Complementary Feeding: Pitfalls for Health Outcomes
Abstract
1. Background
2. Timing of Weaning and Pitfalls for Health Outcomes
2.1. Excess Weight and Obesity
2.2. Blood Pressure
2.3. Food Preferences and Eating Behaviors
2.4. Developmental Milestones
2.5. Food Allergy
3. Macronutrients Composition of CF and Health Outcomes: How Much Is Not Too Much?
3.1. Macronutrients: Proteins
3.2. Carbohydrates
3.3. Lipids
3.4. Micronutrients
4. Mode of Feeding and Health Outcomes
4.1. Diet Diversity and Health Outcome
4.2. Responsive Feeding and Health Outcomes: Weight Gain and Obesity
4.3. Taste and Food Preferences
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Koletzko, B. The power of programming: Developmental origins of health and disease. Am. J. Clin. 2011, 94, 1747S. [Google Scholar] [CrossRef]
- Koletzko, B.; Brands, B.; Poston, L.; Godfrey, K.; Demmelmair, H. Symposium on ‘Metabolic flexibility in animal and human nutrition’ Session I: Early nutrition programming, life performance and cognitive function. Early nutrition programming of long-term health. Proc. Nutr. Soc. 2012, 71, 371–378. [Google Scholar] [CrossRef]
- Koletzko, B.; Brands, B.; Chourdakis, M.; Cramer, S.; Grote, V.; Hellmuth, C.; Kirchberg, F.; Prell, C.; Rzehak, P.; Uhl, O.; et al. The Power of Programming and the Early Nutrition project: Opportunities for health promotion by nutrition during the first thousand days of life and beyond. Ann. Nutr. Metab. 2014, 64, 187–196. [Google Scholar] [CrossRef]
- Koletzko, B. Early nutrition and its later consequences: New opportunities. Adv. Exp. Med. Biol. 2005, 569, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Singhal, A.; Lucas, A. Early origins of cardiovascular disease: Is there a unifying hypothesis? Lancet 2004, 363, 1642–1645. [Google Scholar] [CrossRef]
- D’Auria, E.; Bergamini, M.; Staiano, A.; Banderali, G.; Pendezza, E.; Penagini, F.; Zuccotti, G.V.; Peroni, D.G. Baby-led weaning: What a systematic review of the literature adds on. Ital. J. Pediatr. 2018, 44–49. [Google Scholar] [CrossRef]
- World Health Organization; UNICEF. Global Strategy for Infant and Young Child Feeding; WHO: Geneva, Switzerland, 2002; ISBN 92 4 156221 8. [Google Scholar]
- Fewtrell, M.; Bronsky, J.; Campoy, C.; Domellöf, M.; Embleton, N.; Fidler Mis, N.; Hojsak, I.; Hulst, J.M.; Indrio, F.; Lapillonne, A.; et al. Complementary feeding: A position paper by the European Society for Paediatric Gastroenterology, Hepatology, and Nutrition (ESPGHAN) Committee on nutrition. J. Pediatr. Gastroenterol. Nutr. 2017, 64, 119–132. [Google Scholar] [CrossRef]
- Scientific Advisory Committee on Nutrition. Feeding in the First Year of Life. 2018. Available online: https://www.gov.uk/government/publications/feeding-in-the-first-year-of-life-sacn-report (accessed on 23 April 2020).
- United States Department of Agriculture. Timing of Introduction of Complementary Foods and Beverage and Developmental Milestones: A Systematic Review. Available online: https://nesr.usda.gov/sites/default/files/2019-04/Timing%20of%20CFB-Developmental%20Milestones-NE..._0.pdf (accessed on 23 April 2020).
- DiMaggio, D.M.; Cox, A.; Porto, A.F. Updates in infant nutrition. Pediatr. Rev. 2017, 38, 449–462. [Google Scholar] [CrossRef] [PubMed]
- EFSA Panel in Nutrition, Novel Foods and Food Allergens (NDA). Scientific opionion on the appropriate age for introduction of complementary feeding of infants. EFSA J. 2019, 17, 5780. [Google Scholar] [CrossRef]
- Jonsdottir, O.H.; Thorsdottir, I.; Hibberd, P.L.; Fewtrell, M.S.; Wells, J.C.; Palsson, G.I.; Lucas, A.; Gunnlaugsson, G.; Kleinman, R.E. Timing of the introduction of complementary foods in infancy: A randomized controlled trial. Pediatrics 2012, 130, 1038–1345. [Google Scholar] [CrossRef]
- Cameron, S.L.; Heath, A.L.; Taylor, R.W. How feasible is Baby-led Weaning as an approach to infant feeding? A review of the evidence. Nutrients 2012, 4, 1575–1609. [Google Scholar] [CrossRef]
- Harrison, M.; Brodribb, W.; Hepworth, J. A qualitative systematic review of maternal infant feeding practices in transitioning from milk feeds to family foods. Matern. Child Nutr. 2017, 13, e12360. [Google Scholar] [CrossRef] [PubMed]
- Baldassarre, M.E.; Panza, R.; Farella, I.; Posa, D.; Capozza, M.; Mauro, A.D.; Laforgia, N. Vegetarian and vegan weaning of the infant: How common and how evidence-based? A population-based survey and narrative review. Int. J. Environ. Res. Public Health 2020, 17, 4835. [Google Scholar] [CrossRef] [PubMed]
- Schürmann, S.; Kersting, M.; Alexy, U. Vegetarian diets in children: A systematic review. Eur. J. Nutr. 2017, 56, 1797–1817. [Google Scholar] [CrossRef]
- Pearce, J.; Taylor, M.A.; Langley-Evans, S.C. Timing of the introduction of complementary feeding and risk of childhood obesity: A systematic review. Int. J. Obes. 2013, 37, 1295–1306. [Google Scholar] [CrossRef]
- Moorcroft, K.E.; Marshall, J.L.; McCormick, F.M. Association between timing of introducing solid foods and obesity in infancy and childhood: A systematic review. Matern. Child Nutr. 2011, 7, 3–26. [Google Scholar] [CrossRef]
- Rito, A.I.; Buoncristiano, M.; Spinelli, A.; Salanave, B.; Kunešová, M.; Hejgaard, T.; Solano, M.G.; Fijałkowska, A.; Sturua, L.; Hyska, J.; et al. Association between characteristics at birth, breastfeeding and obesity in 22 countries: The WHO European Childhood Obesity Surveillance Initiative–COSI 2015/2017. Obes. Facts 2019, 12, 226–243. [Google Scholar] [CrossRef] [PubMed]
- Vail, B.; Prentice, P.; Dunger, D.B.; Hughes, I.A.; Acerini, C.L.; Ong, K.K. Age at weaning and infant growth: Primary analysis and systematic review. J. Pediatr. 2015, 167, 317–324. [Google Scholar] [CrossRef] [PubMed]
- English, L.K.; Obbagy, J.E.; Wong, Y.P.; Butte, N.F.; Dewey, K.G.; Fox, M.K.; Greer, F.R. Timing of introduction of complementary foods and beverages and growth, size, and body composition: A systematic review. Am. J. Clin. Nutr. 2019, 109, 935S–955S. [Google Scholar] [CrossRef]
- Gingras, V.; Aris, I.M.; Rifas-Shiman, S.L.; Switkowski, K.M.; Oken, E.; Hivert, M.F. Timing of complementary feeding introduction and adiposity throughout childhood. Pediatrics 2019, 144, e20191320. [Google Scholar] [CrossRef] [PubMed]
- Brambilla, P.; Bedogni, G.; Pietrobelli, A.; Cianfarani, S.; Agostoni, C. Predictors of blood pressure at 7–13 years: The “new millennium baby” study. Nutr. Metab. Cardiovasc. Dis. 2016, 26, 706–712. [Google Scholar] [CrossRef] [PubMed]
- Möller, L.M.; de Hoog, M.L.; van Eijsden, M.; Gemke, R.J.; Vrijkotte, T.G. Infant nutrition in relation to eating behaviour and fruit and vegetable intake at age 5 years. Br. J. Nutr. 2013, 109, 564–571. [Google Scholar] [CrossRef] [PubMed]
- Centers for Disease Control and Prevention. Developmental Milestones. Version 5 December 2019. Available online: https://www.cdc.gov/ncbddd/actearly/milestones/index.html (accessed on 14 April 2020).
- English, L.K.; Obbagy, J.E.; Wong, Y.P.; Butte, N.F.; Dewey, K.G.; Fox, M.K.; Greer, F.R.; Krebs, N.F.; Scanlon, K.S.; Stoody, E.E. Complementary feeding and developmental milestones: A systematic review. Am. J. Clin. Nutr. 2019, 109, 879S–889S. [Google Scholar] [CrossRef] [PubMed]
- Greer, F.R.; Sicherer, S.H.; Burks, A.W. The effects of early nutritional interventions on the development of atopic disease in infants and children: The role of maternal dietary restriction, breastfeeding, hydrolyzed formulas, and timing of introduction of allergenic complementary foods. Pediatrics 2019, 143, e20190281. [Google Scholar] [CrossRef]
- Turner, P.J.; Feeney, M.; Meyer, R.; Perkin, M.R.; Fox, A.T. Implementing primary prevention of food allergy in infants: New BSACI guidance published. Clin. Exp. Allergy 2018, 48, 912–915. [Google Scholar] [CrossRef]
- Togias, A.; Cooper, S.F.; Acebal, M.L.; Assa’ad, A.; Baker, J.R.; Beck, L.A.; Block, J.; Byrd-Bredbenner, C.; Chan, E.S.; Eichenfield, L.F.; et al. Addendum guidelines for the prevention of peanut allergy in the United States: Report of the National Institute of Allergy and Infectious Diseases-sponsored expert panel. Allergy Clin. Immunol. 2017, 139, 29–44. [Google Scholar] [CrossRef]
- Du Toit, G.; Roberts, G.; Sayre, P.H.; Bahnson, H.T.; Radulovic, S.; Santos, A.F.; Broughet, H.A.; Phippard, D.; Basting, M.; Feeney, M.; et al. Randomized trial of peanut consumption in infants at risk for peanut allergy. N. Engl. J. Med. 2015, 37, 803–813. [Google Scholar] [CrossRef]
- Ierodiakonou, D.; Garcia-larsen, V.; Logan, A.; Groome, A.; Cunha, S.; Chivinge, J.; Robinson, Z.; Geoghegan, N.; Jarrold, K.; Reeves, T.; et al. Timing of allergenic food introduction to the infant diet and risk of allergic or autoimmune disease: A systematic review and meta-analysis. JAMA 2016, 316, 1181–1192. [Google Scholar] [CrossRef]
- Roduit, C.; Frei, R.; Depner, M.; Schaub, B.; Loss, G.; Genuneit, J.; Pfefferle, P.; Hyvärinen, A.; Karvonen, A.M.; Riedler, J.; et al. Increased food diversity in the first year of life is inversely associated with allergic diseases. J. Allergy Clin. Immunol. 2014, 133, 1056–1064. [Google Scholar] [CrossRef]
- Venter, C.; Maslin, K.; Holloway, J.W.; Silveira, L.J.; Fleischer, D.M.; Dean, T.; Arshad, S.H. Different measures of diet diversity during infancy and the association with childhood food allergy in a UK birth cohort study. J. Allergy Clin. Immunol. Pract. 2020, 8, 2017–2202. [Google Scholar] [CrossRef]
- Venter, C.; Brown, K.R.; Maslin, K.; Palmer, D.J. Maternal dietary intake in pregnancy and lactation and allergic disease outcomes in offspring. Pediatr. Allergy Immunol. 2017, 28, 135–143. [Google Scholar] [CrossRef] [PubMed]
- Alvisi, P.; Brusa, S.; Alboresi, S.; Amarri, S.; Bottau, P.; Cavagni, G.; Corradini, B.; Landi, L.; Loroni, L.; Marani, M.; et al. Recommendations on complementary feeding for healthy, full-term infants. Ital. J. Pediatr. 2015, 41, 36. [Google Scholar] [CrossRef]
- Koletzko, B.; Demmelmair, H.; Grote, V.; Prell, C.; Weber, M. High protein intake in young children and increased weight gain and obesity risk. Am. J. Clin. Nutr. 2016, 103, 303–304. [Google Scholar] [CrossRef] [PubMed]
- Appleton, J.; Russell, C.G.; Laws, R.; Fowler, C.; Campbell, K.; Denney-Wilson, E. Infant formula feeding practices associated with rapid weight gain: A systematic review. Matern. Child Nutr. 2018, 14, e12602. [Google Scholar] [CrossRef]
- Agostoni, C.; Grandi, F.; Giannì, M.L.; Silano, M.; Torcoletti, M.; Giovannini, M.; Riva, E. Growth patterns of breast fed and formula fed infants in the first 12 months of life: An Italian study. Arch. Dis. Child. 1999, 81, 395–399. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Dewey, K.G. Growth characteristics of breast-fed compared to formula-fed infants. Biol. Neonate 1998, 74, 94–105. [Google Scholar] [CrossRef] [PubMed]
- Bell, K.A.; Wagner, C.L.; Feldman, H.A.; Shypailo, R.J.; Belfort, M.B. Associations of infant feeding with trajectories of body composition and growth. Am. J. Clin. Nutr. 2017, 106, 491–498. [Google Scholar] [CrossRef] [PubMed]
- Horta, B.L.; Victora, C.G. Long-Term Effects of Brestfeeding. A Systematic Review; WHO: Geneva, Switzerland, 2013; ISBN 978 92 4 150530 7. [Google Scholar]
- Brown, A.; Lee, M. Breastfeeding during the first year promotes satiety responsiveness in children aged 18–24 months. Pediatr. Obes. 2012, 7, 382–390. [Google Scholar] [CrossRef] [PubMed]
- Iguacel, I.; Monje, L.; Cabero, M.J.; Aznar, L.A.M.; Samper, M.P.; Rodríguez-Palmero, M.; Rivero, M.; Rodríguez, G. Feeding patterns and growth trajectories in breast-fed and formula-fed infants during the introduction of complementary food. Nutr. Hosp. 2019, 36, 777–785. [Google Scholar] [CrossRef] [PubMed]
- Koletzko, B.; Broekaert, I.; Demmelmair, H.; Franke, J.; Hannibal, I.; Oberle, D.; Schiess, S.; Baumann, B.T.; Verwied-Jorky, S. Protein intake in the first year of life: A risk factor for later obesity? The E.U. Childhood Obesity Project. Adv. Exp. Med. Biol. 2005, 569, 69–79. [Google Scholar] [CrossRef]
- Koletzko, B.; Von Kries, R.; Closa, R.; Escribano, J.; Scaglioni, S.; Giovannini, M.; Beyer, J.; Demmelmair, H.; Gruszfeld, D.; Dobrzanska, A.; et al. Lower protein in infant formula is associated with lower weight up to age 2 y: A randomized clinical trial. Am. J. Clin. Nutr. 2009, 89, 1836–1845. [Google Scholar] [CrossRef] [PubMed]
- Patro-Gołąb, B.; Zalewski, B.M.; Polaczek, A.; Szajewska, H. Duration of breastfeeding and early growth: A systematic review of current evidence. Breastfeed. Med. 2019, 14, 218–229. [Google Scholar] [CrossRef]
- Totzauer, M.; Luque, V.; Escribano, J.; Closa-Monasterolo, R.; Verduci, E.; ReDionigi, A.; Hoyos, J.; Langhendries, J.P.; Gruszfeld, D.; Socha, P.; et al. Effect of lower versus higher protein content in infant formula through the first year on body composition from 1 to 6 years: Follow-up of a randomized clinical trial. Obesity 2018, 26, 1203–1210. [Google Scholar] [CrossRef] [PubMed]
- Pimpin, L.; Jebb, S.; Johnson, L.; Wardle, J.; Ambrosini, G.L. Dietary protein intake is associated with body mass index and weight up to 5 y of age in a prospective cohort of twins. Am. J. Clin. Nutr. 2016, 103, 389–397. [Google Scholar] [CrossRef] [PubMed]
- Hopkins, D.; Steer, C.D.; Northstone, K.; Emmett, P.M. Effects on childhood body habitus of feeding large volumes of cow or formula milk compared with breastfeeding in the latter part of infancy. Am. J. Clin. Nutr. 2015, 102, 1096–1103. [Google Scholar] [CrossRef]
- Michaelsen, K.F.; Greer, F.R. Protein needs early in life and long-term health. Am. J. Clin. Nutr. 2014, 99, 718S–722S. [Google Scholar] [CrossRef]
- Druet, C.; Stettler, N.; Sharp, S.; Simmons, R.K.; Cooper, C.; Smith, G.D.; Ekelund, U.; Lévy-Marchal, C.; Jarvelin, M.R.; Kuh, D.; et al. Prediction of childhood obesity by infancy weight gain: An individual-level meta-analysis. Paediatr. Perinat. Epidemiol. 2012, 26, 19–26. [Google Scholar] [CrossRef]
- Weng, S.F.; Redsell, S.A.; Swift, J.A.; Yang, M.; Glazebrook, C.P. Systematic review and meta-analyses of risk factors for childhood overweight identifiable during infancy. Arch. Dis. Child. 2012, 97, 1019–1026. [Google Scholar] [CrossRef]
- Leermakers, E.T.M.; van den Hooven, E.H.; Franco, O.H.; Jaddoe, V.W.V.; Moll, H.A.; Jong, J.C.K.; Voortman, T. A priori and a posteriori derived dietary patterns in infancy and cardiometabolic health in childhood: The role of body composition. Clin. Nutr. 2018, 37, 1589–1595. [Google Scholar] [CrossRef]
- Pan, L.; Li, R.; Park, S.; Galuska, D.A.; Sherry, B.; Freedman, D.S. A longitudinal analysis of sugar-sweetened beverage intake in infancy and obesity at 6 years. Pediatrics 2014, 134, S29–S35. [Google Scholar] [CrossRef]
- Grote, V.; Theurich, M.; Luque, V.; Gruszfeld, D.; Verduci, E.; Xhonneux, A.; Koletzko, B. Complementary feeding, infant growth, and obesity risk: Timing, composition, and mode of feeding. Nestlé Nutr. Inst. Workshop Ser. 2018, 89, 93–103. [Google Scholar] [CrossRef] [PubMed]
- European Food Safety Authority (EFSA). Scientific opinion on dietary reference values for carbohydrates and dietary fibre. EFSA Panel on Dietetic Products, Nutrition, and Allergies (NDA). EFSA J. 2010, 8, 1462. [Google Scholar] [CrossRef]
- Poskitt, E.M.E.; Breda, J. Complementary feeding and non communicable diseases: Current knowledge and future research needs. Nutr. Metab. Cardiovasc. Dis. 2012, 22, 819–822. [Google Scholar] [CrossRef] [PubMed]
- European Food Safety Authority (EFSA). Scientific opinion on dietary reference values for fats, including saturated fatty acids, polyunsaturated fatty acids, monounsaturated fatty acids, trans fatty acids, and cholesterol. EFSA Panel on Dietetic Products, Nutrition, and Allergies (NDA). EFSA J. 2010, 8, 1461. [Google Scholar] [CrossRef]
- Rolland-Cachera, M.F.; Deheeger, M.; Maillot, M.; Bellisle, F. Early adiposity rebound: Causes and consequences for obesity in children and adults. Int. J. Obes. 2006, 30, S7–S11. [Google Scholar] [CrossRef]
- Hooper, L.; Abdelhamid, A.; Bunn, D.; Brown, T.; Summerbell, C.D.; Skeaff, C.M. Effects of total fat intake on body weight. Cochrane Database Syst. Rev. 2015, CD011834. [Google Scholar] [CrossRef]
- Voortman, T.; Van Den Hooven, E.H.; Braun, K.V.E.; van den Broek, M.; Bramer, W.M.; Chowdhurry, R.; Francoet, O.H. Effects of polyunsaturated fatty acid intake and status during pregnancy, lac-tation, and early childhood on cardiometabolic health: A systematic review. Prog. Lipid Res. 2015, 59, 67–87. [Google Scholar] [CrossRef]
- Nyaradi, A.; Li, j.; Hickling, S.; Foster, J.; Oddy, W.H. The role of nutrition in children’s neurocognitive development, from pregnancy through childhood. Front. Hum. Neurosci. 2013, 7, 97. [Google Scholar] [CrossRef]
- European Food Safety Authority (EFSA). Scientific opinion on nutrient requirements and dietary intakes of infants and young children in the European Union. EFSA NDA Panel (EFSA Panel on Dietetic Products, Nutrition and Allergies). EFSA J. 2013, 11, 3408. [Google Scholar]
- Dube, K.; Schwartz, J.; Mueller, M.J.; Kalhoff, H.; Kersting, M. Iron intake and iron status in breastfed infants during the first year of life. Clin. Nutr. 2010, 29, 773–778. [Google Scholar] [CrossRef]
- Olaya, G.A.; Lawson, M.; Fewtrell, M.S. Efficacy and safety of new complementary feeding guidelines with an emphasis on red meat consumption: A randomized trial in Bogota, Colombia. Am. J. Clin. Nutr. 2013, 98, 983–993. [Google Scholar] [CrossRef] [PubMed]
- Dube, K.; Schwartz, J.; Mueller, M.J.; Kalhoff, H.; Kersting, M. Complementary food with low (8%) or high (12%) meat content as source of dietary iron: A double-blinded randomized controlled trial. Eur. J. Nutr. 2010, 49, 11–18. [Google Scholar] [CrossRef]
- Obbagy, J.E.; English, L.K.; Psota, T.L.; Wong, Y.P.; Butte, N.F.; Dewey, K.G.; Fox, M.K.; Greer, F.R.; Krebs, N.F.; Scanlon, K.S.; et al. Complementary feeding and micronutrient status: A systematic review. Am. J. Clin. Nutr. 2019, 109, 852S–871S. [Google Scholar] [CrossRef] [PubMed]
- Ackland, M.L.; Michalczyk, A.A. Zinc and infant nutrition. Arch. Biochem. Biophys. 2016, 611, 51–57. [Google Scholar] [CrossRef]
- Roohani, N.; Hurrell, R.; Kelishadi, R.; Schulin, R. Zinc and its importance for human health: An integrative review. J. Res. Med. Sci. 2013, 18, 144–157. [Google Scholar] [PubMed]
- Krebs, N.F.; Westcott, J.E.; Butler, N.; Robinson, C.; Bell, M.; Hambidge, K.M. Meat as a first complementary food for breastfed infants: Feasibility and impact on zinc intake and status. J. Pediatr. Gastroenterol. Nutr. 2006, 42, 207–214. [Google Scholar] [CrossRef] [PubMed]
- Villarroel, P.; Villalobos, E.; Reyes, M.; Cifuentes, M. Calcium, obesity, and the role of the calcium-sensing receptor. Nutr. Rev. 2014, 72, 627–637. [Google Scholar] [CrossRef]
- Martini, L.; Pecoraro, L.; Salvottini, C.; Piacentini, G.; Atkinson, R.; Pietrobelli, A.I. Appropriate and inappropriate vitamin supplementation in children. J. Nutr. Sci. 2020, 9, e20. [Google Scholar] [CrossRef]
- Wiseman, E.M.; Bar-El Dadon, S.; Reifen, R. The vicious cycle of vitamin a deficiency: A review. Crit. Rev. Food Sci. Nutr. 2017, 57, 3703–3714. [Google Scholar] [CrossRef]
- Ssentongo, P.; Djibril, M.B.; Ssentongo, A.E.; Fronterre, C.; Whalen, A.; Yang, Y.; Ericson, Y.E.; Chinchilli, V.M. Association of vitamin A deficiency with early childhood stunting in Uganda: A population-based cross-sectional study. PLoS ONE 2020, 15, e0233615. [Google Scholar] [CrossRef]
- Cao, J.; Wei, X.; Tang, X.; Jiang, H.; Fan, Z.; Yu, Q.; Chen, J.; Liu, Y.; Li, T. Effects of egg and vitamin A supplementation on hemoglobin, retinol status and physical growth levels of primary and middle school students in Chongqing, China. Asia Pac. J. Clin. Nutr. 2013, 22, 214–221. [Google Scholar] [CrossRef] [PubMed]
- Azaïs-Braesco, V.; Pascal, G. Vitamin A in pregnancy: Requirements and safety limits. Am. J. Clin. Nutr. 2000, 71, 1325S–1333S. [Google Scholar] [CrossRef] [PubMed]
- Byrne, S.M.; Blaner, W.S. Retinol and retinyl esters: Biochemistry and physiology. J. Lipid Res. 2013, 54, 1731–1743. [Google Scholar] [CrossRef] [PubMed]
- SINU Società Italiana di Nutrizione Umana. LARN: Livelli di Assunzione Italiana, Nutrienti ed Energia per la Popolazione (Italian Intake Levels, Nutrients and Energy for the Population); SICS: Rome, Italy, 2014; ISBN 8890685220. [Google Scholar]
- Imdad, A.; Mayo-Wilson, E.; Herzer, K.; Bhutta, Z.A. Vitamin A supplementation for preventing morbidity and mortality in children from six months to five years of age. Cochrane Database Syst. Rev. 2017, 11, CD008524. [Google Scholar] [CrossRef]
- Grotto, I.; Mimouni, M.; Gdalevich, M.; Mimouni, D. Vitamin A supplementation and childhood morbidity from diarrhea and respiratory infections: A meta-analysis. J. Pediatr. 2003, 142, 297–304. [Google Scholar] [CrossRef]
- Strazzullo, P.; Campanozzi, A.; Avallone, S. Does salt intake in the first two years of life affect the development of cardiovascular disorders in adulthood? Nutr. Metab. Cardiovasc. Dis. 2012, 22, 787–792. [Google Scholar] [CrossRef]
- Guardamagna, O.; Abello, F.; Cagliero, P.; Lughetti, L. Impact of nutrition since early life on cardiovascular prevention. Ital. J. Pediatr. 2012, 38, 73. [Google Scholar] [CrossRef]
- Koletzko, B.; Godfrey, K.M.; Poston, L.; Szajewska, H.; van Goudoever, J.B.; de Waard, M.; Brands, B.; Grivell, R.M.; Deussen, A.R.; Dodd, J.M.; et al. Nutrition during pregnancy, lactation and early childhood and its implications for maternal and long-term child health: The early nutrition project recommendations. Ann. Nutr. Metab. 2019, 74, 93–106. [Google Scholar] [CrossRef]
- Pan American Health Organization; World Health Organization. Guiding Principles for Complementary Feeding of the Breastfed Child; Division of Health Promotion and Protection Food and Nutrition Program: Washington, DC, USA, 2003. [Google Scholar]
- Moursi, M.M.; Arimond, M.; Dewey, K.G.; Treche, S.; Ruel, M.T.; Delpeuch, F. Dietary diversity is a good predictor of the micronutrient density of the diet of 6- to 23-month-old children in Madagascar. J. Nutr. 2008, 138, 2448–2453. [Google Scholar] [CrossRef]
- National Health and Medical Research Council. Literature Review: Infant Feeding Guidelines; National Health and Medical Research Council: Canberra, Australia, 2012; ISBN 1864965762. [Google Scholar]
- Morison, B.J.; Heath, A.M.; Haszard, J.J.; Hein, K.; Fleming, E.A.; Daniels, L.; Erickson, E.W.; Fangupo, L.J.; Wheeler, B.J.; Taylor, B.J.; et al. Impact of a modified version of baby-led weaning on dietary variety and food preferences in infants. Nutrients 2018, 10, 1092. [Google Scholar] [CrossRef]
- Arimond, M.; Ruel, M.T. Dietary diversity is associated with child nutritional status: Evidence from 11 demographic and health surveys. J. Nutr. 2004, 134, 2579–2585. [Google Scholar] [CrossRef] [PubMed]
- Hausner, H.; Nicklaus, S.; Issanchou, S.; Mølgaard, C.; Møller, P. Breastfeeding facilitates acceptance of a novel dietary flavour compound. Clin. Nutr. 2010, 29, 141–148. [Google Scholar] [CrossRef] [PubMed]
- Mennella, J.A. Ontogeny of taste preferences: Basic biology and implications for health. Am. Clin. Nutr. 2014, 99, 704S–711S. [Google Scholar] [CrossRef] [PubMed]
- Byrne, R.; Magarey, A.; Daniels, L. Food and beverage intake in Australian children aged 12–16 months participating in the NOURISH and SAIDI studies. Aust. N. Z. J. Public Health 2014, 38, 326–331. [Google Scholar] [CrossRef]
- Byrne, R.; Yeo, M.E.J.; Mallan, K.; Magarey, A.; Daniels, L. Is higher formula intake and limited dietary diversity in Australian children at 14 months of age associated with dietary quality at 24 months? Appetite 2018, 120, 240–245. [Google Scholar] [CrossRef]
- Stein, A.D. 90th Anniversary Commentary: Dietary diversity is the cornerstone of good nutrition. J. Nutr. 2018, 148, 1683–1685. [Google Scholar] [CrossRef]
- D’Auria, E.; Pendezza, E.; Zuccotti, G.V. Personalized nutrition in food allergy: Tips for clinical practice. Front. Pediatr. 2020, 8, 113. [Google Scholar] [CrossRef]
- Agostoni, C. Docosahexaenoic acid (DHA): From the maternal-foetal dyad to the complementary feeding period. Early Hum. Dev. 2010, 86, 3–6. [Google Scholar] [CrossRef]
- Mok, E.; Vanstone, C.A.; Gallo, S.; Li, P.; Constantin, E.; Weiler, H.A. Diet diversity, growth and adiposity in healthy breastfed infants fed homemade complementary foods. Int. J. Obes. 2017, 41, 776–782. [Google Scholar] [CrossRef]
- Black, M.M.; Hurley, K.M. Responsive feeding: Strategies to promote healthy mealtime interactions. Nestle Nutr. Inst. Workshop Ser. 2017, 87, 153–165. [Google Scholar] [CrossRef]
- Black, M.M.; Aboud, F.E. Responsive feeding is embedded in a theoretical framework of responsive parenting. J. Nutr. 2011, 141, 490–494. [Google Scholar] [CrossRef] [PubMed]
- Hodges, E.A.; Johnson, S.L.; Hughes, S.O.; Hopkinson, J.M.; Butte, N.F.; Fisher, J.O. Development of the responsiveness to child feeding cues scale. Appetite 2013, 65, 210–219. [Google Scholar] [CrossRef] [PubMed]
- Costanzo, P.R.; Woody, E.Z. Domain-specific parenting styles and their impact on the child’s development of particular deviance: The example of obesity proneness. J. Soc. Clin. Psychol. 1985, 3, 425–445. [Google Scholar] [CrossRef]
- DiSantis, K.I.; Hodges, E.A.; Johnson, S.L.; Fisher, J.O. The role of responsive feeding in overweight during infancy and toddlerhood: A systematic review. Int. J. Obes. 2011, 35, 480–492. [Google Scholar] [CrossRef]
- Daniels, L.A. Feeding practices and parenting: A pathway to child health and family happiness. Ann. Nutr. Metab. 2019, 74, 29–42. [Google Scholar] [CrossRef] [PubMed]
- Were, F.N.; Lifschitzb, C. Complementary feeding: Beyond nutrition. Ann. Nutr. Metab. 2018, 73, 20–25. [Google Scholar] [CrossRef] [PubMed]
- Li, R.; Scanlon, K.S.; May, A.; Rose, C.; Birch, L. Bottle-feeding practices during early infancy and eating behaviors at 6 years of age. Pediatrics 2014, 134, S70–S77. [Google Scholar] [CrossRef] [PubMed]
- Paul, I.M.; Savage, J.S.; Anzman, S.L.; Beiler, J.S.; Marini, M.E.; Stokes, J.L.; Birch, L.L. Preventing obesity during Infancy: A pilot study. Obesity 2011, 19, 353–361. [Google Scholar] [CrossRef]
- Daniels, L.A.; Mallan, K.M.; Nicholson, J.M.; Thorpe, K.; Nambiar, S.; Mauch, C.E.; Magarey, A. An early feeding practices intervention for obesity prevention. Pediatrics 2015, 136, e40–e49. [Google Scholar] [CrossRef] [PubMed]
- Daniels, L.A.; Mallan, K.M.; Battistutta, D.; Nicholson, J.M.; Meedeniya, J.E.; Bayer, J.K.; Magarey, A. Child eating behavior outcomes of an early feeding intervention to reduce risk indicators for child obesity: The NOURISH RCT. Obesity 2014, 22, e104–e111. [Google Scholar] [CrossRef]
- Magarey, A.; Mauch, C.; Mallan, K.; Perry, R.; Elovaris, R.; Meedeniya, J.; Byrne, R.; Daniels, L. Child dietary and eating behavior outcomes up to 3.5 years after an early feeding intervention: The NOURISH RCT. Obesity 2016, 24, 1537–1545. [Google Scholar] [CrossRef]
- Hohman, E.E.; Paul, I.M.; Birch, L.L.; Savage, J.S. INSIGHT responsive parenting intervention is associated with healthier patterns of dietary exposures in infants. Obesity 2017, 25, 185–191. [Google Scholar] [CrossRef] [PubMed]
- Savage, J.S.; Birch, L.L.; Marini, M.; Anzman-Frasca, S.; Paul, I.M. Effect of the INSIGHT responsive parenting intervention on rapid infant weight gain and overweight status at age 1 year: A randomized clinical trial. JAMA Pediatr. 2016, 170, 742–749. [Google Scholar] [CrossRef] [PubMed]
- Paul, I.M.; Savage, J.S.; Anzman-Frasca, S.; Marini, M.E.; Beiler, J.S.; Hess, L.B.; Loken, E.; Birch, L.L. Effect of a responsive parenting educational intervention on childhood weight outcomes at 3 years of age: The INSIGHT randomized clinical trial. JAMA 2018, 320, 461–468. [Google Scholar] [CrossRef]
- Redsell, S.A.; Edmonds, B.; Swift, J.A.; Siriwardena, A.N.; Weng, S.; Nathan, D.; Glazebrook, C. Systematic review of randomised controlled trials of interventions that aim to reduce the risk, either directly or indirectly, of overweight and obesity in infancy and early childhood. Matern. Child Nutr. 2016, 12, 24–38. [Google Scholar] [CrossRef]
- Hurley, K.M.; Cross, M.B.; Hughes, S.O. A systematic review of responsive feeding and child obesity in high-income countries. J. Nutr. 2011, 141, 495–501. [Google Scholar] [CrossRef] [PubMed]
- Birch, L.L. Development of food preferences. Annu. Rev. Nutr. 1999, 19, 41–62. [Google Scholar] [CrossRef]
- Fidler, M.N.; Braegger, C.; Bronsky, J.; Campoy, C.; Domellöf, M.; Embleton, N.; Hojsak, I.; Hulst, J.; Indrio, F.; Lapillonne, A.; et al. Sugar in infants, children and adolescents: A Position paper of the european society for paediatric gastroenterology, hepatology and nutrition committee on nutrition. JPGN 2017, 65, 681–696. [Google Scholar] [CrossRef]
- Mennella, J.A.; Beauchamp, G.K. Maternal diet alters the sensory qualqualities of human milk and the nursling’s behavior. Pediatrics 1991, 88, 737–744. [Google Scholar]
- Nicklaus, S. Complementary feeding strategies to facilitate acceptance of fruits and vegetables: A narrative review of the literature. Int. J. Environ. Res. Public Health 2016, 13, 1160. [Google Scholar] [CrossRef]
- Remy, E.; Issanchou, S.; Chabanet, C.; Nicklaus, S. Repeated exposure of infants at complementary feeding to a vegetable puree increases acceptance as effectively as flavor-flavor learning and more effectively than flavor-nutrient learning. J. Nutr. 2013, 143, 1194–1200. [Google Scholar] [CrossRef]
- Nekitsing, C.; Hetherington, M.M.; Blundell-Birtill, P. Developing healthy food preferences in preschool children through taste exposure, sensory learning, and nutrition education. Curr. Obes. Rep. 2018, 7, 60–67. [Google Scholar] [CrossRef] [PubMed]
- Beauchamp, G.K.; Moran, M. Dietary experience and sweet taste preference in human infants. Appetite 1982, 3, 139–152. [Google Scholar] [CrossRef]
- Acceptance of sweet and salty tastes in 2-year-old children. Appetite 1984, 5, 291–305. [CrossRef]
- Stein, L.J.; Cowart, B.J.; Beauchamp, G.K. The development of salty taste acceptance is related to dietary experience in human infants: A prospective study. Am. J. Clin. Nutr. 2012, 95, 123–129. [Google Scholar] [CrossRef] [PubMed]
- Switkowski, K.M.; Gingras, V.; Rifas-Shiman, S.L.; Oken, E. Patterns of complementary feeding behaviors predict diet quality in early childhood. Nutrients 2020, 12, 810. [Google Scholar] [CrossRef] [PubMed]
- Forestell, C.A. Flavor perception and preference development in human infants. Ann. Nutr. Metab. 2017, 70, 17–25. [Google Scholar] [CrossRef] [PubMed]
- Mennella, J.A.; Nicklaus, S.; Jagolino, A.L.; Yourshaw, L.M. Variety is the spice of life: Strategies for promoting fruit and vegetable acceptance during infancy. Physiol. Behav. 2008, 94, 29–38. [Google Scholar] [CrossRef] [PubMed]
- Gerrish, C.J.; Mennella, J.A. Flavor variety enhances food acceptance in formula-fed infants. Am. J. Clin. Nutr. 2001, 73, 1080–1085. [Google Scholar] [CrossRef]
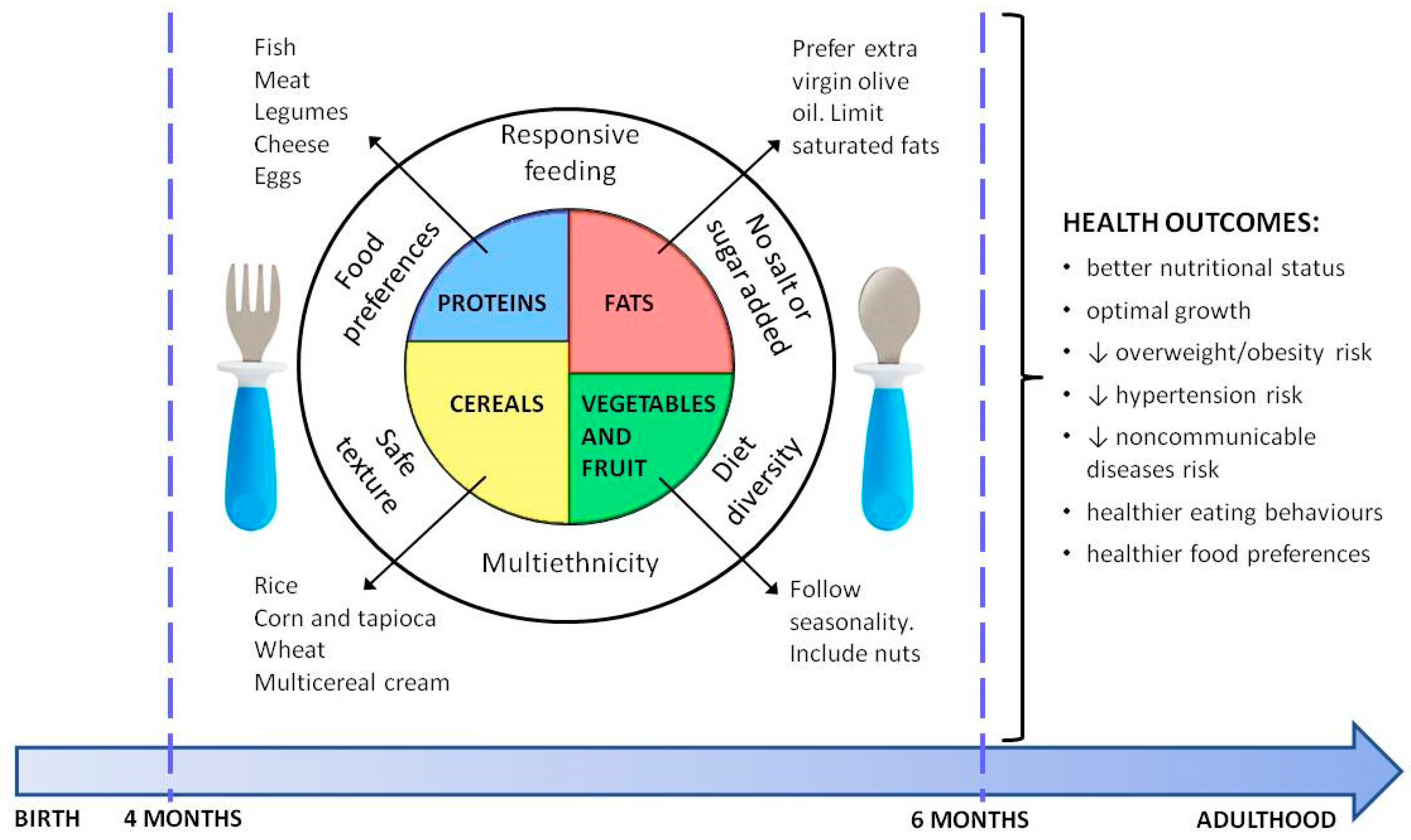
| Practical Tips for Complementary Feeding |
|---|
|
| Examples of Portion Sizes during the Complementary Feeding Phase | ||
|---|---|---|
| 6 Months | 12 Months | |
| Cereals | Cereal creams (rice, corn and tapioca, wheat, multi-cereal cream)20 g | Baby pasta 25 g Rice 25 g Couscous 25 g |
| Homogenized meat | 40 g (half a jar) | 80 g (a jar) |
| Freeze-dried meat | 5 g | 10 g |
| Fresh meat | 15 g | 30 g |
| Homogenized legumes | 40 g (half a jar) | 80 g (a jar) |
| Dry decorticated legumes | 10 g | 15 g |
| Fresh legumes | 25 g | 40 g |
| Homogenized fish | 40 g (half a jar) | 80 g (a jar) |
| Fresh fish | 20 g | 30 g |
| Fresh cheese | 20 g | 30 g |
| Egg | 25 g (half an egg) | 50 g (an egg) |
| Seasonal vegetables | 20 g | 30 g |
| Extra virgin olive oil (during the day) | 10 g | 20 g |
| Vegetable broth (no added salt) | 160–180 mL | |
| Fresh fruit | 80 g | 80 g |
| Research Areas Regarding the Complementary Feeding Period |
|---|
|
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
D’Auria, E.; Borsani, B.; Pendezza, E.; Bosetti, A.; Paradiso, L.; Zuccotti, G.V.; Verduci, E. Complementary Feeding: Pitfalls for Health Outcomes. Int. J. Environ. Res. Public Health 2020, 17, 7931. https://doi.org/10.3390/ijerph17217931
D’Auria E, Borsani B, Pendezza E, Bosetti A, Paradiso L, Zuccotti GV, Verduci E. Complementary Feeding: Pitfalls for Health Outcomes. International Journal of Environmental Research and Public Health. 2020; 17(21):7931. https://doi.org/10.3390/ijerph17217931
Chicago/Turabian StyleD’Auria, Enza, Barbara Borsani, Erica Pendezza, Alessandra Bosetti, Laura Paradiso, Gian Vincenzo Zuccotti, and Elvira Verduci. 2020. "Complementary Feeding: Pitfalls for Health Outcomes" International Journal of Environmental Research and Public Health 17, no. 21: 7931. https://doi.org/10.3390/ijerph17217931
APA StyleD’Auria, E., Borsani, B., Pendezza, E., Bosetti, A., Paradiso, L., Zuccotti, G. V., & Verduci, E. (2020). Complementary Feeding: Pitfalls for Health Outcomes. International Journal of Environmental Research and Public Health, 17(21), 7931. https://doi.org/10.3390/ijerph17217931







