Assessment of Peri-Implant Soft Tissues Conditions around Short and Ultra-Short Implant-Supported Single Crowns: A 3-Year Retrospective Study on Periodontally Healthy Patients and Patients with a History of Periodontal Disease
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Inclusion Criteria
2.2. Surgical Protocol
2.3. Prosthetic Protocol and Follow-Up Evaluation
2.4. Study Variables and Outcomes
2.5. Statistical Analysis
3. Results
3.1. Demographics
3.2. Implant Survival and Marginal Bone Loss
3.3. Soft Tissues’ Conditions and Implant Success
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Appendix A
Appendix A.1. Study Design and Inclusion Criteria
Appendix A.2. Surgical Protocol
Appendix A.3. Prosthetic Protocol and Follow-Up Evaluation
Appendix A.4. Study Variables and Outcomes
Appendix A.5. Statistical Analysis
References
- Thoma, D.S.; Cha, J.-K.; Jung, U.-W. Treatment concepts for the posterior maxilla and mandible: Short implants versus long implants in augmented bone. J. Periodontal Implant. Sci. 2017, 47, 2–12. [Google Scholar] [CrossRef]
- Monje, A.; Suarez, F.; Galindo-Moreno, P.; García-Nogales, A.; Fu, J.H.; Wang, H.L. A systematic review on marginal bone loss around short dental implants (<10 mm) for implant-supported fixed prostheses. Clin. Oral Implants Res. 2014, 25, 1119–1124. [Google Scholar] [CrossRef]
- Lee, J.-S.; Kim, H.-M.; Kim, C.-S.; Choi, S.-H.; Chai, J.-K.; Jung, U.-W. Long-term retrospective study of narrow implants for fixed dental prostheses. Clin. Oral Implants Res. 2013, 24, 847–852. [Google Scholar] [CrossRef]
- Lemos, C.A.A.; Ferro-Alves, M.L.; Okamoto, R.; Mendonça, M.R.; Pellizzer, E.P. Short dental implants versus standard dental implants placed in the posterior jaws: A systematic review and meta-analysis. J. Dent. 2016, 47, 8–17. [Google Scholar] [CrossRef] [PubMed]
- Neugebauer, J.; Nickenig, H.; Zoller, J. Update on short, angulated a diameter-reduced implants. In Proceedings of the 11th European Consensus Conference, European Association of Dental Implantologists, Bonn, Germany, 6 February 2016. [Google Scholar]
- Altaib, F.H.; Alqutaibi, A.Y.; Al-Fahd, A.; Eid, S. Short dental implant as alternative to long implant with bone augmentation of the atrophic posterior ridge: A systematic review and meta-analysis of RCTs. Quintessence Int. 2019, 50, 636–650. [Google Scholar] [PubMed]
- Esposito, M.; Buti, J.; Barausse, C.; Gasparro, R.; Sammartino, G.; Felice, P. Short implants versus longer implants in vertically augmented atrophic mandibles: A systematic review of randomised controlled trials with a 5-year post-loading follow-up. Int. J. Oral Implant. 2019, 12, 267–280. [Google Scholar]
- Ma, M.; Qi, M.; Zhang, D.; Liu, H. The Clinical Performance of Narrow Diameter Implants Versus Regular Diameter Implants: A Meta-Analysis. J. Oral Implant. 2019, 45, 503–508. [Google Scholar] [CrossRef]
- Clelland, N.; Chaudhry, J.; Rashid, R.G.; McGlumphy, E. Split-Mouth Comparison of Splinted and Nonsplinted Prostheses on Short Implants: 3-Year Results. Int. J. Oral Maxillofac. Implants 2016, 31, 1135–1141. [Google Scholar] [CrossRef]
- Naenni, N.; Sahrmann, P.; Schmidlin, P.; Attin, T.; Wiedemeier, D.; Sapata, V.; Hämmerle, C.; Jung, R. Five-Year Survival of Short Single-Tooth Implants (6 mm): A Randomized Controlled Clinical Trial. J. Dent. Res. 2018, 97, 887–892. [Google Scholar] [CrossRef]
- Telles, L.H.; Portella, F.F.; Rivaldo, E. Longevity and marginal bone loss of narrow-diameter implants supporting single crowns: A systematic review. PLoS ONE 2019, 14, e0225046. [Google Scholar] [CrossRef]
- Urdaneta, R.A.; Daher, S.; Leary, J.; Emanuel, K.M.; Chuang, S.-K. The survival of ultrashort locking-taper implants. Int. J. Oral Maxillofac. Implants 2012, 27, 644–654. [Google Scholar]
- Lee, S.-A.; Lee, C.-T.; Fu, M.M.; Elmisalati, W.; Chuang, S.-K. Systematic Review and Meta-Analysis of Randomized Controlled Trials for the Management of Limited Vertical Height in the Posterior Region: Short Implants (5 to 8 mm) vs Longer Implants (>8 mm) in Vertically Augmented Sites. Int. J. Oral Maxillofac. Implants 2014, 29, 1085–1097. [Google Scholar] [CrossRef] [PubMed]
- Fugazzotto, P. Shorter implants in clinical practice: Rationale and treatment results. Int. J. Oral Maxillofac. Implants 2008, 23, 487–496. [Google Scholar] [PubMed]
- Anitua, E.; Piñas, L.; Orive, G. Retrospective Study of Short and Extra-Short Implants Placed in Posterior Regions: Influence of Crown-to-Implant Ratio on Marginal Bone Loss. Clin. Implant. Dent. Relat. Res. 2015, 17, 102–110. [Google Scholar] [CrossRef] [PubMed]
- Malchiodi, L.; Ghensi, P.; Cucchi, A.; Pieroni, S.; Bertossi, D. Peri-implant conditions around sintered porous-surfaced (SPS) implants. A 36-month prospective cohort study. Clin. Oral Implants Res. 2014, 26, 212–219. [Google Scholar] [CrossRef]
- Felice, P.; Pistilli, R.; Barausse, C.; Piattelli, M.; Buti, J.; Esposito, M. Posterior atrophic jaws rehabilitated with prostheses supported by 6-mm-long 4-mm-wide implants or by longer implants in augmented bone. Five-year post-loading results from a within-person randomised controlled trial. Int. J. Oral Implant. 2019, 12, 57–72. [Google Scholar]
- Atieh, M.A.; Alsabeeha, N.H.; Faggion, C.M., Jr.; Duncan, W.J. The Frequency of Peri-Implant Diseases: A Systematic Review and Meta-Analysis. J. Periodontol. 2012, 84, 1–15. [Google Scholar] [CrossRef]
- Derks, J.; Tomasi, C. Peri-implant health and disease. A systematic review of current epidemiology. J. Clin. Periodontol. 2015, 42, S158–S171. [Google Scholar] [CrossRef]
- Lee, C.-T.; Huang, Y.-W.; Zhu, L.; Weltman, R. Prevalences of peri-implantitis and peri-implant mucositis: Systematic review and meta-analysis. J. Dent. 2017, 62, 1–12. [Google Scholar] [CrossRef]
- Konstantinidis, I.; Kotsakis, G.; Gerdes, S.; Walter, M.H. Cross-sectional study on the prevalence and risk indicators of peri-implant diseases. Eur. J. Oral Implant. 2015, 8, 75–88. [Google Scholar]
- Jepsen, S.; Berglundh, T.; Genco, R.; Aass, A.M.; Demirel, K.; Derks, J.; Figuero, E.; Giovannoli, J.L.; Goldstein, M.; Lambert, F.; et al. Primary prevention of peri-implantitis: Managing peri-implant mucositis. J. Clin. Periodontol. 2015, 42, S152–S157. [Google Scholar] [CrossRef] [PubMed]
- Berglundh, T.; Armitage, G.; Araujo, M.G.; Avila-Ortiz, G.; Blanco, J.; Camargo, P.M.; Chen, S.; Cochran, D.; Derks, J.; Figuero, E.; et al. Peri-implant diseases and conditions: Consensus report of workgroup 4 of the 2017 World Workshop on the Classification of Periodontal and Peri-Implant Diseases and Conditions. J. Clin. Periodontol. 2018, 45, S286–S291. [Google Scholar] [CrossRef] [PubMed]
- Caton, J.G.; Armitage, G.; Berglundh, T.; Chapple, I.L.; Jepsen, S.; Kornman, K.S.; Mealey, B.L.; Papapanou, P.N.; Sanz, M.; Tonetti, M.S. A new classification scheme for periodontal and peri-implant diseases and conditions—Introduction and key changes from the 1999 classification. J. Clin. Periodontol. 2018, 45, S1–S8. [Google Scholar] [CrossRef] [PubMed]
- Sanz, M.; Chapple, I.L. Clinical research on peri-implant diseases: Consensus report of Working Group 4. J. Clin. Periodontol. 2012, 39, 202–206. [Google Scholar] [CrossRef]
- Derks, J.; Schaller, D.; Hakansson, J.; Wennstrom, J.L.; Tomasi, C.; Berglundh, T. Effectiveness of Implant Therapy Analyzed in a Swedish Population. J. Dent. Res. 2016, 95, 43–49. [Google Scholar] [CrossRef]
- Romanos, G.E.; Delgado-Ruiz, R.; Sculean, A. Concepts for prevention of complications in implant therapy. Periodontology 2019, 81, 7–17. [Google Scholar] [CrossRef]
- Vehemente, V.; Chuang, S.-K.; Daher, S.; Muftu, A.; Dodson, T.B. Risk factors affecting dental implant survival. J. Oral Implant. 2002, 28, 74–81. [Google Scholar] [CrossRef]
- Abduljabbar, T.; Al-Hamoudi, N.; Al-Sowygh, Z.H.; Alajmi, M.; Javed, F.; Vohra, F. Comparison of peri-implant clinical and radiographic status around short (6 mm in length) dental implants placed in cigarette-smokers and never-smokers: Six-year follow-up results. Clin. Implant. Dent. Relat. Res. 2018, 20, 21–25. [Google Scholar] [CrossRef]
- Chrcanovic, B.; Kisch, J.; Albrektsson, T.; Wennerberg, A. Factors Influencing Early Dental Implant Failures. J. Dent. Res. 2016, 95, 995–1002. [Google Scholar] [CrossRef]
- Klokkevold, P.R.; Han, T.J. How do smoking, diabetes, and periodontitis affect outcomes of implant treatment? Int. J. Oral Maxillofac. Implants 2007, 22, 173–202. [Google Scholar]
- Akram, Z.; Vohra, F.; Sheikh, S.A.; Albaijan, R.; Bukhari, I.A.; Hussain, M. Clinical and radiographic peri-implant outcomes of short dental implants placed in posterior jaws of patients with treated generalized aggressive periodontitis: A 3-year follow-up study. Clin. Implant. Dent. Relat. Res. 2019, 21, 775–780. [Google Scholar] [CrossRef]
- Erbasar, G.N.H.; Hocaoğlu, T.P.; Erbasar, R.C. Risk factors associated with short dental implant success: A long-term retrospective evaluation of patients followed up for up to 9 years. Braz. Oral Res. 2019, 33, e030. [Google Scholar] [CrossRef] [PubMed]
- Lombardo, G.; Signoriello, A.; Simancas-Pallares, M.; Marincola, M.; Nocini, P.F. Survival of Short and Ultra-Short Locking-Taper Implants Supporting Single Crowns in the Posterior Mandible: A 3-Year Retrospective Study. J. Oral Implant. 2020, 46, 396–406. [Google Scholar] [CrossRef] [PubMed]
- Lombardo, G.; Marincola, M.; Signoriello, A.; Corrocher, G.; Nocini, P.F. Single-Crown, Short and Ultra-Short Implants, in Association with Simultaneous Internal Sinus Lift in the Atrophic Posterior Maxilla: A Three-Year Retrospective Study. Materials 2020, 13, 2208. [Google Scholar] [CrossRef] [PubMed]
- Mombelli, A.; Lang, N.P. Clinical parameters for the evaluation of dental implants. Periodontology 1994, 4, 81–86. [Google Scholar] [CrossRef] [PubMed]
- Bhatia, G.; Kumar, A.; Khatri, M.; Bansal, M.; Saxena, S. Assessment of the width of attached gingiva using different methods in various age groups: A clinical study. J. Indian Soc. Periodontol. 2015, 19, 199–202. [Google Scholar] [CrossRef]
- Ferreira, S.D.; Silva, G.L.M.; Cortelli, J.R.; Costa, J.E.; Costa, F.O. Prevalence and risk variables for peri-implant disease in Brazilian subjects. J. Clin. Periodontol. 2006, 33, 929–935. [Google Scholar] [CrossRef]
- Buser, D.; Weber, H.P.; Bragger, U.; Balsiger, C. Tissue integration of one-stage ITI implants: 3-year results of a longitudinal study with Hollow-Cylinder and Hollow-Screw implants. Int J Oral Maxillofac. Implants 1991, 6, 405–412. [Google Scholar] [CrossRef]
- Albrektsson, T.; Zarb, G. Determinants of correct clinical reporting. Int. J. Prosthodont. 1999, 11, 517–521. [Google Scholar]
- StataCorp. Stata Statistical Software: Release 15; StataCorp LLC: College Station, TX, USA, 2017. [Google Scholar]
- Wang, W.C.; Lagoudis, M.; Yeh, C.-W.; Paranhos, K.S. Management of peri-implantitis—A contemporary synopsis. Singap. Dent. J. 2017, 38, 8–16. [Google Scholar] [CrossRef]
- Zitzmann, N.U.; Berglundh, T. Definition and prevalence of peri-implant diseases. J. Clin. Periodontol. 2008, 35, 286–291. [Google Scholar] [CrossRef] [PubMed]
- Schwarz, F.; Derks, J.; Monje, A.; Wang, H.-L. Peri-implantitis. J. Clin. Periodontol. 2018, 45, S246–S266. [Google Scholar] [CrossRef] [PubMed]
- Mombelli, A.; Décaillet, F. The characteristics of biofilms in peri-implant disease. J. Clin. Periodontol. 2011, 38, 203–213. [Google Scholar] [CrossRef]
- Quirynen, M.; Vogels, R.; Peeters, W.; Van Steenberghe, D.; Naert, I.; Haffajee, A. Dynamics of initial subgingival colonization of ‘pristine’ peri-implant pockets. Clin. Oral Implants Res. 2005, 17, 25–37. [Google Scholar] [CrossRef]
- Smeets, R.; Henningsen, A.; Jung, O.; Heiland, M.; Hammächer, C.; Stein, J.M. Definition, etiology, prevention and treatment of peri-implantitis—A review. Head Face Med. 2014, 10, 34. [Google Scholar] [CrossRef]
- Pjetursson, B.E.; Helbling, C.; Weber, H.-P.; Matuliene, G.; Salvi, G.E.; Brägger, U.; Schmidlin, K.; Zwahlen, M.; Lang, N.P. Peri-implantitis susceptibility as it relates to periodontal therapy and supportive care. Clin. Oral Implants Res. 2012, 23, 888–894. [Google Scholar] [CrossRef]
- Salvi, G.E.; Cosgarea, R.; Sculean, A. Prevalence and Mechanisms of Peri-implant Diseases. J. Dent. Res. 2016, 96, 31–37. [Google Scholar] [CrossRef]
- Changi, K.K.; Finkelstein, J.; Papapanou, P.N. Peri-implantitis prevalence, incidence rate, and risk factors: A study of electronic health records at a U.S. dental school. Clin. Oral Implants Res. 2019, 30, 306–314. [Google Scholar] [CrossRef]
- Karoussis, I.K.; Salvi, G.E.; Heitz-Mayfield, L.J.A.; Bragger, U.; Hammerle, C.H.F.; Lang, N.P. Long-term implant prognosis in patients with and without a history of chronic periodontitis: A 10-year prospective cohort study of the ITIR Dental Implant System. Clin. Oral Implants Res. 2003, 14, 329–339. [Google Scholar] [CrossRef]
- Hardt, C.R.E.; Gröndahl, K.; Lekholm, U.; Wennstrom, J.L. Outcome of implant therapy in relation to experienced loss of periodontal bone support. Clin. Oral Implants Res. 2002, 13, 488–494. [Google Scholar] [CrossRef]
- Roccuzzo, M.; De Angelis, N.; Bonino, L.; Aglietta, M. Ten-year results of a three-arm prospective cohort study on implants in periodontally compromised patients. Part 1: Implant loss and radiographic bone loss. Clin. Oral Implants Res. 2010, 21, 490–496. [Google Scholar] [CrossRef] [PubMed]
- Roos-Jansaker, A.-M.; Lindahl, C.; Renvert, H.; Renvert, S. Nine- to fourteen-year follow-up of implant treatment. Part II: Presence of peri-implant lesions. J. Clin. Periodontol. 2006, 33, 290–295. [Google Scholar] [CrossRef] [PubMed]
- Koldsland, O.C.; Scheie, A.A.; Aass, A.M. The association between selected risk indicators and severity of peri-implantitis using mixed model analyses. J. Clin. Periodontol. 2011, 38, 285–292. [Google Scholar] [CrossRef] [PubMed]
- Roccuzzo, M.; Bonino, F.; Aglietta, M.; Dalmasso, P. Ten-year results of a three arms prospective cohort study on implants in periodontally compromised patients. Part 2: Clinical results. Clin. Oral Implants Res. 2012, 23, 389–395. [Google Scholar] [CrossRef] [PubMed]
- Renvert, S.; Aghazadeh, A.; Hallström, H.; Persson, G.R. Factors related to peri-implantitis—A retrospective study. Clin. Oral Implants Res. 2014, 25, 522–529. [Google Scholar] [CrossRef]
- Arunyanak, S.P.; Sophon, N.; Tangsathian, T.; Supanimitkul, K.; Suwanwichit, T.; Kungsadalpipob, K. The effect of factors related to periodontal status toward peri-implantitis. Clin. Oral Implants Res. 2019, 30, 791–799. [Google Scholar] [CrossRef]
- Zhang, H.; Li, W.; Zhang, L.; Yan, X.; Shi, D.; Meng, H. A nomogram prediction of peri-implantitis in treated severe periodontitis patients: A 1-5-year prospective cohort study. Clin. Implant. Dent. Relat. Res. 2018, 20, 962–968. [Google Scholar] [CrossRef]
- Correia, F.; Gouveia, S.; Felino, A.; Costa, A.; Almeida, R.F. Survival Rate of Dental Implants in Patients with History of Periodontal Disease: A Retrospective Cohort Study. Int. J. Oral Maxillofac. Implants 2017, 32, 927–934. [Google Scholar] [CrossRef]
- Demiralp, K.Ö.; Akbulut, N.; Kursun, S.; Argun, D.; Bagis, N.; Orhan, K. Survival Rate of Short, Locking Taper Implants with a Plateau Design: A 5-Year Retrospective Study. BioMed Res. Int. 2015, 2015, 1–8. [Google Scholar] [CrossRef]
- Marincola, M.; Coelho, P.G.; Morgan, V.; Cicconetti, A. The importance of crestal bone preservation in the use of short implants. J. Adv. Dent. Res. 2010, 1, 15–18. [Google Scholar]
- Montemezzi, P.; Ferrini, F.; Pantaleo, G.; Gherlone, E.F.; Capparé, P. Dental Implants with Different Neck Design: A Prospective Clinical Comparative Study with 2-Year Follow-Up. Materials 2020, 13, 1029. [Google Scholar] [CrossRef] [PubMed]
- Ellegaard, B.; Baelum, V.; Karring, T. Implant therapy in periodontally compromised patients. Clin. Oral Implants Res. 1997, 8, 180–188. [Google Scholar] [CrossRef] [PubMed]
- Nevins, M. Will Implants Survive Well in Patients With a History of Inflammatory Periodontal Disease? J. Periodontol. 2001, 72, 113–117. [Google Scholar] [CrossRef] [PubMed]
- Coli, P.; Christiaens, V.; Sennerby, L.; De Bruyn, H. Reliability of periodontal diagnostic tools for monitoring peri-implant health and disease. Periodontology 2016, 73, 203–217. [Google Scholar] [CrossRef] [PubMed]
- Aguirre-Zorzano, L.A.; Estefanía-Fresco, R.; Telletxea, O.; Bravo, M. Prevalence of peri-implant inflammatory disease in patients with a history of periodontal disease who receive supportive periodontal therapy. Clin. Oral Implants Res. 2014, 26, 1338–1344. [Google Scholar] [CrossRef] [PubMed]
- Dibart, S.; Warbington, M.; Su, M.F.; Skobe, Z. In vitro evaluation of the implant-abutment bacterial seal: The locking taper system. Int. J. Oral Maxillofac. Implants 2005, 20, 732–737. [Google Scholar]
- Urdaneta, R.A.; Marincola, M. The Integrated Abutment Crown?, a Screwless and Cementless Restoration for Single-Tooth Implants: A Report on a New Technique. J. Prosthodont. 2007, 16, 311–318. [Google Scholar] [CrossRef]
- Mangano, F.G.; Shibli, J.A.; Sammons, R.L.; Iaculli, F.; Piattelli, A.; Mangano, C. Short (8-mm) locking-taper implants supporting single crowns in posterior region: A prospective clinical study with 1-to 10-years of follow-up. Clin. Oral Implants Res. 2014, 25, 933–940. [Google Scholar] [CrossRef]
- Maiorana, C.; Farronato, D.; Pieroni, S.; Cicciù, M.; Andreoni, D.; Santoro, F. A Four-Year Survival Rate Multicenter Prospective Clinical Study on 377 Implants: Correlations Between Implant Insertion Torque, Diameter, and Bone Quality. J. Oral Implant. 2015, 41, e60–e65. [Google Scholar] [CrossRef]
- Malchiodi, L.; Cucchi, A.; Ghensi, P.; Consonni, D.; Nocini, P.F. Influence of crown-implant ratio on implant success rates and crestal bone levels: A 36-month follow-up prospective study. Clin. Oral Implants Res. 2013, 25, 240–251. [Google Scholar] [CrossRef]
- Urdaneta, R.A.; Rodriguez, S.; McNeil, D.C.; Weed, M.; Chuang, S.-K. The effect of increased crown-to-implant ratio on single-tooth locking-taper implants. Int. J. Oral Maxillofac. Implants 2010, 25, 729–743. [Google Scholar] [PubMed]
- Birdi, H.; Schulte, J.; Kovacs, A.; Weed, M.; Chuang, S.-K. Crown-to-Implant Ratios of Short-Length Implants. J. Oral Implant. 2010, 36, 425–433. [Google Scholar] [CrossRef] [PubMed]
- Gontiya, G.; Galgali, S.R. Evaluation of an innovative radiographic technique-parallel profile radiography-to determine the dimensions of dentogingival unit. Indian J. Dent. Res. 2011, 22, 237–241. [Google Scholar] [CrossRef] [PubMed]
- Blanes, R.J.; Bernard, J.P.; Blanes, Z.M.; Belser, U.C. A 10-year prospective study of ITI dental implants placed in the posterior region. II: Influence of the crown-to-implant ratio and different prosthetic treatment modalities on crestal bone loss. Clin. Oral Implants Res. 2007, 18, 707–714. [Google Scholar] [CrossRef] [PubMed]
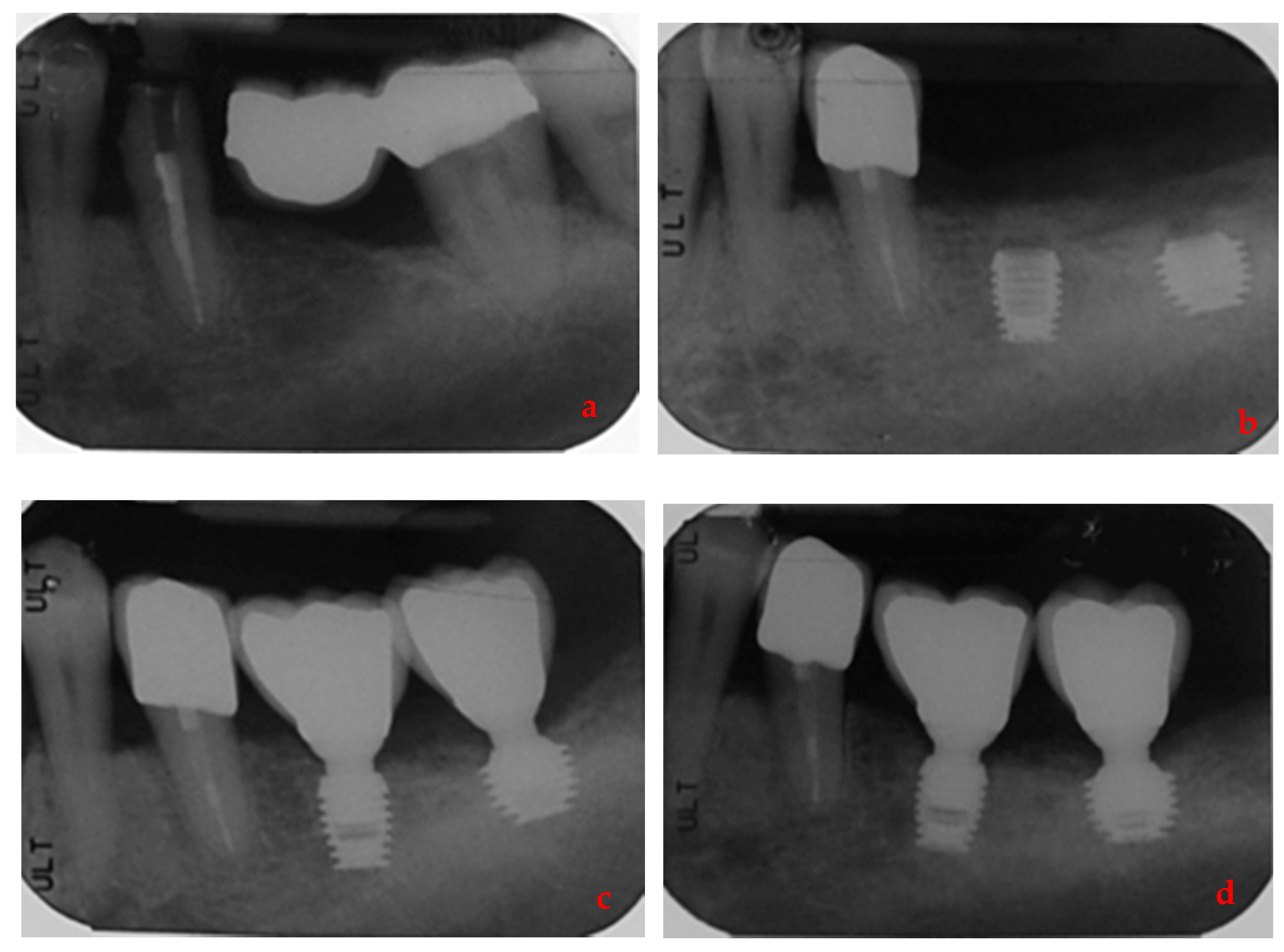
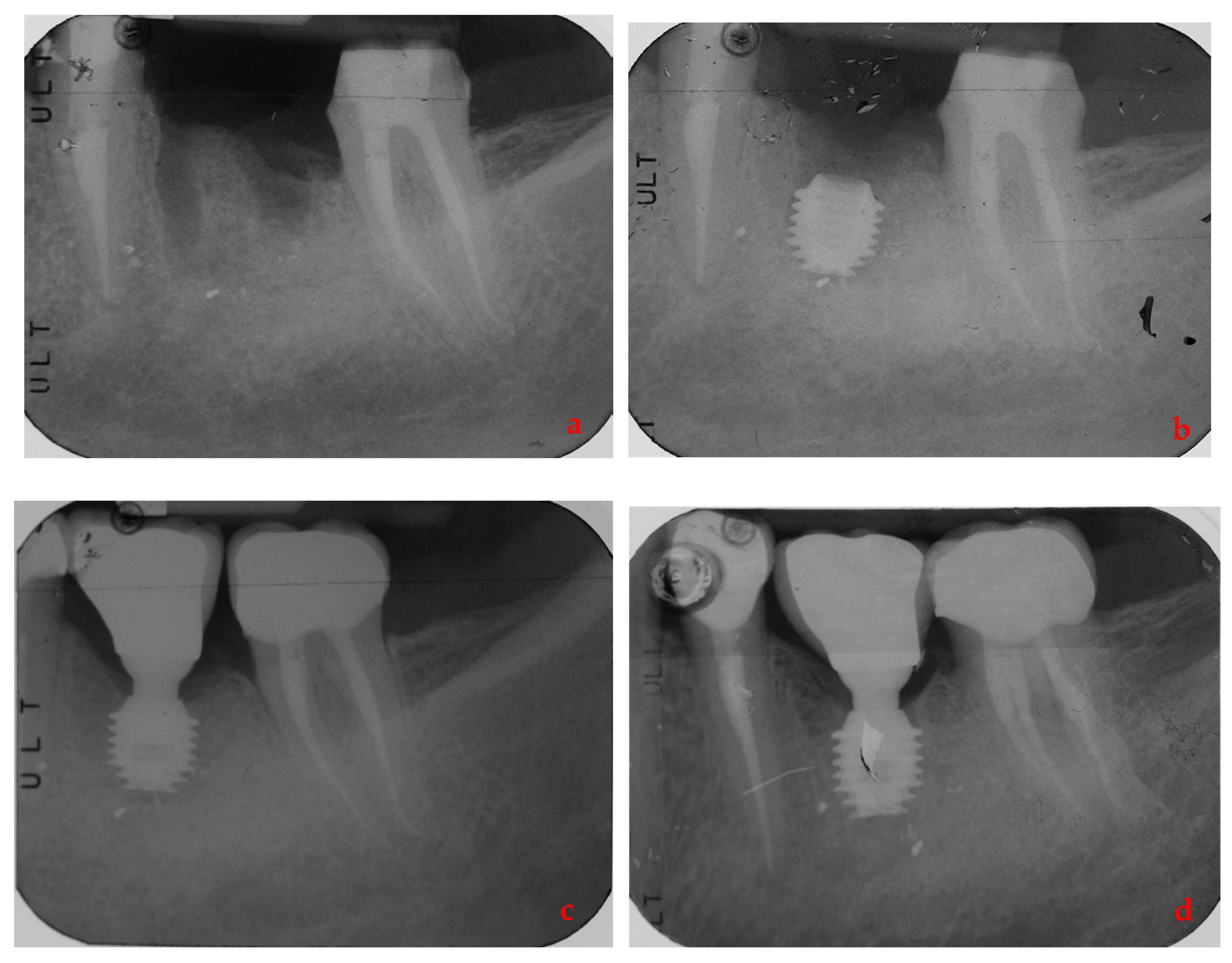
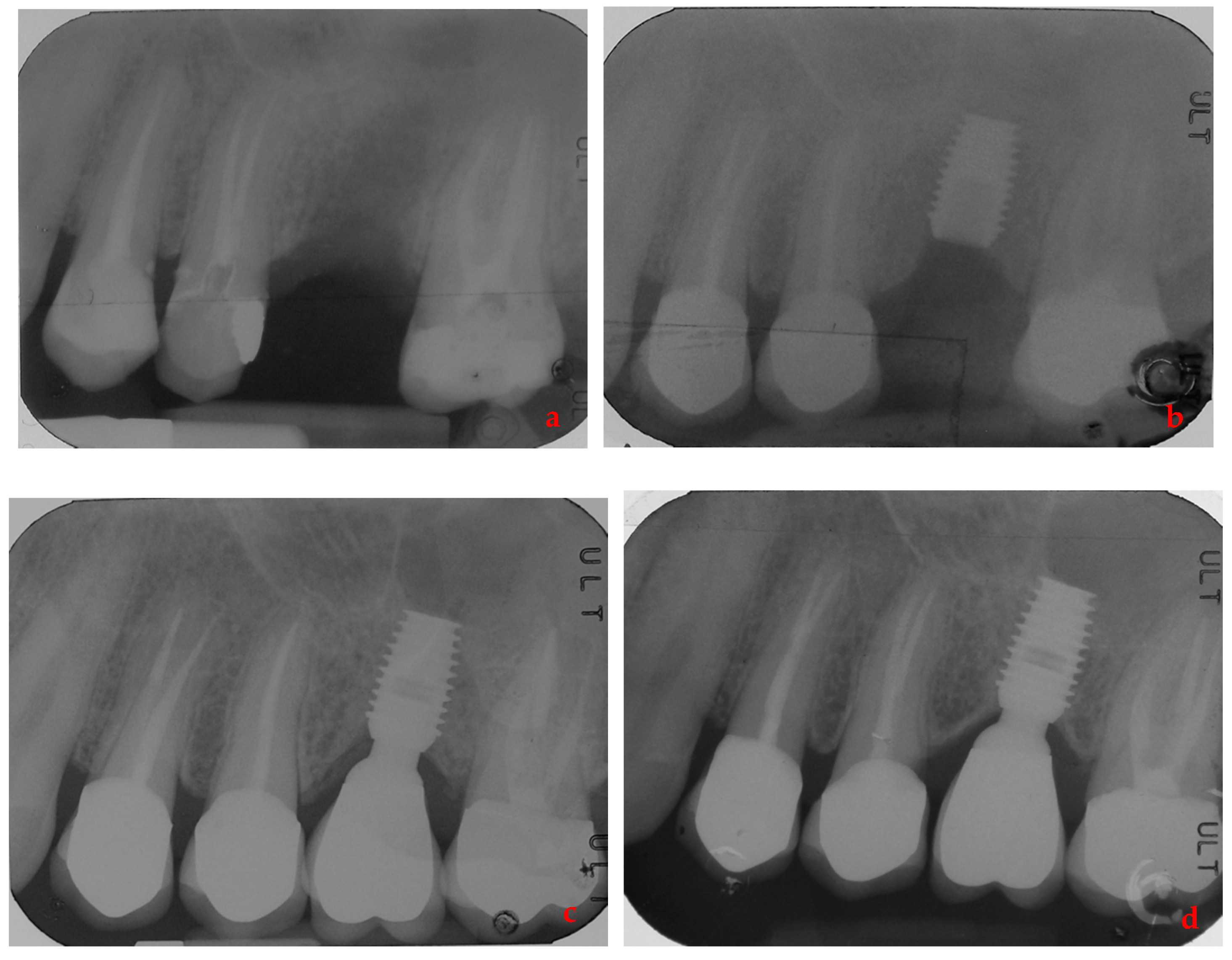
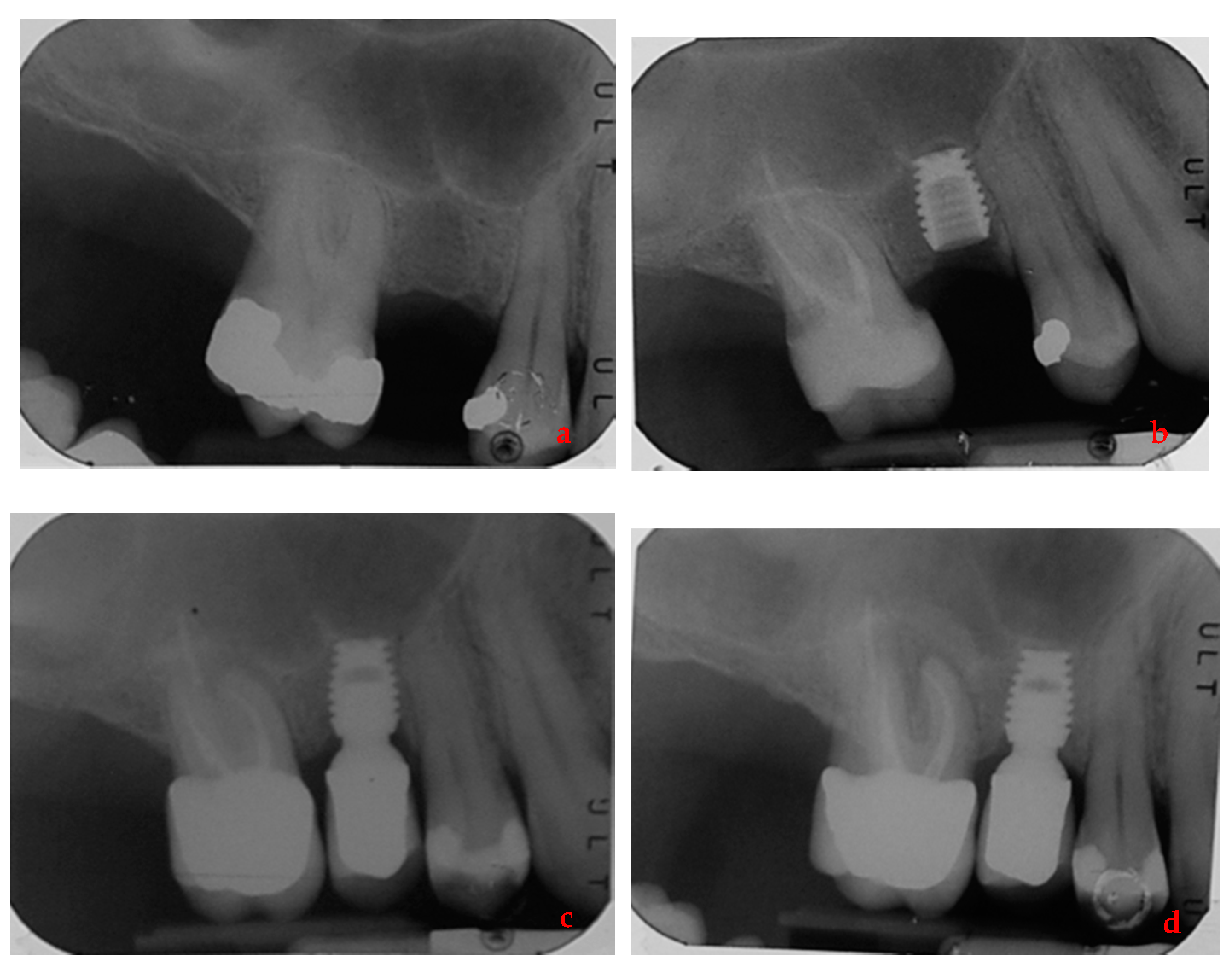
| Variable | NPP | PP | Test Statistic | d.f. | p Value |
|---|---|---|---|---|---|
| Sex | |||||
| male | 53 (45.30) | 89 (42.79) | χ2 = 0.19 | 1 | NS (p = 0.66) |
| female | 64 (54.70) | 119 (57.21) | |||
| Age at follow-up | 55.41 ± 10.56 | 60.56 ± 9.95 | F = 19.18 | 1/325 | <0.001 |
| Smoking history | |||||
| no | 87 (74.36) | 172 (82.69) | χ2 = 3.21 | 1 | NS (p = 0.07) |
| yes | 30 (25.64) | 36 (17.31) | |||
| ASA status | |||||
| I | 65 (55.56) | 80 (38.46) | χ2 = 9.03 | 1 | 0.01 |
| II | 52 (44.44) | 128 (61.54) | |||
| Oral professional hygiene/year | 2.88 ± 1.34 | 2.89 ± 1.11 | F = 14.31 | 1/325 | NS (p = 0.92) |
| Use of interproximal oral hygiene devices | |||||
| no | 30 (25.64) | 51 (24.52) | χ2 = 0.05 | 1 | NS (p = 0.82) |
| yes | 87 (74.36) | 157 (75.48) | |||
| Implant length | |||||
| 5 mm | 32 (27.35) | 44 (21.15) | χ2 = 1.74 | 2 | NS (p = 0.41) |
| 6 mm | 40 (34.19) | 73 (35.10) | |||
| 8 mm | 45 (38.46) | 91 (43.75) | |||
| Implant tooth site | |||||
| premolar | 46 (39.32) | 98 (47.12) | χ2 = 1.84 | 1 | NS (p = 0.17) |
| molar | 71 (60.68) | 110 (52.88) | |||
| Arch | |||||
| posterior mandible | 68 (58.12) | 123 (59.13) | χ2 = 0.03 | 1 | NS (p = 0.85) |
| posterior maxilla | 49 (41.88) | 85 (40.87) | |||
| Implant diameter | |||||
| 3 mm | 1 (0.85) | 0 (0.00) | χ2 = 5.75 | 6 | NS (p = 0.44) |
| 3.5 mm | 6 (5.13) | 7 (3.37) | |||
| 4 mm | 28 (23.93) | 61 (29.33) | |||
| 4.5 mm | 39 (33.33) | 76 (36.54) | |||
| 5 mm | 36 (30.77) | 55 (26.44) | |||
| 6 mm | 6 (5.13) | 9 (4.33) | |||
| 6.5 mm | 1 (0.85) | 0 (0.00) | |||
| Prosthetic material | |||||
| resin | 18 (15.38) | 35 (16.83) | χ2 = 0.11 | 1 | NS (p = 0.73) |
| porcelain | 99 (84.62) | 173 (83.17) | |||
| Crown-to-implant ratio (CIR) | |||||
| <2 | 68 (58.12) | 89 (42.79) | χ2 = 7.75 | 2 | 0.02 |
| 2 < CIR < 2.99 | 48 (41.03) | 113 (54.33) | |||
| >2.99 | 1 (0.85) | 6 (2.88) |
| Site | 45 | 46 | 24 | 47 | 16 | 34 | 44 | 17 |
| Diameter | 6 | 4.5 | 4 | 5 | 5 | 4.5 | 5 | 5 |
| Length | 5 | 8 | 5 | 6 | 6 | 8 | 8 | 6 |
| Sex | male | male | female | female | male | male | male | male |
| Smoking history | no | no | no | no | yes | yes | no | no |
| ASA status | I | I | I | II | II | II | II | I |
| Oral professional hygiene/year | 3 | 4 | 4 | 4 | 3 | 2 | 4 | 4 |
| History of periodontal disease | yes | no | no | no | yes | yes | yes | no |
| Crown-to-implant ratio | 2.76 | 1.38 | 2.25 | 2.17 | 2.68 | 1.69 | 1.62 | / |
| Failure | late | late | late | late | late | late | late | early |
| Variable | Survival | Failure | Test Statistic | d.f. | p Value |
|---|---|---|---|---|---|
| n (%) | n (%) | ||||
| Sex | |||||
| male | 137 (95.80) | 6 (4.20) | χ2 = 3.22 | 1 | NS (p = 0.14) |
| female | 181 (98.91) | 2 (1.09) | |||
| Smoking history | |||||
| no | 254 (97.69) | 6 (2.31) | χ2 = 0.11 | 1 | NS (p = 0.66) |
| yes | 64 (96.97) | 2 (3.03) | |||
| ASA status | |||||
| I | 142 (97.26) | 4 (2.74) | χ2 = 4.41 | 1 | NS (p = 0.11) |
| II | 176 (97.78) | 4 (2.22) | |||
| History of periodontal disease | |||||
| no | 114 (96.61) | 4 (3.39) | χ2 = 0.67 | 1 | NS (p = 0.46) |
| yes | 204 (98.08) | 4 (1.92) | |||
| Implant tooth site | |||||
| premolar | 140 (97.22) | 4 (2.78) | χ2 = 0.11 | 1 | NS (p = 0.73) |
| molar | 178 (97.80) | 4 (2.20) | |||
| Arch | |||||
| posterior mandible | 186 (97.38) | 5 (2.62) | χ2 = 0.05 | 1 | NS (p = 0.56) |
| posterior maxilla | 132 (97.78) | 3 (2.22) | |||
| Implant diameter | |||||
| 3 mm | 1 (100.00) | 0 (0.00) | |||
| 3.5 mm | 13 (100.00) | 0 (0.00) | |||
| 4 mm | 88 (98.88) | 1 (1.12) | χ2 = 3.77 | 6 | NS (p = 0.41) |
| 4.5 mm | 113 (98.26) | 2 (1.74) | |||
| 5 mm | 88 (95.65) | 4 (4.35) | |||
| 6 mm | 14 (93.33) | 1 (6.67) | |||
| 6.5 mm | 1 (100.00) | 0 (0.00) | |||
| Implant length | |||||
| 8 mm | 133 (97.79) | 3 (2.21) | χ2 = 0.06 | 2 | NS (p = 0.97) |
| 6 mm | 111 (97.37) | 3 (2.63) | |||
| 5 mm | 74 (97.37) | 2 (2.63) | |||
| Prosthetic material | |||||
| resin | 53 (100) | 0 (0.00) | χ2 = 1.39 | 1 | NS (p = 0.60) |
| porcelain | 265 (97.43) | 7 (2.57) | |||
| Crown-to-implant ratio | |||||
| <2 | 154 (98.09) | 3 (1.91) | χ2 = 0.33 | 2 | NS (p = 0.76) |
| 2–2.99 | 157 (97.52) | 4 (2.48) | |||
| >2.99 | 7 (100.00) | 0 (0.00) |
| Variable | Overall | History of Periodontal Disease | Implant Length | Arch | ||||
|---|---|---|---|---|---|---|---|---|
| no | yes | 5 mm | 6 mm | 8 mm | Posterior Mandible | Posterior Maxilla | ||
| CBL | ||||||||
| Loading time | 1.97 | 2.17 | 1.93 | 1.82 | 1.87 | 2.20 | 2.10 | 1.88 |
| [median (iqr)] | (1.64) | (1.53) | (1.63) | (1.40) | (1.83) | (1.71) | (1.62) | (1.63) |
| Follow-up time | 1.57 | 1.57 | 1.58 | 1.42 | 1.55 | 1.78 | 1.59 | 1.55 |
| [median (iqr)] | (1.8) | (1.67) | (1.86) | (1.75) | (1.97) | (1.86) | (1.78) | (1.90) |
| ΔCBL | 0.36 | 0.41 | 0.34 | 0.32 | 0.36 | 0.36 | 0.33 | 0.45 |
| [median (iqr)] | (1.03) | (1.08) | (0.95) | (1.05) | (0.96) | (1.11) | (1.00) | (0.99) |
| test statistic | ||||||||
| d.f. | Z = 0.38 | χ2 = 0.23 | Z = −0.82 | |||||
| p value | 2 | |||||||
| NS (p = 0.69) | NS (p = 0.89) | NS (p = 0.40) | ||||||
| F-BIC | ||||||||
| Loading time | 0.22 | 0.01 | 0.28 | 0.37 | 0.18 | 0.18 | 0.23 | 0.21 |
| [median (iqr)] | (0.66) | (0.54) | (0.70) | (0.71) | (0.62) | (0.65) | (0.68) | (0.66) |
| Follow-up time | 0.40 | 0.44 | 0.38 | 0.53 | 0.39 | 0.33 | 0.43 | 0.38 |
| [median (iqr)] | (0.84) | (0.85) | (0.81) | (0.73) | (0.85) | (0.72) | (0.89) | (0.74) |
| ΔF-BIC | 0.05 | 0.14 | 0.01 | 0.19 | 0.09 | 0.01 | 0.09 | 0.01 |
| [median (iqr)] | (0.56) | (0.46) | (0.57) | (0.56) | (0.63) | (0.41) | (0.46) | (0.60) |
| test statistic | ||||||||
| d.f. | Z = 1.73 | χ2 = 2.77 | Z = 1.67 | |||||
| p value | 2 | |||||||
| NS (p = 0.08) | NS (p = 0.24) | NS (p = 0.09) | ||||||
| Variable | mBI | Test Statistic | d.f. | p Value |
|---|---|---|---|---|
| [mean ± sd] | ||||
| Overall | 0.9 ± 0.8 | |||
| History of periodontal disease | ||||
| no | 0.9 ± 0.83 | Z = −0.08 | NS (p = 0.93) | |
| yes | 0.9 ± 0.79 | |||
| Arch | ||||
| posterior mandible | 0.91 ± 0.82 | Z = 0.16 | NS (p = 0.87) | |
| posterior maxilla | 0.88 ± 0.78 | |||
| Implant length | ||||
| 8 mm | 0.86 ± 0.75 | |||
| 6 mm | 0.92 ± 0.79 | χ2 = 0.20 | 2 | NS (p = 0.90) |
| 5 mm | 0.94 ± 0.92 | |||
| Variable | mPLI | Test Statistic | d.f. | p Value |
| [mean ± sd] | ||||
| Overall | 0.52 ± 0.73 | |||
| History of periodontal disease | ||||
| no | 0.56 ± 0.79 | Z = 0.23 | NS (p = 0.81) | |
| yes | 0.5 ± 0.69 | |||
| Arch | ||||
| posterior mandible | 0.5 ± 0.72 | Z = −0.77 | NS (p = 0.43) | |
| posterior maxilla | 0.55 ± 0.74 | |||
| Implant length | ||||
| 8 mm | 0.48 ± 0.67 | |||
| 6 mm | 0.49 ± 0.72 | χ2 = 1.89 | 2 | NS (p = 0.38) |
| 5 mm | 0.64 ± 0.82 | |||
| Variable | PPD | Test Statistic | d.f. | p Value |
| [mean ± sd] | ||||
| Overall | 3.29 ± 1.28 | |||
| History of periodontal disease | ||||
| no | 3.35 ± 1.4 | Z = 0.18 | NS (p = 0.85) | |
| yes | 3.26 ± 1.2 | |||
| Arch | ||||
| posterior mandible | 3.29 ± 1.41 | Z = −0.68 | NS (p = 0.49) | |
| posterior maxilla | 3.29 ± 1.07 | |||
| Implant length | ||||
| 8 mm | 3.33 ± 1.35 | |||
| 6 mm | 3.23 ± 1.08 | χ2 = 0.12 | 2 | NS (p = 0.93) |
| 5 mm | 3.32 ± 1.42 | |||
| Variable | KT | Test Statistic | d.f. | p Value |
| [mean ± sd] | ||||
| Overall | 2.47 ± 1.69 | |||
| History of periodontal disease | ||||
| no | 2.49 ± 1.79 | Z = 0.19 | NS (p = 0.84) | |
| yes | 2.45 ± 1.63 | |||
| Arch | ||||
| posterior mandible | 2.41 ± 1.69 | Z = −0.70 | NS (p = 0.48) | |
| posterior maxilla | 2.54 ± 1.68 | |||
| Implant length | ||||
| 8 mm | 3.2 ± 1.63 | |||
| 6 mm | 1.8 ± 1.41 | χ2 = 44.52 | 2 | <0.001 |
| 5 mm | 2.14 ± 1.68 |
| Variable | No Peri-Mucositis | Peri-Mucositis | χ2 | d.f. | p Value |
|---|---|---|---|---|---|
| n (%) | n (%) | ||||
| History of periodontal disease | |||||
| no | 95 (83.33) | 19 (16.67) | 0.21 | 1 | NS (p = 0.64) |
| yes | 174 (85.29) | 30 (14.71) | |||
| Arch | |||||
| posterior mandible | 148 (79.57) | 38 (20.43) | 8.66 | 1 | <0.01 |
| posterior maxilla | 121 (91.67) | 11 (8.33) | |||
| Implant length | |||||
| 8 mm | 118 (88.72) | 15 (11.28) | 3.98 | 2 | NS (p = 0.13) |
| 6 mm | 93 (83.78) | 18 (16.22) | |||
| 5 mm | 58 (78.38) | 16 (21.62) |
| Variable | No Peri-Implantitis | Peri-Implantitis | χ2 | d.f. | p Value |
|---|---|---|---|---|---|
| n (%) | n (%) | ||||
| History of periodontal disease | |||||
| no | 111 (97.37) | 3 (2.63) | 0.15 | 1 | NS (p = 0.70) |
| yes | 200 (98.04) | 4 (1.96) | |||
| Arch | |||||
| posterior mandible | 182 (97.85) | 4 (2.15) | 0.005 | 1 | NS (p = 0.61) |
| posterior maxilla | 129 (97.73) | 3 (2.27) | |||
| Implant length | |||||
| 8 mm | 131 (98.50) | 2 (1.50) | 1.56 | 2 | NS (p = 0.49) |
| 6 mm | 109 (98.20) | 2 (1.80) | |||
| 5 mm | 71 (95.95) | 3 (4.05) |
| Variable | Success | No Success | χ2 | d.f. | p Value |
|---|---|---|---|---|---|
| n (%) | n (%) | ||||
| History of periodontal disease | |||||
| no | 92 (80.70) | 22 (19.30) | 0.34 | 1 | NS (p = 0.55) |
| yes | 170 (83.33) | 34 (16.67) | |||
| Arch | |||||
| posterior mandible | 144 (77.42) | 42 (22.58) | 7.63 | 1 | <0.01 |
| posterior maxilla | 118 (89.39) | 14 (10.61) | |||
| Implant length | |||||
| 8 mm | 116 (87.22) | 17 (12.78) | 5.46 | 2 | NS (p = 0.06) |
| 6 mm | 91 (81.98) | 20 (18.02) | |||
| 5 mm | 55 (74.32) | 19 (25.68) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lombardo, G.; Signoriello, A.; Marincola, M.; Nocini, P.F. Assessment of Peri-Implant Soft Tissues Conditions around Short and Ultra-Short Implant-Supported Single Crowns: A 3-Year Retrospective Study on Periodontally Healthy Patients and Patients with a History of Periodontal Disease. Int. J. Environ. Res. Public Health 2020, 17, 9354. https://doi.org/10.3390/ijerph17249354
Lombardo G, Signoriello A, Marincola M, Nocini PF. Assessment of Peri-Implant Soft Tissues Conditions around Short and Ultra-Short Implant-Supported Single Crowns: A 3-Year Retrospective Study on Periodontally Healthy Patients and Patients with a History of Periodontal Disease. International Journal of Environmental Research and Public Health. 2020; 17(24):9354. https://doi.org/10.3390/ijerph17249354
Chicago/Turabian StyleLombardo, Giorgio, Annarita Signoriello, Mauro Marincola, and Pier Francesco Nocini. 2020. "Assessment of Peri-Implant Soft Tissues Conditions around Short and Ultra-Short Implant-Supported Single Crowns: A 3-Year Retrospective Study on Periodontally Healthy Patients and Patients with a History of Periodontal Disease" International Journal of Environmental Research and Public Health 17, no. 24: 9354. https://doi.org/10.3390/ijerph17249354
APA StyleLombardo, G., Signoriello, A., Marincola, M., & Nocini, P. F. (2020). Assessment of Peri-Implant Soft Tissues Conditions around Short and Ultra-Short Implant-Supported Single Crowns: A 3-Year Retrospective Study on Periodontally Healthy Patients and Patients with a History of Periodontal Disease. International Journal of Environmental Research and Public Health, 17(24), 9354. https://doi.org/10.3390/ijerph17249354






