-data/infection-prevention-and-control-covid-19-healthcare-settings (accessed on 9 March 2020).
- Samaranayake, L.P.; Reid, J.; Evans, D. The efficacy of rubber dam isolation in reducing atmospheric bacterial contamination. ASDC J. Dent. Child. 1989, 56, 442–444. [Google Scholar] [PubMed]
- Li, Z.Y.; Meng, L.Y. The prevention and control of a new coronavirus infection in department of stomatology. Chin. J. Stomatol. 2020, 55, E001. [Google Scholar] [CrossRef]
- National Institute for Occupational Safety and Hygiene (NIOSH). NIOSH Guide to the Selection and Use of Particulate Respirators Certified under 42 CFR 84; National Institute for Occupational Safety and Hygiene (NIOSH): Cincinnati, OH, USA, 1996; (DHHS (NIOSH) Publication no. 96−101). [Google Scholar]
- Lee, S.-A.; Hwang, D.-C.; Li, H.-Y.; Tsai, C.-F.; Chen, C.-W.; Chen, J.-K. Particle size-selective assessment of protection of european standard FFP respirators and surgical masks against particles-tested with human subjects. J. Healthc. Eng. 2016, 2016, 12. [Google Scholar] [CrossRef] [PubMed]

© 2020 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lo Giudice, R. The Severe Acute Respiratory Syndrome Coronavirus-2 (SARS CoV-2) in Dentistry. Management of Biological Risk in Dental Practice. Int. J. Environ. Res. Public Health 2020, 17, 3067. https://doi.org/10.3390/ijerph17093067
Lo Giudice R. The Severe Acute Respiratory Syndrome Coronavirus-2 (SARS CoV-2) in Dentistry. Management of Biological Risk in Dental Practice. International Journal of Environmental Research and Public Health. 2020; 17(9):3067. https://doi.org/10.3390/ijerph17093067
Chicago/Turabian StyleLo Giudice, Roberto. 2020. "The Severe Acute Respiratory Syndrome Coronavirus-2 (SARS CoV-2) in Dentistry. Management of Biological Risk in Dental Practice" International Journal of Environmental Research and Public Health 17, no. 9: 3067. https://doi.org/10.3390/ijerph17093067
APA StyleLo Giudice, R. (2020). The Severe Acute Respiratory Syndrome Coronavirus-2 (SARS CoV-2) in Dentistry. Management of Biological Risk in Dental Practice. International Journal of Environmental Research and Public Health, 17(9), 3067. https://doi.org/10.3390/ijerph17093067




