Women’s Barriers to Weight Loss, Perception of Future Diabetes Risk and Opinions of Diet Strategies Following Gestational Diabetes: An Online Survey
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants and Recruitment
2.2. Survey Development
2.3. Survey Questions
2.4. Statistics
2.5. Ethics
3. Results
3.1. Knowledge of Weight, Weight Loss, and Perception of Risk of T2DM
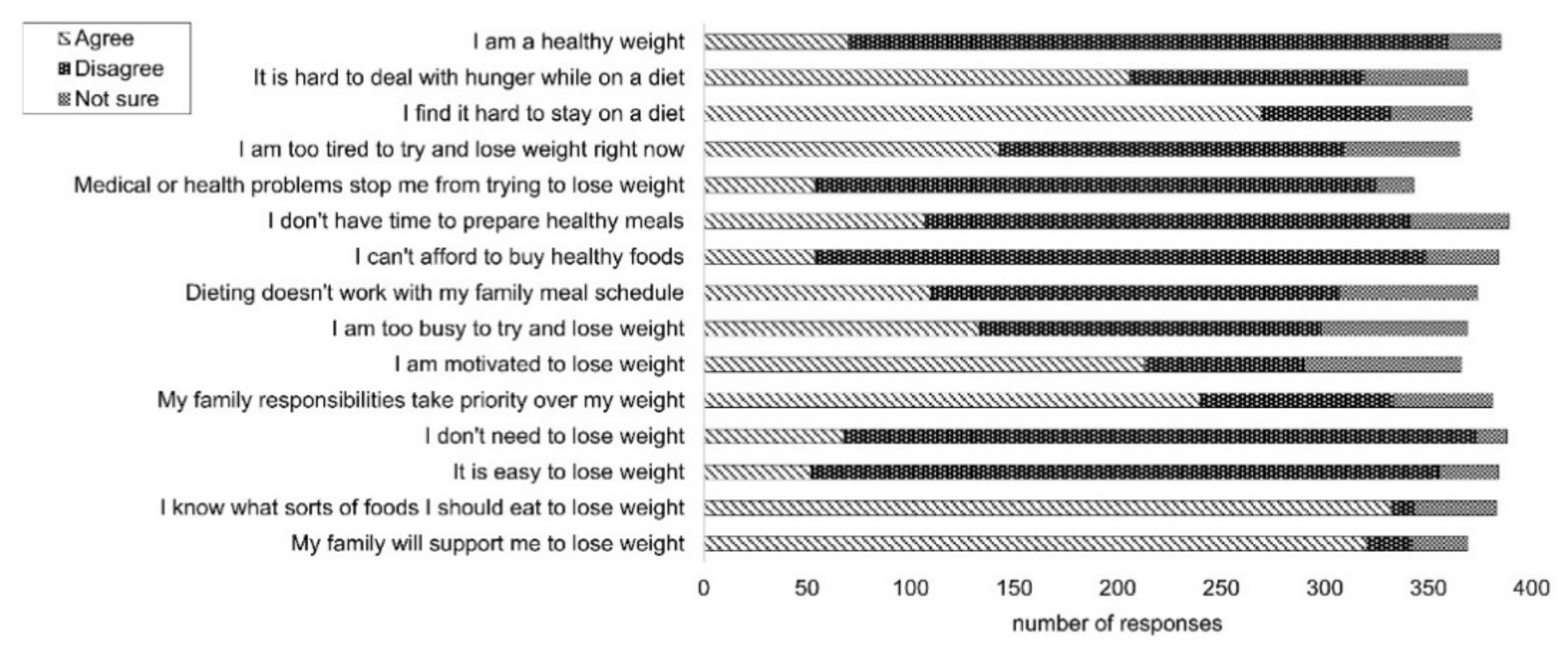
3.2. Barriers and Enablers to Weight Loss after GDM
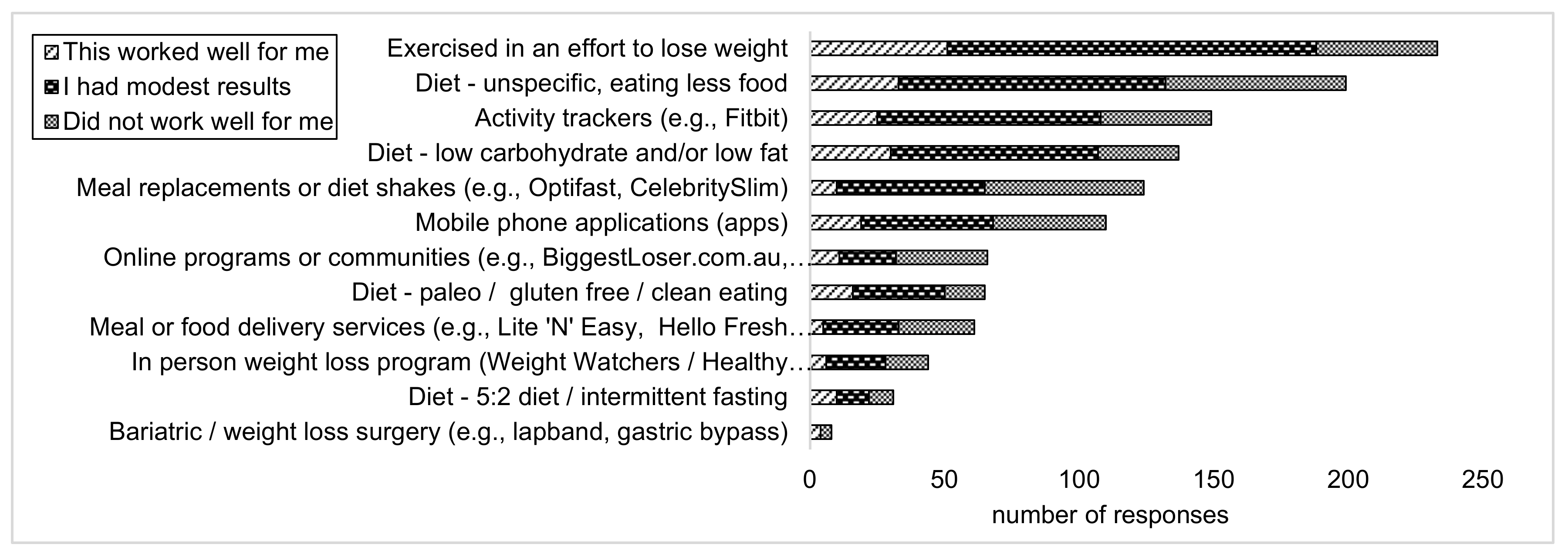
3.3. Diet Strategies
3.4. Weight Loss Services, Programs, and Information
3.5. Intermittent Fasting (the 5:2 Diet)
4. Discussion
5. Limitations
6. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Royal Australian College of General Practitioners. General Practice Management of Type 2 Diabetes: 2016–2018; RACGP: East Melbourne, VIC, Australia, 2016. [Google Scholar]
- Australian Institute of Health and Welfare. Incidence of Gestational Diabetes in Australia; [Cat. no. CVD 85]; AIHW: Canberra, ACT, Australia, 2019.
- International Diabetes Federation. IDF Diabetes Atlas 9th Edition 2019; IDF: Brussels, Belgium, 2019. [Google Scholar]
- Vounzoulaki, E.; Khunti, K.; Abner, S.C.; Tan, B.K.; Davies, M.J.; Gillies, C.L. Progression to type 2 diabetes in women with a known history of gestational diabetes: Systematic review and meta-analysis. BMJ 2020, 369, m1361. [Google Scholar] [CrossRef]
- Bellamy, L.; Casas, J.P.; Hingorani, A.D.; Williams, D. Type 2 diabetes mellitus after gestational diabetes: A systematic review and meta-analysis. Lancet 2009, 373, 1773–1779. [Google Scholar] [CrossRef]
- Kim, S.; England, L.; Wilson, H.; Bish, C.; Satten, G.; Dietz, P. Percentage of gestational diabetes mellitus attributable to overweight and obesity. Am. J. Public Health 2010, 100, 1047–1052. [Google Scholar] [CrossRef]
- Al-Lawati, J.A. Diabetes mellitus: A local and global public health emergency! Oman Med. J. 2017, 32, 177–179. [Google Scholar] [CrossRef]
- Ratner, R.E.; Christophi, C.A.; Metzger, B.E.; Dabelea, D.; Bennett, P.H.; Pi-Sunyer, X.; Fowler, S.; Kahn, S.E. Prevention of diabetes in women with a history of gestational diabetes: Effects of metformin and lifestyle interventions. J. Clin. Endocrinol. Metab. 2008, 93, 4774–4779. [Google Scholar] [CrossRef]
- Gilinsky, A.S.; Kirk, A.F.; Hughes, A.R.; Lindsay, R.S. Lifestyle interventions for type 2 diabetes prevention in women with prior gestational diabetes: A systematic review and meta-analysis of behavioural, anthropometric and metabolic outcomes. Prev. Med. Rep. 2015, 2, 448–461. [Google Scholar] [CrossRef] [PubMed]
- Lipscombe, L.L.; Banerjee, A.T.; McTavish, S.; Mukerji, G.; Lowe, J.; Ray, J.; Evans, M.; Feig, D.S. Readiness for diabetes prevention and barriers to lifestyle change in women with a history of gestational diabetes mellitus: Rationale and study design. Diabetes Res. Clin. Pract. 2014, 106, 57–66. [Google Scholar] [CrossRef] [PubMed]
- Atkins, L.; Francis, J.; Islam, R.; O’Connor, D.; Patey, A.; Ivers, N.; Foy, R.; Duncan, E.M.; Colquhoun, H.; Grimshaw, J.M.; et al. A guide to using the theoretical domains framework of behaviour change to investigate implementation problems. Implement. Sci. 2017, 12, 77. [Google Scholar] [CrossRef] [PubMed]
- Bennett, W.L.; Ennen, C.S.; Carrese, J.A.; Hill-Briggs, F.; Levine, D.M.; Nicholson, W.K.; Clark, J.M. Barriers to and facilitators of postpartum follow-up care in women with recent gestational diabetes mellitus: A qualitative study. J. Women’s Health 2011, 20, 239–245. [Google Scholar] [CrossRef] [PubMed]
- Dennison, R.A.; Ward, R.J.; Griffin, S.J.; Usher-Smith, J.A. Women’s views on lifestyle changes to reduce the risk of developing type 2 diabetes after gestational diabetes: A systematic review, qualitative synthesis and recommendations for practice. Diabet. Med. 2019, 36, 702–717. [Google Scholar] [CrossRef] [PubMed]
- Peacock, A.S.; Bogossian, F.; McIntyre, H.D.; Wilkinson, S. A review of interventions to prevent type 2 diabetes after gestational diabetes. J. Aust. Coll. Midwives 2014, 27, e7–e15. [Google Scholar] [CrossRef] [PubMed]
- Lim, S.; Hill, B.; Teede, H.J.; Moran, L.J.; O’Reilly, S. An evaluation of the impact of lifestyle interventions on body weight in postpartum women: A systematic review and meta-analysis. Obes. Rev. 2020, 21, e12990. [Google Scholar] [CrossRef] [PubMed]
- Cane, J.; O’Connor, D.; Michie, S. Validation of the theoretical domains framework for use in behaviour change and implementation research. Implement. Sci. 2012, 7, 27–37. [Google Scholar] [CrossRef] [PubMed]
- Michie, S.; Atkins, L.; West, R. The Behaviour Change Wheel: A Guide to Designing Interventions; Silverback Publishing: Sutton, UK, 2014. [Google Scholar]
- Hedman, A.S. Using the smog formula to revise a health-related document. Am. J. Health Educ. 2008, 39, 61–64. [Google Scholar] [CrossRef]
- Australian Bureau of Statistics. In Sample size calculator; Australian Bureau of Statistics, Australian Government: Canberra, ACT, Australia, 2018. Available online: https://www.abs.gov.au/websitedbs/D3310114.nsf/home/Sample+Size+Calculator (accessed on 1 March 2018).
- Cowdell, F.; Dyson, J. How is the theoretical domains framework applied to developing health behaviour interventions? A systematic search and narrative synthesis. BMC Public Health 2019, 19, 1180. [Google Scholar] [CrossRef] [PubMed]
- Morrison, M.K.; Lowe, J.M.; Collins, C.E. Perceived risk of type 2 diabetes in australian women with a recent history of gestational diabetes mellitus. Diabet. Med. 2010, 27, 882–886. [Google Scholar] [CrossRef]
- Kim, C.; McEwen, L.N.; Piette, J.D.; Goewey, J.; Ferrara, A.; Walker, E.A. Risk perception for diabetes among women with histories of gestational diabetes mellitus. Diabetes Care 2007, 30, 2281–2286. [Google Scholar] [CrossRef]
- O’Reilly, S.L. Prevention of diabetes after gestational diabetes: Better translation of nutrition and lifestyle messages needed. Healthcare 2014, 2, 468–491. [Google Scholar] [CrossRef]
- Eccles, J.; Wigfield, A. Motivational beliefs, values and goals. Annu. Rev. Psychol. 2002, 53, 109–132. [Google Scholar] [CrossRef]
- Boyle, D.I.R.; Versace, V.L.; Dunbar, J.A.; Scheil, W.; Janus, E.; Oats, J.J.N.; Skinner, T.; Shih, S.; O’Reilly, S.; Sikaris, K.; et al. Results of the first recorded evaluation of a national gestational diabetes mellitus register: Challenges in screening, registration, and follow-up for diabetes risk. PLoS ONE 2018, 13, e0200832. [Google Scholar] [CrossRef]
- McKinley, M.C.; Allen-Walker, V.; McGirr, C.; Rooney, C.; Woodside, J.V. Weight loss after pregnancy: Challenges and opportunities. Nutr. Res. Rev. 2018, 31, 225–238. [Google Scholar] [CrossRef]
- Lim, S.; Hill, B.; Pirotta, S.; O’Reilly, S.; Moran, L. What are the most effective behavioural strategies in changing postpartum women’s physical activity and healthy eating behaviours? A systematic review and meta-analysis. J. Clin. Med. 2020, 9, 237. [Google Scholar] [CrossRef] [PubMed]
- Garber, C.E. The health benefits of exercise in overweight and obese patients. Curr. Sports Med. Rep. 2019, 18, 287–291. [Google Scholar] [CrossRef] [PubMed]
- Headland, M.; Clifton, P.M.; Carter, S.; Keogh, J.B. Weight-loss outcomes: A systematic review and meta-analysis of intermittent energy restriction trials lasting a minimum of 6 months. Nutrients 2016, 8, 354. [Google Scholar] [CrossRef] [PubMed]
- Harvie, M.; Wright, C.; Pegington, M.; McMullan, D.; Mitchell, E.; Martin, B.; Cutler, R.; Evans, G.; Whiteside, S.; Maudsley, S.; et al. The effect of intermittent energy and carbohydrate restriction v. Daily energy restriction on weight loss and metabolic disease risk markers in overweight women. Br. J. Nutr. 2013, 110, 1534–1547. [Google Scholar] [CrossRef]
- Donnelly, L.S.; Shaw, R.L.; Pennington, M.; Armitage, C.J.; Evans, D.G.; Howell, A.; Harvie, M.N. ‘For me it’s about not feeling like i’m on a diet’: A thematic analysis of women’s experiences of an intermittent energy restricted diet to reduce breast cancer risk. J. Hum. Nutr. Diet. 2018, 31, 773–780. [Google Scholar] [CrossRef]
- Welton, S.; Minty, R.; O’Driscoll, T.; Willms, H.; Poirier, D.; Madden, S.; Kelly, L. Intermittent fasting and weight loss: Systematic review. Can. Fam. Physician 2020, 66, 117–125. [Google Scholar] [PubMed]
- Seimon, R.V.; Roekenes, J.A.; Zibellini, J.; Zhu, B.; Gibson, A.A.; Hills, A.P.; Wood, R.E.; King, N.A.; Byrne, N.M.; Sainsbury, A. Do intermittent diets provide physiological benefits over continuous diets for weight loss? A systematic review of clinical trials. Mol. Cell Endocrinol. 2015, 418 Pt 2, 153–172. [Google Scholar] [CrossRef]
- Maukonen, M.; Männistö, S.; Tolonen, H. A comparison of measured versus self-reported anthropometrics for assessing obesity in adults: A literature review. Scand. J. Public Health 2018, 46, 565–579. [Google Scholar] [CrossRef]

| Characteristic | All Responders |
|---|---|
| Age, y | 36.0, 8.0 |
| Weight, kg | 82, 27 |
| BMI, kg/m2 | 30.1, 9.7 |
| SEIFA *, index | 6.0, 5.0 |
| 43 (10) 27 (6) 53 (13) 40 (10) 38 (9) 54 (13) 41 (10) 63 (15) 34 (8) 29 (7) |
| Years postpartum ** y | 2.5, 3.5 |
| Years since GDM, y | 3.0, 5.0 |
| GDM managed, n (%) | |
| 248 (7) 46 (11) 135 (31) |
| Children living at home, n | 2, 1 |
| Employment, n (%) | |
| 99 (23) 180 (42) 126 (29) 24 (5) |
| Family history of diabetes, n (%) | 268 (62) |
| Lost weight gained in pregnancy, n (%) | |
| 218 (62) 177 (42) 30 (7) |
| Breastfeeding time, n (%) | |
| 40 (9) 99 (24) 46 (11) 147 (35) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gray, K.L.; McKellar, L.; O’Reilly, S.L.; Clifton, P.M.; Keogh, J.B. Women’s Barriers to Weight Loss, Perception of Future Diabetes Risk and Opinions of Diet Strategies Following Gestational Diabetes: An Online Survey. Int. J. Environ. Res. Public Health 2020, 17, 9180. https://doi.org/10.3390/ijerph17249180
Gray KL, McKellar L, O’Reilly SL, Clifton PM, Keogh JB. Women’s Barriers to Weight Loss, Perception of Future Diabetes Risk and Opinions of Diet Strategies Following Gestational Diabetes: An Online Survey. International Journal of Environmental Research and Public Health. 2020; 17(24):9180. https://doi.org/10.3390/ijerph17249180
Chicago/Turabian StyleGray, Kristy L., Lois McKellar, Sharleen L. O’Reilly, Peter M. Clifton, and Jennifer B. Keogh. 2020. "Women’s Barriers to Weight Loss, Perception of Future Diabetes Risk and Opinions of Diet Strategies Following Gestational Diabetes: An Online Survey" International Journal of Environmental Research and Public Health 17, no. 24: 9180. https://doi.org/10.3390/ijerph17249180
APA StyleGray, K. L., McKellar, L., O’Reilly, S. L., Clifton, P. M., & Keogh, J. B. (2020). Women’s Barriers to Weight Loss, Perception of Future Diabetes Risk and Opinions of Diet Strategies Following Gestational Diabetes: An Online Survey. International Journal of Environmental Research and Public Health, 17(24), 9180. https://doi.org/10.3390/ijerph17249180








