A Review of Published Literature Regarding Health Issues of Coastal Communities in Sabah, Malaysia
Abstract
1. Introduction
2. Materials and Methods
2.1. Literature Search
2.2. Data Extraction
2.3. Quality Assessment
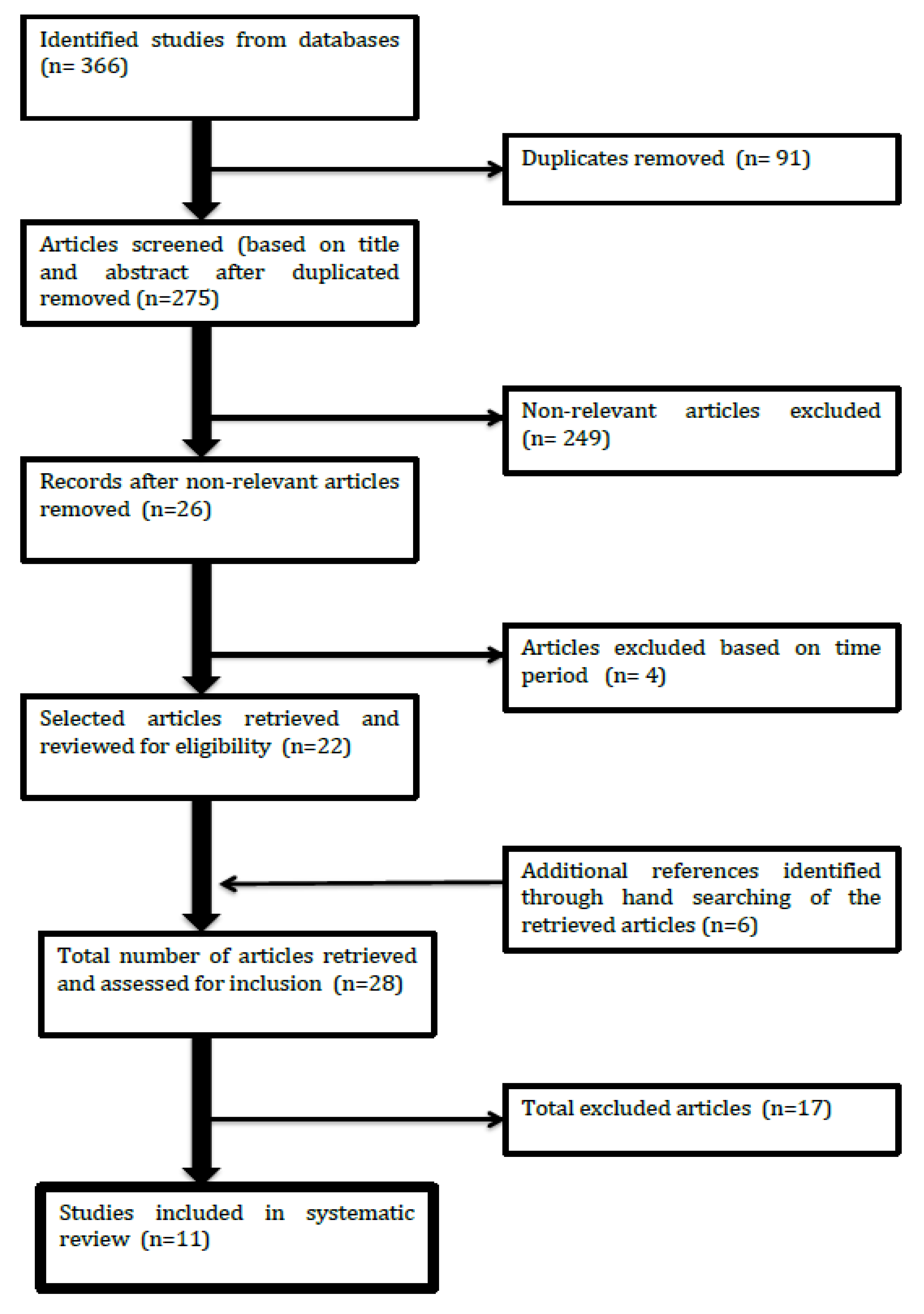
2.4. Flow of Study Selection
2.5. Ethics
3. Results
3.1. General Characteristics of the Included Articles for the Review
3.2. Health Status
3.2.1. Incidence, Distributions, Disease Characteristics, and Factors Associated with Malaria Infection
3.2.2. Demographic Characteristics, Knowledge, and Perceptions of Tuberculosis Patients
3.2.3. Incidence of Seafood Poisoning
3.2.4. Antenatal Problems Experienced by Pregnant Women in the Coastal Areas of Sabah
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Depledge, P.M.; Lovell, R.; Wheeler, B.; Morrissey, K.; White, M.; Fleming, L. Future of the sea: Health and wellbeing of coastal communities. Gov. Off. Sci. 2017. Available online: https://www.gov.uk/government/uploads/system/uploads/attachment_data/file/639432/Health_and_Wellbeing_Final.pdf (accessed on 24 June 2019).
- Cabral, H.; Fonseca, V.; Sousa, T.; Leal, M.C. Synergistic effects of climate change and marine pollution: An overlooked interaction in coastal and estuarine areas. Int. J. Environ. Res. Public Health 2019, 16, 2737. [Google Scholar] [CrossRef] [PubMed]
- Beckman, A.L.; Wilson, M.M.; Prabhu, V.; Soekoe, N.; Mata, H.; Grau, L.E. A qualitative view of the HIV epidemic in coastal Ecuador. PeerJ 2016, 4, e2726. [Google Scholar] [CrossRef]
- Abdullah, S. Coastal Developments in Malaysia—Scope, Issues and Challenges; Department of Irrigation and Drainage Malaysia: Kuala Lumpur, Malaysia, 1993; Volume 1, pp. 1–11. [Google Scholar]
- Bin Nordin, D.Y. Towards sustainable coastal planning and policies from a Malaysian perspective. WIT Trans. Ecol. Environ. 2006, 88, 45–54. [Google Scholar]
- Loi, H.K. Coastal Zone Management in Malaysia—The Need for an Integrated Approach; Department of Irrigation md Drainage Malaysia: Kuala Lumpur, Malaysia, 1994; Volume 1, p. 24. [Google Scholar]
- Tha, N.O.; Shoesmith, W.; Chrystalle, B.Y.T.; Ibrahim, M.Y. Accessibility of Health Care Utilization in Rural Areas of Sabah; Faculty of Medicine and Health Sciences, Universiti Malaysia Sabah: Kota Kinabalu, Malaysia, 2018; Volume 1, p. 1. [Google Scholar]
- Harris, H.; Ooi, Y.B.H.; Lee, J.; Matanjun, P. Non-communicable diseases among low income adults in rural coastal communities in Eastern Sabah, Malaysia. BMC Public Health 2019, 19 (Suppl. 4), 1–13. [Google Scholar] [CrossRef] [PubMed]
- Koiting, R.F.; Saleh, E.; Madin, J.; Ismail, M.N. Beach morphology changes during the northeast and southwest monsoons at Mantanani Besar Island, Sabah, Malaysia. J. Trop. Biol. Conserv. 2017, 14, 83–94. [Google Scholar]
- Department of Statistics Malaysia. Higher Household Income, Lower Poverty Rates; Department of Statistics Malaysia: Putrajaya, Malaysia, 2012.
- Allerton, C. Contested Statelessness in Sabah, Malaysia: Irregularity and the politics of recognition. J. Immigr. Refug. Stud. 2017, 15, 250–268. Available online: http://dx.doi.org/10.1080/15562948.2017.1283457 (accessed on 21 August 2019). [CrossRef]
- Knet, L.M.; Lee, R.C.; Cook, L.S. Standard Quality for Evaluating Primary Research Papers from a Variety of Fields; Health Technology Assessment Unit, Alberta Heritage Foundation for Medical Research: Alberta, AB, Canada, 2004; Volume 1, pp. 4–22. [Google Scholar]
- Grigg, M.J.; Cox, J.; William, T.; Jelip, J.; Fornace, K.M.; Brock, P.M.; von Seidlein, L.; Barber, B.E.; Anstey, N.M.; Yeo, T.W.; et al. Individual-level factors associated with the risk of acquiring human Plasmodium knowlesi malaria in Malaysia: A case-control study. Lancet Planet Health 2017, 1, e97–e104. Available online: http://dx.doi.org/10.1016/S2542-5196(17)30031-1 (accessed on 11 December 2018). [CrossRef]
- Lim, K.K.H.; Chan, Y.Y.; Teh, C.H.; Ismail, H.; Yusof, R.; Muhi, J.; Lim, K.K.H.; Foo, L.H. Iodine status among pregnant women in rural Sabah, Malaysia. Asia Pac. J. Clin. Nutr. 2017, 26, 861–866. Available online: http://www.ncbi.nlm.nih.gov/pubmed/28802296 (accessed on 19 March 2019).
- Suleiman, M.; Muhammad, J.; Jelip, J.; William, T.; Chua, T.H. An outbreak of tetrodotoxin poisoning from consuming horseshoe crabs in Sabah. Southeast Asian J. Trop. Med. Public Health 2017, 48, 197–203. [Google Scholar]
- Suleiman, M.; Jelip, J.; Rundi, C.; Chua, T.H. Case report: Paralytic shellfish poisoning in Sabah, Malaysia. Am. J. Trop. Med. Hyg. 2017, 97, 1731–1736. [Google Scholar] [CrossRef]
- Aye, T.T.; Ibrahim, D.M.Y.; Naing, D.K.S.; Myint, T.; Jical, M.H. Antenatal care practice and pregnancy outcome at Kudat area, Sabah, Northern Borneo. Asian J. Med. Biol. Res. 2017, 3, 31. Available online: http://www.banglajol.info/index.php/AJMBR/article/view/32033 (accessed on 17 December 2018). [CrossRef]
- Rundi, C. Understanding tuberculosis: Perspectives and experiences of the people of Sabah, East Malaysia. J. Health Popul. Nutr. 2010, 28, 114–123. [Google Scholar] [CrossRef] [PubMed]
- Barber, B.E.; William, T.; Dhararaj, P.; Anderios, F.; Grigg, M.J.; Yeo, T.W.; Anstey, N.M. Epidemiology of Plasmodium knowlesi malaria in north-east Sabah, Malaysia: Family clusters and wide age distribution. Malar. J. 2012, 11, 1–8. [Google Scholar] [CrossRef] [PubMed]
- William, T.; Jelip, J.; Menon, J.; Anderios, F.; Mohammad, R.; Awang Mohd, T.A.; Grigg, M.J.; Yeo, T.W.; Anstey, N.M.; Barber, B.E. Changing epidemiology of malaria in Sabah, Malaysia: Increasing incidence of Plasmodium knowlesi. Malar. J. 2014, 13, 1–11. Available online: http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L600192038%0Ahttp://dx.doi.org/10.1186/1475-2875-13-390 (accessed on 19 March 2019). [CrossRef]
- Fornace, K.M.; Abidin, T.R.; Alexander, N.; Brock, P.; Grigg, M.J.; Murphy, A.; William, T.; Menon, J.; Drakeley, C.J.; Cox, J. Association between landscape factors and spatial patterns of Plasmodium knowlesi infections in Sabah, Malaysia. Emerg. Infect. Dis. 2016, 22, 201–207. [Google Scholar] [CrossRef]
- Barber, B.E.; William, T.; Jikal, M.; Jilip, J.; Dhararaj, P.; Menon, J.; Yeo, T.W.; Anstey, N.M. Plasmodium knowlesi malaria in children. Emerg. Infect. Dis. 2011, 17, 814–820. [Google Scholar] [CrossRef]
- William, T.; Parameswaran, U.; Lee, W.K.; Yeo, T.W.; Anstey, N.M.; Ralph, A.P. Pulmonary tuberculosis in outpatients in Sabah, Malaysia: Advanced disease but low incidence of HIV co-infection. BMC Infect. Dis. 2015, 15, 1–9. [Google Scholar] [CrossRef]
- Ministry of Health Malaysia; World Health Organization; University of California. Eliminating Malaria: Case-Study 8 Progress towards Elimination in Malaysia; Ministry of Health Malaysia: Putrajaya, Malaysia, 2015.
- Brien, A.T.O.; Ramírez, J.F.; Martínez, S.P.; Chaves, Y.O.; Guimarães, A.; Luís, M.; Pereira, M.; Vinícius, M.; Lacerda GDe Grazziela, J.; Assis, O.; et al. Management guidelines of malaria in Malaysia. Vector Borne Dis. Sect. Dis. Control Div. Minist. Health 2013, 17, 1–59. [Google Scholar]
- Sanders, K.C.; Rundi, C.; Jelip, J.; Rashman, Y.; Gueye, C.S.; Gosling, R.D. Eliminating malaria in Malaysia: The role of partnerships between the public and commercial sectors in Sabah. Malar. J. 2014, 13, 1–12. [Google Scholar] [CrossRef]
- Joveen-Neoh, W.F.; Chong, K.L.; Wong, C.M.V.L.; Lau, T.Y. Incidence of malaria in the interior division of Sabah, Malaysian borneo, based on nested PCR. J. Parasitol. Res. 2011, 2011, 1–6. [Google Scholar] [CrossRef]
- Wong, M.L.; Chua, T.H.; Leong, C.S.; Khaw, L.T.; Fornace, K.; Wan-Sulaiman, W.-Y.; William, T.; Drakeley, C.; Ferguson, H.M.; Vythilingam, I. Seasonal and spatial dynamics of the primary vector of Plasmodium knowlesi within a major transmission focus in Sabah, Malaysia. PLoS Negl. Trop. Dis. 2015, 9. Available online: https://www.scopus.com/inward/record.uri?eid=2-s2.0-84955089020&doi=10.1371%2Fjournal.pntd.0004135&partnerID=40&md5=6d4604ec72e5d2703c8762b178e7fc10 (accessed on 19 March 2019). [CrossRef] [PubMed]
- World Health Organization. Expert Consultation on Plasmodium Knowlesi Malaria to Guide Malaria Elimination Strategies, Kota Kinabalu, Malaysia, 1–2 March 2017; WHO: Manila, Philippines, 2017. [Google Scholar]
- Ministry of health Malaysia. National Strategic Plan for Tuberculosis Control (2016–2020); Ministry of Health Malaysia: Putrajaya, Malaysia, 2011.
- Nissapatorn, V.; Lim, Y.A.L.; Jamaiah, I.; Man Chin, H.; Ilyana, M.Z.; Nonaziah, M.Z.; Siti Hasifah, A.; Kuppusamy, I. Tuberculosis in Malaysia: A continuing surge. Southeast Asian J. Trop. Med. Public Health 2007, 38, 231. Available online: http://www.tm.mahidol.ac.th/seameo/2007-38-suppl-1/38suppl1-231.pdf (accessed on 21 June 2019).
- Nantha, S. A Review of Tuberculosis Research in Malaysia. Med. J. Malays. 2014, 69, 88–102. [Google Scholar]
- Tajari, A.; Affendi, N. Illegal Immigrant and Security Crisis in Sabah, Malaysia. Int. Conf. Soc. Sci. Res. ICSSR 2015, 2015, 1–13. [Google Scholar]
- Liew, S.M.; Khoo, E.M.; Ho, B.K.; Lee, Y.K.; Mimi, O.; Fazlina, M.Y.; Asmah, R.; Lee, W.K.; Harmy, M.Y.; Chinna, K.; et al. Tuberculosis in Malaysia: Predictors of treatment outcomes in a national registry. Int. J. Tuberc. Lung Dis. 2015, 19, 764–771. [Google Scholar] [CrossRef]
- Occupational Health Unit, Disease Control Division. Management of Tuberculosis for Health Care Workers; Ministry of Health Malaysia: Putrajaya, Malaysia, 2012.
- Atif, M.; Sulaiman, S.A.S.; Shafie, A.A.; Babar, Z.U. Duration of treatment in pulmonary tuberculosis: Are international guidelines on the management of tuberculosis missing something? Public Health 2015, 129, 777–782. Available online: http://dx.doi.org/10.1016/j.puhe.2015.04.010 (accessed on 21 June 2019). [CrossRef]
- Shanmuganathan, R.; Subramaniam, I.D. Clinical, manifestation and risk factors of tuberculosis infection in Malaysia: Case study of a community clinic. Glob. J. Health Sci. 2015, 7, 110–120. [Google Scholar] [CrossRef]
- The Institution of Engineers Malaysia. Water Quality and Cleanliness of Beaches; The Institution of Engineers Malaysia: Petaling Jaya, Malaysia, 2008. [Google Scholar]
- Man, C.N.; Lajis, R.; Mohamad, S.; Centre, N.P. Tetrodotoxin (ttx) poisoning. Am. J. Emerg. Med. 2003, 21, 51–54. [Google Scholar]
- Lim, P.-T.; Usup, G.; Leaw, C.-P. Harmful algal blooms in Malaysian waters. Sains Malays. 2012, 41, 1509–1515. [Google Scholar]
- Mohammad-Noor, N.; Adam, A.; Lim, P.T.; Leaw, C.P.; Lau, W.L.S.; Liow, G.R.; Muhamad-Bunnori, N.; Hamdan, N.A.; Md-Nor, A.; Kemat, N.; et al. First report of paralytic shellfish poisoning (PSP) caused by Alexandrium tamiyavanichii in Kuantan port, Pahang, east coast of Malaysia. Phycol. Res. 2018, 66, 37–44. [Google Scholar] [CrossRef]
- Mobilik, J.M.; Ling, T.Y.; Lokman, M.; Husain, B.; Hassan, R. Type and quantity of marine debris at selected public beaches in Sabah (Tg. Aru & Kosuhoi) during different monsoon seasons. Borneo Sci. 2017, 38, 13–27. [Google Scholar]
- Ministry of Health Malaysia. National Health & Morbidity Suvey 2015; Ministry of Health Malaysia: Putrajaya, Malaysia, 2015.
- Kieny, M.P.; Bekedam, H.; Dovlo, D.; Fitzgerald, J.; Habicht, J.; Harrison, G.; Kluge, H.; Lin, V.; Menabde, N.; Mirza, Z.; et al. Strengthening health systems for universal health coverage and sustainable development. Bull. World Health Organ. 2017, 95, 537. [Google Scholar] [CrossRef] [PubMed]
| Health Status | Coastal | Community | Sabah |
|---|---|---|---|
| Health* ‘health status’ ‘health-status’ ‘health impact*’ ‘health-impact*’ ‘health implication*’ ‘health burden*’ ‘health-burden*’ ‘health-related’ ‘health-related outcome*’ ‘health related outcome*’ ‘health outcome*’ Illness* ‘related illness*’ Disease* ‘disease status’ ‘disease-status’ ‘disease impact*’ ‘disease-impact*’ ‘disease implication*’ ‘disease burden*’ ‘disease-burden*’ ‘disease-related’ ‘disease-related outcome*’ ‘disease related outcome*’ ‘disease outcome*’ ‘quality of life’ ‘quality adjusted life years’ ‘quality-adjusted life years’ ‘health related quality of life’ ‘health-related quality of life’ ‘value of life’ ‘morbid*’ ‘mortalit*’ ‘death’ ‘life expectanc*’ ‘life-expectanc*’ ‘surviv*’ ‘healthcare utili*’ ‘healthcare-utili*’ ‘healthcare admission*’ ‘healthcare-admission*’ ‘healthcare visit*’ ‘healthcare-visit*’ ‘healthcare us*’ ‘healthcare-us*’ | ‘coast*’ ‘fish*’ ‘beach*’ ‘gulf*’ ‘bay*’ ‘sea*’ ‘ocean*’ | ‘communit*’ ‘societ*’ ‘people’ ‘resident*’ ‘popula*’ | ‘Sabah’ ‘borneo’ ‘north borneo’ ‘north-borneo’ ‘east Malaysia’ ‘east-Malaysia’ ‘Tun Mustapha park’ ‘Tun Mustapha marine park’ ‘Kudat’ ‘Pitas’ ‘Kota Marudu’ ‘Sabah park*’ ‘Sabah marine park*’ |
| ‘health’ [MeSH] ‘health status disparities’ [MeSH] ‘health care surveys’ [MeSH] ‘health status indicators’ [MeSH] ‘health status’ [MeSH] ‘health impact assessment’ [MeSH] ‘outcome assessment (healthcare)’ [MeSH] ‘public health’ [MeSH] ‘public health surveillance’ [MeSH] ‘rural health’ [MeSH] ‘quality of life’ [MeSH] ‘quality-adjusted life years’ [MeSH] ‘value of life’ [MeSH] ‘disease*’ [MeSH] ‘morbidity’ [MeSH] ‘mortality’ [MeSH] ‘survival rate’ [MeSH] ‘facilities and services utilisation’ [MeSH] |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Azzeri, A.; Ching, G.H.; Jaafar, H.; Mohd Noor, M.I.; Razi, N.A.; Then, A.Y.-H.; Suhaimi, J.; Kari, F.; Dahlui, M. A Review of Published Literature Regarding Health Issues of Coastal Communities in Sabah, Malaysia. Int. J. Environ. Res. Public Health 2020, 17, 1533. https://doi.org/10.3390/ijerph17051533
Azzeri A, Ching GH, Jaafar H, Mohd Noor MI, Razi NA, Then AY-H, Suhaimi J, Kari F, Dahlui M. A Review of Published Literature Regarding Health Issues of Coastal Communities in Sabah, Malaysia. International Journal of Environmental Research and Public Health. 2020; 17(5):1533. https://doi.org/10.3390/ijerph17051533
Chicago/Turabian StyleAzzeri, Amirah, Goh Hong Ching, Hafiz Jaafar, Mohd Iqbal Mohd Noor, Nurain Amirah Razi, Amy Yee-Hui Then, Julia Suhaimi, Fatimah Kari, and Maznah Dahlui. 2020. "A Review of Published Literature Regarding Health Issues of Coastal Communities in Sabah, Malaysia" International Journal of Environmental Research and Public Health 17, no. 5: 1533. https://doi.org/10.3390/ijerph17051533
APA StyleAzzeri, A., Ching, G. H., Jaafar, H., Mohd Noor, M. I., Razi, N. A., Then, A. Y.-H., Suhaimi, J., Kari, F., & Dahlui, M. (2020). A Review of Published Literature Regarding Health Issues of Coastal Communities in Sabah, Malaysia. International Journal of Environmental Research and Public Health, 17(5), 1533. https://doi.org/10.3390/ijerph17051533





