Changes in Physical Activity, Physical Fitness and Well-Being Following a School-Based Health Promotion Program in a Norwegian Region with a Poor Public Health Profile: A Non-Randomized Controlled Study in Early Adolescents
Abstract
1. Introduction
2. Materials and Methods
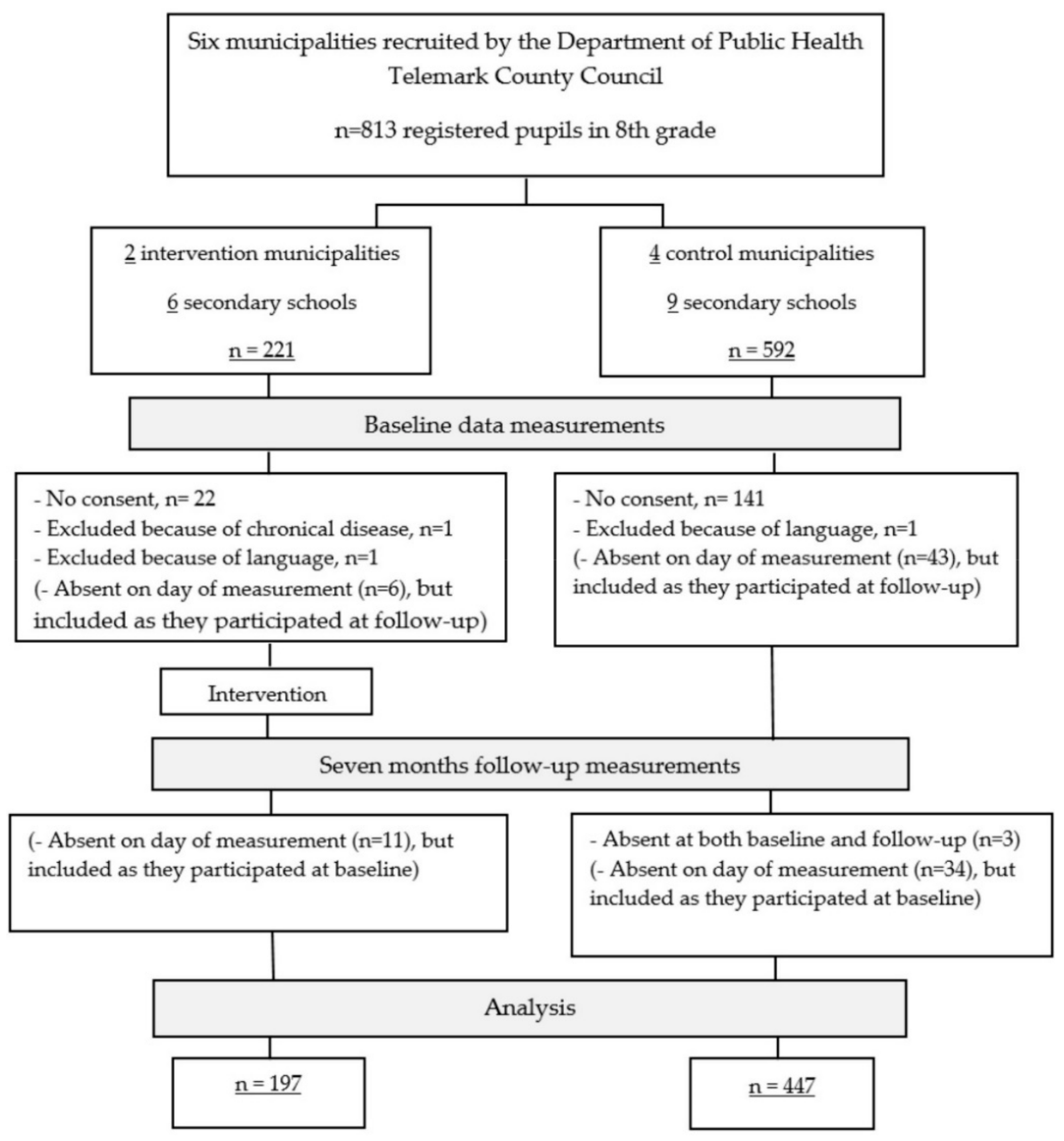
2.1. Participants and Study Design
2.2. Intervention Program
2.3. Instruments and Measures
2.3.1. PA and Sedentary Time
2.3.2. Cardiorespiratory Fitness
2.3.3. Strength
2.3.4. Anthropometric Measurements
2.3.5. HRQoL
2.3.6. Well-Being and Vitality
2.3.7. Demographic Characteristics
2.4. Statistical Analysis
3. Results
Changes in Intervention and Control Group at Baseline and Follow-up
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Biddle, S.J.; Ciaccioni, S.; Thomas, G.; Vergeer, I. Physical activity and mental health in children and adolescents: An updated review of reviews and an analysis of causality. Psychol. Sport Exerc. 2019, 42, 146–155. [Google Scholar] [CrossRef]
- Lubans, D.R.; Morgan, P.J.; Cliff, D.P.; Barnett, L.M.; Okely, A.D. Fundamental Movement Skills in Children and Adolescents: Review of Associated Health Benefits. Sports Med. 2010, 40, 1019–1035. [Google Scholar] [CrossRef] [PubMed]
- Penedo, F.J.; Dahn, J.R. Exercise and well-being: A review of mental and physical health benefits associated with physical activity. Curr. Opin. Psychiatry 2005, 18, 189–193. [Google Scholar] [CrossRef] [PubMed]
- Surén, P. Har ungdommer dårligere psykisk helse enn før? Tidsskr. den Nor. Laegeforening: Tidsskr. Praktisk Med. 2018. [Google Scholar] [CrossRef]
- Reneflot, A.; Aarø, L.; Aase, H.; Reichborn-Kjennerud, T.; Tambs, K.; Øverland, S. Psykisk helse i Norge; Norwegian Institute of Public Health (NIPH): Oslo, Norway, 2018. [Google Scholar]
- Berlin, M.; Salmi, P. Utvecklingen av Psykisk Ohälsa Bland Barn Och Unga Vuxna; Socialstyrelsen: Stockholm, Sverige, 2017. [Google Scholar]
- WHO. Adolescent Mental Health; World Health Organization (WHO): Geneva, Switzerland, 2019. [Google Scholar]
- Dalene, K.; Anderssen, S.; Andersen, L.; Steene-Johannessen, J.; Ekelund, U.; Hansen, B.; Kolle, E. Secular and longitudinal physical activity changes in population-based samples of children and adolescents. Scand. J. Med. Sci. Sports 2018, 28, 161–171. [Google Scholar] [CrossRef] [PubMed]
- Anderssen, S. Fysisk aktivitet blant voksne og eldre i Norge: resultater fra en kartlegging i 2008 og 2009; Helsedirektoratet: Oslo, Norway, 2009. [Google Scholar]
- Aase, K.N.; Bentsen, A.; Møller, G. Ung i Telemark 2015. Kompetencesenter rus - region sør; Telemark fylkeskommune: Skien, Norge, 2015. [Google Scholar]
- FHI. Nasjonalt overvåkingssystem for fysisk aktivitet og fysisk form. Kartlegging av fysisk aktivitet, sedat tid og fysisk form blant barn og unge 2018 (ungKan3); Folkehelseinstituttet (FHI): Oslo, Norway, 2019. [Google Scholar]
- WHO. Global Action Plan on Physical Activity 2018–2030: More Active People for A Healthier World; World Health Organization (WHO): Geneva, Switzerland, 2018. [Google Scholar]
- WHO. Health Promoting School: An Effective Approach for Early Action on NCD Risk Factors; World Health Organization (WHO): Geneva, Switzerland, 2017. [Google Scholar]
- WHO. Global Standards for Health Promoting Schools; World Health Organization (WHO): Geneva, Switzerland, 2018. [Google Scholar]
- NIPH. Public Health Report—Short Version. Health Status in Norway 2018; Norwegian Institute of Public Health (NIPH): Oslo, Norway, 2018. [Google Scholar]
- NIPH. Folkehelseprofil 2019 Telemark 2019; Norwegian Institute of Public Health (NIPH): Oslo, Norway, 2019. [Google Scholar]
- Erwin, H.; Beighle, A.; Carson, R.L.; Castelli, D.M. Comprehensive school-based physical activity promotion: A review. Quest 2013, 65, 412–428. [Google Scholar] [CrossRef]
- Watson, A.; Timperio, A.; Brown, H.; Best, K.; Hesketh, K.D. Effect of classroom-based physical activity interventions on academic and physical activity outcomes: A systematic review and meta-analysis. Int. J. Behav. Nutr. Phys. Act. 2017, 14, 114. [Google Scholar] [CrossRef]
- Donnelly, J.E.; Greene, J.L.; Gibson, C.A.; Smith, B.K.; Washburn, R.A.; Sullivan, D.K.; DuBose, K.; Mayo, M.S.; Schmelzle, K.H.; Ryan, J.J. Physical Activity Across the Curriculum (PAAC): A randomized controlled trial to promote physical activity and diminish overweight and obesity in elementary school children. Prev. Med. 2009, 49, 336–341. [Google Scholar] [CrossRef]
- Resaland, G.K.; Moe, V.F.; Aadland, E.; Steene-Johannessen, J.; Glosvik, Ø.; Andersen, J.R.; Kvalheim, O.M.; McKay, H.A.; Anderssen, S.A. Active Smarter Kids (ASK): Rationale and design of a cluster-randomized controlled trial investigating the effects of daily physical activity on children’s academic performance and risk factors for non-communicable diseases. BMC Public Health 2015, 15, 709. [Google Scholar] [CrossRef]
- Stewart, J.A.; Dennison, D.A.; Kohl, H.W., III; Doyle, J.A. Exercise level and energy expenditure in the TAKE 10!® in-class physical activity program. J. School Health 2004, 74, 397–400. [Google Scholar] [CrossRef]
- Norris, E.; van Steen, T.; Direito, A.; Stamatakis, E. Physically active lessons in schools and their impact on physical activity, educational, health and cognition outcomes: A systematic review and meta-analysis. Br. J. Sports Med. 2019. [Google Scholar] [CrossRef]
- Lonsdale, C.; Rosenkranz, R.R.; Peralta, L.R.; Bennie, A.; Fahey, P.; Lubans, D.R. A systematic review and meta-analysis of interventions designed to increase moderate-to-vigorous physical activity in school physical education lessons. Prev. Med. 2013, 56, 152–161. [Google Scholar] [CrossRef]
- Cale, L.; Harris, J. School-based physical activity interventions: Effectiveness, trends, issues, implications and recommendations for practice. Sport Educ. Soc. 2006, 11, 401–420. [Google Scholar] [CrossRef]
- Lindström, B.; Eriksson, M. Salutogenesis. J. Epidemiol. Community Health 2005, 59, 440–442. [Google Scholar] [CrossRef] [PubMed]
- OECD. The Future of Education and Skills: Education 2030; Organisation for Economic Co-operation and Development (OECD), Directorate for Education and Skills: Paris, France, 2018. [Google Scholar]
- Kriemler, S.; Meyer, U.; Martin, E.; Sluijs, E.M.; Andersen, L.B.; Martin, B.W. Effect of school-based interventions on physical activity and fitness in children and adolescents: A review of reviews and systematic update. Br. J. Sports Med. 2011, 45, 923–930. [Google Scholar] [CrossRef] [PubMed]
- Klakk, H.; Andersen, L.B.; Heidemann, M.; Møller, N.C.; Wedderkopp, N. Six physical education lessons a week can reduce cardiovascular risk in school children aged 6–13 years: A longitudinal study. Scand. J. Public Health 2014, 42, 128–136. [Google Scholar] [CrossRef]
- Resaland, G.; Anderssen, S.; Holme, I.; Mamen, A.; Andersen, L.B. Effects of a 2-year school-based daily physical activity intervention on cardiovascular disease risk factors: the Sogndal school-intervention study. Scand. J. Med. Sci. Sports 2011, 21, 302–309. [Google Scholar] [CrossRef]
- Hoare, E.; Fuller-Tyszkiewicz, M.; Skouteris, H.; Millar, L.; Nichols, M.; Allender, S. Systematic review of mental health and well-being outcomes following community-based obesity prevention interventions among adolescents. BMJ Open 2015, 5, e006586. [Google Scholar] [CrossRef]
- Busch, V.; Loyen, A.; Lodder, M.; Schrijvers, A.J.; van Yperen, T.A.; de Leeuw, J.R. The effects of adolescent health-related behavior on academic performance: A systematic review of the longitudinal evidence. Rev. Educ. Res. 2014, 84, 245–274. [Google Scholar] [CrossRef]
- Mura, G.; Rocha, N.B.; Helmich, I.; Budde, H.; Machado, S.; Wegner, M.; Nardi, A.E.; Arias-Carrión, O.; Vellante, M.; Baum, A. Physical activity interventions in schools for improving lifestyle in European countries. Clin. Pract. Epidemiol. Mental Health CP EMH 2015, 11, 77–101. [Google Scholar] [CrossRef]
- Guérin, E. Disentangling vitality, well-being, and quality of life: A conceptual examination emphasizing their similarities and differences with special application in the physical activity domain. J. Phys. Act. Health 2012, 9, 896–908. [Google Scholar] [CrossRef] [PubMed]
- Nix, G.A.; Ryan, R.M.; Manly, J.B.; Deci, E.L. Revitalization through self-regulation: The effects of autonomous and controlled motivation on happiness and vitality. J. Exp. Soc. Psychol. 1999, 35, 266–284. [Google Scholar] [CrossRef]
- Bailey, R.; Hillman, C.; Arent, S.; Petitpas, A. Physical activity: An underestimated investment in human capital? J. Phys. Act. Health 2013, 10, 289–308. [Google Scholar] [CrossRef]
- Love, R.; Adams, J.; van Sluijs, E.M. Are school-based physical activity interventions effective and equitable? A meta-analysis of cluster randomized controlled trials with accelerometer-assessed activity. Obes. Rev. 2019, 20, 859–870. [Google Scholar] [CrossRef]
- Sallis, J.F.; Cervero, R.B.; Ascher, W.; Henderson, K.A.; Kraft, M.K.; Kerr, J. An ecological approach to creating active living communities. Annu. Rev. Public Health 2006, 27, 297–322. [Google Scholar] [CrossRef] [PubMed]
- Ryan, R.M.; Deci, E.L. Intrinsic and Extrinsic Motivations: Classic Definitions and New Directions. Contemp. Educ. Psychol. 2000, 25, 54–67. [Google Scholar] [CrossRef]
- Resaland, G.K.; Aadland, E.; Moe, V.F.; Aadland, K.N.; Skrede, T.; Stavnsbo, M.; Suominen, L.; Steene-Johannessen, J.; Glosvik, Ø.; Andersen, J.R.; et al. Effects of physical activity on schoolchildren’s academic performance: The Active Smarter Kids (ASK) cluster-randomized controlled trial. Prev. Med. 2016, 91, 322–328. [Google Scholar] [CrossRef]
- Migueles, J.H.; Cadenas-Sanchez, C.; Ekelund, U.; Nyström, C.D.; Mora-Gonzalez, J.; Löf, M.; Labayen, I.; Ruiz, J.R.; Ortega, F.B. Accelerometer data collection and processing criteria to assess physical activity and other outcomes: A systematic review and practical considerations. Sports Med. 2017, 47, 1821–1845. [Google Scholar] [CrossRef]
- Evenson, K.R.; Catellier, D.J.; Gill, K.; Ondrak, K.S.; McMurray, R.G. Calibration of two objective measures of physical activity for children. J. Sports Sci. 2008, 26, 1557–1565. [Google Scholar] [CrossRef]
- Kim, Y.; Beets, M.W.; Welk, G.J. Everything you wanted to know about selecting the “right” Actigraph accelerometer cut-points for youth, but…: a systematic review. J. Sci. Med. Sport 2012, 15, 311–321. [Google Scholar] [CrossRef]
- Trost, S.G.; Loprinzi, P.D.; Moore, R.; Pfeiffer, K.A. Comparison of accelerometer cut points for predicting activity intensity in youth. Med. Sci. Sports Exerc. 2011, 43, 1360–1368. [Google Scholar] [CrossRef] [PubMed]
- Aadland, E.; Terum, T.; Mamen, A.; Andersen, L.B.; Resaland, G.K. The Andersen aerobic fitness test: Reliability and validity in 10-year-old children. PloS ONE 2014, 9, e110492. [Google Scholar] [CrossRef] [PubMed]
- Andersen, L.B.; Andersen, T.E.; Andersen, E.; Anderssen, S.A. An intermittent running test to estimate maximal oxygen uptake: The Andersen test. J. Sports Med. Phys. Fit. 2008, 48, 434–437. [Google Scholar]
- Castro-Piñero, J.; Ortega, F.B.; Artero, E.G.; Girela-Rejón, M.J.; Mora, J.; Sjöström, M.; Ruiz, J.R. Assessing muscular strength in youth: Usefulness of standing long jump as a general index of muscular fitness. J. Strength Cond. Res. 2010, 24, 1810–1817. [Google Scholar] [CrossRef]
- The Kidscreen Group Europe. The Kidscreen Questionnaires: Quality of Life Questionnaires for Children and Adolescents, Handbook; Pabst Science Publishers: Lengerich, Germany, 2006. [Google Scholar]
- Ravens-Sieberer, U.; Herdman, M.; Devine, J.; Otto, C.; Bullinger, M.; Rose, M.; Klasen, F. The European KIDSCREEN approach to measure quality of life and well-being in children: Development, current application, and future advances. Qual. Life Res. Int. J. Qual. Life Asp. Treat. Care Rehabil. 2014, 23, 791–803. [Google Scholar] [CrossRef]
- Deci, E.L.; Ryan, R.M. Handbook of Self-Determination Research; University of Rochester Press: Rochester, NY, USA, 2002. [Google Scholar]
- Ryan, R.M.; Frederick, C. On energy, personality, and health: Subjective vitality as a dynamic reflection of well-being. J. Personal. 1997, 65, 529–565. [Google Scholar] [CrossRef]
- Bostic, T.J.; Rubio, D.M.; Hood, M. A validation of the subjective vitality scale using structural equation modeling. Soc. Indic. Res. 2000, 52, 313–324. [Google Scholar] [CrossRef]
- Adler, N.E.; Newman, K. Socioeconomic disparities in health: Pathways and policies. Health Aff. (Project Hope) 2002, 21, 60–76. [Google Scholar] [CrossRef]
- Ross, C.E.; Wu, C. The links between education and health. Am. Sociol. Rev. 1995, 719–745. [Google Scholar] [CrossRef]
- Dobbins, M.; Husson, H.; DeCorby, K.; LaRocca, R.L. School-based physical activity programs for promoting physical activity and fitness in children and adolescents aged 6 to 18. Cochrane Database Sys. Rev. 2013, 2. [Google Scholar] [CrossRef]
- Gammon, C.; Morton, K.; Atkin, A.; Corder, K.; Daly-Smith, A.; Quarmby, T.; Suhrcke, M.; Turner, D.; van Sluijs, E. Introducing physically active lessons in UK secondary schools: Feasibility study and pilot cluster-randomised controlled trial. BMJ Open 2019, 9, e025080. [Google Scholar] [CrossRef] [PubMed]
- Dumith, S.C.; Gigante, D.P.; Domingues, M.R.; Kohl, H.W., III. Physical activity change during adolescence: A systematic review and a pooled analysis. Int. J. Epidemiol. 2011, 40, 685–698. [Google Scholar] [CrossRef] [PubMed]
- Seljebotn, P.H.; Skage, I.; Riskedal, A.; Olsen, M.; Kvalø, S.E.; Dyrstad, S.M. Physically active academic lessons and effect on physical activity and aerobic fitness. The Active School study: A cluster randomized controlled trial. Prev. Med. Rep. 2019, 13, 183–188. [Google Scholar] [CrossRef] [PubMed]
- Bailey, D.P.; Fairclough, S.J.; Savory, L.A.; Denton, S.J.; Pang, D.; Deane, C.S.; Kerr, C.J. Accelerometry-assessed sedentary behaviour and physical activity levels during the segmented school day in 10–14-year-old children: The HAPPY study. Eur. J. Pediatrics 2012, 171, 1805–1813. [Google Scholar] [CrossRef]
- Kolle, E.; Stokke, J.; Hansen, B.; Anderssen, S. Fysisk aktivitet blant 6-, 9-og 15-åringer i Norge. Resultater fra en kartlegging i 2011; Helsedirektoratet: Oslo, Norge, 2012. [Google Scholar]
- Ortega, F.; Ruiz, J.; Castillo, M.; Sjöström, M. Physical fitness in childhood and adolescence: A powerful marker of health. Int. J. Obes. 2008, 32, 1–11. [Google Scholar] [CrossRef]
- de Greeff, J.W.; Hartman, E.; Mullender-Wijnsma, M.J.; Bosker, R.J.; Doolaard, S.; Visscher, C. Effect of physically active academic lessons on body mass index and physical fitness in primary school children. J. Sch. Health 2016, 86, 346–352. [Google Scholar] [CrossRef]
- de Greeff, J.W.; Hartman, E.; Mullender-Wijnsma, M.J.; Bosker, R.J.; Doolaard, S.; Visscher, C. Long-term effects of physically active academic lessons on physical fitness and executive functions in primary school children. Health Educ. Res. 2016, 31, 185–194. [Google Scholar] [CrossRef]
- Michel, G.; Bisegger, C.; Fuhr, D.C.; Abel, T. Age and gender differences in health-related quality of life of children and adolescents in Europe: A multilevel analysis. Qual. Life Res. 2009, 18, 1147–1157. [Google Scholar] [CrossRef]
- Harrington, D.; Davies, M.; Bodicoat, D.; Chudasama, Y.; Gorely, T.; Khunti, K.; Rowlands, A.; Sherar, L.; Tudor-Edwards, R.; Yates, T. A school-based intervention (Girls Active) to increase physical activity levels among 11-to 14-year-old girls: Cluster RCT. Public Health Res. 2019, 7. [Google Scholar] [CrossRef]
- Storvoll, E.E.; Strandbu, Å.; Wichstrøm, L. A cross-sectional study of changes in Norwegian adolescents’ body image from 1992 to 2002. Body Image 2005, 2, 5–18. [Google Scholar] [CrossRef]
- Ekelund, U.; Tarp, J.; Steene-Johannessen, J.; Hansen, B.H.; Jefferis, B.; Fagerland, M.W.; Whincup, P.; Diaz, K.M.; Hooker, S.P.; Chernofsky, A. Dose-response associations between accelerometry measured physical activity and sedentary time and all cause mortality: Systematic review and harmonised meta-analysis. BMJ 2019, 366, l4570. [Google Scholar] [CrossRef] [PubMed]
| Before Start | Follow-up Training |
|---|---|
| One-day course on how to teach PAL and inspiration to 5-min physical active breaks. | One-day follow-up course on how to facilitate activities indoor. |
| Afternoon meeting at the local school planning PAL | Afternoon meeting at the local school to share experiences and plan PAL |
| (mandatory, however not all teachers participated). | (mandatory, however not all teachers participated). |
| n | Intervention M | n | Control M | p-Values | |
|---|---|---|---|---|---|
| Demographics | |||||
| Age (years) | 197 | 13.2 (0.0) | 447 | 13.2 (0.0) | 0.13 |
| Sex (% girls/boys) | 197 | 47/53 | 447 | 51/49 | 0.314 |
| Anthropometry | |||||
| Body mass (kg) | 197 | 52.5 (0.7) | 447 | 52 (0.5) | 0.503 |
| Height (cm) | 197 | 162.2 (0.6) | 447 | 161.3 (0.3) | 0.15 |
| BMI (kg/m2) | 197 | 19.8 (0.2) | 447 | 20.0 (0.2) | 0.472 |
| PA full day | |||||
| Total PA (CPM) | 197 | 492.2 (13.2) | 447 | 466.2 (9.8) | 0.121 |
| SED (min/day) | 197 | 543.2 (5.7) | 447 | 535.8 (3.9) | 0.266 |
| MVPA (min/day) | 197 | 56.1 (1.7) | 447 | 52.3 (1.2) | 0.067 |
| PA school time | |||||
| Total PA (CPM) | 197 | 440.7 16.3) | 447 | 403.8 (12.5) | 0.099 |
| SED (min/day) | 197 | 175.3 (3.2) | 447 | 177.1 (2.4) | 0.674 |
| MVPA (min/day) | 197 | 17.6 (0.8) | 447 | 16.4 (0.6) | 0.268 |
| Physical fitness | |||||
| CRF (m) | 197 | 1005.1 (8.1) | 447 | 990.5 (6.6) | 0.173 |
| Strength (cm) | 197 | 163.4 (1.8) | 447 | 161.5 (1.3) | 0.423 |
| HRQoL | |||||
| Physical well-being | 197 | 46.3 (0.6) | 447 | 46.3 (0.5) | 0.981 |
| Psychological well-being | 197 | 51.1 (0.6) | 447 | 50.3 (0.5) | 0.369 |
| Autonomy and parents | 197 | 53 (0.7) | 447 | 53.3 (0.5) | 0.707 |
| Peers and social support | 197 | 51.4 (0.7) | 447 | 51.3 (0.5) | 0.840 |
| School environment | 197 | 53.4 (0.7) | 447 | 51.3 (0.5) | 0.018 * |
| Vitality | 197 | 4.7 (0.1) | 447 | 4.8 (0.1) | 0.635 |
| Intervention | Control | Group diff. (SE) | p-Value | |||||
|---|---|---|---|---|---|---|---|---|
| Baseline (SE) | Follow-up (SE) | p-Value | Baseline (SE) | Follow-up (SE) | p-Value | |||
| n | 197 | 447 | ||||||
| BMI (kg/m2 | 19.8 (0.2) | 20.2 (0.2) | 0.000 ** | 20.0 (0.2) | 20.4 (0.2) | 0.007 * | −0.01 (0.1) | 0.934 |
| PA full day | ||||||||
| n | 197 | 447 | ||||||
| Total PA (cpm) | 492 (13.1) | 505 (20.1) | 0.512 | 466 (9.8) | 470 (15.6) | 0.762 | 6,6 (9.1) | 0.467 |
| SED (min/day) | 543 (5.7) | 557 (6) | 0.057 | 536 (3.8) | 553 (0.9) | 0.012 * | −2.68 (3.7) | 0.466 |
| MVPA (min/day) | 56 (1.7) | 55.9 (1.9) | 0.916 | 52 (1.1) | 51 (1.4) | 0.485 | 0.76 (1) | 0.446 |
| PA school time | ||||||||
| n | 197 | 447 | ||||||
| Total PA (cpm) | 492 (13.1) | 505 (20.1) | 0.512 | 466 (9.8) | 471 (15.6) | 0.762 | 54.7 (9.7) | 0.000 ** |
| SED (min/day) | 182 (2.6) | 175 (3.2) | 0.098 | 190 (2.2) | 177 (2.4) | 0.000 ** | 6.5 (2) | 0.001 ** |
| MVPA (min/day) | 17 (0.8) | 17 (10.8) | 0.585 | 16 (0.6) | 13 (0.5) | 0.000 ** | 2.8 (0.4) | 0.000 ** |
| n | 197 | 447 | ||||||
| CRF (m) | 1005 (8.1) | 1021 (7.3) | 0.076 | 990 (6.6) | 999 (5.3) | 0.164 | 8.7 (4.1) | 0.035 * |
| Strength (cm) | 163 (1.8) | 171 (1.8) | 0.000 ** | 161 (1.3) | 167 (1.4) | 0.000 ** | 2 (0.5) | 0.000 ** |
| HRQL | ||||||||
| n | 197 | 447 | ||||||
| Physical | 46 (0.6) | 47 (0.7) | 0.366 | 46.3 (0.5) | 46.1 (0.5) | 0.648 | 0.9 (0.4) | 0.012 * |
| Psychological | 51 (0.6) | 51 (0.8) | 0.845 | 50.3 (0.5) | 49.0 (0.6) | 0.023 * | 1.19 (0.4) | 0.001 ** |
| Autonomy | 53 (0.7) | 55 (0.8) | 0.001 ** | 53.3 (0.5) | 54.7 (0.6) | 0.026 * | 1.2 (0.4) | 0.004 * |
| Peers and social | 51 (0.7) | 50 (0.9) | 0.085 | 51.2 (0.5) | 50 (0.5) | 0.031 * | −0.4 (0.4) | 0.909 |
| School | 53 (0.7) | 53 (0.8) | 0.621 | 51.3 (0.5) | 49.9 (0.6) | 0.016 * | 2 (0.4) | 0.017 * |
| n | 197 | 447 | ||||||
| Vitality | 4.7 (0.1) | 4.8 (0.1) | 0.412 | 4.8 (0.0) | 4.5 (0.1) | 0.000 ** | 0.3 (0.0) | 0.000 ** |
| Group | Time | Group x Time | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| df | F | p | Mean diff (SE) | 95% CI | df | F | p | Mean diff (SE) | 95% CI | df | F | p | |
| PA full day | |||||||||||||
| Total PA (cpm) | 538.32 | 1.44 | 0.23 | 0.06 (0.06) | −0.06–0.19 | 425.27 | 1.26 | 0.26 | −0.02 (0.05) | −0.11–0.07 | 424.27 | 0.01 | 0.91 |
| SED (min/day) | 508.71 | 2.3 | 0.13 | 0.08 (0.63) | −0.42–0.21 | 407.00 | 6.67 | 0.01 * | −0.06 (0.05) | −0.15–0.03 | 407.00 | 0.00 | 0.97 |
| MVPA (min/day) | 510.53 | 3.09 | 0.08 | 0.08 (0.06) | −0.05–0.21 | 392.52 | 0.31 | 0.58 | 0.03 (0.05) | −0.07–0.12 | 392.52 | 0.06 | 0.80 |
| PA school time | |||||||||||||
| Total PA (cpm) | 554.87 | 25.23 | 0.00 ** | 0.23 (0.06) | 0.11–0.34 | 520.83 | 3.11 | 0.08 | 0.10 (0.04) | 0.01–0.19 | 520.83 | 7.99 | 0.005 * |
| SED (min/day) | 5552.18 | 5.91 | 0.02 * | −0.12 (0.05) | −0.22–(−)0.01 | 544.88 | 11.74 | 0.00 ** | 0.08 (0.04) | −0.01–0.16 | 544.88 | 1.12 | 0.29 |
| MVPA (min/day) | 536.04 | 17.17 | 0.00 ** | 0.19 (0.06) | 0.08–0.31 | 483.26 | 9.26 | 0.00 * | 0.12 (0.04) | 0.04–0.21 | 483.26 | 9.04 | 0.003 ** |
| CRF (m) | 582.85 | 7.57 | 0.00 ** | 0.13 (0.07) | −0.00–0.27 | 458.72 | 5.61 | 0.02 * | −0.03 (0.04) | −0.11–0.06 | 458.72 | 5.31 | 0.02 * |
| Strength (cm) | 609.17 | 1.12 | 0.29 | 0.04 (0.07) | −0.1–0.18 | 469.02 | 113.55 | 0.00 ** | −0.14 (0.04) | −0.23–(−)0.05 | 469.02 | 3.87 | 0.050 * |
| HRQoL | |||||||||||||
| Physical | 621.19 | 0.39 | 0.53 | 0.03 (0.06) | −0.1–0.15 | 566.23 | 0.58 | 0.45 | −0.02 (0.04) | −0.10–0.07 | 566.23 | 1.35 | 0.25 |
| Psychological | 621.84 | 4.15 | 0.04 * | 0.01 (0.06) | −0.03–0.22 | 566.62 | 2.28 | 0.13 | 0.05 (0.04) | −0.03–0.14 | 566.62 | 1 | 0.17 |
| Autonomy | 619.73 | 0.14 | 0.71 | 0.02 (0.06) | −0.1–0.13 | 575.67 | 13.72 | 0.00 ** | −0.09 (0.04) | −0.18–(−)0.00 | 575.67 | 1.77 | 0.26 |
| Peers | 606.21 | 0.05 | 0.82 | 0.01 (0.06) | −0.11–0.13 | 560.06 | 4.09 | 0.04 * | 0.05 (0.04) | −0.04–0.14 | 560.06 | 0.00 | 0.99 |
| School | 625.08 | 13 | 0.00 ** | 0.17 (0.06) | 0.05–0.28 | 578.53 | 2.42 | 0.12 | 0.08 (0.04) | −0.01–0.16 | 578.53 | 1.38 | 0.24 |
| Vitality | 608.53 | 1.61 | 0.22 | 0.05 (0.06) | −0.07–0.18 | 550.09 | 1.64 | 0.20 | 0.03 (0.04) | −0.05–0.12 | 550.09 | 7.20 | 0.008 ** |
| Group | Time | Group x Time | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Boys | df | F | p | Mean diff (SE) | 95% CI | df | F | p | Mean diff (SE) | 95% CI | df | F | p |
| PA full day | |||||||||||||
| Total PA (cpm) | 252.01 | 0.02 | 0.88 | 0.08 (0.09) | −0.10–0.26 | 185.93 | 2.26 | 0.14 | 0.13 (0.07) | 0.00–0.27 | 185.93 | 0.09 | 0.758 |
| SED (min/day) | 235.15 | 3.90 | 0.05 * | 0.09 (0.09) | −0.09–0.26 | 204.09 | 9.41 | 0.00 * | −0.18 (0.07) | −0.32- (-)0.04 | 204.09 | 0.04 | 0.842 |
| MVPA (min/day) | 246.53 | 0.32 | 0.57 | 0.14 (0.10) | −0.05–0.33 | 197.17 | 2.99 | 0.09 | 0.19 (0.07) | 0.04–0.33 | 197.17 | 0.80 | 0.373 |
| PA school day | |||||||||||||
| Total PA (cpm) | 288.57 | 10.96 | 0.00 ** | 0.43 (0.09) | 0.25–0.61 | 267.23 | 2.08 | 0.15 | 0.31 (0.07) | 0.17–0.45 | 267.23 | 9.71 | 0.002 * |
| SED (min/day) | 281.09 | 1.69 | 0.19 | −0.24 (0.08) | −0.39–(−)0.09 | 271.58 | 4.37 | 0.04 * | −0.08 (0.07) | −0.21–0.05 | 271.58 | 0.44 | 0.508 |
| MVPA (min/day) | 265.66 | 8.90 | 0.00 * | 0.34 (0.08) | 0.18–0.51 | 235.39 | 5.29 | 0.02 * | 0.28 (0.07) | 0.15–0.41 | 235.39 | 13.05 | 0.000 ** |
| CFR (m) | 293.27 | 9.21 | 0.00 * | 0.45 (0.10) | 0.26–0.64 | 236.81 | 7.22 | 0.01 * | 0.20 (0.06) | 0.07–0.32 | 236.81 | 1.46 | 0.229 |
| Strength (cm) | 305.96 | 6.08 | 0.01 * | 0.38 (0.10) | 0.179 | 243.62 | 74.62 | 0.00 ** | 0.06 (0.06) | −0.06–0.19 | 243.62 | 1.85 | 0.175 |
| HRQoL | |||||||||||||
| Physical | 315.26 | 0.21 | 0.64 | 0.04 (0.09) | −0.13–0.21 | 290.05 | 2.73 | 0.20 | 0.01 (0.06) | −0.11–0.13 | 290.05 | 0.11 | 0.744 |
| Psychological | 308.20 | 0.04 | 0.84 | 0.08 (0.08) | −0.09–0.24 | 282.88 | 0.01 | 0.93 | 0.06 (0.06) | −0.05–0.18 | 282.88 | 0.03 | 0.868 |
| Autonomy | 313.08 | 0.31 | 0.58 | 0.12 (0.08) | −0.15–0.07 | 293.77 | 12.70 | 0.00 ** | −0.15 (0.06) | −0.27–(−)0.02 | 293.77 | 0.07 | 0.785 |
| Peers | 304.80 | 1.31 | 0.25 | −0.17 (0.09) | −0.34–(−)0.00 | 283.45 | 1.29 | 0.26 | −0.07 (0.06) | −0.20–0.05 | 283.45 | 0.05 | 0.830 |
| School | 313.29 | 6.76 | 0.01 * | 0.14 (0.08) | −0.02–0.30 | 293.12 | 0.18 | 0.68 | 0.02 (0.06) | −0.01–0.1 | 293.12 | 0.51 | 0.474 |
| Vitality | 309.28 | 0.11 | 0.74 | 0.08 (0.08) | −0.08–0.25 | 281.71 | 0.45 | 0.51 | 0.05 (0.06) | −0.07–0.16 | 281.71 | 0.58 | 0.447 |
| Group | Time | Group x Time | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Girls | df | F | p | Mean diff (SE) | 95% CI | df | F | p | Mean diff (SE) | 95% CI | df | F | p |
| PA full day | |||||||||||||
| Total PA (cpm) | 286.85 | 1.95 | 0.16 | 0.05 (0.09) | −0.13–0.23 | 237.49 | 8.12 | 0.01 * | −0.25 (0.07) | −2.28–(−)0.02 | 237.49 | 0.01 | 0.916 |
| SED (min/day) | 272.79 | 0.06 | 0.80 | 0.07 (0.09) | −0.10–0.25 | 207.65 | 0.44 | 0.51 | 0.036 (0.06) | −0.09–0.16 | 207.65 | 0.00 | 0.973 |
| MVPA (min/day) | 266.5 | 3.51 | 0.06 | 0.03 (0.08) | −0.14–0.19 | 200.60 | 0.94 | 0.33 | −0.12 (0.06) | −0.22–0.01 | 200.60 | 0.22 | 0.637 |
| PA school time | |||||||||||||
| Total PA (cpm) | 275.84 | 13.4 | 0.00 ** | −0.00 (0.07) | −0.14–0.13 | 256.61 | 1.56 | 0.21 | −0.11 (0.05) | −0.21–(−)0.01 | 256.61 | 0.25 | 0.697 |
| SED (min/day) | 518 | 3.41 | 0.07 | 0.03 (0.07) | −0.12–0.17 | 518 | 7.23 | 0.01 * | 0.23 (0.06) | 0.11–0.35 | 518 | 5.34 | 0.021 * |
| MVPA (min/day) | 274.35 | 6.89 | 0.01 * | 0.014* (0.08) | −0.14–0.17 | 253.28 | 4.93 | 0.03 * | −0.23 (0.06) | −0.12–0.09 | 253.284 | 0.18 | 0.672 |
| CFR (m) | 287 | 0.34 | 0.56 | −0.22 (0.09) | −0.39–(−)0.43 | 221.88 | 0.33 | 0.57 | −0.26 (0.06) | −0.38–(−)0.15 | 221.88 | 5.23 | 0.023 * |
| Strength (cm) | 299.50 | 2.32 | 0.13 | −0.34 (0.09) | −0.52–(−)0.15 | 222.95 | 39.75 | 0.00 ** | −0.36 (0.06) | −0.47–(−)0.25 | 222.95 | 2.15 | 0.144 |
| HRQoL | |||||||||||||
| Physical | 304.15 | 1.68 | 0.20 | 0.01 (0.09) | −0.17–0.18 | 273.98 | 0.38 | 0.54 | −0.04 (0.06) | −0.16–0.08 | 273.98 | 4.13 | 0.043 * |
| Psychological | 310.94 | 6.80 | 0.01 * | 0.11 (0.09) | −0.06–0.29 | 280.61 | 5.00 | 0.03 * | 0.05 (0.06) | −0.08–0.17 | 280.61 | 4.5 | 0.035 * |
| Autonomy | 303.45 | 0.00 | 0.98 | 0.02 (0.09) | −0.15–0.19 | 277.47 | 2.61 | 0.11 | −0.04 (0.06) | −0.15–0.08 | 277.47 | 3.95 | 0.048 * |
| Peers | 297.63 | 3.12 | 0.08 | 0.21 (0.08) | 0.04–0.38 | 273.80 | 0.06 | 0.81 | 0.18 (0.06) | 0.06–0.3 | 273.80 | 0.06 | 0.807 |
| School | 308.58 | 6.46 | 0.01 * | 0.20 (0.08) | 0.03–0.37 | 281.67 | 3.61 | 0.06 | 0.13 (0.06) | 0.01–.25 | 281.67 | 0.89 | 0.348 |
| Vitality | 297.27 | 1.6 | 0.20 | 0.01 (0.09) | −0.17–0.20 | 265.46 | 5.77 | 0.02 * | 0.02 (0.06) | −0.11–0.15 | 265.46 | 8.75 | 0.003 * |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Schmidt, S.K.; Reinboth, M.S.; Resaland, G.K.; Bratland-Sanda, S. Changes in Physical Activity, Physical Fitness and Well-Being Following a School-Based Health Promotion Program in a Norwegian Region with a Poor Public Health Profile: A Non-Randomized Controlled Study in Early Adolescents. Int. J. Environ. Res. Public Health 2020, 17, 896. https://doi.org/10.3390/ijerph17030896
Schmidt SK, Reinboth MS, Resaland GK, Bratland-Sanda S. Changes in Physical Activity, Physical Fitness and Well-Being Following a School-Based Health Promotion Program in a Norwegian Region with a Poor Public Health Profile: A Non-Randomized Controlled Study in Early Adolescents. International Journal of Environmental Research and Public Health. 2020; 17(3):896. https://doi.org/10.3390/ijerph17030896
Chicago/Turabian StyleSchmidt, Sabrina K., Michael S. Reinboth, Geir K. Resaland, and Solfrid Bratland-Sanda. 2020. "Changes in Physical Activity, Physical Fitness and Well-Being Following a School-Based Health Promotion Program in a Norwegian Region with a Poor Public Health Profile: A Non-Randomized Controlled Study in Early Adolescents" International Journal of Environmental Research and Public Health 17, no. 3: 896. https://doi.org/10.3390/ijerph17030896
APA StyleSchmidt, S. K., Reinboth, M. S., Resaland, G. K., & Bratland-Sanda, S. (2020). Changes in Physical Activity, Physical Fitness and Well-Being Following a School-Based Health Promotion Program in a Norwegian Region with a Poor Public Health Profile: A Non-Randomized Controlled Study in Early Adolescents. International Journal of Environmental Research and Public Health, 17(3), 896. https://doi.org/10.3390/ijerph17030896





